Diuretic Agents Part-1. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
|
|
|
- Allen Barrett
- 5 years ago
- Views:
Transcription
1 Diuretic Agents Part-1 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
2 Kidneys eliminates waste products and regulates the volume, electrolyte and ph of the extracellular fluid Approximately 16-20% of the blood plasma entering kidneys is filtered from glomerular capillaries into Bowman capsule. The filtrate normally free from proteins and blood cells, it contain most low-molecularweight plasma components in approximately same concentrations as are found in plasma.
3 These include glucose, sodium bicarbonate, amino acids, and other organic solutes, as well as electrolytes, such as Na+, K+, and CI-. The kidney regulates ionic composition and volume of urine by the active reabsorption or secretion of ions and/or the passive reabsorption of water at five functional zones along the nephron Kidney is main organ by which drugs are eliminated. In the presence of renal failure dose must be adjusted
4
5 Diuretic is an agent that increases urine volume Natriuretic is an agent that causes an increase in renal sodium excretion, they called diuretic (increase water excretion )
6 Thiazide Diuretics Loop Diuretics Potassium- Sparing Diuretics Carbonic Anhydrase Inhibitors Osmotic Diuretics Diuretic Drugs Chlorothiazide,Chlorthalidone Hydrochlorothiazid, Indapamide, Metolazone Bumetanide,Ethacrynic Acid Furosemide, Torsemide Amiloride,Spironolactone, Triamterene Acetazolamide Mannitol
7 Tubule transport systems and sites of action of diuretics ADH, antidiuretic hormone; PTH, parathyroid hormone.
8 Carbonic Anhydrase Inhibitors Acetazolamide They are now rarely used as diuretics because they are much less efficacious than the thiazides or loop diuretics Carbonic anhydrase inhibitors are more often used for their other pharmacologic actions rather than for their diuretic effect Acetazolamide inhibits the enzyme carbonic anhydrase in the proximal tubular epithelial cells.
9 Mechanism of Action Acetazolamide inhibits carbonic anhydrase located intracellularly (cytoplasm) and on the apical membrane of the proximal tubular epithelium. Carbonic anhydrase catalyzes the reaction of CO2 (carbon dioxide) and H2O, leading to H2CO3 (carbonic acid). which spontaneously ionizes to H + and HCO3 - (bicarbonate)
10 The decreased ability to exchange Na+ for H+ in the presence of acetazolamide results in a mild diuresis. Additionally, HCO3 - is retained in the lumen, with marked elevation in urinary ph. The loss of HCO3- causes a hyperchloremic metabolic acidosis and decreased diuretic efficacy following several days of therapy
11
12 Pharmacokinetics Acetazolamide is given orally once a day. An increase in urine ph from the HCO3 diuresis is apparent within 30 minutes, is maximal at 2 hours, and persists for 12 hours after a single dose The drug excretion is by secretion in the proximal tubule Dosing must be reduced in renal insufficiency
13 Clinical Uses Treatment of glaucoma Enhancement renal excretion of weak acids by urine alkalinization Metabolic Alkalosis Mountain sickness
14 Treatment of Glaucoma Acetazolamide decreases the production of aqueous humor, probably by blocking carbonic anhydrase in the ciliary body of the eye (reducing elevated intraocular pressure). It is useful in the chronic treatment of glaucoma but should not be used for an acute attack; pilocarpine is preferred for an acute attack because of its immediate action. Topical carbonic anhydrase inhibitors, such as dorzolamide and brinzolamide, have the advantage of not causing any systemic effects
15 Enhancement renal excretion of weak acids by urine alkalinization Uric acid, cystine, and other weak acids are most easily reabsorbed from acidic urine. Therefore, renal excretion of weak acids can be enhanced by increasing urinary ph with carbonic anhydrase inhibitors
16 Mountain Sickness Acetazolamide can be used in the prophylaxis of acute mountain sickness among healthy individuals who ascend above 10,000 feet. Acetazolamide given nightly for five days before the ascent It prevents the weakness, breathlessness, dizziness, nausea, and cerebral as well as pulmonary edema By decreasing cerebrospinal fluid (CSF) formation &by decreasing the ph of the cerebrospinal fluid Acetazolamide can increase ventilation and diminish symptoms of mountain sickness
17 Adverse Effects 1. Metabolic acidosis (mild), (results from chronic reduction of body HCO3 stores) 2. Renal potassium depletion (hypokalemia) Because the increased Na+ presented to the collecting tubule (with HCO3 ) is partially reabsorbed, increasing the lumen-negative electrical potential in that segment and enhancing K+ secretion, this effect can be counteracted by simultaneous administration of potassium chloride 3. Renal stone formation (calcium salts are relatively insoluble at alkaline ph)
18 4. Drowsiness and paresthesia. 5. The drug should be avoided in patients with hepatic cirrhosis, because it could lead to a decreased excretion of NH Fever, rashes, bone marrow suppression, and interstitial nephritis (these drugs are sulfonamide derivatives)
19 Contraindications Of Carbonic Anhydrase Inhibitor Patients with cirrhosis Carbonic anhydrase inhibitor cause alkalinization of the urine which decreases urinary excretion of NH4+ (by converting it to rapidly reabsorbed NH3) and development of hyperammonemia and hepatic encephalopathy
20 Loop Diuretics Bumetanide, Furosemide, Torsemide And Ethacrynic Acid They are the most efficacious diuretic drugs Furosemide is the most commonly used of these drugs Have their major action on the ascending limb of loop of Henle.
21
22 Ethacrynic acid shows greater side effects than other loop diuretics, and its use is therefore limited. Bumetanide is much more potent than furosemide Bumetanide and furosemide are sulfonamide derivatives.
23 Mechanism of Action of Loop Diuretics Inhibit cotransport of Na+/K+/ +/2Cl by inhibiting the luminal Na+/K+/2Cl transporter in the thick ascending limb of Henle's loop and the reabsorption of these ions is decreased
24 The loop diuretics act, even among patients who have poor renal function or have not responded to thiazides or other diuretics. Loop diuretics increase the Ca2+ content of urine, whereas thiazide diuretics decrease the Ca2+ concentration of the urine.
25 Hypocalcemia does not result in patients with normal serum Ca2+ concentrations because Ca2+ is reabsorbed in the distal convoluted tubule. Hypomagnesemia can occur due to loss of Mg2+.
26 The loop diuretics cause decreased renal vascular resistance and increased renal blood flow. Loop diuretics increase prostaglandin synthesis,the PGs have a role in their diuretic action, indomethacin reduce their diuretic action
27 Therapeutic Uses of Loop Diuretics 1. Acute Pulmonary Edema The loop diuretics are the drugs of choice for reducing the acute pulmonary edema of heart failure Because of their rapid onset of action, particularly when given intravenously The loop diuretics cause rapid, intense diuresis.
28 2. Acute Renal Failure Loop agents can increase the rate of urine flow and enhance K+ excretion in acute renal failure 3. Toxicity by Anion Overdose useful in treating toxic ingestions of bromide, fluoride, and iodide, which are reabsorbed in the thick ascending limb of Henle's loop avoid extracellular fluid volume depletion therefore Saline solution must be administered to replace urinary losses of Na+ and Cl
29 4. Hypercalcemia Loop diuretics (along with hydration) are also useful in treating hypercalcemia, because they stimulate tubular Ca2+ excretion. 5. Hyperkalemia
30 Pharmacokinetics of Loop Diuretics Administered orally or parenterally Their duration of action is 2-4 hours They are secreted into the urine.
31 Adverse Effects of Loop Diuretics 1. Ototoxicity Deafness Particularly when concomitantly with the aminoglycoside antibiotics. Ethacrynic acid is the most likely to cause deafness Disturbance of Vestibular function
32 2. Hyperuricemia Furosemide and ethacrynic acid may cause gouty attacks because they compete with uric acid for the renal and biliary secretory systems, thus blocking its secretion.
33 3. Acute Hypovolemia Loop diuretics can cause a severe and rapid reduction in blood volume, with the possibility of hypotension, shock, and cardiac arrhythmias. 4. Potassium Depletion 5. Hypomagnesemia Chronic use of loop diuretics and low dietary intake of Mg2+ can lead to hypomagnesemia, particularly in the elderly. Hypomagnesemia corrected by oral supplementation.
34 Contraindication: Furosemide, bumetanide, and torsemide may exhibit allergic cross-reactivity in patients who are sensitive to other sulfonamides Overzealous use of any diuretic is dangerous in hepatic cirrhosis, borderline renal failure, or heart failure.
35 Thiazides & Related Compounds Chlorothiazide and hydrochlorothiazide The thiazides are most widely used of diuretic drugs. They are sulfonamide derivatives. Chlorothiazide was active orally, and was capable of affecting the severe edema of cirrhosis and heart failure with a minimum of side effects. Hydrochlorothiazide is more potent than chlorothiazide, required lower dose
36 Thiazides The thiazide diuretics were discovered in 1957, as a result of efforts to synthesize more potent carbonic anhydrase inhibitors. It subsequently became clear that the thiazides inhibit NaCl, rather than NaHCO 3 transport Their action was predominantly in the DCT, rather than the PCT. CHlorthalidone have significant carbonic anhydrase inhibitory activity.
37 Mechanism of Action Thiazides inhibit NaCl reabsorption from the luminal side of epithelial cells in the DCT by blocking the Na+/Cl transporter Thiazides actually enhance Ca 2+ reabsorption. This enhancement result from effects in both the proximal and distal convoluted tubules. In the proximal tubule, thiazide-induced volume depletion leads to enhanced Na + & passive Ca 2+ reabsorption. In the DCT, lowering of intracellular Na + by thiazide-induced blockade of Na + entry enhances Na + /Ca 2+ exchange in the basolateral membrane and increases overall reabsorption of Ca 2+.
38 Thiazides rarely cause hypercalcemia as the result of this enhanced reabsorption but they can unmask hypercalcemia due to other causes (eg, hyperparathyroidism, carcinoma). Thiazides are useful in the treatment of kidney stones caused by hypercalciuria. The action of thiazides depends in part on renal prostaglandin production, thiazides can also be inhibited by NSAIDs
39 Tubule transport systems and sites of action of diuretics. ADH, antidiuretic hormone; PTH, parathyroid hormone.
40
41 Pharmacokinetics Thiazides have an unsubstituted sulfonamide group All thiazides can be administered orally, but there are differences in their metabolism Chlorothiazide, the parent of the group, is not very lipid-soluble and must be given in relatively large doses. It is the only thiazide available for parenteral administration HCTZ is more potent and should be used in much lower doses Chlorthalidone is slowly absorbed and has a longer duration of action.
42 Indapamide is excreted primarily by the biliary system and enough of the active form is cleared by the kidney to exert its diuretic effect in the DCT. It is therefore less likely to accumulate in patients with renal failure, and may be useful in their treatment. All thiazides compete with the secretion of uric acid in the proximal tubule
43 Clinical Indications The major indications for thiazide diuretics are 1. Hypertension 2. Heart failure 3. Nephrolithiasis due to idiopathic hypercalciuria 4. Nephrogenic diabetes insipidus.
44 1. Hypertension: Thiazides are effective in reducing systolic and diastolic blood pressure for extended periods in patients with mild to moderate essential hypertension patients can be continued for years on the thiazides alone, although a small percentage of patients require additional medication, such as beta-adrenergic blockers.
45 2. Heart Failure Thiazide diuretics are used for the treatment of the edema associated with congestive heart failure Note: Thiazide used for the treatment of the edema associated with hepatic cirrhosis nephrotic syndrome, chronic renal failure, and acute glomerulonephritis
46 3. Nephrolithiasis Due to Idiopathic Hypercalciuria Thiazide reduce the urinary excretion of Ca2+ by increase Ca2+ reabsorption in the distal convoluted tubule Used in patients with kidney stones that contain Ca2+ phosphate or Ca2+ oxalate and exhibit a defect in proximal tubular Ca2+ reabsorption that causes hypercalciuria
47 4. Nephrogenic diabetes insipidus Diabetes insipidus is due to either deficient production of ADH (neurogenic or central diabetes insipidus) or inadequate responsiveness to ADH (nephrogenic diabetes insipidus [NDI]). Administration of supplementary ADH is effective only in central diabetes insipidus. Thiazide diuretics can reduce polyuria and polydipsia in nephrogenic diabetes insipidus, which is not responsive to ADH supplementation. Lithium, used in the treatment of manic depressive disorder, is a common cause of NDI, and thiazide diuretics have been found to be very helpful in treating it
48 Adverse Effects 1. Hypokalemic Metabolic Alkalosis and Hyperuricemia (similar to loop diuretics) 2. Impaired Carbohydrate Tolerance Hyperglycemia may occur in patients who are diabetic or have abnormal glucose tolerance tests. The effect is due to both Impaired pancreatic release of insulin Diminished tissue utilization of glucose.
49 Hyperlipidemia Thiazides cause a 5 15% increase in total serum cholesterol and low-density lipoproteins (LDLs). These levels may return toward baseline after prolonged use.
50 Hyponatremia It is caused by a combination of hypovolemia-induced elevation of ADH, reduction in the diluting capacity of the kidney, and increased thirst. It can be prevented by reducing the dose of the drug or limiting water intake
51 Other Toxicities The thiazides are sulfonamides and share crossreactivity with other members of this chemical group. Photosensitivity, dermatitis, acute necrotizing pancreatitis. Hemolytic anemia, thrombocytopenia Weakness, fatigability, and paresthesias similar to those of carbonic anhydrase inhibitors may occur. Impotence related to volume depletion.
52 Contraindications Excessive use of any diuretic is dangerous in patients with hepatic cirrhosis, borderline renal failure, or heart failure
DIURETICS. Assoc. Prof. Bilgen Başgut
 DIURETICS Assoc. Prof. Bilgen Başgut Classification of Diuretics The best way to classify diuretics is to look for their Site of action in the nephron A. Diuretics that inhibit transport in the Proximal
DIURETICS Assoc. Prof. Bilgen Başgut Classification of Diuretics The best way to classify diuretics is to look for their Site of action in the nephron A. Diuretics that inhibit transport in the Proximal
Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari
![Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari](/thumbs/90/104323364.jpg) Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
PRINCIPLES OF DIURETIC ACTIONS:
 DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
Diuretics (Saluretics)
 Diuretics (Saluretics) Diuretics increase urine excretion mainly by reabsorption of salts and water from kidney tubules These agents are ion transport inhibitors that decrease the reabsorption of Na+ at
Diuretics (Saluretics) Diuretics increase urine excretion mainly by reabsorption of salts and water from kidney tubules These agents are ion transport inhibitors that decrease the reabsorption of Na+ at
Diuretics are drugs that increase the volume of urine excreted. Most diuretic agents are inhibitors of renal ion transporters that decrease the
 Diuretics Diuretics are drugs that increase the volume of urine excreted. Most diuretic agents are inhibitors of renal ion transporters that decrease the reabsorption of Na+ at different sites in the nephron.
Diuretics Diuretics are drugs that increase the volume of urine excreted. Most diuretic agents are inhibitors of renal ion transporters that decrease the reabsorption of Na+ at different sites in the nephron.
Therapeutics of Diuretics
 (Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
(Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
DIURETICS-2. Dr. Shariq Syed. Shariq AIKC/TYB/2014
 DIURETICS-2 Dr. Syed Structure of Kidney Blood filtered by functional unit: Nephron Except for cells, proteins, other large molecules, rest gets filtered Structure of Kidney 3 major regions of nephron
DIURETICS-2 Dr. Syed Structure of Kidney Blood filtered by functional unit: Nephron Except for cells, proteins, other large molecules, rest gets filtered Structure of Kidney 3 major regions of nephron
Diuretic Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Chapter 15 Diuretic Agents
 Chapter 15 Diuretic Agents Diuretics Diuretics are agents that increase the rate of urine formation and salt excretion. Diuresis = increased water formation, but the term is also used to indicate increased
Chapter 15 Diuretic Agents Diuretics Diuretics are agents that increase the rate of urine formation and salt excretion. Diuresis = increased water formation, but the term is also used to indicate increased
DIURETICS-4 Dr. Shariq Syed
 DIURETICS-4 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Loop diuretics act on which transporter PKCC NKCC2 AIKTCC I Don t know AIKTC - Knowledge Resources & Relay Center 2 Pop
DIURETICS-4 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Loop diuretics act on which transporter PKCC NKCC2 AIKTCC I Don t know AIKTC - Knowledge Resources & Relay Center 2 Pop
Renal Pharmacology. Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics BIMM118
 Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Low Efficacy Diuretics. Potassium sparing diuretics. Carbonic anhydrase inhibitors. Osmotic diuretics. Miscellaneous
 University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Low Efficacy Diuretics 1. Potassium sparing diuretics 2. Carbonic anhydrase inhibitors 3. Osmotic diuretics 4. Miscellaneous
University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Low Efficacy Diuretics 1. Potassium sparing diuretics 2. Carbonic anhydrase inhibitors 3. Osmotic diuretics 4. Miscellaneous
Chapter 15. Diuretic Agents
 Chapter 15. Diuretic Agents Katzung PHARMACOLOGY, 9e > Section III. Cardiovascular-Renal Drugs > Chapter 15. Diuretic Agents > Diuretic Agents: Introduction Abnormalities in fluid volume and electrolyte
Chapter 15. Diuretic Agents Katzung PHARMACOLOGY, 9e > Section III. Cardiovascular-Renal Drugs > Chapter 15. Diuretic Agents > Diuretic Agents: Introduction Abnormalities in fluid volume and electrolyte
Osmotic Diuretics and Carbonic anhydrase inhibitors
 Lecture : Osmotic Diuretics and Carbonic anhydrase inhibitors Contents : Explanation Summary Questions 1 DIURETICS Definition: Are drugs that increase renal excretion of sodium and water resulting in increase
Lecture : Osmotic Diuretics and Carbonic anhydrase inhibitors Contents : Explanation Summary Questions 1 DIURETICS Definition: Are drugs that increase renal excretion of sodium and water resulting in increase
DIURETICS-3 Dr. Shariq Syed
 DIURETICS-3 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Diuretics primarily prevent the reabsorption of K Na Cl I Don t know, Too busy with periodic exams! AIKTC - Knowledge
DIURETICS-3 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Diuretics primarily prevent the reabsorption of K Na Cl I Don t know, Too busy with periodic exams! AIKTC - Knowledge
Chapter 21. Diuretic Agents. Mosby items and derived items 2008, 2002 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
Diuretic Use in Neonates
 Neonatal Nursing Education Brief: Diuretic Use in the Neonate http://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/ Diuretics
Neonatal Nursing Education Brief: Diuretic Use in the Neonate http://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/ Diuretics
 Page 1 of 23 Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Copyright The McGraw-Hill Companies. All rights reserved. Basic and Clinical Pharmacology
Page 1 of 23 Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Copyright The McGraw-Hill Companies. All rights reserved. Basic and Clinical Pharmacology
Composition: Each Tablet contains. Pharmacokinetic properties:
 Composition: Each Tablet contains Torsemide 5/10/20/40/100mg Pharmacokinetic properties: Torsemide is well absorbed from the gastrointestinal tract. Peak serum concentrations are achieved within 1 hour
Composition: Each Tablet contains Torsemide 5/10/20/40/100mg Pharmacokinetic properties: Torsemide is well absorbed from the gastrointestinal tract. Peak serum concentrations are achieved within 1 hour
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis.
 Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
DIURETICS CARBONIC ANHYDRASE INHIBITORS THIAZIDE THIAZIDE-LIKE OSMOTIC DIURETICS LOOP DIURETICS POTASSIUM SPARING DIURETICS
 DIURETICS A diuretic is any substance that promotes diuresis, that is, the increased production of urine. This includes forced diuresis. There are several categories of diuretics. All diuretics increase
DIURETICS A diuretic is any substance that promotes diuresis, that is, the increased production of urine. This includes forced diuresis. There are several categories of diuretics. All diuretics increase
Diuretics having the quality of exciting excessive excretion of urine. OED. Inhibitors of Sodium Reabsorption Saluretics not Aquaretics
 Diuretics having the quality of exciting excessive excretion of urine. OED Inhibitors of Sodium Reabsorption Saluretics not Aquaretics 1 Sodium Absorption Na Entry into the Cell down an electrochemical
Diuretics having the quality of exciting excessive excretion of urine. OED Inhibitors of Sodium Reabsorption Saluretics not Aquaretics 1 Sodium Absorption Na Entry into the Cell down an electrochemical
Lecture Topics 利尿药. Diuretics. Diuretic Classes. Definition of diuretic:
 利尿药 Diuretics 四川大学药理教研室朱玲副教授 (zhuling529@163.com) Lecture Topics You need to know these things: high efficacy furosemide moderate hydrochlorothiazide low spironolactonum triameterenum Mechanism of action
利尿药 Diuretics 四川大学药理教研室朱玲副教授 (zhuling529@163.com) Lecture Topics You need to know these things: high efficacy furosemide moderate hydrochlorothiazide low spironolactonum triameterenum Mechanism of action
LESSON ASSIGNMENT. Diuretic and Antidiuretic Agents. After you finish this lesson you should be able to:
 LESSON ASSIGNMENT SUBCOURSE MD0806 LESSON 8 Therapeutics III. Diuretic and Antidiuretic Agents. LESSON ASSIGNMENT Paragraphs 8-1--8-7. LESSON OBJECTIVES After you finish this lesson you should be able
LESSON ASSIGNMENT SUBCOURSE MD0806 LESSON 8 Therapeutics III. Diuretic and Antidiuretic Agents. LESSON ASSIGNMENT Paragraphs 8-1--8-7. LESSON OBJECTIVES After you finish this lesson you should be able
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Instrumental determination of electrolytes in urine. Amal Alamri
 Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Acid Base Balance. Chapter 26 Balance. ph Imbalances. Acid Base Balance. CO 2 and ph. Carbonic Acid. Part 2. Acid/Base Balance
 Acid Base Balance Chapter 26 Balance Part 2. Acid/Base Balance Precisely balances production and loss of hydrogen ions (ph) The body generates acids during normal metabolism, tends to reduce ph Kidneys:
Acid Base Balance Chapter 26 Balance Part 2. Acid/Base Balance Precisely balances production and loss of hydrogen ions (ph) The body generates acids during normal metabolism, tends to reduce ph Kidneys:
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Answers and Explanations
 Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Acid-Base Balance 11/18/2011. Regulation of Potassium Balance. Regulation of Potassium Balance. Regulatory Site: Cortical Collecting Ducts.
 Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
NORMAL POTASSIUM DISTRIBUTION AND BALANCE
 NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
Water, Electrolytes, and Acid-Base Balance
 Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Medication Review. Renal Drugs. Pharmacy Technician Training Systems Passassured, LLC
 Medication Review Renal Drugs Pharmacy Technician Training Systems Passassured, LLC Medication Review, Renal Drugs PassAssured's Pharmacy Technician Training Program Medication Review Renal Drugs Click
Medication Review Renal Drugs Pharmacy Technician Training Systems Passassured, LLC Medication Review, Renal Drugs PassAssured's Pharmacy Technician Training Program Medication Review Renal Drugs Click
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
WATER, SODIUM AND POTASSIUM
 WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
Therapeutic Uses of Diuretics
 DIURETICS Diuretics are drugs that promote the output of urine excreted by the Kidneys. The primary action of most diuretics is the direct inhibition of a + transport at one or more of the four major anatomical
DIURETICS Diuretics are drugs that promote the output of urine excreted by the Kidneys. The primary action of most diuretics is the direct inhibition of a + transport at one or more of the four major anatomical
LESSON ASSIGNMENT. After completing this lesson, you will be able to: 4-1. Identify the general characteristics of diuretics.
 LESSON ASSIGNMENT LESSON 4 Diuretics. LESSON ASSIGNMENT Paragraphs 4-1 through 4-6. LESSON OBJECTIVES After completing this lesson, you will be able to: 4-1. Identify the general characteristics of diuretics.
LESSON ASSIGNMENT LESSON 4 Diuretics. LESSON ASSIGNMENT Paragraphs 4-1 through 4-6. LESSON OBJECTIVES After completing this lesson, you will be able to: 4-1. Identify the general characteristics of diuretics.
MS1 Physiology Review of Na+, K+, H + /HCO 3. /Acid-base, Ca+² and PO 4 physiology
 MS1 Physiology Review of,, / /Acidbase, Ca+² and PO 4 physiology I. David Weiner, M.D. Professor of Medicine and Physiology University of Florida College of Medicine Basic principles Proximal tubule Majority
MS1 Physiology Review of,, / /Acidbase, Ca+² and PO 4 physiology I. David Weiner, M.D. Professor of Medicine and Physiology University of Florida College of Medicine Basic principles Proximal tubule Majority
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Osmoregulation and the Excretory System
 Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Furosemide: Properties, Alternatives, and the Medication Approval Process. Heather Brown EMS 209-Advanced Pharmacology Don Knox
 Furosemide: Properties, Alternatives, and the Medication Approval Process Heather Brown EMS 209-Advanced Pharmacology Don Knox Pre-hospital treatment of critical patients is a key factor in determining
Furosemide: Properties, Alternatives, and the Medication Approval Process Heather Brown EMS 209-Advanced Pharmacology Don Knox Pre-hospital treatment of critical patients is a key factor in determining
Major intra and extracellular ions Lec: 1
 Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
Fluid, Electrolyte, and Acid Base Balance
 25 Fluid, Electrolyte, and Acid Base Balance Lecture Presentation by Lori Garrett Note to the Instructor: For the third edition of Visual Anatomy & Physiology, we have updated our PowerPoints to fully
25 Fluid, Electrolyte, and Acid Base Balance Lecture Presentation by Lori Garrett Note to the Instructor: For the third edition of Visual Anatomy & Physiology, we have updated our PowerPoints to fully
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
H 2 O, Electrolytes and Acid-Base Balance
 H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Normal Renal Function
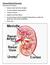 Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Renal Physiology - Lectures
 Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Chapter 24 Water, Electrolyte and Acid-Base Balance
 Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
Chapter 24 Water, Electrolyte and Acid-Base Balance Total body water for 150 lb. male = 40L 65% ICF 35% ECF 25% tissue fluid 8% blood plasma, lymph 2% transcellular fluid (CSF, synovial fluid) Water Movement
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Na concentration in the extracellular compartment is 140
 هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
Renal Excretion of Drugs
 Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
ELECTROLYTES RENAL SHO TEACHING
 ELECTROLYTES RENAL SHO TEACHING Metabolic Alkalosis 2 factors are responsible for generation and maintenance of metabolic alkalosis this includes a process that raises serum bicarbonate and a process that
ELECTROLYTES RENAL SHO TEACHING Metabolic Alkalosis 2 factors are responsible for generation and maintenance of metabolic alkalosis this includes a process that raises serum bicarbonate and a process that
Body water content. Fluid compartments. Regulation of water output. Water balance and ECF osmolallty. Regulation of water intake
 Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Body water content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; females 50% This difference reflects
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretion of Drugs. Prof. Hanan Hagar Pharmacology Unit Medical College
 Excretion of Drugs Prof. Hanan Hagar Pharmacology Unit Medical College Excretion of Drugs By the end of this lecture, students should be able to! Identify main and minor routes of excretion including renal
Excretion of Drugs Prof. Hanan Hagar Pharmacology Unit Medical College Excretion of Drugs By the end of this lecture, students should be able to! Identify main and minor routes of excretion including renal
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Faculty version with model answers
 Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
Chapter 10: Urinary System & Excretion
 Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
PACKAGE LEAFLET: Information for the patient FUROSEMID Tablets - 40 mg Solution for injection - 20 mg / 2 ml (Furosemide)
 PACKAGE LEAFLET: Information for the patient FUROSEMID Tablets - 40 mg Solution for injection - 20 mg / 2 ml (Furosemide) Read this leaflet carefully before you start taking this medicine. - Keep this
PACKAGE LEAFLET: Information for the patient FUROSEMID Tablets - 40 mg Solution for injection - 20 mg / 2 ml (Furosemide) Read this leaflet carefully before you start taking this medicine. - Keep this
ACID-BASE BALANCE URINE BLOOD AIR
 ACIDBASE BALANCE URINE BLOOD AIR H 2 PO 4 NH 4 HCO 3 KIDNEY H H HCO 3 CELLS Hb H LUNG H 2 CO 3 HHb CO 2 H 2 O ph = 7.4 [HCO 3 ] = 24 meq/l PCO 2 = 40 mm Hg CO 2 PRIMARY RENAL MECHANISMS INVOLVED IN ACIDBASE
ACIDBASE BALANCE URINE BLOOD AIR H 2 PO 4 NH 4 HCO 3 KIDNEY H H HCO 3 CELLS Hb H LUNG H 2 CO 3 HHb CO 2 H 2 O ph = 7.4 [HCO 3 ] = 24 meq/l PCO 2 = 40 mm Hg CO 2 PRIMARY RENAL MECHANISMS INVOLVED IN ACIDBASE
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Medical Translation: Welcome to our webinar
 r Welcome to our webinar Medical Translation: The Pharmacodynamics and Physiological Effects of Drug Classes Commonly Studied during Clinical Trials with Carmen Cross 13 February 2014 www.ecpdwebinars.co.uk
r Welcome to our webinar Medical Translation: The Pharmacodynamics and Physiological Effects of Drug Classes Commonly Studied during Clinical Trials with Carmen Cross 13 February 2014 www.ecpdwebinars.co.uk
