Trends in the Management and Outcomes of Kidney Transplantation for Autosomal Dominant Polycystic Kidney Disease
|
|
|
- Leslie Ramsey
- 5 years ago
- Views:
Transcription
1 Trends in the Management and Outcomes of Kidney Transplantation for Autosomal Dominant Polycystic Kidney Disease The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed Citable Link Terms of Use Patel, Madhukar S., Praveen Kandula, David Wojciechowski, James F. Markmann, and Parsia A. Vagefi Trends in the Management and Outcomes of Kidney Transplantation for Autosomal Dominant Polycystic Kidney Disease. Journal of Transplantation 2014 (1): doi: /2014/ doi: /2014/ July 3, :16:41 PM EDT This article was downloaded from Harvard University's DASH repository, and is made available under the terms and conditions applicable to Other Posted Material, as set forth at (Article begins on next page)
2 Hindawi Publishing Corporation Journal of Transplantation Volume 2014, Article ID , 7 pages Clinical Study Trends in the Management and Outcomes of Kidney Transplantation for Autosomal Dominant Polycystic Kidney Disease Madhukar S. Patel, 1 Praveen Kandula, 2 David Wojciechowski, 3 James F. Markmann, 1 and Parsia A. Vagefi 1 1 Department of Surgery, Massachusetts General Hospital, Harvard Medical School, 55 Fruit Street, White 544b, Boston, MA 02114, USA 2 Department of Medicine, Saint Barnabas Medical Center, Livingston, NJ 07039, USA 3 Department of Medicine, University of California, San Francisco, San Francisco, CA 94143, USA Correspondence should be addressed to Parsia A. Vagefi; pvagefi@partners.org Received 27 March 2014; Revised 18 July 2014; Accepted 18 July 2014; Published 3 August 2014 Academic Editor: Bruce Kaplan Copyright 2014 Madhukar S. Patel et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Background. Autosomal dominant polycystic kidney disease (ADPKD) is the most common genetic disorder leading to end-stage renal failure. The objective of this study was to evaluate a longitudinal experience of kidney transplantation for ADPKD. Methods. A single center retrospective review of patients undergoing kidney transplantation was conducted, with comparisons across two time periods: early (02/ /2007, n=66) and late (04/ /2012, n=67). Results. Over the 13.5-year study period, 133 patients underwent transplantation for ADPKD. Overall, no significant difference between the early and late group with regard to intraoperative complications, need for reoperation, readmissions within 30 days, delayed graft function, and mortality was noted. There was a trend towards increase in one-year graft survival (early 93.1% versus late 100%, P = 0.05). In the early group, 67% of recipients had undergone aneurysm screening, compared to 91% of recipients in the late group (P < 0.001). Conclusions. This study demonstrates consistent clinical care with a trend towards improved rates of one-year graft survival. Interestingly, we also note a significantly higher use of cerebral imaging over time, with the majority that were detected requiring surgical intervention which may justify the current practice of nonselective radiological screening until improved screening criteria are developed. 1. Introduction Autosomal dominant polycystic kidney disease (ADPKD) is a disorder characterized by the development of renal cysts that may result in end-stage renal failure. Two main genes, PKD1 and PKD2,arethoughttobeinvolvedinthemajorityofcases [1]. Variability in the genetic phenotype of ADPKD patients, however,isthoughttobeduetotherangeofdifferentgenetic mechanisms as well as environmental factors thought to play a role in phenotypic expression[1]. In addition to affecting the kidneys, ADPKD has a number of extrarenal manifestations including cystic formation in other organs such as the liver, seminal vesicles, pancreas, and arachnoid membrane; vascular malformations such as intracranial aneurysms, thoracic aorta dissections, and coronary artery aneurysms; cardiac manifestations such as mitral valve prolapse; and a higher incidence of colonic diverticulosis and diverticulitis [1]. In those with end-stage renal disease, it is accepted that transplantation is the preferred treatment for ADPKD [1]. Of the patients on the kidney transplant waiting list as of December , 7256 (8.4%) were listed due to cystic kidney disease and of the 16,055 renal transplants performed in 2011, 2057 (12.8%) were done for patients with cystic kidney disease, with 1,189 from deceased donors and 868 from living donors [2]. In patients undergoing transplantation for ADPKD, current reports in the literature debate the timing and need for native nephrectomy [3 14] as well as the operative approach for native nephrectomy [14 17].
3 2 Journal of Transplantation Additionally, due to the potential for catastrophic outcomes perioperatively of undiagnosed cerebral aneurysms, screening for their presence has been suggested at least among subgroups of ADPKD patients [18]. However, there is no clear consensus on management regarding need, timing, or approach to nephrectomy as well as for screening for cerebral aneurysms before undergoing kidney transplantation but rather decisions appear to be patient specific and vary as a function of time and center/surgeon preference. Given this, the objective of this report was to study the longitudinal experience of ADPKD and kidney transplantation at a single center in order to (1) define overall outcomes with management of this disease and (2) identify changes in practice and outcomes over time. 2. Methods A single center retrospective review of consecutive ADPKD patients undergoing transplants from 02/2000 to 08/2012 was conducted. Data collected included recipient demographics, donor type, timing of native nephrectomy if performed (prior, simultaneous, or after transplant), reason for nephrectomy, approach to nephrectomy (laparoscopic versus open), laterality of nephrectomy (unilateral or bilateral), total operative time and estimated blood loss at the time of nephrectomy and transplant, use of ureteral stents, weight of nephrectomy kidney(s), need for intraoperative or postoperative transfusion, intraoperative complications, need for reoperation, need for readmission, delayed graft function, graft failure, and death. Of note, delayed graft function was defined as the need for dialysis within the first seven days after transplant. The censor date for graft failure and death was January 1, In addition to these variables, data collected included screening for intracranial aneurysms via CT or MR and form of treatment for those found to have brain aneurysms needing treatment. If available, family history for brain aneurysms was also noted. In order to assess changes in practice over time, patients were chronologically ordered and divided into two nearly equal groups based on transplant date: (1) early 02/ /2007) and (2) late (04/ /2012). For the purposes of data analysis, for the patients receiving more than one transplant at our institution, each transplant event was counted as a separate case so that outcomes could be analyzed independently. Univariate analysis was performed to look for differences between groups. The independent samples t-test was used for continuous variables and Pearson s chisquare or Fisher s exact test was used for categorical variables. Data analysis was performed using IBM Statistical Products and Service Solutions (SPSS, Inc., Chicago Ill) version 21.0 for Windows. The Institutional Review Board of Partners Healthcare approved this study. 3. Results In the 13.5-year study period, data from 133 ADPKD patients who underwent kidney transplantation was collected. Average overall age was 54.1 ± 10.3 years with 37.6% of patients being female. The average number of months of dialysis before transplant was 18.6 ± 21. The majority of transplants were from deceased donors (45.1%), followed by living unrelated donors (34.6%) and living related donors (20.3%). Extended criteria donors were used in nine transplants (6.8%) and donation after cardiac death in 23 transplants (17.3%). All nonheart beating donors were considered controlled. Of the 133 ADPKD patients transplanted, six received a second kidneytransplant.threeofthesixhadtheirfirsttransplant done at an outside institution. Overall, the average number of days in the hospital after transplant was 5.6 ± 3.5 days. Indications for pretransplant, simultaneous, and posttransplant nephrectomy are listed in Table 1.Some patients had more than one indication for nephrectomy. Overall, 92 patients (69.2%) received a nephrectomy, some patients receiving more than one. With regard to timing, eight patients (6%) underwent pretransplant native nephrectomy with 7 of these (87.5%) being unilateral. Simultaneous nephrectomy was performed in 74 patients (55.6%) with 67 of these (90.5%) being unilateral. All pretransplant and simultaneous nephrectomies were performed using an open technique. Lastly, 25 patients (18.8%) underwent posttransplant native nephrectomywith14ofthese(56%)beingunilateraland17 being laparoscopic (68%). Combined approaches were done in four patients (3%) who underwent both a pretransplant and simultaneous native nephrectomy and 11 patients (8.3%) who underwent both a simultaneous and posttransplant nephrectomy. With regard to pretransplant cerebral aneurysm screening, of the 133 patients analyzed in this study, 105 (78.9%) received radiologic imaging (CT or MR) to screen for brain aneurysms. Of those screened, 12 patients (12.4%) were found to have brain aneurysms with seven undergoing surgical treatment with clipping. Data regarding the size of intracranial aneurysms was available for 10 of the 12 cases, with the average size being 3.75 ± 1.41 mm in those undergoing intervention. The location of intracranial aneurysms was diverse and included the anterior communicating artery, middle cerebral artery, posterior cerebral artery, paraclinoid internal carotid artery, and basilar artery. Six patients were found to have a positive family history for brain aneurysm, but none of these patients were found to have brain aneurysm after undergoing radiological screening. Results of a univariate analysis comparing the first 66 patients in this series (the early group spanning from 02/2000 to 04/2007) to the subsequent 67 patients (the late group spanning from 04/2007 to 08/2012) are present in Tables 2 and 3.Therewasnosignificantdifferenceinthedonorpopulation utilizedbetween thetwo eras (Table 2). Of note, significantly more patients were screened for brain aneurysms in the late group (91% versus 66.7%, P = 0.001) andalthougha higher percentage were found to have brain aneurysms in the late group (14.8% versus 6.8%, P = 0.207), the difference was not statistically significant. With regard to operative technique, ureteral stents were significantly more common in the late group (64.2% versus 21.2%). Other notable findings include significantly less simultaneous nephrectomies in thelategroup(22.4%versus89.4%,p < 0.001) anda
4 Journal of Transplantation 3 Indication Table 1: Indications and timing of nephrectomy. Pretransplant nephrectomy (n =8) Timing of nephrectomy Simultaneous nephrectomy (n =74) Posttransplant nephrectomy (n =25) Size 4 (50%) 55 (74.3%) 4 (16%) Bleeding 2 (25%) 5 (6.8%) 4 (16%) Subjective symptoms (e.g., early satiety and chronic pain) 3 (37.5%) 4 (5.4%) 14 (56%) Infection (16%) Hypertension (12%) Suspicion of neoplasia (4%) Hematuria 0 1 (1.4%) 2 (8%) Not clearly specified 4 (50%) 11 (14.9%) 1 (4%) Note: some patients had more than one indication for nephrectomy. marginally significant higher proportion of posttransplant nephrectomies (25.4% versus 12.1%, P = 0.050). Of the posttransplant nephrectomies, there were significantly less unilateral (35.3% versus 100%, P = 0.003) and open (5.9% versus 87.5%, P < 0.001) in the late group. The total operative time at transplant was lower in the late group (212.9 minutes ± 59.7 versus minutes ± 62.3, P < 0.001). Lastly, there was no significant difference between the early and late group with regard to delayed graft function (12.1% versus 16.4%, P = 0.479) and mortality (8.2% versus 15%, P = 0.242); however, there was a trend towards improved one-year graft survival in the late group (93.1% versus 100%, P = 0.05). Intraoperative complications occurred in 6 patients (4.5%). After transplant, 11 patients (8.3%) required reoperation. Overall, 24 (18%) of patients required readmission within 30 days of discharge. Reasons for readmission are demonstrated in Table 4. With regard to graft and patient outcomes, 19 patients (14.3%) had delayed graft function. The overall mean follow-up was 79.2±108.5 months. Graft failure occurred in 19 patients (14.2%) and the average time to known graft failure was 46.9 ± 41.7 months. Reasons for failure are shown in Table 4. Death occurred in 14 patients (10.5%) and the average time to death was 56.0 ± 44 months. Reasons for death are shown in Table Discussion Of the monogenic disorders, autosomal dominant polycystic kidney disease is the most prevalent [1]. As ADPKD may result in end-stage renal failure, transplantation is often necessary for treatment of this disease. In the current series, 133 patients underwent transplantation for ADPKD at a single center over 13.5 years, with 92 (69.2%) of these patients receiving nephrectomy for indications varying depending upon time of nephrectomy. Over time, simultaneous nephrectomy became less common and posttransplant laparoscopic nephrectomy became the more frequent procedure of choice. With regard to preoperative workup, there was an increasing frequency of screening for intracranial aneurysms in ADPKD recipients. Intraoperative complications remained infrequent; however, the need for readmissions persisted, likelyrelatedtothecomplexityofmanagingtheposttransplant patient. The operative duration shortened in the late time period, likely related to a decreased use of unilateral concomitant native nephrectomy, and there was a trend towards improved one-year graft survival more recently. Advances in conservative management of ADPKD symptoms with the use of pain medication, antibiotics, transfusion, and antihypertensives [13] as well as minimally invasive methods such as laparoscopic cyst decortication [19] for symptomatic relief have impacted the indications for nephrectomy in this disease [13]. Symptoms such as pain, fullness, early satiety, cystic hemorrhage, hypertension, nephrolithiasis, and urinary tract infections serve as relative indications for nephrectomy. In a single center retrospective review of native nephrectomy in 157 kidney transplant patients with ADPKD, Patel et al. noted that, overall, the most common indication for the 20% of patients undergoing native nephrectomy was urinary tract infection (45%), pain (39%), tumor suspicion (10%), hematuria (3%), and space (3%) [20]. The frequency of these indications was quite different than those identified in the current study in which size was the most common indication for patients undergoing pretransplant and simultaneous nephrectomy, whereas subjective symptoms such as early satiety and chronic pain were the most common indication for those undergoing posttransplantnephrectomy.furthermore,itshouldbementionedthat in addition to size considerations, at our institution it was common practice during the early period for surgeons to do simultaneous unilateral nephrectomy in order to then subsequently perform an ureteroureterostomy anastomosis forthetransplantedkidney.assurgeonsbegantoperform ureterocystostomy more commonly in the later period, the overall proportion of simultaneous native nephrectomy becameless,likelyinparttothischangeinpractice. In addition to changes in the timing and approach to nephrectomy, differences in the use of preoperative screening were noted between the early and late groups. Specifically, in the early group 66.7% of recipients underwent screening compared to 91% in the late groups (P < 0.001). There was no significant difference, however, noted in the number found to have brain aneurysms or the number treated for
5 4 Journal of Transplantation Table 2: Comparison of categorical variables among the early and late experience in patients receiving transplantation for adult polycystic kidney disease. Categorical variable Early (n = 66) Late(n = 67) P value Deceased donor 33 (50%) 27 (40.3%) Living related donor 14 (21.2%) 13 (19.4%) Living unrelated donor 19 (28.8%) 27 (40.3%) Donation after cardiac death 12 (18.2%) 11 (16.4%) Extended criteria donor 4 (6.1%) 5 (7.5%) % male 25 (37.9%) 25 (37.3%) Previous native nephrectomy 4 (6.1%) 4 (6.0%) Previous native nephrectomy was unilateral 4 (100%) 3 (75%) Screened for brain aneurysms 44 (66.7%) 61 (91%) Found to have brain aneurysms 3 (6.8%) 9 (14.8%) Treated for brain aneurysms 3 (100%) 5 (55.6%) Simultaneous native nephrectomy 59 (89.4%) 15 (22.4%) <0.001 Simultaneous native nephrectomy was unilateral 53 (89.8%) 14 (93.3%) Simultaneous native nephrectomy was open 59 (100%) 15 (100%) Intraop transfusion required 6 (9.1%) 13 (19.4%) Side of transplant was on the right 44 (66.7%) 61 (92.4%) <0.001 Ureteral stent 14 (21.2%) 43 (64.2%) <0.001 Intraoperative complications 3 (4.5%) 7 (10.4%) Postop transfusion required 23 (34.8%) 20 (29.9%) Need for reoperation 5 (7.6%) 6 (9%) Readmission within 30 days 13 (19.7%) 12 (17.9%) Posttransplant native nephrectomy 8 (12.1%) 17 (25.4%) Posttransplant nephrectomy was unilateral 8 (100%) 6 (35.3%) Posttransplant nephrectomy was open 7 (87.5%) 1 (5.9%) <0.001 DGF dialysis required 8 (12.1%) 11 (16.4%) year graft survival 54 (93.1%) 62 (100%) Death 9 (15%) 5 (8.2%) Fisher s exact test used as 1 cell has expected count less than 5. DGF: delayed graft function. these aneurysms. There are currently no societal guidelines or an established standard of practice to screen for cerebral aneurysms in patients with ADPKD. ADPKD patients with history of subarachnoid hemorrhage, two or more relatives with intracranial aneurysms or rupture, those in high-risk occupations, undergoing major elective surgery, or having a warning headache or severe anxiety regarding the issue are suggested to be screened [18]. Specific information regarding screening prior to kidney transplantation is lacking. In a review of presymptomatic screening with magnetic resonance angiography in ADPKD patients, Irazabal et al. foundthatmostunrupturedintracranialaneurysmshavethe growth and rupture risks that are not higher than unruptured intracranial aneurysms found in the general population thus suggesting selective screening [21]. Similarly, a report by Gibbsetal.designedtostudytheriskofgrowthandrupture of intracranial aneurysms detected suggests that since most aneurysms detected by such screening are small and have a low risk for rupture, presymptomatic screening should not be done in those without a family history of unruptured intracranial aneurysms [22]. Of note, in the current series, all six patients with a family history underwent screening andnonewerefoundtohavebrainaneurysms.although there remains a low level of aneurysm detection overall, the majority detected required surgical intervention which may justify the current practice of nonselective radiological assessment until improved screening criteria are developed for patients preparing to undergo kidney transplantation. With regard to outcomes, it should be noted that over time there was a trend towards improved 1-year graft survival of 100%. Unfortunately this study was not designed to identify independent factors responsible for this observation, but it is possible that some of the above noted changes in practice over time may have contributed. Comparisons of outcomes of ADPKD patients treated with transplantation to other series in the literature are limited in the fact that previously published series often provide outcomes of particular cohorts of patients (e.g., those receiving pretransplant nephrectomy or those undergoing simultaneous nephrectomy and transplantation) as opposed to outcomes for overall experiences.
6 Journal of Transplantation 5 Table 3: Comparison of continuous variables among the early and late experience in patients receiving transplantation for adult polycystic kidney disease. Continuous variable Early (n = 66) Late(n = 67) P value Ageattransplant(years) 53.7± ± Months of dialysis prior to transplant 17.3 ± ± Days in hospital after transplant 6.0 ± ± BMI 25.8 ± ± Previous native nephrectomy total op time (min) ± 59.1 in 3 cases ± 37.9 in 3 cases Previous native nephrectomy EBL (milliliters) 250 ± 70.7 in 2 cases ± 46.2 in 3 cases Total weight of nephrectomy kidney(s) (grams) ± 903 in 57 cases ± in 28 cases <0.001 Total op time at time of transplant (min) ± ± 59.7 <0.001 Intraop transfusion of RBCs (units) 1.25 ± 0.5 in 4 cases 1.86 ± 1.1 in 7 cases Intraop transfusion of FFP (units) 2 ± 0in2cases 3.6± 1.5 in 5 cases Intraop transfusion of platelets (units) ± 0.7 in 2 cases N/A EBL at time of transplant (milliliters) ± in 48 cases ± in 66 cases Postop transfusion of RBCs (units) 3.5 ± 3.6 in 23 cases 2.3 ± 1.2 in 17 cases Postop transfusion of FFP (units) 7.5 ± 6.4 in 2 cases 2.7 ± 1.2 in 6 cases Postop transfusion of platelets (units) 7 ± 1.7 in 3 cases 1 in 1 case N/A Posttransplant native nephrectomy total op time (min) ± 53.9 in 8 cases ± 47.1 in 17 cases Posttransplant native nephrectomy total EBL (milliliters) ± in 6 cases ± 311.5in15cases BMI: body mass index; EBL: estimated blood loss; RBCs: red blood cells; FFP: fresh frozen plasma. Table 4: Reasons for readmission within 30 days of discharge, graft failure, and death in transplant recipients. Reasons for readmission (n =24) Reasonsforgraftfailure(n=19 ) Reasons for death (n =14) Elevated serum creatinine and/or concern for acute rejection (13, 54.2%) Acute rejection (3) Infection (4, 28.6%) Volume overload (2, 8.3%) Chronic rejection (3) Malignancy (3, 21.4%) Nausea (2, 8.3%) Calcineurin toxicity (3) Cardiovascular (1, 7.1%) Chylocele (1, 4.2%) Infection (3) Dementia (1, 7.1%) Diarrhea (1, 4.2%) Cardiovascular (2) Unknown (5, 35.7%) Peritoneal dialysis catheter removal (1, 4.2%) Hyperacute rejection (1) Perforated duodenal ulcer (1, 4.2%) Thrombotic microangiopathy (1) Bladder stone (1, 4.2%) Technical (1) Wound infection (1, 4.2%) Malignancy (1) Hypophosphatemia (1, 4.2%) Unknown (3) Frequencies not calculated due to some patients having multiple reasons. Furthermore, institutional practices vary greatly and given that most reports are of single center retrospective experiences, cross comparisons are difficult. There are several limitations to this study that are inherent to its being a retrospective single center review. Firstly, this study was limited to variables that were available in the electronic medical records of the patients studied. As this study evaluated changes in practice over time, it should be noted that there was generally more electronic medical information available for patients operated on more recently but more longitudinal follow-up available for patients operated on more remotely, thus possibly introducing bias. Secondly,althoughthisisalargeseriesofpatientsovera significant time span, the number of patients available for specific stringent statistical analysis was limited due to the prevalence of disease. Therefore, the possibility of Type II errorshouldbeconsideredinsubcohortanalysesofsmall sample sizes even though appropriate statistical tests were applied. Thirdly, the observations noted in this study about thechangeinpracticepatternsovertimereflectthoseofa single institution that is often dependent on the resources and infrastructure of that particular institution and that may not be directly applicable to the management of this disease at large. Relevant to the current analysis is the fact that it was the practice of this institution to routinely perform ipsilateral nephrectomy at the time of transplant to permit creation of an ureteroneocystostomy. This may have contributed to the high fraction of patients having a nephrectomy with simultaneous transplantation. Lastly, it should be noted that division of groups into early and late was done based on splitting the
7 6 Journal of Transplantation sample in half rather than splitting the time period in half in order to allow for more statistically even comparisons of groups with regard to total number of patients. 5. Conclusions End-stage renal disease caused by autosomal dominant polycystic kidney disease can effectively be managed by renal transplantation. As a component of therapy, native nephrectomy may also be done but there exists a large degree of variability with respect to timing and approach of nephrectomy. As evidenced by this report, even within the same institution, there has been significant change with an increase in the number of posttransplant, bilateral laparoscopic nephrectomies being performed. Although intraoperative complications, need for reoperation, readmission rates, and mortality did not significantly change over time, there was a trend towards improved 1-year graft survival more recently. We also note a significantly higher use of cerebral imaging over time, with the majority that were detected requiring surgical intervention. As mentioned, this may justify the current practice of nonselective radiological screening until improved screening criteria are developed. Disclosure Content from this paper was presented as a poster presentation at the 14th Annual American Society for Transplant Surgery State of the Art Winter Symposium in Miami Beach, FL, in January 24, Conflict of Interests The authors declare that there is no conflict of interests regarding the publication of this paper. References [1] V. E. Torres, P. C. Harris, and Y. Pirson, Autosomal dominant polycystic kidney disease, The Lancet, vol. 369, no. 9569, pp , [2] Annual Report of the U.S. Organ Procurement and Transplantation Network and the Scientific Registry of Transplant Recipients: Transplant Data , Department of Health and Human Services, Health Resources and Services Administration, Healthcare Systems Bureau, Division of Transplantation, Rockville, MD; United Network for Organ Sharing, Richmond, VA, University Renal Research and Education Association, Ann Arbor, Mich, USA, [3] M.H.Skauby,O.Øyen,A.Hartman,T.Leivestad,andJ.Wadström, Kidney transplantation with and without simultaneous bilateral native nephrectomy in patients with polycystic kidney disease: a comparative retrospective study, Transplantation,vol. 94, no. 4, pp , [4] D.T.Glassman,L.Nipkow,S.T.Bartlett,andS.C.Jacobs, Bilateral nephrectomy with concomitant renal graft transplantation for autosomal dominant polycystic kidney disease, The Journal of Urology,vol.164,no.3,part1,pp ,2000. [5] H.R.Ismail,S.M.Flechner,J.H.Kaouketal., Simultaneousvs. sequential laparoscopic bilateral native nephrectomy and renal transplantation, Transplantation, vol. 80, no. 8, pp , [6] M. D. Wagner, J. C. Prather, and J. M. Barry, Selective, concurrent bilateral nephrectomies at renal transplantation for autosomal dominant polycystic kidney disease, The Journal of Urology,vol.177,no.6,pp ,2007. [7] R. Król,J.Ziaja,T.Cierniaketal., Simultaneoustransabdominal bilateral nephrectomy in potential kidney transplant recipients, Transplantation Proceedings, vol. 38, no. 1, pp , [8] T.F.Fuller,T.V.Brennan,S.Feng,S.M.Kang,P.G.Stock,and C. E. Freise, End stage polycystic kidney disease: indications and timing of native nephrectomy relative to kidney transplantation, Journal of Urology, vol. 174, no. 6, pp , [9] A. Tabibi, N. Simforoosh, P. Abadpour, H. R. Gholamrezaie, and M. Nafar, Concomitant nephrectomy of massively enlarged kidneys and renal transplantation in autosomal dominant polycystic kidney disease, Transplantation Proceedings,vol.37, no.7,pp ,2005. [10] A. Kramer, J. Sausville, A. Haririan, S. Bartlett, M. Cooper, and M. Phelan, Simultaneous bilateral native nephrectomy and living donor renal transplantation are successful for polycystic kidney disease: the University of Maryland experience, Journal of Urology,vol.181,no.2,pp ,2009. [11] M. A. Kirkman, D. van Dellen, S. Mehra et al., Native nephrectomy for autosomal dominant polycystic kidney disease: before or after kidney transplantation? BJU International, vol. 108, no. 4, pp , [12]J.Rozanski,I.Kozlowska,M.Myslaketal., Pretransplant nephrectomy in patients with autosomal dominant polycystic kidney disease, Transplantation Proceedings, vol. 37, no. 2, pp , [13] P.Nunes,A.Mota,R.Alvesetal., Simultaneousrenaltransplantation and native nephrectomy in patients with autosomaldominant polycystic kidney disease, Transplantation Proceedings,vol.39,no.8,pp ,2007. [14] S. M. Lucas, T. C. Mofunanya, W. C. Goggins, and C. P. Sundaram, Staged nephrectomy versus bilateral laparoscopic nephrectomy in patients with autosomal dominant polycystic kidney disease, The Journal of Urology,vol.184,no.5,pp , [15] P.J.Desai,E.P.Castle,S.M.Daleyetal., Bilaterallaparoscopic nephrectomy for significantly enlarged polycystic kidneys: a technique to optimize outcome in the largest of specimens, BJU International,vol.101,no.8,pp ,2008. [16] A. D. Martin, K. L. Mekeel, E. P. Castle et al., Laparoscopic bilateral native nephrectomies with simultaneous kidney transplantation, BJU International, vol. 110, no. 11C, pp. E1003 E1007, [17] M. C. Lipke, V. Bargman, M. Milgrom, and C. P. Sundaram, Limitations of laparoscopy for bilateral nephrectomy for autosomal dominant polycystic kidney disease, The Journal of Urology,vol.177,no.2,pp ,2007. [18]M.N.Rozenfeld,S.A.Ansari,A.Shaibani,E.J.Russell,P. Mohan, and M. C. Hurley, hould patients with autosomal dominant polycystic kidney disease be screened for cerebral aneurysms? American Journal of Neuroradiology, vol.35,no. 1, article 3, [19] M. L. McNally, E. Erturk, G. Oleyourryk, and L. Schoeniger, Laparoscopic cyst decortication using the harmonic scalpel for symptomatic autosomal dominant polycystic kidney disease, Journal of Endourology,vol.15,no.6,pp ,2001.
8 Journal of Transplantation 7 [20]P.Patel,C.Horsfield,F.Compton,J.Taylor,G.Koffman,and J. Olsburgh, Native nephrectomy in transplant patients with autosomal dominant polycystic kidney disease, Annals of the Royal College of Surgeons of England,vol.93,no.5,pp , [21] M. V. Irazabal, J. Huston III, V. Kubly et al., Extended follow-up of unruptured intracranialaneurysms detected by presymptomatic screening inpatients with autosomal dominant polycystickidney disease, Clinical Journal of the American Society of Nephrology,vol.6,no.6,pp ,2011. [22] G. F. Gibbs, J. Huston III, Q. Qian et al., Follow-up of intracranial aneurysms in autosomal-dominant polycystic kidney disease, Kidney International, vol. 65, no. 5, pp , 2004.
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE. Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham
 SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
Donor Kidney Recovery Methods and the Incidence of Lymphatic Complications in Kidney Transplant Recipients
 Donor Kidney Recovery Methods and the Incidence of Lymphatic Complications in Kidney Transplant Recipients The Harvard community has made this article openly available. Please share how this access benefits
Donor Kidney Recovery Methods and the Incidence of Lymphatic Complications in Kidney Transplant Recipients The Harvard community has made this article openly available. Please share how this access benefits
Morbidity and Mortality After Living Kidney Donation, : Survey of United States Transplant Centers
 American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA
 1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor
 Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
Single-lung transplantation in the setting of aborted bilateral lung transplantation
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2011 Single-lung transplantation in the setting of aborted bilateral lung transplantation Varun Puri Tracey Guthrie
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2011 Single-lung transplantation in the setting of aborted bilateral lung transplantation Varun Puri Tracey Guthrie
CABG in the Post-Aprotinin Era: Are We Doing Better? Ziv Beckerman, David Kadosh, Zvi Peled, Keren Bitton-Worms, Oved Cohen and Gil Bolotin
 CABG in the Post-Aprotinin Era: Are We Doing Better? Ziv Beckerman, David Kadosh, Zvi Peled, Keren Bitton-Worms, Oved Cohen and Gil Bolotin DISCLOSURES None Objective(s): Our department routinely used
CABG in the Post-Aprotinin Era: Are We Doing Better? Ziv Beckerman, David Kadosh, Zvi Peled, Keren Bitton-Worms, Oved Cohen and Gil Bolotin DISCLOSURES None Objective(s): Our department routinely used
NIH Public Access Author Manuscript J Am Coll Radiol. Author manuscript; available in PMC 2013 June 24.
 NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Radiol. 2010 January ; 7(1): 73 76. doi:10.1016/j.jacr.2009.06.015. Cerebral Aneurysms Janet C. Miller, DPhil, Joshua A.
NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Radiol. 2010 January ; 7(1): 73 76. doi:10.1016/j.jacr.2009.06.015. Cerebral Aneurysms Janet C. Miller, DPhil, Joshua A.
University of Groningen. Acute kidney injury after cardiac surgery Loef, Berthus Gerard
 University of Groningen Acute kidney injury after cardiac surgery Loef, Berthus Gerard IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
University of Groningen Acute kidney injury after cardiac surgery Loef, Berthus Gerard IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
Predictors and outcomes of laparoscopic nephrectomy in autosomal dominant polycystic kidney disease
 Original Article - Robotics/Laparoscopy https://doi.org/10.4111/icu.2018.59.4.238 pissn 2466-0493 eissn 2466-054X Predictors and outcomes of laparoscopic nephrectomy in autosomal dominant polycystic kidney
Original Article - Robotics/Laparoscopy https://doi.org/10.4111/icu.2018.59.4.238 pissn 2466-0493 eissn 2466-054X Predictors and outcomes of laparoscopic nephrectomy in autosomal dominant polycystic kidney
Urologic Surgical Complications In Renal Transplantation
 Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Medical Review Guidelines Magnetic Resonance Angiography
 Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Transperitoneal Laparoscopic Nephrectomy for Autosomal Dominant Polycystic Kidney Disease
 SCIENTIFIC PAPER Transperitoneal Laparoscopic Nephrectomy for Autosomal Dominant Polycystic Kidney Disease Grégory Verhoest, MD, Arnaud Delreux, MD, Romain Mathieu, MD, Jean-Jacques Patard, MD, Cécile
SCIENTIFIC PAPER Transperitoneal Laparoscopic Nephrectomy for Autosomal Dominant Polycystic Kidney Disease Grégory Verhoest, MD, Arnaud Delreux, MD, Romain Mathieu, MD, Jean-Jacques Patard, MD, Cécile
Autosomal Dominant Polycystic Kidney Disease
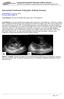 Case Studies [1] July 01, 2014 By Amar Udare, MBBS [2] Case History: 45-year-old female with vague pain in the abdomen. Case History: A 45-year-old female presented with vague pain in the abdomen. A USG
Case Studies [1] July 01, 2014 By Amar Udare, MBBS [2] Case History: 45-year-old female with vague pain in the abdomen. Case History: A 45-year-old female presented with vague pain in the abdomen. A USG
lek Magdalena Puławska-Stalmach
 lek Magdalena Puławska-Stalmach tytuł pracy: Kliniczne i radiologiczne aspekty tętniaków wewnątrzczaszkowych a wybór metody leczenia Summary An aneurysm is a localized, abnormal distended lumen of the
lek Magdalena Puławska-Stalmach tytuł pracy: Kliniczne i radiologiczne aspekty tętniaków wewnątrzczaszkowych a wybór metody leczenia Summary An aneurysm is a localized, abnormal distended lumen of the
2016 Re-Audit of Patient Blood Management in adults undergoing elective, scheduled surgery
 2016 Re-Audit of Patient Blood Management in adults undergoing elective, scheduled surgery 2017 Re-Audit of Red Cell & Platelet Transfusion in Adult Haematology patients South West RTC 2016 Re-Audit of
2016 Re-Audit of Patient Blood Management in adults undergoing elective, scheduled surgery 2017 Re-Audit of Red Cell & Platelet Transfusion in Adult Haematology patients South West RTC 2016 Re-Audit of
Kidney Transplantation
 Kidney Transplantation Current Kidney Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr Current Kidney
Kidney Transplantation Current Kidney Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr Current Kidney
ADPedKD: detailed description of data which will be collected in this registry
 ADPedKD: detailed description of data which will be collected in this registry I. Basic data 1. Patient ID: will be given automatically 2. Personal information - Date of informed consent: DD/MM/YYYY -
ADPedKD: detailed description of data which will be collected in this registry I. Basic data 1. Patient ID: will be given automatically 2. Personal information - Date of informed consent: DD/MM/YYYY -
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Changing Demographics in Death After Devastating Brain Injury
 Changing Demographics in Death After Devastating Brain Injury Andreas H. Kramer MD MSc FRCPC Departments of Critical Care Medicine & Clinical Neurosciences Foothills Medical Center, University of Calgary
Changing Demographics in Death After Devastating Brain Injury Andreas H. Kramer MD MSc FRCPC Departments of Critical Care Medicine & Clinical Neurosciences Foothills Medical Center, University of Calgary
HHS Public Access Author manuscript J Am Coll Surg. Author manuscript; available in PMC 2016 July 30.
 Outcomes and Durability of Hepatic Reduction after Combined Partial Hepatectomy and Cyst Fenestration for Massive Polycystic Liver Disease Fouad T Chebib, MD, Amber Harmon, Maria V Irazabal Mira, MD, Yeon
Outcomes and Durability of Hepatic Reduction after Combined Partial Hepatectomy and Cyst Fenestration for Massive Polycystic Liver Disease Fouad T Chebib, MD, Amber Harmon, Maria V Irazabal Mira, MD, Yeon
Nephrology Case Presentation for PCKD. Douglas A. Stahura 24 January 2002 With update 2018
 Nephrology Case Presentation for PCKD Douglas A. Stahura 24 January 2002 With update 2018 Case Presentation l 48 y/o WM presents with back pain Sharp, over L side/ribs Intermittent but severe 8/10 No radiation
Nephrology Case Presentation for PCKD Douglas A. Stahura 24 January 2002 With update 2018 Case Presentation l 48 y/o WM presents with back pain Sharp, over L side/ribs Intermittent but severe 8/10 No radiation
Expanded Criteria Recipients: Are there any Limits
 Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
Shuma Hirashio 1,2, Shigehiro Doi 1 and Takao Masaki 1*
 Hirashio et al. Renal Replacement Therapy (2018) 4:24 https://doi.org/10.1186/s41100-018-0164-9 CASE REPORT Open Access Magnetic resonance imaging is effective for evaluating the therapeutic effect of
Hirashio et al. Renal Replacement Therapy (2018) 4:24 https://doi.org/10.1186/s41100-018-0164-9 CASE REPORT Open Access Magnetic resonance imaging is effective for evaluating the therapeutic effect of
Michael Minarich, MD General Surgery Resident, PGY4 Cooper University Hospital
 BMI as Major Preoperative Risk Factor for Intraabdominal Infection After Distal Pancreatectomy: an Analysis of National Surgical Quality Improvement Program Database Michael Minarich, MD General Surgery
BMI as Major Preoperative Risk Factor for Intraabdominal Infection After Distal Pancreatectomy: an Analysis of National Surgical Quality Improvement Program Database Michael Minarich, MD General Surgery
Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review
 Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review Jessica Ludolph 1 Lynsey Biondi, MD 1,2 and Michael Moritz, MD 1,2 1 Department of Surgery,
Incidence of Rejection in Renal Transplant Surgery in the LVHN Population Leading to Graft Failure: 6 Year Review Jessica Ludolph 1 Lynsey Biondi, MD 1,2 and Michael Moritz, MD 1,2 1 Department of Surgery,
Patient Name: MRN: DOB: Treatment Location:
 Page 1 of 5 I. TO (Required) This Section is required to be completed by all patients who undergo kidney transplant surgery. I hereby consent to and authorize Dr. and his/her assistant(s), including supervised
Page 1 of 5 I. TO (Required) This Section is required to be completed by all patients who undergo kidney transplant surgery. I hereby consent to and authorize Dr. and his/her assistant(s), including supervised
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Role of Gender in TEVAR and EVAR results from the GREAT registry
 Role of Gender in TEVAR and EVAR results from the GREAT registry Mauro Gargiulo Vascular Surgery University of Bologna - DIMES Policlinico S.Orsola-Malpighi Bologna, Italy mauro.gargiulo2@unibo.it Disclosure
Role of Gender in TEVAR and EVAR results from the GREAT registry Mauro Gargiulo Vascular Surgery University of Bologna - DIMES Policlinico S.Orsola-Malpighi Bologna, Italy mauro.gargiulo2@unibo.it Disclosure
Correspondence should be addressed to Taha Numan Yıkılmaz;
 Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
OUTCOME OF LAPAROSCOPIC DONOR NEPHRECTOMY: OUR INSTITUTIONAL EXPERIENCE
 OUTCOME OF LAPAROSCOPIC DONOR NEPHRECTOMY: OUR INSTITUTIONAL EXPERIENCE Rajaraman Thiagarajan 1, Balaji A. R 2, Ayesha Shaheen 3, Chandramurali Raveendran 4, Subhakanesh S 5, Ashok Kumar R 6, Jessima S
OUTCOME OF LAPAROSCOPIC DONOR NEPHRECTOMY: OUR INSTITUTIONAL EXPERIENCE Rajaraman Thiagarajan 1, Balaji A. R 2, Ayesha Shaheen 3, Chandramurali Raveendran 4, Subhakanesh S 5, Ashok Kumar R 6, Jessima S
For more information about how to cite these materials visit
 Author(s): Silas P. Norman, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Silas P. Norman, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Postoperative monitoring after
 Postoperative monitoring after kidney transplantation Bundit sakulchairungrueng,md Vascular and Transplantation Unit Faculty of Medicine Ramathibodi Hospital Mahidol University Reference Introduction A
Postoperative monitoring after kidney transplantation Bundit sakulchairungrueng,md Vascular and Transplantation Unit Faculty of Medicine Ramathibodi Hospital Mahidol University Reference Introduction A
Uroradiology For Medical Students
 Uroradiology For Medical Students Lesson 8 Computerized Tomography 2 American Urological Association Objectives In this lesson you will: Gain more experience reading CT images Learn how computer generated
Uroradiology For Medical Students Lesson 8 Computerized Tomography 2 American Urological Association Objectives In this lesson you will: Gain more experience reading CT images Learn how computer generated
Neurosurgical decision making in structural lesions causing stroke. Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery)
 Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Pancreas and Pancreas-Kidney Transplantation By: Kay R. Brown, CLCP
 Pancreas and Pancreas-Kidney Transplantation By: Kay R. Brown, CLCP Pancreas transplant recipients are usually under age 50. The majority of pancreas transplants are performed on diabetics, who are generally
Pancreas and Pancreas-Kidney Transplantation By: Kay R. Brown, CLCP Pancreas transplant recipients are usually under age 50. The majority of pancreas transplants are performed on diabetics, who are generally
Management of Cerebral Aneurysms in Polycystic Kidney Disease. Dr H Stockley Consultant Neuroradiologist Greater Manchester Neuroscience Centre
 Management of Cerebral Aneurysms in Polycystic Kidney Disease Dr H Stockley Consultant Neuroradiologist Greater Manchester Neuroscience Centre What is a cerebral aneurysm? Developmental degenerative arterial
Management of Cerebral Aneurysms in Polycystic Kidney Disease Dr H Stockley Consultant Neuroradiologist Greater Manchester Neuroscience Centre What is a cerebral aneurysm? Developmental degenerative arterial
CUAJ Techniques in Urology Techniques: Orthotopic kidney transplantation
 Techniques Orthotopic kidney transplantation in patients with diseased inferior vena cavas E. Chan 1 ; Alp Sener 1,2 ; Vivian C. McAlister 1,2, Patrick P. Luke 1,2 1 Western University Schulich School
Techniques Orthotopic kidney transplantation in patients with diseased inferior vena cavas E. Chan 1 ; Alp Sener 1,2 ; Vivian C. McAlister 1,2, Patrick P. Luke 1,2 1 Western University Schulich School
Preoperative tests (update)
 National Institute for Health and Care Excellence. Preoperative tests (update) Routine preoperative tests for elective surgery NICE guideline NG45 Appendix N: Research recommendations April 2016 Developed
National Institute for Health and Care Excellence. Preoperative tests (update) Routine preoperative tests for elective surgery NICE guideline NG45 Appendix N: Research recommendations April 2016 Developed
Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital
 ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
Living Kidney Donation. Dr. Joseph Keith Melancon
 Living Kidney Donation Dr. Joseph Keith Melancon Thanks to our speaker! Keith Melancon, MD Chief Transplant Institute And Division Of Transplant Surgery; Medical Director GW/ Ron And Joy Paul Kidney Center
Living Kidney Donation Dr. Joseph Keith Melancon Thanks to our speaker! Keith Melancon, MD Chief Transplant Institute And Division Of Transplant Surgery; Medical Director GW/ Ron And Joy Paul Kidney Center
Experience of endovascular procedures on abdominal and thoracic aorta in CA region
 Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UNIVERSITY OF MARYLAND MEDICAL CENTER WE HEAL, WE TEACH, WE DISCOVER, WE CARE
 Kidney Transplant Program Patient Guide Overview The University of Maryland Kidney Transplant Program has saved the lives of thousands of patients who have end stage renal disease. By replacing kidneys
Kidney Transplant Program Patient Guide Overview The University of Maryland Kidney Transplant Program has saved the lives of thousands of patients who have end stage renal disease. By replacing kidneys
JAWDA Bariatric Quality Performance Indicators. JAWDA Quarterly Guidelines for Bariatric Surgery (BS)
 JAWDA Guidelines for Bariatric Surgery (BS) January 2019 1 Table of Contents Executive Summary... 3 About this Guidance... 4 Bariatric Surgery Indicators... 5 Appendix A: Glossary... 19 Appendix B: Approved
JAWDA Guidelines for Bariatric Surgery (BS) January 2019 1 Table of Contents Executive Summary... 3 About this Guidance... 4 Bariatric Surgery Indicators... 5 Appendix A: Glossary... 19 Appendix B: Approved
Case Report Crossed Renal Ectopia without Fusion An Unusual Cause of Acute Abdominal Pain: A Case Report
 Case Reports in Urology Volume 2012, Article ID 728531, 4 pages doi:10.1155/2012/728531 Case Report Crossed Renal Ectopia without Fusion An Unusual Cause of Acute Abdominal Pain: A Case Report D. P. Ramaema,
Case Reports in Urology Volume 2012, Article ID 728531, 4 pages doi:10.1155/2012/728531 Case Report Crossed Renal Ectopia without Fusion An Unusual Cause of Acute Abdominal Pain: A Case Report D. P. Ramaema,
6. Endovascular aneurysm repair
 Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
CYSTIC DISEASES of THE KIDNEY. Dr. Nisreen Abu Shahin
 CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use
 Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Supplementary Online Content
 Supplementary Online Content Smith D, Chudgar A, Daly B, Cooper M. Evaluation of potential renal transplant recipients with computed tomography angiography. Arch Intern Med. doi: 10.1001/archsurg.2012.1466.
Supplementary Online Content Smith D, Chudgar A, Daly B, Cooper M. Evaluation of potential renal transplant recipients with computed tomography angiography. Arch Intern Med. doi: 10.1001/archsurg.2012.1466.
Management of a Recipient with a Failed Kidney Transplant. Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania
 Management of a Recipient with a Failed Kidney Transplant Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Disclosures Grant support: Bristol-Myers and Squibb Pharmaceuticals,
Management of a Recipient with a Failed Kidney Transplant Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Disclosures Grant support: Bristol-Myers and Squibb Pharmaceuticals,
Takashi Yagisawa 1,2*, Makiko Mieno 1,3, Norio Yoshimura 1,4, Kenji Yuzawa 1,5 and Shiro Takahara 1,6
 Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Sara Schaenzer Grand Rounds January 24 th, 2018
 Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
Sara Schaenzer Grand Rounds January 24 th, 2018 Bladder Anatomy Ureter Anatomy Areas of Injury Bladder: Posterior bladder wall above trigone Ureter Crosses beneath uterine vessels At pelvic brim when ligating
KDIGO Controversies Conference on Autosomal Dominant Polycystic Kidney Disease (ADPKD)
 KDIGO Controversies Conference on Autosomal Dominant Polycystic Kidney Disease (ADPKD) January 16 19, 2014 Edinburgh, United Kingdom Kidney Disease: Improving Global Outcomes (KDIGO) is an international
KDIGO Controversies Conference on Autosomal Dominant Polycystic Kidney Disease (ADPKD) January 16 19, 2014 Edinburgh, United Kingdom Kidney Disease: Improving Global Outcomes (KDIGO) is an international
Surgically Discovered Xanthogranulomatous Pyelonephritis Invading Inferior Vena Cava with Coexisting Renal Cell Carcinoma
 Case Study TheScientificWorldJOURNAL (2009) 9, 5 9 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.6 Surgically Discovered Xanthogranulomatous Pyelonephritis Invading Inferior Vena Cava with Coexisting
Case Study TheScientificWorldJOURNAL (2009) 9, 5 9 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2009.6 Surgically Discovered Xanthogranulomatous Pyelonephritis Invading Inferior Vena Cava with Coexisting
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Research Article Propensity Score-Matched Analysis of Open Surgical and Endovascular Repair for Type B Aortic Dissection
 Hindawi Publishing Corporation International Journal of Vascular Medicine Volume 2011, Article ID 364046, 7 pages doi:10.1155/2011/364046 Research Article Propensity Score-Matched Analysis of Open Surgical
Hindawi Publishing Corporation International Journal of Vascular Medicine Volume 2011, Article ID 364046, 7 pages doi:10.1155/2011/364046 Research Article Propensity Score-Matched Analysis of Open Surgical
LIVE KIDNEY DONOR RISK PREDICTION ; NEW PARADIGM, NEW CALCULATORS PEDRAM AHMADPOOR MD
 LIVE KIDNEY DONOR RISK PREDICTION ; NEW PARADIGM, NEW CALCULATORS PEDRAM AHMADPOOR MD Outline: PART 1 : Update on safety of nephrectomy for living donor candidate PART 2 : Latest guideline recommendation
LIVE KIDNEY DONOR RISK PREDICTION ; NEW PARADIGM, NEW CALCULATORS PEDRAM AHMADPOOR MD Outline: PART 1 : Update on safety of nephrectomy for living donor candidate PART 2 : Latest guideline recommendation
ECMO vs. CPB for Intraoperative Support: How do you Choose?
 ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study
 Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
ORIGINAL ARTICLE. Eric F. Martin, 1 Jonathan Huang, 3 Qun Xiang, 2 John P. Klein, 2 Jasmohan Bajaj, 4 and Kia Saeian 1
 LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
CORONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW
 CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
WASHINGTON UNIVERSITY SCHOOL OF MEDICINE. Cranial Health History Form
 WASHINGTON UNIVERSITY SCHOOL OF MEDICINE Cranial Health History Form Welcome to the Neurosurgery Department at Washington University. To help us treat you, please fill this form out completely. Your Name:
WASHINGTON UNIVERSITY SCHOOL OF MEDICINE Cranial Health History Form Welcome to the Neurosurgery Department at Washington University. To help us treat you, please fill this form out completely. Your Name:
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Tubulointerstitial Renal Disease. Anna Vinnikova, MD Division of Nephrology
 Tubulointerstitial Renal Disease Anna Vinnikova, MD Division of Nephrology Part I: Cystic Renal Disease www.pathguy.com Simple cysts Simple cysts May be multiple Usually 1 5cm, may be bigger Translucent,
Tubulointerstitial Renal Disease Anna Vinnikova, MD Division of Nephrology Part I: Cystic Renal Disease www.pathguy.com Simple cysts Simple cysts May be multiple Usually 1 5cm, may be bigger Translucent,
Kidney Transplant Outcomes In Elderly Patients. Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania
 Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
Renal cell carcinoma of the native kidney in a renal transplant recipient
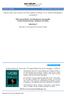 www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Renal cell carcinoma of the native kidney in a renal transplant recipient Vikrampal Bhatti, Ananthalaxmi Vangapalli, Deepti Bhattacharya,
www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Renal cell carcinoma of the native kidney in a renal transplant recipient Vikrampal Bhatti, Ananthalaxmi Vangapalli, Deepti Bhattacharya,
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
International Principles of Deceased Donor Organ Allocation
 International Principles of Deceased Donor Organ Allocation The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Accessed
International Principles of Deceased Donor Organ Allocation The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Accessed
Research Article Abdominal Aortic Aneurysms and Coronary Artery Disease in a Small Country with High Cardiovascular Burden
 ISRN Cardiology, Article ID 825461, 4 pages http://dx.doi.org/10.1155/2014/825461 Research Article Abdominal Aortic Aneurysms and Coronary Artery Disease in a Small Country with High Cardiovascular Burden
ISRN Cardiology, Article ID 825461, 4 pages http://dx.doi.org/10.1155/2014/825461 Research Article Abdominal Aortic Aneurysms and Coronary Artery Disease in a Small Country with High Cardiovascular Burden
Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication for Repeat Metastasectomy
 Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Impact of Screening Colonoscopy on Outcomes in Colon Cancer Surgery
 Impact of Screening Colonoscopy on Outcomes in Colon Cancer Surgery The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation
Impact of Screening Colonoscopy on Outcomes in Colon Cancer Surgery The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation
DIVISION OF NEPHROLOGY
 The Division s funding from the NIH has increased from $3.7 Million in 2001 to over $11 Million in 2006. DIVISION OF NEPHROLOGY DR. BARBARA MURPHY was voted President-Elect of the American Society of Transplantation
The Division s funding from the NIH has increased from $3.7 Million in 2001 to over $11 Million in 2006. DIVISION OF NEPHROLOGY DR. BARBARA MURPHY was voted President-Elect of the American Society of Transplantation
National Vascular Registry
 National Vascular Registry AAA Repair Patient Details Patient Consent* 0 No 1 Yes 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s)
National Vascular Registry AAA Repair Patient Details Patient Consent* 0 No 1 Yes 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s)
The role of Imaging (scans of the kidneys) in the management of Autosomal Dominant Polycystic Kidney Disease
 The role of Imaging (scans of the kidneys) in the management of Autosomal Dominant Polycystic Kidney Disease Dr Roslyn Simms NIHR Clinical Lecturer in Nephrology Saturday 17 th September 2016 Role of Imaging
The role of Imaging (scans of the kidneys) in the management of Autosomal Dominant Polycystic Kidney Disease Dr Roslyn Simms NIHR Clinical Lecturer in Nephrology Saturday 17 th September 2016 Role of Imaging
Impact of ultrasound examination shortly after kidney transplantation
 Eur Surg (2017) 49:140 144 DOI 10.1007/s10353-017-0467-z Impact of ultrasound examination shortly after kidney transplantation Christoph Schwarz Jakob Mühlbacher Georg A. Böhmig Marin Purtic Eleonore Pablik
Eur Surg (2017) 49:140 144 DOI 10.1007/s10353-017-0467-z Impact of ultrasound examination shortly after kidney transplantation Christoph Schwarz Jakob Mühlbacher Georg A. Böhmig Marin Purtic Eleonore Pablik
Transplant surgery: the latest
 Transplant surgery: the latest Professor Nizam Mamode Guy s and St Thomas Hospital Evelina London Children s Hospital Great Ormond Street Hospital What do we do? Page 2 Kidney transplants Living donor
Transplant surgery: the latest Professor Nizam Mamode Guy s and St Thomas Hospital Evelina London Children s Hospital Great Ormond Street Hospital What do we do? Page 2 Kidney transplants Living donor
 Demographic Data Group Study Cohort Control p N 60 20 Age, Mean (years) 36.3 64.4 < 0.001 Age, Median (years) 33.2 64 < 0.001 Male 41 (68.4%) 4 (20%) 0.001 Female 19 (31.6%) 16 (80%) 0.001 Mechanism of
Demographic Data Group Study Cohort Control p N 60 20 Age, Mean (years) 36.3 64.4 < 0.001 Age, Median (years) 33.2 64 < 0.001 Male 41 (68.4%) 4 (20%) 0.001 Female 19 (31.6%) 16 (80%) 0.001 Mechanism of
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH
 ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in Adults: 6 Years Experience in One Center
 Hindawi BioMed Research International Volume 2017, Article ID 6743512, 4 pages https://doi.org/10.1155/2017/6743512 Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in
Hindawi BioMed Research International Volume 2017, Article ID 6743512, 4 pages https://doi.org/10.1155/2017/6743512 Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in
National Vascular Registry
 National Vascular Registry AAA Repair Patient Details Patient Consent* 0 No 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s)
National Vascular Registry AAA Repair Patient Details Patient Consent* 0 No 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s)
Renal Cystic Disease. Dr H Bierman
 Renal Cystic Disease Dr H Bierman Objectives Be able to diagnose renal cystic disease Genetic / non-genetic Be able to describe patterns of various renal cystic disease on routine imaging studies Be able
Renal Cystic Disease Dr H Bierman Objectives Be able to diagnose renal cystic disease Genetic / non-genetic Be able to describe patterns of various renal cystic disease on routine imaging studies Be able
Commonly Asked Questions about Kidney Transplants
 Commonly Asked Questions about Kidney Transplants Should I consider having a kidney We encourage you to get as much information as possible. Ask questions. Talk with other transplant patients and talk
Commonly Asked Questions about Kidney Transplants Should I consider having a kidney We encourage you to get as much information as possible. Ask questions. Talk with other transplant patients and talk
Pediatric Kidney Transplantation
 Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Renal and extrarenal manifestations of autosomal dominant polycystic kidney disease
 Brazilian Journal of Medical and Biological Research (2006) 39: 533-538 Autosomal dominant polycystic kidney disease ISSN 0100-879X 533 Renal and extrarenal manifestations of autosomal dominant polycystic
Brazilian Journal of Medical and Biological Research (2006) 39: 533-538 Autosomal dominant polycystic kidney disease ISSN 0100-879X 533 Renal and extrarenal manifestations of autosomal dominant polycystic
Bilateral hand-assisted laparoscopic nephrectomy in adult polycystic kidney disease patients: a UK centre experience
 Journal of Medicine and Life Vol. 5, Issue 2, April June 2012, pp.226 231 Bilateral hand-assisted laparoscopic nephrectomy in adult polycystic kidney disease patients: a UK centre experience Mak DK-C**,
Journal of Medicine and Life Vol. 5, Issue 2, April June 2012, pp.226 231 Bilateral hand-assisted laparoscopic nephrectomy in adult polycystic kidney disease patients: a UK centre experience Mak DK-C**,
Renal Transplant Surgery
 Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Supplementary Online Content
 1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009
 Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
POLYCYSTIC KIDNEY DISEASE
 PKD YOUR GUIDE TO LIVING WITH POLYCYSTIC KIDNEY DISEASE www.endpkd.ca ABOUT PKD WHAT IS POLYCYSTIC KIDNEY DISEASE? Polycystic kidney disease (PKD) is a group of genetic diseases that cause fl uid-filled
PKD YOUR GUIDE TO LIVING WITH POLYCYSTIC KIDNEY DISEASE www.endpkd.ca ABOUT PKD WHAT IS POLYCYSTIC KIDNEY DISEASE? Polycystic kidney disease (PKD) is a group of genetic diseases that cause fl uid-filled
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies. Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018
 Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Five years of living donor kidney transplantation at University clinical center Tuzla, Bosnia and Herzegovina, from 1999 through 2004
 Clinical Science Five years of living donor kidney transplantation at University clinical center Tuzla, Bosnia and Herzegovina, from 1999 through 2004 Senaid Trnačević 1, Goran Imamović 2, Mustafa Bazardžanović
Clinical Science Five years of living donor kidney transplantation at University clinical center Tuzla, Bosnia and Herzegovina, from 1999 through 2004 Senaid Trnačević 1, Goran Imamović 2, Mustafa Bazardžanović
Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results
 Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Clinical Study Do Renal Cysts Affect the Success of Extracorporeal Shockwave Lithotripsy? A Retrospective Comparative Study
 Advances in Urology Volume 2013, Article ID 978180, 4 pages http://dx.doi.org/10.1155/2013/978180 Clinical Study Do Renal Cysts Affect the Success of Extracorporeal Shockwave Lithotripsy? A Retrospective
Advances in Urology Volume 2013, Article ID 978180, 4 pages http://dx.doi.org/10.1155/2013/978180 Clinical Study Do Renal Cysts Affect the Success of Extracorporeal Shockwave Lithotripsy? A Retrospective
Treatment of choice for end stage renal disease Imaging to establish baseline and diagnosis of potential complications Review common surgical
 Treatment of choice for end stage renal disease Imaging to establish baseline and diagnosis of potential complications Review common surgical techniques Review normal appearance Discuss US diagnosis of
Treatment of choice for end stage renal disease Imaging to establish baseline and diagnosis of potential complications Review common surgical techniques Review normal appearance Discuss US diagnosis of
Supplementary Online Content
 Supplementary Online Content Inohara T, Manandhar P, Kosinski A, et al. Association of renin-angiotensin inhibitor treatment with mortality and heart failure readmission in patients with transcatheter
Supplementary Online Content Inohara T, Manandhar P, Kosinski A, et al. Association of renin-angiotensin inhibitor treatment with mortality and heart failure readmission in patients with transcatheter
Bilateral Simultaneous Anterior Cruciate Ligament Injury: A Case Report and National Survey of Orthopedic Surgeon Management Preference
 Bilateral Simultaneous Anterior Cruciate Ligament Injury: A Case Report and National Survey of Orthopedic Surgeon Management Preference The Harvard community has made this article openly available. Please
Bilateral Simultaneous Anterior Cruciate Ligament Injury: A Case Report and National Survey of Orthopedic Surgeon Management Preference The Harvard community has made this article openly available. Please
