Development of a Computed Tomography-Based Scoring System for Necrotizing Soft-Tissue Infections
|
|
|
- Neil Byrd
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Development of a Computed Tomography-Based Scoring System for Necrotizing Soft-Tissue Infections Edward A. McGillicuddy, MD, Andrew W. Lischuk, MD, Kevin M. Schuster, MD, Lewis J. Kaplan, MD, Adrian Maung, MD, Felix Y. Lui, MD, S. A. Jamal Bokhari, MD, and Kimberly A. Davis, MD Background: Necrotizing soft-tissue infections (NSTIs) are associated with significant morbidity and mortality, but a definitive nonsurgical diagnostic test remains elusive. Despite the widespread use of computed tomography (CT) as a diagnostic adjunct, there is little data that definitively correlate CT findings with the presence of NSTI. Our goal was the development of a CT-based scoring system to discriminate non-nsti from NSTI. Methods: Patients older than 17 years undergoing CT for evaluation of soft-tissue infection at a tertiary care medical center over a 10-year period ( ) were included. Abstracted data included comorbidities and social history, physical examination, laboratory findings, and operative and pathologic findings. NSTI was defined as soft-tissue necrosis in the dictated operative note or the accompanying pathology report. CT scans were reviewed by a radiologist blinded to clinical and laboratory data. A scoring system was developed and the area under the receiver operating characteristic curve was calculated. Results: During the study period, 305 patients underwent CT scanning (57% men; mean age, 47.4 years). Forty-four patients (14.4%) evaluated had an NSTI. A scoring system was retrospectively developed (table). A score 6 points was 86.3% sensitive and 91.5% specific for the diagnosis of NSTI (positive predictive value, 63.3%; negative predictive value, 85.5%). The area under the receiver operating characteristic curve was (95% confidence interval, ). The mean score of the non-nsti group was Conclusions: We have developed a CT scoring system that is both sensitive and specific for the diagnosis of NSTIs. This system may allow clinicians to more accurately diagnose NSTIs. Prospective validation of this scoring system is planned. Key Words: Necrotizing soft-tissue infection, Necrotizing fasciitis, Computed tomography, Debridement of soft-tissue infections. (J Trauma. 2011;70: ) Necrotizing soft-tissue infections (NSTI) represent a spectrum of surgical emergencies associated with significant morbidity and mortality. NSTI is a broad term that encompasses anatomic diagnoses, depth of tissue involvement, and Submitted for publication October 7, Accepted for publication January 31, Copyright 2011 by Lippincott Williams & Wilkins From the Departments of Surgery (E.A.M., K.M.S., L.J.K., A.M., F.Y.L., K.A.D.) and Radiology (A.W.L., S.A.J.B.), Yale University School of Medicine, New Haven, Connecticut. Presented as a poster at the 69th Annual Meeting of the American Association for the Surgery of Trauma, September 22 25, 2010, Boston, Massachusetts. Address for reprints: Edward A. McGillicuddy, MD, Department of Surgery, Yale School of Medicine, P.O. Box , New Haven, CT ; edward.mcgillicuddy@yale.edu. DOI: /TA.0b013e a76 microbial pathogens. 1 Although NSTI is a relatively infrequent diagnosis, a high index of suspicion is required as morbidity and mortality are directly proportional to time to intervention. 2,3 The recommendation of early debridement for NSTI has been entrenched in the medical literature since World War I. 4,5 Because securing the diagnose of NSTI may be difficult based on physical examination alone, 6 laboratory and radiographic studies are often used to facilitate early intervention. Although laboratory analysis is helpful, 7,8 computed tomography (CT) is a useful diagnostic tool for patients in whom the diagnosis and the need for operative management is not clear. NSTI has classically been associated with the presence of air in the soft tissue on plain radiography or CT. 9 However, the presence of soft-tissue gas may be limited to infections with anaerobic organisms or late stages of disease presentation. 10 With recent advancements in the quality and versatility of cross-sectional imaging and reformatting of those images, it is likely that radiographic criteria can be identified in a reproducible fashion to assist clinicians in diagnosing NSTI. 11 The prototypical patient with NSTI is no longer a soldier with a puncture wound, but often an immunocompromised individual with a polymicrobial infection. As such, guidelines for diagnosis and treatment of NSTI must be re-examined in the context of new technology, more widespread intravenous (IV) drug abuse, and the increase in the immunosuppressed populations (diabetics, patient receiving chemotherapy, transplant recipients, etc.). Our hypothesis is that a CT-based scoring system could be developed to assist clinicians in establishing the diagnosis of NSTI. PATIENTS AND METHODS Patient Selection After obtaining approval from the Yale University Human Investigations Committee, the Yale New Haven Hospital patient registry was queried. Through International Classification of Diseases 9th Revision (ICD-9) codes, we identified patients admitted to the hospital between January 1, 2000, and December 21, 2009, with the diagnoses of necrotizing fasciitis (ICD-9 code ), or cellulitis, and abscess (ICD-9 code ). We narrowed our search to include only patients older than 17 years undergoing CT to aid in the diagnosis of NSTI. Basic demographics (gender, age), comorbidities (obesity, diabetes, peripheral vascular 894 The Journal of TRAUMA Injury, Infection, and Critical Care Volume 70, Number 4, April 2011
2 The Journal of TRAUMA Injury, Infection, and Critical Care Volume 70, Number 4, April 2011 CT Scoring System for NSTI disease, human immunodeficiency virus [HIV]), history (organ transplant, trauma at the affected site, history of chemotherapy or radiation therapy), and social history (ethanol or IV drug use) were abstracted. Physical examination findings (temperature, heart rate, and systolic blood pressure on presentation; and presence of tissue erythema, tenderness, crepitance, necrosis, and bullae) and laboratory findings (white blood cell count, hemoglobin, serum sodium, bicarbonate, creatinine, lactic acid, and glucose) were also abstracted. Timing and details of surgical debridement (number of debridements, use of vacuum assisted closure devices, and split-thickness skin grafts) and antibiotic therapy, as well as wound microbiology, were noted. NSTI was defined as softtissue necrosis in the dictated operative note or the final surgical pathology report. Outcomes, including length of stay, in-hospital mortality, and discharge status (home, extended care facility, or against medical advice) were recorded for all patients. Computed Tomography Images were obtained over a 10-year period (January 2000 December 2009), which included upgrades from a 4- to 16-slice scanner (January 2004) and 16- to 64-slice scanner (October 2007). Images were reviewed by a single radiologist blinded to all patient data. The CT scan date, prescription, and use of IV contrast material (contrast was nonionic, isosmolar, and administered in standard volumes) were recorded. If a CT scan was performed without IV contrast, the rationale (allergy, acute or chronic renal insufficiency, or prior contrast administration within 24 hours) was recorded. The radiologist reviewed the depth of inflammation on CT and the following variables, which were treated dichotomously: vessel thrombosis, fluid tracking, perifascial air, skin thickening, lymphadenopathy, abscess, muscle edema, and fat stranding. Statistical Analysis All information was entered and maintained in an Excel (Microsoft Office 2007, Microsoft Corp, Redmond, WA) spreadsheet. SPSS version 16 (SPSS, Chicago, IL) was used for statistical analysis. Univariate analysis was performed with 2 and the Student s t test, or logistic regression analysis was performed whenever appropriate. Normally distributed data are reported as mean values (with SD), and nonnormally distributed data are reported as the median value. A p value 0.05 was considered statistically significant. Based on the disparate incidence of CT scan findings in the NSTI and non-nsti groups, a scoring system was developed and the area under the receiver operating characteristic (ROC) curve was optimized. RESULTS A total of 715 patients were identified by ICD-9 codes. CT scans were performed on 305 patients to aid in the diagnosis of NSTI (in the group that did not undergo CT [n 410]: 22 patients underwent immediate surgical debridement for NSTI; 141 patients underwent surgical therapy for a non-nsti; and 247 patients were treated with antibiotics alone). Based on the criteria identified above, 44 of the 305 patients undergoing CT were assigned to the NSTI group and 261 of the 305 patients were assigned to the non-nsti group (Fig. 1). The median length of stay for the Figure 1. Study design including radiographic variables reviewed Lippincott Williams & Wilkins 895
3 McGillicuddy et al. The Journal of TRAUMA Injury, Infection, and Critical Care Volume 70, Number 4, April 2011 non-nsti and NSTI groups was 6 days and 23 days, respectively (p 0.001). There was no statistically significant difference between the NSTI and non-nsti groups in terms of gender (NSTI, 50% men; non-nsti, 58% men), mean age (NSTI, ; non-nsti, ), incidence of obesity (body mass index 30 kg/m 2 ; 29.5% NSTI, 21.2% non- NSTI), or hemodynamic instability at presentation (systolic blood pressure 90 mm Hg, or heart rate 110 beats/min; 20.4% NSTI, 14.9% non-nsti). The incidence of immunosuppression (diabetes, HIV, chemotherapy or radiation therapy, organ transplant, or a history of prior trauma at the site of infection) was higher in the NSTI group than the non-nsti group (Fig. 2). On physical examination, necrosis (45.4% NSTI, 4.9% non-nsti, p 0.001) and bullae (27.2% NSTI, 3.8% non-nsti, p 0.001) were noted more frequently in the NSTI group, whereas there was no difference in the presence of crepitance, erythema, and tenderness. NSTI was associated with pronounced leukocytosis, anemia, hyponatremia, metabolic acidosis, and acute kidney injury (Table 1). In the NSTI group, parenteral antibiotics were initiated in all 44 patients within 12 hours of arrival at the emergency Figure 2. Presenting comorbidities and social habits in the NSTI and non-nsti groups. An asterisk denotes a p value XRT, radiation therapy; TXP, solid organ transplant; IVDA, intravenous drug abuse; EtOH, alcohol abuse. department (mean 4.2 hours 1.2 hours from emergency department registration to antibiotic administration). These 44 patients underwent a mean of 3.1 ( 1.8) debridements under general anesthesia; with a mean time of 15.1hours ( 7.5 hours; range, 2 72 hours) from initial log in to the emergency department until debridement (5 patients were debrided 24 hours from initial presentation). The anatomic distribution and final microbiological cultures and sensitivities varied (Fig. 3). Eleven of the 44 patients (25%) had a polymicrobial infection. Negative pressure wound therapy and split-thickness skin grafts were used for wound coverage in 11 (25%) and 9 (20.4%) patients, respectively. Mortality in the NSTI group was 3 of the 44 (6.8%); 15 of the 44 (34.1%) patients required discharge to a skilled nursing facility secondary to physical deconditioning and wound management requirements. The CT scans of 305 patients (44 in NSTI group and 261 patients in the non-nsti group) were reviewed by a single blinded radiologist (Fig. 1). IV contrast was used in 220 of the 305 studies (72.1%); the most frequent rationale for a noncontrast study was an evidence of acute kidney injury or chronic renal insufficiency. The incidence of muscle or fascial involvement (86.3% NSTI, 13.7% non-nsti; p 0.001), fluid tracking in subcutaneous tissues (38.6% NSTI, 13.0% non-nsti; p 0.001), perifascial gas (43.1% NSTI, 1.9% non-nsti; p 0.001), lymphadenopathy (45.4% NSTI, 26.8% non-nsti; p 0.03), and subcutaneous edema (100% NSTI, 88.5% non-nsti; p 0.04) were higher in the NSTI group. There was no difference in the frequency of abscess formation, fat stranding, or vessel thrombosis (vessel thrombosis was unable to be assessed, however, in 56.7% of studies; Table 2). Given the increased frequency of perifascial air, muscle/fascial edema, fluid tracking, lymphadenopathy, and subcutaneous edema in the NSTI group, a numerical CT scoring system was developed (Table 3) with more points assigned to those findings associated with higher odds ratios. Validation parameters for a score of 6 points included sensitivity (86.3%), specificity (91.5%), negative predictive value (NPV) (85.5%), and positive predictive value (PPV) (63.3%). Validation parameters for fascial air alone yielded a sensitivity of 44.1%, specificity 61.1%, NPV 35.2%, and PPV 58.9%. The mean scores of the NSTI and non-nsti group were 8.57 ( 1.22) and 2.74 ( 0.65), TABLE 1. Laboratory Values, at Presentation, for the NSTI and Non-NSTI Groups NSTI (n 44) Non-NSTI (n 261) p Mean WBC ( 10 3 ; nl range, 4 10) 18.7 ( 4.4) 12.8 ( 3.3) Mean HgB (mg/dl; nl range, 12 16) 11.8 ( 1.6) 12.6 ( 1.5) 0.02 Mean serum sodium (mm/l; nl range, ) ( 4.4) ( 5.1) 0.13 Mean serum creatinine (mg/dl) 1.89 ( 0.44) 1.11 ( 0.22) Mean serum bicarbonate (meq/l; nl range, ) 21.1 ( 4.1) 23.2 ( 3.1) Mean serum glucose (mg/dl) ( 66.2) ( 44.2) Mean serum glucose (non-diabetic patients) (mg/dl) 112 ( 31.4) 108 ( 21.1) 0.67 Mean serum lactate (mmol/l; nl 2.2) 2.8 ( 1.9) (n 21) 2.1 ( 1.0) (n 53) 0.54 WBC, white blood cell; HgB, hemoglobin Lippincott Williams & Wilkins
4 The Journal of TRAUMA Injury, Infection, and Critical Care Volume 70, Number 4, April 2011 CT Scoring System for NSTI Figure 4. ROC curve for the CT-based scoring system. Figure 3. Anatomic distribution of NSTI (A), with final microbiological results (B). H&N, head and neck; GU, genitourinary; MRSA, methicillin-resistant Staphylococcus aureus; MSSA, methicillin-sensitive Staphylococcus aureus; VRE, vancomycin resistant enterococcus sp.; VSE, vancomycin-sensitive enterococcus sp.; Steno, Stenotrophomonas maltophilia. TABLE 2. Groups CT Scan Findings in the NSTI and Non-NSTI NSTI (n 44) Non-NSTI (n 261) p Odds Ratio Fascial air Muscle/fascial edema Fluid tracking Lymphadenopathy Subcutaneous edema Thrombosis Abscess Fat stranding TABLE 3. NSTI Scoring System Variable Points Fascial air 5 Muscle/fascial edema 4 Fluid tracking 3 Lymphadenopathy 2 Subcutaneous edema 1 respectively. In subset analysis, the mean score for patients in the NSTI group who did not have fascial gas present on CT was 7.19 ( 1.1). An ROC curve was generated for our scoring system and the area under the ROC curve was determined (Fig. 4). The area under the ROC curve was (95% confidence interval ). DISCUSSION NSTIs are associated with significant in-hospital morbidity and mortality 12,13 and limitations in functional status after hospital discharge. 14 Given that early diagnosis and treatment are paramount, investigators have often focused on aspects of patient presentation that may be pathognomonic for NSTI. Immune function is an important factor to consider in the diagnosis of NSTI, and it should be noted that immunocompromise applies not only to traditional populations (i.e., patients with HIV or those status after solid organ transplant) but also to patients with decreased barrier function (trauma), poor nutritional status (EtOH misusers), and poor granulocyte function (diabetics). 15 In addition to immune status, there has been a historical link of NSTI to the physical examination findings of crepitance and gray wound drainage; however, these findings are unreliable and laboratory and radiographic findings are routinely completed in at-risk populations. 6,16 Wong et al. proposed the laboratory risk indicator for necrotizing fasciitis (LRINEC). Using total white cell count, hemoglobin, sodium, glucose, serum creatinine, and C-reactive protein, the authors created a scoring system with reasonable PPV and NPV. 8 Although this scoring system is useful in patients for whom clinicians have either high or low suspicion for NSTI, it is likely that radiographic studies will be pursued in the group of patients who are at moderate risk. Cross-sectional imaging has rapidly evolved, and clinicians are no longer required to rely on gas in soft tissues on plain films as the sole radiographic indicator of NSTI. This may be viewed as a positive development, as soft-tissue gas is often a result of long-standing infection with anaerobic organisms. Furthermore, in patients with recent injury or those who underwent previous wound instrumentation, soft-tissue gas may be incidental rather than pathologic. CT is preferable to plain radiography because CT offers high-resolution analysis of compartmental structures. Although magnetic resonance imaging also offers high-resolution images of subcutaneous compartments, CT is timelier, widely available in U.S. centers, and more amenable to rapid interpretation by nonradiologists. 17,18 Although CT imaging of soft-tissue infections has been examined in detail, 10,19,20 currently, there is a dearth of simple scoring systems that would aid in the diagnosis of NSTI. Of 715 patients initially identified in this study, 305 patients underwent CT scans to aid in the diagnosis of NSTI. It is likely that these 305 patients represent the middle of the soft-tissue infection spectrum; patients at the end of the spectrum (i.e., patients with soft-tissue infections obviously 2011 Lippincott Williams & Wilkins 897
5 McGillicuddy et al. The Journal of TRAUMA Injury, Infection, and Critical Care Volume 70, Number 4, April 2011 requiring debridement or non-toxic appearing patients with relatively benign soft-tissue infections) generally do not routinely undergo cross-sectional imaging. Not surprisingly, the 44 patients who met the criteria for NSTI were more likely to be immunocompromised compared with the non-nsti cohort. Diabetes seemed to be a prominent risk factor for NSTI. The average serum glucose was 100 mg/dl higher in the NSTI group than the non-nsti group. The average time elapsed from emergency department registration to operative debridement was 15 hours, a delay that is concerning and may reflect waiting room time and/or delay in obtaining surgical consultation. Because our institution has an attending radiologist, responsible for interpreting emergency department studies, available in-house 24 hours per day, we do not think that there is a significant time lag in obtaining and interpreting CTs in patients with soft-tissue infections. Furthermore, as soft-tissue infections are predominantly managed by in-house trauma and emergency general surgeons, it is unlikely that there was a delay to operative intervention once the diagnosis of NSTI was made. Operative therapy for NSTI consists of surgical debridement with a low threshold for re-exploration. 13,21,22 Although these tenets have not changed recently, vacuumassisted wound closure (11 of 44) and split-thickness skin grafts (9 of the 44) were used with our NSTI population to manage large soft-tissue defects. Although hyperbaric oxygen therapy and IV immunoglobulin for NSTI have been described, 3,23 these were not used for the patients in this study. Of note, the mortality and long-term morbidity of NSTI in these 44 patients is testament to a need for early diagnosis and therapy, and our data correlate favorably with rates reported in the literature. It is likely that patient characteristics and the diagnostic algorithm for soft-tissue infection in this study are similar to most North American tertiary centers. Thus, a CT scoring system that consists of rapidly identifiable variables may be a valuable tool in the clinician s armamentarium. Our CTbased scoring system, relying partially but not exclusively on the presence of soft-tissue gas, is statistically robust for a cutoff score of 6. Although IV contrast is preferred for imaging soft-tissue infections, using this scoring system, it is not necessary. This is of relevance as many patients with comorbidities that predispose to soft-tissue infections have coincident acute or chronic renal injury and IV contrast may be contraindicated. Finally, this imaging-based scoring system may be used in conjunction with existing laboratorybased scoring systems 24,25 to strengthen diagnostic confidence for soft-tissue infections. Despite yielding clinically relevant results, the limitations of this retrospective study must be acknowledged. Despite the adherence to basic surgical and critical care principles with regard to the diagnosis and treatment of NSTI, the care of each patient may have been influenced by local practice patterns as well as individual clinician s preferences. Additionally, diagnostic imaging technology advances rapidly, and the CT scanner used was upgraded twice during the study period. As CT system upgrades affect image quality and resolution, this has the potential to confound our data. 898 Finally, it would have been advantageous to apply the LRINEC to the NSTI and non-nsti groups to determine whether a combined laboratory-radiographic tool could be developed; however, C-reactive protein, a component of LRINEC analysis, was not routinely measured at our intuition during the study period. Finally, a single, blinded radiologist reviewed the CT scans in this study. As these CT variables are somewhat subjective, inter-rater variability should be assessed before prospective validation of this scoring system. Overall, this study has broad implications with regard to caring for patients with a challenging clinical entity. As the number of patients with NSTI risk factor increases, the number of soft-tissue infections seen in U.S. emergency departments will increase. Use of this CT-based scoring system for soft-tissue infections, along with laboratory analysis and a high clinical suspicion, may improve diagnostic accuracy in patients with soft-tissue infections of indeterminate severity. Prospective validation of this scoring system is planned. REFERENCES 1. Sarani B, Strong M, Pascual J, Schwab CW. Necrotizing fasciitis: current concepts and review of the literature. J Am Coll Surg. 2009;208: Martin DA, Nanci GN, Marlowe SI, Larsen AN. Necrotizing fasciitis with no mortality or limb loss. Am Surg. 2008;74: Cuschieri J. Necrotizing soft tissue infection. Surg Infect (Larchmt). 2008;9: Wallace C. Gas gangrene as seen at the casualty clearing stations. BMJ. 1916;2: Ivens F. A clinical study of anaerobic wound infection, with an analysis of 107 cases of gas gangrene. Proc R Soc Med. 1917;10: Chan T, Yaghoubian A, Rosing D, Kaji A, de Virgilio C. Low sensitivity of physical examination findings in necrotizing soft tissue infection is improved with laboratory values: a prospective study. Am J Surg. 2008;196: ; discussion Barie PS. The laboratory risk indicator for necrotizing fasciitis (LRINEC) score: useful tool or paralysis by analysis? Crit Care Med. 2004;32: Wong CH, Khin LW, Heng KS, Tan KC, Low CO. The LRINEC (Laboratory Risk Indicator for Necrotizing Fasciitis) score: a tool for distinguishing necrotizing fasciitis from other soft tissue infections. Crit Care Med. 2004;32: Fisher JR, Conway MJ, Takeshita RT, Sandoval MR. Necrotizing fasciitis. Importance of roentgenographic studies for soft-tissue gas. JAMA. 1979;241: Fugitt JB, Puckett ML, Quigley MM, Kerr SM. Necrotizing fasciitis. Radiographics. 2004;24: Zacharias N, Velmahos GC, Salama A, et al. Diagnosis of necrotizing soft tissue infections by computed tomography. Arch Surg. 2010; 145: May AK, Stafford RE, Bulger EM, et al. Treatment of complicated skin and soft tissue infections. Surg Infect (Larchmt). 2009;10: Tillou A, St Hill CR, Brown C, Velmahos G. Necrotizing soft tissue infections: improved outcomes with modern care. Am Surg. 2004;70: Pham TN, Moore ML, Costa BA, Cuschieri J, Klein MB. Assessment of functional limitation after necrotizing soft tissue infection. J Burn Care Res. 2009;30: Cainzos M, Gonzalez-Rodriguez FJ. Necrotizing soft tissue infections. Curr Opin Crit Care. 2007;13: Wilson B. Necrotizing fasciitis. Am Surg. 1952;18: Fayad LM, Carrino JA, Fishman EK. Musculoskeletal infection: role of CT in the emergency department. Radiographics. 2007;27: Wysoki MG, Santora TA, Shah RM, Friedman AC. Necrotizing fasciitis: CT characteristics. Radiology. 1997;203: Levenson RB, Singh AK, Novelline RA. Fournier gangrene: role of imaging. Radiographics. 2008;28: Lippincott Williams & Wilkins
6 The Journal of TRAUMA Injury, Infection, and Critical Care Volume 70, Number 4, April 2011 CT Scoring System for NSTI 20. Becker M, Zbaren P, Hermans R, et al. Necrotizing fasciitis of the head and neck: role of CT in diagnosis and management. Radiology. 1997; 202: Bilton BD, Zibari GB, McMillan RW, Aultman DF, Dunn G, McDonald JC. Aggressive surgical management of necrotizing fasciitis serves to decrease mortality: a retrospective study. Am Surg. 1998;64: ; discussion Anaya DA, McMahon K, Nathens AB, Sullivan SR, Foy H, Bulger E. Predictors of mortality and limb loss in necrotizing soft tissue infections. Arch Surg. 2005;140: ; discussion Wilkinson D, Doolette D. Hyperbaric oxygen treatment and survival from necrotizing soft tissue infection. Arch Surg. 2004;139: Su YC, Chen HW, Hong YC, Chen CT, Hsiao CT, Chen IC. Laboratory risk indicator for necrotizing fasciitis score and the outcomes. ANZ J Surg. 2008;78: Yaghoubian A, de Virgilio C, Dauphine C, Lewis RJ, Lin M. Use of admission serum lactate and sodium levels to predict mortality in necrotizing soft-tissue infections. Arch Surg. 2007;142: ; discussion Lippincott Williams & Wilkins 899
Demographics, Microbiology and Outcome in Necrotizing Soft Tissue Infections
 Original Article Demographics, Microbiology and Outcome in Necrotizing Soft Tissue Infections Chance Witt, MD, Sharmila Dissanaike, MD Abstract Background: Necrotizing soft tissue infections (NSTI) are
Original Article Demographics, Microbiology and Outcome in Necrotizing Soft Tissue Infections Chance Witt, MD, Sharmila Dissanaike, MD Abstract Background: Necrotizing soft tissue infections (NSTI) are
Yonekura, Akihiko; Tomita, Masato;
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Fournier's gangrene a case report Miyamoto, Takashi; Fukushima, Tatsu Yonekura, Akihiko; Tomita, Masato; Acta medica Nagasakiensia, 61(1), p Issue
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Fournier's gangrene a case report Miyamoto, Takashi; Fukushima, Tatsu Yonekura, Akihiko; Tomita, Masato; Acta medica Nagasakiensia, 61(1), p Issue
PAPER. Use of Admission Serum Lactate and Sodium Levels to Predict Mortality in Necrotizing Soft-Tissue Infections
 PAPER Use of Admission Serum Lactate and Sodium Levels to Predict Mortality in Necrotizing Soft-Tissue Infections Arezou Yaghoubian, MD; Christian de Virgilio, MD; Christine Dauphine, MD; Roger J. Lewis,
PAPER Use of Admission Serum Lactate and Sodium Levels to Predict Mortality in Necrotizing Soft-Tissue Infections Arezou Yaghoubian, MD; Christian de Virgilio, MD; Christine Dauphine, MD; Roger J. Lewis,
Risk factors for mortality in the late amputation of necrotizing fasciitis: a retrospective study
 Chang et al. World Journal of Emergency Surgery (2018) 13:45 https://doi.org/10.1186/s13017-018-0207-0 RESEARCH ARTICLE Open Access Risk factors for mortality in the late amputation of necrotizing fasciitis:
Chang et al. World Journal of Emergency Surgery (2018) 13:45 https://doi.org/10.1186/s13017-018-0207-0 RESEARCH ARTICLE Open Access Risk factors for mortality in the late amputation of necrotizing fasciitis:
Il ruolo del chirurgo nella gestione delle infezioni di cute e tessuti molli
 Il ruolo del chirurgo nella gestione delle infezioni di cute e tessuti molli Massimo Sartelli U.O. Chirurgia Generale Ospedale di Macerata Surgical Site infections Incisional - Superficial - Deep Non-necrotizing
Il ruolo del chirurgo nella gestione delle infezioni di cute e tessuti molli Massimo Sartelli U.O. Chirurgia Generale Ospedale di Macerata Surgical Site infections Incisional - Superficial - Deep Non-necrotizing
Characteristics and differences in necrotizing fasciitis and gas forming myonecrosis: a series of 36 patients
 Scandinavian Journal of Surgery : 5 55, Characteristics and differences in necrotizing fasciitis and gas forming myonecrosis: a series of 36 patients D. J. Tilkorn, M. Citak, T. Fehmer, A. Ring, J. Hauser,
Scandinavian Journal of Surgery : 5 55, Characteristics and differences in necrotizing fasciitis and gas forming myonecrosis: a series of 36 patients D. J. Tilkorn, M. Citak, T. Fehmer, A. Ring, J. Hauser,
Morbidity & Mortality Conference Downstate Medical Center. Daniel Kaufman, MD
 Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia
 Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Interesting Case Series. A Case of Fournier s Gangrene
 Interesting Case Series A Case of Fournier s Gangrene Anthony Maurice Kordahi, MD, and Ahmed S. Suliman, MD Division of Plastic Surgery, University of California San Diego Correspondence: kordahi.amk@gmail.com
Interesting Case Series A Case of Fournier s Gangrene Anthony Maurice Kordahi, MD, and Ahmed S. Suliman, MD Division of Plastic Surgery, University of California San Diego Correspondence: kordahi.amk@gmail.com
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more)
 Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Interesting Case Series. Fournier s Gangrene and the Reconstructive Challenges for the Plastic Surgeon
 Interesting Case Series Fournier s Gangrene and the Reconstructive Challenges for the Plastic Surgeon David Izadi, MB, BChir, MA(Oxon), MA(Cantab), MRCS, James Coelho, BMBS, MSc, MRCS, Sameer Gurjal, MBBCh,
Interesting Case Series Fournier s Gangrene and the Reconstructive Challenges for the Plastic Surgeon David Izadi, MB, BChir, MA(Oxon), MA(Cantab), MRCS, James Coelho, BMBS, MSc, MRCS, Sameer Gurjal, MBBCh,
-> Education -> Excellence
 Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Case Report The Clock Is Ticking : The Timely Management of a Painful Skin Rash in a Seventy-Year-Old Woman
 Case Reports in Medicine, Article ID 641058, 4 pages http://dx.doi.org/10.1155/2014/641058 Case Report The Clock Is Ticking : The Timely Management of a Painful Skin Rash in a Seventy-Year-Old Woman Susan
Case Reports in Medicine, Article ID 641058, 4 pages http://dx.doi.org/10.1155/2014/641058 Case Report The Clock Is Ticking : The Timely Management of a Painful Skin Rash in a Seventy-Year-Old Woman Susan
General surgery department of SGMU Lecturer ass. Khilgiyaev R.H. Anaerobic infection. Gas gangrene
 Anaerobic infection Gas gangrene Anaerobic bacteria Anaerobic bacteria are the most numerous inhabitants of the normal gastrointestinal tract, including the mouth Bacteroides fragilis and Clostridium The
Anaerobic infection Gas gangrene Anaerobic bacteria Anaerobic bacteria are the most numerous inhabitants of the normal gastrointestinal tract, including the mouth Bacteroides fragilis and Clostridium The
Clinical Case. ! 2am: Call from Surgeon, Ballarat Hospital. ! Suspicion of Necrotizing Fasciitis: ! Need of HBOT?
 Clinical Case! 2am: Call from Surgeon, Ballarat Hospital! Suspicion of Necrotizing Fasciitis:! 59y, Police Officer, diabetic, overweight! 4pm: pain in right arm! 8pm: pain worsening " ED! HD instability
Clinical Case! 2am: Call from Surgeon, Ballarat Hospital! Suspicion of Necrotizing Fasciitis:! 59y, Police Officer, diabetic, overweight! 4pm: pain in right arm! 8pm: pain worsening " ED! HD instability
Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis
 Original Article Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis Wen-Shyan Huang, Shang-Chin Hsieh, Chun-Sheng Hsieh, Jen-Yu Schoung and
Original Article Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis Wen-Shyan Huang, Shang-Chin Hsieh, Chun-Sheng Hsieh, Jen-Yu Schoung and
Objectives. Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection
 Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Necrotizing Soft Tissue Infections
 Necrotizing Soft Tissue Infections Dan Holena, MD MSCE Division of Trauma, Emergency Surgery and Surgical Critical Care University of Pennsylvania School of Medicine Philadelphia, PA Goals of this talk
Necrotizing Soft Tissue Infections Dan Holena, MD MSCE Division of Trauma, Emergency Surgery and Surgical Critical Care University of Pennsylvania School of Medicine Philadelphia, PA Goals of this talk
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections
 Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
A WEATHER FORECAST. It is gonna be cold It is gonna be gray It is gonna last for the rest of your life Groundhog day Bill Murray
 A WEATHER FORECAST It is gonna be cold It is gonna be gray It is gonna last for the rest of your life Groundhog day Bill Murray GOETHE Art is long, Life short, Judgment difficult, Opportunity transient
A WEATHER FORECAST It is gonna be cold It is gonna be gray It is gonna last for the rest of your life Groundhog day Bill Murray GOETHE Art is long, Life short, Judgment difficult, Opportunity transient
Necrotizing Fasciitis. Madhuri Rao, MD June 27 th, 2013 Case from Kings County Hospital Center
 Necrotizing Fasciitis Madhuri Rao, MD June 27 th, 2013 Case from Kings County Hospital Center 31 yo F www.downstatesurgery.org Case Presentation PMH: DM (type 1), CRI, verrucous elephantiasis of LE PSH:
Necrotizing Fasciitis Madhuri Rao, MD June 27 th, 2013 Case from Kings County Hospital Center 31 yo F www.downstatesurgery.org Case Presentation PMH: DM (type 1), CRI, verrucous elephantiasis of LE PSH:
Community-Acquired Pneumonia OBSOLETE 2
 Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
Goal: Look for sources that require surgery in patients that present with severe infections.
 High Risk EM Sukhjit Takhar, MD Assistant Clinical Professor of Emergency Medicine Faculty, Division of Infectious Disease UCSF-Fresno stakhar@fresno.ucsf.edu Goal: Look for sources that require surgery
High Risk EM Sukhjit Takhar, MD Assistant Clinical Professor of Emergency Medicine Faculty, Division of Infectious Disease UCSF-Fresno stakhar@fresno.ucsf.edu Goal: Look for sources that require surgery
CASE STUDY ON INPATIENT MALNUTRITION DISCUSSION
 CASE STUDY ON INPATIENT MALNUTRITION Elena Kret-Sudjian MD, PhD, UC Davis Medical Center A 59 year-old white man with a history of diabetes, severe PVD, CKD IV, chronic hepatitis C admitted for non-healing
CASE STUDY ON INPATIENT MALNUTRITION Elena Kret-Sudjian MD, PhD, UC Davis Medical Center A 59 year-old white man with a history of diabetes, severe PVD, CKD IV, chronic hepatitis C admitted for non-healing
Osteomieliti STEOMIE
 OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
Complicated Skin and Soft Tissue Infection diagnosis and severity stratification
 Complicated Skin and Soft Tissue Infection diagnosis and severity stratification Muhammad Hussein Gasem Div Infectious Disease, TropMed, and Immunology Dr. Kariadi Hospital, Diponegoro University Semarang,
Complicated Skin and Soft Tissue Infection diagnosis and severity stratification Muhammad Hussein Gasem Div Infectious Disease, TropMed, and Immunology Dr. Kariadi Hospital, Diponegoro University Semarang,
A Clinicopathological Study of Necrotizing Fasciitis
 AJMS Al Ameen J Med Sci (2 0 1 1 )4 (1 ):6-1 3 (An US National Library of Medicine enlisted journal) I S S N 0 9 7 4-1 1 4 3 ORIGI NAL ARTICLE A Clinicopathological Study of Necrotizing Fasciitis Madhumita
AJMS Al Ameen J Med Sci (2 0 1 1 )4 (1 ):6-1 3 (An US National Library of Medicine enlisted journal) I S S N 0 9 7 4-1 1 4 3 ORIGI NAL ARTICLE A Clinicopathological Study of Necrotizing Fasciitis Madhumita
Repeated Pneumonia Severity Index Measurement After Admission Increases its Predictive Value for Mortality in Severe Community-acquired Pneumonia
 ORIGINAL ARTICLE Repeated Pneumonia Severity Index Measurement After Admission Increases its Predictive Value for Mortality in Severe Community-acquired Pneumonia Chiung-Zuei Chen, 1 Po-Sheng Fan, 2 Chien-Chung
ORIGINAL ARTICLE Repeated Pneumonia Severity Index Measurement After Admission Increases its Predictive Value for Mortality in Severe Community-acquired Pneumonia Chiung-Zuei Chen, 1 Po-Sheng Fan, 2 Chien-Chung
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
Treatment for sternoclavicular joint infections: a multi-institutional study
 Original Article Treatment for sternoclavicular joint infections: a multi-institutional study Allen Murga, Hannah Copeland, Rachel Hargrove, Jason M. Wallen, Salman Zaheer Department of Thoracic and Cardiovascular
Original Article Treatment for sternoclavicular joint infections: a multi-institutional study Allen Murga, Hannah Copeland, Rachel Hargrove, Jason M. Wallen, Salman Zaheer Department of Thoracic and Cardiovascular
INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis
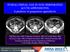 INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis DM Plata Ariza, MD; E Martínez Chamorro, MD; D Castaño Pardo, MD; M Arroyo López, MD; E Peghini Gavilanes,
INTRALUMINAL GAS IN NON-PERFORATED ACUTE APPENDICITIS: A predictor of gangrenous appendicitis DM Plata Ariza, MD; E Martínez Chamorro, MD; D Castaño Pardo, MD; M Arroyo López, MD; E Peghini Gavilanes,
A Validated Practical Risk Score to Predict the Need for RVAD after Continuous-flow LVAD
 A Validated Practical Risk Score to Predict the Need for RVAD after Continuous-flow LVAD SK Singh MD MSc, DK Pujara MBBS, J Anand MD, WE Cohn MD, OH Frazier MD, HR Mallidi MD Division of Transplant & Assist
A Validated Practical Risk Score to Predict the Need for RVAD after Continuous-flow LVAD SK Singh MD MSc, DK Pujara MBBS, J Anand MD, WE Cohn MD, OH Frazier MD, HR Mallidi MD Division of Transplant & Assist
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) doi: To be assigned Early view version published:
: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) doi: To be assigned Early view version published:
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health
 UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Analysis of Urobilinogen and Urine Bilirubin for Intra-Abdominal Injury in Blunt Trauma Patients
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Analysis of Urobilinogen and Urine Bilirubin for Intra-Abdominal Injury in Blunt Trauma Patients
Sofia Fayngold CRC Rotation IRB proposal 9/1/2011
 Sofia Fayngold CRC Rotation IRB proposal 9/1/2011 Sodium Bicarbonate Hydration for the Prevention of Contrast Induced Nephropathy following Computed Tomography Angiography of the Chest for Pulmonary Emoblism
Sofia Fayngold CRC Rotation IRB proposal 9/1/2011 Sodium Bicarbonate Hydration for the Prevention of Contrast Induced Nephropathy following Computed Tomography Angiography of the Chest for Pulmonary Emoblism
ID Emergencies. BUMC-P Internal Medicine Edwin Yu
 ID Emergencies BUMC-P Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
ID Emergencies BUMC-P Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
THE CLINICAL course of severe
 ORIGINAL ARTICLE Improved Prediction of Outcome in Patients With Severe Acute Pancreatitis by the APACHE II Score at 48 Hours After Hospital Admission Compared With the at Admission Arif A. Khan, MD; Dilip
ORIGINAL ARTICLE Improved Prediction of Outcome in Patients With Severe Acute Pancreatitis by the APACHE II Score at 48 Hours After Hospital Admission Compared With the at Admission Arif A. Khan, MD; Dilip
Interesting Case Series. Pyogenic (Suppurative) Flexor Tenosynovitis: Assessment and Management
 Interesting Case Series Pyogenic (Suppurative) Flexor Tenosynovitis: Assessment and Management Renee L. Barry, BS a,nicholass.adams,md a,b, and Matthew D. Martin, MD a,b,c a Michigan State University College
Interesting Case Series Pyogenic (Suppurative) Flexor Tenosynovitis: Assessment and Management Renee L. Barry, BS a,nicholass.adams,md a,b, and Matthew D. Martin, MD a,b,c a Michigan State University College
ID Emergencies. BGSMC Internal Medicine Edwin Yu
 ID Emergencies BGSMC Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
ID Emergencies BGSMC Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
Clinical Evaluation of the Nose: A Cheap and Effective Tool for the Nasal Fracture Diagnosis
 Eplasty. 2012; 12: e3. Published online 2012 January 23. PMCID: PMC3266122 Clinical Evaluation of the Nose: A Cheap and Effective Tool for the Nasal Fracture Diagnosis Joaquín Pérez-Guisado, MD, PhD a
Eplasty. 2012; 12: e3. Published online 2012 January 23. PMCID: PMC3266122 Clinical Evaluation of the Nose: A Cheap and Effective Tool for the Nasal Fracture Diagnosis Joaquín Pérez-Guisado, MD, PhD a
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida
 Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Case History. Introduction
 Although Fournier's gangrene is primarily a disease of adults, It has been rarely described in children. This is a report of our experience with the management of 2 patients aged 14 and36 days. The predisposing
Although Fournier's gangrene is primarily a disease of adults, It has been rarely described in children. This is a report of our experience with the management of 2 patients aged 14 and36 days. The predisposing
Severe and Tertiary Peritonitis
 Severe and Tertiary Peritonitis Addison K. May, MD FACS Professor of Surgery and Anesthesiology Division of Trauma and Surgical Critical Care Vanderbilt University Medical Center PS204: The Bad Infections:
Severe and Tertiary Peritonitis Addison K. May, MD FACS Professor of Surgery and Anesthesiology Division of Trauma and Surgical Critical Care Vanderbilt University Medical Center PS204: The Bad Infections:
Necrotizing Fasciitis. By Lisa Banks
 Necrotizing Fasciitis By Lisa Banks Foot infections are the most common softtissue infections in pts with diabetes Necrotizing fasciitis is the most important soft tissue infection in DM pts involving
Necrotizing Fasciitis By Lisa Banks Foot infections are the most common softtissue infections in pts with diabetes Necrotizing fasciitis is the most important soft tissue infection in DM pts involving
Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center
 CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
Necrotizing fasciitis
 Necrotizing fasciitis Falco Hietbrink Surgeon, MD/PhD Disclosure form No conflict of interest Images with approval for educational purposes Please, no cellphonepictures of slides Soft tissue infections
Necrotizing fasciitis Falco Hietbrink Surgeon, MD/PhD Disclosure form No conflict of interest Images with approval for educational purposes Please, no cellphonepictures of slides Soft tissue infections
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Critical Review Form Clinical Prediction or Decision Rule
 Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
PSOAS ABSCESS. Dr Noman Ullah Wazir
 PSOAS ABSCESS Dr Noman Ullah Wazir Psoas Major muscle The psoas major is a long fusiform muscle located on the side of the lumbar region of the vertebral column and brim of the lesser pelvis. Psoas Major
PSOAS ABSCESS Dr Noman Ullah Wazir Psoas Major muscle The psoas major is a long fusiform muscle located on the side of the lumbar region of the vertebral column and brim of the lesser pelvis. Psoas Major
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 2.417, ISSN: , Volume 3, Issue 10, November 2015
 STAPHYLOCOCCUS AUREUS NECROTIZING FASCIITIS AND ITS OUTCOME IN IMMUNOCOMPETENT SUBJECTS BESMIRA ZAMA** TRITAN KALO* STELA MUCA* *Service of Infectious Disease, UHC, MT, FSHMT ** Prime Clinic Health No.10,
STAPHYLOCOCCUS AUREUS NECROTIZING FASCIITIS AND ITS OUTCOME IN IMMUNOCOMPETENT SUBJECTS BESMIRA ZAMA** TRITAN KALO* STELA MUCA* *Service of Infectious Disease, UHC, MT, FSHMT ** Prime Clinic Health No.10,
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING
 IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING Christopher Hunter, MD, PhD, FACEP Director, Health Services Department Associate Medical Director, Orange County EMS System Medical Director, Orlando Health
IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING Christopher Hunter, MD, PhD, FACEP Director, Health Services Department Associate Medical Director, Orange County EMS System Medical Director, Orlando Health
Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer
 HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
S (17) https://doi.org/ /j.urology Reference: URL 20732
 Accepted Manuscript Title: Presentation and Diagnosis of Fournier's Gangrene Author: Bryan B. Voelzke, Judith C. Hagedorn PII: S0090-4295(17)31174-3 DOI: https://doi.org/10.1016/j.urology.2017.10.031 Reference:
Accepted Manuscript Title: Presentation and Diagnosis of Fournier's Gangrene Author: Bryan B. Voelzke, Judith C. Hagedorn PII: S0090-4295(17)31174-3 DOI: https://doi.org/10.1016/j.urology.2017.10.031 Reference:
Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection?
 ANNALS OF SURGERY Vol. 237, No. 3, 358 362 2003 Lippincott Williams & Wilkins, Inc. Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection? Chesley Richards,
ANNALS OF SURGERY Vol. 237, No. 3, 358 362 2003 Lippincott Williams & Wilkins, Inc. Does Using a Laparoscopic Approach to Cholecystectomy Decrease the Risk of Surgical Site Infection? Chesley Richards,
UNDERTRIAGE and OVERTRIAGE
 UNDERTRIAGE and OVERTRIAGE Alison Wilson, MD, FACS Professor Skewes Family Chair in Trauma Director, Critical Care and Trauma Institute TRIAGE 18 TH century French: Trier = to separate out Minimal use
UNDERTRIAGE and OVERTRIAGE Alison Wilson, MD, FACS Professor Skewes Family Chair in Trauma Director, Critical Care and Trauma Institute TRIAGE 18 TH century French: Trier = to separate out Minimal use
A Case Report of Acute Renal Artery Occlusion Mimicking Acute Appendicitis
 ISPUB.COM The Internet Journal of Surgery Volume 7 Number 1 A Case Report of Acute Renal Artery Occlusion Mimicking Acute Appendicitis S Abouel-Enin, A Douglas, R Morgan Citation S Abouel-Enin, A Douglas,
ISPUB.COM The Internet Journal of Surgery Volume 7 Number 1 A Case Report of Acute Renal Artery Occlusion Mimicking Acute Appendicitis S Abouel-Enin, A Douglas, R Morgan Citation S Abouel-Enin, A Douglas,
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/22997 holds various files of this Leiden University dissertation Author: Wilden, Gwendolyn M. van der Title: The value of surgical treatment in abdominal
Cover Page The handle http://hdl.handle.net/1887/22997 holds various files of this Leiden University dissertation Author: Wilden, Gwendolyn M. van der Title: The value of surgical treatment in abdominal
TOTAL HIP AND KNEE REPLACEMENTS. FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES
 TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute appendicitis is the most common surgical emergency in
 FEATURE Is It Safe to Delay Appendectomy in Adults With Acute Appendicitis? Michael F. Ditillo, DO,* James D. Dziura, PhD, and Reuven Rabinovici, MD* Objective: To examine whether delayed surgical intervention
FEATURE Is It Safe to Delay Appendectomy in Adults With Acute Appendicitis? Michael F. Ditillo, DO,* James D. Dziura, PhD, and Reuven Rabinovici, MD* Objective: To examine whether delayed surgical intervention
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
PSEUDO-CELLULITIS - ALL THAT S RED IS NOT INFECTION
 JAN 18 2018 ASP ECHO CLINIC CHARLES KRASNER, M.D. PSEUDO-CELLULITIS - ALL THAT S RED IS NOT INFECTION FIRST HOSPITALIZATION: 62 YEAR OLD MALE ADMITTED WITH DIAGNOSIS OF CELLULITIS Hx of AODM, Morbid Obesity,
JAN 18 2018 ASP ECHO CLINIC CHARLES KRASNER, M.D. PSEUDO-CELLULITIS - ALL THAT S RED IS NOT INFECTION FIRST HOSPITALIZATION: 62 YEAR OLD MALE ADMITTED WITH DIAGNOSIS OF CELLULITIS Hx of AODM, Morbid Obesity,
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Is Pediatric Appendicitis Score Sufficient to Make the Diagnosis of Acute Appendicitis Among Children?
 Iraqi JMS Published by AlNahrain College of Medicine ISSN 686579 Email: iraqijms@colmedalnahrain.edu.iq http://www.colmednahrain.edu.iq Is Pediatric Appendicitis Score Sufficient to Make the Diagnosis
Iraqi JMS Published by AlNahrain College of Medicine ISSN 686579 Email: iraqijms@colmedalnahrain.edu.iq http://www.colmednahrain.edu.iq Is Pediatric Appendicitis Score Sufficient to Make the Diagnosis
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Cellulitis: a practical guide
 Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
Sepsis 3.0: The Impact on Quality Improvement Programs
 Sepsis 3.0: The Impact on Quality Improvement Programs Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care Warren Alpert Medical School of Brown University
Sepsis 3.0: The Impact on Quality Improvement Programs Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care Warren Alpert Medical School of Brown University
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Information for Patients
 Having a CT Intravenous Urogram (CT IVU) Information for Patients In this leaflet: Introduction 2 What is a CT IVU?...2 How does it work?. 2 Are there any risks?.3 What do I need to do to prepare for my
Having a CT Intravenous Urogram (CT IVU) Information for Patients In this leaflet: Introduction 2 What is a CT IVU?...2 How does it work?. 2 Are there any risks?.3 What do I need to do to prepare for my
Presented at 2015 TQIP conference. Developed by a panel of experts. Evidence based with expert opinion as needed
 Presented at 2015 TQIP conference Developed by a panel of experts Evidence based with expert opinion as needed Orthopaedic Trauma Best Practice Guidelines (BPG) Goals Offer guidance on what is practical
Presented at 2015 TQIP conference Developed by a panel of experts Evidence based with expert opinion as needed Orthopaedic Trauma Best Practice Guidelines (BPG) Goals Offer guidance on what is practical
Foot infections in persons with diabetes are
 DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis?
 Pediatrics Prevention P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis? RESEARCHED BY: Muhammad Amin Chinoy MD, Pakistan Literature:
Pediatrics Prevention P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis? RESEARCHED BY: Muhammad Amin Chinoy MD, Pakistan Literature:
Necrotizing fasciitis - early sonographic diagnosis.
 Necrotizing fasciitis - early sonographic diagnosis. Marek Wronski, Maciej Slodkowski, Wlodzimierz Cebulski, Dominika Karkocha, Ireneusz Wojciech Krasnodebski To cite this version: Marek Wronski, Maciej
Necrotizing fasciitis - early sonographic diagnosis. Marek Wronski, Maciej Slodkowski, Wlodzimierz Cebulski, Dominika Karkocha, Ireneusz Wojciech Krasnodebski To cite this version: Marek Wronski, Maciej
December 3, 2015 Severe Sepsis and Septic Shock Antibiotic Guide
 Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Crush Injury. Professeur D. MATHIEU. Medicine
 Crush Injury Professeur D. MATHIEU Department of Critical Care and Hyperbaric Medicine University Hospital of Lille - France Definitions Crush Injury An injury sustained when a body part is subjected to
Crush Injury Professeur D. MATHIEU Department of Critical Care and Hyperbaric Medicine University Hospital of Lille - France Definitions Crush Injury An injury sustained when a body part is subjected to
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
DTI vs All Things Purple 3 End of life case studies
 Mary M Applegate, BSN RN CWOCN End of life patients are at risk of being misdiagnosed as having a Pressure injury (specifically DTI). This project presents three (3)case studies of patients that the WOC
Mary M Applegate, BSN RN CWOCN End of life patients are at risk of being misdiagnosed as having a Pressure injury (specifically DTI). This project presents three (3)case studies of patients that the WOC
Podcast (Video Recorded Lecture Series): Soft Tissue Infections for the USMLE Step One Exam
 Podcast (Video Recorded Lecture Series): Soft Tissue Infections for the USMLE Step One Exam Howard J. Sachs, MD www.12daysinmarch.com Email: Howard@12daysinmarch.com MSK Infections Bone and Joint Infections
Podcast (Video Recorded Lecture Series): Soft Tissue Infections for the USMLE Step One Exam Howard J. Sachs, MD www.12daysinmarch.com Email: Howard@12daysinmarch.com MSK Infections Bone and Joint Infections
Review of 58 patients with necrotizing fasciitis in the Netherlands
 van Stigt et al. World Journal of Emergency Surgery (2016) 11:21 DOI 10.1186/s13017-016-0080-7 RESEARCH ARTICLE Open Access Review of 58 patients with necrotizing fasciitis in the Netherlands Sander F.
van Stigt et al. World Journal of Emergency Surgery (2016) 11:21 DOI 10.1186/s13017-016-0080-7 RESEARCH ARTICLE Open Access Review of 58 patients with necrotizing fasciitis in the Netherlands Sander F.
Untreated idiopathic pulmonary arterial hypertension
 Congenital Heart Disease Outcomes in Children With Idiopathic Pulmonary Arterial Hypertension Delphine Yung, MD; Allison C. Widlitz, MS, PA; Erika Berman Rosenzweig, MD; Diane Kerstein, MD; Greg Maislin,
Congenital Heart Disease Outcomes in Children With Idiopathic Pulmonary Arterial Hypertension Delphine Yung, MD; Allison C. Widlitz, MS, PA; Erika Berman Rosenzweig, MD; Diane Kerstein, MD; Greg Maislin,
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Case Report Neglected Fournier s Gangrene Caused by Acinetobacter baumannii: A Rare Case Report
 Case Reports in Surgery Volume 2016, Article ID 8461354, 4 pages http://dx.doi.org/10.1155/2016/8461354 Case Report Neglected Fournier s Gangrene Caused by Acinetobacter baumannii: A Rare Case Report Arif
Case Reports in Surgery Volume 2016, Article ID 8461354, 4 pages http://dx.doi.org/10.1155/2016/8461354 Case Report Neglected Fournier s Gangrene Caused by Acinetobacter baumannii: A Rare Case Report Arif
Haemodialysis central venous catheter-related sepsis management guideline Version 3. NAME M. Letheren Chair Clinical Effectiveness Advisory Group
 Lancashire Teaching Hospitals NHS Foundation Trust Haemodialysis central venous catheter-related sepsis management guideline Version 3 AUTHOR APPROVED BY DATE AUTH REF. NO NAME REBG/00018/July12 Michael
Lancashire Teaching Hospitals NHS Foundation Trust Haemodialysis central venous catheter-related sepsis management guideline Version 3 AUTHOR APPROVED BY DATE AUTH REF. NO NAME REBG/00018/July12 Michael
The Diagnostic Accuracy of Kernig s Sign, Brudzinski s Sign, and Nuchal Rigidity in Adults with Suspected Meningitis
 MAJOR ARTICLE The Diagnostic Accuracy of Kernig s Sign, Brudzinski s Sign, and Nuchal Rigidity in Adults with Suspected Meningitis Karen E. Thomas, 1 Rodrigo Hasbun, 1 James Jekel, 2 and Vincent J. Quagliarello
MAJOR ARTICLE The Diagnostic Accuracy of Kernig s Sign, Brudzinski s Sign, and Nuchal Rigidity in Adults with Suspected Meningitis Karen E. Thomas, 1 Rodrigo Hasbun, 1 James Jekel, 2 and Vincent J. Quagliarello
Evaluation of Children with Blunt Abdominal Trauma. James F. Holmes, MD, MPH UC Davis School of Medicine
 Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Hyperbaric Oxygen Therapy (HBO)
 MP9055 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below None Prevea360 Health Plan Medical Policy: 1.0 Hyperbaric Oxygen therapy (HBO)
MP9055 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below None Prevea360 Health Plan Medical Policy: 1.0 Hyperbaric Oxygen therapy (HBO)
The Incidence of Contrast Induced Nephropathy in Trauma Patients.
 The Incidence of Contrast Induced Nephropathy in Trauma Patients. Item Type Thesis Authors Cordeiro, Samuel Publisher The University of Arizona. Rights Copyright is held by the author. Digital access to
The Incidence of Contrast Induced Nephropathy in Trauma Patients. Item Type Thesis Authors Cordeiro, Samuel Publisher The University of Arizona. Rights Copyright is held by the author. Digital access to
MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES
 MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES 1 Marin H. Kollef, MD Professor of Medicine Virginia E. and Sam J. Golman Chair in Respiratory Intensive Care Medicine Washington University School of
MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES 1 Marin H. Kollef, MD Professor of Medicine Virginia E. and Sam J. Golman Chair in Respiratory Intensive Care Medicine Washington University School of
NIH Public Access Author Manuscript J Diabetes Metab. Author manuscript; available in PMC 2014 July 07.
 NIH Public Access Author Manuscript Published in final edited form as: J Diabetes Metab. 2013 November 1; 4(9): 310. doi:10.4172/2155-6156.1000310. Foreign Body with Gas Gangrene in an Elderly Patient
NIH Public Access Author Manuscript Published in final edited form as: J Diabetes Metab. 2013 November 1; 4(9): 310. doi:10.4172/2155-6156.1000310. Foreign Body with Gas Gangrene in an Elderly Patient
Infection Imaging In Nuclear Medicine: Arguing The Case for PET/CT.
 Infection Imaging In Nuclear Medicine: Arguing The Case for PET/CT. LUIS A. TAMARA M.D. NUCLEAR MEDICINE /PET-CT SERVICE CHIEF MEDVAMC DISCLOSURES. 2 3 Not difficult to appreciate the difference! GA-67
Infection Imaging In Nuclear Medicine: Arguing The Case for PET/CT. LUIS A. TAMARA M.D. NUCLEAR MEDICINE /PET-CT SERVICE CHIEF MEDVAMC DISCLOSURES. 2 3 Not difficult to appreciate the difference! GA-67
IMPACT #: Local Inventory #: form 04. Age at admission: d. mo yr. Postal code:
 - Date of birth: birth: Date of admission: year month day year month day Age at admission: d mo yr Postal code: Ethnic code: Hospital: Gender: 1 = male 2 = female 1 = Impact 2 = Other local, specify: Code
- Date of birth: birth: Date of admission: year month day year month day Age at admission: d mo yr Postal code: Ethnic code: Hospital: Gender: 1 = male 2 = female 1 = Impact 2 = Other local, specify: Code
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Fournier s gangrene: analysis of prognostic variables in 34 patients
 Eur J Trauma Emerg Surg (2011) 37:141 145 DOI 10.1007/s00068-010-0028-7 ORIGINAL ARTICLE Fournier s gangrene: analysis of prognostic variables in 34 patients A. García Marín J. Martín Gil A. Vaquero Rodríguez
Eur J Trauma Emerg Surg (2011) 37:141 145 DOI 10.1007/s00068-010-0028-7 ORIGINAL ARTICLE Fournier s gangrene: analysis of prognostic variables in 34 patients A. García Marín J. Martín Gil A. Vaquero Rodríguez
