Pressure Diuresis 9 Sample Student Essays
|
|
|
- Blaise Cross
- 6 years ago
- Views:
Transcription
1 Pressure Diuresis 9 Sample Student Essays Below please find assembled consecutively in one document the brief analyses submitted by nine students in Mammalian Physiology 08 to the Teach Yourself Pressure Diuresis exercise.
2 ALR October 22, 2008 Pressure Diuresis and Pressure Natriuresis Dr. Meyers Pressure- diuresis was induced in web-human by infusing electrolytes to 600 ml over a 60-minute period. Pressure- Diuresis is occurring in this patient because over the 10 minute observation period because the value of urinary exrcretion of water (EXH2O) increased from to 1.276; there was a general increase over time. Pressure- diuresis occurs because of a slight build up in arterial pressure, which occurred by inducing electrolytes. The mean arterial pressure increased from mmhg to mmhg. The diuresis occurred because of the increased mean arterial pressure because there was also an increase in GFR. The slight increase in GFR (from 123 to 139.7) can be accounted for by the increase in arterial pressure. Similarly, pressure- natriuresis is occurring in this patient because over the 10 minute observation period, the urinary concentration of sodium increases from 116 to Therefore, the amount of sodium being excreted from the body increases dramatically, indicating a natriuresis. The natriuresis is pressure indicated by the increase in arterial pressure and the increase in GFR explained above. The three mechanisms that autoregulate the affects of the increase in pressure are also showed. The first is the increase from 123 to in the GFR. The second mechanism that shows that pressure diuresis is occurring is the decrease in angiotensin II formation based on the renal vascular resistance. Angiotensin II increases the renal vascular resistance (RENR), so when the renal vascular resistance is decreased, it demonstrates that there is less angiotensin II in the blood. The third mechanism that occurs is a decrease in the percentage of the filtered load of sodium and water that is
3 reabsorbed. The values that indicate a decrease sodium and water reabsorption are the increases in sodium and water excretion. By the end of the observation period the reabsorption percentage went from 99.35% reabsorption of sodium to 0.8%, indicating that there was a huge decrease in sodium reabsorption.
4 CT Pressure Diuresis The infusion of electrolytes will increase the inter-arterial pressure as the ions are absorbed into the blood. This can be seen as the reason for the increase in AP from up to mmhg (see Fig 1). Accompanying the increase in pressure will be a slight increase in GFR, as autoregulation will not allow for this increase to be very large due to the massive increase of urine output if GFR greatly increased. This was the case as GFR increased from to ml/min. The increase in turn led to an increase in the mount of water excreted in the urine, or the volume flow of the urine. This value of excreted water increased from 0.99 up to 1.26 ml/min. This is strong evidence for the occurrence of a pressure diuresis. The increase in pressure also decreases the percentage of the filtered load of sodium that is reabsorbed by the tubules. The mechanism for this process is an increase in peritubular capillary hydrostatic pressure, which will allow more secretion and less reabsorption. The increase in renal interstitial fluid hydrostatic pressure creates a back leak problem where sodium leaks into the tubular lumen and therefore reducing the reabsorption of water and sodium. The fact that the excretion of sodium, concentration of sodium in the urine and excreted water all increased (reabsorption decreased) is evidence for both pressure natriuresis and pressure diuresis. The raised levels of sodium in the urine and levels of excreted sodium specifically characterize the pressure natriuresis. The increase in pressure should lead to a decrease of the vasoconstrictor Angiotensin II. Therefore, the constriction of the efferent arteriole becomes lessened and blood flow will increase. The decrease in Angiotensin II will also result in a decrease of sodium reabsorption. The renal resistance should also decrease as the Angiotensin II levels drop and constriction is decreased. The
5 large increase in renal blood flow and decrease in renal resistance are sufficient evidence to conclude that the increased arterial pressure resulted in a decrease of Angiotensin II (see Fig 2).
6 Figure 1: Indication of Pressure Diuresis and Natriuresis by Increases Levels of Water and Sodium Excretion
7 Figure 2: Indication of Decrease of Angiotensin II by Increased Renal Resistance and Renal Blood Flow
8 EB October 22, 2008 Mammalian Physiology Professor Meyers Arterial Pressure Induced Pressure-Diuresis and Pressure-Natriuresis The increase in mean arterial pressure has three main effects on the kidney system that will induce a pressure diuresis and a pressure natriuresis. The pressure diuresis, and the pressure natriuresis collectively result in an increase in urine output. The patient was infused with 600 ml of electrolytes over 10 minutes, and evaluated over a period of one hour. A pressure diuresis is indeed occurring because the excreted H20 (EXH20) rises, and then slowly begins to normalize after the infusion of electrolytes. A natriuresis is also occurring because the urinary concentration of Na (UNA) also rises and slowly normalizes after the electrolyte infusion. (Table 1) An increase in arterial pressure results in an increase in afferent arterial pressure into the glomeruli, this increases glomerular hydrostatic pressure, which increases GFR. The increase in GFR, although resisted via the glomerulotubular autoregulation system, still causes an increase in urine output because pressure diuresis and pressure natriures are induced. These results are shown in the decreased renal afferent arterial resistance, which causes an increase in glomerular hydrostatic pressure increasing GFR in table 1. Table1
9 A rise in aterial pressure also causes an increase in peritubular capillary osmotic pressure, which causes a back up of H2O and Na into the tubular lumen, which leads to excess H2O and Na excretion. This process causes a decrease in Na absorption. Before infusion of Na, the patient s Na re-absorption is 99.36% of the filtered value. After the Na infusion, the Na re-absorption drops to 99.34%. The filtered loads, excreted loads, and amounts reabsorbed were calculated from the following data in Table 2. Table2 The final factor associated with increased arterial pressure that affects the urine output through pressure diuresis and pressure natriuresis is reduced angiotensin II production. Angiotensin II is a vasoconstrictor, which ultimately causes a decrease in glomerular hydrostatic pressure, and a decrease in GFR. A decrease in angiotensin II dilates the renal arterioles and increases GFR. The decrease in angiotensin II is seen in the increase in renal blood flow (Table 3). As seen in Table 1, the renal afferent arterial resistance also decreases with a decrease in angiotensin II. Because angiotensin II also increases the secretion of H+, the decrease in angiotensin II also leads to an increase in urine ph. The increase in urine ph, however, may or may not be the result of other factors. Table3
10 E G Pressure Diuresis Pressure diuresis is shown to occur as a result of a 600 ml infusion over the course of 10 minutes. Maximal increase in water excretion (from to ml/min) is seen 15 minutes following the start of infusion. Pressure Natriuresis is shown to occur; maximal increase in sodium excretion (from to meq/min) is seen to occur 15 minutes following the start of infusion. The sodium concentration of the urine is also shown to increase (from to meq/min) which further supports the occurrence of pressure natriuresis. Glomular Filtration Rate (GFR) is shown to increase (122.8 to maximum of ml/min) which supports the role of increased GFR in the occurrence of pressure diuresis and natriuresis in response to increased arterial pressure. Renal resistance is shown to decrease ( to ) which suggests a decrease in angiotensin II formation which acts to constrict efferent arterioles. Decreased levels of angiotensin II would result in decreased renal resistance due to decreased vascular constriction. The percentage of sodium reabsorbed from the renal tubule decreases (99.4 to 99.0 %) following the 600 ml infusion. This suggests an increase in peritubular capillary hydrostatic pressure as well as an increase in renal interstitial fluid hydrostatic pressure as both of which are necessary to increase the amount of sodium excreted.
11
12 H P Mammalian Physiology Pressure Diuresis A pressure diuresis and a pressure natriuresis were successfully induced by infusing the patient with1000 ml of electrolytes for a period of 60 minutes. The presence of diuresis is evident through the patient s increase in excretion of water (EXH2O) as a response to a slight increase in arterial pressure (AP increased from to mmhg in 60 min). Under normal conditions, an increase in blood pressure would not have an apparent effect in renal output due to various autoregulatory mechanisms. Therefore the increase in EXH2O from to ml/min indicates that the autoregulatory mechanisms are impaired. In addition, pressure natriuresis was shown through the patient s increase in excretion of sodium (EXNA) from to meq/min as a response to a change in AP (more than twice the normal amount). The lack of GFR autoregulation is shown through the patient s large increase in GFR with an increase in AP (122 to 149 ml/min). The impaired GFR autoregulation mechanism could be due to the decrease in angiotension II formation. Because angiotensin II preferentially constricts efferent arterioles, a decreased angiotensin II level lowers glomerular hydrostatic pressure while increasing renal blood flow. The increase in renal blood flow in turn leads to an increase in GFR. The decrease in angiotension II production can be seen through the patient s overall decrease in renal resistance (RENR) from to mmhg/ml/min, and his increase in blood flow from 1181 to 1364 ml/min). In addition, the decrease in angiotensin can also be witnessed through the decrease in aldosterone secretion. Since aldosterone increases potassium secretion, an
13 increase in aldosterone would lead to an increase in absorption. This is shown through the decrease in the patient s urine potassium level (decreased from to meq/l). Furthermore, another effect of increased renal arterial pressure that raises urine output is the decrease of the percentage of the filtered load of sodium and water that is reabsorbed by the tubules. The increase in the peritubular capillary hydrostatic pressure is shown through the drastic increase in urine sodium concentration (UNA) from 115 to 180 meq/l, and also the increase in sodium excretion (EXNA) from 0.1 to 0.3 meq/min. Both increased value showed a back-leak of sodium into the tubular lumen due to an increased renal interstitial fluid hydrostatic pressure as a response to a higher AP. The decreased net reabsorbance therefore led to an overall increase in the rate of urine output.
14
15 J R Pressure Diureisis DAY/HR AP GFR EXH2O UNA EXNA PNA 1-12:10 AM :20 AM :30 AM :40 AM :50 AM :00 AM :10 AM DAY/HR AP GFR EXH2O UNA EXNA RBF 1-1:10 AM :10 AM To cause the increase in arterial pressure from mmhg, necessary to induce a pressure diuresis and natriuresis, the patient was infused with 1L electrolytes for 10 min. The patient was then run for 50 minutes following that, while recording arterial pressure (AP), Glomerular Filtration rate (GFR), H20 excretion (EXH20), concentration of Na in the urine (UNA), excretion of urine (EXNA), plasma concentration of Na (PNA), and renal blood flow (RBF). The patient s arterial pressure reached a high of then steadied out at a mmhg. We can see that a pressure-diuresis is occurring from the clear increase in the H20 excretion up to ml/min at its highest. We also can see that a pressure-natriuresis
16 is occurring from the increase in Na excretion up to.4026 meq/min from the normal at its highest.118 meq/min. There is also a higher concentration of Na in the urine, meq/ml, than normal, 118 meq/ml. The first factor that is at play in the pressure diuresis and natriuresis is the slight increase in GFR, as seen here from 123 to ml/min at its highest value. The second factor causing the increase in urine output response to increased arterial pressure is a decrease in the percent of the filtered load that is reabsorbed. This is exhibited in our patient in the increase of Na excretion and concentration of Na in the urine, while the plasma urine remains the same. The % reabsorbed of filtered Na (calculated as ((GFR * PNA) EXNA) /(GFR*PNA)) is down to 98 % from the expected 99.9 %. The last factor in effect is a decrease in angiotensin II that in turn leads to a decrease in sodium reabsorption. Because angiotensin II is a known vasoconstrictor, we can measure the change in angiotensin II levels based on renal blood flow. A decrease in angiotensin II would therefore cause a vasodilation and in turn a higher renal blood flow. This is seen in our patient, with RBF increasing up to 1350 ml/min from a normal value of 1200 ml/min, confirming that angiotensin II levels have dropped.
17 JW October 22, 2008 Pressure Diuresis Lab The increased Arterial Pressure from to mm Hg indicates the primary cause for both a Pressure-Diuresis and a Pressure-Natriuresis. A Pressure-Diuresis is seen to be occurring when 600 ml of electrolytes are infused over a ten-minute period. The increased water loss from time 0 is from ml/min to ml/min. The increase of Na+ excretion ( meq/min to meq/min) indicates a Pressure- Natriuresis is also occurring. Table 1. Arterial Pressure, Urine excretion and Sodium excretion in a patient with 600 ml Electrolytes infused over a 10 minute period. The first mechanism involved with the Pressure-Diuresis and a Pressure- Natriuresis is an increased GFR (from 144 L/24H to L/24H) due to the impairment of GFR autoregulation. The increased GFR can be seen in table 2. The second mechanism is a decreased amount of the filtered load of NA+ that is reabsorbed. The decrease in the percentage of Na+ that is reabsorbed is from 99.3% (normal) to 99.06% (after 60 minutes). These values were determined by calculating the Filtered load and Excreted load and comparing the percent reabsorbed initially to the percent reabsorbed finally.
18 Table 2. Renal Na+ Reabsorption Calculations GFR L/24H PNA meq/l Filtered Load meq/l EXH2O L/24H UNA meq/l Excreted Load meq/l Amount reabsorbed % Reabs. initial final The third mechanism involved is the reduction of Angiotensin II. The angiotensin II restricts the Efferent Arteriole. However, the lack of Angiotensin II causes a decrease in resistance as shown by the data below (Table 3). This lack of resistance indicates a lack of Angiotensin II. The increase in blood flow also indicates the decreased resistance. Table 3. Renal resistance and renal blood flow.
19 K S Pressure Diuresis In order to determine the mechanisms of pressure-natriuresis and pressure-diuresis to counteract increased arterial pressure, an otherwise normal model was infused with 600 ml of electrolytes over 10 minutes and then observed for another 50 minutes at 10 minute intervals (figure 1). Figure 1 It can be determined that a pressure-diuresis is occurring by looking at the increase in excreted water was a result of the electrolyte infusion. While the normal value of excreted urine is ml/minute, this value increases to 1.27 ml/min at the time of the infusion, and increases even further to 1.36 ml/min ten minutes after the infusion (figure 2). This is a result of the function of the kidney to excrete excess water and return arterial pressure to normal, or pressure-duiresis. Likewise, it can be determined that pressure-natriuresis is occurring by looking at the values of sodium concentration in the urine before and after the infusion. Before the infusion, the value of sodium in the urine is meq/l while at the time of the infusion this value increases to meq/l and increases again 10 minutes after the infusion to meq/l(figure 2) which is evidence that the kidney is excreting sodium to attempt to counteract the increased arterial pressure. One of the three mechanisms that is involved in the process is an increase in GFR which can be seen by the value increasing from ml/min to ml/min at the time of infusion and then again to ml/min at ten minutes after the infusion (figure 2). The second mechanism is a decrease in the percentage of the filtered load of sodium and water that is reabsorbed by the tubules. The evidence for this mechanism working can be seen in the lack of change of concentration of sodium in the plasma that is filtered, but an increase in the sodium concentration of the urine (figure 2). This would indicate that
20 although the same amount is being filtered, more is being excreted, which means that less is being reabsorbed. Another of the three mechanisms is a decrease in angiotensin II which leads to a decrease in renal vascular resistance. This is evidenced in the value increasing from mm Hg/ml/min to mm Hg/ml/min at the time of the infusion to mm Hg/ml/min at ten minutes after the infusion (figure 2). The function of angiotensin II is to increase vasoconstriction, therefore this evidenced decrease in vasoconstriction (resistance) points to a decrease in angiotensin II. Figure 2
21 R N Pressure Diuresis An experiment can be set up by the following parameters: Infusion of 600 ml over a 10 minute period gives the following results: After the infusion, as a direct result of an increase in electrolyte infusion, the arterial pressure increases slightly to increase urine output. One effect this has on the kidney is the increase in GFR from the initial value of to ml/min. This increases the volume of urine excreted. Another effect of the increased renal arterial pressure is the decrease in the reabsorption of water and sodium by the tubules. This is indicated by several factors. The sodium concentration in the plasma remains relatively constant, and the GFR increases only slightly. However, the excretion of sodium increases, from the initial value of to ml/min. The sodium concentration increases as well, which gives an overall increase in excreted load. The initial excreted load is meq/min compared
22 to an almost doubled value of meq/min after infusion. This results in a lower reabsorption after the infusion. There is also an increase in the excretion of water from ml/min to after 10 minutes of infusion as well as an increase in the sodium concentration in the urine. Angiotension II increases sodium and water reabsorption using three different techniques. One technique is directly stimulating sodium transport across luminal and basolateral surfaces of the epithelial cell membrane of the tubules. An increase in angiotension II would increase sodium reabsorption by increasing the secretion of aldosterone. Aldosterone regulates not only sodium reabsorption but also potassium secretion. After the infusion of electrolytes, there is a dramatic decrease in aldosterone from ng/dl to ng/dl. This is reflected in the decreased sodium reabsorption and potassium concentration in urine. Angiotensin II also constricts the efferent arterioles, which reduces the hydrostatic pressure in the peritubular capillary. This also reduces renal blood flow, which causes an increase in the colloid osmotic pressure in the peritubular capillaries. Both of these reductions lead to an overall increase in tubular reabsorption. After infusion of the electrolytes, the renal blood flow increased, an indication, along with the lowered aldosterone levels, that angiotensin II levels are reduced. The implication is that less sodium and water are reabsorbed. All the experimental results signifiy there is lower reabsorption of sodium and water in the patient. Lower reabsorption back into the body indicate more excretion of the substances out. This can be referred to as pressure-natriuresis and pressure-diuresis. Because the experiment extended past the infusion, the kidney levels return to autoregulation after infusion.
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology (4) 2/4/2018. Wael abu-anzeh
 Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Renal Blood flow; Renal Clearance. Dr Sitelbanat
 Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Collin College. BIOL Anatomy & Physiology. Urinary System. Summary of Glomerular Filtrate
 Collin College BIOL. 2402 Anatomy & Physiology Urinary System 1 Summary of Glomerular Filtrate Glomerular filtration produces fluid similar to plasma without proteins GFR ~ 125 ml per min If nothing else
Collin College BIOL. 2402 Anatomy & Physiology Urinary System 1 Summary of Glomerular Filtrate Glomerular filtration produces fluid similar to plasma without proteins GFR ~ 125 ml per min If nothing else
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Lab 19 The Urinary System
 Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
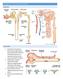 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
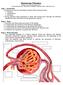 Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
** Accordingly GFR can be estimated by using one urine sample and do creatinine testing.
 This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 25, 2013 Total POINTS: % of grade in class
 NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 25, 2013 Total POINTS: 100 20% of grade in class 1) During exercise, plasma levels of Renin increase moderately. Why should Renin levels be elevated during
NROSCI/BIOSC 1070 and MSNBIO 2070 Exam # 2 October 25, 2013 Total POINTS: 100 20% of grade in class 1) During exercise, plasma levels of Renin increase moderately. Why should Renin levels be elevated during
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
mid ihsan (Physiology ) GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B **
 (Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
(Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION
 3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
Excretory System-Training Handout
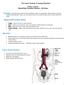 Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Identify and describe. mechanism involved in Glucose reabsorption
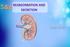 Define tubular reabsorption, tubular secretion, transcellular and paracellular transport. Identify and describe mechanism involved in Glucose reabsorption Describe tubular secretion with PAH transport
Define tubular reabsorption, tubular secretion, transcellular and paracellular transport. Identify and describe mechanism involved in Glucose reabsorption Describe tubular secretion with PAH transport
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Filtration and Reabsorption Amount Filter/d
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Excretory Physiology
 Excretory Physiology Urine production and eliminations are one of the most important mechanisms of body homeostasis composition of blood is determined more by kidney function than by diet all body systems
Excretory Physiology Urine production and eliminations are one of the most important mechanisms of body homeostasis composition of blood is determined more by kidney function than by diet all body systems
URINARY SYSTEM. Primary functions. Major organs & structures
 URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
The kidney. (Pseudo) Practical questions. The kidneys are all about keeping the body s homeostasis. for questions Ella
 The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
2- Maintain the proper balance between water and. 3- Maintain the proper acid base balance. glucose by gluconeogenesis. pressure
 Filter ~180 liters of blood plasma daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine 1 Regulate volume and chemical composition of the blood 2 Maintain the proper balance
Filter ~180 liters of blood plasma daily, allowing toxins, metabolic wastes, and excess ions to leave the body in urine 1 Regulate volume and chemical composition of the blood 2 Maintain the proper balance
Body Fluid Dynamics. I. Body fluids - Must remain constant - Intake = output. Insensible H 2 0 loss Capillary Membrane
 I. Body fluids - Must remain constant - Intake = output Body Fluid Dynamics Metabolic H 2 0 Preformed Free H 2 0 in Urine Feces Sweat H 2 0 Food - Body fluid distribution: Insensible H 2 0 loss Capillary
I. Body fluids - Must remain constant - Intake = output Body Fluid Dynamics Metabolic H 2 0 Preformed Free H 2 0 in Urine Feces Sweat H 2 0 Food - Body fluid distribution: Insensible H 2 0 loss Capillary
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences. Body fluids and.
 By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19](/thumbs/77/74887026.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Therapeutics of Diuretics
 (Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
(Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
Renal Physiology Intro to CRRT Concepts. Catherine Jones September 2017
 Renal Physiology Intro to CRRT Concepts Catherine Jones September 2017 Learning Outcomes To revise anatomy & physiology of kidney in health: To understand basic principles of continuous renal replacement
Renal Physiology Intro to CRRT Concepts Catherine Jones September 2017 Learning Outcomes To revise anatomy & physiology of kidney in health: To understand basic principles of continuous renal replacement
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA. Ahmet Onat Bermede, MD. Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte,
Answers and Explanations
 Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Renal Physiology - Lectures
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Physiology questions review
 Physiology questions review 1- The consumption of O2 by the kidney: a- decrease as blood flow increases b- regulated by erythropoiten c- remains constant as blood flow increase d- direct reflects the level
Physiology questions review 1- The consumption of O2 by the kidney: a- decrease as blood flow increases b- regulated by erythropoiten c- remains constant as blood flow increase d- direct reflects the level
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class XI Chapter 19 Excretory Products and their Elimination Biology
 Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Overview of Kidney Function
 The Kidney Overview of Kidney Function osmolarity of the body fluids volume of ECF plasma ph waste products (urea, uric acid, creatinine, foreign compounds) synthesis of: - EPO, renin, kallikrein, prostaglandins,
The Kidney Overview of Kidney Function osmolarity of the body fluids volume of ECF plasma ph waste products (urea, uric acid, creatinine, foreign compounds) synthesis of: - EPO, renin, kallikrein, prostaglandins,
RENAL PHYSIOLOGY. Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM
 RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
RENAL PHYSIOLOGY Zekeriyya ALANOGLU, MD, DESA Ahmet Onat Bermede, MD, Ankara University School of Medicine Dept. Anesthesiology and ICM Kidneys Stabilize the composition of the ECF (electrolyte, H
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
Renal Reabsorption & Secretion
 Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
I. General Features of Renal Function -Objectives II. Blood Flow and Filtration -Objectives III. Tubular Anatomy and Function -Objectives IV.
 ORGANIZATION This syllabus is divided into ten sections or topics. Each section is divided into objectives. On the contents page, clicking on the section title takes you directly to that section. Clicking
ORGANIZATION This syllabus is divided into ten sections or topics. Each section is divided into objectives. On the contents page, clicking on the section title takes you directly to that section. Clicking
RENAL PHYSIOLOGY. Danil Hammoudi.MD
 RENAL PHYSIOLOGY Danil Hammoudi.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood
RENAL PHYSIOLOGY Danil Hammoudi.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood
Fal Fal P h y s i o l o g y 6 1 1, S a n F r a n c i s c o S t a t e U n i v e r s i t y
 Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Potassium secretion. E k = -61 log ([k] inside / [k] outside).
![Potassium secretion. E k = -61 log ([k] inside / [k] outside). Potassium secretion. E k = -61 log ([k] inside / [k] outside).](/thumbs/80/80478709.jpg) 1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
