Scottish Paediatric Endocrine Group Managed Clinical Network (SPEG MCN) Dynamic Function Test Handbook for Clinicians
|
|
|
- Rebecca Maxwell
- 6 years ago
- Views:
Transcription
1 Scottish Paediatric Endocrine Group Managed Clinical Network (SPEG MCN) Dynamic Function Test Handbook for Clinicians January 2012 Review October 2013
2 CONTENTS INTRODUCTION 1 DYNAMIC FUNCTION TESTS 2 1. GLUCOSE TOLERANCE TEST 3 2. LUTEINISING HORMONE RELEASING HORMONE (LHRH) TEST 5 3. HUMAN CHORIONIC GONADOTROPHIN (HCG) STIMULATION TEST 7 4. GROWTH HORMONE STIMULATION TESTS INSULIN TOLERANCE TEST ARGININE STIMULATION TEST FOR GROWTH HORMONE CLONIDINE TEST FOR GROWTH HORMONE STANDARD SHORT SYNACTHEN TEST WATER DEPRIVATION TEST DEXAMETHASONE SUPPRESSION TEST 20 APPENDIX 1 22 SPEG DFT handbook i
3 INTRODUCTION This handbook is for clinicians managing children with endocrine disorders in Scotland, and sets out standard ways of performing dynamic function tests. This is a consensus document of good practice and evidence where available. It has been collated by the Scottish Paediatric Endocrine Group MCN (SPEGMCN) Protocols sub-group. This document is available in electronic form at: Levels of paediatric endocrine care: The British Society for Paediatric Endocrinology and Diabetes (BSPED) has recently produced standards advising on 3 levels of paediatric endocrine care: df This handbook covers all 3 levels of care. In following the guidelines within, the clinician must be aware of the level of care which they can provide from their centre so should not enter in to the management of cases without understanding these advised standards. For example, although the protocol for the insulin tolerance test is described within this guide, this should only be carried out within centres that do it regularly i.e., more than 12 times per year. If in doubt about the necessity or practicality of performing any of these tests in your local centre, you must discuss this with your local paediatric endocrinologist or named paediatrician. Level 1: Conditions with a low level of anticipated need for input from a paediatrician with an interest in endocrinology - managed in most cases by local general paediatricians. Level 2: Conditions with a need for input from a paediatrician with an interest in endocrinology usually managed at local DGH clinics with occasional input from a paediatric endocrinologist at regional level on a shared care basis with the local teams. For some conditions the initial diagnostic investigations may need to be undertaken at the lead centre. Level 3: Conditions which require all or some management from a paediatric endocrinologist at regional level. These conditions are managed solely by a regional unit or through a network of endocrine clinics at the DGH, performed in combination by a regional paediatric endocrinologist and a local paediatrician with an interest in endocrinology. Some conditions that require Multi-disciplinary team (MDT) input from a number of specialists through joint clinics at regional or supra-regional level will require attendance at specialist centres for some of their visits. SPEG DFT handbook
4 DYNAMIC FUNCTION TESTS SPEG DFT handbook
5 1. GLUCOSE TOLERANCE TEST Indications The 2 hour standard oral glucose tolerance test may be used to: Establish a diagnosis of Diabetes Mellitus. It is unnecessary if a child has symptoms of diabetes and either a random venous plasma laboratory glucose concentration of 11.1 mmol/l or higher, or a fasting concentration of 7.0 mmol/l or higher. [Definition, Diagnosis and Classification of Diabetes Mellitus. WHO criteria 1999]. Glucose is measured at 0 min and 120 min only. Assess Insulin Resistance if indicated ( see insulin resistance section below) In addition to the standard procedure glucose and insulin are measured at 0, 30, 60, 90 and 120 min. Preparation 1. Do not perform glucose tolerance tests on patients known to be suffering from an infection, patients with uncontrolled thyroid dysfunction, or patients recovering from stress (e.g. surgery) as these alter insulin sensitivity. 2. Ensure that the child has had an adequate diet (minimum of 150g/day of carbohydrate) for at least 5 days before the test. Fast the patient overnight (4 hours for infants) but avoid more prolonged fasting. Drinks of water (no sweet drinks) are allowed during this period. 3. Calculate amount of glucose to be given a) Glucose monohydrate g/kg (not to exceed 82.5 g - equivalent to 75g anhydrous glucose, the standard adult dose). Dissolve the dose in mls chilled water. b) Standard Original High Glucose Drink e.g. Lucozade (45g glucose/m 2, max dose 75g (1g glucose per 5.5mls original Lucozade)). Procedure Time 0 min (~9 AM) 0 min Action INSERT a reliable cannula TAKE venous blood sample for laboratory glucose (and insulin if indicated). GIVE Glucose drink. The drink should be fully consumed in 5-10 minutes. 120 min TAKE Venous blood for lab glucose (If test is being carried out to investigate Insulin Resistance collect venous blood samples at 0, 30, 60, 90 and 120 min for glucose + insulin) Interpretation SPEG DFT handbook
6 [Diagnosis and Classification of Diabetes Mellitus. WHO criteria 1999; Expert Committee on the Diagnosis and Classification of Diabetes Mellitus 2003] Normal fasting plasma glucose is <5.6 mmol/l Normal glucose tolerance is defined by a 2 hour plasma glucose <7.8 mmol/l Diabetes Should be diagnosed only when the 2 hour plasma glucose is 11.1 mmol/l or higher. In patients without symptoms diagnosis should not be based on a single glucose determination. At least one additional glucose test result with a value in the diabetic range is required, either fasting, random or 2 hours after a standard glucose load. Impaired glucose tolerance Is defined by a fasting plasma glucose <7.0 mmol/l and a 2 hour glucose between 7.8 and 11.1 mmol/l. Impaired fasting glycaemia Is defined by a fasting plasma glucose between 5.6 and 7.0 mmol/l and a 2 hour concentration <7.8 mmol/l. Insulin resistance According to the recent consensus statement there is no clear cut offs to define insulin resistance in children and surrogate measures such as fasting insulin are not ideal. (For more info, see Insulin resistance in children: consensus, perspective, and future directions. Levy-Marchal C, et al; Insulin Resistance in Children Consensus Conference Group. J Clin Endocrinol Metab Dec; 95(12): ) Based on current screening criteria and methodology, there is no justification for screening children for insulin resistance related to obesity We recommend, in normal individuals, o o o o Fasting insulin is <10 mu/l in children younger than 10 years or <20 mu/l in children older than 10 years. Peak insulin during the test is normally <100 mu/l. Fasting insulin of mu/l or peak insulin of mu/l is suggestive of mild to moderate insulin resistance. Fasting insulin of >50 mu/l or peak insulin of >300 mu/l is suggestive of severe insulin resistance. SPEG DFT handbook
7 2. LUTEINISING HORMONE RELEASING HORMONE (LHRH) TEST Indications LHRH is an oligopeptide hormone secreted by the hypothalamus, which controls the release of luteinising hormone (LH) and follicle stimulating hormone (FSH) by the anterior pituitary gland. In older children and adults, loss of the LH and FSH response to LHRH may be an early indication of anterior pituitary disease. The LHRH test described here assesses the level of LH/FSH pituitary reserve. It may be used to investigate pubertal disorders including precocious puberty, premature breast development in girls (thelarche) and delayed puberty. This test may be combined with Growth Stimulation tests; increase volumes of blood collected accordingly. Avoid HCG injections during the test, as cross-reaction in LH analyses gives falsely elevated results. Preparation There is no need to fast and the time of commencing the test is not important, unless combined with the insulin hypoglycaemia test. Insert cannula 30 min before test. Procedure Time 1 0 min 2 0 min Action INSERT a reliable cannula TAKE Baseline blood for LH, FSH, Oestradiol (females), Testosterone (males) GIVE Dose of LHRH (GnRH, gonadorelin) 100 micrograms IV over 2 min regardless of weight and age 3 20 min TAKE Blood for LH, FSH 4 60 min TAKE Blood for LH, FSH Interpretation The LHRH test is often difficult to interpret and results should be interpreted alongside clinical findings; including full pubertal staging, testicular volume (boys) or ovarian ultrasound (girls). Puberty is a continuum and so is the response to the GnRH test. Prepubertal responses: LH peak <5 U/L (LH increment less than 3-4 U/L above basal). FSH peak greater than LH (FSH increment less than 2-3 U/L above basal). Peripubertal and pubertal responses: higher increments, especially if LH dominant, provide evidence of a pubertal pattern of gonadotrophin response: LH peak >5 U/L, with LH peak greater than FSH peak. Pubertal Delay and Pubertal failure: In children with suspected hypogonadotrophic hypogonadism (HH), a complete lack of response supports the diagnosis. However, a SPEG DFT handbook
8 measurable but low response (in the prepubertal range) may occur both in HH and in constitutional delay of puberty and has limited predictive value. In primary gonadal failure, basal LH and FSH are elevated and their response to GnRH is exaggerated. Precocious puberty: In gonadotrophin-independent precocious puberty spontaneous gonadotrophin secretion is suppressed by the autonomous sex steroid secretion, basal LH/FSH is low and response to LHRH is flat. In gonadotrophin-dependent precocious puberty basal LH/FSH levels are usually (but not always) elevated and the response to LHRH is exaggerated. Precocious puberty (treated): Suppressed basal LH/FSH and flat response to LHRH indicate adequate treatment with LHRH analogues. Premature thelarche and thelarche variant: LH response is usually in the prepubertal range and there is a FSH predominant response. SPEG DFT handbook
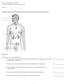
9 3. HUMAN CHORIONIC GONADOTROPHIN (HCG) STIMULATION TEST (From the Scottish DSD Network) Introduction Any child with an external masculinisation score (EMS, refer Figure 1) of below 11 requires further evaluation of the gonadal axis. HCG stimulation of the testes may not be necessary in early infancy and prolonged hcg test stimulation is usually not necessary in infancy. For investigation of gonadal function, the standard hcg stimulation test performed over week 1 is sufficient in many cases but some cases may require prolonged hcg stimulation. The prolonged hcg stimulation test may be a useful means of investigating the endocrine gonadal axis after infancy when the testes are nascent. They may also aid the descent of the undescended testes which are not completely impalpable. The timing of the tests is important and the results may be influenced by age and the test may influence surgical and medical management. If both gonads have never been palpable or detected, a karyotype result should be sought before embarking on the following investigative protocol, particularly in the apparent boy with premature virilisation. Record all investigations performed. Figure 1 SPEG DFT handbook
10 Procedure See table below: WEEK Wk1 Wk2 Wk3 Wk4 >Wk8 Date Day Mon Tue Wed Thu Mon Thu Mon Thu Mon COLLECT: Serum Testosterone, * * * SHBG 1 Serum Androstenedione, * * DHT, DHEAS 2 Serum AMH 3 * Urine Steroid Profile 3 * LHRH Stim Test (0,20,60min) * Karyotype & DNA 3 * GIVE: HCG 1500 IM * * * * * * * EXAMINE: Ultrasound scan of Testes * & Renal Tracts 4 Stretched Penile length * * * Examine for Testes (Scrotal, Ing, Abdo, Absent) * * * Endocrine Follow-up * Table 1 SPEG DFT handbook
11 1 Serum for Testosterone is very important; SHBG is much less important, particularly in infants 2 These androgens are listed in order of priority with Androstenedione being most important 3 These samples should preferably be collected on the first day but can be collected on any visit 4 All children with a DSD should have an ultrasound scan of the renal tracts Follow-Up Arrange endocrine clinic follow-up for 6 weeks after end of investigations. Some children with poor testosterone response to hcg may require further assessment of adrenal function. SPEG DFT handbook
12 4. GROWTH HORMONE STIMULATION TESTS Indication Assessment of growth hormone deficiency These tests are often combined with the LHRH test; the volume of blood collected will need to be increased accordingly. The ITT (Insulin Tolerance Test) The insulin hypoglycaemia test (also known as the insulin tolerance test, ITT) is recognised as the gold standard for assessment of growth hormone deficiency, particularly as it also tests the hypothalamo-pituitary-adrenal axis. This is a potentially high risk test and should only be carried out in a specialist centre where the test is being performed on a regular basis by experienced staff. The Arginine Test for Growth Hormone Where the ITT is not recommended or not suitable the first line test should be the Arginine test. Clonidine test for Growth Hormone The clonidine test is also an acceptable test for growth hormone. Other Tests: The Glucagon test and Exercise test for assessment of growth hormone deficiency are not recommended, due to problems with late hypoglycaemia and poor reproducibility of results, respectively. Priming before the test If the test is to be done on peri-pubertal children (bone age greater than 10 years, no signs of puberty in girls or testicular volume less than 8mL in boys), discuss with local paediatric endocrinologist the advisability of priming with the appropriate sex steroid. SPEG DFT handbook
13 4.1 INSULIN TOLERANCE TEST Indications Any form of stress results in secretion of the hypothalamic hormones, growth hormone releasing hormone (GHRH) and corticotrophin releasing hormone (CRH). These in turn stimulate the release of pituitary growth hormone (GH) and adrenocorticotrophic hormone (ACTH), in the latter case leading to adrenal cortisol secretion. Insulin administration is used to produce stress in the form of hypoglycaemia, and hypothalamic - pituitary - adrenal function is assessed by GH and cortisol responses to the hypoglycaemic stimulus. This test is designed to produce symptomatic hypoglycaemia (palor, sweating). If symptoms are more severe (impaired or loss of consciousness) the child must be treated immediately (see below). Continuous observation for the symptoms of severe hypoglycaemia is essential throughout the test, and for half an hour after its completion. Contraindications No child with a history of epilepsy or cardiac arrhythmias should undergo this test Please use with caution in young children, as symptoms of hypoglycaemia may be difficult to detect. Preparation The patient should be fasted overnight (4 hours for infants); drinks of water are allowed. Before beginning the test, have available glucose drink: 4 heaped teaspoons (equivalent to approximately 40g) dextrose powder dissolved in approximately half a glass of squash. Alternatively standard glucose drink e.g. Lucozade 50mls. Ensure that glucose, and hydrocortisone are also available for intravenous injection, if necessary (see emergency treatment of severe hypoglycaemia, below). Observe the child continuously during the test for symptoms of severe hypoglycaemia, and check the glucose concentration in each blood sample collected using the ward blood glucose meter or more frequently if the child is developing hypoglycaemic symptoms. If symptoms of severe hypoglycaemia do develop they must be treated immediately. See below. Before beginning the test, weigh the patient and insert a cannula at least 30 minutes before taking the baseline samples. The patient should be resting throughout the test. Start the test between 0800h and 0900h. SPEG DFT handbook
14 Emergency treatment of severe hypoglycaemia during the ITT If the child does not tolerate oral glucose, or shows signs of severe hypoglycaemia (reduced conscious level) give iv treatment by giving intravenous glucose 200 mg per kg body weight (10% dextrose, 2mL per kg) over 3 minutes. If the response is poor, give 100 mg hydrocortisone by intravenous injection. Continue with a glucose infusion iv at 10 mg per kg per minute (6 millilitres per kilogram per hour of 10% dextrose). Check blood glucose using the ward meter after 5 min and adjust the glucose infusion to maintain a blood glucose of 5-8 mmol/l and no higher. If there is no improvement in conscious level after normal blood glucose is restored, an alternative explanation should be sought. It is not necessary to discontinue the test and, if possible, continue blood sampling. IMPORTANT 50% dextrose should NEVER be used in the resuscitation of a child with severe hypoglycaemia following an endocrine test. SPEG DFT handbook
15 Procedure 1 2 TIME -30 min 0 min ACTION INSERT a reliable cannula TAKE Blood for glucose, cortisol and GH determinations. (+ ward meter glucose) TAKE baseline blood sample for glucose, cortisol and GH. (+ ward meter glucose) 3 If blood glucose, measured using the ward meter, is less than 3.5 mmol/l in either of the two baseline samples, do NOT give insulin but continue to take blood samples (see below) and record whether child has symptoms (pale, sweating). If blood glucose, measured using the ward meter, is between 3.5 and 4.5 mmol/l in either of the two baseline samples, give half the dose of insulin (see below) and continue the test. 4 0 min GIVE IV soluble insulin (Actrapid) diluted with normal saline to give a solution containing 1 unit per ml. Dose = 0.1 units per kg body weight (Reduced to 0.05 units per kg in patients who might be unduly sensitive to insulin. These include patients with suspected hypofunction, those with severe malnutrition (e.g. due to anorexia nervosa) or those with baseline blood glucose between 3.5 and 4.5 mmol/l) 5 When adequate hypoglycaemia has been established (< 2.2 mmol/l laboratory blood glucose or a 50% reduction in the baseline level), or if the child shows signs of hypoglycaemia (e.g. is sweaty and drowsy), a glucose drink should be given - see preparation notes above. If this is not tolerated, or if there are more severe symptoms of hypoglycaemia (impaired or loss of consciousness), intravenous glucose may be required see above. NOTE ward meters frequently overestimate blood glucose levels min TAKE blood samples for glucose, cortisol and GH (+ ward meter glucose) 7 30 min TAKE blood samples for glucose, cortisol and GH (+ ward meter glucose) 8 60 min TAKE blood samples for glucose, cortisol and GH (+ ward meter glucose) 9 90 min TAKE blood samples for glucose, cortisol and GH (+ ward meter glucose) After the test Give a sweet drink and a meal after the test and ensure that the meal has been eaten. Keep the child under observation for at least 1 hour after the meal has been consumed. Keep the cannula in position until lunch has been assimilated. Ensure that a blood glucose measured on the ward meter reads greater than 4 mmol/l before discharge. If there is any doubt about the child's wellbeing, keep him/her in overnight for observation. SPEG DFT handbook
16 Interpretation If Growth Hormone >5ug/l at any point this indicates there is a normal response, which rules out growth hormone deficiency. If Growth Hormone <5ug/l in the presence of adequate hypoglycaemia (<2.2mmol/l or 50% drop in plasma glucose < 5ug/L indicates a growth hormone deficiency. Hypoglycaemia of this magnitude should also cause an increase in the plasma cortisol. Please check with local labs for cut offs. SPEG DFT handbook
17 4.2 ARGININE STIMULATION TEST FOR GROWTH HORMONE Indications Short stature and/or consistent abnormally low growth velocity. Growth hormone deficiency Preparation Patient to have water only for 8 hours prior to the test. Arginine may cause nausea and some irritation at the infusion site. Procedure 1 2 TIME -30 MINS -30 MINS ACTION INSERT a reliable cannula, TAKE blood for growth hormone baseline test. INFUSE arginine monohydrochloride IV over half an hour in a dose of 0.5g/kg up to a maximum of 30g (discuss with local pharmacist) 3 0 MINS STOP infusion mins + 15 mins (if also LHRH) + 30 mins + 60 mins + 90 mins + 120mins TAKE samples for growth hormone and glucose (+ ward meter glucose) Samples In children with suspected hypopituitarism prolonged fasting may induce hypoglycaemia. Blood glucose should be checked by ward meter with each sample in these patients whenever a sample is taken. Note This test can be combined with synacthen test to assess HPA axis in addition to growth hormone deficiency Interpretation If the plasma GH concentration reaches 6 ug/l or more, further investigations are not indicated. If the response is below this level, then an insulin hypoglycaemia test may be necessary. SPEG DFT handbook
18 4.3 CLONIDINE TEST FOR GROWTH HORMONE Indication This test is used in the investigation of suspected Growth Hormone (GH) deficiency in childhood (not in adults). Clonidine is administered orally to provoke GH release. Preparation Fast the patient overnight (4h for infants), and measure height and weight. Calculate surface area from appropriate tables. Start the test by 0900h whenever possible. Procedure TIME 1-30 min ACTION INSERT reliable canula TAKE blood sample for GH 2 0 min (~09:00) TAKE blood sample for GH 3 0 min GIVE Clonidine (150 micrograms per m 2 body surface area) by mouth with a small, sugar-free drink. Round up the calculated dose to the nearest 25 micrograms. (after completion) 4 30 min TAKE blood sample for GH 5 60 min TAKE blood sample for GH 6 90 min TAKE blood sample for GH min TAKE blood sample for GH min TAKE blood sample for GH After the test Side effects of Clonidine (hypotension and drowsiness) may persist for several hours after the test. Keep the patient lying down for at least an hour after the test, and check pulse and blood pressure half-hourly and also before allowing him/her to get up. Careful observation of the patient is necessary until late afternoon. Interpretation If the plasma GH concentration reaches 6 ug/l or more, further investigations are not indicated. If the response is below this level, then an insulin hypoglycaemia test may be necessary. SPEG DFT handbook
19 5.0 STANDARD SHORT SYNACTHEN TEST Indications The synthetic polypeptide Synacthen (Tetracosactrin BP) has a structure identical to the N-terminal 24 amino acids of Adrenocorticotrophic Hormone (ACTH). It has a short duration of action and permits a rapid and convenient screening test for the assessment of adrenocortical function by measuring cortisol response. Measurement of additional adrenal steroids during the test (at the same time as the samples for cortisol - see below) may also be used to assess the steroid biosynthetic pathway. Plasma 17-hydroxyprogesterone (17-OHP) measurements may assist in the diagnosis of non-salt-losing congenital adrenal hyperplasia. If a defect in steroid biosynthesis is suspected, also collect a random urine specimen for a full steroid profile before the Synacthen test. Preparation 1. Prednisolone and hydrocortisone both interfere with the measurement of cortisol. If the patient is already on hydrocortisone ask the patient to omit their doses the evening before and on the morning of the test. The patient should continue taking the hydrocortisone immediately after the test whilst waiting for results. The Synacthen test should not be performed if the patient has been on Prednisolone within the last 2 weeks. 2. The patient need not be fasting. Insert a cannula at least 30 minutes before taking the baseline sample. Procedure TIME 1 0 min 2 0 min ACTION INSERT a reliable cannula TAKE blood for cortisol GIVE Synacthen (tetracosactride) IV and flush in well with 0.9% saline. For children, the dose is 250 micrograms. For neonates and infants <7kg, dose by weight is 36 micrograms/kg (rounded to the nearest 25 micrograms) 3 30 min TAKE blood for cortisol 4 60 min TAKE blood for cortisol Interpretation Cortisol responses at 60 min are usually >650 nmol/l in children <6y, or >470 nmol/l in children 6-18y. The exact values of cortisol cutoffs will be affected by the method used. Please consult your local laboratory. SPEG DFT handbook
20 Interpretation of plasma 17-OHP depends on age and clinical presentation. Both adults and children usually have baseline 17-hydroxyprogesterone concentrations less than 6 nmol/l. In late onset congenital adrenal hyperplasia, the baseline 17-hydroxyprogesterone may be either normal or high, but there is an exaggerated response (>30nmol/l) to Synacthen stimulation SPEG DFT handbook
21 6.0 WATER DEPRIVATION TEST This test is used when the diagnosis of Diabetes Insipidus (DI) is in doubt. As most cases of DI can be confirmed or excluded on history and baseline investigations, this test is generally not recommended. This test can be potentially dangerous and is very distressing to the patient. We suggest patients should be discussed with the tertiary centre before consideration of the test. It maybe more appropriate for the test to be carried out in the tertiary centre. For this reason, a protocol for the water deprivation test is not part of this handbook PSYCHOGENIC POLYDIPSIA: the vast majority of children who appear to be drinking too much have psychogenic polydipsia (habitual drinking), and are usually able to concentrate their urine appropriately. Many have become habitual juice drinkers and will reduce their intake if only water is offered. Assess after allowing access to water, but restricting juice and other flavoured fluids. (children with DI will continue to drink large amounts). Initially check an early morning urine for osmaolarity: >800 mosm/l will exclude Diabetes Insipidus <300 mosm/l - check an early morning fasting urine. Child should be allowed water only to drink the day before (no juice etc) Unusual features more likely to be seen in Diabetes Insipidus: drinking unusual fluids such as bath water, pets water drinking through the night new onset enuresis. If DI is still considered, please discuss with your tertiary centre. SPEG DFT handbook
22 7.0 DEXAMETHASONE SUPPRESSION TEST Indications This test is used to identify Cushings Syndrome. Initially the The Overnight Dexamethasone Suppression Test is used to screen. If there is a failure of suppression, a prolonged dexamethasone test may be required and this should be discussed with your local tertiary endocrinologist. In this case a The Prolonged (Low or high dose) Dexamethasone Suppression Test may help confirm Cushing s syndrome and elucidate the cause Overnight Dexamethasone Suppression Test Procedure 1 TIME Between 2300h and midnight ACTION GIVE the patient oral Dexamethasone (children 10 micrograms per kg body weight, adults 1 milligram. Dexamethasone is available as scored 500 microgram tablets - round the dose to the nearest 250 micrograms (i.e. half a tablet) h the next day Take blood for cortisol. Interpretation In normal subjects, the 0900h plasma cortisol is suppressed to less than 50 nmol/l. In patients with Cushing s syndrome, such marked suppression is not observed. Patients taking hepatic enzyme-inducing drugs (e.g. phenytoin, phenobarbitone) may have false negative results. SPEG DFT handbook
23 PROLONGED TESTS Low Dose Dexamethasone Suppression Test Indications Diagnosis of Cushing s syndrome. Precautions/Preparation Ensure that urine is collected for 24 hour urinary free cortisol and steroid profile before the test. Procedure TIME 1 Day ACTION TAKE blood samples for cortisol and ACTH. COMMENCE Urine collection for 24h urinary free cortisol and steroid profile 2 Day TAKE blood for cortisol and ACTH 3 Days 2 and 3 4 Day GIVE oral dexamethasone 0.5mg 6 hourly (or 20 micrograms/kg/dose 6-hourly for younger children) (Total of 8 doses) TAKE blood for cortisol and ACTH. Commence urine collection for 24h urinary free cortisol and steroid profile. Interpretation Normal: Cortisol level should suppress to <50nmol/L. Patients with Cushing s syndrome, from whatever cause, lose the normal negative feedback control by circulating glucocorticoids on ACTH release and thus exhibit detectable plasma ACTH and cortisol concentrations after dexamethasone administration. In patients who fail to suppress, a pre-test ACTH level of <5ng/L is highly suggestive of an adrenal cause of Cushing s syndrome. High Dose Dexamethasone Suppression Test Indications To differentiate pituitary-dependent and ectopic causes of Cushing s syndrome. Precautions/Preparation - nil SPEG DFT handbook
24 Procedure TIME ACTION 1 Day * Urine collection for 24h urinary free cortisol and steroid TAKE blood samples for cortisol and ACTH. Commence profile 2 Day TAKE blood for cortisol and ACTH 3 Days 2 and 3 4 Day GIVE oral dexamethasone 2mg 6 hourly (or 80 micrograms/kg/dose 6-hourly for younger children) (total of 8 doses) TAKE blood for cortisol and ACTH. Commence Urine collection for 24h urinary free cortisol and steroid profile. Low and high dose dexamethasone suppression tests may be performed sequentially if desired, in which case start high dose at 0600 on day after low dose test is completed Interpretation Pituitary-dependent hypercortisolism (Cushing s disease): plasma cortisol usually suppresses to at least 50% of basal values. NB Approximately 10% of patients with Cushing s disease fails to suppress and approximately 10% of those with ectopic ACTH secretion will suppress. SPEG DFT handbook
25 APPENDIX 1 Paediatric Endocrinologists Health Board Lothian Edinburgh Royal Hospital for Sick Children Glasgow and Clyde Glasgow Royal Hospital for Sick Children Grampian Royal Aberdeen Children s Hospital Tayside Ninewells Hospital Consultant Endocrinologists Dr Louise Bath, Consultant Endocrinologist Dr Harriet Miles, Consultant Endocrinologist Dr Guftar Shaikh, Consultant Endocrinologist Professor Faisal Ahmed, Consultant Endocrinologist Dr Malcolm Donaldson, Consultant Endocrinologist Dr Amalia Mayo, Consultant Paediatrician Dr Steve Greene, Consultant Paediatrician Paediatricians with an interest in Endocrinology Health Board Dumfries and Galloway Fife Victoria Infirmary Highland Raigmore Hospital Ayrshire and Arran Crosshouse Hospital Forth Valley Forth Valley Royal Borders Borders General Hospital Lanarkshire Wishaw General Hospital Consultant Paediatrician Dr Raj Shyam, Consultant Paediatrician Dr Ahmad Ainine, Consultant Paediatrician Dr George Farmer, Consultant Paediatrician Dr Scott Williamson, Consultant Paediatrician Dr Jon Staines, Consultant Paediatrician Dr John Schulga, Consultant Paediatrician Dr Andy Duncan, Consultant Paediatrician Dr Ian Hunter, Consultant Paediatrician SPEG DFT handbook
Audit of Adrenal Function Tests. Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK
 Audit of Adrenal Function Tests Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK Introduction Audit Overview of adrenal function tests Education Audit why? Explore
Audit of Adrenal Function Tests Kate Davies Senior Lecturer in Children s Nursing London South Bank University London, UK Introduction Audit Overview of adrenal function tests Education Audit why? Explore
Clinical Guideline. SPEG MCN Protocols Sub Group SPEG Steering Group
 Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
Endocrine part one. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE
 Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE Includes guidance for the distinction between adrenarche, precocious puberty and other
Clinical Guideline ADRENARCHE MANAGEMENT OF CHILDREN PRESENTING WITH SIGNS OF EARLY ONSET PUBIC HAIR/BODY ODOUR/ACNE Includes guidance for the distinction between adrenarche, precocious puberty and other
WARD INSTRUCTIONS WEBSITE
 DEPARTMENT OF CLINICAL CHEMISTRY NEW CROSS HOSPITAL WOLVERHAMPTON WARD INSTRUCTIONS WEBSITE Edition 1.1 SOP E1.120P.CHE Date issued: June 2016 Review interval: Authorised copy: Printed copies Author Location
DEPARTMENT OF CLINICAL CHEMISTRY NEW CROSS HOSPITAL WOLVERHAMPTON WARD INSTRUCTIONS WEBSITE Edition 1.1 SOP E1.120P.CHE Date issued: June 2016 Review interval: Authorised copy: Printed copies Author Location
Insulin Tolerance Test Protocol - RNS Endocrinology
 Page 1 of 7 - RNS Endocrinology Test name Insulin tolerance test. Alternate test names. Related Tests. Indication(s) Investigation of the hypothalamic pituitary axis (HPA) with regard to the release of
Page 1 of 7 - RNS Endocrinology Test name Insulin tolerance test. Alternate test names. Related Tests. Indication(s) Investigation of the hypothalamic pituitary axis (HPA) with regard to the release of
ASY-805.1: Insulin Tolerance Test. ASY-805.2: Associated Documents. ASY-805.3: Distribution of Documents. ASY-805.4: Review of Document: a b
 ASY-805.1: Insulin Tolerance Test ASY-805.2: Associated Documents a b Handbook page task print-out ASY-805.3: Distribution of Documents Copy No Number Location 1 Quality Centre 2 3.1 W232 3 3.20 W232 Laminated
ASY-805.1: Insulin Tolerance Test ASY-805.2: Associated Documents a b Handbook page task print-out ASY-805.3: Distribution of Documents Copy No Number Location 1 Quality Centre 2 3.1 W232 3 3.20 W232 Laminated
Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia
 Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY
 1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL SEMINAR: SEX HORMONES PART 1 An Overview What are steroid hormones? Steroid
SEX STERIOD HORMONES I: An Overview. University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences PBL MBBS III VJ Temple
 SEX STERIOD HORMONES I: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences PBL MBBS III VJ Temple 1 What are the Steroid hormones? Hormones synthesized
SEX STERIOD HORMONES I: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences PBL MBBS III VJ Temple 1 What are the Steroid hormones? Hormones synthesized
ASY-857.1: Synacthen Stimulated 17OH-progesterone Test
 ASY-857.1: Synacthen Stimulated 17OH-progesterone ASY-857.2: Associated Documents a Synacthen Standing Order form (ref 0827/2) G:\Division\NDO\common\ETCProtocols\0827 Standing Order Synacthen 2016.pdf
ASY-857.1: Synacthen Stimulated 17OH-progesterone ASY-857.2: Associated Documents a Synacthen Standing Order form (ref 0827/2) G:\Division\NDO\common\ETCProtocols\0827 Standing Order Synacthen 2016.pdf
ULTIMATE BEAUTY OF BIOCHEMISTRY. Dr. Veena Bhaskar S Gowda Dept of Biochemistry 30 th Nov 2017
 ULTIMATE BEAUTY OF BIOCHEMISTRY Dr. Veena Bhaskar S Gowda Dept of Biochemistry 30 th Nov 2017 SUSPECTED CASE OF CUSHING S SYNDROME Clinical features Moon face Obesity Hypertension Hunch back Abdominal
ULTIMATE BEAUTY OF BIOCHEMISTRY Dr. Veena Bhaskar S Gowda Dept of Biochemistry 30 th Nov 2017 SUSPECTED CASE OF CUSHING S SYNDROME Clinical features Moon face Obesity Hypertension Hunch back Abdominal
Clinical Guideline POSITION STATEMENT ON THE INVESTIGATION AND TREATMENT OF GROWTH HORMONE DEFICIENCY IN TRANSITION
 Clinical Guideline POSITION STATEMENT ON THE INVESTIGATION AND TREATMENT OF GROWTH HORMONE DEFICIENCY IN TRANSITION Date of First Issue 01/04/2015 Approved 28/01/2016 Current Issue Date 28/01/2016 Review
Clinical Guideline POSITION STATEMENT ON THE INVESTIGATION AND TREATMENT OF GROWTH HORMONE DEFICIENCY IN TRANSITION Date of First Issue 01/04/2015 Approved 28/01/2016 Current Issue Date 28/01/2016 Review
Provide preventive counseling to parents and patients with specific endocrine conditions about:
 Endocrinology Description: The resident will become familiar with the diagnosis, management, and treatment of endocrine problems. The resident will evaluate patients with a multitude of endocrine problems,
Endocrinology Description: The resident will become familiar with the diagnosis, management, and treatment of endocrine problems. The resident will evaluate patients with a multitude of endocrine problems,
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 2: Precocious Puberty. These podcasts are designed to give medical students an overview
Great Ormond Street Hospital for Children NHS Foundation Trust
 Great Ormond Street Hospital for Children DEPARTMENT OF ENDOCRINOLOGY Great Ormond Street Tel: 2 745 9 Questions answered by Professor Peter Hindmarsh It is true that many centres work differently regarding
Great Ormond Street Hospital for Children DEPARTMENT OF ENDOCRINOLOGY Great Ormond Street Tel: 2 745 9 Questions answered by Professor Peter Hindmarsh It is true that many centres work differently regarding
Diagnosing Growth Disorders. PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health
 Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
PITUITARY: JUST THE BASICS PART 2 THE PATIENT
 PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
NOTTINGHAM UNIVERSITY HOSPITAL NHS TRUST: Clinical Chemistry Guidelines
 Adrenocortical Insufficiency Guideline Document Information Policy Reference: Adrenocortical Insufficiency Issue: 1: Version 3 Author Job Title: Peter Prinsloo Consultant in Chemical Pathology STATUS:
Adrenocortical Insufficiency Guideline Document Information Policy Reference: Adrenocortical Insufficiency Issue: 1: Version 3 Author Job Title: Peter Prinsloo Consultant in Chemical Pathology STATUS:
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Endocrinology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Endocrinology 1. GOAL: Understand the role of the pediatrician in preventing endocrine dysfunction, and in counseling and
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Endocrinology 1. GOAL: Understand the role of the pediatrician in preventing endocrine dysfunction, and in counseling and
CHISCG1: Short Synacthen Test for the Investigation of Adrenal Insufficiency
 Pathology at the Royal Derby Hospital Short Synacthen Test Standard Clinical Guidelines Chemical Pathology Department Valid Until 31 st August 2011 Document Code: CHISCG1 Short Synacthen Test for the Investigation
Pathology at the Royal Derby Hospital Short Synacthen Test Standard Clinical Guidelines Chemical Pathology Department Valid Until 31 st August 2011 Document Code: CHISCG1 Short Synacthen Test for the Investigation
Paul Hofman. Professor. Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland
 Professor Paul Hofman Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland 14:00-14:55 WS #108: Common pubertal variants how to distinguish
Professor Paul Hofman Paediatrician Endocrinologist Liggins Institute, The University of Auckland, Starship Children Hospital, Auckland 14:00-14:55 WS #108: Common pubertal variants how to distinguish
Evaluation and Management of Pituitary Failure. Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS
 Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
THE VALUE OF 24 HOUR PROFILES IN CONGENITAL ADRENAL HYPERPLASIA
 THE VALUE OF 24 HOUR PROFILES IN CONGENITAL ADRENAL HYPERPLASIA This leaflet is a joint production between Professor Peter Hindmarsh and Kathy Geertsma The series editor is Professor Peter Hindmarsh Professor
THE VALUE OF 24 HOUR PROFILES IN CONGENITAL ADRENAL HYPERPLASIA This leaflet is a joint production between Professor Peter Hindmarsh and Kathy Geertsma The series editor is Professor Peter Hindmarsh Professor
Cortisol (serum, plasma)
 Cortisol (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Cortisol 1.2 Alternative names Hydrocortisone, 11β; 17, 21 trihydroxypregn 4 ene 3,20 dione 1.3 NMLC code 1.4 Description
Cortisol (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Cortisol 1.2 Alternative names Hydrocortisone, 11β; 17, 21 trihydroxypregn 4 ene 3,20 dione 1.3 NMLC code 1.4 Description
Reproductive FSH. Analyte Information
 Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Endocrine part two. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
Why is my body not changing? Conflicts of interest. Overview 11/9/2015. None
 Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Puberty and Pubertal Disorders Part 3: Delayed Puberty
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Puberty and Pubertal Disorders Part 3: Delayed Puberty These podcasts are designed to give medical students an overview
Adrenal incidentaloma guideline for Northern Endocrine Network
 Adrenal incidentaloma guideline for Northern Endocrine Network Definition of adrenal incidentaloma Adrenal mass detected on an imaging study done for indications that are not related to an adrenal problem
Adrenal incidentaloma guideline for Northern Endocrine Network Definition of adrenal incidentaloma Adrenal mass detected on an imaging study done for indications that are not related to an adrenal problem
GUIDELINES FOR SPECIALIST PAEDIATRIC BIOCHEMICAL INVESTIGATIONS
 GUIDELINES FOR SPECIALIST PAEDIATRIC BIOCHEMICAL INVESTIGATIONS Version: 1.0 Ratified by: Clinical Biochemistry Senior Staff Meeting Date ratified: 26-7-2016 Name of originator/author: Director responsible
GUIDELINES FOR SPECIALIST PAEDIATRIC BIOCHEMICAL INVESTIGATIONS Version: 1.0 Ratified by: Clinical Biochemistry Senior Staff Meeting Date ratified: 26-7-2016 Name of originator/author: Director responsible
Endocrine Emergencies: Recognition and Management
 Endocrine Emergencies: Recognition and Management John Wass Department of Endocrinology, Oxford University, UK An Update on Acute Medical Emergencies for Psychiatrists Royal College of Psychiatrists' address
Endocrine Emergencies: Recognition and Management John Wass Department of Endocrinology, Oxford University, UK An Update on Acute Medical Emergencies for Psychiatrists Royal College of Psychiatrists' address
I. Provide patient care that is compassionate, appropriate and effective for the prevention and treatment of endocrinologic disorders.
 Endocrinology Curriculum Goal Endocrinology is the diagnosis and care of disorders of the endocrine system. The principal endocrine problems handled by the general internist include goiter, thyroid nodules,
Endocrinology Curriculum Goal Endocrinology is the diagnosis and care of disorders of the endocrine system. The principal endocrine problems handled by the general internist include goiter, thyroid nodules,
Hypothalamus & Pituitary Gland
 Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Children s Hospital & Research Center Oakland. Endocrinology
 Children s Hospital & Research Center Oakland Endocrinology 5.22 GOAL: Prevention, Counseling and Screening (Endocrine). Understand the role of the pediatrician in preventing endocrine PC, MK, dysfunction,
Children s Hospital & Research Center Oakland Endocrinology 5.22 GOAL: Prevention, Counseling and Screening (Endocrine). Understand the role of the pediatrician in preventing endocrine PC, MK, dysfunction,
Precocious Puberty. Disclosures. No financial disclosures 2/28/2019
 Precocious Puberty Bracha Goldsweig, MD Pediatric Endocrinologist Children s Hospital and Medical Center, Omaha, NE University of Nebraska Medical Center Disclosures No financial disclosures 1 Objectives
Precocious Puberty Bracha Goldsweig, MD Pediatric Endocrinologist Children s Hospital and Medical Center, Omaha, NE University of Nebraska Medical Center Disclosures No financial disclosures 1 Objectives
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
Multiple Pituitary Hormone Deficiency (MPHD)
 Multiple Pituitary Hormone Deficiency (MPHD) SERIES 1 SERIES 2 SERIES 3 SERIES 4 SERIES 5 SERIES 6 SERIES 7 SERIES 8 SERIES 9 SERIES 10 SERIES 11 SERIES 12 SERIES 13 SERIES 14 SERIES 15 SERIES 16 CHILD
Multiple Pituitary Hormone Deficiency (MPHD) SERIES 1 SERIES 2 SERIES 3 SERIES 4 SERIES 5 SERIES 6 SERIES 7 SERIES 8 SERIES 9 SERIES 10 SERIES 11 SERIES 12 SERIES 13 SERIES 14 SERIES 15 SERIES 16 CHILD
Clinical Standards for GH Treatment in Childhood & Adolescence.
 Clinical Standards for GH Treatment in Childhood & Adolescence. The Clinical Standards for GH treatment have been produced by the Clinical Committee of the BSPED. They are evidence based where possible
Clinical Standards for GH Treatment in Childhood & Adolescence. The Clinical Standards for GH treatment have been produced by the Clinical Committee of the BSPED. They are evidence based where possible
Growth hormone therapy in a girl with Turner syndrome showing a large increase over the initially predicted ht of 4 5
 Disorders of Growth and Puberty: How to Recognize the Normal Variants vs Patients Who Need to be Evaluated Paul Kaplowitz, M.D Pediatric Endocrinology. VCU School of Medicine Interpretation of Growth Charts
Disorders of Growth and Puberty: How to Recognize the Normal Variants vs Patients Who Need to be Evaluated Paul Kaplowitz, M.D Pediatric Endocrinology. VCU School of Medicine Interpretation of Growth Charts
THE VALUE OF 24 HOUR PROFILES IN ASSESSING CORTISOL REPLACEMENT IN HYPOPITUITARISM
 THE VALUE OF 24 HOUR PROFILES IN ASSESSING CORTISOL REPLACEMENT IN HYPOPITUITARISM Professor Peter Hindmarsh and Kathy Geertsma Cortisol is produced in the body by the adrenal glands and the levels in
THE VALUE OF 24 HOUR PROFILES IN ASSESSING CORTISOL REPLACEMENT IN HYPOPITUITARISM Professor Peter Hindmarsh and Kathy Geertsma Cortisol is produced in the body by the adrenal glands and the levels in
Ch 8: Endocrine Physiology
 Ch 8: Endocrine Physiology Objectives 1. Review endocrine glands of body. 2. Understand how hypothalamus controls endocrine system & sympathetic epinephrine response. 3. Learn anterior pituitary hormones
Ch 8: Endocrine Physiology Objectives 1. Review endocrine glands of body. 2. Understand how hypothalamus controls endocrine system & sympathetic epinephrine response. 3. Learn anterior pituitary hormones
ADHD Medication Prescribing in Scotland in 2016/17
 ADHD Medication Prescribing in Scotland in 2016/17 Scottish ADHD Coalition Analysis March 2018 www.scottishadhdcoalition.org Notes on data sources Prescribing data was obtained through a data request to
ADHD Medication Prescribing in Scotland in 2016/17 Scottish ADHD Coalition Analysis March 2018 www.scottishadhdcoalition.org Notes on data sources Prescribing data was obtained through a data request to
ADRENAL GLANDS. G M Kellerman. Hunter Area Pathology Service
 ADRENAL GLANDS G M Kellerman Hunter Area Pathology Service ADRENAL FUNCTIONS THE ADRENAL GLANDS ACTUALLY HAVE 4 QUITE SEPARATE FUNCTIONS 1. MINERALOCORTICOID SECRETION BY THE ZONA GLOMERULOSA OF THE CORTEX
ADRENAL GLANDS G M Kellerman Hunter Area Pathology Service ADRENAL FUNCTIONS THE ADRENAL GLANDS ACTUALLY HAVE 4 QUITE SEPARATE FUNCTIONS 1. MINERALOCORTICOID SECRETION BY THE ZONA GLOMERULOSA OF THE CORTEX
The analysis of Glucocorticoid Steroids in Plasma, Urine and Saliva by UPLC/MS/MS
 The analysis of Glucocorticoid Steroids in Plasma, Urine and Saliva by UPLC/MS/MS Brett McWhinney, Supervising Scientist, HPLC Section, Pathology Central, Pathology Queensland Overview 1. Overview of Pathology
The analysis of Glucocorticoid Steroids in Plasma, Urine and Saliva by UPLC/MS/MS Brett McWhinney, Supervising Scientist, HPLC Section, Pathology Central, Pathology Queensland Overview 1. Overview of Pathology
Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery
 Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery Background Surgery places physical and emotional stress on the body. This, alongside new surroundings, parental anxiety and
Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery Background Surgery places physical and emotional stress on the body. This, alongside new surroundings, parental anxiety and
Adrenal insufficiency. A guide for parents
 Adrenal insufficiency A guide for parents We have written this leaflet to give you information you may need about adrenal insufficiency in your child. If you have any questions, please talk to your endocrine
Adrenal insufficiency A guide for parents We have written this leaflet to give you information you may need about adrenal insufficiency in your child. If you have any questions, please talk to your endocrine
Objectives. Why is blood glucose important? Hypoglycaemia. Hyperglycaemia. Acute Diabetes Emergencies (DKA,HONK)
 Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow June 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood Glucose
Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow June 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood Glucose
Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury
 Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury BACKGROUND Trauma related acquired brain injury (ABI) is known to
Medical and Rehabilitation Innovations Neuroendocrine Screening and Hormone Replacement Therapy in Trauma Related Acquired Brain Injury BACKGROUND Trauma related acquired brain injury (ABI) is known to
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU)
 ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
Objectives. Why is blood glucose important? Hypoglycaemia. Hyperglycaemia. Acute Diabetes Emergencies (DKA,HONK)
 Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow September 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood
Acute Diabetes Emergencies Ross Buchan, DSN North Glasgow September 2017 Objectives Why is blood glucose important? Hypoglycaemia Hyperglycaemia Acute Diabetes Emergencies (DKA,HONK) Importance of Blood
Prescribing Guidelines Prescribing arrangement for the management of patients transferring from Secondary Care to Primary Care
 Berkshire West Integrated Care System Representing Berkshire West Clinical Commisioning Group Royal Berkshire NHS Foundation Trust Berkshire Healthcare NHS Foundation Trust Berkshire West Primary Care
Berkshire West Integrated Care System Representing Berkshire West Clinical Commisioning Group Royal Berkshire NHS Foundation Trust Berkshire Healthcare NHS Foundation Trust Berkshire West Primary Care
SHARED CARE PRESCRIBING GUIDELINE Triptorelin (Gonapeptyl Depot 3.75 mg TM, Decapeptyl SR mg TM ) for precocious puberty
 WORKING IN PARTNERSHIP WITH SHARED CARE PRESCRIBING GUIDELINE Triptorelin (Gonapeptyl Depot 3.75 mg TM, Decapeptyl SR 11.25 mg TM ) for precocious puberty NHS Surrey s Medicines Management Committee classification:
WORKING IN PARTNERSHIP WITH SHARED CARE PRESCRIBING GUIDELINE Triptorelin (Gonapeptyl Depot 3.75 mg TM, Decapeptyl SR 11.25 mg TM ) for precocious puberty NHS Surrey s Medicines Management Committee classification:
Scottish Diabetes Survey 2012
 Scottish Diabetes Survey 2012 Scottish Diabetes Survey Monitoring Group 1 Scottish Diabetes Survey Monitoring Group Contents Foreword... 3 Executive Summary... 5 Prevalence... 6 Undiagnosed diabetes...
Scottish Diabetes Survey 2012 Scottish Diabetes Survey Monitoring Group 1 Scottish Diabetes Survey Monitoring Group Contents Foreword... 3 Executive Summary... 5 Prevalence... 6 Undiagnosed diabetes...
2.0 Synopsis. Lupron Depot M Clinical Study Report R&D/09/093. (For National Authority Use Only) to Part of Dossier: Name of Study Drug:
 2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: Name of Study Drug: Volume: Abbott-43818 (ABT-818) leuprolide acetate for depot suspension (Lupron Depot ) Name of
2.0 Synopsis Abbott Laboratories Individual Study Table Referring to Part of Dossier: Name of Study Drug: Volume: Abbott-43818 (ABT-818) leuprolide acetate for depot suspension (Lupron Depot ) Name of
Endocrine System. The Endocrine Glands
 Endocrine System Working together with the nervous system, the endocrine system helps maintain homeostasis in the body. Where the nervous system uses electric signals, the endocrine system uses chemical
Endocrine System Working together with the nervous system, the endocrine system helps maintain homeostasis in the body. Where the nervous system uses electric signals, the endocrine system uses chemical
Managing Addison s Disease
 Managing Addison s Disease Dr Charles R Buchanan Consultant Paediatric Endocrinologist Kings College Hospital, London Thomas Addison 1793-1860 Guy s Hospial Described Symptoms 1855 My experience 25 years
Managing Addison s Disease Dr Charles R Buchanan Consultant Paediatric Endocrinologist Kings College Hospital, London Thomas Addison 1793-1860 Guy s Hospial Described Symptoms 1855 My experience 25 years
R ecombinant growth hormone (GH) treatment is recommended
 126 ORIGINAL ARTICLE The investigation of short stature: a survey of practice in Wales and suggested practical guidelines C Evans, J W Gregory, on behalf of the All Wales Clinical Biochemistry Audit Group...
126 ORIGINAL ARTICLE The investigation of short stature: a survey of practice in Wales and suggested practical guidelines C Evans, J W Gregory, on behalf of the All Wales Clinical Biochemistry Audit Group...
Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC
 10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
Rhythm Plus- Comprehensive Female Hormone Profile
 Rhythm Plus- Comprehensive Female Hormone Profile Patient: SAMPLE REPORT DOB: Sex: F Order Number: K00000 Completed: Received: Collected: SAMPLE REPORT Sample # Progesterone (pg/ml) Hormone Results Oestradiol
Rhythm Plus- Comprehensive Female Hormone Profile Patient: SAMPLE REPORT DOB: Sex: F Order Number: K00000 Completed: Received: Collected: SAMPLE REPORT Sample # Progesterone (pg/ml) Hormone Results Oestradiol
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc)
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guideline for the Investigation and Management of Polycystic Ovary Syndrome Author: Contact Name and Job Title
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guideline for the Investigation and Management of Polycystic Ovary Syndrome Author: Contact Name and Job Title
Virilisation in siblings secondary to transdermal bioidentical testosterone exposure
 doi:10.1111/jpc.13466 INSTRUCTIVE CASE Virilisation in siblings secondary to transdermal bioidentical testosterone exposure Tony Huynh 1,2 and Catherine I Stewart 3 1 Department of Endocrinology and Diabetes,
doi:10.1111/jpc.13466 INSTRUCTIVE CASE Virilisation in siblings secondary to transdermal bioidentical testosterone exposure Tony Huynh 1,2 and Catherine I Stewart 3 1 Department of Endocrinology and Diabetes,
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR
 MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
C h a p t e r 3 8 Cushing s Syndrome : Current Concepts in Diagnosis and Management
 C h a p t e r 3 8 Cushing s Syndrome : Current Concepts in Diagnosis and Management Padma S Menon Professor of Endocrinology, Seth G S Medical College & KEM Hospital, Mumbai A clinical syndrome resulting
C h a p t e r 3 8 Cushing s Syndrome : Current Concepts in Diagnosis and Management Padma S Menon Professor of Endocrinology, Seth G S Medical College & KEM Hospital, Mumbai A clinical syndrome resulting
GUIDELINES ON MALE HYPOGONADISM
 GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
Neuroendocrine challenges following hemispherectomy
 Neuroendocrine challenges following hemispherectomy Philip S. Zeitler MD. PhD Professor and Head Section of Endocrinology Children s Hospital Colorado University of Colorado Anschutz Medical Campus I am
Neuroendocrine challenges following hemispherectomy Philip S. Zeitler MD. PhD Professor and Head Section of Endocrinology Children s Hospital Colorado University of Colorado Anschutz Medical Campus I am
ADRENAL HYPOFUNCTION: GUIDELINES FOR INVESTIGATION
 ADRENAL HYPOFUNCTION: GUIDELINES FOR INVESTIGATION Version: 2.0 Ratified by: Clinical Biochemistry Senior Staff meeting Date ratified: 28-01-2014 Name of originator/author: Director responsible for implementation:
ADRENAL HYPOFUNCTION: GUIDELINES FOR INVESTIGATION Version: 2.0 Ratified by: Clinical Biochemistry Senior Staff meeting Date ratified: 28-01-2014 Name of originator/author: Director responsible for implementation:
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018
 Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Dear Colleague. DL (2017) June Additional Funding for CGMs and Adult Insulin Pumps Summary
 The Scottish Government Healthcare Quality & Improvement Directorate DG Health & Social Care Dear Colleague Additional Funding for CGMs and Adult Insulin Pumps 2017-18 Summary On 7 December 2016, the First
The Scottish Government Healthcare Quality & Improvement Directorate DG Health & Social Care Dear Colleague Additional Funding for CGMs and Adult Insulin Pumps 2017-18 Summary On 7 December 2016, the First
Endocrine Dynamic Function Test Protocols for use in Neonates & Children
 Endocrine Dynamic Function Test Protocols for use in Neonates & Children Royal Manchester Children s Hospital April 2014 Review Date: April 2015 Authors Clinical Biochemistry Lesley Tetlow Beverly Hird
Endocrine Dynamic Function Test Protocols for use in Neonates & Children Royal Manchester Children s Hospital April 2014 Review Date: April 2015 Authors Clinical Biochemistry Lesley Tetlow Beverly Hird
2) Storehouse for the hormones produced by the hypothalamus of the brain. 2)
 AP 2 Exam Chapter 16 Endocrie Due Wed. night 4/22 or Thurs. morning 4/23 Name: Matching; match the labeled organ with the most appropriate response or identification. Figure 16.1 Using Figure 16.1, match
AP 2 Exam Chapter 16 Endocrie Due Wed. night 4/22 or Thurs. morning 4/23 Name: Matching; match the labeled organ with the most appropriate response or identification. Figure 16.1 Using Figure 16.1, match
BIOM2010 (till mid sem) Endocrinology. e.g. anterior pituitary gland, thyroid, adrenal. Pineal Heart GI Female
 BIOM2010 (till mid sem) Endocrinology Endocrine system Endocrine gland : a that acts by directly into the which then to other parts of the body to act on (cells, tissues, organs) : found at e.g. anterior
BIOM2010 (till mid sem) Endocrinology Endocrine system Endocrine gland : a that acts by directly into the which then to other parts of the body to act on (cells, tissues, organs) : found at e.g. anterior
Survey Scottish Diabetes. Survey Monitoring Group
 Scottish Diabetes Survey 2009 Scottish Diabetes Survey Monitoring Group 2 Foreword The Scottish Diabetes Survey is now in its ninth year. This 2009 Survey, as with previous versions, continues to demonstrate
Scottish Diabetes Survey 2009 Scottish Diabetes Survey Monitoring Group 2 Foreword The Scottish Diabetes Survey is now in its ninth year. This 2009 Survey, as with previous versions, continues to demonstrate
Summary
 Summary 118 This thesis is focused on the background of elevated levels of FSH in the early follicular phase of women with regular menstrual cycles. In the introduction (chapter 1) we describe the characteristics
Summary 118 This thesis is focused on the background of elevated levels of FSH in the early follicular phase of women with regular menstrual cycles. In the introduction (chapter 1) we describe the characteristics
Department of Paediatric Endocrinology, Royal Manchester Children s Hospital,
 Title: RETROSPECTIVE REVIEW OF SYNACTHEN TESTING IN INFANTS Authors: Timothy Shao Ern Tan 1*, Claire Manfredonia 2*, Rakesh Kumar 1, Julie Jones 1, Elaine O Shea 1, Raja Padidela 1, Mars Skae 1, Sarah
Title: RETROSPECTIVE REVIEW OF SYNACTHEN TESTING IN INFANTS Authors: Timothy Shao Ern Tan 1*, Claire Manfredonia 2*, Rakesh Kumar 1, Julie Jones 1, Elaine O Shea 1, Raja Padidela 1, Mars Skae 1, Sarah
Pre admission & surgery Pre-admission Nurses Association SIG Catherine Prochilo Credentialled Diabetes Nurse Educator Sat 23 March 2013
 Pre admission & surgery Pre-admission Nurses Association SIG Catherine Prochilo Credentialled Diabetes Nurse Educator Sat 23 March 2013 www.diabetesvic.org.au Plan/ overview Issue/ presenting problems
Pre admission & surgery Pre-admission Nurses Association SIG Catherine Prochilo Credentialled Diabetes Nurse Educator Sat 23 March 2013 www.diabetesvic.org.au Plan/ overview Issue/ presenting problems
ENDOCRINE LABORATORY TEST REPERTOIRE
 ENDOCRINE LABORATORY TEST REPERTOIRE Department of Medical Biochemistry and Immunology University Hospital of Wales Heath Park Cardiff CF14 4XW Endocrine Service Open Monday Friday 08:45 to 17:15 For general
ENDOCRINE LABORATORY TEST REPERTOIRE Department of Medical Biochemistry and Immunology University Hospital of Wales Heath Park Cardiff CF14 4XW Endocrine Service Open Monday Friday 08:45 to 17:15 For general
SeCondary Osteoporosis & its Therapy Duchenne Muscular Dystrophy SCOT-DMD
 SeCondary Osteoporosis & its Therapy Duchenne Muscular Dystrophy SCOT-DMD Acknowledgement S Joseph J Dunne M DiMarco C Duncanson I Horrocks S Shepherd and students Research radiographers & MRI Physics
SeCondary Osteoporosis & its Therapy Duchenne Muscular Dystrophy SCOT-DMD Acknowledgement S Joseph J Dunne M DiMarco C Duncanson I Horrocks S Shepherd and students Research radiographers & MRI Physics
TESTOSTERONE DEFINITION
 DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
Robert Wadlow and his father
 Robert Wadlow and his father 1 Robert Wadlow Wadlow reached 8 ft 11.1 in (2.72 m) in height and weighed 485 lb (220 kg) at his death at age 22. Born in Illinois. His great size and his continued growth
Robert Wadlow and his father 1 Robert Wadlow Wadlow reached 8 ft 11.1 in (2.72 m) in height and weighed 485 lb (220 kg) at his death at age 22. Born in Illinois. His great size and his continued growth
Scottish Diabetes Survey
 Scottish Diabetes Survey 2008 Scottish Diabetes Survey Monitoring Group Foreword The information presented in this 2008 Scottish Diabetes Survey demonstrates a large body of work carried out by health
Scottish Diabetes Survey 2008 Scottish Diabetes Survey Monitoring Group Foreword The information presented in this 2008 Scottish Diabetes Survey demonstrates a large body of work carried out by health
Puberty and Pubertal Disorders. Lisa Swartz Topor, MD, MMSc Pediatric Endocrinology July 2018
 Puberty and Pubertal Disorders Lisa Swartz Topor, MD, MMSc Pediatric Endocrinology July 2018 Objectives Review normal pubertal development Recognize common pubertal disorders Identify recent trends in
Puberty and Pubertal Disorders Lisa Swartz Topor, MD, MMSc Pediatric Endocrinology July 2018 Objectives Review normal pubertal development Recognize common pubertal disorders Identify recent trends in
Laboratory Investigation of Male Gonadal Function. Dr N Oosthuizen Dept of Chemical Pathology UP 2010
 Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing
 Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Growth Hormone, Somatostatin, and Prolactin 1 & 2 Mohammed Y. Kalimi, Ph.D.
 Growth Hormone, Somatostatin, and Prolactin 1 & 2 Mohammed Y. Kalimi, Ph.D. I. Growth Hormone (somatotropin): Growth hormone (GH) is a 191 amino acid single chain polypeptide (MW 22,000 daltons). Growth
Growth Hormone, Somatostatin, and Prolactin 1 & 2 Mohammed Y. Kalimi, Ph.D. I. Growth Hormone (somatotropin): Growth hormone (GH) is a 191 amino acid single chain polypeptide (MW 22,000 daltons). Growth
Diabetes Labour guideline (GL820)
 Diabetes Labour guideline (GL820) Approval Approval Group Job Title, Chair of Committee Date Maternity & Childrens Services Mr Mark Selinger, Consultant 6 th June 2014 Clinical Governance Committee Obstetrician
Diabetes Labour guideline (GL820) Approval Approval Group Job Title, Chair of Committee Date Maternity & Childrens Services Mr Mark Selinger, Consultant 6 th June 2014 Clinical Governance Committee Obstetrician
Staff at the Nottingham Children s Hospital. Guidelines process.
 Diabetes and Surgery Title of Guideline Contact Name and Job Title (author) Guideline for the management of children and young people with diabetes aged 18 or under requiring surgery Dr Priyha Santhanam,
Diabetes and Surgery Title of Guideline Contact Name and Job Title (author) Guideline for the management of children and young people with diabetes aged 18 or under requiring surgery Dr Priyha Santhanam,
Effect of cyproterone acetate on adrenocortical function in children with precocious puberty
 Archives of Disease in Childhood, 1981, 56, 218-222 Effect of cyproterone acetate on adrenocortical function in children with precocious puberty D C L SAVAGE AND P G F SWIFT Bristol Royal Hospital for
Archives of Disease in Childhood, 1981, 56, 218-222 Effect of cyproterone acetate on adrenocortical function in children with precocious puberty D C L SAVAGE AND P G F SWIFT Bristol Royal Hospital for
OBJECTIVES. Rebecca McEachern, MD. Puberty: Too early, Too Late or Just Right? Special Acknowledgements. Maryann Johnson M.Ed.
 1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
ROTATION SUMMARY ENDOCRINOLOGY
 ROTATION SUMMARY ENDOCRINOLOGY Rotation Contacts and Scheduling Details Rotation Director: Caroline Buckway, MD cbuckway@stanford.edu 650-721-1811 G313, SUMC Administrator: Ofelia Colin ofeliag@stanford.edu
ROTATION SUMMARY ENDOCRINOLOGY Rotation Contacts and Scheduling Details Rotation Director: Caroline Buckway, MD cbuckway@stanford.edu 650-721-1811 G313, SUMC Administrator: Ofelia Colin ofeliag@stanford.edu
GONADAL FUNCTION: An Overview
 GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
Scottish guideline for the management of Myotonic Dystrophy in adults
 SCOTTISH MUSCLE NETWORK Scottish guideline for the management of Myotonic Dystrophy in adults Contents Page number Scottish Guideline for the management of Myotonic Dystrophy 3 Appendix 1: Cardiologists
SCOTTISH MUSCLE NETWORK Scottish guideline for the management of Myotonic Dystrophy in adults Contents Page number Scottish Guideline for the management of Myotonic Dystrophy 3 Appendix 1: Cardiologists
Activity Report April 2014 March 2015
 North, South East and West of Scotland Cancer Networks Brain/Central Nervous System Tumours National Managed Clinical Network Activity Report April 2014 March 2015 Dr Avinash Kanodia Consultant Radiologist
North, South East and West of Scotland Cancer Networks Brain/Central Nervous System Tumours National Managed Clinical Network Activity Report April 2014 March 2015 Dr Avinash Kanodia Consultant Radiologist
Dr. Nermine Salah El-Din Prof of Pediatrics
 Dr. Nermine Salah El-Din Prof of Pediatrics Diabetes Endocrine Metabolism Pediatric Unit (DEMPU) Children Hospital, Faculty of Medicine Cairo University Congenital adrenal hyperplasia is a common inherited
Dr. Nermine Salah El-Din Prof of Pediatrics Diabetes Endocrine Metabolism Pediatric Unit (DEMPU) Children Hospital, Faculty of Medicine Cairo University Congenital adrenal hyperplasia is a common inherited
Endocrine System. Modified by M. Myers
 Endocrine System Modified by M. Myers 1 The Endocrine System 2 Endocrine Glands The endocrine system is made of glands & tissues that secrete hormones. Hormones are chemicals messengers influencing a.
Endocrine System Modified by M. Myers 1 The Endocrine System 2 Endocrine Glands The endocrine system is made of glands & tissues that secrete hormones. Hormones are chemicals messengers influencing a.
Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation
 CHILDREN S SERVICES Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation Background Surgery places stress on the body and will alter glucose control and insulin
CHILDREN S SERVICES Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation Background Surgery places stress on the body and will alter glucose control and insulin
CUSHING S SYNDROME THE FACTS YOU NEED TO KNOW
 CUSHING S SYNDROME THE FACTS YOU NEED TO KNOW Written by: Paul Margulies, MD, FACE, FACP, Medical Director, NADF. Clinical Associate Professor of Medicine, Zucker School of Medicine at Hofstra/Northwell.
CUSHING S SYNDROME THE FACTS YOU NEED TO KNOW Written by: Paul Margulies, MD, FACE, FACP, Medical Director, NADF. Clinical Associate Professor of Medicine, Zucker School of Medicine at Hofstra/Northwell.
All Wales Paediatric Steroid Replacement Therapy Card
 All Wales Paediatric Steroid Replacement Therapy Card All Wales Paediatric Steroid Replacement Therapy Card 1.0 BACKGROUND Patients that require long-term steroid replacement therapy for adrenal suppression
All Wales Paediatric Steroid Replacement Therapy Card All Wales Paediatric Steroid Replacement Therapy Card 1.0 BACKGROUND Patients that require long-term steroid replacement therapy for adrenal suppression
Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences. Endocrinology. (Review) Year 5 Internal Medicine
 Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Endocrinology (Review) Year 5 Internal Medicine Presented by: Dr. Mona Arekat Prepared by: Ali Jassim Alhashli Case (1):
Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Endocrinology (Review) Year 5 Internal Medicine Presented by: Dr. Mona Arekat Prepared by: Ali Jassim Alhashli Case (1):
14 Girl with Cushing s Disease: An Update. Kristen Dillard, MD Endorama October 17, 2013
 14 Girl with Cushing s Disease: An Update Kristen Dillard, MD Endorama October 17, 2013 Initial Presentation Pt initially presented to pediatrician for school physical in fall 2012. Pt was found to be
14 Girl with Cushing s Disease: An Update Kristen Dillard, MD Endorama October 17, 2013 Initial Presentation Pt initially presented to pediatrician for school physical in fall 2012. Pt was found to be
