1. Recognize universal precautions and body substance isolation (BSI) procedures when performing an intravenous (IV) cannulation.
|
|
|
- Rebecca Scott
- 5 years ago
- Views:
Transcription
1 1 of 15 Intravenous Therapy for Prehospital Providers Objectives At the end of this lesson, the student should be able to: 1. Recognize universal precautions and body substance isolation (BSI) procedures when performing an intravenous (IV) cannulation. 2. Describe how to insert an IV cannula using anatomic landmarks. 3. Differentiate among the different solutions and intravenous cannulation devices used when administering intravenous cannulations for the management of trauma and medical emergencies. 4. Identify possible complications with IV therapy. Case Study You are dispatched to the home of an 82-year-old female who reported to the 911 dispatcher that she is burning up and feels dizzy. On arrival you are met by first responders who report that the patient was very confused when they arrived, but got a bit more alert when they put her on oxygen. Her current oxygen saturation is 96% on oxygen via nasal cannula at 6 L/min, her pulse is 140 beats per minute (BPM), her respirations are 20/min and her blood pressure (BP) is 68/50. The patient has a blood glucose level of 60 mg/dl. You estimate the patient s weight at 50 kg. Your general impression of the patient reveals an elderly lady sitting in the semi-fowler's position on her bed and looking very flushed and clammy. You take the patient s temporal artery temperature which is F. One of the EMTs with fire and rescue assists with the appropriate thermal management of the patient. The electrocardiogram (ECG) reveals a sinus tachycardia and no other abnormalities. You instruct your partner to gain IV access using an 18-gauge IV catheter, 15 dropper fluid administration set, and saline lock and to prepare an IV line with 1,000 ml of normal saline. Lung sounds are equal bilaterally with faint crackles on both sides. The patient has no allergies and is taking metoprolol, an antihypertensive medication 1, for hypertension. The patient reports that she ran out of pills two days ago and hasn t been to the pharmacy for a refill due to her current illness. The patient last ate or drank more than 24 hours ago. You instruct your partner to give a 250 ml bolus of normal saline and to administer IV D50 simultaneously to prevent any irritation of the vein. You further instruct your partner to pay close attention to the patient s breathing which may deteriorate if the patient cannot tolerate the IV fluid. Fire and rescue personnel points out that there is a blood stain with a yellowish tinge at the bottom of the bed. A quick head-to-toe survey reveals an infected laceration to the heel of her foot. The patient states that she stood on a garden rake a few days ago and didn t think anything of it. You also notice 2+ pitting edema in both ankles. At this point you decide to begin transport and move the patient to the ambulance. Transport to the nearest facility is 40 minutes. You reassess the vital signs and your findings are as follows: pulse 130 beats, respirations 19, breath sounds are the same as before and the BP is69/52. The patient continues to be a little bit confused and states that she is very thirsty. You administer an additional 250 ml of normal saline and reassess the blood pressure after 10 minutes which is still 69/52. You contact medical control who advises you to piggyback a vasopressor drip onto your IV to help elevate the blood pressure; you follow the instruction and perform a series of calculations to ensure the patient gets the correct dose which has to be correct to the microgram. You further calculate that at that rate the IV infusion will easily last for the 40minute transport time. You reassess the blood pressure and lung sounds and note that the BP has increased to a respectable 90/70 and the faint crackles you heard earlier have not gotten any worse. The patient has also become significantly more alert. The balance of the transport remains uneventful. Introduction IV therapy is one of the most fundamental and also most invasive skills of emergency medical services. Gaining access directly into a vein allows paramedics to quickly and effectively administer potentially lifesaving medications. Developing IV skills takes time, patience, and a lot of practice. The paramedic, equipped with a thorough knowledge of the anatomy and physiology relevant to IV therapy, expertise with the IV equipment, and a detailed pharmacological knowledge, can make a dramatic improvement on many conditions, such as shock, that might otherwise be fatal. There are only three types of patients who need an IV in the prehospital environment: those who need fluid replacement, those who might need fluid replacement, and those who need (or potentially need) IV medication administration. 2 IV therapy is also a controversial subject and although it is standard practice to gain IV access to keep vein open (TKVO) or to keep open (TKO), which IV fluid and how much of that fluid should be administered is continually being researched. 3 Too little fluid and the patient may progress into conditions such as irreversible shock or renal failure. Too much fluid and pulmonary edema or heart failure can occur. Once again the paramedic needs to find the sweet spot and administer just
2 2 of 15 enough of the right fluid. There are numerous guidelines on how long it should take to establish an IV line and the maximum number of attempts one should make before moving from peripheral veins to intraosseous (IO) or even central lines. Stay-and-play versus load-and-go is a decision that needs to be made early on in the treatment. Typically, the only times one should stay-and-play is when a patient is entrapped, you require assistance to move the patient (such as with bariatric patients), you need to stabilize life threats, you are performing CPR, you are waiting for air transport, or you need to prepare a patient for air transport. In general, an IV line should be established en route to hospital, unless there is a compelling reason such as the administration of life-saving medications that needs to happen on scene. This article will take you through the basics of IV therapy all the way through to IV therapy for some of the more complex trauma and medical conditions. Universal Precautions and Body Substance Isolation Universal precautions are defined as Protective measures that have traditionally been developed by the CDC (Centers for Disease Control) for use in dealing with objects, blood, body fluids, or other potential risks of communicable disease. 4 Body substance isolation (BSI) or standard precautions are defined as The term currently used to describe the infection control practices that will reduce the opportunity for exposure of providers in the daily care of patients; consider all body fluids, except sweat, to present a possible risk. 5 Considering these two definitions one realizes that the responsibility is to protect oneself, the patient, and others from the risk of possible infection. Before establishing a peripheral IV line, wash your hands with normal soap and water or use an alcohol rub. Generally, it is best to experiment with different types of soap and rubs as paramedics may experience difficulty in donning gloves after cleaning their hands. Hand hygiene must be maintained both before and after palpating a vein and inserting or adjusting an IV catheter. If you are establishing a peripheral IV line use clean gloves; if you are inserting a central or arterial line use sterile gloves. The insertion of central and arterial lines is beyond the scope of this article. Do not touch the insertion site after it has been sterilized unless you are using aseptic technique. 6 In order to reduce the chance of infection as much as possible, the upper extremities are preferred to the lower extremities for IV insertion. However, should the only IV location available be in a lower extremity, that IV should be relocated as soon as possible. 7 Peripheral venous catheters are inserted in the forearm or the hand and have a very low risk of bloodstream infection, but they can cause vein irritation with prolonged use. 8 The four major routes of infection via catheterization are: 1) existing skin organisms entered the injection site, traveled along the catheter and colonized the tip of the catheter; 2) the catheter or the catheter hub are contaminated directly by hands, fluids, or other devices; 3) (rarely) the catheter may act as a colonization point for an existing infection; and 4) the IV fluid given may itself be contaminated which will lead to infection. 9 Environmental factors will also influence the risk of infection. A patient being treated on a dirty bed or lying in the gutter may be more at risk than a patient being treated in the emergency department (ED). Depending on the condition of the patient you should wear eye protection or a face mask, N95 or N100 respirators, and a gown. 10 The CDC recommends the following strategies to prevent catheter-related infections: proper and ongoing education on the indications for IVs, that proper procedures are put in place to insert and maintain IV catheters, and that procedures that are implemented to prevent infection. 11 IV catheters, administration sets, and IV fluids are all packaged in sterile packages. As long as this package remains intact and is used before the expiration date on the packet then the item should be sterile. If any of the IV catheters, administration sets or IV fluids are removed but not used, they should be discarded appropriately. The CDC reports that approximately 385,000 sharps injuries occur per year to hospital employees (over 1,000 per day). 12 These injuries occur through the use of unsafe needle equipment and the improper use or disposal of sharps. Injuries are not usually caused by a result of negligence but from unsafe needles. Occupational Safety and Health Administration (OSHA) recommends the use of safer needles that have built in safety features such as needleless and spring-loaded or manual self-sheathing needles. In March 2000, the CDC estimated that 62 to 88 percent of all sharps injuries could have been prevented by using safer needles. 13 According to OSHA the characteristics of safety devices include: needleless devices, integration of safety features, easy and practical to use devices, reliable performance of devices, inability to deactivate safety features, devices that are not detrimental to patient care and are effective, and devices cleared by the Food and Drug Administration (FDA). The FDA further recommends that the safety feature provides a barrier between hands and the needle after use, requires hands to be behind the needle at all times, is integral to the device and not just an add-on, is in place before the needle is disassembled, remains in place after it is disposed of, and is simple enough to use with little or no training. 14
3 3 of 15 Sharps containers should always be available where sharps are used. These containers must also always be used in accordance with the manufacturer s guidelines and should only be filled to the maximum fill line. OSHA regulations stipulate that sharps containers must be closable, resistant to punctures, leak-proof on the sides and bottom, easily accessible, kept upright, not allowed to be filled past the maximum, clearly labeled in fluorescent orange or orange-red with contrasting letters as a biohazard, and the container must be colored red. 15 If you are inadvertently exposed to another person s blood or bodily fluids you should take the following steps: hand over treatment of the patient to a suitably qualified person (you are now also a patient); thoroughly wash the exposed area with soap and water (time is of the essence); and if the eyes are involved rinse them with cool, clean water for at least 20 minutes. Follow your local guidelines for exposure and infection control and comply with all medical instructions to ensure the chance of infection is minimized. 16 Inserting an IV Cannula After safety and BSI, discuss the treatment with the patient. Ask about allergies to the IV fluids, medications, tape, and the swabs that will be used to clean the injection site. Ask if he or she is a hard stick and if he or she has a preferred location for the IV. Prepare all the equipment for the IV cannulation beforehand including gloves, IV cannula, alcohol or iodine swabs, gauze, administration set, IV fluid, and tape or IV dressing. Remove the IV fluid and administration set from their sterile packaging. Move the roller clamp on the administration set to the top of the tubing and close the clamp. Tear the tape or prepare the dressing before you begin as this becomes a one-handed procedure later. 17 There are dozens of different makes and models of IV catheters. The most common styles used in the prehospital environment are over-the-needle catheters and butterfly catheters. 18 Earlier IV catheters did not have any safety features but designs today include retractable and self-sheathing needles. Catheters have different sizes indicated by a number followed by the word "gauge" or G (for example: 18-gauge or 18G). This objective focuses on the use of over-the-needle catheters (shown in Figure 1 below). The lower the gauge, the greater the internal diameter and the length of the catheter. In the prehospital environment 20G, 18G, 16G and 14G needles are most common, while 22G and smaller (down to 27G) and butterfly needles are usually used for pediatric patients. 19 The 20G and 18G are generally used for medical patients who do not require fluid replacement but may require IV medications and the IV line is established to keep the vein open (KVO) or to keep open (TKO). 20 The KVO rate is around 30 ml/hour 21 but local protocol and paramedic judgment must be taken into account. The 16G and 14G are used for trauma patients or those who require rapid fluid replacement. When using the larger gauge needles use proximal IV sites such as the external jugular or antecubital fossa. 22
4 4 of 15 Figure 1-20G, 18G, 16G and 14G Over-the-needle catheters 23 Different colors represent the sizes of the catheters and each size, under ideal gravity conditions, delivers a different flow per minute. The table below gives an example of flow rates: 24 Gauge Length (cm) ml/min Time to Flow 500 ml 24G :00 22G :17 20G :41 20G :20 20G :05 18G :45 18G :15 16G :16 16G :26 14G :28 16G to 24G BD Insyte Autoguard BC Shielded IV Catheter and B Braun Vasocan 14G Safety Flow Rates 25,26 Longer lengths but the same diameter takes slightly longer to deliver the same amount of fluid. A 20G will take almost three times as long as a 16G. It is important to take the size of the catheter into account when determining how much fluid to administer to a patient. Once a catheter has been chosen the next step is to set up the IV solution and the administration set. First, remove the chosen IV solution from its protective bag and inspect the IV solution for expiration, clarity, color, and sedimentation and squeeze it to test for minute leaks. IV bags usually have two ports: one for injecting medication into the bag (see Figure 3 ) and one for attaching the administration set. Remove the protective tab from the IV bag outlet port and do not touch the port or spike. Spike the IV bag ensuring that the spike goes all the way into the bag.
5 5 of 15 Figure 3 - IV Port In and Out Markers 27 Squeeze the drip chamber and fill it to the halfway mark. Open the roller clamp and allow the fluid to prime the set. Some administration sets require you to remove the cap on the end of the tubing for the fluid to flow; others have caps that allow only air but not fluid to escape. Once run through, connect the end of the tubing to the clip on the roller clamp if it has one. Run the fluid into a waste basket or basin to avoid possible slip hazards. Apply a tourniquet to the proximal part of the limb well above the site of the injection. Let the limb hang below the level of the heart and stimulate blood flow in the arm. Figure 4 - Infrared view of veins using a Vein-Eye 28 Choose a vein that is relatively straight and bounces back when pressed. Avoid veins that cross joints or any extremity
6 6 of 15 that has edema or permanent fistulas. 29 Remember the saying Start distally, work proximally. 30 If a vein lower down doesn t work, you can move up. If you require large amounts of fluids or need to give medications in life-threatening situations, start the IV proximally into a large vein. 31 Large veins can roll and can mislead a paramedic into thinking it is the best option for an IV. Figure 5 shows how far a vein can move. The best method to stabilize the vein is to pull the skin tight above the vein. Figure 5 - Rolling Vein 32 Avoid injured, infected, or otherwise medically compromised limbs. Patients who have frequent IVs may present with track marks and stiff veins. 33 Always palpate the vein for a pulse to make sure it is not an artery. The best location for an IV depends on the patient s condition and local protocol. Establishing IVs in the legs should be done with caution as these have a greater risk of venous thrombosis or pulmonary embolism. 34 If extremity cannulation is not possible, external jugular (EJ) vein cannulation is a riskier alternative. The EJ is located behind the angle of the jaw and terminates in the subclavian vein (In Figure 6 the EJ is highlighted between the blue-dotted lines). The EJ easily moves about if improper cannulation technique is used and is perilously close to the carotid artery. If the EJ infiltrates, it will cause a fast-growing and large hematoma. If the carotid artery is punctured there is the risk of hemorrhage. Air embolism is a danger with EJ cannulation. 35 Put the patient in a supine, head-down position (with consideration to cervical spine injury)to facilitate jugular vein distension. Turn the patient s head away from the injection site. Ensure the targeted vein is not an artery (Figure 6 Image 1). Cleanse the site. Gently press on the vein distal to the injection site (between the injection site and the heart) to cause the vein to further enlarge (Figure 6 Image 2). Line up the catheter with the vein. Insert the needle halfway between the angle of the jaw and the mid-clavicular line, stabilizing the vein by putting your finger on the vein just superior to the clavicle (Figure 6 Image 3). It is very important during EJ cannulation that you do not allow air to enter the vein as much as 10 percent of the patient s tidal volume can enter the EJ vein causing an air embolism. Secure the line but do not compress the neck. 36 If needed, a c-collar can be placed over the IV. 37 Figure 6 - External jugular vein cannulation 38 Continuing with extremity IV insertion, clean the injection site with an alcohol or iodine swab. Use a circular motion with a
7 of 15 swab starting with small circles that are gradually made larger. Use a second swab straight down the middle to finish. Once the site is clean, do not touch it unless you are wearing sterile gloves. 39 Remove the IV catheter from its casing and alert others by using a term such as sharp out! Tell the patient there will be a pinch and insert the catheter with the bevel up into the vein at approximately a 45 degre eangle. Once the needle is in the vein you will see a flashback of blood appear in the hub of catheter (make sure the hub is full) and reduce the angle to about 15 degrees and advance the needle a few centimeters to ensure it is properly in the vein. Advance the catheter while holding the needle still until the hub is against the skin. Withdraw the needle completely making sure the catheter is held in place. Do not attempt to reinsert the needle into the catheter. Do not let go of the catheter as it can float out of the vein if the blood pressure is high. If the catheter is not self-occluding, you need to place gentle pressure on the vein to prevent blood from leaving the catheter. All needles should be immediately disposed of in a sharps bin. Do not attempt to recap or bend a sharp, unless local protocol requires such an act for a specific protocol or there is no other feasible alternative. 40 Attach the IV administration set to the catheter, making sure that the catheter is secured. Remove the tourniquet and run the IV line for a few seconds to ensure a patent line and secure the IV with tape or IV dressing. 41 Continually monitor the IV line and fluid or medication administration. IV Solutions and the Management of Medical and Trauma Conditions The choice of the administration set is influenced by the condition of the patient, the type and volume of fluids and medications needed. Administration sets are classified as microdrip or macrodrip sets. Microdrips use 60 drops or gtt (from the Latin word guttae) to make up 1 ml. Macrodrip sets use 10 to20 gtt (as indicated on the packaging) to make up 1 ml. It will take a microdrip set three to six times as long to make up 1 ml compared to a macrodrip set (assuming a constant drip rate). Figure 7 shows three different types of IV administration sets. Note that each of the sets has a particulate filter. Set A is used to administer whole blood products. Sets B and C each have a syringe port to allow fluid to be drawn out of or injected into the administration set. Note that set C (60 gtt/ml) has a characteristic metal spike in the drip chamber.
8 8 of 15 Figure 7 - Different IV administration sets: A) 10 gtt/ml blood admin set, B) 20 gtt/ml macrodrip, C) 60 gtt/ml microdrip 42 There are commercially available multidrip sets that allow paramedics to set the drip rate on the administration set. If you are using the administration set to administer medications or highly controlled amounts of fluid, then the microdrip set is preferred as you can better control the flow. Macrodrip sets are preferred for administrating large amounts of fluid. 43 A special kind of microdrip set called a Volutrol only administers 100 to 200 ml of fluid at a time to prevent inadvertent fluid overload. 44 There are several different types of IV solutions, each intended for a particular condition. IV fluids are broadly categorized as either crystalloids or colloids. Crystalloids are simply solutions of salts or sugar. These fluids can easily move across membranes and are the best choice for replacing fluid or maintaining blood pressure. The movement of water across the cells is called osmosis and is caused when there are different concentrations of sodium on either side of a membrane. 45,46 Colloids most often contain proteins, but may also contain sugars and starches that are too large to move through the capillary membranes. They give the fluid a high osmolarity while remaining in the intravascular space causing additional fluids from the intracellular and interstitial spaces to move into and expand the intravascular space. 47 Osmolarity refers to the number of particles in a solution that exert an osmotic pressure (the pressure difference between high and low solute concentrations). 48 Colloid solutions are rarely used in the prehospital environment, except for interfacility transfers, because they can cause life-threatening fluid shifts. 49 Colloids expand the intravascular volume by causing fluid to shift into the intravascular space. This shift from the interstitial and intracellular spaces into the intravascular space is what makes colloids effective in reducing both cerebral and pulmonary edemas. 50 Colloid solutions can be either natural or artificial and three common types are plasma protein fraction (PPF), Dextran, and Hetastarch. PPF is a natural, protein-containing colloid that is indicated for hypovolemic shock, in particular shock associated with burns, and for low-protein blood states. 51 Dextran is an artificial, sugar-containing colloid that is indicated for hypovolemic shock. 52 Hetastarch is an artificial, starchcontaining colloid that is also indicated for hypovolemic shock, in particular shock associated with burns and sepsis. All colloids run the risk of allergy and have adverse reactions such as nausea and vomiting amongst others. The duration of action of colloids can range from eight to 36 hours. 53
9 9 of 15 Crystalloids can be hypotonic, isotonic, or hypertonic which refer to the tonicity of the fluid relative to the normal sodium level of the body of 0.9%. Colloids are all hypertonic solutions due to their high osmolarity. Hypotonic solutions have a lower concentration of sodium and will producewater to move into the cell causing it to swell and possibly to burst. Hypertonic solutions have a higher concentration of sodium and will produce water to flow out of a cell causing it to shrink and possibly crenate. 54 Isotonic fluids have the osmotic pressure as the body fluids and will not cause a shift in water due to osmosis and are the preferred solution for prehospital care. Figure 8 below shows fluid movement across a cell membrane given a particular solution. Figure 8 - Hypertonic, isotonic and hypotonic effects on fluid movement across a cell membrane 55 The patient s condition and need for fluid replacement or medications will determine which fluid he or she gets. The two most common solutions for fluid replacement are normal saline (NS) and lactated Ringer's (LR) solution, and the most common fluid for medication administration is dextrose 5% in water (D 5 W). NS is an isotonic solution of 0.9% sodium chloride, and LR is an isotonic solution that contains a mixture of sodium chloride, sodium lactate, potassium chloride, and calcium chloride hexahydrate to reach a tonicity equivalent to 0.9 of sodium chloride. The lactate in LR is metabolized by the liver to form bicarbonate which is a buffer for acidosis that occurs during severe blood loss. LR should not be given to patients with liver failure. When administering crystalloids, use the 3-to-1 replacement rule which states that 3 ml of fluid replaces 1 ml of lost fluid. After one hour two-thirds of the fluid will leave the intravascular space and enter the interstitial space or be excreted. 56 Monitoring urine output, although not always possible, is the best indicator of possible renal issues. Fluid replacement should maintain radial pulses and an alert mental state and the BP should not be brought back to normal levels as this could dilute the patient s blood which will interfere with its clotting factors and its ability to carry oxygen. The BP should be maintained at approximately 90 mm Hg or according to local protocol. 57 NS and LR are universally used in the prehospital environment for both fluid replacement and medication administration. NS provides water and electrolytes and is available in 250-, 500- and 1,000-mL bags. 58 NS is used to treat heat illness, freshwater drowning, hypovolemia, diabetic ketoacidosis, and as KVO. The only contraindication for NS is congestive heart failure as this can easily result in circulatory overload. Adverse effects and drug interactions are rare. NS is used for short term therapy and the dose is dependent on the patient s condition and can range from KVO to rapid fluid replacement. 59 LR, also known as Hartmann s Solution, provides water and electrolytes. LR is available in 250-, 500- and 1,000-mL bags. 60 LR is used to treat hypovolemic shock and as KVO. As with NS, the only contraindications for LR are patients with congestive heart failure or renal failure. Adverse effects and drug interactions are rare. LR is used for short term therapy and the dose is dependent on the patient s condition and can range from KVO to rapid fluid replacement. 61 Five percent dextrose in water (D 5 W) is isotonic in the bag butis hypotonic in the body, and is a dextrose-containing solution that provides dextrose and water. D 5 W is used to maintain IV access for the administration of emergency medications, and to act as a diluent for concentrated IV drugs. D 5 W is contraindicated for use as a fluid replacement during hypovolemia. Adverse effects are rare. Phenytoin (an anti-epileptic drug 62 ) and inamrinone (an inotropic agent used to treat heart failure 63 ) should not be administered with D 5 W. 64 D5W is available in 50-, 100-, 150-, 250-, 500- and 1,000 ml bags. D 5 W, since it is not used for fluid replacement, is administered using a microdrip or 60 gtt administration set as KVO. 65 D 5 W has an interesting characteristic in that it is isotonic in the bag, but rapidly becomes hypotonic in the intravascular space as the dextrose is quickly metabolized in the body. 66 Less commonly used IV solutions in the prehospital environment include: 0.45% sodium chloride (half the normal saline), 10% dextrose in water (D 10 W), 5% dextrose in 0.45% sodium chloride (D 5½ NS), 5% dextrose in 0.9% sodium chloride
10 10 of 15 (D 5 NS), and 5% dextrose in LR (D 5 LR). All of these less common IV solutions are simply variations of solutions of sodium chloride, lactated Ringer's, and dextrose in water to achieve a desired tonicity and balance of water, salt, and sugar. 67 When treating a medical or trauma patients determine early on if the patient will require fluid therapy, medication administration, or both. If fluid replacement is required a bolus of 20 ml/kg should be given to restore peripheral pulses and maintain a BP of around 90 mm Hg as discussed above. 68 A patient weighing 80 kg for example, will require 80 x 20 = 1,600 ml. If the patient has an 18G this will take about 15 minutes as per the table in Figure 2.If the patient has a 16G it will take about half that time. In some cases, especially those where the patient has poor veins, you have to settle for smaller catheters, in which case it may be prudent to site more than one IV line. There are many medical conditions that require urgent fluid therapy such as diabetic ketoacidosis (DKA), hyperosmolar nonketotic coma (HONK), anaphylaxis, sickle cell crisis, and hypovolemic shock. DKA patients suffer from severe dehydration and require 1,000 ml in the first 30 minutes, and usually an additional 1,000 ml/hour after that until the dehydration is corrected. 69 HONK requires an initial bolus of 500 ml of normal saline which is the normal treatment for adult patients who are clinically dehydrated and who do not have any cardiac or renal problems (if they do give half the normal bolus). HONK patients may require from 1,000 to 2,000 ml of IV fluid per hour. 70 Anaphylaxis that is refractive to epinephrine will require an initial bolus of 1,000 to 2,000 ml; if there is still no positive response, up to 4,000 ml may be required. To get 4,000 ml of fluid into a patient quickly will usually require two, large bore, wide-open IV lines. 71 Sickle cell crisis requires IV fluid therapy to reverse dehydration and to assist in flushing damaged red blood cells from the body. 72 Hypovolemic shock in medical patients can occur as a result of serious internal bleeding such as esophageal varices which requires aggressive resuscitation. 73 It is not uncommon to give 1,000 ml of fluid in an hour with medical conditions. An IV catheter as small as a 22G could under ideal circumstances allow 1,000 ml to be delivered in 30 minutes. With more immediately life-threatening conditions such as anaphylaxis requiring up to 4,000 ml quickly, this could only be achieved with two large bore catheters. Trauma conditions requiring IV therapy include massive bleeding, hypovolemic shock, crush syndrome, and burns. Blood loss significant enough to cause shock can occur when blood is lost through open wounds, into the chest, retroperitoneum, abdomen, pelvis and upper legs. Injuries that can cause bleeding can be either penetrating, such as gunshot wounds, or blunt, such as falls. 74 Stopping the bleeding is very important using one or more techniques of direct pressure, pressure points, or a tourniquet. If a significant amount of blood has been lost, or if the patient is exhibiting signs and symptoms of shock such as a narrow pulse pressure, delayed capillary refill, cool, pale skin, and increased respirations, then IV fluid therapy is indicated. If the adult patient has a normal BP (100 to 130 mm Hg) but is still exhibiting signs and symptoms of shock, then only give a 250 ml fluid bolus. If the patient is hypotensive (80 to 90 mm Hg) then a fluid bolus of 20 ml/kg should be given to increase the BP to 90 mm Hg and to improve the patient s mental status. If the patient is severely hypotensive (50 to 80 mm Hg) then give a fluid bolus of 1,000 ml, followed by 20 ml/kg to get the patient to 90 to 100 mm Hg. Bilateral, large bore (14G or 16G) catheters and macrodrip sets are usually needed to achieve this. The fluids of choice are either normal saline or lactated ringers. 75 Crush syndrome occurs if part of the body is trapped for more than four hours without adequate arterial blood flow. Crush syndrome results in rhabdomyolysis which is caused from tissue necrosis and in turn causes the release of toxic products such as lactic acid and myoglobin. Patients with crush syndrome can experience instantaneous cardiac arrest when the trapped body part is released or renal failure later on. Renal failure in this case can be prevented with aggressive fluid therapy which can involve the administration of eight to 24 L of NS in the first 24 hours. LR is not recommended as it contains lactate. Typically this level of fluid administration can only be achieved with two large bore IVs. 76 Burns greater than 20percentof total body surface area require fluid resuscitation using either NS or LR (use local protocol). A careful balance of fluid is needed within two hours of the burn or mortality can increase. 77 When inserting the IV try and use an extremity that is not burned unless there is no alternative. Use a large bore catheter (16G or 14G) and macrodrip administration sets. Some severely burned patients may require central venous access. Swelling may make cannulation difficult. To determine the correct volume, use the Consensus formula (formerly known as the Parkland formula) 78 which determines the correct amount of fluid to be administered in the first 24 hours. This formula is 4 ml x body weight in kg x percent of body surface burned. 79 For example, an 80 kg patient with 30 percent burns will require 4 ml x 80 x 30 = 9,600 ml in the first 24 hours, half of which (4,800 ml) should be administered in the first eight hours. 80 IV Therapy Complications As with any medical procedure, IV therapy can cause complications if administered incorrectly or if a patient simply cannot tolerate an IV for various reasons such as weak veins. For the most part the complications can be limited by following the basic IV techniques described in this article. The first step in avoiding IV complications is to check the expiration date, clarity of fluids, and whether or not there are
11 11 of 15 any particles floating in the IV fluid (aka floaties ). IV therapy complications can occur within minutes or up to a few days. Complications can include both local and systemic complications. Local complications include infection, infiltration, occlusion, vein irritation, thrombophlebitis, hematoma, arterial puncture; and damage to nerves, tendons, and ligaments. 81,82 Systemic complications include allergic reactions, pyrogenic reactions, circulatory overload, air embolus, vasovagal reactions, and catheter shear. 83 Infection is most often caused by the lack of aseptic technique and can be avoided using the universal precautions discussed in the previous objective. Infiltration occurs when IV fluid accumulates around the injection site as a result of the catheter passing through the vein, the catheter not entering the vein at all, or the vein rupturing and allowing fluid to escape into the surrounding tissue. This buildup of fluid can create serious problems such as compartment syndrome with nerve damage and scarring, and in extreme cases, may even require surgery. Interestingly, failed or mismanaged peripheral IV lines are a significant source of liability for anesthesiologists. 84 The classic sign of infiltration is the formation of a hematoma around the injection site. The patient may complain of pain, burning or pressure. If infiltration does occur the IV line should be stopped and reestablished in the opposite limb if possible. Take care not to recreate the circumstances that caused the infiltration to occur in the first place such as failing to properly secure the IV or inserting the catheter at too great an angle. 85 Occlusion occurs if the pressure inside the IV administration set is not sufficient enough to keep blood out of the catheter. As the blood begins to clot when it enters the catheter, the flow of fluid will become increasingly restricted until it eventually stops. The occlusion can occur if the flow rate of the IV is too low, if the IV bag is not held high enough or if the IV is in a location that depends on the position of the patient (such as the antecubital fossa). If an IV line becomes occluded the first step is to see if adjusting the patient s position will reestablish the flow. If that doesn t work use a syringe with sterile normal saline to pressurize the IV system in an attempt to release the occlusion. If that doesn t work, the IV line should be discontinued and a new one established proximal to the current IV, or in a different limb. 86 Patients can experience vein irritation from the IV fluid or medications administered through the IV. Typically, the patient will complain of pain, burning or itching at the site. If this happens discontinue the line and be alert for a possible allergic reaction. Irritation can occur if the fluid is administered too quickly, is too cold, or simply if the patient is hypersensitive or allergic to the fluid or medication. 87 Thrombophlebitis, or vein inflammation, most often occurs from breaks in aseptic technique. It is most commonly associated with drug users, long-term IV patients, or from the use of solutions that irritate veins such as those that are acidic or hypertonic. Thrombophlebitis is also known to occur from mechanical action such as when the IV catheter moves around a lot. Thrombophlebitis is not typically seen in the prehospital environment as it takes several hours to develop. Paramedics can spotthrombophlebitis during interfacility transports. Thrombophlebitis presents with pain along the vein as well as redness and swelling around the injection site. It is important for paramedics to be aware of thrombophlebitis, as they can cause it. 88 Hematoma occurs when blood accumulates around the site of the IV and when the vein is perforated during IV insertion or is damaged when the catheter is pulled out incorrectly. Typically, there is rapid swelling around the site as the blood fills up the area surrounding the vein. The patient will experience tenderness and pain in the area. Some patients are more prone than others towards getting hematomas. Diabetics, patients with vascular disease, patients on blood thinners, and patients who have consumed alcohol are all more prone to hematomas during IV insertion. A hematoma can be self-limiting and an IV may still be flowing should a hematoma occur. If the IV line does not flow, discontinue the line and apply pressure to the insertion site. To avoid causing a hematoma when removing a catheter, apply gentle pressure to the injection site and remove the catheter slowly. 89 It is possible to damage ligaments, tendons and nerves while performing peripheral IV cannulation, especially when the IV site is close to joints and areas where major nerves are more superficial. Inserting a catheter into a ligament or tendon usually causes acute pain. Inserting a catheter into a nerve also results in acute pain as well as an electric shock type sensation, numbness and tingling (pins and needles). If a nerve, ligament or tendon is cannulated, the catheter should be removed immediately and relocated into an appropriate vein. 90 If a paramedic is not an expert in identifying the anatomic landmarks it is possible that the incorrect vein or even an artery could be cannulated. Cannulating the wrong vein may be a problem if the vein the paramedic ended up in is a lot smaller or shorter than was intended which may cause issues in delivering fluids or medications. Cannulating an artery will result in bright red arterial blood forcefully flowing into the catheter. If the blood pressure is high enough it can dislodge the cap on the catheter and cause blood to spurt out creating a potential body substance hazard. If an artery is cannulated, and the paramedic manages to connect the administration set to the catheter, bright red blood can flow up the administration set into the IV bag. If this happens the IV should be discontinued immediately. 91 Depending on local protocol or medical control orders, the catheter should either be removed and pressure applied to the artery to stop bleeding, or the catheter should be secured in place as the hospital may end up using it for arterial blood gases (ABGs). Systemic complications resulting from IV therapy can be life-threatening and affect all areas of the body. Contrary to the
12 2 of 15 management of local complications experienced with IV therapy, the IV should not necessarily be removed depending on the systemic complication that occurs. For example, if an allergic reaction occurs (and all IV patients are at risk for an allergic reaction to IV fluid) the flow of IV fluid should be stopped and the IV administration set should be replaced with a saline lock. The saline lock in this instance will provide a route to administer emergency medications such as IV epinephrine 92 to treat the allergic reaction. Manage the patient according to protocol or medical direction and keep all of the infusion equipment for analysis. 93 IV fluids that are contaminated with foreign proteins called pyrogens can cause a rapid and very high temperature (above 41 C) called a pyrogenic reaction. This reaction will usually occur within 30 minutes after the IV administration has begun. The two main initial symptoms are backache and headache, followed by severe chills, weakness, nausea, and vomiting. In this case the IV must be immediately discontinued. Place an IV line in the opposite arm with a new IV solution making doubly sure that the solution is clear and not expired. Once the new IV has been set up, remove the old IV line. Manage the patient for potential shock according to local protocol or medical direction. Keep all of the infusion equipment for further analysis. 94 Circulatory overload occurs when more IV fluid than the patient s circulatory volume can handle is given. A healthy adult can tolerate 2,000 to 3,000 ml of fluid without complications. If the patient has cardiac, pulmonary, or renal problems the patient will not be able to tolerate the excess IV fluid. Typically, circulatory overload occurs when an IV line is flushed and the paramedic forgets to or sets an inappropriately high drip rate. One method of preventing this, other than paying close attention to IV drip rates, is to use a Volutrol in patients who are sensitive to increases in circulatory volume. Signs and symptoms of circulatory overload include difficulty breathing, neck vein distension, and hypertension. 95 Before administering IV fluids you should auscultate the chest for crackles, take the patient s blood pressure, and check for edema in the extremities. Should circulatory overload occur, immediately change the drip rate to KVO, elevate the patient s head, administer high-flow oxygen and use continuous positive air pressure (CPAP) to push fluid out of the lungs and back into circulation if indicated by local protocol or ordered by medical direction. 96 When setting up an IV it is important to always prime the administration set with IV fluid. The volume needed to prime the administration set varies between manufacturers and the different types of administration sets (microdrip vs.macrodrip) but is in the region of 15 to 20 ml of fluid. 97 Should a paramedic connect a non-primed administration set to a patient, and then start the drip 15 to 20 ml of air will be introduced directly into the vascular space. This air embolus will travel straight to the heart and into the lungs. A healthy adult can tolerate 200 ml of air directly into the circulatory system, but a patient who has a compromised cardiopulmonary system might not be able to endure any air directly into the circulatory system. 98 In order to prevent an air embolus make sure the IV is properly connected, the administration set is primed, and that empty IV bags are promptly replaced. The IV bag is designed to collapse as it empties, but small leaks may prevent this from happening. 99 Signs and symptoms of a possible air embolism include sudden respiratory distress, unequal breath sounds, cyanosis not relieved by oxygen administration, shock, loss of consciousness, and respiratory arrest. 100 Treatment for a suspected air embolus should be rapid and include placing the patient in a left lateral recumbent position with the head down (to assist in trapping the air in the right side of the heart), administering 100 percent oxygen, preparing to assist ventilations, and to transport the patient to the nearest and appropriate medical facility. 101 There are few people who enjoy getting an injection and this aversion can go so far as causing such severe anxiety that systemic vasodilation results, causing a sufficient enough drop in blood pressure that the patient passes out. If this happens, treat the patient for shock, administer oxygen as needed, monitor closely, and continue to establish the IV line. 102 Once a needle has been withdrawn from the catheter, it should not be advanced again for risk of creating a catheter shear. Catheter shear occurs when the sharp tip of the needle cuts off a small piece of the catheter which will then travel through the circulatory system where it will most likely end up in the lungs as a pulmonary embolus. Signs and symptoms are similar to an air embolism and the treatment should be the same as for an air embolism. IV access is important in this type of patient and should be established in the opposite arm. 103
13 13 of 15 Figure 9 - IV Catheter Shear Case Study Conclusion Often, IV lines are setup as KVO just in case they are needed. In the case study you were faced with a patient with a complex condition that required several treatments, all of which required a patent IV line. Firstly, a patient like this would definitely require an IV KVO even if you didn t immediately plan to give any fluids or medications. By having a line setup, you were able to administer boluses of normal saline, IV dextrose, and norepinephrine. Although you started out with a normal saline drip, you were ordered to setup and run the norepinephrine drip at a very specific rate. If you ran the drip too slowly, the drug might not have any effect (or even a paradoxical effect);too fast and you could exceed the maximum dose. In addition to the correct dosage, you also need to ascertain if the IV would last the duration of the transport. Not all IV fluids are compatible with all medications, and norepinephrine is best diluted with D5W. If you are switching between fluids and medications, as you were in this case, you need to know how to flush IV lines and switch between different types of administration sets. It is important to familiarize yourself with all the IV equipment that will be used in your service. When the patient is handed over to the ED they would possibly want to draw a blood sample, administer additional IV fluids and medications. Setting up an IV line en route to the hospital can certainly speed up treatment once the patient gets to the ED. The IV was established on scene in this example; however, it was established in parallel with other treatments. Many EMS services will have standard procedures in place to only establish an IV on scene if it is life-threatening or ordered by medical control. Setting up an IV should never delay transport unless the patient s illness or injury requires immediate intervention. Conclusion IV therapy goes far beyond simply sticking a needle into someone s vein. An IV gives you direct access into the vascular system and an express pathway to all the vital organs. If you misjudge or miscalculate fluids or medications that go into an IV, you could cause a patient serious injury or death. First and foremost, you need an in-depth knowledge of anatomy and physiology. This will let you know where to gain IV access, and what each fluid will do to the body once it has been administered. The task of actually gaining access requires that you have expertise in selecting the appropriate equipment, and handling it in a safe manner for you, other medical personnel, and the patient. Secondly, you need to have a firm mathematical understanding to calculate flow, drip,and dosage rates for different treatment protocols. Paramedics will be able to bring all of these requirements together in a matter of a few minutes and
14 4 of 15 be able to continually monitor and adjust the IV therapy as needed. Author Michael Klopper, Peer Reviewers, Rebecca Brazeal, Simon Taxel, George Pettit MD, Copyright CE Solutions. All Rights Reserved. References: 1. Internet. Drugs.com. Metoprolol. Accessed: 11/14/ Nancy Caroline s Emergency Care in the Streets, 7th Edition. Andrew N. Pollak, MD, FAAOS. Page Internet. US National Library of Medicine National Institutes of Health. Controversies in fluid therapy: Type, dose and toxicity. Robert C McDermid et al. Accessed: 11/15/ Op cit. Pollak. Page Ibid. Page Internet. Center for Disease Control. Guidelines for the Prevention of Intravascular Catheter-Related Infections, Naomi P. O'Grady, M.D et al. Accessed: 10/21/ Op cit. O Grady. Page Ibid. Table 1 9. Ibid. Page Op cit. Pollak. Page Op cit. O Grady. Page Internet. United States Department of Labor, Occupation Safety and Health Administration (OSHA). Accessed: 10/27/ Ibid. 14. Ibid. 15. Ibid. 16. Op cit. Pollak. Page Ibid Page Ibid. Page Ibid. 20. Ibid. Page Book. MedSurg Notes. Tracey Hopkins. Page Ibid. Page Photo. CE Solutions Original Photo 24. Internet. BD. Manufacturer. Gravity Based Flow Rates & Infusion Time BD Insyte Autoguard BC Shielded IV Catheter. Accessed: 10/27/ Ibid. 26. Internet. B Braun. /BPR /4F BC0B50E D400106F4F BC0B50E D400106F?vc=CORPORATE_WEBSITE_COM& s=d155214a63282d2f3088e9756e43dca5. Accessed: 11/04/ Photo. CE Solutions Original Photo 28. Photo. CE Solutions Original Photo 29. Ibid. Page Ibid. Page Ibid. 32. Photo. CE Solutions Original Photo 33. Ibid. Page Ibid. 35. Ibid. Page Ibid. 37. Book. International Trauma Life Support. John R Campbell. Page Photo. CE Solutions Original Photo 39. Ibid. Page Op cit. OSHA. 41. Internet. National Registry of Emergency Medical TechniciansAdvanced Level Psychomotor Examination. Accessed: 10/27/ Photo. CE Solutions Original Photo 43. Op cit. Pollak. Page Ibid. Page Ibid. Page Ibid. Page Ibid. Page Ibid. Page Ibid. Page 477
Chapter Goal. Learning Objectives 9/11/2012. Chapter 6. Venous Access
 Chapter 6 Venous Access Chapter Goal Understand basic principles of venous access & IV therapy, as well as relate importance of employing appropriate BSI precautions when employing these precautions Learning
Chapter 6 Venous Access Chapter Goal Understand basic principles of venous access & IV therapy, as well as relate importance of employing appropriate BSI precautions when employing these precautions Learning
Successful IV Starts Revised February 2014
 Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
IV Fluids. Nursing B23. Objectives. Serum Osmolality
 IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
Title: EZ-IO. Effective Date: January SOG Number: EMS Rescinds:
 S O G Title: EZ-IO Effective Date: January 2010 SOG Number: EMS - 25 Rescinds: Scope: Providers Authorized are AIC s in the following certifications EMT-I and EMT-P who have been trained and cleared by
S O G Title: EZ-IO Effective Date: January 2010 SOG Number: EMS - 25 Rescinds: Scope: Providers Authorized are AIC s in the following certifications EMT-I and EMT-P who have been trained and cleared by
IV Fluids Nursing B23 Objectives Serum Osmolality 275 to 295 Isotonic
 1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
Chapter 5. Learning Objectives. Learning Objectives 9/11/2012. Intravenous Fluids and Administration
 Chapter 5 Intravenous Fluids and Administration Learning Objectives Define total body water (TBW) and its two main compartments (intracellular fluid and extracellular fluid) Define osmosis and explain
Chapter 5 Intravenous Fluids and Administration Learning Objectives Define total body water (TBW) and its two main compartments (intracellular fluid and extracellular fluid) Define osmosis and explain
A step-by-step preparation guide
 A step-by-step preparation guide This guide provides detailed instruction on the reconstitution, dilution, and storage of Veletri (epoprostenol) for Injection. It is intended to be used after your healthcare
A step-by-step preparation guide This guide provides detailed instruction on the reconstitution, dilution, and storage of Veletri (epoprostenol) for Injection. It is intended to be used after your healthcare
How Normal Body Processes Are Altered By Disease and Injury
 1 Chapter 4, General Principles of Pathophysiology Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
1 Chapter 4, General Principles of Pathophysiology Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
A step-by-step preparation guide
 A step-by-step preparation guide For needle and needle-free systems This guide provides detailed instructions on the reconstitution, dilution, and storage of VELETRI. It is intended to be used after your
A step-by-step preparation guide For needle and needle-free systems This guide provides detailed instructions on the reconstitution, dilution, and storage of VELETRI. It is intended to be used after your
Complications Associated With IV Therapy
 Occlusion is the partial or complete obstruction of a catheter, which obstructs the infusion of solutions or medications. Occlusions can result from the coagulation of blood (thrombotic) or from obstruction
Occlusion is the partial or complete obstruction of a catheter, which obstructs the infusion of solutions or medications. Occlusions can result from the coagulation of blood (thrombotic) or from obstruction
STEP-BY-STEP GUIDE TO SELF-INFUSION. Subcutaneous Administration of GAMMAGARD LIQUID
 STEP-BY-STEP GUIDE TO SELF-INFUSION Subcutaneous Administration of GAMMAGARD LIQUID This handy guide will help you manage your subcutaneous administration of GAMMAGARD LIQUID. If you have questions on
STEP-BY-STEP GUIDE TO SELF-INFUSION Subcutaneous Administration of GAMMAGARD LIQUID This handy guide will help you manage your subcutaneous administration of GAMMAGARD LIQUID. If you have questions on
Overview. The Team Concept. Chapter 7. Assisting the ALS Provider 9/11/2012. The Team Concept ALS Procedures and Equipment
 Chapter 7 Assisting the ALS Provider Slide 1 Overview The Team Concept ALS Procedures and Equipment Electrocardiogram (ECG) Monitoring Slide 2 The Team Concept Prehospital care involves many individuals
Chapter 7 Assisting the ALS Provider Slide 1 Overview The Team Concept ALS Procedures and Equipment Electrocardiogram (ECG) Monitoring Slide 2 The Team Concept Prehospital care involves many individuals
Venepuncture and Cannulation. Louise Smith Clinical Nurse Specialist
 Venepuncture and Cannulation Louise Smith Clinical Nurse Specialist Outcomes By the end of this session you will be aware of: Basic anatomy Preparation procedures including patient identification Equipment
Venepuncture and Cannulation Louise Smith Clinical Nurse Specialist Outcomes By the end of this session you will be aware of: Basic anatomy Preparation procedures including patient identification Equipment
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
If viewing a printed copy of this policy, please note it could be expired. Got to to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5575 Entity: Fairview Pharmacy Services
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5575 Entity: Fairview Pharmacy Services
EL DORADO COUNTY EMS AGENCY FIELD PROCEDURES
 EL DORADO COUNTY EMS AGENCY FIELD PROCEDURES Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director INTRAOSSEOUS INFUSION PURPOSE: To establish immediate
EL DORADO COUNTY EMS AGENCY FIELD PROCEDURES Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director INTRAOSSEOUS INFUSION PURPOSE: To establish immediate
2. Need for serial arterial blood gas determinations. 2. Anticipation of the initiation of thrombolytic therapy
 I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
Instructions for Use Enbrel (en-brel) (etanercept) for injection, for subcutaneous use Multiple-dose Vial
 Instructions for Use Enbrel (en-brel) (etanercept) for injection, for subcutaneous use Multiple-dose Vial How do I prepare and give an injection with Enbrel multiple-dose vial? A multiple-dose vial contains
Instructions for Use Enbrel (en-brel) (etanercept) for injection, for subcutaneous use Multiple-dose Vial How do I prepare and give an injection with Enbrel multiple-dose vial? A multiple-dose vial contains
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Parkland Health & Hospital System Women & Infant Specialty Health
 Parkland Health & Hospital System Women & Infant Specialty Health NS 1700.04 Nursery Services Procedure Manual Arterial Puncture Practice Statement Upon the written order of the provider, the credentialled
Parkland Health & Hospital System Women & Infant Specialty Health NS 1700.04 Nursery Services Procedure Manual Arterial Puncture Practice Statement Upon the written order of the provider, the credentialled
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
IV Catheter Placement
 Year Group: BVSc3 + Document number: CSL_A06 Equipment for this station: Equipment list: IV catheter model, with giving set and red fluid bag IV catheter Bung or T-port Tape two strips cut to size before
Year Group: BVSc3 + Document number: CSL_A06 Equipment for this station: Equipment list: IV catheter model, with giving set and red fluid bag IV catheter Bung or T-port Tape two strips cut to size before
SALEM HOSPITAL SALEM, OREGON 97309
 SALEM HOSPITAL SALEM, OREGON 97309 Department: Phlebotomy TITLE: BLOOD COLLECTIONS, VENIPUNCTURE Area: Phlebotomy Effective Date: 04/01/96 Authored By: Cindy Humphrey, Diane Duncan Revised: 09/26/2000,
SALEM HOSPITAL SALEM, OREGON 97309 Department: Phlebotomy TITLE: BLOOD COLLECTIONS, VENIPUNCTURE Area: Phlebotomy Effective Date: 04/01/96 Authored By: Cindy Humphrey, Diane Duncan Revised: 09/26/2000,
ATI Skills Modules Checklist for Central Venous Access Devices
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Central Venous Access Devices Student s name Date Verify order Patient record Assess for procedure need Identify, gather,
Standard Operating Procedure for cannulation
 Standard Operating Procedure for cannulation Effective date: 26.07.2017 Review due date: 31.03.2019 Original Author Name: Richard Metcalfe Position: PhD Student Date: 05.12.2012 Reviewer Name: Pippa Heath
Standard Operating Procedure for cannulation Effective date: 26.07.2017 Review due date: 31.03.2019 Original Author Name: Richard Metcalfe Position: PhD Student Date: 05.12.2012 Reviewer Name: Pippa Heath
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
How Normal Body Processes Are Altered By Disease and Injury
 1 Chapter 4, GENERAL PRINCIPLES OF PATHOPHYSIOLOGY. Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
1 Chapter 4, GENERAL PRINCIPLES OF PATHOPHYSIOLOGY. Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
MICAFUNGIN MIXING
 1 1-800-862-2731 MICAFUNGIN MIXING Drug Name: MICAFUNGIN Volume and Rate: over 1 hour Schedule: KEY POINTS: FLUSHING: Saline Micafungin Saline Heparin 1. Always wash your hands with an antibacterial soap
1 1-800-862-2731 MICAFUNGIN MIXING Drug Name: MICAFUNGIN Volume and Rate: over 1 hour Schedule: KEY POINTS: FLUSHING: Saline Micafungin Saline Heparin 1. Always wash your hands with an antibacterial soap
OV United Soccer Club
 Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS
 Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS PRACTICE POINTS Give the right blood product to the right patient at the right time. Failure to correctly check the patient or the pack can be fatal. At the
Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS PRACTICE POINTS Give the right blood product to the right patient at the right time. Failure to correctly check the patient or the pack can be fatal. At the
How to Set Up and Infuse Your TPN
 Page 1 of 10 How to Set Up and Infuse Your TPN Important: Do not change any of the supplies listed here. Keep supplies away from children. Only your home care nurse or persons trained by Fairview Home
Page 1 of 10 How to Set Up and Infuse Your TPN Important: Do not change any of the supplies listed here. Keep supplies away from children. Only your home care nurse or persons trained by Fairview Home
FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
 Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
Chapter 14: Arterial Puncture Procedures
 Objectives Chapter 14: Arterial Puncture Procedures 1. Define the key terms and abbreviations listed at the beginning of this chapter. 2. State the primary reason for performing arterial punctures and
Objectives Chapter 14: Arterial Puncture Procedures 1. Define the key terms and abbreviations listed at the beginning of this chapter. 2. State the primary reason for performing arterial punctures and
INSTRUCTIONS FOR PREPARING AND GIVING AN INJECTION OF ENBREL POWDER
 INSTRUCTIONS FOR PREPARING AND GIVING AN INJECTION OF ENBREL POWDER Introduction The following instructions explain how to prepare and inject Enbrel powder for injection. Please read the instructions carefully
INSTRUCTIONS FOR PREPARING AND GIVING AN INJECTION OF ENBREL POWDER Introduction The following instructions explain how to prepare and inject Enbrel powder for injection. Please read the instructions carefully
Peripherally Inserted Central Catheter (PICC) Booklet
 Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
Education for Self Administration of Intravenous Therapy HOME IV THERAPY PICC. Portacath
 HOME IV THERAPY PICC Portacath Who To contact Cardio-Respiratory Integrated Specialist Services (CRISS) Office hours 0800 1630 hours Ph: 364 0167 Weekends and after hours, phone Christchurch Hospital operator
HOME IV THERAPY PICC Portacath Who To contact Cardio-Respiratory Integrated Specialist Services (CRISS) Office hours 0800 1630 hours Ph: 364 0167 Weekends and after hours, phone Christchurch Hospital operator
SEMINOLE COUNTY EMS PROVISIONAL EMT SKILLS VERIFICATION
 The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
ARROW EZ-IO Intraosseous Vascular Access System Procedure Template
 ARROW EZ-IO Intraosseous Vascular Access System Procedure Template PURPOSE To provide procedural guidance for establishment of intraosseous vascular access using the ARROW EZ-IO Intraosseous Vascular Access
ARROW EZ-IO Intraosseous Vascular Access System Procedure Template PURPOSE To provide procedural guidance for establishment of intraosseous vascular access using the ARROW EZ-IO Intraosseous Vascular Access
EVOGAM. Information for patients Evogam 2014 NZ Patient Brochure Update v11
 EVOGAM Information for patients 11881 Evogam 2014 NZ Patient Brochure Update v11 Information for patients and caregivers about EVOGAM This booklet is designed to help you follow the training you will have
EVOGAM Information for patients 11881 Evogam 2014 NZ Patient Brochure Update v11 Information for patients and caregivers about EVOGAM This booklet is designed to help you follow the training you will have
If viewing a printed copy of this policy, please note it could be expired. Got to to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5555 Entity: Fairview Pharmacy Services
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5555 Entity: Fairview Pharmacy Services
IO considerations. Daniel Dunham
 IO considerations Daniel Dunham If patient is conscious Advise of EMERGENT NEED for this procedure and obtain informed consent Rule out contraindications Fracture. Excessive tissue and/or absence of adequate
IO considerations Daniel Dunham If patient is conscious Advise of EMERGENT NEED for this procedure and obtain informed consent Rule out contraindications Fracture. Excessive tissue and/or absence of adequate
Sierra Sacramento Valley EMS Agency Program Policy. Vascular Access
 Sierra Sacramento Valley EMS Agency Program Policy Vascular Access Effective: 12/01/2017 Next Review: 09/2020 1101 Approval: Troy M. Falck, MD Medical Director Approval: Victoria Pinette Executive Director
Sierra Sacramento Valley EMS Agency Program Policy Vascular Access Effective: 12/01/2017 Next Review: 09/2020 1101 Approval: Troy M. Falck, MD Medical Director Approval: Victoria Pinette Executive Director
KINGSTON GENERAL HOSPITAL NURSING POLICY AND PROCEDURE
 KINGSTON GENERAL HOSPITAL NURSING POLICY AND PROCEDURE SUBJECT Sample (Adult): Advanced Competency (AC) for Nurses (Registered Nurses and Registered Practical Nurses) PAGE 1 of 5 ORIGINAL ISSUE 1985 January
KINGSTON GENERAL HOSPITAL NURSING POLICY AND PROCEDURE SUBJECT Sample (Adult): Advanced Competency (AC) for Nurses (Registered Nurses and Registered Practical Nurses) PAGE 1 of 5 ORIGINAL ISSUE 1985 January
Home Health Foundation, Inc. To create more permanent IV access for patients undergoing long term IV therapy.
 PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
How to Use ENBREL : Vial Adapter Method
 How to Use ENBREL : Vial Adapter Method SETTING UP FOR AN INJECTION Select a clean, well-lit, flat working surface, such as a table. Take the ENBREL dose tray out of the refrigerator and place it on your
How to Use ENBREL : Vial Adapter Method SETTING UP FOR AN INJECTION Select a clean, well-lit, flat working surface, such as a table. Take the ENBREL dose tray out of the refrigerator and place it on your
12/29/2014. IV/IO Therapy & Fluid Administration. Objectives. Cleansing of the soul
 IV/IO Therapy & Fluid Administration Gary Hoertz, EMT-P Spokane County EMS Indications for IV Access Types of Intravenous Access IV fluids Flow Rates Fluid resuscitation Objectives Cleansing of the soul
IV/IO Therapy & Fluid Administration Gary Hoertz, EMT-P Spokane County EMS Indications for IV Access Types of Intravenous Access IV fluids Flow Rates Fluid resuscitation Objectives Cleansing of the soul
QI. Read the following questions and choose the most correct answer (20 Marks):
 Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
Question One: QI. Read the following questions and choose the most correct answer (20 Marks): 1- Some people are very allergic to some drugs like penicillin. This condition is called: a) Septic shock.
SELF-INJECTION GUIDE
 SELF-INJECTION GUIDE (asfotase alfa) 40 mg/ml solution for injection 18 mg/0.45 ml 28 mg/0.7 ml 40 mg/1 ml 100 mg/ml solution for injection 80 mg/0.8 ml asfotase alfa Introduction Contents This Self-Injection
SELF-INJECTION GUIDE (asfotase alfa) 40 mg/ml solution for injection 18 mg/0.45 ml 28 mg/0.7 ml 40 mg/1 ml 100 mg/ml solution for injection 80 mg/0.8 ml asfotase alfa Introduction Contents This Self-Injection
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs
 Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
MODULE 2 THE LABORATORY RAT
 University Animal Care Committee LABORATORY ANIMAL BIOMETHODOLOGY WORKSHOP MODULE 2 THE LABORATORY RAT SUBSTANCE ADMINISTRATION AND BLOOD COLLECTION Substance Administration: Subcutaneous injection Intramuscular
University Animal Care Committee LABORATORY ANIMAL BIOMETHODOLOGY WORKSHOP MODULE 2 THE LABORATORY RAT SUBSTANCE ADMINISTRATION AND BLOOD COLLECTION Substance Administration: Subcutaneous injection Intramuscular
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Table of Contents. Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings
 Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Table of Contents Dialysis Port Care Chemotherapy Port Care G-Tube Care Colostomy Bags Wound Dressings Dialysis Port Care Know What Type of Vascular Access You Have. Fistula: An artery in your forearm
Vascular access device selection & placement. Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University
 Vascular access device selection & placement Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University How to make the right choice of vascular access device.. Peripheral
Vascular access device selection & placement Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University How to make the right choice of vascular access device.. Peripheral
A child in the emergency room has an order for a blood draw. You would approach the child in which of the following scenarios?
 Phlebotomy Career Training Test Name: Being a phlebotomist requires a great amount of concentration. Given the following situations select the best response. 1. A child in the emergency room has an order
Phlebotomy Career Training Test Name: Being a phlebotomist requires a great amount of concentration. Given the following situations select the best response. 1. A child in the emergency room has an order
MABEES. MFR & Basic EMT Epinephrine Study
 MABEES MFR & Basic EMT Epinephrine Study Acknowledgements This program is a State of Michigan approved special study designed by members of the Oakland County Medical Control Authority American CME developed
MABEES MFR & Basic EMT Epinephrine Study Acknowledgements This program is a State of Michigan approved special study designed by members of the Oakland County Medical Control Authority American CME developed
Central Venous Catheter Care and Maintenance (includes catheter troubleshooting guide)
 Central Venous Catheter Care and Maintenance (includes catheter troubleshooting guide) A Guide for Patients in the Home Phone Number: Nurse/Contact: Central Venous Catheters This manual is a guide for
Central Venous Catheter Care and Maintenance (includes catheter troubleshooting guide) A Guide for Patients in the Home Phone Number: Nurse/Contact: Central Venous Catheters This manual is a guide for
EMT OPTIONAL SKILL. Cell Phones and Pagers. Epinephrine Auto-injector. Course Outline 9/2017
 EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
APPENDIX EZ IO ADULT INTRAOSSEOUS INFUSION. Purpose: To establish guidelines for the insertion of an intraosseous catheter for patients > 40 kgs.
 APPENDIX EZ IO ADULT INTRAOSSEOUS INFUSION Purpose: To establish guidelines for the insertion of an intraosseous catheter for patients > 40 kgs. Indications: Any Adult patient (>40 kg) for whom you are
APPENDIX EZ IO ADULT INTRAOSSEOUS INFUSION Purpose: To establish guidelines for the insertion of an intraosseous catheter for patients > 40 kgs. Indications: Any Adult patient (>40 kg) for whom you are
Patient Information Publications Warren Grant Magnuson Clinical Center National Institutes of Health
 Warren Grant Magnuson Clinical Center National Institutes of Health What is a subcutaneous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous
Warren Grant Magnuson Clinical Center National Institutes of Health What is a subcutaneous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous
Central venous access devices for children with lysosomal storage disorders
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
Instructions for Use HEMLIBRA (hem-lee-bruh) (emicizumab-kxwh) injection, for subcutaneous use
 Instructions for Use HEMLIBRA (hem-lee-bruh) (emicizumab-kxwh) injection, for subcutaneous use Be sure that you read, understand, and follow the Instructions for Use before injecting HEMLIBRA. Your healthcare
Instructions for Use HEMLIBRA (hem-lee-bruh) (emicizumab-kxwh) injection, for subcutaneous use Be sure that you read, understand, and follow the Instructions for Use before injecting HEMLIBRA. Your healthcare
Unit 11. Objectives. Indications for IV Therapy. Intravenous Access Devices & Common IV Fluids. 3 categories. Maintenance Replacement Restoration
 Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
EMS Subspecialty Certification Review Course. Conflict of Interest Disclosure. Learning Objectives
 EMS Subspecialty Certification Review Course Cardiovascular 1.4.2.2 Placement of peripheral IV lines 1.4.2.2.1 Access or Placement of Central Venous Lines in the field 1.4.2.2.2 Intraosseous lines 1.4.2.2.3.
EMS Subspecialty Certification Review Course Cardiovascular 1.4.2.2 Placement of peripheral IV lines 1.4.2.2.1 Access or Placement of Central Venous Lines in the field 1.4.2.2.2 Intraosseous lines 1.4.2.2.3.
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
OBJECTIVES 4/27/13 I VE GOT A CRUSH ON YOU! CRUSH INJURIES IN EMS DON T BELIEVE THIS MAN.
 I VE GOT A CRUSH ON YOU! CRUSH INJURIES IN EMS DON T BELIEVE THIS MAN. OBJECTIVES Recognize the differences between Crush Injury and Crush Syndrome List at least 2 complications that occur with Crush Syndrome
I VE GOT A CRUSH ON YOU! CRUSH INJURIES IN EMS DON T BELIEVE THIS MAN. OBJECTIVES Recognize the differences between Crush Injury and Crush Syndrome List at least 2 complications that occur with Crush Syndrome
Infusion Skills Competency Checklist To be used at annual skills fair or at any other time for IV Competency
 Employee Profile Infusion Skills Checklist Last Name First Name Middle Initial Employee Number Employee Discipline Check one: RN LPN Per state specific LPN Practice Acts Direct Supervisor s Name: Date
Employee Profile Infusion Skills Checklist Last Name First Name Middle Initial Employee Number Employee Discipline Check one: RN LPN Per state specific LPN Practice Acts Direct Supervisor s Name: Date
PLEASE READ THIS USER MANUAL BEFORE USE
 USER MANUAL Humalog 200 units/ml KwikPen, solution for injection in a pre-filled pen insulin lispro PLEASE READ THIS USER MANUAL BEFORE USE USE ONLY IN THIS PEN, OR SEVERE OVERDOSE CAN RESULT Read the
USER MANUAL Humalog 200 units/ml KwikPen, solution for injection in a pre-filled pen insulin lispro PLEASE READ THIS USER MANUAL BEFORE USE USE ONLY IN THIS PEN, OR SEVERE OVERDOSE CAN RESULT Read the
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
To understand osmosis, we must focus on the behavior of the solvent, not the solute.
 GCC CHM 130LL Osmosis and Dialysis Purpose: The purpose of this experiment is to observe the closely related phenomena of osmosis and diffusion as it relates to dialysis. It is hoped that you will be able
GCC CHM 130LL Osmosis and Dialysis Purpose: The purpose of this experiment is to observe the closely related phenomena of osmosis and diffusion as it relates to dialysis. It is hoped that you will be able
IV therapy. By: Susan Mberenga, RN, MSN. Copyright 2016, 2013, 2010, 2006, 2002 by Saunders, an imprint of Elsevier Inc.
 IV therapy By: Susan Mberenga, RN, MSN 1 IV Therapy Types of solutions Isotonic Hypotonic Hypertonic Caution: Too rapid or excessive infusion of any IV fluid has the potential to cause serious problems
IV therapy By: Susan Mberenga, RN, MSN 1 IV Therapy Types of solutions Isotonic Hypotonic Hypertonic Caution: Too rapid or excessive infusion of any IV fluid has the potential to cause serious problems
Chapter 64 Administration of Injectable Medications
 Chapter 64 Administration of Injectable Medications Injectable Medications Injection or intravenous (IV) infusion More invasive than administration by mouth, rectum, or through the skin Common methods
Chapter 64 Administration of Injectable Medications Injectable Medications Injection or intravenous (IV) infusion More invasive than administration by mouth, rectum, or through the skin Common methods
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Acting in an Emergency (Video- Acting in an emergency and preventing disease transmission)
 CHAPTER 2 Acting in an Emergency (Video- Acting in an emergency and preventing disease transmission) Lesson Objectives 1. Explain how bloodborne pathogens may be transmitted from an infected person to
CHAPTER 2 Acting in an Emergency (Video- Acting in an emergency and preventing disease transmission) Lesson Objectives 1. Explain how bloodborne pathogens may be transmitted from an infected person to
What employees should know about UNIVERSAL PRECAUTIONS. They re work practices that help prevent contact with blood and certain other body fluids.
 What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
Basic First Aid. Sue Fisher Emergency Management Coordinator CSUF University Police
 Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
Critical Thinking. Beat the Clock!
 Critical Thinking Beat the Clock! Critical Thinking Making good choices by using information from several sources o Training o Policies and procedures o Communicating/collaborating with other dialysis
Critical Thinking Beat the Clock! Critical Thinking Making good choices by using information from several sources o Training o Policies and procedures o Communicating/collaborating with other dialysis
SARASOTA MEMORIAL HOSPITAL. NURSING PROCEDURE INTRAOSSEOUS NEEDLE: INSERTION, CARE, AND REMOVAL (inv08) 12/18 12/18 1 of 7 RESPONSIBILITY:
 SARASOTA MEMORIAL HOSPITAL TITLE: ISSUED FOR: NURSING PROCEDURE INTRAOSSEOUS NEEDLE: INSERTION, CARE, AND REMOVAL (inv08) Nursing DATE: REVIEWED: PAGES: 12/18 12/18 1 of 7 RESPONSIBILITY: PS1094 Insertion-
SARASOTA MEMORIAL HOSPITAL TITLE: ISSUED FOR: NURSING PROCEDURE INTRAOSSEOUS NEEDLE: INSERTION, CARE, AND REMOVAL (inv08) Nursing DATE: REVIEWED: PAGES: 12/18 12/18 1 of 7 RESPONSIBILITY: PS1094 Insertion-
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Effective Date: Approved by: Laboratory Executive Director, Ed Hughes (electronic signature)
 1 Policy #: 406 (PLH-406-02) Effective Date: NA Reviewed Date: 2/1/2008 Subject: VENIPUNCTURE PROCEDURE Approved by: Laboratory Executive Director, Ed Hughes (electronic signature) Approved by: Laboratory
1 Policy #: 406 (PLH-406-02) Effective Date: NA Reviewed Date: 2/1/2008 Subject: VENIPUNCTURE PROCEDURE Approved by: Laboratory Executive Director, Ed Hughes (electronic signature) Approved by: Laboratory
Portage County EMS Annual Skills Labs
 Portage County EMS Annual Skills Labs Scope: Provide skills labs for all Emergency Medical Responders and First Response EMTs to assure proficiency of skills and satisfy the Wisconsin State approved Operational
Portage County EMS Annual Skills Labs Scope: Provide skills labs for all Emergency Medical Responders and First Response EMTs to assure proficiency of skills and satisfy the Wisconsin State approved Operational
Instructions for Use Neulasta (nu-las-tah) (pegfilgrastim) Injection, for subcutaneous use Single-Dose Prefilled Syringe. Plunger rod Used plunger rod
 Instructions for Use Neulasta (nu-las-tah) (pegfilgrastim) Injection, for subcutaneous use Single-Dose Prefilled Syringe Guide to parts Before use After use Plunger rod Used plunger rod Finger grip Label
Instructions for Use Neulasta (nu-las-tah) (pegfilgrastim) Injection, for subcutaneous use Single-Dose Prefilled Syringe Guide to parts Before use After use Plunger rod Used plunger rod Finger grip Label
IMPORTANT: PLEASE READ
 PART III: CONSUMER INFORMATION ALPROLIX [pronounced all prō liks] Coagulation Factor IX (Recombinant), Fc Fusion Protein This leaflet is part III of a three-part "Product Monograph" published when ALPROLIX
PART III: CONSUMER INFORMATION ALPROLIX [pronounced all prō liks] Coagulation Factor IX (Recombinant), Fc Fusion Protein This leaflet is part III of a three-part "Product Monograph" published when ALPROLIX
Presentation Menu. Walk-in Slide. Full Presentation. Access. Site. Needle. Flush. Comfort. Monitor. Removing the EZ-IO catheter.
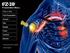 Presentation Menu Walk-in Slide Full Presentation Access Site Needle Flush Comfort Monitor Removing the EZ-IO catheter Clinical Support Explore. Discover. Examine. Vidacare Workshop Programmes www.vidacare.com
Presentation Menu Walk-in Slide Full Presentation Access Site Needle Flush Comfort Monitor Removing the EZ-IO catheter Clinical Support Explore. Discover. Examine. Vidacare Workshop Programmes www.vidacare.com
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Module Summaries: The emergency plan is a crucial part of the total sports program.
 Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Managing Illness 8/9/2010 1
 Managing Illness 1 Fainting Caused by a temporary drop in blood pressure thus causing a reduction in oxygen to the brain. Insufficient oxygen causes casualty to black out and fall. Consciousness normally
Managing Illness 1 Fainting Caused by a temporary drop in blood pressure thus causing a reduction in oxygen to the brain. Insufficient oxygen causes casualty to black out and fall. Consciousness normally
Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System
 1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
Course Syllabus National College of Midwifery /2017
 Course Title: Intrapartum IV Therapy Credits: 0 Course Description: This course covers the indications for IV therapy in labor and delivery, procedures for establishing, administering, and discontinuing
Course Title: Intrapartum IV Therapy Credits: 0 Course Description: This course covers the indications for IV therapy in labor and delivery, procedures for establishing, administering, and discontinuing
Division 1 Introduction to Advanced Prehospital Care
 Division 1 Introduction to Advanced Prehospital Care Chapter 7 Intravenous Access and Medication Administration Part 1 Principles and Routes of Medication Administration Topics Aseptic Technique Medication
Division 1 Introduction to Advanced Prehospital Care Chapter 7 Intravenous Access and Medication Administration Part 1 Principles and Routes of Medication Administration Topics Aseptic Technique Medication
Diabetic Emergencies. Chapter 15
 Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL SERVICES Basic EMT Practical Examination Cardiac Arrest Management
 Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Fluids and electrolytes: the basics
 Fluids and electrolytes: the basics This document is based on the handout from the Surgery for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical
Fluids and electrolytes: the basics This document is based on the handout from the Surgery for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
