More Than Meets the Eye
|
|
|
- Rachel Edwards
- 5 years ago
- Views:
Transcription
1 The new england journal of medicine clinical problem-solving More Than Meets the Eye John S. Nguyen, M.D., Spyridon S. Marinopoulos, M.D., Bimal H. Ashar, M.D., and John A. Flynn, M.D. In this Journal feature, information about a real patient is presented in stages (boldface type) to an expert clinician, who responds to the information, sharing his or her reasoning with the reader (regular type). The authors commentary follows. From the Department of Medicine, Johns Hopkins University School of Medicine, Baltimore. Address reprint requests to Dr. Marinopoulos at 601 N. Caroline St., Suite 7143, Baltimore, MD 21287, or at smarino1@jhmi.edu. N Engl J Med 2006;355: Copyright 2006 Massachusetts Medical Society. A 61-year-old woman was hospitalized with a two-day history of palpitations and dyspnea. She was found to be in atrial fibrillation with a rapid ventricular response, and intravenous diltiazem and a heparin infusion were begun. Her condition improved, but on the third hospital day, she reported feeling weak and nauseated and began passing dark red urine. She did not have a urinary catheter, palpitations, dyspnea, back pain, abdominal pain, dysuria, or dizziness. The presence of dark red urine usually suggests either gross hematuria or pigmenturia (hemoglobinuria or myoglobinuria). Although pigmenturia is commonly manifested by cola- or tea-colored urine, it may also cause urine that is dark red, maroon, or even bright cherry red. The finding of abundant red cells on microscopical examination would suggest hematuria, whereas the presence of hemoglobin on urinary dipstick testing without microscopic red cells would suggest pigmenturia. (An alternative way to distinguish these two conditions would be to centrifuge the urine: red urinary sediment indicates hematuria, and red supernatant indicates pigmenturia. In the latter case, the supernatant can be tested for hemoglobin with a dipstick.) The presence of red urine with a dipstick negative for hemoglobin and without red cells on microscopy would suggest a rare cause, such as beeturia or porphyria. If this patient does have gross hematuria, I would consider the possibility of a urinary tract infection, glomerular causes, cancer, or nephrolithiasis. If there is gross hematuria in the absence of a urinary tract infection, I would evaluate this patient s urinary tract with cystoscopy and computed tomography (CT) of the abdomen and pelvis. The patient had a history of hypertension for which she took hydrochlorothiazide. She was otherwise in good health and took no other medications or herbal supplements. Her weight had not changed during the past several months. She had no history of foreign travel. She did not smoke, drink alcohol, or use illicit drugs. On examination, she was afebrile with a heart rate between 90 and 100 beats per minute, a blood pressure of 120/70 mm Hg, and respirations of 16 breaths per minute, with an oxygen saturation of 95% while breathing room air. Her lungs were clear. Cardiac examination was remarkable only for an irregular rhythm. Abdominal examination revealed no organomegaly, masses, or suprapubic tenderness. There was no costovertebral-angle tenderness. Rectal examination revealed no masses, and a guaiac test of stool was negative for occult blood. She had no skin lesions. Hematuria resulting from a genitourinary cancer remains a possibility. The absence of fever, rigors, and costovertebral-angle tenderness makes pyelonephritis an unlikely diagnosis, although a lower urinary tract infection is still a possibility. Patients with rhabdomyolysis can present with pigmenturia (i.e., myoglobinuria). How- 1048
2 ever, rhabdomyolysis is usually associated with myalgias, and the patient has not taken any medications associated with this complication. Another cause of dark red urine is hemoglobinuria as a result of brisk intravascular hemolysis. Glucose- 6-phosphate dehydrogenase (G6PD) deficiency is possible, but there is no reported history of acute infection or exposure to a drug such as a sulfonamide or nitrofurantoin that is likely to precipitate an associated hemolysis. Other potential considerations would include march hemoglobinuria, valvular disease causing microangiopathic hemolysis, and paroxysmal nocturnal hemoglobinuria (PNH). There is no recent history of vigorous exercise or evidence of a heart murmur. On the third hospital day, the white-cell count was 11,000 per cubic millimeter, as compared with 7000 per cubic millimeter at admission; the hematocrit was 30%, as compared with 35% at admission; the platelet count remained normal. The serum creatinine level was 1.8 mg per deciliter (160 μmol per liter), as compared with 0.9 mg per deciliter (80 μmol per liter) at admission. The ratio of the activated partial-thromboplastin time to a control value was 2.7 while the patient was receiving unfractionated heparin. The creatine kinase level was normal. Urinary dipstick testing revealed high levels of hemoglobin and protein (3+). Results of urine testing for myoglobin were negative. Microscopical examination of a urine specimen showed 2 to 3 red cells, 0 to 1 white cell, and 0 to 1 epithelial cell per high-power field, with few bacteria and no casts or crystals. Despite the patient s grossly dark red urine and hemoglobin on dipstick testing, there were only 2 to 3 red cells per high-power field, suggesting acute hemoglobinuria or myoglobinuria as the cause. The finding of a normal creatine kinase level and negative results for myoglobinuria on urine testing leave hemoglobinuria as the only possibility. The presence of renal failure is worrisome, since hemoglobinuria may induce acute tubular necrosis through the formation of hemoglobin casts. The presence of proteinuria may reflect a transient process, such as infection or stress, or glomerular or tubular disease. Bladder irrigation was initiated, and the patient s urine eventually became clear yellow. She remained afebrile. On the fourth hospital day, repeated laboratory testing revealed a serum creatinine level of 3.1 mg per deciliter (270 μmol per liter) and a blood urea nitrogen level of 29 mg per deciliter (10.4 mmol per liter). The hematocrit was 23%, the white-cell count was 7720 per cubic millimeter, and the platelet count was 203,000 per cubic millimeter. A peripheral-blood smear (Fig. 1) showed normal-appearing white cells and no schistocytes, bite cells, cell fragments, or spherocytes. Rapidly worsening anemia and renal failure are developing. In the absence of overt hemorrhage or aggressive fluid resuscitation, I am concerned about the possibility of massive hemolysis; the presence of hemoglobinuria indicates that the hemolysis is both intravascular and brisk. There is no report of a blood transfusion to suggest an acute hemolytic transfusion reaction. The patient s rising creatinine level may be due to pigment-induced acute tubular necrosis accompanied by extracellular volume depletion with renal ischemia. No mention has been made of possible exposure to a nephrotoxic agent or the intravenous administration of contrast material, but I would want to confirm that this information is correct. In the presence of worsening renal failure and ongoing hemolysis, hyperkalemia is a concern, and the potassium level should be monitored closely. The potassium level was 4.7 mmol per liter, and the lactate dehydrogenase level 1610 IU per liter (normal, 122 to 220). Further evaluation revealed high levels of hemosiderin (4+) in the urine, normal serum levels of G6PD, a reticulocyte count of 4.3% (normal range, 0.5 to 1.8), undetectable haptoglobin levels, and negative direct and indirect Coombs tests. The ferritin level was 30 μg per liter (normal range, 10 to 300), the serum iron level 38 μg per deciliter (7 μmol per liter; normal range, 50 to 170 μg per deciliter [9 to 30 μmol per liter]), the transferrin level 153 mg per deciliter (normal range, 200 to 400), and the iron saturation 20% (normal range, 20 to 55). The markedly elevated lactate dehydrogenase level, undetectable haptoglobin levels, and hemosiderinuria confirm the diagnosis of intravascular hemolytic anemia. The normal G6PD levels and the absence of exposure to oxidative medications make G6PD deficiency unlikely, although normal levels may occasionally be seen in patients with this disease in the setting of acute hemolysis. 1049
3 The new england journal of medicine The absence of hydronephrosis on ultrasonographic examination rules out urinary obstruction as a cause of this patient s illness. Intravenous hydration with normal saline should be continued to enhance renal perfusion and promote urinary output, as well as to prevent further renal damage from pigmenturia. Alkalinization of urine by the intravenous administration of sodium bicarbonate may provide renal protection by increasing the solubility of both myoglobin and hemoglobin and has been suggested in the management of nontraumatic rhabdomyolysis and pigmenturia. However, alkalinization carries a potential risk of hypocalcemia, and it is questionable whether it adds any benefit to volume replacement with saline alone. Figure 1. Peripheral-Blood Smear Showing Normocytic, Normochromic Red Cells (Hematoxylin and Eosin). There is no evidence of schistocytes, bite cells, or spherocytes. The patient has a ferritin level at the low end of the normal range, and iron deficiency, which can be a feature of chronic intravascular hemolysis, may be developing. Most hemolytic processes tend to occur extravascularly, with recovery of iron from the metabolized heme molecules through the reticuloendothelial system. However, massive intravascular hemolysis (as seen, for example, with march hemoglobinuria or PNH and in rare instances in patients with mechanical heart valves) may result in the liberation of a large amount of free hemoglobin intravascularly, which is then lost through renal excretion. The patient has been in the hospital and has no recent history of exertion, nor does she have a mechanical heart valve. Further inquiry into the patient s history is warranted to identify previous episodes of hemoglobinuria that would suggest the presence of PNH. Renal ultrasonography showed no evidence of hydronephrosis, nephrolithiasis, or masses. The patient continued to receive fluids intravenously and a good urine output was maintained, but her serum creatinine level continued to increase and peaked at 3.5 mg per deciliter (310 μmol per liter). She had not received contrast material intravenously or nonsteroidal antiinflammatory drugs during or before her hospitalization. Magnetic resonance angiography and venography revealed no evidence of renal-artery stenosis or renal-vein thrombosis. A renal biopsy was performed (Fig. 2), and examination of the specimen revealed extensive acute tubular injury with hemoglobin casts. Iron deposition was noted in the tubular cells. On further questioning, the patient stated that she had had similar episodes of darkcolored urine intermittently over the past several years; these usually occurred in the setting of a cold or the flu. The additional history of recurrent episodes of dark red urine and iron deposition in the tubular cells suggests a chronic relapsing course of hemolysis, which is characteristic of PNH. Examination of the renal-biopsy specimen indicates acute tubular necrosis from hemoglobin-cast deposition as a result of the patient s hemoglobinuria. Hemosiderin deposition of varying degrees within the proximal tubules has been found in patients with long-standing PNH. Mild chronic renal insufficiency and tubular concentrating defects may develop in patients with this disease. The diagnosis should be confirmed by tests showing the global deficiency of glycosylphosphatidylinositol (GPI) anchors or GPIlinked surface proteins such as CD55 or CD59. Flow-cytometric analysis of the patient s peripheral blood revealed an abnormally low level of GPI-linked protein CD59 on red cells, monocytes, and granulocytes, which is diagnostic for PNH. During the remainder of her hospitalization, she had no further episodes of hemolysis; her serum creatinine level gradually increased to 3.0 mg per deciliter (270 μmol per liter), and she was subsequently discharged home in good health. At that time, her medications included a polysaccharide iron complex twice daily. At a follow-up visit with her internist one month later, she had a serum 1050
4 creatinine level of 1.1 mg per deciliter (97 μmol per liter) and a hematocrit of 36.8%. Commentary Often, clinicians encounter new problems during the course of a patient s hospitalization that are unrelated to the initial reasons for admission. Hemoglobinuria and renal insufficiency developed in this patient while she was being treated with anticoagulants for atrial fibrillation. Because of the initial finding of a declining hematocrit and dark red urine, the first inclination might have been to attribute both to the anticoagulation therapy. Instead, further testing of the urine demonstrated hemoglobinuria rather than hematuria; the combination of this finding and renal failure prompted consideration of a pigment-induced nephropathy. This form of renal injury is seen more commonly with large crush injuries and rhabdomyolysis, in which myoglobin acts as a nephrotoxic agent. Because it is larger than myoglobin and binds to haptoglobin, hemoglobin tends to be poorly filtered across the glomerulus, and much higher serum levels of hemoglobin than myoglobin are required to cause nephrotoxicity. Massive hemoglobinuria has occurred in cases of mismatched blood transfusions, and there have been scattered case reports of hemoglobinuria associated with various medications, including triamterene, rifampin, and methyldopa. 1-3 Other causes of hemoglobinuria that may lead to renal failure include infections (typhoid fever, malaria, mumps, and clostridial sepsis), scorpion and snake bites, heavy exertion (march hemoglobinuria), 4-6 and PNH. Had the history of this patient s hemoglobinuric episodes been obtained sooner, PNH could have been diagnosed earlier. PNH is a rare disorder (with an estimated prevalence of 4 to 6 per million population) and is characterized by recurrent bouts of hemoglobinuria caused by intravascular hemolysis. Commonly, the urine is described as tea-colored or cola-colored, but it has been described in up to a third of patients as bright red. 7 Typically, the urine is darkest in the morning and clears as the day progresses, hence, the origin of the term nocturnal in the name of this disorder. The paroxysmal nature of the disease originates from the intermittent complement-mediated destruction of red cells, which may be triggered by infections, surgery, blood Figure 2. Renal-Biopsy Specimen Showing Extensive Acute Tubular Injury with Hemoglobin Casts (Arrow) in the Distal Tubules (Hematoxylin and Eosin). transfusions, or vaccinations. In many cases of PNH, however, there are no discernible precipitating events. This patient s previous bouts of red urine were temporally associated with presumed viral infections, and thus may have been due to complement activation. PNH is caused by a somatic mutation in the PIG-A gene located on the X chromosome. This gene encodes a protein necessary for the formation of GPI anchors on the surface of the various blood cell lines. Although several surface proteins are absent from the blood cells of patients with this disorder, the two most thoroughly studied are the complement-defense proteins CD55 and CD59, which normally inhibit membrane binding of C9. The absence of these surface proteins on red cells results in hemolysis when the complement cascade is activated. A relatively new technique for the diagnosis of PNH relies on a fluorescently labeled inactive variant of the protein aerolysin, which can selectively bind GPI anchors, to show the absence of GPI anchors on blood cells. 8 Not all cells are affected; the larger the proportion of affected cells (known as the abnormal clone), the greater the severity of hemolysis and the risk of thrombotic complications. 9 Intravascular hemolysis produces cell-free hemoglobin in the plasma, which then acts as a potent nitric oxide scavenger and can thus dramatically lower plasma levels of nitric oxide. The resulting decrease in plasma levels of nitric oxide may be directly responsible for most of the symptoms of PNH, including abdominal pain, esophageal spasms, erectile dysfunction, and venous thrombosis. 10 Thrombosis commonly occurs in 1051
5 the abdominal venous system and can result in intestinal obstruction, ischemic colitis, gastrointestinal bleeding, or hepatic-vein thrombosis. Patients with PNH may have bone marrow hypoplasia with reduced numbers of erythroid and myeloid progenitor cells, and up to 13% may present with aplastic anemia. 11 There are multiple case reports of PNH as a cause of acute renal failure; some cases have been severe enough to warrant temporary hemodialysis. 12,13 Proteinuria of varying degrees, as seen in this case, has also been reported in patients with PNH and is presumed to be due to tubular disease. Renal failure ultimately occurs in approximately 5% of patients with PNH. 14 Patients with PNH commonly have iron deficiency and may require oral iron supplementation. Occasionally, supplementation may initially result in a hemoglobinuric episode, as the bone marrow responds with brisk reticulocytosis. Thrombosis would be an indication for chronic anticoagulation with warfarin. Bone marrow transplantation may be curative, but given its associated risks of complications and death, it is reserved for patients with severe bone marrow hypoplasia or severe thrombotic complications. In a pilot investigation, the use of eculizumab, an antibody against C5 complement factor targeted to inhibit the final step of complement activation, resulted in reduced episodes of hemolysis and hemoglobinuria in patients with PNH. 15 Larger randomized, controlled studies of this novel drug are currently under way. No potential conflict of interest relevant to this article was reported. References 1. De Vriese AS, Robbrecht DL, Vanholder RC, Vogelaers DP, Lameire NH. Rifampicin-associated acute renal failure: pathophysiologic, immunologic, and clinical features. Am J Kidney Dis 1998;31: Woolf DC, Jacobs P. Methyldopa, intravascular haemolysis and renal disease: a case report. S Afr Med J 1990;77: Takahashi H, Tsukada T. Triamtereneinduced immune haemolytic anaemia with acute intravascular haemolysis and acute renal failure. Scand J Haematol 1979;23: Trang TT, Phu NH, Vinh H, et al. Acute renal failure in patients with severe falciparum malaria. Clin Infect Dis 1992; 15: Onwubalili JK. Haemoglobinuric renal failure and typhoid fever. Trans R Soc Trop Med Hyg 1988;82: Malhotra KK, Mirdehghan CM, Tan- don HD. Acute renal failure following scorpion sting. Am J Trop Med Hyg 1978; 27: Parab RB. Paroxysmal nocturnal hemoglobinuria: a study of 17 cases. J Postgrad Med 1990;36: Brodsky RA, Mukhina GL, Li S, et al. Improved detection and characterization of paroxysmal nocturnal hemoglobinuria using fluorescent aerolysin. Am J Clin Pathol 2000;114: Moyo VM, Mukhina GL, Garrett ES, Brodsky RA. Natural history of paroxysmal nocturnal haemoglobinuria using modern diagnostic assays. Br J Haematol 2004; 126: Rother PR, Bell L, Hillmen P, Gladwin MT. The clinical sequelae of intravascular hemolysis and extracellular plasma hemoglobin: a novel mechanism of human disease. JAMA 2005;293: Dacie JV, Lewis SM. Paroxysmal noc- turnal haemoglobinuria: clinical manifestations, haematology, and nature of the disease. Ser Haematol 1972;5: Rubin H. Paroxysmal nocturnal hemoglobinuria with renal failure. JAMA 1971; 215: Chow KM, Lai FM, Wang AY, Chan YL, Tang NL, Li PK. Reversible renal failure in paroxysmal nocturnal hemoglobinuria. Am J Kidney Dis 2001;37:E Clark DA, Butler SA, Braren V, Hartmann RC, Jenkins DE Jr. The kidneys in paroxysmal nocturnal hemoglobinuria. Blood 1981;57: Hillmen P, Hall C, Marsh JC, et al. Effect of eculizumab on hemolysis and transfusion requirements in patients with paroxysmal nocturnal hemoglobinuria. N Engl J Med 2004;350: Copyright 2006 Massachusetts Medical Society. CLINICAL PROBLEM-SOLVING SERIES The Journal welcomes submissions of manuscripts for the Clinical Problem-Solving series. This regular feature considers the step-by-step process of clinical decision making. For more information, please see
Pathophysiology 7/18/2012 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA
 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA OUTLINE OF DISCUSSION WHAT IS IT WHO GETS IT NATURAL HISTORY TYPES RISKS COURSE TREATMENTS SYMPTOMS PREGNANCY Pathophysiology Acquired hematopoietic stem cell disorder
PAROXYSMAL NOCTURNAL HEMOGLOBINURIA OUTLINE OF DISCUSSION WHAT IS IT WHO GETS IT NATURAL HISTORY TYPES RISKS COURSE TREATMENTS SYMPTOMS PREGNANCY Pathophysiology Acquired hematopoietic stem cell disorder
Living with PNH 7/3/2013. Paroxysmal Nocturnal Hemoglobinuria (PNH): A Chronic, Systemic, and Life- Threatening Disease
 Living with PNH Laurence A. Boxer, MD University of Michigan Case Study 15 year old awakened in the morning with chest pain and a sore throat. She experienced chest pain all day accompanied with coughing
Living with PNH Laurence A. Boxer, MD University of Michigan Case Study 15 year old awakened in the morning with chest pain and a sore throat. She experienced chest pain all day accompanied with coughing
Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009
 HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
Acute haemolysis and appearance of PNH-like clones in patients with vitamin B12 deficiency and iron deficiency after iron dextran administration
 Acute haemolysis and appearance of PNH-like clones in patients with vitamin B12 deficiency and iron deficiency after iron dextran administration Chun-Liang Lin 1, Chin-Chan Lin 1,Wen-Jyi Lo 2,Yu-Chien
Acute haemolysis and appearance of PNH-like clones in patients with vitamin B12 deficiency and iron deficiency after iron dextran administration Chun-Liang Lin 1, Chin-Chan Lin 1,Wen-Jyi Lo 2,Yu-Chien
The use of the complement inhibitor eculizumab (Soliris R ) for treating Korean patients with paroxysmal nocturnal hemoglobinuria
 VOLUME 45 ㆍ NUMBER 4 ㆍ December 2010 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE The use of the complement inhibitor eculizumab (Soliris R ) for treating Korean patients with paroxysmal nocturnal
VOLUME 45 ㆍ NUMBER 4 ㆍ December 2010 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE The use of the complement inhibitor eculizumab (Soliris R ) for treating Korean patients with paroxysmal nocturnal
PNH: Current Thinking on the Disease, Diagnosis and Treatment. What is PNH? 7/6/2009. Paroxysmal sudden onset Nocturnal
 PNH: Current hinking on the Disease, Diagnosis and reatment Jaroslaw Maciejewski, MD, PhD Cleveland Clinic Carlos M. de Castro, MD Duke University Medical Center Paroxysmal sudden onset Nocturnal occuring
PNH: Current hinking on the Disease, Diagnosis and reatment Jaroslaw Maciejewski, MD, PhD Cleveland Clinic Carlos M. de Castro, MD Duke University Medical Center Paroxysmal sudden onset Nocturnal occuring
eculizumab, 300mg concentrate for solution for infusion (Soliris ) SMC No. (436/07) Alexion Pharma UK Ltd
 eculizumab, 300mg concentrate for solution for infusion (Soliris ) SMC No. (436/07) Alexion Pharma UK Ltd 8 October 2010 (Amended 11 July 2011) The Scottish Medicines Consortium (SMC) has completed its
eculizumab, 300mg concentrate for solution for infusion (Soliris ) SMC No. (436/07) Alexion Pharma UK Ltd 8 October 2010 (Amended 11 July 2011) The Scottish Medicines Consortium (SMC) has completed its
PNH Glossary of Terms
 AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
Definition : Stages : ( RIFLE vs. AKIN ) Causes and classification : Pre-renal Renal Post- renal Clinical manifestations and Complication Management
 AKI Definition : Stages : ( RIFLE vs. AKIN ) Causes and classification : Pre-renal Renal Post- renal Clinical manifestations and Complication Management and indications for RRT Etiology prerenal causes
AKI Definition : Stages : ( RIFLE vs. AKIN ) Causes and classification : Pre-renal Renal Post- renal Clinical manifestations and Complication Management and indications for RRT Etiology prerenal causes
What is PNH? PNH: What it is Not 9/11/2015. What is Paroxysmal Nocturnal Hemoglobinuria?
 9/11/15 PNH: Current Thinking on the Disease, Diagnosis, and Treatment Joseph H. Antin, MD Professor of Medicine Harvard Medical School Jock and Bunny Adams Chair in Hematology Dana-Farber/Brigham and
9/11/15 PNH: Current Thinking on the Disease, Diagnosis, and Treatment Joseph H. Antin, MD Professor of Medicine Harvard Medical School Jock and Bunny Adams Chair in Hematology Dana-Farber/Brigham and
PNH. PNH A study case 5/9/2012. PNH Current Thinking on the Disease, Diagnosis, and Treatment. Where have we been, where are we going?
 PNH Current Thinking on the Disease, Diagnosis, and Treatment Where have we been, where are we going? Carlos M. de Castro, MD Duke University Medical Center PNH Case What is PNH? What causes PNH? Relationship
PNH Current Thinking on the Disease, Diagnosis, and Treatment Where have we been, where are we going? Carlos M. de Castro, MD Duke University Medical Center PNH Case What is PNH? What causes PNH? Relationship
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
The Urinary System. Lab Exercise 38. Objectives. Introduction
 Lab Exercise The Urinary System Objectives - Be able to identify the structures of the urinary system and give their function - Be able to recognize the gross anatomy of the kidney - Identify the components
Lab Exercise The Urinary System Objectives - Be able to identify the structures of the urinary system and give their function - Be able to recognize the gross anatomy of the kidney - Identify the components
Glucose-6-Phosphate Dehydrogenase
 Glucose-6-Phosphate Dehydrogenase Is the major enzyme in the pentose phosphate pathway (also called the phosphogluconate pathway or the hexose monophosphate shunt) which is a metabolic pathway parallel
Glucose-6-Phosphate Dehydrogenase Is the major enzyme in the pentose phosphate pathway (also called the phosphogluconate pathway or the hexose monophosphate shunt) which is a metabolic pathway parallel
MODULE 5: HEMATURIA LEARNING OBJECTIVES DEFINITION. KEY WORDS: Hematuria, Cystoscopy, Urine Cytology, UTI, bladder cancer
 MODULE 5: HEMATURIA KEY WORDS: Hematuria, Cystoscopy, Urine Cytology, UTI, bladder cancer LEARNING OBJECTIVES At the end of this clerkship, the learner will be able to: 1. Define microscopic hematuria.
MODULE 5: HEMATURIA KEY WORDS: Hematuria, Cystoscopy, Urine Cytology, UTI, bladder cancer LEARNING OBJECTIVES At the end of this clerkship, the learner will be able to: 1. Define microscopic hematuria.
CASE REPORT Assessing donor chimerism using flow cytometry in paroxysmal nocturnal haemoglobinuria after stem cell transplantation - a case report
 Malaysian J Pathol 2006; 28(2) : 107 112 CASE REPORT Assessing donor chimerism using flow cytometry in paroxysmal nocturnal haemoglobinuria after stem cell transplantation - a case report R Z Azma, MBBS,
Malaysian J Pathol 2006; 28(2) : 107 112 CASE REPORT Assessing donor chimerism using flow cytometry in paroxysmal nocturnal haemoglobinuria after stem cell transplantation - a case report R Z Azma, MBBS,
PNH PNH PNH 3/22/2016 PNH. Paroxysmal Nocturnal Hemoglobinuria (PNH): Current Thinking on the Disease PATHOGENESIS OF PNH
 3//1 PATHGENESIS F PIG-A gene Bone Marrow Failure Disease Scientific Symposium Rockville, March 17-1, 1 1 71 9 3 Paroxysmal Nocturnal Hemoglobinuria (): Current Thinking on the Disease 119 5 15 PRTEIN
3//1 PATHGENESIS F PIG-A gene Bone Marrow Failure Disease Scientific Symposium Rockville, March 17-1, 1 1 71 9 3 Paroxysmal Nocturnal Hemoglobinuria (): Current Thinking on the Disease 119 5 15 PRTEIN
Introduction to Clinical Diagnosis Nephrology
 Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
10/27/2017 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA DANIEL LANDAU, MD PNH TYPICAL CASE
 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA Daniel Landau, MD Orlando Health: UF Health Cancer Center Hematologist/ Oncologist Orlando Health University of Florida Cancer Center Section Chief of Hematology/Oncology
PAROXYSMAL NOCTURNAL HEMOGLOBINURIA Daniel Landau, MD Orlando Health: UF Health Cancer Center Hematologist/ Oncologist Orlando Health University of Florida Cancer Center Section Chief of Hematology/Oncology
Non-immune acquired haemolytic anaemias. Dr.Maysem
 Non-immune acquired haemolytic anaemias Dr.Maysem Causes of Non-immune acquired haemolytic anaemias. Infections Infections can cause haemolysis in a variety of ways: -They may precipitate an acute haemolytic
Non-immune acquired haemolytic anaemias Dr.Maysem Causes of Non-immune acquired haemolytic anaemias. Infections Infections can cause haemolysis in a variety of ways: -They may precipitate an acute haemolytic
DRUG NAME: Eculizumab Brand(s): Soliris DOSAGE FORM/ STRENGTH: 10 mg/ml (300 mg per vial)
 Preamble: A confirmed diagnosis of atypical hemolytic uremic syndrome (ahus) is required for eculizumab funding. The information below is to provide clinicians with context for how a diagnosis of ahus
Preamble: A confirmed diagnosis of atypical hemolytic uremic syndrome (ahus) is required for eculizumab funding. The information below is to provide clinicians with context for how a diagnosis of ahus
Dr P Sigwadi 30 May 2012
 Dr P Sigwadi 30 May 2012 Introduction Haematuria Positive blood on urine dipstick 5 red blood cells/ microliter of urine Prevalence Gross haematuria ( macroscopic) 0.13 % Microscopic- 1.5% Haematuria +
Dr P Sigwadi 30 May 2012 Introduction Haematuria Positive blood on urine dipstick 5 red blood cells/ microliter of urine Prevalence Gross haematuria ( macroscopic) 0.13 % Microscopic- 1.5% Haematuria +
Paroxysmal Nocturnal Hemoglobinuria
 Paroxysmal Nocturnal Hemoglobinuria Current Thinking On the Disease Diagnosis and Treatment Ilene Ceil Weitz, MD Associate Clinical Professor of Medicine Jane Anne Nohl Division of Hematology Keck-USC
Paroxysmal Nocturnal Hemoglobinuria Current Thinking On the Disease Diagnosis and Treatment Ilene Ceil Weitz, MD Associate Clinical Professor of Medicine Jane Anne Nohl Division of Hematology Keck-USC
Diagnostic Approach to Patients with Anemia
 J KMA Special Issue Diagnostic Approach to Patients with Anemia Seonyang Park, MD Department of Internal Medicine, Seoul National University College of Medicine E mail : seonpark@snu.ac.kr J Korean Med
J KMA Special Issue Diagnostic Approach to Patients with Anemia Seonyang Park, MD Department of Internal Medicine, Seoul National University College of Medicine E mail : seonpark@snu.ac.kr J Korean Med
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE
 PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
HEMOLY L TIC AN A EMIA
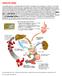 HEMOLYTIC ANEMIA In a healthy person, a red blood cell survives 90 to 120 days in the circulation, so about 1% of human red blood cells break down each day. The spleen (part of the reticulo-endothelial
HEMOLYTIC ANEMIA In a healthy person, a red blood cell survives 90 to 120 days in the circulation, so about 1% of human red blood cells break down each day. The spleen (part of the reticulo-endothelial
3 Ruba hussein Dr. ahmad Dr. ahmad
 3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2014 (2014), Article ID 504318, 21 minipages. DOI:10.5171/2014.504318 www.ibimapublishing.com Copyright 2014 Pinar Tosun Taşar, Sevnaz Sahin, Asu
International Journal of Case Reports in Medicine Vol. 2014 (2014), Article ID 504318, 21 minipages. DOI:10.5171/2014.504318 www.ibimapublishing.com Copyright 2014 Pinar Tosun Taşar, Sevnaz Sahin, Asu
PNH. What is PNH? 7/12/2016 PNH. What is PNH? 1 st published case report of PNH
 AA-MDS Patient Conference Raleigh / Durham July 016 : Current Thinking on the Disease, Diagnosis, and Treatment What is? What causes? What are the clinical symptoms of? How is diagnosed? What are the long-term
AA-MDS Patient Conference Raleigh / Durham July 016 : Current Thinking on the Disease, Diagnosis, and Treatment What is? What causes? What are the clinical symptoms of? How is diagnosed? What are the long-term
Paroxysmal Nocturnal Hemoglobinuria
 Paroxysmal Nocturnal Hemoglobinuria Barry Skikne MD, FACP, FCP(SA) Professor of Hematology Division of Hematologic Malignancies and Cellular Therapeutics Cardinal Clinical Manifestations PNH Clonal disease
Paroxysmal Nocturnal Hemoglobinuria Barry Skikne MD, FACP, FCP(SA) Professor of Hematology Division of Hematologic Malignancies and Cellular Therapeutics Cardinal Clinical Manifestations PNH Clonal disease
PRINCIPLE OF URINALYSIS
 PRINCIPLE OF URINALYSIS Vanngarm Gonggetyai Objective Can explain : the abnormalities detected in urine Can perform : routine urinalysis Can interprete : the results of urinalysis Examination of urine
PRINCIPLE OF URINALYSIS Vanngarm Gonggetyai Objective Can explain : the abnormalities detected in urine Can perform : routine urinalysis Can interprete : the results of urinalysis Examination of urine
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
Soliris (eculizumab) DRUG.00050
 Market DC Soliris (eculizumab) DRUG.00050 Override(s) Prior Authorization Approval Duration 1 year Medications Soliris (eculizumab) APPROVAL CRITERIA Paroxysmal Nocturnal Hemoglobinuria I. Initiation of
Market DC Soliris (eculizumab) DRUG.00050 Override(s) Prior Authorization Approval Duration 1 year Medications Soliris (eculizumab) APPROVAL CRITERIA Paroxysmal Nocturnal Hemoglobinuria I. Initiation of
Abdominal pain in combination with an unexplained hemolytic anemia are crucial signs to test for paroxysmal nocturnal hemoglobinuria: A case report
 Received: 22 January 2018 Revised: 25 April 2018 DOI: 10.1002/ccr3.1771 Accepted: 9 June 2018 CASE REPORT Abdominal pain in combination with an unexplained hemolytic anemia are crucial signs to test for
Received: 22 January 2018 Revised: 25 April 2018 DOI: 10.1002/ccr3.1771 Accepted: 9 June 2018 CASE REPORT Abdominal pain in combination with an unexplained hemolytic anemia are crucial signs to test for
New Phase III Clinical Trial Enrolling Now
 New Phase III Clinical Trial Enrolling Now Paroxysmal Nocturnal Hemoglobinuria (PNH) Designed for Patients 1. At least 18 years of age 2. With a primary diagnosis of PNH confirmed by high-sensitivity flow
New Phase III Clinical Trial Enrolling Now Paroxysmal Nocturnal Hemoglobinuria (PNH) Designed for Patients 1. At least 18 years of age 2. With a primary diagnosis of PNH confirmed by high-sensitivity flow
URINARY CRYSTALS. by Geoffrey K. Dube and Robert S. Brown
 URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
9/19/2017. PNH Understanding your diagnosis and treatment. Paroxysmal Nocturnal Hemoglobinuria (PNH) Paroxysmal Nocturnal Hemoglobinuria
 August_20_2010US Patients Surviving (%) Paroxysmal Nocturnal Hemoglobinuria (PNH) PNH Understanding your diagnosis and treatment Hugo Castro-Malaspina, MD Memorial Sloan Kettering Cancer Center New York,
August_20_2010US Patients Surviving (%) Paroxysmal Nocturnal Hemoglobinuria (PNH) PNH Understanding your diagnosis and treatment Hugo Castro-Malaspina, MD Memorial Sloan Kettering Cancer Center New York,
The Excretory System
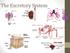 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
Introduction and Approach to Anemia
 2 nd lecture in Hematology by Dr.Alaa Fadhil Alwan Introduction and Approach to Anemia Anemia is defined clinically as a blood hemoglobin or hematocrit value that is below the appropriate reference range
2 nd lecture in Hematology by Dr.Alaa Fadhil Alwan Introduction and Approach to Anemia Anemia is defined clinically as a blood hemoglobin or hematocrit value that is below the appropriate reference range
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University
 RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
رناد زكريا Dr. ahmad Dr. ahmad. P a g e 1
 5 رناد زكريا Dr. ahmad Dr. ahmad P a g e 1 Before we start. -This sheet was written according to section 2 s record and reviewed according to section 1 s record by Ruba Hussien with all thanks and I referred
5 رناد زكريا Dr. ahmad Dr. ahmad P a g e 1 Before we start. -This sheet was written according to section 2 s record and reviewed according to section 1 s record by Ruba Hussien with all thanks and I referred
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY
 THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
AN APPROACH TO HEMATURIA. Dr Saima Ali
 AN APPROACH TO HEMATURIA Dr Saima Ali Definition Microscopic hematuria hematuria is defined as the presence of 5 or more RBCs per high-power field in 3 of 3 consecutive centrifuged specimens obtained at
AN APPROACH TO HEMATURIA Dr Saima Ali Definition Microscopic hematuria hematuria is defined as the presence of 5 or more RBCs per high-power field in 3 of 3 consecutive centrifuged specimens obtained at
3/31/2014 PNH. Jack Goldberg MD FACP. Clinical Professor of Medicine University of Pennsylvania
 PNH Jack Goldberg MD FACP Clinical Professor of Medicine University of Pennsylvania 1 2 3 4 1 5 6 Historically Viewed as a Hemolytic Anemia Normal red blood cells are protected from complement attack by
PNH Jack Goldberg MD FACP Clinical Professor of Medicine University of Pennsylvania 1 2 3 4 1 5 6 Historically Viewed as a Hemolytic Anemia Normal red blood cells are protected from complement attack by
Case Report Recurrent and Progressive Abdominal Pain and Enteritis in a Japanese Patient with Paroxysmal Nocturnal Hemoglobinuria
 Case Reports in Hematology, Article ID 310750, 4 pages http://dx.doi.org/10.1155/2014/310750 Case Report Recurrent and Progressive Abdominal Pain and Enteritis in a Japanese Patient with Paroxysmal Nocturnal
Case Reports in Hematology, Article ID 310750, 4 pages http://dx.doi.org/10.1155/2014/310750 Case Report Recurrent and Progressive Abdominal Pain and Enteritis in a Japanese Patient with Paroxysmal Nocturnal
Soliris (eculizumab) For the Treatment of PNH to Reduce Hemolysis
 Soliris (eculizumab) You have done well to manage your PNH with Soliris. Living with a rare disease, like PNH, can be challenging, but by sticking with your Soliris therapy, you are doing a lot to help
Soliris (eculizumab) You have done well to manage your PNH with Soliris. Living with a rare disease, like PNH, can be challenging, but by sticking with your Soliris therapy, you are doing a lot to help
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Acute kidney injury definition, causes and pathophysiology. Financial Disclosure. Some History Trivia. Key Points. What is AKI
 Acute kidney injury definition, causes and pathophysiology Financial Disclosure Current support: Center for Sepsis and Critical Illness Award P50 GM-111152 from the National Institute of General Medical
Acute kidney injury definition, causes and pathophysiology Financial Disclosure Current support: Center for Sepsis and Critical Illness Award P50 GM-111152 from the National Institute of General Medical
HEMOLYSIS AND JAUNDICE:
 1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL SEMINAR HEMOLYSIS AND JAUNDICE: An overview
1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL SEMINAR HEMOLYSIS AND JAUNDICE: An overview
Physical Characteristics of
 Physical Characteristics of Urine Bởi: OpenStaxCollege The urinary system s ability to filter the blood resides in about 2 to 3 million tufts of specialized capillaries the glomeruli distributed more or
Physical Characteristics of Urine Bởi: OpenStaxCollege The urinary system s ability to filter the blood resides in about 2 to 3 million tufts of specialized capillaries the glomeruli distributed more or
Chapter 14. Blood. Blood Volume. Blood Composition. Blood
 Blood connective tissue transports vital substances maintains stability of interstitial fluid distributes heat Chapter 14 Blood Blood Cells form mostly in red bone marrow red blood cells white blood cells
Blood connective tissue transports vital substances maintains stability of interstitial fluid distributes heat Chapter 14 Blood Blood Cells form mostly in red bone marrow red blood cells white blood cells
Definitions. You & Your New Transplant ` 38
 Definitions Acute Short, relatively severe Analgesic Pain medicine Anemia A low number of red blood cells Anesthetic Medication that dulls sensation in order to reduce pain Acute Tubular Necrosis (ATN)
Definitions Acute Short, relatively severe Analgesic Pain medicine Anemia A low number of red blood cells Anesthetic Medication that dulls sensation in order to reduce pain Acute Tubular Necrosis (ATN)
Dana Alsulaibi. - Ahmad Almuhtaseb. - Tariq Al - Adaily
 - 2 - Dana Alsulaibi - Ahmad Almuhtaseb - Tariq Al - Adaily This sheet will talk about 4 diseases that cause hemolytic anemia, best of luck! 1) Hereditary Spherocytosis Transferred through inheritance
- 2 - Dana Alsulaibi - Ahmad Almuhtaseb - Tariq Al - Adaily This sheet will talk about 4 diseases that cause hemolytic anemia, best of luck! 1) Hereditary Spherocytosis Transferred through inheritance
4/17/2018. Paroxysmal Nocturnal Hemoglobinuria: Paroxysmal Nocturnal Hemoglobinuria. Epidemiology. PNH Stem Cell.
 Paroxysmal Nocturnal Hemoglobinuria: Understanding the Diagnosis, Complications and Treatment Options Iberia Romina Sosa, MD, PhD Assistant Professor of Medicine Baylor College of Medicine April 21, 2018
Paroxysmal Nocturnal Hemoglobinuria: Understanding the Diagnosis, Complications and Treatment Options Iberia Romina Sosa, MD, PhD Assistant Professor of Medicine Baylor College of Medicine April 21, 2018
7/14/2014. SOLIRIS (eculizumab) SOLIRIS PNH Clinical Studies. SOLIRIS Blocks Terminal Complement. 86% Reduction in LDH: TRIUMPH and SHEPHERD
 Proximal Terminal Lactate Dehydrogenase (U/L) 7/1/1 SOLIRIS (eculizumab) Humanized First in Class Anti - C5 Antibody SOLIRIS (eculizumab) Human Framework Regions No mutations Germline SOLIRIS is a Complement
Proximal Terminal Lactate Dehydrogenase (U/L) 7/1/1 SOLIRIS (eculizumab) Humanized First in Class Anti - C5 Antibody SOLIRIS (eculizumab) Human Framework Regions No mutations Germline SOLIRIS is a Complement
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome.
 Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature
 Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Routine urine examination
 Routine urine examination 尿常规检查 Huawei Liang, PhD E-mail: hwliang99@163.com Objectives To examine urine for the presence of normal and abnormal constituents by routine urine analysis Principles Urine formation
Routine urine examination 尿常规检查 Huawei Liang, PhD E-mail: hwliang99@163.com Objectives To examine urine for the presence of normal and abnormal constituents by routine urine analysis Principles Urine formation
URINE DIPSTICK AND SULPHOSALICYLIC ACID TEST. Špela Borštnar UREX 2015, Ljubljana, Slovenia
 URINE DIPSTICK AND SULPHOSALICYLIC ACID TEST Špela Borštnar UREX 2015, Ljubljana, Slovenia KIDNEY DISEASE? severity of kidney disease = estimating GFR cause of kidney disease = urinalysis URINE EXAMINATION
URINE DIPSTICK AND SULPHOSALICYLIC ACID TEST Špela Borštnar UREX 2015, Ljubljana, Slovenia KIDNEY DISEASE? severity of kidney disease = estimating GFR cause of kidney disease = urinalysis URINE EXAMINATION
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acute lymphoblastic leukemia, in India, 439 440 pediatric, global approach to, 420 424 core resources in low- and middle-income countries, 423
Note: Page numbers of article titles are in boldface type. A Acute lymphoblastic leukemia, in India, 439 440 pediatric, global approach to, 420 424 core resources in low- and middle-income countries, 423
ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES ALDO E CELE DACCO
 ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CENTRO MARIO DI NEGRI RICERCHE INSTITUTE CLINICHE FOR PHARMACOLOGICAL PER LE MALATTIE RESEARCH RARE CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES
ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CENTRO MARIO DI NEGRI RICERCHE INSTITUTE CLINICHE FOR PHARMACOLOGICAL PER LE MALATTIE RESEARCH RARE CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES
GENERAL URINE EXAMINATION (URINE ANALYSIS)
 GENERAL URINE EXAMINATION (URINE ANALYSIS) Physiology Lab-8 December, 2018 Lect. Asst. Zakariya A. Mahdi MSc Pharmacology Background Urine (from Latin Urina,) is a typically sterile liquid by-product of
GENERAL URINE EXAMINATION (URINE ANALYSIS) Physiology Lab-8 December, 2018 Lect. Asst. Zakariya A. Mahdi MSc Pharmacology Background Urine (from Latin Urina,) is a typically sterile liquid by-product of
GASTROINESTINAL BLEEDING. Dr.Ammar I. Abdul-Latif
 GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
HEMATOPOIESIS. HEMATOLOGY Introduction. Study of blood & its components Window of rest of body. Introduction
 HEMATOLOGY/ HEMATOPOIESIS Introduction HEMATOLOGY Introduction Study of blood & its components Window of rest of body 1 BLOOD Raison d etre Delivery of nutrients Oxygen Food Vitamins Removal of wastes
HEMATOLOGY/ HEMATOPOIESIS Introduction HEMATOLOGY Introduction Study of blood & its components Window of rest of body 1 BLOOD Raison d etre Delivery of nutrients Oxygen Food Vitamins Removal of wastes
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
CRRT Fundamentals Pre- and Post- Test. AKI & CRRT Conference 2018
 CRRT Fundamentals Pre- and Post- Test AKI & CRRT Conference 2018 Question 1 Which ONE of the following statements regarding solute clearance in CRRT is MOST correct? A. Convective and diffusive solute
CRRT Fundamentals Pre- and Post- Test AKI & CRRT Conference 2018 Question 1 Which ONE of the following statements regarding solute clearance in CRRT is MOST correct? A. Convective and diffusive solute
SOLIRIS is a Complement Inhibitor Indicated for the Treatment of Patients With PNH to Reduce Hemolysis
 SOLIRIS (eculizumab) SOLIRIS is a Complement Inhibitor Indicated for the Treatment of Patients With PNH to Reduce Hemolysis SOLIRIS is the First and Only Approved Therapy for PNH SOLIRIS (eculizumab) [package
SOLIRIS (eculizumab) SOLIRIS is a Complement Inhibitor Indicated for the Treatment of Patients With PNH to Reduce Hemolysis SOLIRIS is the First and Only Approved Therapy for PNH SOLIRIS (eculizumab) [package
HAEMATOLOGICAL EVALUATION OF ANEMIA. Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore
 HAEMATOLOGICAL EVALUATION OF ANEMIA Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore Learning Objectives Laboratory tests for the evaluation of anemia
HAEMATOLOGICAL EVALUATION OF ANEMIA Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore Learning Objectives Laboratory tests for the evaluation of anemia
Hematuria. Ramzi El-Baroudy (ESPNT)
 Hematuria Ramzi El-Baroudy (ESPNT) Hematuria is the presence of RBCs in urine. If the amount of blood in urine is big enough, the urine will, then, look red. Something which is, undoubtedly, terrifying.
Hematuria Ramzi El-Baroudy (ESPNT) Hematuria is the presence of RBCs in urine. If the amount of blood in urine is big enough, the urine will, then, look red. Something which is, undoubtedly, terrifying.
Acute Kidney Injury. I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS
 Acute Kidney Injury I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS 374-6102 David.Weiner@medicine.ufl.edu www.renallectures.com Concentration
Acute Kidney Injury I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS 374-6102 David.Weiner@medicine.ufl.edu www.renallectures.com Concentration
SOLIRIS (eculizumab) Slide # 1. How do we treat PNH?
 Treating PNH How do we treat PNH? Hemolytic anemia Iron, folic acid Transfusion Steroids Eculizumab Thrombosis Coumadin prophylaxis Acute treatment with lytic agents (clot busters) Anticoagulation therapy
Treating PNH How do we treat PNH? Hemolytic anemia Iron, folic acid Transfusion Steroids Eculizumab Thrombosis Coumadin prophylaxis Acute treatment with lytic agents (clot busters) Anticoagulation therapy
Calcium (Ca 2+ ) mg/dl
 Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Key terms: aplastic anemia; complement inhibitors; paroxysmal nocturnal hemoglobinuria
 Cytometry Part B (Clinical Cytometry) 94B:16 22 (2018) Original Article ICCS/ESCCA Consensus Guidelines to detect GPI-deficient cells in Paroxysmal Nocturnal Hemoglobinuria (PNH) and related Disorders
Cytometry Part B (Clinical Cytometry) 94B:16 22 (2018) Original Article ICCS/ESCCA Consensus Guidelines to detect GPI-deficient cells in Paroxysmal Nocturnal Hemoglobinuria (PNH) and related Disorders
Routine Clinic Lab Studies
 Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
Efficacy of eculizumab in paroxysmal nocturnal hemoglobinuria patients with or without aplastic anemia: prospective study of a Korean PNH cohort
 BLOOD RESEARCH VOLUME 52 ㆍ NUMBER 3 September 2017 ORIGINAL ARTICLE Efficacy of eculizumab in paroxysmal nocturnal hemoglobinuria patients with or without aplastic anemia: prospective study of a Korean
BLOOD RESEARCH VOLUME 52 ㆍ NUMBER 3 September 2017 ORIGINAL ARTICLE Efficacy of eculizumab in paroxysmal nocturnal hemoglobinuria patients with or without aplastic anemia: prospective study of a Korean
Evaluation of Anemia. Md. Shafiqul Bari Associate professor (Medicine) SOMC
 Evaluation of Anemia Md. Shafiqul Bari Associate professor (Medicine) SOMC Definition Anemia is operationally defined as a reduction in one or more of the major RBC measurements Hemoglobin concentration
Evaluation of Anemia Md. Shafiqul Bari Associate professor (Medicine) SOMC Definition Anemia is operationally defined as a reduction in one or more of the major RBC measurements Hemoglobin concentration
Hemolytic Anemia. Hemolytic Anemia Classification Intracorpuscular Defects. Hemolytic Anemia Classification
 Hemolytic Anemia Fletcher A. Miller, Jr, MD Mayo Clinic Rochester Valve Related Hemolysis Case Based presentation Shortened survival of red blood cells due to premature destruction Typical RBC lifespan
Hemolytic Anemia Fletcher A. Miller, Jr, MD Mayo Clinic Rochester Valve Related Hemolysis Case Based presentation Shortened survival of red blood cells due to premature destruction Typical RBC lifespan
Extra Notes 3. Warm. In the core (center) of the body, where the temperature is 37 C.
 Extra Notes 3 *The numbers of the slides are according to the last year slides. Slide 33 Autoimmune hemolytic anemia : Abnormal circulating antibodies that target normal antigen on the RBC and cause lysis.
Extra Notes 3 *The numbers of the slides are according to the last year slides. Slide 33 Autoimmune hemolytic anemia : Abnormal circulating antibodies that target normal antigen on the RBC and cause lysis.
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
WARNING: SERIOUS MENINGOCOCCAL INFECTIONS
 Indication and Usage Paroxysmal Nocturnal Hemoglobinuria (PNH) Soliris (eculizumab) is indicated for the treatment of patients with paroxysmal nocturnal hemoglobinuria (PNH) to reduce hemolysis. WARNING:
Indication and Usage Paroxysmal Nocturnal Hemoglobinuria (PNH) Soliris (eculizumab) is indicated for the treatment of patients with paroxysmal nocturnal hemoglobinuria (PNH) to reduce hemolysis. WARNING:
Year 2003 Paper two: Questions supplied by Tricia
 QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
Patient Education. Transplant Services. Benefits and. Of a kidney/pancreas transplant
 Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
A&P of the Urinary System
 A&P of the Urinary System Week 44 1 Objectives Identify the organs of the urinary system, from a Identify the parts of the nephron (the functional unit List the characteristics of a normal urine specimen.
A&P of the Urinary System Week 44 1 Objectives Identify the organs of the urinary system, from a Identify the parts of the nephron (the functional unit List the characteristics of a normal urine specimen.
Anemia. A case-based approach. David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017
 Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Severe falciparum malaria with hypophosphataemia and presumed hypophosphatemia induced rhabdomyolysis: a case report
 142 Case Report Severe falciparum malaria with hypophosphataemia and presumed hypophosphatemia induced rhabdomyolysis: a case report M Perera, V Samarawickrama, K Lokuketagoda, K Thirumavalavan Sri Lankan
142 Case Report Severe falciparum malaria with hypophosphataemia and presumed hypophosphatemia induced rhabdomyolysis: a case report M Perera, V Samarawickrama, K Lokuketagoda, K Thirumavalavan Sri Lankan
IF YOU HAVE PNH, YOU ARE NOT ALONE. Take a closer look and take control of PNH
 IF YOU HAVE PNH, YOU ARE NOT ALONE Take a closer look and take control of PNH Indication and Usage Paroxysmal Nocturnal Hemoglobinuria (PNH) Soliris (eculizumab) is indicated for the treatment of patients
IF YOU HAVE PNH, YOU ARE NOT ALONE Take a closer look and take control of PNH Indication and Usage Paroxysmal Nocturnal Hemoglobinuria (PNH) Soliris (eculizumab) is indicated for the treatment of patients
Examination Tests from Pathological Physiology. Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc.
 Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
Slide # 1. PNH: Comlications and. Long-Term Issues. Long-Term Issues. What is PNH and what is the long term outlook?
 PNH: Complications and Long-Term Issues Carlos M. de Castro, MD Duke University Center What happens to PNH patients? PNH: Comlications and Long-Term Issues What are the long-term complications of PNH and
PNH: Complications and Long-Term Issues Carlos M. de Castro, MD Duke University Center What happens to PNH patients? PNH: Comlications and Long-Term Issues What are the long-term complications of PNH and
Types of Anaemias and their Management. S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014
 Types of Anaemias and their Management S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014 Objectives At the end of the presentations participants should be able to: 1. Define
Types of Anaemias and their Management S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014 Objectives At the end of the presentations participants should be able to: 1. Define
Aplastic anamia & Sideroblastic anemia
 Hematology Lecture 7 كلية التقنيات الصحية والطبية قسم التحليالت المرضية Aplastic anamia & Sideroblastic anemia اإلعداد: ظفر جبار دهاق فؤاد APLASTIC ANEMIA What is Aplastic anemia? Aplastic anemia is a
Hematology Lecture 7 كلية التقنيات الصحية والطبية قسم التحليالت المرضية Aplastic anamia & Sideroblastic anemia اإلعداد: ظفر جبار دهاق فؤاد APLASTIC ANEMIA What is Aplastic anemia? Aplastic anemia is a
C. treatment with Desferal (deferoxamine mesylate USP, iron-chelating agent)
 HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
Chapter 119 Rhabdomyolysis
 Chapter 119 Rhabdomyolysis Episode overview 1. List the pathophysiology of rhabdomyolysis 2. List 8 causes of Rhabdomyolysis 3. List 6 metabolic derangements associated with Rhabdomyolysis 4. List 5 causes
Chapter 119 Rhabdomyolysis Episode overview 1. List the pathophysiology of rhabdomyolysis 2. List 8 causes of Rhabdomyolysis 3. List 6 metabolic derangements associated with Rhabdomyolysis 4. List 5 causes
Hematology Unit Lab 1 Review Material
 Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS
 QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
CHRONIC KIDNEY DISEASE (CKD)
 CHRONIC KIDNEY DISEASE (CKD) CKD implies longstanding (more than 3 months), and usually progressive, impairment in renal function. In many instances, no effective means are available to reverse the primary
CHRONIC KIDNEY DISEASE (CKD) CKD implies longstanding (more than 3 months), and usually progressive, impairment in renal function. In many instances, no effective means are available to reverse the primary
