Rehabilitation of Hip Labral Tears and Femoroacetabular Impingement
|
|
|
- Molly Dalton
- 6 years ago
- Views:
Transcription
1 Rehabilitation of Hip Labral Tears and Femoroacetabular Impingement Michael Newsome PT, OCS, SCS, CSCS
2 Hip injuries account for 3.1% of all injuries in the NFL from (Feeley 2008) 59% strains 33% contusions 5% intra-articular (no labral tears dx before 2004)
3 Intra-articular injuries account for 10.6% of all hip/groin injuries in NHL from (Epstein 2012) 69% labral tears 5% FAI
4 Prevalence of intra-articular hip pathology in asymptomatic athletes 72% male/50% female elite soccer players had radiographic FAI (Gerhardt 2012)
5 Prevalence of intra-articular hip pathology in asymptomatic athletes 64% collegiate and pro hockey players had MRI findings of hip pathology 56% labral tears 39% FAI 90% pro hockey players that were followed from previous study were able to play at 4 year follow up (Gallo 2014)
6 NON-OPERATIVE REHAB Is there a case for non-operative treatment? Not all athletes dx with FAI/labral tears have surgery and are able to return to sports What functional and biomechanical deficits in FAI/labral tear patients that can be addressed with non-operative rehab? Will non-operative rehab help with postoperative recovery?
7 NON-OPERATIVE REHAB Pelvic and hip muscle retraining with functional activities Flexibility Joint mobility Strength Activity modification and education
8 PELVIC/HIP BIOMECHANICS Normal pelvic rhythm (Murray 2002) Pelvic rotation accounts for 18% of ROM with hip flexion in standing Pelvic rotation occurs throughout the movement
9 PELVIC/HIP BIOMECHANICS Patients with CAM FAI have altered hip/pelvic biomechanics during gait (Kennedy 2009) pelvic ROM in the frontal plane total frontal/sagittal plane hip ROM
10 PELVIC/HIP BIOMECHANICS Squat kinematics in patients with CAM FAI (Lamontagne 2009) sagittal pelvic ROM squat depth No difference in hip motion
11 PELVIC/HIP BIOMECHANICS Effect of changes in pelvic tilt on hip ROM in FAI patients (Ross 2014) 10 ant. pelvic tilt 10 post. pelvic tilt - 6 IR - 5 IR - 10 hip flexion - 10 hip flexion FADIR - 7 FADIR
12 PELVIC/HIP BIOMECHANICS Improve dynamic control of the pelvis that would change pelvic tilt in FAI patients
13 NON-OPERATIVE REHAB Double Cross Syndrome Tight hip flexors/lumbar extensors Weak gluteals/abdominals
14 Flexibility NON-OPERATIVE REHAB Patients with post. hip pain will have decreased piriformis and gluteal flexibility Tight hip flexors are common problem before and after hip arthroscopic surgery
15 NON-OPERATIVE REHAB Joint mobility A number of FAI/labral tear patients will have joint restrictions Hip ROM restrictions improve with manual therapy in hip OA patients (Hoeksma 2004)
16 NON-OPERATIVE REHAB Dynamic knee valgus with landing mechanics Hip adduction/ir with dynamic knee valgus Excessive hip adduction and IR during functional activities may contribute to FAI (Austin 2008) S.E.R.F. strap adduction/ir at the hip with drop jumps, running and step down (Austin 2008)
17 NON-OPERATIVE REHAB Dynamic knee valgus with landing mechanics hip abduction/er strength correlates with landing kinematics and kinetics (Jacobs 2007, Lawerence 2008) Female soccer players who completed in-season PEP program had IR and abduction at the hip with drop landing (Pollard 2006)
18 NON-OPERATIVE REHAB Hip Strength Arthrogenic inhibition of gluteus maximus with intra-articular fluid injection (Freeman 2012) Patients years old with chronic hip joint pain had hip ER/IR/Abd weakness of 16-28% and the uninvolved hip had 18% ER and 16% abd strength (Harris-Hayes 2014) Symptomatic FAI patients had strength with hip adduction (28%), flexion (26%), ER (18%) and abduction (11%) (Casartelli 2011)
19 NON-OPERATIVE REHAB Activity modification and education Avoid pivoting and cutting activities Avoid combined flexion/add/ir positions Bike for CV training Focus on proper LE alignment with exercise
20 NON-OPERATIVE REHABILITATION OUTCOME STUDIES Case series of non-surgical treatment of hip labral tears (Yazbek 2011) Phase 1 pain control, trunk stabilization, correction of abnormal movements Phase 2 muscle strengthening, restore ROM, balance training Phase 3 advanced strengthening/balance training, sports specific functional progression *Focus on proper L.E. alignment and stabilization at all phases
21 NON-OPERATIVE REHABILITATION OUTCOME STUDIES Conservative care for 52 patients (avg. age 35) with prearthritic, intra-articular hip disorders (Hunt 2012) Phase 1 treatment included patient education, activity, modification and physical therapy (muscle retraining, strengthening and stretching). 27% of the patients improved and did not need any further treatment. Phase 2 was an intra-articular injection and 17%improved and did not choose surgery Phase 3 surgical intervention was chosen by 56% of the patients. Subjects with higher baseline activity scores were likely to choose surgery.
22 BIOMECHANICS OF THE ACETABULAR LABRUM Acetabular labrum provides hip stability by increasing articular surface area and volume (Tan 2001) The labrum seals the synovial fluid under pressure to produce a fluid film which protects the underlying cartilage (Ferguson 2000) The sealing effect enhances joint stability by providing resistance to distraction of the femoral head from the acetabular socket (Crawford 2007)
23 BIOMECHANICS OF THE ACETABULAR LABRUM The anterior superior region of the labrum has lower compressive and tensile elastic modulus than other quadrants of the labrum (Smith 2009) ER/Abd tensile strain in the anterior part of the acetabular labrum (Dy 2008)
24 BIOMECHANICS OF THE ACETABULAR LABRUM Hip extension with combined ER or abduction force results in large strains in the anterior labrum (Crawford 2007) Hip motion is limited by tension in the capsule with abduction and ER which causes the center of rotation of the joint to shift posterior which puts additional strain on the anterior capsule and labrum (Crawford 2007) Anterior and anterior lateral labral strains are high with hip flexion and IR (Safarn 2011)
25 EMG ANALYSIS OF HIP EXERCISES WB and NWB exercises Exercises that isolate a muscle Highest ranking EMG exercise can be difficult to perform or cause pain Functional exercises Exercises that recruit multiple muscles
26 EMG ANALYSIS OF HIP EXERCISES Hip rehabilitation exercises (Bolgla 2006) G.Med: 1) Pelvic drop 57% MVC 2) WB Abd 42% 3) Sidelying Abd 42% 4) NWB Abd 33%
27 EMG ANALYSIS OF HIP EXERCISES Unilateral WB exercises (Ayotte 2007) G.Med: 1) Wall squat 86% 2) Front step up 74% G.Max: 1) Wall squat 52% 2) Front step up 44%
28 EMG ANALYSIS OF HIP EXERCISES Core trunk, hip and thigh muscles during rehab exercises (Ekstrom 2007) G.Med: 1) Side-bridge 74% 2) Unilateral bridge 47% G.Max: 1) Quad arm/leg raise 56% 2) Unilateral bridge 40%
29 EMG ANALYSIS OF HIP EXERCISES Gluteal muscles activation during therapeutic exercises (Distefano 2009) G.Med: 1) Sidelying hip abd 81% 2) Single limb squat 64% 3) Lat band walk 61% G.Max: 1) Single limb squat 59% 2) Single leg dead lift 59% 3) Transverse lunge 49%
30 EMG ANALYSIS OF HIP EXERCISES Top exercises for gluteus med. and max. (Boran 2011) G. Med. G. Max Front plank with hip ext. 75% 106% Side plank abd up 88% 72% Side plank abd down 103% 70% Single leg squat 82% 70%
31 EMG ANALYSIS OF HIP EXERCISES
32 EMG ANALYSIS OF HIP EXERCISES Rehab exercises for G. Med. with consideration for iliopsoas tendinitis (Philippon 2011) 1) Single leg bridge 2) Sidelying hip abd with IR
33 EMG ANALYSIS OF HIP EXERCISES Exercises that target the gluteal muscles while minimizing TFL activation (Selkowitz 2013) 1) Clam in sidelying with tubing 2) Sidestep with tubing 3) Unilateral bridge
34 REHABILITATION AFTER ARTHROSCOPIC HIP SURGERY Phase I Protection (0 4 weeks) Phase II Strength/Mobility (4 8 weeks) Phase III Functional Training (8 12 weeks) Phase IV Return to Sport (12 26 weeks)
35 PROTECTION PHASE (0 4 WEEKS) Brace: 0-90 to protect labrum and anterior capsule CPM: 4 hrs/day Wt. Bearing: 25% flat foot wt. bearing with brace for 2 weeks then WBAT. NWB=PWB compression forces (Givens Heis 1992). Hip flexor irritation with NWB.
36 PROTECTION PHASE (0 4 WEEKS) ROM: Limit extension 0 /ER 20 Avoid flexion/add/ir Quadriped position to increase hip flexion ROM IR ROM in prone position Upright bike with high seat and minimal resistance Flexibility: Prone lying for hip flexors and modified supine hip flexion stretch.
37 PROTECTION PHASE (0 4 WEEKS) Strength: Lumbopelvic stabilization (post. pelvic tilts/bridging) Quadriceps and submaximal hip isometrics except hip flexion Progress to hip isotonics after 2 weeks Education and activity modification Limit time sitting especially in low chairs Need to assist operative LE with transfers Avoid pivoting or rotating during wt. bearing Avoid active long lever hip flexion (SLR) Anterior hip pain is a common complaint
38 STRENGTH/MOBILITY PHASE (4-8 WEEKS) D/C brace and CPM Gait training: restore stride length and correct frontal plane compensation Aquatic therapy: gait training and CKC exercises ROM: progress to full ROM, can use mobilization belt with ROM, ST mobilization as needed
39 STRENGTH/MOBILITY PHASE (4-8 WEEKS) Flexibility: Static, dynamic, and PNF stretching to all muscle groups Wt bearing hip flexion stretch Strength: Advance lumbopelvic stabilization (single leg bridge and side planks) Multi-hip machine CKC exercises Hip hiking and lateral band walks for glut med
40 STRENGTH/MOBILITY PHASE (4-8 WEEKS) Balance training: progress to single leg CV training: bike/elliptical/stairmaster Education: focus on proper LE alignment with exercises and ambulation
41 FUNCTIONAL TRAINING PHASE (8 12 WEEKS) ROM: add joint mobilization if ROM is still limited Strength: single leg CKC exercises and low impact multiplane functional exercises Balance training: add pertubation training
42 RETURN TO SPORT PHASE (12 26 WEEKS) Running on flat surface Plyometric and agility training Sport specific training
43 RETURN TO SPORT PHASE (12 26 WEEKS) Return to sport 3.9 months (Philippon 2010) 9.4 months (Nho 2011) Return to sport for pro athletes 4.2 months and recreational athletes 6.8 months (Malviya 2013)
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Gluteal Strengthening Exercises: A Review of the Literature
 Common Imbalances Female Athlete Hip Injuries: Exploring the CORE of Patterns and Prevention Kelly McInnis, DO Irene Davis, PhD, PT, FAPTA, FACSM, FASB David Nolan, PT, DPT, MS, OCS, SCS, CSCS Gluteal
Common Imbalances Female Athlete Hip Injuries: Exploring the CORE of Patterns and Prevention Kelly McInnis, DO Irene Davis, PhD, PT, FAPTA, FACSM, FASB David Nolan, PT, DPT, MS, OCS, SCS, CSCS Gluteal
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip. Joy Anderson PT, ATC, CSCS
 Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
Hip Labrum and FAI Post-Surgical Rehabilitation Guideline
 Hip Labrum and FAI Post-Surgical Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Hip Labrum and FAI Post-Surgical Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component
 Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Hip Arthroscopy. Labral Repair/Debridement with Femoroplasty
 Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Initial Exercises (Weeks 1-3)
 Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ACUTE PROXIMAL HAMSTRING TENDON REPAIR BENJAMIN J. DAVIS, MD
 Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
Precautions following Hip Arthroscopy/FAI: (Refixation/Osteochondroplasty)
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
Hip Arthroscopy Labral Repair Protocol
 Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Disclosures. Objectives. Overview. Patellofemoral Syndrome. Etiology. Management of Patellofemoral Pain
 Management of Patellofemoral Pain Implications of Top Down Mechanics Disclosures I have no actual or potential conflict of interest in relation to this presentation David Nolan, PT, DPT, MS, OCS, SCS,
Management of Patellofemoral Pain Implications of Top Down Mechanics Disclosures I have no actual or potential conflict of interest in relation to this presentation David Nolan, PT, DPT, MS, OCS, SCS,
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Labral Repair with a Microfracture
 Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
Travis G. Maak, MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals Precautions:
 Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component. Limited external rotation to 20 degrees (2 weeks)
 General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
Bryan T. Kelly, MD Center for Hip Pain and Preservation Hospital for Special Surgery
 Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
A patient guide to Hip Impingement Non-Surgical Management. Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy
 A patient guide to Hip Impingement Non-Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Contents Page: 1 Cover 2 Contents 3 Hip impingement information 4 Conservative rehabilitation
A patient guide to Hip Impingement Non-Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Contents Page: 1 Cover 2 Contents 3 Hip impingement information 4 Conservative rehabilitation
Hip pain: A comparison of Osteoarthritis and Femoroacetabular Impingement Kristine Flais, PT, DPT
 Hip pain: A comparison of Osteoarthritis and Femoroacetabular Impingement Kristine Flais, PT, DPT Most common cause of hip pain in older adults Prevalence of Hip OA Age Gender Race Developmental disorders
Hip pain: A comparison of Osteoarthritis and Femoroacetabular Impingement Kristine Flais, PT, DPT Most common cause of hip pain in older adults Prevalence of Hip OA Age Gender Race Developmental disorders
Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer. Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component. Normalize gait pattern with brace and crutches
 Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component General Guidelines: Normalize gait pattern with brace and crutches Weightbearing as per procedure performed Continuous Passive
Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component General Guidelines: Normalize gait pattern with brace and crutches Weightbearing as per procedure performed Continuous Passive
BENJAMIN G. DOMB, MD
 Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Training the Joint Replacement Client
 KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
JOHN M. REDMOND, M.D.
 Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Re training Movement Behavior for ACL Injury Prevention and Rehabilitation: A Matter of Strength or Motor Control?
 Re training Movement Behavior for ACL Injury Prevention and Rehabilitation: A Matter of Strength or Motor Control? Christopher M. Powers, PT, PhD, FACSM, FAPTA Beth Fisher, PT, PhD, FAPTA Division of Biokinesiology
Re training Movement Behavior for ACL Injury Prevention and Rehabilitation: A Matter of Strength or Motor Control? Christopher M. Powers, PT, PhD, FACSM, FAPTA Beth Fisher, PT, PhD, FAPTA Division of Biokinesiology
BENJAMIN G. DOMB, M.D.
 Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
Alejandro Verdugo, M.D.
 Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Routine Arthroscopic Procedure
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
Proximal Hamstring Rupture: Physical Therapy Protocol
 Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT
 SPORTS REHABILITATION CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT A case study and rationale for treatment Written by Joanne Kemp and Kay Crossley, Australia BACKGROUND The hip joint and FAI
SPORTS REHABILITATION CONSERVATIVE MANAGEMENT OF FEMOROACETABULAR IMPINGEMENT A case study and rationale for treatment Written by Joanne Kemp and Kay Crossley, Australia BACKGROUND The hip joint and FAI
Rehabilitation. Friday, October 14, :00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA
 Rehabilitation Friday, October 14, 2011 11:00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA Best Tip Srino Bharam, MD USA Best Tip Robroy Martin, PhD, PT USA
Rehabilitation Friday, October 14, 2011 11:00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA Best Tip Srino Bharam, MD USA Best Tip Robroy Martin, PhD, PT USA
HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE
 HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair
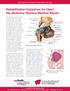 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
Rehabilitation Guidelines For Periacetabular Osteotomy (PAO) Of The Hip
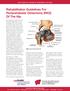 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines For Periacetabular Osteotomy (PAO) Of The Hip The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket formed by
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines For Periacetabular Osteotomy (PAO) Of The Hip The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket formed by
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Running Athlete: Part C. Case Analysis Materials
 Running Athlete: Part C Case Analysis Materials Case 1 Subjective Examination (performed offcamera) Runs very sporadically, but generally 2-3 x per week around 2-4 miles Play recreational soccer Denies
Running Athlete: Part C Case Analysis Materials Case 1 Subjective Examination (performed offcamera) Runs very sporadically, but generally 2-3 x per week around 2-4 miles Play recreational soccer Denies
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Hip Arthroscopy - FAI/Labral Repair Protocol The hip is a ball and
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Hip Arthroscopy - FAI/Labral Repair Protocol The hip is a ball and
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Abductor Repair (Gluteus Medius/Minimus Repair)
 (Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
(Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
BIOMECHANICAL INFLUENCES ON THE SOCCER PLAYER. Planes of Lumbar Pelvic Femoral (Back, Pelvic, Hip) Muscle Function
 BIOMECHANICAL INFLUENCES ON THE SOCCER PLAYER Functional performance of the soccer player reflects functional capability of certain specific muscle and muscle groups of the back, pelvis and hip to work
BIOMECHANICAL INFLUENCES ON THE SOCCER PLAYER Functional performance of the soccer player reflects functional capability of certain specific muscle and muscle groups of the back, pelvis and hip to work
Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
TREATMENT GUIDELINES FOR GRADE 3 PCL TEAR
 GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
GENERAL CONSIDERATIONS Posterior cruciate ligament (PCL) injuries occur less frequently than anterior cruciate ligament (ACL) injuries, but are much more common than previously thought. The PCL is usually
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) Acetabuloplasty
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com This protocol
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com This protocol
Alejandro Verdugo m.d.
 Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information
 Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information Please read entire protocol prior to initiating therapy Please note: Individual hip injuries vary widely. This therapy protocol should
Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information Please read entire protocol prior to initiating therapy Please note: Individual hip injuries vary widely. This therapy protocol should
Knee Multiligament Rehabilitation
 Knee Multiligament Rehabilitation Orlando Valle, PT, MSPT, SCS, CSCS Director Ironman Sports Medicine Institute TMC Orlando.Valle@memorialhermann.org 4 Major Ligaments ACL PCL MCL LCL (PLC) Anatomy Function
Knee Multiligament Rehabilitation Orlando Valle, PT, MSPT, SCS, CSCS Director Ironman Sports Medicine Institute TMC Orlando.Valle@memorialhermann.org 4 Major Ligaments ACL PCL MCL LCL (PLC) Anatomy Function
Dr Schock High Tibial Osteotomy
 Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
Protocol G Arthroscopic Surgery: Therapist Information
 Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Microfracture. This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient.
 This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
HIP_CASE 2_OA. Hip Forces. Function of the Hip. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1
 HIP_CASE 2_OA Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT, OCS, FAAOMPT 62 yo female AM stiffness Hip pain diffuse, variable ant>lateral>post Gradual onset Tennis
HIP_CASE 2_OA Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT, OCS, FAAOMPT 62 yo female AM stiffness Hip pain diffuse, variable ant>lateral>post Gradual onset Tennis
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Hip Arthroscopy
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
ACL and Knee Injury Prevention. Presented by: Zach Kirkpatrick, PT, MPT, SCS
 ACL and Knee Injury Prevention Presented by: Zach Kirkpatrick, PT, MPT, SCS ACL Anatomy ACL Mechanism of Injury Contact ACL Tear Noncontact ACL Tear ACL MOI and Pathology Common in young individual who
ACL and Knee Injury Prevention Presented by: Zach Kirkpatrick, PT, MPT, SCS ACL Anatomy ACL Mechanism of Injury Contact ACL Tear Noncontact ACL Tear ACL MOI and Pathology Common in young individual who
KNEE REHABILITATION PROGRAMME
 Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
Mechanisms of ACL Injury: Implications for Rehabilitation, Injury Prevention & Return to Sport Decisions. Overarching research theme:
 Mechanisms of ACL Injury: Implications for Rehabilitation, Injury Prevention & Return to Sport Decisions Associate Professor Co Director, Musculoskeletal Biomechanics Research Laboratory University of
Mechanisms of ACL Injury: Implications for Rehabilitation, Injury Prevention & Return to Sport Decisions Associate Professor Co Director, Musculoskeletal Biomechanics Research Laboratory University of
Research Theme. Cal PT Fund Research Symposium 2015 Christopher Powers. Patellofemoral Pain to Pathology Continuum. Applied Movement System Research
 Evaluation and Treatment of Movement Dysfunction: A Biomechanical Approach Research Theme Christopher M. Powers, PhD, PT, FAPTA Understanding injury mechanisms will lead to the development of more effective
Evaluation and Treatment of Movement Dysfunction: A Biomechanical Approach Research Theme Christopher M. Powers, PhD, PT, FAPTA Understanding injury mechanisms will lead to the development of more effective
Protocol A Arthroscopic Surgery: Therapist Information
 Protocol A Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol A Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Rehabilitation Following Unilateral Patellar Tendon Repair
 Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Protocol D Arthroscopic Surgery: Therapist Information
 Protocol D Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol D Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
HIP ARTHROSCOPY REHAB 0-2 WEEKS
 HIP ARTHROSCOPY REHAB 0-2 WEEKS Protect the surgical repair Patient education regarding: gait and surgical findings. o Protected weight-bearing (PWB): weight bearing as tolerated with crutches o Ensure
HIP ARTHROSCOPY REHAB 0-2 WEEKS Protect the surgical repair Patient education regarding: gait and surgical findings. o Protected weight-bearing (PWB): weight bearing as tolerated with crutches o Ensure
Theodore Ganley, MD Lawrence Wells, MD J. Todd Lawrence, MD, PhD Anterior Cruciate Ligament Reconstruction Protocol (Revised March 2018)
 Theodore Ganley, MD Lawrence Wells, MD J. Todd Lawrence, MD, PhD Anterior Cruciate Ligament Reconstruction Protocol (Revised March 2018) ***Please refer to written prescription for any special instructions
Theodore Ganley, MD Lawrence Wells, MD J. Todd Lawrence, MD, PhD Anterior Cruciate Ligament Reconstruction Protocol (Revised March 2018) ***Please refer to written prescription for any special instructions
Hip Arthroscopy: State of the Art
 Hip Arthroscopy: State of the Art Seung J. Yi Florida Orthopaedic Institute Orthopaedics for Primary Care and Therapists ER HPI 24 yo F R hip pain x 4 months after twisting injury in flag football C sign
Hip Arthroscopy: State of the Art Seung J. Yi Florida Orthopaedic Institute Orthopaedics for Primary Care and Therapists ER HPI 24 yo F R hip pain x 4 months after twisting injury in flag football C sign
Post Operative Hip Arthroscopy Procedure Form
 Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol
 REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION
 REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below
 Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance
Dynamic Stabilization of the Patellofemoral Joint: Stabilization from above & below Division Biokinesiology & Physical Therapy Co Director, oratory University of Southern California Movement Performance
Sports Rehabilitation & Performance Center Medial Patellofemoral Ligament Reconstruction Guidelines * Follow physician s modifications as prescribed
 The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab Protocol
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
Hip Region. PHTY2020: Lecture
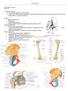 Region PHTY2020: Lecture 2.1 29.02.16 Functional Overview Transfer body weight form trunk to legs Allows leg to adopt numerous positions needed for standing, walking running, stairs, sitting and other
Region PHTY2020: Lecture 2.1 29.02.16 Functional Overview Transfer body weight form trunk to legs Allows leg to adopt numerous positions needed for standing, walking running, stairs, sitting and other
Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of
Post Operative Hip Arthroscopy Procedure Form
 Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Personalized Blood Flow Restriction Rehabilitation. Anterior Cruciate Reconstruction with Meniscal Repair
 Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
Personalized Blood Flow Restriction Rehabilitation Anterior Cruciate Reconstruction with Meniscal Repair ACL with Meniscus Repair 2 PHASE 1 (PROTECTED PHASE) Typically, after an anterior cruciate reconstruction
NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY ( Program)
 Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Exercises to Correct Muscular Imbalances. presented by: Darrell Barnes, LAT, ATC, CSCS
 Exercises to Correct Muscular Imbalances presented by: Darrell Barnes, LAT, ATC, CSCS Objectives Review Functional Anatomy Identify physical imbalances that lead to injury and/or decrease performance
Exercises to Correct Muscular Imbalances presented by: Darrell Barnes, LAT, ATC, CSCS Objectives Review Functional Anatomy Identify physical imbalances that lead to injury and/or decrease performance
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Orthopaedic Surgery - Arthroscopic Surgery - Joint Replacement - Sports Medicine - Fracture Care
 Orthopaedic Surgery - Arthroscopic Surgery - Joint Replacement - Sports Medicine - Fracture Care John R. Chance, M.D., David L. Fox, M.D., Jamie L. Lynch, M.D., Brian E. Schulze, M.D., Patrick M. Simon,
Orthopaedic Surgery - Arthroscopic Surgery - Joint Replacement - Sports Medicine - Fracture Care John R. Chance, M.D., David L. Fox, M.D., Jamie L. Lynch, M.D., Brian E. Schulze, M.D., Patrick M. Simon,
ACL Reconstruction Rehabilitation Protocol
 ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
Connor Hammond. B.Sc., The University of Guelph, 2013 A THESIS SUBMITTED IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE OF
 TRUNK AND LOWER LIMB BIOMECHANICS DURING STAIR CLIMBING IN PEOPLE WITH SYMPTOMATIC FEMOROACETABULAR IMPINGEMENT COMPARED TO ASYMPTOMATIC HEALTHY INDIVIDUALS by Connor Hammond B.Sc., The University of Guelph,
TRUNK AND LOWER LIMB BIOMECHANICS DURING STAIR CLIMBING IN PEOPLE WITH SYMPTOMATIC FEMOROACETABULAR IMPINGEMENT COMPARED TO ASYMPTOMATIC HEALTHY INDIVIDUALS by Connor Hammond B.Sc., The University of Guelph,
Knee PCL Reconstruction Rehabilitation Program
 The Gundersen Health System Sports Medicine PCL Reconstruction Rehabilitation Program is an evidencebased and soft tissue healing dependent program allowing patients to progress to vocational and sports-related
The Gundersen Health System Sports Medicine PCL Reconstruction Rehabilitation Program is an evidencebased and soft tissue healing dependent program allowing patients to progress to vocational and sports-related
Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair
 Page 1 of 7 Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (gradual knee
Page 1 of 7 Rehabilitation Following Acute ACL, PCL, LCL, PL & Lateral Hamstring Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore normal range of motion (gradual knee
Session Objectives. Session Speakers. The Problem of Femoroacetabular Impingement: A Theoretical Framework to Guide Clinical Practice
 The Problem of Femoroacetabular Impingement: A Theoretical Framework to Guide Clinical Practice Christopher Powers, PT, PhD, FAPTA Alex Weber, MD Jennifer Bagwell, PT, PhD Creighton University Session
The Problem of Femoroacetabular Impingement: A Theoretical Framework to Guide Clinical Practice Christopher Powers, PT, PhD, FAPTA Alex Weber, MD Jennifer Bagwell, PT, PhD Creighton University Session
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Test-retest. The therapist can perform test: retest procedures throughout the treatment session as required.
 HIP TREATMENT PROTOCOL Manual Therapy General Guidelines The goal of manual therapy: For this study, manipulative therapy includes specific manipulations (lowamplitude, high-velocity thrust techniques)
HIP TREATMENT PROTOCOL Manual Therapy General Guidelines The goal of manual therapy: For this study, manipulative therapy includes specific manipulations (lowamplitude, high-velocity thrust techniques)
Sheena Black, MD PHYSICAL THERAPY PRESCRIPTION MCL RECONSTRUCTION. Orthopaedic Surgery, Sports Medicine.
 PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
