ABSTRACT. n engl j med 361;21 nejm.org november 19,
|
|
|
- Helen Cooper
- 6 years ago
- Views:
Transcription
1 The new england journal of medicine established in 1812 november 19, 2009 vol. 361 no. 21 A Trial of Darbepoetin Alfa in Type 2 Diabetes and Chronic Kidney Disease Marc A. Pfeffer, M.D., Ph.D., Emmanuel A. Burdmann, M.D., Ph.D., Chao-Yin Chen, Ph.D., Mark E. Cooper, M.D., Dick de Zeeuw, M.D., Ph.D., Kai-Uwe Eckardt, M.D., Jan M. Feyzi, M.S., Peter Ivanovich, M.D., Reshma Kewalramani, M.D., Andrew S. Levey, M.D., Eldrin F. Lewis, M.D., M.P.H., Janet B. McGill, M.D., John J.V. McMurray, M.D., Patrick Parfrey, M.D., Hans-Henrik Parving, M.D., Giuseppe Remuzzi, M.D., Ajay K. Singh, M.D., Scott D. Solomon, M.D., and Robert Toto, M.D., for the TREAT Investigators* ABSTRACT BACKGROUND Anemia is associated with an increased risk of cardiovascular and renal events among patients with type 2 diabetes and chronic kidney disease. Although darbepoetin alfa can effectively increase hemoglobin levels, its effect on clinical outcomes in these patients has not been adequately tested. METHODS In this study involving 4038 patients with diabetes, chronic kidney disease, and anemia, we randomly assigned 2012 patients to darbepoetin alfa to achieve a hemoglobin level of approximately 13 g per deciliter and 2026 patients to placebo, with rescue darbepoetin alfa when the hemoglobin level was less than 9.0 g per deciliter. The primary end points were the composite outcomes of death or a cardiovascular event (nonfatal myocardial infarction, congestive heart failure, stroke, or hospitalization for myocardial ischemia) and of death or end-stage renal disease. RESULTS Death or a cardiovascular event occurred in 632 patients assigned to darbepoetin alfa and 602 patients assigned to placebo (hazard ratio for darbepoetin alfa vs. placebo, 1.05; 95% confidence interval [CI], 0.94 to 1.17; P = 0.41). Death or end-stage renal disease occurred in 652 patients assigned to darbe poetin alfa and 618 patients assigned to placebo (hazard ratio, 1.06; 95% CI, 0.95 to 1.19; P = 0.29). Fatal or nonfatal stroke occurred in 101 patients assigned to darbepoetin alfa and 53 patients assigned to placebo (hazard ratio, 1.92; 95% CI, 1.38 to 2.68; P<0.001). Red-cell transfusions were administered to 297 patients assigned to darbepoetin alfa and 496 patients assigned to placebo (P<0.001). There was only a modest improvement in patient-reported fatigue in the darbepoetin alfa group as compared with the placebo group. CONCLUSIONS The use of darbepoetin alfa in patients with diabetes, chronic kidney disease, and moderate anemia who were not undergoing dialysis did not reduce the risk of either of the two primary composite outcomes (either death or a cardiovascular event or death or a renal event) and was associated with an increased risk of stroke. For many persons involved in clinical decision making, this risk will outweigh the potential benefits. (ClinicalTrials.gov number, NCT ) The affiliations of the authors are listed in the Appendix. Address reprint requests to Dr. Pfeffer at the Cardiovascular Division, Brigham and Women s Hospital, 75 Francis St., Boston, MA 02115, or at mpfeffer@rics.bwh.harvard.edu. *The Trial to Reduce Cardiovascular Events with Aranesp Therapy (TREAT) committees and teams are listed in the Appendix, and investigators and individual sites are listed in the Supplementary Appendix, available with the full text of this article at NEJM.org. This article ( /NEJMoa ) was published on October 30, 2009, at NEJM.org. N Engl J Med 2009;361: Copyright 2009 Massachusetts Medical Society. n engl j med 361;21 nejm.org november 19,
2 The new england journal of medicine Type 2 diabetes mellitus and chronic kidney disease frequently coexist, and each disease independently increases the risk of cardiovascular events and end-stage renal disease. 1,2 Intensive treatment of concomitant conventional risk factors such as hypertension and elevated levels of low-density lipoprotein reduces fatal and nonfatal cardiovascular complications and slows the progression of kidney disease. 3-8 Observational studies suggest that anemia can be considered another biomarker of risk, since a lower hemoglobin level is independently associated with a higher rate of cardiovascular and renal events, 9-11 especially among patients with diabetes. 12,13 Whether the use of erythropoiesisstimulating agents (ESAs) to increase hemoglobin levels lowers this risk is not known. 14 Early studies involving the use of recombinant human erythropoietin in patients with severe anemia who were undergoing dialysis showed a reduced requirement for blood transfusions and improved quality-of-life assessments, which were considered major advances. 15,16 Extrapolations from these favorable effects to other populations, including patients with anemia and earlier stages of chronic kidney disease, led to the wider use of ESAs. The presumption of the benefits associated with the use of ESAs was so pervasive that major clinical trials considered the use of placebo unnecessary or even unethical In fact, there were no placebo-controlled trials in a recent meta-analysis of the use of ESAs in patients with chronic kidney disease. 20 Although ESAs have been available for more than two decades, the hypothesis that this treatment approach would lower the risks associated with anemia and improve the prognosis has not been examined. 21 We conducted the Trial to Reduce Cardiovascular Events with Aranesp Therapy (TREAT) to test the hypothesis that, in patients with type 2 diabetes, chronic kidney disease that does not require dialysis, and concomitant anemia, increasing hemoglobin levels with the use of this agent would lower the rates of death, cardiovascular events, and end-stage renal disease. 22 Methods The TREAT was a randomized, double-blind, placebo-controlled trial conducted at 623 sites in 24 countries (see the Supplementary Appendix, available with the full text of this article at NEJM. org). The institutional review board or ethics committee at each site approved the protocol, and all patients provided written informed consent. Enrollment occurred from August 25, 2004, through December 4, The trial was sponsored by Amgen and designed in collaboration with an academic executive committee. Data collection and management were the responsibility of the sponsor, with oversight by the executive committee. The Statistical Data Analysis Center at the University of Wisconsin prepared the interim unblinded reports for the independent data and safety monitoring committee, which oversaw patient safety and the quality of trial conduct. The independent academic statistical center also performed all analyses for this article and provided the writing group with unrestricted access to the data. The manuscript was prepared by the principal investigator and subsequently revised and edited by all the authors. All the authors decided to submit the article for publication and assume responsibility for the accuracy and completeness of the reported data. Study Population Patients with type 2 diabetes, chronic kidney disease (an estimated glomerular filtration rate [GFR] of 20 to 60 ml per minute per 1.73 m 2 of bodysurface area, calculated with the use of the fourvariable Modification of Diet in Renal Disease formula), anemia (hemoglobin level, 11.0 g per deciliter), and a transferrin saturation of 15% or more were eligible for enrollment. Patients with any of the following factors were excluded: uncontrolled hypertension; previous kidney transplantation or scheduled receipt of a kidney transplant from a living related donor; current use of intravenous antibiotics, chemotherapy, or radiation therapy; cancer (except basal-cell or squamouscell carcinoma of the skin); diagnosed human immunodeficiency virus infection; active bleeding; a hematologic disease; or pregnancy. Patients who had had a cardiovascular event or grand mal seizure, had undergone major surgery, or had received an ESA in the 12 weeks before randomization were also ineligible. Study Procedures During a 2-week screening period, prestudy laboratory assessments were obtained and the eligibility of patients who had provided consent was confirmed. Patients were randomly assigned with the use of a computer-generated, permuted-block 2020 n engl j med 361;21 nejm.org november 19, 2009
3 Darbepoetin Alfa Therapy for reduction of Cardiovascular Events design, in a 1:1 ratio, to receive darbepoetin alfa (Aranesp, Amgen) or placebo. Randomization was stratified according to the study site, the baseline level of proteinuria (with marked proteinuria defined as a ratio of total protein to creatinine [calculated in milligrams per deciliter] of 1.0 in a spot urine sample), and an investigator-designated history of cardiovascular disease. Darbepoetin alfa and placebo were supplied in matching prefilled syringes at 12 different strengths. A third party used a point-of-care device to monitor hemoglobin levels and enter the value into an interactive voice-response system that selected the dosage according to a computer algorithm (see the Supplementary Appendix). This algorithm was designed to adjust the dose in order to maintain the hemoglobin level at approximately 13.0 g per deciliter in the patients assigned to darbepoetin alfa. Patients in the placebo group were assigned to receive darbepoetin alfa as a rescue agent if the hemoglobin level fell below 9.0 g per deciliter, with a return to placebo once the hemoglobin level was 9.0 g per deciliter or higher. The site investigator was to be notified if any patient had a hemoglobin value of 7.0 g per deciliter or less, a value of 16.0 g per deciliter or more, or a decrease of 2.0 g per deciliter or more in a 4-week period. Measurements of hemoglobin levels and vital signs were performed every 2 weeks during the study-drug titration period and monthly thereafter. Transferrin saturation and ferritin levels were measured quarterly; other laboratory assessments and spot urine collections were performed at 24-week intervals. Patient-reported outcomes and health resource utilization were assessed at weeks 1, 13, and 25 and every 24 weeks thereafter. At each visit, information was gathered regarding adverse events, hospitalization, transfusions, and the concomitant use of other medications. Evaluation of Outcomes The primary end points were the time to the composite outcome of death from any cause or a cardiovascular event (nonfatal myocardial infarction, congestive heart failure, stroke, or hospitalization for myocardial ischemia) and the time to the composite outcome of death or end-stage renal disease (see the Supplementary Appendix). The overall alpha level for the primary end points was split: for the cardiovascular composite outcome and for the renal composite outcome. All potential end points were adjudicated by a clinical end-point committee whose members were unaware of the treatment assignments, and the hematocrit and hemoglobin values were redacted from the documents under review. Important secondary end points included time to death, death from cardiovascular causes, and the components of the primary end points, as well as the rate of decline in the estimated GFR and changes in patient-reported outcomes at week 25 measured with the use of the Functional Assessment of Cancer Therapy Fatigue (FACT-Fatigue) instrument (on which scores range from 0 to 52, with higher scores indicating less fatigue) and the 36-Item Short-Form General Health Survey questionnaire (calculated with norm-based scoring so that 50 is the average score, with higher scores indicating a better quality of life) (added after the second protocol amendment in May 2005). Monitoring The independent data and safety monitoring committee reviewed safety reports monthly with formal interim analyses scheduled when approximately 20, 40, 60, and 80% of the total expected cardiovascular composite events had occurred. Initial guidelines for early discontinuation included a symmetric O Brien Fleming alpha-spending function. In April 2006, data from a non placebo-controlled trial of a different ESA in patients with chronic kidney disease showed that treatment aimed at achieving a higher hemoglobin level (13.5 g per deciliter vs g per deciliter) was associated with increased rates of adverse clinical events. 17 This information and more equivocal results from a related, smaller trial 18 were proactively communicated to our patients, investigators, and the data and safety monitoring committee. The committee made no recommendation to alter or terminate the study on the basis of interim data that already reflected more clinical events than the numbers of events in these related trials. The consent form was modified with the addition of the new information regarding potential harm, and all study participants were asked to provide written informed consent again. The executive committee requested that the data and safety monitoring committee adopt a more cautious stopping rule, with the use of a one-sided alpha of 0.05 for harm at each assessment (without adjustment for multiple testing) for either the cardiovascular composite outcome or death. The boundaries for efficacy remained unchanged, and with this new mandatory stop- n engl j med 361;21 nejm.org november 19,
4 The new england journal of medicine ping rule for harm, the committee made no recommendation to terminate the trial before its scheduled conclusion. Statistical Analysis The trial was event driven, with a total of 1203 cardiovascular composite events required to provide 80% statistical power to detect a 20% risk reduction for this outcome, with a two-sided type I error of (unadjusted for interim analyses). We aimed to enroll approximately 4000 patients; assumptions included an annualized rate of events in the placebo group of 12.5%, a 15% loss to follow-up, and attenuation of the treatment effect due to the anticipated use of ESAs in patients who had progression to end-stage renal disease. Time-to-event analyses were performed with the use of life-table methods according to the intention-to-treat principle. Kaplan Meier cumulative incidence curves were compared with the use of a two-sided log-rank test, stratified according to the baseline proteinuria level and the presence or absence of a history of cardiovascular disease. Estimated hazard ratios (for darbepoetin alfa vs. placebo) and 95% confidence intervals were obtained with the use of stratified Cox proportional-hazards models. Patients who discontinued either study drug early, including patients who began treatment with dialysis or underwent transplantation, were followed for study end points. Categorization of adverse events was based on groupings of preferred terms defined by the standardized queries in the Medical Dictionary for Regulatory Activities. 23 Analyses of patientreported outcomes were prespecified to impute missing data with the last-observation-carriedforward method and to use t-tests for treatment comparisons, with means and standard deviations. Reported P values are nominal and have not been adjusted for multiple comparisons. Additional statistical methods are described in the Supplementary Appendix. Results Patients We enrolled a total of 4047 patients, but before unblinding, we excluded all information regarding 9 patients from two sites that did not adhere to Good Clinical Practice guidelines (4 patients who were randomly assigned to darbepoetin alfa and 5 patients who were randomly assigned to placebo). Of the 4038 patients evaluated, 2012 were assigned to receive darbepoetin alfa and 2026 were assigned to receive placebo. The study was event driven and was completed on March 28, 2009, with a median follow-up duration of 29.1 months. At that time, 3523 patients (87.2%) were either still being followed for clinical end points or had died; this group included 1761 patients in the darbepoetin alfa group (87.5%) and 1762 patients in the placebo group (87.0%). The vital status at study termination was unknown for 153 patients in the darbepoetin alfa group (7.6%) and 164 in the placebo group (8.1%) (see the Consolidated Standards for the Reporting of Trials [CONSORT] diagram in the Supplementary Appendix). The median age was 68 years, and 57.3% of the patients were women; 65.4% of the patients had a history of cardiovascular disease, with similar percentages of patients in each group reporting a history of coronary artery disease, stroke, peripheral arterial disease, and myocardial infarction. There was an imbalance in the proportion of patients with a history of heart failure (31.5% in the darbepoetin alfa group vs. 35.2% in the placebo group, unadjusted P = 0.01). There were no clinically meaningful baseline imbalances in vital signs, laboratory data, or the use of medications for cardiovascular disease and diabetes (Table 1). Intervention and Hemoglobin Values The overall median hemoglobin level at baseline was 10.4 g per deciliter (interquartile range, 9.8 to 10.9). Between-group differences in hemoglobin values were apparent less than 1 month after randomization, and the differences were significant by 1 month (Fig. 1). From 3 months to the end of treatment, the median achieved hemoglobin level (based on the area under the curve) was 12.5 g per deciliter (interquartile range, 12.0 to 12.8) in the darbepoetin alfa group and 10.6 g per deciliter (interquartile range, 9.9 to 11.3) in the placebo group (P<0.001) (Fig. 1). A total of 84.6% of patients in the darbepoetin alfa group and 86.9% of patients in the placebo group were switched to monthly dosing. Over the course of the study, 46% of the patients assigned to placebo received at least one dose of darbepoetin alfa as rescue therapy. The median monthly dose in patients assigned to placebo was 0 μg (interquartile range, 0 to 5) as compared with 176 μg (interquartile range, 104 to 305) in patients assigned to darbe n engl j med 361;21 nejm.org november 19, 2009
5 Darbepoetin Alfa Therapy for reduction of Cardiovascular Events Table 1. Baseline Characteristics of the Patients.* Characteristic Darbepoetin Alfa (N = 2012) (N = 2026) P Value Age (yr) 0.22 Median Interquartile range Female sex (%) Race or ethnic group (%) 0.84 White Black Hispanic Other Known duration of diabetes (yr) 0.94 Median Interquartile range Body-mass index 0.11 Median Interquartile range Retinopathy (%) Laser treatment (%) Diabetic neuropathy (%) Amputation History of cardiovascular disease (%) Coronary artery disease Heart failure Myocardial infarction Stroke Peripheral arterial disease** Use of pacemaker Use of automatic implantable cardioverter defibrillator Atrial fibrillation (%) Smoking status (%) 0.88 Current smoker Former smoker Blood pressure (mm Hg) Systolic 0.25 Median Interquartile range Diastolic 0.55 Median Interquartile range Serum creatinine (mg/dl) 0.01 Median Interquartile range Estimated GFR (ml/min/1.73 m 2 ) 0.03 Median Interquartile range n engl j med 361;21 nejm.org november 19,
6 The new england journal of medicine Table 1. (Continued.) Characteristic Darbepoetin Alfa (N = 2012) (N = 2026) P Value Ratio of total protein (in mg/dl) to creatinine (in mg/dl) in urine 0.73 Median Interquartile range <1 (%) (%) Potassium (mmol/liter) 0.73 Median Interquartile range Albumin (g/dl) 0.13 Median Interquartile range Glycated hemoglobin (%) 0.02 Median Interquartile range Hemoglobin (g/dl) 0.15 Median Interquartile range White-cell count ( 10 9 /liter) 0.32 Median Interquartile range Platelet count ( 10 9 /liter) 0.14 Median Interquartile range Transferrin saturation (%) 0.80 Median Interquartile range Serum ferritin (µg/liter) 0.17 Median Interquartile range Cholesterol (mg/dl) Total 0.47 Median Interquartile range LDL 0.41 Median Interquartile range HDL 0.85 Median Interquartile range Triglycerides (mg/dl) 0.97 Median Interquartile range n engl j med 361;21 nejm.org november 19, 2009
7 Darbepoetin Alfa Therapy for reduction of Cardiovascular Events Table 1. (Continued.) Characteristic Medications (%) Darbepoetin Alfa (N = 2012) (N = 2026) P Value Insulin Oral hypoglycemic agent Thiazolidinedione Sulfonamide Biguanide Angiotensin-converting enzyme inhibitor or angiotensinreceptor blocker Angiotensin-converting enzyme inhibitor and angiotensinreceptor blocker Beta-blocker Aldosterone-receptor blocker Statin Statin or other lipid-lowering agent Aspirin Aspirin or other antiplatelet agent Vitamin K antagonist Iron Oral Intravenous Previous use of erythropoietic agent * All tests for baseline laboratory values were performed by a central laboratory except hemoglobin levels, which were measured at the site with the use of a hemoglobin point-of-care device. GFR denotes glomerular filtration rate, HDL high-density lipoprotein, and LDL low-density lipoprotein. To convert the values for cholesterol to millimoles per liter, multiply by To convert the values for triglycerides to millimoles per liter, multiply by P values have not been adjusted for multiple comparisons. Race or ethnic group was self-reported. The body-mass index is the weight in kilograms divided by the square of the height in meters. These data were derived from the clinical database. This category includes coronary artery disease with or without myocardial infarction, coronary-artery bypass grafting, and percutaneous coronary intervention. ** This category includes peripheral arterial disease with or without peripheral arterial revascularization. poetin alfa. Among the patients who had not died or progressed to end-stage renal disease, 93.9% of the patients in the darbepoetin alfa group and 90.4% of those in the placebo group were receiving the assigned treatment at 6 months; 87.4% and 83.7%, respectively, at 1 year; and 74.3% and 69.3%, respectively, at 2 years. There was no significant difference in the proportions of patients receiving oral iron during the study (66.8% of those in the darbepoetin alfa group and 68.6% of those in the placebo group, P = 0.25); however, more patients in the placebo group received intravenous iron (20.4%, vs. 14.8% of patients assigned to darbepoetin alfa; P<0.001). Red-cell transfusions were administered in 297 patients in the darbepoetin alfa group (14.8%) and in 496 patients in the placebo group (24.5%) (hazard ratio for darbepoetin alfa vs. placebo, 0.56; 95% confidence interval [CI], 0.49 to 0.65; P<0.001). Primary Composite Outcomes and Components Death, Myocardial Infarction, Unstable Angina, Heart Failure, and Stroke The primary cardiovascular composite outcome death or a nonfatal cardiovascular event occurred in 632 patients in the darbepoetin alfa group (31.4%) and in 602 patients in the placebo group (29.7%) (hazard ratio for darbepoetin alfa vs. placebo, 1.05; 95% CI, 0.94 to 1.17; P = 0.41) (Table 2 and Fig. 2A). There were no significant n engl j med 361;21 nejm.org november 19,
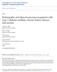
8 The new england journal of medicine Mean Hemoglobin (g/dl) No. of Patients Figure 1. Mean Hemoglobin Levels through 48 Months among Patients Who Were Assigned to Receive Darbepoetin Alfa or. I bars represent standard errors. between-group differences in the time to the first occurrence of the following components, when considered individually: death from any cause, fatal or nonfatal congestive heart failure, fatal or nonfatal myocardial infarction, or hospitalization for myocardial ischemia (Table 2 and Fig. 2B, 2C, and 2D). However, fatal or nonfatal stroke was more likely to occur in the patients assigned to darbepoetin alfa (101 patients [5.0%] vs. 53 patients [2.6%]; hazard ratio, 1.92; 95% CI, 1.38 to 2.68; P<0.001) (Table 2 and Fig. 2E). The prespecified stratification characteristics of a history of cardiovascular disease and marked proteinuria (urinary protein-to-creatinine ratio, 1) both identified higher-risk groups regardless of the assigned treatment for the cardiovascular composite outcome. The overall null effect of darbepoetin alfa was observed in each subgroup, with no significant interaction. Similarly, there were no significant interactions for any of the other five prespecified subgroups based on age, sex, race or ethnic group, region, or baseline estimated GFR (see the Supplementary Appendix). Cardiac revascularization procedures were performed less frequently in the patients assigned to darbepoetin alfa than in those assigned to placebo (84 patients [4.2%] vs. 117 patients [5.8%]; hazard ratio, 0.71; 95% CI, 0.54 to 0.94; P = 0.02). Renal Outcomes Death or end-stage renal disease occurred in 652 patients in the darbepoetin alfa group (32.4%) and in 618 patients in the placebo group (30.5%) (hazard ratio for darbepoetin alfa vs. placebo, 1.06; 95% CI, 0.95 to 1.19; P = 0.29) (Fig. 3A). Endstage renal disease occurred in 338 patients in the darbepoetin alfa group (16.8%) and in 330 patients assigned to placebo (16.3%) (hazard ratio, 1.02; 95% CI, 0.87 to 1.18; P = 0.83) (Fig. 3B). The stratification characteristics of a history of cardiovascular disease and marked proteinuria also identified groups at higher risk for the composite outcome of death or end-stage renal disease, with no significant interaction in either subgroup. No significant interactions were observed in the other five prespecified subgroups, with the exception of a nominally significant interaction for race or ethnic group. The 653 patients described as nonwhite and nonblack in the darbepoetin alfa group had the greatest excess risk (hazard ratio, 1.46; 95% CI, 1.10 to 2026 n engl j med 361;21 nejm.org november 19, 2009
9 Darbepoetin Alfa Therapy for reduction of Cardiovascular Events Table 2. Composite and Component End Points.* End Point Primary end points Darbepoetin Alfa (N = 2012) number (percent) (N = 2026) Hazard Ratio (95% CI) P Value Cardiovascular composite end point 632 (31.4) 602 (29.7) 1.05 ( ) 0.41 Death from any cause 412 (20.5) 395 (19.5) 1.05 ( ) 0.48 Myocardial infarction 124 (6.2) 129 (6.4) 0.96 ( ) 0.73 Stroke 101 (5.0) 53 (2.6) 1.92 ( ) <0.001 Heart failure 205 (10.2) 229 (11.3) 0.89 ( ) 0.24 Myocardial ischemia 41 (2.0) 49 (2.4) 0.84 ( ) 0.40 Renal composite end point (ESRD or death) 652 (32.4) 618 (30.5) 1.06 ( ) 0.29 ESRD 338 (16.8) 330 (16.3) 1.02 ( ) 0.83 Additional adjudicated end points Death from cardiovascular causes 259 (12.9) 250 (12.3) 1.05 ( ) 0.61 Cardiac revascularization 84 (4.2) 117 (5.8) 0.71 ( ) 0.02 * ESRD denotes end-stage renal disease. P values have not been adjusted for multiple comparisons. A patient may have had multiple cardiovascular events of different types. The cardiovascular composite end point reflects only the first occurrence of any of the components. This category includes both fatal and nonfatal events. 1.95); among the 2570 white patients, the hazard ratio was 1.05 (95% CI, 0.92 to 1.21), and among the 815 black patients, the hazard ratio was 0.87 (95% CI, 0.68 to 1.10; P = 0.03 for the interaction, uncorrected for multiple comparisons). Patient-Reported Outcomes The primary prespecified analysis for the patientreported outcomes was the change from baseline to 25 weeks in the FACT-Fatigue score. Among patients with both baseline and week-25 scores, from a baseline score of 30.2 in the group of 1762 patients assigned to darbepoetin alfa and a baseline score of 30.4 in the 1769 patients assigned to placebo, there was a greater degree of improvement in the mean (±SD) score in the darbepoetin alfa group than in the placebo group (an increase of 4.2±10.5 points vs. 2.8±10.3 points, P<0.001 for between-group changes). An increase of three or more points (considered to be a clinically meaningful improvement) occurred in 963 of 1762 patients assigned to darbepoetin alfa (54.7%) and 875 of 1769 patients assigned to placebo (49.5%) (P = 0.002). Other prespecified quality-of-life assessments, in the domains of energy and physical functioning as measured with the 36-Item Short-Form General Health Survey, did not differ significantly between 1138 patients assigned to darbepoetin alfa and 1157 patients assigned to placebo (mean change in the score for energy, 2.6±9.9 points vs. 2.1±9.7 points; P = 0.20; mean change in the score for physical functioning, 1.3±9.2 vs. 1.1±8.8; P = 0.51). Blood Pressure There was no significant difference in systolic blood pressure between the two groups; the median systolic blood pressure over time was 134 mm Hg (interquartile range, 126 to 143) in both groups. Diastolic blood pressure was higher in the patients assigned to darbepoetin alfa than in those assigned to placebo (median over time, 73 mm Hg [interquartile range, 67 to 78] vs. 71 mm Hg [interquartile range, 65 to 77]; P<0.001). Prespecified Categories of Adverse Events Hypertension occurred in 491 patients in the darbepoetin alfa group and in 446 patients in the placebo group (P = 0.07) (see the Supplementary Appendix). Convulsions were reported in nine patients in the darbepoetin alfa group and in four patients in the placebo group. No cases of antibody-mediated pure red-cell aplasia were reported in either group. n engl j med 361;21 nejm.org november 19,
10 The new england journal of medicine A Cardiovascular Composite End Point Hazard ratio, 1.05 (95% CI, ) P=0.41 Patients with Event (%) Patients with Event (%) No. at Risk B Death from Any Cause No. at Risk Hazard ratio, 1.05 (95% CI, ) P= C Fatal or Nonfatal Congestive Heart Failure Hazard ratio, 0.89 (95% CI, ) P=0.24 Patients with Event (%) No. at Risk D Fatal or Nonfatal Myocardial Infarction and Myocardial Ischemia P=0.73 E Fatal or Nonfatal Stroke Hazard ratio, 1.92 (95% CI, ) P<0.001 Patients with Event (%) Patients with Event (%) No. at Risk Fatal or Nonfatal Myocardial Infarction Myocardial Ischemia Fatal or Nonfatal Myocardial Infarction Hazard ratio, 0.96 (95% CI, ) P= Myocardial Ischemia Hazard ratio, 0.84 (95% CI, ) No. at Risk n engl j med 361;21 nejm.org november 19, 2009
11 Darbepoetin Alfa Therapy for reduction of Cardiovascular Events Figure 2 (facing page). Kaplan Meier Estimates of the Probability of the Primary and Secondary End Points. Panel A shows the primary cardiovascular composite end point. The secondary end points of deaths from any cause (Panel B), fatal or nonfatal congestive heart failure (Panel C), fatal or nonfatal myocardial infarction and myocardial ischemia (Panel D), and fatal or nonfatal stroke (Panel E) are also shown. P values are not adjusted for multiple comparison. Venous thromboembolic events were reported in 41 patients in the darbepoetin alfa group (2.0%), as compared with 23 patients in the placebo group (1.1%) (P = 0.02). Arterial thromboembolic events (some of which were adjudicated as cardiovascular events) were also reported more frequently in the darbepoetin alfa group (in 178 patients [8.9%] vs. 144 patients [7.1%], P = 0.04). Cancer There was no significant between-group difference in the number of patients reporting a cancerrelated adverse event: 139 in the darbepoetin alfa group (6.9%) and 130 in the placebo group (6.4%) (P = 0.53). Overall, 39 deaths were attributed to cancer in the 2012 patients in the darbepoetin alfa group and 25 deaths were attributed to cancer in the 2026 patients in the placebo group (P = 0.08 by the log-rank test). Among patients with a history of a malignant condition at baseline, there were 60 deaths from any cause in the 188 patients assigned to darbepoetin alfa and 37 deaths in the 160 patients assigned to placebo (P = 0.13 by the log-rank test). In this subgroup, 14 of the 188 patients assigned to darbepoetin alfa died from cancer, as compared with 1 of the 160 patients assigned to placebo (P = by the log-rank test). Discussion The main purpose of the TREAT was to determine whether treatment of a low hemoglobin level with darbepoetin alfa would reduce the risk of death and major cardiovascular and renal events among patients with type 2 diabetes mellitus, chronic kidney disease, and anemia. There was no significant difference in the overall rates of either the primary cardiovascular composite end point or the primary renal composite end point with the use of the therapeutic strategy of increasing the hemoglobin level with darbepoetin alfa (to attempt to reach a target hemoglobin level of 13.0 g per deciliter) versus placebo (with darbepoetin alfa as rescue therapy if hemoglobin values decreased below 9.0 g per deciliter). In this study involving 4038 patients randomly assigned to a study group, with 9941 patient-years of follow-up and with 1234 patients who had a composite outcome of a cardiovascular event and 1270 patients who had a composite outcome of a renal event, we found no overall significant differences in the hazard rates for these clinically important outcomes or in the rates of death, heart failure, myocardial infarction, admission for myocardial ischemia, or end-stage renal disease. Although there was no significant increase in the overall cardiovascular composite outcome in the group assigned to darbepoetin alfa, there was an increased incidence of stroke (annualized event rate, 2.1%, vs. 1.1% in the placebo group). Data from a study of patients undergoing dialysis suggested this risk of stroke 19 ; however, this risk was not identified in either the Correction of Hemoglobin and Outcomes in Renal Insufficiency (CHOIR) study (ClinicalTrials.gov number, NCT ) 17 or a meta-analysis. 24 This previously undocumented and clinically important finding of a heightened risk of stroke is not explained by an increase in systolic blood pressure. In a recent report of a randomized, placebo-controlled trial of intravenous erythropoietin in the early phase of an acute ischemic stroke, 25 there were more deaths in the group assigned to the ESA (42 of 256 patients [16.4%]) as compared with the group assigned to placebo (24 of 266 patients [9.0%]). This study also provides support for an adverse relationship between ESAs and stroke. We also confirmed previous findings of increased rates of venous thromboembolic events among patients treated with ESAs. Our findings appear to differ from those of the CHOIR trial, the next largest trial involving patients with chronic kidney disease who were not undergoing dialysis, which used epoetin alfa and was discontinued prematurely after a median follow-up of 16 months and after 222 patients had a primary event. 17 Both groups in the CHOIR trial were randomly assigned to receive epoetin alfa, and in that study, there was a higher risk of cardiovascular events in the group assigned to a target hemoglobin level of 13.5 g per deciliter than in the group assigned to a target level of 11.3 g per deciliter (hazard ratio, 1.34; 95% CI, 1.03 to 1.74; P = 0.03). This excess of cardiovas- n engl j med 361;21 nejm.org november 19,
12 The new england journal of medicine A Renal Composite (ESRD or Death) Patients with Event (%) Hazard ratio, 1.06 (95% CI, ) 30 P= No. at Risk B ESRD Patients with Event (%) Hazard ratio, 1.02 (95% CI, ) P=0.83 No. at Risk Figure 3. Kaplan Meier Estimates of the Probability of Renal Outcomes. Panel A shows the primary renal composite end point (end-stage renal disease [ESRD] or death), and Panel B shows the end-point component of ESRD. P values have not been adjusted for multiple comparisons. cular events was largely accounted for by more deaths and heart-failure events; only 12 patients in each group had a stroke. These findings led to the suggestion that our trial should be discontinued. 26 However, by that time, there were more accumulated cardiovascular composite events in our trial than in the CHOIR trial, and the independent data and safety monitoring committee recommended continuation. 27 The TREAT executive committee updated the consent form to reflect the results from the CHOIR trial, and our patients again were asked to provide written informed consent. The final results of our study demonstrate the importance of completing the planned follow-up of trials and the potential to draw misleading conclusions when premature discontinuation results in an insufficient number of events to allow for a reliable estimation of the effect of treatment. 28,29 Before we conducted our study, there was a suggestion that ESAs might increase mortality among patients with cancer, so patients with an active malignant condition were excluded from our trial. 30 During the trial, mounting concern led to new regulatory warnings about the use of ESAs in patients with anemia of cancer, 31 prompting a protocol amendment to discontinue the study drug in patients in whom cancer developed. Al n engl j med 361;21 nejm.org november 19, 2009
13 Darbepoetin Alfa Therapy for reduction of Cardiovascular Events though the number of these patients did not differ significantly between the study groups, among the 348 patients with a history of cancer at baseline, mortality was higher among those assigned to darbepoetin alfa than among those assigned to placebo; these findings are consistent with those in a recent meta-analysis. 32 Our trial provides long-term, placebo-controlled data on the use of ESAs in patients with diabetes, chronic kidney disease, and moderate anemia who are not undergoing dialysis. No single trial can address the multitude of pertinent issues without limitations, and our data may not be fully applicable to other patient populations. It is possible that other dosing strategies could be developed to mitigate the risk of stroke while conserving the modest benefits of treatment. In light of the baseline imbalances between the study groups, additional sensitivity analyses were conducted, and they did not alter our results. More extensive analyses of the patient-reported outcome measures are needed to assess the durability of the rather modest improvement we observed only in the FACT-Fatigue score. The long-standing presumption of a benefit of ESAs in this patient population led to non placebo-controlled trials, which, by design, cannot provide a reliable assessment of risk and benefit. 21 The present trial supplies these missing data, which may assist physicians and patients in making more informed decisions about individual care. It is our view that, in many patients with diabetes, chronic kidney disease, and moderate anemia who are not undergoing dialysis, the increased risk of stroke and possibly death among patients with a history of a malignant condition will outweigh any potential benefit of an ESA. Supported by Amgen, which provided independent statistical support through a contract with the board of regents for the University of Wisconsin System for data analysis for the TREAT Data and Safety Monitoring Committee as well as for the study. Dr. Pfeffer reports receiving consulting fees from Abbott, Amgen, AstraZeneca, Biogen, Boehringer Ingelheim, Boston Scientific, Bristol-Myers Squibb, Centocor, CVRx, Genentech, Cytokinetics, Daiichi Sankyo, Genzyme, Medtronic, Novartis, Roche, Sanofi-Aventis, Servier, and VIA Pharmaceutics and grant support from Amgen, Baxter, Celladon, Novartis, and Sanofi- Aventis, and being named coinventor on a patent for the use of inhibitors of the renin angiotensin system in selected survivors of myocardial infarction; Dr. Burdmann, receiving consulting fees from Amgen and Sigma Pharma and grant support from Amgen and Roche; Drs. Chen and Kewalramani, being employees of and owning stock in Amgen; Dr. Cooper, receiving consulting fees from Amgen; Dr. de Zeeuw, receiving consulting fees from Amgen and Novartis and lecture fees from Amgen; Dr. Eckardt, receiving consulting fees from Amgen, Ortho Biotech, Roche, Affymax, Stada, and Sandoz Hexal and lecture fees from Amgen, Ortho Biotech, and Roche; Dr. Ivanovich, receiving consulting fees from Amgen, Baxter, Biogen, and Reata; Dr. Levey, receiving grant support from Amgen; Dr. Lewis, receiving consulting fees from Amgen and grant support from Amgen and the Robert Wood Johnson Foundation; Dr. McGill, receiving consulting fees from Amgen and Boehringer Ingelheim, lecture fees from Novartis, and grant support from Novartis and Boehringer Ingel heim; Dr. McMurray, receiving consulting fees from Menarini, Bristol-Myers Squibb, Roche, Novocardia, Boehringer Ingelheim, Novartis, BioMérieux, and Boston Scientific, lecture fees from AstraZeneca, Solvay, Takeda, Novartis, BMS Sanofi, and Vox Media, and grant support from BMS, Novartis, Amgen, AstraZeneca, Cytokinetics, Hoffmann La Roche, Pfizer, Scios, and GlaxoSmithKline; Dr. Parfrey, receiving consulting and lecture fees from Amgen and lecture fees from Ortho Biotech; Dr. Parving, receiving consulting fees from Amgen and Novartis and lecture fees from Novartis; Dr. Singh, receiving consulting fees from Johnson & Johnson and Watson, lecture fees from Johnson & Johnson, Amgen, and Watson, and grant support from Johnson & Johnson, Amgen, Roche, AMAG Pharmaceuticals, and Watson; Dr. Solomon, receiving grant support from Amgen; and Dr. Toto, receiving consulting and lecture fees from Amgen and grant support from Novartis, Reata, and Abbott. No other potential conflict of interest relevant to this article was reported. Appendix From the Department of Medicine, Brig ham and Women s Hospital, Harvard Medical School (M.A.P., E.F.L., A.K.S., S.D.S.); and the Division of Nephrology, Tufts Medical Center (A.S.L.) both in Boston; Hospital de Base, Faculdade de Medicina de São José do Rio Preto, São José do Rio Preto, Brazil (E.A.B.); Global Biostatistics and Epidemiology and Global Clinical Development, Amgen, Thousand Oaks, CA (C.-Y.C., R.K.); Baker Heart Research Institute, Melbourne, VIC, Australia (M.E.C.); the Division of Clinical Pharmacology, University Medical Center, Groningen, the Netherlands (D.Z.); the Department of Nephrology and Hypertension, University of Erlangen-Nuremberg, Erlangen, Germany (K.-U.E.); the Department of Biostatistics and Medical Informatics, University of Wisconsin, Madison (J.M.F.); the Department of Medicine, Northwestern University Feinberg School of Medicine, Chicago (P.I.); the Department of Medicine, Washington University School of Medicine, St. Louis (J.B.M.); the Department of Cardiology, British Heart Foundation Glasgow Cardiovascular Research Centre, Glasgow, United Kingdom (J.J.V.M.); the Division of Nephrology, Health Sciences Centre, St. John s, NF, Canada (P.P.); the Department of Medical Endocrinology, Rigshospitalet, University of Copenhagen, Copenhagen, and Faculty of Health Science, Aarhus University, Aarhus (H.-H.P.) both in Denmark; Mario Negri Institute for Pharmacological Research, Bergamo, Italy (G.R.); and the Department of Medicine, University of Texas Southwestern Medical Center, Dallas (R.T.). The TREAT committees and teams are as follows: protocol development committee R. Brenner and M. Pfeffer (cochairs), N. Abrouk, W. Carroll, D. Green, P. Klassen, J. Lubina, J. McMurray, L. Messer, R. Newmark, P. Parfrey, S. Solomon; executive committee M. Pfeffer (chair), E. Burdmann, M. Cooper, D. de Zeeuw, K.-U. Eckardt, P. Ivanovich, A. Levey, J. McGill, J. McMurray, P. Parfrey, H.-H. Parving, B. Pereira, G. Remuzzi, A. Singh, S. Solomon, R. Toto; hemoglobin monitoring committee P. Ivanovich (chair), S. Fishbane, A. Nissenson; statistical data analysis center R. Bechhofer, D. DeMets, J. Feyzi; data and safety monitoring committee C. Hennekens (chair), G. Chertow, E. Frohlich, P. O Brien, J. Rouleau; clinical end-point center S. Solomon (chair), E. Lewis (cochair), A. Desai, C. Duong, P. Finn, L.H. Hartley, S. Kesari, J. Lin, J. Meadows, L. Mielniczuk, F. Shamshad, A. Singh, O. Vasylyeva, L. Weinrauch; study team A. Adee, A. Ahmed, P. Blaisdell, P. Brady, L. Bucker, J. Cap, W. Carroll, D. Chaparro, C.-Y. Chen, B. Condon, R. n engl j med 361;21 nejm.org november 19,
14 Darbepoetin Alfa Therapy for reduction of Cardiovascular Events Cravario, R. Damato, K. Dellacroce, K. DiRocco, D. Donovan, B. Doria, M. Dougherty, J. Droge, A. Grewal, L. Guimaraes, P. Haynes, J. Hevy, T. Jambusaria, N. James, A. Kacprzak, M. Kasenda, S.R.K. Reddy, R. Kewalramani, H. Kirby, C. Klacker, T. Kocsis, A. Kondo, M. Lauw, M. Liebelt, P. McElligott, B. Mesquita, C. Mix, A. Mueller, S. O Callaghan, H. Ocampo, K. Olson, S. Perez, J. Pillai, A. Pollock, F. Poloni, K. Polu, R. Poston, G. Ramirez, A. Rasmussen, L. Reeves, M. Rocha, A.P. Ross, J. Rossert, B. Sahl, T. See, S. Shahinfar, K. Shart, C. Stehman-Breen, A. Teh, L. Tierra, M. Vaghela, C. White. Enrollment by country was as follows (numbers of patients are in parentheses): Argentina (84), Australia (58), Austria (3), Brazil (190), Bulgaria (28), Canada (176), Chile (14), Czech Republic (96), Denmark (10), Estonia (16), France (11), Germany (135), Hungary (70), Italy (87), Latvia (51), Mexico (150), Poland (213), Portugal (17), Romania (47), Russia (117), Slovakia (65), Slovenia (12), United Kingdom (49), United States (2339). References 1. Stamler J, Vaccaro O, Neaton JD, Wentworth D. Diabetes, other risk factors, and 12-yr cardiovascular mortality for men screened in the Multiple Risk Factor Intervention Trial. Diabetes Care 1993; 16: Booth GL, Kapral MK, Fung K, Tu JV. Relation between age and cardiovascular disease in men and women with diabetes compared with non-diabetic people: a population-based retrospective cohort study. Lancet 2006;368: Turnbull F, Neal B, Algert C, et al. Effects of different blood pressure-lowering regimens on major cardiovascular events in individuals with and without diabetes mellitus: results of prospectively designed overviews of randomized trials. Arch Intern Med 2005;165: Baigent C, Keech A, Kearney PM, et al. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet 2005;366: [Errata, Lancet 2005;366:1358, 2008;371:2084.] 5. Gaede P, Lund-Andersen H, Parving H-H, Pedersen O. Effect of a multifactorial intervention on mortality in type 2 diabetes. N Engl J Med 2008;358: Brenner BM, Cooper ME, de Zeeuw D, et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001;345: Lewis EJ, Hunsicker LG, Clarke WR, et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001;345: Tonelli M, Isles C, Craven T, et al. Effect of pravastatin on rate of kidney function loss in people with or at risk for coronary disease. Circulation 2005;112: Locatelli F, Pisoni RL, Combe C, et al. Anaemia in haemodialysis patients of five European countries: association with morbidity and mortality in the Dialysis Outcomes and Practice Patterns Study (DOPPS). Nephrol Dial Transplant 2004;19: [Erratum, Nephrol Dial Transplant 2004; 19:1666.] 10. Foley RN, Parfrey PS, Harnett JD, Kent GM, Murray DC, Barre PE. The impact of anemia on cardiomyopathy, morbidity, and mortality in end-stage renal disease. Am J Kidney Dis 1996;28: Keane WF, Brenner BM, de Zeeuw D, et al. The risk of developing end-stage renal disease in patients with type 2 diabetes and nephropathy: the RENAAL study. Kidney Int 2003;63: Vlagopoulos PT, Tighiouart H, Weiner DE, et al. Anemia as a risk factor for cardiovascular disease and all-cause mortality in diabetes: the impact of chronic kidney disease. J Am Soc Nephrol 2005;16: Tong PCY, Kong APS, So W-Y, et al. Hematocrit, independent of chronic kidney disease, predicts adverse cardiovascular outcomes in Chinese patients with type 2 diabetes. Diabetes Care 2006;29: Pfeffer MA, Solomon SD, Singh AK, Ivanovich P, McMurray JJ. Uncertainty in the treatment of anemia in chronic kidney disease. Rev Cardiovasc Med 2005;Suppl 3: S35-S Eschbach JW, Abdulhadi MH, Browne JK, et al. Recombinant human erythropoietin in anemic patients with end-stage renal disease: results of a phase III multicenter clinical trial. Ann Intern Med 1989;111: Canadian Erythropoietin Study Group. Association between recombinant human erythropoietin and quality of life and exercise capacity of patients receiving haemodialysis. BMJ 1990;300: Singh AK, Szczech L, Tang KL, et al. Correction of anemia with epoetin alfa in chronic kidney disease. N Engl J Med 2006;355: Drueke TB, Locatelli F, Clyne N, et al. Normalization of hemoglobin level in patients with chronic kidney disease and anemia. N Engl J Med 2006;355: Parfrey PS, Foley RN, Wittreich BH, Sullivan DJ, Zagari MJ, Frei D. Doubleblind comparison of full and partial anemia correction in incident hemodialysis patients without symptomatic heart disease. J Am Soc Nephrol 2005;16: Phrommintikul A, Haas SJ, Elsik M, Krum H. Mortality and target haemoglobin concentrations in anemic patients with chronic kidney disease treated with erythropoietin: a meta-analysis. Lancet 2007; 369: Pfeffer MA. Critical missing data in erythropoiesis-stimulating agents in CKD: first beat placebo. Am J Kidney Dis 2008; 51: Pfeffer MA, Burdmann EA, Chen CY, et al. Baseline characteristics in the Trial to Reduce Cardiovascular Events With Aranesp Therapy (TREAT). Am J Kidney Dis 2009;54: Mozzicato P. Standardised MedDRA queries: their role in signal detection. Drug Saf 2007;30: Strippoli GF, Navaneethan SD, Craig JC. Haemoglobin and haematocrit targets for the anaemia of chronic kidney disease. Cochrane Database Syst Rev 2006;4: CD Ehrenreich H, Weissenborn K, Prange H, et al. Recombinant human erythropoietin in the treatment of acute ischemic stroke. Stroke 2009 October 15 (Epub ahead of print). 26. Strippoli GFM, Tognoni G, Navaneethan SD, Nicolucci A, Craig JC. Hemoglobin targets: we were wrong, time to move on. Lancet 2007;369: Pfeffer MA. An ongoing study of anemia correction in chronic kidney disease. N Engl J Med 2007;356: DeMets DL, Pocock SJ, Julian DG. The agonising negative trend in monitoring of clinical trials. Lancet 1999;354: Califf RM, DeMets DL. Principles from clinical trials relevant to clinical practice: Part I. Circulation 2002;106: Leyland-Jones B, Semiglazov V, Pawlicki M, et al. Maintaining normal hemoglobin levels with epoetin alfa in mainly nonanemic patients with metastatic breast cancer receiving first-line chemotherapy: a sur vival study. J Clin Oncol 2005;23: FDA black box warning for Aranesp. Silver Spring, MD: Food and Drug Administration. (Accessed October 23, 2009, at _docs/label/2008/103951s5195pi.pdf.) 32. Bohlius J, Schmidlin K, Brillant C, et al. Recombinant human erythropoiesisstimulating agents and mortality in patients with cancer: a meta-analysis of randomised trials. Lancet 2009;373: [Erratum, Lancet 2009;374:28.] Copyright 2009 Massachusetts Medical Society n engl j med 361;21 nejm.org november 19, 2009
Trial to Reduce. Aranesp* Therapy. Cardiovascular Events with
 Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
Erythropoiesis Stimulation and Heart Failure: Current Status
 Erythropoiesis Stimulation and Heart Failure: Current Status Marc A. Pfeffer, MD, PhD Dzau Professor of Medicine, Harvard Medical School Cardiovascular Division, Brigham & Women s Hospital Boston, Massachusetts
Erythropoiesis Stimulation and Heart Failure: Current Status Marc A. Pfeffer, MD, PhD Dzau Professor of Medicine, Harvard Medical School Cardiovascular Division, Brigham & Women s Hospital Boston, Massachusetts
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
The use of surrogates as key performance indicators
 REPLY The use of surrogates as key performance indicators Dr José Vinhas Department of Nephrology, Centro Hospitalar de Setúbal. Setúbal, Portugal Received for publication: 24/08/2012 Accepted: 31/08/2012
REPLY The use of surrogates as key performance indicators Dr José Vinhas Department of Nephrology, Centro Hospitalar de Setúbal. Setúbal, Portugal Received for publication: 24/08/2012 Accepted: 31/08/2012
Published trials point to a detrimental relationship
 ANEMIA, CHRONIC KIDNEY DISEASE, AND CARDIOVASCULAR DISEASE: THE CLINICAL TRIALS Steven Fishbane, MD* ABSTRACT Clinical trials have shown a strong detrimental relationship among anemia, chronic kidney disease
ANEMIA, CHRONIC KIDNEY DISEASE, AND CARDIOVASCULAR DISEASE: THE CLINICAL TRIALS Steven Fishbane, MD* ABSTRACT Clinical trials have shown a strong detrimental relationship among anemia, chronic kidney disease
Bariatric Surgery versus Intensive Medical Therapy for Diabetes 3-Year Outcomes
 The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
journal of medicine The new england Rosuvastatin to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Abstract
 The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
Conversion Dosing Guide:
 Conversion Dosing Guide: From epoetin alfa to Aranesp in patients with anemia due to CKD on dialysis Indication Aranesp (darbepoetin alfa) is indicated for the treatment of anemia due to chronic kidney
Conversion Dosing Guide: From epoetin alfa to Aranesp in patients with anemia due to CKD on dialysis Indication Aranesp (darbepoetin alfa) is indicated for the treatment of anemia due to chronic kidney
Epogen / Procrit. Epogen / Procrit (epoetin alfa) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.10.06 Section: Prescription Drugs Effective Date: April1, 2014 Subject: Epogen / Procrit Page: 1 of 7
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.10.06 Section: Prescription Drugs Effective Date: April1, 2014 Subject: Epogen / Procrit Page: 1 of 7
N Engl J Med 2018;378: DOI: /NEJMoa Lin, Wan-Ting 2018/06/27
 N Engl J Med 2018;378:1200-10. DOI: 10.1056/NEJMoa1710895 Lin, Wan-Ting 2018/06/27 1 Introduction Gout is a chronic illness characterized by hyperuricemia, arthropathy, tophus development, and urolithiasis
N Engl J Med 2018;378:1200-10. DOI: 10.1056/NEJMoa1710895 Lin, Wan-Ting 2018/06/27 1 Introduction Gout is a chronic illness characterized by hyperuricemia, arthropathy, tophus development, and urolithiasis
GSK Medicine: Study Number: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY. Harvey D White on behalf of The STABILITY Investigators
 STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
STABILITY Stabilization of Atherosclerotic plaque By Initiation of darapladib TherapY Harvey D White on behalf of The STABILITY Investigators Lipoprotein- associated Phospholipase A 2 (Lp-PLA 2 ) activity:
The CARI Guidelines Caring for Australians with Renal Impairment. Cardiovascular Risk Factors
 Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Anemia Update. Target Hb TREAT study Functional iron deficiency - Hepcidin Biosimilar epoetins
 Anemia Update Peter Bárány Department of Renal Medicine/ Karolinska University Hospital and Division of Renal Medicine Department of Clinical Science, Intervention and Technology Karolinska Institutet,
Anemia Update Peter Bárány Department of Renal Medicine/ Karolinska University Hospital and Division of Renal Medicine Department of Clinical Science, Intervention and Technology Karolinska Institutet,
Published trials point to a detrimental relationship
 ANEMIA, CHRONIC KIDNEY DISEASE, AND CARDIOVASCULAR DISEASE: THE CLINICAL TRIALS Steven Fishbane, MD* ABSTRACT Clinical trials have shown a strong detrimental relationship among anemia, chronic kidney disease
ANEMIA, CHRONIC KIDNEY DISEASE, AND CARDIOVASCULAR DISEASE: THE CLINICAL TRIALS Steven Fishbane, MD* ABSTRACT Clinical trials have shown a strong detrimental relationship among anemia, chronic kidney disease
John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam
 Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
Latest Insights from the JUPITER Study John J.P. Kastelein MD PhD Professor of Medicine Dept. of Vascular Medicine Academic Medial Center / University of Amsterdam Inflammation, hscrp, and Vascular Prevention
Erythropoiesis-stimulating Agents and Anemia in Patients with Non-dialytic Chronic Kidney Disease
 ORIGINAL ARTICLE Nephrology http://dx.doi.org/1.3346/jkms.216.31.1.55 J Korean Med Sci 216; 31: 55- Erythropoiesis-stimulating Agents and Anemia in Patients with Non-dialytic Chronic Kidney Disease Sun
ORIGINAL ARTICLE Nephrology http://dx.doi.org/1.3346/jkms.216.31.1.55 J Korean Med Sci 216; 31: 55- Erythropoiesis-stimulating Agents and Anemia in Patients with Non-dialytic Chronic Kidney Disease Sun
CARDIOVASCULAR SAFETY OF FEBUXOSTAT OR ALLOPURINOL IN PATIENTS WITH GOUT AND CARDIOVASCULAR DISEASE (The CARES Trial)
 CARDIOVASCULAR SAFETY OF FEBUXOSTAT OR ALLOPURINOL IN PATIENTS WITH GOUT AND CARDIOVASCULAR DISEASE (The CARES Trial) William B. White, MD for the CARES Investigators Calhoun Cardiology Center University
CARDIOVASCULAR SAFETY OF FEBUXOSTAT OR ALLOPURINOL IN PATIENTS WITH GOUT AND CARDIOVASCULAR DISEASE (The CARES Trial) William B. White, MD for the CARES Investigators Calhoun Cardiology Center University
Table 1 Baseline characteristics of 60 hemodialysis patients with atrial fibrillation and warfarin use
 Table 1 Baseline characteristics of 60 hemodialysis patients with atrial fibrillation and warfarin use Baseline characteristics Users (n = 28) Non-users (n = 32) P value Age (years) 67.8 (9.4) 68.4 (8.5)
Table 1 Baseline characteristics of 60 hemodialysis patients with atrial fibrillation and warfarin use Baseline characteristics Users (n = 28) Non-users (n = 32) P value Age (years) 67.8 (9.4) 68.4 (8.5)
Predicting and changing the future for people with CKD
 Predicting and changing the future for people with CKD I. David Weiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University
Predicting and changing the future for people with CKD I. David Weiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University
Alirocumab Treatment Effect Did Not Differ Between Patients With and Without Low HDL-C or High Triglyceride Levels in Phase 3 trials
 Alirocumab Treatment Effect Did Not Differ Between Patients With and Without Low HDL-C or High Triglyceride Levels in Phase 3 trials G. Kees Hovingh, 1 Richard Ceska, 2 Michael Louie, 3 Pascal Minini,
Alirocumab Treatment Effect Did Not Differ Between Patients With and Without Low HDL-C or High Triglyceride Levels in Phase 3 trials G. Kees Hovingh, 1 Richard Ceska, 2 Michael Louie, 3 Pascal Minini,
Renal Protection Staying on Target
 Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
FOURIER STUDY GREYLOCK PRESS: CTS PRODUCT SAMPLE - FOURIER YES. Did the study achieve its main objective?
 FOURIER STUDY Did the study achieve its main objective? 2 15% 1 5% 9.8% YES FOURIER compared Repatha with placebo in patients who were taking a statin and had hardening or narrowing of the arteries and
FOURIER STUDY Did the study achieve its main objective? 2 15% 1 5% 9.8% YES FOURIER compared Repatha with placebo in patients who were taking a statin and had hardening or narrowing of the arteries and
Disclosures. Dr. Scirica has also served as a consultant for Lexicon, Arena, Gilead, and Eisai.
 Disclosures Benjamin M. Scirica, MD, MPH, is employed by the TIMI Study Group, which has received research grants from Abbott, AstraZeneca, Amgen, Bayer HealthCare Pharmaceuticals, Bristol-Myers Squibb,
Disclosures Benjamin M. Scirica, MD, MPH, is employed by the TIMI Study Group, which has received research grants from Abbott, AstraZeneca, Amgen, Bayer HealthCare Pharmaceuticals, Bristol-Myers Squibb,
Aranesp. Aranesp (darbepoetin alfa) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.85.01 Subject: Aranesp Page: 1 of 6 Last Review Date: September 15, 2017 Aranesp Description Aranesp
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.85.01 Subject: Aranesp Page: 1 of 6 Last Review Date: September 15, 2017 Aranesp Description Aranesp
The FIND-CKD Study Background Study design (Results)
 The FIND-CKD Study Background Study design (Results) The FIND-CKD Study An open-label, multicentre, randomized, 3 arm study comparing the 12-month efficacy and safety of Ferric carboxymaltose (FCM, Ferinject
The FIND-CKD Study Background Study design (Results) The FIND-CKD Study An open-label, multicentre, randomized, 3 arm study comparing the 12-month efficacy and safety of Ferric carboxymaltose (FCM, Ferinject
University of Groningen. Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste
 University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Retinopathy and clinical outcomes in patients with type 2 diabetes mellitus, chronic kidney disease, and anemia
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2014 Retinopathy and clinical outcomes in patients with type 2 diabetes mellitus, chronic kidney disease, and anemia
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2014 Retinopathy and clinical outcomes in patients with type 2 diabetes mellitus, chronic kidney disease, and anemia
Treatment Of Preserved Cardiac Function Heart Failure with an Aldosterone antagonist (TOPCAT) AHA Nov 18, 2014 Update on Randomized Trials
 Treatment Of Preserved Cardiac Function Heart Failure with an Aldosterone antagonist (TOPCAT) AHA Nov 18, 2014 Update on Randomized Trials Marc A. Pfeffer, MD, PhD; Brian Claggett, PhD; Susan F. Assmann,
Treatment Of Preserved Cardiac Function Heart Failure with an Aldosterone antagonist (TOPCAT) AHA Nov 18, 2014 Update on Randomized Trials Marc A. Pfeffer, MD, PhD; Brian Claggett, PhD; Susan F. Assmann,
ARANESP (darbepoetin alfa) injection, for intravenous or subcutaneous use Initial U.S. Approval: 2001
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use ARANESP safely and effectively. See full prescribing information for ARANESP. ARANESP (darbepoetin
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use ARANESP safely and effectively. See full prescribing information for ARANESP. ARANESP (darbepoetin
Cedars Sinai Diabetes. Michael A. Weber
 Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Antihypertensive Trial Design ALLHAT
 1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
Experiences with interim trial monitoring, particularly with early stopped trials
 Experiences with interim trial monitoring, particularly with early stopped trials 1 Robert J Glynn, ScD Divisions of Preventive Medicine and Pharmacoepidemiology & Pharmacoeconomics, Brigham & Women s
Experiences with interim trial monitoring, particularly with early stopped trials 1 Robert J Glynn, ScD Divisions of Preventive Medicine and Pharmacoepidemiology & Pharmacoeconomics, Brigham & Women s
The Framingham Coronary Heart Disease Risk Score
 Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
The Seventh Report of the Joint National Commission
 The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
The Effect of a Lower Target Blood Pressure on the Progression of Kidney Disease: Long-Term Follow-up of the Modification of Diet in Renal Disease Study Mark J. Sarnak, MD; Tom Greene, PhD; Xuelei Wang,
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
(renoprotective (end-stage renal disease, ESRD) therapies) (JAMA)
 [1], 1., 2. 3. (renoprotective (end-stage renal disease, ESRD) therapies) (JAMA) (multiple risk (renal replacement therapy, RRT) factors intervention treatment MRFIT) [2] ( 1) % (ESRD) ( ) ( 1) 2001 (120
[1], 1., 2. 3. (renoprotective (end-stage renal disease, ESRD) therapies) (JAMA) (multiple risk (renal replacement therapy, RRT) factors intervention treatment MRFIT) [2] ( 1) % (ESRD) ( ) ( 1) 2001 (120
Iron Deficiency: New Therapeutic Target in Heart Failure. Stefan D. Anker, MD PhD
 Iron Deficiency: New Therapeutic Target in Heart Failure Stefan D. Anker, MD PhD Department of Cardiology, Applied Cachexia Research, Charité Campus Virchow-Klinikum, Universitätsmedizin Berlin, Germany.
Iron Deficiency: New Therapeutic Target in Heart Failure Stefan D. Anker, MD PhD Department of Cardiology, Applied Cachexia Research, Charité Campus Virchow-Klinikum, Universitätsmedizin Berlin, Germany.
Effects of Intensive Blood-Pressure Control in Type 2 Diabetes Mellitus
 original article Effects of Blood-Pressure Control in Type 2 Diabetes Mellitus The ACCORD Study Group* ABSTRACT Background There is no evidence from randomized trials to support a strategy of lowering
original article Effects of Blood-Pressure Control in Type 2 Diabetes Mellitus The ACCORD Study Group* ABSTRACT Background There is no evidence from randomized trials to support a strategy of lowering
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Randomized Comparison of the Safety, Tolerability, and Efficacy of Long-term Administration of AMG 145: 52-Week Results From the OSLER Study
 Randomized Comparison of the Safety, Tolerability, and Efficacy of Long-term Administration of AMG 145: 52-Week Results From the OSLER Study Michael J Koren 1, Robert P Giugliano 2, Frederick Raal 3, David
Randomized Comparison of the Safety, Tolerability, and Efficacy of Long-term Administration of AMG 145: 52-Week Results From the OSLER Study Michael J Koren 1, Robert P Giugliano 2, Frederick Raal 3, David
A bs tr ac t. n engl j med 368;4 nejm.org january 24,
 The new england journal of medicine established in 1812 january 24, 2013 vol. 368 no. 4 in Patients with Anemia Undergoing Hemodialysis Steven Fishbane, M.D., Brigitte Schiller, M.D., Francesco Locatelli,
The new england journal of medicine established in 1812 january 24, 2013 vol. 368 no. 4 in Patients with Anemia Undergoing Hemodialysis Steven Fishbane, M.D., Brigitte Schiller, M.D., Francesco Locatelli,
Product: Darbepoetin alfa Clinical Study Report: Date: 22 August 2007 Page 2 of 14145
 Date: 22 ugust 2007 Page 2 of 14145 2. SYNOPSIS Name of Sponsor: mgen Inc., Thousand Oaks, C, US Name of Finished Product: ranesp Name of ctive Ingredient: Darbepoetin alfa Title of Study: Randomized,
Date: 22 ugust 2007 Page 2 of 14145 2. SYNOPSIS Name of Sponsor: mgen Inc., Thousand Oaks, C, US Name of Finished Product: ranesp Name of ctive Ingredient: Darbepoetin alfa Title of Study: Randomized,
Saudi Arabia February Pr Michel KOMAJDA. Université Pierre et Marie Curie Hospital Pitié Salpétrière
 Prevention of Cardiovascular events with Ivabradine: The SHIFT Study Saudi Arabia February 2011 Pr Michel KOMAJDA Université Pierre et Marie Curie Hospital Pitié Salpétrière Paris FRANCE Declaration Of
Prevention of Cardiovascular events with Ivabradine: The SHIFT Study Saudi Arabia February 2011 Pr Michel KOMAJDA Université Pierre et Marie Curie Hospital Pitié Salpétrière Paris FRANCE Declaration Of
Effective Health Care
 Number 3 Effective Health Care Comparative Effectiveness of Epoetin and Darbepoetin for Managing Anemia in Patients Undergoing Cancer Treatment Executive Summary Background Anemia (deficiency of red blood
Number 3 Effective Health Care Comparative Effectiveness of Epoetin and Darbepoetin for Managing Anemia in Patients Undergoing Cancer Treatment Executive Summary Background Anemia (deficiency of red blood
Chronic kidney disease (CKD) has received
 Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Once-weekly darbepoetin alfa is as effective as three-times weekly epoetin
 Artigo Original ONCE-WEEKLY DARBEPOETIN ALFA IS AS EFFECTIVE AS THREE-TIMES WEEKLY EPOETIN Rev Port Nefrol Hipert 2004; 18 (1): 33-40 Once-weekly darbepoetin alfa is as effective as three-times weekly
Artigo Original ONCE-WEEKLY DARBEPOETIN ALFA IS AS EFFECTIVE AS THREE-TIMES WEEKLY EPOETIN Rev Port Nefrol Hipert 2004; 18 (1): 33-40 Once-weekly darbepoetin alfa is as effective as three-times weekly
Expert Meeting on Large Simple Trials (LST s)
 Expert Meeting on Large Simple Trials (LST s) Clinical Trials Transformation Initiative Justification for the Use of statins in Prevention: an Intervention Trial Evaluating Rosuvastatin JUPITER Johannes
Expert Meeting on Large Simple Trials (LST s) Clinical Trials Transformation Initiative Justification for the Use of statins in Prevention: an Intervention Trial Evaluating Rosuvastatin JUPITER Johannes
Literature Scan: Erythropoiesis Stimulating Agents
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Intravenous Iron Requirement in Adult Hemodialysis Patients
 Intravenous Iron Requirement in Adult Hemodialysis Patients Timothy V. Nguyen, PharmD The author is a clinical pharmacy specialist with Holy Name Hospital in Teaneck, New Jersey. He is also an adjunct
Intravenous Iron Requirement in Adult Hemodialysis Patients Timothy V. Nguyen, PharmD The author is a clinical pharmacy specialist with Holy Name Hospital in Teaneck, New Jersey. He is also an adjunct
Kenneth W. Mahaffey, MD and Keith AA Fox, MB ChB
 Once-daily oral direct factor Xa inhibition Compared with vitamin K antagonism for prevention of stroke and Embolism Trial in Atrial Fibrillation Kenneth W. Mahaffey, MD and Keith AA Fox, MB ChB on behalf
Once-daily oral direct factor Xa inhibition Compared with vitamin K antagonism for prevention of stroke and Embolism Trial in Atrial Fibrillation Kenneth W. Mahaffey, MD and Keith AA Fox, MB ChB on behalf
Disclosures for Presenter
 A Comparison of Angiotensin Receptor- Neprilysin Inhibition (ARNI) With ACE Inhibition in the Long-Term Treatment of Chronic Heart Failure With a Reduced Ejection Fraction Milton Packer, John J.V. McMurray,
A Comparison of Angiotensin Receptor- Neprilysin Inhibition (ARNI) With ACE Inhibition in the Long-Term Treatment of Chronic Heart Failure With a Reduced Ejection Fraction Milton Packer, John J.V. McMurray,
Title: Statins for haemodialysis patients with diabetes? Long-term follow-up endorses the original conclusions of the 4D study.
 Manuscript type: Invited Commentary: Title: Statins for haemodialysis patients with diabetes? Long-term follow-up endorses the original conclusions of the 4D study. Authors: David C Wheeler 1 and Bertram
Manuscript type: Invited Commentary: Title: Statins for haemodialysis patients with diabetes? Long-term follow-up endorses the original conclusions of the 4D study. Authors: David C Wheeler 1 and Bertram
LEADER Liraglutide and cardiovascular outcomes in type 2 diabetes
 LEADER Liraglutide and cardiovascular outcomes in type 2 diabetes Presented at DSBS seminar on mediation analysis August 18 th Søren Rasmussen, Novo Nordisk. LEADER CV outcome study To determine the effect
LEADER Liraglutide and cardiovascular outcomes in type 2 diabetes Presented at DSBS seminar on mediation analysis August 18 th Søren Rasmussen, Novo Nordisk. LEADER CV outcome study To determine the effect
Classification of CKD by Diagnosis
 Classification of CKD by Diagnosis Diabetic Kidney Disease Glomerular diseases (autoimmune diseases, systemic infections, drugs, neoplasia) Vascular diseases (renal artery disease, hypertension, microangiopathy)
Classification of CKD by Diagnosis Diabetic Kidney Disease Glomerular diseases (autoimmune diseases, systemic infections, drugs, neoplasia) Vascular diseases (renal artery disease, hypertension, microangiopathy)
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease
 KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease
 KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
KDIGO Controversies Conference on Management of Patients with Diabetes and Chronic Kidney Disease February 5-8, 2015 Vancouver, Canada Kidney Disease: Improving Global Outcomes (KDIGO) is an international
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
An acute fall in estimated glomerular filtration rate during treatment with losartan predicts a slower decrease in long-term renal function
 original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
SYNOPSIS. Issue Date: 04 February 2009 Document No.: EDMS -USRA
 SYNOPSIS Issue Date: 04 February 2009 Document No.: EDMS -USRA-10751204 Name of Sponsor/Company Name of Finished Product Name of Active Ingredient(s) Johnson & Johnson Pharmaceutical Research & Development,
SYNOPSIS Issue Date: 04 February 2009 Document No.: EDMS -USRA-10751204 Name of Sponsor/Company Name of Finished Product Name of Active Ingredient(s) Johnson & Johnson Pharmaceutical Research & Development,
Clinical Trial Synopsis TL-OPI-518, NCT#
 Clinical Trial Synopsis, NCT# 00225264 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl vs Glimepiride
Clinical Trial Synopsis, NCT# 00225264 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl vs Glimepiride
Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects
 ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
The CARI Guidelines Caring for Australasians with Renal Impairment. Blood Pressure Control role of specific antihypertensives
 Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
Blood Pressure Control role of specific antihypertensives Date written: May 2005 Final submission: October 2005 Author: Adrian Gillian GUIDELINES a. Regimens that include angiotensin-converting enzyme
Combined Angiotensin Inhibition for the Treatment of Diabetic Nephropathy
 The new england journal of medicine original article Combined Angiotensin Inhibition for the Treatment of Diabetic Nephropathy Linda F. Fried, M.D., M.P.H., Nicholas Emanuele, M.D., Jane H. Zhang, Ph.D.,
The new england journal of medicine original article Combined Angiotensin Inhibition for the Treatment of Diabetic Nephropathy Linda F. Fried, M.D., M.P.H., Nicholas Emanuele, M.D., Jane H. Zhang, Ph.D.,
Reducing proteinuria
 Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
Date written: May 2005 Final submission: October 2005 Author: Adrian Gillin Reducing proteinuria GUIDELINES a. The beneficial effect of treatment regimens that include angiotensinconverting enzyme inhibitors
A bs tr ac t. n engl j med 357;15 october 11,
 The new england journal of medicine established in 1812 october 11, 2007 vol. 357 no. 15 Long-Term Follow-up of the West of Scotland Coronary Prevention Study Ian Ford, Ph.D., Heather Murray, M.Sc., Chris
The new england journal of medicine established in 1812 october 11, 2007 vol. 357 no. 15 Long-Term Follow-up of the West of Scotland Coronary Prevention Study Ian Ford, Ph.D., Heather Murray, M.Sc., Chris
Medication Prior Authorization Form
 Procrit, Aranesp and (Epoetin Alfa) Policy Number: 1043 Policy History Approve Date: 12/11/2015 Effective Date: 12/11/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not
Procrit, Aranesp and (Epoetin Alfa) Policy Number: 1043 Policy History Approve Date: 12/11/2015 Effective Date: 12/11/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not
Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures
 Supplementary Data Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures Quintiles of Systolic Blood Pressure Quintiles of Diastolic Blood Pressure Q1 Q2
Supplementary Data Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures Quintiles of Systolic Blood Pressure Quintiles of Diastolic Blood Pressure Q1 Q2
CAN WE PREDICT THE RISK FOR ADVERSE EVENTS? Andrzej Wiecek, Katowice, Poland
 CAN WE PREDICT THE RISK FOR ADVERSE EVENTS? Andrzej Wiecek, Katowice, Poland Chair: Kai- Uwe Eckardt, Erlangen, Germany Pierre- Yves Martin, Geneva, Switzerland Prof. Andrzej Więcek Departm ent of Nephrology,
CAN WE PREDICT THE RISK FOR ADVERSE EVENTS? Andrzej Wiecek, Katowice, Poland Chair: Kai- Uwe Eckardt, Erlangen, Germany Pierre- Yves Martin, Geneva, Switzerland Prof. Andrzej Więcek Departm ent of Nephrology,
7 th Munich Vascular Conference
 7 th Munich Vascular Conference Secondary prevention of major cardiovascular events in patients with CHD or PAD - What can we learn from EUCLID and COMPASS, evaluating Clopidogrel, Ticagrelor and Univ.-Prof.
7 th Munich Vascular Conference Secondary prevention of major cardiovascular events in patients with CHD or PAD - What can we learn from EUCLID and COMPASS, evaluating Clopidogrel, Ticagrelor and Univ.-Prof.
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
AETNA BETTER HEALTH Prior Authorization guideline for Erythropoiesis Stimulating Agents (ESA)
 AETNA BETTER HEALTH Prior Authorization guideline for Erythropoiesis Stimulating Agents (ESA) Drugs Covered Procrit Epogen Aranesp Authorization guidelines For patients who meet all of the following: Does
AETNA BETTER HEALTH Prior Authorization guideline for Erythropoiesis Stimulating Agents (ESA) Drugs Covered Procrit Epogen Aranesp Authorization guidelines For patients who meet all of the following: Does
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Methoxy polyethylene glycol-epoetin beta (Mircera) Reference Number: CP.CPA.322 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Commercial Coding Implications Revision
Clinical Policy: Methoxy polyethylene glycol-epoetin beta (Mircera) Reference Number: CP.CPA.322 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Commercial Coding Implications Revision
Moderators: Heather A. Nyman, Pharm.D., BCPS Clinical Pharmacist, Dialysis, University of Utah Dialysis Program, Salt Lake City, Utah
 Immunology/Transplantation and Nephrology PRNs Focus Session Long-term Management of the Renal Transplant Recipient Activity No. 0217-0000-11-076-L01-P (Knowledge-Based Activity) Monday, October 17 1:30
Immunology/Transplantation and Nephrology PRNs Focus Session Long-term Management of the Renal Transplant Recipient Activity No. 0217-0000-11-076-L01-P (Knowledge-Based Activity) Monday, October 17 1:30
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
April 12, Coverage of ESAs for Patients with Conditions Other than End-Stage Renal Disease
 [ASH Comments to the Centers for Medicare and Medicaid Services on coverage for Erythropoiesis Stimulating Agents (ESAs) filed electronically on April 12, 2007] April 12, 2007 The American Society of Hematology
[ASH Comments to the Centers for Medicare and Medicaid Services on coverage for Erythropoiesis Stimulating Agents (ESAs) filed electronically on April 12, 2007] April 12, 2007 The American Society of Hematology
Why is Earlier and More Aggressive Treatment of T2 Diabetes Better?
 Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
ANEMIA & HEMODIALYSIS
 ANEMIA & HEMODIALYSIS The anemia of CKD is, in most patients, normocytic and normochromic, and is due primarily to reduced production of erythropoietin by the kidney and to shortened red cell survival.
ANEMIA & HEMODIALYSIS The anemia of CKD is, in most patients, normocytic and normochromic, and is due primarily to reduced production of erythropoietin by the kidney and to shortened red cell survival.
Soo LIM, MD, PHD Internal Medicine Seoul National University Bundang Hospital
 Soo LIM, MD, PHD Internal Medicine Seoul National University Bundang Hospital Agenda Association between Cardiovascular Disease and Type 2 Diabetes Importance of HbA1c Management esp. High risk patients
Soo LIM, MD, PHD Internal Medicine Seoul National University Bundang Hospital Agenda Association between Cardiovascular Disease and Type 2 Diabetes Importance of HbA1c Management esp. High risk patients
HMO: Medical (provider setting); Rx (out patient) PPO/CDHP: Rx
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Epogen, Procrit (epoetin alfa, injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Epogen, Procrit (epoetin alfa, injection) Commercial HMO/PPO/CDHP
The efficacy of intravenous darbepoetin alfa administered once every 2 weeks in chronic kidney disease patients on haemodialysis
 Nephrol Dial Transplant (2006) 21: 2846 2850 doi:10.1093/ndt/gfl387 Advance Access publication 5 August 2006 Original Article The efficacy of intravenous darbepoetin alfa administered once every 2 weeks
Nephrol Dial Transplant (2006) 21: 2846 2850 doi:10.1093/ndt/gfl387 Advance Access publication 5 August 2006 Original Article The efficacy of intravenous darbepoetin alfa administered once every 2 weeks
Stages of chronic kidney disease
 For mass reproduction, content licensing and permissions contact Dowden Health Media. Jonathan J. Taliercio, DO Department of Nephrology and Hypertension, Cleveland Clinic, Cleveland, Ohio talierj@ccf.org
For mass reproduction, content licensing and permissions contact Dowden Health Media. Jonathan J. Taliercio, DO Department of Nephrology and Hypertension, Cleveland Clinic, Cleveland, Ohio talierj@ccf.org
Aliskiren, Enalapril, or Aliskiren and Enalapril in Heart Failure
 The new england journal of medicine Original Article,, or and in Heart Failure John J.V. McMurray, M.D., Henry Krum, M.B., B.S., Ph.D.,* William T. Abraham, M.D., Kenneth Dickstein, M.D., Ph.D., Lars V.
The new england journal of medicine Original Article,, or and in Heart Failure John J.V. McMurray, M.D., Henry Krum, M.B., B.S., Ph.D.,* William T. Abraham, M.D., Kenneth Dickstein, M.D., Ph.D., Lars V.
Treatment of Anemia with Dar be po e tin Alfa in Systolic Heart Failure
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Treatment of Anemia with Dar be po e tin Alfa in Systolic Heart Failure Karl Swedberg, M.D., Ph.D., James B. Young, M.D., Inder S.
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Treatment of Anemia with Dar be po e tin Alfa in Systolic Heart Failure Karl Swedberg, M.D., Ph.D., James B. Young, M.D., Inder S.
1. Albuminuria an early sign of glomerular damage and renal disease. albuminuria
 1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
Individual Study Table Referring to Part of Dossier: Volume: Page:
 Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
A: Epidemiology update. Evidence that LDL-C and CRP identify different high-risk groups
 A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
Hypertension targets: sorting out the confusion. Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town
 Hypertension targets: sorting out the confusion Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town Historical Perspective The most famous casualty of this approach was the
Hypertension targets: sorting out the confusion Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town Historical Perspective The most famous casualty of this approach was the
PROs for Drug Development. Melanie Blank, MD
 PROs for Drug Development in Chronic Kidney Disease Melanie Blank, MD Disclaimer The views expressed here represent my opinions and do not necessarily represent the views of the FDA. Overview Stagnation
PROs for Drug Development in Chronic Kidney Disease Melanie Blank, MD Disclaimer The views expressed here represent my opinions and do not necessarily represent the views of the FDA. Overview Stagnation
Troponin and Cardiac Events in Stable Ischemic Heart Disease and Diabetes
 The new england journal of medicine Original Article Troponin and Cardiac Events in Stable Ischemic Heart Disease and Diabetes Brendan M. Everett, M.D., M.P.H., Maria Mori Brooks, Ph.D., Helen E.A. Vlachos,
The new england journal of medicine Original Article Troponin and Cardiac Events in Stable Ischemic Heart Disease and Diabetes Brendan M. Everett, M.D., M.P.H., Maria Mori Brooks, Ph.D., Helen E.A. Vlachos,
CARDIOVASCULAR SAFETY OF FEBUXOSTAT OR ALLOPURINOL IN PATIENTS WITH GOUT AND CARDIOVASCULAR DISEASE (The CARES Trial)
 CARDIOVASCULAR SAFETY OF FEBUXOSTAT OR ALLOPURINOL IN PATIENTS WITH GOUT AND CARDIOVASCULAR DISEASE (The CARES Trial) William B. White, MD, for the CARES Investigators Calhoun Cardiology Center University
CARDIOVASCULAR SAFETY OF FEBUXOSTAT OR ALLOPURINOL IN PATIENTS WITH GOUT AND CARDIOVASCULAR DISEASE (The CARES Trial) William B. White, MD, for the CARES Investigators Calhoun Cardiology Center University
Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial
 Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial Embargoed until 10:45 a.m. CT, Monday, Nov. 14, 2016 David
Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial Embargoed until 10:45 a.m. CT, Monday, Nov. 14, 2016 David
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS
 GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
GALECTIN-3 PREDICTS LONG TERM CARDIOVASCULAR DEATH IN HIGH-RISK CORONARY ARTERY DISEASE PATIENTS Table of Contents List of authors pag 2 Supplemental figure I pag 3 Supplemental figure II pag 4 Supplemental
Clinical and Economic Value of Rivaroxaban in Coronary Artery Disease
 CHRISTOPHER B. GRANGER, MD Professor of Medicine Division of Cardiology, Department of Medicine; Director, Cardiac Care Unit Duke University Medical Center, Durham, NC Clinical and Economic Value of Rivaroxaban
CHRISTOPHER B. GRANGER, MD Professor of Medicine Division of Cardiology, Department of Medicine; Director, Cardiac Care Unit Duke University Medical Center, Durham, NC Clinical and Economic Value of Rivaroxaban
Figure 1 LVH: Allowed Cost by Claim Volume (Data generated from a Populytics analysis).
 Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Chronic Kidney Disease (CKD): The New Silent Killer Nelson Kopyt D.O. Chief of Nephrology, LVH Valley Kidney Specialists For the past several decades, the health care needs of Americans have shifted from
Journal of the American College of Cardiology Vol. 54, No. 25, by the American College of Cardiology Foundation ISSN /09/$36.
 Journal of the American College of Cardiology Vol. 54, No. 25, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2009.10.005
Journal of the American College of Cardiology Vol. 54, No. 25, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2009.10.005
The ACC Heart Failure Guidelines
 The ACC Heart Failure Guidelines Fakhr Alayoubi, Msc,R Ph President of SCCP Cardiology Clinical Pharmacist Assistant Professor At King Saud University King Khalid University Hospital Riyadh-KSA 2017 ACC/AHA/HFSA
The ACC Heart Failure Guidelines Fakhr Alayoubi, Msc,R Ph President of SCCP Cardiology Clinical Pharmacist Assistant Professor At King Saud University King Khalid University Hospital Riyadh-KSA 2017 ACC/AHA/HFSA
Long-term outcomes in nondiabetic chronic kidney disease
 original article http://www.kidney-international.org & 28 International Society of Nephrology Long-term outcomes in nondiabetic chronic kidney disease V Menon 1, X Wang 2, MJ Sarnak 1, LH Hunsicker 3,
original article http://www.kidney-international.org & 28 International Society of Nephrology Long-term outcomes in nondiabetic chronic kidney disease V Menon 1, X Wang 2, MJ Sarnak 1, LH Hunsicker 3,
