Pharmacokinetics of Tobramycin in Adults with Cystic Fibrosis: Implications for Once-Daily Administration
|
|
|
- Jasper McCoy
- 6 years ago
- Views:
Transcription
1 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 2000, p Vol. 44, No /00/$ Copyright 2000, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Tobramycin in Adults with Cystic Fibrosis: Implications for Once-Daily Administration P. M. BERINGER, 1,2 * A. A. T. M. M. VINKS, 3 R. W. JELLIFFE, 2,4 AND B. J. SHAPIRO 4 School of Pharmacy, 1 Laboratory of Applied Pharmacokinetics, 2 and School of Medicine, 4 University of Southern California, Los Angeles, California, and The Hague Central Hospital Pharmacy, The Hague, The Netherlands 3 Received 17 August 1998/Returned for modification 20 February 1999/Accepted 15 December 1999 Once-daily administration of aminoglycosides is routinely used in many institutions. However, comparative efficacy data for patients with cystic fibrosis (CF) are lacking. The purpose of the present study was to compare the predicted pharmacodynamic activity of tobramycin at 10 mg/kg of body weight/day administered every 24 h (q24h), q12h, and q8h. Pharmacokinetic (PK) data were derived from analysis of data on the drug concentration in sera from 60 adult CF patients. Individual maximum a posteriori probability Bayesian PK parameter values were used to construct serum concentration-versus-time curves and to determine various indices (peak concentration/mic ratio [peak/mic], area under the concentration-time curve/mic ratio [AUC/MIC], and time that the concentration was less than the MIC [T<MIC]) for the three regimens described above. MICs of 1, 2, and 4 g/ml for Pseudomonas aeruginosa were assumed in the simulations. Irrespective of the MIC, significantly lower peak/mic but shorter T<MIC were noted when regimens of q8h versus q12h (P < 0.001), q8h versus q24h (P < 0.001), and q12h versus q24h (P < 0.001) were compared. This analysis suggests that the potential benefit of achieving a greater peak/mic with once-daily aminoglycoside administration may be offset by the significantly greater T<MIC in CF patients compared with that achieved with multiple-dailydosing regimens. Clinical trials are necessary to determine if once daily aminoglycoside administration is efficacious in the CF population before its routine use can be recommended. Lung disease is a major cause of morbidity and mortality in patients with cystic fibrosis (CF). Impaired mucociliary clearance and host defense mechanisms in the airway lead to eventual colonization with Pseudomonas aeruginosa and other organisms. The ensuing chronic infection and inflammation lead to bronchiectasis and progressive loss of lung function (8, 25, 30). Intermittent courses of intravenous antibiotics administered during acute pulmonary exacerbations significantly reduce the bacterial load and improve lung function (26). The combination of a beta-lactam and an aminoglycoside is frequently used due to their potential synergistic activity and for prevention of the development of resistance (27). Traditionally, aminoglycosides have been administered by intermittent infusions three to four times daily. Recently, oncedaily administration of aminoglycosides has been advocated (24). Several theoretical advantages to this dosing modality have been suggested. Data from in vitro studies and studies with animals have demonstrated that aminoglycosides exhibit concentration-dependent bactericidal activity (6, 17, 19, 33). The killing effect has therefore been correlated with the peak concentration achieved. These studies have also demonstrated that the aminoglycosides exhibit a short (1- to 3-h) in vitro postantibiotic effect (PAE) (10, 18) and a more prolonged (10-h) in vivo PAE (7). The presence of a PAE prevents organism regrowth from occurring for short periods of time after antibiotic concentrations fall below the MIC at the site of the infection. In addition, studies with animals have demonstrated saturable uptake mechanisms within the renal cortex and inner ear (23). Accumulation of aminoglycosides within these tissues has been demonstrated to cause nephrotoxicity and ototoxicity in these animals. Less frequent dosing but administration of * Corresponding author. Mailing address: School of Pharmacy, 1985 Zonal Ave., Los Angeles, CA Phone: (323) Fax: (626) beringer@hsc.usc.edu. larger doses reduces the relative accumulation of the aminoglycosides within these tissues; however, the degree of reduction is unknown. Taken together, these properties suggest that dosing strategies which maximize the peak concentration and allow trough concentrations to drop below the MIC for a short period of time should maximize bactericidal activity and minimize the risk of nephrotoxicity and ototoxicity. Various pharmacodynamic indices have been proposed to predict clinical and bacteriological responses to antibiotic therapy. Data from in vitro models and studies with animals suggest that the aminoglycoside peak concentration/mic ratio (peak/mic) and the area under the concentration-versus-time curve/mic ratio (AUC/MIC) are significantly correlated with microbiological outcome (17, 19, 33). However, if the dosing interval is sufficiently long compared to the half-life of the antibiotic, the time below the MIC (T MIC) also becomes a significant predictor of microbiological outcome (17, 33). Evaluations with humans confirm these relationships (15). Moore et al. (22) demonstrated that aminoglycoside peak/mics that exceed 10 provide optimal clinical outcomes for patients with pneumonia caused by gram-negative organisms. Furthermore, others noted that subinhibitory levels of gentamicin were associated with recurrent bacteremia (1). On the basis of these data, it has been suggested that the dosing interval for aminoglycosides should allow concentrations to fall below the MIC only for a short duration of time (i.e., the duration of the PAE). Considering the relatively short elimination half-life of aminoglycosides in patients with CF (9), which may lead to the possibility of organism regrowth at the end of the dosing interval, some have recommended against the use of extendedinterval aminoglycoside dosing in this population (29). Evidence supporting the use of once-daily dosing of aminoglycosides in patients with CF is limited. The purpose of this study was to evaluate three different tobramycin dosing regimens for the treatment of Pseudomonas lung infections in 809
2 810 BERINGER ET AL. ANTIMICROB. AGENTS CHEMOTHER. patients with CF by comparing predicted pharmacodynamic indices. MATERIALS AND METHODS Patients. CF patients from two centers were included in the study. Patients were included in the analysis if they met the following criteria: (i) were age 18 years or older, (ii) had acute pulmonary exacerbation due to Pseudomonas aeruginosa that required hospitalization, and (iii) had received therapy with tobramycin and had available at least one set of measured peak and trough serum tobramycin concentrations. Study design and procedures. The chart records of study patients admitted over a 1-year period were reviewed. The following information was recorded: tobramycin dosing history, serum tobramycin concentration data, age, height, weight, gender, and serum creatinine concentration. Blood samples for determination of peak tobramycin concentrations were obtained within 30 min after the end of a 30-min infusion. Trough concentrations were obtained within 30 min of the next scheduled administration time. The exact administration and sampling times were determined from the nursing medication administration record and the laboratory data sheets. Pharmacokinetic model. Pharmacokinetic analysis was performed for each patient by using the USC*PACK clinical programs (version 10.7; Laboratory of Applied Pharmacokinetics, University of Southern California School of Medicine, Los Angeles). Serum tobramycin concentrations for each individual were fitted to a one-compartment open model by using maximum a posteriori probability Bayesian (MAP-B) analysis. The Bayesian a priori parameter values were derived from an adult CF population (28), as follows: volume of distribution, liter/kg; elimination rate constant (in hours 1 ), (CL CR ) 0.01, where CL CR is creatinine clearance. CL CR was estimated on the basis of the patient s demographics and serum creatinine concentration(s) by the method developed by Jelliffe and Jelliffe (16). Serum tobramycin concentrations were weighted by the inverse of the measured assay error variance. The individual MAP-B parameters were used to construct simulated serum concentration-time curves for three different tobramycin dosage regimens for each patient: 3.3 mg/kg of body weight every 8 h (q8h), 5 mg/kg q12h, and 10 mg/kg q24h. Simulations were performed by using individual rather than mean pharmacokinetic data in order to determine the variability in the concentrations and pharmacodynamic indices achieved. Determination of pharmacodynamic indices. The serum concentration-time curves for each regimen were used to compute the following pharmacodynamic indices: peak/mic, AUC/MIC, and T MIC. Since actual MICs were not available, values of 1, 2, and 4 g/ml for P. aeruginosa were assumed in the simulations. These values are consistent with the range of tobramycin sensitivities reported in a recent clinical trial (12). A total of 540 simulations were performed (three dosage regimens and three different MICs with 60 patients). Successful tobramycin dosing regimens were defined as those which (i) achieved a peak/ MIC greater than 10 and (ii) attained a T MIC of not greater than the duration of the PAE (3 h in vitro or 10 h in vivo). Tobramycin assay. Serum tobramycin concentrations were determined by a fluorescence polarization immunoassay technique (TDx; Abbott Laboratories, Chicago, Ill.) at one institution and an enzyme immunoassay (ACA; Dupont, Wilmington, Del.) at the other. The assay error pattern for each method was determined by performing replicate measures of concentrations representing the expected range of measured concentrations. Curve fitting applied to the measured concentrations and standard deviations (SDs) at each concentration resulted in the following second-order polynomial equations: for TDx, SD (in milligrams/liter) [C] [C 2 ]; for ACA, SD (in milligrams/liter) [C] [C 2 ], where SD is the standard deviation of the assay and [C] and [C 2 ] are the observed concentration and the concentration squared, respectively. Statistical analysis. Statistical analysis was performed with GraphPad Prism software (version 3.00 for Windows; GraphPad Software, San Diego, Calif.). Differences in predicted peak and trough concentrations and pharmacodynamic indices between dosage regimens were determined by Kruskal-Wallis analysis of variance with Dunn s multiple comparisons test. Significance was defined as a P value of less than TABLE 1. Predicted peak and trough concentrations and pharmacodynamic parameters a Parameter and concentration 3.3 mg/kg q8h 5 mg/kg q12h 10 mg/kg q24h Peak concn ( g/ml) b,c b,d c,d Trough concn ( g/ml) b,c b,d c,d MIC, 1 g/ml Peak/MIC b,c b,d c,d T MIC b,c b,d c,d AUC/MIC MIC, 2 g/ml Peak/MIC b,c b,d c,d T MIC b,c b,d c,d AUC/MIC MIC, 4 g/ml Peak/MIC b,c b,d c,d T MIC b,c b,d c,d AUC/MIC a Values are medians SDs. b P c P d P RESULTS Patients. Sixty adult CF patients treated with intravenous tobramycin at two different care centers were evaluated. Patient characteristics and clinical data are as follows: 33 males and 27 females were evaluated. The median age was 27 6 years, the median weight was kilograms, and the estimated median CL CR was ml/min/1.73 m 2 (range, 42.4 to 260 ml/min/1.73 m 2 ). The median tobramycin dosage received was 3.4 mg/kg of body weight q8h. Pharmacokinetic analysis. Bayesian analysis performed with the measured tobramycin concentrations resulted in the following fitted pharmacokinetic parameter values (median SD): total body clearance, ml/min/1.73 m 2 (range, 43.7 to ml/min/1.73 m 2 ); volume of distribution liters/kg (range, 0.18 to 0.74 liters/kg); elimination rate constant, h 1 (range, 0.12 to 0.47 h 1 ); and halflife, h (range, 1.5 to 5.6 h). A comparison of the predicted peak and trough concentrations and the variability indicates significant differences between the three regimens (Table 1). These differences are shown graphically in Fig. 1, which was constructed by using the medians of the MAP-B fitted parameter values. Pharmacodynamic comparisons. Differences in pharmacodynamic indices paralleled the differences in predicted peak and trough concentrations. Significantly lower peak/mics but shorter T MICs were noted when the q8h versus q12h, q8h FIG. 1. Computer simulations of concentration-time curves of tobramycin at 10 mg/kg/24 h during intermittent infusions. -, 3.3 mg/kg q8h over 30 min;, 5 mg/kg q12h over 30 min; -----, 10 mg/kg q24h over 60 min; and, MIC of 2 g/ml. Simulations were performed with the USC PACK package of programs with the median MAP-B fitted parameter values.
3 VOL. 44, 2000 ONCE-DAILY TOBRAMYCIN DOSING IN ADULT CF PATIENTS 811 versus q24h, and q12h versus q24h regimens were compared, regardless of the MIC (Table 1; Fig. 1). Similarly, with increasing MICs, the peak/mic decreased significantly while the T MIC increased significantly within each dosing group (data not shown). As expected, since the same total daily dose was provided by all three dosing regimens, no differences in AUC/ MIC between regimens were observed. A comparison of pharmacodynamic indices between dosing regimens in relationship to achievement of the desired goals (peak/mic of 10 and T MIC not to exceed the duration of the PAE) was also performed (Table 1). Regardless of the MIC, all once-daily regimens resulted in prolonged drug-free intervals that exceeded the duration of the PAE (both in vitro and in vivo). Only the two multiple-daily-dosing regimens (q8h and q12h) at an MIC of 1 g/ml met the desired goals. However, at higher MICs the multiple-daily-dosing regimens failed to achieve the desired peak/mic. Somewhat favored is the q12h regimen, which more effectively balances achievement of the desired peak/mic while minimizing T MIC. DISCUSSION The objective of the present investigation was to compare the predicted pharmacodynamic activities of three tobramycin dosing regimens in adult patients with CF. While few studies describe the pharmacokinetics and safety (3, 5) of this dosing modality in patients with CF, data on clinical efficacy are scant. Vic et al. (31) performed a prospective open-label evaluation of once-daily amikacin with 20 pediatric CF patients with acute pulmonary exacerbations. Patients received amikacin at 35 mg/kg q24h in combination with either ceftazidime or imipenem at 200 mg/kg/day for 14 days. Significant improvements in respiratory and inflammatory indices were observed. However, without a comparison group, the efficacy of once-daily aminoglycoside administration remains in question. In a subsequent study, the same investigators performed a prospective comparative trial of tobramycin given once daily versus three times daily to 22 pediatric CF patients experiencing acute pulmonary exacerbations (32). Patients received ceftazidime at 200 mg/kg/day in combination with tobramycin at 5 mg/kg q8h or 15 mg/kg/day for 14 days. Improvements in pulmonary function and inflammatory indices were not different between the two groups. However, that study was underpowered and therefore does not provide definitive evidence in support of oncedaily dosing of aminoglycosides in CF patients. Powell et al. (23) evaluated the efficacies of three different tobramycin dosages with 52 adult CF patients with moderately severe pulmonary exacerbations. Twenty-six patients received 9 mg/kg q24h, 10 patients received 15 mg/kg q24h, and 16 patients received 11 mg/kg as a continuous infusion. Efficacy was evaluated by using a 15-point scale for paroxysmal cough, nocturnal cough, orthopnea, dyspnea at rest, and dyspnea with exertion. There were no differences in the rate of resolution of the five symptoms between the patients receiving the different dosages. Although these data are interesting, subsequent studies have shown that clinical symptom scores do not correlate with objective measures of pulmonary function during acute pulmonary exacerbations (4). Various pharmacodynamic indices such as peak/mic, AUC/ MIC, and T MIC have been suggested as useful indicators of the clinical and microbiological effectiveness of an antibiotic regimen. In particular, the aminoglycoside peak/mic has been demonstrated to correlate significantly with successful treatment of pneumonia (15). In the present study we showed that peak/mic is significantly greater with once-daily administration than with either q12h or q8h regimens. However, our data also show that T MIC is significantly prolonged with oncedaily administration than with either q12h or q8h regimens (Table 1). These two factors would be expected to have opposing pharmacodynamic effects. A greater peak/mic would provide greater bactericidal activity, while a longer T MIC would allow greater organism regrowth to occur within the dosing interval. The PAE is frequently cited as one of the principal factors that enables extended-interval aminoglycoside dosing. While the PAE has been described in numerous in vitro studies and several studies with animals, the reported duration varies significantly between studies. The most likely explanation for this variation relates to the experimental methods used including exposure to fixed versus fluctuating antibiotic concentrations and differences in the availability of nutritional factors necessary for microorganism recovery. Many studies measured the PAE in vitro by comparing growth curves following dilution to remove the antibiotic, with the duration reported to be 2 to 3 h. A limitation of this approach is that it does not mimic in vivo conditions. In vivo, aminoglycoside concentrations decline exponentially. Den Hollander et al. (10) have recently demonstrated a more prolonged growth inhibition of tobramycin against P. aeruginosa (6 h) using an in vitro pharmacokineticpharmacodynamic model, which provided fluctuating tobramycin concentrations similar to those achieved under in vivo conditions. The investigators attributed the more prolonged growth inhibition to a postantibiotic sub-mic effect which would not be detected by standard methods for measurement of PAE. More recently, Mouton et al. (J. W. Mouton, N. J. Jacobs, P. DeGraaf, J. G. Hollander Den, and A. M. Horrevorts, Abst. 39th Intersci. Conf. Antimicrob. Agents Chemother. abstr. 539, p. 22, 1999) have demonstrated that the in vitro PAE varies with the concentration of nutritional factors from the broth used for microorganism recovery. The results of these studies correlate better with the limited in vivo data available from studies with animals. Craig et al. (7) measured a PAE of 10 h with amikacin using a once-daily regimen in a murine neutropenic thigh infection model. These data suggest that the PAE in humans may be longer than the 2 to 3 h obtained by standard in vitro techniques. The tobramycin pharmacokinetic parameters found in the present study are similar to those reported by other investigators evaluating adult CF patients (3, 28). Considering the relatively short elimination half-life of approximately 2 h in our CF population, concentrations in serum would be expected to be undetectable within 10 h. If a short PAE (i.e., 3 h) is assumed, a prolonged drug-free interval (or T MIC) is observed. The expected result is significant organism regrowth within the dosing interval that may more than offset any benefit achieved from a higher peak associated with once-daily dosing. In contrast, in general medicine patients, a slower clearance and longer half-life would be expected to result in a substantially reduced drug-free interval compared with that in our CF population (13). Thus, less potential for organism regrowth within the dosing interval would be expected. These observations offer a possible explanation for the similar efficacy seen with once-daily and multiple-daily-dosing regimens in general medicine patients (24), while the same may or may not be seen with CF patients. Alternatively, if a more prolonged PAE is assumed (i.e., 10 h), the greater peak-associated bactericidal activity of the once-daily regimen may outweigh the relatively short period of time when the PAE has been exceeded. Comparative bactericidal activity data for CF patients are lacking. On the basis of our analysis, it is unclear whether once-daily administration would offer improved or poorer outcomes com-
4 812 BERINGER ET AL. ANTIMICROB. AGENTS CHEMOTHER. pared to those achieved with traditional multiple-daily-dosing regimens. The analysis applied in this study does not consider the effects of concomitant antibiotic therapy. In clinical practice, combination therapy with an aminoglycoside and a beta-lactam is frequently prescribed in order to provide potentially synergistic activity and to reduce the likelihood for development of antibiotic resistance. In an experimental model of P. aeruginosa pneumonia in neutropenic guinea pigs, once-daily dosing of tobramycin was less active than every 4 h for dosing a similar overall dose. The addition of mezlocillin to both regimens resulted in similar killing activities (17). These data suggest that combination therapy is likely to obscure differences in aminoglycoside regimens at lower MICs (i.e., an MIC of 0.8 g/ml was used in the earlier study [17]). It would be important to know whether this relationship holds true for the isolates for which MICs are relatively higher and which are commonly encountered in patients with CF. Additionally, once-daily administration of aminoglycosides in our patients would result in drug concentrations below 0.5 mg/liter for nearly half of the dosing interval (Fig. 1). Whether this provides similar activity in terms of synergy and deterring the development of resistance as conventional multiple daily dosing regimens is unclear. Profiles of the concentration in serum were used to predict the efficacy of tobramycin on the basis of pharmacodynamic indices. The tobramycin concentrations within the lung airways have been demonstrated to be significantly lower than those in serum due to decreased penetration (21). In addition, binding to sputum mucins also contributes to reduced tobramycin activity (20). While these factors would predict decreased killing activity in the lungs compared with that in the serum, results from a murine pneumonitis model indicate that aminoglycoside elimination is slower from the lungs than from serum (19). The prolonged elimination from the lungs resulted in a more sustained antibacterial activity within the lungs. While the net effect of these factors in patients with CF is not clear, it would be expected to similarly effect the activities of all tobramycin dosing regimens. Therefore, the relative differences between dosing regimens as suggested by the current pharmacodynamic analysis are likely to be retained. The results of this study are equivocal with regard to the predicted comparative efficacy of once-daily and multiple-daily tobramycin dosing regimens in adult CF patients. In the presence of a short PAE the potential benefit of achieving a greater peak/mic with once-daily aminoglycoside dosing may be more than offset by the significantly greater T MIC in CF patients compared with that achieved with either a q12h or a q8h regimen. In contrast, with a more prolonged PAE, as observed in studies with animals, once-daily dosing regimens may provide greater bactericidal activity. Comparative evaluations of administration of single daily doses versus multiple daily doses of an aminoglycoside in CF patients are necessary to determine definitively the efficacy of the once-daily dosing modality. A comparison of pulmonary function between treatment groups would enable objective comparison of the efficacies of the dosing regimens and should serve as the primary outcome parameter. Reduced bacterial densities in sputum have been demonstrated to correlate with improvement in pulmonary function during acute exacerbations in patients with CF and would provide a useful secondary measure of the comparative activity of once-daily and traditional multiple-daily dosing regimens (26). Additionally, development of standardized measurements of pulmonary inflammation (i.e., cytokine measurements) may provide useful measures of outcome besides lung function itself. The dosages and timing of administration of concomitantly administered antibiotics (e.g., beta-lactams and fluoroquinolones) in relation to the aminoglycoside administration should be documented since these are also likely to affect the relationship (2). Routine use of once-daily aminoglycoside administration should be avoided in patients with CF until such data are available to confirm the efficacy of this dosing modality. REFERENCES 1. Anderson, E. T., L. S. Young, and W. L. Hewitt Simultaneous antibiotic levels in break through gram-negative bacteremia. Am. J. Med. 61: Barclay, M. L., E. J. Begg, S. T. Chambers, and D. R. Boswell Improved efficacy with nonsimultaneous administration of first doses of gentamicin and ceftazidime in vitro. Antimicrob. Agents Chemother. 39: Bates, R. D., M. C. Nahata, J. W. Jones, K. McCoy, G. Young, S. Cox, and W. J. Barson Pharmacokinetics and safety of tobramycin after oncedaily administration in patients with cystic fibrosis. Chest 112: Bosso, J. A., and K. B. Walker Lack of correlation between objective indicators and clinical-response scores during antimicrobial therapy for acute pulmonary exacerbations of cystic fibrosis. Clin. Pharm. 7: Canis, F., M. O. Husson, D. Turck, P. Vic, V. Launay, S. Ategbo, A. Vincent, and R. J. Courcol Pharmacokinetics and bronchial diffusion of single daily dose amikacin in cystic fibrosis patients. J. Antimicrob. Chemother. 39: Craig, W. A., and S. C. Ebert Killing and regrowth of bacteria in vitro: a review. Scand. J. Infect. Dis. 74(Suppl.): Craig, W. A., J. Redington, and S. C. Ebert Pharmacodynamics of amikacin in vitro and in mouse thigh and lung infections. J. Antimicrob. Chemother. 27(Suppl. C): Davis, P. B., M. Drumm, and M. Konstan Cystic fibrosis. Am. J. Respir. Crit. Care Med. 154: De Groot, R., and A. L. Smith Antibiotic pharmacokinetics in cystic fibrosis: differences and clinical significance. Clin. Pharmacokinet. 13: Den Hollander, J. G., K. Fuursted, H. A. Verbrugh, and J. W. Mouton Duration and clinical relevance of postantibiotic effect in relation to the dosing interval. Antimicrob. Agents Chemother. 42: DuBois, D., and E. F. DuBois A formula to estimate appropriate surface area if height and weight are known. Arch. Intern. Med. 17: Eisenberg, J., M. Pepe, J. Williams-Warren, M. Vasiliev, A. B. Montgomery, A. L. Smith, and B. W. Ramsey A comparison of peak sputum tobramycin concentration in patients with cystic fibrosis using jet and ultrasonic nebulizer systems. Chest 111: Garrelts, J. C Exploration of once-daily dosing of aminoglycosides through Bayesian simulation. Pharmacotherapy 16: Hallynck, T. H., H. H. Soep, J. A. Thomis, J. Boelaert, R. Daneels, and L. Dettli Should clearance be normalized to body surface or to lean body mass? Br. J. Clin. Pharmacol. 11: Hyatt, J. M., P. S. McKinnon, G. S. Zimmer, and J. J. Schentag The importance of pharmacokinetic/pharmacodynamic surrogate markers to outcome: focus on antibacterial agents. Clin. Pharmacokinet. 28: Jelliffe, R. W., and S. M. Jelliffe A computer program for estimation of creatinine clearance from unstable serum creatinine levels, age, sex and weight. Math. Biosci. 14: Kapusnik, J. E., C. J. Hackbarth, H. F. Chambers, T. Carpenter, M. A. Sande Single, large, daily dosing versus intermittent dosing of tobramycin for treating experimental Pseudomonas pneumonia. J. Infect. Dis. 158: Karlowsky, J. A., G. G. Zhanel, R. J. Davidson, and D. J. Hoban Postantibiotic effect in Pseudomonas aeruginosa following single and multiple aminoglycoside exposures in vitro. J. Antimicrob. Chemother. 33: Leggett, J. E., B. Fantin, S. Ebert, K. Totsuka, B. Vogelman, W. Calame, H. Mattie, and W. A. Craig Comparative antibiotic dose-effect relations at several dosing intervals in murine pneumonitis and thigh-infection models. J. Infect. Dis. 159: Levy, J., A. L. Smith, M. A. Kenny, B. Ramsey, and F. D. Schoenknecht Bioactivity of gentamicin in purulent sputum from patients with cystic fibrosis or bronchiectasis: comparison with activity in serum. J. Infect. Dis. 148: Mendelman, P. M., A. L. Smith, J. Levy, A. Weber, B. Ramsey, and R. L. Davis Aminoglycoside penetration, inactivation, and efficacy in cystic fibrosis. Am. Rev. Respir. Dis. 132: Moore, R. D., C. R. Smith, and P. S. Lietman Association of aminoglycoside plasma levels with therapeutic outcome in gram-negative pneumonia. Am. J. Med. 77: Powell, S. H., W. L. Thompson, M. A. Luthe, R. C. Stern, D. A. Grossniklaus, D. D. Bloxham, D. L. Groden, M. R. Jacobs, A. O. DiScenna, H. A. Cash, and J. D. Klinger Once-daily vs. continuous aminoglycoside dosing: efficacy and toxicity in animal and clinical studies of gentamicin, netilmicin, and
5 VOL. 44, 2000 ONCE-DAILY TOBRAMYCIN DOSING IN ADULT CF PATIENTS 813 tobramycin. J. Infect. Dis. 5: Preston, S. L., and L. L. Briceland Single daily dosing of aminoglycosides. Pharmacotherapy 15: Ramsey, B. W Management of pulmonary disease in patients with cystic fibrosis. N. Engl. J. Med. 335: Regelmann, W. E., G. R. Elliott, W. J. Warwick, and C. C. Clawson Reduction of sputum Pseudomonas aeruginosa density by antibiotics improves lung function in cystic fibrosis more than do bronchodilators and chest physiotherapy alone. Am. Rev. Respir. Dis. 141: Saiman, L., F. Mehar, W. W. Niu, H. C. Neu, K. J. Shaw, G. Miller, and A. Prince Antibiotic susceptibility of multiply resistant Pseudomonas aeruginosa isolated from patients with cystic fibrosis, including candidates for transplantation. Clin. Infect. Dis. 23: Touw, D. J., A. A. T. M. M. Vinks, and C. Neef Pharmacokinetic modelling of intravenous tobramycin in adolescent and adult patients with cystic fibrosis using the nonparametric expectation maximization (NPEM) algorithm. Pharm. World Sci. 19: Touw, D. J., A. A. T. M. M. Vinks, J. W. Mouton, and A. M. Horevorts Pharmacokinetic optimisation of antibacterial treatment in patients with cystic fibrosis. Clin. Pharmacokinet. 35: Turpin, S. V., and M. R. Knowles Treatment of pulmonary disease in patients with cystic fibrosis, p In P. B. Davis (ed.), Lung biology in health and disease, vol. 64. Cystic fibrosis. Marcel Dekker, Inc., New York, N.Y. 31. Vic, P., S. Ategbo, D. Turck, M. O. Husson, E. Tassin, G. A. Loeuille, A. Deschildre, D. Druon, J. C. Elian, C. Arrouet-Lagandre, and J. P. Farriaux Tolerance, pharmacokinetics and efficacy of once daily amikacin for treatment of Pseudomonas aeruginosa pulmonary exacerbations in cystic fibrosis patients. Eur. J. Pediatr. 155: Vic, P., S. Ategbo, D. Turck, M. O. Husson, V. Launay, G. A. Loeuille, A. Sardet, A. Deschildre, D. Druon, and C. Arrouet-Lagande Efficacy, tolerance, and pharmacokinetics of once daily tobramycin for pseudomonas exacerbations in cystic fibrosis. Arch. Dis. Child. 78: Vogelman, B., S. Gudmundsson, J. Leggett, J. Turnidge, S. Ebert, and W. A. Craig Correlation of antimicrobial pharmacokinetic parameters with therapeutic efficacy in an animal model. J. Infect. Dis. 158:
ICU Volume 11 - Issue 3 - Autumn Series
 ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
Experience with a Once-Daily Aminoglycoside Program Administered to 2,184 Adult Patients
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
Antimicrobial practice. Monitoring serum concentrations for once-daily netilmicin dosing regimens
 Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
/01/$ DOI: /AAC Copyright 2001, American Society for Microbiology. All Rights Reserved.
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Dec. 2001, p. 3468 3473 Vol. 45, No. 12 0066-4804/01/$04.00 0 DOI: 10.1128/AAC.45.12.3468 3473.2001 Copyright 2001, American Society for Microbiology. All Rights
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Dec. 2001, p. 3468 3473 Vol. 45, No. 12 0066-4804/01/$04.00 0 DOI: 10.1128/AAC.45.12.3468 3473.2001 Copyright 2001, American Society for Microbiology. All Rights
%T MIC MIC. Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration time-killing-curve 1990.
 THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
Pharmacologyonline 1: (2010) ewsletter Singh and Kochbar. Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of
 Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS
 THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
Pharmacodynamics: the methods
 Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
SBUH Aminoglycoside Dosing Protocol
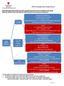 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Comparisons between Antimicrobial Pharmacodynamic Indices and Bacterial Killing as Described by Using the Zhi Model
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1998, p. 1731 1737 Vol. 42, No. 7 0066-4804/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Comparisons between Antimicrobial
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1998, p. 1731 1737 Vol. 42, No. 7 0066-4804/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Comparisons between Antimicrobial
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS
 PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics
 Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN
 ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
Lessons from recent studies. João Gonçalves Pereira UCIP DALI
 Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Received 4 December 2006/Returned for modification 8 March 2007/Accepted 9 June 2007
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2007, p. 3049 3055 Vol. 51, No. 9 0066-4804/07/$08.00 0 doi:10.1128/aac.01522-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Pharmacokinetics
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2007, p. 3049 3055 Vol. 51, No. 9 0066-4804/07/$08.00 0 doi:10.1128/aac.01522-06 Copyright 2007, American Society for Microbiology. All Rights Reserved. Pharmacokinetics
Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in Children
 Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 2003 Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in
Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 2003 Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence
 Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally
 INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
MRSA Micro Scan Pos Combo 6J DADE BEHRING VCM
 PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
PHARMONITOR II. Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling. Pierre Wallemacq
 PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
PHA Spring First Exam. 8 Aminoglycosides (5 points)
 PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
TRANSPARENCY COMMITTEE OPINION. 15 October Date of Marketing Authorisation (national procedure): 16 April 1997, variation of 18 February 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
Comparing Methods for Once Daily Tobramycin Exposure Predictions in Children with Cystic Fibrosis
 Comparing Methods for Once Daily Tobramycin Exposure Predictions in Children with Cystic Fibrosis Stefanie HENNIG, Franziska STILLER, Beverly TEO, Christine STAATZ, Brisbane Cystic fibrosis (CF) & Once
Comparing Methods for Once Daily Tobramycin Exposure Predictions in Children with Cystic Fibrosis Stefanie HENNIG, Franziska STILLER, Beverly TEO, Christine STAATZ, Brisbane Cystic fibrosis (CF) & Once
Challenges in Therapeutic Drug Monitoring:
 Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Use ideal body weight (IBW) unless actual body weight is less. Use the following equation to calculate IBW:
 Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Disclosures. Efficacy of the drug. Optimizing Dosing Based on PKPD- An overview. Dose Finding - The Past
 Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Professor of Medicine Vice-Chairman, Department of Medicine SUNY at Stony Brook
 Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
without the permission of the author Not to be copied and distributed to others
 Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Pharmacokinetic modelling of a once-daily dosing regimen for intravenous tobramycin in paediatric cystic fibrosis patients
 Journal of Antimicrobial Chemotherapy Advance Access published April 19, 2007 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkm097 Pharmacokinetic modelling of a once-daily dosing regimen for intravenous
Journal of Antimicrobial Chemotherapy Advance Access published April 19, 2007 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkm097 Pharmacokinetic modelling of a once-daily dosing regimen for intravenous
A Survey of Extended-Interval Aminoglycoside Dosing Practices in United States Adult Cystic Fibrosis Programs
 A Survey of Extended-Interval Aminoglycoside Dosing Practices in United States Adult Cystic Fibrosis Programs William A Prescott Jr PharmD INTRODUCTION: The Cystic Fibrosis Foundation recently deemed the
A Survey of Extended-Interval Aminoglycoside Dosing Practices in United States Adult Cystic Fibrosis Programs William A Prescott Jr PharmD INTRODUCTION: The Cystic Fibrosis Foundation recently deemed the
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis
 Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES
 Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
Is the package insert correct? PK considerations
 Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Inhaled antibiotic therapy: What drug? What dose? What regimen? What formulation?
 Journal of Cystic Fibrosis 1 (2002) S189 S193 Inhaled antibiotic therapy: What drug? What dose? What regimen? What formulation? A.L. Smith* Department of Molecular Microbiology & Immunology, University
Journal of Cystic Fibrosis 1 (2002) S189 S193 Inhaled antibiotic therapy: What drug? What dose? What regimen? What formulation? A.L. Smith* Department of Molecular Microbiology & Immunology, University
Inhalational antibacterial regimens in non-cystic fibrosis patients. Jeff Alder Bayer HealthCare
 Inhalational antibacterial regimens in non-cystic fibrosis patients Jeff Alder Bayer HealthCare Alder - Inhaled therapy for non-cf - EMA 25-26 Oct 2012 1 Inhalational antibacterials: two approaches 1.
Inhalational antibacterial regimens in non-cystic fibrosis patients Jeff Alder Bayer HealthCare Alder - Inhaled therapy for non-cf - EMA 25-26 Oct 2012 1 Inhalational antibacterials: two approaches 1.
THE AMINOGLYCOSIDE ANTIBIOTICS
 4 THE AMINOGLYCOSIDE ANTIBIOTICS INTRODUCTION The aminoglycoside antibiotics are widely used for the treatment of severe gram-negative infections such as pneumonia or bacteremia, often in combination with
4 THE AMINOGLYCOSIDE ANTIBIOTICS INTRODUCTION The aminoglycoside antibiotics are widely used for the treatment of severe gram-negative infections such as pneumonia or bacteremia, often in combination with
prophylaxis for endocarditis in patients at high risk prophylaxis for major surgical procedures
 1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
La farmacologia in aiuto
 Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Adult Institutional Pharmacokinetics Protocol
 Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Pharmacodynamic indices in targeting therapy of critical infections
 Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
BSWH Pharmacist Continuing Education PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin
 BSWH Pharmacist Continuing Education 2015 PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin Objectives Define basic pharmacodynamic and pharmacokinetic principles Describe
BSWH Pharmacist Continuing Education 2015 PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin Objectives Define basic pharmacodynamic and pharmacokinetic principles Describe
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
CAT. Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators. Apr. Glynis Frans Supervisor: Prof. Apr.
 CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
Arnold L. Smith, MD; Stanley B. Fiel, MD, FCCP; Nicole Mayer-Hamblett, PhD; Bonnie Ramsey, MD; and Jane L. Burns, MD
 Susceptibility Testing of Pseudomonas aeruginosa Isolates and Clinical Response to Parenteral Antibiotic Administration Lack of Association in Cystic Fibrosis Arnold L. Smith, MD; Stanley B. Fiel, MD,
Susceptibility Testing of Pseudomonas aeruginosa Isolates and Clinical Response to Parenteral Antibiotic Administration Lack of Association in Cystic Fibrosis Arnold L. Smith, MD; Stanley B. Fiel, MD,
Paul Beringer,* Amir Aminimanizani,* Timothy Synold, and Christy Scott
 Therapeutic Drug Monitoring 24:315 321 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Development of Population Pharmacokinetic Models and Optimal Sampling Times for Ibuprofen Tablet and Suspension
Therapeutic Drug Monitoring 24:315 321 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Development of Population Pharmacokinetic Models and Optimal Sampling Times for Ibuprofen Tablet and Suspension
VANCOMYCIN DOSING AND MONITORING GUIDELINES
 VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
Optimizing Drug Exposure
 Optimizing Drug Exposure All Patients Are Not Average Michael Neely, MD, MSc Associate Professor, Pediatrics Keck School of Medicine, University of Southern California Laboratory of Applied Pharmacokinetics
Optimizing Drug Exposure All Patients Are Not Average Michael Neely, MD, MSc Associate Professor, Pediatrics Keck School of Medicine, University of Southern California Laboratory of Applied Pharmacokinetics
AMINOGLYCOSIDES TDM D O N E B Y
 AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
TDM of Aminoglycoside Antibiotics
 TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
Policy: Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
 ProMedica Health System Clinical Interdepartmental Policy and Procedure: Section: Policy: Date: Subject: Pharmacy Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
ProMedica Health System Clinical Interdepartmental Policy and Procedure: Section: Policy: Date: Subject: Pharmacy Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia
 Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects
 Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients
 Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Reassessment of Recommended Imipenem Doses in Febrile Neutropenic Patients with. Haematological Malignancies ACCEPTED
 AAC Accepts, published online ahead of print on 1 December 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00891-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 1 December 2008 Antimicrob. Agents Chemother. doi:10.1128/aac.00891-08 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions.
Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first dose: Can we do it with standard dosing?
 Oral session: PK/PD-based optimized broad-spectrum beta-lactam therapy (Sunday 10 April, 11:30) Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first
Oral session: PK/PD-based optimized broad-spectrum beta-lactam therapy (Sunday 10 April, 11:30) Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first
SCMID Online Lecture Library. by author. Optimizing antimicrobial therapy in the elderly. Dose Finding - The Past
 Optimizing antimicrobial therapy in the elderly Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Dosing should be such that the level of antmicrobial activity is associated
Optimizing antimicrobial therapy in the elderly Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Dosing should be such that the level of antmicrobial activity is associated
Pharmacokinetic parameters: Halflife
 Pharmacokinetic parameters: Halflife (t 1/2 ) 1. By definition t 1/2 is the time required for the concentration to fall by one half. For drugs with first order kinetics this is a constant. 2. Half-life
Pharmacokinetic parameters: Halflife (t 1/2 ) 1. By definition t 1/2 is the time required for the concentration to fall by one half. For drugs with first order kinetics this is a constant. 2. Half-life
Medication Dosing in CRRT
 Medication Dosing in CRRT Linda Awdishu, PharmD, MAS Associate Clinical Professor of Pharmacy and Medicine Learning Objectives 1. List the pharmacokinetic changes associated with AKI. 2. Determine the
Medication Dosing in CRRT Linda Awdishu, PharmD, MAS Associate Clinical Professor of Pharmacy and Medicine Learning Objectives 1. List the pharmacokinetic changes associated with AKI. 2. Determine the
D DAVID PUBLISHING. 1. Introduction. Kathryn Koliha 1, Julie Falk 1, Rachana Patel 1 and Karen Kier 2
 Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Novel Therapies for NTM
 NTM Lecture Series for Providers Novel Therapies for NTM Kenneth N Olivier, MD, MPH Laboratory of Chronic Airway Infection Chief, Pulmonary Branch/DIR October 20, 2017 Disclosures Past: Cooperative Research
NTM Lecture Series for Providers Novel Therapies for NTM Kenneth N Olivier, MD, MPH Laboratory of Chronic Airway Infection Chief, Pulmonary Branch/DIR October 20, 2017 Disclosures Past: Cooperative Research
JAC Efficacy and tolerance of roxithromycin versus clarithromycin in the treatment of lower respiratory tract infections
 Journal of Antimicrobial Chemotherapy (1998) 41, Suppl. B, 69 73 JAC Efficacy and tolerance of roxithromycin versus clarithromycin in the treatment of lower respiratory tract infections G. Tatsis*, G.
Journal of Antimicrobial Chemotherapy (1998) 41, Suppl. B, 69 73 JAC Efficacy and tolerance of roxithromycin versus clarithromycin in the treatment of lower respiratory tract infections G. Tatsis*, G.
Cystic Fibrosis: Pulmonary Exacerbations Management Guidelines
 Cystic Fibrosis: Pulmonary Exacerbations Management Guidelines Inclusion Criteria: Age 1 year with cystic fibrosis admitted for a pulmonary exacerbation. Exclusion Criteria: ICU Admission Newborn with
Cystic Fibrosis: Pulmonary Exacerbations Management Guidelines Inclusion Criteria: Age 1 year with cystic fibrosis admitted for a pulmonary exacerbation. Exclusion Criteria: ICU Admission Newborn with
D DAVID PUBLISHING. Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within a Therapeutic Range. 1.
 Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece
 A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
Full title of guideline INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS. control
 Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Marcos I. Restrepo, MD, MSc, FCCP
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS:
 MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
The promise of nebulized antibiotic therapy
 1 st ATHENA International Conference Athens, 19-20 November 2015 Let s Talk About Inhaled Antibiotics Inhaled Antibiotics: The Story Stijn BLOT Dept. of Internal Medicine Faculty of Medicine & Health Science
1 st ATHENA International Conference Athens, 19-20 November 2015 Let s Talk About Inhaled Antibiotics Inhaled Antibiotics: The Story Stijn BLOT Dept. of Internal Medicine Faculty of Medicine & Health Science
CCLI. Bronchiectasis Treatment Antibiotics. Charles Haworth. Physician / Patient Conference, Georgetown University, May 2017
 Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
British Journal of Clinical Pharmacology
 British Journal of Clinical Pharmacology DOI:10.1111/j.1365-2125.2006.02730.x Continuous vs. intermittent cefotaxime administration in patients with chronic obstructive pulmonary disease and respiratory
British Journal of Clinical Pharmacology DOI:10.1111/j.1365-2125.2006.02730.x Continuous vs. intermittent cefotaxime administration in patients with chronic obstructive pulmonary disease and respiratory
Antibiotic Usage Related to Microorganisms Pattern and MIC
 Antibiotic Usage Related to Microorganisms Pattern and MIC DR. Dr. Latre Buntaran Sp.MK(K) Secretary General PERDALIN Head of Compartment of Infection Control PERSI Doripenem: Potent
Antibiotic Usage Related to Microorganisms Pattern and MIC DR. Dr. Latre Buntaran Sp.MK(K) Secretary General PERDALIN Head of Compartment of Infection Control PERSI Doripenem: Potent
Pharmacokinetic-Pharmacodynamic (PKPD) Modeling Characterizing Resistance for Predictions of Bacterial Kill in vivo
 Pharmacokinetic-Pharmacodynamic (PKPD) Modeling Characterizing Resistance for Predictions of Bacterial Kill in vivo Anders Kristoffersson Pascale David- Pierson, Neil John Parrott, Olaf Kuhlmann, Thierry
Pharmacokinetic-Pharmacodynamic (PKPD) Modeling Characterizing Resistance for Predictions of Bacterial Kill in vivo Anders Kristoffersson Pascale David- Pierson, Neil John Parrott, Olaf Kuhlmann, Thierry
Therapeutic drug monitoring of β-lactams
 CORATA Belgique Reims 1-2/10/2014 Therapeutic drug monitoring of β-lactams Frédéric Cotton Clinical Chemistry Erasme Hospital Faculty of Pharmacy ULB TDM of β-lactams β-lactams pharmacokinetics pharmacodynamics
CORATA Belgique Reims 1-2/10/2014 Therapeutic drug monitoring of β-lactams Frédéric Cotton Clinical Chemistry Erasme Hospital Faculty of Pharmacy ULB TDM of β-lactams β-lactams pharmacokinetics pharmacodynamics
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
Terapia delle infezioni da Pseudomonas aeruginosa MDR
 Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Title: Cefoxitin Continuous Infusion for Lung Infection Caused by M. abscessus group
 AAC Accepts, published online ahead of print on 14 April 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.02763-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 Title: Cefoxitin
AAC Accepts, published online ahead of print on 14 April 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.02763-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 Title: Cefoxitin
ASHP Therapeutic Position Statements 623
 ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
Approximately 70,000 patients worldwide have cystic fibrosis
 crossmark Bayesian Estimation of Tobramycin Exposure in Patients with Cystic Fibrosis Michael A. Barras, a,b * David Serisier, c Stefanie Hennig, b Katrina Jess, c Ross L. G. Norris a,b * Pharmacy Department,
crossmark Bayesian Estimation of Tobramycin Exposure in Patients with Cystic Fibrosis Michael A. Barras, a,b * David Serisier, c Stefanie Hennig, b Katrina Jess, c Ross L. G. Norris a,b * Pharmacy Department,
ESCMID Online Lecture Library. by author
 Novel PK/PD data on the optimisation of colistin and the carbapenems Diamantis Plachouras Athens, Greece Hot Topics on Infections in the Critically Ill Patient, ESCMID Postgraduate Education Course, 31
Novel PK/PD data on the optimisation of colistin and the carbapenems Diamantis Plachouras Athens, Greece Hot Topics on Infections in the Critically Ill Patient, ESCMID Postgraduate Education Course, 31
PHARMACOKINETICS SMALL GROUP II:
 PHARMACOKINETICS SMALL GROUP II: Question 1 Why are some drug therapies initiated with a loading dose? Emphasize that LD establishes initial therapeutic level quickly. The time to reach the steady-state
PHARMACOKINETICS SMALL GROUP II: Question 1 Why are some drug therapies initiated with a loading dose? Emphasize that LD establishes initial therapeutic level quickly. The time to reach the steady-state
Joint Trust Guideline for the Use of Intravenous Vancomycin in Paediatrics
 A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
The CLSI Approach to Setting Breakpoints
 The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
NORLAND AVENUE PHARMACY PRESCRIPTION COMPOUNDING FOR GENERAL PRACTICE
 APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
Journal Club The ELITE Trial. Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010
 Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
There has been a renewed interest in the use of
 consensus conference Use of Aerosolized Antibiotics in Patients With Cystic Fibrosis Chairpersons: Preston W. Campbell III, MD, and Lisa Saiman, MD* (CHEST 1999; 116:775 788) Abbreviations: CF cystic fibrosis;
consensus conference Use of Aerosolized Antibiotics in Patients With Cystic Fibrosis Chairpersons: Preston W. Campbell III, MD, and Lisa Saiman, MD* (CHEST 1999; 116:775 788) Abbreviations: CF cystic fibrosis;
Setting The setting was hospital and the economic analysis was carried out in the Netherlands.
 Impact of goal-oriented and model-based clinical pharmacokinetic dosing of aminoglycosides on clinical outcome: a cost-effectiveness analysis van Lent-Evers N A, Mathot R A, Geus W P, van Hout B A, Vinks
Impact of goal-oriented and model-based clinical pharmacokinetic dosing of aminoglycosides on clinical outcome: a cost-effectiveness analysis van Lent-Evers N A, Mathot R A, Geus W P, van Hout B A, Vinks
NIH Public Access Author Manuscript Am J Nephrol. Author manuscript; available in PMC 2015 January 22.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Nephrol. 2012 ; 36(2): 144 150. doi:10.1159/000339937. Gentamicin Pharmacokinetics and Pharmacodynamics during Short-daily Hemodialysis
NIH Public Access Author Manuscript Published in final edited form as: Am J Nephrol. 2012 ; 36(2): 144 150. doi:10.1159/000339937. Gentamicin Pharmacokinetics and Pharmacodynamics during Short-daily Hemodialysis
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2016
 Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2016 Sarah Gierhart and Uzo Chukwuma Approved for public release. Distribution is unlimited. The views
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2016 Sarah Gierhart and Uzo Chukwuma Approved for public release. Distribution is unlimited. The views
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review)
 Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches
 Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Pseudomonas aeruginosa eradication guideline
 SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
High-Dose Levofloxacin for the Treatment of Community-Acquired Pneumonia
 High-Dose Levofloxacin for the Treatment of Community-Acquired Pneumonia Review Andrew F. Shorr, MD, MPH, FCCP Department of Medicine Pulmonary and Critical Care Medicine, Washington Hospital Center, Washington,
High-Dose Levofloxacin for the Treatment of Community-Acquired Pneumonia Review Andrew F. Shorr, MD, MPH, FCCP Department of Medicine Pulmonary and Critical Care Medicine, Washington Hospital Center, Washington,
Department of Clinical Pharmacy, University of Michigan College of Pharmacy, Pharmacy Faculty, Siam University, Bangkok, Thailand
 1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
TDM. Measurement techniques used to determine cyclosporine level include:
 TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
Cubicin A Guide to Dosing
 Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Nephrotoxicity. Pros and Cons of the article: Relationship between Initial Vancomycin
 Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Aminoglycosides. Not orally absorbed. Interact with negatively charged lipopolysaccharide on Gram- cell wall. Aminoglycoside properties
 Aminoglycosides Tobramycin Kanamycin H2N Gentamicin Amikacin NHCOCHCH2CH2NH2 OH Aminoglycosides made of linked sugars. Decorated with many OH and NH2 groups, which render these compounds positively charged
Aminoglycosides Tobramycin Kanamycin H2N Gentamicin Amikacin NHCOCHCH2CH2NH2 OH Aminoglycosides made of linked sugars. Decorated with many OH and NH2 groups, which render these compounds positively charged
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
