Education for secondary prevention of foot ulcers in people with diabetes: a randomised controlled trial
|
|
|
- Wendy Williamson
- 5 years ago
- Views:
Transcription
1 Diabetologia (2008) 51: DOI /s ARTICLE Education for secondary prevention of foot ulcers in people with diabetes: a randomised controlled trial N. B. Lincoln & K. A. Radford & F. L. Game & W. J. Jeffcoate Received: 14 April 2008 / Accepted: 2 July 2008 / Published online: 30 August 2008 # Springer-Verlag 2008 Abstract Aims/hypothesis This observer-blind, randomised controlled trial was designed to determine the effect of a foot care education programme in the secondary prevention of foot ulcers. Methods People with newly healed foot ulcers attending one of three specialist clinics were allocated to receive either targeted, one-to-one education or usual care, using a computer-generated random allocation sequence that had been prepared in advance but which was concealed from the clinical researcher. The primary outcome was ulcer incidence at 12 months. Secondary outcomes were ulcer incidence at 6 months and incidence of amputation, mood (Hospital Anxiety and Depression Scale) and quality of life (Diabetic Foot Ulcer Scale) at 6 and 12 months. Protective foot care behaviours (Nottingham Assessment of Functional Footcare) were assessed at 12 months. Results There were 87 (mean [SD] age 63.5 [12.1] years) patients in the intervention group and 85 control patients (mean [SD] age 64.9 [10.9] years). The groups were comparable at baseline. No significant differences (p> 0.05) were observed between groups in ulcer incidence at either 6 months (intervention 30%, control 21%) or 12 months (intervention 41%, control 41%). Recommended foot care behaviours at 12 months were better in the N. B. Lincoln Institute of Work, Health and Organisations, University of Nottingham, Nottingham, UK K. A. Radford : F. L. Game : W. J. Jeffcoate (*) Foot Ulcer Trials Unit, Department of Diabetes and Endocrinology, Nottingham University Hospitals Trust, City Hospital Campus, Nottingham NG5 1PB, UK wjeffcoate@futu.co.uk intervention than in the control group (p=0.03), but education had no significant (p>0.05) effect on mood, quality of life or amputations. Conclusions/interpretation Even though the intervention was associated with improved foot care behaviour, there was no evidence that this programme of targeted education was associated with clinical benefit in this population when compared with usual care. The usefulness and optimal delivery of education to such a high-risk group requires further evaluation. Trial registration: ClinicalTrials.gov NCT Funding: Diabetes UK project grant RD02/ Keywords Behaviour. Diabetes. Education. Foot. Ulcer Abbreviations DFS Diabetic Foot Scale DFS-SF Short Form Diabetic Foot Scale HADS Hospital Anxiety and Depression Scale NAFF Nottingham Assessment of Functional Footcare Introduction Disease of the foot represents a major health problem in diabetes and is the source of enormous cost to healthcare services [1]. Healing is delayed and uncertain [2], and the incidence of amputation has been reported to be as high as 27% even in expert centres [3]. Since the options for specific therapy are limited [4], great emphasis is placed on prevention and on foot care education in particular [5 8]. While the importance of patient knowledge is undeniable, the effectiveness of education in reducing ulcer incidence has not been clearly demonstrated, as indicated by recent
2 Diabetologia (2008) 51: systematic [9] and non-systematic [10, 11] reviews. A reduced incidence of new foot ulcers has been shown when foot care education was included as part of an integrated package of diabetes care delivered to selected and relatively disadvantaged groups in the USA [12, 13], but has not been confirmed in other studies [14 19]. If education does have an impact on ulcer incidence, it might be expected to be most marked in patients at greatest risk, i.e. those who have had an ulcer before [19, 20]. In a Swedish cohort study of 558 people managed between 1983 and 1990 ulcers recurred in 34, 61 and 70% at 1, 3 and 5 years, and major amputation in 3, 10 and 12% [21]. Of 226 patients with healed ulcers who were managed in the UK, 91 (40.3%) developed a recurrent or new ulcer after a median 126 days (range ) [22]. However, only one study of education has specifically targeted patients who had a previous lesion [23]. In that study, 203 patients admitted to hospital for a foot problem (ulcer, amputation, infection) were randomised to receive a single 1-h education session, including graphic images of foot problems, or to receive the usual care. While details of allocation concealment and blinding were not specified, the intervention group was reported to have a threefold, highly significant reduction in the incidence of both new ulcers and amputation within 13 months. If confirmed, this observation should inform clinical practice and structured foot care education should be adopted as part of the routine management of all patients with a healed foot lesion. The purpose of the present study was to seek to confirm those findings [23] by evaluating the provision of education in the secondary prevention of foot ulcers in patients attending three specialist footcare centres. Methods This study was funded by Diabetes UK and approved by the Local Research Ethics Committees of Nottingham and Southern Derbyshire, UK. Patients attending specialist foot clinics in Nottingham (Nottingham City Hospital and Queen s Medical Centre) and Derby (Derbyshire Royal Infirmary) were considered for inclusion in the study. Patients with diabetes and recently healed ulcers of the foot (on or below the malleoli) were eligible if they had remained ulcer-free for 28 days. Patients were excluded if they: lived in institutional care, had a documented history of dementia, had other serious medical problems, were non- English-speaking and did not have an English-speaking carer, lived at a distance of more than 50 miles, were in another study, withheld consent or if they were members of the focus group involved in developing the education programme used in the study. Biographical details were recorded, including age, sex, educational level, social status and whether participants were living alone or with a partner or carer. Socio-economic groupings were established using the Standard Occupational Classification system [24] (I, professional; II, managerial and technical; III, skilled non-manual and manual; IV, partly skilled; V, unskilled occupations). Information was extracted from medical records on diabetes type and duration, diabetes control (HbA 1c in the previous 3 months), nephropathy (serum creatinine >120 μmol/l or persistent proteinuria) and retinopathy. Details of the previously healed ulcer were documented. Baseline examination was conducted by a diabetes research nurse specialist or a research occupational therapist (K. A. Radford) trained in foot examination. The presence of sensory neuropathy was established using a 10 g monofilament on three sites (the plantar aspect of the hallux and under the 1st and 5th metatarsophalangeal joints). Pin prick sensation (Neurotips: Owen-Mumford, Woodstock, UK) was documented as being either present or absent on the dorsum of the foot. Vibration perception was recorded on the pulp of the hallux using a Neurosthesiometer (Horwell Scientific Laboratory Supplies, Nottingham, UK), with a recording of 25 V taken as abnormal. The presence of peripheral arterial disease was defined as having both pedal pulses missing. The Hospital Anxiety and Depression Scale (HADS) [25] was used as a measure of mood. Participants were randomised 1:1 to receive either education or not by telephoning an independent randomisation centre which held a computer-generated random allocation sequence prepared in advance of the study. The sequence of random allocations was concealed from the researcher (K. A. Radford) recruiting participants. The intervention group received a single 1-h education session within 4 weeks of randomisation. The education session was delivered to participants in their own homes, with or without their carers, by the researcher (K. A. Radford), who had been specifically trained. The content of the education session was based on the International Consensus on the Diabetic Foot [26], as well as the programme described by Malone and colleagues [23]. The content and wording of the educational material and the style of illustrations was also informed by discussion with a consumer focus group. The objective of the educational intervention was to prevent ulcer recurrence by lessening the impact of factors known to precipitate new ulcers. Participants were given a brief explanation of the principal causes of foot ulcers (impaired circulation, loss of sensation and secondary infection) [27, 28]. Their feet were examined and any personal risk factors (such as deformity, ischaemia and neuropathy) were identified and explained. Shoes and insoles were examined for wear and tear and patterns of use and to determine whether choice of footwear constituted a particular risk for new ulceration.
3 1956 Diabetologia (2008) 51: Participants were shown illustrations of foot lesions, since the use of illustrations was a feature of the intervention in the study reported by Malone and colleagues [23]. Illustrations included pictures of a foot with poor blood supply, signs of infection, a typical neuropathic ulcer, athlete s foot, Charcot s foot, a gangrenous toe and examples of accidental damage (burnt feet from dozing in front of a fire; a shoe sole penetrated by a nail). There was also a cartoon illustrating the development of a plantar neuropathic ulcer. Emphasis was placed on avoiding accidental damage by adopting preventive behaviours, such as checking the temperature of bath water, not walking barefoot and promoting foot health by washing, drying, moisturising and daily self-examination. Participants were also advised to contact the clinic at the first sign of any new or recurrent foot problem. Education sessions were supplemented by handouts to reinforce the information given. These handouts were those used routinely in the clinics and included information about the causes of foot ulcers (neuropathy, arteriopathy and infection), foot care and ways to reduce the likelihood of accidents. Patients were telephoned 4 weeks after the educational visit and a semistructured format used to discuss issues raised at the time of the home visit and to determine whether any points needed clarification or reinforcement. Those randomised to usual care received the same foot care leaflets but were otherwise managed according to usual practice. Such usual practice included no structured education and many patients were discharged to the care of their general practitioner, with or without input from a community podiatrist. Any education regarding prevention of ulcer recurrence was unstructured and opportunistic. The clinical care of patients in both groups was otherwise unaffected by the study. They were provided with regular podiatry and suitable orthoses when appropriate. Their overall medical care followed national UK guidelines and was supervised by GP, specialist clinic or both according to individual circumstances. Outcomes were assessed at 6 and 12 months after randomisation, by observers blind to the group allocation of the participants. The success of blinding was not assessed, but it was believed to be complete. The primary outcome measure was the occurrence of any new ulcers and was determined by medical and foot clinic records in the three hospitals supported by questionnaires sent to the patient. Outcomes at 12 months were also corroborated by writing to participants general practitioners. Where a discrepancy between the patient report and medical records was found, the latter were re-checked and the probable cause of the discrepancy determined by blinded observers. A random sample of 20 cases in whom no recurrent foot problems were reported by the patient or GP, or recorded in the medical records was further cross-checked against community podiatry records by a blinded observer. Secondary outcomes were assessed by questionnaires that were posted to participants with a reply-paid envelope. Those who did not return the questionnaires within 3 weeks were contacted by telephone and reminded. If questionnaires were returned incomplete, a blinded researcher also contacted the participants by telephone to ask them to complete the missing items. The outcome questionnaire included questions about the incidence of new ulcers and whether the patient had had any major or minor amputations. Participants were also asked to complete HADS as a measure of mood, which comprises seven items on anxiety and seven on depression and is suitable for people with physical illness. The Diabetic Foot Scale (DFS) [29] was included as a disease-specific measure of quality of life (although only items contained in the short form DFS [DFS-SF] [30] were analysed). This assesses the effect of foot problems on aspects of daily life, such as leisure, physical health, daily activities, emotions, family, friends and satisfaction. Participants were also asked to complete the Nottingham Assessment of Functional Footcare (NAFF) questionnaire [31] at 12 months, by which the frequency of 29 foot care behaviours was assessed. This questionnaire was developed specifically to assess foot care behaviour for the study, as no previous measure was identified as being suitable. The questionnaire had not been fully assessed at the time the study was started and was used only at 12 months. All questionnaires were scored by a researcher blind to the group allocation of participants and entered on the database. The relative risk was calculated for ulcers and amputations, using analysis by intention to treat. For secondary outcome questionnaires, the area under the curve was calculated only in returned questionnaires and compared using Mann Whitney U tests, with significance being set at p=0.05. To detect a reduction in 12-month incidence of new ulceration from 35 to 15% (two-sided, 80%, p= 0.05), 82 participants were required in each group. Although sizeable, such a reduction would have been less than that reported by Malone and colleagues [23]. Results were analysed using SPSS version 14. Results During the 30 month recruitment period (April 2003 to September 2005), 1729 patients attended foot clinics in Nottingham (Nottingham City Hospital and Queen s Medical Centre) and at Derbyshire Royal Infirmary. Of these, 264 had had a foot ulcer that had recently healed, with 259 remaining healed and ulcer-free for 28 days. A total of 81 of these were excluded: five living in institutional care, one with documented dementia, one who died before giving consent, one who lived too far away, eleven with other serious medical problems, three in other studies, one who
4 Diabetologia (2008) 51: was involved in developing the education programme, four who were missed by error and 54 who refused consent. The recruitment and follow-up of participants is shown in Fig. 1. Altogether, 178 patients gave informed consent and were randomised to the study. Six were withdrawn: one who was randomised twice by mistake, two who became ill before being seen (one in treatment group, one in control group), one who withdrew consent before being seen and one who was erroneously recruited because his previous ulcer had been above the malleoli. The remaining 172 were included in the analysis (85 control, 87 intervention group); their baseline characteristics are summarised in Table 1. Patients recruited to the two groups were well matched at baseline. Ten participants died: five before the 6 month follow-up (two intervention, three control) and a further five by 12 months (four intervention, one control). Questionnaire completion rates are shown in Fig. 1. There were no significant differences in the occurrence of either new ulceration or amputation (Table 2). Only two of the amputations were major, one in each group. A small number of answers was missing from the questionnaire replies. At 6 months there were six returned DFS-SF forms with questions unanswered. Three of these had one question unanswered and one had two unanswered. In all four, the mean of all other responses in the subscale was inserted. In the other two cases, more than two replies were missing and these were not extrapolated. At 12 months, nine replies had missing items. The answer was provided by inserting the mean score in the six with one missing response and in the one with two missing responses. In the two other cases with more replies missing, these were not filled in by extrapolation. One participant left two questions unanswered on the HADS; these were replaced with the relevant mean scores. For the secondary outcomes, HADS and DFS-SF, summary measures of the area under the curve were calculated for each participant and compared using a Mann Whitney U test. These showed no significant differences between the groups on the HADS or DFS-SF (p>0.05) (Table 3). There were also no significant differences on any of the DFS-SF subscales. A total of 26 participants failed to complete some of the questions in the NAFF. In 25 patients missing values were replaced by the mean for that individual. The other participant had omitted several questions and so these were not replaced. A Mann Whitney U test comparing the groups at 12 months showed that patients in the intervention group engaged in more of the recommended foot care behaviours, as assessed by the NAFF, than patients in the Fig. 1 Flow diagram: recruitment and follow-up of participants 259 patients identified with healed ulcers 54 refused consent 27 excluded for other criteria 178 randomised 172 included 1 recruited twice by mistake 2 ill 1 withdrew consent 1 above ankle ulcer recruited by mistake 87 education programme 85 usual care Died 2 Alive but did not return questionnaires 4 Died 3 Alive but did not return questionnaires completed questionnaire, outcomes at 6 months 70 completed questionnaire, outcomes at 6 months Died 4 Alive but did not return questionnaires 9 (2 who did not complete at 6 months did complete at 12 months) Died 1 Alive but did not return questionnaires 13 (5 who did not complete at 6 months did complete at 12 months) 72 completed questionnaire outcomes at 12 months 68 completed questionnaire outcomes at 12 months
5 1958 Diabetologia (2008) 51: Table 1 Baseline characteristics of participants Characteristics Intervention Control n=87 n=85 n % n % Sex Male Female Centre CHN QMC DRI Diabetes type Type Type Retinopathy Yes No Nephropathy Yes No Ethnic origin UK white Other Living Alone With partner Currently working Yes No Social class a Site of ulcer Forefoot Mid and hindfoot Previous amputation, other leg None Minor Major Previous amputation, same leg None Minor g monofilament All three stimuli felt Only one or two felt None felt Neurotip Felt Not felt Vibration perception 25 V felt V not felt Foot pulses Both palpable Table 1 (continued) Characteristics Intervention Control n=87 n=85 n n=87 % n n=85 % One palpable or both diminished Neither palpable Fitted footwear Yes No CHN City Hospital, Nottingham, DRI Derbyshire Royal Infirmary, QMC Queen s Medical Centre, Nottingham a The Standard Occupation Classification system grades occupations as: I, professional; II, managerial and technical; skilled non-manual and manual; IV, partly-skilled; V, unskilled control group: the median score in the intervention group was 42.0 compared with 38.7 in the controls (p=0.03). Discussion n % n % We found no indication of any effect on the primary outcome, new ulceration, even though the intervention appeared to be associated with improved foot care behaviour in the intervention group. Although the study was powered to detect a sizeable reduction in recurrence, this was less than the threefold reduction reported by Malone et al. [23], on whose data our sample size calculation was based. As it happens, the incidence of new ulceration in the two groups was identical, at 41%, without even a trend towards benefit in the intervention group. Similarly, no indication of an effect on the incidence of major or minor amputation, or on mood or on quality of life was seen. The primary outcome measure was the incidence of new ulceration at any site on either foot and was determined by examination of medical records, supplemented by information derived from questionnaires sent to the patients and to their GPs. Occasional discrepancies concerning ulcer occurrence and amputation were found between the medical records and the patient reports, but after reviewing the medical records, these were explained by errors in recall (with patients reporting ulcers and amputations which had actually occurred before the date of randomisation), by occasional confusion between ulcers of the foot and of the leg and by the known tendency of some patients not to acknowledge an ulcer which they have actually had. Our findings are in contrast to those of Malone et al. [23], who found that education led to a major reduction in ulcer incidence and amputation within 13 months. Possible reasons for the difference may be that the earlier study was
6 Diabetologia (2008) 51: Table 2 Frequency of new ulceration and of amputation Outcome Intervention Control Comparison n=87 n=85 n % n % RR a 95% CI a Relative risk or risk ratio expressed as the ratio of the estimated risk of a good outcome (no ulcer or no amputation) in the intervention group to that in the control group Outcome at 6 months Foot ulcer No foot ulcer Amputation No amputation Outcome at 12 months Foot ulcer No foot ulcer Amputation No amputation apparently not blinded and was conducted on in-patients who may have been more aware of the potential threat to their limb. We also noted that the incidence of major amputation was very much higher in the earlier study, while the incidence of new ulceration was very much lower. These differences might reflect a major difference in population selection, clinical practice or both. Nevertheless, the incidence of new ulceration observed is very similar to that reported earlier by both ourselves [22, 27] and others [21, 28]. It is also possible that the earlier study involved a patient population which had not previously had access to expert diabetes care and that the quality of education and support provided for those in the control group may have differed from the usual care available (almost 20 years later) for those attending specialist clinics in UK. Nevertheless, we noted that the NAFF scores achieved by both groups at 12 months in the present study (Table 3) were lower than those of the validation samples involved in the development of the NAFF [31], suggesting that the standard of protective foot care behaviour among our participants was not particularly good. Some caution should be attached to these observations because, although this was a randomised study and we had no reason to suspect a difference between groups, it is possible that these observations reflect chance differences between groups at baseline. It should also be noted that the previously reported internal consistency of the NAFF was only just adequate [31], but there was no alternative measure available. The educational intervention was designed to be systematic and yet both personalised and acceptable to the patient. It was delivered by the same healthcare professional and was followed after 1 month by a phone call from the same person, in which the principal issues raised at the earlier visit were reinforced. While it is possible that a more intensive programme might have led to greater benefit, it is difficult to envisage that such an intensive programme could ever be incorporated into routine management without major investment. Moreover, the intervention adopted in this study was associated with an apparent improvement in reported foot care behaviour in the intervention group. Differences observed consisted of the intervention group having higher scores in certain foot care items, such as checking shoes before putting them on, daily washing and the use of moisturising cream. No differences were reported for items concerned with choice of footwear Table 3 Comparison of groups on secondary outcomes Outcome Intervention Control Comparison a n Baseline 6 months 12 months n Baseline 6 months 12 months Median Median Median Median Median Median p value DFS-SF 67 NA NA HAD-A HAD-D NAFF 72 NA NA NA NA Higher scores indicate better quality of life (DFS-SF) and foot care behaviour (NAFF) but lower mood (HADS) a Using Mann Whitney U test. Area under the curve was compared for DFS-SF (6 and 12 months) and HADS scales (baseline, 6 and 12 months). The numbers assessed are from patients who returned questionnaire on both (DFS-SF) and all three (HADS) occasions HAD-A HAD scale, anxiety, HAD-D HAD scale, depression, NA not administered
7 1960 Diabetologia (2008) 51: or with prevention of accidental damage, although it is known that accidents and factors relating to footwear are most often implicated in the cause of new ulcers [29, 30]. This failure to change aspects of behaviour most likely to be associated with increased risk is important and suggests that even though these items were specifically targeted in the educational interview, they might need even greater emphasis in any future work. There were no significant effects of the intervention on mood or quality of life. The sample size was also relatively small for studies on quality of life and determined on the basis of the primary endpoint, so it is possible that a real effect was missed. Overall, the results of this study suggest that a targeted programme of education for people with foot ulcers that had been managed in specialist foot clinics in UK and had healed, improved some aspects of foot care behaviour but had no effect on the incidence of new ulceration at either 6 or 12 months. There is therefore no evidence to justify the adoption of such a programme of education to reduce new ulcer incidence in such a population. Paradoxically, it is possible that an education programme may fail to reduce ulcer incidence in a very high-risk population such as this simply because the influence of the factors that put them at risk may be far greater than can be offset by any change in foot care behaviour. But although we have been unable to document a benefit from the particular intervention chosen for study, we feel that every effort should continue to be made to ensure that patients with healed ulcers reduce riskassociated behaviour as much as possible. It is possible that this could be achieved by a more intensive programme of education, but until the effectiveness of such a programme has been shown, educational effort must necessarily be unstructured and targeted at the needs of each individual. It is relevant that our failure to observe a fall in ulcer incidence echoes the observations of McCabe and colleagues in a similar, but only partly randomised study of a population at high risk in UK [14]. This group, however, did observe that the incidence of amputation was lower in their intervention group and one interpretation of this finding is that the education programme may encourage a patient with a new ulcer to seek expert help earlier and that this may lead to an improved outcome. If so, this might also explain some of the benefit observed by Malone and colleagues [23], but not observed in the present study because the incidence of major amputation was very low in both our study groups. This possible indirect benefit of patient education in improving the outcome of new ulceration as much as its incidence needs further study. Acknowledgements We thank Diabetes UK for supporting this study (grant RD02/ ). We also thank V. Savage, B. Kirk, S. Stevenson, M. Smith, P. Ince and A. Musgrove for their considerable help in recruiting patients to the study, data entry and checking outcome measures. Thanks also to S. Page and colleagues at the Queen s Medical Centre, Nottingham, and P. Amin and colleagues at Derbyshire Royal Infirmary for enabling us to study their patients. We are particularly grateful to S. Lewis for statistical advice. Duality of interest The authors declare that there is no duality of interest associated with this manuscript. References 1. Boulton AJ, Vileikyte L, Ragnarson-Tennvall G, Apelqvist J (2005) The global burden of diabetic foot disease. Lancet 366: Treece KA, Macfarlane RM, Pound N, Game FL, Jeffcoate WJ (2004) Validation of a system of foot ulcer classification in diabetes mellitus. Diabet Med 21: Armstrong DG, Lavery LA, Harkless LB (1998) Validation of a diabetic wound classification system. The contribution of depth, infection, and ischemia to risk of amputation. Diabetes Care 21: Cavanagh PR, Lipsky BA, Bradbury AW, Botek G (2005) Treatment for diabetic foot ulcers. Lancet 366: American Diabetes Association (2007) Standards of medical care in diabetes Diabetes Care 30(Suppl 1):S4 S41 6. National Institute for Health and Clinical Excellence (2004) Key criteria that a structured education programme should meet to fulfil the NICE requirements. Available from CG10, accessed 14 July National Institute for Clinical Excellence (2003) Guidance on the use of patient-education models for diabetes. Technology Appraisal 60. Available from o=ta060guidance, accessed 29 November Scottish Intercollegiate Guidelines Network, Management of diabetic foot disease. Available from lines/fulltext/55/section7.html, accessed 29 November Valk GD, Kriegsman DM, Assendelft WJ (2005) Patient education for preventing diabetic foot ulceration (Cochrane Review). The Cochrane Library, Issue 2, Oxford, Update Software 10. Radford K, Chipchase S, Jeffcoate W (2005) Education in the management of the foot in diabetes. In: Boulton AJM, Cavanagh PR, Rayman G (eds) The foot in diabetes. 4th edn. Wiley, London, pp Singh N, Armstrong DG, Lipsky BA (2005) Preventing foot ulcers in patients with diabetes. JAMA 293: Litzelman DK, Slemenda CW, Langeveld CD et al (1993) Reduction of lower extremity clinical abnormalities in patients with non-insulindependent diabetes mellitus. Ann Intern Med 119: Rith-Najarian S, Branchaud C, Beaulieu O, Gohdes D, Simonson G, Mazze R (1998) Reducing lower-extremity amputations due to diabetes: application of the staged diabetes management approach in a primary care setting. J Fam Pract 47: McCabe CJ, Stevenson RC, Dolan AM (1998) Evaluation of a diabetic foot screening and protection programme. Diabet Med 15: Rettig BA, Shrauger DG, Recker RR, Gallagher TF, Wiltse H (1996) A randomized study of the effects of a home diabetes education program. Diabetes Care 9: Bloomgarden ZT, Karmally W, Metzger MJ et al (1997) Randomized, controlled trial of diabetic patient education: improved knowledge without improved metabolic status. Diabetes Care 10: Hamalainen H, Ronnemaa T, Toikka T, Liukkonen I (1998) Longterm effects of one year of intensified podiatric activities on footcare knowledge and self-care habits in patients with diabetes. Diabetes Educ 24:
8 Diabetologia (2008) 51: Ronnemaa T, Hamalainen H, Toikka T, Liukkonen I (1997) Evaluation of the impact of podiatrist care in the primary prevention of foot problems in diabetic subjects. Diabetes Care 20: Peters EJ, Lavery LA (2001) Effectiveness of the diabetic foot risk classification system of the International Working Group on the Diabetic Foot. Diabetes Care 24: Leese GP, Reid F, Green V et al (2005) Predicting foot ulceration in diabetes: validation of a clinical tool in population-based study. Int J Clin Pract 60: Apelqvist J, Larsson J, Agardh C-D (1993) Long-term prognosis for diabetic patients with foot ulcers. J Intern Med 233: Pound N, Chipchase S, Treece K, Game F, Jeffcoate W (2005) Ulcer-free survival following management of foot ulcers in diabetes. Diabet Med 22: Malone JM, Snyder M, Anderson G, Bernhard VM, Holloway GA, Bunt TJ (1989) Prevention of amputation by diabetic education. Am J Surg 158: Office for Population Censuses and Surveys (1991) Standard occupational classification system. HMSO, London 25. Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67: International Consensus on the Diabetic Foot. International Working Group on the Diabetic Foot, Available from accessed 14 July Macfarlane RM, Jeffcoate WJ (1997) Factors contributing to the presentation of diabetic foot ulcers. Diabet Med 14: Pecoraro RE, Reiber GE, Burgess EM (1980) Pathways to diabetic limb amputation. Basis for prevention. Diabetes Care 13: Abetz L, Sutton M, Brady L, McNulty P, Gagnon D (2002) The Diabetic Foot Ulcer Scale (DFS): a quality of life instrument for use in clinical trials. Pract Diabetes Int 19: Bann CM, Fehnel SE, Gagnon DD (2003) Development and validation of the Diabetic Foot Ulcer Scale-Short Form (DFS-SF). Pharmacoeconomics 21: Lincoln NB, Jeffcoate WJ, Ince P, Smith M, Radford KA (2007) Validation of a new measure of protective footcare behaviour: the Nottingham Assessment of Functional Footcare (NAFF). Pract Diabetes Int 24:
Patient education for preventing diabetic foot ulceration
 DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 101 106. Published online in Wiley Online Library (wileyonlinelibrary.com).2237 REVIEW ARTICLE Patient education for preventing
DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 101 106. Published online in Wiley Online Library (wileyonlinelibrary.com).2237 REVIEW ARTICLE Patient education for preventing
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/108980
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/108980
Patients perceptions of a shoe-fitting service at a diabetic foot clinic
 Patients perceptions of a shoe-fitting service at a diabetic foot clinic Catherine Gooday, Kevin Panter, Ketan Dhatariya Provision of adequate and acceptable footwear for people with at-risk diabetic feet
Patients perceptions of a shoe-fitting service at a diabetic foot clinic Catherine Gooday, Kevin Panter, Ketan Dhatariya Provision of adequate and acceptable footwear for people with at-risk diabetic feet
Use of the SINBAD classification system and score in comparing outcome of foot ulcer management in three continents
 Diabetes Care Publish Ahead of Print, published online February 25, 2008 Use of the SINBAD classification system and score in comparing outcome of foot ulcer management in three continents 1 Ince P, BSc,
Diabetes Care Publish Ahead of Print, published online February 25, 2008 Use of the SINBAD classification system and score in comparing outcome of foot ulcer management in three continents 1 Ince P, BSc,
Putting feet first: national minimum skills framework
 In partnership with Putting feet first: national minimum skills framework The national minimum skills framework for commissioning of footcare services for people with diabetes Revised March 2011 This report
In partnership with Putting feet first: national minimum skills framework The national minimum skills framework for commissioning of footcare services for people with diabetes Revised March 2011 This report
Risk factors for recurrent diabetic foot ulcers: Site matters. Received for publication 5 March 2007 and accepted in revised form
 Diabetes Care In Press, published online May 16, 2007 Risk factors for recurrent diabetic foot ulcers: Site matters Received for publication 5 March 2007 and accepted in revised form Edgar J.G. Peters
Diabetes Care In Press, published online May 16, 2007 Risk factors for recurrent diabetic foot ulcers: Site matters Received for publication 5 March 2007 and accepted in revised form Edgar J.G. Peters
Patient education for preventing diabetic foot ulceration (Review)
 Patient education for preventing diabetic foot ulceration (Review) Dorresteijn JAN, Kriegsman DMW, Assendelft WJJ, Valk GD This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Patient education for preventing diabetic foot ulceration (Review) Dorresteijn JAN, Kriegsman DMW, Assendelft WJJ, Valk GD This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Assessment of Ulcer Related Outcomes in Type 2 Diabetic Patients with Foot Ulceration in India
 Assessment of Ulcer Related Outcomes in Type 2 Diabetic Patients with Foot Ulceration in India Authors: Vijay Viswanathan, MD, PhD 1, Satyavanij Kumpatla, MSc, MTech, PhD 2, Saraswathy Gnanasundaram, ME,
Assessment of Ulcer Related Outcomes in Type 2 Diabetic Patients with Foot Ulceration in India Authors: Vijay Viswanathan, MD, PhD 1, Satyavanij Kumpatla, MSc, MTech, PhD 2, Saraswathy Gnanasundaram, ME,
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Keeping the diabetic foot healed How effective is the Newcastle Foot Protection Team?
 Keeping the diabetic foot healed How effective is the Newcastle Foot Protection Team? Linda Robertshaw Advanced Podiatrist Nicola Coates Principal Podiatrist (Diabetes) Background Risk factors for diabetic
Keeping the diabetic foot healed How effective is the Newcastle Foot Protection Team? Linda Robertshaw Advanced Podiatrist Nicola Coates Principal Podiatrist (Diabetes) Background Risk factors for diabetic
Health-related quality of life of diabetic foot ulcer patients and their caregivers
 Diabetologia (2005) 48: 1906 1910 DOI 10.1007/s00125-005-1856-6 ARTICLE M. H. Nabuurs-Franssen. M. S. P. Huijberts. A. C. Nieuwenhuijzen Kruseman. J. Willems. N. C. Schaper Health-related quality of life
Diabetologia (2005) 48: 1906 1910 DOI 10.1007/s00125-005-1856-6 ARTICLE M. H. Nabuurs-Franssen. M. S. P. Huijberts. A. C. Nieuwenhuijzen Kruseman. J. Willems. N. C. Schaper Health-related quality of life
Type 2 diabetes: prevention and management of foot problems
 Type 2 diabetes: prevention and management of foot problems NICE guideline Revised version Second draft for consultation, August 2003 If you wish to comment on the recommendations, please make your comments
Type 2 diabetes: prevention and management of foot problems NICE guideline Revised version Second draft for consultation, August 2003 If you wish to comment on the recommendations, please make your comments
CHAPTER.7 CARING THE DIABETIC FOOT
 CHAPTER.7 CARING THE DIABETIC FOOT Introduction Diabetes has become a global epidemic(144). The long term complications due to diabetes impose huge social and economic burden, mental and physical misery
CHAPTER.7 CARING THE DIABETIC FOOT Introduction Diabetes has become a global epidemic(144). The long term complications due to diabetes impose huge social and economic burden, mental and physical misery
How can DIABETES affect my FEET? Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
Clinical assessment of diabetic foot in 5 minutes
 Clinical assessment of diabetic foot in 5 minutes Assoc. Prof. N. Tentolouris, MD 1 st Department of Propaedeutic Internal Medicine Medical School Laiko General Hospital Leading Innovative Vascular Education
Clinical assessment of diabetic foot in 5 minutes Assoc. Prof. N. Tentolouris, MD 1 st Department of Propaedeutic Internal Medicine Medical School Laiko General Hospital Leading Innovative Vascular Education
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Practices related to foot care among type ll diabetes mellitus patients who attend diabetes clinics in General Hospital Kurunegala, Sri Lanka
 International Journal of Scientific and Research Publications, Volume 7, Issue 1, January 2017 46 Practices related to foot care among type ll diabetes mellitus patients who attend diabetes clinics in
International Journal of Scientific and Research Publications, Volume 7, Issue 1, January 2017 46 Practices related to foot care among type ll diabetes mellitus patients who attend diabetes clinics in
Foot protection for people with diabetes a focus on prevention
 Foot protection for people with diabetes a focus on prevention Presentation by Mike Townson Independent Podiatry Consultant. Facilitated by Angela Farrell Neubourg Pharma UK Ltd. Foot Assessment training
Foot protection for people with diabetes a focus on prevention Presentation by Mike Townson Independent Podiatry Consultant. Facilitated by Angela Farrell Neubourg Pharma UK Ltd. Foot Assessment training
National Diabetes Foot Care Audit (NDFA) of England and Wales: 2014-
 National Diabetes Foot Care Audit (NDFA) of England and Wales: 2014- NDFA is part of the National Diabetes Audit programme family William Jeffcoate Clinical Lead of the National Diabetes Foot Care Audit
National Diabetes Foot Care Audit (NDFA) of England and Wales: 2014- NDFA is part of the National Diabetes Audit programme family William Jeffcoate Clinical Lead of the National Diabetes Foot Care Audit
Diabetic Foot-Evidence that counts
 Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Family Physician Corner Diabetic Foot-Evidence that counts Abeer Al-Saweer, MD* Evidence-based medicine has systemized the medical thinking in each
Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Family Physician Corner Diabetic Foot-Evidence that counts Abeer Al-Saweer, MD* Evidence-based medicine has systemized the medical thinking in each
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES
 ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR
 ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
Shaping Diabetes Services in Southern Derbyshire. A vision for Diabetes Services For Southern Derbyshire CCG
 Shaping Diabetes Services in Southern Derbyshire A vision for Diabetes Services For Southern Derbyshire CCG Vanessa Vale Commissioning Manager September 2013 Contents 1. Introduction 3 2. National Guidance
Shaping Diabetes Services in Southern Derbyshire A vision for Diabetes Services For Southern Derbyshire CCG Vanessa Vale Commissioning Manager September 2013 Contents 1. Introduction 3 2. National Guidance
Helen Gelly, MD, FUHM, FCCWS
 Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Practical advice when treating feet
 Practical advice when treating feet Helen Mandic Clinical Lead Podiatrist in Health Promotion and Student Mentor Department of Podiatry and Foot Health Dawlish Hospital Falls Prevention The Role of the
Practical advice when treating feet Helen Mandic Clinical Lead Podiatrist in Health Promotion and Student Mentor Department of Podiatry and Foot Health Dawlish Hospital Falls Prevention The Role of the
Smoking cessation interventions and services
 National Institute for Health and Care Excellence Guideline version (Final) Smoking cessation interventions and services [E] Evidence reviews for advice NICE guideline NG92 Evidence reviews FINAL These
National Institute for Health and Care Excellence Guideline version (Final) Smoking cessation interventions and services [E] Evidence reviews for advice NICE guideline NG92 Evidence reviews FINAL These
Renal Foot Care. Christian Pankhurst
 Renal Foot Care Christian Pankhurst The consequences of poor management of the renal foot are considerable: prolonged ulceration and ill health, gangrene and amputation, depression and death. The health
Renal Foot Care Christian Pankhurst The consequences of poor management of the renal foot are considerable: prolonged ulceration and ill health, gangrene and amputation, depression and death. The health
Appendices R1 R2 R3 R4 R5 R6 R7 R8 R9
 0 Appendices Appendix A Characteristics of care by diabetes care group Managed Protocolized Usual Organisation care care care Senior leader Systematic quality check on different levels Incentives for improving
0 Appendices Appendix A Characteristics of care by diabetes care group Managed Protocolized Usual Organisation care care care Senior leader Systematic quality check on different levels Incentives for improving
HOW TO SPOT A FOOT ATTACK PREVENTING SERIOUS FOOT PROBLEMS
 HOW TO SPOT A FOOT ATTACK PREVENTING SERIOUS FOOT PROBLEMS Your foot check has shown that there is a high risk that you could develop serious foot problems 2 YOUR FEET MATTER If you ve been given this
HOW TO SPOT A FOOT ATTACK PREVENTING SERIOUS FOOT PROBLEMS Your foot check has shown that there is a high risk that you could develop serious foot problems 2 YOUR FEET MATTER If you ve been given this
Volume 5 Issue 8, August
 Effect of Structured Teaching Programme on Knowledge and Practice Regarding Foot Care among Chronic Diabetic Patients Sruthy Vinod Mahatma Gandhi University, Kerala, India Abstract: A study on Effect of
Effect of Structured Teaching Programme on Knowledge and Practice Regarding Foot Care among Chronic Diabetic Patients Sruthy Vinod Mahatma Gandhi University, Kerala, India Abstract: A study on Effect of
Six step guide to improving diabetes footcare. Putting feet. first
 Six step guide to improving diabetes footcare Putting feet first In England there are over 140 leg, foot or toe amputations a week. Diabetes related amputations and foot ulcers cost the NHS in England
Six step guide to improving diabetes footcare Putting feet first In England there are over 140 leg, foot or toe amputations a week. Diabetes related amputations and foot ulcers cost the NHS in England
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
of :07
 he diabetic foot ulcer - management and outcomes of 6 3-12-2012 11:07 The diabetic foot ulcer - management and outcomes Impaired perfusion Infection Extent and depth Condition of the ulcer Site Sensation
he diabetic foot ulcer - management and outcomes of 6 3-12-2012 11:07 The diabetic foot ulcer - management and outcomes Impaired perfusion Infection Extent and depth Condition of the ulcer Site Sensation
DIABETES AND THE AT-RISK LOWER LIMB:
 DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
Advice for rheumatoid patients at risk of developing foot related problems
 Advice for rheumatoid patients at risk of developing foot related problems Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Advice for rheumatoid patients at risk of developing foot related problems Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Predictive Value of Foot Pressure Assessment as Part of a Population- Based Diabetes Disease Management Program
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Predictive Value of Foot Pressure Assessment as Part of a Population- Based Diabetes Disease Management Program LAWRENCE
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Predictive Value of Foot Pressure Assessment as Part of a Population- Based Diabetes Disease Management Program LAWRENCE
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME QOF indicator area: Diabetes Briefing paper Potential output: Recommendations
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME QOF indicator area: Diabetes Briefing paper Potential output: Recommendations
LOOKING AFTER YOUR FEET
 LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers. Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT
 Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
Clinical Guideline for: Diagnosis and Management of Charcot Foot
 Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
A comparison of the monofilament with other testing modalities for foot ulcer susceptibility
 Diabetes Research and Clinical Practice 70 (2005) 8 12 www.elsevier.com/locate/diabres A comparison of the monofilament with other testing modalities for foot ulcer susceptibility B. Miranda-Palma a, J.M.
Diabetes Research and Clinical Practice 70 (2005) 8 12 www.elsevier.com/locate/diabres A comparison of the monofilament with other testing modalities for foot ulcer susceptibility B. Miranda-Palma a, J.M.
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme
 Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Peripheral Neuropathy
 Peripheral Neuropathy Neuropathy affects 30-50% of patient population with diabetes and this prevalence tends to increase proportionally with duration of diabetes and dependant on control. Often presents
Peripheral Neuropathy Neuropathy affects 30-50% of patient population with diabetes and this prevalence tends to increase proportionally with duration of diabetes and dependant on control. Often presents
INTRODUCTION Chronic foot ulcers are among the many serious complications associated with diabetes mellitus. Lifetime incidence of foot ulcers in
 ORIGINAL ARTICLE Quality of life in patients with diabetic foot ulcers: validation of the Cardiff Wound Impact Schedule in a Canadian population Peter J Jaksa, James L Mahoney Jaksa PJ, Mahoney JL. Quality
ORIGINAL ARTICLE Quality of life in patients with diabetic foot ulcers: validation of the Cardiff Wound Impact Schedule in a Canadian population Peter J Jaksa, James L Mahoney Jaksa PJ, Mahoney JL. Quality
Chiropodist-podiatrist consultations for preventing foot lesions in diabetics
 Chiropodist-podiatrist consultations for preventing foot lesions in diabetics Summary document July 2007 Department for the Assessment of Medical and Surgical Procedures 2 avenue du Stade de France 93218
Chiropodist-podiatrist consultations for preventing foot lesions in diabetics Summary document July 2007 Department for the Assessment of Medical and Surgical Procedures 2 avenue du Stade de France 93218
Epidemiology and Health Care Costs for Diabetic Foot Problems
 2 Epidemiology and Health Care Costs for Diabetic Foot Problems Gayle E. Reiber, MPH, PhD and Lynne V. McFarland, MS, PhD INTRODUCTION The global prevalence of diabetes is predicted to double by the year
2 Epidemiology and Health Care Costs for Diabetic Foot Problems Gayle E. Reiber, MPH, PhD and Lynne V. McFarland, MS, PhD INTRODUCTION The global prevalence of diabetes is predicted to double by the year
A Comparison of Two Diabetic Foot Ulcer Classification Systems. The Wagner and the University of Texas wound classification systems
 Pathophysiology/Complications O R I G I N A L A R T I C L E A Comparison of Two Diabetic Foot Ulcer Classification Systems The Wagner and the University of Texas wound classification systems SAMSON O.
Pathophysiology/Complications O R I G I N A L A R T I C L E A Comparison of Two Diabetic Foot Ulcer Classification Systems The Wagner and the University of Texas wound classification systems SAMSON O.
Is Neuropathy the root of all evil in the diabetic foot?
 Is Neuropathy the root of all evil in the diabetic foot? Andrew J M Boulton, Manchester UK and Miami, FL Vice-President and Director of International Postgraduate Education, EASD The Global Burden of Diabetes
Is Neuropathy the root of all evil in the diabetic foot? Andrew J M Boulton, Manchester UK and Miami, FL Vice-President and Director of International Postgraduate Education, EASD The Global Burden of Diabetes
Preventing Foot Ulcers in the Neuropathic Diabetic Foot. Glossary of Terms
 Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT DISEASE - 1 -
 ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT DISEASE - 1 - THE ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT
ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT DISEASE - 1 - THE ORTHOTICS COMPETENCY FRAMEWORK FOR THE PREVENTION, TREATMENT AND MANAGEMENT OF DIABETIC FOOT
Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems
 Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Diabetes Foot Health and Prevention Program:
 Diabetes Foot Health and Prevention Program: A Podiatrist / RN Collaborative Practice Dr. Pamela Monk Visiting Podiatrist drpamelamonk@live.ca(204) 391-9719 Danna Ferry RN Ferry RN Services dlferry@live.ca
Diabetes Foot Health and Prevention Program: A Podiatrist / RN Collaborative Practice Dr. Pamela Monk Visiting Podiatrist drpamelamonk@live.ca(204) 391-9719 Danna Ferry RN Ferry RN Services dlferry@live.ca
Root Cause Analysis The Tools. Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon
 Root Cause Analysis The Tools Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon Why do RCA s? To understand if the amputation was avoidable or unavoidable Learn and improve Identify
Root Cause Analysis The Tools Angie Abbott Head of Podiatry and Orthotics Torbay and Southern Devon Why do RCA s? To understand if the amputation was avoidable or unavoidable Learn and improve Identify
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Li, R., Cooper, C., Barber, J., Rapaport, P., Griffin, M., & Livingston, G. (2014). Coping strategies as mediators of the effect of the START (strategies for RelaTives)
CRITICALLY APPRAISED PAPER (CAP) Li, R., Cooper, C., Barber, J., Rapaport, P., Griffin, M., & Livingston, G. (2014). Coping strategies as mediators of the effect of the START (strategies for RelaTives)
THE DIABETIC FOOT. Nicola Kilburn Diabetes Specialist Podiatrist
 THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
The diabetic foot a focus on ischemia and infection
 The diabetic foot a focus on ischemia and infection Stephan Morbach, MD Department of Diabetes and Angiology Marienkrankenhaus ggmbh Soest, Germany s.morbach@mkh-soest.de Epidemiology of Diabetic Foot
The diabetic foot a focus on ischemia and infection Stephan Morbach, MD Department of Diabetes and Angiology Marienkrankenhaus ggmbh Soest, Germany s.morbach@mkh-soest.de Epidemiology of Diabetic Foot
A New Wound-Based Severity Score for Diabetic Foot Ulcers
 Clinical Care/Education/Nutrition O R I G I N A L A R T I C L E A New Wound-Based Severity Score for Diabetic Foot Ulcers A prospective analysis of 1,000 patients STEFAN BECKERT, MD MARIA WITTE, MD CORINNA
Clinical Care/Education/Nutrition O R I G I N A L A R T I C L E A New Wound-Based Severity Score for Diabetic Foot Ulcers A prospective analysis of 1,000 patients STEFAN BECKERT, MD MARIA WITTE, MD CORINNA
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
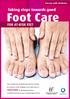 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus
 Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
ARTERIAL BYPASS GRAFTS IN THE LEG
 The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
Looking after your diabetic foot ulcer
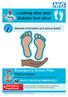 Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY.
Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY.
DIABETIC FOOT BOOK THE. A guide to keeping it simple and preventing complications. Practice genii. the Diabetic Foot Book
 DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
Outcomes of diabetes care in England and Wales. A summary of findings from the National Diabetes Audit : Complications and Mortality reports
 Outcomes of diabetes care in England and Wales A summary of findings from the National Diabetes Audit 2015 16: Complications and Mortality reports About this report This report is for people with diabetes
Outcomes of diabetes care in England and Wales A summary of findings from the National Diabetes Audit 2015 16: Complications and Mortality reports About this report This report is for people with diabetes
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
a health care guide Care of your high-risk feet
 a health care guide Care of your high-risk feet Why is it important? Certain medical conditions for example, diabetes, rheumatoid arthritis and circulation disorders can place your feet at high risk of
a health care guide Care of your high-risk feet Why is it important? Certain medical conditions for example, diabetes, rheumatoid arthritis and circulation disorders can place your feet at high risk of
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
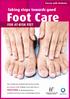 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Looking after your diabetic foot ulcer
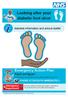 Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have breaks in the skin PHONE 07786250788 IMMEDIATELY.
Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have breaks in the skin PHONE 07786250788 IMMEDIATELY.
Diabetes Public Meeting: Improving Diabetes Care in Hounslow
 Diabetes Public Meeting: Improving Diabetes Care in Hounslow Report from the Public Meeting held on: Wednesday 18th March 2015 at Days Inn Hotel, 8 10, Lampton Rd, Hounslow Hounslow CCG Diabetes Public
Diabetes Public Meeting: Improving Diabetes Care in Hounslow Report from the Public Meeting held on: Wednesday 18th March 2015 at Days Inn Hotel, 8 10, Lampton Rd, Hounslow Hounslow CCG Diabetes Public
Implementing the updated NICE Guidance on the Diabetic Foot
 Implementing the updated NICE Guidance on the Diabetic Foot Rachel Berrington Senior Diabetes Specialist Nurse Foot Lead University Hospitals of Leicester NHS Trust Key Priorities for Implementation NG19
Implementing the updated NICE Guidance on the Diabetic Foot Rachel Berrington Senior Diabetes Specialist Nurse Foot Lead University Hospitals of Leicester NHS Trust Key Priorities for Implementation NG19
Foot problems are a major source of
 Article Diabetic foot education and Inlow s 60-second foot screen Citation: McDonald A, Shah A, Wallace W (2013) Diabetic foot education and Inlow s 60-second foot screen. Diabetic Foot Canada 1: 18 22
Article Diabetic foot education and Inlow s 60-second foot screen Citation: McDonald A, Shah A, Wallace W (2013) Diabetic foot education and Inlow s 60-second foot screen. Diabetic Foot Canada 1: 18 22
DIAGNOSIS OF DIABETIC NEUROPATHY
 DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
Comparison of three systems of classification in predicting the outcome of diabetic foot ulcers in a Brazilian population
 European Journal of Endocrinology (2008) 159 417 422 ISSN 0804-4643 CLINICAL STUDY Comparison of three systems of classification in predicting the outcome of diabetic foot ulcers in a Brazilian population
European Journal of Endocrinology (2008) 159 417 422 ISSN 0804-4643 CLINICAL STUDY Comparison of three systems of classification in predicting the outcome of diabetic foot ulcers in a Brazilian population
Appendix A: Guideline development group membership and declarations of interest
 Appendix A: Guideline development group membership and declarations of A.1 Guideline development group Damien Longson (Guideline Chair) Consultant Liaison Psychiatrist, Manchester Mental Health and Social
Appendix A: Guideline development group membership and declarations of A.1 Guideline development group Damien Longson (Guideline Chair) Consultant Liaison Psychiatrist, Manchester Mental Health and Social
You have high risk feet
 You have high risk feet diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY. Emergency Department
You have high risk feet diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY. Emergency Department
National Diabetes Foot Care Audit Third Annual Report
 National Diabetes Foot Care Audit Third Annual Report England and Wales 14 July 2014 to 31 March 2017 V1.0 14 March 2018 Introduction: Contents Key Introduction Key messages Care structures survey Participation
National Diabetes Foot Care Audit Third Annual Report England and Wales 14 July 2014 to 31 March 2017 V1.0 14 March 2018 Introduction: Contents Key Introduction Key messages Care structures survey Participation
University of Huddersfield Repository
 University of Huddersfield Repository Newton, Veronica and Roberts, Peter Foot Inspection or Foot Assessment? Original Citation Newton, Veronica and Roberts, Peter (2011) Foot Inspection or Foot Assessment?
University of Huddersfield Repository Newton, Veronica and Roberts, Peter Foot Inspection or Foot Assessment? Original Citation Newton, Veronica and Roberts, Peter (2011) Foot Inspection or Foot Assessment?
Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes
 Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes Irving Building Occupational Therapy, Rehabilitation Services 0161 206 519 G1809190W. Design Services, Salford Royal NHS Foundation
Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes Irving Building Occupational Therapy, Rehabilitation Services 0161 206 519 G1809190W. Design Services, Salford Royal NHS Foundation
Diabetes Foot and Skin Care. Diabetes and the feet. Foot problems: Major cause of morbidity and mortality
 Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
PSYCHOLOGICAL CHALLENGES OF DIABETICS
 PSYCHOLOGICAL CHALLENGES OF DIABETICS Does Depression Correlate to Diabetic Foot Ulcer Outcomes? Garneisha Torrence, PGY-3 DVA Puget Sound Health Care System Disclosure No relevant financial or non-financial
PSYCHOLOGICAL CHALLENGES OF DIABETICS Does Depression Correlate to Diabetic Foot Ulcer Outcomes? Garneisha Torrence, PGY-3 DVA Puget Sound Health Care System Disclosure No relevant financial or non-financial
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Lesser toe surgery. Exceptional healthcare, personally delivered
 Lesser toe surgery Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed as needing lesser toe surgery. This leaflet
Lesser toe surgery Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed as needing lesser toe surgery. This leaflet
Model of care for the diabetic foot
 Model of care for the diabetic foot Item type Authors Citation Publisher Report National Diabetes Programme Working Group National Diabetes Programme Working Group. Model of care for the diabetic foot.
Model of care for the diabetic foot Item type Authors Citation Publisher Report National Diabetes Programme Working Group National Diabetes Programme Working Group. Model of care for the diabetic foot.
HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
 Review Article Allied Science International Journal of Pharma and Bio Sciences ISSN 0975-6299 HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
Review Article Allied Science International Journal of Pharma and Bio Sciences ISSN 0975-6299 HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
Clinical Guidelines for Type 2 Diabetes
 FINAL VERSION Clinical Guidelines for Type 2 Diabetes Prevention and management of foot problems Revised version The prevention and management of foot problems 1 This work is undertaken by ScHARR, University
FINAL VERSION Clinical Guidelines for Type 2 Diabetes Prevention and management of foot problems Revised version The prevention and management of foot problems 1 This work is undertaken by ScHARR, University
Gypsy and Traveller thoughts around wellbeing
 Report BCCG Funded engagement December 2013 - March 2014 Gypsy and Traveller thoughts around wellbeing A summary of the report compiled for Brighton and Hove CCG by Michelle Gavin, Friends Families and
Report BCCG Funded engagement December 2013 - March 2014 Gypsy and Traveller thoughts around wellbeing A summary of the report compiled for Brighton and Hove CCG by Michelle Gavin, Friends Families and
Custom-made total contact insoles and prefabricated functional diabetic insoles: A case report
 Custom-made total contact insoles and prefabricated functional diabetic insoles: A case report Joanne Paton, Elizabeth Stenhouse, Ray Jones, Graham Bruce Insoles are commonly prescribed to offload the
Custom-made total contact insoles and prefabricated functional diabetic insoles: A case report Joanne Paton, Elizabeth Stenhouse, Ray Jones, Graham Bruce Insoles are commonly prescribed to offload the
Consensus Statement Foot care education in patients with diabetes at low risk of complications: a consensus statement
 DIABETICMedicine Consensus Statement Foot care education in patients with diabetes at low risk of complications: a consensus statement A. McInnes, W. Jeffcoate*, L. Vileikyte, F. Game*, K. Lucas, N. Higson,
DIABETICMedicine Consensus Statement Foot care education in patients with diabetes at low risk of complications: a consensus statement A. McInnes, W. Jeffcoate*, L. Vileikyte, F. Game*, K. Lucas, N. Higson,
BUNION (AND OTHER PAINFUL TOE CONDITION) SURGICAL TREATMENT POLICY PRIOR APPROVAL
 BUNION (AND OTHER PAINFUL TOE CONDITION) SURGICAL TREATMENT POLICY PRIOR APPROVAL Version: 1718.v3 Recommendation by: Somerset CCG Clinical Commissioning Policy Forum (CCPF) Date Ratified: 12 July 2017
BUNION (AND OTHER PAINFUL TOE CONDITION) SURGICAL TREATMENT POLICY PRIOR APPROVAL Version: 1718.v3 Recommendation by: Somerset CCG Clinical Commissioning Policy Forum (CCPF) Date Ratified: 12 July 2017
FOCUS: Fluoxetine Or Control Under Supervision Results. Martin Dennis on behalf of the FOCUS collaborators
 FOCUS: Fluoxetine Or Control Under Supervision Results Martin Dennis on behalf of the FOCUS collaborators Background Pre clinical and imaging studies had suggested benefits from fluoxetine (and other SSRIs)
FOCUS: Fluoxetine Or Control Under Supervision Results Martin Dennis on behalf of the FOCUS collaborators Background Pre clinical and imaging studies had suggested benefits from fluoxetine (and other SSRIs)
Case Study 2 - Mr J. Medical history
 Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Clinical Guidelines for Type 2 Diabetes
 Clinical Guidelines for Type 2 Diabetes Prevention management of foot problems Revised version The prevention management of foot problems 103 13. Appendices (This file contains Appendices 1 10. Appendices
Clinical Guidelines for Type 2 Diabetes Prevention management of foot problems Revised version The prevention management of foot problems 103 13. Appendices (This file contains Appendices 1 10. Appendices
Diabetes is a serious disease that can develop from lack of insulin production in the body or due to
 Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
