Total knee replacement
|
|
|
- Gervais Bell
- 5 years ago
- Views:
Transcription
1 Total knee replacement Your guide to a successful outcome following surgery Orthopaedic Department Patient information leaflet
2 Contents About the knee 3 Advice while you are waiting for your knee replacement 6 Enhanced recovery programme and Preload 7 8 What happens before your operation 9 Pre-operative knee group 9 Pre-assessment clinic 10 Admission day and the operation Physiotherapy 13 Bed exercises Discharge from hospital 18 Advice from six weeks 20 Maintenance exercises Possible complications 25 General advice 27 Appointments record 28 Reference source 29 Helpful telephone numbers 29 2
3 Introduction This booklet has been written to help prepare you before you come into hospital for your Total Knee Replacement (TKR) operation. Other treatment options will have been discussed with you by your Consultant. Please read this booklet carefully and ask the ward physiotherapist if you are unsure about any information or instructions within the booklet, when you come into hospital or at your pre-operative knee group appointment. Remember, once the surgeon has replaced your knee, it is up to you, with guidance from the ward staff, to follow the advice and carry out the exercises in order to achieve the best results from your new knee. About the knee Your knee has three parts: your thigh bone (femur), shin bone (tibia) and knee cap (patella). Where the bones meet, they are covered with a smooth substance called articular cartilage which helps them slide over each other easily. The joint is held together with tough bands of tissue called ligaments and is lubricated with a special fluid. Arthritis is a process in which the articular cartilage is destroyed: once cartilage has been damaged or destroyed it is gone for good as it cannot repair or heal itself. Serious injury, wear and tear and a family history of arthritis all seem to play a part. Arthritis can develop over many years or fairly rapidly and can follow serious injury. What is a Total Knee Replacement? Total knee replacement is a surgical procedure in which the knee is resurfaced with artificial parts. Your knee replacement will consist of a metal shell on the end of the femur and a metal and plastic trough on the tibia. A plastic button will be used to resurface the back of the kneecap if needed. 3
4 An artificial knee is not a normal knee but aims to: Provide pain relief Allow you to walk a good distance again Correct deformity i.e. give you a straight leg Remove symptoms such as giving way and locking Improve your quality of life The consultant will recommend this operation, however it is your choice to have this operation and the outcome is reliant on the amount of work you do. After the operation your deep osteoarthritic pain should resolve, however for a period of time this will be replaced with surgical pain from the trauma of the operation. It is important to take regular pain relief to allow you to perform your exercises. A total knee replacement is a large commitment and you must be motivated and prepared to spend time making the process a success. How long will I be in hospital? The average length of stay for a total knee replacement is 2-4 days, however this is dependant on your previous level of fitness, medical complications and home circumstances. If you are motivated you may be able to get home sooner. How long will my knee replacement last? All knee replacements have a limited life expectancy dependant on an individual s age, weight and level of activity. Their longevity will vary but all knee replacements will eventually wear out. Currently years is the expected life span but up to 5% of knee replacements will not last 10 years. There is no guarantee that your particular implant will last a specific length of time. It is important to follow your Surgeon s advice after surgery. 4
5 Why do implants fail? The most common reason for failure in a knee replacement is loosening or wear of the implant. This can usually be replaced with another one which is called a revision. Will I have restrictions after surgery? You will be advised against participating in high impact activities such as running, jumping, squash, singles tennis and contact sports. Will I notice anything different about my knee? You will notice some numbness on the outside of the scar. The area around your scar may feel warm for up to six months. In the initial post-operative period you will find your knee becomes stiff, this will improve with regular exercises. Initial swelling in your knee should settle in six weeks however your knee can continue to swell following activity for about a year. You may also notice some clicking as you move your knee due to the artificial surfaces coming together, this should improve in time. When will I be able to return to work? We recommend that most people will need at least six weeks off from work. Patients with more sedentary jobs may be able to return to work sooner. The timing of your return to work will depend on your progress. When will I be able to drive? Most people would not be fit to drive in the first six weeks. If you have had your right knee replaced you must be able to perform an emergency stop effectively. Driving will depend on your progress and individual circumstances. Please seek advice from a health professional or at your six week follow up if you are unsure. Remember to let your insurance company know you have had an operation. 5
6 Advice while you are waiting for your knee replacement General exercise General exercise is always of benefit and continues to be so whilst you are on the waiting list. It will also help your recovery following your operation. You may find that gentle exercise (within your limits of pain) such as cycling, swimming, or walking with periods of rest in between are of benefit. Specific exercise Exercising the muscles around the joint will help to maintain or possibly improve the strength of your muscles and also the range of movement of the joint. This will also benefit you after your operation. These exercises will be taught to you at the Pre-operative Knee Group. General health Keep yourself as fit and healthy as possible whilst you await your operation. This will greatly help with your recovery. If your general health deteriorates, it is important to contact your GP so that problems may be dealt with before your operation. In particular it is beneficial to stop or at least reduce, smoking. Pain relief If you are experiencing pain in your joint and you are not taking any pain medication, or the medication you are taking is not effective, your GP may be able to prescribe something to relieve your pain. Load reduction Reducing the pressure taken through the knee may also help with the pain. You may find that using a walking stick, (held in the hand on the opposite side to the affected knee) will help reduce pressure whilst you are walking. Dieting to lose weight will reduce your anaesthetic risks and improve the life of the prosthesis. Adequate rest periods and avoidance of unnecessary strain also help to reduce the pressure on your knee joint. 6
7 Skin and dental care If you have any cuts, abrasions, rashes or other skin conditions around your knee, leg or foot please see your GP as this may delay your surgery if left untreated. It is important to pay particular attention to foot hygiene. It is advisable to visit a dentist to ensure your teeth and gums are in good order prior to your operation. Infection in your teeth or gums may spread to your knee joint if left untreated. Enhanced Recovery Programme When you are admitted to hospital for your operation you will be taking part in an enhanced recovery programme. This programme of care aims to help you recover quickly and safely. The Enhanced Recovery Programme is about improving outcomes and speeding up the recovery period after your surgery, as well as reducing complications. For the programme to be successful, it is important that you actively participate in your own recovery programme and take responsibility for certain aspects of your recovery. This programme is different to traditional care and can improve your recovery considerably. The programme particularly focuses on: Reducing the physical stress of the operation A structured approach to immediate post-operative management, including pain relief Early mobilisation Early return to normal diet Some patients will be able to benefit from all aspects of this programme, whilst others will be able to benefit from just some aspects of it. This will depend on several factors, particularly your state of health and fitness at the outset. However we will endeavour to use as much of the programme as is practicable in each individual patients case. 7
8 Preload A key aspect of your enhanced recovery programme is that you will be given a carbohydrate (sugary) drink before your surgery. This drink is called preload. These drinks have several benefits to your recovery. They will: give you energy to help you recover reduce the risk of nausea (sickness) help your wounds heal reduce the risk of infection generally aid your recovery. You will receive the carbohydrate drinks at your pre-assessment clinic appointment. Preload: Preparation Guidelines Step 1 Pour 400ml of water into a cup Step 2 Add the contents of the sachet/s of preload into the cup, stir continuously until the powder has dissolved Step 3 Drink as directed below When to take preload Evening before surgery Eat your normal evening meal along with 2 sachets of preload 2 sachets of preload in 400mls of water 8
9 If your surgery is scheduled for the morning You should have nothing to eat or drink after 2am, but you may have a small amount of water and your carbohydrate drink, up to 2 hours before your operation. 1 sachet of preload in 400mls to be finished by 6am If your surgery is scheduled for the afternoon You should have a light breakfast before 6.30am, and then have nothing except a small amount of water and your carbohydrate drink up to 2 hours before your operation. 1 sachet of preload in 400mls to be finished by 10.30am These instructions will be clarified during a phone call that you will receive the evening prior to admission from the Elective Surgical Unit (ESU). It may be unknown whether you are on a morning or afternoon list at the preadmission clinic stage. On the day before your surgery you will be able to eat and drink as normal. In order to maximise your nutritional status we recommend you include a few extra snacks in your diet. You can eat a normal diet up to 6 hours before your surgery. What happens before the operation? Pre-operative Knee Group It is essential that you attend the group at any time before your operation as it will be beneficial in order to help you prepare for your operation. The group is run by the Orthopaedic Physiotherapy team and it includes an informative talk on what to expect during your post-operative recovery, the importance of exercises for your knee replacement, and preparing for your discharge. It also includes a practical session involving exercise and mobility aid (elbow crutches) demonstrations. You will have the opportunity to meet others who are going to have a total knee replacement and you can ask questions. Please telephone the Physiotherapy Department to book your place in the Pre-operative Knee Group Call
10 Pre-assessment Clinic A few weeks before your operation you will be asked to attend the Pre-assessment Clinic. A thorough medical assessment will be carried out to make sure you are medically fit enough for surgery. At this clinic routine pre-operative tests including urine, blood, ECG (heart trace) and x-rays will be carried out. You will also be screened for MRSA (Methicillin Resistant Staphylococcus Aureus), a normally harmless bacterium that can on occasions cause wound infections. Part of the pre-admission process involves gathering accurate information regarding current medication, which is important for us to give you the best possible care. Please bring a list of your regular medication, including any inhalers, eye drops, patches or creams as you will be asked what medication you usually take, the dosage and how often. It may also be helpful for you to bring in the repeat prescription request forms from your GP surgery. Please also remember to mention any medicines you buy regularly (that are not prescribed by your doctor) and any herbal or vitamin supplements that you might be taking. In anticipation of the surgery you may be asked to stop taking some of your medications before coming in to hospital (e.g. if you take warfarin) and you may be prescribed alternative medications leading up to the operation. You will be advised by a Nurses or a Doctor if this is necessary. This appointment will also provide you with a further opportunity to speak to your Consultant, their Registrar or an Extended Scope Practitioner. You will also be asked to sign a consent form if you have not already done so. 10 You can be in clinic for 3-4 hours Before coming in to Hospital Ensure that you assess your home for ease of walking with crutches, sticks or a walking frame. Remove any loose rugs, which may cause you to trip Put objects that you use regularly within easy reach so that you do not have to bend or stretch
11 Identify people who will help you do your shopping, washing and cleaning Arrange transport in and out of hospital Please make sure that you have at least 2-3 weeks supply of any regular medication which you are taking. It is very important that we know what medications you are taking. Admission day In addition to your personal belongings you will need to bring the following: Any regular medication you are taking (at least 2 weeks supply and in their original containers) along with a copy of your repeat prescription request forms from your GP surgery if you have them. Please also bring any medications which you were asked to stop taking before the procedure, as you may need to restart these whilst in hospital. Please let us know if there have been any changes to your regular medications between your pre-assessment visit and the day of surgery Appropriate foot wear e.g. trainers or well fitting shoes (NOT mules or flip flops ) Loose comfortable clothing (you will be encouraged to dress normally the day after your operation) Nightwear Towels and toiletry bag Please leave any valuables at home The operation The operation will usually take place under a general anaesthetic, but it is sometimes done with a spinal anaesthetic where your legs will be completely numb. The anaesthetist will discuss this with you before your operation takes place. The surgery takes approximately 1-2 hours. You will remain in the recovery area until your condition is stable and your pain is well controlled. 11
12 Recovery Following surgery you will be returned to the ward lying on your back with a thick dressing over your knee. Nerve blocks inserted by the Anaesthetist in the operating theatre may leave your leg feeling weak and numb. You may have some of the following drains or tubes attached to you:- Wound drain(s): there may be a bottle attached via a tube to your knee wound. It prevents excess swelling and bruising and is usually removed after 24 hours Fluids: you may have a tube in your arm connected to a drip to give you fluid until you are eating and drinking properly Catheter: if you are unable to pass water following your operation, you may need a short term catheter Changes to medications It is normal to have some pain after the surgery and so you will be offered regular painkillers. It is very important that you take the painkillers regularly to keep your pain under control and speed up your rehabilitation. The painkillers can cause constipation but early walking and exercise can help this and if necessary you may be prescribed laxatives. If you wish to know more about the types of pain relief available, please discuss it with your doctor or pharmacist. If you want any other information before you come into hospital, booklets about pain relief are available in the orthopaedic clinic. You may also be prescribed some medications to help the strength of your bones, such as calcium & vitamin D supplements and possibly a bisphosphonate to help bind the calcium into the bones. Please follow the instructions on how to take these carefully. You may also be prescribed medications to reduce the risk of a venous thromboembolism or VTE, which is a type of blood clot. The risk of developing a VTE may be increased by having surgery and being less mobile. During your hospital stay you may be prescribed medications to thin the blood. You may also need to complete a course when you go home. 12
13 Please read the patient information leaflets supplied with new medications discuss any concerns with your Doctor or Pharmacist. Physiotherapy You will begin physiotherapy as soon as possible after your operation. This can be the same day as your operation. The physiotherapist will teach you knee exercises, which you should continue independently. You will be shown how to safely get out of bed, stand and transfer into a chair. The physiotherapist will progress your mobility as able and prior to discharge you will be shown how to climb stairs safely with aids, if needed. Bed exercises following knee surgery These exercises should be performed at least 4 times a day. 1. Deep Breathing Exercises (to prevent a chest infection) Sit upright in your bed or chair. Take 3 slow deep breaths, in through your nose and out through your mouth. Keep your shoulders relaxed. Repeat every minutes you are awake. 2. Ankle Pumping (To prevent blood clots) In the bed or chair, pump your feet up and down. If your heel becomes sore please elevate using pillows Repeat as often as possible. 13
14 3. Bridging (To prevent bedsores) Lying on your back, bend your non-operated leg and push through this and your arms to lift your bottom off the bed. Repeat as often as possible Please only perform the exercises marked with a tick in the Repeat all exercises at least 4 times per day 4. Static Quads Lying on your back. Pull your foot up and push your operated knee into the bed tightening your thigh muscles. Hold for 5 seconds Repeat 10 times 5. Hanging Out Place heel on roll (heel must be high enough so calf and knee are off the surface). Hold for up to 20 minutes This should be done when icing and resting your leg. You can also tighten and relax thigh muscle in this position. 14
15 6. Heel slides in bed Lying on the bed, place a plastic bag under the heel of your operated leg and slide your heel towards your bottom, you can use your hands to obtain as much bend in your knee as possible. You may use a plastic bag or doughnut under your heel to reduce friction. Hold for 5 seconds, then bend knee a little further before releasing. Repeat 10 times 7. Heel digs Lying on your back, bend the operated knee slightly. Push your heel into the bed. Hold for the count of 10 Repeat 10 times 8. Buttock clenching Lying on your back. Squeeze your buttocks firmly together. Hold for 5 seconds Repeat 10 times 15
16 9. Knee extension over roll (Inner Range Quads) Place a rolled towel under your knee, pull your foot up and keep the knee in contact with the pillow whilst straightening the knee. Hold for 5 seconds Repeat 10 times DO NOT LEAVE YOUR OPERATED KNEE RESTING ON A PILLOW AS THIS WILL STOP YOU GETTING A STRAIGHT KNEE Straight leg raise 11. Assisted knee flexion in sitting Lying on a bed. Pull your foot up and brace your knee straight. Lift the leg 5 inches off the bed keeping your knee straight. You should have your non operated leg bent up during this exercise. Hold for 5 seconds Then lower slowly back down to the bed. Repeat 10 times Sitting in a chair, slide your operated foot backwards along the floor to bend your knee as much as possible. Keeping your foot still, hold the arms of the chair and move your bottom forwards slowly. You should feel a stretch down the front of your knee as your knee bends. Hold for 5 seconds, then move your bottom back in the chair. Repeat 10 times.
17 Steps and stairs the safest technique Use a banister if available and take one step at a time Going up Un-operated leg Operated leg Walking Aid(s) Coming down Walking Aid(s) Operated Leg Un-operated leg PRICE regime Good leg up... Bad leg down Protection Use walking aids to help you carry out your daily life until advised by your Physiotherapist. Rest You should increase the amount of walking you do slowly and take regular periods of rest. Ice Ice is used to reduce the amount of swelling, and can help to relieve pain. Do not use ice if you have cold allergies or circulatory problems. On the ward the physiotherapist will show you how to use a Cryocuff. Before using ice make sure you have normal sensation on the knee. Do not put ice directly on the skin. At home apply a bag of frozen peas or crushed ice wrapped in a damp towel onto the knee. Rest the ice on top of the knee, never rest the knee onto the ice. It is normal for the area to go red and slightly numb during icing. After the ice has been on for 5 minutes check the skin. If you notice that the area has gone white remove the ice immediately. If not, leave the ice in place for 20 minutes if you can tolerate it. 17
18 Compression Your Physiotherapist may provide you with a tubigrip which you should wear throughout the day. Elevation Elevate the area as much as possible to help reduce swelling. The most effective way to do this is by spending one hour in the morning and afternoon lying flat on the bed with your operated leg resting on pillows so that your heel is higher than your heart. Ensure that your knee is straight whilst the leg is elevated. Discharge from hospital Before you go home you must; Have an acceptable range of movement Be able to get up from a low toilet (you may be referred to the Occupational Therapist if this is problematic for you) Be able to walk independently and safely with the walking aid of choice Be able to safely negotiate stairs with the same set up as yours at home Be able to independently carry out your individualised home exercise program On discharge the nursing staff will give you; Medication as appropriate A letter for your GP A sick certificate if required Your physiotherapist will discuss follow-up physiotherapy arrangements. If you are coming back to the RSCH, an appointment will be made for you. If not, a referral will be sent to your local hospital and they will contact you with an appointment. If they have not contacted you within 2 weeks please let us know 18
19 Written instructions regarding follow up care for your wound and further appointments etc. You may be given stockings to wear at home. Practice nurse appointment Please do the following: Continue your exercises as instructed by your physiotherapist. You will need to continue to take your pain medication to allow you to do these. Apply your ice pack/frozen peas regularly Try to take regular daily walks increasing the distance as you are able (however walking does not replace your exercise program) Keep your wound clean and dry Take a daily rest on your bed for at least an hour elevating your knee above heart level Contact your GP if there is increased pain or swelling in your calf Contact your GP if you are worried about signs of infection in your knee e.g. red, hot and swollen and/or oozing wound Please avoid the following: Sitting for too long as you may become stiff and find it difficult to get up and going again Resting with a pillow under your knee Stepping your operated foot in front when sitting onto the chair Walking with a stiff knee It will take at least 12 weeks for your knee to feel like a knee and it will go on improving for 18 months 19
20 Advice after six weeks Housework Increase the amount of housework that you do over the next few months. Be careful when bending or twisting. You may kneel on your knee replacement if it is comfortable to do so but always kneel on something soft. It may take 1-2 years to be able to kneel on your knee. Wound If your wound is tender to touch you may massage it firmly using moisturising cream to desensitise the skin and underlying tissues. You should only begin to massage once the stitches/staples have been removed and the wound is clean and dry (normally at around 2 weeks post operation). Sleeping You may adopt any sleeping position that is comfortable. You may wish to put a pillow between your knees. Avoid placing a pillow under your knee. If you are having problems sleeping because of pain please see your GP. Sport/leisure Most sporting activities can be resumed after 3-6 months depending on comfort and level of competition. Low impact sports are such as swimming, cycling, and golf are usually not a problem after your knee replacement. High impact sports, such as jogging, squash and football are not recommended. Gardening should be done with care. If possible use a kneeling stool and long handled tools. Travelling Ideally you should not travel within 3 months of your surgery. Sitting for prolonged periods increases the risk of developing Venous Thromboembolism (VTE). We do not recommended any form of prolonged travel within 6 weeks of surgery. 20
21 Exercise Continue with the exercises as instructed by your physiotherapist. This will increase your strength and maintain a functional range of movement. You will need to continue some of your exercises to successfully regain your knee strength for the first year, and possibly the life of the knee replacement. Progress your walking distance, as you feel comfortable. Maintenance exercises Please only perform the exercises marked with a tick in the Repeat the exercises once per day. 1. Wall Slides Place your back against the wall, step your feet 2 foot from the wall. Slide your back down the wall performing a small squat. Keep your knees over your toes. Repeat 10 times. 21
22 2. Balance Stand by a stable surface. Stand on your operated leg with your knee slightly bent. Try to take your hands off the supporting surface for 10 seconds. Progress by standing barefoot on different surfaces e.g. carpet/pillow. Progress again by moving your arms around. 3. Standing from a chair Sitting in a chair, place both feet level with one another. Stand up from the chair without using your hands, try to take the weight evenly through your legs. Repeat 10 times 22
23 4. Resisted Knee Flexion Sit in a chair, hook your non-operated leg behind the operated leg. Attempt to pull your operated leg under the chair and resist this movement with the other leg. Repeat 10 times 5. Resisted Knee Extension Sitting in a chair. Place your non-operated leg in front of the operated leg. Attempt to straighten your operated leg whilst resisting with your other leg. Repeat 10 times 23
24 6. Patellar Mobilisation Hold your kneecap as shown. Move your kneecap from side to side 5 times and up and down 5 times. 7. Hanging out (See Post Op Exercise 5) Continue to hang out your knee to maintain extension 24
25 Possible complications (Your Consultant will discuss possible complications with you) Anaesthetic and medical We will make sure you are medically fit for your operation and measures will be used to reduce the risk of blood clots occurring. Any anaesthetic and major operation carries a very small increased risk of being complicated by the following medical conditions: Heart attack Stroke Venous Thromboembolism (VTE) (blood clot in the vein) Complications affecting the knee are less common. These include; Stiffness Persistent knee pain Infection in the joint Loosening of the prosthesis Fractures around the prosthesis Blood transfusion During and after the operation you will lose some blood. The blood you lose will usually be made up by your own body in the weeks after surgery. A blood transfusion is required in roughly less than 2% of patients. Blood needed for transfusion is always tested and matched to your own blood but still carries a very small risk associated with it such as:- 1. Rejection and reaction to the donor blood 2. Transmission of infection 25
26 Infection An infection can occur after any operation but it is particularly important that you understand its consequences when undergoing a knee replacement. You must look out for signs of an infection e.g. red, hot skin around the knee, feeling unwell or fever. Prophylactic antibiotics (to reduce the risk of infection at the time of the surgery) are routinely used. If you are concerned you may have an infection you should see the Orthopaedic team at the hospital via Accident and Emergency or Fracture Clinic. Venous thromboembolism This is possible following any surgery. You will be given daily medication to reduce this risk and will also be taught preventative circulatory exercises by your physiotherapist which you should begin immediately after your operation. Haematoma Bruising can develop around the wound and this can seep down towards your ankle and foot. This is not usually a problem and will resolve over a few weeks. Occasionally a more significant bruise (haematoma) occurs under the wound and this can delay healing. An operation may be required to release this collection of blood. This is more likely to happen if you are taking aspirin, clopidogrel, warfarin or an anti-inflammatory medication (e.g. Ibuprofen, Voltarol). Please inform us at your preassessment appointment if you are taking this type of medication. The risk is reduced by stopping it for a week before your operation. Leg swelling Leg swelling is quite common after the operation. It tends to improve each night with rest and elevation. You are advised to use the PRICE regime to reduce swelling. If it is worsening or becomes painful then you need to seek advice as one of the causes of swelling in the first six weeks is venous thromboembolism. Swelling may remain around the knee for up to 12 months after the operation. 26
27 Vascular injury Where there is pre-existing vascular damage there may be damage to the arteries behind the knee. This will be identified and treated quickly should it arise. Nerve damage During the operation nerves in your leg can be damaged but this is rare. Nerve damage causes numbness and tingling in your leg. It can also weaken your ankle or foot. Instability If your knee gives way or buckles this can interfere with your daily life and can be painful. It also increases the wear and tear on your new knee. This will be improved by strengthening exercises, however, you should seek advice if this persists. You may need to wear a brace for a period of time. General advice If you develop pain in your calf or chest, or your wound becomes red, swollen, hot and/or oozing, please contact your GP urgently, or come to the Accident & Emergency department at the hospital. If you have any further questions that are not answered by this booklet, please ask the ward staff who are there to help you. You still have pain in your knee Your knee may carry on hurting despite the operation. Your surgeon will investigate to see if a cause can be found but sometimes they won t be able to find one. Usually the pain will improve but this can take several months and a background ache may persist. You have problems bending your knee If you had a stiff knee before your operation you may not gain a full range of movement afterwards. Less than 100 degrees of movement can lead to functional problems. If you have not achieved this by 3 months post surgery you may benefit from Manipulation Under Anaesthetic (MUA). 27
28 Please bring this booklet with you to all your appointments regarding your knee replacement. Appointments record Pre-assessment Clinic (in Fracture Clinic, RSCH) on: Pre-Operative Knee Group Date: Operation Date: Estimated Discharge Date Post Operative Physiotherapy appointment: At: On: If you are not having physiotherapy at the RSCH a referral will be sent to your local hospital and they will contact you with an appointment. Follow up Orthopaedic Appointment (in fracture clinic) on: 28
29 Reference source National Joint Registry (NJR) Website Further information NHS Website British Orthopaedic Association Website boa.ac.uk Arthritis Research UK Website arthritisresearchuk.org Helpful telephone numbers Fracture Clinic: Admissions Desk: ext 4355 Physiotherapy Department: Occupational Therapy Department: ext 4766 Bramshott Ward: ext 4064/4065 Ewhurst Ward: ext 4073/
30 Notes 30
31 Notes 31
32 Contact details If you require any further physiotherapy advice please leave a message for the Orthopaedic Physiotherapists on We will then call you back. PALS and Advocacy contact details Contact details of independent advocacy services can be provided by our Patient Advice and Liaison Service (PALS) who are located on the right hand side as you enter the main reception area. PALS are also your first point of contact for health related issues, questions or concerns surrounding RSCH patient services. Telephone: rsc-tr.pals@nhs.net Opening hours: 9.00am 3.00pm, Monday to Friday If you would like information documents in large print, on tape or in another language or form please contact PALS. Past review date: October 2017 Future review date: October 2020 Author: Susie Golding & Laura Holdway PIN Royal Surrey County Hospital NHS Foundation Trust 2017
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Non weight bearing advice (post operative)
 Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET
 TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Anterior Cruciate Ligament (ACL) Reconstruction
 Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Northumbria Healthcare NHS Foundation Trust. Knee Arthroscopy. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Information for Patients having Total Knee Replacement Surgery
 Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Total hip replacement with hip precautions
 Total hip replacement with hip precautions Your guide to a successful outcome following a surgery Orthopaedic Department Patient information leaflet Contents What is a hip replacement? 3 Advice while you
Total hip replacement with hip precautions Your guide to a successful outcome following a surgery Orthopaedic Department Patient information leaflet Contents What is a hip replacement? 3 Advice while you
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet
 Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet Page 1 Arthroscopy of the knee joint Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. This booklet
Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet Page 1 Arthroscopy of the knee joint Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. This booklet
Arthroscopic subacromial decompression of the shoulder
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Arthroscopic subacromial decompression of the shoulder Physiotherapy Department Information booklet for Name of Patient: Date:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Arthroscopic subacromial decompression of the shoulder Physiotherapy Department Information booklet for Name of Patient: Date:
Stabilisation of the shoulder joint
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Knee arthroscopy surgery
 Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
Cheilectomy. Your guide to a successful outcome following surgery. Orthopaedic Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Cheilectomy Your guide to a successful outcome following surgery Orthopaedic Department What is Cheilectomy? This is surgery
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Cheilectomy Your guide to a successful outcome following surgery Orthopaedic Department What is Cheilectomy? This is surgery
Total Elbow Replacement Operation
 Total Elbow Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact:
Total Elbow Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact:
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
Physiotherapy following peri acetabular osteotomy (PAO) surgery
 Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
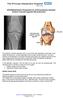 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
Excision of Morton s Neuroma
 Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
Physiotherapy advice prior to your. Total Knee Replacement
 Physiotherapy advice prior to your Total Knee Replacement Important Please read this booklet and start the exercises before coming in for your surgery. Remember to bring this booklet in to hospital with
Physiotherapy advice prior to your Total Knee Replacement Important Please read this booklet and start the exercises before coming in for your surgery. Remember to bring this booklet in to hospital with
Total knee replacement
 Total knee replacement Inpatient and home exercises Information for patients MSK Orthopaedic Inpatients (Therapy) When you go home from hospital following your knee replacement, a referral will be made
Total knee replacement Inpatient and home exercises Information for patients MSK Orthopaedic Inpatients (Therapy) When you go home from hospital following your knee replacement, a referral will be made
For more information on arthritis and knee replacements please see:
 Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Physiotherapy Services. Physiotherapy Guide. Hip Replacement
 Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Knee arthroscopy surgery
 Golden Jubilee National Hospital NHS National Waiting Times Centre Knee arthroscopy surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Arthroplasty
Golden Jubilee National Hospital NHS National Waiting Times Centre Knee arthroscopy surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Arthroplasty
Patient Information Leaflet. Knee Joint Replacement
 Patient Information Leaflet Knee Joint Replacement Appointments Pre-operative assessment clinic Date: Time: Date of admission to hospital Date: Time: Operation date Date: Time: Follow-up clinic appointments
Patient Information Leaflet Knee Joint Replacement Appointments Pre-operative assessment clinic Date: Time: Date of admission to hospital Date: Time: Operation date Date: Time: Follow-up clinic appointments
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Knee Replacement Patient Information
 Knee Replacement Patient Information This information sheet is designed to help you to understand what a knee replacement involves. I perform knee replacements frequently, several times each week, and
Knee Replacement Patient Information This information sheet is designed to help you to understand what a knee replacement involves. I perform knee replacements frequently, several times each week, and
Pa#ent Informa#on for Consent
 Pa#ent Informa#on for Consent ER_OS02 Total Knee Replacement Enhanced Recovery Expires end of November 2018 Local Informa#on For further informa0on locally you can contact the Pa0ent Advice & Liaison Service
Pa#ent Informa#on for Consent ER_OS02 Total Knee Replacement Enhanced Recovery Expires end of November 2018 Local Informa#on For further informa0on locally you can contact the Pa0ent Advice & Liaison Service
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
Knee Replacement Surgery
 Knee Replacement Surgery Physiotherapy Department Patient information Experience has shown that patients undergoing an operation recover more quickly if they understand what is going to happen. Being aware
Knee Replacement Surgery Physiotherapy Department Patient information Experience has shown that patients undergoing an operation recover more quickly if they understand what is going to happen. Being aware
TOTAL KNEE ARTHROPLASTY (Total Knee Replacement) The Knee Joint
 (Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
(Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
Arthroscopy Day Case. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Arthroscopy Day Case An information guide Arthroscopy Day Case Arthroscopy Day case Post-operative regime The post-operative rehabilitation
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Arthroscopy Day Case An information guide Arthroscopy Day Case Arthroscopy Day case Post-operative regime The post-operative rehabilitation
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron
 Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
Rehabilitation programme after hemiarthroplasty surgery
 Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Physiotherapy advice prior to your. Total Knee Replacement
 Physiotherapy advice prior to your Total Knee Replacement IMPORTANT NOTICE Please read this booklet prior to your surgery. Please bring it onto hospital with you. 2 About your knee Your knee has 3 parts;
Physiotherapy advice prior to your Total Knee Replacement IMPORTANT NOTICE Please read this booklet prior to your surgery. Please bring it onto hospital with you. 2 About your knee Your knee has 3 parts;
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
Knee arthroscopy surgery
 Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Bunion Surgery. Patient information Leaflet
 Bunion Surgery Patient information Leaflet April 2017 What is a bunion? A bunion is a bony lump on the side of your foot at the base of your big toe (see figure 1). This may be an isolated problem but
Bunion Surgery Patient information Leaflet April 2017 What is a bunion? A bunion is a bony lump on the side of your foot at the base of your big toe (see figure 1). This may be an isolated problem but
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Lower back pain. Physiotherapy Department
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Lower back pain Physiotherapy Department Lower back pain This leaflet is intended for people who have been diagnosed with generalised
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Lower back pain Physiotherapy Department Lower back pain This leaflet is intended for people who have been diagnosed with generalised
Manipulation under Anaesthetic (MUA) and Arthroscopic Release Operation
 Manipulation under Anaesthetic (MUA) and Arthroscopic Release Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats.
Manipulation under Anaesthetic (MUA) and Arthroscopic Release Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats.
Arthroscopic capsular release. Information for patients Orthopaedics - Upper Limb
 Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Your home exercise and activity diary. Information for thoracic patients having lung resection surgery
 Your home exercise and activity diary Information for thoracic patients having lung resection surgery Contents Introduction 3 Physiotherapy at home before your operation General advice regarding exercises
Your home exercise and activity diary Information for thoracic patients having lung resection surgery Contents Introduction 3 Physiotherapy at home before your operation General advice regarding exercises
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Reversed geometry shoulder replacement
 Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Rehabilitation following your hip fracture
 Page 1 of 8 Rehabilitation following your hip fracture Introduction The information in this leaflet is a general guide to help you to have the best recovery following your hip fracture. If you have any
Page 1 of 8 Rehabilitation following your hip fracture Introduction The information in this leaflet is a general guide to help you to have the best recovery following your hip fracture. If you have any
Facet joint injection advice
 Patient Information Service Day surgery unit Facet joint injection advice SOU425_034175_0615_V1.indd 1 26/02/2016 09:11 Facet joints (Also known as Zygoapophyseal joints) Facet joints are the joints between
Patient Information Service Day surgery unit Facet joint injection advice SOU425_034175_0615_V1.indd 1 26/02/2016 09:11 Facet joints (Also known as Zygoapophyseal joints) Facet joints are the joints between
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Lumbar decompression or discectomy
 Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
ACL Reconstruction Physiotherapy advice for patients
 ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
INFORMATION FOR PATIENTS. Reverse shoulder replacement operation
 INFORMATION FOR PATIENTS Reverse shoulder replacement operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
INFORMATION FOR PATIENTS Reverse shoulder replacement operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
About Knee Replacements
 Why have I received this leaflet? About Knee Replacements You have decided or are considering undergoing total knee replacement surgery. I will have discussed with you in clinic that knee replacements
Why have I received this leaflet? About Knee Replacements You have decided or are considering undergoing total knee replacement surgery. I will have discussed with you in clinic that knee replacements
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Total Knee Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Patient Information Physiotherapy after Total Knee Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Physiotherapy after your hip arthroscopy
 Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
This booklet has been developed to help guide you through your post-operative rehabilitation.
 Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients
 Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients This leaflet will provide you with general information about capsular release surgery. It will briefly explain the operation procedure
Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients This leaflet will provide you with general information about capsular release surgery. It will briefly explain the operation procedure
Total Knee Replacement: Your Guide to Preparation and Recovery
 Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Information for Patients having
 Total Hip Replacement Surgery Information for Patients having Total Hip Replacement Surgery Hello! You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written
Total Hip Replacement Surgery Information for Patients having Total Hip Replacement Surgery Hello! You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written
High Tibial Osteotomy surgery
 Golden Jubilee National Hospital NHS National Waiting Times Centre High Tibial Osteotomy surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Golden Jubilee National Hospital NHS National Waiting Times Centre High Tibial Osteotomy surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
A patient s guide to the. physiotherapy exercises and advice following excision of ilium with fibula strut
 A patient s guide to the physiotherapy exercises and advice following excision of ilium with fibula strut This booklet outlines the likely physiotherapy treatment you will receive while in hospital. Although
A patient s guide to the physiotherapy exercises and advice following excision of ilium with fibula strut This booklet outlines the likely physiotherapy treatment you will receive while in hospital. Although
GUIDELINES FOR REHABILITATION OF TOTAL KNEE REPLACEMENTS
 Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Knee Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Chester Knee Clinic at Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Consultant Orthopaedic Knee Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Chronic Low Back Pain
 Chronic Low Back Pain This leaflet has been produced by Senior Physiotherapists working at the Queen Victoria Hospital NHS Foundation Trust. It has been designed to give you accurate up-to-date knowledge
Chronic Low Back Pain This leaflet has been produced by Senior Physiotherapists working at the Queen Victoria Hospital NHS Foundation Trust. It has been designed to give you accurate up-to-date knowledge
Femoral endarterectomy
 Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Arthroscopy of the Knee
 Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Further information You can get more information and share your experience at
 OS02 Total Knee Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS02 Total Knee Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
Northumbria Healthcare NHS Foundation Trust. Preparing For Foot and Ankle Surgery. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Preparing For Foot and Ankle Surgery Issued by the Orthopaedic Department This leaflet gives you information about what is involved in foot and ankle surgery.
Northumbria Healthcare NHS Foundation Trust Preparing For Foot and Ankle Surgery Issued by the Orthopaedic Department This leaflet gives you information about what is involved in foot and ankle surgery.
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Tibia intramedullary nail operation physiotherapy advice
 Tibia intramedullary nail operation physiotherapy advice This leaflet gives you advice about recovering after your operation. It also explains exercises you should do each day, things to look out for and
Tibia intramedullary nail operation physiotherapy advice This leaflet gives you advice about recovering after your operation. It also explains exercises you should do each day, things to look out for and
Foot and Ankle Surgery
 Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Hip Resurfacing Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you will
Patient Information Physiotherapy after Hip Resurfacing Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you will
Physiotherapy Following Your Spinal Discectomy
 Physiotherapy Following Your Spinal Discectomy Patient information How to contact us Physiotherapy Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire,
Physiotherapy Following Your Spinal Discectomy Patient information How to contact us Physiotherapy Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire,
PILGRIM HOSPITAL Department of Orthopaedics TOTAL KNEE REPLACEMENT. Patient Information & Exercise Folder
 PILGRIM HOSPITAL Department of Orthopaedics TOTAL KNEE REPLACEMENT Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Boston Lincolnshire
PILGRIM HOSPITAL Department of Orthopaedics TOTAL KNEE REPLACEMENT Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Boston Lincolnshire
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated
 Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
Exercises following Copeland Surface Replacement Arthroplasty (CSRA)
 Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Total Hip Replacement. Information and exercises for patients
 Total Hip Replacement Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy
Total Hip Replacement Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy
This advice and exercises have been selected to help you manage the symptoms of your arthritis
 This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
You and Your Knee Joint Replacement. Joint School Surgical Rehabilitation Team
 You and Your Knee Joint Replacement Joint School Surgical Rehabilitation Team Housekeeping Length of Session Questions during the session Fire Toilet Facilities Moving around to relieve discomfort Enhanced
You and Your Knee Joint Replacement Joint School Surgical Rehabilitation Team Housekeeping Length of Session Questions during the session Fire Toilet Facilities Moving around to relieve discomfort Enhanced
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan
 Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Endovenous Laser Treatment (EVLT)
 Endovenous Laser Treatment (EVLT) Day Surgery Unit Patient information leaflet What is Endovenous Laser Treatment (EVLT)? Endovenous laser therapy is a treatment for varicose veins which seals the vein
Endovenous Laser Treatment (EVLT) Day Surgery Unit Patient information leaflet What is Endovenous Laser Treatment (EVLT)? Endovenous laser therapy is a treatment for varicose veins which seals the vein
Knee joint arthroscopy
 Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Maternity Information Leaflet
 Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
Maternity Information Leaflet Recovery following your Caesarean Section This leaflet provides information to help you recover following a Caesarean Section (CS) birth. Recovery after a CS may take a little
INFORMATION FOR PATIENTS. SLAP lesion repair operation
 INFORMATION FOR PATIENTS SLAP lesion repair operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions you may have
INFORMATION FOR PATIENTS SLAP lesion repair operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions you may have
Leg artery bypass (fem-pop bypass)
 Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
