Association of Renal Graft Survival with Matching at the HLA-DR Locus
|
|
|
- Oswin Pearson
- 6 years ago
- Views:
Transcription
1 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 14, No. 6 Copyright 1984, Institute for Clinical Science, Inc. Association of Renal Graft Survival with Matching at the HLA-DR Locus KARLA J. LAUENSTEIN, M.S., FREDERICK R. DAVEY, M.D., CHARLENE HUBBELL, B.S., ANN BURLESON, R.N., RICHARD P. OATES, Ph.D., and RICHARD L. BURLESON, M.D. Division o f Clinical Pathology, and Departments of Surgery, Urology, and Preventive Medicine, SUNY Upstate Medical Center, Syracuse, NY ABSTRACT The influence of HLA-DR antigen matching in 70 cadaver transplants was studied for up to four years. The overall cumulative renal graft survival at one year was 62 percent, and at two and four years it was 60 percent. The one, two, and four year cumulative graft survival for patients receiving one or two HLA-DR antigen matched grafts was 74 percent, 69 percent, and 69 percent, respectively. In contrast, the one, two, and four year cumulative graft survival for patients receiving zero HLA-DR antigen matched grafts was 51 percent, 47 percent, and 47 percent, respectively. The cumulative graft survival for patients receiving one or two HLA-DR antigen matched grafts was significantly different (p < 0.05) than for patients receiving zero HLA-DR antigen matched grafts. No significant differences in the distribution of other prognostic factors were observed between patients receiving one or two HLA-DR antigen matched grafts and patients receiving zero HLA-DR antigen matched grafts. The present authors conclude that matching for HLA-DR antigens exerts an independent beneficial effect on renal graft survival in transplant patients, most of whom have been previously transfused. Introduction In humans, the human lymphocyte antigen (HLA) genes encode for the major histocompatibility antigens which are normally present on many tissues of the body.11 In rodents, the major histocompatibility antigens (H2) are the primary determinants which affect the length of survival of skin, renal or tumor allografts.11 Therefore, it would be expected that matching for HLA antigens in humans would also enhance survival of cadaveric renal grafts. Although the effect of matching for HLA-A and B or Class I antigens has been correlated to survival of cadaveric renal grafts, the association has been weak.18 Other fac /84/ $01.20 Institute for Clinical Science, Inc.
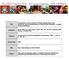
2 R E N A L G R A F T SU RV IV A L tors have also been reported to affect the survival of cadaveric renal grafts and, thus, may lessen the effect of matching for HLA-A and B locus antigens. These factors include the sex19 and age of the recipient,28 the ABO types of the recip ients and donors,18 the num ber of trans fusions the recipients have received prior to transplantation,10 the presence of lymphocytotoxic antibodies in the recipients serum,17 and the presence of warm anti bodies in the recipients serum reacting specifically with lym phocytes from the donor.21 Several reports have indicated that th ere is a clear association betw een matching for HLA-DR and survival of cadaveric renal grafts.16,26 H ow ever, other studies have not confirmed these findings.9,12 In addition, the results of a large international collaborative study involving over 2000 cadaveric transplants were disappointing.20 No significant cor relation between HLA-DR matching and renal graft survival was observed when the overall data from North America and Europe were analyzed. However, when the data from North American transplant centers were analyzed alone, a weak cor relation between HLA-DR matching and renal graft survival was observed. Since there exists a variation in HLA-DR typ ing techniques and in treatm en t of patients among the various participating hospital centers in large collaborative studies, several investigators have now examined the effects of HLA-DR match ing on cadaveric graft survival within a single transplant center.3,13 The purpose of this rep o rt is to describe the usefulness of HLA-DR typ ing as a prognostic factor in patients transplanted with a cadaveric renal graft at the SUNY Upstate M edical Center. This report confirm s our prelim inary observations indicating that DR match ing is associated with increased graft sur vival JZL Age of Recipients Figure 1. grafts. A ge of re c ip ie n ts of cadaveric re n a l Methods and Materials P a t ie n t s The study group consisted of 70 indi viduals, 49 males and 21 females with an age range of nine to 61 years (figure 1), treated at the SUNY U pstate M edical C enter for end stage renal disease between Septem ber 1, 1978 and Decem ber 31, Sixty-four patients received a primary renal transplant, whereas six patients received a second transplant. From 1978 to 1981, cadaveric kidneys removed in Upstate New York under the direction of the transplant team w ere m aintained using a Belzer perfusion apparatus and a modified albumin per fusate.5 Kidneys obtained from other centers, during this period, were transfered upon arrival at the Upstate Medical C en ter to the Belzer apparatus. A fter 1981, kidneys w ere m aintained on a MOX-lOO Waters Perfusion machine.
3 4 5 2 LAUENSTEIN, DAVEY, HUBBELL, BURLESON, OATES, AND BURLESON Immunosuppression was initiated on the day of transplantation for recipients of cadaveric kidneys. Therapy usually consisted of a combination of azathioprine and steroids given by established protocols that provide for high initial doses with gradual tapering of the dose of steroids to low maintenance levels.6 After seven days, the patients were switched from methylprednisolone to prednisone. In addition, episodes of rejection were treated with one gram i.v. doses of methylprednisolone and with irradiation of the graft during the first rejection episode. After 1981, patients with sustained episodes of rejection were given antithymocyte globulin. HLA a n d ABO T y p i n g If accepted as a potential renal transplant recipient, the patient s ABO erythrocyte type and the HLA-A and B lymphocyte phenotype were determined using standardized methods.24,25 HLA-A and B lymphocytic antisera were obtained.* All donor-recipient pairs were serocrossmatched immediately prior to transplant and a negative result was a prerequisite for transplantation. HLA- DR typing was performed on cadaveric lymphocytes from lymph nodes, spleen, or freshly drawn heparinized blood. Mononuclear cells were isolated from other blood elements using a Hypaque- Ficoll gradient and centrifugation at 400 X g for 30 minutes. Non-T cells were separated from T cells by incubating mononuclear cells (previously harvested from the interface layer of the Hypaque- Ficoll gradient) on nylon-wool columns.25 T cells were non-adherent to the nylon-wool columns, whereas non-t cells were recovered by adding three to five ml of Hanks balanced salt solution with * National Institutes of H ealth, UCLA Tissue Typing L aboratory an d Bio-Accugenics, In c., G arden Grove, CA percent fetal calf serum to the column and agitating the nylon wool column. The adherent non-t cells were collected and shown to have less than five percent T cells. Non-T cells were typed for HLA- DR antigens by incubating cells in microtiter plates with HLA-DR specific antisera obtained from the UCLA Tissue Typing Laboratories. Eight different HLA-DR antigens (HLA-DR 1-8) were identified by this procedure. In 44 of 70 (63 percent) recipients, two HLA-DR antigens were determined and in 26 of 70 (37 percent) one HLA-DR antigen was observed. In 41 of 70 (59 percent) of the donors two HLA-DR antigens were found, and in 29 of 70 (41 percent) one antigen was observed. S t a t i s t i c a l A n a l y s i s The distribution of known prognostic factors between HLA-DR one or two antigen matched donor-recipient pairs and zero antigen matched donor-recipient pairs was compared utilizing thé chisquare test and when appropriate the Fisher s exact test.8 The life table method is the analytical method of choice in prospective studies where time until the occurrence of a defined event is observed. In the present study, the endpoint was renal graft rejection. Patients entered the study at the time of their graft and were followed prospectively for varying lengths of time. The life table analysis sequentially determines the proportion of patients remaining after each time ordered event occurs. For some patients, the endpoint or event did not occur during the observation period. Censored observations such as these are included in the time ordered analysis for their entire follow-up time duration. If censored observations were excluded from the analysis, a considerable bias would result. In the current study, four cumulative graft survival curves (figures 3 and 4)
4 RENAL GRAFT SURVIVAL were compared (two at a time), i.e., patients with renal grafts having (i) zero HLA-DR antigen matched donors versus one or two HLA-DR antigen matched donors and (ii) zero HLA-DR antigen incompatibility versus patients with renal grafts having one or two HLA-DR antigen incompatibilities. When two survival curves are to be tested for a statistically significant difference, the method of choice is the logrank test23 which is based on the chi-square distribution. The difference between the usual chi-square calculation and the logrank test rests on the definition of observed (0) and expected (E) values. In survival analysis, 0 becomes the number of renal graft rejections observed in each group compared to E the amount of exposure to the risk of renal graft rejection in each group. Prospective data is necessary in order to determine the risk of rejection so that real differences in graft rejections between groups may be determined if they exist. The chi-square calculation involves the summation of (0-E)2/E in the two groups. One compares this value with the standard chi-square table with one degree of freedom to determine the level of statistical significance. Results The overall graft survival of patients receiving a renal graft is given in figure 2. Thirty-four of 70 patients (49 percent) were followed for one year, 19 of 70 (27 percent) for two years, 15 of 70 (21 percent) for three years and eight of 70 (11 percent) for four years. The cumulative renal graft survived at two and four years was 60 percent. Two of 70 (three percent) patients received a two HLA-DR antigen matched graft, 38 of 70 (54 percent) received a one HLA-DR matched graft, and 30 of 70 (42 percent) received a zero HLA-DR antigen matched graft. Patients receiving a renal graft with either a one or two HLA-DR antigen matched graft Months F i g u r e 2. T he overall renal graft survival of 70 patients treated at SUNY U pstate M edical Center. The num ber at the top of the curve represents the n u m ber of patients followed for each tim e period (six months). had a higher cumulative graft survival than those patients receiving zero HLA- DR antigen matched graft (p < 0.05; figure 3). At one year, the cumulative graft survival for patients receiving a one or two HLA-DR antigen matched graft was 74 percent, whereas the graft survival for those patients receiving a zero HLA-DR antigen matched graft was 51 percent. At two and four years, the cumulative graft survival for patients receiving one or two HLA-DR antigen matched grafts was 69 percent where the cumulative graft survival at two and four years for those with zero HLA-DR antigen matched grafts was 47 percent. When all of the patient-donor graft combinations with unidentifiable HLA- DR antigens were excluded from the analysis, the total number of pairs under
5 4 5 4 LAUENSTEIN, DAVEY, HUBBELL, BURLESON, OATES, AND BURLESON F i g u r e 3. R enal g ra ft su rv iv al for p a tie n ts m atched at the H LA -D R locus. T he cum ulative renal graft survival for patients w ith one and two HLA-DR antigen m atched grafts is significantly greater than for p atients w ith zero H LA -D R antigen m atched grafts (p < 0.05). T he n u m ber at th e top o f the curve represents the n u m ber of patients followed for each time period (six months). consideration was reduced to 26. The subgroup (19 individuals) with one or two HLA-DR antigen matched grafts had a 12 month cumulative survival of 72 percent, whereas the subgroup (seven individuals) with zero HLA-DR antigen matched grafts had a 12 month cumulative survival of 57 percent. Because of the small size at these subgroups, a statistical analysis could not be performed. When HLA-DR antigen incompatibilities were analyzed, 18 of 70 (26 percent) patients had two HLA-DR incompatibilities, 35 of 70 (50 percent) had one incompatibility and 17 of 70 (24 percent) had no HLA-DR incompatibility. Recipients with no HLA-DR antigen incompatibility had a higher cumulative graft survival than those individuals with one or two antigen incompatibilities, but not at a significant level (figure 4). To determine if a maldistribution of known prognostic factors existed between patients with one or two HLA-DR matched grafts and zero HLA-DR matched grafts, both groups were compared according to sex, age, ABO type, HLA-A and B antigen matches, number of blood transfusions, and causes of graft F i g u r e 4. Renal graft survival for p atients w ith zero or one and two HLA -DR antigen incompatibilities. T he two curves are not significant at the 0.05 level. T he n u m ber at th e top of the curve represents the n u m ber of patients followed for each tim e period (six months). failure (table I). No significant differences were observed in the distribution of these parameters between patients with one or two HLA-DR antigen matched grafts and zero HLA-DR antigen matched grafts. No significant differences were observed in the distribution of these parameters when zero HLA-DR antigen incompatibility was compared to patients with one or two HLA-DR antigen incompatibilities (data not shown). In addition, no significant differences were observed in graft survival when the number of matches or incompatibilities between donors and recipients at the HLA-A and B loci were examined (data not shown). There were 18 different original diseases responsible for renal failure in this group of patients. Because of the small sample size of the subgroups, a statistical analysis regarding the prognostic value of the original disease on graft survival was not performed. Discussion Since 1978 there have been numerous studies correlating the association of HLA-DR matching with cadaveric renal graft survival ,20 26 Most of these stud-
6 T A B L E I Correlation of HLA-DR Antigen Matched Grafts With Other Prognostic Factors 1-2 Antigen 0 Antigen Match Match p Value No. % No. % Sex Male NS Female Age < MS > ABO Type NS Non HLA-A and B Match* NS No. Transfusions NS > No. Transfusions Not Known Causes of Failure of Grafts Acute & chronic rejection NS Non-immunologic mechanisms Represents the number of HLA-A and B antigens shared by the donor and the recipient. ies were performed in Europe, some were retrospective and others were extensions or continuations of previous reports.116 Most of the studies indicating an association between HLA-DR typing and renal graft survival were performed in single centers. In contrast, a large multicenter international study suggested that HLA-DR typing is not associated with subsequent graft survival.20 However, when renal transplants were performed in multiple centers and HLA- DR typings were performed by a single laboratory, a correlation between HLA- DR matching and cadaveric renal graft survival was observed.3 These and the current data suggest that when the variables of multicenter typing for HLA-DR matching are reduced to one center, an association between HLA-DR matching and renal graft survival is realized. RENAL GRAFT SURVIVAL The current study confirms our former data14 and others26 indicating that patients with grafts matched for one or two HLA-DR antigens have a superior graft survival. This difference cannot be attributed to other prognostic factors such as sex, age, ABO typing, HLA-A and B antigen matching, number of transfusions, or causes of graft failure because these characteristics were found in similar proportion in both matched and nonmatched groups. Since not all of the HLA-DR determinants are known, the presence of blank antigens complicates the analysis of the influence of HLA-DR matching on renal graft survival. In the current study, two HLA-DR antigens were identified in 61 percent of the donors and recipients, and one HLA-DR antigen was identified in 39 percent of the donors and recipients. In this study, the percentage of individuals with one identifiable HLA- DR antigen is similar to the percentage observed in normal control individuals studied in our institution. Although HLA-DR antigens are more difficult to detect on lymphocytes from patients with end-stage renal disease or from blood of cadaveric donors than from lymphocytes of normal healthy individuals,2 accurate HLA-DR typing can be performed on lymphocytes from these patients. To examine the relationship of HLA- DR matching and graft survival free of the problem of blanks, the survival data in donor-recipient pairs with two identifiable HLA-DR antigens was examined by the present authors. Although the numbers in each subgroup were small, individuals with a one or two HLA-DR antigen matched graft still had a superior graft survival compared to those with zero HLA-DR antigen matched grafts. Some studies16 22'27 have indicated that transfusions improve graft survival predominately in patients receiving DRmismatched transplants. These data sug
7 45 6 LAUENSTEIN, DAVEY, HUBBELL, BURLESON, OATES, AND BURLESON gest that recipients, who have not been transfused, would benefit greatly from receiving HLA-DR matched grafts. In the current study, only four patients did not receive any transfusions. Thus, the detrimental effect of no transfusions on patients receiving renal grafts could not be determined. Nevertheless, a similar distribution in the number of transfusions was observed in recipients receiving one or two antigen matched grafts and in those receiving zero antigen matched grafts. Thus, the beneficial effect of HLA-DR matching in the current study appears to be independent of the number of transfusions received by the recipients. In summary, our data strongly suggest that matching for HLA-DR antigens correlate with a beneficial renal graft survival. In addition, HLA-DR matching appears to be an independent prognostic factor. References 1. A l b r e c h t s e n, D., B r a t l i e, A., N o u s i a i n e n, H., S o l h e i m, B. G., W i n t e r s, N., and T h o r s b y, E.: Serologic typing o f H L A - D : Predictive value o f mixed lym phocyte cultures (MLC). Im m unogenetics 6 : , A y o u b, G. and T e r a s a k i, P. I.: Im p ro v ed D R typing of cadaver donors by lymphocyte incubation. Tissue A ntigens 18: , Ayoub, G. and T e r a s a k i, P. I. : H LA -D R m atching in m ulticenter, single-typing laboratory data. Transplantation 3 3 : , Bach, F. H. and Voynow, N. K.: O ne way stim ulation in m ixed leukocyte cu ltures. Science : 5 4 5, B u r l e s o n, R. L., J o n e s, D. B., Y e n i k o m s h i a n, A. M., C o r n w a l l, C., D e V o e, C., an d D e R ito, J. : Clinical renal preservation by cryoperfusion w ith an album in perfusate. Arch. Surg. 113: , B u r l e s o n, R. L., S c r u g g s, B. F., and B r e n n a n, A. : Successful imm unosuppression of renal allograft recipients with alternate date steroid therapy. Clin. N eph. 10: , C h e i g h, J. S., C h a m i, J., S t e n z e l, K. H., R i g - g i o, R. R., S a a l, S., M o u r a d i a n, J. A., F o t i n o, M., S t u d e n b o r d, W. T., an d R u b i n, A. L.: Renal tran sp lantatio n b etw een HLA identical siblings. Comparison with transplants from HLA sem i-id entical re la te d donors. N ew E ngl. J. M ed. 296: , Colton, T.: Statistics in M edicine. Boston, Little, Brown and Company, D e w a r, P. J., Wilkinson, R., Elliott, R. W., W a r d, M. K., Kerr, D. N. S., K e n w a r d, D. H., Proud, G., and Taylor, R. M. R.: Superio rity o f B locus m atch in g o v er o th e r H LA m atching in renal graft survival. Brit. M ed. J. 284: , Festenstein, H., Sachs, J. A., Paris, A. M. I., Pelgrum, G. D., and M o o r h e a d, J. F.: Influence of HLA m atching and blood transfusion on outcom e of 502 London transplant group renalgraft recipients. Lancet 1: , Festenstein, H. and Demant, P.: Basic im m u- nogenetics biology and clinical relevance, C urrent Top. Immunol. 9:1, Festenstein, H., Pachoula-Papasteriadis, C., Sachs, J. A., Jaraquemada, D., an d Burke, J. M. : Collaborative schem e for tissue typing and m atching in renal transplantation X. E ffect of HLA-A, B, D and D R m atching and p retran s p lan t blood transfusion on 769 cadaver renal grafts. Transpl. Proc. 11: , G oeken, N. E., Thompson, J. S., and Corry, R. J. : A 2 year trial of prospective H LA -D R matching. Transplantation 32: , Lauenstein, K., Burleson, R., Lachant, N., Davey, F. R., and Henry, J.: T he correlation of mixed lym phocyte reactions and H LA -D R typing in renal allograft survival. Transfusion 20:639, Me n d e z, R., Iwaki, Y., Me n d e z, R., Bogaard, T., and Self, B.: Prospective H LA -D R m atching in cadaveric renal transplants: A single center study. J. Urol. 129: , M o e n, T., Albrechtsen, D., Flatmark, A., Jakobsen, A., Jervell, J., Halvorsen, S., Solheim, B. G., and Thorsby, E.: Im portance of HLA-DR matching in cadaveric renal transplantation. A prospective center study of 170 transplants. N ew Engl. J. Med. 303: , Opelz, G., Mickey, M. R., and Terasaki, P. I.: H LA m atching and cadaver kidney tran sp lant su rv iv al in N o rth A m erica. T ra n sp lan ta tio n 23: , Opelz, G. and Terasaki, P. I. : Effect o f bloodgroup on relation betw een H LA m atch and outcom e o f cadav er kid n ey tran sp la n ts. L an cet i: , Opelz, G. and Terasaki, P. I. : Influence of sex on histocom patibility m atching in renal transplantation. Lancet 2: , Opelz, G. and Terasaki, P. I.: Internatio n al study of histocompatibility in renal transplantation. Transplantation 33:87-95, Patel, R. and Terasaki, P. I. : Significance of the positive crossmatch test in kidney transplantation. N ew Engl. J. Med. 280: , Persijn, G. G., van Leeuwen, A., Parlevliet, J., Cohen, B., Lansbergen, O., D Amaro, J., and van Rood, J. J. : Two major factors influencing kidney graft survival in E urotransplant: H L A -
8 D R m atching and blood transfusions. Transpl. Proc. i3 : , Peto, R., Pike, M. C., Armitage, P., Breslow, N. E., Cox, D. R., H o w a r d, S. V., Mantel, N., M c P h e r s o n, K., Peto, J., and Smith, P. G.: D esign and analysis of random ized clinical trials requiring prolonged observation of each patient.' II. Analysis and examples. Brit. J. Cancer 35:1-39, Ray, J. G., Hare, D. B., Pederson, P. D., and Muu.ally, D. I. eds. : NIA ID M anual of Tissue Typing T echniques. B ethesda, M D, N ational Institutions of Health, 1976, p Terasaki, P. I., B e r noco, D., Park, M. S., RENAL GRAFT SURVIVAL Ozturk, G., and Iwaki, Y.: M icrodroplet testing for HLA-A, B, C, and D antigens. Amer. J. Clin. Pathol. 69: , Ting, A. and Morris, P. J. : M atching for B-cell antigens of th e H LA -D R series in cadaver renal transplantation. Lacet 1: , Ting, A., Williams, K. A., änd Morris, P. J.: H LA -D R m atching and B-cell crossm atching in renal transplantation. Transplant. Proc. 12: , V o l l m e r, W. M., W a h l, P. W., and Blagg, C. R. : Survival w ith dialysis and transplantation in patients w ith end-stage renal disease. New Engl. J. M ed. 308: , 1983.
HUMAN LEUCOCYTE ANTIGEN (HLA) CLASS I AND II FREQUENCIES IN SELECTED GROUPS IN LEBANON
 Journal Scientifique Libanais, Vol. 1, No. 1, 2000 119 HUMAN LEUCOCYTE ANTIGEN (HLA) CLASS I AND II FREQUENCIES IN SELECTED GROUPS IN LEBANON Alexander M. Abdelnoor, May Abdelnoor, Walid Heneine, Firas
Journal Scientifique Libanais, Vol. 1, No. 1, 2000 119 HUMAN LEUCOCYTE ANTIGEN (HLA) CLASS I AND II FREQUENCIES IN SELECTED GROUPS IN LEBANON Alexander M. Abdelnoor, May Abdelnoor, Walid Heneine, Firas
HLA Alloimmunization with Leukocyte Concentrates from HLA-matched and HLA-non-m atched Donors in Patients with H unter s Syndrom e*
 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 15, No. 5 Copyright 1985, Institute for Clinical Science, Inc. HLA Alloimmunization with Leukocyte Concentrates from HLA-matched and HLA-non-m atched Donors
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 15, No. 5 Copyright 1985, Institute for Clinical Science, Inc. HLA Alloimmunization with Leukocyte Concentrates from HLA-matched and HLA-non-m atched Donors
SINCE the introduction of Imuran and
 Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
S plantation has become an accepted therapy for endstage
 HLA Histocompatibility Affects Cardiac Transplant Rejection and May Provide One Basis for Organ Allocation Verdi J. DiSesa, MD, Paul C. Kuo, MD, Keith A. Horvath, MD, Gilbert H. Mudge, MD, John J. Collins,
HLA Histocompatibility Affects Cardiac Transplant Rejection and May Provide One Basis for Organ Allocation Verdi J. DiSesa, MD, Paul C. Kuo, MD, Keith A. Horvath, MD, Gilbert H. Mudge, MD, John J. Collins,
Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function
 ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
Should red cells be matched for transfusions to patients listed for renal transplantation?
 Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
HLA-D, DR CLINICAL SIGNIFICANCE
 HLA-D, DR CLINICAL SIGNIFICANCE Α New Strategy to Improve Kidney Graft Survival: The Induction of CML Nonresponsiveness J J. van Rood, G. G. Persijn, A. van Leeuwen, E. Goulmy, and Β W. Gabb Α LTHOUGH
HLA-D, DR CLINICAL SIGNIFICANCE Α New Strategy to Improve Kidney Graft Survival: The Induction of CML Nonresponsiveness J J. van Rood, G. G. Persijn, A. van Leeuwen, E. Goulmy, and Β W. Gabb Α LTHOUGH
Dr. Yi-chi M. Kong August 8, 2001 Benjamini. Ch. 19, Pgs Page 1 of 10 TRANSPLANTATION
 Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
XM-ONE XM-ONE XM-ONE. References XMO_V4.0_100205_CE.EU
 Transplantation Cross match Transplantation Cross match XMO_V4._125_CE.EU Manufactured by: ABSORBER AB Address: Drottninggatan 33 SE-13 95 Stockholm, Sweden E-mail: info-ssp@olerup.com Tel: +46 8 5 89
Transplantation Cross match Transplantation Cross match XMO_V4._125_CE.EU Manufactured by: ABSORBER AB Address: Drottninggatan 33 SE-13 95 Stockholm, Sweden E-mail: info-ssp@olerup.com Tel: +46 8 5 89
XIV. HLA AND TRANSPLANTATION MEDICINE
 XIV. HLA AND TRANSPLANTATION MEDICINE A. Introduction 1. The HLA system includes a complex array of genes and their molecular products that are involved in immune regulation and cellular differentiation.
XIV. HLA AND TRANSPLANTATION MEDICINE A. Introduction 1. The HLA system includes a complex array of genes and their molecular products that are involved in immune regulation and cellular differentiation.
Hong Kong Journal Nephrol of 2000;(2): Nephrology 2000;2(2): BR HAWKINS ORIGINAL A R T I C L E A point score system for allocating cadaver
 Hong Kong Journal Nephrol of 2000;(2):79-83. Nephrology 2000;2(2):79-83. ORIGINAL A R T I C L E A point score system for allocating cadaveric kidneys for transplantation based on patient age, waiting time
Hong Kong Journal Nephrol of 2000;(2):79-83. Nephrology 2000;2(2):79-83. ORIGINAL A R T I C L E A point score system for allocating cadaveric kidneys for transplantation based on patient age, waiting time
- Transplantation: removing an organ from donor and gives it to a recipient. - Graft: transplanted organ.
 Immunology Lecture num. (21) Transplantation - Transplantation: removing an organ from donor and gives it to a recipient. - Graft: transplanted organ. Types of Graft (4 types): Auto Graft - From a person
Immunology Lecture num. (21) Transplantation - Transplantation: removing an organ from donor and gives it to a recipient. - Graft: transplanted organ. Types of Graft (4 types): Auto Graft - From a person
Analysis of Two Types of Granulocyte Transfusions in Patients with Acute Leukemia and Septicemia
 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 12, No. 2 Copyright 1982, Institute for Clinical Science, Inc. Analysis of Two Types of Granulocyte Transfusions in Patients with Acute Leukemia and Septicemia
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 12, No. 2 Copyright 1982, Institute for Clinical Science, Inc. Analysis of Two Types of Granulocyte Transfusions in Patients with Acute Leukemia and Septicemia
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Evaluation of Two New Antibody Detection Techniques in Kidney Transplantation. Doctoral Thesis. Dr. Petra Gombos
 Evaluation of Two New Antibody Detection Techniques in Kidney Transplantation Doctoral Thesis Dr. Petra Gombos Semmelweis University Doctoral School of Pathology Supervisor: Dr. Róbert Langer, Ph.D. Consultant:
Evaluation of Two New Antibody Detection Techniques in Kidney Transplantation Doctoral Thesis Dr. Petra Gombos Semmelweis University Doctoral School of Pathology Supervisor: Dr. Róbert Langer, Ph.D. Consultant:
HLA Compatibility and Cardiac Transplant Recipient Survival
 HLA Compatibility and Cardiac Transplant Recipient Survival William H. Frist, M.D., Philip E. Oyer, M.D., Ph.D., John C. Baldwin, M.D., Edward B. Stinson, M.D., and Norman E. Shumway, M.D., Ph.D. ABSTRACT
HLA Compatibility and Cardiac Transplant Recipient Survival William H. Frist, M.D., Philip E. Oyer, M.D., Ph.D., John C. Baldwin, M.D., Edward B. Stinson, M.D., and Norman E. Shumway, M.D., Ph.D. ABSTRACT
AGGRESSIVE PROMOTION of
 PAPER Prolonged Cold Ischemia Time Obviates the Benefits of HLA Mismatches in Renal Transplantation Crystine M. Lee, MD; Jonathan T. Carter; Edward J. Alfrey, MD; Nancy L. Ascher, MD, PhD; John P. Roberts,
PAPER Prolonged Cold Ischemia Time Obviates the Benefits of HLA Mismatches in Renal Transplantation Crystine M. Lee, MD; Jonathan T. Carter; Edward J. Alfrey, MD; Nancy L. Ascher, MD, PhD; John P. Roberts,
Chui, AKK; Lo, ACY; Chan, DTM; Tam, PC; Ho, KK; Hawkins, BR; Wong, J; Cheng, IKP
 Title Author(s) Comparison of the outcome of living related donor and cadaveric renal transplantation in Queen Mary Hospital - a single centre experience Chui, AKK; Lo, ACY; Chan, DTM; Tam, PC; Ho, KK;
Title Author(s) Comparison of the outcome of living related donor and cadaveric renal transplantation in Queen Mary Hospital - a single centre experience Chui, AKK; Lo, ACY; Chan, DTM; Tam, PC; Ho, KK;
PROTOCOLLED BLOOD TRANSFUSIONS IN RECIPIENTS OF A SIMULTANEOUS PANCREAS-KIDNEY TRANSPLANT REDUCE SEVERE ACUTE GRAFT REJECTION
 2 PROTOCOLLED BLOOD TRANSFUSIONS IN RECIPIENTS OF A SIMULTANEOUS PANCREAS-KIDNEY TRANSPLANT REDUCE SEVERE ACUTE GRAFT REJECTION 1,4 1 2 2 Marloes M. Waanders, Dave L. Roelen, Johan W. de Fijter, Marko
2 PROTOCOLLED BLOOD TRANSFUSIONS IN RECIPIENTS OF A SIMULTANEOUS PANCREAS-KIDNEY TRANSPLANT REDUCE SEVERE ACUTE GRAFT REJECTION 1,4 1 2 2 Marloes M. Waanders, Dave L. Roelen, Johan W. de Fijter, Marko
Organ transplantation in Bulgaria
 Cell Tissue Banking (28) 9:337 342 DOI 1.17/s1561-7-935-2 Organ transplantation in Bulgaria Elissaveta Naumova Æ Petar Panchev Æ Pencho J. Simeonov Æ Anastassia Mihaylova Æ Kalina Penkova Æ Petia Boneva
Cell Tissue Banking (28) 9:337 342 DOI 1.17/s1561-7-935-2 Organ transplantation in Bulgaria Elissaveta Naumova Æ Petar Panchev Æ Pencho J. Simeonov Æ Anastassia Mihaylova Æ Kalina Penkova Æ Petia Boneva
A Guide to Better Living
 Transplantation What Is a Kidney Transplant? Kidney transplantation is placing a kidney from one person (donor) into a patient with kidney failure (recipient). This is done by surgery where the donated
Transplantation What Is a Kidney Transplant? Kidney transplantation is placing a kidney from one person (donor) into a patient with kidney failure (recipient). This is done by surgery where the donated
Indian Journal of Nephrology Indian J Nephrol 2001;11: 88-97
 88 Indian Journal of Nephrology Indian J Nephrol 2001;11: 88-97 ARTICLE HLA gene and haplotype frequency in renal transplant recipients and donors of Uttar Pradesh (North India) S Agrawal, AK Singh, RK
88 Indian Journal of Nephrology Indian J Nephrol 2001;11: 88-97 ARTICLE HLA gene and haplotype frequency in renal transplant recipients and donors of Uttar Pradesh (North India) S Agrawal, AK Singh, RK
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS
 COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Transplantation. Immunology Unit College of Medicine King Saud University
 Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
HLA HISTOCOMPATIBILITY AND LIVER TRANSPLANT SURVIVAL
 HLA HISTOCOMPATIBILITY AND LIVER TRANSPLANT SURVIVAL Bernd H. Markus*, John J. Fung, Robert D. Gordon, Marian Vanek, Thomas E. Starzl, and Rene J. Duquesnoy From the Department of Surgery and the Division
HLA HISTOCOMPATIBILITY AND LIVER TRANSPLANT SURVIVAL Bernd H. Markus*, John J. Fung, Robert D. Gordon, Marian Vanek, Thomas E. Starzl, and Rene J. Duquesnoy From the Department of Surgery and the Division
TRANSPLANT IMMUNOLOGY. Shiv Pillai Ragon Institute of MGH, MIT and Harvard
 TRANSPLANT IMMUNOLOGY Shiv Pillai Ragon Institute of MGH, MIT and Harvard Outline MHC / HLA Direct vs indirect allorecognition Alloreactive cells: where do they come from? Rejection and Immunosuppression
TRANSPLANT IMMUNOLOGY Shiv Pillai Ragon Institute of MGH, MIT and Harvard Outline MHC / HLA Direct vs indirect allorecognition Alloreactive cells: where do they come from? Rejection and Immunosuppression
Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents
 BUMC Proceedings 1999;12:110-112 Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents CHERYLE GURK-TURNER, RPH Department of Pharmacy Services, BUMC wo mouse/human
BUMC Proceedings 1999;12:110-112 Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents CHERYLE GURK-TURNER, RPH Department of Pharmacy Services, BUMC wo mouse/human
The MHC and Transplantation Brendan Clark. Transplant Immunology, St James s University Hospital, Leeds, UK
 The MHC and Transplantation Brendan Clark Transplant Immunology, St James s University Hospital, Leeds, UK Blood Groups Immunofluorescent staining has revealed blood group substance in the cell membranes
The MHC and Transplantation Brendan Clark Transplant Immunology, St James s University Hospital, Leeds, UK Blood Groups Immunofluorescent staining has revealed blood group substance in the cell membranes
10/18/2012. A primer in HLA: The who, what, how and why. What?
 A primer in HLA: The who, what, how and why What? 1 First recognized in mice during 1930 s and 1940 s. Mouse (murine) experiments with tumors Independent observations were made in humans with leukoagglutinating
A primer in HLA: The who, what, how and why What? 1 First recognized in mice during 1930 s and 1940 s. Mouse (murine) experiments with tumors Independent observations were made in humans with leukoagglutinating
This study is currently recruiting participants.
 A Two Part, Phase 1/2, Safety, PK and PD Study of TOL101, an Anti-TCR Monoclonal Antibody for Prophylaxis of Acute Organ Rejection in Patients Receiving Renal Transplantation This study is currently recruiting
A Two Part, Phase 1/2, Safety, PK and PD Study of TOL101, an Anti-TCR Monoclonal Antibody for Prophylaxis of Acute Organ Rejection in Patients Receiving Renal Transplantation This study is currently recruiting
Strategies for Desensitization
 Strategies for Desensitization Olwyn Johnston MB, MRCPI, MD, MHSc BC Nephrology Day October 8 th 2010 Pre-transplant crossmatch (CMX) with donor lymphocytes has been standard of practice Positive CDC CXM
Strategies for Desensitization Olwyn Johnston MB, MRCPI, MD, MHSc BC Nephrology Day October 8 th 2010 Pre-transplant crossmatch (CMX) with donor lymphocytes has been standard of practice Positive CDC CXM
Transplant Applications of Solid phase Immunoassays Anti HLA antibody testing in solid organ transplantation
 AACC Professional Course BETH ISRAEL DEACONESS MEDICAL CENTER HARVARD MEDICAL SCHOOL Transplant Applications of Solid phase Immunoassays Anti HLA antibody testing in solid organ transplantation J. Ryan
AACC Professional Course BETH ISRAEL DEACONESS MEDICAL CENTER HARVARD MEDICAL SCHOOL Transplant Applications of Solid phase Immunoassays Anti HLA antibody testing in solid organ transplantation J. Ryan
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
Histocompatibility Evaluations for HSCT at JHMI. M. Sue Leffell, PhD. Professor of Medicine Laboratory Director
 Histocompatibility Evaluations for HSCT at JHMI M. Sue Leffell, PhD Professor of Medicine Laboratory Director JHMI Patient Population Adults Peds NMDP data >20,000 HSCT JHMI HSCT Protocols Bone marrow
Histocompatibility Evaluations for HSCT at JHMI M. Sue Leffell, PhD Professor of Medicine Laboratory Director JHMI Patient Population Adults Peds NMDP data >20,000 HSCT JHMI HSCT Protocols Bone marrow
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use
 Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
25/10/2017. Clinical Relevance of the HLA System in Blood Transfusion. Outline of talk. Major Histocompatibility Complex
 Clinical Relevance of the HLA System in Blood Transfusion Dr Colin J Brown PhD FRCPath. October 2017 Outline of talk HLA genes, structure and function HLA and immune complications of transfusion TA-GVHD
Clinical Relevance of the HLA System in Blood Transfusion Dr Colin J Brown PhD FRCPath. October 2017 Outline of talk HLA genes, structure and function HLA and immune complications of transfusion TA-GVHD
Solid phase radioimmunoassay for /^-microglobulin; a sensitive index for renal allograft evaluation
 Solid phase radioimmunoassay for /^-microglobulin; a sensitive index for renal allograft evaluation Manjula S. Kumar, Ph.D. Department of Immunopathology William E. Braun, M.D. Department of Hypertension
Solid phase radioimmunoassay for /^-microglobulin; a sensitive index for renal allograft evaluation Manjula S. Kumar, Ph.D. Department of Immunopathology William E. Braun, M.D. Department of Hypertension
Human leukocyte antigen (HLA) matching has a beneficial
 IMMUNOBIOLOGY AND GENOMICS Predicting the Immunogenicity of Human Leukocyte Antigen Class I Alloantigens Using Structural Epitope Analysis Determined by HLAMatchmaker Vasilis Kosmoliaptsis, 1,2 J. Andrew
IMMUNOBIOLOGY AND GENOMICS Predicting the Immunogenicity of Human Leukocyte Antigen Class I Alloantigens Using Structural Epitope Analysis Determined by HLAMatchmaker Vasilis Kosmoliaptsis, 1,2 J. Andrew
Donor-Specific HLA Class I and CREG Antibodies in Complement-Dependent Cytotoxicity-Negative Renal Transplants
 Available online at www.annclinlabsci.org 330 Annals of Clinical & Laboratory Science, vol. 40, no. 4, 2010 Donor-Specific HLA Class I and CREG Antibodies in Complement-Dependent Cytotoxicity-Negative
Available online at www.annclinlabsci.org 330 Annals of Clinical & Laboratory Science, vol. 40, no. 4, 2010 Donor-Specific HLA Class I and CREG Antibodies in Complement-Dependent Cytotoxicity-Negative
IV.13 Analysis of patient and graft survival. Guidelines. Commentary on Guidelines IV.13: Analysis of patient and graft survival
 60 SECTION IV: Long-term management of the transplant recipient IV.13 Analysis of patient and graft survival Guidelines A. It is important for a transplant unit to follow-up on the results of their transplant
60 SECTION IV: Long-term management of the transplant recipient IV.13 Analysis of patient and graft survival Guidelines A. It is important for a transplant unit to follow-up on the results of their transplant
IMMUNOBIOLOGY OF TRANSPLANTATION. Wasim Dar
 IMMUNOBIOLOGY OF TRANSPLANTATION Wasim Dar Immunobiology of Transplantation Overview Transplantation: A complex immunologic process Contributions Innate Immunity Adaptive immunity T Cells B Cells HLA Consequences
IMMUNOBIOLOGY OF TRANSPLANTATION Wasim Dar Immunobiology of Transplantation Overview Transplantation: A complex immunologic process Contributions Innate Immunity Adaptive immunity T Cells B Cells HLA Consequences
Thyroid Screening in the Newborn: Utah Experience
 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 13, No. 1 Copyright 1983, Institute for Clinical Science, Inc. Thyroid Screening in the Newborn: Utah Experience BRUCE A. BUEHLER. M.D.,* MELVIN J. GORTATOUSKI,
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 13, No. 1 Copyright 1983, Institute for Clinical Science, Inc. Thyroid Screening in the Newborn: Utah Experience BRUCE A. BUEHLER. M.D.,* MELVIN J. GORTATOUSKI,
Is it safe to transplant against HLA DSA in cardiothoracic patients? development and implementation of national Guidelines
 Is it safe to transplant against HLA DSA in cardiothoracic patients? development and implementation of national Guidelines Dr Martin Howell. Laboratory Director. Department of H&I, NHS Blood and Transplant,
Is it safe to transplant against HLA DSA in cardiothoracic patients? development and implementation of national Guidelines Dr Martin Howell. Laboratory Director. Department of H&I, NHS Blood and Transplant,
The Lecture s topics
 The Lecture s topics Blood groups -ABO system *Transfusion reaction -Rhesus factor *Hemolytic disease of newborn Blood transfusion and Tissue transplant The ABO System Discovered in 1901 by Dr. Karl Landsteiner
The Lecture s topics Blood groups -ABO system *Transfusion reaction -Rhesus factor *Hemolytic disease of newborn Blood transfusion and Tissue transplant The ABO System Discovered in 1901 by Dr. Karl Landsteiner
The Acceptable Mismatch program of Eurotransplant.
 The Acceptable Mismatch program of Eurotransplant. Frans Claas Leiden University Medical Center Eurotransplant Reference Laboratory Leiden, the Netherlands. Hinterzarten, December 7, 2013 Main problem
The Acceptable Mismatch program of Eurotransplant. Frans Claas Leiden University Medical Center Eurotransplant Reference Laboratory Leiden, the Netherlands. Hinterzarten, December 7, 2013 Main problem
APHERESIS FOR DESENSITIZATION OF NON-RENAL TRANSPLANTS
 APHERESIS FOR DESENSITIZATION OF NON-RENAL TRANSPLANTS GOW AREPALLY, MD MEDICAL DIRECTOR DUKE THERAPEUTIC APHERESIS SERVICE ASSOCIATE PROFESSOR, MEDICINE AMERICAN SOCIETY FOR APHERESIS MAY 25 TH 2013 OVERVIEW
APHERESIS FOR DESENSITIZATION OF NON-RENAL TRANSPLANTS GOW AREPALLY, MD MEDICAL DIRECTOR DUKE THERAPEUTIC APHERESIS SERVICE ASSOCIATE PROFESSOR, MEDICINE AMERICAN SOCIETY FOR APHERESIS MAY 25 TH 2013 OVERVIEW
1980s-1990s1990s 9/24/2010. David Wojciechowski and. Mary Kennedy-Breiner. Laurie Carlson. Janine Sabatte- Caspillo
 Factors Influencing Length of Stay: 1980s-1990s1990s Mail the Get Well Cards Home!! Effectively Managing Shorter Length of Stays David Wojciechowski and Higher rejection rates Longer duration of induction
Factors Influencing Length of Stay: 1980s-1990s1990s Mail the Get Well Cards Home!! Effectively Managing Shorter Length of Stays David Wojciechowski and Higher rejection rates Longer duration of induction
James E. Cooper, M.D. Assistant Professor, University of Colorado at Denver Division of Renal Disease and Hypertension, Kidney and PancreasTransplant
 James E. Cooper, M.D. Assistant Professor, University of Colorado at Denver Division of Renal Disease and Hypertension, Kidney and PancreasTransplant Program Has no real or apparent conflicts of interest
James E. Cooper, M.D. Assistant Professor, University of Colorado at Denver Division of Renal Disease and Hypertension, Kidney and PancreasTransplant Program Has no real or apparent conflicts of interest
Renal transplantation in children less than
 Archives of Disease in Childhood, 980, 55, 532-536 Renal transplantation in children less than 5 years of age GIANFRANCO RIZZONI, MOHAMMAD H MALEKZADEH, ALFRED J PENNISI, ROBERT B ETTENGER, CHRISTEL H
Archives of Disease in Childhood, 980, 55, 532-536 Renal transplantation in children less than 5 years of age GIANFRANCO RIZZONI, MOHAMMAD H MALEKZADEH, ALFRED J PENNISI, ROBERT B ETTENGER, CHRISTEL H
Basel - 6 September J.-M. Tiercy National Reference Laboratory for Histocompatibility (LNRH) University Hospital Geneva
 Basel - 6 eptember 2012 J.-M. Tiercy National Reference Laboratory for Histocompatibility (LNRH) University Hospital Geneva Outline the HLA system is (a) complex anti-hla immunisation and alloreactivity
Basel - 6 eptember 2012 J.-M. Tiercy National Reference Laboratory for Histocompatibility (LNRH) University Hospital Geneva Outline the HLA system is (a) complex anti-hla immunisation and alloreactivity
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
Chronic Kidney Disease (CKD) Stages. CHRONIC KIDNEY DISEASE Treatment Options. Incident counts & adjusted rates, by primary diagnosis Figure 2.
 Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant
 SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
Clinical Relevance of the HLA System in Blood Transfusion. Dr Colin J Brown PhD FRCPath. October 2017
 Clinical Relevance of the HLA System in Blood Transfusion Dr Colin J Brown PhD FRCPath. October 2017 Outline of talk HLA genes, structure and function HLA and immune complications of transfusion TA-GVHD
Clinical Relevance of the HLA System in Blood Transfusion Dr Colin J Brown PhD FRCPath. October 2017 Outline of talk HLA genes, structure and function HLA and immune complications of transfusion TA-GVHD
Should Pediatric Patients Wait for HLA-DR-Matched Renal Transplants?
 American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
DR-Bearing T Lymphocytes in Thoracic Duct Lymph 1
 CLINICAL IMMUNOLOGY AND IMMUNOPATHOLOGY 18.32-38 (l98\) DR-Bearing T Lymphocytes in Thoracic Duct Lymph 1 J. C. CICCIARELLi. P. 1. TERASAKI, Y. IWAKI, R. BILLING, T. YAMAGUCHI, H. TAKAHASHI, AND T. STARZL
CLINICAL IMMUNOLOGY AND IMMUNOPATHOLOGY 18.32-38 (l98\) DR-Bearing T Lymphocytes in Thoracic Duct Lymph 1 J. C. CICCIARELLi. P. 1. TERASAKI, Y. IWAKI, R. BILLING, T. YAMAGUCHI, H. TAKAHASHI, AND T. STARZL
CTS Collaborative Transplant Study
 CTS Collaborative Transplant Study Newsletter : February, The year marks the th anniversary of the Collaborative Transplant Study. Credit goes to all participants for their contribution to a priceless
CTS Collaborative Transplant Study Newsletter : February, The year marks the th anniversary of the Collaborative Transplant Study. Credit goes to all participants for their contribution to a priceless
Steroid Minimization: Great Idea or Silly Move?
 Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ
 Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation
 CLINICAL AND TRANSLATIONAL RESEARCH Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation Bernadette A. Magee, 1,4 Jeanie Martin, 1 Miceal P. Cole, 1 Kieran G. Morris, 2
CLINICAL AND TRANSLATIONAL RESEARCH Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation Bernadette A. Magee, 1,4 Jeanie Martin, 1 Miceal P. Cole, 1 Kieran G. Morris, 2
A POTENTIAL EXPANSION OF THERAPEUTIC APHERESIS UTILIZATION
 THE NEW KIDNEY ALLOCATION SYSTEM: A POTENTIAL EXPANSION OF THERAPEUTIC APHERESIS UTILIZATION Paul Warner, PhD, D(ABHI) Director, HLA/Immunogenetics Laboratory Bloodworks Northwest Seattle, Washington Disclosure
THE NEW KIDNEY ALLOCATION SYSTEM: A POTENTIAL EXPANSION OF THERAPEUTIC APHERESIS UTILIZATION Paul Warner, PhD, D(ABHI) Director, HLA/Immunogenetics Laboratory Bloodworks Northwest Seattle, Washington Disclosure
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
50 years Anniversary of First Kidney Transplant at Manchester Royal Infirmary
 50 years Anniversary of First Kidney Transplant at Manchester Royal Infirmary Consultant Transplant Surgeon Clinical Lead for Manchester /North west Paediatric Transplantation & Abdominal National Organ
50 years Anniversary of First Kidney Transplant at Manchester Royal Infirmary Consultant Transplant Surgeon Clinical Lead for Manchester /North west Paediatric Transplantation & Abdominal National Organ
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Lefaucheur C, Loupy A, Vernerey D, et al. Antibody-mediated
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Lefaucheur C, Loupy A, Vernerey D, et al. Antibody-mediated
ORIGINAL ARTICLE. Received April 30, 2007; accepted June
 LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
Vol. 29, pp.585 ~ 589, ml. 1.6 mg/dl 1 MRSA. Table 1 MRI
 Vol. 29, pp.585 ~ 589, 2001 8 13 10 22 8 7 1 14 49 26.1 6 2 ABO 7 1 400 800 ml 5 4 10 4 3 3 ABO 3 4 5 5 1 3 4 1 0.8 1.6 mg/dl 1 MRSA 10 7 1 10 7 22 40 8 CYA+ AZ+ MP 3 4 7 GSP 4 1 Table 1 23 1 15 11 5 Alport
Vol. 29, pp.585 ~ 589, 2001 8 13 10 22 8 7 1 14 49 26.1 6 2 ABO 7 1 400 800 ml 5 4 10 4 3 3 ABO 3 4 5 5 1 3 4 1 0.8 1.6 mg/dl 1 MRSA 10 7 1 10 7 22 40 8 CYA+ AZ+ MP 3 4 7 GSP 4 1 Table 1 23 1 15 11 5 Alport
Mary Keogan, on Mary behalf Keogan of all in NHISSOT On behalf of all in NHISSOT. 4th April 2014
 Solid Organ Transplantation How the Lab Contributes to Improved Patient Outcomes Mary Keogan, on Mary behalf Keogan of all in NHISSOT On behalf of all in NHISSOT 4th April 2014 Solid Organ Transplantation
Solid Organ Transplantation How the Lab Contributes to Improved Patient Outcomes Mary Keogan, on Mary behalf Keogan of all in NHISSOT On behalf of all in NHISSOT 4th April 2014 Solid Organ Transplantation
Patient Education Transplant Services. Glossary of Terms. For a kidney/pancreas transplant
 Patient Education Glossary of Terms For a kidney/pancreas transplant Glossary of Terms Page 18-2 Antibody A protein substance made by the body s immune system in response to a foreign substance. Antibodies
Patient Education Glossary of Terms For a kidney/pancreas transplant Glossary of Terms Page 18-2 Antibody A protein substance made by the body s immune system in response to a foreign substance. Antibodies
Transplant Success in Sensitized Patients Receiving a Standardized Desensitization Therapy: 3 Year Outcomes
 Transplant Success in Sensitized Patients Receiving a Standardized Desensitization Therapy: 3 Year Outcomes INTRODUCTION In patients awaiting a transplant, having antibodies reactive to HLA antigens present
Transplant Success in Sensitized Patients Receiving a Standardized Desensitization Therapy: 3 Year Outcomes INTRODUCTION In patients awaiting a transplant, having antibodies reactive to HLA antigens present
Management of Rejection
 Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Oxford Transplant Centre. Live donor kidney transplantation what if we are not a match?
 Oxford Transplant Centre Live donor kidney transplantation what if we are not a match? page 2 You will already have been provided with information about different types of kidney transplant and the tests
Oxford Transplant Centre Live donor kidney transplantation what if we are not a match? page 2 You will already have been provided with information about different types of kidney transplant and the tests
Desensitization in Kidney Transplant. James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver
 Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation
 Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 2, by the Massachusetts Medical Society VOLUME 342 M ARCH 2, 2 NUMBER 9 IMPROVED GRAFT SURVIVAL AFTER RENAL TRANSPLANTATION IN THE UNITED STATES, 1988 TO
The New England Journal of Medicine Copyright, 2, by the Massachusetts Medical Society VOLUME 342 M ARCH 2, 2 NUMBER 9 IMPROVED GRAFT SURVIVAL AFTER RENAL TRANSPLANTATION IN THE UNITED STATES, 1988 TO
European Risk Management Plan. Measures impairment. Retreatment after Discontinuation
 European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
Corneal transplantation: HLA and age
 L Aquila, 24 novembre 2012 Corneal transplantation: HLA and age Federico Genzano Besso*, Paola Magistroni, Piera Santoro*, Silvano Battaglio*, Raffaella Giacometti, Morteza Mansouri and Antonio Amoroso
L Aquila, 24 novembre 2012 Corneal transplantation: HLA and age Federico Genzano Besso*, Paola Magistroni, Piera Santoro*, Silvano Battaglio*, Raffaella Giacometti, Morteza Mansouri and Antonio Amoroso
Chapter 10. Histocompatibility Testing
 Chapter 10 Histocompatibility Testing Chapter 10 Histocompatibility Testing Table of Contents 10.1 General... 3 10.1.1 Registration of renal transplant patients...3 10.1.2 Material for histocompatibility
Chapter 10 Histocompatibility Testing Chapter 10 Histocompatibility Testing Table of Contents 10.1 General... 3 10.1.1 Registration of renal transplant patients...3 10.1.2 Material for histocompatibility
FIT Board Review Corner March 2016
 FIT Board Review Corner March 2016 Welcome to the FIT Board Review Corner, prepared by Sarah Spriet, DO, and Tammy Peng, MD, senior and junior representatives of ACAAI's Fellows-In-Training (FITs) to the
FIT Board Review Corner March 2016 Welcome to the FIT Board Review Corner, prepared by Sarah Spriet, DO, and Tammy Peng, MD, senior and junior representatives of ACAAI's Fellows-In-Training (FITs) to the
Blood Transfusion Effects in Kidney Transplantation
 Blood Transfusion Effects in Kidney Transplantation The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Accessed Citable
Blood Transfusion Effects in Kidney Transplantation The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Accessed Citable
1. Discuss the basic pathophysiology of end-stage liver and kidney failure.
 TRANSPLANT SURGERY ROTATION (PGY1, 2) A. Medical Knowledge Goal: The resident will achieve a detailed knowledge of the evaluation and treatment of a variety of disease processes. The resident will be exposed
TRANSPLANT SURGERY ROTATION (PGY1, 2) A. Medical Knowledge Goal: The resident will achieve a detailed knowledge of the evaluation and treatment of a variety of disease processes. The resident will be exposed
THE CLINICAL USE OF ANTILYMPHOCYTE GLOBULIN IN RENAL HOMOTRANSPLANTATION'
 TRANSPLANTATION Copyright @ 1967 by The Williams & Wilkins Co Vol. 5, No. 4, Part 2 of 2 parts Printed in U.S.A. THE CLINICAL USE OF ANTILYMPHOCYTE GLOBULIN IN RENAL HOMOTRANSPLANTATION' Department of
TRANSPLANTATION Copyright @ 1967 by The Williams & Wilkins Co Vol. 5, No. 4, Part 2 of 2 parts Printed in U.S.A. THE CLINICAL USE OF ANTILYMPHOCYTE GLOBULIN IN RENAL HOMOTRANSPLANTATION' Department of
Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab
 ORIGINAL ARTICLE Advance Access publication 1 February 2010 Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab Ana Carina Ferreira 1, Sandra Brum 1, Vasco
ORIGINAL ARTICLE Advance Access publication 1 February 2010 Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab Ana Carina Ferreira 1, Sandra Brum 1, Vasco
Tolerance Induction in Transplantation
 Tolerance Induction in Transplantation Reza F. Saidi, MD, FACS, FICS Assistant Professor of Surgery Division of Organ Transplantation Department of Surgery University of Massachusetts Medical School Percent
Tolerance Induction in Transplantation Reza F. Saidi, MD, FACS, FICS Assistant Professor of Surgery Division of Organ Transplantation Department of Surgery University of Massachusetts Medical School Percent
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20898 holds various files of this Leiden University dissertation. Author: Jöris, Monique Maria Title: Challenges in unrelated hematopoietic stem cell transplantation.
Cover Page The handle http://hdl.handle.net/1887/20898 holds various files of this Leiden University dissertation. Author: Jöris, Monique Maria Title: Challenges in unrelated hematopoietic stem cell transplantation.
HLA ANTIGEN FREQUENCY OF NORTHERN IRELAND BLOOD DONORS
 HLA ANTIGEN FREQUENCY OF NORTHERN IRELAND BLOOD DONORS by D. MIDDLETON Transplantation and Clinical Immunology, Belfast City Hospital J. MARTIN * Transplantation and Clinical Immunology, Belfast City Hospital
HLA ANTIGEN FREQUENCY OF NORTHERN IRELAND BLOOD DONORS by D. MIDDLETON Transplantation and Clinical Immunology, Belfast City Hospital J. MARTIN * Transplantation and Clinical Immunology, Belfast City Hospital
Improved Immunodiagnosis of Neutrophil Dysfunction in the Newborn and Infant
 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 12, No. 2 Copyright 1982, Institute for Clinical Science, Inc. Improved Immunodiagnosis of Neutrophil Dysfunction in the Newborn and Infant ALAN B. LOREN,
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 12, No. 2 Copyright 1982, Institute for Clinical Science, Inc. Improved Immunodiagnosis of Neutrophil Dysfunction in the Newborn and Infant ALAN B. LOREN,
Long-term efficacy and safety of conversion to tacrolimus in heart. transplant recipients with ongoing or recurrent acute cellular.
 Long-term efficacy and safety of conversion to tacrolimus in heart transplant recipients with ongoing or recurrent acute cellular rejection Blanka Skalická, Ivan Málek, Miloš Kubánek, Jevgenija Vymětalová,
Long-term efficacy and safety of conversion to tacrolimus in heart transplant recipients with ongoing or recurrent acute cellular rejection Blanka Skalická, Ivan Málek, Miloš Kubánek, Jevgenija Vymětalová,
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
Transplantation Immunology Booklet C
 Booklet C Pretest Correct Answers 3. (C) is correct. One of the major barriers to successful hematopoietic stem cell transplantation is the antigens coded for by the major histocompatibility gene complex.
Booklet C Pretest Correct Answers 3. (C) is correct. One of the major barriers to successful hematopoietic stem cell transplantation is the antigens coded for by the major histocompatibility gene complex.
Post-Transplant Monitoring for the Development of Anti-Donor HLA Antibodies
 Post-Transplant Monitoring for the Development of Anti-Donor HLA Antibodies Lorita M Rebellato, Ph.D., D (ABHI) Associate Professor Department of Pathology The Brody School of Medicine at ECU Scientific
Post-Transplant Monitoring for the Development of Anti-Donor HLA Antibodies Lorita M Rebellato, Ph.D., D (ABHI) Associate Professor Department of Pathology The Brody School of Medicine at ECU Scientific
Background & objectives
 Indian J Med Res 145, February 2017, pp 222-228 DOI: 10.4103/ijmr.IJMR_222_16 Quick Response Code: Comparative analysis of Luminex-based donor-specific antibody mean fluorescence intensity values with
Indian J Med Res 145, February 2017, pp 222-228 DOI: 10.4103/ijmr.IJMR_222_16 Quick Response Code: Comparative analysis of Luminex-based donor-specific antibody mean fluorescence intensity values with
Organ perfusion prior to transplantation
 Organ perfusion prior to transplantation Benedict Phillips SpR Transplant Surgery Research Fellow Guy s Hospital, London Introduction Organ perfusion with blood products prior to transplantation is an
Organ perfusion prior to transplantation Benedict Phillips SpR Transplant Surgery Research Fellow Guy s Hospital, London Introduction Organ perfusion with blood products prior to transplantation is an
Virtual Crossmatch in Kidney Transplantation
 Virtual Crossmatch in Kidney Transplantation Shiva Samavat Associate Professor of Nephrology Labbafinejad Hospital SBMU 2018.11.21 All transplant candidates are screened to determine the degree of humoral
Virtual Crossmatch in Kidney Transplantation Shiva Samavat Associate Professor of Nephrology Labbafinejad Hospital SBMU 2018.11.21 All transplant candidates are screened to determine the degree of humoral
The new Banff vision of the role of HLA antibodies in organ transplantation: Improving diagnostic system and design of clinical trials
 The new Banff vision of the role of HLA antibodies in organ transplantation: Improving diagnostic system and design of clinical trials Carmen Lefaucheur 1 2 Banff 2015: Integration of HLA-Ab for improving
The new Banff vision of the role of HLA antibodies in organ transplantation: Improving diagnostic system and design of clinical trials Carmen Lefaucheur 1 2 Banff 2015: Integration of HLA-Ab for improving
