Methoxycarbonyl-etomidate
|
|
|
- Victoria Morrison
- 5 years ago
- Views:
Transcription
1 Anesthesiology 2009; 111:240 9 Methoxycarbonyl-etomidate Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. A Novel Rapidly Metabolized and Ultra short-acting Etomidate Analogue that Does Not Produce Prolonged Adrenocortical Suppression Joseph F. Cotten, M.D., Ph.D.,* S. Shaukat Husain, D.Phil., Stuart A. Forman, M.D., Ph.D., Keith W. Miller, D.Phil., Elizabeth W. Kelly, B.A., Hieu H. Nguyen, B.A., Douglas E. Raines, M.D. This article is featured in This Month in Anesthesiology. Please see this issue of ANESTHESIOLOGY, page 9A. This article is accompanied by an Editorial View. Please see: Egan TD: Is anesthesiology going soft?: Trends in fragile pharmacology. ANESTHESIOLOGY 2009; 110: * Instructor of Anesthesia, Harvard Medical School, Boston, Massachusetts, and Assistant Anesthetist, Department of Anesthesia and Critical Care, Massachusetts General Hospital. Principal Associate, Harvard Medical School, and Research Associate, Department of Anesthesia and Critical Care, Massachusetts General Hospital. Associate Professor of Anesthesia, Harvard Medical School, and Associate Anesthetist, Department of Anesthesia and Critical Care, Massachusetts General Hospital. Mallinckrodt Professor of Anesthesia, Harvard Medical School, and Department of Anesthesia and Critical Care, Massachusetts General Hospital. Research Assistant, Department of Anesthesia and Critical Care, Massachusetts General Hospital. Received from the Department of Anesthesia and Critical Care, Massachusetts General Hospital, Boston, Massachusetts. Submitted for publication November 7, Accepted for publication April 22, Supported by grant P01-GM58448 from the National Institutes of Health, Bethesda, Maryland, by the Foundation for Anesthesia Education and Research, Rochester, Minnesota, and by the Department of Anesthesia and Critical Care, Massachusetts General Hospital, Boston, Massachusetts. The Massachusetts General Hospital has submitted a patent application for MOC-etomidate and related analogues. Five authors (Drs. Raines, Cotten, Forman, Husain, and Miller), their laboratories, the Department of Anesthesia and Critical Care at the Massachusetts General Hospital, and the Massachusetts General Hospital could receive royalties relating to the development or sale of these drugs. Address correspondence to Dr. Raines: Department of Anesthesia and Critical Care, Massachusetts General Hospital, 55 Fruit Street, GRB444, Boston, Massachusetts, draines@partners.org. This article may be accessed for personal use at no charge through the Journal Web site, Background: Etomidate is a rapidly acting sedative-hypnotic that provides hemodynamic stability. It causes prolonged suppression of adrenocortical steroid synthesis; therefore, its clinical utility and safety are limited. The authors describe the results of studies to define the pharmacology of (R)-3-methoxy- 3-oxopropyl1-(1-phenylethyl)-1H-imidazole-5-carboxylate (MOCetomidate), the first etomidate analogue designed to be susceptible to ultra-rapid metabolism. Methods: The -aminobutyric acid type A receptor activities of MOC-etomidate and etomidate were compared by using electrophysiological techniques in human 1 2 2L receptors. MOCetomidate s hypnotic concentration was determined in tadpoles by using a loss of righting reflex assay. Its in vitro metabolic half-life was measured in human liver S9 fraction, and the resulting metabolite was provisionally identified by using highperformance liquid chromatography/mass spectrometry techniques. The hypnotic and hemodynamic actions of MOC-etomidate, etomidate, and propofol were defined in rats. The abilities of MOC-etomidate and etomidate to inhibit corticosterone production were assessed in rats. Results: MOC-etomidate potently enhanced -aminobutyric acid type A receptor function and produced loss of righting reflex in tadpoles. Metabolism in human liver S9 fraction was first-order, with an in vitro half-life of 4.4 min versus more than 40 min for etomidate. MOC-etomidate s only detectable metabolite was a carboxylic acid. In rats, MOC-etomidate produced rapid loss of righting reflex that was extremely brief and caused minimal hemodynamic changes. Unlike etomidate, MOC-etomidate produced no adrenocortical suppression 30 min after administration. Conclusions: MOC-etomidate is an etomidate analogue that retains etomidate s important favorable pharmacological properties. However, it is rapidly metabolized, ultra short-acting, and does not produce prolonged adrenocortical suppression after bolus administration. ETOMIDATE is a rapidly acting imidazole-based intravenous (IV) sedative-hypnotic that is used to induce general anesthesia. In common with other IV induction agents, etomidate s hypnotic action in humans terminates after bolus delivery as it redistributes from the brain to other tissues and ultimately undergoes elimination by the liver with a half-life of several hours. 1,2 However, etomidate is distinguished from other induction agents by its ability to maintain hemodynamic stability, even in the setting of cardiovascular compromise. 3 6 It has consequently emerged as an agent of choice for use in critically ill patients. Etomidate also potently inhibits 11 -hydroxylase, an enzyme in the biosynthetic pathway leading to adrenocortical steroid synthesis Etomidate s potency for inhibiting 11 -hydroxylase is at least 100-fold greater than its hypnotic potency. 11 Therefore, inhibition of steroid synthesis occurs even with subhypnotic doses of etomidate. At the doses necessary to produce hypnosis, etomidate causes adrenocortical suppression that can persist for more than 4 days after discontinuing a prolonged infusion, resulting in significantly increased mortality in critically ill patients. 7,8,10 Recent studies and reports of critically ill patients show that adrenocortical suppression after even a single induction dose of etomidate can last for 24 h or more, and several suggest that it increases morbidity and/or mortality On the basis of our previous studies of etomidate analogues, 22,23 we hypothesized that analogues of etomidate could be designed that are metabolized quickly, providing etomidate s favorable pharmacological properties (e.g., rapid onset of action, high hypnotic potency, and hemodynamic stability) but also ultra-rapid recovery from both hypnosis and adrenal suppression. In this report, we describe the results of studies characterizing (R)-3-methoxy-3-oxopropyl1-(1-phenylethyl)-1H-imidazole-5-carboxylate (MOC-etomidate), the first etomidate analogue designed to undergo ultra-rapid metabolism by esterases. 240
2 ULTRA-RAPIDLY METABOLIZED ETOMIDATE ANALOGUE 241 Fig. 1. (A) Synthesis of methoxycarbonyletomidate (MOC-etomidate). (B) Structure of etomidate. Materials and Methods Animals All animal studies were conducted in accordance with rules and regulations of the Subcommittee on Research Animal Care at the Massachusetts General Hospital, Boston, Massachusetts. Early prelimb-bud stage Xenopus laevis tadpoles and adult female Xenopus laevis frogs were purchased from Xenopus One (Ann Arbor, MI) and maintained in our laboratory (tadpoles) or in the Massachusetts General Hospital Center for Comparative Medicine animal care facility (frogs). Adult male Sprague-Dawley rats ( g) were purchased from Charles River Laboratories (Wilmington, MA) and housed in the Massachusetts General Hospital Center for Comparative Medicine animal care facility. All blood draws and all IV drug administrations used a lateral tail vein IV catheter (24 gauge, 19 mm) placed under brief (approximately 1 5 min) sevoflurane anesthesia delivered using an agent-specific variable bypass vaporizer with continuous gas monitoring. Animals were weighed immediately before IV catheter placement and were allowed to fully recover from sevoflurane exposure (at least 15 to 30 min) before any study. IV catheters were secured with tape and the tail was further secured with tape to a 1-inch by 6-inch rigid, acrylic support to prevent catheter dislodgement. During all studies, rats were placed on a warming stage (Kent Scientific, Torrington, CT). Rectal temperatures were maintained between 36 and 38 C (BAT-12; Kent Scientific) as confirmed immediately upon recovery of righting reflexes and/or completion of measurements. Synthesis of MOC-Etomidate Synthesis of (R)-1-(1-phenylethyl)-1H-imidazole- 5-carboxylic acid (1). A solution of (R)-ethyl-1-(1-phenylethyl)-1H-imidazole-5-carboxylate ((R)-etomidate, 281 mg, 1.2 mmol) in methanol (5 ml) and 10% aqueous NaOH (1.7 ml) was refluxed for 30 min. After cooling, the solution was neutralized with 12 M HCl (0.351 ml). The mixture was dried by rotary evaporation, the residue was suspended in methanol-dichloromethane 1:4 v/v, and the sodium chloride was removed by filtration. (R)- 1-(1-phenylethyl)-1H-imidazole-5-carboxylic acid 1 was obtained by chromatography on a silica gel column, equilibrated with methanol-dichloromethane 1:4 v/v to give 220 mg (85% yield) of the product (fig. 1). 1 HNMR spectrum: (CD 3 OD) 9.30(d, 1H, imidazole CH), 8.23 (d, 1H, imidazole CH), 7.37 (m, 5H, phenyl), 6.64 (q, 1H, methine), 1.97 (d, 3H, methyl). Synthesis of Methyl-3-hydroxypropanoate (2). The compound was prepared essentially as described by Bartlett and Rylander. 24 -Propriolactone (4.36 g, 60.5 mmol) was added dropwise to a stirred solution of sodium methoxide (121 mg, 2.24 mmol) in anhydrous methanol (15 ml) at 78 C. The mixture was neutralized by adding an equivalent amount of HCl (2.24 ml of 1 M HCl). The mixture was filtered and rotary evaporated to remove methanol, and the oily residue was distilled at reduced pressure to obtain methyl-3-hydroxypropanoate 2 (2.72 g, 43% yield). 1 HNMR spectrum: (CDCl 3 ) 3.88 (t, 2H, methylene), 3.73 (s, 3H, methyl), 2.59 (d, 2H, methylene). Synthesis of (R)-3-methoxy-3-oxopropyl1-(1-phenylethyl)-1H-imidazole-5-carboxylate (MOC-etomidate, 3). To a mixture of (R)-1-(1-phenylethyl)-1H-imidazole-5-carboxylic acid 1 (220 mg, 1 mmol) and methyl-3-hydroxypropanoate 2 (115 mg, 1.1 mmol) in anhydrous dichloromethane (3.5 ml) was added dicyclohexylcarbodiimide (139 mg, 1.1 mmol) and p-dimethylaminopyridine (134 mg, 1.1 mmol). The solution was stirred at room temperature for 48 h. The precipitate was removed by
3 242 COTTEN ET AL. filtration, and the clear solution was applied to a silica gel column equilibrated with dichloromethane. Elution with 10% ether in dichloromethane gave the product, which was further purified by preparative thin layer chromatography with hexane-ethyl acetate 1:1 v/v on 1-mm-thick silica gel plate. The oily product was treated with HCl in anhydrous ether to obtain white, crystalline (R)-3 -methoxy-3-oxopropyl1-(1-phenylethyl)-1h-imidazole- 5-carboxylate.HCl (MOC-etomidate.hydrochloride; 198 mg, 59% yield). This product was pure as judged by high-performance liquid chromatography. 1 HNMR spectrum: (CDCl 3 ) 8.92 (d, 1H, imidazole CH), 7.76 (d, 1H, imidazole CH), 7.36 (m, 5H, phenyl), 6.49 (q, 1H, methine), 4.60 (m, 2H, methylene), 3.73 (s, 3H, methyl), 2.76 (t, 2H, methylene), 2.01 (d, 3H, methyl). Tadpole LORR Groups of five early prelimb-bud stage Xenopus laevis tadpoles were placed in 100 ml of oxygenated water buffered with 2.5 mm Tris HCl buffer (ph 7.4) and containing a concentration of MOC-etomidate ranging from M. Tadpoles were manually tipped every 5 min with a flame-polished pipette until the response stabilized. Tadpoles were judged to have loss of righting reflex (LORR) if they failed to right themselves within 5 s after being turned supine. At the end of each study, tadpoles were returned to fresh water to assure reversibility of hypnotic action. The EC 50 for LORR was determined from the MOC-etomidate concentration-dependence of LORR using the method of Waud. 25 GABA A Receptor Electrophysiology Adult female Xenopus laevis frogs were anesthetized with 0.2% tricaine (ethyl-m-aminobenzoate) and hypothermia. Ovary lobes were then excised through a small laparotomy incision and placed in OR-2 solution (82 mm NaCl, 2 mm KCl, 2 mm MgCl 2,5mM HEPES, ph 7.5) containing collagenase 1A (1 mg/ml) for 3 h to separate oocytes from connective tissue. Stage 4 and 5 oocytes were injected with messenger RNA encoding the 1, 2, and 2L subunits of the human -aminobutyric Acid Type A (GABA A ) receptor (40 ng of messenger RNA total at a subunit ratio of 1:1:2). This messenger RNA was transcribed from complementary DNA encoding for GABA A receptor 1, 2, and 2L subunits by using the mmessage mmachine High-Yield Capped RNA Transcription Kit (Ambion, Austin, Tx). Injected oocytes were incubated in ND-96 buffer solution (96 mm NaCl, 2 mm KCl, 1 mm CaCl 2, 0.8 mm MgCl 2, 10 mm HEPES, ph 7.5) containing 50 U/ml penicillin and 50 g/ml streptomycin at 17 C for at least 18 h before electrophysiological experiments. All electrophysiological recordings were performed using the whole cell two-electrode voltage-clamp technique. Oocytes were placed in a 0.04-ml recording chamber and impaled with capillary glass electrodes filled with 3 M KCl and possessing open tip resistances less than 5 M. Oocytes were then voltage-clamped at 50 mv by using a GeneClamp 500B amplifier (Axon Instruments, Union City, CA), and constantly perfused with ND-96 buffer at a rate of 4 6 ml/min. Buffer perfusion was controlled by using a six-channel valve controller (Warner Instruments, Hamden, CT) interfaced with a Digidata 1322A data acquisition system (Axon Instruments), and driven by a Dell personal computer (Round Rock, TX). Current responses were recorded by using Clampex 9.2 software (Axon Instruments), and they were processed using a Bessel (8-pole) low-pass filter with a cutoff at 50 Hz using Clampfit 9.2 software (Axon Instruments). For each oocyte, the concentration of -aminobutyric acid (GABA) that produces 5 10% of the maximal current response (EC 5 10 GABA) was determined by measuring the peak current responses evoked by a range of GABA concentrations (in ND-96 buffer) and comparing them to the maximal peak current response evoked by 1 mm GABA. The effect of each hypnotic (i.e., MOC-etomidate or etomidate) on EC 5 10 GABA-evoked currents was then assessed by first perfusing the oocyte with EC 5 10 GABA for 90 s and measuring the control peak evoked current. After a 5-min recovery period, the oocyte was perfused with drug for 90 s and then with EC 5 10 GABA plus hypnotic for 90 s and the peak evoked current was measured again. After another 5-min recovery period, the control experiment (i.e., no drug) was repeated to assure reversibility. The peak current response in the presence of drug was then normalized to the average peak current response of the two control experiments. Drug-induced potentiation was quantified from the normalized current responses in the presence versus absence of hypnotic. The effects of hypnotics on the GABA EC 50 for peak current activation were determined as described above, except that a wide range of GABA concentrations was used to evoke GABA A receptor current responses. All currents were normalized to that evoked by 1 mm GABA in the same oocyte in the absence of hypnotic. The EC 50 for peak current activation was then calculated from the GABA concentration-dependence of the normalized peak current response using a Hill equation. Metabolic Stability and Metabolite Identification The metabolic stabilities of MOC-etomidate and etomidate were assessed in vitro by adding each (20 M from a 10 mm ethanolic stock solution) to a 1-ml incubation mixture containing 0.3 mg of pooled liver S9 fraction with 1 mm nicotinamide adenine dinucleotide phosphate in phosphate buffer. After the desired time interval (5 40 min) at 37 C, 100- l aliquots of the mixture were withdrawn, and metabolism stopped by vortexing with 200 l of acetonitrile. After centrifugation (10,000g for 15 min), the supernatant was removed and evaporated
4 ULTRA-RAPIDLY METABOLIZED ETOMIDATE ANALOGUE 243 to dryness under vacuum. The drug was then reconstituted in H 2 O/acetonitrile (98/2%), and its relative levels were determined by liquid chromatography (LC)/mass spectrometry (MS) by using a Thermo Finnigan TSQ 7000 mass spectrometer (Thermo Finnigan, San Jose, CA) operating in electrospray ionization mode and interfaced with a Michrom BioResources Paradigm MS4 highperformance liquid chromatograph (Michrom Bioresources, Auburn, CA). The spectrometer was operating under the following conditions: polarity positive, capillary temperature 375 C, spray voltage 4.5 V, sheath gas (nitrogen) pressure 70 psi, and auxillary gas flow 5 l/m. Argon was used as the collision gas at 2.0 mt. The MS was operated in the selected reaction monitoring mode using a MS/MS transition unique to the parent compound. The LC method used water (A) and acetonitrile (B) as the mobile phase, 0.1% formic acid as a mobile phase modifier, a rapid linear gradient from 2% A to 100% B in 3 min at 0.7 l/min, and a 2.1 mm 20 mm MAGIC C18-AQ Bullet column from Michrom BioResources. The retention times of MOC-etomidate and its metabolite were 11.5 min and 9.4 min, respectively. In vitro half-life was calculated by curve fitting a plot of percent parent drug remaining values. Each percent parent drug remaining value was calculated from the ratio of parent compound signal (MS peak area) observed at each time point versus the time zero sample. Although this rapid in vitro approach is not useful for determining absolute concentrations in a given sample, it is satisfactory for estimating and comparing metabolic stability among related analogues. For metabolite identification, an aliquot obtained after 40 min of incubation with liver S9 fraction (same as above) was analyzed using highperformance LC/ion trap MS. The same ion source and LC devices were used for the profiling analysis. The LC method was modified for detailed analysis using a longer linear gradient (75% B in 24 min at 300 l/min) and longer column (150 mm). The ion trap MS (Thermo Finnegan LTQ equipped with an Ion Max Source) was operated in data-dependent MS/MS mode; whereby full and product ion spectra were obtained on all major components/ions observed throughout the LC run. The spectrometer was operating under the following conditions: polarity positive, capillary temperature 350 C, capillary voltage 40 V, spray voltage 4.00 kv, and tube lens voltage 100 V. Proposed structures were generated by comparing a given metabolite s product ion spectra with the product ion spectrum of the known parent compound. In addition, MS/MS spectra were observed on several source-generated fragments from each metabolite. These source fragments matched expected fragment ions produced in the corresponding product ion spectra of each parent compound and were used for elucidative purposes as well. Rat LORR Rats were briefly restrained in a 3-inch-diameter, 9-inch-long acrylic chamber with a tail exit port. The desired dose of hypnotic was injected through a lateral tail vein catheter followed by an approximately 1-ml normal saline flush. Immediately after injection, rats were removed from the restraint device and turned supine. A rat was judged to have LORR if it failed to right itself (onto all four paws) within 5 s of drug administration. A stopwatch was used to measure the duration of LORR, which was defined as the time from drug injection until the animal spontaneously righted itself. The ED 50 for LORR upon bolus administration was determined from the dose-dependence of LORR by using the method of Waud. 25 Rat Hemodynamics Femoral arterial catheters, tunneled between the scapulas, were preimplanted by the vendor (Charles River Laboratories). Animals were fully recovered from the placement procedure upon arrival. During housing and between studies, catheter patency was maintained with a heparin (500 U/ml) and hypertonic (25%) dextroselocking solution, which was withdrawn before each use and replaced just after. On the day of study and after weighing and lateral tail vein IV catheter placement, rats were restrained in the acrylic tube with a tail exit port and allowed to acclimate for approximately 15 to 20 min before data collection. The signal from the pressure transducer (TruWave, Edwards Lifesciences, Irvine, CA) was amplified by using a custom built amplifier (AD620 operational amplifier; Jameco Electronics, Belmont, CA) and digitized (1 khz) using a USB-6009 data acquisition board (National Instruments, Austin, TX) without additional filtering. All data were acquired and analyzed by using LabView Software (version 8.5 for Macintosh OS X; National Instruments). Data used for heart rate and blood pressure analysis were recorded for 5 min immediately before drug administration and for 15 min thereafter. All drugs were administered through the tail vein catheter followed by approximately 1-ml normal saline flush. Rat Adrenocortical Suppression Methods for study of rat adrenal function were adapted and optimized from several previously published reports Immediately after weighing and IV catheter placement, dexamethasone (0.2 mg/kg IV; American Regent, Shirley, NY) was administered to each rat to inhibit endogenous adrenocorticotropic hormone (ACTH) release, to suppress baseline corticosterone production, and to inhibit the variable stress response to restraint and handling. The IV tail vein catheter, used for both drug administration and blood draws, was heparinlocked after each use with 10 U/ml heparin to maintain patency; the heparin locking solution was wicked out of
5 244 COTTEN ET AL. the catheter before drug administration and blood draws to minimize rat and sample heparinization. All blood draws were approximately 0.3 ml in volume. All drugs administrations were followed by a1mlnormal saline flush to assure complete drug delivery. Two hours after dexamethasone treatment, blood was drawn (for baseline measurement of serum corticosterone concentration) and a second dose of dexamethasome (0.2 mg/kg) was administered along with either IV MOC-etomidate, etomidate, or vehicle (35% propylene glycol v/v in water) as a control. Fifteen minutes later, ACTH 1 24 (25 g/kg; Sigma-Aldrich Chemical Co, St. Louis, MO) was given intravenously to stimulate corticosterone production. Fifteen minutes after ACTH 1 24 administration (i.e., 30 min after drug or vehicle administration), a second blood sample was drawn to measure the ACTH 1 24 stimulated serum corticosterone concentration. ACTH 1 24 was dissolved in 1 mg/ml deoxygenated water as stock, aliquoted, and frozen ( 20 C); a fresh aliquot was thawed just before each use. Rats in all three groups (vehicle, etomidate, and MOC-etomidate) received the same volume of propylene glycol. Blood samples were allowed to clot at room temperature (10 to 60 min) before centrifugation at 3,500g for 5 min. Serum was carefully expressed from any resulting superficial fibrin clot by using a clean pipette tip before a second centrifugation at 3,500g for 5 min. After the second centrifugation, the resultant straw-colored, clotfree serum layer was transferred to a fresh vial for a final, high-speed centrifugation (16,000g for 5 min) to pellet any contaminating red blood cells or particulates. The serum was transferred to a clean vial and promptly frozen ( 20 C) pending corticosterone measurement within 1 to 2 days. After thawing and heat inactivation of corticosterone-binding globulins (65 C for 20 min), serum baseline and ACTH 1 24 stimulated corticosterone concentrations were quantified by using an enzyme-linked immunosorbent assay (ELISA; Diagnostic Systems Laboratories, Webster, TX) and a 96-well plate reader (Molecular Devices, Sunnyvale, CA). Statistical Analysis All data are reported as mean SD. Statistical analysis and curve fitting (using linear or nonlinear least squares regression) were done using either Prism v4.0 for Macintosh (GraphPad Software, Inc., LaJolla, CA) or Igor Pro 4.01 (Wavemetrics, Lake Oswego, OR). Metabolic halflife data were linearized by log transformation before analysis. Statistical significance indicates P 0.05 unless otherwise indicated. For multiple comparisons of physiologic data derived from rats, we performed a one-way analysis of variance (ANOVA) followed by either a Newman-Keuls or a Bonferroni post-test (which relies on an unpaired t test with a Bonferroni correction). Results LORR No LORR [MOC-etomidate] µm Fig. 2. Methoxycarbonyl-etomidate (MOC-etomidate) concentration response curve for loss of righting reflex (LORR) in tadpoles. Each data point represents the results from a single tadpole. The curve is a fit of the data set yielding an EC 50 of 8 2 M. All tadpoles recovered when removed from methoxycarbonyl-etomidate and returned to fresh water. Loss of Righting Reflexes in Tadpoles by MOC-Etomidate The MOC-etomidate concentration-response relationship for LORR in Xenopus laevis tadpoles (n 100) is shown in figure 2. The fraction of tadpoles that had LORR increased with MOC-etomidate concentration and at the highest MOC-etomidate concentrations studied ( M), all tadpoles had LORR. All tadpoles that had LORR recovered their righting reflexes when removed from MOC-etomidate and returned to fresh water. MOC-etomidate s EC 50 for LORR was 8 2 M (mean SD), a value that is 3.5-fold higher than etomidate s previously reported EC 50 for LORR from this laboratory. 22 GABA A Receptor Modulation by MOC-etomidate and Etomidate At the molecular level, there is compelling evidence that etomidate produces hypnosis by modulating the function of GABA A receptors containing 2 or 3 subunits To test whether MOC-etomidate acts by a similar mechanism, we defined its effects on human 1 2 2L GABA A receptors. Figure 3A shows representative current traces recorded upon perfusing an oocyte expressing 1 2 2L GABA A receptors with EC 5 10 GABA alone or along with either MOC-etomidate or etomidate at their respective EC 50 s for producing LORR in tadpoles. Both MOC-etomidate and etomidate significantly potentiated GABA-evoked currents. MOC-etomidate enhanced the peak current amplitudes of GABA-evoked currents by % (n 6 oocytes). In the same six oocytes, etomidate enhanced peak currents by %, a value that was not significantly different from that produced by MOC-etomidate (Student t test). Although both drugs enhanced currents evoked by low GABA concentrations, they had relatively little effect on currents evoked by high GABA concentrations (fig.
6 ULTRA-RAPIDLY METABOLIZED ETOMIDATE ANALOGUE 245 Fig. 3. Methoxycarbonyl-etomidate (MOCetomidate) and etomidate modulation of human 1 2 2L -aminobutyric acid type A receptor function. (A) Representative traces showing enhancement of currents evoked by EC aminobutyric acid (GABA) by methoxycarbonyl-etomidate and etomidate. (B) GABA concentrationresponse curves for peak current activation in the absence (control) or presence of either methoxycarbonyl-etomidate or etomidate. Error bars indicate the SD. Both drugs shifted the GABA concentration-response curves leftward, reducing the GABA EC 50 from M in the absence of drug to M and M in the presence of 8 M methoxycarbonyl-etomidate and 2 M etomidate, respectively (n 3 for each data point). 3B). This produced a statistically significant leftward shift in the GABA concentration-response curves, reducing the GABA EC 50 from M in the absence of drug to M and M in the presence of 8 M MOC-etomidate and 2 M etomidate, respectively. In Vitro Metabolism of MOC-etomidate and Etomidate As the first step towards evaluating MOC-etomidate metabolism, we defined its stability in pooled human liver S9 fraction. Figure 4 plots the percentage of unmetabolized drug remaining as a function of incubation time in pooled human liver S9 fraction ( nicotinamide adenine dinucleotide phosphate) on a semilogarithmic scale. Even after 40 min, we could detect no reduction in the concentration of etomidate, indicating that its metabolic half-life was much longer than 40 min. In contrast, MOC-etomidate was rapidly metabolized in human liver S9 fraction. The concentration of MOC-etomidate decreased as a first-order process reaching less than 1% of the original concentration by 40 min. From this data, the metabolic half-life of MOC-etomidate was determined to be approximately 4.4 min. In these studies, buspirone Fig. 4. Metabolic stability of methoxycarbonyl-etomidate (MOCetomidate) versus etomidate in pooled human liver S9 fraction. The metabolic half-life of methoxycarbonyl-etomidate was approximately 4.4 min. There was no detectable metabolism of etomidate during the 40-min incubation period. was used as an internal standard to confirm metabolic activity in the liver fraction. Its metabolic half-life was approximately 15.4 min (data not shown). The structure of the metabolite formed after 40 min of incubation in pooled human liver S9 fraction ( nicotinamide adenine dinucleotide phosphate) was analyzed by using high performance LC/ion trap MS. The ion chromatogram detected the presence of only one major metabolite. It had an m/z of 289.2, which is consistent with the carboxylic acid formed upon hydrolysis of MOCetomidate s distal ester moiety. Figure 5A shows the MS/MS spectra of the major metabolite (main spectrum) and its major fragment ion (left inset spectrum). The right inset shows a possible fragmentation pathway supporting the proposed metabolite structure. On the basis of these results, we conclude that rapid metabolism of MOC-etomidate likely occurs exclusively via the designed pathway shown in figure 5B in which the distal ester moiety of MOC-etomidate is hydrolyzed to form the corresponding carboxylic acid along with methanol as the leaving group. LORR in Rats by Propofol, Etomidate, and MOC-etomidate The hypnotic potencies and durations of hypnotic action of MOC-etomidate were compared with those of etomidate and propofol in a rat model. Figure 6A shows the propofol, etomidate, and MOC-etomidate dose-response relationships for LORR in rats. The fraction of rats that had LORR increased with the dose. At the highest doses, all rats had LORR, and there was no obvious toxicity. From these data, the ED 50 s for LORR after bolus administration of etomidate, propofol, and MOC-etomidate were determined to be mg/kg (n 18), mg/kg (n 20), and mg/kg (n 20), respectively. At doses sufficient to produce LORR in rats, all three drugs produced LORR within several seconds of IV bolus administration. The duration of LORR increased approximately linearly with the logarithm of the dose (fig. 6B); however, the slope of this relationship, which depends on the drug s half-life in the brain, 32,33 was an order of
7 246 COTTEN ET AL. Fig. 5. Methoxycarbonyl-etomidate (MOCetomidate) metabolite identification. (A) Mass spectrometry spectra of the major metabolite (main spectrum; m/z 289.2) and its major fragment ion (left inset spectrum; m/z 185.2). The metabolite produced a single major fragment ion at m/z with a neutral loss of m/z 104, consistent with a conserved region of the parent compound. Subsequent mass spectrometry/ mass spectrometry analysis of m/z produced three major ions at m/z 94.96, , and Right inset shows a possible fragmentation pathway supporting the proposed metabolite structure. (B) Metabolic pathway for methoxycarbonyletomidate upon incubation with human liver S9 fraction based on analysis of the metabolite s major fragment ion. magnitude lower for MOC-etomidate ( ) than for etomidate (27 7) or propofol (22 4). The slopes for etomidate and propofol were not significantly different from one another. Hemodynamic Actions of Propofol, Etomidate, and MOC-etomidate in Rats Etomidate is often chosen for induction over other agents in the critically ill patient because it better preserves hemodynamic stability. To determine whether MOC-etomidate similarly preserves hemodynamic stability, we measured and compared the actions of propofol, etomidate, MOC-etomidate, and vehicle (35% v/v propylene glycol in water) on heart rate and blood pressure in rats. To compare these drugs at equihypnotic doses, each was administered intravenously at twice its ED 50 for LORR (i.e., 2 mg/kg etomidate, 10 mg/kg MOCetomidate, and 8 mg/kg propofol). The volume of propylene glycol administered was the same for vehicle, etomidate, and MOC-etomidate groups. After animal acclimatization, data were recorded for 5 min before (baseline) and for 15 min after drug/vehicle injection (fig. 7). Rats in each group had similar mean heart rates and blood pressure at baseline over the first 5 min ( Fig. 6. Dose-response curves for loss of righting reflex (LORR) and duration of LORR in rats. Each data point represents the results from a single rat. (A) Etomidate, propofol, and methoxycarbonyl-etomidate (MOC-etomidate) produced LORR with ED 50 s of mg/kg, mg/ kg, and mg/kg, respectively. (B) For all three drugs, the duration of LORR increased linearly with the logarithm of the dose. The slope of this relationship was 27 7, 22 4, and for etomidate, propofol, and methoxycarbonyl-etomidate, respectively.
8 ULTRA-RAPIDLY METABOLIZED ETOMIDATE ANALOGUE 247 Fig. 7. The effects of methoxycarbonyl-etomidate (MOC-etomidate), propofol, and etomidate on mean blood pressure (BP) in rats. Drugs were given at doses equal to twice their respective ED 50 s for loss of righting reflex. Drug was injected at time 0. Each data point represents the average ( SD) change in mean blood pressure from three rats during each 30-s epoch. The inset shows a representative arterial blood pressure trace before drug administration. beats/min, mm Hg). Vehicle caused no significant change in mean blood pressure relative to baseline (5 11 mm Hg, n 3, at 90 s); data not shown in figure 7 for clarity. However, MOC-etomidate, etomidate, and propofol (n 3 animals each) each caused a significant decrease in mean blood pressure relative to baseline and to each other in this rank order for both maximum magnitude ( mm Hg, mm Hg, and mm Hg, respectively) and duration of significant effect (30 s, 6.5 min, and 7 min, respectively). For all groups, vehicle (36 14 beats/min), MOC-etomidate (24 33 beats/min), etomidate (49 67 beats/min), and propofol (64 56 beats/min), there was a small, transient, and variable increase in heart rate shortly after injection. Fig. 8. Adrenocorticotropic hormone 1 24 stimulated serum corticosterone concentrations in rats 30 min after administration of vehicle, etomidate, or methoxycarbonyl-etomidate (MOC-etomidate). Drugs were given at doses equal to twice their respective ED 50 s for loss of righting reflex. Four rats were studied in each group. Average serum corticosterone concentrations ( SD) were ng/ml, ng/ml, and ng/ml after administration of vehicle, etomidate, and methoxycarbonyl-etomidate, respectively. * P < N.S. no significant difference. Adrenocortical Suppression after Administration of Etomidate and MOC-etomidate To test whether MOC-etomidate produced prolonged adrenocortical suppression, we measured ACTH stimulated serum corticosterone concentrations in dexamethasone pretreated rats that had received MOC-etomidate, etomidate, or vehicle. Baseline serum corticosterone concentrations in rats (n 12) after dexamethasone administration averaged ng/ml and were not significantly different among the three groups (vehicle, etomidate, and MOC-etomidate). Injection of ACTH 1 24 stimulated adrenocortical steroid production as all rats had significantly higher serum corticosterone concentrations fifteen minutes after ACTH 1 24 administration. However figure 8 shows that rats that had received etomidate fifteen minutes prior to ACTH 1 24 stimulation had significantly lower serum corticosterone concentrations than those that had received either vehicle or an equi-hypnotic dose of MOC-etomidate. In contrast, rats that had received MOC-etomidate had serum corticosterone concentrations that were not different from those that had received only vehicle. Discussion MOC-etomidate is a well-tolerated etomidate analogue that retains etomidate s important favorable pharmacological properties, including rapid onset of action, high hypnotic potency, and hemodynamic stability. Like etomidate, it potently enhances GABA A receptor function. However, in contrast to etomidate, MOC-etomidate is very rapidly metabolized, ultra short-acting, and does not produce prolonged adrenocortical suppression after single IV bolus administration. MOC-etomidate is a soft analogue of etomidate. A soft analogue is a derivative of a parent compound that is specifically designed to undergo rapid and predictable metabolism after exerting its therapeutic actions. 34 Commonly used soft analogues include the opioid remifentanil and the -blocker esmolol. Both of these compounds contain labile carboxylate ester moieties that are rapidly hydrolyzed to carboxylic acids by esterases found in various organs and/or blood. The elimination half-life of these two drugs in humans is 1 2 orders of magnitude shorter than their non ester-containing analogues fentanyl and propranolol Etomidate also contains a carboxylate ester moiety that is hydrolyzed by liver esterases
9 248 COTTEN ET AL. to a carboxylic acid, but it is a poor substrate for these esterases as reflected by its several hour elimination halflife. Comparison of the structures of remifentanil and esmolol with that of etomidate suggests two reasons for etomidate s slow rate of ester hydrolysis. First, the ester moiety in etomidate is attached directly to its imidazole ring, whereas the labile ester moieties in remifentanil and esmolol are attached to ring structures via a spacer composed of two CH 2 groups. This spacer may be critical because it reduces steric hindrance, allowing esterases freer access to the carbonyl group. In support of this, as esmolol s spacer is decreased in length, its rate of ester hydrolysis decreases. 34 Second, the electrons in etomidate s carbonyl group contribute to a electron system that extends into the imidazole ring. This reduces the carbonyl carbon s partial positive charge, making it a poorer substrate for nucleophilic attack by esterases. On the basis of this reasoning, we developed the strategy of adding a new ester moiety to etomidate that is both sterically unhindered and electronically isolated from the electron systems in the imidazole ring to produce an etomidate analogue that would be rapidly metabolized. We expected that this ester moiety, like those in remifentanil and esmolol, would be rapidly hydrolyzed by esterases present in various tissues and/or blood. This was confirmed by our in vitro metabolic studies of MOC-etomidate that showed that this moiety was rapidly metabolized to a carboxylic acid in S9 liver fraction, a commonly used in vitro drug biotransformation assay. Future work will need to define the specific in vivo site (e.g., blood, plasma, and/or liver) and to confirm the identity of in vivo metabolites. In addition, a more complete understanding of MOC-etomidate metabolism may suggest methods by which the duration of action of future related drugs might be further optimized through changes in drug structure (e.g., changes in spacer length or leaving group). Our studies demonstrated that MOC-etomidate is a hypnotic in two species. It has a potency that is onefourth to one-fifth of etomidate s potency and likely produces hypnosis via the same receptor mechanism. Our rat studies further demonstrated that MOC-etomidate is an ultra short-acting hypnotic, even when given at large multiples of its ED 50 for LORR. For example, when given at dose that is 4 times its ED 50 for LORR (20 mg/kg), MOC-etomidate produced LORR in rats for only s. In comparison, propofol and etomidate produced LORR for min and 24 7 min, respectively, at approximately equihypnotic doses. Recovery from IV bolus administration of propofol and etomidate is considered to reflect redistribution of drug from the brain to other tissues rather than metabolism. Therefore, the similar slopes in the relationship between the duration of LORR and the logarithm of the drug dose (fig. 6B) suggests that propofol and etomidate redistribute from the brain at similar rates. The much faster recovery of righting reflexes and shallower slope of this relationship with MOC-etomidate suggests that ultra-rapid metabolism contributes significantly to the termination of MOC-etomidate s hypnotic action. MOC-etomidate produced a correspondingly brief (30-s) reduction in blood pressure, suggesting that MOC-etomidate s hemodynamic effects also terminate upon metabolism. In addition, we found that the maximum magnitude of this reduction was significantly less after administration of MOC-etomidate than after administration of equihypnotic doses of etomidate or propofol. Thus, it is possible to modify etomidate s chemical structure while retaining its favorable hemodynamic effects. In common with other hydrophobic imidazole-containing compounds, etomidate suppresses adrenocortical steroid production. 9,10,41,42 The primary mechanism underlying this suppression is inhibition of 11 -hydroxylase, a critical enzyme in the biosynthetic pathway leading to adrenocortical synthesis of cortisol, corticosterone, and aldosterone. 43 It has been hypothesized that etomidate inhibits 11 -hydroxylase by competing with steroid precursors at the enzyme s presumably hydrophobic catalytic site. 44 MOC-etomidate was designed to be rapidly metabolized by esterases to a highly polar carboxylic acid; therefore, we expected that MOC-etomidate would not produce prolonged adrenocortical suppression after administration. This expectation was realized as 30 minutes after administration, MOC-etomidate produced no reduction in the ACTH 1-24 stimulated serum corticosterone concentration, whereas an equihypnotic dose of etomidate significantly reduced it. Our results also imply that any effect of MOC-etomidate s rapidly formed metabolite(s) on corticosterone synthesis is negligible after administration of a single IV dose; however, additional studies will be necessary to determine whether the metabolite could reach sufficiently high levels after repeat dosing or a continuous infusion to produce significant adrenocortical suppression. We also acknowledge the possibility that MOC-etomidate may spare adrenal function, at least in part, by binding to 11 -hydroxylase with lower affinity than etomidate. This would open the possibility that MOC-etomidate or other etomidate analogues might be developed for continuous infusion, regardless of mode of metabolism, without suppressing adrenal function. In our studies, we used rats as our experimental model to assess duration of action. Rats and other small animals usually metabolize drugs significantly faster than humans. For example, the elimination half-life of remifentanil is less than 1 min in Sprague-Dawley rats as compared to 10 min (or longer) in humans. 35,45 47 Therefore, the duration of hypnosis produced by MOC-etomidate will almost certainly be longer in humans than in rats and probably be similar to those of remifentanil and esmolol (5 10 min), the prototypical esterase-metabolized drugs after which MOC-etomidate was modeled.
10 ULTRA-RAPIDLY METABOLIZED ETOMIDATE ANALOGUE 249 The authors thank Jeffrey Whitney B.S., Vice President of Novatia LLC, Monmouth Junction, New Jersey, for analytical assistance. References 1. de Ruiter G, Popescu DT, de Boer AG, Smeekens JB, Breimer DD: Pharmacokinetics of etomidate in surgical patients. Arch Int Pharmacodyn Ther 1981; 249: Hebron BS, Edbrooke DL, Newby DM, Mather SJ: Pharmacokinetics of etomidate associated with prolonged i.v. infusion. Br J Anaesth 1983; 55: McCollum JS, Dundee JW: Comparison of induction characteristics of four intravenous anaesthetic agents. Anaesthesia 1986; 41: Gooding JM, Weng JT, Smith RA, Berninger GT, Kirby RR: Cardiovascular and pulmonary responses following etomidate induction of anesthesia in patients with demonstrated cardiac disease. Anesth Analg 1979; 58: Gooding JM, Corssen G: Effect of etomidate on the cardiovascular system. Anesth Analg 1977; 56: Ebert TJ, Muzi M, Berens R, Goff D, Kampine JP: Sympathetic responses to induction of anesthesia in humans with propofol or etomidate. ANESTHESIOLOGY 1992; 76: Watt I, Ledingham IM: Mortality amongst multiple trauma patients admitted to an intensive therapy unit. Anaesthesia 1984; 39: Ledingham IM, Watt I: Influence of sedation on mortality in critically ill multiple trauma patients. Lancet 1983; 1: Wagner RL, White PF: Etomidate inhibits adrenocortical function in surgical patients. ANESTHESIOLOGY 1984; 61: Wagner RL, White PF, Kan PB, Rosenthal MH, Feldman D: Inhibition of adrenal steroidogenesis by the anesthetic etomidate. N Engl J Med 1984; 310: Zolle IM, Berger ML, Hammerschmidt F, Hahner S, Schirbel A, Peric-Simov B,: New selective inhibitors of steroid 11beta-hydroxylation in the adrenal cortex. Synthesis and structure-activity relationship of potent etomidate analogues. J Med Chem 2008; 51: Absalom A, Pledger D, Kong A: Adrenocortical function in critically ill patients 24 h after a single dose of etomidate. Anaesthesia 1999; 54: Malerba G, Romano-Girard F, Cravoisy A, Dousset B, Nace L, Levy B, Bollaert PE: Risk factors of relative adrenocortical deficiency in intensive care patients needing mechanical ventilation. Intensive Care Med 2005; 31: den Brinker M, Joosten KF, Liem O, de Jong FH, Hop WC, Hazelzet JA, van Dijk M, Hokken-Koelega AC: Adrenal insufficiency in meningococcal sepsis: bioavailable cortisol levels and impact of interleukin-6 levels and intubation with etomidate on adrenal function and mortality. J Clin Endocrinol Metab 2005; 90: den Brinker M, Hokken-Koelega AC, Hazelzet JA, de Jong FH, Hop WC, Joosten KF: One single dose of etomidate negatively influences adrenocortical performance for at least 24h in children with meningococcal sepsis. Intensive Care Med 2007; 34: Lundy JB, Slane ML, Frizzi JD: Acute adrenal insufficiency after a single dose of etomidate. J Intensive Care Med 2007; 22: Lipiner-Friedman D, Sprung CL, Laterre PF, Weiss Y, Goodman SV, Vogeser M, Briegel J, Keh D, Singer M, Moreno R, Bellissant E, Annane D: Adrenal function in sepsis: The retrospective Corticus cohort study. Crit Care Med 2007; 35: Vinclair M, Broux C, Faure P, Brun J, Genty C, Jacquot C, Chabre O, Payen JF: Duration of adrenal inhibition following a single dose of etomidate in critically ill patients. Intensive Care Med 2008; 34: Sprung CL, Annane D, Keh D, Moreno R, Singer M, Freivogel K, Weiss YG, Benbenishty J, Kalenka A, Forst H, Laterre PF, Reinhart K, Cuthbertson BH, Payen D, Briegel J: Hydrocortisone therapy for patients with septic shock. N Engl J Med 2008; 358: Hildreth AN, Mejia VA, Maxwell RA, Smith PW, Dart BW, Barker DE: Adrenal suppression following a single dose of etomidate for rapid sequence induction: A prospective randomized study. J Trauma 2008; 65: Cotton BA, Guillamondegui OD, Fleming SB, Carpenter RO, Patel SH, Morris JA Jr, Arbogast PG: Increased risk of adrenal insufficiency following etomidate exposure in critically injured patients. Arch Surg 2008; 143: Husain SS, Ziebell MR, Ruesch D, Hong F, Arevalo E, Kosterlitz JA, Olsen RW, Forman SA, Cohen JB, Miller KW: 2-(3-Methyl-3H-diaziren-3-yl)ethyl 1-(1- phenylethyl)-1h-imidazole-5-carboxylate: a derivative of the stereoselective general anesthetic etomidate for photolabeling ligand-gated ion channels. J Med Chem 2003; 46: Husain SS, Nirthanan S, Ruesch D, Solt K, Cheng Q, Li GD, Arevalo E, Olsen RW, Raines DE, Forman SA, Cohen JB, Miller KW: Synthesis of trifluoromethylaryl diazirine and benzophenone derivatives of etomidate that are potent general anesthetics and effective photolabels for probing sites on ligand-gated ion channels. J Med Chem 2006; 49: Bartlett PD, Rylander PN: -Propriolactone. XII Mechanisms involved in the reaction of -propriolactone with acids and bases. J Am Chem Soc 1951; 73: Waud DR: On biological assays involving quantal responses. J Pharmacol Exp Ther 1972; 183: Fish KJ, Rice SA, Margary J: Contrasting effects of etomidate and propylene glycol upon enflurane metabolism and adrenal steroidogenesis in Fischer 344 rats. ANESTHESIOLOGY 1988; 68: Cole MA, Kim PJ, Kalman BA, Spencer RL: Dexamethasone suppression of corticosteroid secretion: Evaluation of the site of action by receptor measures and functional studies. Psychoneuroendocrinology 2000; 25: Johnson EO, Kamilaris TC, Calogero AE, Gold PW, Chrousos GP: Experimentally-induced hyperthyroidism is associated with activation of the rat hypothalamic-pituitary-adrenal axis. Eur J Endocrinol 2005; 153: Belelli D, Muntoni AL, Merrywest SD, Gentet LJ, Casula A, Callachan H, Madau P, Gemmell DK, Hamilton NM, Lambert JJ, Sillar KT, Peters JA: The in vitro and in vivo enantioselectivity of etomidate implicates the GABAA receptor in general anaesthesia. Neuropharmacology 2003; 45: Rusch D, Zhong H, Forman SA: Gating allosterism at a single class of etomidate sites on alpha1beta2gamma2l GABA A receptors accounts for both direct activation and agonist modulation. J Biol Chem 2004; 279: Jurd R, Arras M, Lambert S, Drexler B, Siegwart R, Crestani F, Zaugg M, Vogt KE, Ledermann B, Antkowiak B, Rudolph U: General anesthetic actions in vivo strongly attenuated by a point mutation in the GABA(A) receptor beta3 subunit. Faseb J 2003; 17: Shafer SL: Principles of Pharmacokinetics and Pharmacodynamics Anesthesiology, Edited by Longnecker DE, Tinker JH, Morgan GE. St. Louis, Mosby Publishers, 1998, pp Liao M, Sonner JM, Husain SS, Miller KW, Jurd R, Rudolph U, Eger EI 2nd: R( ) etomidate and the photoactivable R ( ) azietomidate have comparable anesthetic activity in wild-type mice and comparably decreased activity in mice with a N265M point mutation in the gamma-aminobutyric acid receptor beta3 subunit. Anesth Analg 2005; 101: Bodor N, Buchwald P: Soft drug design: General principles and recent applications. Med Res Rev 2000; 20: Westmoreland CL, Hoke JF, Sebel PS, Hug CC Jr, Muir KT: Pharmacokinetics of remifentanil (GI87084B) and its major metabolite (GI90291) in patients undergoing elective inpatient surgery. ANESTHESIOLOGY 1993; 79: Sum CY, Yacobi A, Kartzinel R, Stampfli H, Davis CS, Lai CM: Kinetics of esmolol, an ultra-short-acting beta blocker, and of its major metabolite. Clin Pharmacol Ther 1983; 34: Wiest DB, Trippel DL, Gillette PC, Garner SS: Pharmacokinetics of esmolol in children. Clin Pharmacol Ther 1991; 49: Schleimer R, Benjamini E, Eisele J, Henderson G: Pharmacokinetics of fentanyl as determined by radioimmunoassay. Clin Pharmacol Ther 1978; 23: Bentley JB, Borel JD, Nenad RE Jr, Gillespie TJ: Age and fentanyl pharmacokinetics. Anesth Analg 1982; 61: Williams FM, Leeser JE, Rawlins MD: Pharmacodynamics and pharmacokinetics of single doses of ketanserin and propranolol alone and in combination in healthy volunteers. Br J Clin Pharmacol 1986; 22: Como JA, Dismukes WE: Oral azole drugs as systemic antifungal therapy. N Engl J Med 1994; 330: Pont A, Williams PL, Loose DS, Feldman D, Reitz RE, Bochra C, Stevens DA: Ketoconazole blocks adrenal steroid synthesis. Ann Intern Med 1982; 97: de Jong FH, Mallios C, Jansen C, Scheck PA, Lamberts SW: Etomidate suppresses adrenocortical function by inhibition of 11 beta-hydroxylation. J Clin Endocrinol Metab 1984; 59: Roumen L, Sanders MP, Pieterse K, Hilbers PA, Plate R, Custers E, de Gooyer M, Smits JF, Beugels I, Emmen J, Ottenheijm HC, Leysen D, Hermans JJ: Construction of 3D models of the CYP11B family as a tool to predict ligand binding characteristics. J Comput Aided Mol Des 2007; 21: Haidar SH, Moreton JE, Liang Z, Hoke JF, Muir KT, Eddington ND: Evaluating a possible pharmacokinetic interaction between remifentanil and esmolol in the rat. J Pharm Sci 1997; 86: Egan TD, Minto CF, Hermann DJ, Barr J, Muir KT, Shafer SL: Remifentanil versus alfentanil: Comparative pharmacokinetics and pharmacodynamics in healthy adult male volunteers. ANESTHESIOLOGY 1996; 84: Egan TD, Lemmens HJ, Fiset P, Hermann DJ, Muir KT, Stanski DR, Shafer SL: The pharmacokinetics of the new short-acting opioid remifentanil (GI87084B) in healthy adult male volunteers. ANESTHESIOLOGY 1993; 79:881 92
Determination of 6-Chloropicolinic Acid (6-CPA) in Crops by Liquid Chromatography with Tandem Mass Spectrometry Detection. EPL-BAS Method No.
 Page 1 of 10 Determination of 6-Chloropicolinic Acid (6-CPA) in Crops by Liquid Chromatography with Tandem Mass Spectrometry Detection EPL-BAS Method No. 205G881B Method Summary: Residues of 6-CPA are
Page 1 of 10 Determination of 6-Chloropicolinic Acid (6-CPA) in Crops by Liquid Chromatography with Tandem Mass Spectrometry Detection EPL-BAS Method No. 205G881B Method Summary: Residues of 6-CPA are
O O H. Robert S. Plumb and Paul D. Rainville Waters Corporation, Milford, MA, U.S. INTRODUCTION EXPERIMENTAL. LC /MS conditions
 Simplifying Qual/Quan Analysis in Discovery DMPK using UPLC and Xevo TQ MS Robert S. Plumb and Paul D. Rainville Waters Corporation, Milford, MA, U.S. INTRODUCTION The determination of the drug metabolism
Simplifying Qual/Quan Analysis in Discovery DMPK using UPLC and Xevo TQ MS Robert S. Plumb and Paul D. Rainville Waters Corporation, Milford, MA, U.S. INTRODUCTION The determination of the drug metabolism
Analytical Method for 2, 4, 5-T (Targeted to Agricultural, Animal and Fishery Products)
 Analytical Method for 2, 4, 5-T (Targeted to Agricultural, Animal and Fishery Products) The target compound to be determined is 2, 4, 5-T. 1. Instrument Liquid Chromatograph-tandem mass spectrometer (LC-MS/MS)
Analytical Method for 2, 4, 5-T (Targeted to Agricultural, Animal and Fishery Products) The target compound to be determined is 2, 4, 5-T. 1. Instrument Liquid Chromatograph-tandem mass spectrometer (LC-MS/MS)
Supporting information
 Supporting information Figure legends Supplementary Table 1. Specific product ions obtained from fragmentation of lithium adducts in the positive ion mode comparing the different positional isomers of
Supporting information Figure legends Supplementary Table 1. Specific product ions obtained from fragmentation of lithium adducts in the positive ion mode comparing the different positional isomers of
Onesingledoseofetomidatenegatively influences adrenocortical performance for at least 24 h in children with meningococcal sepsis
 Intensive Care Med (2008) 34:163 168 DOI 10.1007/s00134-007-0836-3 BRIEF REPORT Marieke den Brinker Anita C. S. Hokken-Koelega Jan A. Hazelzet Frank H. de Jong Wim C. J. Hop Koen F. M. Joosten Onesingledoseofetomidatenegatively
Intensive Care Med (2008) 34:163 168 DOI 10.1007/s00134-007-0836-3 BRIEF REPORT Marieke den Brinker Anita C. S. Hokken-Koelega Jan A. Hazelzet Frank H. de Jong Wim C. J. Hop Koen F. M. Joosten Onesingledoseofetomidatenegatively
Robust extraction, separation, and quantitation of structural isomer steroids from human plasma by SPE-UHPLC-MS/MS
 TECHNICAL NOTE 21882 Robust extraction, separation, and quantitation of structural isomer steroids human plasma by SPE-UHPLC-MS/MS Authors Jon Bardsley 1, Kean Woodmansey 1, and Stacy Tremintin 2 1 Thermo
TECHNICAL NOTE 21882 Robust extraction, separation, and quantitation of structural isomer steroids human plasma by SPE-UHPLC-MS/MS Authors Jon Bardsley 1, Kean Woodmansey 1, and Stacy Tremintin 2 1 Thermo
Determination of β2-agonists in Pork Using Agilent SampliQ SCX Solid-Phase Extraction Cartridges and Liquid Chromatography-Tandem Mass Spectrometry
 Determination of β2-agonists in Pork Using Agilent SampliQ SCX Solid-Phase Extraction Cartridges and Liquid Chromatography-Tandem Mass Spectrometry Application Note Food Safety Authors Chenhao Zhai Agilent
Determination of β2-agonists in Pork Using Agilent SampliQ SCX Solid-Phase Extraction Cartridges and Liquid Chromatography-Tandem Mass Spectrometry Application Note Food Safety Authors Chenhao Zhai Agilent
Student Handout. This experiment allows you to explore the properties of chiral molecules. You have
 Student Handout This experiment allows you to explore the properties of chiral molecules. You have learned that some compounds exist as enantiomers non-identical mirror images, such as your left and right
Student Handout This experiment allows you to explore the properties of chiral molecules. You have learned that some compounds exist as enantiomers non-identical mirror images, such as your left and right
Application Note. Author. Abstract. Introduction. Food Safety
 Determination of β2-agonists in Pork with SPE eanup and LC-MS/MS Detection Using Agilent BondElut PCX Solid-Phase Extraction Cartridges, Agilent Poroshell 120 column and Liquid Chromatography-Tandem Mass
Determination of β2-agonists in Pork with SPE eanup and LC-MS/MS Detection Using Agilent BondElut PCX Solid-Phase Extraction Cartridges, Agilent Poroshell 120 column and Liquid Chromatography-Tandem Mass
SUPPLEMENTARY DATA. Materials and Methods
 SUPPLEMENTARY DATA Materials and Methods HPLC-UV of phospholipid classes and HETE isomer determination. Fractionation of platelet lipid classes was undertaken on a Spherisorb S5W 150 x 4.6 mm column (Waters
SUPPLEMENTARY DATA Materials and Methods HPLC-UV of phospholipid classes and HETE isomer determination. Fractionation of platelet lipid classes was undertaken on a Spherisorb S5W 150 x 4.6 mm column (Waters
Supplementary Material (ESI) for Chemical Communications This journal is (c) The Royal Society of Chemistry 2008
 Experimental Details Unless otherwise noted, all chemicals were purchased from Sigma-Aldrich Chemical Company and were used as received. 2-DOS and neamine were kindly provided by Dr. F. Huang. Paromamine
Experimental Details Unless otherwise noted, all chemicals were purchased from Sigma-Aldrich Chemical Company and were used as received. 2-DOS and neamine were kindly provided by Dr. F. Huang. Paromamine
Detection of Low Level of Chloramphenicol in Milk and Honey with MIP SPE and LC-MS-MS
 Detection of Low Level of Chloramphenicol in Milk and Honey with MIP SPE and LC-MS-MS Olga Shimelis, An Trinh, and Michael Ye Supelco, Div. of Sigma-Aldrich, Bellefonte, PA T407125 Introduction Molecularly
Detection of Low Level of Chloramphenicol in Milk and Honey with MIP SPE and LC-MS-MS Olga Shimelis, An Trinh, and Michael Ye Supelco, Div. of Sigma-Aldrich, Bellefonte, PA T407125 Introduction Molecularly
Pharmacokinetics of drug infusions
 SA Hill MA PhD FRCA Key points The i.v. route provides the most predictable plasma concentrations. Pharmacodynamic effects of a drug are related to plasma concentration. Both plasma and effect compartments
SA Hill MA PhD FRCA Key points The i.v. route provides the most predictable plasma concentrations. Pharmacodynamic effects of a drug are related to plasma concentration. Both plasma and effect compartments
Designer Fentanyls Drugs that kill and how to detect them. Cyclopropylfentanyl
 Designer Fentanyls Drugs that kill and how to detect them Cyclopropylfentanyl Science for a safer world The in vitro metabolism of cyclopropylfentanyl Simon Hudson & Charlotte Cutler, Sport and Specialised
Designer Fentanyls Drugs that kill and how to detect them Cyclopropylfentanyl Science for a safer world The in vitro metabolism of cyclopropylfentanyl Simon Hudson & Charlotte Cutler, Sport and Specialised
Supporting Information
 Supporting Information Schlosburg et al. 10.1073/pnas.1219159110 SI Materials and Methods: Quantification of Heroin Metabolites Sample Collection. Trunk blood was collected in a 1:1 ratio with acetate
Supporting Information Schlosburg et al. 10.1073/pnas.1219159110 SI Materials and Methods: Quantification of Heroin Metabolites Sample Collection. Trunk blood was collected in a 1:1 ratio with acetate
SPE-LC-MS/MS Method for the Determination of Nicotine, Cotinine, and Trans-3-hydroxycotinine in Urine
 SPE-LC-MS/MS Method for the Determination of Nicotine, Cotinine, and Trans-3-hydroxycotinine in Urine J. Jones, Thermo Fisher Scientific, Runcorn, Cheshire, UK Application Note 709 Key Words SPE, SOLA
SPE-LC-MS/MS Method for the Determination of Nicotine, Cotinine, and Trans-3-hydroxycotinine in Urine J. Jones, Thermo Fisher Scientific, Runcorn, Cheshire, UK Application Note 709 Key Words SPE, SOLA
LC-MS/MS Method for the Determination of Tenofovir from Plasma
 LC-MS/MS Method for the Determination of Tenofovir from Plasma Kimberly Phipps, Thermo Fisher Scientific, Runcorn, Cheshire, UK Application Note 687 Key Words SPE, SOLA CX, Hypersil GOLD, tenofovir Abstract
LC-MS/MS Method for the Determination of Tenofovir from Plasma Kimberly Phipps, Thermo Fisher Scientific, Runcorn, Cheshire, UK Application Note 687 Key Words SPE, SOLA CX, Hypersil GOLD, tenofovir Abstract
A Novel Solution for Vitamin K₁ and K₂ Analysis in Human Plasma by LC-MS/MS
 A Novel Solution for Vitamin K₁ and K₂ Analysis in Human Plasma by LC-MS/MS By Shun-Hsin Liang and Frances Carroll Abstract Vitamin K₁ and K₂ analysis is typically complex and time-consuming because these
A Novel Solution for Vitamin K₁ and K₂ Analysis in Human Plasma by LC-MS/MS By Shun-Hsin Liang and Frances Carroll Abstract Vitamin K₁ and K₂ analysis is typically complex and time-consuming because these
Rapid and Robust Detection of THC and Its Metabolites in Blood
 Rapid and Robust Detection of THC and Its Metabolites in Blood Application Note Forensics/Doping Control Author Stephan Baumann Agilent Technologies, Inc. Santa Clara CA 95051 USA Abstract A robust method
Rapid and Robust Detection of THC and Its Metabolites in Blood Application Note Forensics/Doping Control Author Stephan Baumann Agilent Technologies, Inc. Santa Clara CA 95051 USA Abstract A robust method
Edgar Naegele. Abstract
 Simultaneous determination of metabolic stability and identification of buspirone metabolites using multiple column fast LC/TOF mass spectrometry Application ote Edgar aegele Abstract A recent trend in
Simultaneous determination of metabolic stability and identification of buspirone metabolites using multiple column fast LC/TOF mass spectrometry Application ote Edgar aegele Abstract A recent trend in
Dienes Derivatization MaxSpec Kit
 Dienes Derivatization MaxSpec Kit Item No. 601510 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL INFORMATION
Dienes Derivatization MaxSpec Kit Item No. 601510 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL INFORMATION
Supporting Information for. Boronic Acid Functionalized Aza-Bodipy (azabdpba) based Fluorescence Optodes for the. analysis of Glucose in Whole Blood
 Supporting Information for Boronic Acid Functionalized Aza-Bodipy (azabdpba) based Fluorescence Optodes for the analysis of Glucose in Whole Blood Yueling Liu, Jingwei Zhu, Yanmei Xu, Yu Qin*, Dechen Jiang*
Supporting Information for Boronic Acid Functionalized Aza-Bodipy (azabdpba) based Fluorescence Optodes for the analysis of Glucose in Whole Blood Yueling Liu, Jingwei Zhu, Yanmei Xu, Yu Qin*, Dechen Jiang*
Determination of Chlorophenoxyacetic Acid and Other Acidic Herbicides Using a QuEChERS Sample Preparation Approach and LC-MS/MS Analysis
 Determination of Chlorophenoxyacetic Acid and Other Acidic Herbicides Using a QuEChERS Sample Preparation Approach and LC-MS/MS Analysis UCT Product Number: ECQUEU75CT-MP - Mylar pouch containing extraction
Determination of Chlorophenoxyacetic Acid and Other Acidic Herbicides Using a QuEChERS Sample Preparation Approach and LC-MS/MS Analysis UCT Product Number: ECQUEU75CT-MP - Mylar pouch containing extraction
Synthesis and Blastocyst Implantation Inhibition Potential of Lupeol Derivatives in Female Mice
 Supporting Information Rec. Nat. Prod. 9:4 (2015) 561-566 Synthesis and Blastocyst Implantation Inhibition Potential of Lupeol Derivatives in Female Mice Anita Mahapatra 1*, Purvi Shah 1, Mehul Jivrajani
Supporting Information Rec. Nat. Prod. 9:4 (2015) 561-566 Synthesis and Blastocyst Implantation Inhibition Potential of Lupeol Derivatives in Female Mice Anita Mahapatra 1*, Purvi Shah 1, Mehul Jivrajani
Tenofovir disoproxil fumarate (Tenofoviri disoproxili fumaras)
 C 19 H 30 N 5 O 10 P. C 4 H 4 O 4 Relative molecular mass. 635.5. Chemical names. bis(1-methylethyl) 5-{[(1R)-2-(6-amino-9H-purin-9-yl)-1-methylethoxy]methyl}-5-oxo-2,4,6,8-tetraoxa-5-λ 5 - phosphanonanedioate
C 19 H 30 N 5 O 10 P. C 4 H 4 O 4 Relative molecular mass. 635.5. Chemical names. bis(1-methylethyl) 5-{[(1R)-2-(6-amino-9H-purin-9-yl)-1-methylethoxy]methyl}-5-oxo-2,4,6,8-tetraoxa-5-λ 5 - phosphanonanedioate
Naoya Takahashi, Keiya Hirota and Yoshitaka Saga* Supplementary material
 Supplementary material Facile transformation of the five-membered exocyclic E-ring in 13 2 -demethoxycarbonyl chlorophyll derivatives by molecular oxygen with titanium oxide in the dark Naoya Takahashi,
Supplementary material Facile transformation of the five-membered exocyclic E-ring in 13 2 -demethoxycarbonyl chlorophyll derivatives by molecular oxygen with titanium oxide in the dark Naoya Takahashi,
A biocatalytic hydrogenation of carboxylic acids
 Electronic Supplementary Information (ESI) for: A biocatalytic hydrogenation of carboxylic acids Yan Ni, Peter-Leon Hagedoorn,* Jian-He Xu, Isabel Arends, Frank Hollmann* 1. General Chemicals All the carboxylic
Electronic Supplementary Information (ESI) for: A biocatalytic hydrogenation of carboxylic acids Yan Ni, Peter-Leon Hagedoorn,* Jian-He Xu, Isabel Arends, Frank Hollmann* 1. General Chemicals All the carboxylic
A Robustness Study for the Agilent 6470 LC-MS/MS Mass Spectrometer
 A Robustness Study for the Agilent 7 LC-MS/MS Mass Spectrometer Application Note Clinical Research Authors Linda Côté, Siji Joseph, Sreelakshmy Menon, and Kevin McCann Agilent Technologies, Inc. Abstract
A Robustness Study for the Agilent 7 LC-MS/MS Mass Spectrometer Application Note Clinical Research Authors Linda Côté, Siji Joseph, Sreelakshmy Menon, and Kevin McCann Agilent Technologies, Inc. Abstract
Is action potential threshold lowest in the axon?
 Supplementary information to: Is action potential threshold lowest in the axon? Maarten H. P. Kole & Greg J. Stuart Supplementary Fig. 1 Analysis of action potential (AP) threshold criteria. (a) Example
Supplementary information to: Is action potential threshold lowest in the axon? Maarten H. P. Kole & Greg J. Stuart Supplementary Fig. 1 Analysis of action potential (AP) threshold criteria. (a) Example
ph Switchable and Fluorescent Ratiometric Squarylium Indocyanine Dyes as Extremely Alkaline Sensors
 ph Switchable and Fluorescent Ratiometric Squarylium Indocyanine Dyes as Extremely Alkaline Sensors Jie Li, Chendong Ji, Wantai Yang, Meizhen Yin* State Key Laboratory of Chemical Resource Engineering,
ph Switchable and Fluorescent Ratiometric Squarylium Indocyanine Dyes as Extremely Alkaline Sensors Jie Li, Chendong Ji, Wantai Yang, Meizhen Yin* State Key Laboratory of Chemical Resource Engineering,
Supporting Information (SI)
 Electronic Supplementary Material (ESI) for Analyst. This journal is The Royal Society of Chemistry 2015 Supporting Information (SI) Title: Optimization of Metabolite Extraction of Human Vein Tissue for
Electronic Supplementary Material (ESI) for Analyst. This journal is The Royal Society of Chemistry 2015 Supporting Information (SI) Title: Optimization of Metabolite Extraction of Human Vein Tissue for
Human TRPC6 Ion Channel Cell Line
 TECHNICAL DATA SHEET ValiScreen Ion Channel Cell Line Caution: For Laboratory Use. A research product for research purposes only Human TRPC6 Ion Channel Cell Line Product No.: AX-012-C Lot No.: 512-548-A
TECHNICAL DATA SHEET ValiScreen Ion Channel Cell Line Caution: For Laboratory Use. A research product for research purposes only Human TRPC6 Ion Channel Cell Line Product No.: AX-012-C Lot No.: 512-548-A
Etomidate is a short-acting, sedative hypnotic
 Hosp Pharm 2014;49(2):177 183 2014 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj4902-177 Original Article Effects of Etomidate on Adrenal Suppression: A Review of Intubated Septic
Hosp Pharm 2014;49(2):177 183 2014 Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj4902-177 Original Article Effects of Etomidate on Adrenal Suppression: A Review of Intubated Septic
LC/MS Method for Comprehensive Analysis of Plasma Lipids
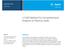 Application Note omics LC/MS Method for Comprehensive Analysis of Plasma s Authors Tomas Cajka and Oliver Fiehn West Coast Metabolomics Center, University of California Davis, 451 Health Sciences Drive,
Application Note omics LC/MS Method for Comprehensive Analysis of Plasma s Authors Tomas Cajka and Oliver Fiehn West Coast Metabolomics Center, University of California Davis, 451 Health Sciences Drive,
Analysis of anti-epileptic drugs in human serum using an Agilent Ultivo LC/TQ
 Application Note Clinical Research Analysis of anti-epileptic drugs in human serum using an Agilent Ultivo LC/TQ Authors Jennifer Hitchcock 1, Lauren Frick 2, Peter Stone 1, and Vaughn Miller 2 1 Agilent
Application Note Clinical Research Analysis of anti-epileptic drugs in human serum using an Agilent Ultivo LC/TQ Authors Jennifer Hitchcock 1, Lauren Frick 2, Peter Stone 1, and Vaughn Miller 2 1 Agilent
VaTx1 VaTx2 VaTx3. VaTx min Retention Time (min) Retention Time (min)
 a Absorbance (mau) 5 2 5 3 4 5 6 7 8 9 6 2 3 4 5 6 VaTx2 High Ca 2+ Low Ca 2+ b 38.2 min Absorbance (mau) 3 2 3 4 5 3 2 VaTx2 39.3 min 3 4 5 3 2 4. min 3 4 5 Supplementary Figure. Toxin Purification For
a Absorbance (mau) 5 2 5 3 4 5 6 7 8 9 6 2 3 4 5 6 VaTx2 High Ca 2+ Low Ca 2+ b 38.2 min Absorbance (mau) 3 2 3 4 5 3 2 VaTx2 39.3 min 3 4 5 3 2 4. min 3 4 5 Supplementary Figure. Toxin Purification For
UPLC-MS/MS Analysis of Azole Antifungals in Serum for Clinical Research
 Stephen Balloch and Gareth Hammond Waters Corporation, Wilmslow, UK APPLICATION BENEFITS Analytical selectivity afforded by mass selective detection Wide linear measuring range Simple, inexpensive sample
Stephen Balloch and Gareth Hammond Waters Corporation, Wilmslow, UK APPLICATION BENEFITS Analytical selectivity afforded by mass selective detection Wide linear measuring range Simple, inexpensive sample
EXPERIMENT 13: Isolation and Characterization of Erythrocyte
 EXPERIMENT 13: Isolation and Characterization of Erythrocyte Day 1: Isolation of Erythrocyte Steps 1 through 6 of the Switzer & Garrity protocol (pages 220-221) have been performed by the TA. We will be
EXPERIMENT 13: Isolation and Characterization of Erythrocyte Day 1: Isolation of Erythrocyte Steps 1 through 6 of the Switzer & Garrity protocol (pages 220-221) have been performed by the TA. We will be
Extraction of a Comprehensive Steroid Panel from Human Serum Using ISOLUTE. SLE+ Prior to LC/MS-MS Analysis
 Application Note AN890 Extraction of a Comprehensive Steroid Panel from Human Serum Using ISOLUTE SLE+ Page Extraction of a Comprehensive Steroid Panel from Human Serum Using ISOLUTE SLE+ Prior to LC/MS-MS
Application Note AN890 Extraction of a Comprehensive Steroid Panel from Human Serum Using ISOLUTE SLE+ Page Extraction of a Comprehensive Steroid Panel from Human Serum Using ISOLUTE SLE+ Prior to LC/MS-MS
Identification of Steroids in Water by Ion Trap LC/MS/MS Application
 Identification of Steroids in Water by Ion Trap LC/MS/MS Application Environmental Author Paul Zavitsanos and Christine Miller Agilent Technologies, Inc. Centerville Road Wilmington, DE 9- USA Abstract
Identification of Steroids in Water by Ion Trap LC/MS/MS Application Environmental Author Paul Zavitsanos and Christine Miller Agilent Technologies, Inc. Centerville Road Wilmington, DE 9- USA Abstract
Step 3: muscle, nasal sprays and drops or used as topical
 Extraction of Corticosteroids using 96-well Supported Liquid Extraction (SLE) and LC-MS/MS Analysis Lee Williams, Matthew Cleeve, elen Lodder, Steve Jordan, Richard Calverley & Joanna Smith Biotage GB
Extraction of Corticosteroids using 96-well Supported Liquid Extraction (SLE) and LC-MS/MS Analysis Lee Williams, Matthew Cleeve, elen Lodder, Steve Jordan, Richard Calverley & Joanna Smith Biotage GB
Summary Chapter 8 CHAPTER 8. Summary. Page 173
 CHAPTER 8 Summary Page 173 Chapter 2: Liquid Chromatography/Tandem Mass Spectrometry Method for Quantitative Estimation of PEG 400 and its Applications A rapid sensitive and selective MRM based method
CHAPTER 8 Summary Page 173 Chapter 2: Liquid Chromatography/Tandem Mass Spectrometry Method for Quantitative Estimation of PEG 400 and its Applications A rapid sensitive and selective MRM based method
Pharmacology of intravenous induction agents
 Pharmacology of intravenous induction agents Ákos Csomós MD, PhD Professor, Head of Department Medical Centre, Hungarian Defence Force, Budapest What do we have in the market? Thiopental Metohexital Etomidate
Pharmacology of intravenous induction agents Ákos Csomós MD, PhD Professor, Head of Department Medical Centre, Hungarian Defence Force, Budapest What do we have in the market? Thiopental Metohexital Etomidate
Supporting Information
 Notes Bull. Korean Chem. Soc. 2013, Vol. 34, No. 1 1 http://dx.doi.org/10.5012/bkcs.2013.34.1.xxx Supporting Information Chemical Constituents of Ficus drupacea Leaves and their α-glucosidase Inhibitory
Notes Bull. Korean Chem. Soc. 2013, Vol. 34, No. 1 1 http://dx.doi.org/10.5012/bkcs.2013.34.1.xxx Supporting Information Chemical Constituents of Ficus drupacea Leaves and their α-glucosidase Inhibitory
Determination of Patulin in Apple Juice Using SPE and UHPLC-MS/MS Analysis
 Determination of Patulin in Apple Juice Using SPE and UHPLC-MS/MS Analysis UCT Part Numbers ECHLD126-P ENVIRO-CLEAN HLDVB mg/6ml SPE cartridge PE Frit SLDAID21-18UM Selectra DA UHPLC column ( 2.1 mm, 1.8
Determination of Patulin in Apple Juice Using SPE and UHPLC-MS/MS Analysis UCT Part Numbers ECHLD126-P ENVIRO-CLEAN HLDVB mg/6ml SPE cartridge PE Frit SLDAID21-18UM Selectra DA UHPLC column ( 2.1 mm, 1.8
Title Revision n date
 A. THIN LAYER CHROMATOGRAPHIC TECHNIQUE (TLC) 1. SCOPE The method describes the identification of hydrocortisone acetate, dexamethasone, betamethasone, betamethasone 17-valerate and triamcinolone acetonide
A. THIN LAYER CHROMATOGRAPHIC TECHNIQUE (TLC) 1. SCOPE The method describes the identification of hydrocortisone acetate, dexamethasone, betamethasone, betamethasone 17-valerate and triamcinolone acetonide
Supporting Information for
 Supporting Information for Tandem Mass Spectrometry Assays of Palmitoyl Protein Thioesterase and Tripeptidyl Peptidase Activity in Dried Blood Spots for the Detection of Neuronal Ceroid Lipofuscinoses
Supporting Information for Tandem Mass Spectrometry Assays of Palmitoyl Protein Thioesterase and Tripeptidyl Peptidase Activity in Dried Blood Spots for the Detection of Neuronal Ceroid Lipofuscinoses
Ultra Performance Liquid Chromatography Coupled to Orthogonal Quadrupole TOF MS(MS) for Metabolite Identification
 22 SEPARATION SCIENCE REDEFINED MAY 2005 Ultra Performance Liquid Chromatography Coupled to Orthogonal Quadrupole TOF MS(MS) for Metabolite Identification In the drug discovery process the detection and
22 SEPARATION SCIENCE REDEFINED MAY 2005 Ultra Performance Liquid Chromatography Coupled to Orthogonal Quadrupole TOF MS(MS) for Metabolite Identification In the drug discovery process the detection and
Amphetamines, Phentermine, and Designer Stimulant Quantitation Using an Agilent 6430 LC/MS/MS
 Amphetamines, Phentermine, and Designer Stimulant Quantitation Using an Agilent 643 LC/MS/MS Application Note Forensics Authors Jason Hudson, Ph.D., James Hutchings, Ph.D., and Rebecca Wagner, Ph.D. Virginia
Amphetamines, Phentermine, and Designer Stimulant Quantitation Using an Agilent 643 LC/MS/MS Application Note Forensics Authors Jason Hudson, Ph.D., James Hutchings, Ph.D., and Rebecca Wagner, Ph.D. Virginia
DIRECT EXTRACTION OF BENZODIAZEPINE METABOLITE WITH SUPERCRITICAL FLUID FROM WHOLE BLOOD
 DIRECT EXTRACTION OF BENZODIAZEPINE METABOLITE WITH SUPERCRITICAL FLUID FROM WHOLE BLOOD Kenichi TAKAICHI, Shuji SAITOH, Yoshio KUMOOKA, Noriko TSUNODA National Research Institute of Police Science, Chiba,
DIRECT EXTRACTION OF BENZODIAZEPINE METABOLITE WITH SUPERCRITICAL FLUID FROM WHOLE BLOOD Kenichi TAKAICHI, Shuji SAITOH, Yoshio KUMOOKA, Noriko TSUNODA National Research Institute of Police Science, Chiba,
Improving Benzodiazepine Immunoassay Sensitivity by Rapid Glucuronide Hydrolysis Technology
 Improving Benzodiazepine Immunoassay Sensitivity by Rapid Glucuronide Hydrolysis Technology Pongkwan (Nikki) Sitasuwan, Margarita Marinova, and L. Andrew Lee Integrated Micro-Chromatography Systems, LLC
Improving Benzodiazepine Immunoassay Sensitivity by Rapid Glucuronide Hydrolysis Technology Pongkwan (Nikki) Sitasuwan, Margarita Marinova, and L. Andrew Lee Integrated Micro-Chromatography Systems, LLC
A RAPID AND SENSITIVE ANALYSIS METHOD OF SUDAN RED I, II, III & IV IN TOMATO SAUCE USING ULTRA PERFORMANCE LC MS/MS
 A RAPID AD SESITIVE AALYSIS METD OF SUDA RED I, II, III & IV I TOMATO SAUCE USIG ULTRA PERFORMACE LC MS/MS Choon Keow G, aomi TAAKA, Michelle KIM, Swee Lee YAP Waters Asia, Regional Technology Center,
A RAPID AD SESITIVE AALYSIS METD OF SUDA RED I, II, III & IV I TOMATO SAUCE USIG ULTRA PERFORMACE LC MS/MS Choon Keow G, aomi TAAKA, Michelle KIM, Swee Lee YAP Waters Asia, Regional Technology Center,
Synthetic chemistry-led creation of a difluorinated biaryl ether non-nucleoside reverse transcriptase inhibitor
 upplementary Material for rganic & Biomolecular Chemistry ynthetic chemistry-led creation of a difluorinated biaryl ether non-nucleoside reverse transcriptase inhibitor Lyn. Jones* Amy Randall, scar Barba
upplementary Material for rganic & Biomolecular Chemistry ynthetic chemistry-led creation of a difluorinated biaryl ether non-nucleoside reverse transcriptase inhibitor Lyn. Jones* Amy Randall, scar Barba
Designer Cannabinoids
 Liquid Chromatography Mass Spectrometry SSI-LCMS-010 Designer Cannabinoids LCMS-8030 Summary A rapid LC-MS-MS method for determination of designer cannabinoids in smokeable herbs was developed. Background
Liquid Chromatography Mass Spectrometry SSI-LCMS-010 Designer Cannabinoids LCMS-8030 Summary A rapid LC-MS-MS method for determination of designer cannabinoids in smokeable herbs was developed. Background
Fig.S1 ESI-MS spectrum of reaction of ApA and THPTb after 16 h.
 Electronic Supplementary Material (ESI) for RSC Advances. This journal is The Royal Society of Chemistry 2014 Experiment Cleavage of dinucleotides Dinucleotides (ApA, CpC, GpG, UpU) were purchased from
Electronic Supplementary Material (ESI) for RSC Advances. This journal is The Royal Society of Chemistry 2014 Experiment Cleavage of dinucleotides Dinucleotides (ApA, CpC, GpG, UpU) were purchased from
Thiol-Activated gem-dithiols: A New Class of Controllable. Hydrogen Sulfide (H 2 S) Donors
 Thiol-Activated gem-dithiols: A New Class of Controllable Hydrogen Sulfide (H 2 S) Donors Yu Zhao, Jianming Kang, Chung-Min Park, Powell E. Bagdon, Bo Peng, and Ming Xian * Department of Chemistry, Washington
Thiol-Activated gem-dithiols: A New Class of Controllable Hydrogen Sulfide (H 2 S) Donors Yu Zhao, Jianming Kang, Chung-Min Park, Powell E. Bagdon, Bo Peng, and Ming Xian * Department of Chemistry, Washington
Phospholipid characterization by a TQ-MS data based identification scheme
 P-CN1716E Phospholipid characterization by a TQ-MS data based identification scheme ASMS 2017 MP-406 Tsuyoshi Nakanishi 1, Masaki Yamada 1, Ningombam Sanjib Meitei 2, 3 1 Shimadzu Corporation, Kyoto, Japan,
P-CN1716E Phospholipid characterization by a TQ-MS data based identification scheme ASMS 2017 MP-406 Tsuyoshi Nakanishi 1, Masaki Yamada 1, Ningombam Sanjib Meitei 2, 3 1 Shimadzu Corporation, Kyoto, Japan,
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen This full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/14779
PDF hosted at the Radboud Repository of the Radboud University Nijmegen This full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/14779
Small Scale Preparative Isolation of Corticosteroid Degradation Products Using Mass-Based Fraction Collection Application
 Small Scale Preparative Isolation of Corticosteroid Degradation Products Using Mass-Based Fraction Collection Application Pharmaceutical Author Cliff Woodward Agilent Technologies, Inc. 285 Centerville
Small Scale Preparative Isolation of Corticosteroid Degradation Products Using Mass-Based Fraction Collection Application Pharmaceutical Author Cliff Woodward Agilent Technologies, Inc. 285 Centerville
Jose Castro-Perez, Henry Shion, Kate Yu, John Shockcor, Emma Marsden-Edwards, Jeff Goshawk Waters Corporation, Milford, MA, U.S. and Manchester, UK
 HIGH-THRUGHPUT REACTIVE METABLITE SCREEIG FR DICLFEAC BY UPLC AD XEV TQ MS WITH SCAWAVE Jose Castro-Perez, Henry Shion, Kate Yu, John Shockcor, Emma Marsden-Edwards, Jeff Goshawk Waters Corporation, Milford,
HIGH-THRUGHPUT REACTIVE METABLITE SCREEIG FR DICLFEAC BY UPLC AD XEV TQ MS WITH SCAWAVE Jose Castro-Perez, Henry Shion, Kate Yu, John Shockcor, Emma Marsden-Edwards, Jeff Goshawk Waters Corporation, Milford,
Measuring Phytosterols in Health Supplements by LC/MS. Marcus Miller and William Schnute Thermo Fisher Scientific, San Jose, CA, USA
 Measuring Phytosterols in Health Supplements by LC/MS Marcus Miller and William Schnute Thermo Fisher Scientific, San Jose, CA, USA Overview Purpose: Develop a method for the extraction of phytosterols
Measuring Phytosterols in Health Supplements by LC/MS Marcus Miller and William Schnute Thermo Fisher Scientific, San Jose, CA, USA Overview Purpose: Develop a method for the extraction of phytosterols
Efficient and green, microwave assisted synthesis of haloalkylphosphonates via Michaelis-Arbuzov reaction
 ELECTRONIC SUPPORTING INFORMATION Efficient and green, microwave assisted synthesis of haloalkylphosphonates via Michaelis-Arbuzov reaction Petr Jansa, Antonín Holý, Martin Dračinský, Ondřej Baszczyňski,
ELECTRONIC SUPPORTING INFORMATION Efficient and green, microwave assisted synthesis of haloalkylphosphonates via Michaelis-Arbuzov reaction Petr Jansa, Antonín Holý, Martin Dračinský, Ondřej Baszczyňski,
Vitamin D Metabolite Analysis in Biological Samples Using Agilent Captiva EMR Lipid
 Vitamin D Metabolite Analysis in Biological Samples Using Agilent Captiva EMR Lipid Application Note Clinical Research Authors Derick Lucas and Limian Zhao Agilent Technologies, Inc. Abstract Lipids from
Vitamin D Metabolite Analysis in Biological Samples Using Agilent Captiva EMR Lipid Application Note Clinical Research Authors Derick Lucas and Limian Zhao Agilent Technologies, Inc. Abstract Lipids from
Electronic Supplementary Information
 Electronic Supplementary Information A Novel and Facile Zn-mediated Intramolecular Five-membered Cyclization of β-tetraarylporphyrin Radicals from β-bromotetraarylporphyrins Dong-Mei Shen, Chao Liu, Qing-Yun
Electronic Supplementary Information A Novel and Facile Zn-mediated Intramolecular Five-membered Cyclization of β-tetraarylporphyrin Radicals from β-bromotetraarylporphyrins Dong-Mei Shen, Chao Liu, Qing-Yun
Lewis acid-catalyzed regioselective synthesis of chiral α-fluoroalkyl amines via asymmetric addition of silyl dienolates to fluorinated sulfinylimines
 Supporting Information for Lewis acid-catalyzed regioselective synthesis of chiral α-fluoroalkyl amines via asymmetric addition of silyl dienolates to fluorinated sulfinylimines Yingle Liu a, Jiawang Liu
Supporting Information for Lewis acid-catalyzed regioselective synthesis of chiral α-fluoroalkyl amines via asymmetric addition of silyl dienolates to fluorinated sulfinylimines Yingle Liu a, Jiawang Liu
Core E Analysis of Neutral Lipids from Human Plasma June 4, 2010 Thomas J. Leiker and Robert M. Barkley
 Core E Analysis of Neutral Lipids from Human Plasma June 4, 2010 Thomas J. Leiker and Robert M. Barkley This protocol describes the extraction and direct measurement of cholesterol esters (CEs) and triacylglycerols
Core E Analysis of Neutral Lipids from Human Plasma June 4, 2010 Thomas J. Leiker and Robert M. Barkley This protocol describes the extraction and direct measurement of cholesterol esters (CEs) and triacylglycerols
Triptycene-Based Small Molecules Modulate (CAG) (CTG) Repeat Junctions
 Electronic Supplementary Material (ESI) for Chemical Science. This journal is The Royal Society of Chemistry 2015 Triptycene-Based Small Molecules Modulate (CAG) (CTG) Repeat Junctions Stephanie A. Barros
Electronic Supplementary Material (ESI) for Chemical Science. This journal is The Royal Society of Chemistry 2015 Triptycene-Based Small Molecules Modulate (CAG) (CTG) Repeat Junctions Stephanie A. Barros
Pharmacology of intravenous induction agents. Frederique S Servin APHP - Hôpital Bichat Paris FRANCE
 Pharmacology of intravenous induction agents Frederique S Servin APHP - Hôpital Bichat Paris FRANCE Intravenous induction agents currently available thiopental propofol etomidate midazolam ketamine Common
Pharmacology of intravenous induction agents Frederique S Servin APHP - Hôpital Bichat Paris FRANCE Intravenous induction agents currently available thiopental propofol etomidate midazolam ketamine Common
Comprehensive Study of SLE as a Sample. Preparation Tool for Bioanalysis
 Comprehensive Study of SLE as a Sample Preparation Tool for Bioanalysis Wan Wang, Warren Chen, Jerry Wang Bonna-Agela Technologies 179 Southern Street, West TEDA, Tianjin, China Abstract A simple, fast,
Comprehensive Study of SLE as a Sample Preparation Tool for Bioanalysis Wan Wang, Warren Chen, Jerry Wang Bonna-Agela Technologies 179 Southern Street, West TEDA, Tianjin, China Abstract A simple, fast,
SUPPLEMENTAL FIGURE 1 Structures and IC50 values of compounds 13 32
 SUPPLEMETAL FIGURE 1 Structures and IC50 values of compounds 13 32 THE JURAL F UCLEAR MEDICIE Vol. 53 o. 11 ovember 2012 Synthesis of [ 19 F]1 ([ 19 F]--(2-{4-[5-(benzyloxy)pyridin-2-yl]piperazin-1-yl}-2-oxoethyl)-
SUPPLEMETAL FIGURE 1 Structures and IC50 values of compounds 13 32 THE JURAL F UCLEAR MEDICIE Vol. 53 o. 11 ovember 2012 Synthesis of [ 19 F]1 ([ 19 F]--(2-{4-[5-(benzyloxy)pyridin-2-yl]piperazin-1-yl}-2-oxoethyl)-
Supporting Information. First synthetic entry to the trimer stage of 5,6-dihydroxyindole polymerization: orthoalkynylaniline-based
 Supporting Information First synthetic entry to the trimer stage of 5,6-dihydroxyindole polymerization: orthoalkynylaniline-based access to the missing 2,7 :2,7 -triindole Luigia Capelli, Paola Manini,*
Supporting Information First synthetic entry to the trimer stage of 5,6-dihydroxyindole polymerization: orthoalkynylaniline-based access to the missing 2,7 :2,7 -triindole Luigia Capelli, Paola Manini,*
UPLC/MS Monitoring of Water-Soluble Vitamin Bs in Cell Culture Media in Minutes
 UPLC/MS Monitoring of Water-Soluble Vitamin Bs in Cell Culture Media in Minutes Catalin E. Doneanu, Weibin Chen, and Jeffrey R. Mazzeo Waters Corporation, Milford, MA, U.S. A P P L I C AT ION B E N E F
UPLC/MS Monitoring of Water-Soluble Vitamin Bs in Cell Culture Media in Minutes Catalin E. Doneanu, Weibin Chen, and Jeffrey R. Mazzeo Waters Corporation, Milford, MA, U.S. A P P L I C AT ION B E N E F
Enantioselective synthesis of anti- and syn-β-hydroxy-α-phenyl carboxylates via boron-mediated asymmetric aldol reaction
 Enantioselective synthesis of anti- and syn-β-hydroxy-α-phenyl carboxylates via boron-mediated asymmetric aldol reaction P. Veeraraghavan Ramachandran* and Prem B. Chanda Department of Chemistry, Purdue
Enantioselective synthesis of anti- and syn-β-hydroxy-α-phenyl carboxylates via boron-mediated asymmetric aldol reaction P. Veeraraghavan Ramachandran* and Prem B. Chanda Department of Chemistry, Purdue
Supplementary Information
 Hyperpolarization-activated cation channels inhibit EPSPs by interactions with M-type K + channels Meena S. George, L.F. Abbott, Steven A. Siegelbaum Supplementary Information Part 1: Supplementary Figures
Hyperpolarization-activated cation channels inhibit EPSPs by interactions with M-type K + channels Meena S. George, L.F. Abbott, Steven A. Siegelbaum Supplementary Information Part 1: Supplementary Figures
Isolation of five carotenoid compounds from tangerine tomatoes
 Isolation of five carotenoid compounds from tangerine tomatoes Thesis Thomas Haufe Advisor: Steven J. Schwartz, Ph.D Department of Food Science and Technology Presented in fulfillment of the requirements
Isolation of five carotenoid compounds from tangerine tomatoes Thesis Thomas Haufe Advisor: Steven J. Schwartz, Ph.D Department of Food Science and Technology Presented in fulfillment of the requirements
MS/MS as an LC Detector for the Screening of Drugs and Their Metabolites in Race Horse Urine
 Application Note: 346 MS/MS as an LC Detector for the Screening of Drugs and Their Metabolites in Race Horse Urine Gargi Choudhary and Diane Cho, Thermo Fisher Scientific, San Jose, CA Wayne Skinner and
Application Note: 346 MS/MS as an LC Detector for the Screening of Drugs and Their Metabolites in Race Horse Urine Gargi Choudhary and Diane Cho, Thermo Fisher Scientific, San Jose, CA Wayne Skinner and
Analysis of Testosterone, Androstenedione, and Dehydroepiandrosterone Sulfate in Serum for Clinical Research
 Analysis of Testosterone, Androstenedione, and Dehydroepiandrosterone Sulfate in Serum for Clinical Research Dominic Foley, Michelle Wills, and Lisa Calton Waters Corporation, Wilmslow, UK APPLICATION
Analysis of Testosterone, Androstenedione, and Dehydroepiandrosterone Sulfate in Serum for Clinical Research Dominic Foley, Michelle Wills, and Lisa Calton Waters Corporation, Wilmslow, UK APPLICATION
Supporting Information. for. Pd-catalyzed decarboxylative Heck vinylation of. 2-nitro-benzoates in the presence of CuF 2
 Supporting Information for Pd-catalyzed decarboxylative Heck vinylation of 2-nitro-benzoates in the presence of CuF 2 Lukas J. Gooßen*, Bettina Zimmermann, Thomas Knauber Address: Department of Chemistry,
Supporting Information for Pd-catalyzed decarboxylative Heck vinylation of 2-nitro-benzoates in the presence of CuF 2 Lukas J. Gooßen*, Bettina Zimmermann, Thomas Knauber Address: Department of Chemistry,
Determination of Amantadine Residues in Chicken by LCMS-8040
 Liquid Chromatography Mass Spectrometry Determination of Amantadine Residues in Chicken by LCMS-8040 A method for the determination of amantadine in chicken was established using Shimadzu Triple Quadrupole
Liquid Chromatography Mass Spectrometry Determination of Amantadine Residues in Chicken by LCMS-8040 A method for the determination of amantadine in chicken was established using Shimadzu Triple Quadrupole
Supporting Information File S2
 Pulli et al. Measuring Myeloperoxidase Activity in Biological Samples Page 1 of 6 Supporting Information File S2 Step-by-Step Protocol Reagents: Sucrose (Sigma, S3089) CaCl 2 (Sigma, C5770) Heparin Sodium
Pulli et al. Measuring Myeloperoxidase Activity in Biological Samples Page 1 of 6 Supporting Information File S2 Step-by-Step Protocol Reagents: Sucrose (Sigma, S3089) CaCl 2 (Sigma, C5770) Heparin Sodium
A pillar[2]arene[3]hydroquinone which can self-assemble to a molecular zipper in the solid state
![A pillar[2]arene[3]hydroquinone which can self-assemble to a molecular zipper in the solid state A pillar[2]arene[3]hydroquinone which can self-assemble to a molecular zipper in the solid state](/thumbs/86/93673402.jpg) A pillar[2]arene[3]hydroquinone which can self-assemble to a molecular zipper in the solid state Mingguang Pan, Min Xue* Department of Chemistry, Zhejiang University, Hangzhou 310027, P. R. China Fax:
A pillar[2]arene[3]hydroquinone which can self-assemble to a molecular zipper in the solid state Mingguang Pan, Min Xue* Department of Chemistry, Zhejiang University, Hangzhou 310027, P. R. China Fax:
Sulfate Radical-Mediated Degradation of Sulfadiazine by CuFeO 2 Rhombohedral Crystal-Catalyzed Peroxymonosulfate: Synergistic Effects and Mechanisms
 Supporting Information for Sulfate Radical-Mediated Degradation of Sulfadiazine by CuFeO 2 Rhombohedral Crystal-Catalyzed Peroxymonosulfate: Synergistic Effects and Mechanisms Submitted by Yong Feng, Deli
Supporting Information for Sulfate Radical-Mediated Degradation of Sulfadiazine by CuFeO 2 Rhombohedral Crystal-Catalyzed Peroxymonosulfate: Synergistic Effects and Mechanisms Submitted by Yong Feng, Deli
Supporting Information
 Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2018 Supporting Information Facile Three-Step Synthesis and Photophysical Properties of [8]-, [9]-,
Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2018 Supporting Information Facile Three-Step Synthesis and Photophysical Properties of [8]-, [9]-,
THIN LAYER CHROMATOGRAPHY
 THIN LAYER CHROMATOGRAPHY Thin layer chromatography is the best known technique of plant biochemistry. TLC is used for preliminary separation and determination of plant constituents. It is helpful for
THIN LAYER CHROMATOGRAPHY Thin layer chromatography is the best known technique of plant biochemistry. TLC is used for preliminary separation and determination of plant constituents. It is helpful for
Reduced Ion Suppression and Improved LC/MS Sensitivity with Agilent Bond Elut Plexa
 Reduced Ion Suppression and Improved LC/MS Sensitivity with Agilent Bond Elut Plexa Application Note Small Molecule Pharmaceuticals & Generics Author Mike Chang Agilent Technologies, Inc. 5 Commercentre
Reduced Ion Suppression and Improved LC/MS Sensitivity with Agilent Bond Elut Plexa Application Note Small Molecule Pharmaceuticals & Generics Author Mike Chang Agilent Technologies, Inc. 5 Commercentre
TENOFOVIR TABLETS: Final text for addition to The International Pharmacopoeia (June 2010)
 June 2010 TENOFOVIR TABLETS: Final text for addition to The International Pharmacopoeia (June 2010) This monograph was adopted at the Forty-fourth WHO Expert Committee on Specifications for Pharmaceutical
June 2010 TENOFOVIR TABLETS: Final text for addition to The International Pharmacopoeia (June 2010) This monograph was adopted at the Forty-fourth WHO Expert Committee on Specifications for Pharmaceutical
PosterREPRINT EVALUATION OF A RF-ONLY STACKED RING BASED COLLISION CELL WITH AXIAL FIELD FOR THE LC-MS-MS ANALYSIS OF THE METABOLITES OF RABEPRAZOLE
 OVERVIEW Comparison of the performance of a stacked ring based collision cell with axial field and a hexapole collision cell. Full scan LC-MS/MS-MS using precursor, product and neutral loss modes of operation
OVERVIEW Comparison of the performance of a stacked ring based collision cell with axial field and a hexapole collision cell. Full scan LC-MS/MS-MS using precursor, product and neutral loss modes of operation
Electronic Supplementary Information
 Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2015 Electronic Supplementary Information ovel pseudo[2]rotaxanes constructed by selfassembly of dibenzyl
Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2015 Electronic Supplementary Information ovel pseudo[2]rotaxanes constructed by selfassembly of dibenzyl
Analysis of Acrylamide in French Fries using Agilent Bond Elut QuEChERS AOAC kit and LC/MS/MS
 Analysis of Acrylamide in French Fries using Agilent Bond Elut QuEChERS AOAC kit and LC/MS/MS Food Application Author Fadwa Al-Taher Institute for Food Safety and Health Illinois Institute of Technology
Analysis of Acrylamide in French Fries using Agilent Bond Elut QuEChERS AOAC kit and LC/MS/MS Food Application Author Fadwa Al-Taher Institute for Food Safety and Health Illinois Institute of Technology
nachr α 4 β 2 CHO Cell Line
 B SYS GmbH nachr α 4 β 2 CHO Cell Line Cell Culture Conditions B SYS GmbH B SYS GmbH nachr α 4 β 2 CHO Page 2 TABLE OF CONTENTS 1 BACKGROUND...3 1.1 Human Nicotinic Acetylcholine Receptors...3 1.2 B SYS
B SYS GmbH nachr α 4 β 2 CHO Cell Line Cell Culture Conditions B SYS GmbH B SYS GmbH nachr α 4 β 2 CHO Page 2 TABLE OF CONTENTS 1 BACKGROUND...3 1.1 Human Nicotinic Acetylcholine Receptors...3 1.2 B SYS
Determination of Bath Salts (Pyrovalerone Analogs) in Biological Samples
 Determination of Bath Salts (Pyrovalerone Analogs) in Biological Samples Application Note Forensic Toxicology Authors Joe Crifasi Saint Louis University Forensic Toxicology Laboratory Saint Louis, Mo.
Determination of Bath Salts (Pyrovalerone Analogs) in Biological Samples Application Note Forensic Toxicology Authors Joe Crifasi Saint Louis University Forensic Toxicology Laboratory Saint Louis, Mo.
RITONAVIRI COMPRESSI RITONAVIR TABLETS. Final text for addition to The International Pharmacopoeia (July 2012)
 July 2012 RITONAVIRI COMPRESSI RITONAVIR TABLETS Final text for addition to The International Pharmacopoeia (July 2012) This monograph was adopted at the Forty-sixth WHO Expert Committee on Specifications
July 2012 RITONAVIRI COMPRESSI RITONAVIR TABLETS Final text for addition to The International Pharmacopoeia (July 2012) This monograph was adopted at the Forty-sixth WHO Expert Committee on Specifications
Detection of Cotinine and 3- hydroxycotine in Smokers Urine
 Detection of Cotinine and 3- hydroxycotine in Smokers Urine Behavioural and Situational Research Group School of Medicine, University of Tasmania Version number: 2 Effective date: 01/12/2015 Review due:
Detection of Cotinine and 3- hydroxycotine in Smokers Urine Behavioural and Situational Research Group School of Medicine, University of Tasmania Version number: 2 Effective date: 01/12/2015 Review due:
Application Note. Abstract. Authors. Pharmaceutical
 Analysis of xycodone and Its Metabolites-oroxycodone, xymorphone, and oroxymorphone in Plasma by LC/MS with an Agilent ZRBAX StableBond SB-C18 LC Column Application ote Pharmaceutical Authors Linda L.
Analysis of xycodone and Its Metabolites-oroxycodone, xymorphone, and oroxymorphone in Plasma by LC/MS with an Agilent ZRBAX StableBond SB-C18 LC Column Application ote Pharmaceutical Authors Linda L.
LC-MS/MS quantitative analysis of Polyunsaturated Omega 3, 6,7 and 9 Fatty Acids in Serum for
 POSTER NOTE 64921 LC-MS/MS quantitative analysis of Polyunsaturated Omega 3, 6,7 and 9 Fatty Acids in Serum for Research Use LC-MS/MS quantitative analysis of Poly Rory M Doyle*, Thermo Scientific, Inc,
POSTER NOTE 64921 LC-MS/MS quantitative analysis of Polyunsaturated Omega 3, 6,7 and 9 Fatty Acids in Serum for Research Use LC-MS/MS quantitative analysis of Poly Rory M Doyle*, Thermo Scientific, Inc,
Supporting Information. Efficient copper-catalyzed Michael addition of acrylic derivatives with primary alcohols in the presence of base
 Supporting Information Efficient copper-catalyzed Michael addition of acrylic derivatives with primary alcohols in the presence of base Feng Wang, a Haijun Yang, b Hua Fu, b,c * and Zhichao Pei a * a College
Supporting Information Efficient copper-catalyzed Michael addition of acrylic derivatives with primary alcohols in the presence of base Feng Wang, a Haijun Yang, b Hua Fu, b,c * and Zhichao Pei a * a College
PTM Discovery Method for Automated Identification and Sequencing of Phosphopeptides Using the Q TRAP LC/MS/MS System
 Application Note LC/MS PTM Discovery Method for Automated Identification and Sequencing of Phosphopeptides Using the Q TRAP LC/MS/MS System Purpose This application note describes an automated workflow
Application Note LC/MS PTM Discovery Method for Automated Identification and Sequencing of Phosphopeptides Using the Q TRAP LC/MS/MS System Purpose This application note describes an automated workflow
Facile Isolation of Carotenoid Antioxidants from Solanum lycopersicum using Flash Chromatography
 Facile Isolation of Carotenoid Antioxidants from Solanum lycopersicum using Flash Chromatography Jack E. Silver, jsilver@teledyne.com, Paul Bellinghausen, Nancy Fowler, and Ruth Pipes, Teledyne Isco, Inc.,
Facile Isolation of Carotenoid Antioxidants from Solanum lycopersicum using Flash Chromatography Jack E. Silver, jsilver@teledyne.com, Paul Bellinghausen, Nancy Fowler, and Ruth Pipes, Teledyne Isco, Inc.,
