Chapter 17. Lecture Outline. See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes.
|
|
|
- Justina Reed
- 5 years ago
- Views:
Transcription
1 Chapter 17 Lecture Outline See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
2 I. Structure and Function of the Kidneys
3 A. Kidney Functions 1. Regulation of the extracellular fluid environment in the body, including: a. Volume of blood plasma (affects blood pressure) b. Wastes c. Electrolytes d. ph
4 B. Gross structure of the urinary system 1. Introduction a. Urine made in the kidney drains into the renal pelvis, then down the ureter to the urinary bladder. b. It passes from the bladder through the urethra to exit the body. c. Urine is transported using.
5 Organs of the urinary system Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Inferior vena cava Renal artery Renal vein Kidney Renal vein Renal artery Abdominal aorta Ureter Urinary bladder Urethra
6 2. Kidney Structure a. The kidney has two distinct regions: 1) Renal cortex 2) Renal medulla, made up of renal pyramids and columns b. Each pyramid drains into a minor calyx major calyx renal pelvis.
7 Radiograph of the urinary system Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Twelfth thoracic vertebra Twelfth rib Minor calyx Renal pelvis Kidney Ureter Urinary bladder SPL/Photo Researchers
8 C. Control of Micturition 1. Detrusor muscles line the wall of the urinary bladder. a. Gap junctions connect smooth muscle cells. b. Innervated by parasympathetic neurons, which release acetylcholine onto muscarinic ACh receptors 2. Sphincters surround urethra. a. Internal urethral sphincter: smooth muscle b. External urethral sphincter: skeletal muscle
9 Control of Micturition, cont 3. Stretch receptors in the bladder send information to S2 S4 regions of the spinal cord. a. These neurons normally inhibit parasympathetic nerves to the detrusor muscles, while somatic motor neurons to the external urethral sphincter are stimulated. b. Called the guarding reflex c. Prevents involuntary emptying of bladder
10 Control of Micturition, cont 4. Stretch of the bladder initiates the voiding reflex. a. Information about stretch passes up the spinal cord to the micturition center of the. b. Parasympathetic neurons cause detrusor muscles to contract rhythmically c. Inhibition of sympathetic innervation of the internal urethral sphincter causes it to relax. d. Person feels the need to urinate and can control when with external urethral sphincter.
11 D. Microscopic Kidney Structure 1. : functional unit of the kidney a. Each kidney has more than a million nephrons. b. Nephron consists of small tubules and associated blood vessels. c. Blood is filtered, fluid enters the tubules, is modified, then leaves the tubules as urine
12 Kidney Structure Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Renal cortex Renal medulla Renal pyramid Minor calyx Major calyx Renal cortex Nephron Renal column Renal pelvis I Renal artery Renal vein Renal medulla Ureter Renal papilla (a) Renal papilla Minor calyx Glomerular capsule (b) Distal convoluted tubule Collecting duct Proximal convoluted tubule Loop of Henle (c)
13 2. Renal Blood Vessels Renal artery Interlobar arteries Arcuate arteries Interlobular arteries Afferent arterioles Glomerulus Efferent arterioles Peritubular capillaries Interlobular veins Arcuate veins Interlobar veins Renal vein Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Interlobular artery and vein Renal cortex Arcuate artery and vein Interlobar artery and vein Renal medulla Renal artery Renal pelvis Renal vein Ureter
14 3. Nephron Tubules a. Glomerular (Bowman s) capsule surrounds the glomerulus. Together, they make up the. a. Filtrate produced in renal corpuscle passes into the. b. Next, fluid passes into the descending and ascending limbs of the. c. After the loop of Henle, fluid passes into the. d. Finally, fluid passes into the. e. The fluid is now urine and will drain into a minor calyx.
15 Nephron Tubules & Associated Blood Vessels Glomerulus Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Peritubular capillaries Distal convoluted tubule Glomerular capsule Efferent arteriole Afferent arteriole Interlobular artery Proximal convoluted tubule Interlobular vein Arcuate artery and vein Interlobar artery and vein Nephron loop (of Henle) Descending limb Ascending limb Peritubular capillaries (vasa recta) Collecting duct
16 4. Two Types of Nephrons a. Juxtamedullary: better at making concentrated urine b. Cortical Cortical nephron Juxtamedullary nephron (a) Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Renal cortex Glomerulus Renal medulla Blood flow (b) Collecting duct
17 II. Glomerular Filtration
18 A. Glomerular Corpuscle 1. Capillaries of the glomerulus are fenestrated. a. Large pores allow water and solutes to leave but not blood cells and plasma proteins. 2. Fluid entering the glomerular capsule is called filtrate
19 Glomerular Corpuscle, cont 3. Filtrates must pass through: a. Capillary fenestrae b. Glomerular basement membrane c. Visceral layer of the glomerular capsule composed of cells called podocytes with extensions called pedicels
20 Glomerular Capillaries & Capsule Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Podocyte cell body Primary process of podocyte Branching pedicels Professor P.M. Motta and M. Sastellucci/SPL/Photo Researchers
21 Glomerular Corpuscle & Filtration Barrier Afferent arteriole Blood flow Efferent arteriole Parietal layer of glomerular capsule Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Glomerulus Proximal convoluted tubule Glomerular (Bowman s) capsule Podocyte of visceral layer of glomerular capsule Filtrate Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Slit diaphragm Foot processes Fenestrae Pedicel (foot process) Basement membrane Fenestrae Capillary endothelium Glomerular basement membrane Slit diaphragm Filtration slits Plasma Capillary lumen Erythrocyte Fenestra Podocyte foot process Donald Fawcett & D. Friend/Visuals Unlimited, Inc
22 Glomerular Corpuscle, cont d. Slits in the pedicels called slit diaphragm pores are the major barrier for the filtration of plasma proteins. 1) Defect here causes proteinuria = proteins in urine. 2) Some albumin is filtered out but is reabsorbed by active endocytosis.
23 B. Glomerular Ultrafiltrate 1. Fluid in glomerular capsule gets there via hydrostatic pressure of the blood, colloid osmotic pressure, and very permeable capillaries. 2. These forces produce a net filtration pressure of about 10mmHg
24 Formation of Glomerular Ultrafiltrate Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Glomerular (Bowman s) capsule Protein Afferent arteriole Glomerular ultrafiltrate Other solutes Efferent arteriole
25 3. Filtration Rates a. Glomerular filtration rate (GFR): volume of filtrate produced by both kidneys each minute = ml. 1) 180 L/day (~45 gal) 2) Total blood volume is filtered every 40 minutes 3) Most must be reabsorbed immediately
26 C. Regulation of Glomerular Filtration Rate 1. Vasoconstriction or dilation of afferent arterioles changes filtration rate. a. Extrinsic regulation via sympathetic nervous system b. Intrinsic regulation via signals from the kidneys; called renal autoregulation
27 2. Sympathetic Nerve Effects a. In a fight/flight reaction, there is vasoconstriction of the afferent arterioles. b. Helps divert blood to heart and muscles c. Urine formation decreases to compensate for the drop in blood pressure
28 Sympathetic Nerve Effects Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Stimuli Blood pressure Exercise Baroreceptor reflex Sympathetic nerve activity Cardiac output Vasoconstriction of afferent arterioles in kidneys Vasoconstriction in skin, GI tract GFR Total peripheral resistance Urine production Blood volume Negative feedback corrections
29 3. Renal Autoregulation a. GFR is maintained at a constant level even when blood pressure (BP) fluctuates greatly. 1) Afferent arterioles dilate if BP < 70. 2) Afferent arterioles constrict if BP > normal. b. Myogenic constriction: Smooth muscles in arterioles sense an increase in blood pressure.
30 Renal Autoregulation, cont c. Tubuloglomerular feedback: Cells in the ascending limb of the loop of Henle called sense a rise in water and sodium as occurs with increased blood pressure (and filtration rate). 1) They send a chemical signal (ATP) to constrict the afferent arterioles.
31 Regulation of Glomerular Filtration Rate
32 III. Reabsorption of Salt and Water
33 A. Introduction 1. return of filtered molecules to the blood L of water is filtered per day, but only 1 2 L is excreted as urine. a. This will increase when well hydrated and decrease when dehydrated. b. A minimum 400 ml must be excreted to rid the body of wastes = obligatory water loss. c. 85% of reabsorption occurs in the proximal tubules and descending loop of Henle. This portion is unregulated.
34 Filtration and Reabsorption Reabsorption Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Filtration Glomerular (Bowman s) capsule Glomerulus
35 B. Reabsorption in the Proximal Tubule 1. The osmolality of filtrate in the glomerular capsule is equal to that of blood plasma (isoosmotic). 2. Na + is actively transported out of the filtrate into the peritubular blood to set up a concentration gradient to drive osmosis.
36 3. Active Transport a. Cells of the proximal tubules are joined by tight junctions on the apical side (facing inside the tubule). b. The apical side also contains microvilli. c. These cells have a lower Na + concentration than the filtrate inside the tubule due to Na + /K + pumps on the basal side of the cells and low permeability to Na +. d. Na + from the filtrate diffuses into these cells and is then pumped out the other side.
37 4. Passive Transport a. The pumping of sodium into the interstitial space attracts negative Cl out of the filtrate. b. Water then follows Na + and Cl into the tubular cells and the interstitial space. c. The salts and water diffuses into the peritubular capillaries.
38 Salt and Water Reabsorption in the Proximal Tubule Cl transport (passive) Reabsorption Na + transport (active) Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. H 2 O follows salt by osmosis Filtration Glomerular (Bowman s) capsule Fluid reduced to 1 / 3 original volume, but still isosmotic
39 5. Significance of proximal tubule reabsorption a. 65% of the salt and water is reabsorbed, but that is still too much filtrate b. An additional 20% of water is reabsorbed through the descending limb of the Loop of Henle. 1) Happens continuously and is unregulated 2) The final 15% of water (~27 L) is absorbed later in the nephron under hormonal control. 3) Fluid entering loop of Henle is isotonic to extracellular fluids.
40 C. Countercurrent Multiplier System 1. Water cannot be actively pumped out of the tubes, and it will not cross if isotonic to extracellular fluid. a. The structure of the loop of Henle allows for a concentration gradient to be set up for the osmosis of water. b. The ascending portion sets up this gradient.
41 2. Ascending Limb of the Loop of Henle a. Salt (NaCl) is actively pumped into the interstitial fluid from the thick segment of the limb 1) Movement of Na + down its electrochemical gradient from filtrate into tubule cells powers the secondary active transport of Cl and K +. 2) Na + is moved into interstitial space via Na + /K + pump. Cl follows Na + passively due to electrical attraction, and K + passively diffuses back into filtrate.
42 Transport of Ions in the Ascending Limb of the Loop of Henle Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Ascending limb of loop Filtrate (tubular lumen) Interstitial space Apical membrane 2 Cl 2 Cl 2 Na + Na + ATP ADP Na + 1 Na + K + K + K + K + 3 K + Cl Cl K + Cl K + Cl Basolateral membrane
43 Ascending Limb of the Loop of Henle, cont b. Walls are not permeable to water, so osmosis cannot occur from the ascending part of the loop. c. Surrounding interstitial fluid becomes increasingly solute concentrated at the bottom of the tube. d. Tubular fluid entering the ascending loop of Henle becomes more hypotonic as it ascends the loop.
44 3. Descending Limb of the Loop of Henle a. Is not permeable to salt but is permeable to water b. Water is drawn out of the filtrate and into the interstitial space where it is quickly picked up by capillaries. c. As it descends, the fluid becomes more solute concentrated. 1) This is perfect for salt transport out of the fluid in the ascending portion.
45 1, Countercurrent Multiplier System Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. 300 mosm Loop of Henle Cortex Medulla 2 H 2 O H 2 O H 2 O ,000 Na + Cl Na + Cl Na + Cl Na + Cl 1 Na + Cl Na + Cl Na + Cl Na + Cl Capillary 3 1,400 Descending limb Passively permeable to water Ascending limb Active transport of Na +, Cl follows passively; impermeable to water
46 4. Countercurrent Multiplication a. Positive feedback mechanism is created between the two portions of the loop of Henle. 1) The more salt the ascending limb removes, the saltier the fluid entering it will be (due to loss of water in descending limb).
47 b. Steps of countercurrent mechanism 1) Interstitial fluid is hypertonic due to NaCl pumped out of the ascending limb 2) Water leaves descending limb by osmosis, making the filtrate hypertonic going into the ascending limb 3) More NaCl in the ascending limb can now be pumped out into the interstitial fluid 4) The greater concentration of the interstitial fluid draws more water from the descending limb 5) Filtrate in ascending limb now more concentrated 6) Continues until the maximum NaCl concentration of the inner medulla is reached.
48 c. Vasa Recta 1) Specialized blood vessels around loop of Henle, which also have a descending and ascending portion 2) Help create the countercurrent system because they take in salts in the descending region but lose them again in the ascending region a) Keep salts in the interstitial space
49 Vasa Recta, cont 3) High salt concentration (oncotic pressure) at the beginning of the ascending region pulls in water, which is removed from the interstitial space. a) Also keeps salt concentration in the interstitial space high 4) There are also urea transporters and aquaporins to aid in the countercurrent exchanges
50 Countercurrent Exchange in the Vasa Recta Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Blood flow Capillary 300 Tissue fluid Renal cortex Outer renal medulla ,075 Inner renal medulla 1,025 1,200 Diffusion of NaCl and urea Osmosis of water
51 5. Effects of Urea a. Urea is a waste product of protein metabolism b. Contributes to countercurrent system 1) Transported out of collecting duct and into interstitial fluid 2) Diffuses back into ascending limb and cycles around continuously 3) Helps set up solute concentration gradients
52 Role of Urea in Urine Concentration Cortex Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Distal tubule H 2 O Outer medulla H 2 O Collecting duct H 2 O Inner medulla H 2 O H 2 O H 2 O NaCl Urea Water Loop of Henle H 2 O
53 Renal Tubule Transport Properties
54 Renal Tubule Osmolality Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Proximal tubule Distal tubule Collecting duct Cortex Vasa recta H 2 O Outer medulla H 2 O Descending limb of loop H 2 O Ascending limb of loop H 2 O Inner medulla 1,200 1,200 1,200 1,400 1,400 1,400 H 2 O
55 D. Collecting Duct and ADH 1. Last stop in urine formation 2. Impermeable to NaCl but permeable to water a. Also influenced by hypertonicity of interstitial space water will leave via osmosis if able to b. Permeability to water depends on the number of aquaporin channels in the cells of the collecting duct c. Availability of aquaporins determined by ADH (antidiuretic hormone)
56 Collecting Duct and ADH, cont 3. ADH binds to receptors on collecting duct cells camp Protein kinase Vesicles with aquaporin channels fuse to plasma membrane. a) Water channels are removed without ADH. 4. ADH is produced by neurons in the hypothalamus but stored and released from the posterior pituitary gland a) Release stimulated by an increase in blood osmolality
57 ADH Stimulation of Aquaporin Channels Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Extracellular fluid Cytoplasm ADH Vesicle Aquaporin channels Fusion of exocytotic vesicle (a) No ADH (b) ADH No ADH Plasma membrane with aquaporin channels (d) Formation of endocytotic vesicle (c)
58 Homeostasis of Plasma Concentration by ADH Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Stimulus Stimulus Low water intake (dehydration) High water intake (over-hydration) Plasma osmolality Plasma osmolality Osmoreceptors in hypothalamus Sensor Integrating center Effector Posterior pituitary ADH ADH Kidneys Water reabsorption Water reabsorption Negative feedback correction Less water excreted in urine More water excreted in urine Negative feedback correction
59 ADH Secretion and Action
60 IV. Renal Plasma Clearance
61 A. Transport processes affecting renal clearance 1. Kidneys must also remove excess ions and wastes from the blood. a. Sometimes called renal clearance b. Filtration in the glomerular capsule begins this process. c. Reabsorption returns some substances to the blood (decreases renal clearance) d. Secretion finishes the process when substances are moved from the peritubular capillaries into the tubules. (increases renal clearance)
62 2. Excretion Rate a. Excretion rate = (filtration rate + secretion rate) reabsorption rate b. Used to measure glomerular filtration rate (GFR), an indicator of renal health
63 Secretion is the reverse of reabsorption Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Secretion Reabsorption Filtration Excretion
64 3. Secretion of Drugs a. Membrane carriers specific to foreign substances transport them into the tubules. b. Called organic anion transporters (OATs) or organic cation transporters (OCTs) c. Carriers are polyspecific overlap in function d. Very fast; may interfere with action of therapeutic drugs
65 B. Clearance of Inulin 1. Inulin is a compound found in garlic, onion, dahlias, and artichokes. a. Great marker of glomerular filtration rate because it is filtered but not reabsorbed or secreted V X U GFR = P V = rate of urine formation U = inulin concentration in urine P = inulin concentration in plasma
66 Renal Clearance of Inulin Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Inulin (a) (b) Renal artery with inulin To peritubular capillaries Renal vein inulin concentration lower than in renal artery (c) Ureter urine containing all inulin that was filtered
67 2. Renal Plasma Clearance Calculation a. Volume of plasma from which a substance is completely removed by the kidneys in 1 minute 1) Inulin is filtered only. Clearance = GFR 2) Anything that can be reabsorbed has a clearance < GFR. 3) If a substance is filtered and secreted, it will have a clearance > GFR. 4) Renal plasma clearance uses same formula as GFR. b. Clearance of urea is less than GFR means some is reabsorbed
68 Renal Plasma Clearance
69 C. Clearance of PAH 1. Not all blood delivered to the glomeruli is filtered in each pass, so blood must make several passes to completely clear a substance. 2. PAH (para-aminohippuric acid) is an exogenous molecule injected for measurement of total renal blood flow. 3. Substances not filtered must be secreted into the tubules by active transport from the peritubular capillaries 4. All PAH in the peritubular capillaries will be secreted by OATs, so the time it takes to clear all PAH injected indicates blood flow to these capillaries.
70 Renal Clearance of PAH Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. PAH Filtration (a) To peritubular capillaries Renal artery containing PAH Renal vein almost no PAH (c) Peritubular capillaries To renal vein Filtration plus secretion (d) Ureter urine containing almost all PAH that was in renal artery
71 D. Reabsorption of Glucose 1. Glucose (and amino acids) is easily filtered out into the glomerular capsule 2. Completely reabsorbed in the proximal tubule via secondary active transport with sodium, facilitated diffusion, and simple diffusion
72 Mechanism of Reabsorption in the proximal tubule Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Lumen of kidney tubule Glucose Apical membrane Na + 1 Cotransport Proximal tubule cell Basolateral membrane ATP ADP K + 3 Facilitated diffusion Primary active transport 2 Simple diffusion Glucose K + Na + Capillary
73 Reabsorption of Glucose, cont 3. Glucose/Na + cotransporters have a transport maximum (T m ). a. If there is too much glucose in the filtrate, it will not be completely reabsorbed because all the carriers are in use (saturated). b. Extra glucose spills over into the urine = glycosuria and is a sign of diabetes mellitus. c. Extra glucose in the blood also results in decreased water reabsorption and possible dehydration.
74 V. Renal Control of Electrolyte and Acid-Base Balance
75 A. Introduction 1. Kidneys match electrolyte (Na +, K +, Cl, bicarbonate, phosphate) excretion to ingestion. a. Control of Na + levels is important in blood pressure and blood volume. b. Control of K + levels is important in healthy skeletal and cardiac muscle activity. c. Aldosterone plays a big role in Na + and K + balance.
76 B. Role of Aldosterone in Na + /K + Balance 1. About 90% of filtered Na + and K + is reabsorbed early in the nephron. a. This is not regulated. 2. An assessment of what the body needs is made, and aldosterone controls additional reabsorption of Na + and secretion of K + in the distal tubule and collecting duct.
77 3. Potassium Secretion a. Aldosterone independent response: Increase in blood K + triggers an increase in the number of K + channels in the cortical collecting duct. 1) When blood K + levels drop, these channels are removed. b. Aldosterone-dependent response: Increase in blood K + triggers adrenal cortex to release aldosterone. 1) This increases K + secretion in the distal tubule and collecting duct.
78 Potassium is Reabsorbed and Secreted Filtered Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Reabsorbed K + Secreted K + K + Cortical portion of collecting duct Proximal convoluted tubule Excreted
79 c. Sodium and Potassium 1) Increases in sodium absorption drive extra potassium secretion. 2) Due to: a) Potential difference created by Na + reabsorption driving K + through K + channels b) Stimulation of renin-angiotensin-aldosterone system by water and Na + in filtrate c) Increased flow rates bend cilia on the cells of the distal tubule, resulting in activation of K + channels
80 4. Control of Aldosterone Secretion a. A rise in blood K + directly stimulates production of aldosterone in the adrenal cortex. b. A fall in blood Na + indirectly stimulates production of aldosterone via the renin- angiotensinaldosterone system.
81 C. Juxtaglomerular Apparatus 1. Located where the afferent arteriole comes into contact with the distal tubule Glomerular capsule Glomerulus Region of the juxtaglomerular apparatus Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Glomerulus Afferent arteriole Efferent arteriole Distal tubule Afferent arteriole Granular cells Efferent arteriole Macula densa Juxtaglomerular apparatus (a) Loop of Henle (b) Thick ascending limb
82 Juxtaglomerular Apparatus, cont 2. A decrease in plasma Na + results in a fall in blood volume. a. Sensed by juxtaglomerular apparatus b. Granular cells secrete renin into the afferent arteriole. c. This converts angiotensinogen into angiotensin I. d. Angiotensin-converting enzyme (ACE) converts this into angiotensin II.
83 Juxtaglomerular Apparatus 3. Stimulates adrenal cortex to make aldosterone a. Promotes the reabsorption of Na + from cortical collecting duct b. Promotes secretion of K + c. Increases blood volume and raises blood pressure
84 4. Regulation of Renin Secretion a. Low salt levels result in lower blood volume due to inhibition of ADH secretion. 1) Less water is reabsorbed in collecting ducts and more is excreted in urine. b. Reduced blood volume is detected by granular cells that act as baroreceptors. They then secrete renin. 1) Granular cells are also stimulated by sympathetic innervation from the baroreceptor reflex.
85 Homeostasis of Plasma Na + Sensor Integrating center Effector Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Stimulus Low Na + intake Negative feedback correction Na + retention in blood Low plasma Na + concentration Na + reabsorption in cortical collecting duct Hypothalamus Aldosterone Posterior pituitary Adrenal cortex ADH Angiotensin II Water reabsorption in collecting ducts Renin Urine volume Blood volume Juxtaglomerular apparatus Sympathetic nerve activity
86 5. Macula Densa a. Part of the distal tubule that forms the juxtaglomerular apparatus b. Sensor for tubuloglomerular feedback needed for regulation of glomerular filtration rate 1) When there is more Na + and H 2 O in the filtrate, a signal is sent to the afferent arteriole to constrict limiting filtration rate. 2) Controlled via negative feedback
87 Macula Densa, cont c. When there is more Na + and H 2 O in the filtrate, a signal is sent to the afferent arteriole to inhibit the production of renin. 1) This results in less reabsorption of Na +, allowing more to be excreted. 2) This helps lower Na + levels in the blood.
88 D. Atrial Natriuretic Peptide 1. Increases in blood volume also increase the release of atrial natriuretic peptide hormone from the atria of the heart when atrial walls are stretched. 2. Stimulates kidneys to excrete more salt and therefore more water 3. Decreases blood volume and blood pressure
89 Regulation of Renin and Aldosterone Secretion
90 E. Relationship Between Na +, K +, and H + 1. Reabsorption of Na + stimulates the secretion of other positive ions; K + and H + compete. 2. Acidosis stimulates the secretion of H + and inhibits the secretion of K + ions; acidosis can lead to hyperkalemia. 3. Alkalosis stimulates the secretion and excretion of more K Hyperkalemia stimulates the secretion of K + and inhibits secretion of H + ; can lead to acidosis
91 Reabsorption of Na + and Secretion of K +, and H + Blood Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Peritubular capillaries Na + K + or H + Na + Na + Na + Na + Na + Na + K + /H + Distal tubule Cortical collecting duct Na + K + K + H + Na+ Na + Na + K + H + K + Na + Ascending limb of Henle s loop Medullary collecting duct
92 F. Acid-Base Regulation 1. Kidneys maintain blood ph by reabsorbing bicarbonate and secreting H + ; urine is thus acidic. 2. Proximal tubule uses Na + /H + pumps to exchange Na + out and H + in. a. Some of the H + brought in is used for the reabsorption of bicarbonate. b. Antiport secondary active transport
93 Acid-Base Regulation, cont 3. Bicarbonate cannot cross the inner tubule membrane so must be converted to CO 2 and H 2 O using carbonic anhydrase. a. Bicarbonate + H + carbonic acid b. Carbonic acid (w/ carbonic anhydrase) H 2 O + CO 2 c. CO 2 can cross into tubule cells, where the reaction reverses and bicarbonate is made again. d. This diffuses into the interstitial space.
94 Acidification of the Urine Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. HCO 3 Na + Na + HCO 3 Proximal tubule CA H 2 CO 3 H 2 O + CO 2 Na + ATPase Distal tubule K + Blood H + H + Filtration Lumen Na + HCO 3 + H + CA Na + H + H + 2 O CO 2 2 HPO H 2 CO 4 3 NH 3 H + H 2 PO 4 NH 4 + Proximal tubule cell
95 Acid-Base Regulation, cont 4. Aside from the Na + /H + pumps in the proximal tubule, the distal tubule has H + ATPase pumps to increase H + secretion.
96 5. ph Disturbances a. Kidneys can help compensate for respiratory problems b. Alkalosis: Less H + is available to transport bicarbonate into tubule cells, so less bicarbonate is reabsorbed; extra bicarbonate secretion compensates for alkalosis.
97 ph Disturbances, cont c. Acidosis: Proximal tubule can make extra bicarbonate through the metabolism of the amino acid glutamine. 1) Extra bicarbonate enters the blood to compensate for acidosis. 2) Ammonia stays in urine to buffer H +.
98 Disturbances of Acid-Base Balance
99 G. Urinary Buffers 1. Nephrons cannot produce urine with a ph below To increase H + secretion, urine must be buffered. a. Phosphates and ammonia buffer the urine. b. Phosphates enter via filtration. c. Ammonia comes from the deamination of amino acids.
100 VI. Clinical Applications
101 A. Use of Diuretics 1. Used clinically to control blood pressure and relieve edema (fluid accumulation) a. Diuretics increase urine volume, decreasing blood volume and interstitial fluid volume. b. Many types act on different portions of the nephron.
102 2. Types of Diuretics a. Loop diuretics: most powerful; inhibit salt transport out of ascending loop of Henle 1) Example: Lasix 2) Can inhibit up to 25% of water reabsorption b. Thiazide diuretics: inhibit salt transport in distal tubule 1) Can inhibit up to 8% of water reabsorption c. Carbonic anhydrase inhibitors: much weaker; inhibit water reabsorption when bicarbonate is reabsorbed 1) Also promote excretion of bicarbonate
103 Types of Diuretics, cont d. Osmotic diuretics: reduce reabsorption of water by adding extra solutes to the filtrate 1) Example: Mannitol 2) Can occur as a side effect of diabetes e. Potassium-sparing diuretics: Aldosterone antagonists block reabsorption of Na + and secretion of K +.
104 Actions of Classes of Diuretics
105 Sites of Action of Clinical Diuretics Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Carbonic anhydrase inhibitors Proximal convoluted tubule Thick ascending limb Distal convoluted tubule Thiazide diuretics Na + NaCl Cortex Amino acids Glucose HCO 3 3, PO 4 Passive Potassium-sparing diuretics H 2 O (with ADH) H 2 O no ADH Cortical collecting duct Glomerulus Loop diuretics K + Na + Collecting duct Medulla Increasing NaCl and urea concentrations H 2 O H 2 O Descending limb Ascending limb H 2 O (with ADH) H 2 O no ADH Medullary collecting duct NaCl Passive Urea
106 B. Renal Function Tests 1. PAH and inulin clearance a. Can diagnose nephritis or renal insufficiency 2. Urinary albumin excretion rate: detects abovenormal albumin excretion a. Called microalbuminuria b. Signifies renal damage due to hypertension or diabetes 3. Proteinuria: overexcretion of proteins; signifies nephrotic syndrome
107 C. Kidney Diseases 1. Acute Renal Failure a. Ability of kidneys to regulate blood volume, ph, and solute concentrations deteriorates in a matter of hours/days. b. Usually due to decreased blood flow through kidneys due to: 1) Atherosclerosis of renal arteries 2) Inflammation of renal tubules 3) Use of certain drugs (NSAIDs)
108 2. Glomerulonephritis a. Inflammation of the glomerulus b. Autoimmune disease with antibodies produced in response to streptococcus infection c. Many glomeruli are destroyed, and others are more permeable to proteins. d. Loss of proteins from blood reduces blood osmotic pressure and leads to edema.
109 3. Renal Insufficiency a. Any reduction in renal activity b. Can be caused by glomerulonephritis, diabetes, atherosclerosis, or blockage by kidney stones c. Can lead to high blood pressure, high blood K + and H +, and uremia = urea in the blood. d. Patients with uremia are placed on a dialysis machine to clear blood of these solutes.
110 4. Dialysis a. Artificial kidney b. Hemodialysis blood cleansed of wastes as it passes through dialysis fluid c. CAPD continuous ambulatory peritoneal dialysis dialysis fluid introduced to the abdominal cavity where wastes can pass out of abdominal blood vessels; fluid is then pumped out of the abdominal cavity
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Urinary System Review Questions:
 Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Chapter 16 Lecture Outline
 Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
osmoregulation mechanisms in gills, salt glands, and kidneys
 Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Chapter 23. The Nephron. (functional unit of the kidney
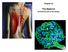 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Chapter 11 Lecture Outline
 Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Lab Activity 31. Anatomy of the Urinary System. Portland Community College BI 233
 Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Figure 26.1 An Introduction to the Urinary System
 Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Chapter 25: Urinary System
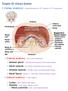 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
CHAPTER 25 URINARY. Urinary system. Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1. functions
 CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Waste Products & Kidney Function
 Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
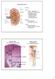 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Urinary System kidneys, ureters, bladder & urethra
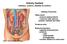 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
URINARY SYSTEM. Primary functions. Major organs & structures
 URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
URINARY SYSTEM CHAPTER 28 I ANATOMY OF THE URINARY SYSTEM. Student Name
 Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Copyright 2010 Pearson Education, Inc. Urinary System
 Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Urinary System. Chapter 17 7/19/11. Introduction
 7/19/11 Chapter 17 Urinary System Introduction A. The urinary system consists of two kidneys that filter the blood, two ureters, a urinary bladder, and a urethra to convey waste substances to the outside.
7/19/11 Chapter 17 Urinary System Introduction A. The urinary system consists of two kidneys that filter the blood, two ureters, a urinary bladder, and a urethra to convey waste substances to the outside.
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden
 Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Hill et al. 2004, Fig. 27.6
 Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
Unit #4 Waste and Excretion. The Kidneys
 Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
The Urinary System. Jim Swan
 The Urinary System Jim Swan These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best
The Urinary System Jim Swan These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best
Chapter 26 The Urinary System. Overview of Kidney Functions. External Anatomy of Kidney. External Anatomy of Kidney
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19](/thumbs/77/74887026.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
Func%ons of the Urinary System
 Func%ons of the Urinary System Excre%on Regula%on of blood volume Regula%on of blood pressure Regula%on of blood- solute concentra%on Regula%on of ph of extracellular fluid Regula%on of erythropoiesis
Func%ons of the Urinary System Excre%on Regula%on of blood volume Regula%on of blood pressure Regula%on of blood- solute concentra%on Regula%on of ph of extracellular fluid Regula%on of erythropoiesis
active transport of! Na. C. Tubular Reabsorption of Nutrients, Water, and Ions (p. 979; Fig )
 The Urinary System Outline 25.1 The kidneys have three distinct regions and a rich blood supply (pp. 963 965; Figs. 25.1 25.5) A. Location and External Anatomy (p. 963; Figs. 25.1 25.3) 1. The kidneys
The Urinary System Outline 25.1 The kidneys have three distinct regions and a rich blood supply (pp. 963 965; Figs. 25.1 25.5) A. Location and External Anatomy (p. 963; Figs. 25.1 25.3) 1. The kidneys
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
URINARY SYSTEM. These organs lie posterior or inferior to the. (membrane).
 URINARY SYSTEM I. INTRODUCTION Each kidney is made up of about a million tiny tubules called nephrons. Each nephron individually filters the blood and makes urine and it does the job completely, from start
URINARY SYSTEM I. INTRODUCTION Each kidney is made up of about a million tiny tubules called nephrons. Each nephron individually filters the blood and makes urine and it does the job completely, from start
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Collin College. BIOL Anatomy & Physiology WEEK 12. Urinary System INTRODUCTION. Main functions of the kidneys are
 Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
Urinary System (Anatomy & Physiology)
 Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Chapter 13 The Urinary System
 Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
