Age-Related Macular Degeneration
|
|
|
- Baldwin Manning
- 6 years ago
- Views:
Transcription
1 Age-Related Macular Degeneration Age-Related Macular Degeneration Age-related macular degeneration (AMD) is one of the most common causes of poor vision after age 60. AMD is a deterioration or breakdown of the macula. The macula is a small area at the center of the retina in the back of the eye that allows us to see fine details clearly and perform activities such as reading and driving. The visual symptoms of AMD involve loss of central vision. While peripheral (side) vision is unaffected, with AMD, one loses the sharp, straight-ahead vision necessary for driving, reading, recognizing faces, and looking at detail. Although the specific cause is unknown, AMD seems to be part of aging. While age is the most significant risk factor for developing AMD, heredity, blue eyes, high blood pressure, cardiovascular disease, and smoking have also been identified as risk factors. AMD accounts for 90% of new cases of legal blindness in the United States. Nine out of 10 people who have AMD have atrophic or dry AMD, which results in thinning of the macula. Dry AMD takes many years to develop. A specific vitamin regimen has been shown to slow progression of dry AMD. Exudative or wet AMD is less common (occurring in one out of 10 people with AMD) but is more serious. In the wet form of AMD, abnormal blood vessels may grow in a layer beneath the retina, leaking fluid and blood and creating distortion or a large blind spot in the center of your vision. If the blood vessels are not growing directly beneath the macula, laser surgery is usually the treatment of choice. The procedure usually does not improve vision but tries to prevent further loss of vision. For those patients with wet AMD whose blood vessels are growing directly under the center of the macula, a procedure called photodynamic therapy (PDT), which causes fewer visual side effects, is sometimes used. Intravitreal injections of certain medications can also be used in these cases. Promising AMD research is being done on many fronts. In the meantime, high-intensity reading lamps, magnifiers, and other low vision aids help people with AMD make the most of their remaining vision. file:///c /Documents%20and%20Settings/Det/My%20Documents/...es/Retina_and_Vitreous/AgeRelatedMacularDegeneration.html1/8/ :23:27 AM
2 Central Retinal Artery Occlusion Central Retinal Artery Occlusion You probably know that high blood pressure and other vascular diseases pose risks to your overall health, but you may not know that they can affect your eyesight by damaging the arteries in your eye. Central retinal artery occlusion (CRAO) usually occurs in people between the ages of 50 and 70. The most common medical problem associated with CRAO is arteriosclerosis (hardening of the arteries). Carotid artery disease is found in almost half the people with CRAO. The most common cause of CRAO is a thrombosis (an abnormal blood clot formation). CRAO can also be caused by an embolus, a clot that breaks off from another area of the body and is carried to the retina by the bloodstream. CRAO blocks the central artery in your retina, the light-sensitive nerve layer at the back of the eye. The first sign of CRAO is a sudden and painless loss of vision that leaves you barely able to count fingers or determine light from dark. Loss of vision can be permanent without immediate treatment. Irreversible retinal damage occurs after 90 minutes, but even 24 hours after symptoms begin, vision can still be saved. The goal of emergency treatment is to restore retinal blood flow. After emergency treatment, you should have a thorough medical evaluation. file:///c /Documents%20and%20Settings/Det/My%20Documents/M...ces/Retina_and_Vitreous/CentralRetinalArteryOcclusion.html1/8/ :23:27 AM
3 Indocyanine Green Angiography Indocyanine Green Angiography Indocyanine green angiography (ICG) is a clinical test used to detect abnormal blood vessels in the choroid, the layer of blood vessels under the retina. These abnormal blood vessels, typically associated with macular degeneration, may cause bleeding, scarring, and vision loss. If the blood vessels can be restricted with treatment, vision loss may be stabilized or improved. Indocyanine, a harmless green dye, gives off infrared light. When injected into the bloodstream, the dye travels through the veins to the blood vessels in the eye. A video camera connected to a computer picks up the infrared light and makes a picture of the blood s circulation. No film or X-rays are involved. Following the test, the liver removes the dye from the body. There is little risk in having an ICG angiogram. Some people may have mild allergic reactions and, although rare, a few severe allergic reactions have been reported in people allergic to iodine, X-ray dyes, and shellfish. file:///c /Documents%20and%20Settings/Det/My%20Documents/...rces/Retina_and_Vitreous/IndocyanineGreenAngiography.html1/8/ :23:27 AM
4 Fluorescein Angiography Fluorescein Angiography Fluorescein angiography, a clinical test to look at blood circulation inside the back of the eye, aids in the diagnosis of retinal conditions associated with diabetes, age-related macular degeneration, and other eye abnormalities. The test can also help follow the course of a disease and monitor its treatment. It may be repeated on multiple occasions with no harm to the eye or body. Fluorescein is an orange-red dye that is injected into a vein in the arm. The dye travels through the body to the blood vessels in the retina, the light-sensitive nerve layer at the back of the eye. A special camera with a green filter flashes a blue light into the eye and takes multiple photographs of the retina. The technique uses regular photographic film, or, more commonly, is performed with digital equipment. No X-rays are involved. If there are abnormal blood vessels, the dye leaks into the retina or stains the blood vessels. Damage to the lining of the retina or atypical new blood vessels may be revealed as well. These abnormalities are determined by a careful interpretation of the photographs by an ophthalmologist (Eye M.D.). The dye can discolor skin and urine until it is removed from the body by the kidneys. There is little risk in having fluorescein angiography, though some people may have mild allergic reactions to the dye. Severe allergic reactions have been reported but only very rarely. Being allergic to X-ray dyes with iodine does not mean you will be allergic to fluorescein. Occasionally, some of the dye leaks out of the vein at the injection site, causing a slight burning sensation that usually goes away quickly. file:///c /Documents%20and%20Settings/Det/My%20Documents/...Resources/Retina_and_Vitreous/FluoresceinAngiography.html1/8/ :23:27 AM
5 Birdshot Retinochoroidopathy Birdshot Retinochoroidopathy Birdshot retinochoroidopathy (BR) is a rare, inflammatory condition of the retina and choroid, the layer of blood vessels under the retina. BR is a chronic disease that flares up and then goes into remission. Although some people eventually lose vision, others maintain or recover good vision. The cause of BR is unknown. It usually occurs in white women over the age of 40, and usually affects both eyes. Symptoms are poor vision, night blindness, and disturbance of color vision. Pain is rare. Fluorescein angiography, a test used to evaluate the retina and choroid, detects BR s characteristic cream-colored spots, similar in appearance to the splattered pattern of birdshot from a shotgun. If you have been diagnosed with birdshot retinochoroidopathy, it is important to see your ophthalmologist (Eye M.D.) regularly. file:///c /Documents%20and%20Settings/Det/My%20Documents/...s/titamadeeh/PatientResources/Retina_and_Vitreous/BR.html1/8/ :23:27 AM
6 Anti-VEGF Treatment for Wet AMD Anti-VEGF Treatment for Wet Age-Related Macular Degeneration Anti-VEGF treatment is a way to slow vision loss in people who have a condition known as wet agerelated macular degeneration (AMD). AMD is the leading cause of vision loss in people 50 years or older in the United States. This condition damages the macula, which is located in the center of the retina and enables you to see fine details clearly. You rely on your macula whenever you read, drive, or do other activities that require you to focus on precise details. A person with AMD loses the ability to perceive fine details both up close and at a distance. This vision loss usually affects only your central vision. There are two types of AMD. About 90% of people with AMD have the atrophic or dry form of AMD, which develops when the tissues of the macula grow thin with age. About 10% have the exudative or wet form of AMD. With wet AMD, abnormal blood vessels grow underneath the retina. These unhealthy vessels leak blood and fluid, which can scar the macula. Vision loss can be rapid and severe. Researchers have found that a chemical called vascular endothelial growth factor, or VEGF, is critical in causing abnormal blood vessels to grow under the retina. Scientists have developed several new drugs that can block the trouble-causing VEGF. These are referred to as anti-vegf drugs, and they help block abnormal blood vessels, slow their leakage, and help reduce vision loss. Treatment with the anti-vegf drug is usually performed by injecting the medicine with a very fine needle into the back of your eye. Your ophthalmologist (Eye M.D.) will clean your eye to prevent infection and will administer an anesthetic into your eye to reduce pain. Usually, patients receive multiple anti-vegf injections over the course of many months. There is a small risk of complications with anti-vegf treatment, usually resulting from the injection itself. However, for most people, the benefits of this treatment outweigh the small risk of complications. Anti-VEGF medications are a step forward in the treatment of wet AMD because they target the underlying cause of abnormal blood vessel growth. This treatment offers new hope to those affected with wet AMD. Although not every patient benefits from anti-vegf treatment, a large majority of patients achieve stabilized vision, and a significant percentage can improve to some degree. file:///c /Documents%20and%20Settings/Det/My%20Document.../AntiVEGFTreatmentWetAgeRelatedMacularDegeneration.html1/8/ :23:28 AM
7 Coats' Disease Coats Disease Coats disease is a chronic, progressive disorder that affects the retina, the light-sensitive nerve layer at the back of the eye. Coats disease is an abnormal growth spurt of the small blood vessels (capillaries) that nourish the retina. The fragile abnormal vessels break and leak the clear serum part of the blood into the retina, causing the retina to swell. Coats disease usually affects children (especially boys) in the first ten years of life, but it can also affect young adults. The condition affects central vision, typically in only one eye. Severity can range from mild vision loss to total retinal detachment and blindness. No cause has yet been identified for Coats disease. The leaking blood vessels can be treated with laser surgery or cryotherapy (freezing). If the retina is detached, a vitrectomy to replace the vitreous (the clear gel-like substance inside the eye) with a gas bubble may be necessary to restore vision. file:///c /Documents%20and%20Settings/Det/My%20Documents/...eh/PatientResources/Retina_and_Vitreous/CoatsDisease.html1/8/ :23:28 AM
8 Cytomegalovirus Retinitis Cytomegalovirus Retinitis Cytomegalovirus retinitis (CMV retinitis) is a serious eye infection of the retina, the light-sensing nerve layer that lines the back of the eye. It is a significant threat to people with weak immune systems, such as people with HIV and AIDS, newborns, the elderly, people undergoing chemotherapy, and recipients of organ transplants. About 20% to 30% of people with AIDS develop CMV retinitis. Infection with cytomegalovirus, one of the herpes viruses, is extremely common and does not pose a problem for someone with a strong immune system. But when immunity is weak, the CMV can reactivate and spread to the retina through the bloodstream. First signs of CMV retinitis are loss of peripheral vision or a blind spot that can progress to loss of central vision. Without treatment or improvement in the immune system, CMV retinitis destroys the retina and damages the optic nerve, which results in blindness. Treatment is possible for CMV retinitis. Ganciclovir and other antiviral medicines are available, and they can be administered orally, intravenously, as an intraocular injection, and, in some cases, via a sustained-release intraocular implant. Warning signs that should prompt an immediate examination by an ophthalmologist (Eye M.D.) are the appearance of floating spots or spider webs, flashing lights, blind spots, or blurred vision. Recurrence of CMV retinitis is common, so monthly checkups with an ophthalmologist are important. file:///c /Documents%20and%20Settings/Det/My%20Documents/M...esources/Retina_and_Vitreous/CytomegalovirusRetinitis.html1/8/ :23:28 AM
9 Branch Retinal Artery Occlusion Branch Retinal Artery Occlusion Most people know that high blood pressure and other vascular diseases pose risks to overall health, but many may not know that high blood pressure can affect vision by damaging the arteries in the eye. Branch retinal artery occlusion (BRAO) blocks the small arteries in the retina, the light-sensing nerve layer lining the back of the eye. The most common cause of BRAO is a thrombosis, the formation of a blood clot. Sometimes the blockage is caused by an embolus, a clot carried by the blood from another part of the body. Central vision is lost suddenly if the blocked retinal artery is one that nourishes the macula, the part of the retina responsible for fine, sharp vision. Following BRAO, vision can range from normal (20/20) to being barely able to detect hand movement. BRAO poses significant risks to vision. If you have had a branch retinal artery occlusion, regular visits to your ophthalmologist are essential. file:///c /Documents%20and%20Settings/Det/My%20Documents/...ces/Retina_and_Vitreous/BranchRetinalArteryOcclusion.html1/8/ :23:28 AM
10 Branch Retinal Vein Occlusion Branch Retinal Vein Occlusion Most people know that high blood pressure and other vascular diseases pose risks to overall health, but many may not know that high blood pressure can affect vision by damaging the veins in the eye. High blood pressure is the most common condition associated with branch retinal vein occlusion (BRVO). About 10% to 12% of the people who have BRVO also have glaucoma (high pressure in the eye). BRVO blocks small veins in the retina, the layer of light-sensing cells at the back of the eye. If the blocked retinal veins are ones that nourish the macula, the part of the retina responsible for straightahead vision, some central vision is lost. During the course of vein occlusion, 60% or more will have swelling of the central macular area. In about one-third of people, this macular edema will last for more than one year. BRVO causes a painless decrease in vision, resulting in misty or distorted vision. If the veins cover a large area, new abnormal vessels may grow on the retinal surface, which can bleed into the eye and cause blurred vision. There is no cure for BRVO. Finding out what caused the blockage is the first step in treatment. Your ophthalmologist (Eye M.D.) may recommend a period of observation, since hemorrhages and excess fluid may subside on their own. Depending on how damaged the veins are, laser surgery may help reduce the swelling and improve vision. Laser surgery may also shrink abnormal new blood vessels that can grow and that are at risk of bleeding. Newer injectable medicines are being investigated for treating BRVO. If you have had a branch retinal vein occlusion, regular visits to your ophthalmologist are essential to protect vision. file:///c /Documents%20and%20Settings/Det/My%20Documents/...urces/Retina_and_Vitreous/BranchRetinalVeinOcclusion.html1/8/ :23:28 AM
11 Central Serous Retinopathy Central Serous Retinopathy Central serous retinopathy (CSR) is a small, round, shallow swelling that develops on the retina, the light-sensitive nerve layer that lines the back of the eye. Although the swelling reduces or distorts vision, the effects are usually temporary. Vision generally recovers on its own within a few months. In the initial stages of CSR, vision may suddenly become blurred and dim. If the macula (the area of the retina responsible for central vision) is not affected, there may be no obvious symptoms. CSR typically affects adults between the ages of 20 and 50. People with CSR often find that their retinal swelling resolves without treatment and their original vision returns within six months of the onset of symptoms. Some people with frequent episodes may have some permanent vision loss. Recurrences are common and can affect 20% to 50% of people with CSR. While the cause of CSR is unknown, it seems to occur at times of personal or work-related stress. As CSR usually resolves on its own, no treatment may be necessary. Sometimes laser surgery can reduce the swelling sooner, but the final visual outcome is usually about the same. If retinal swelling persists for more than three or four months, or if an examination reveals early retinal degeneration, laser surgery may be helpful. file:///c /Documents%20and%20Settings/Det/My%20Documents/...sources/Retina_and_Vitreous/CentralSerousRetinopathy.html1/8/ :23:28 AM
12 Epiretinal Membrane Epiretinal Membrane The retina is a layer of light-sensing cells lining the back of your eye. As light rays enter your eye, the retina converts the rays into signals that are sent through the optic nerve to your brain, where they are recognized as images. The macula is the small area at the center of your retina that allows you to see fine details. The macula normally lies flat against the back of the eye, like film lining the back of a camera. As you age, the clear, gel-like substance that fills the middle of your eye begins to shrink and pull away from the retina. In some cases, a thin scar tissue or membrane can grow on the surface of the macula. When wrinkles, creases, or bulges form on the macula due to this scar tissue, this is known as an epiretinal membrane or macular pucker. Damage to your macula causes blurred central vision, making it difficult to perform tasks such as reading small print or threading a needle. Peripheral (side) vision is not affected. Symptoms, which can be mild or severe and affect one or both eyes, may include: blurred detail vision; distorted or wavy vision; gray or cloudy area in central vision; and blind spot in central vision. Your ophthalmologist (Eye M.D.) detects an epiretinal membrane by examination and special photographic techniques. If your symptoms are mild, no treatment may be necessary. Updating your eyeglass prescription or wearing bifocals may improve your vision sufficiently. If you have more severe symptoms that interfere with your daily routine, your ophthalmologist may recommend vitrectomy surgery to peel and remove the abnormal scar tissue. During this outpatient procedure, your ophthalmologist uses tiny instruments to remove the wrinkled tissue. Vision often improves. Be sure to discuss your options with your ophthalmologist. If surgery is recommended, you should be aware that as with any surgical procedure, rare complications can occur, including infection, bleeding, retinal detachment, recurrence of the epiretinal membrane, and earlier onset of cataract. file:///c /Documents%20and%20Settings/Det/My%20Documents/...ientResources/Retina_and_Vitreous/EpiretinalMembrane.html1/8/ :23:28 AM
13 Cotton-Wool Spots Cotton-Wool Spots Cotton-wool spots are tiny white areas on the retina, the layer of light-sensing cells lining the back of the eye. Caused by a lack of blood flow to the small retinal blood vessels, they usually disappear without treatment and do not threaten vision. However, they can be an indication of a serious medical condition. Diabetes is the most common cause of cotton-wool spots. The presence of more than eight cotton-wool spots has been associated with a higher risk of the more severe form of diabetic retinopathy known as proliferative diabetic retinopathy (PDR). Cotton-wool spots are also a common sign of infection with the human immunodeficiency virus (HIV). They are present in more than half of the people with full-blown AIDS. Their presence can be an important sign of the severity of HIV-related disease. file:///c /Documents%20and%20Settings/Det/My%20Documents/...PatientResources/Retina_and_Vitreous/CottonWoolSpots.html1/8/ :23:28 AM
14 Floaters and Flashes Floaters and Flashes Small specks or clouds moving in your field of vision as you look at a blank wall or a clear blue sky are known as floaters. Most people have some floaters normally but do not notice them until they become numerous or more prominent. In most cases, floaters are part of the natural aging process. Floaters look like cobwebs, squiggly lines, or floating bugs. They appear to be in front of the eye but are actually floating inside. As we get older, the vitreous (the clear, gel-like substance that fills the inside of the eye) tends to shrink slightly and detach from the retina, forming clumps within the eye. What you see are the shadows these clumps cast on the retina, the light-sensitive nerve layer lining the back of the eye. The appearance of flashing lights comes from the traction of the vitreous gel on the retina at the time of vitreous separation. Flashes look like twinkles or lightning streaks. You may have experienced the same sensation if you were ever hit in the eye and saw stars. Floaters can get in the way of clear vision, often when reading. Try looking up and then down to move the floaters out of the way. While some floaters may remain, many of them will fade over time. Floaters and flashes are sometimes associated with retinal tears. When the vitreous shrinks, it can pull on the retina and cause a tear. A torn retina is a serious problem. It can lead to a retinal detachment and blindness. If new floaters appear suddenly or you see sudden flashes of light, see an ophthalmologist (Eye M.D.) immediately. file:///c /Documents%20and%20Settings/Det/My%20Documents/M.../PatientResources/Retina_and_Vitreous/FloatersFlashes.html1/8/ :23:28 AM
15 Detached and Torn Retina Detached and Torn Retina A retinal detachment is a very serious problem that usually causes blindness unless treated. The appearance of flashing lights, floating objects, or a gray curtain moving across the field of vision are all indications of a retinal detachment. If any of these occur, see an ophthalmologist (Eye M.D.) right away. As one gets older, the vitreous (the clear, gel-like substance that fills the inside of the eye) tends to shrink slightly and take on a more watery consistency. Sometimes as the vitreous shrinks, it exerts enough force on the retina to make it tear. Retinal tears can lead to a retinal detachment. Fluid vitreous, passing through the tear, lifts the retina off the back of the eye like wallpaper peeling off a wall. Laser surgery or cryotherapy (freezing) are often used to seal retinal tears and prevent detachment. If the retina is detached, it must be reattached before sealing the retinal tear. There are three ways to repair retinal detachments. Pneumatic retinopexy involves injecting a special gas bubble into the eye that pushes on the retina to seal the tear. The scleral buckle procedure requires the fluid to be drained from under the retina before a flexible piece of silicone is sewn on the outer eye wall to give support to the tear while it heals. Vitrectomy surgery removes the vitreous gel from the eye, replacing it with a gas bubble, which is slowly replaced by the body s fluids. file:///c /Documents%20and%20Settings/Det/My%20Documents/...ientResources/Retina_and_Vitreous/DetachedTornRetina.html1/8/ :23:28 AM
16 Central Retinal Vein Occlusion Central Retinal Vein Occlusion You probably know that high blood pressure and other vascular diseases pose risks to overall health, but you may not know that they can affect eyesight by damaging the veins in the eye. Central retinal vein occlusion (CRVO) blocks the main vein in the retina, the light-sensitive nerve layer at the back of the eye. The blockage causes the walls of the vein to leak blood and excess fluid into the retina. When this fluid collects in the macula (the area of the retina responsible for central vision), vision becomes blurry. Floaters in your vision are another symptom of CRVO. When retinal blood vessels are not working properly, the retina grows new fragile vessels that can bleed into the vitreous, the fluid that fills the center of the eye. Blood in the vitreous clumps and is seen as tiny dark spots, or floaters, in the field of vision. In severe cases of CRVO, the blocked vein causes painful pressure in the eye. Retinal vein occlusions commonly occur with glaucoma, diabetes, age-related vascular disease, high blood pressure, and blood disorders. The first step of treatment is finding what is causing the vein blockage. There is no cure for CRVO. Your ophthalmologist (Eye M.D.) may recommend a period of observation, since hemorrhages and excess fluid often subside on their own. Laser surgery may be effective in preventing further bleeding into the vitreous or for treating glaucoma, but it cannot remove a hemorrhage or cure glaucoma once it is present. New experimental treatments are now under investigation. file:///c /Documents%20and%20Settings/Det/My%20Documents/...rces/Retina_and_Vitreous/CentralRetinalVeinOcclusion.html1/8/ :23:28 AM
17 Anti-VEGF Treatment for Non-AMD Disease Anti-VEGF Treatment for Non-AMD Disease Researchers have found that a chemical called vascular endothelial growth factor, or VEGF, is critical in causing abnormal blood vessels to grow under the retina. Scientists have developed several new drugs that can block the trouble-causing VEGF known as anti-vegf drugs. They help block abnormal blood vessels, slow their leakage, and help reduce vision loss. Certain anti-vegf treatments are approved for a condition known as wet age-related macular degeneration (AMD), in which abnormal blood vessels grow underneath the retina. These unhealthy vessels leak blood and fluid that can swell and scar the macula (the central part of the retina), and vision loss may be rapid and severe. Since anti-vegf therapies have shown good potential for slowing vascular leakage and preventing vision loss associated with wet AMD, ophthalmologists (Eye M.D.s) are using them to treat other causes of macular edema. If your ophthalmologist has diagnosed you with diabetic retinopathy, retinal venous occlusion, or other conditions, you may benefit from anti-vegf treatment if other therapies are not producing the desired results or if your ophthalmologist thinks that anti-vegf therapy is the best first course of action. Treatment with the anti-vegf drug is usually performed by injecting the medicine with a very fine needle into the back portion of your eye. Your ophthalmologist will clean your eye to prevent infection and will administer an anesthetic into your eye to reduce pain. Usually, patients receive multiple anti- VEGF injections over the course of many months. There is a small risk of complications with anti- VEGF treatment, usually resulting from the injection itself. However, for most people, the benefits of this treatment outweigh the small risk of complications. file:///c /Documents%20and%20Settings/Det/My%20Document...Retina_and_Vitreous/AntiVEGFTreatmentNonAMDDisease.html1/8/ :23:28 AM
18 Face-Down Recovery After Retinal Surgery Face-Down Recovery After Retinal Surgery The retina is a layer of light-sensing cells lining the back of your eye. As light enters your eye, the retina converts the rays into signals that are sent through the optic nerve to your brain, where they are recognized as images. To repair a damaged or detached retina, your ophthalmologist may remove some of your eye s vitreous (the gel-like substance that fills the inside of your eye) and inject a gas bubble into the eye to take its place. This bubble holds the retina in place as it re-attaches to the back of your eye. With time, the bubble disappears and is replaced with your normal eye fluid. You must keep your head facing downward or turned to a particular side for up to several weeks after surgery so that the bubble will remain in the right position. In some cases the positioning requirements are full-time, and in others it may be part-time. If you lie in the wrong position, such as face-up, pressure may be applied to other parts of the eye, causing further problems like cataract or glaucoma. To assist you in keeping your face pointed downward, special equipment is available, including adjustable facedown chairs, tabletop face cradles, face-down pillows, and mirrors. file:///c /Documents%20and%20Settings/Det/My%20Documents/...ina_and_Vitreous/FaceDownRecoveryAfterRetinalSurgery.html1/8/ :23:28 AM
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
Flashers and Floaters
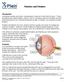 Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Age-Related Macular Degeneration (AMD)
 Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Introduction How the eye works
 1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
GENERAL INFORMATION DIABETIC EYE DISEASE
 GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
Brampton Hurontario Street Brampton, ON L6Y 0P6
 Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Eye Disease
 Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Retinal Tears and Detachments
 Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
Diabetic Retinopathy
 Diabetic Retinopathy Introduction People with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina that is caused by diabetes.
Diabetic Retinopathy Introduction People with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina that is caused by diabetes.
Diabetic Retinopathy A Presentation for the Public
 Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
X-Plain Diabetic Retinopathy Reference Summary
 X-Plain Diabetic Retinopathy Reference Summary Introduction Patients with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina
X-Plain Diabetic Retinopathy Reference Summary Introduction Patients with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Information for Patients. Retinal Detachment
 Information for Patients Retinal Detachment Manchester Royal Eye Hospital Retinal services Your eye doctor has told you that you have a retinal detachment. This leaflet will help you understand your condition
Information for Patients Retinal Detachment Manchester Royal Eye Hospital Retinal services Your eye doctor has told you that you have a retinal detachment. This leaflet will help you understand your condition
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? WHAT CAUSES DIABETIC RETINOPATHY? WHAT ARE THE STAGES OF DIABETIC RETINOPATHY?
 Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Retinal detachment When to see a doctor How retinal detachment occurs
 Retinal detachment Retinal detachment describes an emergency situation in which a thin layer of tissue (the retina) at the back of the eye pulls away from its normal position. Retinal detachment separates
Retinal detachment Retinal detachment describes an emergency situation in which a thin layer of tissue (the retina) at the back of the eye pulls away from its normal position. Retinal detachment separates
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
Understanding Diabetic Retinopathy
 Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy Information
 http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Age-Related. macular degeneration.
 Age-Related Macular Degeneration This pamphlet is designed to help people with age-related macular degeneration and their families better understand the disease. It describes the causes, symptoms, diagnosis,
Age-Related Macular Degeneration This pamphlet is designed to help people with age-related macular degeneration and their families better understand the disease. It describes the causes, symptoms, diagnosis,
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
INFORMED CONSENT FOR AVASTIN TM (BEVACIZUMAB) INTRAVITREAL INJECTION
 INFORMED CONSENT FOR AVASTIN TM (BEVACIZUMAB) INTRAVITREAL INJECTION INDICATIONS: Age-related macular degeneration (AMD) is the leading cause of blindness in people over 50 years of age. It is caused by
INFORMED CONSENT FOR AVASTIN TM (BEVACIZUMAB) INTRAVITREAL INJECTION INDICATIONS: Age-related macular degeneration (AMD) is the leading cause of blindness in people over 50 years of age. It is caused by
Treatment of Retinal Vein Occlusion (RVO)
 Manchester Royal Eye Hospital Medical Retina Services Information for Patients Treatment of Retinal Vein Occlusion (RVO) What is a Retinal Vein Occlusion (RVO)? The retina is the light sensitive layer
Manchester Royal Eye Hospital Medical Retina Services Information for Patients Treatment of Retinal Vein Occlusion (RVO) What is a Retinal Vein Occlusion (RVO)? The retina is the light sensitive layer
DIABETIC RETINOPATHY
 DIABETIC RETINOPATHY INTRODUCTION Diabetic Retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with Diabetes
DIABETIC RETINOPATHY INTRODUCTION Diabetic Retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with Diabetes
Retinal Detachments
 Retinal Detachments What is a retinal detachment? The retina is the light sensitive layer covering the inside of the back of the eye. It is analogous to the film in a camera. The retina has many layers.
Retinal Detachments What is a retinal detachment? The retina is the light sensitive layer covering the inside of the back of the eye. It is analogous to the film in a camera. The retina has many layers.
Retinal Detachment PATIENT EDUCATION
 Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
Age-Related Eye Diseases and Conditions. Jonathan M. Frantz, MD, F.A.C.S. Cataract and Refractive Surgeon
 Age-Related Eye Diseases and Conditions Jonathan M. Frantz, MD, F.A.C.S. Cataract and Refractive Surgeon Vision Changes Patients notice vision changes with aging. Many changes are common and can often
Age-Related Eye Diseases and Conditions Jonathan M. Frantz, MD, F.A.C.S. Cataract and Refractive Surgeon Vision Changes Patients notice vision changes with aging. Many changes are common and can often
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Intravitreal Injection
 for patients Eye Clinic Ipswich Hospital Tel: 01473 703230 Intravitreal Injection What is an intravitreal injection? An intravitreal injection is the injection of a drug into the vitreous body (the jelly
for patients Eye Clinic Ipswich Hospital Tel: 01473 703230 Intravitreal Injection What is an intravitreal injection? An intravitreal injection is the injection of a drug into the vitreous body (the jelly
Treatment of Age Related Macular Degeneration (AMD) by Intravitreal Injection
 Information for Patients Manchester Royal Eye Hospital Medical Retina Services Treatment of Age Related Macular Degeneration (AMD) by Intravitreal Injection What is age related macular degeneration (AMD)?
Information for Patients Manchester Royal Eye Hospital Medical Retina Services Treatment of Age Related Macular Degeneration (AMD) by Intravitreal Injection What is age related macular degeneration (AMD)?
OAKLEIGH EYE CENTRE. THE EYE Before looking at diabetic retinopathy it is important to understand what the healthy eye looks like and how it works.
 ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
EYLEA. (aflibercept solution for injection) Patient Guide
 EYLEA (aflibercept solution for injection) Patient Guide Eylea is used to treat Wet Age-Related Macular Degeneration (Wet AMD), macular oedema secondary to Branch and Central Retinal Vein Occlusion (BRVO
EYLEA (aflibercept solution for injection) Patient Guide Eylea is used to treat Wet Age-Related Macular Degeneration (Wet AMD), macular oedema secondary to Branch and Central Retinal Vein Occlusion (BRVO
Information for patients
 Information for patients Intravitreal Anti-VEGF Treatment (vascular endothelial growth factor) This leaflet gives you information that will help you decide whether to have intravitreal treatment. It also
Information for patients Intravitreal Anti-VEGF Treatment (vascular endothelial growth factor) This leaflet gives you information that will help you decide whether to have intravitreal treatment. It also
Ophthamology Directorate. Eye Injection for Macular Disorders Information for Patients
 Ophthamology Directorate Eye Injection for Macular Disorders Information for Patients As discussed at your appointment today, please call the Medical Retinal Services Coordinator as soon as possible (within
Ophthamology Directorate Eye Injection for Macular Disorders Information for Patients As discussed at your appointment today, please call the Medical Retinal Services Coordinator as soon as possible (within
What you can expect with OZURDEX
 Important Information About Macular Edema Following Branch or Central Retinal Vein Occlusion (RVO) and Treatment For patients with RVO What you can expect with OZURDEX Approved Use OZURDEX (dexamethasone
Important Information About Macular Edema Following Branch or Central Retinal Vein Occlusion (RVO) and Treatment For patients with RVO What you can expect with OZURDEX Approved Use OZURDEX (dexamethasone
RVO RETINAL VEIN OCCLUSION
 RVO RETINAL VEIN OCCLUSION A guide to understanding RVO Take some time to learn about RVO - it may help you hold on to your vision Retinal vein occlusion is a common disorder of the retina and a leading
RVO RETINAL VEIN OCCLUSION A guide to understanding RVO Take some time to learn about RVO - it may help you hold on to your vision Retinal vein occlusion is a common disorder of the retina and a leading
VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz)
 PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
Diabetic Retinopathy. What should know
 Diabetic Retinopathy What should know Diabetic Retinopathy: What you should know This booklet is for people with diabetic retinopathy and their families and friends. It provides information about diabetic
Diabetic Retinopathy What should know Diabetic Retinopathy: What you should know This booklet is for people with diabetic retinopathy and their families and friends. It provides information about diabetic
Macular Hole. Helpline
 Macular Hole The retina is a light-sensitive layer of tissue lining the back of the eye. The macula is a small area at the centre of the retina responsible for all of our central vision, most of our colour
Macular Hole The retina is a light-sensitive layer of tissue lining the back of the eye. The macula is a small area at the centre of the retina responsible for all of our central vision, most of our colour
Detached and Torn. Se Habla Español
 Detached and Torn Retina www.fleyedocs.com Se Habla Español Retinal Detachments Occur in 1 Out of 10,000 Americans Each Year A retinal detachment is not as common as other eye conditions such as glaucoma
Detached and Torn Retina www.fleyedocs.com Se Habla Español Retinal Detachments Occur in 1 Out of 10,000 Americans Each Year A retinal detachment is not as common as other eye conditions such as glaucoma
MAGNITUDE OF DIABETIC EYE DISEASE IN INDIA
 Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Uveitis. There are different types of uveitis:
 Uveitis Uveitis The uvea is the middle layer in the eye sandwiched between the retina (innermost layer) and the sclera (outermost layer). The uvea contains many blood vessels that carry blood to and from
Uveitis Uveitis The uvea is the middle layer in the eye sandwiched between the retina (innermost layer) and the sclera (outermost layer). The uvea contains many blood vessels that carry blood to and from
Patient & Family Guide. Diabetes and the Eye. Aussi disponible en français : Le diabète et les yeux (FF )
 Patient & Family Guide Diabetes and the Eye 2017 Aussi disponible en français : Le diabète et les yeux (FF85-1784) www.nshealth.ca Diabetes and the Eye What is diabetes? Diabetes is a disease in which
Patient & Family Guide Diabetes and the Eye 2017 Aussi disponible en français : Le diabète et les yeux (FF85-1784) www.nshealth.ca Diabetes and the Eye What is diabetes? Diabetes is a disease in which
Patient information. Retinal Detachment Surgery St. Paul s Eye Unit PIF 024 V7
 Patient information Retinal Detachment Surgery St. Paul s Eye Unit PIF 024 V7 Your eye specialist has advised you to have retinal detachment surgery. This leaflet gives you information that will help you
Patient information Retinal Detachment Surgery St. Paul s Eye Unit PIF 024 V7 Your eye specialist has advised you to have retinal detachment surgery. This leaflet gives you information that will help you
Photodynamic Therapy (PDT) for agerelated
 Page 1 of 5 Photodynamic Therapy (PDT) for agerelated eye conditions Introduction This leaflet gives you information about Photodynamic Therapy (PDT) for the age--related eye conditions macular degeneration
Page 1 of 5 Photodynamic Therapy (PDT) for agerelated eye conditions Introduction This leaflet gives you information about Photodynamic Therapy (PDT) for the age--related eye conditions macular degeneration
ILUVIEN 190 micrograms intravitreal implant in applicator (fluocinolone acetonide)
 ILUVIEN 190 micrograms intravitreal implant in applicator (fluocinolone acetonide) Read all of this information carefully before you are given this medicine because it contains important information for
ILUVIEN 190 micrograms intravitreal implant in applicator (fluocinolone acetonide) Read all of this information carefully before you are given this medicine because it contains important information for
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015
 Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
Diabetes Eye Q Quiz. 1) Diabetes is the leading cause of new blindness among adults in the US under the age of 74.
 Diabetes Eye Q Quiz From 1997 to 2011, the number of adults with diagnosed diabetes who reported visual impairment, that is, trouble seeing even with their glasses or contact lenses, increased from 2.7
Diabetes Eye Q Quiz From 1997 to 2011, the number of adults with diagnosed diabetes who reported visual impairment, that is, trouble seeing even with their glasses or contact lenses, increased from 2.7
Cataract Surgery. This reference summary will help you understand what cataracts are and how they can be treated surgically.
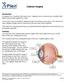 Cataract Surgery Introduction A cataract is a clouding of the eye s lens. Cataracts are a common eye condition that affect many people aged 65 or older. Your doctor may recommend cataract surgery to enhance
Cataract Surgery Introduction A cataract is a clouding of the eye s lens. Cataracts are a common eye condition that affect many people aged 65 or older. Your doctor may recommend cataract surgery to enhance
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
What is Age-Related Macular Degeneration?
 Intravitreal Injections Eylea / Lucentis Patient Information What is Age-Related Macular Degeneration? Age-related macular degeneration (AMD) is an eye condition found in older people, which may lead to
Intravitreal Injections Eylea / Lucentis Patient Information What is Age-Related Macular Degeneration? Age-related macular degeneration (AMD) is an eye condition found in older people, which may lead to
AgePage. Aging And Your Eyes. Steps To Protect Your Eyesight
 National Institute on Aging AgePage Aging And Your Eyes Are you holding the newspaper farther away from your eyes than you used to? Join the crowd age can bring changes that affect your eyesight. Some
National Institute on Aging AgePage Aging And Your Eyes Are you holding the newspaper farther away from your eyes than you used to? Join the crowd age can bring changes that affect your eyesight. Some
When Eyes Show Their Age
 When Eyes Show Their Age A guide to preserving the gift of sight for as long as possible with the compliments of Division of Health Services Diocese of Camden Expect Vision Changes Some loss of visual
When Eyes Show Their Age A guide to preserving the gift of sight for as long as possible with the compliments of Division of Health Services Diocese of Camden Expect Vision Changes Some loss of visual
GHPI0100_06_10 Contact: Ophthalmology Review due: June What is a Cataract?
 GHPI0100_06_10 Contact: Ophthalmology Review due: June 2013 What is a Cataract? Further information If you or a relative have access to the internet, you can use the following websites for further information:
GHPI0100_06_10 Contact: Ophthalmology Review due: June 2013 What is a Cataract? Further information If you or a relative have access to the internet, you can use the following websites for further information:
Diabetic Retinopathy What You Should Know. U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute
 Diabetic Retinopathy What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research
Diabetic Retinopathy What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research
Outline. Preventing & Treating Diabetes Related Blindness. Eye Care Center Doctors. Justin Kanoff, MD. Eye Care Center of Northern Colorado
 Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
Ophthalmology. Ophthalmology Services
 Ophthalmology Ophthalmology Services The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems
Ophthalmology Ophthalmology Services The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems
Glaucoma. Cornea. Iris
 Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Vitrectomy for diabetic vitreous haemorrhage
 Vitrectomy for diabetic vitreous haemorrhage Why have I been given this leaflet? If you have been given this leaflet it is likely that you have been asked to think about whether you want to go ahead with
Vitrectomy for diabetic vitreous haemorrhage Why have I been given this leaflet? If you have been given this leaflet it is likely that you have been asked to think about whether you want to go ahead with
Macular Hole Surgery
 What is the macula? Macular Hole Surgery The macula is the part of the retina that enables us to make out things clearly and see colours. Rays of light enter the eye and are focused on the macular area
What is the macula? Macular Hole Surgery The macula is the part of the retina that enables us to make out things clearly and see colours. Rays of light enter the eye and are focused on the macular area
The Foundation WHAT IS THE RETINA?
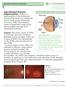 Age-Related Macular Degeneration (AMD) is a deterioration of the retina and choroid that leads to a substantial loss in visual acuity (sharpness of vision). AMD is the leading cause of significant visual
Age-Related Macular Degeneration (AMD) is a deterioration of the retina and choroid that leads to a substantial loss in visual acuity (sharpness of vision). AMD is the leading cause of significant visual
Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection
 Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection Kenalog/SS/ST/04.2012/v1.1 review 05.2013 Page 1 Introduction Your doctor has found that you have leakage of
Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection Kenalog/SS/ST/04.2012/v1.1 review 05.2013 Page 1 Introduction Your doctor has found that you have leakage of
Vision & Age - 40 s and 50 s Eyes
 Vision & Age - 40 s and 50 s Eyes You rely on your sight to enjoy life to the fullest, but as you reach your 40 s and 50 s, you may notice your vision starting to change. As you age, the lens within your
Vision & Age - 40 s and 50 s Eyes You rely on your sight to enjoy life to the fullest, but as you reach your 40 s and 50 s, you may notice your vision starting to change. As you age, the lens within your
Treatment of wet macular degeneration by intravitreal injection with Ranibizumab (Lucentis) or Aflibercept (Eylea): Information and consent
 Patient information Treatment of wet macular degeneration by intravitreal injection with Ranibizumab (Lucentis) or Aflibercept (Eylea): Information and consent Introduction You have an eye condition called
Patient information Treatment of wet macular degeneration by intravitreal injection with Ranibizumab (Lucentis) or Aflibercept (Eylea): Information and consent Introduction You have an eye condition called
The Eye: Homeostatic Imbalance. Ms. Nobis s 3rd hour Anatomy & Physiology
 The Eye: Homeostatic Imbalance Ms. Nobis s 3rd hour Anatomy & Physiology Your assignment... 1. 2. 3. Find the slide with your name in the notes section at the bottom (they are alphabetical by last name).
The Eye: Homeostatic Imbalance Ms. Nobis s 3rd hour Anatomy & Physiology Your assignment... 1. 2. 3. Find the slide with your name in the notes section at the bottom (they are alphabetical by last name).
RETINAL SURGERY. Shifa. Shifa Ophthalmology Clinic Sector H-8/4 Islamabad - Pakistan For Appointment & Information:
 RETINAL SURGERY An Informatory Guide for Retinal Disorders and Surgeries Shifa International Hospitals Ltd. Shifa Ophthalmology Clinic Sector H-8/4 Islamabad - Pakistan For Appointment & Information: 051-8464646
RETINAL SURGERY An Informatory Guide for Retinal Disorders and Surgeries Shifa International Hospitals Ltd. Shifa Ophthalmology Clinic Sector H-8/4 Islamabad - Pakistan For Appointment & Information: 051-8464646
Patient Information Cataract Surgery
 Patient Information Cataract Surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Patient Information Cataract Surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Retina of Auburn & Metro-Columbus
 INFORMED CONSENT FOR VITRECTOMY SURGERY What is a vitrectomy? Vitrectomy is the surgical removal of the vitreous gel from the middle of the eye. This procedure may be done for several reasons. To remove
INFORMED CONSENT FOR VITRECTOMY SURGERY What is a vitrectomy? Vitrectomy is the surgical removal of the vitreous gel from the middle of the eye. This procedure may be done for several reasons. To remove
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV)
 Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV) About photodynamic therapy for Retinal Conditions The macula is the central part of the retina at
Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV) About photodynamic therapy for Retinal Conditions The macula is the central part of the retina at
Package leaflet: information for the user. OZURDEX 700 micrograms intravitreal implant in applicator dexamethasone
 Package leaflet: information for the user OZURDEX 700 micrograms intravitreal implant in applicator dexamethasone Read all of this leaflet carefully before you are given this medicine because it contains
Package leaflet: information for the user OZURDEX 700 micrograms intravitreal implant in applicator dexamethasone Read all of this leaflet carefully before you are given this medicine because it contains
Floaters & Flashes. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Floaters & Flashes An information guide Floaters & Flashes What are floaters? Floaters are small specks or clouds in your field of vision.
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Floaters & Flashes An information guide Floaters & Flashes What are floaters? Floaters are small specks or clouds in your field of vision.
Chapter 32. Hearing, Speech, and Vision Problems. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 32 Hearing, Speech, and Vision Problems Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 32.1 Define the key terms and key abbreviations in this chapter. Describe the common ear, speech,
Chapter 32 Hearing, Speech, and Vision Problems Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 32.1 Define the key terms and key abbreviations in this chapter. Describe the common ear, speech,
Myopia and pathological myopia. Fundus Photo, Right Eye (OD)
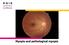 Myopia and pathological myopia Fundus Photo, Right Eye (OD) Contents 3 What is myopia and pathological myopia 3 How does the eye focus light? 3 What is myopia? 4 Development of myopia 4 What causes myopia?
Myopia and pathological myopia Fundus Photo, Right Eye (OD) Contents 3 What is myopia and pathological myopia 3 How does the eye focus light? 3 What is myopia? 4 Development of myopia 4 What causes myopia?
Repairing Macular Hole and Macular Pucker
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/revealing-retina/repairing-macular-hole-and-macular-pucker/3924/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/revealing-retina/repairing-macular-hole-and-macular-pucker/3924/
Screening saves sight. The importance of regular testing for diabetic retinopathy
 Screening saves sight The importance of regular testing for diabetic What is diabetic? The only way of knowing whether you have diabetic is by having an eye examination How can diabetic affect your vision?
Screening saves sight The importance of regular testing for diabetic What is diabetic? The only way of knowing whether you have diabetic is by having an eye examination How can diabetic affect your vision?
Retinal detachment. What is retinal detachment?
 Patient information Retinal detachment We hope this information will answer some of your questions about retinal detachment. If there is anything you do not understand, or if you have any concerns, please
Patient information Retinal detachment We hope this information will answer some of your questions about retinal detachment. If there is anything you do not understand, or if you have any concerns, please
3/14/2016. Fact. Nutrition for Your Eyes. Eyes are highly metabolic organs. Deep Green Vegetables & Bright Fruits. Lutein.
 Fact Good nutrition is essential for eye health Nutrition for Your Eyes Deborah Willcox, RD, LMNT Eyes are highly metabolic organs Deep Green Vegetables & Bright Fruits This means our eyes require a lot
Fact Good nutrition is essential for eye health Nutrition for Your Eyes Deborah Willcox, RD, LMNT Eyes are highly metabolic organs Deep Green Vegetables & Bright Fruits This means our eyes require a lot
Preparing for laser treatment for diabetic retinopathy and maculopathy
 Preparing for laser treatment for diabetic retinopathy and maculopathy Information for patients Preparing for laser treatment for diabetic retinopathy and maculopathy. This leaflet sets out to answer the
Preparing for laser treatment for diabetic retinopathy and maculopathy Information for patients Preparing for laser treatment for diabetic retinopathy and maculopathy. This leaflet sets out to answer the
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient
 Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Ophthalmology. Glaucoma
 Ophthalmology Glaucoma The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems ranging
Ophthalmology Glaucoma The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems ranging
Cataracts are a normal feature of aging. About half of adults aged 65 to 74 have cataracts.
 Cataract Mr Constable specialises in modern small incision phacoemulsification surgery for the treatment of cataracts using the latest microincision systems and implants. Most patients with cataracts can
Cataract Mr Constable specialises in modern small incision phacoemulsification surgery for the treatment of cataracts using the latest microincision systems and implants. Most patients with cataracts can
PATIENT INFORMATION LEAFLET MACULAR HOLE. What is the macula?
 What is the macula? The back of the eye has a light-sensitive lining called the retina, similar to the film in a camera. Light is focused through the eye onto the retina, allowing us to see. The centre
What is the macula? The back of the eye has a light-sensitive lining called the retina, similar to the film in a camera. Light is focused through the eye onto the retina, allowing us to see. The centre
Glaucoma. What is glaucoma? Eye Words to Know. What causes glaucoma?
 2014 2015 Glaucoma What is glaucoma? Glaucoma is a disease that damages your eye s optic nerve. It usually happens when fluid builds up in the front part of your eye. That extra fluid increases the pressure
2014 2015 Glaucoma What is glaucoma? Glaucoma is a disease that damages your eye s optic nerve. It usually happens when fluid builds up in the front part of your eye. That extra fluid increases the pressure
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
Cataract. A cataract is a clouding of the lens in your eye. It
 Cataract A cataract is a clouding of the lens in your eye. It affects your vision. Cataracts are very common in older people. By age 80, more than half of all Americans either have a cataract or have had
Cataract A cataract is a clouding of the lens in your eye. It affects your vision. Cataracts are very common in older people. By age 80, more than half of all Americans either have a cataract or have had
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Retina. Chapter 4. The Eyes Have It. by Tim Root
 Chapter 4 Retina The Eyes Have It There are certain rules of etiquette you should follow when performing PRP laser. For example, never say you re Killing, Burning, Zapping, or Liquidating the retina by
Chapter 4 Retina The Eyes Have It There are certain rules of etiquette you should follow when performing PRP laser. For example, never say you re Killing, Burning, Zapping, or Liquidating the retina by
Retinal detachment. What is retinal detachment?
 Patient information We hope this information will answer some of your questions about retinal detachment. If there is anything you do not understand, or if you have any concerns, please tell us as it is
Patient information We hope this information will answer some of your questions about retinal detachment. If there is anything you do not understand, or if you have any concerns, please tell us as it is
Retinal detachment surgery
 Retinal detachment surgery Information for patients Ophthalmology (Vitreal Retina) Large Print This booklet gives you information about retinal detachment surgery. It is important that you understand this
Retinal detachment surgery Information for patients Ophthalmology (Vitreal Retina) Large Print This booklet gives you information about retinal detachment surgery. It is important that you understand this
Information for Patients. Macular Hole
 Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Macular Hole Your eye doctor has told you that you have a macular hole. This leaflet will help you understand your condition
Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Macular Hole Your eye doctor has told you that you have a macular hole. This leaflet will help you understand your condition
The Foundation WHAT IS THE RETINA?
 The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Branch Retinal Vein Occlusion Retinal vein occlusions occur when there
The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Branch Retinal Vein Occlusion Retinal vein occlusions occur when there
