RESEARCH. What is already known about this subject. What this study adds
|
|
|
- Clara Cunningham
- 6 years ago
- Views:
Transcription
1 RESEARCH Impact of a Clinical Pharmacy Program on Changes in Hemoglobin A1c, Diabetes-Related Hospitalizations, and Diabetes-Related Emergency Department Visits for Patients with Diabetes in an Underserved Population Nancy Chung, PharmD, BCACP; Karen Rascati, PhD; Debra Lopez, PharmD, CDE, BCPS, BCACP; Jason Jokerst, PharmD, BCPS; and Aida Garza, PharmD, CDE, BCACP ABSTRACT BACKGROUND: Diabetes mellitus is associated with substantial morbidity and mortality. With the rise in prevalence of diabetes, there has been an increased need for clinical pharmacy services focused on diabetes management in ambulatory clinics. However, more data IS needed to determine the overall impact that clinical pharmacists have on preventing diabetesrelated inpatient admissions and emergency department (ED) visits for patients with diabetes, especially in an underserved population. OBJECTIVES: To assess the impact of clinical pharmacy services on the change in hemoglobin A1c measurements, the number of diabetes-related hospitalizations, and the number of diabetes-related ED visits for patients with uncontrolled diabetes. METHODS: This was a retrospective study that evaluated outcomes for patients referred to a clinical pharmacist for management of diabetes, compared with patients who were not seen by a clinical pharmacist. Adult patients aged between 18 and 89 years with a diagnosis of type 1 or type 2 diabetes mellitus were identified, using the electronic medical records from CommUnityCare outpatient clinics in central Texas during the period July 1, 2007, through July 1, Patients enrolled had poor glycemic control, defined as an A1c 9% at baseline (index), with at least 3 visits with a clinical pharmacist or 3 visits to usual care. Patients with at least 1 year of pre-index data, 1 year of post-index follow-up, and a post-index A1c measure were included in the study. Propensity score (PS) matching was used to create a 1:1 cohort. T-tests were used to calculate results for the main outcome variables (change in A1c, change in number of diabetes-related hospitalizations, and change in number of diabetes-related ED visits). In addition, general linear models (GLM) were used to control for baseline demographic and clinical characteristics. RESULTS: A total of 782 patients met inclusion criteria, 557 in the usual care (control) group and 225 in the clinical pharmacy (intervention) group. PS matching provided a 1:1 matched sample of 220 patients per cohort. When assessing the change in the number of diabetes-related hospitalizations from the pre-index year to the post-index year, patients in the control group had an increase of 8 hospitalizations (8 visits per 220 patients, mean = 0.036, SD = 0.284), while the intervention group had a decrease of 1 hospitalization (-1 visit per 220 patients, mean = , SD=0.278). Both the t-test (P = 0.06) and GLM model (P = 0.06) indicated that the difference was statistically significant. When assessing the change in the number of diabetes-related ED visits from the pre-index year to the post-index year, we found patients in the control group had an increase of 16 ED visits (16 visits per 220 patients, mean = 0.073, SD = 0.584), while the interven- tion group had an increase of 4 ED visits (4 visits per 220 patients, mean = , SD=0.641). Both the t-test (P = 0.18) and GLM model (P = 0.28) indicated that the difference was not statistically significant. A1c levels were reduced in the post-index period for both groups. For the control group, A1c reduction was 1.50 (from to 9.67, SD = 2.49). For the intervention group, A1c reduction was 1.90 (from to 9.19, SD = 2.44). Both the t-test (P = 0.04) and GLM model (P = 0.05) indicated that the A1c difference was statistically significant. CONCLUSIONS: Underserved patients with baseline uncontrolled diabetes who were managed by a clinical pharmacist in the outpatient setting had a higher decrease in A1c compared with usual care. The changes in diabetes-related hospitalizations and diabetes-related ED visits were in the hypothesized direction, but the comparison for ED visits was not statistically significant. J Manag Care Pharm. 2014;20(9): Copyright 2014, Academy of Managed Care Pharmacy. All rights reserved. What is already known about this subject Diabetes mellitus imposes a substantial economic burden on society, and hospitalization costs comprise the largest expenditure. Additionally, elevated hemoglobin A1c is associated with increased diabetes-related complications, including hospitalizations. Clinical pharmacist interventions have been associated with mostly positive clinical outcomes on A1c; however, there is limited data on the impact of clinical pharmacy services in preventing diabetes-related hospitalizations and diabetes-related emergency department (ED) visits. Indigent populations have barriers to diabetes care that may include, but are not limited to, access to health care, cultural beliefs, and language. What this study adds Patients managed by a clinical pharmacist working under a collaborative drug therapy management protocol had a decrease in the number of hospitalizations during the 1-year follow-up period, while those in the usual care group had an increase in the number of hospitalizations. 914 Journal of Managed Care & Specialty Pharmacy JMCP September 2014 Vol. 20, No. 9
2 What this study adds (continued) While both cohorts (usual care vs. clinical pharmacy group) showed a decrease in A1c scores at the 1-year follow-up, there was greater A1c reduction in the clinical pharmacy group. Clinical pharmacist management of patients with uncontrolled diabetes was associated with improved clinical outcomes in a federally qualified health center. Diabetes mellitus is a major cause of illness in the United States and is a growing public health problem. The diabetes epidemic affects approximately 8.3% of the U.S. population, and its prevalence is increasing, with approximately 79 million Americans at increased risk for diabetes. 1 Besides the risk of complications and the burden of disease on the patient, the cost associated with diabetes is a significant economic burden. Medical expenses for people living with diabetes are more than 2 times higher than for people living without diabetes, and inpatient care continues to be the largest expenditure (43% of total cost). In fact, the American Diabetes Association (ADA) estimates that the total annual cost of diagnosed diabetes rose to $245 billion in 2012 from $174 billion in ,3 Furthermore, the ADA estimated that nearly one-third of patients with diabetes may require 2 or more hospitalizations per year. 4 With the prevalence of diabetes expected to rise, inpatient costs will likely remain a major contributor to diabetes-related costs. Pharmacy services have expanded from traditional dispensing roles to include comprehensive clinical pharmacy services as part of the health care team. Currently, at least 70% of state boards of pharmacy authorize collaborative drug therapy management (CDTM) protocols between a clinical pharmacist and prescriber in the outpatient setting. 5 In the state of Texas, pharmacists working with a CDTM protocol can initiate, modify, or continue drug therapy for a referred patient. Previous studies have shown the value of clinical pharmacy services in improving health outcomes and reducing economic costs for patients with diabetes. 6 Benefits of CDTM include, but are not limited to, improving patient adherence, decreasing adverse events, avoiding drug interactions, and using the knowledge of the clinical pharmacist to promote enhanced services via direct patient care. 6-8 Previous studies have shown that patients with diabetes who receive clinical pharmacist interventions demonstrate significantly improved hemoglobin A1c Furthermore, the data have shown that increased A1c is associated with increased costs per hospitalization. In fact, patients with a mean A1c of at least 10% or greater have significantly higher rates of diabetes-related hospital utilization, compared with patients with a mean A1c of < 7%. 13 However, there is a lack of data for clinical pharmacists impact on inpatient utilization, especially in underserved populations. The purpose of this study was to assess the effect of clinical pharmacist involvement in a federally qualified health center (FQHC) on the change in A1c and frequency of diabetesrelated hospitalizations and emergency department (ED) visits. Methods Study Setting CommUnityCare is a FQHC with outpatient clinics in Austin, Texas, serving about 66,000 underserved and uninsured patients ( The majority of patients are enrolled in the Medical Access Program, which is available to Travis County residents who have a household income below the federal poverty guidelines, followed by patients who have federal insurance (i.e., Medicaid, Medicare). The clinical pharmacy program at CommUnityCare is comprised of pharmacists who have completed at least 1 year of a postdoctoral residency training program. Many of them hold advanced certifications in patient care (i.e., certified diabetes educator) and medication management (i.e., board certified ambulatory care pharmacist). CommUnityCare clinical pharmacists and participating prescribers update the CDTM protocol annually. Some services provided by the individual clinical pharmacists include, but are not limited to, implementing new medications, titrating medications, ordering laboratory panels, counseling on lifestyle modification, providing diabetes education, and managing associated comorbid conditions (i.e., hypertension, dyslipidemia). Under a CDTM protocol, patients referred to the clinical pharmacists for diabetes management are scheduled for a 30-minute visit as often as required to reach the patient s goals (i.e., A1c) and as clinically necessary for patient safety (i.e., to monitor laboratory values). Data from CommUnityCare covering the period between July 1, 2007, through July 1, 2011 (study period), were used to explore the relationship between clinical pharmacists interventions and changes in A1c, diabetes-related hospitalizations, and diabetes-related ED visits. This study was a retrospective review via electronic medical records from CommUnityCare, and the patients data were de-identified. The study was approved by the University of Texas Institutional Review Board and by CommUnityCare. Patient Selection Adult patients aged between 18 and 89 years with a diagnosis of type 1 or type 2 diabetes mellitus were identified during the time period of July 1, 2007, through July 1, Documentation of an A1c value at baseline (defined as within 3 months before or after initial visit with clinical pharmacy or usual care) was required. For enrollment in the study, patients must have had poor glycemic control, defined as an A1c 9% at baseline, and at least 3 visits with a clinical pharmacist or usual care. Usual care patients were followed by their primary care providers and had no appointments with a clinical pharmacist during the study period. Patients must have been Vol. 20, No. 9 September 2014 JMCP Journal of Managed Care & Specialty Pharmacy 915
3 TABLE 1 ICD-9-CM Codes for Diabetes and Diabetes-Related Complications Complication Identifier (ICD-9-CM Code) Description Hyperglycemia 250.1x Diabetes with ketoacidosis 250.2x Diabetes with hyperosmolarity 250.3x Diabetes with other coma Diabetic nephropathy 250.4x Diabetes with renal manifestations Diabetic retinopathy 250.5x Diabetes with ophthalmic complications 362.xx Diabetic retinopathy (e.g., proliferative) Diabetic neuropathy 250.6x Diabetes with neurological manifestations 357.2x Neuropathy in diabetes Diabetic peripheral circulatory disorders 250.7x Diabetes with peripheral circulatory disorders Hypoglycemia 250.8x Diabetes with other specified manifestations ICD-9-CM = International Classification of Diseases, Ninth Edition, Clinical Modification. eligible for at least 1 year before and 1 year after their index dates. In addition, a follow-up A1c (at least 1 year post-index) must have been documented in the database. Patients were excluded if they had a clinical pharmacy visit for any disease state before the study initiation, or if they had a diagnosis of cancer or human immunodeficiency virus, were pregnant, or had diagnosis codes for motor vehicle accidents or chronic pain (i.e., back pain, generalized pain, myalgia). Study Outcomes The outcomes of this study were 1-year post-index change in A1c, diabetes-related hospitalizations, and diabetes-related ED visits. Follow-up A1c values at least 1 year post-index were used to calculate the change in A1c from baseline for each patient. The International Classification of Diseases, Ninth Edition, Clinical Modification (ICD-9-CM) was used to identify diabetes-related diagnoses (Table 1). The ICD-9-CM codes identified are shortterm complications of diabetes that include hyperglycemia and hypoglycemia, as well as long-term complications of diabetes that include microvascular and macrovascular conditions. A hospitalization or ED visit was considered diabetes-related if 1 of the designated ICD-9-CM codes was documented in the diagnosis fields (up to 5 ICD-9-CM codes could be listed). Diabetes-related ED and hospital visits for 1 year pre-index and 1 year post-index were identified, and the difference in number of events for each patient was calculated. Statistical Analysis Clinical pharmacy and usual care groups were propensity score (PS) matched using a 1:1 ratio. Variables used for PS matching were age, gender, pre-index hospitalizations, preindex ED visits, and index A1c values. Sample size estimations FIGURE 1 Patient Sample Extraction Data extracted for patients with A1c baseline > 9% and at least 3 provider visits n = 1,716 (C = 1,256, I = 460) At least 1 year eligibility post-index visit n = 1,231 (C = 903, I = 328) At least 1 year follow-up and A1c follow-up n = 782 (C = 557, I = 225) Exclusion: less than 1 year eligibility post-index visit n = 485 (C = 353, I = 132) Exclusion: no follow-up A1c measure n = 449 (C = 346, I = 103) C = control group (usual care group); I = intervention group (clinical pharmacy group). were based on change in A1c, which was the primary outcome variable. For a 1-sided t-test of 2 independent means, with an effect size of 0.25, an alpha error P of 0.10, and a power of 95%, we estimated that 275 patients were needed in each group. In addition, to assess the change in A1c values, a general linear model (GLM) was conducted to control for baseline demographics (age, gender, race/ethnicity) and clinical characteristics (pre-index diabetes-related hospitalizations, pre-index diabetes-related ED visits, and index A1c). For the outcomes with count results and a high number of zeros (hospitalizations and ED visits), zero-inflated negative binomial regressions were conducted, again controlling for baseline characteristics. All analyses were conducted with an a priori alpha level of P < 0.10, using SAS version 9.2 (SAS Institute, Inc., Cary, NC). Results Patient Characteristics A total of 782 patients met inclusion criteria (Figure 1), with 225 intervention patients and 557 control patients. PS matching produced a 1:1 match of 220 patients per group. Demographics characteristics of the 2 cohorts before and after matching are listed in Table 2. Diabetes-Related Outcomes Table 3 provides information on the change in outcomes for both unmatched and matched samples to show similarity for both. T-test results for the matched groups (220 in each group) will be discussed. For the usual care group, the number of 916 Journal of Managed Care & Specialty Pharmacy JMCP September 2014 Vol. 20, No. 9
4 TABLE 2 Baseline Demographic Characteristics for Unmatched and Matched Groups Variable Unmatched (N = 557) Clinical Pharmacy Group Unmatched (N = 225) Matched Clinical Pharmacy Group Matched Age, mean ± SD 51.1 ± ± ± ± 11.5 Female, n (%) 304 (54.6) 140 (62.2) 132 (60.0) 135 (61.4) Hispanic, n (%) 418 (75.0) 156 (69.3) 167 (75.9) 153 (69.6) White, n (%) 58 (10.4) 30 (13.3) 24 (10.9) 29 (13.2) Black, n (%) 69 (12.4) 33 (14.7) 25 (11.4) 32 (14.5) Other, n (%) 12 (2.2) 6 (2.7) 4 (1.8) 6 (2.7) SD = standard deviation. hospitalizations for 220 patients was 8 for the pre-index year and 16 for the post-index year, for an increase of 8 hospitalizations (8 per 220, mean = 0.036, standard deviation [SD] = 0.284, or 3.6 hospitalizations per 100 patients). For the clinical pharmacist group, the number of hospitalizations for 220 patients was 6 for the pre-index year and 5 for the post-index year for a decrease of 1 hospitalization (-1 per 220, mean = , SD = 0.278). The difference in these changes was statistically significant (P = 0.06). For the usual care group, the number of ED visits for 220 patients was 28 for the pre-index year and 44 for the post-index year, for an increase of 16 visits (16 per 220, mean = 0.073, SD = 0.584, or 7.3 ED visits per 100 patients). For the clinical pharmacist group, the number of ED visits for 220 patients was 30 for the pre-index year and 34 for the post-index year, for an increase of 4 visits (4 per 220, mean = 0.018, SD = 0.641). The difference in these changes was not statistically significant (P = 0.18). For the matched cohorts, the mean change in A1c was (SD = 2.49) for the usual care group, while the mean change for the clinical pharmacist group was (SD = 2.44). The difference in A1c reduction was statistically significant (P = 0.04). In addition to t-tests, GLMs were conducted for these outcomes, controlling for the following covariates: gender, race/ ethnicity, age, number of pre-index diabetes-related ED visits, number of pre-index diabetes-related hospitalizations, and baseline A1c values. The difference in the number of diabetesrelated hospitalizations and the number of ED visits was not normally distributed, as both variables had a high number of zeros and a standard deviation higher than the mean; thus, a negative binomial distribution was assumed for these 2 models. Similar to the t-test results, the difference in the change in hospitalizations and the difference in A1c values were significantly different at the a priori level of significance (P = 0.06 and P = 0.05, respectively), while the change in the number of ED visits was not statistically different (P = 0.26). Discussion This study demonstrated that patients with uncontrolled type 1 or type 2 diabetes who had at least 3 visits with a clinical pharmacist had an additional improvement in A1c and diabetes-related hospital visits. In addition, the change in the number of diabetes-related ED visits was different in the expected direction, but this difference was not statistically significant. Previous studies have shown that patients who received pharmacist-managed care demonstrated improved A1c values Increased A1c is associated with increased costs per hospitalization, and these inpatient costs account for the major expenditure in health spending for patients with diabetes in the United States. Hospitalizations were considered to be diabetes-related if patients had an ICD-9-CM code listed in any of their diagnosis fields that matched at least 1 of 10 of the study s selected ICD-9-CM codes. Up to 5 ICD-9-CM codes could be listed per event. In contrast, a previous study required the ICD-9-CM code to be listed as the primary or secondary diagnosis to be included for analysis. 8 In our case, all diagnosis field entries were accepted for analysis, since the goal of the study was to identify diabetes-related events, regardless of prioritization of the ICD-9-CM codes. The 10 ICD-9-CM codes identified microvascular complications (i.e., nephropathy, neuropathy, retinopathy) because pharmacologic interventions to normalize glucose can reduce the risk of microvascular complications by 37% for every 1% drop in A1c. 14 A 2010 study used a broader range of ICD-9-CM codes that accounted for macrovascular complications such as ischemic heart disease and stroke, as well as acute complications such as infections. 15 However, a meta-analysis revealed that intensive glucose-lowering therapy modestly reduced major macrovascular events after an average follow-up of 4.4 years in patients with type 2 diabetes. 16 Thus, the length of time to see an effect on macrovascular outcomes precluded the necessity of including ICD-9-CM codes that identified these complications. Because there is large variability in the design of studies that rely on procedural codes for analysis, these are important considerations in designing future strategies to document disease-state complications. Our study identified important findings regarding clinical pharmacy intervention and the effect on inpatient usage in a FQHC. This study did not look at secondary outcome measures that have been documented in previous studies assessing Vol. 20, No. 9 September 2014 JMCP Journal of Managed Care & Specialty Pharmacy 917
5 TABLE 3 Comparison of Change in Outcomes for Unmatched and Matched Groups Variable Unmatched (N = 557) Clinical Pharmacy Group Unmatched (N = 225) Matched Clinical Pharmacy Group Matched Pre-index diabetes hospitalization: n, mean ± SD ± ± ± ± Post-index diabetes hospitalization: n, mean ± SD ± ± ± ± Change in diabetes hospitalizations: a mean ± SD ± ± b ± ± b Pre-index diabetes ED visits: n, mean ± SD ± ± ± ± Post-index diabetes ED visits: n, mean ± SD ± ± ± ± Change in diabetes ED visits: c mean ± SD ± ± d ± ± d Baseline A1c: mean, SD ± ± ± ± 1.55 Follow-up A1c: mean, SD 9.42 ± ± ± ± 2.30 Change in A1c: e mean, SD ± ± 2.50 b ± ± 2.44 b at-tests: unmatched comparison of change, P = 0.01; matched comparison of change, P = b P < c T-tests: unmatched comparison of change, P = 0.17; matched comparison of change, P = d Not significant at P < e T-tests: unmatched comparison of change, P = 0.09; matched comparison of change, P = A1c = hemoglobin A1c; ED = emergency department; SD = standard deviation. pharmacist impact on diabetes care. However, clinical pharmacist intervention has been shown to improve patient adherence with the ADA guidelines for preventive care. Significant improvement in health indicators after clinical pharmacy intervention include a decrease in low-density lipoprotein, increase in frequency of microalbumin screening, increase in annual eye and foot examination, and increase in daily aspirin use as appropriate. 17 Furthermore, improvement of quality-of-life measures (i.e., patient satisfaction) have been documented in the literature. 18 Limitations Since the analysis was retrospective in nature, only associations can be reported, not causality. In addition, retrospective studies do not allow for randomization, so selection bias is possible. Matching was conducted to address this issue, but unmeasured confounders could have played a role in group differences. One common limitation to similar studies comes from small sample sizes. Since less than 300 patients met the inclusion criteria for the intervention group, this limitation reduced the power of the analyses, and a P value less than 0.10 was chosen, based on expected sample size and expected effect size. The use of ICD-9-CM codes rather than medical records may raise concerns about clinical accuracy. For example, it is possible that the ICD-9-CM code was incorrectly documented, since it cannot be ascertained who input the code into the diagnosis field and whether the code matched the final diagnosis at discharge. Additionally, flaws in the ICD-9-CM system could not be avoided. For example, if a patient was admitted for a diabetes-related foot infection, the provider may not have included the diagnosis because a code does not exist for this exact wording. Another limitation was the number of hospitals contracted with the database that submitted information relating to hospitalizations and ED visits. Only 2 hospital systems submitted this information; thus, the outcomes were affected by the availability of only local data if a patient was hospitalized or went to the ED at a noncontracted hospital outside of the city. We assumed that patients only had clinical pharmacist intervention during this time period, but we did not know whether patients received other services that could impact outcomes. For example, if a patient saw a dietician for diabetes nutrition counseling, this interaction could be a variable to improvement of A1c. In addition, the degree/level of clinical pharmacist intervention is not standardized. Clinical pharmacists who work under a CDTM have a variety of roles, depending on the nature and need of the visit. In many instances, the first visit focuses on diabetes education, which includes, but is not limited to, insulin pen administration, glucose monitoring recommendations, nutrition, and preventive services (i.e., immunization recommendations). This study attempted to control for this unknown by requiring that a patient have 3 visits to be included in the study to determine the impact of clinical pharmacist intervention as shown in previous studies. 8,11 This study was conducted in a FQHC setting; thus, generalizability of the results is limited to underinsured and underserved populations. The majority of the study population was Hispanic 918 Journal of Managed Care & Specialty Pharmacy JMCP September 2014 Vol. 20, No. 9
6 (about 70%). Minority populations, especially Hispanic patients, have a higher prevalence of diabetes, worse glycemic control, poor adherence, and more complications than non-hispanic white patients with diabetes. 11 Previous studies have observed that Hispanics have a lower rate of diabetes-related hospitalizations. 11,19,20 Multiple factors contribute to this finding, such as cultural stigma associated with the hospital setting. In this study s demographic, socioeconomic status could prohibit a patient from going to the hospital or ED even when needed. Barriers to health care access also include low English proficiency, low health literacy, lack of personal identification, and misunderstanding of the disease state. 21,22 Conclusions For this underserved population of patients with either type 1 or type 2 diabetes, a significant and beneficial relationship was seen in the change in A1c and the change in the number of diabetes-related hospitalizations after 3 visits with a clinical pharmacist when compared with usual care. While the change in ED visits trended in the expected direction, this comparison was not statistically significant. Future research to examine utilization patterns and changes for clinical pharmacy services may be important for expanding CDTM protocols to further improve outcomes for patients with diabetes. Authors NANCY CHUNG, PharmD, BCACP, is Clinical Assistant Professor, University of Houston College of Pharmacy, Houston, Texas. KAREN RASCATI, PhD, is Professor of Health Outcomes and Pharmacy Practice, and DEBRA LOPEZ, PharmD, CDE, BCPS, BCACP, is Clinical Associate Professor, University of Texas College of Pharmacy, Austin, Texas. JASON JOKERST, PharmD, BCPS, is Clinical Pharmacist, and AIDA GARZA, PharmD, CDE, BCACP, is Clinical Pharmacist, CommUnityCare, Austin, Texas. AUTHOR CORRESPONDENCE: Nancy Chung, PharmD, BCACP, Clinical Assistant Professor, University of Houston College of Pharmacy, 1441 Moursund St., Houston, TX Tel.: ; nchung@central.uh.edu. DISCLOSURES The authors report no conflicts of interest regarding this study. All authors collaborated in the concept and design of this study. Chung and Rascati collected the data and were primarily responsible for data interpretation, with assistance from the other authors. The manuscript was written by Chung, and all authors participated in the revision. REFERENCES 1. U.S. Centers for Disease Control and Prevention. National diabetes fact sheet, Available at: pdf. Accessed June 11, American Diabetes Association. Economic costs of diabetes in the U.S. in Diabetes Care. 2013;36(4): American Diabetes Association. Economic costs of diabetes in the U.S. in Diabetes Care. 2008;31(3): Jiang HJ, Stryer D, Friedman B, Andrews R. Multiple hospitalizations for patients with diabetes. Diabetes Care. 2003;26(5): Hammond RW, Schwartz AH, Campbell MJ, et al. Collaborative drug therapy management by pharmacists Pharmacotherapy. 2003;23(9): Chisholm-Burns MA, Graff Zivin JS, Lee JK, et al. Economic effects of pharmacists on health outcomes in the United States: a systematic review. Am J Health Syst Pharm. 2010;67(19): Cranor CW, Bunting BA, Christensen DB. The Asheville Project: longterm clinical and economic outcomes of a community pharmacy diabetes care program. J Am Pharm Assoc (Wash). 2003;43(2): Anaya JP, Rivera JO, Lawson K, Garcia J, Luna J Jr, Ortiz M. Evaluation of pharmacist-managed diabetes mellitus under a collaborative drug therapy agreement. Am J Health Syst Pharm. 2008;65(19): Sease JM, Franklin MA, Gerrald KR. Pharmacist management of patients with diabetes mellitus enrolled in a rural free clinic. Am J Health Syst Pharm. 2013;70(1): Ip EJ, Shah BM, Yu J, Nguyen LT, Bhatt DC. Enhancing diabetes care by adding a pharmacist to the primary care team. Am J Health Syst Pharm. 2013;70(10): Johnson KA, Chen S, Cheng IN, et al. The impact of clinical pharmacy services integrated into medical homes on diabetes-related clinical outcomes. Ann Pharmacother. 2010;44(12): Choe HM, Mitrovich S, Dubay D, Hayward RA, Krein SL, Vijan S. Proactive case management of high-risk patients with type 2 diabetes mellitus by a clinical pharmacist: a randomized controlled trial. Am J Manag Care. 2005;11(4): Coast-Senior EA, Kroner BA, Kelley CL, Trilli LE. Management of patients with type 2 diabetes by pharmacists in primary care clinics. Ann Pharmacother. 1998;32(6): UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes. Lancet. 1998;352(9131): Menzin J, Korn JR, Cohen J, et al. Relationship between glycemic control and diabetes-related hospital costs in patients with type 1 or type 2 diabetes mellitus. J Manag Care Pharm. 2010;16(4): Available at: amcp.org/workarea/downloadasset.aspx?id= Turnbull FM, Abraira C, Anderson RJ, et al. Intensive glucose control and macrovascular outcomes in type 2 diabetes. Diabetologia. 2009;52(11): Kiel PJ, McCord AD. Pharmacist impact on clinical outcomes in a diabetes disease management program via collaborative practice. Ann Pharmacother. 2005;39(11): Scott DM, Boyd ST, Stephan M, Augustine SC, Reardon TP. Outcomes of pharmacist-managed diabetes care services in a community health center. Am J Health Syst Pharm. 2006;63(21): Cook CB, Naylor DB, Hentz JB, et al. Disparities in diabetes-related hospitalizations: relationship of age, sex, and race/ethnicity with hospital discharges, lengths of stay, and direct inpatient charges. Ethn Dis. 2006;16(1): Davis SK, Liu Y, Gibbons GH. Disparities in trends of hospitalization for potentially preventable chronic conditions among African Americans during the 1990s: implications and benchmarks. Am J Public Health. 2003;93(3): Dilworth TJ, Mott D, Young H. Pharmacists communication with Spanish-speaking patients: a review of the literature to establish an agenda for future research. Res Social Adm Pharm. 2009;5(2): Gerber BS, Cano AI, Caceres ML, et al. A pharmacist and health promoter team to improve medication adherence among Latinos with diabetes. Ann Pharmacother. 2010;44(1): Vol. 20, No. 9 September 2014 JMCP Journal of Managed Care & Specialty Pharmacy 919
Diabetes affects 25.8 million people in the United
 Impact of Clinical Pharmacy Services on Outcomes and Costs for Indigent Patients With Diabetes Marissa Escobar Quinones, PharmD, CDE; Margaret Youngmi Pio, PharmD, BCPS, CDE; Diem Hong Chow, PharmD, CDE;
Impact of Clinical Pharmacy Services on Outcomes and Costs for Indigent Patients With Diabetes Marissa Escobar Quinones, PharmD, CDE; Margaret Youngmi Pio, PharmD, BCPS, CDE; Diem Hong Chow, PharmD, CDE;
Effectiveness of a Multidisciplinary Patient Assistance Program in Diabetes Care
 University of Rhode Island DigitalCommons@URI Senior Honors Projects Honors Program at the University of Rhode Island 2009 Effectiveness of a Multidisciplinary Patient Assistance Program in Diabetes Care
University of Rhode Island DigitalCommons@URI Senior Honors Projects Honors Program at the University of Rhode Island 2009 Effectiveness of a Multidisciplinary Patient Assistance Program in Diabetes Care
DUPLICATION DISTRIBUTION PROHIBBITED AND. Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity
 General Session IV Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity Accreditation UAN 0024-0000-12-012-L04-P Participation in this activity earns 2.0 contact
General Session IV Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity Accreditation UAN 0024-0000-12-012-L04-P Participation in this activity earns 2.0 contact
LOUISIANA MEDICAID PROGRAM ISSUED: 02/01/12 REPLACED: 02/01/94 CHAPTER 5: PROFESSIONAL SERVICES SECTION 5.1: COVERED SERVICES PAGE(S) 6
 Diabetes Education Management Training Diabetes self management training (DSMT) is a collaborative process through which recipients with diabetes gain knowledge and skills needed to modify behavior and
Diabetes Education Management Training Diabetes self management training (DSMT) is a collaborative process through which recipients with diabetes gain knowledge and skills needed to modify behavior and
Glycemic Control in Pharmacist-Managed Insulin Titration Versus Standard Care in an Indigent Population
 Glycemic Control in Pharmacist-Managed Insulin Titration Versus Standard Care in an Indigent Population Jamie M. Pitlick, PharmD, BCPS, and Amie D. Brooks, PharmD, BCPS Address correspondence to Jamie
Glycemic Control in Pharmacist-Managed Insulin Titration Versus Standard Care in an Indigent Population Jamie M. Pitlick, PharmD, BCPS, and Amie D. Brooks, PharmD, BCPS Address correspondence to Jamie
Diabetes affects 29.1 million
 Evaluation of Diabetes Education and Pharmacist Interventions in a Rural, Primary Care Setting Lisa T. Meade, 1,2 Rebecca C. Tart, 2 and Hillary L. Buzby 3 1 Wingate University, Hickory, NC 2 Catawba Valley
Evaluation of Diabetes Education and Pharmacist Interventions in a Rural, Primary Care Setting Lisa T. Meade, 1,2 Rebecca C. Tart, 2 and Hillary L. Buzby 3 1 Wingate University, Hickory, NC 2 Catawba Valley
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH:
 A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
RESEARCH. What this study adds
 RESEARCH to Type 2 Diabetes and Its Effect on Health Care Costs in Low-Income and Insured Patients with Prediabetes: A Retrospective Study Using Medicaid Claims Data Jun Wu, PhD; Eileen Ward, PharmD, BCACP;
RESEARCH to Type 2 Diabetes and Its Effect on Health Care Costs in Low-Income and Insured Patients with Prediabetes: A Retrospective Study Using Medicaid Claims Data Jun Wu, PhD; Eileen Ward, PharmD, BCACP;
Key Elements in Managing Diabetes
 Key Elements in Managing Diabetes Presentor Disclosure No conflicts of interest to disclose Presented by Susan Cotey, RN, CDE Lennon Diabetes Center Stephanie Tubbs Jones Health Center Cleveland Clinic
Key Elements in Managing Diabetes Presentor Disclosure No conflicts of interest to disclose Presented by Susan Cotey, RN, CDE Lennon Diabetes Center Stephanie Tubbs Jones Health Center Cleveland Clinic
Student Paper PRACTICE-BASED RESEARCH
 The Role of Clinical Pharmacists in Modifying Cardiovascular Disease Risk Factors Autumn Bagwell, PharmD. 1 ; Jessica W. Skelley, PharmD 2 ; Lana Saad, PharmD 3 ; Thomas Woolley, PhD 4 ; and DeeAnn Dugan,
The Role of Clinical Pharmacists in Modifying Cardiovascular Disease Risk Factors Autumn Bagwell, PharmD. 1 ; Jessica W. Skelley, PharmD 2 ; Lana Saad, PharmD 3 ; Thomas Woolley, PhD 4 ; and DeeAnn Dugan,
medicaid and the The Role of Medicaid for People with Diabetes
 on medicaid and the uninsured The Role of for People with Diabetes November 2012 Introduction Diabetes is one of the most prevalent chronic conditions and a leading cause of death in the United States.
on medicaid and the uninsured The Role of for People with Diabetes November 2012 Introduction Diabetes is one of the most prevalent chronic conditions and a leading cause of death in the United States.
An Evaluation of the Barriers to Patient use of Glucometer Control Solutions: A Survey of Patients, Pharmacists, and Providers
 AADE14 ANNUAL MEETING & EXHIBITION AUGUST 6-9, 2014 ORLANDO, FL An Evaluation of the Barriers to Patient use of Glucometer s: A Survey of Patients, Pharmacists, and Providers Katherine S. O Neal, Pharm.D.,
AADE14 ANNUAL MEETING & EXHIBITION AUGUST 6-9, 2014 ORLANDO, FL An Evaluation of the Barriers to Patient use of Glucometer s: A Survey of Patients, Pharmacists, and Providers Katherine S. O Neal, Pharm.D.,
Pharmacists Role in Improving Diabetes Medication Management. Marie Smith, Pharm.D.
 Journal of Diabetes Science and Technology Volume 3, Issue 1, January 2009 Diabetes Technology Society CLINICAL APPLICATIONS Pharmacists Role in Improving Diabetes Medication Management Marie, Pharm.D.
Journal of Diabetes Science and Technology Volume 3, Issue 1, January 2009 Diabetes Technology Society CLINICAL APPLICATIONS Pharmacists Role in Improving Diabetes Medication Management Marie, Pharm.D.
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Lack of documentation on overweight & obese status in patients admitted to the coronary care unit: Results from the CCU study
 Lack of documentation on overweight & obese status in patients admitted to the coronary care unit: Results from the CCU study Meriam F. Caboral,, RN, MSN, NP-C Clinical Coordinator Heart Failure Components
Lack of documentation on overweight & obese status in patients admitted to the coronary care unit: Results from the CCU study Meriam F. Caboral,, RN, MSN, NP-C Clinical Coordinator Heart Failure Components
PHARMACOTHERAPY Volume 27, Number 5, 2007
 Pharmacist-Managed Vaccination Program Increased Influenza Vaccination Rates in Cardiovascular Patients Enrolled in a Secondary Prevention Lipid Clinic Susan M. Loughlin, Pharm.D., Ali Mortazavi, M.D.,
Pharmacist-Managed Vaccination Program Increased Influenza Vaccination Rates in Cardiovascular Patients Enrolled in a Secondary Prevention Lipid Clinic Susan M. Loughlin, Pharm.D., Ali Mortazavi, M.D.,
Effects of a Community Pharmacist-Based Diabetes Patient-Management Program on Intermediate Clinical Outcome Measures
 RESEARCH Effects of a Community Pharmacist-Based Diabetes Patient-Management Program on Intermediate Clinical Outcome Measures OBJECTIVES: Evaluate a community pharmacist-based diabetes patient-management
RESEARCH Effects of a Community Pharmacist-Based Diabetes Patient-Management Program on Intermediate Clinical Outcome Measures OBJECTIVES: Evaluate a community pharmacist-based diabetes patient-management
Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States
 Diabetes Care In Press, published online February 8, 007 Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States Received
Diabetes Care In Press, published online February 8, 007 Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States Received
A nationwide population-based study. Pai-Feng Hsu M.D. Shao-Yuan Chuang PhD
 The Association of Clinical Symptomatic Hypoglycemia with Cardiovascular Events and Total Death in Type 2 Diabetes Mellitus A nationwide population-based study Pai-Feng Hsu M.D. Shao-Yuan Chuang PhD Taipei
The Association of Clinical Symptomatic Hypoglycemia with Cardiovascular Events and Total Death in Type 2 Diabetes Mellitus A nationwide population-based study Pai-Feng Hsu M.D. Shao-Yuan Chuang PhD Taipei
Clinical and Economic Summary Report. for Employers
 Clinical and Economic Summary Report for Employers Magaly Rodriguez de Bittner, PharmD, CDE, FAPhA Director, P 3 Program Dawn Shojai, PharmD Assistant Director, P 3 Program P 3 Clinical & Economic Summary
Clinical and Economic Summary Report for Employers Magaly Rodriguez de Bittner, PharmD, CDE, FAPhA Director, P 3 Program Dawn Shojai, PharmD Assistant Director, P 3 Program P 3 Clinical & Economic Summary
Diabetes mellitus affects 23 million people in the United
 n clinical n Pharmacist Collaborative Management of Poorly Controlled Diabetes Mellitus: A Randomized Controlled Trial John P. Jameson, PharmD; and Philip J. Baty, MD Objective: To investigate the effect
n clinical n Pharmacist Collaborative Management of Poorly Controlled Diabetes Mellitus: A Randomized Controlled Trial John P. Jameson, PharmD; and Philip J. Baty, MD Objective: To investigate the effect
Addressing Racial and Ethnic Disparities in Diabetes Care. Development and Support. Accreditation Information
 Addressing Racial and Ethnic Disparities in Diabetes Care Jennifer D. Smith, PharmD, CPP, BC ADM, CDE Associate Professor College of Pharmacy and Health Sciences Campbell University Clinical Pharmacist
Addressing Racial and Ethnic Disparities in Diabetes Care Jennifer D. Smith, PharmD, CPP, BC ADM, CDE Associate Professor College of Pharmacy and Health Sciences Campbell University Clinical Pharmacist
Finland and Sweden and UK GP-HOSP datasets
 Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Monthly Campaign Webinar February 21, 2019
 Monthly Campaign Webinar February 21, 2019 2 Today s Webinar Together 2 Goal Updates Webinar Reminders AMGA Annual Conference New Campaign Partnership 2019 Million Hearts Hypertension Control Challenge
Monthly Campaign Webinar February 21, 2019 2 Today s Webinar Together 2 Goal Updates Webinar Reminders AMGA Annual Conference New Campaign Partnership 2019 Million Hearts Hypertension Control Challenge
Provider Bulletin December 2018 Coding spotlight: diabetes provider guide to coding the diagnosis and treatment of diabetes
 Medi-Cal Managed Care L. A. Care Provider Bulletin December 2018 provider guide to coding the diagnosis and treatment of diabetes Diabetes mellitus is a chronic disorder caused by either an absolute decrease
Medi-Cal Managed Care L. A. Care Provider Bulletin December 2018 provider guide to coding the diagnosis and treatment of diabetes Diabetes mellitus is a chronic disorder caused by either an absolute decrease
Evaluation Report ICC Asthma Network Project Integrated Care Collaboration and Seton Family of Hospitals July 2008
 Evaluation Report ICC Asthma Network Project Integrated Care Collaboration and Seton Family of Hospitals July 2008 By Anjum Khurshid, PhD Contributors: Steve Conti, Cindy Batcher, Sandy Coe Simmons, &
Evaluation Report ICC Asthma Network Project Integrated Care Collaboration and Seton Family of Hospitals July 2008 By Anjum Khurshid, PhD Contributors: Steve Conti, Cindy Batcher, Sandy Coe Simmons, &
About the Highmark Foundation
 About the Highmark Foundation The Highmark Foundation, created in 2000 as an affiliate of Highmark Inc., is a charitable organization and a private foundation that supports initiatives and programs aimed
About the Highmark Foundation The Highmark Foundation, created in 2000 as an affiliate of Highmark Inc., is a charitable organization and a private foundation that supports initiatives and programs aimed
Diabetes. Health Care Disparities: Medical Evidence. A Constellation of Complications. Every 24 hours.
 Health Care Disparities: Medical Evidence Diabetes Effects 2.8 Million People in US 7% of the US Population Sixth Leading Cause of Death Kenneth J. Steier, DO, MBA, MPH, MHA, MGH Dean of Clinical Education
Health Care Disparities: Medical Evidence Diabetes Effects 2.8 Million People in US 7% of the US Population Sixth Leading Cause of Death Kenneth J. Steier, DO, MBA, MPH, MHA, MGH Dean of Clinical Education
Chapter. CPT only copyright 2008 American Medical Association. All rights reserved. 15Diabetic Equipment and Supplies
 Chapter 15Diabetic Equipment and Supplies 15 15.1 Enrollment...................................................... 15-2 15.2 Benefits, Limitations, and Authorization Requirements......................
Chapter 15Diabetic Equipment and Supplies 15 15.1 Enrollment...................................................... 15-2 15.2 Benefits, Limitations, and Authorization Requirements......................
A comparison of diabetic complications and health care utilization in diabetic patients with and without
 John A. Dufton, DC, MD, Wilson W. Li, BSc (Pharm), MD, Mieke Koehoorn, PhD A comparison of diabetic complications and health care utilization in diabetic patients with and without comorbid A Canadian cross-sectional
John A. Dufton, DC, MD, Wilson W. Li, BSc (Pharm), MD, Mieke Koehoorn, PhD A comparison of diabetic complications and health care utilization in diabetic patients with and without comorbid A Canadian cross-sectional
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES
 HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
July, Years α : 7.7 / 10, Years α : 11 / 10,000 < 5 Years: 80 / 10, Reduce emergency department visits for asthma.
 What are the Healthy People 1 objectives? July, 6 Sponsored by the U.S. Department of Health and Human Services, the Healthy People 1 initiative is a comprehensive set of disease prevention and health
What are the Healthy People 1 objectives? July, 6 Sponsored by the U.S. Department of Health and Human Services, the Healthy People 1 initiative is a comprehensive set of disease prevention and health
Why Do We Treat Obesity? Epidemiology
 Why Do We Treat Obesity? Epidemiology Epidemiology of Obesity U.S. Epidemic 2 More than Two Thirds of US Adults Are Overweight or Obese 87.5 NHANES Data US Adults Age 2 Years (Crude Estimate) Population
Why Do We Treat Obesity? Epidemiology Epidemiology of Obesity U.S. Epidemic 2 More than Two Thirds of US Adults Are Overweight or Obese 87.5 NHANES Data US Adults Age 2 Years (Crude Estimate) Population
Chapter 6: Medicare Expenditures for CKD
 Chapter 6: Medicare Expenditures for CKD Introduction Determining the economic impact of chronic kidney disease (CKD) on the health care system is challenging on several levels. There is, for instance,
Chapter 6: Medicare Expenditures for CKD Introduction Determining the economic impact of chronic kidney disease (CKD) on the health care system is challenging on several levels. There is, for instance,
Coding spotlight: diabetes provider guide to coding the diagnosis and treatment of diabetes
 Medicaid Managed Care December 2018 provider guide to coding the diagnosis and treatment of diabetes Diabetes mellitus is a chronic disorder caused by either an absolute decrease in the amount of insulin
Medicaid Managed Care December 2018 provider guide to coding the diagnosis and treatment of diabetes Diabetes mellitus is a chronic disorder caused by either an absolute decrease in the amount of insulin
Financial Disclosure. Diabetes in the State of Florida. The Scope of Diabetes in Florida(cont.) The Scope of Diabetes in Florida
 Financial Disclosure Diabetes in the State of Florida Alina M. Alonso, M.D. Director November 17, 2017 I do not have any financial relationship relative to the content of this presentation. Florida Department
Financial Disclosure Diabetes in the State of Florida Alina M. Alonso, M.D. Director November 17, 2017 I do not have any financial relationship relative to the content of this presentation. Florida Department
Clinical Therapeutics/Volume 33, Number 1, 2011
 Clinical Therapeutics/Volume 33, Number 1, 2011 Concurrent Control of Blood Glucose, Body Mass, and Blood Pressure in Patients With Type 2 Diabetes: An Analysis of Data From Electronic Medical Records
Clinical Therapeutics/Volume 33, Number 1, 2011 Concurrent Control of Blood Glucose, Body Mass, and Blood Pressure in Patients With Type 2 Diabetes: An Analysis of Data From Electronic Medical Records
Shaping our future: a call to action to tackle the diabetes epidemic and reduce its economic impact
 Shaping our future: a call to action to tackle the diabetes epidemic and reduce its economic impact Task Force for the National Conference on Diabetes: The Task Force is comprised of Taking Control of
Shaping our future: a call to action to tackle the diabetes epidemic and reduce its economic impact Task Force for the National Conference on Diabetes: The Task Force is comprised of Taking Control of
Outcomes of pharmacists interventions in the collaborative care of patients with diabetes
 Pharmacy Education, January 2009; 9 (1): 18-22 Outcomes of pharmacists interventions in the collaborative care of patients with diabetes AZUKA C. OPARAH 1*, AKINTOYE J FAMAKINDE 2 & ADEBAYO OJ2 1 Department
Pharmacy Education, January 2009; 9 (1): 18-22 Outcomes of pharmacists interventions in the collaborative care of patients with diabetes AZUKA C. OPARAH 1*, AKINTOYE J FAMAKINDE 2 & ADEBAYO OJ2 1 Department
Health literacy is associated with patients adherence-related knowledge and motivation, but not adherence or clinical outcomes
 Health literacy is associated with patients adherence-related knowledge and motivation, but not adherence or clinical outcomes Connor S. Corcoran, BS 1 Lindsay S. Mayberry, PhD, MS 2 Chandra Y. Osborn,
Health literacy is associated with patients adherence-related knowledge and motivation, but not adherence or clinical outcomes Connor S. Corcoran, BS 1 Lindsay S. Mayberry, PhD, MS 2 Chandra Y. Osborn,
Building Systems to Evaluate Food Insecurity Screening and Diabetes Within an FQHC
 Building Systems to Evaluate Food Insecurity Screening and Diabetes Within an FQHC Danielle Lazar, Director of Research, Access Community Health Network Kathleen Gregory, Principal, Kathleen Gregory Consulting,
Building Systems to Evaluate Food Insecurity Screening and Diabetes Within an FQHC Danielle Lazar, Director of Research, Access Community Health Network Kathleen Gregory, Principal, Kathleen Gregory Consulting,
A Summary Report: 2003
 D iabetes in Idaho A Summary Report: 2003 Idaho Department of Health and Welfare Division of Health Bureau of Community and Environmental Health This publication was supported by Grant No. U32/CCU022691-02
D iabetes in Idaho A Summary Report: 2003 Idaho Department of Health and Welfare Division of Health Bureau of Community and Environmental Health This publication was supported by Grant No. U32/CCU022691-02
Disparities in Epilepsy Care: What is Known/Not Known December 4, 2011
 Disparities in Epilepsy Care: What is Known/Not Known December 4, 2011 Charles E. Begley, Ph.D. University of Texas School of Public Health Disclosure Name of Commercial Interest Type of Financial Relationship
Disparities in Epilepsy Care: What is Known/Not Known December 4, 2011 Charles E. Begley, Ph.D. University of Texas School of Public Health Disclosure Name of Commercial Interest Type of Financial Relationship
Prevalence of Mental Illness
 Section 1 Prevalence of Mental Illness The prevalence of mental health problems or mental illness appears to be quite stable over time. Full epidemiological surveys of prevalence, reported using complex
Section 1 Prevalence of Mental Illness The prevalence of mental health problems or mental illness appears to be quite stable over time. Full epidemiological surveys of prevalence, reported using complex
Community Health Profile: Minnesota, Wisconsin, & Michigan Tribal Communities 2006
 Community Health Profile: Minnesota, Wisconsin, & Michigan Tribal Communities 26 This report is produced by: The Great Lakes EpiCenter If you would like to reproduce any of the information contained in
Community Health Profile: Minnesota, Wisconsin, & Michigan Tribal Communities 26 This report is produced by: The Great Lakes EpiCenter If you would like to reproduce any of the information contained in
Senior Leaders and the Strategic Alignment of Community Benefit Programs: The Example of Diabetes
 Senior Leaders and the Strategic Alignment of Community Benefit Programs: The Example of Diabetes Posted: February 17, 2009 By Patsy Matheny, Community Benefit Consultant. Sugar Grove, Ohio Moving community
Senior Leaders and the Strategic Alignment of Community Benefit Programs: The Example of Diabetes Posted: February 17, 2009 By Patsy Matheny, Community Benefit Consultant. Sugar Grove, Ohio Moving community
Camden Citywide Diabetes Collaborative
 Camden Citywide Diabetes Collaborative The Camden Coalition of Healthcare Providers is an organization that seeks to improve the quality, capacity and accessibility of the health care system for vulnerable,
Camden Citywide Diabetes Collaborative The Camden Coalition of Healthcare Providers is an organization that seeks to improve the quality, capacity and accessibility of the health care system for vulnerable,
AN INDIRECT EVALUATION OF THE NATIONAL PROGRAM OF DIABETES MELLITUS STUDY CASE OF ROMANIA
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2013 vol. 117, no. 2 PREVENTIVE MEDICINE - LABORATORY ORIGINAL PAPERS AN INDIRECT EVALUATION OF THE NATIONAL PROGRAM OF DIABETES MELLITUS STUDY CASE OF ROMANIA Maria
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2013 vol. 117, no. 2 PREVENTIVE MEDICINE - LABORATORY ORIGINAL PAPERS AN INDIRECT EVALUATION OF THE NATIONAL PROGRAM OF DIABETES MELLITUS STUDY CASE OF ROMANIA Maria
Evaluating the Effectiveness of Physician and Clinical Pharmacist Patient Education and Disease Management in Diabetes Mellitus
 Evaluating the Effectiveness of Physician and Clinical Pharmacist Patient Education and Disease Management in Diabetes Mellitus By Sotheavy Vann MD Candidate 2017, Morehouse School of Medicine GE-NMF Primary
Evaluating the Effectiveness of Physician and Clinical Pharmacist Patient Education and Disease Management in Diabetes Mellitus By Sotheavy Vann MD Candidate 2017, Morehouse School of Medicine GE-NMF Primary
Diabetes affects 29.1 million people in the United States
 RESEARCH Predictors of Change in Adherence Status from 1 Year to the Next Among Patients with Type 2 Diabetes Mellitus on Oral Antidiabetes Drugs Vishal Saundankar, MS; Xiaomei Peng, MD, PhD; Haoda Fu,
RESEARCH Predictors of Change in Adherence Status from 1 Year to the Next Among Patients with Type 2 Diabetes Mellitus on Oral Antidiabetes Drugs Vishal Saundankar, MS; Xiaomei Peng, MD, PhD; Haoda Fu,
School of Health Science & Nursing, Wuhan Polytechnic University, Wuhan , China 2. Corresponding author
 2017 International Conference on Medical Science and Human Health (MSHH 2017) ISBN: 978-1-60595-472-1 Association of Self-rated Health Status and Perceived Risk Among Chinese Elderly Patients with Type
2017 International Conference on Medical Science and Human Health (MSHH 2017) ISBN: 978-1-60595-472-1 Association of Self-rated Health Status and Perceived Risk Among Chinese Elderly Patients with Type
Hypoglycemics, Lantus Insulin
 Texas Prior Authorization Program PDL Edit Criteria Drug/Drug Class Hypoglycemics, Lantus Insulin Information Included in this Document Hypoglycemics, Lantus Insulin Drugs requiring prior authorization:
Texas Prior Authorization Program PDL Edit Criteria Drug/Drug Class Hypoglycemics, Lantus Insulin Information Included in this Document Hypoglycemics, Lantus Insulin Drugs requiring prior authorization:
Original Research PHARMACY PRACTICE
 The Role of Ambulatory Care Pharmacists in an HIV Multidisciplinary Team within a Free and Bilingual Clinic Radha S. Vanmali, Pharm.D., BCACP; Sallie D. Mayer, Pharm.D., MBA, BCPS, CDE; and Ann M. Fugit,
The Role of Ambulatory Care Pharmacists in an HIV Multidisciplinary Team within a Free and Bilingual Clinic Radha S. Vanmali, Pharm.D., BCACP; Sallie D. Mayer, Pharm.D., MBA, BCPS, CDE; and Ann M. Fugit,
Diabetes Management: Interventions Engaging Community Health Workers
 Diabetes Management: Interventions Engaging Community Health Workers Community Preventive Services Task Force Finding and Rationale Statement Ratified April 2017 Table of Contents Intervention Definition...
Diabetes Management: Interventions Engaging Community Health Workers Community Preventive Services Task Force Finding and Rationale Statement Ratified April 2017 Table of Contents Intervention Definition...
Pharmacists Attitudes and Role in Diabetes Management in Kuwait
 Original Paper Received: April 5, 2016 Accepted: January 15, 2017 Published online: January 18, 2017 Pharmacists Attitudes and Role in Diabetes Management in Kuwait Asmaa A. Al Haqan a Dalal M. Al-Taweel
Original Paper Received: April 5, 2016 Accepted: January 15, 2017 Published online: January 18, 2017 Pharmacists Attitudes and Role in Diabetes Management in Kuwait Asmaa A. Al Haqan a Dalal M. Al-Taweel
Role of the Clinical Pharmacist in Primary Care
 Role of the Clinical Pharmacist in Primary Care Amy Kramer, Pharm.D., Manager Clinical Pharmacy Services Kaiser Permanente Holly Miller, Pharm.D., BCACP, Primary Care Clinical Pharmacist Kaiser Permanente
Role of the Clinical Pharmacist in Primary Care Amy Kramer, Pharm.D., Manager Clinical Pharmacy Services Kaiser Permanente Holly Miller, Pharm.D., BCACP, Primary Care Clinical Pharmacist Kaiser Permanente
Community Health Workers Make Cents: A return on investment analysis MHP SALUD WORKS TO UNDERSTAND THE FINANCIAL IMPACT OF COMMUNITY HEALTH WORKERS
 Community Health Workers Make Cents: A return on investment analysis MHP SALUD WORKS TO UNDERSTAND THE FINANCIAL IMPACT OF COMMUNITY HEALTH WORKERS Overview Background Literature Methods Results Conclusion
Community Health Workers Make Cents: A return on investment analysis MHP SALUD WORKS TO UNDERSTAND THE FINANCIAL IMPACT OF COMMUNITY HEALTH WORKERS Overview Background Literature Methods Results Conclusion
DIABETES MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
New Approaches Focusing on Dynamic Variables Related to Changes in. New Approaches Focusing on Dynamic
 New Approaches Focusing on Dynamic New Approaches Focusing on Dynamic Variables Related to Changes in Variables Related to Changes in Member s Health Status: Member s Health Status: Diabetic HbA1c Predictive
New Approaches Focusing on Dynamic New Approaches Focusing on Dynamic Variables Related to Changes in Variables Related to Changes in Member s Health Status: Member s Health Status: Diabetic HbA1c Predictive
Medical Policy An independent licensee of the Blue Cross Blue Shield Association.
 Insulin Pump Page 1 of 12 Medical Policy An independent licensee of the Blue Cross Blue Shield Association. Title: Insulin Pump Professional Original Effective Date: January 1, 1999 Revision Date(s): June
Insulin Pump Page 1 of 12 Medical Policy An independent licensee of the Blue Cross Blue Shield Association. Title: Insulin Pump Professional Original Effective Date: January 1, 1999 Revision Date(s): June
Effects of Antiepileptic Drug Substitutions on Epileptic Events Requiring Acute Care
 Effects of Antiepileptic Drug Substitutions on Epileptic Events Requiring Acute Care Karen L. Rascati, Ph.D., Kristin M. Richards, Ph.D., Michael T. Johnsrud, Ph.D., and Teresa A. Mann, Pharm.D. Study
Effects of Antiepileptic Drug Substitutions on Epileptic Events Requiring Acute Care Karen L. Rascati, Ph.D., Kristin M. Richards, Ph.D., Michael T. Johnsrud, Ph.D., and Teresa A. Mann, Pharm.D. Study
DIABETES AND THE AT-RISK LOWER LIMB:
 DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
Jae Jin An, Ph.D. Michael B. Nichol, Ph.D.
 IMPACT OF MULTIPLE MEDICATION COMPLIANCE ON CARDIOVASCULAR OUTCOMES IN PATIENTS WITH TYPE II DIABETES AND COMORBID HYPERTENSION CONTROLLING FOR ENDOGENEITY BIAS Jae Jin An, Ph.D. Michael B. Nichol, Ph.D.
IMPACT OF MULTIPLE MEDICATION COMPLIANCE ON CARDIOVASCULAR OUTCOMES IN PATIENTS WITH TYPE II DIABETES AND COMORBID HYPERTENSION CONTROLLING FOR ENDOGENEITY BIAS Jae Jin An, Ph.D. Michael B. Nichol, Ph.D.
Brigham and Women s Hospital Type 2 Diabetes Management Program Physician Pharmacist Collaborative Drug Therapy Management Protocol
 Brigham and Women s Hospital Type 2 Diabetes Management Program Physician Pharmacist Collaborative Drug Therapy Management Protocol *Please note that this guideline may not be appropriate for all patients
Brigham and Women s Hospital Type 2 Diabetes Management Program Physician Pharmacist Collaborative Drug Therapy Management Protocol *Please note that this guideline may not be appropriate for all patients
Nancy Merriman, Executive Director Alaska Primary Care Association
 Nancy Merriman, Executive Director Alaska Primary Care Association nancy@alaskapa.org 907-929-2725 1. Must serve a high needs area (designated Medically Underserved Area or Population) 2. Comprehensive
Nancy Merriman, Executive Director Alaska Primary Care Association nancy@alaskapa.org 907-929-2725 1. Must serve a high needs area (designated Medically Underserved Area or Population) 2. Comprehensive
Diabetes Education and Diabetes Prevention Education Needs Assessment, Las Vegas, Nevada
 Diabetes Education and Diabetes Prevention Education Needs Assessment, Las Vegas, Nevada Julie Plasencia, MS, RD University of Nevada Cooperative Extension 2009 1 Table of Contents Introduction... 3 Objective...
Diabetes Education and Diabetes Prevention Education Needs Assessment, Las Vegas, Nevada Julie Plasencia, MS, RD University of Nevada Cooperative Extension 2009 1 Table of Contents Introduction... 3 Objective...
Impact and Value of Pharmacist Interventions in Different Settings
 Impact and Value of Pharmacist Interventions in Different Settings Cheryl Pegus MD MPH Chief Medical Officer Walgreen Co. March 15, 2011 Chronic Care Management Today: The Challenge Less Effective Lower
Impact and Value of Pharmacist Interventions in Different Settings Cheryl Pegus MD MPH Chief Medical Officer Walgreen Co. March 15, 2011 Chronic Care Management Today: The Challenge Less Effective Lower
A Call to Action: Addressing Diabetes Medication Safety
 A Call to Action: Addressing Diabetes Medication Safety Evan M. Klass, M.D., F.A.C.P. Senior Associate Dean, Statewide Initiatives Reducing ED visits for insulin induced hypoglycemia is a Healthy People
A Call to Action: Addressing Diabetes Medication Safety Evan M. Klass, M.D., F.A.C.P. Senior Associate Dean, Statewide Initiatives Reducing ED visits for insulin induced hypoglycemia is a Healthy People
Asian Journal of Pharmaceutical and Clinical Research Vol. 3, Issue 3, 2010 ISSN
 Asian Journal of Pharmaceutical and Clinical Research Vol. 3, Issue 3, 2010 ISSN - 0974-2441 Research Article INFLUENCE OF STRUCTURED PATIENT EDUCATION ON THERAPEUTIC OUTCOMES IN DIABETES AND HYPERTENSIVE
Asian Journal of Pharmaceutical and Clinical Research Vol. 3, Issue 3, 2010 ISSN - 0974-2441 Research Article INFLUENCE OF STRUCTURED PATIENT EDUCATION ON THERAPEUTIC OUTCOMES IN DIABETES AND HYPERTENSIVE
Page # 1. Objectives. History of Clinical Trials. Developing New Therapies Clinical Studies and Trials. FDA Classification of Clinical Studies/Trials
 Developing New Therapies Clinical Studies and Trials Richard C. Eastman M.D. Objectives Discuss how new treatments are studied in humans. Explain how the rights of human volunteers are safeguarded. Discuss
Developing New Therapies Clinical Studies and Trials Richard C. Eastman M.D. Objectives Discuss how new treatments are studied in humans. Explain how the rights of human volunteers are safeguarded. Discuss
The Burden of Cardiovascular Disease in North Carolina June 2009 Update
 The Burden of Cardiovascular Disease in North Carolina June 2009 Update Sara L. Huston, Ph.D. Heart Disease & Stroke Prevention Branch Chronic Disease & Injury Section Division of Public Health North Carolina
The Burden of Cardiovascular Disease in North Carolina June 2009 Update Sara L. Huston, Ph.D. Heart Disease & Stroke Prevention Branch Chronic Disease & Injury Section Division of Public Health North Carolina
Zhao Y Y et al. Ann Intern Med 2012;156:
 Zhao Y Y et al. Ann Intern Med 2012;156:560-569 Introduction Fibrates are commonly prescribed to treat dyslipidemia An increase in serum creatinine level after use has been observed in randomized, placebocontrolled
Zhao Y Y et al. Ann Intern Med 2012;156:560-569 Introduction Fibrates are commonly prescribed to treat dyslipidemia An increase in serum creatinine level after use has been observed in randomized, placebocontrolled
Continuous Glucose Monitoring System
 Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2016 Section: DME Place(s)
Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2016 Section: DME Place(s)
Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly?
 Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly? Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Division of Nephrology, Department of Medicine University
Home Hemodialysis or Transplantation of the Treatment of Choice for Elderly? Miklos Z Molnar, MD, PhD, FEBTM, FERA, FASN Associate Professor of Medicine Division of Nephrology, Department of Medicine University
Teleretinal Screening for Diabetic Retinopathy: A Novel Approach to Reduce Screening Burden on the Healthcare Systems within Central Texas
 Teleretinal Screening for Diabetic Retinopathy: A Novel Approach to Reduce Screening Burden on the Healthcare Systems within Central Texas Robert W. Wong, MD; Maria Benson, BS; Jose A. Martinez, MD; Mark
Teleretinal Screening for Diabetic Retinopathy: A Novel Approach to Reduce Screening Burden on the Healthcare Systems within Central Texas Robert W. Wong, MD; Maria Benson, BS; Jose A. Martinez, MD; Mark
Based on Medicare FFS Beneficiaries Assigned July 1, 2011 December 31, 2011
 July 2012 Multi-payer Advanced Primary Care Practice (MAPCP) Demonstration Medical Home Feedback Report Based on Medicare FFS Beneficiaries Assigned July 1, 2011 December 31, 2011 Practice Number Practice
July 2012 Multi-payer Advanced Primary Care Practice (MAPCP) Demonstration Medical Home Feedback Report Based on Medicare FFS Beneficiaries Assigned July 1, 2011 December 31, 2011 Practice Number Practice
Diabetes is a chronic disease
 N.C. Diabetes Education Recognition Program: ADA Recognition for a Combined Program at Local Health Departments and Community Health Centers in North Carolina Joanne Rinker, MS, RD, CDE, LDN, and Marti
N.C. Diabetes Education Recognition Program: ADA Recognition for a Combined Program at Local Health Departments and Community Health Centers in North Carolina Joanne Rinker, MS, RD, CDE, LDN, and Marti
ATRIAL FIBRILLATION AND ETHNICITY. Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE)
 ATRIAL FIBRILLATION AND ETHNICITY Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE) Atrial fibrillation (AF) and ethnicity The known The unknown The paradox Why
ATRIAL FIBRILLATION AND ETHNICITY Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE) Atrial fibrillation (AF) and ethnicity The known The unknown The paradox Why
High-quality diabetes care can
 Development and Evolution of a Primary Care Based Diabetes Disease Management Program Robb Malone, PharmD, CDE, CPP; Betsy Bryant Shilliday, PharmD, CDE, CPP; Timothy J. Ives, PharmD, MPH; and Michael
Development and Evolution of a Primary Care Based Diabetes Disease Management Program Robb Malone, PharmD, CDE, CPP; Betsy Bryant Shilliday, PharmD, CDE, CPP; Timothy J. Ives, PharmD, MPH; and Michael
Disclosures. How to Become Even Better Allies 10/18/2016 LANGUAGE AND LITERACY THE PAS DE DEUX
 Disclosures LANGUAGE AND LITERACY THE PAS DE DEUX Alicia Fernandez, MD Professor of Medicine University of California, San Francisco Zuckerberg San Francisco General NIH-NIDDK; NIMHD; NHLBI; Arnold P.
Disclosures LANGUAGE AND LITERACY THE PAS DE DEUX Alicia Fernandez, MD Professor of Medicine University of California, San Francisco Zuckerberg San Francisco General NIH-NIDDK; NIMHD; NHLBI; Arnold P.
HEALTH DISPARITIES AMONG ADULTS IN OHIO
 OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio HEALTH DISPARITIES AMONG ADULTS IN OHIO Amy K. Ferketich, PhD 1 Ling Wang, MPH 1 Timothy R. Sahr, MPH, MA 2 1The Ohio State University
OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio HEALTH DISPARITIES AMONG ADULTS IN OHIO Amy K. Ferketich, PhD 1 Ling Wang, MPH 1 Timothy R. Sahr, MPH, MA 2 1The Ohio State University
Identifying Geographic & Socioeconomic Disparities in Access to Care for Pediatric Cancer Patients in Texas
 Identifying Geographic & Socioeconomic Disparities in Access to Care for Pediatric Cancer Patients in Texas Mary T. Austin, MD, MPH Assistant Professor, Pediatric Surgery University of Texas Health Science
Identifying Geographic & Socioeconomic Disparities in Access to Care for Pediatric Cancer Patients in Texas Mary T. Austin, MD, MPH Assistant Professor, Pediatric Surgery University of Texas Health Science
CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO
 OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio CHRONIC DISEASE PREVALENCE AMONG ADULTS IN OHIO Amy Ferketich, PhD Ling Wang, MPH The Ohio State University College of Public Health
SCIENTIFIC STUDY REPORT
 PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
Diabetes Champions: Culture Change Through Education. In Brief
 In Brief This article describes a diabetes champion program in its fifth year of operation. This educational intervention was designed to increase direct diabetes patient education and has grown into a
In Brief This article describes a diabetes champion program in its fifth year of operation. This educational intervention was designed to increase direct diabetes patient education and has grown into a
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach
 Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Chapman University Digital Commons. Chapman University. Michael S. Kelly Chapman University,
 Chapman University Chapman University Digital Commons Pharmacy Faculty Articles and Research School of Pharmacy 12-30-2016 Assessment of Achieved Systolic Blood Pressure in Newly Treated Hypertensive Patients
Chapman University Chapman University Digital Commons Pharmacy Faculty Articles and Research School of Pharmacy 12-30-2016 Assessment of Achieved Systolic Blood Pressure in Newly Treated Hypertensive Patients
Diabetic Equipment and Supplies
 Diabetic Equipment and Supplies Chapter.1 Enrollment..................................................................... -2.2 Benefits, Limitations, and Authorization Requirements...........................
Diabetic Equipment and Supplies Chapter.1 Enrollment..................................................................... -2.2 Benefits, Limitations, and Authorization Requirements...........................
Impact of Poor Healthcare Services
 Competency 3 Impact of Poor Healthcare Services Updated June 2014 Presented by: Lewis Foxhall, MD VP for Health Policy Professor, Clinical Cancer Prevention UT MD Anderson Cancer Center Competency 3 Objectives
Competency 3 Impact of Poor Healthcare Services Updated June 2014 Presented by: Lewis Foxhall, MD VP for Health Policy Professor, Clinical Cancer Prevention UT MD Anderson Cancer Center Competency 3 Objectives
Diabetes in the Latino/Hispanic Population The case for education and outreach
 Diabetes in the Latino/Hispanic Population The case for education and outreach Enrique Caballero MD Endocrinologist/Clinical Investigator Director of the Latino Diabetes Initiative Director, International
Diabetes in the Latino/Hispanic Population The case for education and outreach Enrique Caballero MD Endocrinologist/Clinical Investigator Director of the Latino Diabetes Initiative Director, International
Diabetic Foot Ulcers Data Points #1
 Prevalence of diabetes, diabetic foot ulcer, and lower extremity amputation among Medicare beneficiaries, 2006 to 2008 Diabetic Foot Ulcers Data Points #1 More than 16 million people in the United States
Prevalence of diabetes, diabetic foot ulcer, and lower extremity amputation among Medicare beneficiaries, 2006 to 2008 Diabetic Foot Ulcers Data Points #1 More than 16 million people in the United States
An estimated 20.8 million Americans 7% of the population
 Provider Organization Performance Assessment Utilizing Diabetes Physician Recognition Program Bruce Wall, MD, MMM; Evelyn Chiao, PharmD; Craig A. Plauschinat, PharmD, MPH; Paul A. Miner, PharmD; James
Provider Organization Performance Assessment Utilizing Diabetes Physician Recognition Program Bruce Wall, MD, MMM; Evelyn Chiao, PharmD; Craig A. Plauschinat, PharmD, MPH; Paul A. Miner, PharmD; James
Diabetes is an illness that affects an estimated. Outcomes and Medication Use in a Longitudinal Cohort of Type 2 Diabetes Patients, 2006 to 2012
 Original Research Outcomes and Medication Use in a Longitudinal Cohort of Type 2 Diabetes Patients, 2006 to 2012 Julienne K. Kirk, PharmD, Stephen W. Davis, MA, Kathryn Lawrence, MD, Carol A. Hildebrandt,
Original Research Outcomes and Medication Use in a Longitudinal Cohort of Type 2 Diabetes Patients, 2006 to 2012 Julienne K. Kirk, PharmD, Stephen W. Davis, MA, Kathryn Lawrence, MD, Carol A. Hildebrandt,
Continuous Glucose Monitoring System
 Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017 Section: DME Place(s)
Continuous Glucose Monitoring System Policy Number: Original Effective Date: MM.02.003 03/13/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017 Section: DME Place(s)
Contractor Name: Novitas Solutions, Inc. Contractor Number: Contractor Type: MAC B. LCD ID Number: L34834 Status: A-Approved
 LCD for Blood Glucose Monitoring in a Skilled Nursing Facility (SNF) (L34834) Contractor Name: Novitas Solutions, Inc. Contractor Number: 12502 Contractor Type: MAC B LCD ID Number: L34834 Status: A-Approved
LCD for Blood Glucose Monitoring in a Skilled Nursing Facility (SNF) (L34834) Contractor Name: Novitas Solutions, Inc. Contractor Number: 12502 Contractor Type: MAC B LCD ID Number: L34834 Status: A-Approved
Improved IPGM: Demonstrating the Value to both Patients and Hospitals
 Improved IPGM: Demonstrating the Value to both Patients and Hospitals Osama Hamdy, MD, PhD, FACE Medical Director, Inpatient Diabetes Program Joslin Diabetes Center Harvard Medical School, Boston, MA Cost
Improved IPGM: Demonstrating the Value to both Patients and Hospitals Osama Hamdy, MD, PhD, FACE Medical Director, Inpatient Diabetes Program Joslin Diabetes Center Harvard Medical School, Boston, MA Cost
Diabetes Mellitus and the Dental Healthcare Professional
 Diabetes Mellitus and the Dental Healthcare Professional Jerry A. Brown DMD, CDE University of South Florida Department of Internal Medicine jabrown7@health.usf.edu Learning Objectives Diabetes- The Disease
Diabetes Mellitus and the Dental Healthcare Professional Jerry A. Brown DMD, CDE University of South Florida Department of Internal Medicine jabrown7@health.usf.edu Learning Objectives Diabetes- The Disease
In each hospital-year, we calculated a 30-day unplanned. readmission rate among patients who survived at least 30 days
 Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Erectile Dysfunction as a Motivational Tool for Health Behavior Change in Men with Diabetes
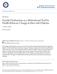 Brigham Young University BYU ScholarsArchive All Student Publications 2014-06-24 Erectile Dysfunction as a Motivational Tool for Health Behavior Change in Men with Diabetes Camille W. Allred Donna Freeborn
Brigham Young University BYU ScholarsArchive All Student Publications 2014-06-24 Erectile Dysfunction as a Motivational Tool for Health Behavior Change in Men with Diabetes Camille W. Allred Donna Freeborn
Reducing COPD Exacerbation Readmissions in a Community-Based Teaching Hospital
 Reducing COPD Exacerbation Readmissions in a Community-Based Teaching Hospital Dawn Waddell, PharmD, BCPS Clinical Pharmacy Manager Lisa Kingdon, PharmD, BCPS Clinical Pharmacy Specialist Dawn Waddell
Reducing COPD Exacerbation Readmissions in a Community-Based Teaching Hospital Dawn Waddell, PharmD, BCPS Clinical Pharmacy Manager Lisa Kingdon, PharmD, BCPS Clinical Pharmacy Specialist Dawn Waddell
