Renal Function Recovery in Donors and Recipients after Live Donor Nephrectomy: Hand-Assisted Laparoscopic vs. Open Procedures
|
|
|
- Eustace Green
- 5 years ago
- Views:
Transcription
1 DOI: /kju Laparoscopy/Robotics Renal Function Recovery in s and s after Live Nephrectomy: Hand-Assisted Laparoscopic vs. Open Procedures Bum Soo Kim, Eun Sang Yoo, Tae-Hwan Kim, Tae Gyun Kwon Department of Urology, School of Medicine, Kyungpook National University, Daegu, Korea Purpose: Laparoscopic donor nephrectomy is associated with less postoperative pain and faster recovery times in living kidney donors. However, pneumoperitoneum, which is required in laparoscopic donor nephrectomy, can result in adverse effects on renal function in donors and recipients. We compared renal function in donors and recipients after hand-assisted laparoscopic donor nephrectomy () and open donor nephrectomy (). Materials and Methods: Between January 1997 and January 2008, 241 live donor nephrectomies were performed by either or. Preoperative patient characteristics were not significantly different between the donors and recipients. We monitored the changes in serum creatinine levels of the donors and recipients preoperatively and on postoperative days 1, 5, 28, 84, and 365. Results: The mean operative times of and were 171 and 163 minutes (p=0.284), and the mean warm ischemic times were 292 and 236 seconds (p=0.207), respectively. The mean serum creatinine level in the recipients on postoperative day 1 was significantly higher after than after (3.48 vs mg/dl, p=0.003). However, from postoperative day 5 to 1 year, there was no significant difference between the two groups. The mean serum creatinine level in the donors was not significantly different between the and groups throughout the study period. Conclusions: Renal function recovery in the donors was similar with both and. Graft renal function recovery after was comparable with that after, except immediately after surgery (postoperative day 1). Key Words: Creatinine; Laparoscopy; Living donors; Transplant recipients Article History: received 3 March, 2010 accepted 1 April, 2010 Corresponding Author: Tae Gyun Kwon Department of Urology, School of Medicine, Kyungpook National University, 200, Dongduk-ro, Jung-gu, Daegu , Korea TEL: FAX: tgkwon@knu.ac.kr INTRODUCTION Kidney transplantation is the preferred treatment for endstage renal failure; however, there is still a lack of transplantable organs [1]. In addition to the increased utilization of marginal cadaveric donors, living organ donation has become an alternative means to increase the number of available organs. Before the laparoscopic technique was introduced in the urologic field, open donor nephrectomy () had been the standard method for live donor nephrectomy (LDN). However, a rapid postoperative recovery and return to an active social life have always been concerns, because most donors are healthy and socially active people. Since the first laparoscopic LDN was performed in 1995 by Ratner et al [2], several studies have shown shorter hospital stays, less postoperative pain, and faster times to return to work after LDN than after. However, LDN has its limitations, including potentially longer operating times, longer warm ischemic times, and longer learning curves for the surgeons compared with [3-5]. It also has been reported that laparoscopic surgery causes more ureteral complications and that pneumoperitoneum has adverse effects, which can trigger rejection or delayed graft function as well as poor recovery of the remaining kidney in the donor [1,6,7]. However, hand-assisted laparoscopic donor nephrectomy () has achieved widespread success because it is a safer procedure for both recipient and donor than are the open or the pure laparoscopic procedures [8-10]. Although several recent studies reported that pure LDN had similar or better results than [11,12], is generally easier to perform than is pure Korean Journal of Urology C The Korean Urological Association,
2 246 Kim et al LDN. Despite the advantages of, the impact of pneumoperitoneum on kidney function in the donor and recipient remains controversial. Some studies have shown a decrease in short-term graft function in recipients of laparoscopically procured kidneys [13,14], whereas other studies have shown no differences [3,15,16]. We compared renal function in both donors and recipients after and. MATERIALS AND METHODS We retrospectively reviewed the medical records of donors and recipients after 118 s and 123 s performed between January 1997 and February All donors underwent a routine preoperative evaluation, including a renal scan with glomerular filtration rate (GFR) measurement, three-dimensional magnetic resonance angiography, and/or aortography. The rationale for donor kidney selection for was identical to the standard principles used for. When the kidneys were equal, the left kidney was selected to take advantage of the longer renal vein. However, if the left renal vascular anatomy was unfavorable compared with that of the right, the right kidney was selected. was performed transperitoneally, and was performed retroperitoneally through a flank incision. Mannitol was given before renal vascular clamping in all patients. Surgery in the recipient was performed through a Gibson incision with creation of standard vascular anastomoses and extravesical ureteroneocystostomy. Preoperative demographic data of the donors and recipients are shown in Table 1. Although this was a nonrandomized and retrospective study, characteristics at baseline (e.g., age, sex, and body mass index) were not significantly different between the donors and the recipients. There were 24 and 19 patients with multiple renal arteries in the and groups, respectively (p=0.321). A right side nephrectomy was performed in 30 patients in the group and in 25 patients in the group (p= 0.346) (Table 1). Serum creatinine levels were measured TABLE 1. Preoperative characteristics of the donors and recipients Characteristics Age (years) 39.5 (18-67) 40.5 (23-67) Sex (male/female) 65/53 75/ BMI (kg/m 2 ) Multiple renal artery Left/Right 88/30 98/ Age (years) 35.4 (18-67) 36.5 (19-61) Sex (male/female) 81/37 81/ BMI (kg/m 2 ) : hand-assisted laparoscopic donor nephrectomy, : open donor nephrectomy, BMI: body mass index preoperatively and on days 1, 5, 28, 84, and 365 postoperatively. The GFR measured by renal scan was checked preoperatively and on days 84 and 365 postoperatively. The warm ischemic time was defined as the time from renal artery occlusion to kidney reperfusion. Categorical variables were compared with the chi-square test. Continuous variables were compared with Student s t-test. All analyses were conducted by using SPSS 12.0 for Windows, and statistical significance was accepted at a less than RESULTS The mean operative times of and were 171 and 163 minutes (p=0.284), and the mean warm ischemic times were 292 and 236 seconds (p=0.207), respectively. There was less use of analgesics and shorter lengths of surgical wounds in the group than in the group. If a short ureter length or swelling at the anastomosis site was found, a double-j stent was inserted in the ureter of the recipient (: 12; : 10; p=0.583). Four ureteral complications occurred in the group, and seven occurred in the group (p=0.392) (Table 2). There were no significant differences in preoperative baseline serum creatinine levels between the donors and the recipients of either the or the group. Postoperative changes in serum creatinine levels in both TABLE 2. Comparison of operative parameters between the and the groups Variables Operation time 171±47 163± (min, Mean±SD) Warm ischemic time 292± ± (sec, Mean±SD) Estimated blood loss 207±78 232± (ml, Mean±SD) Time to oral intake 1.4± ± (days, Mean±SD) Surgical complications 2 (1.7%) 0 (0%) (No. of patients [%]) Hospital stay 5.9± ± (days, Mean±SD) Mean analgesics use 168±54 302± (diclofenac sodium, mg, Mean±SD) Mean length of surgical 7.5± ± wound (cm, Mean±SD) Double-J stent insertion (%) 12 (10.2) 10 (8.1) Ureteral complications (No. of patients [%]) 4 (3.4) 7 (5.7) : hand-assisted laparoscopic donor nephrectomy, : open donor nephrectomy, SD: standard deviation
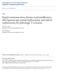
3 Renal Function after Live Nephrectomy 247 TABLE 3. Perioperative mean serum creatinine levels and GFR in donors and recipients Variables FIG. 1. Changes in serum creatinine levels in donors after handassisted laparoscopic donor nephrectomy and open donor nephrectomy. FIG. 2. Changes in serum creatinine levels in recipients after hand-assisted laparoscopic donor nephrectomy and open donor nephrectomy. the donors and the recipients are shown in Fig. 1 and Fig. 2, respectively. The mean serum creatinine level in the recipients on postoperative day 1 was significantly higher in the than in the group (3.48 vs mg/dl, p=0.003). However, from postoperative day 5 to 1 year, there was no significant difference between the two groups. Mean serum creatinine was not significantly different between the two donor groups throughout the study periods. From the third postoperative month, serum creatinine in the and donor groups remained 39% ( mg/dl) and 37% ( mg/dl) higher than preoperative values, respectively. The mean GFR in the donors and the recipients was not significantly different between the two groups on days 84 and 365 postoperatively. Acute rejection occurred in 8 patients in the group (6.8%) and in 7 in the group (5.1%) (p=0.435). Oneyear graft survival rates in the and groups were 96.6% (114/118) and 98.4% (121/123), respectively (p=0.382) (Table 3). Serum creatinine (mg/dl, Mean±SD) Preoperative 0.81± ± POD ± ± POD ± ± POD ± ± POD ± ± POD ± ± Preoperative 10.35± ± POD ± ± POD ± ± POD ± ± POD ± ± POD ± ± GFR (ml/min, Mean±SD) Preoperative ± ± POD ± ± POD ± ± Preoperative 9.09± ± POD ± ± POD ± ± Acute rejection (%) 8 (6.8) 7 (5.1) year graft survival (%) 114 (96.6) 121 (98.4) GFR: glomerular filtration rate, : hand-assisted laparoscopic donor nephrectomy, : open donor nephrectomy, SD: standard deviation, POD: postoperative day DISCUSSION Since 1995, when Ratner et al reported their first experience with laparoscopic live donor nephrectomy [2], the advantages for donors have interested many transplant centers worldwide. The advantages include less postoperative pain, shorter hospital stay, faster recovery times, and fewer long-term complications, such as neuralgia and herniation [1,6]. However, the pure laparoscopic technique for living donor nephrectomy is a technically difficult procedure, and the longer operating times and warm ischemic times compared with the open technique are also perceived as disadvantages of LDN. In contrast, the hand-assisted procedure, which was first successfully performed by Wolf et al [17], has more advantages with the early incision that is necessary for intact organ removal. Several studies have reported more advantages of, such as shorter operating times and warm ischemic times compared with pure LDN [18,19]. In addition to these advantages, has operating times and warm ischemic times comparable with those of and is associated with less postoperative pain, faster recovery times, and better cosmesis [9,20]. Our
4 248 Kim et al study also showed similar results. Although recent studies have reported that pure LDN had similar or better results compared with [11,12], those studies were performed by experienced laparoscopic surgeons. In general, is still considered an effective and safe procedure. It is commonly known that pneumoperitoneum, which is required in laparoscopic procedures, may cause adverse intraoperative effects on the cardiovascular system and renal function [21]. In addition, since the first LDN was performed, adverse effects of donor and graft renal function have been questioned. We investigated renal function in donors and recipients after and on the basis of serum creatinine. Our data suggested no significant differences in renal functional recovery between the and groups in donors (p>0.05). One study reported that the decline in renal function was significantly greater in laparoscopic donors than in open donors on the first postoperative day [7]. However, this difference was no longer evident by the third postoperative day. They speculated that this difference may be secondary to the effect of prolonged pneumoperitoneum on the GFR. Few data exist on the effect of pneumoperitoneum on renal histology. In one experimental study in rats, a prolonged period of pneumoperitoneum did not cause any histologic changes in the kidneys [22]. Hazebroek et al also reported that abdominal insufflation does not have a deleterious effect on histomorphology [23]. However, intraabdominal pressure is known to be a significant factor in decreased renal function. McDougall et al and Kirsch et al showed a decrease in urine output and in GFR with increasing intraabdominal pressure in animal models [24,25]. A pneumoperitoneum of 15 mmhg for 4 hours resulted in a decrease in renal blood flow to 70% of baseline. In our series, we maintained an intraabdominal pressure of 10 to 12 mmhg during. The serum creatinine levels of the donors on the first postoperative day were elevated in both the (1.11 mg/ dl) and the (1.19 mg/dl) groups. However, there was no significant difference between the two groups (p=0.055). Of interest was the similarity in serum creatinine levels between both donor groups, which remained 39% ( mg/dl) and 37% ( mg/dl) higher than preoperative levels in the and groups, respectively. This finding was comparable with that of Goldfarb et al, who found an increase of approximately 30% [26]. Although, in our study, was performed through a transperitoneal approach and was performed through a retroperitoneal approach, the difference in technique did not seem to have an effect on renal function recovery. A previous study by Dols et al reported that there was no significant difference on renal function between retroperitoneoscopic donor nephrectomy and transperitoneal laparoscopic donor nephrectomy groups [27]. Several previous studies have reported the effects of LDN on recipient graft function [2,13]. Nogueira et al compared graft function in recipients after 132 LDNs and 99 s [13]. The mean serum creatinine was significantly higher in the LDN group during the first week after transplant, but was similar between groups at 3 months. In another study, by Ratner et al, 110 LDN patients were compared with 48 patients [14]. This study also showed a higher serum creatinine level on days 2 and 3 in the LDN group, but no significant difference by day 4. Early graft function was also compared between LDNs and s by using information in the United Network for Organ Sharing database [28]. This study compared 2734 LDNs and 2576 s that were performed over a 13-month period from 1999 to In this study, significantly more patients in the LDN group than in the group had creatinine levels greater than 1.4 or 2 mg/dl at discharge. However, all subsequent serum creatinine levels and graft survival at 1 year were similar between the two groups. In our study, the mean serum creatinine level in recipients was higher in the group (3.48 mg/dl) than in the group (2.62 mg/dl) on the first postoperative day (p=0.003). After the fifth postoperative day, however, the mean serum creatinine level was comparable until 1 year after transplant (1.41 vs mg/dl, p=0.920). Pure LDN might cause relatively long warm ischemic times, mainly because of the long time required to extract the kidney through a small incision. However, may reduce kidney extraction and warm ischemic times, even for a non-experienced laparoscopic surgeon, because of the early incision that is necessary for intact organ removal. In our study, the mean warm ischemic time was not significantly different between the and groups. Moreover, in a review of 100 LDNs, only recipients of kidneys with a warm ischemic time greater than 10 minutes had serum creatinine levels greater than 2 mg/dl on postoperative day 7 [5]. In animal models, postoperative serum creatinine levels were significantly increased when the warm ischemic time was greater than 30 minutes [29]. Although the warm ischemic time in our group (290 seconds) was longer than that reported in other studies [18], it was acceptably low and did not appear to cause any significant renal ischemic injury or affect short-term functional recovery or our longer-term results. Our 1-year and graft survival rates were 96.6% and 98.4%, respectively, and were not significantly different between the two groups (p=0.382). Other studies of laparoscopic graft survival have shown results (91-95%) similar to those of our study [14,28,30]. The number of rejection episodes also did not differ significantly between the (8/118, 6.8%) and the (7/123, 5.1%) groups (p=0.435), nor did other complications, such as ureteral complications (p=0.392). Recently published data provide additional support for the benefits of laparoscopic living donor nephrectomies. Peritransplantation morbidity and mortality data have been reported after both open and laparoscopic procedures. Our data indicate almost no significant differences in renal function recovery between donors and recipients between the and groups, although serum creatinine levels in the recipients were higher in the group than in the group on the first postoperative day. Renal
5 Renal Function after Live Nephrectomy 249 function recovery was comparable between the and groups. CONCLUSIONS This retrospective study showed that, although serum creatinine levels in the recipients were higher in the group than in the group on the first postoperative day, renal function recovery was similar in donors and recipients in both the and groups. The results of our study indicate that long-term functional outcomes are not significantly different between kidneys obtained laparoscopically or via the open approach at our institution. Conflicts of Interest The authors have nothing to disclose. REFERENCES 1. Giessing M. Laparoscopic living-donor nephrectomy. Nephrol Dial Transplant 2004;19(Suppl 4): Ratner LE, Ciseck LJ, Moore RG, Cigarroa FG, Kaufman HS, Kavoussi LR. Laparoscopic live donor nephrectomy. Transplantation 1995;60: Ratner LE, Kavoussi LR, Schulam PG, Bender JS, Magnuson TH, Montgomery R. Comparison of laparoscopic live donor nephrectomy versus the standard open approach. Transplant Proc 1997;29: Yoo KY, Hong SH, Hwang TK. nephrectomy: comparison of open, hand-assisted and laparoscopic donor nephrectomy. Korean J Urol 2006;47: Sasaki TM, Finelli F, Bugarin E, Fowlkes D, Trollinger J, Barhyte DY, et al. Is laparoscopic donor nephrectomy the new criterion standard? Arch Surg 2000;135: Lennerling A, Blohme I, Ostraat O, Lönroth H, Olausson M, Nyberg G. Laparoscopic or open surgery for living donor nephrectomy. Nephrol Dial Transplant 2001;16: Vats HS, Rayhill SC, Thomas CP. Early postnephrectomy donor renal function: laparoscopic versus open procedure. Transplantation 2005;79: Rawlins MC, Hefty TL, Brown SL, Biehl TR. Learning laparoscopic donor nephrectomy safely: a report on 100 cases. Arch Surg 2002;137: Slakey DP, Hahn JC, Rogers E, Rice JC, Gauthier PM, Ruiz-Deya G. Single-center analysis of living donor nephrectomy: hand-assisted laparoscopic, pure laparoscopic, and traditional open. Prog Transplant 2002;12: Waller JR, Hiley AL, Mullin EJ, Veitch PS, Nicholson ML. Living kidney donation: a comparison of laparoscopic and conventional open operations. Postgrad Med J 2002;78: Branco AW, Kondo W, Branco Filho AJ, George MA, Rangel M, Stunitz LC. A comparison of hand-assisted and pure laparoscopic techniques in live donor nephrectomy. Clinics 2008;63: Percegona LS, Bignelli AT, Adamy A Jr, Pilz F, Chin EW, Meyer F, et al. Hand-assisted laparoscopic donor nephrectomy: comparison to pure laparoscopic donor nephrectomy. Transplant Proc 2008;40: Nogueira JM, Cangro CB, Fink JC, Schweitzer E, Wiland A, Klassen DK, et al. A comparison of recipient renal outcomes with laparoscopic versus open live donor nephrectomy. Transplantation 1999;67: Ratner LE, Montgomery RA, Maley WR, Cohen C, Burdick J, Chavin KD, et al. Laparoscopic live donor nephrectomy: the recipient. Transplantation 2000;69: Philosophe B, Kuo PC, Schweitzer EJ, Farney AC, Lim JW, Johnson LB, et al. Laparoscopic versus open donor nephrectomy: comparing ureteral complications in the recipients and improving the laparoscopic technique. Transplantation 1999;68: Wolf JS Jr, Merion RM, Leichtman AB, Campbell DA Jr, Magee JC, Punch JD, et al. Randomized controlled trial of hand-assisted laparoscopic versus open surgical live donor nephrectomy. Transplantation 2001;72: Wolf JS Jr, Tchetgen MB, Merion RM. Hand-assisted laparoscopic live donor nephrectomy. Urology 1998;52: Gershbein AB, Fuchs GJ. Hand-assisted and conventional laparoscopic live donor nephrectomy: a comparison of two contemporary techniques. J Endourol 2002;16: Kokkinos C, Nanidis T, Antcliffe D, Darzi AW, Tekkis P, Papalois V. Comparison of laparoscopic versus hand-assisted live donor nephrectomy. Transplantation 2007;83: Baik S, Rho J, Kim CS. Comparison of hand-assisted laparoscopic donor nephrectomy with open donor nephrectomy. Korean J Urol 2005;46: London ET, Ho HS, Neuhaus AM, Wolfe BM, Rudich SM, Perez RV. Effect of intravascular volume expansion on renal function during prolonged CO2 pneumoperitoneum. Ann Surg 2000;231: Lee BR, Cadeddu JA, Molnar-Nadasdy G, Enriquez D, Nadasdy T, Kavoussi LR, et al. Chronic effect of pneumoperitoneum on renal histology. J Endourol 1999;13: Hazebroek EJ, de Bruin RW, Bouvy ND, Marquet RL, Bonthuis F, Bajema IM, et al. Long-term impact of pneumoperitoneum used for laparoscopic donor nephrectomy on renal function and histomorphology in donor and recipient rats. Ann Surg 2003;237: McDougall EM, Monk TG, Wolf JS Jr, Hicks M, Clayman RV, Gardner S, et al. The effect of prolonged pneumoperitoneum on renal function in an animal model. J Am Coll Surg 1996;182: Kirsch AJ, Hensle TW, Chang DT, Kayton ML, Olsson CA, Sawczuk IS. Renal effects of CO2 insufflation: oliguria and acute renal dysfunction in a rat pneumoperitoneum model. Urology 1994;43: Goldfarb DA, Matin SF, Braun WE, Schreiber MJ, Mastroianni B, Papajcik D, et al. Renal outcome 25 years after donor nephrectomy. J Urol 2001;166: Dols LF, Kok NF, Terkivatan T, Tran KT, Alwayn IP, Weimar W, et al. Optimizing left-sided live kidney donation: hand-assisted retroperitoneoscopic as alternative to standard laparoscopic donor nephrectomy. Transpl Int 2009;Epub ahead of print 28. Troppmann C, Ormond DB, Perez RV. Laparoscopic (vs open) live donor nephrectomy: a UNOS database analysis of early graft function and survival. Am J Transplant 2003;3: Jablonski P, Howden BO, Rae DA, Birrell CS, Marshall VC, Tange J. An experimental model for assessment of renal recovery from warm ischemia. Transplantation 1983;35: Jacobs SC, Cho E, Dunkin BJ, Flowers JL, Schweitzer E, Cangro C, et al. Laparoscopic live donor nephrectomy: the University of Maryland 3-year experience. J Urol 2000;164:
Does carbon dioxide pneumoperitoneum affect the renal function in donors following laparoscopic donor nephrectomy? A prospective study
 Original Article Does carbon dioxide pneumoperitoneum affect the renal function in donors following laparoscopic donor nephrectomy? A prospective study Murali Vinodh, Vijaykumar Mohankumar, Arvind Ganpule,
Original Article Does carbon dioxide pneumoperitoneum affect the renal function in donors following laparoscopic donor nephrectomy? A prospective study Murali Vinodh, Vijaykumar Mohankumar, Arvind Ganpule,
OUTCOME OF LAPAROSCOPIC DONOR NEPHRECTOMY: OUR INSTITUTIONAL EXPERIENCE
 OUTCOME OF LAPAROSCOPIC DONOR NEPHRECTOMY: OUR INSTITUTIONAL EXPERIENCE Rajaraman Thiagarajan 1, Balaji A. R 2, Ayesha Shaheen 3, Chandramurali Raveendran 4, Subhakanesh S 5, Ashok Kumar R 6, Jessima S
OUTCOME OF LAPAROSCOPIC DONOR NEPHRECTOMY: OUR INSTITUTIONAL EXPERIENCE Rajaraman Thiagarajan 1, Balaji A. R 2, Ayesha Shaheen 3, Chandramurali Raveendran 4, Subhakanesh S 5, Ashok Kumar R 6, Jessima S
Study on outcome of laparoscopic donor nephrectomy
 International Surgery Journal Kanesh SSK et al. Int Surg J. 2017 Aug;4(8):2811-2815 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20173424
International Surgery Journal Kanesh SSK et al. Int Surg J. 2017 Aug;4(8):2811-2815 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20173424
Impact of Intraoperative Donor Management on Short-Term Renal Function After Laparoscopic Donor Nephrectomy
 ANNALS OF SURGERY Vol. 236, No. 1, 127 132 2002 Lippincott Williams & Wilkins, Inc. Impact of Intraoperative Donor Management on Short-Term Renal Function After Laparoscopic Donor Nephrectomy Eric J. Hazebroek,
ANNALS OF SURGERY Vol. 236, No. 1, 127 132 2002 Lippincott Williams & Wilkins, Inc. Impact of Intraoperative Donor Management on Short-Term Renal Function After Laparoscopic Donor Nephrectomy Eric J. Hazebroek,
THE NEW ZEALAND MEDICAL JOURNAL
 THE NEW ZEALAND MEDICAL JOURNAL Vol 116 No 1178 ISSN 1175 8716 The Auckland experience with laparoscopic donor nephrectomy Carl Muthu, John McCall, John Windsor, Richard Harman, Ian Dittmer, Pat Smith
THE NEW ZEALAND MEDICAL JOURNAL Vol 116 No 1178 ISSN 1175 8716 The Auckland experience with laparoscopic donor nephrectomy Carl Muthu, John McCall, John Windsor, Richard Harman, Ian Dittmer, Pat Smith
Donor Kidney Recovery Methods and the Incidence of Lymphatic Complications in Kidney Transplant Recipients
 Donor Kidney Recovery Methods and the Incidence of Lymphatic Complications in Kidney Transplant Recipients The Harvard community has made this article openly available. Please share how this access benefits
Donor Kidney Recovery Methods and the Incidence of Lymphatic Complications in Kidney Transplant Recipients The Harvard community has made this article openly available. Please share how this access benefits
Critical Analysis of Laparoscopic Donor Nephrectomy in the Setting of Complex Renal Vasculature: Initial Experience and Intermediate Outcomes
 JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 451 455 DOI: 10.1089=end.2008.0242 Critical Analysis of Laparoscopic Donor Nephrectomy in the Setting of Complex Renal
JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 451 455 DOI: 10.1089=end.2008.0242 Critical Analysis of Laparoscopic Donor Nephrectomy in the Setting of Complex Renal
K idney transplantation is widely accepted as the best form
 153 ORIGINAL ARTICLE Living kidney donation: a comparison of laparoscopic and conventional open operations J R Waller, A L Hiley, E J Mullin, P S Veitch, M L Nicholson... See end of article for authors
153 ORIGINAL ARTICLE Living kidney donation: a comparison of laparoscopic and conventional open operations J R Waller, A L Hiley, E J Mullin, P S Veitch, M L Nicholson... See end of article for authors
Early Experience of a Living Donor Kidney Transplant Program
 european urology 50 (2006) 542 548 available at www.sciencedirect.com journal homepage: www.europeanurology.com Laparoscopy Early Experience of a Living Donor Kidney Transplant Program Antonio Alcaraz
european urology 50 (2006) 542 548 available at www.sciencedirect.com journal homepage: www.europeanurology.com Laparoscopy Early Experience of a Living Donor Kidney Transplant Program Antonio Alcaraz
Morbidity and Mortality After Living Kidney Donation, : Survey of United States Transplant Centers
 American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
Renal Function Outcomes in Patients Undergoing Open or Laparoscopic Radical Nephrectomy
 Renal Function Outcomes in Patients Undergoing Open or Laparoscopic Radical Nephrectomy Koo Han Yoo, Hyung-Lae Lee, Sung-Goo Chang, Seung Hyun Jeon From the Department of Urology, Kyung Hee University
Renal Function Outcomes in Patients Undergoing Open or Laparoscopic Radical Nephrectomy Koo Han Yoo, Hyung-Lae Lee, Sung-Goo Chang, Seung Hyun Jeon From the Department of Urology, Kyung Hee University
Postoperative Pain and Convalescence in Living Kidney Donors Laparoscopic Versus Open Donor Nephrectomy: A Randomized Study
 American Journal of Transplantation 2006; 6: 1438 1443 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2006; 6: 1438 1443 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
COMPARISON OF LAPAROSCOPIC LIVE DONOR NEPHRECTOMY VERSUS THE TRADITIONAL OPEN TECHNIQUE
 Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 394-402, September - October, 2002 COMPARISON OF LAPAROSCOPIC LIVE DONOR NEPHRECTOMY VERSUS
Clinical Urology International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 394-402, September - October, 2002 COMPARISON OF LAPAROSCOPIC LIVE DONOR NEPHRECTOMY VERSUS
Right Versus Left Laparoscopic Living-Donor Nephrectomy: A Meta-Analysis
 ARTICle Right Versus Left Laparoscopic Living-Donor Nephrectomy: A Meta-Analysis Kun Wang, Peijin Zhang, Xianlin Xu, Min Fan Abstract Objectives: We assessed the safety and efficacy of right versus left
ARTICle Right Versus Left Laparoscopic Living-Donor Nephrectomy: A Meta-Analysis Kun Wang, Peijin Zhang, Xianlin Xu, Min Fan Abstract Objectives: We assessed the safety and efficacy of right versus left
Laparoscopic donor nephrectomy in unusual venous anatomy donor and recepient implications
 ORIGINAL ARTICLE Vol. 43 (4): 671-678, July - August, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0309 Laparoscopic donor nephrectomy in unusual venous anatomy donor and recepient implications Avinash Bapusaheb
ORIGINAL ARTICLE Vol. 43 (4): 671-678, July - August, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0309 Laparoscopic donor nephrectomy in unusual venous anatomy donor and recepient implications Avinash Bapusaheb
25. Fluid Management and Renal Function During a Laparoscopic Case Done Under CO 2 Pneumoperitoneum
 25. Fluid Management and Renal Function During a Laparoscopic Case Done Under CO 2 Pneumoperitoneum Gamal Mostafa, M.D. Frederick L. Greene, M.D. Minimally invasive surgery aims to attenuate the stress
25. Fluid Management and Renal Function During a Laparoscopic Case Done Under CO 2 Pneumoperitoneum Gamal Mostafa, M.D. Frederick L. Greene, M.D. Minimally invasive surgery aims to attenuate the stress
Laparoscopic Living-Donor Nephrectomy: Analysis of the Existing Literature
 EUROPEAN UROLOGY 58 (2010) 498 509 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Collaborative Review Transplantation Editorial by Eric Lechevallier on
EUROPEAN UROLOGY 58 (2010) 498 509 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Collaborative Review Transplantation Editorial by Eric Lechevallier on
Hand-Assisted Laparoscopic Right Donor Nephrectomy: Safety and Feasibility
 www.kjurology.org DOI:10.4111/kju.2010.51.1.34 Laparoscopy/Robotics Hand-Assisted Laparoscopic Right Donor Nephrectomy: Safety and Feasibility Moon-Soo Chung, Su Jin Kim, Hyuk Jin Cho, U-Syn Ha, Sung-Hoo
www.kjurology.org DOI:10.4111/kju.2010.51.1.34 Laparoscopy/Robotics Hand-Assisted Laparoscopic Right Donor Nephrectomy: Safety and Feasibility Moon-Soo Chung, Su Jin Kim, Hyuk Jin Cho, U-Syn Ha, Sung-Hoo
Back-to-back comparison of mini-open vs. laparoscopic technique for living kidney donation
 Original research Back-to-back comparison of mini-open vs. laparoscopic technique for living kidney donation Christie Rampersad, MD; 1 Premal Patel, MD; 2 Joshua Koulack, MD; 3 Thomas McGregor, MD 2 1
Original research Back-to-back comparison of mini-open vs. laparoscopic technique for living kidney donation Christie Rampersad, MD; 1 Premal Patel, MD; 2 Joshua Koulack, MD; 3 Thomas McGregor, MD 2 1
Obesity Is an Adverse Factor on Laparoscopic Radical Nephrectomy for T2 but Not T1 Renal Cell Carcinoma
 Endourology www.kjurology.org http://dx.doi.org/.4/kju.2.52.8.58 Obesity Is an Adverse Factor on Laparoscopic Radical Nephrectomy for T2 but Not T Renal Cell Carcinoma Se Yun Kwon, Jae Jun Bae, Jung Gon
Endourology www.kjurology.org http://dx.doi.org/.4/kju.2.52.8.58 Obesity Is an Adverse Factor on Laparoscopic Radical Nephrectomy for T2 but Not T Renal Cell Carcinoma Se Yun Kwon, Jae Jun Bae, Jung Gon
ORIGINAL ARTICLE. Experience With Laparoscopic Donor Nephrectomy Among More Than 1000 Cases. Low Complication Rates, Despite More Challenging Cases
 ORIGINAL ARTICLE Experience With Laparoscopic Donor Nephrectomy Among More Than 1000 Cases Low Complication Rates, Despite More Challenging Cases Aaron J. Ahearn, MD, PhD; Andrew M. Posselt, MD, PhD; Sang-Mo
ORIGINAL ARTICLE Experience With Laparoscopic Donor Nephrectomy Among More Than 1000 Cases Low Complication Rates, Despite More Challenging Cases Aaron J. Ahearn, MD, PhD; Andrew M. Posselt, MD, PhD; Sang-Mo
Anaesthesia for living donor renal transplant nephrectomy
 Anaesthesia for living donor renal transplant nephrectomy Benjamin O Brien MD FRCA FFICM Marta Koertzen FRCA 2A07 2C06 Key points Living donor nephrectomy involves unique ethical considerations. Fit and
Anaesthesia for living donor renal transplant nephrectomy Benjamin O Brien MD FRCA FFICM Marta Koertzen FRCA 2A07 2C06 Key points Living donor nephrectomy involves unique ethical considerations. Fit and
Laparoscopic Nephrectomy: New Standard of Care?
 Original Article Laparoscopic Nephrectomy: New Standard of Care? Hong Gee Sim, Sidney K.H. Yip, Chee Yong Ng, Yee Sze Teo, Yeh Hong Tan, Woei Yun Siow and Wai Sam Cheng, Department of Urology, Singapore
Original Article Laparoscopic Nephrectomy: New Standard of Care? Hong Gee Sim, Sidney K.H. Yip, Chee Yong Ng, Yee Sze Teo, Yeh Hong Tan, Woei Yun Siow and Wai Sam Cheng, Department of Urology, Singapore
Clinical Study Morbidity of 200 Consecutive Cases of Hand-Assisted Laparoscopic Living Donor Nephrectomies: A Single-Center Experience
 Transplantation Volume 212, Article ID 121523, 7 pages doi:1.1155/212/121523 Clinical Study Morbidity of 2 Consecutive Cases of Hand-Assisted Laparoscopic Living Donor Nephrectomies: A Single-Center Experience
Transplantation Volume 212, Article ID 121523, 7 pages doi:1.1155/212/121523 Clinical Study Morbidity of 2 Consecutive Cases of Hand-Assisted Laparoscopic Living Donor Nephrectomies: A Single-Center Experience
R.C. Minnee*, M.M. Idu
 R e v i e w Laparoscopic donor nephrectomy R.C. Minnee*, M.M. Idu Department of Surgery, Academic Medical Centre, Amsterdam, the Netherlands, *corresponding author: tel.: +31 (0)20-566 78 32, fax: +31
R e v i e w Laparoscopic donor nephrectomy R.C. Minnee*, M.M. Idu Department of Surgery, Academic Medical Centre, Amsterdam, the Netherlands, *corresponding author: tel.: +31 (0)20-566 78 32, fax: +31
Retroperitoneoscopic Radical Nephrectomy: Initial Experience
 Retroperitoneoscopic Radical Nephrectomy: Initial Experience A. Hasegan 1, D. Bratu 2, V. Pirvut 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Department of Urology 2 Lucian Blaga University
Retroperitoneoscopic Radical Nephrectomy: Initial Experience A. Hasegan 1, D. Bratu 2, V. Pirvut 1, I. Mihai 1, N. Grigore 1 1 Lucian Blaga University of Sibiu, Department of Urology 2 Lucian Blaga University
Over the past decade, the annual supply of renal allografts
 ORIGINAL ARTICLE Laparoscopic Live Donor Nephrectomy Trends in Donor and Recipient Morbidity Following 381 Consecutive Cases Li-Ming Su, MD,* Lloyd E. Ratner, MD, Robert A. Montgomery, MD, PhD, Thomas
ORIGINAL ARTICLE Laparoscopic Live Donor Nephrectomy Trends in Donor and Recipient Morbidity Following 381 Consecutive Cases Li-Ming Su, MD,* Lloyd E. Ratner, MD, Robert A. Montgomery, MD, PhD, Thomas
Transition From Hand-Assisted to Pure Laparoscopic Donor Nephrectomy
 SCIENTIFIC PAPER Transition From Hand-Assisted to Pure Laparoscopic Donor Nephrectomy Dalsan You, MD, PhD, Chunwoo Lee, MD, In Gab Jeong, MD, PhD, Duck Jong Han, MD, PhD, Bumsik Hong, MD, PhD ABSTRACT
SCIENTIFIC PAPER Transition From Hand-Assisted to Pure Laparoscopic Donor Nephrectomy Dalsan You, MD, PhD, Chunwoo Lee, MD, In Gab Jeong, MD, PhD, Duck Jong Han, MD, PhD, Bumsik Hong, MD, PhD ABSTRACT
Kidney transplantation is the last stage of kidney INTRODUCTION MATERIALS AND METHODS KIDNEY TRANSPLANTATION
 KIDNEY TRANSPLANTATION Bolus Injection Versus Infusion of Furosemide in Kidney Transplantation: A Randomized Clinical Trial Afshar Zomorrodi 1, Hassan Mohammadipoor Anvari 2 *, Farzad Kakaei 3, Farzin
KIDNEY TRANSPLANTATION Bolus Injection Versus Infusion of Furosemide in Kidney Transplantation: A Randomized Clinical Trial Afshar Zomorrodi 1, Hassan Mohammadipoor Anvari 2 *, Farzad Kakaei 3, Farzin
Review Article Donor Complications Following Laparoscopic Compared to Hand-Assisted Living Donor Nephrectomy: An Analysis of the Literature
 Journal of Transplantation Volume 2010, Article ID 825689, 10 pages doi:10.1155/2010/825689 Review Article Donor Complications Following Laparoscopic Compared to Hand-Assisted Living Donor Nephrectomy:
Journal of Transplantation Volume 2010, Article ID 825689, 10 pages doi:10.1155/2010/825689 Review Article Donor Complications Following Laparoscopic Compared to Hand-Assisted Living Donor Nephrectomy:
Surgical techniques in living donor nephrectomy GUIDELINES
 88..95 NEPHROLOGY 2010; 15, S88 S95 doi:10.1111/j.1440-1797.2009.01214.x Surgical techniques in living donor Date written: September 2007nep_1214 Final submission: October 2008 Author: Norma Gibbons, David
88..95 NEPHROLOGY 2010; 15, S88 S95 doi:10.1111/j.1440-1797.2009.01214.x Surgical techniques in living donor Date written: September 2007nep_1214 Final submission: October 2008 Author: Norma Gibbons, David
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
Postoperative monitoring after
 Postoperative monitoring after kidney transplantation Bundit sakulchairungrueng,md Vascular and Transplantation Unit Faculty of Medicine Ramathibodi Hospital Mahidol University Reference Introduction A
Postoperative monitoring after kidney transplantation Bundit sakulchairungrueng,md Vascular and Transplantation Unit Faculty of Medicine Ramathibodi Hospital Mahidol University Reference Introduction A
Vascular Management During Live Donor Nephrectomy: An Online Survey Among Transplant Surgeons
 American Journal of Transplantation 2015; 15: 1701 1707 Wiley Periodicals Inc. Brief Communication C Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons
American Journal of Transplantation 2015; 15: 1701 1707 Wiley Periodicals Inc. Brief Communication C Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
Transplant surgery: the latest
 Transplant surgery: the latest Professor Nizam Mamode Guy s and St Thomas Hospital Evelina London Children s Hospital Great Ormond Street Hospital What do we do? Page 2 Kidney transplants Living donor
Transplant surgery: the latest Professor Nizam Mamode Guy s and St Thomas Hospital Evelina London Children s Hospital Great Ormond Street Hospital What do we do? Page 2 Kidney transplants Living donor
Anesthetic Management of Laparoscopic Surgery for a Patient with
 Anesthetic Management of Laparoscopic Surgery for a Patient with a Ventriculoperitoneal shunt Abstract With the advances in the management of hydrocephalus, patients with ventriculoperitoneal shunt are
Anesthetic Management of Laparoscopic Surgery for a Patient with a Ventriculoperitoneal shunt Abstract With the advances in the management of hydrocephalus, patients with ventriculoperitoneal shunt are
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study
 Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor
 Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
Laparoscopic Radical Nephrectomy- the current gold standard
 Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Single-center comparison of purely laparoscopic, hand-assisted laparoscopic, and open radical nephrectomy in patients at high anesthetic risk
 Single-center comparison of purely laparoscopic, hand-assisted laparoscopic, and open radical nephrectomy in patients at high anesthetic risk Baldwin D D, Dunbar J A, Parekh D J, Wells N, Shuford M D,
Single-center comparison of purely laparoscopic, hand-assisted laparoscopic, and open radical nephrectomy in patients at high anesthetic risk Baldwin D D, Dunbar J A, Parekh D J, Wells N, Shuford M D,
Laparoscopic versus open living donor nephrectomy
 Laparoscopic versus open living donor nephrectomy M.Y. Smits-Lind This thesis was financially supported by: Nierstichting Nederland Johnson & Johnson Medical B.V. Fujisawa Holland B.V. Roche Nederland
Laparoscopic versus open living donor nephrectomy M.Y. Smits-Lind This thesis was financially supported by: Nierstichting Nederland Johnson & Johnson Medical B.V. Fujisawa Holland B.V. Roche Nederland
C.I. Villeda-Sandoval, et al.: Gender matching in renal transplantation. Contents available at PubMed Gac Med Mex. 2016;152:
 Contents available at PubMed www.anmm.org.mx PERMANYER Gac Med Mex. 206;52:579-83 www.permanyer.com GACETA MÉDICA DE MÉXICO ORIGINAL ARTICLE The impact of donor-to-recipient gender match and mismatch on
Contents available at PubMed www.anmm.org.mx PERMANYER Gac Med Mex. 206;52:579-83 www.permanyer.com GACETA MÉDICA DE MÉXICO ORIGINAL ARTICLE The impact of donor-to-recipient gender match and mismatch on
Who are Candidates for Laparoscopic or Open Radical Nephrectomy. Arieh Shalhav
 Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
PAPER. More Than 500 Consecutive Laparoscopic Donor Nephrectomies Without Conversion or Repeated Surgery
 PAPER More Than 500 Consecutive Laparoscopic Donor Nephrectomies Without Conversion or Repeated Surgery Marc L. Melcher, MD, PhD; Jonathan T. Carter, MD; Andrew Posselt, MD, PhD; Quan-Yang Duh, MD; Marshall
PAPER More Than 500 Consecutive Laparoscopic Donor Nephrectomies Without Conversion or Repeated Surgery Marc L. Melcher, MD, PhD; Jonathan T. Carter, MD; Andrew Posselt, MD, PhD; Quan-Yang Duh, MD; Marshall
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE. Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham
 SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA
 1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Pediatric Kidney Transplantation
 Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Identifying unrecognized collecting system entry and the integrity of repair during open partial nephrectomy: comparison of two techniques
 ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments
 Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Secondary surgery for vesicoureteral reflux after failed endoscopic injection: Comparison to primary surgery
 Original Article - Pediatric Urology pissn 2466-0493 eissn 2466-054X Secondary surgery for vesicoureteral reflux after failed endoscopic injection: Comparison to primary surgery Seungsoo Lee, Seung Chan
Original Article - Pediatric Urology pissn 2466-0493 eissn 2466-054X Secondary surgery for vesicoureteral reflux after failed endoscopic injection: Comparison to primary surgery Seungsoo Lee, Seung Chan
Acute kidney injury and outcomes in acute decompensated heart failure in Korea
 Acute kidney injury and outcomes in acute decompensated heart failure in Korea Mi-Seung Shin 1, Seong Woo Han 2, Dong-Ju Choi 3, Eun Seok Jeon 4, Jae-Joong Kim 5, Myeong-Chan Cho 6, Shung Chull Chae 7,
Acute kidney injury and outcomes in acute decompensated heart failure in Korea Mi-Seung Shin 1, Seong Woo Han 2, Dong-Ju Choi 3, Eun Seok Jeon 4, Jae-Joong Kim 5, Myeong-Chan Cho 6, Shung Chull Chae 7,
Open and laparoscopic living donor nephrectomy in Switzerland: a retrospective assessment of clinical outcomes and the motivation to donate
 Nephrol Dial Transplant (2006) 21: 2563 2568 doi:10.1093/ndt/gfl207 Advance Access publication 15 May 2006 Original Article Open and laparoscopic living donor nephrectomy in Switzerland: a retrospective
Nephrol Dial Transplant (2006) 21: 2563 2568 doi:10.1093/ndt/gfl207 Advance Access publication 15 May 2006 Original Article Open and laparoscopic living donor nephrectomy in Switzerland: a retrospective
Rapid communication chronic renal insufficiency after laparoscopic partial nephrectomy and radical nephrectomy for pathologic T1a lesions
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 Rapid communication chronic renal insufficiency after laparoscopic partial nephrectomy and radical nephrectomy
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 Rapid communication chronic renal insufficiency after laparoscopic partial nephrectomy and radical nephrectomy
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic partial nephrectomy 308 Introduction This overview has been
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic partial nephrectomy 308 Introduction This overview has been
Bariatric Surgery For Patients With End-Organ Failure
 Bariatric Surgery For Patients With End-Organ Failure Arnold D. Salzberg, M.D. Andrew M. Posselt, M.D., PhD Divisions of Transplant and Minimally Invasive Surgery University of California, San Francisco
Bariatric Surgery For Patients With End-Organ Failure Arnold D. Salzberg, M.D. Andrew M. Posselt, M.D., PhD Divisions of Transplant and Minimally Invasive Surgery University of California, San Francisco
Outcome and Complications of Living Donor Pediatric Renal Transplant: A Tertiary Center Experience
 Outcome and Complications of Living Donor Pediatric Renal Transplant: A Tertiary Center Experience Dr Priyank Bijalwan, Dr Balagopal Nair, Dr Appu Thomas, Dr Ginil Kumar, Dr Georgie Mathew, Dr KV Sanjeevan,
Outcome and Complications of Living Donor Pediatric Renal Transplant: A Tertiary Center Experience Dr Priyank Bijalwan, Dr Balagopal Nair, Dr Appu Thomas, Dr Ginil Kumar, Dr Georgie Mathew, Dr KV Sanjeevan,
Assessment of Deceased Donor Kidneys Using a Donor Scoring System
 Original Article DOI 1.3349/ymj.1.51.6.87 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 51(6):87-876, 1 Assessment of Deceased Donor Kidneys Using a Donor Scoring System Kitae Bang, 1 Han Kyu Lee, 1 Wooseong
Original Article DOI 1.3349/ymj.1.51.6.87 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 51(6):87-876, 1 Assessment of Deceased Donor Kidneys Using a Donor Scoring System Kitae Bang, 1 Han Kyu Lee, 1 Wooseong
Ureteral length in live donor kidney transplantation; Does size matter?
 Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Ureteral length in live donor kidney transplantation; Does size matter? Liselotte S. S. Ooms, 1 Inez K. B. Slagt, 1 Frank J. M. F. Dor, 1 Hendrikus
Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Ureteral length in live donor kidney transplantation; Does size matter? Liselotte S. S. Ooms, 1 Inez K. B. Slagt, 1 Frank J. M. F. Dor, 1 Hendrikus
Comparison of Video-Assisted Minilaparotomy, Open, and Laparoscopic Partial Nephrectomy for Renal Masses
 Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.151 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):151-157, 2012 Comparison of Video-Assisted Minilaparotomy, Open, and Laparoscopic Partial
Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.151 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):151-157, 2012 Comparison of Video-Assisted Minilaparotomy, Open, and Laparoscopic Partial
Vol. 29, pp.585 ~ 589, ml. 1.6 mg/dl 1 MRSA. Table 1 MRI
 Vol. 29, pp.585 ~ 589, 2001 8 13 10 22 8 7 1 14 49 26.1 6 2 ABO 7 1 400 800 ml 5 4 10 4 3 3 ABO 3 4 5 5 1 3 4 1 0.8 1.6 mg/dl 1 MRSA 10 7 1 10 7 22 40 8 CYA+ AZ+ MP 3 4 7 GSP 4 1 Table 1 23 1 15 11 5 Alport
Vol. 29, pp.585 ~ 589, 2001 8 13 10 22 8 7 1 14 49 26.1 6 2 ABO 7 1 400 800 ml 5 4 10 4 3 3 ABO 3 4 5 5 1 3 4 1 0.8 1.6 mg/dl 1 MRSA 10 7 1 10 7 22 40 8 CYA+ AZ+ MP 3 4 7 GSP 4 1 Table 1 23 1 15 11 5 Alport
Complications in robotic surgery!! Review of the literature! RALP, RAPN and RARC!
 Complications in robotic surgery Review of the literature RALP, RAPN and RARC Anna Wallerstedt, MD Karolinska University Hospital Stockholm, Sweden Agenda The importance of reporting surgical complications
Complications in robotic surgery Review of the literature RALP, RAPN and RARC Anna Wallerstedt, MD Karolinska University Hospital Stockholm, Sweden Agenda The importance of reporting surgical complications
RENAL EVENING SPECIALTY CONFERENCE
 RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
Laparoscopic nephrectomy Pfannenstiel or expanded port site specimen extraction: a systematic review and meta-analysis
 322 Central European Journal of Urology O R I G I N A L P A P E R UROLOGICAL ONCOLOGY Laparoscopic nephrectomy Pfannenstiel or expanded port site specimen extraction: a systematic review and meta-analysis
322 Central European Journal of Urology O R I G I N A L P A P E R UROLOGICAL ONCOLOGY Laparoscopic nephrectomy Pfannenstiel or expanded port site specimen extraction: a systematic review and meta-analysis
PAPER. Increased Transplantation of Kidneys With Multiple Renal Arteries in the Laparoscopic Live Donor Nephrectomy Era
 PAPER Increased Transplantation of Kidneys With in the Laparoscopic Live Donor Nephrectomy Era Surgical Technique and Surgical and Nonsurgical Donor and Recipient Outcomes Christoph Troppmann, MD; Kevin
PAPER Increased Transplantation of Kidneys With in the Laparoscopic Live Donor Nephrectomy Era Surgical Technique and Surgical and Nonsurgical Donor and Recipient Outcomes Christoph Troppmann, MD; Kevin
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Expanded Criteria Recipients: Are there any Limits
 Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of robot-assisted kidney transplant A kidney transplant is an effective treatment
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of robot-assisted kidney transplant A kidney transplant is an effective treatment
In the past radical nephrectomy necessitated a large
 A Prospective Study of Laparoscopic Radical Nephrectomy for T1 Tumors Is Transperitoneal, Retroperitoneal or Hand Assisted the Best Approach? Robert B. Nadler,* Stacy Loeb, J. Quentin Clemens, Robert A.
A Prospective Study of Laparoscopic Radical Nephrectomy for T1 Tumors Is Transperitoneal, Retroperitoneal or Hand Assisted the Best Approach? Robert B. Nadler,* Stacy Loeb, J. Quentin Clemens, Robert A.
Retroperitoneoscopic donor nephrectomy with a gel-sealed hand-assist access device
 rai et al. BMC Urology 2013, 13:7 http://www.biomedcentral.com/1471-2490/13/7 RESERCH RTICLE Open ccess Retroperitoneoscopic donor nephrectomy with a gel-sealed hand-assist access device Kei rai, Tsutomu
rai et al. BMC Urology 2013, 13:7 http://www.biomedcentral.com/1471-2490/13/7 RESERCH RTICLE Open ccess Retroperitoneoscopic donor nephrectomy with a gel-sealed hand-assist access device Kei rai, Tsutomu
Live Kidney Donation A plea for the laparoscopic approach
 Live Kidney Donation A plea for the laparoscopic approach Live Kidney Donation A plea for the laparoscopic approach Nierdonatie bij leven Een pleidooi voor de laparoscopische benadering Proefschrift ter
Live Kidney Donation A plea for the laparoscopic approach Live Kidney Donation A plea for the laparoscopic approach Nierdonatie bij leven Een pleidooi voor de laparoscopische benadering Proefschrift ter
Laparoendoscopic Pfannenstiel Nephrectomy using Conventional Laparoscopic Instruments - Preliminary Experience
 Surgical Technique Laparoendoscopic Pfannenstiel Nephrectomy International Braz J Urol Vol. 36 (6): 718-723, November - December, 2010 doi: 10.1590/S1677-55382010000600010 Laparoendoscopic Pfannenstiel
Surgical Technique Laparoendoscopic Pfannenstiel Nephrectomy International Braz J Urol Vol. 36 (6): 718-723, November - December, 2010 doi: 10.1590/S1677-55382010000600010 Laparoendoscopic Pfannenstiel
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of robot-assisted kidney transplant A kidney transplant is an effective treatment
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of robot-assisted kidney transplant A kidney transplant is an effective treatment
Donation from Old Living Donors How safe is it? Safe for recipient or donor?
 Donation from Old Living Donors How safe is it? Safe for recipient or donor? Pr Lionel Rostaing Service de Néphrologie, Hémodialyse, Aphérèses et Transplantation CHU Grenoble Alpes France lrostaing@chu-grenoble.fr
Donation from Old Living Donors How safe is it? Safe for recipient or donor? Pr Lionel Rostaing Service de Néphrologie, Hémodialyse, Aphérèses et Transplantation CHU Grenoble Alpes France lrostaing@chu-grenoble.fr
ORIGINAL ARTICLES Endourology
 Urology Journal UNRC/IUA Vol. 1, No. 3, 165-169 Summer 2004 Printed in IRAN ORIGINAL ARTICLES Endourology A Comparison between Laparoscopic and Open Pyeloplasty in Patients with Ureteropelvic Junction
Urology Journal UNRC/IUA Vol. 1, No. 3, 165-169 Summer 2004 Printed in IRAN ORIGINAL ARTICLES Endourology A Comparison between Laparoscopic and Open Pyeloplasty in Patients with Ureteropelvic Junction
Is a 22 cm Ureteric Stent Appropriate for Korean Patients Smaller than 175 cm in Height?
 www.kjurology.org DOI:10.4111/kju.2010.51.9.642 Endourology Is a 22 cm Ureteric Stent Appropriate for Korean Patients Smaller than 175 cm in Height? Byung Ki Lee, Sung Hyun Paick, Hyoung Keun Park, Hyeong
www.kjurology.org DOI:10.4111/kju.2010.51.9.642 Endourology Is a 22 cm Ureteric Stent Appropriate for Korean Patients Smaller than 175 cm in Height? Byung Ki Lee, Sung Hyun Paick, Hyoung Keun Park, Hyeong
Association between R.E.N.A.L. nephrometry score and perioperative outcomes following open partial nephrectomy under cold ischemia
 original research Association between R.E.N.A.L. nephrometry score and perioperative outcomes following open partial nephrectomy under cold ischemia Dong Soo Park, MD; * Jin Ho Hwang, MD; * Moon Hyung
original research Association between R.E.N.A.L. nephrometry score and perioperative outcomes following open partial nephrectomy under cold ischemia Dong Soo Park, MD; * Jin Ho Hwang, MD; * Moon Hyung
Renal Artery Embolization for the Treatment of Renal Artery Pseudoaneurysm Following Partial Nephrectomy
 The Ochsner Journal 13:259 263, 2013 Ó Academic Division of Ochsner Clinic Foundation Renal Artery Embolization for the Treatment of Renal Artery Pseudoaneurysm Following Partial Nephrectomy Cara Irwine,
The Ochsner Journal 13:259 263, 2013 Ó Academic Division of Ochsner Clinic Foundation Renal Artery Embolization for the Treatment of Renal Artery Pseudoaneurysm Following Partial Nephrectomy Cara Irwine,
Renal Transplant Surgery
 Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Facing Surgery. for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option
 Facing Surgery for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option The Condition: Urinary Tract Obstruction The urinary system is the group of organs that produces,
Facing Surgery for Urinary Tract Conditions? Learn why da Vinci Surgery may be your best treatment option The Condition: Urinary Tract Obstruction The urinary system is the group of organs that produces,
Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report
 CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
En bloc transplantation of horseshoe kidney in Korea
 CASE REPORT pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.92.3.168 Annals of Surgical Treatment and Research En bloc transplantation of horseshoe kidney in Korea Jun Bae Bang, Jae Myeong
CASE REPORT pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.92.3.168 Annals of Surgical Treatment and Research En bloc transplantation of horseshoe kidney in Korea Jun Bae Bang, Jae Myeong
Assessment of Erectile and Ejaculatory Function after Penile Prosthesis Implantation
 www.kjurology.org DOI:.4/kju.2.5.3.22 Sexual Dysfunction/Infertility Assessment of Erectile and Ejaculatory Function after Penile Prosthesis Implantation Jang Ho Bae, Phil Hyun Song, Hyun Tae Kim, Ki Hak
www.kjurology.org DOI:.4/kju.2.5.3.22 Sexual Dysfunction/Infertility Assessment of Erectile and Ejaculatory Function after Penile Prosthesis Implantation Jang Ho Bae, Phil Hyun Song, Hyun Tae Kim, Ki Hak
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use
 Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Fluid Balance in an Enhanced Recovery Pathway. Edwin Itenberg, DO, FACS, FASCRS St. Joseph Mercy Oakland MSQC/ASPIRE Meeting April 28, 2017
 Fluid Balance in an Enhanced Recovery Pathway Edwin Itenberg, DO, FACS, FASCRS St. Joseph Mercy Oakland MSQC/ASPIRE Meeting April 28, 2017 No Disclosures 2 Introduction The optimal intravenous fluid regimen
Fluid Balance in an Enhanced Recovery Pathway Edwin Itenberg, DO, FACS, FASCRS St. Joseph Mercy Oakland MSQC/ASPIRE Meeting April 28, 2017 No Disclosures 2 Introduction The optimal intravenous fluid regimen
Use of preoperative embolization prior to Transplant nephrectomy
 ORIGINAL ARTICLE Vol. 42 (1): 107-112, January - February, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0052 Use of preoperative embolization prior to Transplant nephrectomy Carrie Yeast 1, Julie M. Riley 2,
ORIGINAL ARTICLE Vol. 42 (1): 107-112, January - February, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0052 Use of preoperative embolization prior to Transplant nephrectomy Carrie Yeast 1, Julie M. Riley 2,
Laparoscopic Orchiopexy for a Nonpalpable Testis
 www.kjurology.org DOI:1.4111/kju.21.51.2.16 Laparoscopy/Robotics Laparoscopic Orchiopexy for a Nonpalpable Testis Jongwon Kim, Gyeong Eun Min 1, Kun Suk Kim Department of Urology, University of Ulsan College
www.kjurology.org DOI:1.4111/kju.21.51.2.16 Laparoscopy/Robotics Laparoscopic Orchiopexy for a Nonpalpable Testis Jongwon Kim, Gyeong Eun Min 1, Kun Suk Kim Department of Urology, University of Ulsan College
Retroperitoneal LESS Donor Nephrectomy
 Surgical Technique Retroperitoneal LESS Donor Nephrectomy International Braz J Urol Vol. 36 (5): 602-608, September - October, 2010 doi: 10.1590/S1677-55382010000500010 Retroperitoneal LESS Donor Nephrectomy
Surgical Technique Retroperitoneal LESS Donor Nephrectomy International Braz J Urol Vol. 36 (5): 602-608, September - October, 2010 doi: 10.1590/S1677-55382010000500010 Retroperitoneal LESS Donor Nephrectomy
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation
 IJMS Vol 34, No 2, June 2009 Original Article Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation Reza Hekmat, Hamid Eshraghi Abstract Background:
IJMS Vol 34, No 2, June 2009 Original Article Comparison of Serum Cystatin C and Creatinine Levels to Evaluate Early Renal Function after Kidney Transplantation Reza Hekmat, Hamid Eshraghi Abstract Background:
Research Article Assessment of Potential Live Kidney Donors and Computed Tomographic Renal Angiograms at Christchurch Hospital
 Advances in Urology Volume 2016, Article ID 4924320, 4 pages http://dx.doi.org/10.1155/2016/4924320 Research Article Assessment of Potential Live Kidney Donors and Computed Tomographic Renal Angiograms
Advances in Urology Volume 2016, Article ID 4924320, 4 pages http://dx.doi.org/10.1155/2016/4924320 Research Article Assessment of Potential Live Kidney Donors and Computed Tomographic Renal Angiograms
Renal transplantation is the preferred treatment method of endstage
 Technical Aspects of Renal Transplantation John M. Barry Renal transplantation is the preferred treatment method of endstage renal disease (ESRD). It is more cost-effective than is maintenance dialysis
Technical Aspects of Renal Transplantation John M. Barry Renal transplantation is the preferred treatment method of endstage renal disease (ESRD). It is more cost-effective than is maintenance dialysis
Satisfaction with facial laceration repair by provider specialty in the emergency department
 Clin Exp Emerg Med 15;2(3):179-183 http://dx.doi.org/.15441/ceem.15.5 Satisfaction with facial laceration repair by provider specialty in the emergency department eissn: 2383-4625 Original Article Sang-Jae
Clin Exp Emerg Med 15;2(3):179-183 http://dx.doi.org/.15441/ceem.15.5 Satisfaction with facial laceration repair by provider specialty in the emergency department eissn: 2383-4625 Original Article Sang-Jae
Kidney Allograft Stone after Kidney Transplantation and its Association with Graft Survival
 Original Article Kidney Allograft Stone after Kidney Transplantation and its Association with Graft Survival M. S. Rezaee-Zavareh 1,2, R. Ajudani 1, M. Ramezani Binabaj 1, F. Heydari 2, B. Einollahi 2
Original Article Kidney Allograft Stone after Kidney Transplantation and its Association with Graft Survival M. S. Rezaee-Zavareh 1,2, R. Ajudani 1, M. Ramezani Binabaj 1, F. Heydari 2, B. Einollahi 2
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal Approach During the Learning Curve
 JOURNAL OF ENDOUROLOGY Volume 23, Number 6, June 2009 ª Mary Ann Liebert, Inc. Pp. 953 957 DOI: 10.1089=end.2008.0055 Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal
JOURNAL OF ENDOUROLOGY Volume 23, Number 6, June 2009 ª Mary Ann Liebert, Inc. Pp. 953 957 DOI: 10.1089=end.2008.0055 Laparoscopic Ureterolithotomy: A Comparison Between the Transperitoneal and the Retroperitoneal
Obesity is perhaps the most significant public health problem
 Obesity and Its Effect on Survival in Patients Undergoing Orthotopic Liver Transplantation in the United States Satheesh Nair, 1 Sumita Verma, 2 and Paul J. Thuluvath 2 Studies assessing morbidity and
Obesity and Its Effect on Survival in Patients Undergoing Orthotopic Liver Transplantation in the United States Satheesh Nair, 1 Sumita Verma, 2 and Paul J. Thuluvath 2 Studies assessing morbidity and
