GREATER TROCHANTERIC PAIN SYNDROME CLINICAL PRACTICE GUIDELINE
|
|
|
- Madeleine Wilson
- 6 years ago
- Views:
Transcription
1 GREATER TROCHANTERIC PAIN SYNDROME CLINICAL PRACTICE GUIDELINE Disclaimer This guideline is intended as an aid for clinicians treating patients diagnosed with greater trochanteric pain syndrome, utilizing an -based load management treatment strategy. Progression is time and criterionbased, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine at if questions arise. Background Greater trochanteric pain syndrome (GTPS) has been defined as lateral hip pain to palpation of the peritrochanteric region. The pain can radiate down the thigh and into the posterior hip, but rarely distal to the knee. Previously, the cause of pain has been attributed solely to trochanteric bursitis. However, the origin of pain can include the trochanteric bursa, gluteus medius and minimus tendons, and iliotibial band. MRI examination in studies involving GTPS show trochanteric bursitis was an uncommon finding and was not found in isolation; when found, bursal distension coexisted with gluteal pathology. 15 Recent studies have shown gluteal tendinopathy to be the primary cause of lateral hip pain. 1 The greatest incidence of GTPS often occurs between the fourth and sixth decades of life with a female to male ratio of 4:1. 15 Recent studies of gluteal tendinopathy demonstrate the deep undersurface fibers of the gluteal tendons preferentially develop pathology and tears and yet are relatively stress-shielded from tensile load in the lower ranges of hip abduction. 1 They are exposed to high compressive loads in the ranges of hip adduction against the bony insertion. 1 Normal daily function of the hip is in the low ranges of abduction or slight hip adduction. 1 These compressed sides of the tendons adapt to form somewhat of a cartilaginous or atrophic area in response to a lack of tensile load. 15 This makes the tendon vulnerable to becoming symptomatic even with small changes in activity. For this reason, tendinopathy can occur in the absence of a traditional overuse injury model and explains how tendinopathy is more common in the older patients. 15 Because the turnover rate of collagen decreases with advancing age, it may take longer for older athletes to recover from tendinopathy. 10 Compressive forces (not solely tensile loads) may be at fault and need correction for treatment of GTPS. A key determinant in rehabilitation progression of tendinopathy is whether or not a tendon reacts, or develops an increase in pain that does not return to baseline pain level within 24 hours. 5 Load management and prescribing effective loading variables (duration, frequency, nature, magnitude, direction, and intensity is important in guiding the rehabilitation process. Monitoring changes in pain and immediate adjustment of load is essential. The painmonitoring model includes use of an objective measure to assess pain intensity 0-10/10 to monitor exercise progression. It is recommended to assess at the same time every day at home. Progressive mechanical loading has been found to be an effective management strategy. Different modes of strength training, including isometric, isotonic, isolated eccentric, and isokinetic can be used to control pain, improve motor control, and enhance function in pathological tissue. Although traditional rehabilitation approaches have focused on isolated eccentric tissue loading, recent literature suggests that isolated eccentric exercise may not be a superior choice compared with other types of loading, particularly heavy-slow resistance (HSR) loading (resistance performed up to an individual s 6RM). 4 In fact, eccentric-based exercise may contribute to worse outcomes for an in-season athlete or be too high load for the tendon to tolerate to begin treatment. 5 HSR loading also has been found to promote better collagen turnover than isolated eccentric loading. 4 Important throughout rehabilitation, isometrics have been found to reduce pain while reducing cortical inhibition of muscles. Emerging research is indicating the presence of changes in central pain processing, such as central sensitization, in some cases of tendinopathy. Generally clinical management of tendinopathy should include aspects of load management and education, progressive mechanical loading, treatment of kinetic chain deficits, and a graded return to activity.
2 Definitions Strong level : supported by systematic review, meta-analysis, or >5 RCT Moderate level : supported by 3-4 RCT Low level : supported in 1-2 RCT or clinical case series Expert opinion: supported by case studies, s or opinions of the authors Summary of Recommendations Risk factors Sudden increase in activity Repetitive compressive/tensile loads Lumbopelvic and LE mechanics Female>40 years Differential Diagnosis Gluteal tendon tear Ischiofemoral impingement, quadratus femoris tear, piriformis syndrome Intra-articular hip pathology (hip OA, AVN, FAI/labral tear, SCFE) Stress fracture Lumbar/SI pathology Systemic disease (CA, RA) Examination Gait, posture (lumbopelvic), kinetic chain, functional movement assessment Lumbar/SI screen Special tests: 30 second SLS, resisted external derotation test, TTP over Greater trochanter, painful hip abductor MMT Outcome tools: VISA-G, HOOS, HOS Pain Reduction and Load Management (isometric loading and avoiding positions of compression)- refer to appendix Isotonic Loading (Heavy-slow resistance through concentric-eccentric phases) Energy-Storage Loading (plyometric loading) Return to Activity/Sport Phases of Progression Interventions Criteria for Discharge Patient education regarding load management (Lateral hip precautions) Gluteal isometric contractions with tendon in shortened positions Progressive muscle-tendon loading program Correction of kinetic chain deficits (emphasis on mechanics during gait and ADLs) Full ROM/strength/power Pain-free resistance test, high load, in compressed positions Achieved patient goal(s) Proper long-term maintenance program implemented for self-management of symptoms RTS activity without reactive pain
3 Examination Subjective Symptoms commonly attributed to GTPS include pain/difficulty with: lying on the ipsilateral side prolonged standing or walking climbing up or down stairs sit to stand transfers walking up/down hills or inclines sitting Objective MMT hip abduction/dynamometry Hip ROM Lumbar spine and SI screening Pain provocation with palpation to greater trochanteric region Examination of gait on level surfaces and stairs/examination of body mechanics with transfers and sport-specific activity Lumbopelvic control during high and low level tasks Special Tests 30 second single leg stand test: Recommended for up to 30 seconds (or until onset of greater trochanteric pain) allowing light fingertip support with trunk maintained in vertical position. Although not part of the test, observing the patient s ability to control the pelvis can help guide treatment (Low load test) 1 Lateral hip pain with resisted external derotation test 3 Patient: supine with hip and knee passively flexed up to 90 degrees. Hip passively placed into external rotation. If any pain is present in that position, slightly decrease the external rotation position just enough to relieve pain. Clinician: standing just to the side of the leg being tested. One hand supporting knee, other hand at lateral ankle. Movement: Patient is asked to return the leg to the neutral hip position against resistance of the clinicians hand at the ankle. The test is positive when the lateral hip pain is reproduced. Outcome Study In a recent study, maximum walking distance and ability to manipulate shoes and socks on Harris Hip Score domains helped differentiate GTPS from hip osteoarthritis. 23
4 Classification Tendinopathy has been described as a continuum of tissue pathology, which can be classified as reactive, degenerative, or reactive-on-degenerative phases. 18 Reactive tendinopathy is a non-inflammatory proliferative response in the cell and matrix. It is usually a result of a burst of unaccustomed physical activity and is more common in a younger person. At this stage, it remains possible for the tendon to regain its normal structure with optimal management. Treatment at this stage should be aimed at improving the load capacity of the area of aligned fibrillar structure through a progressive loading program. Unloading or performing heavy load, eccentric exercise could cause deleterious effects in this stage. Degenerative tendinopathy demonstrates progression of both matrix and cell changes. There is little capacity for reversibility of pathological changes at this stage. Progressive loading does not necessarily result in a restructure of the matrix. Reactive-on-degenerative describes the concept of some areas of the tendon may be in different stages of tendinopathy at the same time. Structurally normal areas of the tendon may be vulnerable to reactive tendinopathy concurrent with other areas in the tendon in the degenerative phase. Treatment strategies should be directed at optimizing adaptation of the tendon as a whole. Image from Cook et al Corrective Interventions Patient education in reducing compression (including postural changes to sitting and sleeping posture, transfers and exercise) for reducing hip adduction: Avoid lying on affected side (change to supine with pillow under knees or ¼ position from prone) Avoid crossing legs Avoid piriformis, ITB, and adduction stretching Avoid standing and hanging on one hip (uneven LE weight bearing) Avoid running on uneven surfaces/hills and improve lumbopelvic stability See appendix for patient education handout.
5 Phase I: Pain Reduction and Load Management Indications Activity Modifications Prolonged Isometric Contractions Treatment of Kinetic Chain Impairments Criteria to Progress to Phase 2 1. Patient experiences reactive pain (More than 3/10 pain during or after activity/isotonic loading that lasts greater than 24 hours). Range of acceptable pain levels may vary dependent on patient tolerance and understanding of therapeutic ranges 2. Unable to maintain current activity levels due to pain 3. Localized tenderness at tendon 4. Pain with single leg standing test and external derotation test 5. Pain lying on affected side 1. Patient education in reducing compressive forces on the tendon (including no end-range stretching) and the pain-monitoring model 2. Reduced loading and modified volume of activity 3. Patient Education: expected recovery progression, cognitive behavioral therapy if indicated 4. If indicated, use of crutch or STC for load management and gait normalization 5. Cross training with biking, swimming, as tolerated 6. Increase in night pain may indicate load was too high and needs to be adjusted Perform with tendon in shortened/non-compressed/midrange position. Prescription: 5 repetitions of seconds, 2-3 times per day, progressing from 40% to 70% maximal voluntary contraction. 1-2 minute rest periods between contractions. Daily. Isometrics can be done with theraband, side lying abduction (affected side uppermost and pillow between legs), or standing. All exercises should be done in slight abduction to avoid compression. (See appendix) 1. Correction of kinetic chain deficits and restore active trunk stability 2. Functional retraining in weight-bearing double-leg and single-leg tasks with emphasis on avoiding hip adduction during dynamic tasks. 1. Can complete isotonic loading with minimal reactive pain (<3/10 pain or no increase in baseline pain lasting longer than 24 hours) 2. Decreased pain with ADLs 3. Normalized gait
6 Phase II: Isotonic Loading Progression Indications Heavy, Slow Resistance Exercise (HSR) Stretching exercises low level Prolonged Isometric Contractions Cognitive Behavioral Therapy/ Graded Exposure low level Criteria to Progress to Phase 3 1. Strength deficits of the gluteus medius and minimus 2. History of painful loading Prescription: 3-4 sets of concentric-eccentric exercise starting at 15 repetitions and progressing to 6 repetitions, performed every other day *Initially, complete exercise in modified ROM (avoiding hip adduction) to avoid compression of tendon then progress into full ROM as strength and pain levels allow Suggested exercises: upright skating, skating in squat, sidestepping, band side glide, bridges, clamshells, and side lying hip abduction. (See appendix) End-range stretching to address ROM deficits (avoid stretching ITB and piriformis) Perform with tendon in shortened/non-compressed/midrange position. Prescription: 5 repetitions of seconds, 2-3 times per day, progressing from 40% to 70% maximal voluntary contraction. 1-2 minute rest periods between contractions. Daily. Only indicated for cases of chronic pain or central sensitization 1. Full ROM 2. Able to complete 3-4 sets of 6 repetitions throughout full ROM with minimal pain and no increase in pain lasting greater than 24 hours (patients should be at about 7/10 on Borg Rate of Perceived Exertion scale for strengthening purposes) 3. No pain with ADLs 4. No tenderness to palpation of gluteal tendons 5. Able to perform single leg stand test for 30 seconds without pain or trunk deviation
7 Phase III: Energy Storage Loading Progression (Plyometrics) Indications Sport or Activity- Specific Movements Heavy, Slow Resistance Prolonged Isometric Contractions Criteria to Progress to Phase 4 1. Symmetrical strength bilaterally (recommended strength tests: 10 RM, Manual muscle testing) 2. Tolerates introduction of energy storage exercises (hop testing) with minimal pain 1. Progressing volume then intensity. Prescription: every third day, progressing to a volume required by the sport/activity 2. Functional corrections including squats/lunges/single leg activities keeping pelvis level and avoiding hip adduction Prescription: 3-4 sets of concentric-eccentric exercise starting at 15 repetitions and progressing to 6 repetitions, performed every other day *Initially, complete exercise in modified ROM to avoid compression of tendon then progress into full ROM as strength and pain levels allow Perform with tendon in shortened/non-compressed/midrange position. This is done as needed at this phase for pain management. Prescription: 5 repetitions of seconds, 2-3 times per day, progressing from 40% to 70% maximal voluntary contraction. 1-2 minute rest periods between contractions. Daily. 1. Able to complete energy storage exercises with minimal pain and at a volume that would replicate the demands of the sport/activity 2. Proper long-term maintenance implemented for self-management of symptoms Example of Initial Weekly Structure at Phases III and IV Day 1: Plyometrics/return to play, isometrics if needed Day 2: Strengthening, isometrics if needed Day 3: Isometrics Day 4: Rest Day 5: Plyometrics/Return to play, isometrics if needed Day 6: Strengthening, isometrics if needed Day 7: Isometrics
8 Phase IV: Return to Sport/Activity It is important to have a gradual and controlled progression that allows the athlete sufficient time to recover and gives the therapist time to evaluate symptoms. The evaluation of symptoms such as stiffness, pain, and swelling after training, especially the following day, can assist in determining appropriate increases in training intensity or volume. Because individual patients have different baseline abilities, using their perceived exertion will assist in determining how to progress the specific sport activities. Indications Proper Warmup Routine Sport/ Activity- Specific Drills Heavy, Slow Resistance Prolonged Isometric Contractions Criteria for Discharge Can complete introduction of sport/activity-specific exercise with minimal pain Gentle, dynamic movement relevant for the sport or activity Reintegration into competition (no greater than every three days initially) Prescription: 3-4 sets of concentric-eccentric exercise starting at 15 repetitions and progressing to 6 repetitions, performed at least twice per week *Initially, complete exercise in modified ROM to avoid compression of tendon then progress into full ROM as strength and pain levels allow Perform with tendon in shortened/non-compressed/midrange position. This is done as needed at this phase for pain management. Prescription: 5 repetitions of seconds, 2-3 times per day, progressing from 40% to 70% maximal voluntary contraction. 1-2 minute rest periods between contractions. Daily. 1. Full ROM and strength/power 2. Pain-free high load resistance test, ensuring no pain in positions that normally compress the tendon 3. Full training with minimal pain Failing to maintain a customary level of mechanical loading will result in a rapid tissue-specific shift towards catabolic activity. It is vital to emphasize the importance in the off-season management because tendons require a certain level of load maintenance. Continuing the loading program to prevent reduction in tendon integrity and stiffness is important.
9 Authors: Ann-Marie Walters, PT, cert MDT; Robin A. Sopher, PT, DPT; J.J. Kuczynski, PT, DPT, OCS Reviewer: Kate Glaws, PT, DPT, SCS; John Ryan, MD Date: July 12, 2017 References 1. Allison K, Wrigley T et al. Kinematics and Kinetics During Walking in Individuals with Gluteal Tendinopathy. Clinical Biomechanics. 2016; 32: Almekinders LC, Weinhold PS and Maffulli N. Compression Etiology in Tendinopathy. Clin Sports Medicine. 2003; 22 (4); Bird PA, Oakley SP, Shnier R and Kirkham BW. Prospective Evaluation of Magnetic Resonance Imaging and Physical Examination Findings in Patients with Greater Trochanteric Pain Syndrome. Arthritis and Rheumatism. 2001; 44 (9): Malliaras P, Cook J, Purdam c, Rio E. Patellar Tendinopathy: Clinical Diagnosis, Load Management, and Advice for Challenging Case Presentations. JOSPT. 2015; 45: Collee G, Dijkmans BA et al. Greater Trochanteric Pain Syndrome (Trochanteric Bursitis) in Low Back Pain. Scand. J. Rheumatol. 1991; 20 (4): Cook JL, Purdam CR. Is Compressive Load a Factor in the Development of Tendinopathy? Br J of Sports Med. 2012; 46 (3): Cook JL, Purdam CR. Is Tendon Pathology a Continuum? A Pathology Model to Explain the Clinical Presentation of Load- Induced Tendinopathy. Br J Sports Med. 2009; 43 (6): Cook JL, Purdam CR. The Challenge of Managing Tendinopathy in Competing Athletes. Br J Sports Med. 2014; 48(7): Cook JL, Rio E, Purdam CR and Docking SI. Revisiting the Continuum Model of Tendon Pathology:What is its Merit in Clinical Practice and Research? Br J of Sports Med. 2016; 50(19): Del Buono A, Papalia R et al. Management of the Greater Trochanteric Pain Syndrome: A Systematic Review. Br. Med. Bull. 2012; 102 (1): Fearon AM, Ganderton C. Development and Validation of a VISA Tendinopathy Questionnaire for Greater Trochanteric Pain Syndrome, the Visa-G. Manual Therapy. 2015; Fearon AM, Scarvell JM, Neeman T, Cook JL, Cormick W and Smith PN. Greater Trochanteric Pain Syndrome: Defining the Clinical Syndrome. Br J Sports Med. 2013; 47(10): Fearon AM, Stephens S, Cook JL et al. The Relationship of Femoral Neck Shaft Angle and Adiposity to Greater Trochanteric Pain Syndrome in Women. A Case Control Morphology and Anthropometric Study. Br J Sports Med. 2012; 46; Grimaldi A and Fearson A. Gluteal Tendinopathy: Integrating Pathomechanics and Clinical Features in its Management. JOSPT. 2015; 45 (11): Hart DA, Scott A. Getting the Dose Right When Prescribing Exercise for Connective Tissue Conditions; the Yin and the Yang of Tissue Homeostasis. 2012; 46 (13): Lequesne M, Mathieu P et al. Gluteal Tendinopathy in Refractory Greater Trochanter Pain Syndrome: Diagnostic Value of Two Clinical Tests. Arthritis and Rheumatism. 2008; 59 (2): Naugle KM, Fillingim RB, Riley JL. A Meta-Analytic Review of the Hypoalgesic Effects of Exercise. The Journal of Pain. 2012; 13(12); Rio E, Van Ark M, Docking S et al. Isometric Contractions are More Analgesic than Isotonic Contractions for Patellar Tendon Pain: An in Season Randomized Clinical Trial. Clin J Sport Med. 2017; 27(3) Scott A, Backman L et al. Tendinopathy- Update on Pathophysiology. JOSPT. 2015; 45 (11) Scott A, Docking S. et al. Sports and Exercise-Related Tendinopathies: A Review of Selected Topical Issues by Participants of the Second International Scientific Tendinopathy Symposium. Br J Sports Med. 2013; 47 (12): Silbernagel KG, Crossley KM. A proposed Return to Sport Program for Patients with Midportion Achilles Tendinopathy: Rationale and Implementation. JOSPT. 2015;45 (11): Tyler T, Fukunaga T, Gellert J. Rehabilitation of Soft Tissue Injuries of the Hip and Pelvis. Int J. Sports Phys. Ther. 2014; 9(6): Van Ark M et al. Do Isometric and Isotonic Exercise Programs Reduce Pain in Athletes with Patellar Tendinopathy In- Season? A Randomised Clinical Trial. Journal of Science and Medicine in Sport. 2016; 19 (9): OSU Tendinopathy. J.J. Kuczynski, PT, DPT
10 Appendix A: Activities to Avoid/Change The structures at the side of your hip have increased compression when your hips are flexed over 90⁰ and when you cross your leg past the midline of your body. This compression causes pain and irritation to occur. Activities to Avoid Avoid crossing legs while sitting Irritation or pain at the side of your hip will delay tissue healing, and the pain cycle will continue. Modifying your activities is necessary to allow for healing to occur. It is important you follow these changes to notice a decrease in your symptoms, and to eventually alleviate pain. Activities to Change Use towel roll between knees to avoid knees coming together Avoid sitting in figure 4 position Raise seat height so that hips are at an angle greater than 90⁰ Avoid hanging on either hip while standing When sleeping on your non-painful side, put two pillows between our knees Avoid flexibility and stretching exercises targeting IT Band/piriformis Avoid sleeping on painful hip If you must sleep on painful hip, use an egg crate to soften surface
11 Appendix B: Abduction Low-Load Isometric Abduction Cue patients for attention on gentle trochanteric abductor activation (gluteus medius and minimus) while attempting to keep the iliotibial band tensioners relaxed (TFL, upper gluteus maximus, and vastus lateralis Low-Velocity, High-Load Abduction Supine with belt/band Upright skating or skating in squat Sidelying abduction isometric (cue patient to imagine preparing to lift the top leg into abduction-shin horizontal) Alternative home version: Band side slides. Maintain optimal pelvic and trunk alignment Upright side stepping with band Standing (instruct patient to imagine doing the side splits (without movement occurring) Alternative home version: Upright side stepping with band
Greater Trochanteric Pain Syndrome (GTPS): Assessment & Management
 Greater Trochanteric Pain Syndrome (GTPS): Assessment & Management Rachael Mary McMillan Physiotherapist, Alphington Sports Medicine Clinic & FFA Australian Women s National Football Teams PhD Candidate
Greater Trochanteric Pain Syndrome (GTPS): Assessment & Management Rachael Mary McMillan Physiotherapist, Alphington Sports Medicine Clinic & FFA Australian Women s National Football Teams PhD Candidate
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
HIP_CASE 2_OA. Hip Forces. Function of the Hip. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1
 HIP_CASE 2_OA Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT, OCS, FAAOMPT 62 yo female AM stiffness Hip pain diffuse, variable ant>lateral>post Gradual onset Tennis
HIP_CASE 2_OA Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT, OCS, FAAOMPT 62 yo female AM stiffness Hip pain diffuse, variable ant>lateral>post Gradual onset Tennis
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
BENJAMIN G. DOMB, MD
 Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ACUTE PROXIMAL HAMSTRING TENDON REPAIR BENJAMIN J. DAVIS, MD
 Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
JOHN M. REDMOND, M.D.
 Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
NETWORK FITNESS FACTS THE PELVIS
 NETWORK FITNESS FACTS THE PELVIS The Pelvis The pelvis has 3 joints connecting it together 2 sacro-iliac joints at the back (posterior) and the pubic symphysis joint which is at the front (anterior). A
NETWORK FITNESS FACTS THE PELVIS The Pelvis The pelvis has 3 joints connecting it together 2 sacro-iliac joints at the back (posterior) and the pubic symphysis joint which is at the front (anterior). A
Proximal Hamstring Rupture: Physical Therapy Protocol
 Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals Precautions:
 Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
Sports Rehabilitation & Performance Center Medial Patellofemoral Ligament Reconstruction Guidelines * Follow physician s modifications as prescribed
 The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
NICHOLAS J. AVALLONE, M.D.
 NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme
 Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
ACL REHABILITATION PROGRAMME
 Jessica Barrow BSc Physiotherapy (WITS) 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 ACL REHABILITATION PROGRAMME Rehabilitation
Jessica Barrow BSc Physiotherapy (WITS) 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 ACL REHABILITATION PROGRAMME Rehabilitation
Bryan T. Kelly, MD Center for Hip Pain and Preservation Hospital for Special Surgery
 Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Microfracture. This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient.
 This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
Abductor Repair (Gluteus Medius/Minimus Repair)
 (Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
(Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
KNEE REHABILITATION PROGRAMME
 Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
2. Iliotibial Band syndrome
 2. Iliotibial Band syndrome Iliotibial band (ITB) syndrome (so called runners knee although often seen in other sports e.g. cyclists and hill walkers). It is usually an overuse injury with pain felt on
2. Iliotibial Band syndrome Iliotibial band (ITB) syndrome (so called runners knee although often seen in other sports e.g. cyclists and hill walkers). It is usually an overuse injury with pain felt on
Knee Capsular Disorder. ICD-9-CM: Stiffness in joint of lower leg, not elsewhere classified
 1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
Precautions following Hip Arthroscopy/FAI: (Refixation/Osteochondroplasty)
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
Initial Exercises (Weeks 1-3)
 Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
Clinical diagnosis of hip dysfunction
 Clinical diagnosis of hip dysfunction Trish Wisbey-Roth Specialist Sport Physiotherapist (FACP), Olympic Physio, Masters of Sport Physiotherapy ( AIS/UC) Active Rehabilitation Consultant. Case Study: Jane,
Clinical diagnosis of hip dysfunction Trish Wisbey-Roth Specialist Sport Physiotherapist (FACP), Olympic Physio, Masters of Sport Physiotherapy ( AIS/UC) Active Rehabilitation Consultant. Case Study: Jane,
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Meniscus Repair Rehabilitation Protocol
 Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip. Joy Anderson PT, ATC, CSCS
 Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
Travis G. Maak, MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol
 Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Alejandro Verdugo m.d.
 Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Alejandro Verdugo, M.D.
 Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer. Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
CLINICAL PROTOCOL FOR ACHILLES TENDON ALLOGRAFT PCL RECONSTRUCTION REHABILITATION
 CLINICAL PROTOCOL FOR ACHILLES TENDON ALLOGRAFT PCL RECONSTRUCTION REHABILITATION FREQUENCY: 2-3 times per week. DURATION: Average estimate of formal treatment is 2-3 times per week X 2-3 months based
CLINICAL PROTOCOL FOR ACHILLES TENDON ALLOGRAFT PCL RECONSTRUCTION REHABILITATION FREQUENCY: 2-3 times per week. DURATION: Average estimate of formal treatment is 2-3 times per week X 2-3 months based
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The evaluation and management of patients with
 Greater Trochanteric Hip Pain 1.5 ANCC Contact Hours Diane M. Kimpel Chadwick C. Garner Kevin M. Magone Jedediah H. May Matthew W. Lawless In the patient with lateral hip pain, there is a broad differential
Greater Trochanteric Hip Pain 1.5 ANCC Contact Hours Diane M. Kimpel Chadwick C. Garner Kevin M. Magone Jedediah H. May Matthew W. Lawless In the patient with lateral hip pain, there is a broad differential
Labral Repair with a Microfracture
 Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Hip Arthroscopy Labral Repair Protocol
 Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Adam N. Whatley, M.D Main St., STE Zachary, LA Phone(225) Fax(225)
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Evaluating the Athlete Questionnaire
 Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
Hip Arthroscopy. Labral Repair/Debridement with Femoroplasty
 Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of Patellofemoral Instability *
 Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of The following guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital
Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of The following guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft
 Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Gluteal Strengthening Exercises: A Review of the Literature
 Common Imbalances Female Athlete Hip Injuries: Exploring the CORE of Patterns and Prevention Kelly McInnis, DO Irene Davis, PhD, PT, FAPTA, FACSM, FASB David Nolan, PT, DPT, MS, OCS, SCS, CSCS Gluteal
Common Imbalances Female Athlete Hip Injuries: Exploring the CORE of Patterns and Prevention Kelly McInnis, DO Irene Davis, PhD, PT, FAPTA, FACSM, FASB David Nolan, PT, DPT, MS, OCS, SCS, CSCS Gluteal
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
BENJAMIN G. DOMB, M.D.
 Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT
 SPORTS REHABILITATION CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT A case study and rationale for treatment Written by Joanne Kemp and Kay Crossley, Australia BACKGROUND The hip joint and FAI
SPORTS REHABILITATION CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT A case study and rationale for treatment Written by Joanne Kemp and Kay Crossley, Australia BACKGROUND The hip joint and FAI
MATRIX-INDUCED AUTOLOGOUS CHONDROCYTE IMPLANTATION PHYSICAL THERAPY PRESCRIPTION
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline
 Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
Routine Arthroscopic Procedure
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Ilio-Tibial Band Syndrome
 Ilio-Tibial Band Syndrome Ilio-Tibial band syndrome (ITBS) is the most common cause of lateral knee pain in runners and cyclists. It is recognized by the sharp, burning pain that feels almost as if you
Ilio-Tibial Band Syndrome Ilio-Tibial band syndrome (ITBS) is the most common cause of lateral knee pain in runners and cyclists. It is recognized by the sharp, burning pain that feels almost as if you
APTA Intro to Identity. The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee THE HUMAN MOVEMENT SYSTEM
 The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
The Movement System The Kinesiopathologic Model Movement System Impairment Syndromes of the Knee Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Statement of Privacy To protect the privacy of the subjects
Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies
 Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies Melodie Kondratek, PT, DScPT, OMPT Bryan Kuhlman, PT, DPT, OMPT Oakland University Orthopedic Spine and Sports
Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies Melodie Kondratek, PT, DScPT, OMPT Bryan Kuhlman, PT, DPT, OMPT Oakland University Orthopedic Spine and Sports
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol
 REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
Home Exercise Program Progression and Components of the LTP Intervention. HEP Activities at Every Session Vital signs monitoring
 Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component. Limited external rotation to 20 degrees (2 weeks)
 General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
SPORTS INJURIES IN CYCLING. dr. Luthfi Hidayat, Sp. OT (K)
 SPORTS INJURIES IN CYCLING dr. Luthfi Hidayat, Sp. OT (K) But, injury can happen Acute traumatic injuries due to fall Overuse injuries develop gradually overtime (due to repeated movement patterns or
SPORTS INJURIES IN CYCLING dr. Luthfi Hidayat, Sp. OT (K) But, injury can happen Acute traumatic injuries due to fall Overuse injuries develop gradually overtime (due to repeated movement patterns or
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
WHEN THE HIP IS NOT THE HIP
 WHEN THE HIP IS NOT THE HIP M Cusí MBBS, FACSP, FFSEM (UK) Conditions that can be confused with hip pain 1. Referred pain lumbar spine Conditions that can be confused with hip pain 1. Referred pain lumbar
WHEN THE HIP IS NOT THE HIP M Cusí MBBS, FACSP, FFSEM (UK) Conditions that can be confused with hip pain 1. Referred pain lumbar spine Conditions that can be confused with hip pain 1. Referred pain lumbar
Rehabilitation Guidelines for Meniscal Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Sheena Black, MD PHYSICAL THERAPY PRESCRIPTION MCL RECONSTRUCTION. Orthopaedic Surgery, Sports Medicine.
 PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component
 Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Hip Region. PHTY2020: Lecture
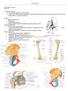 Region PHTY2020: Lecture 2.1 29.02.16 Functional Overview Transfer body weight form trunk to legs Allows leg to adopt numerous positions needed for standing, walking running, stairs, sitting and other
Region PHTY2020: Lecture 2.1 29.02.16 Functional Overview Transfer body weight form trunk to legs Allows leg to adopt numerous positions needed for standing, walking running, stairs, sitting and other
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
2/02/2011. Purdam et al , Silbernagel 2004 Structure towards high, low, medium
 The cornerstones Define the tendon as pain source Defining the stage of tendinopathy Patient history Diagnostic ultrasound Quantify tendon symptoms & function VISA - medium term Loading tests 24 hr response
The cornerstones Define the tendon as pain source Defining the stage of tendinopathy Patient history Diagnostic ultrasound Quantify tendon symptoms & function VISA - medium term Loading tests 24 hr response
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair
 Page 1 of 7 Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (gradual knee
Page 1 of 7 Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (gradual knee
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description Maintain appropriate conditioning: The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the
ILIOTIBIAL BAND SYNDROME Description Maintain appropriate conditioning: The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
