Diabetic Foot Ulcers (DFUs) Mehr Ali Rahimi Endocrinologist Associate Proffessor of Kermansha University of Medical Scinces
|
|
|
- Justin Johnston
- 5 years ago
- Views:
Transcription
1 بسم الله الرحمن الرحیم Diabetic Foot Ulcers (DFUs) Mehr Ali Rahimi Endocrinologist Associate Proffessor of Kermansha University of Medical Scinces ١
2 Case ۵۶ year old woman with DM٢ admitted with a diabetesrelated foot infection which may require surgical debridement in the near future, eating regular meals. - Weight: ٨٠ kg - Home medical regimen: Glibenchamide ١٠ mg po bid, Metformin ١٠٠٠ mg po bid, Control: - A recent HbA١c is ١٠%, POC glucose in ED ٢۴٠ mg/dl What are your initial orders?
3 Stop orals Initial Orders Basal Insulin: ٢٠-٣٠ units Nutritional Insulin: ٢١-٣٠ units (٧-١٠ units each meal) Moderate dose correction scale Monitor for ٢۴ hours and begin adjusting
4 INTRODUCTION The lifetime risk of a foot ulcer for patients with diabetes (type ١ or ٢) may be as high as ٢۵ percent ١۵% of diabetic patients will develop a diabetic foot ulcer. ٢٠% of diabetic admissions to hospital due to foot problems. Foot ulcerations are the commonest cause of hospital admission in diabetics
5 Epidemiology- amputations Diabetic foot ulcers precede >٨٠% of amputations in Diabetic patients amputation rate ١۵ fold higher than non diabetics Greater than ۵٠% of all non-traumatic amputations are diabetics
6 Epidemiology Individuals who develop a DFU are at greater risk of; premature death, MI stroke than those without a history of DFU.
7 Epidemiology- Mortality DFU patients have ٢.۴ times the mortality rate of non-ulcerated diabetic patients.
8 Epidemiology Cellulitis occurs ٩ times more frequently in diabetics than non-diabetics Osteomyelitis of the foot ١٢ times more frequently in diabetics than non-diabetics
9 Key epidemiologic points about diabetic foot ulcer can be summarized by the Rule of ١۵ : Rule of ١۵ ١۵% of diabetes patients Foot ulcer in lifetime ١۵% of foot ulcers Osteomyelitis ١۵% of foot ulcers Amputation ٢٠٠۶. American Colleg of Physicians. All Rights Reserved. ٩
10
11 Pathophysiology Factors leading to development of diabetic foot: Diabetic macroangiopathy PVD Diabetic microangiopathy thickening of basement membranes Diabetic polyneuropathy Diabetic osteoathropathy abnormal foot biomechanics Reduced resistance to infection Delayed wound healing Reduced rate of collateral vessel formation
12 Pathophysiology of DFUs In most patients, peripheral neuropathy and peripheral arterial disease (PAD) (or both) play a central role and DFUs are therefore commonly classified as : Neuropathic Ischaemic Neuroischaemic (Figures).
13 Neuropathic DFU Ischaemic DFU Neuroischaemic DFU
14
15 Important factors for development of diabetic foot infections include Hyperglycemia PVD Neuropathy ١۵
16 Neuropathy Neuropathy is present in over ٨٠ percent of patients with foot ulcers Sensory neuropathy Motor Neuropathy (can lead to foot deformities) Autonomic Neuropathy - Anhidrosis Dry, cracked skin, (thereby allowing infection to penetrate below the skin.) -Arterial to venous shunting -Temperature regulation disorders
17 Anhidrosis Autonomic Neuropathy Dry, cracked skin, (thereby allowing infection to penetrate below the skin.) Arterial to venous shunting Temperature regulation disorders Lack of autonomic tone in the capillary circulation causes shunting of blood from arteries directly into veins, bypassing the tissues that need nutrition. This results in a foot that feels warm and has distended veins and bounding pulses vasodilation and absent sweating thus foot is warm, dry, scaly which predisposes to fissure formation
18 Peripheral arterial disease Can Lead to impaired blood supply needed for healing of ulcers and infections. People with diabetes are twice as likely to have PAD as those without diabetes.it is also a key risk factor for lower extremity amputation ONLINE ١۶.٣ ١٨
19 Poor Immune Function Poor PMN functions Migration, phagocytosis, intracellular killing, chemotaxis Ketosis impairs leukocyte function Monocyte mediated immune function diminished Hyperglycemia impairs complement fixation Hyperglycemia impairs neutrophil function and reduces host defenses
20 Clinical manifestations The cardinal manifestations of inflammation (erythema, warmth, swelling, and tenderness) and/or the presence of pus in an ulcer or sinus tract
21 DIAGNOSIS The diagnosis of a diabetic foot infection is primarily based on suggestive clinical manifestations. The presence of two or more features of inflammation (erythema, warmth, tenderness, swelling, induration and purulent secretions) can establish the diagnosis.
22 Evaluation of a Diabetic foot
23 Evaluation The evaluation of a patient with a diabetic foot infection involves three key steps: ١) determining the extent and severity of infection, ٢) identifying underlying factors that predispose to and promote infection ٣) assessing the microbial etiology.
24 Evaluation Of The Diabetic Foot Risk factors Risk classification Wound classification Laboratory evaluation Imaging
25 Risk factors Male sex DM > ١٠ years duration Peripheral neuropathy Abnormal foot structure PVD Smoking previous ulceration / amputation Poor glycemic control (HbA١c > ٧%) presence of micro- or macrovascular disease presence of claudication
26 Early recognition and management of risk factors is important for reducing morbidity of foot ulceration Risk of PVD and Peripheral neuropathy to increase with the duration of type ٢ diabetes
27 Predictors of amputation were foot ulceration R.F+ Visual impairment Diabetic nephropathy (especially patients on dialysis) ankle brachial index <٠.٩ ADA٢٠١۴
28 Risk classification International Working Group on the Diabetic Foot can be used to design preventive and monitoring strategies Group ٠ no evidence of neuropathy Group ١ neuropathy present but no evidence of foot deformity or PVD Group ٢ neuropathy with evidence of deformity or PVD Group ٣ history of foot ulceration or lower extremity amputation ulcers occurred in ۵, ١۴, ١٣, and ۶۵ percent of patients in groups ٠, ١, ٢, and ٣, respectively. Only patients in groups ٢ and ٣ had amputations (٢ and ٢۶ percent, respectively)
29 Risk categories High risk previous ulcer/amputation At risk - neuropathy and or vascular impairment with foot deformity Low risk no neuropathy, no vascular problems or foot deformities
30 Classification of Foot Ulcers Many different classification systems have been reported in the literature. The one developed by Wagner for grading diabetic foot ulcers has been widely used and accepted. More recently, the University of Texas (UT) group has developed an alternative classification system that, in addition to ulcer depth (as in the Wagner system), takes into account the presence or absence of infection and ischemia A prospective study from ٢٠٠١ assessed and compared these two wound classification systems and concluded that the UT scheme is a better predictor of outcome than the older Wagner system. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
31 Classification (Wagner ) Grade ٠ No ulcer in a high risk foot. Grade ١ Superficial ulcer involving the full skin thickness but not underlying tissues. ONLINE ١۶.٣ ٣١
32 CLASSIFICATION (Wagner ) Grade ٢ Deep ulcer, penetrating down to ligaments and muscle, but no bone involvement or abscess formation. ONLINE ١۶.٣ ٣٢
33 CLASSIFICATION (Wagner ) Grade ٣ Deep ulcer with cellulitis or abscess formation, often with osteomyelitis. Grade ۴ Localized gangrene. Grade ۵ Extensive gangrene involving the whole foot. ONLINE ١۶.٣ ٣٣
34 This classification was based upon clinical evaluation (depth of ulcer and presence of necrosis) alone and did not account for variability in the vascular status of the foot
35 University of Texas system An update to th e Wagner system.while similar to Wagner in its first three categories, this later system eliminated grades ۴ and ۵ and added stages A to D for each of the grades
36 Grade UT system Grade ٠: Pre- or postulcerative (Stages A to D) Grade ١: superficial ulcer not involving tendon, capsule, or bone (Stages A to D) Grade ٢: Tendon or capsular involvement without bone palpable (Stages A to D) Grade ٣: Probes to bone (Stages A to D) Stage: A : Noninfected B : Infected C : Ischemic D : Infected and ischemic
37
38 Laboratory evaluation ١. CBC ٢. BS & HbA١C ٣. Electrolytes ۴. renal function &Urinalysis ۵. ESR ۶. CRP can be useful for monitoring response to therapy ٧. procalcitonin (PCT), a novel inflammatory marker, may also be useful if laboratory facilities that test this
39 Laboratory evaluation Organisms cultured from superficial swabs are not reliable for predicting the pathogens responsible for deeper infection. Deep tissue cultures are required; for evaluation of osteomyelitis, bone biopsy is needed. Aerobic and anaerobic cultures of deep tissue or bone biopsies should be obtained at the time of debridement if deep tissue infection or osteomyelitis is suspected ONLINE ١۶.٣ ٣٩
40 Laboratory Evaluation Risk For Osteomyelitis Evaluation for osteomyelitis is an important consideration in the management of diabetic foot infections. ۴٠
41 Factors increase the likelihood of osteomyelitis Grossly visible bone or ability to probe to bone Ulcer size larger than ٢ X ٢ cm Ulcer depth >٣ mm Ulcer duration longer than ١ to ٢ weeks ESR >٧٠ mm/h ۴١
42 Imaging ١. Initial evaluation should include conventional radiographs to evaluate for bony deformity, foreign bodies, and gas in the soft tissu eand may be able to detect osteomyelitis ٢. In select cases, (MRI) can be performed to better evaluate for soft tissue abnormalities and osteomyelitis ٣. Other imaging techniques that have been used include radionuclide bone imaging, and imaging with indium-labeled leukocyte
43 Imaging If bone is grossly visible, supportive radiographic findings may not be necessary to make A diagnosis of osteomyelitis.
44 Evaluation for osteomyelitis Patients with diabetic foot infections should have initial evaluation with conventional radiographs. Those with one or more of the above factors whose radiographs are indeterminate for osteomyelitis should undergo magnetic resonance imaging (MRI). ONLINE ١۶.٣ ۴۴
45 Osteomyelitis Evidence of osteomyelitis by these imaging modalities should prompt a bone biopsy to confirm the diagnosis and to guide antimicrobial therapy. In the absence of osteomyelitis by these alternative imaging modalities, osteomyelitis is unlikely. ۴۵
46 Laboratory evaluation MICROBIOLOGY Most diabetic foot infections are polymicrobial, with up to five to seven different specific organisms often involved. The microbiology of diabetic foot wounds is variable depending on the extent of involvement
47 Management of Diabetic Foot
48 MANAGEMENT Management of diabetic foot infections requires Glycemic Control Pressure Relieving Strategies Good nutrition Antimicrobial therapy Effective local wound care Fluid and electrolyte balance. Restoring pulsatile blood flow ۴٨
49 Management of DFU Basically, a diabetic foot ulcer will heal if the following three conditions are satisfied: Pressure is removed from the wound and the immediate surrounding area Arterial inflow is adequate. Infection is treated appropriately. Although this approach might seem simplistic, failure of diabetic foot ulcers to heal is usually a result of failure to pay sufficient attention to one or more contributing conditions, including pressure on the wound, infection, ischemia, and inadequate débridement. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
50 Pressure is removed from the wound and the immediate surrounding area Off loading The most common cause of nonhealing of neuropathic foot ulcers is the failure to remove pressure from the wound and immediate surrounding area. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
51 ١-The most common cause of nonhealing of neuropathic foot ulcers is the failure to remove pressure from the wound and immediate surrounding area strongly suggest that Pressure is removed from the wound and the immediate surrounding are ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
52 ٢-The next most common error is inappropriate management of infection. Topical applications are usually unhelpful, and if clinical infection is present, it must be treated appropriately. ٣-Another common error is the failure to appreciate ischemic symptoms that are atypical due to altered pain sensation as a result of neuropathy. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
53 The most difficult ulcer to heal is the neuroischemic ulcer, and symptoms and even signs of ischemia may be altered in the diabetic state. Therefore, appropriate noninvasive investigation and arteriography are indicated for patients with a nonhealing diabetic foot ulcer if there is any question about the vascular status. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
54 Inappropriate wound débridement is another reason for slow healing or nonhealing of a diabetic foot ulcer. Appropriate débridement and removal of all dead and macerated tissue is essential in the local treatment of a diabetic foot ulcer and has been shown to result in more rapid healing of ulcers compared with wounds that are inadequately débrided. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
55 ULCER CLASSIFICATION The first step in managing diabetic foot ulcers is assessing, grading,and classifying the ulcer. Classification is based upon clinical evaluation of the extent and depth of the ulcer and the presence of infection or ischemia, which determine the nature and intensity of treatment. To assess for ischemia, all patients with diabetic foot ulcers should have ankle-brachial index and toe pressure measurements. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
56 Neuropathic Foot Ulcer Without Osteomyelitis (Wagner Grades ١, ٢; UT Grades ١a, ١b, ٢a, ٢b) that typically occur under weight-bearing areas off-loading a foot wound In the treatment of neuropathic ulcers with a good peripheral circulation, antibiotics are not indicated unless there are clear clinical signs of infection, including prominent discharge, local erythema, and cellulitis.
57 Theoretically, complete healing of all superficial and neuropathic ulcers should be possible without the need for amputation. In the treatment of neuropathic ulcers with a good peripheral circulation, antibiotics are not indicated unless there are clear clinical signs of infection, including prominent discharge, local erythema, and cellulitis. The presence of any of these features in Wagner grade ١ or ٢ ulcers would warrant reclassification in the UT system from ١a or ٢a to ١b or ٢b. In such cases, deep wound swabs should be taken and broad-spectrum oral antibiotic treatment should be started ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
58 Neuroischemic Ulcers (Wagner Grades ١, ٢; University of Texas Grades ١c, ١d) similar to those for neuropathic ulcers, with the following important exceptions. Antibiotic therapy is usually recommended for most neuroischemic ulcers. Investigation of the circulation is indicated, including noninvasive assessment and, if required, arteriography with appropriate subsequent surgical management or angioplasty
59 Osteomyelitis (Wagner Grade ٣; UT Grades ٣b, ٣d) Wagner or UT grade ٣ ulcers are deeper and involve underlying bone, often with abscess formation. Osteomyelitis isa serious complication of foot ulceration and may be present in as many as ۵٠% of diabetic patients with moderate to severe foot infections. If the physician can probe down to bone in a deep ulcer, the presence of osteomyelitis is strongly suggested. Plain radiographs are indicated for any nonhealing foot ulcer and are useful in the diagnosis of osteomyelitis in more than two thirds of patients, although the radiologic changes may be delayed. In difficult cases, further investigation, such as MRI, bone scans, or an indium-١١١ (١١١In)-labeled white blood cell scan can be useful in diagnosing bone infection. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
60 Although the treatment of osteomyelitis is traditionally surgical and involves resection of the infected bone, there have been reports of successful long-term treatment with antibiotics effective against the underlying bacterium, most commonly Staphylococcus aureus. Therefore, agents such as clindamycin (which penetrates bone well) or flucloxacillin are often used. Most recently, a randomized controlled trial has confirmed that antibiotic therapy for ٩٠ days was equally efficacious when compard to local surgery for diabetic foot osteomyelitis. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
61 Gangrene (Wagner Grades ۴, ۵) The presence of gangrene or areas of tissue death is always a serious sign in the diabetic foot. However, localized areas of gangrene, especially in the toes, that are without cellulitis, spreading infection, or discharge can occasionally be left to spontaneously autoamputate. The presence of more extensive gangrene requires urgent hospital admission; treatment of infection, often with multiple antibiotics; control of the diabetes, usually with intravenous insulin; and detailed vascular assessment. It is in this area that the team approach is most important, with close collaboration among the diabetes specialist, the vascular surgeon, and the radiologist. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
62 CLASSIFICATION OF INFECTION Mild infection Moderate infection Severe infection ۶٢
63 Mild infection Presence of ٢ manifestations of ١. Inflammation (purulence, or erythema, pain, tenderness, warmth, or induration), ٢. Any Cellulitis/erythema extends ٢ cm around the ulcer, ٣. Infection is limited to the skin or superficial subcutaneous tissues ۴. No other local complications or systemic illness. ONLINE ۶٣
64 Mild infection ١.Treated with outpatient oral antimicrobial therapy. ٢.Treated with outpatient OHA ٣.Or insulin therapy(type ١ or type٢treated by insul) ۶۴
65 Moderate infection Infection in a patient who is ١. Systemically well and metabolically stable ٢. Which has ١ of the following characteristics: cellulitis extending >٢ cm, deep-tissue abscess, gangrene, and involvement of muscle, tendon, joint or bone.
66 Severe infection Infection in a patient with Limb threatening diabetic foot infections. Systemic toxicity or metabolic instability (eg, fever, chills, tachycardia, hypotension, confusion, vomiting, leukocytosis, acidosis, severe hyperglycemia, or azotemia).
67 Duration of therapy Mild infection : ١-٢ weeks Moderate infection : ٢ to ۴ weeks, unless osteomyelitis Severe infection : soft tissue up to ۴ weeks unless osteomyelitis Osteomyelitis: depends on degree of resection ۶٧
68 severe infections warrant hospitalization for urgent surgical consultation, antimicrobial administration, and medical stabilization, most mild infections and many moderate infections can be managed in the outpatient setting with close follow-up
69 Hospitalization may be needed for mild or moderate infections if the patient; cannot manage glycemic control at home, is unable to obtain or comply with proper wound careor offloading, needs parenteral antibiotics and or needs more urgent diagnostic studies or surgical consultation
70 Glycemic control
71 Glycemic control Optimized glucose control Decreases by ۵٠% chance of foot problems
72 Management aims ١- No excess mortality. ٢- No complication ٣- Normal wound healing. ۴- No increase duration of hospitalization. ۵- No D.K.A or sever hyperglycemia. ۶- No hypoglycemia ٧٢
73 Glucose targets Glucose targets greater than >١٨٠ mg/dl or <١١٠ mg/dl are not recommended in DFU
74 Which limit is Ideal? BS between ١٠٠ ١٨٠ mg/dl. HbA١c<٧.۵ ٧۴
75 Which limit is critical? BS more than ٢٠٠ mg/dl ٧۵
76 Glycemic Goals BAD GOOD BAD Hypoglycemia Somewhere in the Middle Hyperglycemia <۴٠ ٧٠ ١١٠ ١۴٠ ١٧٠ >٢٠٠
77 Side Effects of BG >٢٠٠ mg/dl Reduced Intravascular Volume Dehydration Electrolyte Fluxes Impaired WBC Function Immunoglobulin Inactivation Complement Disabling Increased Collagenase, Decreased Wound Collagen
78 Adverse Effects of Hyperglycemia Hyperglycemia Increases risks of postoperative infections and delirium Prolonged hospital stay, resource utilization Increased renal dysfunction and renal allograft rejection in transplant
79 Glycemic control hospitalized patients outpatient Only Insulin (IV or SC) Insu. or OHA (SC)
80 indications for insulin therapy in relation to Wagners Classification of diabetic foot Grade ٠ No ulceration in a high-risk foot ١ Superfi cial ulceration ٢ Deep ulceration that penetrates to thetendon, bone or joint ٣ Osteomyelitis or a deep abscess ۴ Localized gangrene ۵ Extensive gangrene requiring a major amputation Note: Optional where OHAs alone are ineffective Insulin Therapy Optional Optional Mandatory Mandatory Mandatory Mandatory
81 Diet O.H.A Insulin mild O.H.A Insulin infection sever Insulin Insulin Insulin infection ٨١
82 Insulin, (IV or SC), is the preferred regimen for effectively treating hyperglycemia in the hospital The use of oral antidiabetic agents should be avoided in the hospital setting because no data are available on their safety and efficacy in the inpatient setting. ٨٢
83 Sulfonylureas may increase the risk of hypoglycemia in hospitalized patients with poor appetite or ordered dietary restrictions. they may worsen cardiac and cerebral ischemia( by inhibiting ATP-sensitive potassium channels, resulting in cell membrane depolarization and increased intracellular calcium concentration) ٨٣
84 As majority of foot ulcerations are associated with infections and eventually require some or other surgery, insulin therapy becomes a main- stay to achieve a good glycaemic control
85 Beneficial Mechanistic Effects of Insulin Therapy The positive effects of insulin administration are attributed to its anti-inflammatory, vasodilatory(stimulate nitric oxide release and induce the expression of endothelial nitric oxide synthase ), antioxidant effects as well as its ability to inhibit lipolysis and platelet aggregation ٨۵
86 Several studies have reported that elevated levels of cytokines and inflammatory markers associated with severe hyperglycemia return to normal shortly after the treatment with insulin and resolution of hyperglycemia
87 Insulin therapy in diabetic foot subcutaneous insulin therapy: Multiple injections of short acting insulin along with intermediate or long acting insulin, are indicated in patients with foot lesions who are being managed as outpatients Intravenous insulin therapy: Patients with advanced diabetic foot lesions who require hospitalization, have invariably a poor glycaemic control as evident by a raised plasma glucose and HbA١c values, ketonuria or even ketoacidosis.
88 Intravenous insulin therapy: Patients with advanced diabetic foot lesions who require hospitalization, have invariably a poor glycaemic control as evident by a raised plasma glucose and HbA١c values, ketonuria or even ketoacidosis.
89 Step ٢: Estimate the Amount of Insulin Adequate Nutrition = Total Daily Dose (TDD) For patients already treated with insulin, subcutaneous regimen Weight-based estimate: TDD = ٠.۴ units x Wt in Kg Adjust down to ٠.٣ units x Wt in Kg for those with hypoglycemia risk factors, including kidney failure, type ١ diabetes (especially if lean), frail/low body weight/ malnourished elderly,. Adjust up to ٠.۵-٠.۶ units (or more) x Wt in Kg for those with hyperglycemia risk factors, including obesity and high-dose glucocorticoid treatment
90 Step ٣: Decide Which Components of Insulin the Patient Will Require, and Which Percentage of the TDD Each Should Represent Basal insulin can generally be estimated to be ١/٢ of the TDD Nutritional insulin makes up the remaining ١/٢ of the TDD
91 How to Initiate Insulin Therapy (if not already on insulin OR if uncontrolled diabetes) Regimen Tracts Dose Low Standard Moderate Aggressive (DM I, Lean DM II) (Normal weight DM) (Overweight DM) (Obese DM) Total Daily Dose (TDD) ٠.٣ units/kg/da y ٠.۴ units/kg/d ٠.۵unit/kg/ d ٠.۶unit/kg/ d Basal ½ TDD Prandial ½ TDD divided into ٣ meals Correction Scale Yup, they will also receive this too It should be the same rapid/short acting insulin as used for prandial insulin See next page
92 Correction Scale with Meals Regimen Tracts Dose Low Standard Moderate Aggressive (DM I, Lean DM II) (Normal weight DM) (Overweight DM) (Obese DM) Total Daily Dose (TDD) ٠.٣ units/kg/d ٠.۴ units/kg/d ٠.۵unit/kg/ d ٠.۶unit/kg/ d ١۶١-٢٠٠ ١ units ٢ units ٣ units ۴ units ٢٠١-٢۵٠ ٢ units ۴ units ۵ units ۶ units ٢۵١-٣٠٠ ٣ units ۶ units ٧ units ٨ units Note that correction scale can be given at night
93 If ٢ readings >١٨٠ in ٢۴ hours, diabetes is uncontrolled ٩٣
94 Glycemic Goals If ٢ readings >١٨٠ in ٢۴ hours, diabetes is uncontrolled and a change should be made to scheduled insulin Our definitions: >٣٠٠ Severe Hyperglycemia ١٨٠-٢٩٩ Hyperglycemia ١٠٠-١٨٠ Controlled <٧٠ Hypoglycmia <۴٠ Severe Hypoglycemia
95 Initiating Insulin Therapy in the Hospital Obtain patient weight in kg Calculate total daily dose (TDD) as ٠.٣ U/kg to ٠.۵ U/ kg/day Choose the dosing schedule Give ۵٠%-۶٠ ۶٠% % of TDD as basal insulin Give ۴٠%-۵٠ ۵٠% % of TDD as nutritional insulin Use correction insulin for BG above goal range Adjust according to results of bedside glucose monitoring Adjust dose for NPO status or changes in clinical status ٩۵
96 Glucose Monitoring in Hospital Bedside capillary point of care (POC) testing is the preferred method for guiding ongoing glycemic management of individual patients POC testing is usually performed ۴ times aday: before meals and at bedtime for patients who are eating For patients who are restricted to nothing by mouth or are receiving continuous enteral nutrition,: POC testing is recommended every ۴ to ۶ hours ٩۶
97
98
99 Neuropathic Foot Ulcer Without Osteomyelitis (Wagner Grades ١, ٢; UT Grades ١a, ١b, ٢a, ٢b) The most important feature in the management of neuropathic foot ulcers that typically occur under weight-bearing areas such as the metatarsal heads and great toe is the provision of adequate pressure relief This is usually achieved by a cast such as a TCC or a removable Scotch cast boot. The TCC has long been recognized as the gold standard for offloading a foot wound and was confirmed as correct in a randomized, controlled trial in which Armstrong and colleagues compared three off-loading techniques and found that the TCC was associated with the shortest healing time. the removable cast walker (RCW) resulted in slower healing than the TCC, ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
100 Neuroischemic Ulcers (Wagner Grades ١, ٢; University of Texas Grades ١c, ١d) The principles of management of neuroischemic Wagner grade ١ and ٢ ulcers are similar to those for neuropathic ulcers, with the following important exceptions. TCCs are not usually recommended for management of neuroischemic ulcers, although removable casts and pneumatic cast boots (Aircast) may be used in cases without infection. Antibiotic therapy is usually recommended for most neuroischemic ulcers. Investigation of the circulation is indicated, including noninvasive assessment and, if required, arteriography with appropriate subsequent surgical management or angioplasty. ١٣TH EDITION WILLIAMS textbook of ENDOCRINOLOGY
101 Recommendations: Foot Care Perform a comprehensive foot evaluation annually to identify risk factors for ulcers & amputations. B All patients with diabetes should have their feet inspected at every visit. C History should contain prior hx of ulceration, amputation, Charcot foot, angioplasty or vascular surgery, cigarette smoking, retinopathy & renal disease; and should assess current symptoms of neuropathy and vascular disease. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care ٢٠١٧; ۴٠ (Suppl. ١): S٨٨-S٩٨
102 Recommendations: Foot Care (٢) Exam should include inspection of the skin, assessment of foot deformities, neurologic assessment & vascular assessment including pulses in the legs and feet. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care ٢٠١٧; ۴٠ (Suppl. ١): S٨٨-S٩٨
103 Recommendations: Foot Care (٣) Patients with symptoms of claudication, decreased, or absent pedal pulses should be referred for ABI & further vascular assessment. C A multidisciplinary approach is recommended for individuals with foot ulcers and high-risk feet. B The use of specialized therapeutic footwear is recommended for patients with high-risk feet. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care ٢٠١٧; ۴٠ (Suppl. ١): S٨٨-S٩٨
104 Recommendations: Foot Care (۴) Refer patients who smoke or who have hx of lower-extremity complications, loss of protective sensation, structural abnormalities or PAD to foot care specialists for ongoing preventive care and lifelong surveillance. C Provide general foot self-care education to all patients with diabetes. B American Diabetes Association Standards of Medical Care in Diabetes. Microvascular complications and foot care. Diabetes Care ٢٠١٧; ۴٠ (Suppl. ١): S٨٨-S٩٨
105 Recommendations: Foot Care (۵) To perform the ١٠-g monofilament test, place the device perpendicular to the skin; Apply pressure until monofilament buckles. Hold in place for ١ second & release. The monofilament test should be performed at the highlighted sites while the patient s eyes are closed. Boulton A, Armstrong D, Albert, S et. al. Comprehensive Foot Examination and Risk Assessment. Diabetes Care. ٢٠٠٨; ٣١: ١۶٧٩-١۶٨۵
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers. Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT
 Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
Diabetic Foot Complications
 Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Diabetic Foot Pathophysiology. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Aetiology Macroangiopathy occurs mainly distally ie Popliteal artery There is arterial wall calcification Microangiopathy is less common
 DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections
 Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
I have no financial interests to disclose in regards to this lecture.
 Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA
 Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Diabetes Mellitus and the Associated Complications
 Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
The Diabetic Foot Latest Statistics
 The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
Charcot Arthropathy of the Foot & Ankle. MTAPA Annual Meeting June 2018 Emily Harnden, MD
 Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Front line management of the Diabetic Foot
 Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
1 of :19
 1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
Training Your Caregiver: Diabetes
 Diabetes, often referred to by doctors as diabetes mellitus, describes a group of metabolic diseases in which the person has high blood glucose (blood sugar), either because insulin production is inadequate,
Diabetes, often referred to by doctors as diabetes mellitus, describes a group of metabolic diseases in which the person has high blood glucose (blood sugar), either because insulin production is inadequate,
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Foot infections in persons with diabetes are
 DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Rapid Recovery Hyperbarics 9439 Archibald Ave. Suite 104 Rancho Cucamonga CA,
 Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Chapter 37: Exercise Prescription in Patients with Diabetes
 Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Person s Name: ID Number: Date:
 South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
Chapter 24 Diabetes Mellitus
 Chapter 24 Diabetes Mellitus Classification of Diabetes Mellitus Acute Effects of Diabetes Mellitus Chronic Complications of Diabetes Mellitus: Early Stages Chronic Complications of Diabetes Mellitus:
Chapter 24 Diabetes Mellitus Classification of Diabetes Mellitus Acute Effects of Diabetes Mellitus Chronic Complications of Diabetes Mellitus: Early Stages Chronic Complications of Diabetes Mellitus:
DISCLOSURE STATEMENT 10/8/ BASIC OF ELEMENTS OF LIMB SALVAGE MANAGEMENT
 LI MB SALVAGE MANAGEMENT October 11, 2018 DISCLOSURE STATEMENT My opinions do not represent the VA s opinions in regards to product preference No specific proprietary data from the VA has been included
LI MB SALVAGE MANAGEMENT October 11, 2018 DISCLOSURE STATEMENT My opinions do not represent the VA s opinions in regards to product preference No specific proprietary data from the VA has been included
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Peripheral Arterial Disease. Westley Smith MD Vascular Fellow
 Peripheral Arterial Disease Westley Smith MD Vascular Fellow Background (per 10,000) Goodney P, et al. Regional intensity of vascular care and lower extremity amputation rates. JVS. 2013; 6: 1471-1480.
Peripheral Arterial Disease Westley Smith MD Vascular Fellow Background (per 10,000) Goodney P, et al. Regional intensity of vascular care and lower extremity amputation rates. JVS. 2013; 6: 1471-1480.
Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections
 Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections Version 7.2 PAGL Inclusion Approved at January 2017 PGC APPROVED BY: TRUST REFERENCE: B3/2017 AWP REF: UHL Policies and
Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections Version 7.2 PAGL Inclusion Approved at January 2017 PGC APPROVED BY: TRUST REFERENCE: B3/2017 AWP REF: UHL Policies and
Diabetic Foot Services. Ketan Dhatariya Elsie Bertram Diabetes Centre Norfolk & Norwich University Hospital
 Diabetic Foot Services Ketan Dhatariya Elsie Bertram Diabetes Centre Norfolk & Norwich University Hospital Objectives 1. Background 2. Foot Screening 3. First line management ulceration 4. Management
Diabetic Foot Services Ketan Dhatariya Elsie Bertram Diabetes Centre Norfolk & Norwich University Hospital Objectives 1. Background 2. Foot Screening 3. First line management ulceration 4. Management
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
THE DIABETIC FOOT. Nicola Kilburn Diabetes Specialist Podiatrist
 THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
COMPLICATIONS OF DIABETES
 End-stage renal failure the uraemia phase Diabetes should not exclude patients from renal replacement therapy programmes. The mode of therapy (dialysis or transplantation) depends on clinical judgement
End-stage renal failure the uraemia phase Diabetes should not exclude patients from renal replacement therapy programmes. The mode of therapy (dialysis or transplantation) depends on clinical judgement
DIABETES MELLITUS. IAP UG Teaching slides
 DIABETES MELLITUS 1 DIABETES MELLITUS IN CHILDREN Introduction, Definition Classification, pathogenesis Clinical features Investigations and diagnosis Therapy and follow up Complications Carry home message
DIABETES MELLITUS 1 DIABETES MELLITUS IN CHILDREN Introduction, Definition Classification, pathogenesis Clinical features Investigations and diagnosis Therapy and follow up Complications Carry home message
The Diabetic Foot. Michael Anthony, DPM. 422 million diabetic million % adult population 90% Type II
 The Diabetic Foot Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center Prevalence of Diabetes 422 million diabetic 2016 382 million
The Diabetic Foot Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center Prevalence of Diabetes 422 million diabetic 2016 382 million
The Diabetic Foot. Prevalence of Diabetes United States. Prevalence of Diabetes
 The Diabetic Foot Prevalence of Diabetes Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center 422 million diabetic 2016 382 million
The Diabetic Foot Prevalence of Diabetes Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center 422 million diabetic 2016 382 million
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29
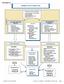 PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
American Diabetes Association: Standards of Medical Care in Diabetes 2015
 American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
A new classification of the diabetic ischaemic foot promotes a modern approach to treatment. Michael Edmonds King s College Hospital London
 A new classification of the diabetic ischaemic foot promotes a modern approach to treatment Michael Edmonds King s College Hospital London Disclosure Speaker name: Michael Edmonds... I have the following
A new classification of the diabetic ischaemic foot promotes a modern approach to treatment Michael Edmonds King s College Hospital London Disclosure Speaker name: Michael Edmonds... I have the following
National Vascular Registry
 National Vascular Registry Bypass Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or postcode.
National Vascular Registry Bypass Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or postcode.
Diabetic Feet. Juanita Muller
 Diabetic Feet Juanita Muller Mr RR 69 year old male CHARCOT ARTHROPATHY Diabetic Feet Callus Acute injury and ulceration Infection Osteomylitis Chronic ulceration Ischaemic necrosis Charcot s arthropathy
Diabetic Feet Juanita Muller Mr RR 69 year old male CHARCOT ARTHROPATHY Diabetic Feet Callus Acute injury and ulceration Infection Osteomylitis Chronic ulceration Ischaemic necrosis Charcot s arthropathy
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
DIABETIC FOOT SCOPE OF THE PROBLEM. Hanan Gawish, Mansoura University Egypt Representative of the IWGDF
 DIABETIC FOOT SCOPE OF THE PROBLEM Hanan Gawish, Mansoura University Egypt Representative of the IWGDF Agenda Definition of DF Diabetic Foot among Diabetes complication Risk factors for amputation Risk
DIABETIC FOOT SCOPE OF THE PROBLEM Hanan Gawish, Mansoura University Egypt Representative of the IWGDF Agenda Definition of DF Diabetic Foot among Diabetes complication Risk factors for amputation Risk
Rapid Foot Screening
 GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
Clinical Guideline for: Diagnosis and Management of Charcot Foot
 Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 17 Caring for Clients with Diabetes Mellitus Diabetes Mellitus Chronic disease Not a single disorder
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 17 Caring for Clients with Diabetes Mellitus Diabetes Mellitus Chronic disease Not a single disorder
Vascular dysfunction and vulnerable skin
 Vascular dysfunction and vulnerable skin Professor Peter Vowden Honorary Consultant Vascular Surgeon Clinical Director WoundTec HTC Bradford, UK 1 Exploring the clinical problem associated with the application
Vascular dysfunction and vulnerable skin Professor Peter Vowden Honorary Consultant Vascular Surgeon Clinical Director WoundTec HTC Bradford, UK 1 Exploring the clinical problem associated with the application
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Diabetes (DIA) Measures Document
 Diabetes (DIA) Measures Document DIA Version: 2.1 - covering patients discharged between 01/07/2016 and present. Programme Lead: Liz Kanwar Clinical Lead: Dr Aftab Ahmad Number of Measures In Clinical
Diabetes (DIA) Measures Document DIA Version: 2.1 - covering patients discharged between 01/07/2016 and present. Programme Lead: Liz Kanwar Clinical Lead: Dr Aftab Ahmad Number of Measures In Clinical
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
AIM OF MASTERCLASS. Overview of the diabetic foot disease. Modern approach to management
 AIM OF MASTERCLASS Overview of the diabetic foot disease Modern approach to management DIABETIC FOOT DISEASE THROUGHOUT THE WORLD, THERE IS AN AMPUTATION EVERY 20 SECONDS MOST OF THESE AMPUTATIONS ARE
AIM OF MASTERCLASS Overview of the diabetic foot disease Modern approach to management DIABETIC FOOT DISEASE THROUGHOUT THE WORLD, THERE IS AN AMPUTATION EVERY 20 SECONDS MOST OF THESE AMPUTATIONS ARE
Practical Point in Diabetic Foot Care 3-4 July 2017
 Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
My Diabetic Patient Has No Pulses; What Should I Do?
 Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태
 Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태 DMF Protocol VIPS approach V : Vascular I : infection P : Pressure off S : specific wound care Ulcer/Pressure off& Biomechanics PVD vs Peripheral neuropathy NP
Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태 DMF Protocol VIPS approach V : Vascular I : infection P : Pressure off S : specific wound care Ulcer/Pressure off& Biomechanics PVD vs Peripheral neuropathy NP
Αναγκαιότητα και τρόπος ρύθμισης του διαβήτη στους νοσηλευόμενους ασθενείς
 Αναγκαιότητα και τρόπος ρύθμισης του διαβήτη στους νοσηλευόμενους ασθενείς Αναστασία Θανοπούλου Επίκουρη Καθηγήτρια Β Παθολογικής Κλινικής Πανεπιστημίου Αθηνών Διαβητολογικό Κέντρο, Ιπποκράτειο Νοσοκομείο
Αναγκαιότητα και τρόπος ρύθμισης του διαβήτη στους νοσηλευόμενους ασθενείς Αναστασία Θανοπούλου Επίκουρη Καθηγήτρια Β Παθολογικής Κλινικής Πανεπιστημίου Αθηνών Διαβητολογικό Κέντρο, Ιπποκράτειο Νοσοκομείο
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems
 Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
A Children s Bedtime Story
 A Children s Bedtime Story Setting: University Medical Center, Big Town, USA Scenario: 0500, last admission of the night, 10 previous admissions, all tucked in for the night Patient: 75 year old male with
A Children s Bedtime Story Setting: University Medical Center, Big Town, USA Scenario: 0500, last admission of the night, 10 previous admissions, all tucked in for the night Patient: 75 year old male with
DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR
 ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
Jack W. Hutter DPM, FACFAS, C.ped
 Jack W. Hutter DPM, FACFAS, C.ped First Described in 1883 as osteoarthropathy seen in cases of syphilis The typical presentation of the rocker bottom foot As imaging techniques improved the extent of severity
Jack W. Hutter DPM, FACFAS, C.ped First Described in 1883 as osteoarthropathy seen in cases of syphilis The typical presentation of the rocker bottom foot As imaging techniques improved the extent of severity
AGONY FEET. The. of the. Prevention and management of diabetic foot ulcers
 The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
APPENDIX American Diabetes Association. Published online at
 APPENDIX 1 INPATIENT MANAGEMENT OF TYPE 2 DIABETES No algorithm applies to all patients with diabetes. These guidelines apply to patients with type 2 diabetes who are not on glucocorticoids, have no
APPENDIX 1 INPATIENT MANAGEMENT OF TYPE 2 DIABETES No algorithm applies to all patients with diabetes. These guidelines apply to patients with type 2 diabetes who are not on glucocorticoids, have no
Case 1. July 14, th week wound gel 3 cm x 2.5 cm = 7.5 cm². May 25, st wound gel on 290 days PI treatment 4 cm x 2.4 cm = 9.
 2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
NIH Public Access Author Manuscript J Diabetes Metab. Author manuscript; available in PMC 2014 July 07.
 NIH Public Access Author Manuscript Published in final edited form as: J Diabetes Metab. 2013 November 1; 4(9): 310. doi:10.4172/2155-6156.1000310. Foreign Body with Gas Gangrene in an Elderly Patient
NIH Public Access Author Manuscript Published in final edited form as: J Diabetes Metab. 2013 November 1; 4(9): 310. doi:10.4172/2155-6156.1000310. Foreign Body with Gas Gangrene in an Elderly Patient
Deepika Reddy MD Department of Endocrinology
 Deepika Reddy MD Department of Endocrinology Management of hyperglycemic crisis Review need for inpatient glycemic control Brief overview of relevant trials Case based review of diabetes management strategies/review
Deepika Reddy MD Department of Endocrinology Management of hyperglycemic crisis Review need for inpatient glycemic control Brief overview of relevant trials Case based review of diabetes management strategies/review
10/19/2017. Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI. Consultant with J&J-Depuy-Synthesis
 Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease
 Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Wounds and Infections: Wound Management From the ID Physician Standpoint. Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department
 Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
Address: Left Leg. other: Nails: thick yellow brittle fungus abnormal thick yellow brittle fungus abnormal
 South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
A one year cross sectional study on role of Wagner s classification in predicting the outcome in diabetic foot ulcer patients
 International Surgery Journal Praveena DL et al. Int Surg J. 2018 Jul;5(7):2537-2542 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182769
International Surgery Journal Praveena DL et al. Int Surg J. 2018 Jul;5(7):2537-2542 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182769
Insights on Diabetic Foot Management in UK
 Insights on Diabetic Foot Management in UK Presented by Helen CHU KEC POD I / TKOH POD i/c 2015/16 Overseas Corporate Scholarship Program for podiatrists in Diabetic Foot Management London / Leicester,
Insights on Diabetic Foot Management in UK Presented by Helen CHU KEC POD I / TKOH POD i/c 2015/16 Overseas Corporate Scholarship Program for podiatrists in Diabetic Foot Management London / Leicester,
Statistics on DM and DFU risk
 Disclosure NOTHING Statistics on DM and DFU risk National Institute of Diabetes Digestive & Kidney Diseases: As of September 2011 an estimated 16 million Americans are known to have diabetes, with many
Disclosure NOTHING Statistics on DM and DFU risk National Institute of Diabetes Digestive & Kidney Diseases: As of September 2011 an estimated 16 million Americans are known to have diabetes, with many
CHAPTER.7 CARING THE DIABETIC FOOT
 CHAPTER.7 CARING THE DIABETIC FOOT Introduction Diabetes has become a global epidemic(144). The long term complications due to diabetes impose huge social and economic burden, mental and physical misery
CHAPTER.7 CARING THE DIABETIC FOOT Introduction Diabetes has become a global epidemic(144). The long term complications due to diabetes impose huge social and economic burden, mental and physical misery
Foot infections are now among the most
 Article Progress in a pedestrian problem: A review of the revised Infectious Diseases Society of America diabetic foot infection guidelines Benjamin A Lipsky This article was first published in The Diabetic
Article Progress in a pedestrian problem: A review of the revised Infectious Diseases Society of America diabetic foot infection guidelines Benjamin A Lipsky This article was first published in The Diabetic
Autonomic neuropathy
 3. Neuropathy Autonomic neuropathy MACROVASCULAR: Accelerated atherosclerosis Coronary artery disease IHD / MI Cerebrovascular disease CVA Peripheral vascular disease gangrene / amputations NB: association
3. Neuropathy Autonomic neuropathy MACROVASCULAR: Accelerated atherosclerosis Coronary artery disease IHD / MI Cerebrovascular disease CVA Peripheral vascular disease gangrene / amputations NB: association
Physical Activity/Exercise Prescription with Diabetes
 Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
Diabetes Foot and Skin Care. Diabetes and the feet. Foot problems: Major cause of morbidity and mortality
 Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Practical guidelines on the management and prevention of the diabetic foot 2011
 DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 225 231. Published online in Wiley Online Library (wileyonlinelibrary.com).2253 IWGDF GUIDELINES Practical guidelines
DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 225 231. Published online in Wiley Online Library (wileyonlinelibrary.com).2253 IWGDF GUIDELINES Practical guidelines
Preventing Foot Ulcers in the Neuropathic Diabetic Foot. Glossary of Terms
 Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
CRITICAL LIMB ISCHEMIA UNITED STATES EPIDEMIOLOGY TABLE OF CONTENTS
 CRITICAL LIMB ISCHEMIA UNITED STATES EPIDEMIOLOGY TABLE OF CONTENTS CRITICAL LIMB ISCHEMIA... 1 CONCLUSION... 9 U.S. CRITICAL LIMB ISCHEMIA PREVALENCE... 9 MARKET OPPORTUNITY ENDOVASCULAR... 9 MARKET OPPORTUNITY
CRITICAL LIMB ISCHEMIA UNITED STATES EPIDEMIOLOGY TABLE OF CONTENTS CRITICAL LIMB ISCHEMIA... 1 CONCLUSION... 9 U.S. CRITICAL LIMB ISCHEMIA PREVALENCE... 9 MARKET OPPORTUNITY ENDOVASCULAR... 9 MARKET OPPORTUNITY
Project I - Background Worksheet. Team Members: Kira Brown, Paige Fallu. Clinical problem Diabetic Foot Ulcers
 Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
FOOT CARE ETIOLOGY OF DIABETIC FOOT PROBLEMS INTRODUCTION DIABETIC FOOT ULCERS. LIM HWEE BOON, Director, Singhealth Polyclinics Marine Parade
 DIABETES MELLITUS: REVISITED UNIT N. 5 FT CARE Dr Lim Hwee Boon ABSTRACT There is an increasing incidence of diabetes worldwide; the morbidity and the mortality is expected to increase. Early recognition
DIABETES MELLITUS: REVISITED UNIT N. 5 FT CARE Dr Lim Hwee Boon ABSTRACT There is an increasing incidence of diabetes worldwide; the morbidity and the mortality is expected to increase. Early recognition
Current Vascular and Endovascular Management in Diabetic Vasculopathy
 Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Disclosures. Critical Limb Ischemia. Vascular Testing in the CLI Patient. Vascular Testing in Critical Limb Ischemia UCSF Vascular Symposium
 Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Diabetes. HED\ED:NS-BL 037-3rd
 Diabetes HED\ED:NS-BL 037-3rd Diabetes Diabetes mellitus is an epidemic disease and based on a recent study published on 2011, the estimated number of affected people is 366 million worldwide and the number
Diabetes HED\ED:NS-BL 037-3rd Diabetes Diabetes mellitus is an epidemic disease and based on a recent study published on 2011, the estimated number of affected people is 366 million worldwide and the number
The recommended protocol is for all patients suffering from diabetes to have yearly foot checks. This was checking the foot pulses and doing
 Foot disease is a common long-term complication of diabetes. There are different types of foot disease caused by diabetes, but they all stem from a similar process. Raised blood sugar for a prolonged amount
Foot disease is a common long-term complication of diabetes. There are different types of foot disease caused by diabetes, but they all stem from a similar process. Raised blood sugar for a prolonged amount
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme
 Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital
 Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
