Diabetic Foot Ulcers:
|
|
|
- Jemima Webster
- 5 years ago
- Views:
Transcription
1 TREATMENT Diabetic Foot Ulcers: How to Assess, Treat, and Prevent Them General public awareness of diabetes has grown in recent years, thanks in part to the warnings about childhood obesity and its relationship to diabetes. Caregivers involved with long-term-care residents are already familiar with diabetes mellitus and its consequences. Unless lifestyle changes occur, it is likely we will continue to see an increase in diabetes in our elderly patients. Janet L. Jones, RN, BSN, PHN, ET, CWOCN, DAPWCA 36 HEALTHY SKIN
2 Let s look at the statistics Foot complications are one of the most common reasons for hospital admissions among patients with diabetes mellitus. The incidence of diabetic ulceration is as high as 4.1% annually, and the lifetime risk for foot ulcers in persons with diabetes is estimated at 15%. 1 Nonhealing diabetic ulcers are the most common cause of lower extremity amputations in the industrialized world. 2 Research has shown that early diagnosis and treatment can prevent a majority of these amputations. Costs associated with ulcer care Diabetic ulcers account for 25% to 50% of the cost of inpatient diabetic care, recurring at a rate of greater than 50% over a two- to five-year period. 3 It is clearly evident that treating neuropathic/diabetic ulcers has a huge financial impact on health care. Several studies have examined the direct treatment costs. One study determined that the average cost to heal an ulcer is $6,664; the cost rises to $44,790 following an amputation. 4 Pathophysiology of diabetic ulcers The pathophysiology of neuropathic diabetic ulcers includes a triad of events angiopathy, neuropathy, and infection sometimes related to minor trauma. Angiopathy: Occlusion begins distally with smaller vessels in areas (multisegmental) along the leg. Both limbs may be affected. The patient can present with dry gangrene. Auto-amputation of the digits or limb is not uncommon. Sensory neuropathy: Hyperesthesia or an exaggerated sensation of pain may occur. Alternatively, the patient can have hypoesthesia or a lack of sensation. Having no sensation poses greater concern. For example, if a patient steps on a nail and the nail becomes embedded in the tissue, the patient with hypoesthesia will be unaware of its presence. This situation can lead to infection and threatened loss of limb. Motor neuropathy: Approximately 10% of residents with neuropathy experience a progressive deformity, dislocation, and destruction of the bones of the foot called Charcot foot. If hammertoes or crunched-up toes are present and the patient is wearing inappropriate footwear, ulcers can occur on the tops of the toes from the skin rubbing (friction) on the shoe. When severe foot deformity occurs, custom footwear is essential. Calluses can form over bony prominences such as under the metatarsal heads or on the plantar surface of the foot. These calluses become thick, acting as a foreign object that can lead to ulceration. To avoid these problems, routine foot care, with debridement of the callus, and appropriate footwear are essential. Autonomic neuropathy: The patient can also experience anhydrosis or a lack of perspiring or sweating, which can promote bacterial invasion and lead to infection. Keeping the feet clean and dry helps prevent bacterial invasion. The toenails of the diabetic often become infected with fungus, which can lead to severe nail deformity. 37
3 Diabetic Foot Ulcers: How to Assess, Treat, and Prevent Them continued Assessing residents with diabetic neuropathy A comprehensive medical history is vital to the assessment and treatment of residents with neuropathic/diabetic ulcerations. Many components contribute to poor or slow healing; these include increasing age, increasing duration of the diabetes, smoking, hypertension, hypercholesterolemia, and abnormal blood sugar levels. Neuropathic/diabetic ulcers usually occur below the ankle at any site of pressure, friction, shear, or trauma. The wound margins are often characterized by a periwound callus, and the wound is likely to be round. The presence of diabetes increases the risk for infection. Diabetic wounds heal at approximately half the rate of venous ulcers. Expect them to make slow progress. 5 If it has been determined that the arterial perfusion is adequate to support wound healing, then treatment of the wound should be based on optimal moisture. If the wound is dry, apply a product that creates moisture or supports what moisture is already present. If the wound is moderately to heavily draining, choose a dressing that absorbs excess drainage, thereby bringing the moisture level back into balance. Because a person with diabetes experiences reduced blood flow to the skin, consider improving circulation through vascular bypass, percutaneous angioplasty, laser treatment, and hemorrhagic agents like Trental. Vascular assessment includes arteriography to assess the level of blood flow and determine if vascular reconstruction is appropriate. Results compare favorably with those achieved in nondiabetics. The results include increased healing, elimination of pain, improved function, and overall increased well-being. A decrease in amputation rates has also been demonstrated. Managing infection is crucial in the treatment of a diabetic ulcer in order to preserve the limb. Treating neuropathic/diabetic ulcers The treatment plan for the neuropathic/diabetic ulcer is complex and involves the following: The primary treatment is removing the pressure from the foot (off-loading). This can be accomplished in multiple ways, e.g., contact casting, therapeutic boots, specialty footwear, or off-loading devices. Radical local debridement of the callus, tissue, and bone should be performed as appropriate. Evidence does not support soaking, whirlpool, or other hydrotherapies, which can lead to maceration, mild burns, or infection. General skin care of the extremity includes keeping the foot clean and dry. Emolliating the leg to the wound margin is essential in regaining and maintaining skin integrity and skin health. Adjunctive medical therapies are important in the treatment of neuropathic/diabetic ulcers and should not be overlooked. Such modalities as normalizing blood glucose (macrophages perform less efficiently if blood glucose is greater than 180), treating edema, providing for nutritional therapy, and controlling comorbid conditions have been proven beneficial. 38 HEALTHY SKIN
4 Infection and antibiotic therapy Managing infection is crucial in the treatment of a neuropathic/diabetic ulcer in order to preserve the limb. All of these wounds are colonized with bacteria, and most have a high surface overgrowth of bacteria or bioburden. An infection diagnosis that would require systemic antibiotics includes the presence of purulent secretions (pus) and two or more signs of inflammation (erythema, pain, warmth, and edema). Literature suggests that osteomyelitis is present in 89% of infected neuropathic/diabetic ulcers that probe to the bone. 6 When should antibiotic therapy be considered? If assessment reveals a nonlimb-threatening infection, begin antibiotic therapy on the day the infection is diagnosed. If assessment reveals a limbthreatening infection, the patient requires hospitalization and parenteral antibiotic therapy should be initiated. Amputation: the last resort Limb loss is a common event associated with neuropathic/diabetic ulcers. Its pathophysiology follows a fairly predictable course. The baseline neuropathy, when combined with a minor trauma, may result in ulceration. This can lead to poor healing, gangrene, infection, and cellular failure. These events can lead to amputation. 7 Preventing ulcer recurrence Ultimately, preventing ulcer recurrence is the key to longterm success, and patient education tops the list of strategies. Educating your residents should include demonstrating how to inspect the feet, explaining the difference between improper and proper nail care, and discussing the importance of never walking barefoot. Patients with foot deformities or those wearing customized footwear or orthotics also need to be educated in observing any changes in foot condition. There are no conclusive studies to support prophylactic foot surgery, although some patients have experienced improvement. It is certain, however, that diabetics do benefit from regular foot care by specialists. Regular exercise, proper diet, controlling blood sugar, and being alert to changes in the skin before an ulcer develops are key components to managing diabetes. If the resident smokes, it is essential for him or her to stop smoking and to understand the reasons why this is so important. These issues are all part of diabetic education. It is obvious that responding to a neuropathic/diabetic ulcer is not merely treating the wound; rather, the treatment is complex and multidisciplinary and involves making the resident a participating member of the care team. Amputation should be considered when perfusion is below the threshold necessary for healing. Amputation may be preferred for patients who have endured an unsuccessful course of therapy, or for patients who are not candidates for revascularization. References: 1. Warriner III, R. Chief Medical Officer, Wound Care Group Medical Director, Southeast Texas Center for Wound Care and Hyperbaric Medicine Moss S, Klein R, Klein B. The 14-year incidence of lower-extremity amputations in a diabetic population: the Wisconsin epidemiologic study of diabetic retinopathy. Diabetes Care, 22(6): , Harris, M.I., Cowie, C., Stern, M., Boydo, E., Reiber, G., & Bennett, P. (Eds). (1995). Diabetes in America. Bethesda, MD: U.S. Department of Health and Human Services. 4. Appelqvist J. Wound healing in diabetes. Outcome and costs. Clin Podiatric Med Surg 1998; 15: Kantor J, Margolis D. Expected Healing Rates for Chronic Wounds. Wounds 12 (6): , Wound, Ostomy, and Continence Nurses Society (2004). Guideline for management in patients with lower-extremity neuropathic disease. Glenview, IL. 7. Reiber G, et al. Causal pathway for incident lower extremity ulcers in patients with diabetes from two settings. Diabetes Care,
5 TREATMENT COMPRESSION: HOW MUCH IS NEEDED TO BE THERAPEUTIC? Elizabeth O Connell-Gifford and Jackie Young Mrs. PJ enters your facility with a family-reported vague diagnosis of poor circulation and a lot of swelling in both of her legs. You note a small shallow wound in the gaiter area of her left lower extremity. She is 76 years old and obese; she has stress incontinence that is managed by panty liner; she has dementia; and she is no longer able to perform her ADLs. After the initial assessment, you realize that more information is needed to initiate appropriate treatment.you call the primary care physician s office and learn that Mrs. PJ has been diagnosed with venous hypertension or lower extremity venous disease (LEVD). Her arterial perfusion is adequate. Let s discuss the treatment for LEVD and the best plan for Mrs. PJ. 41
6 TREATMENT COMPRESSION: HOW MUCH IS NEEDED TO BE THERAPEUTIC The gold standard of treatment for LEVD is to use adequate compression. Before any form of compression is applied, the arterial perfusion status must be evaluated. If the lower extremity has either arterial or mixed (arterial and venous) disease, applying compression is usually contraindicated and could lead to negative results. A fairly simple diagnostic test, the ABI or ankle-brachial index, is often all that is needed to decide if compression is appropriate or not. (1) This article focuses on compression, but it is important to realize that the wound itself may also need to be dressed. The dressing is chosen based on multiple factors including wound characteristics, frequency of dressing change (a daily dressing is not the best choice with a seven-day compression wrap, for example), the ability of the patient or caregiver to apply the dressing, as well as reimbursement and availability issues. There are no studies showing that one type of dressing or specific frequency of dressing change is appropriate for all LEVD wounds. A short course (approximately two weeks) of a topical antimicrobial may be considered if the ulcer has a high level of bacteria. (1) About the ankle-brachial index (ABI): ABI = ankle blood pressure divided by brachial (arm) blood pressure.the result will be close to 1 (meaning they are about the same) in a normal person. Results of 0.8 to 1 are within the normal range. Residents with an ABI of less than 0.8 may have peripheral arterial disease, in which case compression would be contraindicated. In a diabetic, because of small vessel calcification, this test is not as reliable. Applying compression in any form to a patient with venous hypertension can be challenging! One of the most common complaints from clinicians is, My patients are noncompliant; they won t leave their compression system in place because they say it hurts. Realize that edema associated with LEVD can be very painful. The challenge is to get the patient to leave the product on until the edema is reduced. Once that happens, it is likely the pain will lessen or be nonexistent. Discuss with the patient that this pain is not uncommon and usually lessens over time with treatment. Talk with the physician about prescribing appropriate analgesics for the first several weeks of therapy. There is research that supports therapeutic compression as an effective means of treatment. But how much compression is enough? It is documented that some compression therapy is more effective than no compression therapy for the treatment of LEVD wounds. High compression (30 50 mmhg) is more effective than low compression, but there are no differences in the effectiveness of the different types of products available for high compression. (1) The most commonly used products for compression are wraps or stocking-like products. Application of wraps should not be performed by an inexperienced person. Proper technique is crucial and requires training. Wraps that are applied incorrectly can create too much compression, leading to limb loss or damage, or too little compression, causing a delay in healing or even a decline in condition. There are several different ways to address wounds on the lower extremity. As with Mrs. PJ, the initial assessment leads to further investigation and some detective work on the part of the nurse. Obtaining all the information from the family as well as the primary care physician s office allowed Mrs. PJ to receive the best treatment for her LEVD. The wound was small and had some drainage that needed to be managed. Because there was a concern about bioburden, a silver alginate dressing and a four-layer compression wrap was the dressing of choice. The entire dressing was changed every five days. 42 HEALTHY SKIN
7 Easy Guide to Compression Therapy Type of Amount of Application of Performance Compression Examples Compression Compression Characteristics Long stretch elastic bandages *Matrix, *Swift-Wrap, *Sure-Wrap, Ace, Curity 17 mmhg pressure Applied in a figureof-eight from toe to knee with a 50% overlap on an ankle circumference of cm (3) Not washable or reusable, loses stretch after first application Zinc paste bandages (inelastic compression) *Primer Boot, Unna Boot, Dome Paste Bandage Applies initial pressure of 29.8 mmhg at the ankle but falls to 10.4 mmhg at 24 hours (2) Applied in an overlap fashion from the toe to the knee with a 50% overlap Not reusable Light compression, support *Medigrip, Tubigrip If the product is shaped, it applies mmhg pressure in a single layer (3) Cannot apply graduated compression because it does not conform to the leg. May fit at the calf but be too loose at the ankle. Washable (not dryersafe) for up to 6 months Multilayer *FourFlex, Profore, Dynaflex, Four-Press Can maintain 40 mmhg pressure on an ankle circumference of cm for up to (2, 4) one week Various layers are applied differently. Please refer to package insert for instructions. High compression. Cut off entire dressing at change. Cohesive or selfadherent bandage *Co-Flex, Coban, *PowerFlex, Flex-Wrap 23 mmhg pressure Applied at mid stretch with a 50% overlap in a spiral from toe to knee on an ankle circumference (3, 4) of cm Used with other products to produce therapeutic compression. Not washable or reusable. High elastic compression Setopress, Surepress Can apply up to 40 (3, 4) mmhg pressure Please refer to individual package Therapeutic compression to treat LEVD * These products are available through Medline. References: 1. Johnson J and Paustian C. Guideline for Management of Wounds in Patients with Lower Extremity Venous Disease. Number four in WOCN Clinical Practice Guideline Series. Wound Ostomy and Continence Nurses Society, 2005, Glenview IL, p Blair SD, Wright DDI, Backhouse CM et al. Sustained compression and healing of chronic venous ulcers. British Medical Journal 1988:297: Moffatt CJ. Compression bandaging the state of the art. Journal of Wound Care 1992:1:1: Moffatt CJ, Dickson D. The Charing Cross high compression four-layer bandage system. Journal of Wound Care 1992:2:2:
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Preventing Foot Ulcers in the Neuropathic Diabetic Foot. Glossary of Terms
 Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
4-layer compression bandaging system (includes microbe binding wound contact layer) Latex-free, 4-layer compression bandaging system
 JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
AGONY FEET. The. of the. Prevention and management of diabetic foot ulcers
 The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Diabetes - Foot Care
 Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Patient & Family Guide. Diabetic Foot Ulcer.
 Patient & Family Guide Diabetic Foot Ulcer 2018 www.nshealth.ca Diabetic Foot Ulcer What is a diabetic foot ulcer? The term foot ulcer is used to describe an open sore that happens below the ankle and
Patient & Family Guide Diabetic Foot Ulcer 2018 www.nshealth.ca Diabetic Foot Ulcer What is a diabetic foot ulcer? The term foot ulcer is used to describe an open sore that happens below the ankle and
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Arterial & Venous Ulcers. A Comprehensive Review Assessment & Management
 Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Diabetes is a serious disease that can develop from lack of insulin production in the body or due to
 Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
UNIT FOUR LESSON 11 OUTLINE
 UNIT FOUR LESSON 11 OUTLINE Tell participants: Taking care of your feet is an important part of diabetes management. Diabetes is the leading cause of amputations of the lower limbs. In Kentucky, there
UNIT FOUR LESSON 11 OUTLINE Tell participants: Taking care of your feet is an important part of diabetes management. Diabetes is the leading cause of amputations of the lower limbs. In Kentucky, there
Patient Product Information
 Patient Product Information REGEN-D 150 (India's First Recombinant Human Epidermal Growth Factor (rhegf) Gel for Diabetic Foot Ulcers) Generic name: [Recombinant Human Epidermal Growth Factor (rhegf)]
Patient Product Information REGEN-D 150 (India's First Recombinant Human Epidermal Growth Factor (rhegf) Gel for Diabetic Foot Ulcers) Generic name: [Recombinant Human Epidermal Growth Factor (rhegf)]
Podiatric Medicine: Best Foot Forward. Dr. Kevin J. DeAngelis, DPM Brandywine Family Foot Care 213 Reeceville Rd. Suite 13 Coatesville, PA
 Podiatric Medicine: Best Foot Forward Dr. Kevin J. DeAngelis, DPM Brandywine Family Foot Care 213 Reeceville Rd. Suite 13 Coatesville, PA What is a Podiatrist? Specially trained physician specializing
Podiatric Medicine: Best Foot Forward Dr. Kevin J. DeAngelis, DPM Brandywine Family Foot Care 213 Reeceville Rd. Suite 13 Coatesville, PA What is a Podiatrist? Specially trained physician specializing
Lower Extremity Venous Disease (LEVD)
 Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Rapid Recovery Hyperbarics 9439 Archibald Ave. Suite 104 Rancho Cucamonga CA,
 Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Diabetes Mellitus and the Associated Complications
 Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
A Guide for People With Diabetes. Take Care of Your Feet for a
 A Guide for People With Diabetes Take Care of Your Feet for a You can take care of your feet! Do you want to avoid serious foot problems that can lead to a toe, foot, or leg amputation? Take Care of Your
A Guide for People With Diabetes Take Care of Your Feet for a You can take care of your feet! Do you want to avoid serious foot problems that can lead to a toe, foot, or leg amputation? Take Care of Your
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
DIABETES AND FOOTCARE
 DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy.
 Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Podiatry in Practice. Alan M. Singer, DPM, FACFAS
 Podiatry in Practice Alan M. Singer, DPM, FACFAS Podiatry in Practice Alan Singer, D.P.M. UNIVERSITY PODIATRY GROUP Onychomycosis Anti-fungals Onychocryptosis (Ingrown Nails) Ingrown Nails Partial Nail
Podiatry in Practice Alan M. Singer, DPM, FACFAS Podiatry in Practice Alan Singer, D.P.M. UNIVERSITY PODIATRY GROUP Onychomycosis Anti-fungals Onychocryptosis (Ingrown Nails) Ingrown Nails Partial Nail
Total Contact Cast System
 Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
Helen Gelly, MD, FUHM, FCCWS
 Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
10/19/2017. Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI. Consultant with J&J-Depuy-Synthesis
 Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Diabetic Foot Pathophysiology. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device
 VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
Why do I need Diabetic Footwear?
 Why do I need Diabetic Footwear? A guide to healthier, happier feet for people with diabetes. To find a provider near you, go to www.drcomfort.com and click on Find a Footwear Professional. Or call Dr.
Why do I need Diabetic Footwear? A guide to healthier, happier feet for people with diabetes. To find a provider near you, go to www.drcomfort.com and click on Find a Footwear Professional. Or call Dr.
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Diabetic Foot Exams. Comprehensive. The Foot & Ankle Center Located on the Campus of Johnston-Willis Hospital
 Comprehensive Diabetic Foot Exams The Foot & Ankle Center Located on the Campus of Johnston-Willis Hospital Dr. Mitchell R. Waskin Dr. Jeffrey P. Frost Diabetes is a serious illness that causes numerous
Comprehensive Diabetic Foot Exams The Foot & Ankle Center Located on the Campus of Johnston-Willis Hospital Dr. Mitchell R. Waskin Dr. Jeffrey P. Frost Diabetes is a serious illness that causes numerous
My Diabetic Patient Has No Pulses; What Should I Do?
 Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING
 HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
Aetiology Macroangiopathy occurs mainly distally ie Popliteal artery There is arterial wall calcification Microangiopathy is less common
 DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
10/9/2015. Differential Assessment of Lower Extremity Wounds. Disclosure Statement. Program Objectives
 3M 2015. All Rights Reserved 3M 2015. All Rights Reserved 2 3M 2015. All Rights Reserved 3 Differential Assessment of Lower Extremity Wounds Presented by: Lynn Peterson RN, BSN, CWOCN 3M Health Care November
3M 2015. All Rights Reserved 3M 2015. All Rights Reserved 2 3M 2015. All Rights Reserved 3 Differential Assessment of Lower Extremity Wounds Presented by: Lynn Peterson RN, BSN, CWOCN 3M Health Care November
Frank K. Galbraith D.P.M. Dr. Frank Galbraith
 Frank K. Galbraith D.P.M. Dr. Frank Galbraith Ingrown Toenails Paronychia (infected toenail) Onychomycosis (fungal nails) From improper trimming, leaving nail sharp corners Curved nails Thick (Hypertrophic)
Frank K. Galbraith D.P.M. Dr. Frank Galbraith Ingrown Toenails Paronychia (infected toenail) Onychomycosis (fungal nails) From improper trimming, leaving nail sharp corners Curved nails Thick (Hypertrophic)
Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014
 Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014 Dr. Michael Yan, MD, CCFP Clinical Lecturer, Department of Family Medicine, University of
Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014 Dr. Michael Yan, MD, CCFP Clinical Lecturer, Department of Family Medicine, University of
Localized collection of pus in a cavity
 Localized collection of pus in a cavity Loss of feeling or sensation induced to permit surgery Common example: Injection given to numb up the toe prior to performing an ingrown toenail procedure Mechanical
Localized collection of pus in a cavity Loss of feeling or sensation induced to permit surgery Common example: Injection given to numb up the toe prior to performing an ingrown toenail procedure Mechanical
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Front line management of the Diabetic Foot
 Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Conservative Management to Restore and Maintain Function in Limb Preservation Patients
 Conservative Management to Restore and Maintain Function in Limb Preservation Patients Tyson Green, DPM Department Chair Imperial Health Center for Orthopaedics Lake Charles, LA Founder & Medical Director
Conservative Management to Restore and Maintain Function in Limb Preservation Patients Tyson Green, DPM Department Chair Imperial Health Center for Orthopaedics Lake Charles, LA Founder & Medical Director
JOURNAL OF WOUND CARE. VOLUME 8. NUMBER 9. October A comparison of sub-bandage pressures produced with two multi-layer bandaging systems
 JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
CHAPTER.7 CARING THE DIABETIC FOOT
 CHAPTER.7 CARING THE DIABETIC FOOT Introduction Diabetes has become a global epidemic(144). The long term complications due to diabetes impose huge social and economic burden, mental and physical misery
CHAPTER.7 CARING THE DIABETIC FOOT Introduction Diabetes has become a global epidemic(144). The long term complications due to diabetes impose huge social and economic burden, mental and physical misery
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Charcot Arthropathy of the Foot & Ankle. MTAPA Annual Meeting June 2018 Emily Harnden, MD
 Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
How to manage leg ulcers in the elderly
 How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
INTEGRATED THERAPEUTIC SOLUTIONS TO MANAGE AND PREVENT DIABETIC FOOT ULCERS
 INTEGRATED THERAPEUTIC SOLUTIONS TO MANAGE AND PREVENT DIABETIC FOOT ULCERS UE REMOVE EXU D R IA ER T C D TISS UIL EB ATE AN DB A REMOVE REBUILD REDUCE Cutimed Siltec Sorbact featuring DACC Technology
INTEGRATED THERAPEUTIC SOLUTIONS TO MANAGE AND PREVENT DIABETIC FOOT ULCERS UE REMOVE EXU D R IA ER T C D TISS UIL EB ATE AN DB A REMOVE REBUILD REDUCE Cutimed Siltec Sorbact featuring DACC Technology
Project I - Background Worksheet. Team Members: Kira Brown, Paige Fallu. Clinical problem Diabetic Foot Ulcers
 Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
LOOKING AFTER YOUR FEET
 LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
Available Reproducibles
 A Guide to Common Foot Deformities A Shoe for Every Sport A True or False Quiz About Walking Aerobics and Your Feet Aging and Your Feet All Toes On-Deck Alternatives to Walking Amputation Prevention Checklist
A Guide to Common Foot Deformities A Shoe for Every Sport A True or False Quiz About Walking Aerobics and Your Feet Aging and Your Feet All Toes On-Deck Alternatives to Walking Amputation Prevention Checklist
Integra. PriMatrix Dermal Repair Scaffold PATIENT INFORMATION. Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1
 Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT. SCOPE: Western Australia. Clinical Protocol for Venous Leg Ulcer Management
 CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
Diabetic Foot Complications
 Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Measure #127 (NQF 0416): Diabetes Mellitus: Diabetic Foot and Ankle Care, Ulcer Prevention Evaluation of Footwear National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR INDIVIDUAL MEASURES:
Measure #127 (NQF 0416): Diabetes Mellitus: Diabetic Foot and Ankle Care, Ulcer Prevention Evaluation of Footwear National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR INDIVIDUAL MEASURES:
Contents. The Diabetic Foot 3. Essentials of Diabetic Foot Care 5. Numbness in Feet, But No Diabetes? Here s What Else It Could Be 7
 Contents The Diabetic Foot 3 Essentials of Diabetic Foot Care 5 Numbness in Feet, But No Diabetes? Here s What Else It Could Be 7 Proper Shoes For Diabetics 9 How to Treat and Prevent a Diabetic Foot Ulcer
Contents The Diabetic Foot 3 Essentials of Diabetic Foot Care 5 Numbness in Feet, But No Diabetes? Here s What Else It Could Be 7 Proper Shoes For Diabetics 9 How to Treat and Prevent a Diabetic Foot Ulcer
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
PALLIATIVE WOUND CARE
 PALLIATIVE WOUND CARE Scott Bolhack, MD, FACP President/CEO TLC HealthCare Companies Learning Objectives: Describe the aspects of palliative wound care.. Demonstrate palliative practices used in the care
PALLIATIVE WOUND CARE Scott Bolhack, MD, FACP President/CEO TLC HealthCare Companies Learning Objectives: Describe the aspects of palliative wound care.. Demonstrate palliative practices used in the care
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Diabetes-Diabetes Mellitus About one in five people with diabetes will enter the hospital for foot problems. DIABETIC FOOT PROBLEMS by Robert
 Diabetes-Diabetes Mellitus About one in five people with diabetes will enter the hospital for foot problems. DIABETIC FOOT PROBLEMS by Robert Frykberg, DPM Foot problems are leading causes of hospitalization
Diabetes-Diabetes Mellitus About one in five people with diabetes will enter the hospital for foot problems. DIABETIC FOOT PROBLEMS by Robert Frykberg, DPM Foot problems are leading causes of hospitalization
Surgical Off-loading. Reiber et al Goals of Diabetic Foot Surgery 4/28/2012. The most common causal pathway to a diabetic foot ulceration
 Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Education Module. Application of Compression Therapy for the Management of Venous and Mixed Venous/Arterial Insufficiency
 Developed by the British Columbia Provincial Nursing Skin and Wound Committee in collaboration with Wound Clinicians from: / Education Module Application of Compression Therapy for the Management of Venous
Developed by the British Columbia Provincial Nursing Skin and Wound Committee in collaboration with Wound Clinicians from: / Education Module Application of Compression Therapy for the Management of Venous
ORTHOTI MANAGEMENT OF DIABETIC FEET. Tarun Kumar Kulshreshtha, Clinical Prosthetist & Orthotist, Guest Facutly, University of Delhi, New Delhi, India
 ORTHOTI MANAGEMENT OF DIABETIC FEET Tarun Kumar Kulshreshtha, Clinical Prosthetist & Orthotist, Guest Facutly, University of Delhi, New Delhi, India INTRODUCTION Diabetic Melitus is a group of metabolic
ORTHOTI MANAGEMENT OF DIABETIC FEET Tarun Kumar Kulshreshtha, Clinical Prosthetist & Orthotist, Guest Facutly, University of Delhi, New Delhi, India INTRODUCTION Diabetic Melitus is a group of metabolic
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
EDUCATION. Peripheral Artery Disease
 EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #127 (NQF 0416): Diabetes Mellitus: Diabetic Foot and Ankle Care, Ulcer Prevention Evaluation of Footwear National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL
Quality ID #127 (NQF 0416): Diabetes Mellitus: Diabetic Foot and Ankle Care, Ulcer Prevention Evaluation of Footwear National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL
Our Vision NADA BoD Strategic Planning Session -
 Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA
 Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Case 1. July 14, th week wound gel 3 cm x 2.5 cm = 7.5 cm². May 25, st wound gel on 290 days PI treatment 4 cm x 2.4 cm = 9.
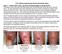 2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 6 Roller Bandages. LESSON ASSIGNMENT Paragraphs 6-1 through 6-10. LESSON OBJECTIVES After completing this lesson, you should be able to: 6-1. Identify the functions of roller bandages.
LESSON ASSIGNMENT LESSON 6 Roller Bandages. LESSON ASSIGNMENT Paragraphs 6-1 through 6-10. LESSON OBJECTIVES After completing this lesson, you should be able to: 6-1. Identify the functions of roller bandages.
Case Study 2 - Mr J. Medical history
 Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
Index. Foot Ankle Clin N Am 11 (2006) Note: Page numbers of article titles are in boldface type.
 Foot Ankle Clin N Am 11 (2006) 865 869 Index Note: Page numbers of article titles are in boldface type. A Alpha-lipoic acid, in diabetic neuropathy, 764 Amputation(s), lower-extremity, in diabetes, 791
Foot Ankle Clin N Am 11 (2006) 865 869 Index Note: Page numbers of article titles are in boldface type. A Alpha-lipoic acid, in diabetic neuropathy, 764 Amputation(s), lower-extremity, in diabetes, 791
INTERIOR DESIGN: Optimize Your Environment for Healing or Preventing Skin Breakdown. While the idea is not new, the term
 INTERIOR DESIGN: Optimize Your Environment for Healing or Preventing Skin Breakdown By Heather L. Orsted, RN, BN, ET, MSc and Sue Rosenthal, BA, MA INTERIOR DESIGN is a concept that is useful for both
INTERIOR DESIGN: Optimize Your Environment for Healing or Preventing Skin Breakdown By Heather L. Orsted, RN, BN, ET, MSc and Sue Rosenthal, BA, MA INTERIOR DESIGN is a concept that is useful for both
Address: Left Leg. other: Nails: thick yellow brittle fungus abnormal thick yellow brittle fungus abnormal
 South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
Velcro Compression Devices
 Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
Velcro Compression Devices Joseph A. Caprini, MD, MS, FACS, RVT, FACCWS Louis W. Biegler Chair of Surgery NorthShore University HealthSystem, Evanston, IL Clinical Professor of Surgery University of Chicago
Care of the Diabetic Patient
 Care of the Diabetic Patient Aarti Deshpande, CPO Clinic Manager Zuckerberg San Francisco General Department of Orthopaedic Surgery University of California, San Francisco March 16, 2017 Diabetes Diabetes
Care of the Diabetic Patient Aarti Deshpande, CPO Clinic Manager Zuckerberg San Francisco General Department of Orthopaedic Surgery University of California, San Francisco March 16, 2017 Diabetes Diabetes
Person s Name: ID Number: Date:
 South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
South West Regional Wound Care Program Person s Name: ID Number: Interdisciplinary Diabetic/Neuropathic Foot Assessment Form MEDICAL HISTORY: Question Year diabetes diagnosed: Characteristics of onset
