HIP FOLLOW-UP. 2) Please sign the Mission statement and disclosure form and send it to us
|
|
|
- Bertha Morris
- 6 years ago
- Views:
Transcription
1 HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year and every other year postoperatively thereafter for your safety even though you are feeling great. Long distance follow-up evaluations for out-ofstate patients are fine. We would like to ask you to complete the following evaluation protocol. 1) We keep track of each hip separately in our database. Therefore, I would like to request that you fill out TWO separate Hip Follow-Up Patient Self Rating forms if we are evaluating both hips, even if both are identical. 2) Please sign the Mission statement and disclosure form and send it to us 3) Physical Therapy : Add your name to the physical therapy evaluation request Give the order and physical exam form to your physical therapist Send the results to us. 4) Hip X-Ray: Add your name to the x-ray request; Have the x-ray of your hip(s) done at your local hospital, and request a CD copy of this x-ray Mail a CD of the digital x-ray images (preferred) or x-ray films to us 5) Metal Ion Test: Add your name to the prescription Have the test done at the nearest lab Send the results to us As soon as we receive all of the above, I will review them and send you a written response. If you prefer to travel here for an office visit for evaluation, please call our appointment line to arrange this (803) (routine office charges will apply). If you are having significant problems with your hip, I will need to see you in the office for complete examination to best diagnose it.
2 Thank you for your attention to this matter. If you have any questions, please contact us for assistance. Thomas P. Gross MD Lee Webb, N.P. Attached Forms: 1. Follow up hip questions 2. Mission statement and disclosure 3. Physical exam form* 4. Physical therapy evaluation letter * 5. Physical therapy evaluation request* 6. Hip XR request 7. Phase II hip exercises 8. Metal ion test # * These forms are not needed after 2 years if your range of motion exam was previously done. # This test is ONLY needed for two-year follow-up and afterwards. Currently, if you have done this test and have sent the result to us, you do NOT need to do it again. Also, if you are a bilateral patient, you should wait until both of your operated hips have reached twoyear follow-up after the latest surgery. Please contact us with any follow-up questions: grosspatientfollowup@midlandsortho.com Call: (803) FAX: (803) If you don t have any questions, please follow the protocol and fill out each form below, then FEDEX the packet to: Dr. Thomas P. Gross Attn: hip follow-up Midlands Orthopaedics 1910 Blanding St. Columbia, SC 29201
3 Important instructions Print Form Submit by Thomas P.Gross, M.D Updated Jan-2008 Hip Follow-Up Patient Self Rating Form Current Date 7/14/08 All information will be treated as strictly confidential! Last Name First Name Medical Record # Date A. INTRODUCTION: The purpose of this questionnaire is to objectively grade the severity of your hip problem as accurately as possible. Of course the questions are subjective. I ask people to answer these questions when initially evaluating their hip, and again at intervals after surgery to assess our results. We keep track of each hip separately in our database. Therefore, I would like to request that you fill out two separate forms if we are evaluating both hips today, even if both are identical. Thank you for your assistance in this matter. 1. This questionnaire is filled out for the purpose of evaluation of my: Right hip Left hip 2. I have significant problems with my: Right hip Left hip Both hips Neither of my hips 3. Dr. Gross has operated on: Right hip Left hip Both hips Neither of my hips 4. Another surgeon has performed a major hip surgery on: Right hip Left hip Both hips Neither of my hips 5. If Dr. Gross has operated on my hip(s), please check off the operation (more than one may apply): Total hip replacement (with a stem) Hip surface replacement Revision of a hip replacement (redo operation) Other 6. Please list the date of your latest operation performed by Dr. Gross on the hip being evaluated by this form: N/A Date Page 1 of 6
4 7. Please indicate the closest follow-up interval calculated from the date of your surgery: 6 weeks 8 years 3 months 9 years 6 months 1 year 11 years 2 years 3 years 4 years 5 years None Wound Infection Deep Venous Thrombosis (blood clot in the leg) Pulmonary Embolus (blood clot traveling to the lungs) Partial Sciatic Palsy (foot drop, nerve injury) Dislocation Fracture Implant came loose Other No Yes None: or it is so insignificant that I ignore it. 10 years 12 years 13 years 14 years 15 years 6 years 16 years 7 years B. COMPLICATIONS: 1. Did you have any complications after surgery: Longer 2. If you had a complication, did it require further surgery: C. CLINICAL SCORE: This score should reflect how your hip has been functioning now (post surgery). The questionnaire was modified to allow scoring a standard Harris Hip Score (HHS). Please mark the category that fits your condition best. People with arthritis have good and bad days; your answers should reflect your usual days. I understand that the answers may not always exactly fit your condition. 1. What category most closely represents your pain level in your hip? Slight: regular slight pain. I have no compromise in activity. Mild: there is no effect on ordinary activity; I have pain after unusual activity Moderate: the pain is tolerable. I may use aspirin or anti-inflammatory medicine. I make concessions. Severe: I have serious limitations to my lifestyle. I may occasionally use Vicodin or some other narcotic I am totally disabled by this hip Page 2 of 6
5 2. If you have some pain, where is it located? (Check all that apply) None Groin Side of hip near the scar Front of thigh Side of thigh Buttock Others 3. Pain Assessment - Visual Analog Scale: Please circle your current level of pain using the scale below. On most regular days: On my worst days: 4. Limp: None Slight Moderate Severe Unable to walk 5. Use of walking support: None required I use a cane or stick for long walks I almost always use a cane or stick I use one crutch most of the time I use two crutches or a walker I am unable walk across the room Page 3 of 6
6 6. Without stopping for a break, on most days, I am usually able to walk: Over one mile The equivalent of 6 average city blocks 2-3 average city blocks Less than one block I can only get from bed to chair 7. Stair climbing: Normally foot over foot without pulling on a rail Normally foot over foot with some help from the rail Usually not foot over foot; but instead, leading up with the non-painful hip one step at a time I can't manage to walk up stairs 8. Putting on socks and tying shoelaces: I can put them on with ease I can put them on, but it is difficult, I may use an assistive device I can't put them on, except for slip-on shoes 9. Sitting: I can sit in any chair for more than one hour I can only sit in a high chair, or I can only sit for one half an hour I am unable to sit in any chair 10. Transportation: I am able to get in and out of a car or public transportation by myself I need help to get in and out of a car or public transportation 11. Please name any unrelated orthopedic or medical problems that are severe enough to adversely affect your overall hip score. Please briefly explain: N Other problems: Page 4 of 6
7 12. At this point is your hip better than before your surgery? What statement most accurately describes your new hip?: It is better than my pre-arthritic normal hip was It feels just like a normal hip It is much better than before surgery, but still has some minor aches and pains It is slightly better than before surgery It is about the same I am worse D. ACTIVITY SCORE: PLEASE MOVE ON TO SECTION E AND SKIP THIS SECTION (SECTION D, UCLA ACTIVITY SCORE) IF YOU ARE LESS THAN 8 MONTHS POSTOPERATIVE (AFTER YOUR SURGERY). 1. UCLA Activity Score When this section is applicable, please choose the one response that most closely fits your activity level: Whole inactive, dependent on others, and can not leave residence 1 Mostly inactive or restricted to minimum activities of daily living 2 Sometimes participants in mild activities, such as walking, limited housework and limited shopping 3 Regularly participates in mild activities 4 Sometimes participates in moderate activities such as swimming or could do unlimited housework or shopping 5 Regularly participates in moderate activities 6 Regularly participates in active events such as bicycling 7 Regularly participates in active events such as golf or bowling 8 Sometimes participates in impact sports such as jogging, tennis, skiing, acrobatics, ballet, heavy labor or backpacking 9 Regularly participates in impact sports If possible, please list 2-3 activities for each of the first two questions. An exhaustive list is not necessary. a. Please list activities you are regularly participating in: Page 5 of 6
8 b. Please list the most vigorous activities that you have occasionally participated in since your surgery: c. My activity level now is (similar to, lower than, greater than) when my hip(s) first became arthritic? E. CONCLUSION: 1. Knowing what you now know, do you feel you made the right decision to have this surgery? Yes No 2. Do you have any other comments that you would like to share? If your address or phone number has changed since your last visit, please enter your new address or phone number: Address City State Zip Code Country Phone Number Page 6 of 6
9 Mission Statement and Disclosure Form Thomas P. Gross, M.D. Revised Jan, 17, 2008 Practice limited to hip and knee reconstruction, Midlands Orthopaedics, p.a Blanding Street, Columbia, SC I am a specialist in the field of hip and knee replacement. I am in private practice, but I am also heavily involved in clinical research, teaching and orthopaedic implant development. I perform all of my surgery personally, with the assistance of Lee Webb, Nurse Practitioner. No residents or fellows will do your operation. Visiting surgeons are frequently present to observe my operations to learn the latest techniques; they do not participate in the operations themselves. I do receive royalties and research support from various orthopaedic implant companies. I do not get paid directly for the implants used in your surgery. Joint replacement implants in the Columbia marketplace are excluded from my royalty contract. I will be happy to answer specific questions you have regarding implants I intend to use in your operation. It is generally recognized as the standard of care for joint replacement surgeons to provide long-term follow up evaluations for patients they have operated on. Although we do bill for these services, we primarily earn our living from performing surgery. As a surgeon involved in clinical research, it is particularly important to me to continue a long-term relationship with all patients on whom I operate. I use all information gathered in my practice as material for teaching and scientific presentations and papers. Patient identity is carefully protected in all presentations. (The only exception is for patients who specifically agree to provide testimonials about their cases. These patients write up a description of their experience for public presentation.) Every medical treatment has potential to result in complications. Surgical treatments all have their own sets of possible complications. I will disclose the most common ones to you; most are posted on my website. If you should have a complication, I will deal with it promptly and directly. Even out of state patients should keep me well informed of any that develop. It is my preference (and in your best interest) for me to deal with all surgical complications personally. Nonsurgical (medical) complications can be dealt with by your local primary care physician or other non-orthopaedic specialist, but please keep me informed and let me advise you. Surgical complications may require extra unexpected trips to Columbia, SC, but this is essential for you to achieve the best possible outcome. One reason you may have chosen me as a surgeon is because my experience allows me to perform surgery with a very low complication rate. However, equally important is my knowledge in how to deal with postoperative
10 complications appropriately. Even after they occur, a good outcome can often be achieved with appropriate skilled intervention. I expect to see all patients for follow up evaluations at four to six weeks postoperatively and one year postoperatively in my office. If you are an out of state patient, local follow up can be arranged (but is not preferred). If your case is routine and stable, long-term follow up (two years, five years, 10 years, and 15 years) can be done via online questionnaire and digital x-ray. I will provide you with a written reply and will not charge you for reviewing your online questionnaire and x-rays. If a phone consultation is required (after three months post-op) a fee may be assessed. If you do have specific problems, on site personal evaluation by me is recommended. I have read the above statement and agree to honor my commitment to provide timely follow up information. I understand that providing this information will benefit not only me, but also Dr. Gross and many future patients of his practice and elsewhere. I hereby agree to play my part in furthering the practice and science of joint replacement surgery. This contract is not legally enforceable, but represents my good faith agreement under which I wish to establish a doctor-patient relationship with Dr. Gross. Patient s Signature Date Thank you. My commitment to you is the highest level of care, both technically and personally. I strive to continue to elevate the level of my expertise by dealing with complications directly and promptly and by continuing a rigorous and systematic scientific review of my surgical outcomes. Thomas P. Gross, MD 1/31/2008 Date
11 HIP FOLLOWUP PHYSICAL EXAM Thomas P. Gross M.D Midlands Orthopaedics 1910 Blanding St Columbia SC Name of patient being evaluated: Date of Surgery: Right: Left: Type of Surgery: Right: Left: Interval from Surgery: Right: N/A Left: N/A 6 weeks 6 weeks 1 year 1 year 2 year 2 year Or Or Office Use Only Date Received: / / Office Record Number: TO BE COMPLETED BY A PHYSICAL THERAPIST 1. Patient Charnley Category: A1: Unilateral with opposite hip normal A2: Bilateral with satisfactory function of opposite hip B: Unilateral other hip impaired C: Multiple arthritis or medical infirmity 2. Range of Motion: Right Left a. Flexion Contracture* b. Flexion to** c. abduction at 45 degees of flexion to d. adduction at 45 degrees of flexion to e. external rotation at 45 degrees of flexion to f. internal rotation at 45 degrees of flexion to g. IR with knee flexed to 90 degrees *** * Enter 0 if the leg is able to lie flat on the exam table. ** Do not push past 100 degrees before 1 year ***Do not perform this one until one year after surgery please 3. Gait: o o o o o Normal Antalgic Trendelenburg Short Leg Other 4. Trendelenburg Sign:
12 o Positive o Negative 5. Active SLR painful? o No o Yes If Yes Where? 6. Strength SLR (grade 0-5): 7. Strength Abduction (grade 0-5): 8. Leg Length: Equal Left short Right short 9. Tender: o No o Yes If yes, where? 10. Condition of incision: Physical Therapist Signature: Date: Print Name: Address: Please give a copy to the patient and mail one to me at the above address. Thank you. Updated 1/31/08
13 (803) Fax: (803) Blanding St. Columbia,SC Lake Murray Blvd. Irmo,SC Dear Physical Therapist: The person presenting this form has had a hip surface replacement performed by Dr. Thomas P. Gross weeks/years ago. We are asking that you objectively evaluate his/her hip and send me a report. If the patient is less than one year postop, the hip cannot be pushed into extreme flexion, adduction and internal rotation. (See form). Please record the range of motion that can be achieved by gentle examination in this case. If the patient is approximately six weeks postop, please review and assist them with my Phase II Hip Exercise Program. The patient has been instructed to bring this with him/her in this situation. Thomas P. Gross M.D Please FAX to: and give the patient a copy.
14 (803) Blanding St. Columbia,SC Lake Murray Blvd. Irmo,SC FOR RADDRESS DATE Please evaluate both hips in the above patient for range of motion and strength and provide a report on my standardized form included. Thomas P. Gross M.D Please FAX to: and give the patient a copy.
15 (803) Blanding St. Columbia,SC Lake Murray Blvd. Irmo,SC R FOR ADDRESS DATE Please select/circle ONE section (either 1, 2, or 3) to ensure the appropriate xrays are obtained from the patient s radiology facility. 1. LEFT a. Diagnoses: i. Osteoarthritis (OA) of the hip M16.12 ii. Hip pain M RIGHT a. Diagnoses: i. Osteoarthritis (OA) of the hip M16.11 ii. Hip pain M BILATERAL a. Diagnoses: i. Osteoarthritis (OA) of the hip M16.10 ii. Hip pain M Views (please include all of the following): 1. AP Pelvis Standing (Please label as STANDING ) 2. AP Pelvis Supine (Please label as SUPINE ) 3. Johnson Lateral Please provide the patient with a CD digital copy of these x-rays for my review, and mail to: Midlands Orthopaedics & Neurosurgery ATTN: Gross follow-up 1910 Blanding Street Columbia, SC 29201
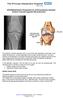
16 Instructions for Johnson Lateral for patients post hip resurfacing The perfect true lateral: Visualize the anterior and posterior neck, just inferior to the femoral component. The more neck Anteversion, the more the hip needs to be flexed Need to see cortex at Component-Neck junction C Fig True-lateral (Johnson or cross-table) lateral view. (A) Position of patient. The long axis of the left femoral neck is localized by imaging a line drawn between the anterosuperior iliac spine and the superior border of the symphysis pubis, determining the midpoint of the line, and then palpating the greater trochanter and imaging a point 1 inch
17 distal to it. A line drawn between these two points parallels the long axis of the femoral neck. (B) The cassette is placed in the vertical position with its cephalad border in contact with the body at the level of the iliac crest; it is parallel with the long axis of the femoral neck. The central ray is perpendicular to the long axis of the femoral neck and cassette and is centered 2.5 inches below the point of intersection of the localization lines. (C) Roentgenogram of hybrid surface arthroplasty. The ischium is toward the bottom of the image. (Fig. B, from Ballinger PW: Merill s Atlas of Radiographic Positions and Radiologic Procedures, 6 th Ed., Vol. 1. CV Mosby, St. Louis, 1986, with permission.)
18 Thomas P. Gross, M.D. Total Joint Replacement Midlands Orthopaedics 1910 Blanding Street Columbia, SC Phase II hip exercise/instruction sheet (after 6 weeks) Fast Recovery and Slow Down (Updated 6/29/2008 LAW) PHASE II: At six weeks, twelve weeks or later, it will be decided that you can progress to this phase. Do not attempt these exercises prior to formal instructions. 1. a.) Rapid Recovery Program: You should now be walking 1 mile or more without a cane or crutch. If you still feel somewhat weak or unbalanced, use of a cane for a few more weeks is occasionally necessary. You should start practicing climbing stairs; foot over foot with a handrail. Continue a progressive walking program; 1 to 2 miles per day is best. b.) Modified (slow down) recovery program: 10% weightbearing on operative leg with crutches for first six weeks post op. Use a cane for four weeks thereafter, no foot-over-foot stair climbing until off the cane at 2.5 months postoperatively. Do not start # 4 or # 6 until 2.5 months postoperatively. Refer to our website under current topics regarding bone health and hip resurfacing for guidance on managing your bone health over the long term. 2. Position precautions: You may now bend your hip past 90. Avoid extreme stretching or bending until 6 months post op. You can get to your feet safely by flexing your hip while keeping your knees out to the side. A foot stool may be helpful. It is perfectly safe to put on your shoes and socks. 3. Exercises: a. Stretching I. Sit in a chair with the knees apart and the feet together. Gently bend, reaching for the foot of the involved leg, feel the pulling and stretching. You should not feel sharp pain. Eventually, you will be able to reach your feet. II. Lie back on the bed; bend the knees up, keeping your feet together on the bed. Let the knees fall widely apart. Place your hands on the inside
19 of your thighs and gently push your knees apart. Feel the pulling and stretching in the groin. Again, sharp pain should not be felt. III. Quad stretching: lie prone on a surface as shown. Hold on to your ankle and bend the knee so that you feel a stretch. Hold for 30 seconds. Do 10 repetitions 3 times per day. IV. Psoas stretching: Stand grasping your operative ankle as shown. Bend knee further by pulling ankle toward buttocks. Do not lean forward or allow the back to arch. Hold 30 seconds. Do 10 repetitions 3 times per day. b. Leg Lifts - These should be done in two positions: supine (lying on your back), side (lying on the opposite side). I. Begin first in the supine position. Lift the leg approximately 12 inches off of the bed and hold it for a slow count of 10. During this count, contract all the muscles in the leg, performing an isometric contraction, and then slowly let the leg down to the bed. Work up to the point where you can do of these. When you can do 30 repetitions easily, add one pound of weight at the ankle and drop back to 15 repetitions, again working slowly back up to 30. You may either purchase commercial ankle weights or use a purse and hang it over your ankle. Put one can of food in it (approximately one pound). When you again reach 30 repetitions easily with one pound of weight, add a second pound, drop back to 15 and slowly work back up to 30. When you can perform 30 repetitions with two pounds, the muscles will be of normal strength.
20 II. After completing the exercises in the supine position, turn into the side lying position with the opposite hip down. Lift the leg approximately two feet away from the lower leg, keeping the knee straight, and hold for a count of five while performing an isometric contraction. Repeat again. Follow the same instructions as above for the number of repetitions and the addition of ankle weights. 4. Exercycle: If you have available an Exercycle, this will be a good exercise. The seat should be in a high position so that your hip is not flexed beyond 90 degrees. You should begin with gentle resistance to pedaling and work up to a normal resistance. You should use the Exercycle for between 10 and 20 minutes. This exercise is not essential, but is helpful if you have one available. Elliptical trainer or Nordic tracks are also excellent substitutes. Regular bicycles are fine at 6 months post op. We do not want you on a regular bike before this because your femur is weak and prone to fracture if you fall. (Patients on slow down program please don t start until you are off the cane.) 5. Swimming: This is an excellent exercise. You should use a gentle flutter kick and avoid the frog kick. The side stroke with a scissors kick is also allowable. Water aerobics are also an excellent form of exercise. 6. Workouts: If you have a gym membership to the gym, we encourage a gradually increasing program of light weight exercises gradually increasing to nor more than 50 lbs by 6 months post op. (Patients on slow down program please don t start until you are off the cane.) 7. Driving: If you have an automatic car, as soon as you feel strong and are not taking narcotics, you may drive. If the operative leg is the right, use the left to brake until you can walk without a limp. 8. Sexual Intercourse: As comfort will allow. Just remember not to flex the hip to extremes. 9. Dental Visits and surgical procedures: This is a recommendation you should follow all of your life. This is controversial in the medical and dental community, but it is my recommendation to you. Life time risk for infection spreading to your joint is less than ½%. You will need to take antibiotics prior to any dental procedure. The following is a guide but your dentist may substitute. If you are not allergic to penicillin, take: Amoxicillin 500 mgs x 4 tablets 1 hour prior to any dental procedure. If you are allergic to Amoxicillin or Penicillin, take: Clindamycin 600 mgs 1 hour prior to procedure. If possible, all dental work should be delayed until 6 weeks following surgery.
21 Antibiotic coverage for other surgical procedure or infections is individualized according to the possible bacterial contamination, and therefore, you should notify the respective physician or surgeon so they can prescribe the appropriate medication. Any infection should be treated promptly by your primary care physician 10. Moderation: In general, over the first year post op, all exercises and sports attempted should be approached gradually. There should be no sudden increase in activity level. You will be allowed full activity without restrictions after 6 months. Moderation will allow your implant to last longer. 11. Full Healing It takes up to one year for your hip to fully heal. Expect some soreness, swelling, and minor aches and pains during this time. At 6 months you have passed the risk period for femoral neck fracture. 12. Limitations until 6 months post op: 1. No bending the hip into extreme flexion (eg squatting) or crossing the legs at the knees 2. No lifting more than 50 lbs. routinely 3. No impact loading such as jumping and jogging If an activity (that you are contemplating performing prior to 6 months postop) does not violate these rules, you may do it. 13. Wound/scar appearance: Your scar will gradually fade over 1 year. It will get smoother and the purple color will disappear. There are many wound potions and scar lotions being sold. You may use them now, but be advised that there is no scientific evidence that they will improve the eventual appearance of your wound. Your wound will naturally mature and become fainter over 1 year whether or not you apply any potions. 14. Routine Follow up: I would like to see you personally here in the office for a checkup at 1 year post op. This is when you have reached the maximum medical improvement. There after we will ask you to provide us computer based followups at 2, 5, 10, and 15 years. Please do not hesitate to call us or come in at other times if you have a problem or concern. For out of state patients who can not travel here for the 1 year visit, we can arrange local follow up with a complete 4 part evaluation as follows: Computer based questions Brief narrative of your progress X-ray: AP of the pelvis and a frog lateral of your hip digitized on a CD Physical therapy exam
22 This information is available on our website 15. Bone Health: Even if you have good bone quality it is a smart general health policy to consume 1500mg of calcium and 1000 IU of vitamin D plus a multivitamin daily. If you have poor bone quality with a DEXAscan less than -1.5 please read more detailed information under bone health under current topics on our website. Do not hesitate to contact us for any reason, Dr. Gross and Lee Webb
23 Dear, I am writing to request that you obtain blood testing for metal ions as a part of your routine follow up of your hip A prescription is enclosed for Cobalt, Chromium, and Titanium levels. The test must be done at a Quest laboratory. This is a national lab with branches throughout the US. Please check the Internet for a location near you. You must avoid vitamins and other supplements for one week prior to testing. Recent scientific data suggests that this is a good method of evaluating metal bearing implants for wear. Enough evidence now exists for us to begin using blood levels for metal ions to monitor patients for implant wear problems. If we do discover elevated levels, I advocate closer follow up and further evaluation. All artificial implants wear at the bearing surface. If the bearing is metal on metal, this wear debris is cobalt and chromium. It usually gets absorbed by the body and transported to the kidney where it is removed from the body. In rare cases there is a higher than expected wear rate and these wear particles accumulate in the local tissues around the hip. If the load of particles gets too high, a local inflammation can result. If levels in the blood are high, this may indicate that the local tissues are overloaded. Therefore, measuring the blood levels is a good way to screen patients for high wear and possible local tissue reaction in the hip. I have personally performed over 3000 metal bearing hip resurfacings/ replacements in the last 10 years. I have only twice had to revise implants for this wear problem. The overall failure rate has been very low and other types of failures like fracture or loosening are far more common. Furthermore, in all revisions that I have performed for loosening of the cemented femoral resurfacing component, I have never come across a case of accelerated wear at the time of surgery. Furthermore, about 300,000 total knee replacements are done in the US yearly and research has shown that similar ion levels are measured with these implants as in hip resurfacings. Total Knee replacements have been performed in much higher numbers and for many more years than hip resurfacings. We therefore know that typical ion levels are well tolerated by most people. Nevertheless, I have become convinced that closer monitoring with metal levels is desirable. I suggest that we obtain levels beginning at 2 years post surgery and then repeat them every other year at the time of your routine follow up. If you come to see me in the office, I suggest that you have the levels drawn 2 4 weeks in advance so that the results are available for our visit. If your surgery was done over 2 years ago, anytime is a good time to get the first level. We should then recheck at the time of your every other year routine follow up dates. A prescription can be downloaded from my website. It is very important that the same laboratory always does these levels, because the results vary widely between labs. I have chosen Quest Laboratories, because they have a nationwide presence and have a good reputation. You should look up Quest labs online and make sure that your levels are done at one of their facilities or at a facility that sends their labs to Quest. If labs are drawn at Providence Northeast Hospital in Columbia, they are sent to Quest. Quest is specifically listed on my prescription as well to serve as a reminder. If your levels are done at any other lab, the results may not be comparable to the rest in my database. It is important that you avoid taking vitamin or mineral supplements for at least 1 week before testing. Many of these supplements contain chromium and can lead to false reports on the blood tests.
24 Any joint implants that contain cobalt chrome metal can raise your levels. This includes total knees, total hips, resurfacings, and total shoulders. I recommend routine follow up for all patients with joint replacements even if they are doing well. I constantly make an effort to contact patients and try to remind them that follow up is important. It is particularly important to monitor new technology regularly. My currently recommended follow up intervals are at 6 weeks, 1 year, 2 years, and every other year thereafter. The first two visits are best done at my office in person. After that time, remote follow up is adequate. Of course, you are always welcome to come see me at any time! At 2 years and beyond, information on how to complete remote follow up is on my website. The following items are now recommended at each evaluation: 1. Standing AP pelvis XR labeled standing (We require a digital DICOM image on a disc). 2. Questionnaire filled out online. Directions on my website. 3. Blood test: metal ion levels Cobalt and Chromium. A prescription is available on my website. If you have only one implant in your body, and the cobalt and Chromium levels are below 10ug/L each, we will just continue routine monitoring. If the levels are higher, further evaluation may be advised. If we receive your levels, I will send you a note that the levels are in the expected range, or I will contact you within 2 weeks of receiving the test results. If you don t hear from us, we have not received your test results. Please contact our office or the lab and be sure that the levels get to us. There will be no charge for reviewing your XR, questionnaire, and metal ion levels and sending you a notification. I would like to continue to monitor your results at routine intervals to be sure that you are doing well. If you have had revision surgery, I want to know about it. If you are having a problem, I would like to help you resolve it, if possible. Please keep in touch. With best Regards, Thomas P. Gross, MD
25 ( 803) Blanding St. Co lumbia,sc L ake Murray Blvd. Irmo, SC R FOR Address: Date: Request for a blood test for me tal ion leve ls of CO BA LT n a d C HROM I UM _ STOP TAKING VITAMINS AND MINERAL SUPPLEMENTS 1 WEEK PRIOR TO TEST. We request that test be performed at the patient s local QUEST laboratories, if possible. DIAGNOSIS: (choose one that applies) _OA, left hip (M16.12) _OA, right hip (M16.11) _OA, unspecified hip (M16.10) _Left hip pain (M25.552) _Right hip pain (M25.551) _Unspecified hip pain (M25.559) If you require an electronic prescription, please call: Tami Rhodes-Turner, Research Assistant to Dr. Thomas P Gross Phone: Please FAX to and give the patient a copy.
26 If you can't find a lab for metal ion tests from the following address, you can locate a lab from the link by yourself as well: NAME ADDRESS CITY STATE ZIP PHONE Quest Diagnostics Myrtle Beach 909 Medical Cir Myrtle Beach SC Quest Diagnostics Aiken 156 University Pkwy Ste 100 Aiken SC Quest Diagnostics Bluffton 25 Sherington Dr. Ste B Bluffton SC Quest Diagnostics Charleston West Ashley 1470 Tobias Gadson Blvd Suite 101 Charleston SC Quest Diagnostics James Island 418 Foly Road Sutie C Charleston SC Quest Diagnostics Columbia 3010 Farrow Rd Ste 110 Columbia SC Baptist Easley Hospital Specimen Collection Agreement 200 Fleetwood Dr Easley SC Quest Diagnostics Greenville 1003 Grove Rd Suite A Greenville SC Quest Diagnostics Greenwood 105 Vine Crest Court Suite 1300 Greenwood SC Quest Diagnostics Hilton Head Heritage 460 William Hilton Pkwy Hilton Head Island SC Marion County Medical Center Third Party Specimen Collection 2829 E Highway 76 Mullins SC Newberry County Memorial Hospital Purchased Service 2669 Kinard St Newberry SC Quick Draws Third Party Collection Site 10135d Clemson Blvd Seneca SC Quest Diagnostics Summerville 104 Morgan Pl Ste C Summerville SC
27 Quest Diagnostics Asheville 41 Oakland Rd Ste 150 Asheville NC Quest Diagnostics Charlotte University Mallard Creek Rd Ste 290 Charlotte NC Quest Diagnostics Fayetteville 3186 Village Dr Ste 202 Fayetteville NC Caldwell Memorial Hospital Specimen Collection Agreement 321 Mulberry St SW Lenoir NC Clinical Laboratory Service Third Party Collection Site 102 Lincoln Medical Park Lincolnton NC Lake Norman Regional Medical Center Third Party Specimen Collection 171 Fairview Rd Mooresville NC Medac 1 Third party Collection 4402 Shipyard Blvd Wilmington NC Medac II Third Party Collection Site 1142 Military Cutoff rd Wilmington NC Medac III Third Party Collection Site 8115 Market St Wilmington NC Quest Diagnostics Athens 1000 Hawthorne Ave Ste Q Athens GA Quest Diagnostics Augusta 1109 Medical Center Drive Suite 2A Augusta GA Evans Memorial Hosptial 200 N River St Claxton GA Eatonton Medical and Surgical Center 132 Sparta Highway Eatonton GA Candler Hosptia Rapid Response Testing and Specimen 5353 Reynolds St Savannah GA East Georgia Regional Medical Center PSA 1499 Fair Rd Statesboro GA McDuffie Regional Medical Center Third Party Specimen Collection 521 Hill Street, Southwest Thomson GA Vidalia Lab Services, Inc Specimen Collection Agreement 1802 Teston Ln Vidalia GA
HIP FOLLOW-UP. Thank you for your attention to this matter. If you have any questions, please contact us for assistance. Thomas P.
 HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety even
HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety even
KNEE FOLLOW-UP. Thank you for your attention to this matter. If you have any questions, please contact us for assistance. Thomas P.
 KNEE FOLLOW-UP It is important to review the status of your knee implant(s) during an office visit at four weeks, six months, one year and every other year postoperatively thereafter even though you are
KNEE FOLLOW-UP It is important to review the status of your knee implant(s) during an office visit at four weeks, six months, one year and every other year postoperatively thereafter even though you are
2-YEAR HIP FOLLOW-UP. 4) Metal Ion Test: Add your name to the prescription Have the test done at the nearest lab
 2-YEAR HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety
2-YEAR HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety
6-WEEK HIP FOLLOW-UP. 2) Please sign the Mission statement and disclosure form and send it to us
 6-WEEK HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety
6-WEEK HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year, two years, and every other year postoperatively thereafter for your safety
HIP FOLLOW-UP. 2) Please sign the Mission statement and disclosure form and send it to us
 HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year and every other year postoperatively thereafter for your safety even though you are
HIP FOLLOW-UP It is important to review the status of your hip implant(s) during an office visit at six weeks, one year and every other year postoperatively thereafter for your safety even though you are
KNEE FOLLOW-UP. Thank you for your attention to this matter. If you have any questions, please contact us for assistance. Thomas P.
 KNEE FOLLOW-UP It is important to review the status of your knee implant(s) during an office visit at four weeks, six months, one year, two years, and every other year postoperatively thereafter even if
KNEE FOLLOW-UP It is important to review the status of your knee implant(s) during an office visit at four weeks, six months, one year, two years, and every other year postoperatively thereafter even if
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated
 Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
Postoperative Days 1-7
 ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty
![Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty](/thumbs/90/102636395.jpg) Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Introduction Hip arthritis is a common problem, most often due to osteoarthritis. In hip arthritis affects a patient,
Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Introduction Hip arthritis is a common problem, most often due to osteoarthritis. In hip arthritis affects a patient,
Move your ankle inward toward your other foot and then outward away from your other foot.
 TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Total Hip Replacement Exercise Guide
 Total Hip Replacement Exercise Guide Regular exercise to restore strength and mobility to your hip and a gradual return to everyday activities are important for your full recovery after hip replacement.
Total Hip Replacement Exercise Guide Regular exercise to restore strength and mobility to your hip and a gradual return to everyday activities are important for your full recovery after hip replacement.
ILIOTIBIAL BAND SYNDROME
 Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Diagnosis: s/p ( LEFT / RIGHT ) Injury to MCL of the Knee -- Surgery Date:
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET
 TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Speed Your Recovery. After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint.
 FO R THE TO TAL KNEE REPLACEMENT PATIENT Speed Your Recovery After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint. The exercises may
FO R THE TO TAL KNEE REPLACEMENT PATIENT Speed Your Recovery After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint. The exercises may
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description Maintain appropriate conditioning: The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the
ILIOTIBIAL BAND SYNDROME Description Maintain appropriate conditioning: The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
Rehabilitation After Patellar Tendon Debridement Surgery
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Hip Replacement PROGRAM. Nightingale. Home Healthcare
 Hip Replacement PROGRAM TM Nightingale Home Healthcare Why Do I Need A Hip Replacement? Hip replacements are performed for one reason; something has happened to the hip joint that has made it 1) too painful
Hip Replacement PROGRAM TM Nightingale Home Healthcare Why Do I Need A Hip Replacement? Hip replacements are performed for one reason; something has happened to the hip joint that has made it 1) too painful
Total Knee Replacement
 Total Knee Replacement STEPHEN M. DESIO, M.D. Hospital Stay Most patients are in the hospital for two to three days. A Case Manager is part of our team whom you will meet after surgery. We will work together
Total Knee Replacement STEPHEN M. DESIO, M.D. Hospital Stay Most patients are in the hospital for two to three days. A Case Manager is part of our team whom you will meet after surgery. We will work together
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
While it s unlikely you ll meet all of us you can expect to see more than one physio during your stay in hospital.
 Introduction: This information is provided to give you and your family a basic knowledge of the total hip replacement operation, outlining the things you should know, both before and after surgery. The
Introduction: This information is provided to give you and your family a basic knowledge of the total hip replacement operation, outlining the things you should know, both before and after surgery. The
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises. Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises
 Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Lesson Sixteen Flexibility and Muscular Strength
 Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
Total Knee Replacement Exercise Guide
 Total Knee Replacement Exercise Guide This article is also available in Spanish: Ejercicio después de reemplazo de rodilla (topic.cfm?topic=a00494). Regular exercise to restore your knee mobility and strength
Total Knee Replacement Exercise Guide This article is also available in Spanish: Ejercicio después de reemplazo de rodilla (topic.cfm?topic=a00494). Regular exercise to restore your knee mobility and strength
Knee Arthroscopy Exercise Guide
 Importance of Exercise Patrick J McGahan, MD http://orthodoc.aaos.org/patrickmcgahan Sacramento Orthopedic Center 2801 K St, Suite 330 Sacramento, CA 95816 USA Phone: 916-733-5049 Fax: 916-733-8914 Knee
Importance of Exercise Patrick J McGahan, MD http://orthodoc.aaos.org/patrickmcgahan Sacramento Orthopedic Center 2801 K St, Suite 330 Sacramento, CA 95816 USA Phone: 916-733-5049 Fax: 916-733-8914 Knee
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
Knee Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers
 CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
Hofmann Arthritis Institute Precision Joint Replacement 24 South 1100 East Suite 101 Salt Lake City, UT JOINT
 Hofmann Arthritis Institute Precision Joint Replacement 24 South 1100 East Suite 101 Salt Lake City, UT 84102 801-35-JOINT AFTER YOUR TOTAL HIP REPLACEMENT Your full recovery from your total hip replacement
Hofmann Arthritis Institute Precision Joint Replacement 24 South 1100 East Suite 101 Salt Lake City, UT 84102 801-35-JOINT AFTER YOUR TOTAL HIP REPLACEMENT Your full recovery from your total hip replacement
Patellofemoral Pain Syndrome
 What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella)
 Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
BACK AND LEG PAIN ASSESSMENT (Prior Surgery)
 ANSWER EVERY QUESTION! SPINE SURGERY LTD. (IMPORTANT PATIENT INFORMATION FORM) BACK AND LEG PAIN ASSESSMENT (Prior Surgery) 1. NAME: DATE TODAY: 2. AGE: SEX: 3. PRESENTLY EMPLOYED? NO YES, How long there?
ANSWER EVERY QUESTION! SPINE SURGERY LTD. (IMPORTANT PATIENT INFORMATION FORM) BACK AND LEG PAIN ASSESSMENT (Prior Surgery) 1. NAME: DATE TODAY: 2. AGE: SEX: 3. PRESENTLY EMPLOYED? NO YES, How long there?
LOW BACK PAIN. Contents What causes Low Back Pain?... 3
 YOUR GUIDE TO LOW BACK PAIN An IPRS Guide to provide you with exercises and advice to ease your condition Contents What causes Low Back Pain?....... 3 What treatment can I receive?..... 4 What about exercise?...............
YOUR GUIDE TO LOW BACK PAIN An IPRS Guide to provide you with exercises and advice to ease your condition Contents What causes Low Back Pain?....... 3 What treatment can I receive?..... 4 What about exercise?...............
Knee Exercises. Having strong, flexible muscles is the best way to keep knees healthy and prevent further injury.
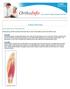 Knee Exercises If my knee hurts, why exercise? Having strong, flexible muscles is the best way to keep knees healthy and prevent further injury. Strength Strengthening the muscles that support your knee
Knee Exercises If my knee hurts, why exercise? Having strong, flexible muscles is the best way to keep knees healthy and prevent further injury. Strength Strengthening the muscles that support your knee
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY
 REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
Source: Exercise in Arthritis
 Exercise in Arthritis Regular exercise boosts fitness and helps reverse joint stiffness with RA. Decrease Pain, Increase Energy Exercise more to decrease pain and feel more energetic? Hardly seems possible
Exercise in Arthritis Regular exercise boosts fitness and helps reverse joint stiffness with RA. Decrease Pain, Increase Energy Exercise more to decrease pain and feel more energetic? Hardly seems possible
This advice and exercises have been selected to help you manage the symptoms of your arthritis
 This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
Knee Conditioning Program
 Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
GETTING READY FOR TOTAL HIP REPLACEMENT
 GETTING READY FOR TOTAL HIP REPLACEMENT Pre-Op Exercises for a Better Recovery Your Recovery Begins Now Even if your hip replacement surgery is weeks or months away, start getting ready now. People who
GETTING READY FOR TOTAL HIP REPLACEMENT Pre-Op Exercises for a Better Recovery Your Recovery Begins Now Even if your hip replacement surgery is weeks or months away, start getting ready now. People who
STRETCHING. Low Back Rotation. Double Leg Pull. Single Leg Pull. Core Home Exercise Program
 Core Home Exercise Program Seth L. Sherman, M.D. Tamara L. Young, ATC, OTC, M.Ed Department of Sports Medicine STRETCHING Low Back Rotation While lying on your back with both of your knees bent. Rotate
Core Home Exercise Program Seth L. Sherman, M.D. Tamara L. Young, ATC, OTC, M.Ed Department of Sports Medicine STRETCHING Low Back Rotation While lying on your back with both of your knees bent. Rotate
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Home Program
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
Hip Resurfacing with Precautions. Therapy Resources. xpe045 (4/2015) AHC
 Hip Resurfacing with Precautions Therapy Resources xpe045 (4/2015) AHC Hip Resurfacing Home Exercise Program - Phase I 1. Breathing Exercises Exercise can be done while sitting or lying down. Action: Place
Hip Resurfacing with Precautions Therapy Resources xpe045 (4/2015) AHC Hip Resurfacing Home Exercise Program - Phase I 1. Breathing Exercises Exercise can be done while sitting or lying down. Action: Place
Hip Replacement Recovery Guide
 Hip Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Safe Activities & Movements... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering...
Hip Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Safe Activities & Movements... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering...
It s your knee. Help keep it that way PERSONALIZED TOTAL KNEE IMPLANTS
 It s your knee Help keep it that way PERSONALIZED TOTAL KNEE IMPLANTS Osteoarthritis the disease Osteoarthritis (OA) is the most common form of arthritis, affecting tens of millions of people worldwide.
It s your knee Help keep it that way PERSONALIZED TOTAL KNEE IMPLANTS Osteoarthritis the disease Osteoarthritis (OA) is the most common form of arthritis, affecting tens of millions of people worldwide.
Integra. Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION
 Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
Lumbar decompression or discectomy
 Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
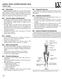 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
Physiotherapy Services. Physiotherapy Guide. Hip Replacement
 Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Post Lung Transplant Exercises
 Post Lung Transplant Exercises Post Lung Transplant Physical activity improves our strength and stamina, maintains optimal functioning of our major organs and increases our vitality, energy and overall
Post Lung Transplant Exercises Post Lung Transplant Physical activity improves our strength and stamina, maintains optimal functioning of our major organs and increases our vitality, energy and overall
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
return to sports after injury IMPROVING STRENGTH, POWER, AND AGILITY
 return to sports after injury IMPROVING STRENGTH, POWER, AND AGILITY This booklet is designed for people recovering from a knee or leg injury who participate in recreational or competitive sports such
return to sports after injury IMPROVING STRENGTH, POWER, AND AGILITY This booklet is designed for people recovering from a knee or leg injury who participate in recreational or competitive sports such
Total hip replacement
 Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Post-Op Physical Therapy Protocol for ACL-MCL Reconstruction. Post-Operative Weeks 0-2: Weight-bearing: 1. Non-weightbearing x 4 weeks.
 Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Op Physical Therapy Protocol
Adam J. Farber, MD Sports Medicine and Orthopaedic Surgery Board Certified; Fellowship-trained in Sports Medicine & Arthroscopic Surgery P: 480-219-3342; F: 480-219-3271 Post-Op Physical Therapy Protocol
ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE
 ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE PHASE 1: THE FIRST SIX WEEKS AFTER INJURY (grade 2 and 3) THREE WEEKS AFTER INJURY (grade 1) The knee should be
ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE PHASE 1: THE FIRST SIX WEEKS AFTER INJURY (grade 2 and 3) THREE WEEKS AFTER INJURY (grade 1) The knee should be
Knee Replacement Rehabilitation
 Knee Replacement Rehabilitation The following exercises may be given to you to help get you moving and become more independent. Please bring this copy of the exercises with you to hospital. After your
Knee Replacement Rehabilitation The following exercises may be given to you to help get you moving and become more independent. Please bring this copy of the exercises with you to hospital. After your
Physical Therapy for Distal Femoral Replacement
 PATIENT EDUCATION patienteducation.osumc.edu Physical Therapy for Distal Femoral Replacement This book has information about your distal femoral replacement and the exercises you will need to do after
PATIENT EDUCATION patienteducation.osumc.edu Physical Therapy for Distal Femoral Replacement This book has information about your distal femoral replacement and the exercises you will need to do after
Iliotibial Band Tendinitis (Runner s Knee)
 Iliotibial Band Tendinitis (Runner s Knee) ANATOMY The iliotibial band (or tract) is a thick band of tissue that starts on the pelvis and upper thigh and passes along the outside of the knee and attaches
Iliotibial Band Tendinitis (Runner s Knee) ANATOMY The iliotibial band (or tract) is a thick band of tissue that starts on the pelvis and upper thigh and passes along the outside of the knee and attaches
Developed by: Physiotherapy Department Surrey Memorial Hospital. Printshop #
 Developed by: Physiotherapy Department Surrey Memorial Hospital Printshop # 255171 The following exercises are intended for you to continue at home. Your physiotherapist will teach and mark the exercises
Developed by: Physiotherapy Department Surrey Memorial Hospital Printshop # 255171 The following exercises are intended for you to continue at home. Your physiotherapist will teach and mark the exercises
Knee Home Exercise Program Clayton W. Nuelle, MD RANGE OF MOTION
 Knee Home Exercise Program Clayton W. Nuelle, MD RANGE OF MOTION Heel Prop/Quad Isometric While lying flat on a table with knee straight, place heel on a rolled towel. Heel must be high enough so that
Knee Home Exercise Program Clayton W. Nuelle, MD RANGE OF MOTION Heel Prop/Quad Isometric While lying flat on a table with knee straight, place heel on a rolled towel. Heel must be high enough so that
Iliotibial (IT) Band Syndrome
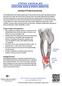 Iliotibial (IT) Band Syndrome The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon passes
Iliotibial (IT) Band Syndrome The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon passes
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
YOUR TOTAL HIP REPLACEMENT. General Guide to getting you back to function.
 YOUR TOTAL HIP REPLACEMENT General Guide to getting you back to function. Topics to Cover Walking, step climbing, functional mobility, use of assistive devices Transfers in and out of bed, car, chairs
YOUR TOTAL HIP REPLACEMENT General Guide to getting you back to function. Topics to Cover Walking, step climbing, functional mobility, use of assistive devices Transfers in and out of bed, car, chairs
Stretching. Knees: Rotate your knees in a circle, keeping them together and bending down slightly.
 Stretching Stretching the Major Muscle Groups Static Stretches Hamstrings: Hang down and try to reach your toes; don t push it. Keep legs and back straight. Just go down to a comfortable level for your
Stretching Stretching the Major Muscle Groups Static Stretches Hamstrings: Hang down and try to reach your toes; don t push it. Keep legs and back straight. Just go down to a comfortable level for your
Ex Fix Rehab Phase II Strengthening
 Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Copyright Cardiff University
 This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life
 Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
21-Day Belly Blast Challenge!
 21-Day Belly Blast Challenge! "BONUS" Workouts! Copyright 2013 by LifeFuel Fitness and BrightLion Fitness LLC DISCLAIMER: This e-book is for information purposes only. The information presented is in no
21-Day Belly Blast Challenge! "BONUS" Workouts! Copyright 2013 by LifeFuel Fitness and BrightLion Fitness LLC DISCLAIMER: This e-book is for information purposes only. The information presented is in no
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
A FROZEN SHOULDER YOUR GUIDE TO. An IPRS Guide to provide you with exercises and advice to ease your condition
 YOUR GUIDE TO A FROZEN SHOULDER Contents Introduction................................................... 2 What is Frozen Shoulder?........................................ 3 What are the symptoms of Frozen
YOUR GUIDE TO A FROZEN SHOULDER Contents Introduction................................................... 2 What is Frozen Shoulder?........................................ 3 What are the symptoms of Frozen
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
PGYVC Volleyball Circuit Athletic Plan
 PGYVC Volleyball Circuit Athletic Plan Workout Plan: This workout plan is to introduce and promote off court training for PGYVC athletes as well as to build confidence for athletes who have not done physical
PGYVC Volleyball Circuit Athletic Plan Workout Plan: This workout plan is to introduce and promote off court training for PGYVC athletes as well as to build confidence for athletes who have not done physical
Patellofemoral Osteoarthritis
 Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Strategies to live better and preserve function with knee arthritis Thursday, 06 November :06
 WHILE it seems counterintuitive that exercise would be good for an already sore joint, Cleveland Clinic experts say that even with knee arthritis, you can (and should) stay active and, by doing so, you
WHILE it seems counterintuitive that exercise would be good for an already sore joint, Cleveland Clinic experts say that even with knee arthritis, you can (and should) stay active and, by doing so, you
Body Bar FLEX. Exercises for the Core and Abdominals. by Gordon L. Brown, Jr. for Body Bar, Inc.
 Body Bar FLEX Exercises for the Core and Abdominals by Gordon L. Brown, Jr. for Body Bar, Inc. 1 Exercises for the Core and Abdominals This presentation features stretching and strengthening exercises
Body Bar FLEX Exercises for the Core and Abdominals by Gordon L. Brown, Jr. for Body Bar, Inc. 1 Exercises for the Core and Abdominals This presentation features stretching and strengthening exercises
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
Plantar Fasciitis and Heel Pain
 PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
Please review the below items in preparation for your visit.
 2001 Santa Monica Blvd., Suite #760W Santa Monica, CA 90404 (310) 582-7474 (Office) (310) 582-7481 (Fax) http://california.providence.org/saint-johns/services/orthopedics/ http://www.totaljoints.net/ Dear
2001 Santa Monica Blvd., Suite #760W Santa Monica, CA 90404 (310) 582-7474 (Office) (310) 582-7481 (Fax) http://california.providence.org/saint-johns/services/orthopedics/ http://www.totaljoints.net/ Dear
Reversed geometry shoulder replacement
 Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
