More than 1.8 million New York State residents have diabetes, 1
|
|
|
- Blanche Lyons
- 6 years ago
- Views:
Transcription
1 September 1 New York State Health Foundation s DIABETES Policy Center DIABETES: A HIDDEN HEALTH CARE COST DRIVER IN NEW YORK An Analysis of Health Care Utilization and Trends of Patients with Diabetes in New York State Andrea Mathis, MPH, CPH; Yasmine Legendre, MPA; Wanda Montalvo, RN, MSN, ANP; and Deborah Zahn, MPH More than 1.8 million New York State residents have diabetes, 1 and diabetes prevalence continues to rise (see Figure 1). Another 3.7 million to 4.2 million New Yorkers are estimated to have pre-diabetes. 2 The total cost for New Yorkers with diabetes was almost $12.9 billion in 6. This includes excess medical costs of approximately $8.7 billion and lost productivity costs of $4.2 billion. 3 On average, the cost of health care for a person with diabetes is more than five times as much as the cost for those without diabetes $13, vs. $2,5. 4 In response, the New York State Health Foundation (NYSHealth) launched a $35 million, five-year Diabetes Campaign in 8 to reverse the diabetes epidemic. As part of this initiative, the Campaign is working with Healthcare Association of New York State (HANYS) to improve diabetes care and outcomes. Figure 1. Estimated Adult Diabetes Prevalence in New York State, % 8.2% 8.4% % 7.4% 7.5% 7.6% Source: New York State specific BRFSS estimates, CDC million New Yorkers have been diagnosed with diabetes and approximately 76, more have diabetes but do not know it. 2 Cowie C., et al. (8). Full accounting of diabetes and pre-diabetes in the U.S. population in and 5 6. Diabetes Care, 32(2): American Diabetes Association, The Estimated Prevalence and Cost of Diabetes in New York, American Diabetes Association Web site, State%29, accessed July 7, 1. 4 Hogan P., Dall T, Nikolov P. (3). Economic costs of diabetes in the U.S. in 2. Diabetes Care, 26(3): , cited in diabqguideref.htm#hogan3. n 1 n
2 In order to better understand how diabetes contributes to health care costs in New York State, HANYS analyzed New York health care utilization by patients diagnosed with diabetes. Using 8 Statewide Planning and Research Cooperative System (SPARCS) data, 7 Medicare Limited Data Set Standard Analytic Files 5% version, and the Behavioral Health Risk Factor Surveillance System (BRFSS), HANYS revealed several important findings that illustrate the role that diabetes is playing in driving costly health care utilization. EMERGENCY DEPARTMENT UTILIZATION Finding: More than half of emergency department (ED) visits for people with uncontrolled diabetes resulted in a hospital admission compared to % for all others. Analysis of the 7 and 8 SPARCS data revealed that more than 5% of the visits to New York EDs by those presenting with a primary diagnosis of diabetes 5 were admitted to the hospital. This is compared to % of people without a primary diagnosis of diabetes (see Figure 2). Figure 2. Emergency Department Utilization with a Primary Diagnosis of Diabetes, Primary Diabetes All Other % of Total Patients Treated in the ED %.5% 51.9% 19.8% 7 Source: SPARCS, 7 8. Admitted as inpatient 8 Finding: More than 6% of the visits to the ED by patients with diabetes regardless of the reason for the visit resulted in an admission to the hospital compared to 17% of visits by people without diabetes. More than 6% of the visits to the ED by patients with diabetes resulted in admission to the hospital. This includes those with the primary and secondary diagnoses of diabetes. This is a striking contrast to the 17% of people without diabetes who are admitted as an inpatient following a visit to an ED (see Figure 3). 5 Primary diagnosis of diabetes mellitus was identified using International Classification for Diseases, 9th Revision Clinical Modification (ICD-9-CM) Codes 25 and n 2 n
3 Figure 3. Emergency Department Utilization with a Primary or Secondary Diagnosis of Diabetes, All Diabetes % of Total Patients Treated in the ED % 17.3% All Other 61.8% 16.7% Source: SPARCS, Admitted as inpatient 8 INPATIENT ADMISSIONS Finding: The percentage of hospitalizations for diabetes in New York has steadily increased, rising by nearly 3% from to 8. Although the number of inpatient admissions in New York State is rising each year, the percentage of those visits that occur by patients with diabetes is rising at a larger rate. In 8, 18.7% of total admissions were patients with a primary or secondary diagnosis of diabetes. 6 This shows a steady increase from 2 where only 14.4% of total admissions were patients with diabetes (see Figure 4). Figure 4. Total Inpatient Admissions for Patients with Diabetes as a Percentage of Total Inpatient Admissions in New York State, % 15.% 15.7% 16.4% 17.% 17.5% 17.9% 18.4% 18.7% Source: SPARCS, 8. 6 Diabetes admissions were identified if they had a primary or secondary diagnosis of diabetes mellitus. Primary or secondary diagnosis of diabetes mellitus was defined using International Classification for Diseases, 9th Revision Clinical Modification (ICD-9-CM) Codes 25 and n 3 n
4 Finding: Diabetes accounts for 84% of all admissions growth from 8. Further analysis of admissions data reveals that 84% of all admissions growth is attributable to patients with diabetes. Total inpatient admissions have increased by nearly 163, and admissions for patients with either a primary or secondary diagnosis of diabetes increased by nearly 137, since. INPATIENT READMISSIONS Finding: Overall, patients with diabetes are 1.6 times more likely than patients without diabetes to be readmitted to a hospital within 3 days. Patients with diabetes have an overall readmission rate of.6%, which is 1.6 times the rate of patients without diabetes (12.5%.) 7 When looking at the most common reasons for initial admissions, patients with diabetes are more likely to be readmitted regardless of the reason for their initial admission (see Figure 5). Figure 5. Readmission Rates of the Top 1 Admission Diagnosis-Related Groups (DRGs), % 28.8% Patients with Diabetes Patients without Diabetes Readmission % Rate % 24.9% 16.4% 18.1% 19.% 1.5%.% 11.9% 23.% 15.8% 19.6% 12.8% 22.3% 13.5% 14.1% 8.3% 16.% 11.6% 5 Heart failure & shock Alcohol/ drug abuse or dependence w/o rehabilitation therapy Chronic obstructive pulmonary disease Esophagitis, gastroent & misc digest disorders Simple pneumonia & pleurisy Septicemia w/ MV 96+ hours Cardiac arrhythmia & conduction disorders Nutritional & misc metabolic disorders Chest pain Perc cardiovasc proc w/ drug-eluting stent Source: SPARCS, Dec 1, 7 Dec 31, 8. Excludes rehabilitation, neonates, obstetrics, and transfers. Finding: Readmission rates are higher for patients with diabetes across all payers. The readmission rates for patients with diabetes are higher than rates for patients without diabetes regardless of payer 8 (see Figure 6). Government beneficiaries have the highest rates with rates for Medicaid fee-for-service patients at 25.%, Medicare fee-for-service at 22.8%, Medicare managed care at.9%, and Medicaid managed care at 19.3%. Commercial payers have the lowest readmission rate (15.1%); however, that rate is still higher than the readmission rate for patients without diabetes (12.5%). 7 Readmission rates were determined using 8 SPARCS data and include all acute inpatient admissions in New York State hospitals. If a patient is admitted to an acute care hospital within 3 days of being discharged from an acute care hospital, it is counted as a readmission. Readmissions can occur in the same facility or a different facility within New York State. The readmission analysis produced 3-day, unadjusted, all-cause readmission rates. All-cause rates mean that the second admission may or may not be clinically related to the initial admission. 8 Payer was identified using the primary payer reporting on the initial admission. In the case of an initial admission involving a transfer, the primary payer recorded by the receiving institution was used. n 4 n
5 Figure 6. 3-Day Readmission Rates of Patients with Diabetes by Payer, % 22.8%.9% 19.3% Readmission % Rate % 5 Medicaid FFS Medicare FFS Medicare HMO Medicaid HMO All Other Commerical Source: SPARCS, Dec 1, 7 Dec 31, 8. Excludes rehabilitation, neonates, obstetrics, and transfers. ROUTINE DIABETES CARE Finding: Only an estimated 39% of the patients in New York s Medicare population are receiving recommended routine testing and evidence-based practices, and 1% are not receiving any of the recommended routine testing and evidence-based practices. The utilization findings are not surprising given the suboptimal care many patients with diabetes receive. A national study indicated that people with diabetes receive only 45% of recommended clinical care based on national guidelines for screening, diagnosis, treatment, and follow-up. 9 HANYS analysis 1 of sample data of more than 33, Medicare patients showed that in New York, patients with Medicare were not receiving all of the screening tests that are critical to managing diabetes and preventing complications. In 7, although 74.4% had at least one A1C test, 74.8% had at least one lipid profile test, and 54.8% had at least one eye exam, most were not receiving all the screening tests. (See Figure 7.) Only 39% received all of the recommended tests, and 1% did not receive any tests. Figure 7. Percentage of Patients with Diabetes Receiving Routine Diabetes Care in a Professional or Outpatient Setting, 7 Source: 7 Medicare Limited Data Set Standard Analytic Files 5% version. 8,346 (25.%) Lipid Profile 1,643 (4.9%) A1C Test 1,746 (5.2%) 12,969 (38.9%) 1,955 (5.9%) 1,719 (5.%) Eye Exam 1,622 (4.9%) 9 McGlynn EA., et al. (3). The quality of health care delivered to adults in the United States. The New England Journal of Medicine 348(26): HANYS identified the utilization of routine care components on the Medicare Limited Data Set Standard Analytic Files 5% version using common procedural terminology (CPT) codes according to the CMS National Measurement Specifications Diabetes Quality of Care Measures, 6. n 5 n
6 DISCUSSION The data presented in this brief highlight the urgent need to address diabetes as an important and often hidden driver of increasing health care utilization. The data show that patients with diabetes incur higher rates of admission to hospital EDs and higher rates of 3-day readmissions, regardless of primary diagnosis. The data also confirm that patients with diabetes are not getting the preventative care they need. There is ample evidence about what works to prevent diabetes and its complications, yet there is not a simple solution to reduce potentially avoidable readmissions, hospitalizations, and ED visits related to diabetes, or to ensure that New Yorkers with diabetes get the best care and achieve the best outcomes. Addressing this issue requires comprehensive solutions with contributions from multiple stakeholders. The current health care landscape offers numerous opportunities: the passage of Federal health reform; the expanded body of evidence regarding clinical practice; a shift toward more comprehensive care management payment models; the implementation of new models of health care delivery, such as the Patient-Centered Medical Home; the availability of Federal incentives for achieving meaningful use through health information technology; and the advent of efforts to create bundled payment programs and Accountable Care Organizations. These forces have increased the focus on the management of chronic conditions, as well as outcomes-based payment incentives and other payment reforms. With this new focus come opportunities to implement solutions that better measure, monitor, manage, and pay for diabetes care and better outcomes. These opportunities have the potential to lead New York away from a historically misaligned payment and delivery system, one that has been characterized by paying for volume instead of value, incentivizing suboptimal care, and merely shifting escalating costs instead of containing them. Hospitals are only one player in the care continuum, and thus cannot achieve significant improvements in these outcomes on their own. Success depends on the availability and coordination of adequate primary care services, and the engagement of patients through the provision of diabetes self-management education (DSME). Moreover, policy and payment systems must be aligned across the system to enable providers to smoothly integrate transitions in care and services. RECOMMENDATIONS Based on this preliminary assessment in New York, we offer the following recommendations for the health care payment and delivery system: Health Care Payment Provide Financial Incentives to Providers Well designed financial incentive programs are critical to rewarding physicians and practices for implementing successful patient care delivery systems and improving patient outcomes. Many payers are engaged in efforts to transform the delivery system, and some not all are providing financial incentives to providers for improving their diabetes outcomes. However, New York needs a critical mass to drive broader change. The more payers providing incentives for diabetes standards of care and the more alignment among programs, the clearer the validation signal will be to providers about what matters most in diabetes care and outcomes, and the greater providers motivation will be to implement practices that improve outcomes into their delivery of care. Both payers and the system as a whole will reap the benefits of doing this through reduced readmissions, hospitalizations, and ED visits. Emphasize Patient Outcomes in Financial Incentives Programs Of the incentive programs that currently exist, many emphasize clinical process or care delivery process measures to assess quality and to trigger incentive payments. These measures assess whether diabetes-related screenings, such as blood pressure screenings or eye exams, are administered to patients. Although process measures are important, in and of themselves they do not guarantee that patient outcomes will improve. For that reason, we recommend including intermediate outcome measures for diabetes, particularly those that are most tightly linked to patient risk reduction in their incentive programs. These intermediate outcome measures also known as the diabetes ABCs are the poor and superior control measures for Hemoglobin A1c, Blood pressure, and LDL Cholesterol (see sidebar). These measures, as well as four critical process measures, can be demonstrated and verified by achieving recognition through the National Committee on Quality Assurance s (NCQA s) Diabetes Recognition Program n 6 n
7 or Bridges to Excellence s (BTE s) Diabetes Care Recognition Program. Working with HANYS and other statewide partners, the NYSHealth Diabetes Campaign is supporting efforts to encourage and assist 3, primary care providers to improve their care and obtain recognition under these programs. We recommend that payers incorporate these programs to trigger rewards or incentive payments. Reimburse for What Produces Positive Patient Outcomes Improvements in diabetes outcomes require adequate reimbursement to create and sustain the health care infrastructure and systems of care that produce positive patient outcomes. This includes reimbursement for DSME and training, team-based care, and care coordination. Health Care Delivery Ensure the Adoption of, and Adherence to, Evidence-Based Clinical Practice Guidelines Adoption of, and adherence to, diabetes clinical practice guidelines is critical to improve diabetes outcomes in both inpatient and outpatient settings. This requires building systems to ensure that patients with diabetes get the right care at the right time and in the right place. It also requires ongoing monitoring to ensure that the systems and patient outcomes are sustained over time. Many hospitals and their outpatient clinics employ a variety of strategies to monitor their diabetes outcomes, including quality dashboards and individual provider and practice reports. Recognition under the NCQA and BTE programs also enables hospitals and providers to assess, improve, and monitor their diabetes outcomes. DIABETES MEASURES Hemoglobin A1c > 9.%* Hemoglobin A1c < 8.% Hemoglobin A1c < 7.%** Blood pressure 14/9 mm Hg* Blood pressure < 13/8 mm Hg LDL cholesterol 13 mg/dl* LDL cholesterol < 1 mg/dl (dl) Eye examination Foot examination Nephropathy assessment Smoking status and cessation advice or treatment * Denotes poor control ** When appropriate Support Diabetes Self-Management Education Evidence shows that DSME can improve outcomes for people with diabetes by helping them manage their disease and prevent complications. Hospitals can develop and support DSME programs, certified diabetes educators, 11 diabetes centers, 12 and community health workers. Hospitals also might consider ways to expand the roles of staff, such as nurses or medical assistants, to better support DSME. 11 As of January 1, 9, New York State Medicaid began reimbursing for select CDE services in some clinical settings. Medicare also reimburses for similar CDE services. 12 Diabetes centers that are recognized by the American Diabetes Association or accredited by the American Association of Diabetes Educators are eligible for Medicare reimbursement for some services. Acknowledgements James R. Knickman, President and CEO, NYSHealth Jacqueline Martinez, Senior Program Director, NYSHealth Margaret L. Figley, Communications Officer, NYSHealth Kathy Ciccone, Executive Vice President, Quality Institute, HANYS Nancy Landor, Senior Director, Strategic Quality Initiatives, HANYS Kelly O Connor, Manager, Quality Initiatives, HANYS Kate Lichten, Manager, Quality Initiatives, HANYS CONTACT Nancy Landor, HANYS Quality Institute at (518) or nlandor@hanys.org or to join the Campaign visit the website n 7 n
MANAGING DIABETES CARE: Moving an Underlying Chronic Condition to the Forefront
 December 2011 A DIABETES CAMPAIGN COLLABORATION MANAGING DIABETES CARE: Moving an Underlying Chronic Condition to the Forefront Nancy Landor, R.N., M.S., C.P.H.Q. a ; Amy Jones, M.P.H., C.H.E.S. a ; and
December 2011 A DIABETES CAMPAIGN COLLABORATION MANAGING DIABETES CARE: Moving an Underlying Chronic Condition to the Forefront Nancy Landor, R.N., M.S., C.P.H.Q. a ; Amy Jones, M.P.H., C.H.E.S. a ; and
Kansas Care Coordination Quarterly Report October 2018
 Kansas Care Coordination Quarterly Report October 2018 Background Communities across the Great Plains Quality Innovation Network (QIN) region are collaborating to improve care coordination and medication
Kansas Care Coordination Quarterly Report October 2018 Background Communities across the Great Plains Quality Innovation Network (QIN) region are collaborating to improve care coordination and medication
HEALTHCARE REFORM. September 2012
 HEALTHCARE REFORM Accountable Care Organizations: ACOs 101 September 2012 The enclosed slides are intended to provide you with a general overview of accountable care organizations (ACOs), created within
HEALTHCARE REFORM Accountable Care Organizations: ACOs 101 September 2012 The enclosed slides are intended to provide you with a general overview of accountable care organizations (ACOs), created within
The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis
 Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Achieving Quality and Value in Chronic Care Management
 The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
Key Findings. Mortality Rates
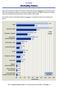 Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from federal fiscal year to federal fiscal year in 12 of the 15 conditions reported. The largest decrease
Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from federal fiscal year to federal fiscal year in 12 of the 15 conditions reported. The largest decrease
Key Findings. Mortality Rates
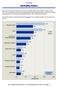 Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Bridges to Excellence: Recognizing High-Quality Care. Meredith B. Rosenthal, Ph.D. October 19, 2008
 Bridges to Excellence: Recognizing High-Quality Care Meredith B. Rosenthal, Ph.D. October 19, 2008 1 Acknowledgements My coauthors: Francois DeBrantes, Anna Sinaiko, Matt Frankel, Russell Robbins, Sara
Bridges to Excellence: Recognizing High-Quality Care Meredith B. Rosenthal, Ph.D. October 19, 2008 1 Acknowledgements My coauthors: Francois DeBrantes, Anna Sinaiko, Matt Frankel, Russell Robbins, Sara
Lowering epilepsy-related treatment costs in the era of patient choice and value-based care
 Lowering epilepsy-related treatment costs in the era of patient choice and value-based care In-home EEG offers cost-effective, reliable alternative to traditional diagnostic services 01 Introduction One
Lowering epilepsy-related treatment costs in the era of patient choice and value-based care In-home EEG offers cost-effective, reliable alternative to traditional diagnostic services 01 Introduction One
Commercial Bundling. National Bundled Payment Summit Integrated Healthcare Association. George Washington University, Washington, DC.
 Commercial Bundling National Bundled Payment Summit Integrated Healthcare Association George Washington University, Washington, DC June 12, 2012 Copyright 2012. This presentation as a whole and all of
Commercial Bundling National Bundled Payment Summit Integrated Healthcare Association George Washington University, Washington, DC June 12, 2012 Copyright 2012. This presentation as a whole and all of
Objectives. Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers
 Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010
 Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Senior Leaders and the Strategic Alignment of Community Benefit Programs: The Example of Diabetes
 Senior Leaders and the Strategic Alignment of Community Benefit Programs: The Example of Diabetes Posted: February 17, 2009 By Patsy Matheny, Community Benefit Consultant. Sugar Grove, Ohio Moving community
Senior Leaders and the Strategic Alignment of Community Benefit Programs: The Example of Diabetes Posted: February 17, 2009 By Patsy Matheny, Community Benefit Consultant. Sugar Grove, Ohio Moving community
Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap
 Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap Avalere Health An Inovalon Company November 16, 2017 In Partnership with GSK Agenda 1 2 3 4 5 Welcome & Introductions Overview:
Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap Avalere Health An Inovalon Company November 16, 2017 In Partnership with GSK Agenda 1 2 3 4 5 Welcome & Introductions Overview:
Value Based Pay for Performance Results & Highlights Measurement Year September 2017
 Value Based Pay for Performance Results & Highlights Measurement Year 2016 September 2017 IHA s Value Based Pay for Performance (VBP4P) ~200 Medical Groups & IPAs 9 Health Plans Common Measurement Public
Value Based Pay for Performance Results & Highlights Measurement Year 2016 September 2017 IHA s Value Based Pay for Performance (VBP4P) ~200 Medical Groups & IPAs 9 Health Plans Common Measurement Public
REVIEW AND FREQUENTLY ASKED QUESTIONS (FAQ) 8/5/2015. Outline. Navigating the DSMT Reimbursement Maze in Todays Changing Environment
 Patty Telgener RN, MBA, CPC VP of Reimbursement Emerson Consultants Navigating the DSMT Reimbursement Maze in Todays Changing Environment Patty Telgener, RN, MBA, CPC VP of Reimbursement Emerson Consultants
Patty Telgener RN, MBA, CPC VP of Reimbursement Emerson Consultants Navigating the DSMT Reimbursement Maze in Todays Changing Environment Patty Telgener, RN, MBA, CPC VP of Reimbursement Emerson Consultants
From Channeling to GRACE: Approaching Reduction in Readmissions and Adverse Drug Events
 From Channeling to GRACE: Approaching Reduction in Readmissions and Adverse Drug Events Michael Wasserman, MD, CMD Executive Director, Care Continuum Health Services Advisory Group September 15, 2016 Quality
From Channeling to GRACE: Approaching Reduction in Readmissions and Adverse Drug Events Michael Wasserman, MD, CMD Executive Director, Care Continuum Health Services Advisory Group September 15, 2016 Quality
COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS
 COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS Community Oncology Alliance 2 Physician Ratings Consumers want information about quality Have become used to
COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS Community Oncology Alliance 2 Physician Ratings Consumers want information about quality Have become used to
OPIOID USE DISORDER CENTERS OF EXCELLENCE APPLICATION GENERAL INFORMATION
 OPIOID USE DISORDER CENTERS OF EXCELLENCE APPLICATION GENERAL INFORMATION The Department of Human Services (DHS) is implementing 50 opioid use disorder (OUD) Health Homes or Centers of Excellence (COE)
OPIOID USE DISORDER CENTERS OF EXCELLENCE APPLICATION GENERAL INFORMATION The Department of Human Services (DHS) is implementing 50 opioid use disorder (OUD) Health Homes or Centers of Excellence (COE)
HEART FAILURE QUALITY IMPROVEMENT. American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement
 HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Improving Quality of Care for Medicare Patients: Accountable Care Organizations
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
Battling Opioid Addiction: Public Policy and Healthcare Strategies for an Epidemic
 Battling Opioid Addiction: Public Policy and Healthcare Strategies for an Epidemic Speakers: Margarita Pereyda, M.D., Principal, Moderator: Carl Mercurio, Information Services September 29, 2015 HealthManagement.com
Battling Opioid Addiction: Public Policy and Healthcare Strategies for an Epidemic Speakers: Margarita Pereyda, M.D., Principal, Moderator: Carl Mercurio, Information Services September 29, 2015 HealthManagement.com
CHI Franciscan. Matt Levi Director Virtual Health Services. March 31, 2015
 CHI Franciscan Matt Levi Director Virtual Health Services March 31, 2015 Reflection / 2 Agenda Introduction and background Matt Levi Director of Franciscan Health System Virtual Health Katie Farrell Manager
CHI Franciscan Matt Levi Director Virtual Health Services March 31, 2015 Reflection / 2 Agenda Introduction and background Matt Levi Director of Franciscan Health System Virtual Health Katie Farrell Manager
Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania
 Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania Keith T. Kanel, MD, MHCM, FACP Colleen Vrbin Susan Elster, PhD Jason Kunzman, MBA Michelle Murawski,
Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania Keith T. Kanel, MD, MHCM, FACP Colleen Vrbin Susan Elster, PhD Jason Kunzman, MBA Michelle Murawski,
Potentially Preventable Hospitalizations in Pennsylvania
 Potentially Preventable Hospitalizations in Pennsylvania Pennsylvania Health Care Cost Containment Council June 2012 About PHC4 The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent
Potentially Preventable Hospitalizations in Pennsylvania Pennsylvania Health Care Cost Containment Council June 2012 About PHC4 The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent
Medicare and Medicaid Payments
 and Payments The following table includes information about payments made by and for the 17 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on
and Payments The following table includes information about payments made by and for the 17 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on
Initial Hospital Care/Day. Subsequent Hospital Care/Day
 Inpatient Charges Daily Room Rates CM CM Intensive Care $4,305 Maternity $1,137 Cardiovascular Care $3,338 Newborn Care $669 Medical/Surgical $1,297 NICU $2,938 Hospital Care Hospital New Patient Consult
Inpatient Charges Daily Room Rates CM CM Intensive Care $4,305 Maternity $1,137 Cardiovascular Care $3,338 Newborn Care $669 Medical/Surgical $1,297 NICU $2,938 Hospital Care Hospital New Patient Consult
Texas Council Endorsed Measurement Strategy
 Texas Council Endorsed Measurement Strategy During 2013, the Data Work Group of the Texas Council of Community Centers met to identify a set of clinical quality measures that can be used across the entire
Texas Council Endorsed Measurement Strategy During 2013, the Data Work Group of the Texas Council of Community Centers met to identify a set of clinical quality measures that can be used across the entire
2016 Community Service Plan & Community Health Improvement Plan
 2016 Community Service Plan & Community Health Improvement Plan A.O. Fox Memorial Hospital The Mary Imogene Bassett Hospital (dba: Bassett Medical Center) & Otsego County Health Department Service Area:
2016 Community Service Plan & Community Health Improvement Plan A.O. Fox Memorial Hospital The Mary Imogene Bassett Hospital (dba: Bassett Medical Center) & Otsego County Health Department Service Area:
2017 Diabetes. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2017 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2017 December
2017 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2017 December
HIV Health Improvement Affinity Group
 HIV Health Improvement Affinity Group Improving Quality of Care for Medicaid Beneficiaries Living with HIV: Strategies to Engage Managed Care Plans and Providers August 17, 3:30pm-4:45pm ET Moderator CDR
HIV Health Improvement Affinity Group Improving Quality of Care for Medicaid Beneficiaries Living with HIV: Strategies to Engage Managed Care Plans and Providers August 17, 3:30pm-4:45pm ET Moderator CDR
2017 PGIP Fact Sheet Electronic Prescribing of Controlled Substances (EPCS)
 2017 PGIP Fact Sheet Electronic Prescribing of Controlled Substances (EPCS) Overview Value Partnerships, in conjunction with the Blue Cross Pharmacy team, has created the Electronic Prescribing of Controlled
2017 PGIP Fact Sheet Electronic Prescribing of Controlled Substances (EPCS) Overview Value Partnerships, in conjunction with the Blue Cross Pharmacy team, has created the Electronic Prescribing of Controlled
Heart Attack Readmissions in Virginia
 Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Submitted to the House Energy and Commerce Committee. Federal Efforts to Combat the Opioid Crisis
 STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
Preventing 1 Million Heart Attacks and Strokes by 2022
 Preventing 1 Million Heart Attacks and Strokes by 2022 Miriam Patanian, MPH Senior Consultant for Health Systems and Cardiovascular Health National Association of Chronic Disease Directors Million Hearts
Preventing 1 Million Heart Attacks and Strokes by 2022 Miriam Patanian, MPH Senior Consultant for Health Systems and Cardiovascular Health National Association of Chronic Disease Directors Million Hearts
BPCI Advanced Episode Selection
 BPCI Advanced Episode Selection Analytic Framework and Strategies from Northwestern Medicine Presented June 7, 2018 to: Insert relevant presenter information Calibri 16pt Presented Jessica Walradt on:
BPCI Advanced Episode Selection Analytic Framework and Strategies from Northwestern Medicine Presented June 7, 2018 to: Insert relevant presenter information Calibri 16pt Presented Jessica Walradt on:
Determining MS-DRGs. Kimberly Cunningham CPC, CIC, CCS. Copyright/Disclaimer text
 Determining MS-DRGs Kimberly Cunningham CPC, CIC, CCS Copyright/Disclaimer text No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or
Determining MS-DRGs Kimberly Cunningham CPC, CIC, CCS Copyright/Disclaimer text No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or
APR DRG Data Discovery
 APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
The National Vaccine Advisory Committee: Reducing Patient and Provider Barriers to Maternal Immunizations
 The National Vaccine Advisory Committee: Reducing Patient and Provider Barriers to Maternal Immunizations Executive Summary Maternal immunization provides important health benefits for pregnant women and
The National Vaccine Advisory Committee: Reducing Patient and Provider Barriers to Maternal Immunizations Executive Summary Maternal immunization provides important health benefits for pregnant women and
Diabetes. Chronic Condition Clinical Advisory Group Value Based Payment Recommendation Report. NYS Medicaid Value Based Payment.
 Diabetes Chronic Condition Clinical Advisory Group Value Based Payment Recommendation Report September 2016 NYS Medicaid Value Based Payment Introduction Delivery System Reform Incentive Payment (DSRIP)
Diabetes Chronic Condition Clinical Advisory Group Value Based Payment Recommendation Report September 2016 NYS Medicaid Value Based Payment Introduction Delivery System Reform Incentive Payment (DSRIP)
Implementing Performance Measurement Programs: The Blue Cross Blue Shield of Massachusetts Perspective
 Implementing Performance Measurement Programs: The Blue Cross Blue Shield of Massachusetts Perspective Dana Gelb Safran, Sc.D. Senior Vice President Performance Measurement and Improvement Massachusetts
Implementing Performance Measurement Programs: The Blue Cross Blue Shield of Massachusetts Perspective Dana Gelb Safran, Sc.D. Senior Vice President Performance Measurement and Improvement Massachusetts
Overview of the NC Diabetes Prevention and Management Guide. Ronny Bell, Ph.D., MS, Chair Jan Nicollerat, MSN, RN, ACNS-BC, CDE, Vice Chair
 Overview of the NC Diabetes Prevention and Management Guide Ronny Bell, Ph.D., MS, Chair Jan Nicollerat, MSN, RN, ACNS-BC, CDE, Vice Chair 1,030,000 in North Carolina 2,500,000 in North Carolina Age-adjusted
Overview of the NC Diabetes Prevention and Management Guide Ronny Bell, Ph.D., MS, Chair Jan Nicollerat, MSN, RN, ACNS-BC, CDE, Vice Chair 1,030,000 in North Carolina 2,500,000 in North Carolina Age-adjusted
Why is oral health important?
 An Ounce of Preventive Oral Health, a Pound of Savings Colin Reusch Senior Policy Analyst Children s Dental Health Project Why is oral health important? Oral Health impacts: Nutrition Speaking Learning
An Ounce of Preventive Oral Health, a Pound of Savings Colin Reusch Senior Policy Analyst Children s Dental Health Project Why is oral health important? Oral Health impacts: Nutrition Speaking Learning
Webinar Series: Diabetes Epidemic & Action Report (DEAR) for Washington State - How We Are Doing and How We Can Improve.
 Webinar Series: Diabetes Epidemic & Action Report (DEAR) for Washington State - How We Are Doing and How We Can Improve April 22, 2015 Qualis Health A leading national population health management organization
Webinar Series: Diabetes Epidemic & Action Report (DEAR) for Washington State - How We Are Doing and How We Can Improve April 22, 2015 Qualis Health A leading national population health management organization
Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States
 Diabetes Care In Press, published online February 8, 007 Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States Received
Diabetes Care In Press, published online February 8, 007 Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States Received
2015 Diabetes. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2015 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Care Program Evaluation Program Title: Diabetes Care Program Evaluation Period: January
2015 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Care Program Evaluation Program Title: Diabetes Care Program Evaluation Period: January
Suffolk Care Collaborative Diabetes Wellness & Self-Management Program (DWSP)
 Suffolk Care Collaborative Diabetes Wellness & Self-Management Program (DWSP) 3.c.i Evidence based strategies for disease management in high risk/affected populations. (Adult only) Project Charter Executive
Suffolk Care Collaborative Diabetes Wellness & Self-Management Program (DWSP) 3.c.i Evidence based strategies for disease management in high risk/affected populations. (Adult only) Project Charter Executive
The Burden Report: Cardiovascular Disease & Stroke in Texas
 The Burden Report: Cardiovascular Disease & Stroke in Texas Texas Cardiovascular Health and Wellness Program www.dshs.state.tx.us/wellness Texas Council on Cardiovascular Disease and Stroke www.texascvdcouncil.org
The Burden Report: Cardiovascular Disease & Stroke in Texas Texas Cardiovascular Health and Wellness Program www.dshs.state.tx.us/wellness Texas Council on Cardiovascular Disease and Stroke www.texascvdcouncil.org
Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years
 Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
Key Trends for Ambulatory Surgery Centers in 2018
 Key Trends for Ambulatory Surgery Centers in 2018 Don Phalen Vice President Business Development, Regent Surgical Health Mark Murphy Chief Strategy Officer, St Joseph s Hospital MOVING TOWARDS VALUE-BASED
Key Trends for Ambulatory Surgery Centers in 2018 Don Phalen Vice President Business Development, Regent Surgical Health Mark Murphy Chief Strategy Officer, St Joseph s Hospital MOVING TOWARDS VALUE-BASED
Ministry of Health and Long-Term Care. Palliative Care. Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW
 Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
Measuring and Improving Quality in Accountable Care Organizations
 Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
Some key findings from ABC Clinic's report: Risk Score Clinic. Summary by Service Category
 Dear Administrator or Medical Director, QCorp is pleased to release its second round of Comparison Reports. This report includes claims incurred from January 2014 to December 2014. As a reminder, the goal
Dear Administrator or Medical Director, QCorp is pleased to release its second round of Comparison Reports. This report includes claims incurred from January 2014 to December 2014. As a reminder, the goal
Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings
 CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
The Changing Landscape of Palliative Care
 The Changing Landscape of Palliative Care KAHPC 17th Annual Conference August 2015 Brian Jones Joe Rotella Elizabeth Wessels Turner West Kay Williams Why Home-based Palliative Care? Turner West, MPH, MTS
The Changing Landscape of Palliative Care KAHPC 17th Annual Conference August 2015 Brian Jones Joe Rotella Elizabeth Wessels Turner West Kay Williams Why Home-based Palliative Care? Turner West, MPH, MTS
At the Intersection of Public Health and Health Care: CDC s National Asthma Control Program
 At the Intersection of Public Health and Health Care: CDC s National Asthma Control Program Shirl Ellis Odem Maureen Wilce Elizabeth Herman Asthma Initiative of Michigan Partnership Forum June 3, 2016
At the Intersection of Public Health and Health Care: CDC s National Asthma Control Program Shirl Ellis Odem Maureen Wilce Elizabeth Herman Asthma Initiative of Michigan Partnership Forum June 3, 2016
Dana L. Gilbert Chief Operating Officer Sharon Rudnick Vice President Outpatient Care Management
 Ambulatory Sensitive Admissions Dana L. Gilbert Chief Operating Officer Sharon Rudnick Vice President Outpatient Care Management 1 Sites Of Care Advocate Health Care 12 Hospitals 10 acute care hospitals
Ambulatory Sensitive Admissions Dana L. Gilbert Chief Operating Officer Sharon Rudnick Vice President Outpatient Care Management 1 Sites Of Care Advocate Health Care 12 Hospitals 10 acute care hospitals
More than 1.8 million New York State residents have diabetes, and diabetes prevalence has doubled in the last decade.
 March 2010 New York State Health Foundation s DIABETES Policy Center CERTIFIED DIABETES EDUCATORS IN NEW YORK: Findings From a Statewide Market Analysis and Recommendations for Improving Access to Diabetes
March 2010 New York State Health Foundation s DIABETES Policy Center CERTIFIED DIABETES EDUCATORS IN NEW YORK: Findings From a Statewide Market Analysis and Recommendations for Improving Access to Diabetes
Getting to Safe, Affordable, Effective, Patient-Centered Care: Good Data Are Only the Beginning
 Getting to Safe, Affordable, Effective, Patient-Centered Care: Good Data Are Only the Beginning Dana Gelb Safran, Sc.D. Senior Vice President Performance Measurement & Improvement Transformation Vision:
Getting to Safe, Affordable, Effective, Patient-Centered Care: Good Data Are Only the Beginning Dana Gelb Safran, Sc.D. Senior Vice President Performance Measurement & Improvement Transformation Vision:
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
Medicare Payments. PHC4 Hospital Performance Report Oct 2015 through Sept 2016 Data 2015 Medicare Payments 1
 The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from calendar
The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from calendar
Transitional Care With Palliative Medicine
 Bridging The Gaps: Providing Transitional Care With Palliative Medicine Angie Hollis-Sells, RN, CHPN President AseraCare Robert Parker, RN, MSN Ed., CHPN Program Manager Bridging The Gaps: Proving Transitional
Bridging The Gaps: Providing Transitional Care With Palliative Medicine Angie Hollis-Sells, RN, CHPN President AseraCare Robert Parker, RN, MSN Ed., CHPN Program Manager Bridging The Gaps: Proving Transitional
Understanding Hierarchical Condition Categories (HCC)
 Understanding Hierarchical Condition Categories (HCC) How hierarchical condition category coding will impact your practice and how you can use these codes to increase quality, improve the patient experience,
Understanding Hierarchical Condition Categories (HCC) How hierarchical condition category coding will impact your practice and how you can use these codes to increase quality, improve the patient experience,
PA Optometric Association Annual Congress
 May 18, 2012 PA Optometric Association Annual Congress Andrew Bloschichak MD, MBA Senior Medical Director, Highmark Emerging Health Care Reform Delivery and Reimbursement Systems Introduction Key Drivers
May 18, 2012 PA Optometric Association Annual Congress Andrew Bloschichak MD, MBA Senior Medical Director, Highmark Emerging Health Care Reform Delivery and Reimbursement Systems Introduction Key Drivers
NORTH CAROLINA CARDIOVASCULAR STATE PLAN I N T R O D U C T I O N S, G O A L S, O B J E C T I V E S A N D S T R A T E G I E S
 NORTH CAROLINA CARDIOVASCULAR STATE PLAN 2011-2016 I N T R O D U C T I O N S, G O A L S, O B J E C T I V E S A N D S T R A T E G I E S PRIMARY PREVENTION OF CARDIOVASCULAR DISEASE THROUGH HEALTHY LIVING
NORTH CAROLINA CARDIOVASCULAR STATE PLAN 2011-2016 I N T R O D U C T I O N S, G O A L S, O B J E C T I V E S A N D S T R A T E G I E S PRIMARY PREVENTION OF CARDIOVASCULAR DISEASE THROUGH HEALTHY LIVING
Carolinas HealthCare System Fragility Fracture Program
 Carolinas HealthCare System Fragility Fracture Program Presented By: Monica C. Mowry, MSN, RN, NE-BC, ONC Director, Clinical Program Development Carolinas HealthCare System Charlotte, NC Objectives Expand
Carolinas HealthCare System Fragility Fracture Program Presented By: Monica C. Mowry, MSN, RN, NE-BC, ONC Director, Clinical Program Development Carolinas HealthCare System Charlotte, NC Objectives Expand
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report. User s Guide Sixth Edition. Prepared by
 Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare
 Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
Drug Overdose Morbidity and Mortality in Kentucky,
 Drug Overdose Morbidity and Mortality in Kentucky, 2000-2010 An examination of statewide data, including the rising impact of prescription drug overdose on fatality rates, and the parallel rise in associated
Drug Overdose Morbidity and Mortality in Kentucky, 2000-2010 An examination of statewide data, including the rising impact of prescription drug overdose on fatality rates, and the parallel rise in associated
PREVENTATIVE COMMUNITY PHARMACY DIABETES MANAGEMENT PROGRAMS BROOKE HUDSPETH, PHARMD, CDE, MLDE KROGER DIABETES CARE
 PREVENTATIVE COMMUNITY PHARMACY DIABETES MANAGEMENT PROGRAMS BROOKE HUDSPETH, PHARMD, CDE, MLDE KROGER DIABETES CARE DISCLOSURE STATEMENT Brooke Hudspeth is employed by The Kroger Co. No other conflicts
PREVENTATIVE COMMUNITY PHARMACY DIABETES MANAGEMENT PROGRAMS BROOKE HUDSPETH, PHARMD, CDE, MLDE KROGER DIABETES CARE DISCLOSURE STATEMENT Brooke Hudspeth is employed by The Kroger Co. No other conflicts
Home-Based Asthma Interventions: Keys to Success
 Home-Based Asthma Interventions: Keys to Success Setting the Stage Asthma affects 25 million Americans (one in every 12 people), including six million children. The costs of uncontrolled asthma -- including
Home-Based Asthma Interventions: Keys to Success Setting the Stage Asthma affects 25 million Americans (one in every 12 people), including six million children. The costs of uncontrolled asthma -- including
Dennis P. Scanlon, Ph.D. Jeff Beich, Ph.D. Patti Simino Boyce RN, Ph.D. AcademyHealth, June 30, 2009
 Dennis P. Scanlon, Ph.D. Jeff Beich, Ph.D. Patti Simino Boyce RN, Ph.D. AcademyHealth, June 30, 2009 Many policymakers and stakeholder organizations have suggested the need for sustainable community level
Dennis P. Scanlon, Ph.D. Jeff Beich, Ph.D. Patti Simino Boyce RN, Ph.D. AcademyHealth, June 30, 2009 Many policymakers and stakeholder organizations have suggested the need for sustainable community level
Advancing Cardiovascular Care of the Oncology Patient
 Advancing Cardiovascular Care of the Oncology Patient Why Are We Here? The Intersection Between Cardiology and Oncology Feb 17, 2017 Mary Norine Walsh, MD, FACC Medical Director, HF and Cardiac Transplantation
Advancing Cardiovascular Care of the Oncology Patient Why Are We Here? The Intersection Between Cardiology and Oncology Feb 17, 2017 Mary Norine Walsh, MD, FACC Medical Director, HF and Cardiac Transplantation
Fifth Annual National ACO Summit
 Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database
 TECHNICAL SPECIFICATIONS AND METHODS SUPPLEMENT Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database MAY 2017 Minnesota Department of Health Health Economics Program 85 E. 7th
TECHNICAL SPECIFICATIONS AND METHODS SUPPLEMENT Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database MAY 2017 Minnesota Department of Health Health Economics Program 85 E. 7th
Medicare Severity-adjusted Diagnosis Related Groups (MS-DRGs) Coding Adjustment
 American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
The Patient-Centered MEDICAL HOME. The Dietitian s Role in This Healthcare Model That Improves Diabetes Outcomes
 The Patient-Centered MEDICAL HOME The Dietitian s Role in This Healthcare Model That Improves Diabetes Outcomes By Constance Brown-Riggs, MSEd, RD, CDE, CDN With the advent of healthcare reform, new models
The Patient-Centered MEDICAL HOME The Dietitian s Role in This Healthcare Model That Improves Diabetes Outcomes By Constance Brown-Riggs, MSEd, RD, CDE, CDN With the advent of healthcare reform, new models
Opportunities for Developing Measures for Adult Vaccines
 Opportunities for Developing s for Adult Vaccines May 15, 2012 National Adult Immunization Summit Tilithia McBride Avalere Health LLC Why s? VA Program Demonstrates Success of ment to Improve Vaccination
Opportunities for Developing s for Adult Vaccines May 15, 2012 National Adult Immunization Summit Tilithia McBride Avalere Health LLC Why s? VA Program Demonstrates Success of ment to Improve Vaccination
Disclosures. Preventing Heart Failure Re-admissions in Deaths Due to Cardiovascular Disease (United States: ) Heart Failure
 29 th Annual Cardiology for Clinicians Spring Symposium Workshop #3 Alumni Hallway, Northeastern Conference Room, 1-9525 Thursday, May 5, 2016 Preventing Heart Failure Re-admissions in 2016 Leway Chen,
29 th Annual Cardiology for Clinicians Spring Symposium Workshop #3 Alumni Hallway, Northeastern Conference Room, 1-9525 Thursday, May 5, 2016 Preventing Heart Failure Re-admissions in 2016 Leway Chen,
Medicare Payments. PHC4 Hospital Performance Report Oct 2016 through Sept 2017 Data FFY 2017 Medicare Payments 1
 The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from federal
The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from federal
Statewide Statistics and Key Findings 1
 % s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
% s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
HEALTH REFORM & HEALTH CARE FOR THE HOMELESS POLICY BRIEF JUNE 2010
 HEALTH REFORM & HEALTH CARE FOR THE HOMELESS CREATING HEALTHIER COMMUNITIES: CHRONIC DISEASE PREVENTION INITIATIVES OF INTEREST TO HEALTH CENTERS Chronic disease is the leading cause of death and disability
HEALTH REFORM & HEALTH CARE FOR THE HOMELESS CREATING HEALTHIER COMMUNITIES: CHRONIC DISEASE PREVENTION INITIATIVES OF INTEREST TO HEALTH CENTERS Chronic disease is the leading cause of death and disability
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights
 Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Strategic Plan
 Strategic Plan 2013-2015 The key to a strong, responsive organization is a clearly defined mission, complete with specific goals and intended outcomes. Our strategic goals are essential to the association
Strategic Plan 2013-2015 The key to a strong, responsive organization is a clearly defined mission, complete with specific goals and intended outcomes. Our strategic goals are essential to the association
Gerald Bernstein, MD, Director, Diabetes Management Program. Marina Krymskaya, RN, MSN, ANP, CDE FDI Assistant Director
 Gerald Bernstein, MD, Director, Diabetes Management Program Marina Krymskaya, RN, MSN, ANP, CDE FDI Assistant Director November, 2010 1 Epidemiology CDC: 1 of 3 born in 2000 will develop diabetes. 42.3%
Gerald Bernstein, MD, Director, Diabetes Management Program Marina Krymskaya, RN, MSN, ANP, CDE FDI Assistant Director November, 2010 1 Epidemiology CDC: 1 of 3 born in 2000 will develop diabetes. 42.3%
OCTOBER EOEA and the Alzheimer s Association have organized implementation of the plan around its five major recommendations:
 1 MASSACHUSETTS ALZHEIMER S DISEASE AND RELATED DISORDERS STATE PLAN RECOMMENDATIONS TWO-YEAR PROGRESS REPORT OCTOBER 2014 In February 2012, Massachusetts released a set of Alzheimer s Disease and Related
1 MASSACHUSETTS ALZHEIMER S DISEASE AND RELATED DISORDERS STATE PLAN RECOMMENDATIONS TWO-YEAR PROGRESS REPORT OCTOBER 2014 In February 2012, Massachusetts released a set of Alzheimer s Disease and Related
Fractional Flow Reserve (FFR) and instant wave-free Ratio (The ifr modality)
 2017 Coding and Medicare payment guide Fractional Flow Reserve (FFR) and instant wave-free Ratio (The ifr modality) All coding, coverage, billing and payment information provided herein by Philips Volcano
2017 Coding and Medicare payment guide Fractional Flow Reserve (FFR) and instant wave-free Ratio (The ifr modality) All coding, coverage, billing and payment information provided herein by Philips Volcano
Quality Innovation Network - Quality Improvement Organization Adult Immunization Task. May 14, Agenda
 Quality Innovation Network - Quality Improvement Organization Adult Immunization Task National Adult and Influenza Immunization Summit Centers for Medicare & Medicaid Services 1 May 14, 2015 Agenda Quick
Quality Innovation Network - Quality Improvement Organization Adult Immunization Task National Adult and Influenza Immunization Summit Centers for Medicare & Medicaid Services 1 May 14, 2015 Agenda Quick
Longitudinal Care Management. September 2016
 Longitudinal Care Management September 2016 Risk Score Assignment of Longitudinal CM Other C M Referral sources Screening: Need CM? Clinical Assessment tools Program Services Integrated Care Management
Longitudinal Care Management September 2016 Risk Score Assignment of Longitudinal CM Other C M Referral sources Screening: Need CM? Clinical Assessment tools Program Services Integrated Care Management
8/12/2016. Outline. New CPT Code for Pre-Diabetes Education. Medicare Proposed Coverage for DPP. Medicare Proposed Coverage for DPP cont.
 New CPT Code for Pre-Diabetes Education 0403T: Preventive behavior change, intensive program of prevention of diabetes using a standardized diabetes prevention program curriculum, provided to individuals
New CPT Code for Pre-Diabetes Education 0403T: Preventive behavior change, intensive program of prevention of diabetes using a standardized diabetes prevention program curriculum, provided to individuals
The New Medtech Economic Reality MassMEDIC Annual Meeting
 The New Medtech Economic Reality MassMEDIC Annual Meeting Susan Posner Vice President sposner@healthadvances.com May 1, 2012 The New Medtech Reality The economic downturn coupled with the focus on health
The New Medtech Economic Reality MassMEDIC Annual Meeting Susan Posner Vice President sposner@healthadvances.com May 1, 2012 The New Medtech Reality The economic downturn coupled with the focus on health
Ensuring Access to Mental Health Services For All Chicagoans
 Ensuring Access to Mental Health Services For All Chicagoans August 19, 2014 Bechara Choucair, MD Commissioner City of Chicago Mayor Rahm Emanuel Chicago Department of Public Health Commissioner Bechara
Ensuring Access to Mental Health Services For All Chicagoans August 19, 2014 Bechara Choucair, MD Commissioner City of Chicago Mayor Rahm Emanuel Chicago Department of Public Health Commissioner Bechara
Value of Hospice Benefit to Medicaid Programs
 One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
2012 Diabetes. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2012 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2012 December
2012 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2012 December
INFLUENZA & PNEUMOCCOCAL VACCINATIONS
 INFLUENZA & PNEUMOCCOCAL VACCINATIONS ONE HEALTH PLAN S PERSPECTIVE Paige Reichert, MD Senior Medical Director of Quality May 2015 THE CIGNA-HEALTHSPRING FOOTPRINT o Cigna-HealthSpring serves the senior
INFLUENZA & PNEUMOCCOCAL VACCINATIONS ONE HEALTH PLAN S PERSPECTIVE Paige Reichert, MD Senior Medical Director of Quality May 2015 THE CIGNA-HEALTHSPRING FOOTPRINT o Cigna-HealthSpring serves the senior
Palliative Care Quality Improvement Program (QIP) Measurement Specifications
 Palliative Care Quality Improvement Program (QIP) 2017-18 Measurement Specifications Developed by: QIP Team Contact: palliativeqip@partnershiphp.org Published on: October 6, 2017 Table of Contents Program
Palliative Care Quality Improvement Program (QIP) 2017-18 Measurement Specifications Developed by: QIP Team Contact: palliativeqip@partnershiphp.org Published on: October 6, 2017 Table of Contents Program
Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians
 Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
SIM Outcomes and Data Acquisition Report CY 2015 and CY Policy Report. October 2017
 Policy Report October 2017 SIM Outcomes Data Acquisition Report CY 2015 CY 2016 Elizabeth T. Momany, PhD Associate Research Scientist Assistant Director, Health Policy Research Program Suzanne Bentler,
Policy Report October 2017 SIM Outcomes Data Acquisition Report CY 2015 CY 2016 Elizabeth T. Momany, PhD Associate Research Scientist Assistant Director, Health Policy Research Program Suzanne Bentler,
