Empagliflozin and Progression of Kidney Disease in Type 2 Diabetes
|
|
|
- Ashley Adams
- 6 years ago
- Views:
Transcription
1 The new england journal of medicine Original Article and Progression of Kidney Disease in Type 2 Diabetes Christoph Wanner, M.D., Silvio E. Inzucchi, M.D., John M. Lachin, Sc.D., David Fitchett, M.D., Maximilian von Eynatten, M.D., Michaela Mattheus, Dipl. Biomath., Odd Erik Johansen, M.D., Ph.D., Hans J. Woerle, M.D., Uli C. Broedl, M.D., and Bernard Zinman, M.D., for the EMPA-REG OUTCOME Investigators* ABSTRACT BACKGROUND Diabetes confers an increased risk of adverse cardiovascular and renal events. In the EMPA-REG OUTCOME trial, empagliflozin, a sodium glucose cotransporter 2 inhibitor, reduced the risk of major adverse cardiovascular events in patients with type 2 diabetes at high risk for cardiovascular events. We wanted to determine the long-term renal effects of empagliflozin, an analysis that was a prespecified component of the secondary microvascular outcome of that trial. METHODS We randomly assigned patients with type 2 diabetes and an estimated glomerular filtration rate of at least 30 ml per minute per 1.73 m 2 of body-surface area to receive either empagliflozin (at a dose of 10 mg or 25 mg) or placebo once daily. Prespecified renal outcomes included incident or worsening nephropathy (progression to macroalbuminuria, doubling of the serum creatinine level, initiation of renal-replacement therapy, or death from renal disease) and incident albuminuria. RESULTS Incident or worsening nephropathy occurred in 525 of 4124 patients (12.7%) in the empagliflozin group and in 388 of 2061 (18.8%) in the placebo group (hazard ratio in the empagliflozin group, 0.61; 95% confidence interval, 0.53 to 0.70; P<0.001). Doubling of the serum creatinine level occurred in 70 of 4645 patients (1.5%) in the empagliflozin group and in 60 of 2323 (2.6%) in the placebo group, a significant relative risk reduction of 44%. Renal-replacement therapy was initiated in 13 of 4687 patients (0.3%) in the empagliflozin group and in 14 of 2333 patients (0.6%) in the placebo group, representing a 55% lower relative risk in the empagliflozin group. There was no significant between-group difference in the rate of incident albuminuria. The adverse-event profile of empagliflozin in patients with impaired kidney function at baseline was similar to that reported in the overall trial population. From the Department of Medicine, Division of Nephrology, Würzburg University Clinic, Würzburg (C.W.), and Boehringer Ingelheim Pharma, Ingelheim (M.E., M.M., H.J.W., U.C.B.) both in Germany; the Section of Endocrinology, Yale University School of Medicine, New Haven, CT (S.E.I.); the Biostatistics Center, George Washington University, Rockville, MD (J.M.L.); the Divisions of Cardiology (D.F.) and Endocrinology (B.Z.), University of Toronto, and the Lunenfeld Tanenbaum Research Institute, Mount Sinai Hospital (B.Z.) both in Toronto; and Boehringer Ingelheim Norway, Asker, Norway (O.E.J.). Address reprint requests to Dr. Wanner at the University Clinic, Oberdürrbacherstr. 6, D Würzburg, Germany, or at wanner_c@ukw.de. * A complete list of investigators in the EMPA-REG OUTCOME trial is provided in the Supplementary Appendix, available at NEJM.org. This article was published on June 14, 2016, at NEJM.org. N Engl J Med 2016;375: DOI: /NEJMoa Copyright 2016 Massachusetts Medical Society. CONCLUSIONS In patients with type 2 diabetes at high cardiovascular risk, empagliflozin was associated with slower progression of kidney disease and lower rates of clinically relevant renal events than was placebo when added to standard care. (Funded by the Boehringer Ingelheim and Eli Lilly and Company Diabetes Alliance; EMPA-REG OUTCOME ClinicalTrials.gov number, NCT ) n engl j med 375;4 nejm.org July 28,
2 The new england journal of medicine Type 2 diabetes is a major risk factor for macrovascular and microvascular disease. 1 Kidney disease develops in approximately 35% of patients with type 2 diabetes 2 and is associated with increased mortality. 3 Intensive glucose-lowering strategies have been shown to reduce surrogate markers of renal complications in patients with type 2 diabetes; however, evidence for improvement in advanced renal complications is limited. 4-8 Thus, despite optimized glucose control and the use of single-agent blockade of the renin angiotensin aldosterone system (RAAS), patients with type 2 diabetes remain at increased risk for death and complications from cardiorenal causes. 9,10, a selective sodium glucose cotransporter 2 inhibitor, reduces hyperglycemia in patients with type 2 diabetes by reducing the renal reabsorption of glucose, thereby increasing urinary glucose excretion. 11 The use of empagliflozin has been associated with a lowering of glycated hemoglobin levels in patients with type 2 diabetes, including those with stage 2 or 3a chronic kidney disease, and with reductions in weight and blood pressure, without increases in heart rate has been shown to reduce intraglomerular pressure and improve hyperfiltration in patients with type 1 diabetes, 20,21 and it has been suggested that these effects may translate into improved renal outcomes. 22 However, concern has been raised that sodium glucose cotransporter 2 inhibitors may be associated with long-term adverse renal effects. In the recent EMPA-REG OUTCOME trial, 23 the primary goal was to assess cardiovascular outcomes. Here we report the results of a prespecified secondary objective of that trial, which was to examine the effects of empagliflozin on microvascular outcomes and, in particular, progression of kidney disease in patients with type 2 diabetes at high risk for cardiovascular events. Methods Trial Design and Oversight The design and methods of the EMPA-REG OUTCOME trial have been described previously. 24 In addition, the trial protocol is available with the full text of this article at NEJM.org. Briefly, the study population included patients who had type 2 diabetes, established cardiovascular disease, and an estimated glomerular filtration rate (egfr) of at least 30 ml per minute per 1.73 m 2 of body-surface area, according to the four-variable Modification of Diet in Renal Disease (MDRD) formula. Patients were randomly assigned to receive either empagliflozin (at a dose of 10 mg or 25 mg) or placebo once daily in addition to standard care. All the authors were involved in the trial design and had access to the data, which were gathered and analyzed by Boehringer Ingelheim, one of the trial sponsors. Medical writing assistance was provided by FleishmanHillard Fishburn, with funding from Boehringer Ingelheim. All the authors vouch for the accuracy and completeness of the data analyses and for the fidelity of the trial to the protocol. The first and fifth authors wrote the first draft of the manuscript. All the authors submitted revisions and made the decision to submit the manuscript for publication. Primary and Key Secondary Cardiovascular Outcomes The primary outcome of the EMPA-REG OUT- COME trial was a composite of three major adverse cardiovascular events (3-point MACE), which was defined as the first occurrence of death from cardiovascular causes, nonfatal myocardial infarction, or nonfatal stroke. The key secondary outcome was a composite of the primary outcome plus hospitalization for unstable angina (4-point MACE). Microvascular and Renal Outcomes A secondary outcome of the EMPA-REG OUT- COME trial was a composite microvascular outcome that included the first occurrence of any of the following: the initiation of retinal photocoagulation, vitreous hemorrhage, diabetes-related blindness, or incident or worsening nephropathy. In this report, we focus on the results of the renal microvascular outcomes, as prespecified in the statistical analysis plan (available at NEJM.org). The first renal microvascular outcome was incident or worsening nephropathy, defined as progression to macroalbuminuria (urinary albuminto-creatinine ratio, >300 mg of albumin per gram of creatinine); a doubling of the serum creatinine level, accompanied by an egfr of 45 ml per minute per 1.73 m 2, as calculated by the MDRD formula; the initiation of renal-replacement therapy; or death from renal disease. Other prespecified renal microvascular outcomes were a composite of incident or worsening nephropathy or death from cardiovascular causes, 324 n engl j med 375;4 nejm.org July 28, 2016
3 and Kidney Disease in Type 2 Diabetes the individual components of incident or worsening nephropathy, and incident albuminuria (urinary albumin-to-creatinine ratio, 30) in patients with a normal albumin level (urinary albumin-to-creatinine ratio, <30) at baseline. We conducted post hoc analyses in a subgroup of patients with prevalent kidney disease (defined as an egfr of 59 ml per minute per 1.73 m 2 or less, as calculated by the MDRD formula, or macroalbuminuria) at baseline. In addition, we performed post hoc analyses of a composite of a doubling of the serum creatinine level, the initiation of renal-replacement therapy, or death from renal disease. Safety and Laboratory Assessments We performed assessments of safety and adverseevent profiles, as described previously. 24 We evaluated the incidence of acute renal failure using the narrow standardized Medical Dictionary for Regulatory Activities (MedDRA) query, which included the preferred term acute kidney injury. We also evaluated the incidence of hyperkalemia using two MedDRA preferred terms (hyperkalemia and increased blood potassium). Serum creatinine and urinary albumin in spot urine samples obtained during regular study visits were measured in central laboratories with the use of standardized procedures. Events that were consistent with changes in the albuminuria category were captured if any laboratory assessment during the trial fulfilled the given criteria on one occasion. We used the MDRD formula to assess the egfr at baseline. 25 For prespecified assessments of renal function over time, we used the creatinine equation developed by the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI). 26 Statistical Analysis We used a modified intention-to-treat approach to perform analyses in patients who had received at least one dose of a study drug. All analyses were performed at the nominal alpha level of 0.05 without correction for multiple hypothesis testing. No formal power calculations were performed a priori for microvascular outcomes. The trial protocol specified that the outcomes of incident or worsening nephropathy (and incident or worsening nephropathy or cardiovascular death) would be analyzed in treated patients who did not have macroalbuminuria at baseline, who had available measurements of serum creatinine at baseline and after baseline, and who had postbaseline measurements of the urinary albumin-to-creatinine ratio (unless patients who did not fulfill these criteria had at least one of the other components of the composite renal outcome). A post hoc sensitivity analysis included all treated patients. Data from patients who did not have an event were censored on the last day they were known to be free of the outcome. We used a Cox proportional-hazards model to assess between-group differences in the risk of an outcome after adjustment for study group, age, sex, baseline body-mass index, baseline glycated hemoglobin level, baseline egfr, and region. We also performed subgroup analyses that included additional factors for subgroup and for interaction between the study group and subgroup. Prespecified analyses included comparisons of the pooled empagliflozin doses (10 mg and 25 mg) and the individual doses versus placebo. A mixed-model, repeated-measures analysis was used to evaluate changes in the egfr over time and included the glycated hemoglobin level and egfr (according to CKD-EPI criteria) at baseline as linear covariates and region, baseline body-mass index, the last week a patient could have had an egfr measurement, study group, visit, interaction between visit and study group, interaction between the baseline glycated hemoglobin level and visit, and interaction between the baseline egfr and visit as fixed effects. We used a random-intercept and time-coefficient model to assess differences between the study groups in the average rate of change in the egfr for prespecified time periods, with study group, baseline body-mass index, and region as fixed classification effects and baseline glycated hemoglobin level, time, and interaction between the study group and time as linear covariates. Intercepts and slopes over time were allowed to vary randomly between patients by including the patient and time as random effects. Results Patients A total of 7020 patients at 590 sites in 42 countries received at least one dose of a study drug. According to the trial design, more than 99% of the patients had established cardiovascular disease. At baseline, the egfr was 45 to 59 ml per minute per 1.73 m 2 in 17.8% of the patients and n engl j med 375;4 nejm.org July 28,
4 The new england journal of medicine 30 to 44 ml per minute per 1.73 m 2 in 7.7%; 28.7% had microalbuminuria, and 11.0% had macroalbuminuria. In total, 80.7% of the patients were taking angiotensin-converting enzyme inhibitors or angiotensin-receptor blockers at baseline. The patients were categorized according to whether the egfr was 60 ml per minute per 1.73 m 2 or more or 59 ml per minute per 1.73 m 2 or less at baseline. The baseline characteristics of the patients were generally similar in the two study groups (Table 1; and Table S1 in the Supplementary Appendix, available at NEJM.org). A higher percentage of patients in the placebo group received additional cardiovascular medications during the trial (Table S2 in the Supplementary Appendix). The median duration of treatment was 2.6 years, and the median observation time was 3.1 years. Cardiovascular Outcomes The primary outcome that was reported previously showed a significantly lower risk of 3-point MACE in the pooled empagliflozin group than in the placebo group, a difference that was driven by a lower rate of death from cardiovascular causes. 23 Prespecified secondary and additional cardiovascular outcomes that were reported previously included the 4-point MACE (and components of this composite outcome), hospitalization for heart failure, and death from any cause. 23 Microvascular Outcome The prespecified composite microvascular outcome in the overall trial population occurred in 577 of 4132 patients (14.0%) in the empagliflozin group and in 424 of 2068 patients (20.5%) in the placebo group, a significant relative risk reduction of 38% (Table S3 in the Supplementary Appendix). Because the overall result for this composite microvascular outcome was driven entirely by the renal component, we have focused on renal outcomes in this report. Renal Outcomes An assessment of renal outcomes was a prespecified objective of the trial, and outcomes were defined in a secondary statistical analysis plan. Incident or worsening nephropathy occurred in 525 of 4124 patients (12.7%) in the empagliflozin group and in 388 of 2061 patients (18.8%) in the placebo group, a significant relative risk reduction of 39% (Fig. 1A and Fig. 2). A consistent benefit of empagliflozin was seen across prespecified subgroups (Fig. S1 in the Supplementary Appendix) and across the two doses of empagliflozin (Fig. S2 in the Supplementary Appendix). The composite outcome of incident or worsening nephropathy or cardiovascular death was significantly lower in the empagliflozin group than in the placebo group (Fig. 2, and Fig. S3A in the Supplementary Appendix). Equivalent results were seen across the two doses of empagliflozin (Fig. S3B in the Supplementary Appendix). Progression to macroalbuminuria occurred in 459 of 4091 patients (11.2%) in the empagliflozin group and in 330 of 2033 (16.2%) in the placebo group, a significant relative risk reduction of 38% (Fig. 2). A doubling of the serum creatinine level occurred in 70 of 4645 patients (1.5%) in the empagliflozin group and in 60 of 2323 (2.6%) in the placebo group, a significant relative risk reduction of 44%. The initiation of renal-replacement therapy occurred in 13 of 4687 patients (0.3%) in the empagliflozin group and in 14 of 2333 (0.6%) in the placebo group, a significant relative risk reduction of 55%. There were three deaths from renal disease in the empagliflozin group (0.1%) and none in the placebo group. There was no significant between-group difference in the rate of incident albuminuria, which occurred in 1430 of 2779 patients (51.5%) in the empagliflozin group and in 703 of 1374 (51.2%) in the placebo group (Fig. 2). Post Hoc Assessments of Renal Outcomes Results for the composite renal outcomes were validated in a post hoc sensitivity analysis (Table S4 in the Supplementary Appendix) and in a subgroup analysis of patients with prevalent kidney disease at baseline (Table S5 and Fig. S4 in the Supplementary Appendix). The effect of empagliflozin was consistent in further analyses in which progression to macroalbuminuria was excluded from the composite renal outcome (Fig. 1B and Fig. 2) with no heterogeneity among subgroups of patients with a normal albumin level or microalbuminuria or macroalbuminuria at baseline and in subgroups according to the egfr at baseline (Figs. S5 and S6 in the Supplementary Appendix). Renal Function over Time Renal function over time, as measured by the egfr, is shown in Fig. 3A. Similar patterns in 326 n engl j med 375;4 nejm.org July 28, 2016
5 and Kidney Disease in Type 2 Diabetes Characteristic Patients with egfr of 59 ml per Minute per 1.73 m 2 or Less (N = 607) (N = 1212) Patients with egfr of 60 ml per Minute per 1.73 m 2 or More (N = 1726) (N = 3473) Age yr 67.1± ± ± ±8.5 Male sex no. (%) 418 (68.9) 816 (67.3) 1262 (73.1) 2518 (72.5) Body-mass index 30.9± ± ± ±5.2 Glycated hemoglobin % 8.03± ± ± ±0.84 Interval of >10 yr since diagnosis of type 2 diabetes no. (%) 422 (69.5) 794 (65.5) 917 (53.1) 1876 (54.0) Blood pressure mm Hg Systolic 136.4± ± ± ±16.6 Diastolic 74.6± ± ± ±9.5 Estimated glomerular filtration rate ml/min/1.73 m ± ± ± ±17.1 Urinary albumin-to-creatinine ratio no. (%) < (46.6) 566 (46.7) 1099 (63.7) 2223 (64.0) 30 to (33.8) 411 (33.9) 470 (27.2) 926 (26.7) > (18.9) 223 (18.4) 145 (8.4) 286 (8.2) Cholesterol mg/dl Low-density lipoprotein 85.0± ± ± ±36.0 High-density lipoprotein 42.9± ± ± ±11.7 Triglycerides mg/dl 180.4± ± ± ±136.4 Coronary artery disease 482 (79.4) 938 (77.4) 1281 (74.2) 2606 (75.0) History of stroke** 156 (25.7) 293 (24.2) 397 (23.0) 791 (22.8) Peripheral artery disease 130 (21.4) 314 (25.9) 349 (20.2) 667 (19.2) Cardiac failure 89 (14.7) 174 (14.4) 155 (9.0) 288 (8.3) Concomitant medication no. (%) Angiotensin-converting enzyme inhibitor or angiotensinreceptor blocker 502 (82.7) 1031 (85.1) 1366 (79.1) 2766 (79.6) Beta-blocker 415 (68.4) 829 (68.4) 1083 (62.7) 2226 (64.1) Diuretic 355 (58.5) 710 (58.6) 633 (36.7) 1336 (38.5) Calcium-channel blocker 227 (37.4) 446 (36.8) 561 (32.5) 1082 (31.2) Statin 461 (75.9) 966 (79.7) 1312 (76.0) 2663 (76.7) Aspirin 495 (81.5) 981 (80.9) 1432 (83.0) 2894 (83.3) Metformin 369 (60.8) 711 (58.7) 1365 (79.1) 2746 (79.1) Sulfonylurea 234 (38.6) 480 (39.6) 758 (43.9) 1534 (44.2) Insulin 357 (58.8) 699 (57.7) 778 (45.1) 1551 (44.7) * Plus minus values are means ±SD. The GFR at baseline was estimated according to the four-variable Modification of Diet in Renal Disease formula. Data on egfr at baseline were not available for two patients in the empagliflozin group. There were no significant differences between the study groups except with respect to high-density lipoprotein cholesterol (P = 0.02) and peripheral artery disease (P = 0.04) in patients with an egfr of 59 ml per minute per 1.73 m 2 or less. To convert the values for cholesterol to millimoles per liter, multiply by To convert the values for triglycerides to millimoles per liter, multiply by The body-mass index is the weight in kilograms divided by the square of the height in meters. The glycated hemoglobin value was missing for one patient in the empagliflozin group in patients with an egfr of 60 ml per minute per 1.73 m 2 or more. This ratio was measured in milligrams of albumin per grams of creatinine. Low-density lipoprotein cholesterol was measured in 598 patients in the placebo group and 1201 in the empagliflozin group in patients with an egfr of 59 ml per minute per 1.73 m 2 or less and in 1711 patients in the placebo group and 3421 in the empagliflozin group in patients with an egfr of 60 ml per minute per 1.73 m 2 or more. Table 1. Characteristics of the Patients at Baseline, According to the Estimated Glomerular Filtration Rate (egfr).* High-density lipoprotein cholesterol and triglycerides were measured in 598 patients in the placebo group and 1202 in the empagliflozin group in patients with an egfr of 59 ml per minute per 1.73 m 2 or less and in 1711 patients in the placebo group and 3423 in the empagliflozin group in patients with an egfr of 60 ml per minute per 1.73 m 2 or more. ** Information on stroke history was not available for one patient in the placebo group in patients with an egfr of 60 ml per minute per 1.73 m 2 or more. Information on peripheral artery disease was not available for one patient in the placebo group and one patient in the empagliflozin group in patients with an egfr of 60 ml per minute per 1.73 m2 or more. Cardiac failure was determined according to the narrow standardized Medical Dictionary for Regulatory Activities query for the condition. n engl j med 375;4 nejm.org July 28,
6 The new england journal of medicine the egfr were observed in patients with an egfr of 60 ml per minute per 1.73 m 2 or more and in patients with an egfr of 59 ml per minute per 1.73 m 2 or less at baseline (Fig. S7 in the Supplementary Appendix). The initial decrease in the egfr in the empagliflozin group was completely reversed after the cessation of the study drug (Fig. 3B). At the follow-up visit, the adjusted mean difference from placebo in the change from baseline in the egfr with each of the two doses of empagliflozin was 4.7 ml per minute per 1.73 m 2 (95% confidence interval, 4.0 to 5.5; P<0.001 for both comparisons) (Fig. 3B). We quantified the difference between the study groups in the average rate of change in the egfr for three prespecified time periods, using the CKD-EPI creatinine equation. From baseline to week 4 (period 1), there was a short-term decrease in the egfr in the empagliflozin groups, with mean (±SE) adjusted estimates of weekly decreases of 0.62±0.04 ml per minute per 1.73 m 2 in the 10-mg group and 0.82±0.04 ml per minute per 1.73 m 2 in the 25-mg group, as compared with a small increase (of 0.01±0.04 ml per minute per 1.73 m 2 ) in the placebo group (P<0.001 for both comparisons with placebo). Thereafter, during long-term administration (period 2; from week 4 to the last week of treatment), the egfr remained stable in the empagliflozin groups and declined steadily in the placebo group, with adjusted estimates of annual decreases of 0.19±0.11 ml per minute per 1.73 m 2 in the 10-mg and 25-mg empagliflozin groups, as compared with a decrease of 1.67±0.13 ml per minute per 1.73 m 2 in the placebo group (P<0.001 for both comparisons with placebo). After the cessation of the study drug (period 3; last week of treatment to follow-up), the egfr increased with both doses of empagliflozin, with adjusted estimates for weekly increases of 0.48±0.04 ml per minute per 1.73 m 2 in the 10-mg group and 0.55±0.04 ml per minute per 1.73 m 2 in the 25-mg group, as compared with a small decrease (of 0.04±0.04 ml per minute per 1.73 m 2 ) in the placebo group (P<0.001 for both comparisons with placebo). Safety and Adverse Events The percentages of patients who had an adverse event, a serious adverse event, or an adverse event leading to study-drug discontinuation were similar in the empagliflozin group and the placebo group in patients with an egfr of 60 ml per minute per 1.73 m 2 or more and in patients with an egfr of 59 ml per minute per 1.73 m 2 or less (Table 2, and Table S6 and Fig. S8 in the Supplementary Appendix). Genital infections were reported in a higher percentage of patients in the empagliflozin group than in the placebo group. There were similar rates of overall urinary tract infection, complicated urinary tract infection, and pyelonephritis in the two study groups. Urosepsis was reported infrequently, but the proportion of patients with events was higher with empagliflozin than with placebo (Table S7 in the Supplementary Appendix). The percentages of patients with confirmed hypoglycemic episodes, diabetic ketoacidosis, thromboembolic events, bone fractures, and events consistent with volume depletion were similar in the two study groups. Events that were consistent with acute renal failure, including acute kidney injury, and hyperkalemia were reported in a lower percentage of patients in the empagliflozin group than in the placebo group (Figs. S8 and S9 in the Supplementary Appendix). Clinical laboratory measurements are provided in Table S8 in the Supplementary Appendix. Discussion In patients with type 2 diabetes at high risk for cardiovascular events, those who received empagliflozin in addition to standard care had a significantly lower risk of microvascular outcome events than did those receiving placebo, a difference that was driven by a lower risk of progression of kidney disease (as defined by incident or worsening nephropathy). Patients in the empagliflozin group also had a significantly lower risk of progression to macroalbuminuria or clinically relevant renal outcomes, such as a doubling of the serum creatinine level and initiation of renal-replacement therapy, than did those in the placebo group. The magnitude of the renal effect associated with empagliflozin was consistent with respect to the competing risk of death from cardiovascular causes, as well as between empagliflozin doses of 10 mg and 25 mg and across prespecified subgroups, including patients with prevalent kidney disease. These results were observed in a population of patients whose blood pressure was well managed, with extensive use of RAAS blockers, the recommended treatment for kidney 328 n engl j med 375;4 nejm.org July 28, 2016
7 and Kidney Disease in Type 2 Diabetes disease in patients with type 2 diabetes. However, the renal effects of empagliflozin cannot necessarily be generalized to patients with type 2 diabetes at lower cardiovascular risk. Generalization of the findings to black patients also has limitations because of the small sample size that we studied. Further clinical research is warranted to validate our findings in broader populations at risk for adverse renal outcomes. was associated with lower rates of hyperglycemia and lower values for weight and blood pressure than was placebo. 23 A trial comparing an intensive multifactorial intervention with conventional therapy in patients with type 2 diabetes and microalbuminuria did not show significant differences in the decline in renal function after 7.8 years. 27 Thus, in our trial, the magnitude of the observed effect on these risk factors over a median follow-up period of 3.1 years is unlikely to fully account for the observed difference in renal function among patients receiving empagliflozin. The mechanisms behind the renal effects of empagliflozin are probably multifactorial, but direct renovascular effects may play an important role. 21,28,29 reduces proximal tubular sodium reabsorption, thereby increasing distal sodium delivery to the macula densa, which has been shown to activate tubuloglomerular feedback, leading to afferent vasomodulation and a decrease in hyperfiltration. 30 In patients with type 1 diabetes and hyperfiltration, empagliflozin reduces the intraglomerular pressure. 20 Despite the low-pressure environment of renal glomeruli, a reduction in glomerular hypertension of approximately 6 to 8 mm Hg was observed with empagliflozin. 20 Other effects, such as those on arterial stiffness, 28,29 vascular resistance, 28 serum uric acid levels, 23 and the systemic and renal neurohormonal systems, 29,31,32 may also contribute to the improvements in the progression of renal disease observed with empagliflozin. Further research is needed to explore whether empagliflozin-associated changes in blood volume or renal perfusion may alter serum creatinine turnover and renal-function assessments. Previous trials have focused on the role of RAAS blockade for improving renal outcomes in type 2 diabetes Such blockade causes vasodilation of the efferent arteriolar system of the glomerulus and a reduction in intraglomerular A Incident or Worsening Nephropathy Cumulative Probability of Event (%) No. at Risk Hazard ratio, 0.61 (95% CI, ) 70 P< Month B Post Hoc Renal Composite Outcome Cumulative Probability of Event (%) No. at Risk Figure 1. Kaplan Meier Analysis of Two Key Renal Outcomes. Shown are estimates of the probability of a first occurrence of a prespecified renal composite outcome of incident or worsening nephropathy (Panel A) and of a post hoc renal composite outcome (a doubling of the serum creatinine level, the initiation of renal-replacement therapy, or death from renal disease) (Panel B) among patients who received at least one dose of either empagliflozin or placebo. The inset in Panel B shows the data on an expanded y axis. Hazard ratios are based on Cox regression analyses. Because of the declining numbers of patients at risk, Kaplan Meier curves have been truncated at 48 months. pressure. 36,37 This vasomodulatory mechanism is known to cause a short-term decrease in the egfr, 38 which is accompanied by a smaller decline in renal function during continued treatment. 39 In our trial, empagliflozin showed a similar pattern of change in renal function (i.e., a short-term decrease followed by stabilization Hazard ratio, 0.54 (95% CI, ) 6 P< Month n engl j med 375;4 nejm.org July 28,
8 The new england journal of medicine Renal Outcome Measure Incident or worsening nephropathy or cardiovascular death no. with event/ rate/1000 patient-yr no. with event/ no. analyzed (%) rate/1000 patient-yr no. analyzed (%) Hazard Ratio (95% CI) 675/4170 (16.2) /2102 (23.6) ( ) P Value <0.001 Incident or worsening nephropathy 525/4124 (12.7) /2061 (18.8) ( ) <0.001 Progression to macroalbuminuria 459/4091 (11.2) /2033 (16.2) ( ) <0.001 Doubling of serum creatinine level accompanied by egfr of 45 ml/min/1.73 m 2 70/4645 (1.5) /2323 (2.6) ( ) <0.001 Initiation of renal-replacement therapy 13/4687 (0.3) /2333 (0.6) ( ) 0.04 Doubling of serum creatinine level accompanied by egfr of 45 ml/min/1.73 m 2, initiation of renal-replacement therapy, or death from renal disease 81/4645 (1.7) /2323 (3.1) ( ) <0.001 Incident albuminuria in patients with a normal albumin level at baseline 1430/2779 (51.5) /1374 (51.2) ( ) better better Figure 2. Risk Comparison for Seven Renal Outcomes. All the analyses shown were performed with the use of Cox regression in patients who received at least one dose of either empagliflozin or placebo. All the analyses were prespecified except for the composite outcome of a doubling of the serum creatinine level, the initiation of renal-replacement therapy, or death from renal disease. The abbreviation egfr denotes estimated glomerular filtration rate. 330 n engl j med 375;4 nejm.org July 28, 2016
9 and Kidney Disease in Type 2 Diabetes A Change in egfr over 192 Wk 78 Adjusted Mean egfr (ml/min/1.73 m 2 ) , 10 mg, 25 mg No. at Risk, 10 mg, 25 mg No. in Follow-up Analysis Total 66 Baseline Week B Change in egfr from Baseline to Last Measurement during Treatment and Follow-up (N=1555), 10 mg (N=1642), 25 mg (N=1686) 78 Adjusted Mean egfr (ml/min/1.73 m 2 ) Baseline Last measurement during treatment Follow-up Median, 3.0 years Median, 34 days Figure 3. Renal Function over Time. Shown are the adjusted means for the estimated glomerular filtration rate (egfr) over a period of 192 weeks (Panel A) and at the last measurement during treatment and at follow-up (Panel B) among patients who received empagliflozin (at a dose of 10 mg or 25 mg) or placebo. Baseline values are means, and the I bars indicate standard errors. The egfr was calculated according to the creatinine formula developed by the Chronic Kidney Disease Epidemiology Collaboration. Among patients in the empagliflozin group, the adjusted mean difference from placebo in the change from baseline at follow-up (Panel B) was 4.7 ml per minute per 1.73 m 2 in both the 10-mg and 25-mg groups (P<0.001 for both comparisons). Panel A is based on prespecified mixed-model, repeated-measures analysis in patients who received at least one dose of a study drug and had a baseline and postbaseline measurement. Panel B is based on a prespecified analysis of a covariance model (with the baseline egfr and glycated hemoglobin level as linear covariates and baseline body-mass index, region, and study group as fixed effects) in patients who underwent measurements at all three time points. n engl j med 375;4 nejm.org July 28,
10 The new england journal of medicine Table 2. Adverse Events.* Event Patients with Baseline egfr of 59 ml per Minute per 1.73 m 2 or Less Patients with Baseline egfr of 60 ml per Minute per 1.73 m 2 or More (N= 607) (N = 1212) (N = 1726) (N = 3473) no. (%) rate per 100 patient-yr no. (%) rate per 100 patient-yr no. (%) rate per 100 patient-yr no. (%) rate per 100 patient-yr Any adverse event 577 (95.1) (91.3) (90.5) (89.9) Severe adverse event 208 (34.3) (29.7) (22.2) (21.3) 9.1 Serious adverse event 321 (52.9) (45.5) (38.6) (35.6) 17.0 Death 40 (6.6) (5.6) (4.6) (3.1) 1.2 Adverse event leading to 167 (27.5) (22.9) (16.6) (15.4) 6.2 discontinuation Confirmed hypoglycemic adverse event Any 233 (38.4) (32.3) (24.2) (26.3) 12.8 Requiring assistance 18 (3.0) (1.9) (1.0) (1.2) 0.4 Event consistent with urinary tract infection Any 132 (21.7) (22.9) (16.9) (16.2) 6.9 Complicated 17 (2.8) (3.1) (1.4) (1.3) 0.5 Event consistent with genital 10 (1.6) (5.3) (1.9) (6.8) 2.7 infection Event consistent with volume 49 (8.1) (6.7) (3.8) (4.5) 1.8 depletion** Acute renal failure 87 (14.3) (11.2) (3.9) (3.2) 1.2 Acute kidney injury 22 (3.6) (2.1) (0.9) (0.5) 0.2 Diabetic ketoacidosis 1 (0.2) (0.2) (0.1) <0.1 Thromboembolic event 7 (1.2) (1.1) (0.8) (0.5) 0.2 Bone fracture 32 (5.3) (4.7) (3.4) (3.5) 1.4 Hyperkalemia 42 (6.9) (3.9) (2.1) (1.3) 0.5 * Data are for patients who received at least one dose of a study drug and include events that occurred during treatment or within 7 days after the last receipt of a study drug. A serious adverse event is defined as an event that is fatal or life-threatening, results in persistent or significant disability, requires or prolongs hospitalization, is associated with a congenital anomaly or birth defect, or is deemed to be serious for any other reason. A severe adverse event is one that is incapacitating or that results in an inability to work or perform usual activities. Hypoglycemia was defined as a plasma glucose level of 70 mg per deciliter (3.9 mmol per liter) or less or an event requiring assistance. The definition of urinary tract infection was based on 79 preferred terms in the Medical Dictionary for Regulatory Activities (MedDRA). Complicated urinary tract infection comprised pyelonephritis, urosepsis, and a serious adverse event consistent with urinary tract infection. The definition of genital infection was based on 88 MedDRA preferred terms. ** The definition of volume depletion was based on 8 MedDRA preferred terms. The definition of acute renal failure was based on the narrow standardized MedDRA query for the condition. The definition of diabetic ketoacidosis was based on 4 MedDRA preferred terms. The definition of thromboembolic event was based on 1 standardized MedDRA query. The definition of bone fracture was based on 62 MedDRA preferred terms. The definition of hyperkalemia was based on 2 MedDRA preferred terms. in the egfr over time). Moreover, measures of renal function significantly improved after the discontinuation of empagliflozin, indicating that glomerular hemodynamic changes were reversed even after long-term treatment. Most patients in this trial were receiving background RAAS blockade, so the renal effects of empagliflozin were still apparent even with the use of these 332 n engl j med 375;4 nejm.org July 28, 2016
11 and Kidney Disease in Type 2 Diabetes agents. This finding supports the potential use of empagliflozin in combination with RAAS blockers in patients with type 2 diabetes and chronic kidney disease. However, empagliflozin did not prevent incident albuminuria despite previous evidence that the drug lowers the intraglomerular pressure. 20 The adverse-event profile of empagliflozin in patients who had impaired kidney function at baseline, a potentially vulnerable population, was consistent with that reported in the overall trial population. The proportion of patients with genital infection was greater in the empagliflozin group than in the placebo group, which was consistent with findings in previous studies. Rates of adverse events consistent with acute renal failure (including acute kidney injury) or hyperkalemia in the empagliflozin group were lower than or similar to those in the placebo group, regardless of whether patients had impaired kidney function at baseline. In conclusion, among patients with type 2 diabetes who were at high risk for cardiovascular events, the use of empagliflozin was associated with slower progression of kidney disease than was placebo when added to standard care. was also associated with a significantly lower risk of clinically relevant renal events. Supported by the Boehringer Ingelheim and Eli Lilly and Company Diabetes Alliance. Disclosure forms provided by the authors are available with the full text of this article at NEJM.org. We thank all the patients who participated in this trial; and Elizabeth Ng and Wendy Morris of FleishmanHillard Fishburn for their medical writing assistance. References 1. The Emerging Risk Factors Collaboration. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet 2010; 375: de Boer IH, Rue TC, Hall YN, Heagerty PJ, Weiss NS, Himmelfarb J. Temporal trends in the prevalence of diabetic kidney disease in the United States. JAMA 2011; 305: Afkarian M, Sachs MC, Kestenbaum B, et al. Kidney disease and increased mortality risk in type 2 diabetes. J Am Soc Nephrol 2013; 24: UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet 1998; 352: Coca SG, Ismail-Beigi F, Haq N, Krumholz HM, Parikh CR. Role of intensive glucose control in development of renal end points in type 2 diabetes mellitus: systematic review and meta-analysis intensive glucose control in type 2 diabetes. Arch Intern Med 2012; 172: The ADVANCE Collaborative Group. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med 2008; 358: Perkovic V, Heerspink HL, Chalmers J, et al. Intensive glucose control improves kidney outcomes in patients with type 2 diabetes. Kidney Int 2013; 83: Zoungas S, Chalmers J, Neal B, et al. Follow-up of blood-pressure lowering and glucose control in type 2 diabetes. N Engl J Med 2014; 371: Roscioni SS, Heerspink HJ, de Zeeuw D. The effect of RAAS blockade on the progression of diabetic nephropathy. Nat Rev Nephrol 2014; 10: Molitch ME, Adler AI, Flyvbjerg A, et al. Diabetic kidney disease: a clinical update from Kidney Disease: Improving Global Outcomes. Kidney Int 2015; 87: Heise T, Seewaldt-Becker E, Macha S, et al. Safety, tolerability, pharmacokinetics and pharmacodynamics following 4 weeks treatment with empagliflozin once daily in patients with type 2 diabetes. Diabetes Obes Metab 2013; 15: Häring HU, Merker L, Seewaldt-Becker E, et al. as add-on to metformin plus sulfonylurea in patients with type 2 diabetes: a 24-week, randomized, double-blind, placebo-controlled trial. Diabetes Care 2013; 36: Häring HU, Merker L, Seewaldt-Becker E, et al. as add-on to metformin in patients with type 2 diabetes: a 24-week, randomized, double-blind, placebo-controlled trial. Diabetes Care 2014; 37: Kovacs CS, Seshiah V, Swallow R, et al. improves glycaemic and weight control as add-on therapy to pioglitazone or pioglitazone plus metformin in patients with type 2 diabetes: a 24-week, randomized, placebo-controlled trial. Diabetes Obes Metab 2014; 16: Roden M, Weng J, Eilbracht J, et al. monotherapy with sitagliptin as an active comparator in patients with type 2 diabetes: a randomised, doubleblind, placebo-controlled, phase 3 trial. Lancet Diabetes Endocrinol 2013; 1: Rosenstock J, Jelaska A, Frappin G, et al. Improved glucose control with weight loss, lower insulin doses, and no increased hypoglycemia with empagliflozin added to titrated multiple daily injections of insulin in obese inadequately controlled type 2 diabetes. Diabetes Care 2014; 37: Rosenstock J, Jelaska A, Zeller C, Kim G, Broedl UC, Woerle HJ. Impact of empagliflozin added on to basal insulin in type 2 diabetes inadequately controlled on basal insulin: a 78-week randomized, doubleblind, placebo-controlled trial. Diabetes Obes Metab 2015; 17: Tikkanen I, Narko K, Zeller C, et al. reduces blood pressure in patients with type 2 diabetes and hypertension. Diabetes Care 2015; 38: Barnett AH, Mithal A, Manassie J, et al. Efficacy and safety of empagliflozin added to existing antidiabetes treatment in patients with type 2 diabetes and chronic kidney disease: a randomised, doubleblind, placebo-controlled trial. Lancet Diabetes Endocrinol 2014; 2: Skrtić M, Yang GK, Perkins BA, et al. Characterisation of glomerular haemodynamic responses to SGLT2 inhibition in patients with type 1 diabetes and renal hyperfiltration. Diabetologia 2014; 57: Cherney DZ, Perkins BA, Soleymanlou N, et al. Renal hemodynamic effect of sodium-glucose cotransporter 2 inhibition in patients with type 1 diabetes mellitus. Circulation 2014; 129: Škrtić M, Cherney DZ. Sodium-glucose cotransporter-2 inhibition and the potential for renal protection in diabetic nephropathy. Curr Opin Nephrol Hypertens 2015; 24: Zinman B, Wanner C, Lachin JM, et al., cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med 2015; 373: Zinman B, Inzucchi SE, Lachin JM, et al. Rationale, design, and baseline characteristics of a randomized, placebo-controlled cardiovascular outcome trial of n engl j med 375;4 nejm.org July 28,
12 and Kidney Disease in Type 2 Diabetes empagliflozin (EMPA-REG OUTCOME). Cardiovasc Diabetol 2014; 13: Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, Roth D. A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Ann Intern Med 1999; 130: Levey AS, Stevens LA, Schmid CH, et al. A new equation to estimate glomerular filtration rate. Ann Intern Med 2009; 150: Gaede P, Vedel P, Larsen N, Jensen GV, Parving HH, Pedersen O. Multifactorial intervention and cardiovascular disease in patients with type 2 diabetes. N Engl J Med 2003; 348: Chilton R, Tikkanen I, Cannon CP, et al. Effects of empagliflozin on blood pressure and markers of arterial stiffness and vascular resistance in patients with type 2 diabetes. Diabetes Obes Metab 2015; 17: Cherney DZ, Perkins BA, Soleymanlou N, et al. The effect of empagliflozin on arterial stiffness and heart rate variability in subjects with uncomplicated type 1 diabetes mellitus. Cardiovasc Diabetol 2014; 13: Vallon V, Gerasimova M, Rose MA, et al. SGLT2 inhibitor empagliflozin reduces renal growth and albuminuria in proportion to hyperglycemia and prevents glomerular hyperfiltration in diabetic Akita mice. Am J Physiol Renal Physiol 2014; 306: F Cherney DZ, Perkins BA, Soleymanlou N, et al. Sodium glucose cotransport-2 inhibition and intrarenal RAS activity in people with type 1 diabetes. Kidney Int 2014; 86: Jordan J, Tank J, Heusser K, et al. has no discernable effect on muscle sympathetic nerve activity in patients with type 2 diabetes despite reductions in blood pressure and weight. Diabetes 2014; 63: Suppl 1: A265 (poster). 33. Lewis EJ, Hunsicker LG, Clarke WR, et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001; 345: Brenner BM, Cooper ME, de Zeeuw D, et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001; 345: Parving H-H, Brenner BM, McMurray JJV, et al. Cardiorenal end points in a trial of aliskiren for type 2 diabetes. N Engl J Med 2012; 367: Brown NJ, Vaughan DE. Angiotensinconverting enzyme inhibitors. Circulation 1998; 97: Kobori H, Nangaku M, Navar LG, Nishiyama A. The intrarenal renin-angiotensin system: from physiology to the pathobiology of hypertension and kidney disease. Pharmacol Rev 2007; 59: Schoolwerth AC, Sica DA, Ballermann BJ, Wilcox CS. Renal considerations in angiotensin converting enzyme inhibitor therapy: a statement for healthcare professionals from the Council on the Kidney in Cardiovascular Disease and the Council for High Blood Pressure Research of the American Heart Association. Circulation 2001; 104: Holtkamp FA, de Zeeuw D, Thomas MC, et al. An acute fall in estimated glomerular filtration rate during treatment with losartan predicts a slower decrease in long-term renal function. Kidney Int 2011; 80: Copyright 2016 Massachusetts Medical Society. clinical trial registration The Journal requires investigators to register their clinical trials in a public trials registry. The members of the International Committee of Medical Journal Editors (ICMJE) will consider most reports of clinical trials for publication only if the trials have been registered. Current information on requirements and appropriate registries is available at n engl j med 375;4 nejm.org July 28, 2016
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes
 Original Article, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes Bernard Zinman, M.D., Christoph Wanner, M.D., John M. Lachin, Sc.D., David Fitchett, M.D., Erich Bluhmki, Ph.D., Stefan Hantel,
Original Article, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes Bernard Zinman, M.D., Christoph Wanner, M.D., John M. Lachin, Sc.D., David Fitchett, M.D., Erich Bluhmki, Ph.D., Stefan Hantel,
Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes
 The new england journal of medicine Original Article, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes Bernard Zinman, M.D., Christoph Wanner, M.D., John M. Lachin, Sc.D., David Fitchett, M.D.,
The new england journal of medicine Original Article, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes Bernard Zinman, M.D., Christoph Wanner, M.D., John M. Lachin, Sc.D., David Fitchett, M.D.,
Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes
 The new england journal of medicine Original Article Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes Bernard Zinman, M.D., Christoph Wanner, M.D., John M. Lachin, Sc.D., David
The new england journal of medicine Original Article Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes Bernard Zinman, M.D., Christoph Wanner, M.D., John M. Lachin, Sc.D., David
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection
 SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
The EMPA-REG OUTCOME trial: Design and results. David Fitchett, MD University of Toronto, Canada
 The EMPA-REG OUTCOME trial: Design and results David Fitchett, MD University of Toronto, Canada Asian Cardio Diabetes Forum April 23 24, 2016 Kuala Lumpur, Malaysia Life Expectancy Is Reduced by ~12 Years
The EMPA-REG OUTCOME trial: Design and results David Fitchett, MD University of Toronto, Canada Asian Cardio Diabetes Forum April 23 24, 2016 Kuala Lumpur, Malaysia Life Expectancy Is Reduced by ~12 Years
Variability in drug response: towards more personalized diabetes care Petrykiv, Sergei
 University of Groningen Variability in drug response: towards more personalized diabetes care Petrykiv, Sergei IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
University of Groningen Variability in drug response: towards more personalized diabetes care Petrykiv, Sergei IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
Managing patients with renal disease
 Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
PROTEZIONE DAL DANNO RENALE NEL DIABETE TIPO 2: RUOLO DEI NUOVI FARMACI. Massimo Boemi UOC Malattie Metaboliche e Diabetologia IRCCS INRCA Ancona
 PROTEZIONE DAL DANNO RENALE NEL DIABETE TIPO 2: RUOLO DEI NUOVI FARMACI Massimo Boemi UOC Malattie Metaboliche e Diabetologia IRCCS INRCA Ancona Disclosure Dr Massimo Boemi has been granted as speaker
PROTEZIONE DAL DANNO RENALE NEL DIABETE TIPO 2: RUOLO DEI NUOVI FARMACI Massimo Boemi UOC Malattie Metaboliche e Diabetologia IRCCS INRCA Ancona Disclosure Dr Massimo Boemi has been granted as speaker
Prevention And Treatment of Diabetic Nephropathy. MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan
 Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
An acute fall in estimated glomerular filtration rate during treatment with losartan predicts a slower decrease in long-term renal function
 original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
Bariatric Surgery versus Intensive Medical Therapy for Diabetes 3-Year Outcomes
 The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
Canagliflozin and Cardiovascular and Renal Events in Type 2 Diabetes
 The new england journal of medicine Original Article and Cardiovascular and Renal Events in Type 2 Diabetes Bruce Neal, M.B., Ch.B., Ph.D., Vlado Perkovic, M.B., B.S., Ph.D., Kenneth W. Mahaffey, M.D.,
The new england journal of medicine Original Article and Cardiovascular and Renal Events in Type 2 Diabetes Bruce Neal, M.B., Ch.B., Ph.D., Vlado Perkovic, M.B., B.S., Ph.D., Kenneth W. Mahaffey, M.D.,
Renal Protection Staying on Target
 Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
Cedars Sinai Diabetes. Michael A. Weber
 Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Metabolic Syndrome and Chronic Kidney Disease
 Metabolic Syndrome and Chronic Kidney Disease Definition of Metabolic Syndrome National Cholesterol Education Program (NCEP) Adult Treatment Panel (ATP) III Abdominal obesity, defined as a waist circumference
Metabolic Syndrome and Chronic Kidney Disease Definition of Metabolic Syndrome National Cholesterol Education Program (NCEP) Adult Treatment Panel (ATP) III Abdominal obesity, defined as a waist circumference
Liraglutide and Renal Outcomes in Type 2 Diabetes
 The new england journal of medicine Original Article and Renal Outcomes in Type 2 Diabetes Johannes F.E. Mann, M.D., David D. Ørsted, M.D., Ph.D., Kirstine Brown Frandsen, M.D., Steven P. Marso, M.D.,
The new england journal of medicine Original Article and Renal Outcomes in Type 2 Diabetes Johannes F.E. Mann, M.D., David D. Ørsted, M.D., Ph.D., Kirstine Brown Frandsen, M.D., Steven P. Marso, M.D.,
Canagliflozin and Cardiovascular and Renal Events in Type 2 Diabetes
 Original Article and Cardiovascular and Renal Events in Type Diabetes Bruce Neal, M.B., Ch.B., Ph.D., Vlado Perkovic, M.B., B.S., Ph.D., Kenneth W. Mahaffey, M.D., Dick de Zeeuw, M.D., Ph.D., Greg Fulcher,
Original Article and Cardiovascular and Renal Events in Type Diabetes Bruce Neal, M.B., Ch.B., Ph.D., Vlado Perkovic, M.B., B.S., Ph.D., Kenneth W. Mahaffey, M.D., Dick de Zeeuw, M.D., Ph.D., Greg Fulcher,
ADVANCE post trial ObservatioNal Study
 Hot Topics in Diabetes 50 th EASD, Vienna 2014 ADVANCE post trial ObservatioNal Study Sophia Zoungas The George Institute The University of Sydney Rationale and Study Design Sophia Zoungas The George Institute
Hot Topics in Diabetes 50 th EASD, Vienna 2014 ADVANCE post trial ObservatioNal Study Sophia Zoungas The George Institute The University of Sydney Rationale and Study Design Sophia Zoungas The George Institute
Study Duration (Weeks) Reference Number
 Supplementary Table 1. SGLT2 Inhibitor Monotherapy SGLT2 Inhibitor vs /Comparator Canagliflozin 100 mg Canagliflozin 300 mg 26 26 (n) 195 197 in 0.91 1.16 in FPG 36.0 43.2 Canagliflozin 100 mg Canagliflozin
Supplementary Table 1. SGLT2 Inhibitor Monotherapy SGLT2 Inhibitor vs /Comparator Canagliflozin 100 mg Canagliflozin 300 mg 26 26 (n) 195 197 in 0.91 1.16 in FPG 36.0 43.2 Canagliflozin 100 mg Canagliflozin
Supplementary Online Content
 Supplementary Online Content Afkarian M, Zelnick L, Hall YN, et al. Clinical manifestations of kidney disease among US adults with diabetes, 1988-2014. JAMA. doi:10.1001/jama.2016.10924 emethods efigure
Supplementary Online Content Afkarian M, Zelnick L, Hall YN, et al. Clinical manifestations of kidney disease among US adults with diabetes, 1988-2014. JAMA. doi:10.1001/jama.2016.10924 emethods efigure
Drug Class Monograph
 Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease
 KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
Sodium-Glucose Cotransporter 2 Inhibitors Reduce Prandial Insulin Doses in Type 2 Diabetic Patients Treated With the Intensive Insulin Therapy
 Original Article J Clin Med Res. 2018;10(6):493-498 Sodium-Glucose Cotransporter 2 Inhibitors Reduce Prandial Insulin Doses in Type 2 Diabetic Patients Treated With the Intensive Insulin Therapy Mariko
Original Article J Clin Med Res. 2018;10(6):493-498 Sodium-Glucose Cotransporter 2 Inhibitors Reduce Prandial Insulin Doses in Type 2 Diabetic Patients Treated With the Intensive Insulin Therapy Mariko
CANVAS Program Independent commentary
 CANVAS Program Independent commentary Cliff Bailey Aston University, Birmingham, UK 2017 Disclosures and disclaimers Clifford J Bailey CJB has attended advisory boards, undertaken ad hoc consultancy, received
CANVAS Program Independent commentary Cliff Bailey Aston University, Birmingham, UK 2017 Disclosures and disclaimers Clifford J Bailey CJB has attended advisory boards, undertaken ad hoc consultancy, received
Intensive Diabetes Therapy and Glomerular Filtration Rate in Type 1 Diabetes
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Diabetes and Glomerular Filtration Rate in Type 1 Diabetes The DCCT/EDIC Research Group* A BS TR AC T The members of the writing group
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Diabetes and Glomerular Filtration Rate in Type 1 Diabetes The DCCT/EDIC Research Group* A BS TR AC T The members of the writing group
The albuminuria-lowering response to dapagliflozin is variable and reproducible among individual patients
 Received: 5 February 217 Revised: 1 March 217 Accepted: 8 March 217 DOI: 1.1111/dom.12936 ORIGINAL ARTICLE The albuminuria-lowering response to dapagliflozin is variable and reproducible among individual
Received: 5 February 217 Revised: 1 March 217 Accepted: 8 March 217 DOI: 1.1111/dom.12936 ORIGINAL ARTICLE The albuminuria-lowering response to dapagliflozin is variable and reproducible among individual
Soo LIM, MD, PHD Internal Medicine Seoul National University Bundang Hospital
 Soo LIM, MD, PHD Internal Medicine Seoul National University Bundang Hospital Agenda Association between Cardiovascular Disease and Type 2 Diabetes Importance of HbA1c Management esp. High risk patients
Soo LIM, MD, PHD Internal Medicine Seoul National University Bundang Hospital Agenda Association between Cardiovascular Disease and Type 2 Diabetes Importance of HbA1c Management esp. High risk patients
Diabetic Nephropathy 2009
 Diabetic Nephropathy 2009 Michael T McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetic Nephropathy Clinical Stages Hyperfunction
Diabetic Nephropathy 2009 Michael T McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetic Nephropathy Clinical Stages Hyperfunction
University of Groningen. Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste
 University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease
 KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
Gli endpoint micro-vascolari nei trial di outcome cardiovascolare
 Gli endpoint micro-vascolari nei trial di outcome cardiovascolare Giorgio Sesti University Magna Graecia of Catanzaro ITALY Potenziali conflitti di interesse Il Prof Giorgio Sesti dichiara di aver ricevuto
Gli endpoint micro-vascolari nei trial di outcome cardiovascolare Giorgio Sesti University Magna Graecia of Catanzaro ITALY Potenziali conflitti di interesse Il Prof Giorgio Sesti dichiara di aver ricevuto
Reducing proteinuria
 Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
The effect of sodium glucose cotransporter 2 inhibition with empagliflozin on microalbuminuria and macroalbuminuria in patients with type 2 diabetes
 https://helda.helsinki.fi The effect of sodium glucose cotransporter 2 inhibition with empagliflozin on microalbuminuria and macroalbuminuria in patients with type 2 diabetes Cherney, David 216-9 Cherney,
https://helda.helsinki.fi The effect of sodium glucose cotransporter 2 inhibition with empagliflozin on microalbuminuria and macroalbuminuria in patients with type 2 diabetes Cherney, David 216-9 Cherney,
Empagliflozin: Role in Treatment Options for Patients with Type 2 Diabetes Mellitus
 Diabetes Ther (2017) 8:33 53 DOI 10.1007/s13300-016-0211-x REVIEW Empagliflozin: Role in Treatment Options for Patients with Type 2 Diabetes Mellitus John E. Anderson. Eugene E. Wright Jr.. Charles F.
Diabetes Ther (2017) 8:33 53 DOI 10.1007/s13300-016-0211-x REVIEW Empagliflozin: Role in Treatment Options for Patients with Type 2 Diabetes Mellitus John E. Anderson. Eugene E. Wright Jr.. Charles F.
Dapagliflozin and cardiovascular outcomes in type 2
 EARN 3 FREE CPD POINTS diabetes Leader in digital CPD for Southern African healthcare professionals Dapagliflozin and cardiovascular outcomes in type 2 diabetes Introduction People with type 2 diabetes
EARN 3 FREE CPD POINTS diabetes Leader in digital CPD for Southern African healthcare professionals Dapagliflozin and cardiovascular outcomes in type 2 diabetes Introduction People with type 2 diabetes
No Increased Cardiovascular Risk for Lixisenatide in ELIXA
 ON ISSUES IN THE MANAGEMENT OF TYPE 2 DIABETES JUNE 2015 Coverage of data from ADA 2015, June 5 9 in Boston, Massachusetts No Increased Cardiovascular Risk for Lixisenatide in ELIXA First Cardiovascular
ON ISSUES IN THE MANAGEMENT OF TYPE 2 DIABETES JUNE 2015 Coverage of data from ADA 2015, June 5 9 in Boston, Massachusetts No Increased Cardiovascular Risk for Lixisenatide in ELIXA First Cardiovascular
Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin
 Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin Disclosures I have no financial relationship with the manufacturers of any commercial product discussed during this
Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin Disclosures I have no financial relationship with the manufacturers of any commercial product discussed during this
Diabetic Nephropathy. Objectives:
 There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol
 Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has
Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has
1. Albuminuria an early sign of glomerular damage and renal disease. albuminuria
 1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
Comparison between the efficacy of double blockade and single blockade of RAAS in diabetic kidney disease
 International Journal of Advances in Medicine Gupta A et al. Int J Adv Med. 2018 Aug;5(4):931-935 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183122
International Journal of Advances in Medicine Gupta A et al. Int J Adv Med. 2018 Aug;5(4):931-935 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183122
Introduction. Naveed Sattar 1 & David Fitchett 2 & Stefan Hantel 3 & Jyothis T. George 3 & Bernard Zinman 4
 Diabetologia (2018) 61:2155 2163 https://doi.org/10.1007/s00125-018-4702-3 ARTICLE Empagliflozin is associated with improvements in liver enzymes potentially consistent with reductions in liver fat: results
Diabetologia (2018) 61:2155 2163 https://doi.org/10.1007/s00125-018-4702-3 ARTICLE Empagliflozin is associated with improvements in liver enzymes potentially consistent with reductions in liver fat: results
The CARI Guidelines Caring for Australasians with Renal Impairment. ACE Inhibitor and Angiotensin II Antagonist Combination Treatment GUIDELINES
 ACE Inhibitor and Angiotensin II Antagonist Combination Treatment Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES No recommendations possible based on Level
ACE Inhibitor and Angiotensin II Antagonist Combination Treatment Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES No recommendations possible based on Level
Multi-factor approach to reduce cardiovascular risk in diabetes
 Multi-factor approach to reduce cardiovascular risk in diabetes Prof. Nicola Napoli, MD PhD Division of Endocrinology and Diabetes Università Campus Bio-Medico di Roma Washington University in St Louis
Multi-factor approach to reduce cardiovascular risk in diabetes Prof. Nicola Napoli, MD PhD Division of Endocrinology and Diabetes Università Campus Bio-Medico di Roma Washington University in St Louis
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
Department of Pharmacy, Peking University Third Hospital, Beijing, China
 This is the author's manuscript of the article published in final edited form as: Tang, H., Zhang, X., Zhang, J., Li, Y., Gobbo, L. C. D., Zhai, S., & Song, Y. (2016). Elevated serum magnesium associated
This is the author's manuscript of the article published in final edited form as: Tang, H., Zhang, X., Zhang, J., Li, Y., Gobbo, L. C. D., Zhai, S., & Song, Y. (2016). Elevated serum magnesium associated
Data Analysis Plan for assessing clinical efficacy and safety of ER niacin/laropiprant in the HPS2-THRIVE trial
 Data Analysis Plan for assessing clinical efficacy and safety of ER niacin/laropiprant in the HPS2-THRIVE trial 1 Background This Data Analysis Plan describes the strategy, rationale and statistical methods
Data Analysis Plan for assessing clinical efficacy and safety of ER niacin/laropiprant in the HPS2-THRIVE trial 1 Background This Data Analysis Plan describes the strategy, rationale and statistical methods
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes
 A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
The Seventh Report of the Joint National Commission
 The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
Diabetes and New Meds for Cardiovascular Risk Reduction. F. Dwight Chrisman, MD, FACC. Disclosures: BI Boehringer Ingelheim speaker
 Diabetes and New Meds for Cardiovascular Risk Reduction F. Dwight Chrisman, MD, FACC Disclosures: BI Boehringer Ingelheim speaker 1 Prevalence of DM DM state specific prevalence 2006 4%-6% 6-8% 8-10% 10-12%
Diabetes and New Meds for Cardiovascular Risk Reduction F. Dwight Chrisman, MD, FACC Disclosures: BI Boehringer Ingelheim speaker 1 Prevalence of DM DM state specific prevalence 2006 4%-6% 6-8% 8-10% 10-12%
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
The CARI Guidelines Caring for Australasians with Renal Impairment. Blood Pressure Control role of specific antihypertensives
 Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
Empagliflozin (Jardiance ) for the treatment of type 2 diabetes mellitus, the EMPA REG OUTCOME study
 Empagliflozin (Jardiance ) for the treatment of type 2 diabetes mellitus, the EMPA REG OUTCOME study POSITION STATEMENT: Clinicians should continue to follow MHRA advice and NICE technology appraisal guidance
Empagliflozin (Jardiance ) for the treatment of type 2 diabetes mellitus, the EMPA REG OUTCOME study POSITION STATEMENT: Clinicians should continue to follow MHRA advice and NICE technology appraisal guidance
Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects
 ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
Can We Reduce Heart Failure by Treating Diabetes? CVOT Data on SGLT2 Inhibitors and GLP-1Receptor Agonists
 Can We Reduce Heart Failure by Treating Diabetes? CVOT Data on SGLT2 Inhibitors and GLP-1Receptor Agonists Robert R. Henry, MD Professor of Medicine University of California, San Diego Relevant Conflict
Can We Reduce Heart Failure by Treating Diabetes? CVOT Data on SGLT2 Inhibitors and GLP-1Receptor Agonists Robert R. Henry, MD Professor of Medicine University of California, San Diego Relevant Conflict
2 Furthermore, quantitative coronary angiography
 ORIGINAL PAPER Estimated Glomerular Filtration Rate Reversal by Blood Pressure Lowering in Chronic Kidney Disease: Japan Multicenter Investigation for Cardiovascular DiseaseB CKD Study Yoshiki Yui, MD;
ORIGINAL PAPER Estimated Glomerular Filtration Rate Reversal by Blood Pressure Lowering in Chronic Kidney Disease: Japan Multicenter Investigation for Cardiovascular DiseaseB CKD Study Yoshiki Yui, MD;
The CARI Guidelines Caring for Australasians with Renal Impairment. Protein Restriction to prevent the progression of diabetic nephropathy GUIDELINES
 Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Dapagliflozin reduces albuminuria in patients with diabetes and hypertension receiving reninangiotensin
 University of Groningen Dapagliflozin reduces albuminuria in patients with diabetes and hypertension receiving reninangiotensin blockers Heerspink, H. J. L.; Johnsson, E.; Gause-Nilsson, I.; Cain, V. A.;
University of Groningen Dapagliflozin reduces albuminuria in patients with diabetes and hypertension receiving reninangiotensin blockers Heerspink, H. J. L.; Johnsson, E.; Gause-Nilsson, I.; Cain, V. A.;
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Risk Factors, Mortality, and Cardiovascular Outcomes in Patients with Type 2 Diabetes
 The new england journal of medicine Original Article Risk Factors, Mortality, and Cardiovascular Outcomes in Patients with Type 2 Diabetes Aidin Rawshani, M.D., Araz Rawshani, M.D., Ph.D., Stefan Franzén,
The new england journal of medicine Original Article Risk Factors, Mortality, and Cardiovascular Outcomes in Patients with Type 2 Diabetes Aidin Rawshani, M.D., Araz Rawshani, M.D., Ph.D., Stefan Franzén,
Combined Angiotensin Inhibition for the Treatment of Diabetic Nephropathy
 The new england journal of medicine original article Combined Angiotensin Inhibition for the Treatment of Diabetic Nephropathy Linda F. Fried, M.D., M.P.H., Nicholas Emanuele, M.D., Jane H. Zhang, Ph.D.,
The new england journal of medicine original article Combined Angiotensin Inhibition for the Treatment of Diabetic Nephropathy Linda F. Fried, M.D., M.P.H., Nicholas Emanuele, M.D., Jane H. Zhang, Ph.D.,
IJBCP International Journal of Basic & Clinical Pharmacology. Empagliflozin: an exciting prospect in the treatment of diabetes
 Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175669 Review Article : an exciting prospect in
Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175669 Review Article : an exciting prospect in
LEADER Liraglutide and cardiovascular outcomes in type 2 diabetes
 LEADER Liraglutide and cardiovascular outcomes in type 2 diabetes Presented at DSBS seminar on mediation analysis August 18 th Søren Rasmussen, Novo Nordisk. LEADER CV outcome study To determine the effect
LEADER Liraglutide and cardiovascular outcomes in type 2 diabetes Presented at DSBS seminar on mediation analysis August 18 th Søren Rasmussen, Novo Nordisk. LEADER CV outcome study To determine the effect
empagliflozin 10mg and 25mg tablet (Jardiance ) SMC No. (993/14) Boehringer Ingelheim / Eli Lilly
 empagliflozin 10mg and 25mg tablet (Jardiance ) SMC No. (993/14) Boehringer Ingelheim / Eli Lilly 05 September 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
empagliflozin 10mg and 25mg tablet (Jardiance ) SMC No. (993/14) Boehringer Ingelheim / Eli Lilly 05 September 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Management of Type 2 Diabetes Cardiovascular Outcomes Trials Tom Blevins MD Texas Diabetes and Endocrinology Austin, Texas
 Management of Type 2 Diabetes Cardiovascular Outcomes Trials 2018 Tom Blevins MD Texas Diabetes and Endocrinology Austin, Texas Speaker Disclosure Dr. Blevins has disclosed that he has received grant support
Management of Type 2 Diabetes Cardiovascular Outcomes Trials 2018 Tom Blevins MD Texas Diabetes and Endocrinology Austin, Texas Speaker Disclosure Dr. Blevins has disclosed that he has received grant support
Update on Diabetes Cardiovascular Outcome Trials
 Update on Diabetes Cardiovascular Outcome Trials Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine
Update on Diabetes Cardiovascular Outcome Trials Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine
journal of medicine The new england Rosuvastatin to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Abstract
 The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications
 Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Sodium-glucose cotransporter 2 inhibitors and death and heart failure in type 2 diabetes
 Editorial Page 1 of 5 Sodium-glucose cotransporter 2 inhibitors and death and heart failure in type 2 diabetes Hidekatsu Yanai Department of Internal Medicine, National Center for Global Health and Medicine
Editorial Page 1 of 5 Sodium-glucose cotransporter 2 inhibitors and death and heart failure in type 2 diabetes Hidekatsu Yanai Department of Internal Medicine, National Center for Global Health and Medicine
Effect of SGLT-2 Inhibitors on the Heart. Robert Zimmerman MD Vice Chairman Endocrinology Director Diabetes Center Cleveland Clinic
 Effect of SGLT-2 Inhibitors on the Heart Robert Zimmerman MD Vice Chairman Endocrinology Director Diabetes Center Cleveland Clinic Disclosures Speaker - Johnson and Johnson - Merck Research - Merck - Novo
Effect of SGLT-2 Inhibitors on the Heart Robert Zimmerman MD Vice Chairman Endocrinology Director Diabetes Center Cleveland Clinic Disclosures Speaker - Johnson and Johnson - Merck Research - Merck - Novo
Diabetes and kidney disease.
 Diabetes and kidney disease. What are the implications? Can it be prevented? Nice 18 june 2010 Lars G Weiss. M.D. Ph.D. Department of Neprology Central Hospital Karlstad Sweden Diabetic nephropathy vs
Diabetes and kidney disease. What are the implications? Can it be prevented? Nice 18 june 2010 Lars G Weiss. M.D. Ph.D. Department of Neprology Central Hospital Karlstad Sweden Diabetic nephropathy vs
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy
 Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin
 Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin Disclosures I have no financial relationship with the manufacturers of any commercial product discussed during this
Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin Disclosures I have no financial relationship with the manufacturers of any commercial product discussed during this
Top HF Trials to Impact Your Practice
 Top HF Trials to Impact Your Practice Biykem Bozkurt, MD, FACC The Mary and Gordon Cain Chair & Professor of Medicine Medical Care Line Executive, DeBakey VA Medical Center, Director, Winters Center for
Top HF Trials to Impact Your Practice Biykem Bozkurt, MD, FACC The Mary and Gordon Cain Chair & Professor of Medicine Medical Care Line Executive, DeBakey VA Medical Center, Director, Winters Center for
Paolo Fornengo SCDU Medicina Interna 3 AOU Città della Salute e della Scienza di Torino
 Paolo Fornengo SCDU Medicina Interna 3 AOU Città della Salute e della Scienza di Torino The KID-ney behind the curtain Altered Renal Glucose Control in Diabetes Gluconeogenesis is increased in postprandial
Paolo Fornengo SCDU Medicina Interna 3 AOU Città della Salute e della Scienza di Torino The KID-ney behind the curtain Altered Renal Glucose Control in Diabetes Gluconeogenesis is increased in postprandial
TRANSPARENCY COMMITTEE
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 17 December 2014 JARDIANCE 10 mg, film-coated tablet B/30 tablets (CIP: 34009 278 928 5 1) JARDIANCE 25 mg, film-coated
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 17 December 2014 JARDIANCE 10 mg, film-coated tablet B/30 tablets (CIP: 34009 278 928 5 1) JARDIANCE 25 mg, film-coated
Journal of Global Trends in Pharmaceutical Sciences
 An Elsevier Indexed Journal ISSN-2230-7346 Journal of Global Trends in Pharmaceutical Sciences ARTICLE INFO PHARMACOKINETICS, SAFETY AND TOLERABILITY OF EMPAGLIFLOZIN/METFORMIN FIXED-DOSE COMBINATION VS
An Elsevier Indexed Journal ISSN-2230-7346 Journal of Global Trends in Pharmaceutical Sciences ARTICLE INFO PHARMACOKINETICS, SAFETY AND TOLERABILITY OF EMPAGLIFLOZIN/METFORMIN FIXED-DOSE COMBINATION VS
Tread Carefully Because you Tread on my Nephrons. Prescribing Hints in Renal Disease
 Tread Carefully Because you Tread on my Nephrons Prescribing Hints in Renal Disease David WP Lappin,, MB PhD FRCPI Clinical Lecturer in Medicine and Consultant Nephrologist and General Physician, Merlin
Tread Carefully Because you Tread on my Nephrons Prescribing Hints in Renal Disease David WP Lappin,, MB PhD FRCPI Clinical Lecturer in Medicine and Consultant Nephrologist and General Physician, Merlin
384 Diabetes Care Volume 38, March 2015
 INHIBITION OF SODIUM GLUCOSE COTRANSPORTERS 384 Diabetes Care Volume 38, March 2015 Combination of and Linagliptin as Second-Line Therapy in Subjects With Type 2 Diabetes Inadequately Controlled on Metformin
INHIBITION OF SODIUM GLUCOSE COTRANSPORTERS 384 Diabetes Care Volume 38, March 2015 Combination of and Linagliptin as Second-Line Therapy in Subjects With Type 2 Diabetes Inadequately Controlled on Metformin
Diabete: terapia nei pazienti a rischio cardiovascolare
 Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
DIABETES MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
Index. Note: Page numbers of article titles are in boldface type.
 Heart Failure Clin 2 (2006) 101 105 Index Note: Page numbers of article titles are in boldface type. A ACE inhibitors, in diabetic hypertension, 30 31 Adipokines, cardiovascular events related to, 6 Advanced
Heart Failure Clin 2 (2006) 101 105 Index Note: Page numbers of article titles are in boldface type. A ACE inhibitors, in diabetic hypertension, 30 31 Adipokines, cardiovascular events related to, 6 Advanced
Hypertension management and renin-angiotensin-aldosterone system blockade in patients with diabetes, nephropathy and/or chronic kidney disease
 Hypertension management and renin-angiotensin-aldosterone system blockade in patients with diabetes, nephropathy and/or chronic kidney disease July 2017 Indranil Dasgupta DM FRCP, Debasish Banerjee MD
Hypertension management and renin-angiotensin-aldosterone system blockade in patients with diabetes, nephropathy and/or chronic kidney disease July 2017 Indranil Dasgupta DM FRCP, Debasish Banerjee MD
University of Groningen. Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste
 University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
SGLT2 Inhibitors
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.19 Subject: SGLT2 Inhibitors Page: 1 of 5 Last Review Date: December 3, 2015 SGLT2 Inhibitors Description
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.19 Subject: SGLT2 Inhibitors Page: 1 of 5 Last Review Date: December 3, 2015 SGLT2 Inhibitors Description
Comparative Effectiveness and Safety of Empagliflozin on Cardiovascular Mortality and Morbidity in Adults with Type 2 Diabetes
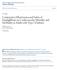 Touro College and University System Touro Scholar NYMC Faculty Publications Faculty 12-1-2017 Comparative Effectiveness and Safety of Empagliflozin on Cardiovascular Mortality and Morbidity in Adults with
Touro College and University System Touro Scholar NYMC Faculty Publications Faculty 12-1-2017 Comparative Effectiveness and Safety of Empagliflozin on Cardiovascular Mortality and Morbidity in Adults with
Effects of Intensive Blood-Pressure Control in Type 2 Diabetes Mellitus
 original article Effects of Blood-Pressure Control in Type 2 Diabetes Mellitus The ACCORD Study Group* ABSTRACT Background There is no evidence from randomized trials to support a strategy of lowering
original article Effects of Blood-Pressure Control in Type 2 Diabetes Mellitus The ACCORD Study Group* ABSTRACT Background There is no evidence from randomized trials to support a strategy of lowering
According to the US Renal Data System,
 DIABETIC NEPHROPATHY * Mohamed G. Atta, MD ABSTRACT *Based on a presentation given by Dr Atta at a CME dinner symposium for family physicians. Assistant Professor of Medicine, Division of Nephrology, Johns
DIABETIC NEPHROPATHY * Mohamed G. Atta, MD ABSTRACT *Based on a presentation given by Dr Atta at a CME dinner symposium for family physicians. Assistant Professor of Medicine, Division of Nephrology, Johns
SPRINT: Consequences for CKD patients
 SPRINT: Consequences for CKD patients 29 e Workshop Nierziekten Papendal 2018 December 12, 2018 MICHAEL ROCCO, MD, MSCE VARDAMAN M. BUCKALEW JR. PROFESSOR OF MEDICINE PROFESSOR OF PUBLIC HEALTH SCIENCES
SPRINT: Consequences for CKD patients 29 e Workshop Nierziekten Papendal 2018 December 12, 2018 MICHAEL ROCCO, MD, MSCE VARDAMAN M. BUCKALEW JR. PROFESSOR OF MEDICINE PROFESSOR OF PUBLIC HEALTH SCIENCES
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease
 Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meetings 1 st and 2 nd September 2016 - London and Leeds Prof Sunil
Angiotensin Converting Enzyme inhibitor (ACEi) / Angiotensin Receptor Blocker (ARB) To STOP OR Not in Advanced Renal Disease Investigator Meetings 1 st and 2 nd September 2016 - London and Leeds Prof Sunil
Canagliflozin Slows Progression of Renal Function Decline Independently of Glycemic Effects
 CLINICAL RESEARCH www.jasn.org Canagliflozin Slows Progression of Renal Function Decline Independently of Glycemic Effects Hiddo J. L. Heerspink,* Mehul Desai, Meg Jardine, Dainius Balis, Gary Meininger,
CLINICAL RESEARCH www.jasn.org Canagliflozin Slows Progression of Renal Function Decline Independently of Glycemic Effects Hiddo J. L. Heerspink,* Mehul Desai, Meg Jardine, Dainius Balis, Gary Meininger,
ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES
 ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES Pr. Michel KOMAJDA Institute of Cardiology - IHU ICAN Pitie Salpetriere Hospital - University Pierre and Marie Curie, Paris (France) DEFINITION A
ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES Pr. Michel KOMAJDA Institute of Cardiology - IHU ICAN Pitie Salpetriere Hospital - University Pierre and Marie Curie, Paris (France) DEFINITION A
Glycemic Control Patterns and Kidney Disease Progression among Primary Care Patients with Diabetes Mellitus
 ORIGINAL RESEARCH Glycemic Control Patterns and Kidney Disease Progression among Primary Care Patients with Diabetes Mellitus Doyle M. Cummings, PharmD, Lars C. Larsen, MD, Lisa Doherty, MD, MPH, C. Suzanne
ORIGINAL RESEARCH Glycemic Control Patterns and Kidney Disease Progression among Primary Care Patients with Diabetes Mellitus Doyle M. Cummings, PharmD, Lars C. Larsen, MD, Lisa Doherty, MD, MPH, C. Suzanne
Supplementary Online Content
 Supplementary Online Content Tangri N, Stevens LA, Griffith J, et al. A predictive model for progression of chronic kidney disease to kidney failure. JAMA. 2011;305(15):1553-1559. eequation. Applying the
Supplementary Online Content Tangri N, Stevens LA, Griffith J, et al. A predictive model for progression of chronic kidney disease to kidney failure. JAMA. 2011;305(15):1553-1559. eequation. Applying the

 www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to
www.usrds.org www.usrds.org 1 1,749 + (2,032) 1,563 to