Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting
|
|
|
- Ronald Jackson
- 6 years ago
- Views:
Transcription
1 Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 REVIEW Open Access Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting Marcel Cerqueira Cesar Machado 1,2* and Fabiano Pinheiro da Silva 1,2 Abstract Disorders of the urea cycle are secondary to a defect in the system that converts ammonia into urea, resulting in accumulation of ammonia and other products. This results in encephalopathy, coma, and death if not recognized and treated rapidly. Late-onset urea cycle disorders may be precipitated by acute disease and can be difficult to recognize because patients are already ill. Diagnosis of urea cycle disorders is based on clinical suspicion and determination of blood ammonia in suspected patients with neurological symptoms in the intensive care setting. Treatment is based on the removal of ammonia by dialysis or hemofiltration, reduction of the catabolic state, abolishment of nitrogen administration, and use of pharmacological nitrogen scavenging agents. Keywords: Hyperammonemia, Neurological disorders, Intensive care unit Introduction Recently, we reported a case of a 49-year-old man with biliary acute pancreatitis who developed high fever and a large pancreatic abscess. Upon admission, this patient underwent necrosectomy, cholecystectomy, and abscess drainage in a single surgical setting. Parenteral nutrition was initiated, but on the 8th day, the patient developed progressive lethargy, confusion, and coma, requiring intubation. Computed tomography and magnetic resonance imaging showed no brain lesions. Laboratory tests indicated normal liver function, with enzyme levels and serum bilirubin within the normal range. The etiology of the encephalopathy was not suspected until hyperammonemia (137 μ/l) was observed. Lactulose treatment produced no improvement in clinical signs, and the patient remained in a deep coma, with ammonia levels elevated up to 254 μ/l. Because there was no evidence of liver disease, hyperammonemia must have been caused by a metabolism disorder. To deal with these types of cases, physicians need to understand the principles of the * Correspondence: mccm37@uol.com.br 1 Emergency Medicine Department, University of Sao Paulo, Sao Paulo , Brazil 2 Faculdade de Medicina, USP, Av Dr Arnaldo 455 Room 3189 LIM 51, Sao Paulo , Brazil pathophysiology of ammonia metabolism and how to treat these patients in the intensive care setting. Review Ammonia metabolism The urea cycle is the only effective system that converts waste nitrogen from protein intake and the breakdown of endogenous protein (catabolism) into urea, which is excreted from the body. This system consists of five consecutive enzymatic reactions that convert one molecule of nitrogen from ammonia, two molecules of nitrogen from ornithine, and one molecule from aspartate to urea in each cycle (Figure 1). There is also a cofactor-producing enzyme (N-acetyl glutamate synthetase) and two transporters (ornithine transporter-1 and citrin) that are involved in the urea cycle. Disorders of the urea cycle are the result of total or partial in any of the factors mentioned (Figure 1). This leads to defects in the metabolism of waste products from breakdown of protein and other nitrogen-containing substances, with accumulation of ammonia and other products [1,2]. The most common presentation of these defects is in newborns who typically present with somnolence, poor feeding, hyperventilation, and seizures, followed by lethargy and coma [3]. However, there are several reports concerning urea cycle disorders (UCDs) that manifest in 2014 Machado and Pinheiro da Silva; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited.
2 Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 Page 2 of 5 HCO 3 + NH ATP CPSI N-acetylglutamate Carbamyl Phosphate Aspartate OTC Citruline ASS Argininosuccinate Ornithine ASL Urea ARG Arginine Fumarate Figure 1 The urea cycle. CPS-1 cabamoyl phosphate synthetase 1, OTC ornithine transcarbamylase, ASS argininosuccinic acid synthetase, ASL argininosuccinic acid lyase, ARG arginase. adulthood, mainly in the presence of an acute injury [2]. In most cases in the intensive care setting, underlying UCDs are difficult to recognize because patients are in a critical condition for other reasons. There is also an insufficient awareness of medical staff because of the rarity of this disease and because the plasma ammonia levels are not routinely determined. Prompt diagnosis and treatment of this disorder are required to avoid death or severe neurological damage. In the last few decades, there has been a dramatic improvement in the recognition and treatment of UCDs [3-7]. In partial of urea cycle enzymes, symptoms may develop late in life. These symptoms are frequently triggered by acute stress or illness, such as sepsis, surgery, trauma, or drugs (e.g., valproic acid), because of their effect on the function of the enzyme carbamoyl phosphate synthetase-1 (CPS-1) [2] especially in patients on parenteral nutrition [8]. In these situations, elevation of blood ammonia and symptoms may be subtle or occur acutely only during metabolic decompensation related to catabolic stress, such as in surgery, sepsis, or hemodynamic alterations. Recognition and treatment are crucial to improve the outcome of UCDs. Ammonemia may be normal when an individual is healthy. We present here a review of the clinical features, diagnosis, and treatment of these disorders in late-onset diseases related to partial enzyme decompensated by acute stress. Partial UCDs or late-onset UCDs Patients with partial of any enzyme in the urea cycle may develop symptoms at any time of life, usually as a result of increased catabolic stress [9,10]. Partial enzyme allows a patient to have a normal life for decades before there is increased production of ammonia or interference with any enzyme of the urea cycle. In patients with partial urea cycle enzyme, symptoms may be delayed for months or years and vary with the specific enzyme. In most hyperammonemic episodes, patients may present with a loss of appetite, vomiting, lethargy, and behavior abnormalities associated with hallucinations, sleep disorders, ataxia, and even seizures. These episodes are usually related to periods of high protein intake, systemic infection, or catabolic stress. In the intensive care unit, patients with acute neurological and psychiatric symptoms or coma should have plasma ammonia levels measured to disclose a possible late-onset UCDs if there is any suspicion. Prompt diagnosis of UCDs is essential for treatment to be effective; otherwise, the prognosis of these patients is poor. UCDs are usually difficult to recognize because many of these patients are frequently ill for other reasons, such as sepsis, acute pancreatitis, trauma, or other acute diseases. Plasma ammonia determination is carried out in venous or arterial blood collected in chilled tubes with ammonia-free sodium heparin or EDTA tubes placed on ice. These are immediately sent to the laboratory because hemolysis, an increase in temperature, and delays in processing may falsely increase plasma ammonia levels (normal levels less than 30 μ/l). An elevated plasma ammonia level is associated with normal blood glucose levels. A normal anion gap suggests UCDs because hyperammonemia associated with hyperglycemia and an abnormal anion gap are found in organic acidemias (a different inborn error of metabolism). Plasma and urine must be frozen for future diagnostic tests to identify the specific enzyme. The following
3 Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 Page 3 of 5 are the conditions that may induce hyperammonemia in partial UCDs: 1. Postpartum stress 2. Parenteral nutrition with high protein administration 3. Gastrointestinal bleeding 4. Administration of valproic acid 5. Infection and postoperative stress Neurological disorders in UCDs Hyperammonemia may damage the brain by a variety of mechanisms. The most important mechanism is brain edema, probably induced by disruption of the aquaporin system (membrane water channels) and brain electrolyte homeostasis. The central feature of hyperammonemiainduced encephalopathy is an increase in astrocytes glutamine synthesis, and swelling of astrocytes in response to the osmotic effect of glutamine accumulation, resulting in increased intracranial pressure [11]. A recent study using N-ammonia positron emission tomography suggested that the magnitude of the flux of ammonia from the blood into intracellular glutamine in the brain is primarily correlated with blood ammonia concentrations [12]. In infancy, brain damage in acute hyperammonemia is similar to that seen in hypoxic-ischemic situations, with white matter disruption and lacunar infarcts. Brain damage due to hyperammonemia may result in seizures and coma [13]. Subclinical seizures are common in acute hyperammonemia and may be considered in the treatment of these conditions. In many cases, modern imaging techniques may provide information related to the extent and intensity of brain injury. However, routine neurological images may not detect brain damage [14]. Newer technologies, such as magnetic resonance spectroscopy, diffusion tensor imaging, and functional magnetic resonance may provide information about the many types of neurological damage seen in UCDs. Therapy of a rapid decrease in plasma ammonia concentrations to normal levels In patients, including the one we recently reported, with high ammonia plasma levels higher than 100 μ/l, the first option is to decrease plasma ammonia levels by using an extracorporeal therapy to achieve a rapid reduction in plasma ammonia levels. Renal replacement therapy (RRT) allows efficient removal of toxic metabolites, minimizing the duration of the metabolic disturbance. The use of RRT has changed since the studies of Donn et al. [15], concluding that hemodialysis is the preferred modality for the treatment of hyperammonemia secondary to UCDs. Currently, the choice of treatment for hyperammonemia is hemodialysis or continuous RRT, or even both modalities as early as possible [16-18]. The clearance of ammonia and other low-molecular-weight toxins is much greater with hemodialysis than with other RRTs [16,17,19]. Hemodialysis is the first-line therapy for the initial treatment of hyperammonemia in UCDs. Because ammonia is a gas, its rapid removal by hemodiafiltration is not associated with osmotic problems, and no special care must be taken to avoid dialysis disequilibrium syndrome [17,18]. Peritoneal dialysis is not effective for this purpose and should not be used. Hemodialysis may be discontinued when plasma levels fall below 80 μ/l. However, clinical evaluation is the best parameter to be used for discontinuation of dialysis. Patients with severe encephalopathy from acute hyperammonemia may completely recover unless prolonged cerebral edema results in cerebral damage [11]. In fact, in our patient, 36 h after continuous hemofiltration, ammonia levels had decreased to 82 μ/l, with improvement in the patient's mental status. The patient was weaned from the respirator and became completely awake. Rebound hyperammonemia with clinical worsening may also occur, requiring further dialysis. In our patient, discontinuation of hemofiltration was accompanied by deterioration in the patient's mental status. Any oral or parenteral protein administration must be immediately discontinued when hyperammonemia is detected. Pharmacological treatment Nitrogen scavenger therapy Sodium phenylacetate and sodium benzoate, or sodium phenylbutyrate, are available for intravenous or oral administration. The basis for use of these drugs was established by Brusilow et al. [20] in 1979, who proposed the use of alternative pathway treatment to reduce ammonia plasma levels in UCDs. Alternative pathway treatment diverts nitrogen from the urea cycle to alternative routes of excretion. Sodium phenylacetate combines with glutamine, producing phenylacetylglutamine. Phenylacetylglutamine is excreted by the kidneys and sodium benzoate conjugates with glycine, producing sodium hippurate, which is also excreted by the kidneys [21]. Replacement of deficient urea cycle intermediates Arginine administration in patients without a definitive diagnosis of the specific type of UCD is also important because ornithine transcarbamylase (OTC) is the most common type of late-onset UCDs [2,20,22]. Low plasma arginine levels observed in patients with OTC may also be related to increased vascular thrombosis [23]. To prevent future episodes of hyperammonemia, plasma ammonia should be maintained below 80 μ/l, glutamine below 1,000 μ/l, and arginine between 80 and 150 μ/l [14]. In our patient, we administered sodium benzoate (3 g) and arginine (3 g) every 4 h via a nasogastric tube, maintaining plasma ammonia levels within the normal range. Recently, it was found that glycerol phenylbutyrate,
4 Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 Page 4 of 5 which has excellent pharmacokinetics, controls plasma ammonia, improving executive function in adult and pediatric patients [24]. Reduction of protein catabolism Restriction of protein intake for a period of 24 to 48 h and administration of calories from glucose and fat are important in patients on hemodialysis or hemofiltration for the prevention of an excessive catabolic state. Maintenance of adequate plasma levels of essential amino acids is also necessary to avoid the catabolic state. Lowdose continuous infusion of insulin with glucose may be used to potentially alleviate the catabolic state. Liver transplantation Liver transplantation is considered only in patients with recurrent hyperammonemia or in those resistant to conventional medical therapy. The decision for liver transplantation is also based on the extent of brain and liver damage. Diagnosis, genetic tests, and differential diagnosis of UCDs The elevation in plasma ammonia concentrations is the main alteration in UCDs. Normal ammonia levels in adults are less than 30 μ/l. Quantitative plasma amino acid concentrations are used to determine specific enzyme in UCDs (Table 1). Plasma levels of citrulline can be used to evaluate the type of UCD and to separate proximal from distal urea cycle defects. Plasma citrulline levels are absent or present in trace amounts in CPS-1 and in low, or even normal, concentrations in late onset of OTC. Plasma citrulline levels are present in high concentrations (tenfold) in argininosuccinic acid synthetase. Moderate elevation in plasma citrulline levels is seen with argininosuccinic acid lyase, accompanied by an elevation in argininosuccinic acid in plasma and urine (Table 1). Plasma concentrations of arginine are reduced in every type of UCD, except in arginase (elevation five to sevenfold). In late onset or in partial enzyme defects, arginine concentrations may be normal. Plasma concentrations of glutamine, asparagine, and alanine are elevated in UCDs. Urine concentrations of orotic acid help to distinguish CPS-1 from OTC because they are Table 1 Analysis of plasma amino acids and urinary orotic acid CPS-1 OTC ASS-1 Citrulline Absent Low Elevated (tenfold) ASL Elevated (twofold) Arginine Reduced Reduced Reduced Reduced Orotic acid Low Elevated Elevated Elevated normal or low in CPS-1 and elevated in OTC. Urinary orotic acid concentrations are also elevated in arginase and in citrullinemia type 1 (Table 1). Diagnosis may be further refined by enzyme analysis in appropriate tissues as follows: liver biopsy (CPS-1, N-acetyl glutamate synthetase, and OTC deficiencies); red blood cells (arginase ); and fibroblasts (skin biopsy, argininosuccinic acid synthetase and argininosuccinic acid lyase deficiencies). Genetic tests There are several genetic tests available for the diagnosis of UCDs. In late-onset hyperammonemia, DNA testing for OTC should be the first test for evaluation because this is the most common type of late-onset UCD, and many mutations have been described in this condition. Recently, a more sophisticated DNA mutation analysis has been introduced, which allows identification of variants in most coding genes [25]. Differential diagnosis of UCDs Several disorders disturbing liver function may mimic UCDs. These include hepatic encephalopathy in patients with advanced liver disease, vascular bypass of the liver, valproic acid or cyclophosphamide poisoning, herpes simplex infection, and gastrointestinal bacterial overgrowth. In the last two conditions, the plasma ammonia levels are usually moderately elevated. A number of inborn errors of metabolism may also cause hyperammonemia: Tyrosinemia type 1 Galactosemia Mitochondrial disorders Fatty acid oxidation disorders Citrin leading to citrullinemia type II (CTLN2) and neonatal intrahepatic cholestasis caused by citrin (NICCD) Citrin (CTLN2) is a late-onset disorder characterized by recurrent periods of hyperammonemia, delirium, irritability, and liver fatty infiltration, but there is no hepatic dysfunction. Citrin is an aspartate glutamate transporter across the mitochondrial membrane [2]. Citrin leads to a decrease in cytoplasmic aspartate, limiting the activity of the enzyme argininosuccinic acid synthase [2]. Diagnosis of this alteration is based on findings of hyperammonemia and increased plasma concentrations of citrulline and arginine. SLC25A13 is a gene mutated in patients with citrin. Ornithine translocase is a rare disease that results in hyperornithinemia, homocitrullinuria, and hyperammonemia, similar to those in UCDs. A reduction in ornithine transport into the mitochondria results in orotic aciduria and
5 Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 Page 5 of 5 of urea synthesis. In this situation, plasma levels of ornithine are high and can be reduced by a low-protein diet. Citrin and hyperammonemia may be included in UCDs as transporter defects. Therefore, UCDs is related to eight defects, with deficiencies in six enzymes and two transporters. Conclusions Hyperammonemia in an acutely ill patient can cause irreversible neurological damage, or even death, if not recognized. Determination of plasma ammonia levels should be included in a laboratory work-up in case of acute psychiatric and neurological symptoms or unexplained coma in the intensive care unit. Competing interests The authors declare no competing interests. Authors' contributions MCCM reviewed the literature and wrote the paper. FPS contributed to the selection and review of papers, as well as to the manuscript. Both authors read and approved the final manuscript. Received: 5 June 2013 Accepted: 19 February 2014 Published: 13 March 2014 References 1. Batshaw ML, Monahan PS: Treatment of urea cycle disorders. Enzyme 1987, 38(1 4): Lanpher BC, Gropman A, Chapman KA, Lichter-Konecki U, Urea Cycle Disorders C, Summar ML: Urea cycle disorders overview. In GeneReviews. Edited by Pagon RA, Bird TD, Dolan CR, Stephens K, Adam MP. Seattle: NCBI1993. Updated September 1, Summar M: Current strategies for the management of neonatal urea cycle disorders. J Pediatric 2001, 138(Suppl 1):S30 S Enns GM, Berry SA, Berry GT, Rhead WJ, Brusilow SW, Hamosh A: Survival after treatment with phenylacetate and benzoate for urea-cycle disorders. N Engl J Med 2007, 356(22): Summar ML, Dobbelaere D, Brusilow S, Lee B: Diagnosis, symptoms, frequency and mortality of 260 patients with urea cycle disorders from a 21-year, multicentre study of acute hyperammonaemic episodes. Acta Paediatr 2008, 97(10): Klein OD, Kostiner DR, Weisiger K, Moffatt E, Lindeman N, Goodman S, Tuchman M, Packman S: Acute fatal presentation of ornithine transcarbamylase in a previously healthy male. Hepatol Int 2008, 2(3): Krivitzky L, Babikian T, Lee HS, Thomas NH, Burk-Paull KL, Batshaw ML: Intellectual, adaptive, and behavioral functioning in children with urea cycle disorders. Pediatr Res 2009, 66(1): Pillai U, Kahlon R, Sondheimer J, Cadnapaphorncai P, Bhat Z: A rare case of hyperammonemia complication of high-protein parenteral nutrition. JPEN J Parenter Enteral Nutr 2013, 37(1): Arn PH, Hauser ER, Thomas GH, Herman G, Hess D, Brusilow SW: Hyperammonemia in women with a mutation at the ornithine carbamoyltransferase locus. A cause of postpartum coma. N Engl J Med 1990, 322(23): Tuchman M, Yudkoff M: Blood levels of ammonia and nitrogen scavenging amino acids in patients with inherited hyperammonemia. Mol Genet and Metab 1999, 66(1): Brusilow SW, Koehler RC, Traystman RJ, Cooper AJ: Astrocyte glutamine synthetase: importance in hyperammonemic syndromes and potential target for therapy. Neurotherapeutics 2010, 7(4): Keiding S, Sørensen M, Bender D, Munk OL, Ott P, Vilstrup H: Brain metabolism of 13 N-ammonia during acute hepatic encephalopathy in cirrhosis measured by positron emission tomography. Hepatol 2006, 43(1): Albrecht J, Zielinska M, Norenberg MD: Glutamine as a mediator of ammonia neurotoxicity: a critical appraisal. Biochem Pharmacol 2010, 80(9): Lichter-Konecki U: Profiling of astrocyte properties in the hyperammonaemic brain: shedding new light on the pathophysiology of the brain damage in hyperammonaemia. J Inherit Metab Dis 2008, 31(4): Donn SM, Swartz RD, Thoene JG: Comparison of exchange transfusion, peritoneal dialysis, and hemodialysis for the treatment of hyperammonemia in an anuric newborn infant. J Pediatr 1979, 95(1): Wong KY, Wong SN, Lam SY, Tam S, Tsoi NS: Ammonia clearance by peritoneal dialysis and continuous arteriovenous hemodiafiltration. Pediatr Nephrol 1998, 12(7): Wiegand C, Thompson T, Bock GH, Mathis RK, Kjellstrand CM, Mauer SM: The management of life-threatening hyperammonemia: a comparison of several therapeutic modalities. J Pediatr 1980, 96(1): McBryde KD, Kershaw DB, Bunchman TE, Maxvold NJ, Mottes TA, Kudelka TL, Brophy PD: Renal replacement therapy in the treatment of confirmed or suspected inborn errors of metabolism. J Pediatr 2006, 148(6): Rutledge SL, Havens PL, Haymond MW, McLean RH, Kan JS, Brusilow SW: Neonatal hemodialysis: effective therapy for the encephalopathy of inborn errors of metabolism. J Pediatr 1990, 116(1): Brusilow SW, Valle DL, Batshaw M: New pathways of nitrogen excretion in inborn errors of urea synthesis. Lancet 1979, 2(8140): Maillot F, Crenn P: [Urea cycle disorders in adult patients]. Revue neurologique 2007, 163(10): Wilcken B: Problems in the management of urea cycle disorders. Mol Genet Metab 2004, 81(Suppl 1):S86 S Venkateswaran L, Scaglia F, McLin V, Hertel P, Shchelochkov OA, Karpen S, Mahoney D Jr: Ornithine transcarbamylase : a possible risk factor for thrombosis. Pediatr Blood Cancer 2009, 53(1): Diaz GA, Krivitzky LS, Mokhtarani M, Rhead W, Bartley J, Feigenbaum A, Longo N, Berquist W, Berry SA, Gallagher R, Lichter-Konecki U, Bartholomew D, Harding CO, Cederbaum S, McCandless SE, Smith W, Vockley G, Bart SA, Korson MS, Kronn D, Zori R, Merritt JL 2nd, C S Nagamani S, Mauney J, Lemons C, Dickinson K, Moors TL, Coakley DF, Scharschmidt BF, Lee B: Ammonia control and neurocognitive outcome among urea cycle disorder patients treated with glycerol phenylbutyrate. Hepatol 2012: Bamshad MJ, Ng SB, Bigham AW, Tabor HK, Emond MJ, Nickerson DA, Shendure J: Exome sequencing as a tool for Mendelian disease gene discovery. Nat Rev Genet 2011, 12(11): doi: / Cite this article as: Machado and Pinheiro da Silva: Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting. Journal of Intensive Care :22. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UPDATE ON UREA CYCLE DISORDERS TREATMENT
 UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Disorders Prior Authorization Program Summary
 Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
TRANSAMINATION AND UREA CYCLE
 TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment
 Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment June 2013 DISCLAIMER: This document was originally drafted in French by the Institut national d'excellence en santé et en services sociaux
Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment June 2013 DISCLAIMER: This document was originally drafted in French by the Institut national d'excellence en santé et en services sociaux
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
Jana Novotná, Bruno Sopko. Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ.
 Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable
 Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
Proceedings of a Consensus Conference for the
 Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency)
 Received: 14 June 2017 Accepted: 20 June 2017 DOI: 10.1111/jcpt.12593 CASE REPORT First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency) E. Kose
Received: 14 June 2017 Accepted: 20 June 2017 DOI: 10.1111/jcpt.12593 CASE REPORT First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency) E. Kose
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease
 Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders Gregory M. Enns, M.B., Ch.B., Susan A. Berry, M.D.,
T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders Gregory M. Enns, M.B., Ch.B., Susan A. Berry, M.D.,
Senior Vice President, Medical Affairs and Health Outcomes, 150 South Saunders Road, Lake Forest, IL 60045, Horizon Pharma USA, Inc, USA
 Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Urea is the major end product of nitrogen catabolism in humans One nitrogen free NH3 other nitrogen aspartate. carbon oxygen CO2 liver,
 Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual cause of seizures: a case report and review of the literature
 Wang et al. Journal of Medical Case Reports (2018) 12:208 https://doi.org/10.1186/s13256-018-1750-8 CASE REPORT Open Access Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual
Wang et al. Journal of Medical Case Reports (2018) 12:208 https://doi.org/10.1186/s13256-018-1750-8 CASE REPORT Open Access Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual
Take a closer look at UCD management
 Take a closer look at UCD management An evaluation tool to help determine whether patients with urea cycle disorders (UCDs) may be experiencing treatment failure What is treatment failure and how do you
Take a closer look at UCD management An evaluation tool to help determine whether patients with urea cycle disorders (UCDs) may be experiencing treatment failure What is treatment failure and how do you
AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE
 AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE SOURCE & FATE OF AA The aminoacids obtained from DIETARY SOURCE or BODY PROTEIN TURNOVER are utilized for protein biosynthesis and the production of
AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE SOURCE & FATE OF AA The aminoacids obtained from DIETARY SOURCE or BODY PROTEIN TURNOVER are utilized for protein biosynthesis and the production of
Ammonia Control and Neurocognitive Outcome Among Urea Cycle Disorder Patients Treated With Glycerol Phenylbutyrate
 STEATOHEPATITIS/METABOLIC LIVER DISEASE Ammonia Control and Neurocognitive Outcome Among Urea Cycle Disorder Patients Treated With Glycerol Phenylbutyrate George A. Diaz, 1 Lauren S. Krivitzky, 2 Masoud
STEATOHEPATITIS/METABOLIC LIVER DISEASE Ammonia Control and Neurocognitive Outcome Among Urea Cycle Disorder Patients Treated With Glycerol Phenylbutyrate George A. Diaz, 1 Lauren S. Krivitzky, 2 Masoud
Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation
 Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Amino Acid Metabolism
 Amino Acid Metabolism The continuous degradation and synthesis of cellular proteins occur in all forms of life. Each day humans turn over 1 2% of their total body protein, principally muscle protein. Approximately
Amino Acid Metabolism The continuous degradation and synthesis of cellular proteins occur in all forms of life. Each day humans turn over 1 2% of their total body protein, principally muscle protein. Approximately
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Drug-induced Hyperammonemia (HA)
 Drug-induced hyperammonemia: are there specific therapies? NACCT Boston 2016 Florian Eyer Department of Clinical Toxicology & Poison Control Centre Munich TUM School of Medicine Technical University of
Drug-induced hyperammonemia: are there specific therapies? NACCT Boston 2016 Florian Eyer Department of Clinical Toxicology & Poison Control Centre Munich TUM School of Medicine Technical University of
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children
 Malaysian J Pathol 2010; 32(2) : 87 95 ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children CHEN Bee Chin Msc, NGU Lock Hock MRCP and *ZABEDAH Md
Malaysian J Pathol 2010; 32(2) : 87 95 ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children CHEN Bee Chin Msc, NGU Lock Hock MRCP and *ZABEDAH Md
Amino Acid Oxidation and the Urea Cycle
 Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Volume 3 (2017) Issue 10 ISSN Keywords. Introduction. Case Report. Open Journal of Clinical & Medical Case Reports
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 10 ISSN 2379-1039 Recurrent hyperammonemia in an 80-year-old woman with congenital urea cycle abnormality Junji Yamaguchi, MD*; Koichi
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 10 ISSN 2379-1039 Recurrent hyperammonemia in an 80-year-old woman with congenital urea cycle abnormality Junji Yamaguchi, MD*; Koichi
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Urea cycle disorders (UCD) compromise a group of inherited metabolic disorders with an estimated overall prevalence
 Early Clinical Manifestations and Eating Patterns in Patients with Urea Cycle Disorders Thatjana Gardeitchik, MD 1,2, Maureen Humphrey, APD 1,3, Judy Nation, APD 1,3, and Avihu Boneh, MD, PhD 1,4 Objectives
Early Clinical Manifestations and Eating Patterns in Patients with Urea Cycle Disorders Thatjana Gardeitchik, MD 1,2, Maureen Humphrey, APD 1,3, Judy Nation, APD 1,3, and Avihu Boneh, MD, PhD 1,4 Objectives
Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15. Policy Number: MCP-242. Revision Date(s):
 Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15 Policy Number: MCP-242 Revision Date(s): Review Date(s): 12/15/2016; 6/22/2017 DISCLAIMER This Medical Policy is intended to
Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15 Policy Number: MCP-242 Revision Date(s): Review Date(s): 12/15/2016; 6/22/2017 DISCLAIMER This Medical Policy is intended to
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid
 How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
AMINO ACID METABOLISM
 AMINO ACID METABOLISM Synthesis of Urea in Liver The series of reactions that form urea is known as the Urea Cycle or the Krebs-Henseleit Cycle. The urea cycle operates only to eliminate excess nitrogen.
AMINO ACID METABOLISM Synthesis of Urea in Liver The series of reactions that form urea is known as the Urea Cycle or the Krebs-Henseleit Cycle. The urea cycle operates only to eliminate excess nitrogen.
New developments in Urea Cycle Disorders and its impact on patients
 New developments in Urea Cycle Disorders and its impact on patients Johannes Häberle University Children s Hospital Zurich, Division of Metabolism 16 June 2015 SFEIM 2015, Lille, France The urea cycle
New developments in Urea Cycle Disorders and its impact on patients Johannes Häberle University Children s Hospital Zurich, Division of Metabolism 16 June 2015 SFEIM 2015, Lille, France The urea cycle
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
UNDERSTANDING UREA CYCLE DISORDERS
 UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
Late-onset ornithine transcarbamylase deficiency: a potentially fatal yet treatable cause of coma
 Late-onset ornithine transcarbamylase deficiency: a potentially fatal yet treatable cause of coma David C Crosbie, Hariharan Sugumar, Marion A Simpson, Susan P Walker, Helen M Dewey and Michael C Reade
Late-onset ornithine transcarbamylase deficiency: a potentially fatal yet treatable cause of coma David C Crosbie, Hariharan Sugumar, Marion A Simpson, Susan P Walker, Helen M Dewey and Michael C Reade
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory
 ISPUB.COM The Internet Journal of Laboratory Medicine Volume 1 Number 2 Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory A Rao, P Varma, Sumitra, S Dhanya Citation A Rao, P Varma, Sumitra,
ISPUB.COM The Internet Journal of Laboratory Medicine Volume 1 Number 2 Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory A Rao, P Varma, Sumitra, S Dhanya Citation A Rao, P Varma, Sumitra,
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
CLINICAL PHARMACOLOGY
 BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
METABOLISMO DE AMINOÁCIDOS
 DEZ 2015 METABOLISMO DE AMINOÁCIDOS Licenciatura em Ciências da Saúde (Ano 2015-2016) Isabel Tavares de Almeida Faculdade de Farmácia da ULisboa PROTEIN DEGRADATION - DIGESTION AMINO ACID STRUCTURE 2-,
DEZ 2015 METABOLISMO DE AMINOÁCIDOS Licenciatura em Ciências da Saúde (Ano 2015-2016) Isabel Tavares de Almeida Faculdade de Farmácia da ULisboa PROTEIN DEGRADATION - DIGESTION AMINO ACID STRUCTURE 2-,
Amino acid Catabolism
 Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
NITROGEN METABOLISM An Overview
 1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL Seminar & Health Sciences NITROGEN METABOLISM
1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL Seminar & Health Sciences NITROGEN METABOLISM
Clinical course of 63 patients with neonatal onset urea cycle disorders in the years
 Unsinn et al. Orphanet Journal of Rare Diseases (2016) 11:116 DOI 10.1186/s13023-016-0493-0 RESEARCH Open Access Clinical course of 63 patients with neonatal onset urea cycle disorders in the years 2001
Unsinn et al. Orphanet Journal of Rare Diseases (2016) 11:116 DOI 10.1186/s13023-016-0493-0 RESEARCH Open Access Clinical course of 63 patients with neonatal onset urea cycle disorders in the years 2001
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Scottish Medicines Consortium
 Scottish Medicines Consortium carglumic acid 200mg dispersible tablets (Carbaglu ) No. 299/06 Orphan Europe 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium carglumic acid 200mg dispersible tablets (Carbaglu ) No. 299/06 Orphan Europe 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Salicylate (Aspirin) Ingestion California Poison Control Background 1. The prevalence of aspirin-containing analgesic products makes
 Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Nitrogen Metabolism. Overview
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Neonatal presentation of citrullinemia
 SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2014 Neonatal presentation of citrullinemia May 2014 2 Anastaze-Stelle K, Hagerman A, Fluss J, Borradori-Tolsa C, Kanavaki A, Sizonenko
SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2014 Neonatal presentation of citrullinemia May 2014 2 Anastaze-Stelle K, Hagerman A, Fluss J, Borradori-Tolsa C, Kanavaki A, Sizonenko
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN *
 For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
Urea cycle: Urea cycle is discovered by Krebs andhanseleit(1932).
 Urea cycle: Urea cycle is discovered by Krebs andhanseleit(1932). Urea cycle is the removal of excess of NH2 derived from amino acids catabolism in the tissues and excreted in urine. Site of synthesis:
Urea cycle: Urea cycle is discovered by Krebs andhanseleit(1932). Urea cycle is the removal of excess of NH2 derived from amino acids catabolism in the tissues and excreted in urine. Site of synthesis:
Glycogen Storage Disease
 Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle
 BIOC 423: Introductory Biochemistry Biochemistry Education Department of Biochemistry & Molecular Biology University of New Mexico Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle OBJECTIVES Describe
BIOC 423: Introductory Biochemistry Biochemistry Education Department of Biochemistry & Molecular Biology University of New Mexico Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle OBJECTIVES Describe
Hepatic Encephalopathy
 Hepatic Encephalopathy John Barber UMassMedical Student, Class of 2019 www.12daysinmarch.com Outline Overview Normal Physiology Pathology Symptoms Diagnosis Treatment Overview Ammonia (NH 3 ) is a byproduct
Hepatic Encephalopathy John Barber UMassMedical Student, Class of 2019 www.12daysinmarch.com Outline Overview Normal Physiology Pathology Symptoms Diagnosis Treatment Overview Ammonia (NH 3 ) is a byproduct
NIH Public Access Author Manuscript Pediatr Res. Author manuscript; available in PMC 2010 July 1.
 NIH Public Access Author Manuscript Published in final edited form as: Pediatr Res. 2009 July ; 66(1): 96 101. doi:10.1203/pdr.0b013e3181a27a16. Intellectual, Adaptive, and Behavioral Functioning in Children
NIH Public Access Author Manuscript Published in final edited form as: Pediatr Res. 2009 July ; 66(1): 96 101. doi:10.1203/pdr.0b013e3181a27a16. Intellectual, Adaptive, and Behavioral Functioning in Children
Drug-induced Hyperammonemia
 Drug-induced Hyperammonemia EAPCCT Madrid 2016 - Pre-Congress Florian Eyer Division of Clinical Toxicology & PCC Munich School of Medicine Klinikum rechts der Isar Technical University of Munich 24.5.2016
Drug-induced Hyperammonemia EAPCCT Madrid 2016 - Pre-Congress Florian Eyer Division of Clinical Toxicology & PCC Munich School of Medicine Klinikum rechts der Isar Technical University of Munich 24.5.2016
Blood ammonia and glutamine as predictors of hyperammonemic crises in patients with urea cycle disorder
 American College of Medical Genetics and Genomics Original Research Article Open Blood ammonia and glutamine as predictors of hyperammonemic crises in patients with urea cycle disorder Brendan Lee, MD,
American College of Medical Genetics and Genomics Original Research Article Open Blood ammonia and glutamine as predictors of hyperammonemic crises in patients with urea cycle disorder Brendan Lee, MD,
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-Protein Nitrogenous Compounds. Non-Protein Nitrogenous Compounds. NPN s. Urea (BUN) Creatinine NH 3. University of Cincinnati MLS Program 1
 Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
TYPE I CITRULLINEMIA: A REVIEW OF A RARE UREA CYCLE DISORDER AND APPROACH TO MANAGEMENT
 TYPE I CITRULLINEMIA: A REVIEW OF A RARE UREA CYCLE DISORDER AND APPROACH TO MANAGEMENT Denise M. Kolanczyk,PharmD 1,2, Jenna Applegate, RD 3, Evelina Lin, PharmD 2, Allyson Wexler, PharmD 4, and Megan
TYPE I CITRULLINEMIA: A REVIEW OF A RARE UREA CYCLE DISORDER AND APPROACH TO MANAGEMENT Denise M. Kolanczyk,PharmD 1,2, Jenna Applegate, RD 3, Evelina Lin, PharmD 2, Allyson Wexler, PharmD 4, and Megan
Yves Kibleur Dries Dobbelaere Magalie Barth Anaïs Brassier Nathalie Guffon
 Pediatr Drugs (2014) 16:407 415 DOI 10.1007/s40272-014-0081-5 ORIGINAL RESEARCH ARTICLE Results from a Nationwide Cohort Temporary Utilization Authorization (ATU) Survey of Patients in France Treated with
Pediatr Drugs (2014) 16:407 415 DOI 10.1007/s40272-014-0081-5 ORIGINAL RESEARCH ARTICLE Results from a Nationwide Cohort Temporary Utilization Authorization (ATU) Survey of Patients in France Treated with
NUCDF. National Urea Cycle Disorders Foundation Conference Presentation Effects of UCD on the Brain. July 20, 2013
 Understanding the effect of UCDs on brain function and behavior conference Andrea L. Gropman, M.D., FAAP, FACMG Children s National Medical Center, Washington, D.C. Conference goals Talk about neurological
Understanding the effect of UCDs on brain function and behavior conference Andrea L. Gropman, M.D., FAAP, FACMG Children s National Medical Center, Washington, D.C. Conference goals Talk about neurological
Nitrogen Metabolism. Pratt and Cornely Chapter 18
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
Inborn Errors of Metabolism (IEM)
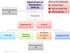 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
NITROGEN METABOLISM: An Overview
 NITROGEN METABOLISM: An Overview University of PNG School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology VJ Temple 1 How are nitrogen-containing
NITROGEN METABOLISM: An Overview University of PNG School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology VJ Temple 1 How are nitrogen-containing
Introduction. Clinical manifestations
 Carbamyl phosphate synthetase I deficiency Roland Posset MD ( Dr. Posset of the University Center for Child and Adolescent Medicine in Heidelberg has no relevant financial relationships to disclose. )
Carbamyl phosphate synthetase I deficiency Roland Posset MD ( Dr. Posset of the University Center for Child and Adolescent Medicine in Heidelberg has no relevant financial relationships to disclose. )
Nitrogen Metabolism. Overview
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Part III => METABOLISM and ENERGY. 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle
 Part III => METABOLISM and ENERGY 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle Section 3.5a: Protein Degradation Synopsis 3.5a - Dietary proteins are degraded
Part III => METABOLISM and ENERGY 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle Section 3.5a: Protein Degradation Synopsis 3.5a - Dietary proteins are degraded
The Chronic Liver Disease Foundation (CLDF) and the International Coalition of Hepatology Education Providers (IC-HEP) present:
 The Chronic Liver Disease Foundation (CLDF) and the International Coalition of Hepatology Education Providers (IC-HEP) present: Certified by: Provided by: Endorsed by: Hepatic Encephalopathy Hepatic Encephalopathy:
The Chronic Liver Disease Foundation (CLDF) and the International Coalition of Hepatology Education Providers (IC-HEP) present: Certified by: Provided by: Endorsed by: Hepatic Encephalopathy Hepatic Encephalopathy:
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
Fate of Dietary Protein
 Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal lining: proteases
Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal lining: proteases
Amino Acid Metabolism
 Amino Acid Metabolism Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal
Amino Acid Metabolism Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Lecture 10 - Protein Turnover and Amino Acid Catabolism
 Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Amino acid metabolism
 Amino acid metabolism The important reaction commonly employed in the breakdown of an amino acid is always the removal of its -amino group. The product ammonia is excreted after conversion to urea or other
Amino acid metabolism The important reaction commonly employed in the breakdown of an amino acid is always the removal of its -amino group. The product ammonia is excreted after conversion to urea or other
*Sections or subsections omitted from the full prescribing information are not listed.
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use RAVICTI safely and effectively. See full prescribing information for RAVICTI. RAVICTI (glycerol phenylbutyrate)
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use RAVICTI safely and effectively. See full prescribing information for RAVICTI. RAVICTI (glycerol phenylbutyrate)
Metabolic Precautions & ER Recommendations
 Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Ornithine carbamoyltransferase deficiency
 84 Arch Dis Child 2001;84:84 88 CURRENT TOPIC Willink Biochemical Genetics Unit, Royal Manchester Children s Hospital, Manchester M27 4HA, UK J E Wraith Correspondence to: Dr Wraith ed@willink.demon.co.uk
84 Arch Dis Child 2001;84:84 88 CURRENT TOPIC Willink Biochemical Genetics Unit, Royal Manchester Children s Hospital, Manchester M27 4HA, UK J E Wraith Correspondence to: Dr Wraith ed@willink.demon.co.uk
BIOB111 - Tutorial activity for Session 25
 BIOB111 - Tutorial activity for Session 25 General topics for week 14 Session 25 The metabolism of proteins Students are asked to draw the concept map showing all details of protein metabolism 1 Instructions:
BIOB111 - Tutorial activity for Session 25 General topics for week 14 Session 25 The metabolism of proteins Students are asked to draw the concept map showing all details of protein metabolism 1 Instructions:
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
 Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Altered mental status: a common complaint that led to a rare diagnosis - Ornithine Transcarbamylase Deficiency
 Altered mental status: a common complaint that led to a rare diagnosis - Ornithine Transcarbamylase Deficiency Joshua J. White, OMS3 Charles C. Finch, D.O., FACOEP Arizona College Of Osteopathic Medicine
Altered mental status: a common complaint that led to a rare diagnosis - Ornithine Transcarbamylase Deficiency Joshua J. White, OMS3 Charles C. Finch, D.O., FACOEP Arizona College Of Osteopathic Medicine
Liver failure &portal hypertension
 Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
