J Am Soc Nephrol 13: , 2002
|
|
|
- Dorothy Manning
- 5 years ago
- Views:
Transcription
1 J Am Soc Nephrol 13: , 2002 The Pharmacokinetic-Pharmacodynamic Relationship for Total and Free Mycophenolic Acid in Pediatric Renal Transplant Recipients: A Report of the German Study Group on Mycophenolate Mofetil Therapy LUTZ T. WEBER,* MARIA SHIPKOVA, VICTOR W. ARMSTRONG, NATALIE WAGNER,* EKKEHARD SCHÜTZ, OTTO MEHLS,* LOTHAR B. ZIMMERHACKL, MICHAEL OELLERICH, and BURKHARD TÖNSHOFF* *Division of Pediatric Nephrology, University Children s Hospital, Heidelberg, Germany; Department of Clinical Chemistry, Georg-August University, Göttingen, Germany; and University Children s Hospital Freiburg, Germany. Abstract. It is currently being debated whether pharmacokinetic monitoring of mycophenolic acid (MPA), the active constituent of mycophenolate mofetil (MMF), can optimize MMF therapy after organ transplantation. This open-label longitudinal study in pediatric renal transplant recipients was designed to investigate the pharmacokinetic (PK)/pharmacodynamic relationship of total and free MPA and to establish PK values for the assessment of an individual s MPA PK parameters. Fifty-four children, aged 2.2 to 17.8 yr, on an immunosuppressive triple regimen consisting of cyclosporin A, prednisone, and MMF (600 mg/m 2 body surface area twice daily) were investigated 1 wk and 3 wk (initial phase) and 3 mo and 6 mo (stable phase) after renal transplantation. MPA was measured by reverse phase HPLC, free MPA by HPLC after separation by ultrafiltration. There was an association between the risk of acute rejection episodes and MPA-AUC 0-12 values or MPA predose levels; by receiver operating characteristic analysis, an AUC 0-12 of 33.8 mg h/l in the initial phase posttransplant had a diagnostic sensitivity of 75% and a diagnostic specificity of 64% for discrimination of patients with acute rejections. The respective discrimination threshold for the MPA predose concentration was 1.2 mg/l with a sensitivity of 83% and a specificity of 64%. In contrast, high free, but not total, MPA-AUC 0-12 values were associated with an increased risk of the MMF-related side effects leukopenia and/or infections. These data indicate that therapeutic drug monitoring of MPA has the potential for optimization of MMF efficacy in this patient population by steering patients away from the low values of MPA PK variables that are associated with an increased rejection risk. For the assessment of the toxic risk of MMF regarding leukopenia and/or infections, measurement of free MPA appears to be more appropriate. Received March 21, Accepted September 14, Correspondence to: Dr. Burkhard Tönshoff, Division of Pediatric Nephrology, University Children s Hospital, Im Neuenheimer Feld 150, Heidelberg, Germany. Phone: ; Fax: ; Burkhard_Toenshoff@med.uni-heidelberg.de / Journal of the American Society of Nephrology Copyright 2002 by the American Society of Nephrology Three randomized, double-blinded, controlled trials in adult renal transplant recipients demonstrated that mycophenolate mofetil (MMF) is more effective than azathioprine or placebo in combination with cyclosporin A and corticosteroids for prevention of allograft rejection (1). MMF is now widely used for maintenance immunosuppressive therapy also in pediatric renal transplant recipients (2). However, data on the pharmacokinetics and pharmacodynamics of MMF in this patient population are still limited. MMF is rapidly metabolized in vivo to its active constituent, mycophenolic acid (MPA), a reversible, uncompetitive inhibitor of inosine monophosphate dehydrogenase (IMPDH). Inhibition of IMPDH-II in activated lymphocytes causes a reduction in intracellular guanine nucleotide pools and leads to an arrest of lymphocyte proliferation. MPA is extensively bound to albumin, with a range of protein binding of 97% to 99% in patients with normal renal and liver function (3 5). On the basis of in vitro investigations, free MPA concentrations are presumed to be responsible for its immunosuppressive action (4). The primary metabolite of MPA is the phenolic glucuronide 7 0 MPAG. Two further metabolites have been identified in humans, namely the acyl glucuronide (AcMPAG) and the phenolic glucoside of MPA (6). Of these three metabolites, only the acyl glucuronide is capable of inhibiting human IMPDH-II in vitro (7). The pharmacokinetics of MPA shows large interindividual and intraindividual variability. Pharmacokinetic monitoring of MPA with the aim of optimizing the dosage of this drug to achieve adequate immunosuppression with minimized risk of graft rejection or toxicity has therefore been under investigation (8). In adult renal transplant recipients on cyclosporine,
2 760 Journal of the American Society of Nephrology J Am Soc Nephrol 13: , 2002 MMF, and steroids, pharmacokinetic/pharmacodynamic (PK/ PD) relationships between MPA-AUC or predose MPA levels and the risk of acute rejection have been established on the basis of measurements by reverse-phase HPLC with ultraviolet detection (9,10). The interpretation of the PK/PD relationship of MPA in different patient populations can be influenced by several factors, such as the nature of the organ transplanted, the age of the patient, use of concomitant immunosuppressive therapy, protein binding, the presence of active metabolites, and the assay used. The purposes of this investigation were therefore (1) to establish the PK/PD relationships for total and free MPA in pediatric renal transplant recipients on an immunosuppressive regimen with cyclosporin A, MMF, and corticosteroids and (2) to establish the therapeutic ranges for MPA-AUC 0 12 values and predose MPA levels in this patient population. Materials and Methods Patients This study was an open-label longitudinal evaluation of the pharmacokinetic-pharmacodynamic relationship for total and free MPA in pediatric renal transplant recipients. The inclusion and exclusion criteria have been described in previous reports (5,11). The analysis of the clinical results of this study is being published elsewhere (12). The present analysis of the PK/PD relationship involved 54 patients (33 boys) with a median age of 11.7 yr (range, 2.2 to 17.8 yr). All patients were white. Forty-four of 54 children had primary transplant function, ten patients had delayed graft function defined as the requirement for dialysis in the first 3 wk posttransplant. No graft loss occurred in the delayed graft function group. Immunosuppressive therapy consisted of methylprednisolone (300 mg/m 2 body surface area [BSA]) on the day of transplant surgery which was then tapered to 60 mg/m 2 for the first, 30 mg/m 2 for the second, 15 mg/m 2 for the third, 12 mg/m 2 for the fourth, 9 mg/m 2 for the fifth, and 6 mg/m 2 for the sixth week after transplantation and 4 mg/m 2 thereafter. Cyclosporin A (microemulsion formulation) was administered in a dose of 500 mg/m 2 per day given in two divided doses for 24 h, starting 6 h after surgery. Thereafter, doses (approximately 300 mg/m 2 BSA per d) were adjusted to achieve 12-h trough levels of 150 to 250 ng/ml, as measured by whole blood monoclonal fluorescence polarization immunoassay (mfpia, Abbott, Chicago, IL), in the first 3 mo posttransplant; thereafter, 12-h trough levels of 100 to 200 ng/ml were targeted. The mean cyclosporine dose and the respective 12-h predose levels at the four pharmacokinetic sampling time points are listed in Table 1. Dosage of MMF MMF was administered orally in a dose of 600 mg/m 2 BSA twice a day up to a maximum of 2 g/d. This dose was based on a preliminary report of a dose-finding study in pediatric renal transplant recipients (13). If the dose could not be exactly administered by use of 250 mg capsules, MMF capsules were opened and the exact dose for each individual child was refilled into gelatin capsules comparable to those produced by the MMF manufacturer. BSA was calculated by the formula of Du Bois and Du Bois (14). Pharmacokinetic Protocol Patients were studied after informed (parental) consent was obtained. Blood samples for pharmacokinetic assessments were drawn on days 7 and 21 posttransplant (initial phase) and 3 and 6 mo posttransplant (stable phase). It was mandatory that all patients had at least 2 full days of the same MMF dose given twice a day before pharmacokinetic investigations. The study was performed under inpatient conditions, starting in the morning. Patients were required to fast from 10 p.m. the night before sampling until after the 75-min sample had been obtained on the following morning. Blood samples were collected at the following times: before dosing and 20 min, 40 min, 75 min, and 2, 4, 6, 8, and 12 h after dosing. The study protocol was approved by the local ethics committee of each contributing center. All blood samples were collected in tubes containing ethylenediaminetetraacetic acid as an anticoagulant. For determination of MPA, free MPA, and MPAG concentrations, plasma was separated and stored at 20 C until analysis. Measurement of Total and Free MPA and MPAG The procedure for the determination of total MPA and MPAG in plasma, as well as for the determination of the free concentration of MPA in plasma water has been described in detail elsewhere (5,15). The limit of quantification for free MPA (at 215 nm) was set at 10 g/l because the imprecision at the detection limit of 5 g/l was 20%. The within-day imprecision ranged from 6.5% (209.2 g/l) to 11.6% (18.4 g/l) and the between-days imprecision ranged from 7.2% (200.6 g/l) to 14.6% (22.8 g/l) for measurement of free MPA at 215 nm (19). Pharmacokinetic Analyses The following pharmacokinetic data for MPA, free MPA, and MPAG were determined: predose concentration (C 0 ), time to maximum concentration (t max [h]), maximum concentration (C max [mg/l]), area under the curve (AUC) from 0 to 12 h using the linear trapezoidal rule, and the evening predose (i.e., the 12-h) concentration (C 12 [mg/l]). An abbreviated three-point AUC based on the sampling times 0 min, 75 min, and 4 h (MPA-AUC 0,75 min,4 h ) was calculated according to a previously published algorithm (20): estimated AUC C C 75 min 3.9 C 4h, where C 0 is the predose MPA concentration, and C 75 min and C 4h are MPA concentrations 75 min and 4 h, respectively, after MMF dosing. In addition, a published algorithm based on an empiric equation using a limited sampling strategy up to 2 h postdose (MPA-AUC 0 2 ) was taken for the calculation of the full AUC (21). The pharmacokinetic analysis was performed using the computer program BiAS (Epsilon-Verlag Hochheim-Darmstadt, Germany). Acute Rejection Episodes The primary outcome criterion for the determination of the PK/PD relationship for MPA was the occurrence of acute rejection episodes over the 6-mo study period after transplantation. Fifteen of 54 patients experienced at least one acute rejection episode during the 6-mo study period; two of these patients had two rejection episodes, resulting in a total number of 17 acute rejection episodes. Twelve of 17 acute rejection episodes were biopsy-proven, and histologic examination and classification of a core biopsy was done according to the Banff criteria (16). If a biopsy was logistically impossible or clinically contraindicated, the diagnosis of presumed rejection was based on clinical judgment (supported by one or more of the following clinical findings: increased body temperature, graft swelling, graft tenderness, rise in serum creatinine level of more than 20% from the baseline level, or oliguria). The clinical diagnoses were made without any knowledge of the MPA concentration data. Acute rejection episodes were treated initially with high-dose intravenous corticosteroids (methylprednisolone, 400, 200, 200, and 100 mg/m 2 BSA on 4 con-
3 J Am Soc Nephrol 13: , 2002 PK/PD Relationship for MPA in Pediatric Renal Transplant Recipients 761 secutive days, respectively, or 300 mg/m 2 BSA for 3 to 5 d). If the rejection episode failed to respond to this therapy, treatment with OKT3 or antithymocyte globulin was started or patients were converted from cyclosporine to tacrolimus according to center practice. The acute rejection episodes occurred 27 d (range, 8 to 170 d) after renal transplantation; 14 of 17 rejections occurred within the first 70 d posttransplant. Adverse Event Monitoring Adverse events, defined as an abnormal change in physical signs, symptoms, or laboratory values whether or not deemed to be causally related with the study medication, were recorded throughout the study when reported by a patient or noted by an investigator. Thrombocytopenia was defined as a thrombocyte count /L. Leukopenia was defined as a granulocyte count 2000/ l and graded according to its severity: mild (1600 to 1999 granulocytes); moderate (1000 to 1599 granulocytes) (n 5); severe (500 to 999 granulocytes). Diarrhea was graded as follows: mild diarrhea (n 7), transient diarrhea 2 d; moderate diarrhea (n 3), tolerable diarrhea lasting 2 d; and severe diarrhea (n 1), intolerable diarrhea requiring therapy. Infections were classified as moderate when requiring specific antibiotic or antiviral therapy and as severe when requiring hospitalization. The following infections were recorded: herpes labialis (n 5), herpes zoster (n 1), oral mucocutaneous candidiasis (n 1), urinary tract infection (n 8), cytomegalovirus (CMV) pneumonia (n 1), CMV-colitis (n 1), bacterial septicemia (n 3), pneumonia (n 1), pharyngitis (n 1), febrile viral infection (n 4). Statistical Analyses The Shapiro-Wilks test was used to confirm normal distribution of data (17). Because some parameters were normally distributed and some were not, data in Table 1 and 2 are given as median (range). For comparison of more than two groups, one-way ANOVA on repeated measurements followed by all pairwise comparison (Student Newman-Keuls test) was used. Forward stepwise regression analysis was performed to assess which variables contribute independently to the prediction of MPA-AUC 0 12 values. Differences were considered to be statistically significant at a P Receiver operating characteristic (ROC) plots of sensitivity versus 1-specificity were generated to determine whether a particular pharmacokinetic variable could discriminate patients with an acute rejection from those who experienced no rejection. Areas under the ROC curves and the 95% confidence interval (CI) limits were calculated using the method of Hanley and McNeil (18). The ROC curve analysis was carried out with Analyze-It version 1.44 (Analyze-It Software, Leeds, UK). Results Pharmacokinetic Results In agreement with our previous finding, there was a large interindividual variation of PK data, despite the fact that all patients were receiving the same body surface adjusted MMF dosage (Table 2). For example, MPA-AUC 0 12 values at 3 mo posttransplant ranged from 28.6 to 139 mg h/l. The interindividual coefficient of variation was comparable in the initial (18%) and stable phase (22%) posttransplant. In an attempt to explain the variability in MPA-AUC 0 12 values, correlation analyses with clinical parameters were performed. At the PK sampling period 1 wk posttransplant, there were significant positive correlations between patient age, serum albumin, GFR, and the MPA-AUC 0 12 values (Table 3). However, none of these correlations remained significant at the three later PK sampling periods (Table 3). Because of the multiple interrelations between age, serum albumin, and GFR, forward stepwise regression analysis was performed to further assess which variables contribute independently to the prediction of MPA- AUC MPA-AUC 0 12 at 1 wk posttransplant could be predicted from a linear combination of the independent variables age, GFR, and serum albumin (r 0.73; P ). Patients with MPA-AUC 0 12 levels at 1 wk posttransplant below the median of 36 mg h/l tended to be younger ( versus yr; P 0.067) and had significantly lower serum albumin levels ( versus g/l; P 0.03) and significantly lower GFR ( versus ml/min per 1.73 m 2 ; P 0.05) than those with MPA- AUC 0 12 above 36 mg h/l. Hence, in the first week posttransplant, but not at later PK sampling periods, low MPA- AUC 0 12 values were associated with young age, low serum albumin levels, and decreased renal transplant function. Whereas the PK parameters at 1 wk and 3 wk posttransplant were not significantly different, there was an increase of the PK parameters C 0 (132%), C 12 (79%), and AUC 0 12 (89%) between the 3-wk and the 3-mo sampling period (Table 2). There was no further statistically significant increase of MPA PK parameters between the 3-mo and 6-mo sampling period, in agreement with our previous report in a smaller cohort of patients (11). In contrast to total MPA-AUC 0 12, the AUC 0 12 of free MPA did not change over time (Table 2), as reported previously (11). Because a full MPA-AUC requires at least 8 blood samples during a 12-h dose interval and is therefore impractical in Table 1. Cyclosporine dose and whole blood predose levels in 54 pediatric renal transplant recipients at the four pharmacokinetic sampling periods posttransplant a Cyclosporine A Pharmacokinetic Sampling Period 1wk 3wk 3mo 6mo Dose (mg/kg per d) 7.85 (3.13 to 17.7) 6.98 (3.81 to 20.7) 5.90 (2.65 to 13.4) 5.70 (3.06 to 13.8) Predose level (ng/ml) 185 (31 to 452) 193 (126 to 306) 172 (73 to 258) 144 (85 to 199) a Data are median (range).
4 762 Journal of the American Society of Nephrology J Am Soc Nephrol 13: , 2002 Table 2. Comparison of the pharmacokinetic (PK) parameters for MPA and free MPA at the four PK sampling periods posttransplant in 54 pediatric renal transplant recipients a Parameter 1wk 3wk 3mo 6mo MPA Free MPA MPA Free MPA MPA Free MPA MPA Free MPA C (mg/l) 1.06 a 0.01 c 0.97 a 0.01 c 2.25 b 0.02 c 2.92 b 0.02 c 0 (0.11 to 4.13) ( 0.01 to 0.09) (0.06 to 15.6) ( 0.01 to 0.15) (0.35 to 11.2) ( 0.01 to 0.17) (0.18 to 12.6) ( 0.01 to 0.11) 12 C (mg/l) 0.92 a 0.01 c 0.92 a 0.01 c 1.65 a 0.01 c 2.31 b 0.02 c (0.11 to 6.96) ( 0.01 to 0.11) (0.00 to 13.2) ( 0.01 to 0.10) (0.28 to 6.89) ( 0.01 to 0.10) (0.25 to 12.2) ( 0.01 to 0.22) max C (mg/l) 9.95 a 0.17 c 15.3 a 0.20 c 24.9 b 0.23 c 26.0 b 0.21 c (1.50 to 42.3) (0.03 to 0.61) (3.53 to 45.7) (0.03 to 0.65) (7.20 to 53.5) (0.08 to 0.61) (9.40 to 52.5) (0.07 to 0.57) 0 12 AUC 36.0 a 0.41 c 33.6 a 0.41 c 63.5 b 0.49 c 65.7 b 0.51 c (3.12 to 95.0) (0.07 to 1.58) (12.8 to 89.1) (0.13 to 1.19) (28.6 to 139) (0.17 to 1.40) (21.3 to 117) (0.18 to 1.34) a Data are median (range). Values sharing common superscripts are not significantly different, whereas values without common superscripts are significantly different (P 0.05). Table 3. Patient age, serum albumin levels, and GFR at the four PK sampling periods posttransplant in 54 pediatric renal transplant recipients and the coefficients of correlation of these parameters with the respective MPA-AUC 0 12 values a Parameter 1wk 3wk 3mo 6mo Mean SE (Range) Correlation Mean SE (Range) Correlation Mean SE (Range) Correlation Mean SE (Range) Correlation Age (yr) r r r r 0.03 (3.17 to 16.0) P (3.17 to 16.0) P 0.45 (3.42 to 16.3) P 0.73 (3.67 to 16.5) P 0.86 Albumin (g/l) r r r r 0.31 (24.0 to 51.0) P (27.0 to 53.0) P 0.59 (23.0 to 47.0) P (36.0 to 47.0) P 0.11 GFR (ml/min per r r r r m 2 ) (9.0 to 133) P 0.04 (14.0 to 143) P 0.48 (39.0 to 139) P 0.09 (45.0 to 123) P 0.12 a Data are mean SE (range).
5 J Am Soc Nephrol 13: , 2002 PK/PD Relationship for MPA in Pediatric Renal Transplant Recipients 763 clinical routine practice, we investigated whether a single time point MPA concentration or an abbreviated AUC derived from a limited number of samples correlate with the full MPA-AUC. Only a moderate correlation was observed between either the predose MPA trough concentration (C 0 ) or the 12-h evening trough concentration (C 12 ) and the full MPA-AUC 0 12.Although the C 0 concentration may have been taken after a more variable time interval subsequent to the previous dose than the C 12 concentration that was sampled exactly 12 h after a supervised dose, the correlation of C 12 with the full AUC was not superior to that of C 0 (Table 4). There was also only a moderate correlation between the MPA peak concentration (C max ) and the respective MPA-AUC 0 12 (Table 4). Because MPA C max increases during the first 3 mo posttransplant more markedly than the MPA predose concentrations (Table 2), the coefficients of correlation of MPA C max with the respective full AUC in the stable phase posttransplant were higher and the coefficients of correlation of MPA predose levels were lower than in the initial phase posttransplant. The abbreviated MPA- AUC 0,75 min,4 h gave a reasonable correlation with the full AUC that was somewhat superior to that seen between the abbreviated profile MPA-AUC 0 2 and the full AUC (Table 4). To provide the context for an assessment of an individual s PK parameter in relation to the pediatric population distribution, 5 th to 95 th percentiles for MPA-AUC 0 12 and predose (C 12 ) levels were calculated (Figure 1). PK/PD Analyses Regarding Acute Rejections There were 17 acute rejection episodes in 54 patients during the 6-mo study period. Figure 1 shows the MPA-AUC 0 12 and MPA-C 12 values of the rejectors in relation to the respective percentiles of the whole study population; in the initial phase posttransplant, both the AUC 0 12 and MPA-C 12 values were distributed in the lower PK percentiles (Figure 1). Ten of fourteen patients with rejections in the initial phase posttransplant had MPA-AUC values below 33.8 mg h/l, before they experienced an acute rejection episode. The comparison to those patients who neither suffered from an acute rejection nor an adverse event yielded a relative risk of acute rejection of 41% with total MPA-AUC 0 12 values being below 33.8 mg h/l compared with 14% with total MPA-AUC values being above 33.8 mg h/l. The cyclosporine dose (rejectors, 7.5 [4.2 to 13] mg/kg per d; nonrejectors, 8.0 [3.1 to 14] mg/kg per d), and the 12-h predose whole blood levels (rejectors, 187 [76 to 330] mg/l; nonrejectors, 190 [88 to 331] mg/l) were not significantly different between the two groups (data are median [range] of the respective mean data calculated from the PK sampling time points at 1 wk and 3 wk posttransplant). To establish which pharmacokinetic parameter is the best predictor for the risk of acute rejection, ROC curves were computed for each of the four PK parameters. For these calculations, the mean values from the 1-wk and 3-wk sampling time points were taken for each variable and patient. Diagnostic sensitivities (true positive) were calculated for each individual PK value as the fraction of those patients with an acute rejection who had a value below this discrimination threshold. The corresponding diagnostic specificities (false negatives) were calculated as the fraction of patients with no rejection episode who had a value below this decision value. The ROC plots of sensitivity versus 1-specificity for the PK variables AUC 0 12 and C 12 are shown in Figure 2, and the statistical comparison of the areas under the ROC curves is given in Table 5. C 12, AUC 0 12, and the two abbreviated AUC estimations were able to discriminate patients with acute rejections from patients with no rejection. An AUC 0 12 of 33.8 mg h/l had a diagnostic sensitivity of 75.0% and a diagnostic specificity of 64.3%. For the PK parameter C 12, a concentration of 1.2 mg/l gave a sensitivity of 83.3% and a specificity of 64.3%. In contrast, the PK variables derived from the measurements of free MPA were not effective for the discrimination of rejectors from nonrejectors (Table 5). PK/PD Analyses Regarding Adverse Events High free MPA-AUC 0 12 values were associated with an increased risk of certain MMF-related side effects. Free MPA- AUC 0 12 values of patients with infections and/or leukopenia Table 4. Correlation of the MPA PK parameters, C 0,C 12, and C max, and the abbreviated profiles, MPA-AUC 0,75min,4h and MPA-AUC 0 2, with the full-time MPA-AUC 0 12 at the four PK sampling periods posttransplant in 54 pediatric renal transplant recipients PK Parameter 1 wk 3 wk 3 mo 6 mo Entire Study Period MPA C 0 r 0.65 r 0.70 r 0.59 r 0.50 r 0.64 P P P P 0.01 P MPA C 12 r 0.69 r 0.56 r 0.49 r 0.47 r 0.52 P P P 0.01 P 0.01 P MPA-C max r 0.53 r 0.52 r 0.68 r 0.64 r 0.71 P P P P P MPA-AUC 0,75min,4h r 0.89 r 0.86 r 0.80 r 0.85 r 0.90 P P P P P MPA-AUC 0 2 r 0.82 r 0.86 r 0.77 r 0.77 r 0.85 P P P P P
6 764 Journal of the American Society of Nephrology J Am Soc Nephrol 13: , 2002 Figure 1. Time course of MPA-AUC 0 12 (A) and predose (C 12 ) plasma levels (B) derived from HPLC measurements in the first 6 mo after grafting in pediatric renal transplant recipients; data are the median and the 5 to 95% centiles of the total patient population (n 54). All patients had received the full MMF dose of 600 mg/m 2 body surface area (BSA) twice daily for at least 2 d before PK sampling. ( ) Episode of an acute rejection. The respective acute rejection episodes are graphically assigned to the nearest PK sampling period preceding the clinical event. The median time period between an acute rejection episode and the preceding PK sampling period was 10 d (range, 0 to 90 d). Table 5. Areas under the receiver operating characteristic (ROC) curves for pharmacokinetic parameters of total and free MPA to discriminate between patients with (n 12) or without an acute rejection episode during the first 70 d posttransplant PK Parameter Area Under the ROC Curve 95% Confidence Interval P MPA C 0 (mg/l) to MPA C 12 (mg/l) to MPA C max (mg/l) to MPA-AUC to MPA-AUC 0,75min,4h to MPA-AUC to Free MPA C 0 (mg/l) to Free MPA C 12 (mg/l) to Free MPA C max (mg/l) to Free MPA-AUC to Figure 2. Receiver operating characteristic (ROC) curves illustrating the ability of the pharmacokinetic variables MPA-AUC 0 12 ( ) and predose (C 12 ) concentration ( ) to discriminate between patients with (n 12) and without (n 42) an acute rejection episode during the first 70 d posttransplant. The broken line represents the theoretical ROC curve for no discrimination between the two groups. were distributed in the upper PK centiles (Figure 3). The ROC plot of sensitivity versus 1-specificity for the PK variables free MPA-AUC 0 12 and C max is shown in Figure 4, and the statistical comparison of the areas under the ROC curves is given in Table 6 (initial phase) and Table 7 (stable phase posttransplant). Free MPA-AUC 0 12 and free MPA-C max were better able to discriminate patients with infections and/or leukopenia from those without these complications. The decision level in the initial phase after renal transplantation above which there is an enhanced risk of leukopenia and/or infections in the initial phase posttransplant was a free MPA-AUC 0 12 of 0.4 mg h/l with a diagnostic sensitivity of 92.3% and a diagnostic specificity of 61.0%. In contrast, PK variables of total MPA were discriminatory for these side effects in neither the initial (Table 6) nor the stable phase posttransplant (Table 7). There was also no association between the incidence of diarrhea or thrombocytopenia and any of the PK parameters derived from measurements of total or free MPA (results not shown).
7 J Am Soc Nephrol 13: , 2002 PK/PD Relationship for MPA in Pediatric Renal Transplant Recipients 765 Table 6. Areas under the ROC curves for pharmacokinetic parameters of total and free MPA to discriminate between patients with or without adverse events of infections (n 18) and/or leukopenia (n 2) during the first 70 d posttransplant PK Parameter Area Under the ROC Curve 95% Confidence Interval P Figure 3. Time course of free MPA-AUC 0 12 values in the first 6 mo after grafting in pediatric renal transplant recipients; data are the median and the 5 to 95% centiles of the total patient population (n 54). All patients had received the full MMF dose of 600 mg/m 2 BSA twice daily for at least 2 d before PK sampling. Moderate ( ) or severe ( ) adverse events of leukopenia and/or infection are indicated accordingly. The respective adverse events are graphically assigned to the nearest PK sampling period preceding the event. The median time period between an adverse event and the preceding PK sampling period was 14 d (range, 0 to 38 d). MPA C 0 (mg/l) to MPA C 12 (mg/l) to MPA C max (mg/l) to MPA-AUC to MPA-AUC 0,75min,4h to MPA-AUC to Free MPA C 0 (mg/l) to Free MPA C 12 (mg/l) to Free MPA C max (mg/l) to Free MPA-AUC to Table 7. Areas under the ROC curves for pharmacokinetic parameters of total and free MPA to discriminate between patients with or without adverse events of infections (n 9) and/or leukopenia (n 3) in the stable phase posttransplant PK Parameter Area Under the ROC Curve 95% Confidence Interval P MPA C 0 (mg/l) to MPA C 12 (mg/l) to MPA C max (mg/l) to MPA-AUC to MPA-AUC 0,75min,4h to MPA-AUC to Free MPA C 0 (mg/l) to Free MPA C 12 (mg/l) to Free MPA C max (mg/l) to Free MPA-AUC to Figure 4. Receiver operating characteristic curves illustrating the ability of the pharmacokinetic variables free MPA-AUC 0 12 ( ) and C max concentration (}) to discriminate between patients with (n 13) and without (n 41) adverse events of leukopenia (n 3) and/or infection (n 10) during the first 70 d posttransplant. The broken line represents the theoretical ROC curve for no discrimination between the two groups. Discussion This is the first study that investigated the PK/PD relationship for MMF in immunosuppressive therapy in pediatric renal transplant recipients and the first that establishes the role for measurement of free MPA for the assessment of the toxic risk of MMF therapy. We have shown that both MPA-AUC 0 12 and predose MPA levels are significantly associated with the risk of acute rejection in this patient population. By ROC analysis, an AUC 0 12 of 33.8 mg h/l in the initial phase posttransplant had a diagnostic sensitivity of 75% and a diagnostic specificity of 64% for discrimination of patients with acute rejections. The respective discrimination threshold for the
8 766 Journal of the American Society of Nephrology J Am Soc Nephrol 13: , 2002 MPA predose concentration was 1.2 mg/l with a sensitivity of 83% and a specificity of 64%. The incidence of the MMF-related adverse events, diarrhea, vomiting, or abdominal pain, was not associated with MPA PK variables, which is consistent with previous findings in adult renal transplant recipients (10). These adverse events might also reflect local effects of MMF in the gastrointestinal system and not only systemic exposure. The adverse events, leukopenia and/or infections, were also not associated with any of the PK variables derived from total MPA measurements but with the AUC 0 12 of free MPA. Most of these adverse events were associated with free MPA-AUC 0 12 levels 0.4 mg h/l (Figure 3). MPA is extensively bound to albumin, with a range of protein binding of 97% to 99% in patients with normal renal and liver function (3 5). Factors that alter protein binding can affect the relationship between total concentration and free concentration. The pharmacologically inactive phenolic glucuronide metabolite of MPA, MPAG, competes for the albumin binding sites and can increase the fraction of unbound active MPA when present at high concentrations, for example as a consequence of renal failure (5,19). The presence of hyperbilirubinemia, uremia, low ph, and low albumin concentrations also can decrease MPA binding (3 5,19). For this reason, under circumstances of perturbed binding, the interpretation of total MPA plasma concentrations must take into account the altered MPA binding. This observation of an increased toxic risk of MMF therapy in patients with hypoalbuminemia and/or reduced renal function is clinically important, because MMF is increasingly used for immunosuppressive therapy in patients with chronic glomerulonephritis and the nephrotic syndrome (22). In this context, it is of interest to note that Kaplan et al. (23) reported a case of severe leukopenia that was associated with renal insufficiency in a pancreas/renal transplant recipient receiving 0.75 g of MMF twice daily. In this case, the free MPA-AUC 0 12 was substantially elevated (5.1 mg h/l) and the total MPA-AUC 0 12 was in the range observed for stable renal transplant recipients. The apparent discrepancy that the AUC 0 12 of total MPA was associated with the incidence of acute rejection episodes, whereas the AUC 0 12 of free MPA was associated with side effects reflecting the systemic exposure to MMF deserves comment. It is possible that a low protein binding of MPA favors its access from the circulation to the bone marrow, where it induces leukopenia by inhibition of leukocyte maturation from precursor cells, whereas inhibition of proliferation of circulating lymphocytes is mainly responsible for its immunosuppressive effect. A recent preliminary report in stable kidney transplant recipients has confirmed the relation between free MPA levels and the incidence of leukopenia (24). In agreement with our previous reports in smaller cohorts of patients (5,11), there was a large interindividual variation of PK data (Table 2). In the first week posttransplant, but not at later PK sampling periods, low MPA-AUC 0 12 values were associated with young age, low serum albumin, and decreased transplant function. This transient association between impaired renal function and low MPA-AUC 0 12 values in the initial but not stable phase posttransplant has recently been reported in adult renal transplant recipients (25). Patients with decreased renal function have an increased MPA free fraction because the accumulation of the renal metabolite MPAG competes with MPA for binding sites on albumin (5,26,27). Hence, the most likely explanation for the association between low MPA-AUC 0 12 values and impaired renal function is that decreased protein binding in these patients leads to an enhanced MPA metabolism, because it is the free drug that is primarily available for metabolism and excretion. Other possible causes of the interindividual variability of MPA-AUC 0 12 values include differences in the absorption of MMF and/or in the metabolism via the glucuronidation pathway. Our study has demonstrated a significant relationship between both MPA-AUC 0 12 and predose MPA levels and the risk of acute rejection. This observation provides some encouragement that therapeutic drug monitoring with individualized dosing of MMF could optimize the usage of this immunosuppressive drug. There are additional lines of evidence that favor such a monitoring. First, MPA displays highly variable interindividual pharmacokinetics; in the initial phase posttransplant, there is also considerable intraindividual PK variability (3,5,8,11). Second, there is a time-dependent increase in MPA- AUC 0 12 in both adult and pediatric renal transplant recipients on concomitant immunosuppression with cyclosporin A and corticosteroids (8,11) that might require time-dependent dose adjustments of MMF. Third, the pharmacokinetics of MPA is also dependent on the concomitant immunosuppression (28). However, it has to be emphasized that the value of therapeutic drug monitoring of MPA has not been formally tested yet. Only a prospective trial in which kidney transplant recipients treated with the same triple regimen are randomized for treatment with a fixed dose of MMF versus treatment with an MMF dose adjusted to the results of plasma concentration monitoring could establish the scientific basis of therapeutic drug monitoring of MPA. Such rigorous criteria are required to justify the additional effort and expense involved, before a general therapeutic drug monitoring of MPA can be recommended. Moreover, attempts to define the PK/PD relationship for gastrointestinal disturbances have not been successful, which is consistent with the results in this study. Instead, the dose of MMF provides the most predictive information for adverse events such as diarrhea (10), presumably because of the local toxicity of MPA on the gastrointestinal epithelium. However, given the association between MPA PK variables and the risk of acute rejection, therapeutic drug monitoring of MPA in the initial phase posttransplant could be helpful in selected highrisk patients. It would be reasonable to aim at achieving MPA- AUC values or predose MPA levels somewhat higher than those achieved in the lower percentiles by individual adjustment of the MMF dose. For such an approach, the patientspecific and immunosuppressive regimen specific percentiles for MPA-AUC and MPA predose levels from this study could serve as a guideline for optimization of MMF therapy in pediatric renal transplant recipients. On the basis of data from this and other studies, a consensus is arising that for minimizing the risk of rejection after transplantation, total MPA-AUC values in the early stages posttransplant should be maintained
9 J Am Soc Nephrol 13: , 2002 PK/PD Relationship for MPA in Pediatric Renal Transplant Recipients 767 within the therapeutic window of 30 to 60 mg h/l, based on HPLC data, or the predose concentration in the range of 1 to 3.5 mg/l. Because some fluctuations are to be expected as a consequence of the enterohepatic circulation of MPA, extreme values or a large change should be verified by repeat measurement before a change in the MMF dose is undertaken. The question arises of which PK parameter of total and free MPA is best suited for therapeutic drug monitoring of MMF therapy in clinical practice. In this study, the parameters MPA- AUC 0 12, MPA-AUC 0,75 min,4 h, and MPA C 12 were comparable for assessing the risk of acute rejection episodes, whereas MPA C 0 and MPA-AUC 0 2 had a somewhat poorer predictive value (Table 5). In two previous studies in adult renal transplant recipients, the MPA-AUC was a better predictor of outcome than the predose concentration (21,29). Predose levels are more convenient than measurements of AUC that are complex and increase the cost of routine clinical monitoring. However, the predose C 12, i.e., the concentration measured 12 h after a supervised dose, is not the predose sample commonly collected in a clinic. This is the C 0 predose concentration, which may be sampled at a more variable time interval after the last dose. Hence, the calculation of AUC using a three-point limited sampling strategy up to 4 h after MMF dosing (MPA-AUC 0,75 min,4 h ) appears to be a more precise approach for the assessment of the risk of acute rejection than the predose C 0 level. In conclusion, we have observed an association between the risk of acute rejection episodes and MPA-AUC values or MPA predose levels in pediatric renal transplant recipients on an immunosuppressive triple drug therapy with cyclosporin A, MMF, and corticosteroids. We have established 5 th to 95 th percentiles for these PK parameters on the basis of HPLC measurements in this specific patient population. These reference data could facilitate the therapeutic drug monitoring of MPA for optimization of MMF efficacy by steering patients away from the extreme values of MPA PK variables indicated by the lower percentiles. For the assessment of the toxic risk of MMF regarding leukopenia and/or infections, measurement of free MPA appears to be more appropriate. Acknowledgments We thank the following contributing clinical investigators (in alphabetical order of the centers): Michael Böswald, Wolfgang Rascher (Erlangen), Monika Schröder, Jürgen Dippell (Frankfurt), Lothar B. Zimmerhackl, Astrid Staskewitz, Matthias Brandis, (Freiburg), Lutz Weber, Natalie Wagner, Burkhard Tönshoff (Heidelberg, coordinators), Ulrike John, Ludwig Patzer, Joachim Misselwitz (Jena), Uwe Querfeld (Köln), Christel Greiner, Hertha Eichstätt, (Leipzig), Günter Klaus, Hannsjörg W. Seyberth (Marburg), Bernd Klare (München), Monika Bulla, Eberhard Kuwertz-Bröking (Münster), Martin Holder, Heinz E. Leichter (Stuttgart). This study was supported by a research grant from Hoffmann-La Roche AG, Grenzach-Wyhlen, Germany. We also thank Tanja Schneider and Christa Scholz for their excellent technical assistance. References 1. Mele TS, Halloran PF: The use of mycophenolate mofetil in transplant recipients. Immunopharmacology 47: , Benfield MR, Stablein D, Tejani A: Trends in immunosuppressive therapy: a report of the North American Pediatric Renal Transplant Cooperative Study (NAPRTCS). Pediatr Transplant 3: 27 32, Bullingham RES, Nicholls A, Hale M: Pharmacokinetics of mycophenolate mofetil (RS 61443). A short review. Transplant Proc 28: , Nowak J, Shaw LM: Mycophenolic acid binding to human serum albumin: Characterization and relation to pharmacodynamics. Clin Chem 41: , Weber LT, Shipkova M, Lamersdorf T, Niedmann PD, Wiesel M, Mandelbaum A, Zimmerhackl LB, Schütz E, Mehls O, Oellerich M, Armstrong VW, Tönshoff B: Pharmacokinetics of mycophenolic acid (MPA) and determinants of MPA free fraction in pediatric and adult renal transplant recipients. JAmSoc Nephrol 9: , Shipkova M, Armstrong VW, Wieland E, Niedmann PD, Schutz E, Brenner-Weiss G, Voihsel M, Braun F, Oellerich M: Identification of glucoside and carboxyl-linked glucuronide conjugates of mycophenolic acid in plasma of transplant recipients treated with mycophenolate mofetil. Br J Pharmaco 126: , Schütz E, Shipkova M, Armstrong VW, Wieland E, Oellerich M: Identification of a pharmacologically active metabolite of mycophenolic acid in plasma of transplant recipients treated with mycophenolate mofetil. Clin Chem 45: , Shaw LM, Nicholls A, Hale M, Armstrong VW, Oellerich M, Yatscoff R, Morris RE, Holt DW, Venkataramanan R, Haley J, Halloran P, Ettenger R, Keown P, Morris RG: Therapeutic monitoring of mycophenolic acid. A consensus panel report. Clin Biochem 31: , Hale MD, Nicholls AJ, Bullingham RE, Hene R, Hoitsma A, Squifflet JP, Weimar W, Vanrenterghem Y, Van de Woude FJ, Verpooten GA: The pharmacokinetic-pharmacodynamic relationship for mycophenolate mofetil in renal transplantation. Clin Pharmacol Ther 64: , van Gelder T, Hilbrands LB, Vanrenterghem Y, Weimar W, de Fijter JW, Squifflet JP, Hene RJ, Verpooten GA, Navarro MT, Hale MD, Nicholls AJ: A randomized double-blind, multicenter plasma concentration controlled study of the safety and efficacy of oral mycophenolate mofetil for the prevention of acute rejection after kidney transplantation. Transplantation 68: , Weber LT, Lamersdorf T, Shipkova M, Niedmann PD, Wiesel M, Zimmerhackl LB, Staskewitz A, Schutz E, Mehls O, Oellerich M, Armstrong VW, Tönshoff B: Area under the plasma concentration-time curve for total, but not for free, mycophenolic acid increases in the stable phase after renal transplantation: a longitudinal study in pediatric patients. German Study Group on Mycophenolate Mofetil Therapy in Pediatric Renal Transplant Recipients. Ther Drug Monit 2: , Staskewitz A, Kirste G, Tönshoff B, Weber LT, Böswald M, Burghard R, Helmchen U, Brandis M, Zimmerhackl LB: Mycophenolate mofetil in pediatric renal transplantation without induction therapy: Results after 12 months of treatment. Transplantation 71: , Ettenger RB, Warshaw B, Mentser M, Potter D, Moulton L, Marik J, Cohen A, Nast C, Gales B, Nichols A, Hale M, Linna J: Mycophenolate mofetil (MMF) in pediatric renal transplantation [abstract]. Pediatric Nephrology 10: C39, 1996
10 768 Journal of the American Society of Nephrology J Am Soc Nephrol 13: , DuBois D, DuBois EF: A formula to estimate the approximate surface area if height and weight be known. Arch Intern Med 17: , Shipkova M, Niedmann PD, Armstrong VW, Schutz E, Wieland E, Shaw LM, Oellerich M: Simultaneous determination of mycophenolic acid and its glucuronide in human plasma using a simple high-performance liquid chromatography procedure. Clin Chem 44: , Solez K, Axelsen RA, Benediktsson H, Burdick JF, Cohen AH, Colvin RB, Croker BP, Droz D, Dunnill MS, Halloran PF: International standardization of criteria for the histologic diagnosis of renal allograft rejection: The Banff working classification of kidney transplant pathology. Kidney Int 44: , Zar JH: Biostatistical Analysis. Englewood Cliffs, NJ, Prentice Hall, Hanley JA, McNeil BJ: A method of comparing the areas under receiver operating characteristic curves derived from the same cases. Radiology 148: , Kaplan B, Meier-Kriesche HU, Friedman G, Mulgaonkar S, Gruber S, Korecka M, Brayman KL, Shaw LM: The effect of renal insufficiency on mycophenolic acid protein binding. J Clin Pharmacol 39: , Oellerich M, Shipkova M, Schutz E, Wieland E, Weber L, Tönshoff B, Armstrong VW: Pharmacokinetic and metabolic investigations of mycophenolic acid in pediatric patients after renal transplantation: implications for therapeutic drug monitoring. German Study Group on Mycophenolate Mofetil Therapy in Pediatric Renal Transplant Recipients. Ther Drug Monit 22: 20 26, Hale MD, Nicholls AJ, Bullingham RE, Hene R, Hoitsma A, Squifflet JP, Weimar W, Vanrenterghem Y, Van de Woude FJ, Verpooten GA: The pharmacokinetic-pharmacodynamic relationship for mycophenolate mofetil in renal transplantation. Clin Pharmacol Ther 64: , Briggs WA, Choi MJ, Scheel PJ: Successful mycophenolate mofetil treatment of glomerular disease. Am J Kidney Dis 31: , Kaplan B, Gruber SA, Nallamathou R, Katz SM, Shaw LM: Decreased protein binding of mycophenolic acid associated with leukopenia in a pancreas transplant recipient with renal failure. Transplantation 65: , Perico N, Gotti E, Remuzzi G, Gaspari F: Pharmacokinetic and trough concentrations help optimize mycophenolate dosing in kidney transplant patients [abstract]. J Am Soc Nephrol 11: 682, Shaw LM, Korecka M, Aradhye S, Grossman R, Bayer L, Innes C, Cucciara A, Barker C, Naji A, Nicholls A, Brayman K: Mycophenolic acid area under the curve values in African American and Caucasian renal transplant patients are comparable. J Clin Pharmacol 40: , Shaw LM, Mick R, Nowak I, Korecka M: Pharmacokinetics of mycophenolic acid in renal transplant patients with delayed graft function. J Clin Pharmacol 38: , Kaplan B, Meier-Kriesche HU, Friedman G, Mulgaonkar S, Gruber S, Korecka M, Brayman KL, Shaw LM: The effect of renal insufficiency on mycophenolic acid protein binding. J Clin Pharmacol 39: , Gregoor PJ, de Sevaux RG, Hene RJ, Hesse CJ, Hilbrands LB, Vos P, van Gelder T, Hoitsma AJ, Weimar W: Effect of cyclosporine on mycophenolic acid trough levels in kidney transplant recipients. Transplantation 68: , Takahashi K, Ochiai T, Uchida K, Yasumura T, Ishibashi M, Suzuki S, Otsubo O, Isono K, Takagi H, Oka T, et al: Pilot study of mycophenolate mofetil (RS-61443) in the prevention of acute rejection following renal transplantation in Japanese patients. RS Investigation Committee Japan. Transplant Proc 27: , 1995
Lothar Bernd Zimmerhackl
 What works in current paediatric practice of off-label dose adjustment of adult doses? Lothar Bernd Zimmerhackl Medical University Innsbruck Austria AGAH Workshop: Pediatric Investigation Plan. Bonn 13-14.1.
What works in current paediatric practice of off-label dose adjustment of adult doses? Lothar Bernd Zimmerhackl Medical University Innsbruck Austria AGAH Workshop: Pediatric Investigation Plan. Bonn 13-14.1.
Mycophenolate mofetil (MMF) has become the single
 Diagnostic & Therapeutic Corner Therapeutic Monitoring of Mycophenolate Mofetil Hyunyoung Jeong* and Bruce Kaplan *Department of Pharmacy Practice and Department of Medicine, University of Illinois at
Diagnostic & Therapeutic Corner Therapeutic Monitoring of Mycophenolate Mofetil Hyunyoung Jeong* and Bruce Kaplan *Department of Pharmacy Practice and Department of Medicine, University of Illinois at
Mycophenolate mofetil (MMF) is a purine analogue. Mycophenolic Acid Pharmacokinetics in Pediatric Liver Transplant Recipients
 Mycophenolic Acid Pharmacokinetics in Pediatric Liver Transplant Recipients Marion M. Aw, Nigel W. Brown, Toshi Itsuka, Christopher E. Gonde, Jemimah E. Adams, Nigel D. Heaton, J. Michael Tredger, Giorgina
Mycophenolic Acid Pharmacokinetics in Pediatric Liver Transplant Recipients Marion M. Aw, Nigel W. Brown, Toshi Itsuka, Christopher E. Gonde, Jemimah E. Adams, Nigel D. Heaton, J. Michael Tredger, Giorgina
Original Article. This PDF is available for free download from a site hosted by Medknow Publications. (
 Original Article www.jpgmonline.com A six-hour extrapolated sampling strategy for monitoring mycophenolic acid in renal transplant patients in the Indian subcontinent Fleming DH, Mathew BS, John GT*, Chandy
Original Article www.jpgmonline.com A six-hour extrapolated sampling strategy for monitoring mycophenolic acid in renal transplant patients in the Indian subcontinent Fleming DH, Mathew BS, John GT*, Chandy
Mycophenolate mofetil (MMF) is an immunosuppressive
 Explaining Variability in Mycophenolic Acid Exposure to Optimize Mycophenolate Mofetil Dosing: A Population Pharmacokinetic Meta-Analysis of Mycophenolic Acid in Renal Transplant Recipients Reinier M.
Explaining Variability in Mycophenolic Acid Exposure to Optimize Mycophenolate Mofetil Dosing: A Population Pharmacokinetic Meta-Analysis of Mycophenolic Acid in Renal Transplant Recipients Reinier M.
Mycophenolic acid (MPA) is the active immunosuppressant
 Monitoring Mycophenolate in Liver Transplant Recipients: Toward a Therapeutic Range John Michael Tredger, 1 Nigel William Brown, 1 Jemimah Adams, 1 Chris Elton Gonde, 1 Anil Dhawan, 2 Mohamed Rela, 3 and
Monitoring Mycophenolate in Liver Transplant Recipients: Toward a Therapeutic Range John Michael Tredger, 1 Nigel William Brown, 1 Jemimah Adams, 1 Chris Elton Gonde, 1 Anil Dhawan, 2 Mohamed Rela, 3 and
Mycophenolate Blood Level Monitoring: Recent Progress
 American Journal of Transplantation 2009; 9: 1495 1499 Wiley Periodicals Inc. Minireview C 2009 The Author Journal compilation C 2009 The American Society of Transplantation and the American Society of
American Journal of Transplantation 2009; 9: 1495 1499 Wiley Periodicals Inc. Minireview C 2009 The Author Journal compilation C 2009 The American Society of Transplantation and the American Society of
Proton Pump Inhibitors do not Interact with the Immunosuppressant Enteric-Coated Mycophenolate Sodium
 Proton Pump Inhibitors do not Interact with the Immunosuppressant Enteric-Coated Mycophenolate Sodium S. Kofler, C. Wolf, Z. Sisic, J. Behr, M. Vogeser, M. Shipkova, B. Meiser, G. Steinbeck, B. Reichart,
Proton Pump Inhibitors do not Interact with the Immunosuppressant Enteric-Coated Mycophenolate Sodium S. Kofler, C. Wolf, Z. Sisic, J. Behr, M. Vogeser, M. Shipkova, B. Meiser, G. Steinbeck, B. Reichart,
British Journal of Clinical Pharmacology
 British Journal of Clinical Pharmacology DOI:1.1111/j.1365-2125.29.3612.x Pharmacokinetic and pharmacodynamic analysis of enteric-coated mycophenolate sodium: limited sampling strategies and clinical outcome
British Journal of Clinical Pharmacology DOI:1.1111/j.1365-2125.29.3612.x Pharmacokinetic and pharmacodynamic analysis of enteric-coated mycophenolate sodium: limited sampling strategies and clinical outcome
TDM. Measurement techniques used to determine cyclosporine level include:
 TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
ORIGINAL ARTICLE. Received March 9, 2009; accepted July 14, 2009.
 LIVER TRANSPLANTATION 15:1473-1480, 2009 ORIGINAL ARTICLE Comparison of Pharmacokinetics of Mycophenolic Acid and Its Metabolites Between Living Donor Liver Transplant Recipients and Deceased Donor Liver
LIVER TRANSPLANTATION 15:1473-1480, 2009 ORIGINAL ARTICLE Comparison of Pharmacokinetics of Mycophenolic Acid and Its Metabolites Between Living Donor Liver Transplant Recipients and Deceased Donor Liver
Tomoyuki Enokiya 1, Kouhei Nishikawa 2, Yuichi Muraki 1, Takuya Iwamoto 1, Hideki Kanda 2, Yoshiki Sugimura 2 and Masahiro Okuda 1*
 Enokiya et al. Journal of Pharmaceutical Health Care and Sciences (2017) 3:17 DOI 10.1186/s40780-017-0086-7 RESEARCH ARTICLE Open Access Usefulness of limited sampling strategy for mycophenolic acid area
Enokiya et al. Journal of Pharmaceutical Health Care and Sciences (2017) 3:17 DOI 10.1186/s40780-017-0086-7 RESEARCH ARTICLE Open Access Usefulness of limited sampling strategy for mycophenolic acid area
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function
 ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
Organ rejection is one of the serious
 Original Article Outcomes of Late Corticosteroid Withdrawal after Renal Transplantation in Patients Exposed to Tacrolimus and/or Mycophenolate Mofetil: Meta-Analysis of Randomized Controlled Trials A.
Original Article Outcomes of Late Corticosteroid Withdrawal after Renal Transplantation in Patients Exposed to Tacrolimus and/or Mycophenolate Mofetil: Meta-Analysis of Randomized Controlled Trials A.
Nephrology Dialysis Transplantation
 Nephrol Dial Transplant (1999) 14: 394 399 Original Article Nephrology Dialysis Transplantation Reduced kidney transplant rejection rate and pharmacoeconomic advantage of mycophenolate mofetil Rudolf P.
Nephrol Dial Transplant (1999) 14: 394 399 Original Article Nephrology Dialysis Transplantation Reduced kidney transplant rejection rate and pharmacoeconomic advantage of mycophenolate mofetil Rudolf P.
Validation of Limited Sampling Strategy for the Estimation of Mycophenolic Acid Exposure in Chinese Adult Liver Transplant Recipients
 LIVER TRANSPLANTATION 13:1684-1693, 2007 ORIGINAL ARTICLE Validation of Limited Sampling Strategy for the Estimation of Mycophenolic Acid Exposure in Chinese Adult Liver Transplant Recipients Chen Hao,
LIVER TRANSPLANTATION 13:1684-1693, 2007 ORIGINAL ARTICLE Validation of Limited Sampling Strategy for the Estimation of Mycophenolic Acid Exposure in Chinese Adult Liver Transplant Recipients Chen Hao,
Pediatric Pharmacotherapy
 Pediatric Pharmacotherapy A Monthly Review for Health Care Professionals of the Children's Medical Center Volume 4 Number 8, August 1998 Mycophenolate mofetil: Use in pediatrics Beth Ann Fullmer, R.Ph.,
Pediatric Pharmacotherapy A Monthly Review for Health Care Professionals of the Children's Medical Center Volume 4 Number 8, August 1998 Mycophenolate mofetil: Use in pediatrics Beth Ann Fullmer, R.Ph.,
SYNOPSIS (PROTOCOL WX17796)
 TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant
 SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
CELLCEPT Composition Properties Pharmacokinetics
 CELLCEPT Roche Composition Active ingredient: Mycophenolate mofetil. Capsules with 250 mg mycophenolate mofetil. Excipients: coloring agent E132, excipients for capsules. TABLETS with 500 mg mycophenolate
CELLCEPT Roche Composition Active ingredient: Mycophenolate mofetil. Capsules with 250 mg mycophenolate mofetil. Excipients: coloring agent E132, excipients for capsules. TABLETS with 500 mg mycophenolate
OUT OF DATE. Choice of calcineurin inhibitors in adult renal transplantation: Effects on transplant outcomes
 nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
Effect of Ganciclovir on Pharmacokinetics of Mycophenolic Mofetil, in Kidney Transplant Patients
 Iranian Journal of Basic Medical Sciences Vol. 10, No. 4, Winter 2008, 233-238 Received: December 5, 2007; Accepted: March 2, 2008 Effect of Ganciclovir on Pharmacokinetics of Mycophenolic Mofetil, in
Iranian Journal of Basic Medical Sciences Vol. 10, No. 4, Winter 2008, 233-238 Received: December 5, 2007; Accepted: March 2, 2008 Effect of Ganciclovir on Pharmacokinetics of Mycophenolic Mofetil, in
Optimization of the Dosing Regimen of Mycophenolate Mofetil in Pediatric Liver Transplant Recipients
 LIVER TRANSPLANTATION 17:1152 1158, 2011 ORIGINAL ARTICLE Optimization of the Dosing Regimen of Mycophenolate Mofetil in Pediatric Liver Transplant Recipients Caroline Barau, 1 Aurélie Barrail-Tran, 1
LIVER TRANSPLANTATION 17:1152 1158, 2011 ORIGINAL ARTICLE Optimization of the Dosing Regimen of Mycophenolate Mofetil in Pediatric Liver Transplant Recipients Caroline Barau, 1 Aurélie Barrail-Tran, 1
Oral mizoribine pulse therapy for patients with steroid-resistant and frequently relapsing steroid-dependent nephrotic syndrome
 Nephrol Dial Transplant (2005) 20: 2243 2247 doi:10.1093/ndt/gfh996 Advance Access publication 19 July 2005 Brief Report Oral mizoribine pulse therapy for patients with steroid-resistant and frequently
Nephrol Dial Transplant (2005) 20: 2243 2247 doi:10.1093/ndt/gfh996 Advance Access publication 19 July 2005 Brief Report Oral mizoribine pulse therapy for patients with steroid-resistant and frequently
Use of mycophenolate mofetil in steroid-dependent and -resistant nephrotic syndrome
 Pediatr Nephrol (2003) 18:833 837 DOI 10.1007/s00467-003-1175-4 BRIEF REPORT Gina-Marie Barletta William E. Smoyer Timothy E. Bunchman Joseph T. Flynn David B. Kershaw Use of mycophenolate mofetil in steroid-dependent
Pediatr Nephrol (2003) 18:833 837 DOI 10.1007/s00467-003-1175-4 BRIEF REPORT Gina-Marie Barletta William E. Smoyer Timothy E. Bunchman Joseph T. Flynn David B. Kershaw Use of mycophenolate mofetil in steroid-dependent
Renal Impairment From Dettli to Guideline: What can we learn?
 Renal Impairment From Dettli to Guideline: What can we learn? SocraMetrics GmbH Mainzerhofplatz 14 99084 Erfurt phone: ++49-361-6020526 fax: ++49-361-6020525 e-mail: meinolf.wonnemann@socrametrics.de SocraMetrics
Renal Impairment From Dettli to Guideline: What can we learn? SocraMetrics GmbH Mainzerhofplatz 14 99084 Erfurt phone: ++49-361-6020526 fax: ++49-361-6020525 e-mail: meinolf.wonnemann@socrametrics.de SocraMetrics
General Introduction. 1 general introduction 13
 General Introduction In The Netherlands 13,000 patients suffer from end stage renal disease (ESRD), which left untreated inevitably results in death. Every year this number increases with approximately
General Introduction In The Netherlands 13,000 patients suffer from end stage renal disease (ESRD), which left untreated inevitably results in death. Every year this number increases with approximately
Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents
 BUMC Proceedings 1999;12:110-112 Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents CHERYLE GURK-TURNER, RPH Department of Pharmacy Services, BUMC wo mouse/human
BUMC Proceedings 1999;12:110-112 Pharmacology notes Interleukin-2 receptor-blocking monoclonal antibodies: evaluation of 2 new agents CHERYLE GURK-TURNER, RPH Department of Pharmacy Services, BUMC wo mouse/human
Mycophenolic acid (MPA)-based therapies are widely
 balt5/cjn-cjasn/cjn-cjasn/cjn00507/cjn2381-07a CJASN epress. Published hurtr on August S 13 8/15/07 16, 2007 13:24as 4/Color doi: 10.2215/CJN.03861106 Figure(s): 1&2 Art: 03861106 Input-ch Diagnostic and
balt5/cjn-cjasn/cjn-cjasn/cjn00507/cjn2381-07a CJASN epress. Published hurtr on August S 13 8/15/07 16, 2007 13:24as 4/Color doi: 10.2215/CJN.03861106 Figure(s): 1&2 Art: 03861106 Input-ch Diagnostic and
Why and How to Perform Therapeutic Drug Monitoring for Mycophenolate Mofetil
 Trends in Transplantation 2007;1:24-34 Why and How to Perform Therapeutic Drug Monitoring for Mycophenolate Mofetil Brenda de Winter and Teun van Gelder Department of Hospital Pharmacy, Clinical Pharmacology
Trends in Transplantation 2007;1:24-34 Why and How to Perform Therapeutic Drug Monitoring for Mycophenolate Mofetil Brenda de Winter and Teun van Gelder Department of Hospital Pharmacy, Clinical Pharmacology
Variability in the pharmacokinetics of mycophenolic acid
 Variability in the pharmacokinetics of mycophenolic acid Implications for therapeutic drug monitoring Brenda de Winter The publication of this thesis was financially supported by the Dutch Transplantation
Variability in the pharmacokinetics of mycophenolic acid Implications for therapeutic drug monitoring Brenda de Winter The publication of this thesis was financially supported by the Dutch Transplantation
tients with insufficient TOR inhibitor therapy that are at risk for rejection.
 Kidney International, Vol. 68 (05), pp. 2593 2598 Biochemical monitoring of mtor inhibitor based immunosuppression following kidney transplantation: A novel approach for tailored immunosuppressive therapy
Kidney International, Vol. 68 (05), pp. 2593 2598 Biochemical monitoring of mtor inhibitor based immunosuppression following kidney transplantation: A novel approach for tailored immunosuppressive therapy
The CARI Guidelines Caring for Australasians with Renal Impairment. Idiopathic membranous nephropathy: use of other therapies GUIDELINES
 Idiopathic membranous nephropathy: use of other therapies Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES No recommendations possible based on Level I or II evidence
Idiopathic membranous nephropathy: use of other therapies Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES No recommendations possible based on Level I or II evidence
Public Assessment Report. EU worksharing project paediatric data. Valcyte. Valganciclovir
 Public Assessment Report EU worksharing project paediatric data Valcyte Valganciclovir Currently approved indication(s): Pharmaceutical form(s) affected by this project: Strength(s) affected by this variation:
Public Assessment Report EU worksharing project paediatric data Valcyte Valganciclovir Currently approved indication(s): Pharmaceutical form(s) affected by this project: Strength(s) affected by this variation:
Health technology Two prophylaxis schemes against organ rejection in renal transplantation were compared in the study:
 An economic and quality-of-life assessment of basiliximab vs antithymocyte globulin immunoprophylaxis in renal transplantation Polsky D, Weinfurt K P, Kaplan B, Kim J, Fastenau J, Schulman K A Record Status
An economic and quality-of-life assessment of basiliximab vs antithymocyte globulin immunoprophylaxis in renal transplantation Polsky D, Weinfurt K P, Kaplan B, Kim J, Fastenau J, Schulman K A Record Status
Pharmacokinetic study of mycophenolic acid in Iranian kidney transplant patients.
 2013 jpc.tums.ac.ir Pharmacokinetic study of mycophenolic acid in Iranian kidney transplant patients. Kheirollah Gholami 1, Mohammadreza Rouini 2, Niayesh Mohebbi 3, Iman Karimzadeh 3, Mehdi Ahadi barzoki
2013 jpc.tums.ac.ir Pharmacokinetic study of mycophenolic acid in Iranian kidney transplant patients. Kheirollah Gholami 1, Mohammadreza Rouini 2, Niayesh Mohebbi 3, Iman Karimzadeh 3, Mehdi Ahadi barzoki
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Emerging Drug List EVEROLIMUS
 Generic (Trade Name): Manufacturer: Everolimus (Certican ) Novartis Pharmaceuticals NO. 57 MAY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence: For use with cyclosporine
Generic (Trade Name): Manufacturer: Everolimus (Certican ) Novartis Pharmaceuticals NO. 57 MAY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence: For use with cyclosporine
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Low toxicity immunosuppressive protocols in renal transplantation. Ron Shapiro
 LECTURE Low toxicity immunosuppressive protocols in renal transplantation Ron Shapiro Department of Surgery, Director, Renal Transplantation, Thomas E. Starzl, Transplantation Institute University of Pittsburgh,
LECTURE Low toxicity immunosuppressive protocols in renal transplantation Ron Shapiro Department of Surgery, Director, Renal Transplantation, Thomas E. Starzl, Transplantation Institute University of Pittsburgh,
Proton pump inhibitors do not increase the risk of acute rejection
 ORIGINAL ARTICLE Proton pump inhibitors do not increase the risk of acute rejection G.A.J. van Boekel*, C.H.H. Kerkhofs, F. van de Logt, L.B. Hilbrands Department of Nephrology, Radboud University Medical
ORIGINAL ARTICLE Proton pump inhibitors do not increase the risk of acute rejection G.A.J. van Boekel*, C.H.H. Kerkhofs, F. van de Logt, L.B. Hilbrands Department of Nephrology, Radboud University Medical
Laboratory Monitoring of Cyclosporine Pre-dose Concentration (C 0 ) After Kidney Transplantation in Isfahan
 IJMS Vol 28, No.2, June 2003 Original Article Laboratory Monitoring of Cyclosporine Pre-dose Concentration (C 0 ) After Kidney Transplantation in Isfahan Z. Tolou-Ghamari*, A.A. Palizban. Abstract Background:
IJMS Vol 28, No.2, June 2003 Original Article Laboratory Monitoring of Cyclosporine Pre-dose Concentration (C 0 ) After Kidney Transplantation in Isfahan Z. Tolou-Ghamari*, A.A. Palizban. Abstract Background:
Monitoring of Blood Cyclosporine Concentration in Steroid-Resistant Nephrotic Syndrome
 ORIGINAL ARTICLE Monitoring of Blood Cyclosporine Concentration in Steroid-Resistant Nephrotic Syndrome Masayo Naito, Takashi Takei, Aya Eguchi, Keiko Uchida, Ken Tsuchiya and Kosaku Nitta Abstract Objective
ORIGINAL ARTICLE Monitoring of Blood Cyclosporine Concentration in Steroid-Resistant Nephrotic Syndrome Masayo Naito, Takashi Takei, Aya Eguchi, Keiko Uchida, Ken Tsuchiya and Kosaku Nitta Abstract Objective
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation
 Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Literature Review: Transplantation July 2010-June 2011
 Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
For Immediate Release Contacts: Jenny Keeney Astellas US LLC (847)
 For Immediate Release Contacts: Jenny Keeney Astellas US LLC (847) 317-5405 Lauren McDonnell GolinHarris (312) 729-4233 ASTELLAS RECEIVES FDA APPROVAL FOR USE OF PROGRAF (TACROLIMUS) IN CONJUNCTION WITH
For Immediate Release Contacts: Jenny Keeney Astellas US LLC (847) 317-5405 Lauren McDonnell GolinHarris (312) 729-4233 ASTELLAS RECEIVES FDA APPROVAL FOR USE OF PROGRAF (TACROLIMUS) IN CONJUNCTION WITH
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
European Risk Management Plan. Measures impairment. Retreatment after Discontinuation
 European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
Date: 23 June Context and policy issues:
 Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
American Journal of Transplantation 2009; 9 (Suppl 3): S1 S157 Wiley Periodicals Inc.
 American Journal of Transplantation 2009; 9 (Suppl 3): S1 S157 Wiley Periodicals Inc. 2009 The Authors Journal compilation 2009 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2009; 9 (Suppl 3): S1 S157 Wiley Periodicals Inc. 2009 The Authors Journal compilation 2009 The American Society of Transplantation and the American Society of Transplant
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
KDIGO GN Guideline update Evidence summary. Steroid-sensitive nephrotic syndrome. Corticosteroid therapy for nephrotic syndrome in children
 KDIGO GN Guideline update Evidence summary Steroid-sensitive nephrotic syndrome Corticosteroid therapy for nephrotic syndrome in children PICO question In children (aged 3 to 18 years of age) with steroid-sensitive
KDIGO GN Guideline update Evidence summary Steroid-sensitive nephrotic syndrome Corticosteroid therapy for nephrotic syndrome in children PICO question In children (aged 3 to 18 years of age) with steroid-sensitive
BK Virus (BKV) Management Guideline: July 2017
 BK Virus (BKV) Management Guideline: July 2017 BK virus has up to a 60-80% seroprevalence rate in adults due to a primary oral or respiratory exposure in childhood. In the immumocompromised renal transplant
BK Virus (BKV) Management Guideline: July 2017 BK virus has up to a 60-80% seroprevalence rate in adults due to a primary oral or respiratory exposure in childhood. In the immumocompromised renal transplant
Overview of New Approaches to Immunosuppression in Renal Transplantation
 Overview of New Approaches to Immunosuppression in Renal Transplantation Ron Shapiro, M.D. Professor of Surgery Surgical Director, Kidney/Pancreas Transplant Program Recanati/Miller Transplantation Institute
Overview of New Approaches to Immunosuppression in Renal Transplantation Ron Shapiro, M.D. Professor of Surgery Surgical Director, Kidney/Pancreas Transplant Program Recanati/Miller Transplantation Institute
Cyclosporine absorption profiles in pediatric kidney and liver transplant patients
 Pediatr Nephrol (2003) 18:1275 1279 DOI 10.1007/s00467-003-1260-8 ORIGINAL ARTICLE J. M. Kovarik Peter F. Hoyer Robert Ettenger Jeffrey Punch Marianne Soergel Cyclosporine absorption profiles in pediatric
Pediatr Nephrol (2003) 18:1275 1279 DOI 10.1007/s00467-003-1260-8 ORIGINAL ARTICLE J. M. Kovarik Peter F. Hoyer Robert Ettenger Jeffrey Punch Marianne Soergel Cyclosporine absorption profiles in pediatric
Progress in Pediatric Kidney Transplantation
 Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
This study is currently recruiting participants.
 A Two Part, Phase 1/2, Safety, PK and PD Study of TOL101, an Anti-TCR Monoclonal Antibody for Prophylaxis of Acute Organ Rejection in Patients Receiving Renal Transplantation This study is currently recruiting
A Two Part, Phase 1/2, Safety, PK and PD Study of TOL101, an Anti-TCR Monoclonal Antibody for Prophylaxis of Acute Organ Rejection in Patients Receiving Renal Transplantation This study is currently recruiting
Steroid Minimization: Great Idea or Silly Move?
 Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Normal adult height after steroid-withdrawal within 6 months of pediatric kidney transplantation: a 20 years single center experience
 Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Normal adult height after steroid-withdrawal within 6 months of pediatric kidney transplantation: a 20 years single center experience Bernd Klare,
Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Normal adult height after steroid-withdrawal within 6 months of pediatric kidney transplantation: a 20 years single center experience Bernd Klare,
Can modifications of the MDRD formula improve the estimation of glomerular filtration rate in renal allograft recipients?
 Nephrol Dial Transplant (7) 22: 361 3615 doi:1.193/ndt/gfm282 Advance Access publication 22 September 7 Original Article Can modifications of the MDRD formula improve the estimation of glomerular filtration
Nephrol Dial Transplant (7) 22: 361 3615 doi:1.193/ndt/gfm282 Advance Access publication 22 September 7 Original Article Can modifications of the MDRD formula improve the estimation of glomerular filtration
Intruduction PSI MODE OF ACTION AND PHARMACOKINETICS
 Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation
 IJMS Vol 34, No 2, June 2009 Original Article Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation Reza Hekmat, Hamid Eshraghi Abstract Background:
IJMS Vol 34, No 2, June 2009 Original Article Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation Reza Hekmat, Hamid Eshraghi Abstract Background:
Nonlinear Relationship between Mycophenolate Mofetil Dose and Mycophenolic Acid Exposure: Implications for Therapeutic Drug Monitoring
 Article Nonlinear Relationship between Mycophenolate Mofetil Dose and Mycophenolic Acid Exposure: Implications for Therapeutic Drug Monitoring Brenda C.M. de Winter,* Ron A.A. Mathot,* Ferdi Sombogaard,*
Article Nonlinear Relationship between Mycophenolate Mofetil Dose and Mycophenolic Acid Exposure: Implications for Therapeutic Drug Monitoring Brenda C.M. de Winter,* Ron A.A. Mathot,* Ferdi Sombogaard,*
WHY INTRAMUSCULAR METHOTREXATE MAY BE MORE EFFICACIOUS THAN ORAL DOSING IN PATIENTS WITH RHEUMATOID ARTHRITIS
 British Journal of Rheumatology 1997;36:86 90 WHY INTRAMUSCULAR METHOTREXATE MAY BE MORE EFFICACIOUS THAN ORAL DOSING IN PATIENTS WITH RHEUMATOID ARTHRITIS R. A. HAMILTON and J. M. KREMER Albany College
British Journal of Rheumatology 1997;36:86 90 WHY INTRAMUSCULAR METHOTREXATE MAY BE MORE EFFICACIOUS THAN ORAL DOSING IN PATIENTS WITH RHEUMATOID ARTHRITIS R. A. HAMILTON and J. M. KREMER Albany College
Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, ; doi: /kisup.2012.
 http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
http://www.kidney-international.org & 2012 KDIGO Chapter 4: Steroid-resistant nephrotic syndrome in children Kidney International Supplements (2012) 2, 172 176; doi:10.1038/kisup.2012.17 INTRODUCTION This
Long-term prognosis of BK virus-associated nephropathy in kidney transplant recipients
 Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Controversies in Renal Transplantation. The Controversial Questions. Patrick M. Klem, PharmD, BCPS University of Colorado Hospital
 Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
Section 5.2: Pharmacokinetic properties
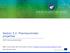 Section 5.2: Pharmacokinetic properties SmPC training presentation Note: for full information refer to the European Commission s Guideline on summary of product characteristics (SmPC) SmPC Advisory Group
Section 5.2: Pharmacokinetic properties SmPC training presentation Note: for full information refer to the European Commission s Guideline on summary of product characteristics (SmPC) SmPC Advisory Group
Random pharmacokinetic profiles of EC-MPS in children with autoimmune disease
 RESEARCH Open Access Random pharmacokinetic profiles of EC-MPS in children with autoimmune disease Guido Filler *, Ajay Parkash Sharma, Deborah M Levy, Abeer Yasin Abstract Background: Therapy with mycophenolate
RESEARCH Open Access Random pharmacokinetic profiles of EC-MPS in children with autoimmune disease Guido Filler *, Ajay Parkash Sharma, Deborah M Levy, Abeer Yasin Abstract Background: Therapy with mycophenolate
Mycophenolate Mofetil
 Mycophenolate Mofetil Cynthia L. Chen, MD The Permanente Medical Group, Northern California Diablo Service Area February 17, 2018 January 23, 2018 2011 Kaiser Foundation Health Plan, Inc. For internal
Mycophenolate Mofetil Cynthia L. Chen, MD The Permanente Medical Group, Northern California Diablo Service Area February 17, 2018 January 23, 2018 2011 Kaiser Foundation Health Plan, Inc. For internal
REACH Risk Evaluation to Achieve Cardiovascular Health
 Dyslipidemia and transplantation History: An 8-year-old boy presented with generalized edema and hypertension. A renal biopsy confirmed a diagnosis of focal segmental glomerulosclerosis (FSGS). After his
Dyslipidemia and transplantation History: An 8-year-old boy presented with generalized edema and hypertension. A renal biopsy confirmed a diagnosis of focal segmental glomerulosclerosis (FSGS). After his
Sirolimus versus Calcineurin Inhibitor-based Immunosuppressive Therapy in Kidney Transplantation A 4-year Follow-up
 Transplantation Sirolimus versus Calcineurin Inhibitor-based Immunosuppressive Therapy in Kidney Transplantation A 4-year Follow-up Mohsen Nafar, 1 Behrang Alipour, 2 Pedram Ahmadpoor, 1 Fatemeh Pour-Reza-Gholi,
Transplantation Sirolimus versus Calcineurin Inhibitor-based Immunosuppressive Therapy in Kidney Transplantation A 4-year Follow-up Mohsen Nafar, 1 Behrang Alipour, 2 Pedram Ahmadpoor, 1 Fatemeh Pour-Reza-Gholi,
Cyclosporine Lymphocyte Maximum Level Monitoring in De Novo Kidney Transplant Patients: A Prospective Study
 Cyclosporine Lymphocyte Maximum Level Monitoring in De Novo Kidney Transplant Patients: A Prospective Study AG Barbari, MA Masri, AG Stephan, B El Ghoul, S Rizk, N Mourad, GS Kamel, HE Kilani, AS Karam
Cyclosporine Lymphocyte Maximum Level Monitoring in De Novo Kidney Transplant Patients: A Prospective Study AG Barbari, MA Masri, AG Stephan, B El Ghoul, S Rizk, N Mourad, GS Kamel, HE Kilani, AS Karam
Additional file 2: Details of cohort studies and randomised trials
 Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Acute rejection and late renal transplant failure: Risk factors and prognosis
 Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
INTERNET-BASED HOME MONITORING OF PULMONARY FUNCTION AFTER LUNG TRANSPLANTATION. 2000, 25 patients underwent heart lung (HLT) or bilateral-lung (BLT)
 Online Supplement for: INTERNET-BASED HOME MONITORING OF PULMONARY FUNCTION AFTER LUNG TRANSPLANTATION METHODS Patients Between the start of the study in June 1998 and the end of the study in September
Online Supplement for: INTERNET-BASED HOME MONITORING OF PULMONARY FUNCTION AFTER LUNG TRANSPLANTATION METHODS Patients Between the start of the study in June 1998 and the end of the study in September
Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new (MDRD) prediction equation
 Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
Fixed- or Controlled-Dose Mycophenolate Mofetil with Standard- or Reduced-Dose Calcineurin Inhibitors: The Opticept Trial
 American Journal of Transplantation 2009; 9: 1607 1619 Wiley Periodicals Inc. C 2009 The Authors Journal compilation C 2009 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2009; 9: 1607 1619 Wiley Periodicals Inc. C 2009 The Authors Journal compilation C 2009 The American Society of Transplantation and the American Society of Transplant
Tacrolimus-Induced Neutropenia in Renal Transplant Recipients
 CJASN epress. Published on January 21, 2011 as doi: 10.2215/CJN.07320810 Special Features Tacrolimus-Induced Neutropenia in Renal Transplant Recipients Anja De Rycke,* Daan Dierickx, and Dirk R. Kuypers*
CJASN epress. Published on January 21, 2011 as doi: 10.2215/CJN.07320810 Special Features Tacrolimus-Induced Neutropenia in Renal Transplant Recipients Anja De Rycke,* Daan Dierickx, and Dirk R. Kuypers*
Renal Biopsy Findings in Children Receiving Long-Term Treatment with Cyclosporine A Given as a Single Daily Dose
 Tohoku J. Exp. Med., Posttreatment 2006, 209, 191-196 Renal Biopsy Following Once-daily CsA Treatment 191 Renal Biopsy Findings in Children Receiving Long-Term Treatment with Cyclosporine A Given as a
Tohoku J. Exp. Med., Posttreatment 2006, 209, 191-196 Renal Biopsy Following Once-daily CsA Treatment 191 Renal Biopsy Findings in Children Receiving Long-Term Treatment with Cyclosporine A Given as a
Mycophenolate mofetil (MMF) is an effective anti proliferative
 OVERVIEW Controlled-Dose Versus Fixed-Dose Mycophenolate Mofetil for Kidney Transplant Recipients: A Systematic Review and Meta-Analysis of Randomized Controlled Trials Xianding Wang, 1 Xin Qin, 1 Yong
OVERVIEW Controlled-Dose Versus Fixed-Dose Mycophenolate Mofetil for Kidney Transplant Recipients: A Systematic Review and Meta-Analysis of Randomized Controlled Trials Xianding Wang, 1 Xin Qin, 1 Yong
Alemtuzumab Induction in Non-Hepatitis C Positive Liver Transplant Recipients
 LIVER TRANSPLANTATION 17:32-37, 2011 ORIGINAL ARTICLE Alemtuzumab Induction in Non-Hepatitis C Positive Liver Transplant Recipients Josh Levitsky, 1,2 Kavitha Thudi, 1 Michael G. Ison, 1,3 Edward Wang,
LIVER TRANSPLANTATION 17:32-37, 2011 ORIGINAL ARTICLE Alemtuzumab Induction in Non-Hepatitis C Positive Liver Transplant Recipients Josh Levitsky, 1,2 Kavitha Thudi, 1 Michael G. Ison, 1,3 Edward Wang,
NAPRTCS Annual Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 27 Annual Report Renal Transplantation Dialysis Chronic Renal Insufficiency This is a privileged communication not for publication.
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 27 Annual Report Renal Transplantation Dialysis Chronic Renal Insufficiency This is a privileged communication not for publication.
Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients
 Original article Annals of Oncology 15: 291 295, 2004 DOI: 10.1093/annonc/mdh079 Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients G.
Original article Annals of Oncology 15: 291 295, 2004 DOI: 10.1093/annonc/mdh079 Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients G.
North American Pediatric Renal Transplant Cooperative Study (NAPRTCS) 2005 Annual Report. Renal Transplantation. Chronic Renal Insufficiency
 North American Pediatric Renal Transplant Cooperative Study (NAPRTCS) 2005 Annual Report Renal Transplantation Dialysis Chronic Renal Insufficiency This is a privileged communication not for publication.
North American Pediatric Renal Transplant Cooperative Study (NAPRTCS) 2005 Annual Report Renal Transplantation Dialysis Chronic Renal Insufficiency This is a privileged communication not for publication.
Cyclosporine (CsA) dose adjustments based on. C 2 Monitoring of Cyclosporine in De Novo Liver Transplant Recipients: The Clinician s Perspective
 REVIEW C 2 Monitoring of Cyclosporine in De Novo Liver Transplant Recipients: The Clinician s Perspective Federico Villamil 1 and Stephen Pollard 2 Adjusting cyclosporine (CsA) dose based on blood concentration
REVIEW C 2 Monitoring of Cyclosporine in De Novo Liver Transplant Recipients: The Clinician s Perspective Federico Villamil 1 and Stephen Pollard 2 Adjusting cyclosporine (CsA) dose based on blood concentration
Effects of pretransplant plasmapheresis and rituximab on recurrence of focal segmental glomerulosclerosis in adult renal transplant recipients
 ORIGINAL ARTICLE Korean J Intern Med 2014;29:482-488 Effects of pretransplant plasmapheresis and rituximab on recurrence of focal segmental glomerulosclerosis in adult renal transplant recipients Hoon
ORIGINAL ARTICLE Korean J Intern Med 2014;29:482-488 Effects of pretransplant plasmapheresis and rituximab on recurrence of focal segmental glomerulosclerosis in adult renal transplant recipients Hoon
Rejection after simultaneous pancreas kidney transplantation
 Nephrol Dial Transplant (2005) 20 [Suppl 2]: ii11 ii17 doi:10.1093/ndt/gfh1077 Rejection after simultaneous pancreas kidney transplantation Helmut Arbogast 1, Jacques Malaise 3, Wolf-Dieter Illner 1, Anwar
Nephrol Dial Transplant (2005) 20 [Suppl 2]: ii11 ii17 doi:10.1093/ndt/gfh1077 Rejection after simultaneous pancreas kidney transplantation Helmut Arbogast 1, Jacques Malaise 3, Wolf-Dieter Illner 1, Anwar
Out of date SUGGESTIONS FOR CLINICAL CARE (Suggestions are based on level III and IV evidence)
 Membranous nephropathy role of cyclosporine therapy Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES a. The use of cyclosporine therapy alone to prevent progressive
Membranous nephropathy role of cyclosporine therapy Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES a. The use of cyclosporine therapy alone to prevent progressive
Drug Dosing in Renal Insufficiency. Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila
 Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
The CARI Guidelines Caring for Australasians with Renal Impairment. Membranous nephropathy role of steroids GUIDELINES
 Membranous nephropathy role of steroids Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES There is currently no data to support the use of short-term courses of
Membranous nephropathy role of steroids Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES There is currently no data to support the use of short-term courses of
ORIGINAL ARTICLE. GH Cochin-Saint Vincent-de-Paul, Paris, France; and 3 EA 3738, Université Lyon 1, Université de Lyon, Lyon, France
 LIVER TRANSPLANTATION 14:1745-1751, 2008 ORIGINAL ARTICLE Comparison of a New Enzymatic Assay with a High-Performance Liquid Chromatography/ Ultraviolet Detection Method for Therapeutic Drug Monitoring
LIVER TRANSPLANTATION 14:1745-1751, 2008 ORIGINAL ARTICLE Comparison of a New Enzymatic Assay with a High-Performance Liquid Chromatography/ Ultraviolet Detection Method for Therapeutic Drug Monitoring
NAPRTCS Annual Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2006 Annual Report Renal Transplantation Dialysis Chronic Renal Insufficiency This is a privileged communication not for publication.
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2006 Annual Report Renal Transplantation Dialysis Chronic Renal Insufficiency This is a privileged communication not for publication.
Desensitization in Kidney Transplant. James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver
 Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
Original Article Estimation of optimal minimum dosage of mycophenolate mofetil in children with various glomerular diseases
 Int J Clin Exp Med 2018;11(1):316-326 www.ijcem.com /ISSN:1940-5901/IJCEM0050850 Original Article Estimation of optimal minimum dosage of mycophenolate mofetil in children with various glomerular diseases
Int J Clin Exp Med 2018;11(1):316-326 www.ijcem.com /ISSN:1940-5901/IJCEM0050850 Original Article Estimation of optimal minimum dosage of mycophenolate mofetil in children with various glomerular diseases
Pediatric Kidney Transplantation
 Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
