Treatment of Gastroesophageal Reflux Disease: Use of Algorithms to Aid in Management
|
|
|
- Louisa Lewis
- 6 years ago
- Views:
Transcription
1 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 94, No. 11, Suppl., by Am. Coll. of Gastroenterology ISSN /99/$20.00 Published by Elsevier Science Inc. PII S (99) Treatment of Gastroesophageal Reflux Disease: Use of Algorithms to Aid in Management Philip O. Katz, M.D., F.A.C.G. Department of Medicine, The Graduate Hospital, Philadelphia, Pennsylvania ABSTRACT Effective treatment of gastroesophageal reflux disease demands an awareness of several factors: the disease spectrum, its varied symptom presentation, and potential complications; when to refer to a gastroenterologist or surgeon; and the various treatment options available. By taking these factors into consideration, algorithms can provide a useful framework within which clinicians can approach decision making regarding management of gastroesophageal reflux disease. As such, algorithms can be a good clinical tool for meeting the goals of effective disease management. Presented below are treatment algorithms for the primary care physician, gastroenterologist, and surgeon. Improved understanding of these algorithms can assist clinicians in the care of patients with this common disease. (Am J Gastroenterol 1999;94(Suppl.):S3 S by Am. Coll. of Gastroenterology) INTRODUCTION Gastroesophageal reflux disease (GERD) is perhaps the most common problem seen in medical practice. Approximately 10% of the U.S. population experiences heartburn daily, and 40% of the population has heartburn monthly. Almost 40 million individuals use over-the-counter antacids or histamine-2 (H2) receptor antagonists at least twice weekly to relieve symptoms. Effective treatment requires an awareness of the clinical spectrum of GERD, its varied symptomatology and potential complications, the reasons for referral, and the many treatment options available. An effective management algorithm, care pathway, or clinical roadmap for GERD can assist physicians in selecting appropriate treatment. At the same time, it can educate physicians by providing a review of symptom presentation, indications for specialist referral, and a stepped-care treatment approach. The ideal algorithm is flexible, with appropriate emphasis on the inherent variability of disease presentation and the treatment options available. This review discusses the components of three GERD management algorithms for primary care physicians, subspecialists, and surgeons useful to physicians who regularly treat and refer patients with GERD. The primary care algorithm (Fig. 1) (1) provides a framework for management that focuses on both acute and longterm maintenance therapy the key to managing a disease that is usually chronic. The algorithm emphasizes the typical presentations of GERD, those that may be treated empirically, and the atypical and alarm symptoms that suggest early referral to a specialist. The subspecialist algorithm (Fig. 2) (1) uses endoscopy as a focal point for evaluation and ambulatory ph monitoring as a diagnostic adjunct. As such, it outlines different management approaches for erosive and nonerosive esophagitis and intestinal metaplasia (Barrett s esophagus). The surgery algorithm reviews the indications and preoperative workup for antireflux surgery (Fig. 3) (1). CLINICAL PRESENTATION AND NATURAL HISTORY Typical Symptoms The most common symptom of GERD is heartburn, a sometimes burning pain behind the breastbone, which is seen daily in up to 10% of the U.S. population and at least monthly in about 40% of the population (2 4). Millions seek treatment regularly using over-the-counter antireflux products. Regurgitation, the spontaneous return of gastric contents into the esophagus or mouth, is another common symptom (3). When present together, heartburn and regurgitation establish the diagnosis of GERD with more than 90% certainty, and patients can be treated empirically without further diagnostic testing (Fig. 1). Large meals, high-fat meals, spicy foods, and citrus products are more likely to produce heartburn. Cola drinks, coffee, tea, and beer can have an acidic ph and alter the pressure of the lower esophageal sphincter, causing symptoms when ingested. Late-night meals, eaten before bedtime or accompanied by alcohol, can predispose patients to nighttime symptoms (Table 1). Heartburn is highly specific for GERD, and it is almost always diagnostic. If it is the only presenting esophageal symptom, it is likely due to GERD. There is one major exception. A heartburn-like symptom, believed to be due to esophageal stasis from outflow obstruction, is often described in patients with achalasia. Fermentation of undigested food in the esophagus, coupled with inflammation, can create a heartburn-like sensation in the absence of true GERD. The presence or the frequency of heartburn is not predic-
2 S4 Katz AJG Vol. 94, No. 11, Suppl., 1999 Figure 1. A primary care approach to gastroesophageal reflux disease. LSM lifestyle modifications; OTC over the counter; H 2 RA H2-receptor antagonist; PPI proton pump inhibitor. Adapted with permission from (1). tive of the degree of endoscopic damage to the distal esophagus. Only 50 60% of patients with heartburn who seek medical attention have erosive esophagitis on endoscopy. The remainder will be diagnosed with nonerosive GERD (5). Severe disease, including Barrett s esophagus and peptic strictures, can occur with infrequent or no heartburn, just as many patients with daily heartburn will show no endoscopic abnormalities. The natural history of GERD is not well studied. Although symptoms are chronic and recurrent, most patients with esophagitis will not progress beyond the endoscopic stage seen at initial examination. In a series of 701 patients followed for up to 29 years, only 23% progressed to a more serious grade of esophagitis (6). Among patients with reflux symptoms and no esophagitis (nonerosive GERD), less than 15% progressed to a higher grade over 6 months (7). Extraesophageal (Atypical) Symptoms Many atypical or extraesophageal symptoms (Fig. 1) are associated with GERD, including unexplained substernal chest pain without evidence of coronary artery disease (noncardiac chest pain), asthma, bronchitis, chronic cough, recurrent pneumonia, hoarseness, chronic posterior laryngitis, globus sensation, otalgia, aphthous ulcers, hiccups, and erosion of dental enamel. The prevalence of these atypical or extraesophageal symptoms and their frequency in the general population have not been studied as extensively as has heartburn. A large survey (3) designed to assess the prevalence of GERD in the general population found that 23% experienced unexplained chest pain at some point within a year and 40% had symptoms occurring over more than 5 years. Asthma was reported by 9%, bronchitis by 20%, and chronic hoarseness by 15% of patients with typical GERD
3 AJG November, Suppl., 1999 Algorithms for GERD S5 Figure 2. A subspecialist (gastroenterologist) approach to diagnosing heartburn/gastroesophageal reflux disease (GERD) symptoms that are severe, atypical, or refractory to therapy. H 2 RA H2-receptor antagonist; PPI proton pump inhibitor. Adapted with permission from (1). symptoms. In comparison, asthma and bronchitis each affect about 6% of the general population (8). The frequency of heartburn and regurgitation among patients with atypical symptoms has been debated. In the population-based study noted above (3), patients with heartburn and regurgitation experienced atypical symptoms about 80% of the time. Such symptoms were more common among patients with frequent heartburn than among those Figure 3. A surgical approach to gastroesophageal reflux disease (GERD). Adapted with permission from (1).
4 S6 Katz AJG Vol. 94, No. 11, Suppl., 1999 Table 1. Lifestyle Modifications Useful in Patients With GERD Elevate head of bed (6 inches); avoid waterbed Sleep on left side Make dietary modifications Eat less fat, more protein Avoid irritants Citrus juice Tomato products Coffee Cola Alcohol Chocolate Do not eat before sleeping (allow 2 h) Decrease or stop smoking Avoid potentially harmful medications Anticholinergics Sedatives/tranquilizers Theophylline Prostaglandins Calcium channel blockers Alendronate Take antacids or alginic acid Take over-the-counter doses of H2-receptor antagonists (can be used prophylactically) with no GERD symptoms. Among patients with unexplained chest pain, more than 80% had heartburn or regurgitation. Among patients with asthma, bronchitis, hoarseness, or pneumonia, approximately 60% had heartburn or regurgitation. Heartburn was not predictive of otolaryngological symptoms (3). In a recent case-control study from the Veterans Administration, patients with a discharge diagnosis of erosive esophagitis had twice the prevalence of associated otolaryngological symptoms as control patients without esophagitis (9). The absence of heartburn and regurgitation should not preclude a diagnosis of GERD in patients with atypical symptoms. Prospective studies using endoscopy and ambulatory ph monitoring have found GERD in as many as 75% of patients with chronic hoarseness (10), in 70 80% of patients with asthma (11, 12), and in 20% of patients with chronic cough (13). Approximately 45% of patients with unexplained chest pain and normal coronary arteries have GERD (14). Esophagitis is seen in less than 10% of patients with GERD (15). Endoscopic esophagitis is seen in 30 40% of patients with asthma (16, 17) and in about 20% of patients with reflux laryngitis. The cause-and-effect relation between GERD and asthma is unclear. A careful history among patients with asthma reveals heartburn or regurgitation in 50%. Late onset, the absence of a seasonal or allergic component, and onset after ingestion of a large meal or alcohol suggest GERD-related asthma. Reflux is the third most common cause of chronic cough, after postnasal drip and bronchitis. Hoarseness is the most common otolaryngological symptom of GERD. Although most studies suggest that heartburn is present in about 50% of patients who experience hoarseness, in our experience a careful history reveals heartburn in about 75% (18). Other associated symptoms include halitosis, throat clearing, dry cough, coated tongue, globus sensation, tickle in the throat, chronic sore throat, and postnasal drip. Nausea and erosion of dental enamel can also occur with GERD. GERD COMPLICATIONS GERD can present with severe complications, including peptic stricture, ulceration, iron deficiency anemia, and, most important, Barrett s esophagus. The latter is characterized by a change from normal squamous epithelium to a metaplastic intestinal-type epithelium with typical special staining. It is a premalignant condition. Approximately 2 10% of GERD patients have strictures (10) and 9 12% have Barrett s esophagus (5, 19). Complicated GERD is suggested by a number of warning symptoms: dysphagia, odynophagia, early satiety, vomiting, or bleeding (Fig. 1). Slowly progressive dysphagia, particularly for solids, suggests peptic strictures. Liquid and solid dysphagia suggests a GERD-related motility disorder. Odynophagia is rare in reflux and, when present, suggests ulceration or inflammation, most frequently associated with infectious or pillinduced esophagitis. Ineffective esophageal motility is also more prevalent among reflux patients with associated respiratory symptoms (20). Occasionally, esophagitis presents with occult upper GI bleeding or iron deficiency anemia (21). These warning symptoms mandate early diagnostic intervention to rule out a diagnosis other than GERD (Fig. 2). GERD CHRONICITY Ample evidence shows that patients with reflux esophagitis will have endoscopic and symptomatic relapse up to 80% of the time if therapy is discontinued or drug dosage is decreased. Studies in patients with extraesophageal (atypical) GERD suggest similar findings. Recurrence of hoarseness was seen within 6 months of therapy in one study (22). The clinical impression is that all GERD is chronic, with individual patients expressing this chronicity in different ways. Most patients, especially those with erosive esophagitis or extraesophageal disease, will require continuous medical therapy or surgery to achieve adequate symptom relief. TREATMENT Patient Education and Lifestyle Modification Patient education regarding lifestyle modification is the foundation of therapy in GERD. Simple changes in lifestyle can be effective in controlling heartburn and dyspepsia (Table 1). The basics of therapy include instructing patients to decrease their fat intake, eat small meals, refrain from eating within 2 3 hours of bedtime, avoid lying down after meals, stop smoking, and elevate the head of the bed 6 inches. Overnight ph-monitoring studies show that a significant decrease in total esophageal acid exposure is
5 AJG November, Suppl., 1999 Algorithms for GERD S7 achieved by elevating the head of the bed, with the improvement more pronounced in combination with drug therapy (23). A similar effect can be achieved by placing a foam rubber wedge (10-inch maximal elevation) under the patient s head on top of the mattress. A recent study suggests that sleeping on the right side results in more frequent reflux compared with sleeping on the left side or in the supine position (24). Potential esophageal irritants such as citrus juices, tomato products, coffee, colas, and alcohol should be restricted. Medications that can decrease esophageal pressures and promote reflux include anticholinergics, sedatives or tranquilizers (particularly benzodiazepines), tricyclic antidepressants, theophylline, prostaglandins, and calcium channel blockers. Pills such as potassium tablets, nonsteroidal anti-inflammatory drugs, and alendronate can cause esophagitis. The intermittent use of antacids, alginic acid, or over-the-counter H2-receptor antagonists (which are available in half the prescription strength and are indicated for up to 2 weeks of continuous use) can improve symptoms. These medications can be used as they are needed or expected to be needed. H2-Receptor Antagonists H2-receptor antagonists have been the mainstays of therapy for patients with heartburn and dyspepsia. The four such available agents cimetidine, ranitidine, famotidine, and nizatidine have only one known mechanism of action in treating patients with reflux disease, namely, a decrease in gastric acid production. They have no clinical effect on lower esophageal sphincter pressure or esophageal or gastric emptying. Used in standard doses (equivalent to ranitidine 150 mg twice daily), these drugs can achieve symptomatic relief in about 60% of patients (25, 26). Endoscopic resolution of documented esophagitis is seen in about 50% of patients (27). Smaller doses are effective in symptom relief or prevention, thus supporting the over-the-counter availability of half-strength H2-receptor antagonists. High-dose H2-receptor antagonists (ranitidine 150 mg q.i.d. or its equivalent) result in healing rates of up to 75% (28). The cost of this larger dosage, coupled with compliance issues, makes this choice a less efficacious one than proton pump inhibitors (PPIs), which provide equal or greater efficacy with once-daily therapy. Prokinetic Agents The pathogenesis of GERD is related to defects in esophagogastric motility, lower esophageal sphincter incompetence, poor esophageal clearance, and delayed gastric emptying. Therapy directed at correcting these defects allows improvement in GERD symptoms without suppression of gastric acid. Cisapride, the most widely prescribed prokinetic agent, increases GI motility and enhances salivary flow, thus enhancing its buffering capacity. Improvements in daytime and nocturnal heartburn have been demonstrated with cisapride 10 mg q.i.d. (29) and 20 mg b.i.d. (30). GERD symptoms suggestive of dysmotility, such as postprandial bloating, fullness, early satiety, belching, and regurgitation, are also significantly reduced by cisapride (31, 32). Cisapride and H2-receptor antagonists show comparable efficacy (32) and healing of mild to moderate esophagitis (33, 34). The combination of cisapride with cimetidine or ranitidine enhances healing and symptom relief compared with either agent alone (35 37). However, the cost and side effects of this regimen compared with PPIs have diminished its use. Cisapride 10 mg b.i.d. and 20 mg at bedtime is effective in preventing relapse (38, 39), especially among patients with grade I or II esophagitis. Ample evidence demonstrates that both H2-receptor antagonists and cisapride can provide effective long-term control of GERD in about 50% of patients, and both are most likely to be effective in patients with less severe degrees of esophagitis (40). Proton Pump Inhibitors Many studies suggest that PPIs are the most effective medical therapy to control GERD symptoms and heal esophagitis. Omeprazole 20 mg or lansoprazole 30 mg daily is more effective than either placebo or standard-dose H2-receptor antagonists in this regard, with mean symptomatic relief in more than 80% of patients and esophagitis healing in upward of 90% (41 43) over 4 8 weeks. Omeprazole 20 mg and lansoprazole 30 mg have shown equal healing rates ( 90%) in direct comparisons (44). In grades III and IV esophagitis, however, the healing rate is lower (80%), often necessitating higher doses (45). Recent evidence shows that some patients will continue to secrete gastric acid and have gastroesophageal reflux even at doses of omeprazole as high as 20 mg b.i.d. or lansoprazole 30 mg b.i.d. (46). Klinkenberg-Knol et al. (47) first documented effective long-term control of GERD with a PPI. Continuous therapy with omeprazole at mg/d maintained esophagitis healing for up to 5 years. They also emphasized the need for larger doses among some patients for effective long-term maintenance. Other investigators have reported similar findings (48). These reports suggest that long-term maintenance therapy can be effective in up to 100% of GERD patients if appropriate doses are used. The study of Klinkenberg-Knol et al. has been extended to 11 years and supports continued efficacy (49). Rabeprazole, a new agent in this class awaiting U.S. clinical approval, has been shown in comparative clinical trials to be similar in efficacy to omeprazole for the treatment of GERD (50, 51). Initial clinical trials suggest that it is highly effective in preventing long-term relapse of esophagitis and heartburn among patients with erosive or ulcerative GERD. Moreover, it appears to be well tolerated and to have a favorable safety profile in early clinical trials (51, 52). Pantoprazole, another new PPI awaiting clinical approval, has been shown in a 1-year clinical trial to be highly effective for long-term prophylaxis of reflux esophagitis
6 S8 Katz AJG Vol. 94, No. 11, Suppl., 1999 (53). Results of this study indicate that it also has a good safety profile. The need for larger doses of PPIs has increased the use of combined intragastric and esophageal ph monitoring to evaluate the adequacy of acid suppression and reflux control among patients with continued symptoms or in those in whom profound acid suppression is desired (e.g., patients with Barrett s esophagus) (54 56). The same technique can be used to monitor the level of PPI therapy required for each patient and, as such, it has redefined medical failure (57). This technique has an important use in the patient who fails to respond to treatment because of overnight recovery of acid secretion accompanied by reflux, which might not cause symptoms during sleep (46). Antireflux Surgery Refinements, including the use of laparoscopic techniques, have changed our approach to antireflux surgery. The good success rate of fundoplication about 90% after 3 years, with minimal complications makes it an attractive option for some patients. Use of a short, loose, floppy fundoplication markedly reduces the postoperative sequelae associated with antireflux surgery, including dysphagia and gas bloat (58, 59). Most patients are able to belch normally, and long-term dysphagia is now uncommon after fundoplication. These benefits are achieved without sacrificing efficacy in controlling reflux of gastric contents in the esophagus. Indications for surgery (Fig. 3) in the patient with GERD are controversial. Medical failure is rare and in itself is not an indication for surgery. Antireflux surgery should be considered for the treatment of patients with objectively documented, relatively severe GERD, including patients with erosive esophagitis, stricture, and Barrett s esophagus, and for those without severe mucosal injury who require continuous high-dose PPIs for long-term symptom relief. Patients with atypical or respiratory symptoms who respond well to intensive medical treatment should be considered. The option of antireflux surgery should be given to all patients who require long-term aggressive medical therapy, particularly if escalating doses of PPIs are needed to control symptoms. Antireflux surgery may be the preferred option for patients less than 50 years of age, for those whose medications are a financial burden, for those who are noncompliant with their drug regimen, and for those who prefer a single intervention to long-term drug treatment. Patients who do not respond to PPI therapy and those with atypical chest pain are not likely to benefit from surgery. Diagnostic evaluation before surgery is critical to determine whether gastroesophageal reflux is the underlying cause of the patient s symptoms (60). Objective evidence of GERD is usually obtained by 24-hour esophageal ph testing. The preferred surgical approach is based on an assessment of esophageal motility (61). Patients with normal contractions do well with a 360 Nissen fundoplication. When peristalsis is absent or severely disordered ( 50% simultaneous contractions) or when motility is ineffective (amplitude 30 mm Hg or nontransmitted contractions in 30% of wet swallows), partial fundoplication is the procedure of choice. A short esophagus can affect the ability to perform an adequate repair and thereby increase the risk of surgical failure. Esophageal length is best assessed using barium swallow and endoscopy. A short esophagus should be suspected if a large ( 5 cm) hiatal hernia is present, particularly if it fails to reduce in the upright position on a video barium esophagram. Complications after elective antireflux surgery are uncommon, particularly with laparoscopic fundoplication. Death is rare, whether the procedure is open or closed. In a recent collective review, 4 of 2453 patients died (62). Complications arise, on average, in 10 15% of patients and tend to be minor (63). Laparoscopic fundoplication has further decreased the complications associated with surgical access and postoperative recovery. Unrecognized perforation of the esophagus or stomach is the most life-threatening sequela and is related to the surgeon s experience (58). The results of several series of laparoscopic fundoplication have now been published (59, 64, 65). Relief of typical reflux symptoms (heartburn, regurgitation, and dysphagia) is seen in more than 90% of patients after up to 3 years of follow-up. A conversion rate of 4.2% to open surgery, a 0.5% rate of early reoperation, and excellent to good symptomatic improvement in 91% of patients are reported. Postoperative dysphagia has decreased to a rate of 3 5% with increasing experience and attention to technical details (66). Esophageal acid exposure returns to normal in nearly all patients. Although the laparoscopic technique is exciting, these excellent results are from centers with extensive experience. Accordingly, when deciding whether to recommend surgical treatment, one must evaluate the experience and results obtained at a particular surgical center and also consider whether referral to a more experienced surgical center is appropriate. APPROACH TO THE PATIENT The approach to the patient must be individualized. Patients with heartburn and regurgitation as their primary symptoms can be treated empirically with consideration given to the stepped-care approach outlined in Figure 1. Each level of therapeutic trial should last 4 8 weeks before moving to the next step. Several options are available at each step, and decisions should be based on cost, patient and physician familiarity with the agent, and the possibility of side effects from drug interactions. Complete symptom relief should be the goal of acute therapy. Maintenance should be attempted with the least costly agent available. Consideration should be given to a trial off medications (continuing lifestyle modifications) to see whether symptoms recur. Early diagnostic evaluation is suggested for patients with extraesophageal (atypical) symptoms (Fig. 1) or warning
7 AJG November, Suppl., 1999 Algorithms for GERD S9 symptoms of dysphagia, early satiety, weight loss, or bleeding (Figs. 1 and 2). Referral should be considered in patients with persistent symptoms after a course of empirical therapy or in patients who require continuous daily therapy. Diagnostic evaluation usually begins with endoscopy (Fig. 2), with ambulatory ph monitoring used in patients with negative findings or atypical symptoms. Patients with grade III or IV erosive esophagitis or atypical symptoms should be treated with PPIs, with increasing dosage if symptoms are refractory. Combination therapy with a prokinetic agent can be considered, particularly in patients with abnormal gastric emptying. Antireflux surgery should also be considered for such patients after documentation of adequate symptom relief. Every patient should be treated with the goal of achieving complete long-term symptom relief. A careful, thoughtful approach to the patient with GERD should produce a successful outcome in nearly all patients. The algorithms presented here will aid in that process. Reprint requests and correspondence: Philip O. Katz, M.D., F.A.C.G., The Graduate Hospital, Department of Medicine, 1800 Lombard Street, Suite 501, Pepper Pavilion, Philadelphia, PA Received Mar. 29, 1999; accepted Aug. 3, REFERENCES 1. Castell DO, Brunton SA, Earnest DL, et al. GERD: Management algorithms for the primary care physician and the specialist. Pract Gastroenterol 1998;22: A Gallup survey on heartburn across America. The Gallup Organization, Locke GR, Talley NJ, Fett SL, et al. Prevalence and clinical spectrum of gastroesophageal reflux: A population-based study in Olmstead County, Minnesota. Gastroenterology 1997;112: Nebel OT, Fornes MF, Castell DO. Symptomatic gastroesophageal reflux: Incidence and precipitating factors. Am J Dig Dis 1976;21: Winters C, Spurling TJ, Chobanian SJ, et al. Barrett s esophagus: A prevalent, occult complication of gastroesophageal reflux disease. Gastroenterology 1987;92: Ollyo JB, Monnier P, Fontolliet C, et al. The natural history, prevalence and incidence of reflux esophagitis. Gullet 1993; 3(suppl): Pace F, Santalucia F, Bianchi Porro G. Natural history of gastro-oesophageal reflux disease without esophagitis. Gut 1991;32: Centers for Disease Control. Vital Health Statistics 1995; 10(199): El-Serag HB, Sonnenberg A. Comorbid occurrence of laryngeal or pulmonary disease with esophagitis in United States military veterans. Gastroenterology 1997;113: Koufman JA. The otolaryngologic manifestations of gastroesophageal reflux disease (GERD): A clinical investigation of 225 patients using ambulatory 24-hour ph monitoring and an experimental investigation of the role of acid and pepsin in the development of laryngeal injury. Laryngoscope 1991;101: Harding SM, Guzzo MR, Richter JE. Prevalence of GERD in asthmatics without reflux symptoms: A prospective study. Gastroenterology 1997;4:A141 (abstract). 12. Sontag SJ, O Connell S, Khandelwal S, et al. Most asthmatics have gastroesophageal reflux with or without bronchodilator therapy. Gastroenterology 1990;99: Irwin RS, French CL, Curley FJ, et al. Chronic cough due to gastroesophageal reflux. Clinical, diagnostic and pathogenic aspects. Chest 1993;104: Hewson EG, Sinclair JW, Dalton CB, et al. Twenty-four-hour esophageal ph monitoring: The most useful test for evaluating noncardiac chest pain. Am J Med 1991;90: Cherian P, Smith LF, Bardhan KD, et al. Esophageal tests in the evaluation of non-cardiac chest pain. Dis Esophagus 1995; 8: Larrain A, Carrasco E, Galleguillos F, et al. Medical and surgical treatment of nonallergic asthma associated with gastroesophageal reflux. Chest 1991;99: Sontag SJ, Schnell TG, Miller TQ, et al. Prevalence of oesophagitis in asthmatics. Gut 1992;33: Govil Y, Katz P, Srinivasan R, et al. Anti-reflux therapy improves symptoms in patients with reflux laryngitis. Gastroenterology 1998;114:A138 (abstract). 19. Lieberman DA, Oehlke M, Helfand M, et al. Risk factors for Barrett s esophagus in community-based practice. Am J Gastroenterol 1997;92: Fouad YM, Khoury R, Hatlebakk JG, et al. Ineffective esophageal motility (IEM) is more prevalent in reflux patients with respiratory symptoms. Gastroenterology 1998;114:A123 (abstract). 21. Spechler SJ. Complications of gastroesophageal reflux disease. In: Castell DO, ed. The esophagus. Boston: Little Brown and Company; 1992: Kamel PL, Hanson D, Kahrilas PJ. Omeprazole for the treatment of posterior laryngitis. Am J Med 1994;96: Johnson LF, DeMeester TR. Evaluation of elevation of the head of the bed, bethanechol, and antacid foam tablets on gastroesophageal reflux. Dig Dis Sci 1981;26: Khoury R, Mohiuddin M, Katz P, et al. Influence of body position on nighttime recumbent reflux in patients with GERD. Gastroenterology 1998;114:A174 (abstract). 25. DeVault KR, Castell DO. Current diagnosis and treatment of gastroesophageal reflux disease. Mayo Clin Proc 1994;69: Tougas G, Armstrong D. Efficacy of H 2 receptor antagonists in the treatment of gastroesophageal reflux disease and its symptoms. Can J Gastroenterol 1997;11(suppl B):51 4B. 27. Chiba N, de Gara CJ, Wilkinson JM, et al. Speed of healing and symptom relief in grade II to IV gastroesophageal reflux disease: A meta-analysis. Gastroenterology 1997;112: McCarty-Dawson D, Sue SO, Morill B, et al. Ranitidine versus cimetidine in the healing of erosive esophagitis. Clin Ther 1996;18: Richter JE, Long JF. Cisapride for gastroesophageal reflux disease: A placebo-controlled, double-blind study. Am J Gastroenterol 1995;90: Castell D, Sigmund C, Patterson D, et al. Cisapride 20 mg BID provides effective daytime and nighttime relief in patients with symptoms of chronic gastroesophageal reflux disease. Gastroenterology 1997;112:A84 (abstract). 31. Robertson CS, Evans DF, Ledingham SJ, et al. Cisapride in the treatment of gastro-oesophageal reflux disease. Aliment Pharmacol Ther 1993;7: Tytgat GNJ, Anker Hansen OJ, Carling L, et al. Effect of cisapride on relapse of reflux oesophagitis, healed with an antisecretory drug. Scand J Gastroenterol 1992;27: Janisch HD, Huttemann W, Bouzo MH. Cisapride versus
8 S10 Katz AJG Vol. 94, No. 11, Suppl., 1999 ranitidine in the treatment of reflux esophagitis. Hepatogastroenterology 1988;35: Galmiche JP, Fraitag B, Filoche B, et al. Double-blind comparison of cisapride and cimetidine in the treatment of reflux esophagitis. Dig Dis Sci 1990;35: Galmiche JP, Brandstatter G, Evreux M, et al. Combined therapy with cisapride and cimetidine in severe reflux oesophagitis: A double blind controlled trial. Gut 1988;29: Inauen W, Emde C, Weber B, et al. Effects of ranitidine and cisapride on acid reflux and oesophageal motility in patients with reflux oesophagitis: A 24 hour ambulatory combined ph and manometry study. Gut 1993;34: McKenna CJ, Mills JG, Goodwin C, et al. Combination of ranitidine and cisapride in the treatment of reflux oesophagitis. Eur J Gastroenterol Hepatol 1995;7: Toussaint J, Gossuin A, Deruyttere M, et al. Healing and prevention of relapse of reflux oesophagitis by cisapride. Gut 1991;32: Blum AL, Adami B, Bouzo MH, et al. Effect of cisapride on relapse of esophagitis: A multinational, placebo-controlled trial in patients healed with an antisecretory drug. Dig Dis Sci 1993;38: Vigneri S, Termini R, Leandro G, et al. A comparison of five maintenance therapies for reflux esophagitis. N Engl J Med 1995;333: Hallerback B, Unge P, Carling L, et al. Omeprazole or ranitidine in long-term treatment of reflux esophagitis. Gastroenterology 1994;107: Klinkenberg-Knol EC, Festen HP, Jansen JM, et al. Doubleblind multicentre comparison of omeprazole and ranitidine in the treatment of reflux oesophagitis. Lancet 1987;1: Havelund T, Laursen LS, Skoubo-Kristensen E, et al. Omeprazole and ranitidine in treatment of reflux oesophagitis: Double blind comparative trial. BMJ 1988;296: Castell DO, Richter JE, Robinson M, et al. Efficacy and safety of lansoprazole in the treatment of erosive reflux esophagitis. Am J Gastroenterol 1996;91: Leite LP, Johnston BT, Just RJ, et al. Persistent acid secretion during omeprazole therapy: A study of gastric acid profiles in patients demonstrating failure of omeprazole therapy. Am J Gastroenterol 1996;91: Peghini P, Katz P, Bracy NA, et al. Nocturnal recovery of gastric acid secretion with twice-daily dosing of proton pump inhibitors. Am J Gastroenterol 1998;93: Klinkenberg-Knol EC, Festen HPM, Jansen JBMJ, et al. Long-term treatment with omeprazole for refractory reflux esophagitis: Efficacy and safety. Ann Intern Med 1994;121: Hendel J, Hendel L, Hage E, et al. Monitoring of omeprazole treatment in gastro-oesophageal reflux disease. Eur J Gastroenterol Hepatol 1996;8: Klinkenberg-Knol EC. Eleven years experience of continuous maintenance treatment with omeprazole in GERD-patients. Gastroenterology 1998;114:A180 (abstract). 50. Dekkers CPM, Beker JA, Thjodleifsson B, et al. Double-blind, placebo-controlled comparison of rabeprazole 20 mg vs. omeprazole 20 mg in the treatment of erosive or ulcerative gastrooesophageal reflux disease. Aliment Pharmacol Ther 1999;13: Humphries TJ, Dekkers CPM, Beker JA, et al. Rabeprazole vs omeprazole for maintenance therapy of healed erosive GERD: Results of a 1-year European Multicenter Trial. Am J Gastroenterol 1998;93:1616 (abstract). 52. Birbara C, Breiter J, Collins D, et al. Rabeprazole: Preventing endoscopic and symptomatic relapse in erosive or ulcerative GERD. Am J Gastroenterol 1998;93:1630 (abstract). 53. Mossner J, Koop H, Porst H, et al. One-year prophylactic efficacy and safety of pantoprazole in controlling gastrooesophageal reflux symptoms in patients with healed reflux oesophagitis. Aliment Pharmacol Ther 1997;11: Klinkenberg-Knol EC, Meuwissen S. Combined gastric and oesophageal 24-hour ph monitoring and oesophageal manometry in patients with reflux disease resistant to treatment with omeprazole. Aliment Pharmacol Ther 1990;4: Castell DO. Omeprazole works best when used properly. Eur J Gastroenterol Hepatol 1996;8: Katzka DA, Castell DO. Successful elimination of reflux symptoms does not insure adequate control of acid reflux in Barrett s esophagus. Am J Gastroenterol 1994;89: Katzka DA, Paoletti V, Leite L, et al. Prolonged ambulatory ph monitoring in patients with persistent gastroesophageal reflux disease symptoms: Testing while on therapy identifies need for more aggressive anti-reflux therapy. Am J Gastroenterol 1996;91: Schauer PR, Meyers WC, Eubanks S, et al. Mechanisms of gastric and esophageal perforations during laparoscopic Nissen fundoplication. Ann Surg 1996;223: Hinder RA, Filipi CJ, Wetscher G, et al. Laparoscopic Nissen fundoplication is an effective treatment for gastroesophageal reflux disease. Ann Surg 1994;220: Waring JP, Hunter JG, Oddsdottir M, et al. The preoperative evaluation of patients considered for laparoscopic antireflux surgery. Am J Gastroenterol 1995;90: Kauer WK, Peters JH, DeMeester TR, et al. A tailored approach to antireflux surgery. J Thorac Cardiovasc Surg 1995; 110: Perdikis G, Hinder RA, Lund RJ, et al. Laparoscopic Nissen fundoplication: Where do we stand? Surg Laparosc Endosc 1997;7: Urschel JD. Complications of antireflux surgery. Am J Surg 1993;165: Hunter JG, Trus TL, Branum GD, et al. A physiologic approach to laparoscopic fundoplication for gastroesophageal reflux disease. Ann Surg 1996;223: Jamieson GG, Watson DI, Britten-Jones R, et al. Laparoscopic Nissen fundoplication. Ann Surg 1994;220: Peters JH, Heimbucher J, Kauer WKH, et al. Clinical and physiologic comparison of laparoscopic and open Nissen fundoplication. J Am Coll Surg 1995;180:
Unmet Needs in the Management of Gastroesophageal Reflux Disease
 Unmet Needs in the Management of Gastroesophageal Reflux Disease Ronnie Fass MD Professor of Medicine Case Western Reserve University Chairman, Division of Gastroenterology and Hepatology Director, Esophageal
Unmet Needs in the Management of Gastroesophageal Reflux Disease Ronnie Fass MD Professor of Medicine Case Western Reserve University Chairman, Division of Gastroenterology and Hepatology Director, Esophageal
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease
 ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
SASKATCHEWAN REGISTERED NURSES ASSOCIATION
 DEFINITION Reflux of gastric contents into the esophagus, which results in esophageal irritation or inflammation. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dysphagia (solid food, progressive)
DEFINITION Reflux of gastric contents into the esophagus, which results in esophageal irritation or inflammation. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dysphagia (solid food, progressive)
GASTROESOPHAGEAL REFLUX DISEASE. William M. Brady
 Drugs of Today 1998, 34(1): 25-30 Copyright PROUS SCIENCE GASTROESOPHAGEAL REFLUX DISEASE William M. Brady Section of General Internal Medicine, Temple University School of Medicine, Philadelphia, Pennsylvania,
Drugs of Today 1998, 34(1): 25-30 Copyright PROUS SCIENCE GASTROESOPHAGEAL REFLUX DISEASE William M. Brady Section of General Internal Medicine, Temple University School of Medicine, Philadelphia, Pennsylvania,
Putting Chronic Heartburn On Ice
 Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Gastroesophageal reflux (GER) Gastroesophageal reflux (GER), the passage of gastric contents into the esophagus, is a normal physiologic process that
 Gastroesophageal reflux (GER) Gastroesophageal reflux (GER), the passage of gastric contents into the esophagus, is a normal physiologic process that may occur daily in healthy infants, children and adults.
Gastroesophageal reflux (GER) Gastroesophageal reflux (GER), the passage of gastric contents into the esophagus, is a normal physiologic process that may occur daily in healthy infants, children and adults.
GERD: A linical Clinical Clinical Update Objectives
 GERD: A Clinical Update Jeff Gilbert, M.D. University i of Kentucky Gastroenterology 11/6/08 Objectives To review the basic pathophysiology underlying gastroesophageal reflux disease To highlight current
GERD: A Clinical Update Jeff Gilbert, M.D. University i of Kentucky Gastroenterology 11/6/08 Objectives To review the basic pathophysiology underlying gastroesophageal reflux disease To highlight current
Maximizing Outcome of Extraesophageal Reflux Disease. (GERD) is often accompanied
 ...PRESENTATIONS... Maximizing Outcome of Extraesophageal Reflux Disease Based on a presentation by Peter J. Kahrilas, MD Presentation Summary Gastroesophageal reflux disease (GERD) accompanied by regurgitation
...PRESENTATIONS... Maximizing Outcome of Extraesophageal Reflux Disease Based on a presentation by Peter J. Kahrilas, MD Presentation Summary Gastroesophageal reflux disease (GERD) accompanied by regurgitation
GERD. Gastroesophageal reflux disease, or GERD, occurs when acid from the. stomach backs up into the esophagus. Normally, food travels from the
 GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
Gastroesophageal Reflux Disease, Paraesophageal Hernias &
 530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
Gastroesophageal Reflux Disease (GERD)
 Gastroesophageal Reflux Disease (GERD) Information for patients UHN Read this handout to learn about: What gastroesohageal reflux (GERD) is Signs and symptoms How your doctor will know if you have it Tests
Gastroesophageal Reflux Disease (GERD) Information for patients UHN Read this handout to learn about: What gastroesohageal reflux (GERD) is Signs and symptoms How your doctor will know if you have it Tests
GERD DIAGNOSIS & TREATMENT DISCLOSURES 4/18/2018
 GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
Speaker disclosure. Objectives. GERD: Who and When to Treat 7/21/2015
 GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
Review article: gastric acidity ) comparison of esomeprazole with other proton pump inhibitors
 Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 10 15. Review article: gastric acidity ) comparison of esomeprazole with other proton pump inhibitors J. G. HATLEBAKK Department of Medicine, Haukeland Sykehus,
Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 10 15. Review article: gastric acidity ) comparison of esomeprazole with other proton pump inhibitors J. G. HATLEBAKK Department of Medicine, Haukeland Sykehus,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Achalasia, barium esophagography for, 57 58 Acid pocket, 18 19 Acid-sensing ion, 20 Acupuncture, 128 Adiponectin, in obesity, 166 ADX10059 metabotropic
Note: Page numbers of article titles are in boldface type. A Achalasia, barium esophagography for, 57 58 Acid pocket, 18 19 Acid-sensing ion, 20 Acupuncture, 128 Adiponectin, in obesity, 166 ADX10059 metabotropic
Refractory GERD : case presentation and discussion
 Refractory GERD : case presentation and discussion Ping-Huei Tseng National Taiwan University Hospital May 19, 2018 How effective is PPI based on EGD? With GERD symptom 75% erosive 25% NERD Endoscopy 81%
Refractory GERD : case presentation and discussion Ping-Huei Tseng National Taiwan University Hospital May 19, 2018 How effective is PPI based on EGD? With GERD symptom 75% erosive 25% NERD Endoscopy 81%
GASTROESOPHAGEAL REFLUX
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (404) 270-7479 GASTROESOPHAGEAL REFLUX DEFINITION: *MONTREAL CONSENSUS DEFINED GERD AS A CONDITION WHICH
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (404) 270-7479 GASTROESOPHAGEAL REFLUX DEFINITION: *MONTREAL CONSENSUS DEFINED GERD AS A CONDITION WHICH
https://www.uptodate.com/contents/acid-reflux-gastroesophageal-reflux-disease-in-adults-...
 Page 1 of 10 Official reprint from UpToDate www.uptodate.com 2017 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment.
Page 1 of 10 Official reprint from UpToDate www.uptodate.com 2017 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment.
Refractory GERD. Kenneth R. DeVault, MD, FACG President American College of Gastroenterology Chair Department of Medicine Mayo Clinic Florida
 Refractory GERD Kenneth R. DeVault, MD, FACG President American College of Gastroenterology Chair Department of Medicine Mayo Clinic Florida Objectives Define the terminology associated with refractory
Refractory GERD Kenneth R. DeVault, MD, FACG President American College of Gastroenterology Chair Department of Medicine Mayo Clinic Florida Objectives Define the terminology associated with refractory
NEGATIVE ENDOSCOPY, What is the Diagnosis and Treatment?
 NEGATIVE ENDOSCOPY, PPI REFRACTORY REFLUX: What is the Diagnosis and Treatment? Michael F. Vaezi, MD, PhD, MSc, FACG Professor of Medicine Clinical Director Division of Gastroenterology, Hepatology and
NEGATIVE ENDOSCOPY, PPI REFRACTORY REFLUX: What is the Diagnosis and Treatment? Michael F. Vaezi, MD, PhD, MSc, FACG Professor of Medicine Clinical Director Division of Gastroenterology, Hepatology and
Refractory GERD: What s a Gastroenterologist To Do?
 Refractory GERD: What s a Gastroenterologist To Do? Philip O. Katz, MD, FACG Chairman, Division of Gastroenterology Einstein Medical Center Clinical Professor of Medicine Jefferson Medical College Philadelphia,
Refractory GERD: What s a Gastroenterologist To Do? Philip O. Katz, MD, FACG Chairman, Division of Gastroenterology Einstein Medical Center Clinical Professor of Medicine Jefferson Medical College Philadelphia,
TBURN TBURN BURN ARTBURN EARTBURN EART HEARTBURN: HOW TO GET IT OFF YOUR CHEST
 TBURN BURN TBURN ARTBURN. EARTBURN EART N EARTBURN HEARTBURN: HOW TO GET IT OFF YOUR CHEST Do you sometimes wake up at night with a sharp, burning sensation in your chest? Does this sometimes happen during
TBURN BURN TBURN ARTBURN. EARTBURN EART N EARTBURN HEARTBURN: HOW TO GET IT OFF YOUR CHEST Do you sometimes wake up at night with a sharp, burning sensation in your chest? Does this sometimes happen during
ACID REFLUX & GERD: The Unsettling Reality in Canada
 ACID REFLUX & GERD: The Unsettling Reality in Canada gerd fact 1 see page 8 Canadian Society of Intestinal Research On average, ARD patients wait over two years before seeking care 1. 1 gerd fact 2 see
ACID REFLUX & GERD: The Unsettling Reality in Canada gerd fact 1 see page 8 Canadian Society of Intestinal Research On average, ARD patients wait over two years before seeking care 1. 1 gerd fact 2 see
Gastroesophageal reflux disease (GERD) is the. Gastroesophageal Reflux Disease in the Elderly A SPECIAL ARTICLE INTRODUCTION PATHOGENESIS
 Gastroesophageal Reflux Disease in the Elderly Maxwell Chait Gastroesophageal reflux disease (GERD) is the most common upper gastrointestinal problem seen in adults. Although the elderly have fewer complaints
Gastroesophageal Reflux Disease in the Elderly Maxwell Chait Gastroesophageal reflux disease (GERD) is the most common upper gastrointestinal problem seen in adults. Although the elderly have fewer complaints
Reflux of gastric contents, particularly acid, into the esophagus
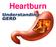 Heartburn Reflux of gastric contents, particularly acid, into the esophagus Patient assessment with GERD 1-signs and symptoms The hallmark of typical symptom of GERD is heartburn (restrosternal),acid regurgitation,
Heartburn Reflux of gastric contents, particularly acid, into the esophagus Patient assessment with GERD 1-signs and symptoms The hallmark of typical symptom of GERD is heartburn (restrosternal),acid regurgitation,
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Effective Health Care
 Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
Achalasia is a rare disease with an annual incidence estimated REVIEWS. Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
Management of reflux disease
 iv67 DYSPEPSIA MANAGEMENT Management of reflux disease J Dent... The management of reflux disease can be divided into three major phases, the first being diagnosis and severity assessment, the second,
iv67 DYSPEPSIA MANAGEMENT Management of reflux disease J Dent... The management of reflux disease can be divided into three major phases, the first being diagnosis and severity assessment, the second,
Review article: pharmacology of esomeprazole and comparisons with omeprazole
 Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 5 9. Review article: pharmacology of esomeprazole and comparisons with omeprazole J. DENT Department of Gastroenterology, Hepatology and General Medicine, Royal
Aliment Pharmacol Ther 2003; 17 (Suppl. 1): 5 9. Review article: pharmacology of esomeprazole and comparisons with omeprazole J. DENT Department of Gastroenterology, Hepatology and General Medicine, Royal
Disclosures. Proton Pump Inhibitors Deprescribing? Deprescribing PPI Objectives. Deprescribing. Proton Pump Inhibitors (PPI) 5/28/2018.
 Proton Pump Inhibitors Deprescribing? None Disclosures Chad Burski, MD Assistant Professor of Medicine UAB Gastroenterology Deprescribing PPI Objectives AR Why? Who? How? The mechanism of action of Proton
Proton Pump Inhibitors Deprescribing? None Disclosures Chad Burski, MD Assistant Professor of Medicine UAB Gastroenterology Deprescribing PPI Objectives AR Why? Who? How? The mechanism of action of Proton
James Paget University Hospitals. NHS Foundation Trust. Hiatus hernia. Patient Information
 James Paget University Hospitals NHS Foundation Trust Hiatus hernia Patient Information What is a hiatus hernia? A hiatus hernia can cause highly irritating stomach contents, such as acid, to move up into
James Paget University Hospitals NHS Foundation Trust Hiatus hernia Patient Information What is a hiatus hernia? A hiatus hernia can cause highly irritating stomach contents, such as acid, to move up into
GERD: 2014 Dilemmas and Solutions. Ronnie Fass MD, FACP Professor of Medicine Case Western Reserve University
 GERD: 2014 Dilemmas and Solutions Ronnie Fass MD, FACP Professor of Medicine Case Western Reserve University How to Maximize Your PPI Treatment? Improve compliance and adherance Fass R. Am J Gastroenterol.
GERD: 2014 Dilemmas and Solutions Ronnie Fass MD, FACP Professor of Medicine Case Western Reserve University How to Maximize Your PPI Treatment? Improve compliance and adherance Fass R. Am J Gastroenterol.
Optimizing Medical Therapy for Gastroesophageal Reflux Disease: State of the Art Philip O. Katz, MD
 TREATMENT UPDATE Optimizing Medical Therapy for Gastroesophageal Reflux Disease: State of the Art Philip O. Katz, MD Department of Medicine, Graduate Hospital, Philadelphia, PA Potential interventions
TREATMENT UPDATE Optimizing Medical Therapy for Gastroesophageal Reflux Disease: State of the Art Philip O. Katz, MD Department of Medicine, Graduate Hospital, Philadelphia, PA Potential interventions
Burning Issues in Gastroesophageal Reflux Disease (GERD)
 3:45 4:45pm Burning Issues in GERD SPEAKER Prateek Sharma, MD, FACG, FACP Presenter Disclosure Information The following relationships exist related to this presentation: Prateek Sharma, MD, FACG, FACP,
3:45 4:45pm Burning Issues in GERD SPEAKER Prateek Sharma, MD, FACG, FACP Presenter Disclosure Information The following relationships exist related to this presentation: Prateek Sharma, MD, FACG, FACP,
Gastroesophageal Reflux Disease (GERD)
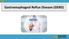 Gastroesophageal Reflux Disease (GERD) Acid Reflux Acid reflux occurs when acid from the stomach moves backwards into the esophagus. Heartburn Heartburn is a symptom of acid reflux and GERD. It may feel
Gastroesophageal Reflux Disease (GERD) Acid Reflux Acid reflux occurs when acid from the stomach moves backwards into the esophagus. Heartburn Heartburn is a symptom of acid reflux and GERD. It may feel
The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality
 Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Definition: gas tro e soph a ge al re f lux dis ease (GERD) from Stedman's Medical Dictionary for the Health Professions and Nursing
 Topic Page: Gastroesophageal reflux Definition: gas tro e soph a ge al re f lux dis ease (GERD) from Stedman's Medical Dictionary for the Health Professions and Nursing (gas trō-ĕ-sof ă-jē ăl rē flŭks
Topic Page: Gastroesophageal reflux Definition: gas tro e soph a ge al re f lux dis ease (GERD) from Stedman's Medical Dictionary for the Health Professions and Nursing (gas trō-ĕ-sof ă-jē ăl rē flŭks
Treatment Options for GERD or Acid Reflux Disease A Review of the Research for Adults
 Treatment Options for GERD or Acid Reflux Disease A Review of the Research for Adults hur till återvinna från prostataoperation Is This Information Right for Me? Yes, if: A doctor said that you have gastroesophageal
Treatment Options for GERD or Acid Reflux Disease A Review of the Research for Adults hur till återvinna från prostataoperation Is This Information Right for Me? Yes, if: A doctor said that you have gastroesophageal
Gastro-oesophageal reflux disease and peptic ulcer disease. By: Dr. Singanamala Suman Assistant Professor Department of Pharm.D
 Gastro-oesophageal reflux disease and peptic ulcer disease By: Dr. Singanamala Suman Assistant Professor Department of Pharm.D Gastro-oesophageal reflux disease and peptic ulcer disease Learning objectives:
Gastro-oesophageal reflux disease and peptic ulcer disease By: Dr. Singanamala Suman Assistant Professor Department of Pharm.D Gastro-oesophageal reflux disease and peptic ulcer disease Learning objectives:
Many patients with gastroesophageal reflux
 ... HEALTH ECONOMICS... Efficacy and Cost Effectiveness of Lansoprazole Versus Omeprazole in Maintenance Treatment of Symptomatic Gastroesophageal Reflux Disease Eva Vivian, PharmD; Anthony Morreale, PharmD,
... HEALTH ECONOMICS... Efficacy and Cost Effectiveness of Lansoprazole Versus Omeprazole in Maintenance Treatment of Symptomatic Gastroesophageal Reflux Disease Eva Vivian, PharmD; Anthony Morreale, PharmD,
Peptic ulcer disease Disorders of the esophagus
 Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Oesophageal Disorders
 Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
GERD. More Than Just Heartburn. written by Harvard Medical School
 GERD More Than Just Heartburn written by Harvard Medical School www.patientedu.org Doctors call it gastroesophageal reflux disease, or GERD. Millions of Americans call it heartburn. Many more also have
GERD More Than Just Heartburn written by Harvard Medical School www.patientedu.org Doctors call it gastroesophageal reflux disease, or GERD. Millions of Americans call it heartburn. Many more also have
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Page 1. Objectives. The Role of the Pharmacist as Gatekeeper to the Appropriate Use of OTC PPI Therapy in Frequent Heartburn
 Page 1 The Role of the Pharmacist as Gatekeeper to the Appropriate Use of OTC PPI Therapy in The Role of the Pharmacist as Gatekeeper to the Appropriate Use of OTC PPI Therapy in Colin W. Howden, MD, FRCP
Page 1 The Role of the Pharmacist as Gatekeeper to the Appropriate Use of OTC PPI Therapy in The Role of the Pharmacist as Gatekeeper to the Appropriate Use of OTC PPI Therapy in Colin W. Howden, MD, FRCP
Lansoprazole Treatment of Patients With Chronic Idiopathic Laryngitis: A Placebo-Controlled Trial
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 4, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02244-4 Lansoprazole Treatment
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 4, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02244-4 Lansoprazole Treatment
Gastroesophageal Reflux (GER) and Gastroesophageal Reflux Disease (GERD) in Adults
 Gastroesophageal Reflux (GER) and Gastroesophageal Reflux Disease (GERD) in Adults National Digestive Diseases Information Clearinghouse What is GER? Gastroesophageal reflux (GER) occurs when stomach contents
Gastroesophageal Reflux (GER) and Gastroesophageal Reflux Disease (GERD) in Adults National Digestive Diseases Information Clearinghouse What is GER? Gastroesophageal reflux (GER) occurs when stomach contents
Eosinophilic Esophagitis (EoE)
 Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Heartburn, also referred to acid reflux, happens when stomach acid flows back (refluxes) into your esophagus.
 WHILE almost everyone experiences mild heartburn from time to time and many individuals have some antacids or another medication on hand for its relief, talk to your doctor, if you have heartburn more
WHILE almost everyone experiences mild heartburn from time to time and many individuals have some antacids or another medication on hand for its relief, talk to your doctor, if you have heartburn more
SELF CARE OF HEARTBURN
 O P I N I O N SelfCare 2010;1(2):77-82 In each issue, UK General Practitioner Dr. James Kennedy considers a common medical problem and summarises the pragmatic evidence-based advice that can be offered
O P I N I O N SelfCare 2010;1(2):77-82 In each issue, UK General Practitioner Dr. James Kennedy considers a common medical problem and summarises the pragmatic evidence-based advice that can be offered
Gastroesophageal Reflux Disease (GERD)
 Quality Department Guidelines for Clinical Care Ambulatory GERD Guideline Team Team Leader Joel J Heidelbaugh, MD Family Medicine Team Members R Van Harrison, PhD Learning Health Sciences Mark A McQuillan,
Quality Department Guidelines for Clinical Care Ambulatory GERD Guideline Team Team Leader Joel J Heidelbaugh, MD Family Medicine Team Members R Van Harrison, PhD Learning Health Sciences Mark A McQuillan,
Medical Policy Manual. Topic: Gastric Reflux Surgery Date of Origin: November Section: Surgery Last Reviewed Date: March 2014
 Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
235 60th Street, West New York, NJ T: (201) F: (201) Main Street, Hackensack, NJ T: (201)
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Barrett's Esophagus WHAT IS BARRETTT'S ESOPHAGUS? Barrett's esophagus
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Barrett's Esophagus WHAT IS BARRETTT'S ESOPHAGUS? Barrett's esophagus
Gastro esophageal reflux disease DR. AMMAR I. ABDUL-LATIF
 Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
Nexium 24HR Pharmacy Training
 Nexium 24HR Pharmacy Training Your pharmacist's advice is required. Always read the label. Use only as directed. If symptoms persist, consult your doctor/ healthcare professional. Pfizer Consumer Healthcare
Nexium 24HR Pharmacy Training Your pharmacist's advice is required. Always read the label. Use only as directed. If symptoms persist, consult your doctor/ healthcare professional. Pfizer Consumer Healthcare
Extraesophageal presentations of gastroesophageal reflux disease: the case for aggressive diagnosis and treatment
 JOEL E. RICHTER, MD Dr. Richter is chairman of the Department of Gastroenterology at the Cleveland Clinic Foundation, specializing in esophageal diseases with particular interest in GERD, achalasia, and
JOEL E. RICHTER, MD Dr. Richter is chairman of the Department of Gastroenterology at the Cleveland Clinic Foundation, specializing in esophageal diseases with particular interest in GERD, achalasia, and
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Intragastric acidity during treatment with esomeprazole 40 mg twice daily or pantoprazole 40 mg twice daily a randomized, two-way crossover study
 Aliment Pharmacol Ther 2005; 21: 963 967. doi: 10.1111/j.1365-2036.2005.02432.x Intragastric acidity during treatment with esomeprazole 40 mg twice daily or pantoprazole 40 mg twice daily a randomized,
Aliment Pharmacol Ther 2005; 21: 963 967. doi: 10.1111/j.1365-2036.2005.02432.x Intragastric acidity during treatment with esomeprazole 40 mg twice daily or pantoprazole 40 mg twice daily a randomized,
Perspectives in Primary Care Clinical Cases: Gastroesophageal Reflux Disease
 VOLUME 1 AUGUST 2004 Perspectives in Primary Care Clinical Cases: Gastroesophageal Reflux Disease Case 1: 74-Year-Old Male Burning in chest, worsening at night Former smoker Taking calcium channel blocker
VOLUME 1 AUGUST 2004 Perspectives in Primary Care Clinical Cases: Gastroesophageal Reflux Disease Case 1: 74-Year-Old Male Burning in chest, worsening at night Former smoker Taking calcium channel blocker
Patient information. Laryngopharyngeal Reflux ( LPR) Ear Nose and Throat Directorate PIF 1423/V4
 Patient information Laryngopharyngeal Reflux ( LPR) Ear Nose and Throat Directorate PIF 1423/V4 You have been diagnosed with laryngopharyngeal reflux (LPR), otherwise known as extra-oesophageal reflux
Patient information Laryngopharyngeal Reflux ( LPR) Ear Nose and Throat Directorate PIF 1423/V4 You have been diagnosed with laryngopharyngeal reflux (LPR), otherwise known as extra-oesophageal reflux
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
Hold the Wrap! There is so much more to be done!
 Hold the Wrap! There is so much more to be done! (Well, a few things that can be done.) (Well, not all that much, really ) (But Blair has never killed anyone with a PPI!) Nicholas Shaheen, MD, MPH Center
Hold the Wrap! There is so much more to be done! (Well, a few things that can be done.) (Well, not all that much, really ) (But Blair has never killed anyone with a PPI!) Nicholas Shaheen, MD, MPH Center
Barrett s Oesophagus Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
Number of studies. Endoscopic finding. Number of subjects. Pooled prevalence 95% CI
 Clinical Approach to the Patient t with Dyspepsia William D. Chey, MD, FACG Professor of Medicine University of Michigan Prevalence of Endoscopic Findings in Individuals with Dyspepsia Systematic Review
Clinical Approach to the Patient t with Dyspepsia William D. Chey, MD, FACG Professor of Medicine University of Michigan Prevalence of Endoscopic Findings in Individuals with Dyspepsia Systematic Review
Review article: management of mild and severe gastro-oesophageal reflux disease
 Aliment Pharmacol Ther 2003; 17 (Suppl. 2): 52 56. Review article: management of mild and severe gastro-oesophageal reflux disease G. N. J. TYTGAT Department of Gastroenterology and Hepatology, Academic
Aliment Pharmacol Ther 2003; 17 (Suppl. 2): 52 56. Review article: management of mild and severe gastro-oesophageal reflux disease G. N. J. TYTGAT Department of Gastroenterology and Hepatology, Academic
PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Heartburn is a common symptom among adults in
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:553 563 Early Heartburn Relief With Proton Pump Inhibitors: A Systematic Review and Meta-analysis of Clinical Trials KENNETH R. MCQUAID*, and LOREN LAINE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:553 563 Early Heartburn Relief With Proton Pump Inhibitors: A Systematic Review and Meta-analysis of Clinical Trials KENNETH R. MCQUAID*, and LOREN LAINE
Inflammation of the Esophagus (Esophagitis) Basics
 Inflammation of the Esophagus (Esophagitis) Basics OVERVIEW Inflammation of the esophagus typically involves the tubular area of the esophagus itself (known as the esophageal body ) and the muscular area
Inflammation of the Esophagus (Esophagitis) Basics OVERVIEW Inflammation of the esophagus typically involves the tubular area of the esophagus itself (known as the esophageal body ) and the muscular area
Gastro-oesophageal reflux disease
 Abdominal pain THEME Gastro-oesophageal reflux disease Current concepts in management BACKGROUND Gastro-oesophageal reflux disease (GORD) is defined as recurring symptoms or mucosal damage resulting from
Abdominal pain THEME Gastro-oesophageal reflux disease Current concepts in management BACKGROUND Gastro-oesophageal reflux disease (GORD) is defined as recurring symptoms or mucosal damage resulting from
GERD is a condition which develops when the reflux of stomach contents causes troublesome symptoms and/or complications
 GERD is a condition which develops when the reflux of stomach contents causes troublesome symptoms and/or complications Esophageal Syndromes Extra - esophageal Syndromes Symptomatic Syndromes Typical reflux
GERD is a condition which develops when the reflux of stomach contents causes troublesome symptoms and/or complications Esophageal Syndromes Extra - esophageal Syndromes Symptomatic Syndromes Typical reflux
GUIDELINES FOR CLINICIANS. Gastro-Oesophageal Reflux Disease in Adults. Reflux Disease. 4th Edition Digestive Health Foundation
 GUIDELINES FOR CLINICIANS Gastro-Oesophageal Reflux Disease in Adults Reflux Disease 4th Edition 2008 Digestive Health Foundation Digestive Health Foundation Table of contents Page 4 Gastro-oesophageal
GUIDELINES FOR CLINICIANS Gastro-Oesophageal Reflux Disease in Adults Reflux Disease 4th Edition 2008 Digestive Health Foundation Digestive Health Foundation Table of contents Page 4 Gastro-oesophageal
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
Heartburn. Understanding and Treating. Heal n Cure For appointments call
 A C P S P E C I A L R E P O R T Understanding and Treating Heartburn What is Heartburn? It begins as a burning pain in the middle of your chest, behind the breastbone, often after a big meal. The burning
A C P S P E C I A L R E P O R T Understanding and Treating Heartburn What is Heartburn? It begins as a burning pain in the middle of your chest, behind the breastbone, often after a big meal. The burning
OTC PPI Therapy in Frequent Heartburn
 Page 1 Gate Keeper to the Appropriate Use of OTC PPI Therapy for Conflicts of Interest Gatekeeper to the Appropriate Use of OTC PPI Therapy in Colin W. Howden, MD, FRCP (Glasg), FACP, FACG, FCP Professor
Page 1 Gate Keeper to the Appropriate Use of OTC PPI Therapy for Conflicts of Interest Gatekeeper to the Appropriate Use of OTC PPI Therapy in Colin W. Howden, MD, FRCP (Glasg), FACP, FACG, FCP Professor
GASTROESOPHAGEAL reflux
 ORIGINAL INVESTIGATION Lansoprazole Compared With Ranitidine for the Treatment of Nonerosive Gastroesophageal Reflux Disease Joel E. Richter, MD; Donald R. Campbell, MD; Peter J. Kahrilas, MD; Bidan Huang,
ORIGINAL INVESTIGATION Lansoprazole Compared With Ranitidine for the Treatment of Nonerosive Gastroesophageal Reflux Disease Joel E. Richter, MD; Donald R. Campbell, MD; Peter J. Kahrilas, MD; Bidan Huang,
The role of the modified barium swallow study & esophagram in patients with GERD/Globus sensation
 The role of the modified barium swallow study & esophagram in patients with GERD/Globus sensation James P. Dworkin, Ph.D. Jayme Dowdall, M.D. Adam Folbe, M.D. Tom Willis, M.S. Richard Culatta, Ph.D. Wayne
The role of the modified barium swallow study & esophagram in patients with GERD/Globus sensation James P. Dworkin, Ph.D. Jayme Dowdall, M.D. Adam Folbe, M.D. Tom Willis, M.S. Richard Culatta, Ph.D. Wayne
 Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2017 UpToDate Patient education: Acid reflux (gastroesophageal reflux disease) in adults (The Basics) Written by the doctors and editors at UpToDate
Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2017 UpToDate Patient education: Acid reflux (gastroesophageal reflux disease) in adults (The Basics) Written by the doctors and editors at UpToDate
Disclosures. Heartburn and Barrett s Esophagus. Heartburn and Barrett s Esophagus. GERD is common in the U.S. None
 Heartburn and Barrett s Esophagus None Disclosures Christian Mathy, MD University of California, San Francisco 2015 Heartburn and Barrett s Esophagus Heartburn and GERD GERD therapy Extraesophageal GERD
Heartburn and Barrett s Esophagus None Disclosures Christian Mathy, MD University of California, San Francisco 2015 Heartburn and Barrett s Esophagus Heartburn and GERD GERD therapy Extraesophageal GERD
National Digestive Diseases Information Clearinghouse
 Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
QUICK QUERIES. Topical Questions, Sound Answers
 QUICK QUERIES Topical Questions, Sound Answers Dyspepsia: An Evidence-Based Approach Alan B. R. Thomson, MD, PhD, FRCPC, FACP, FACG Presented at the University of Alberta s Medical Grand Rounds, University
QUICK QUERIES Topical Questions, Sound Answers Dyspepsia: An Evidence-Based Approach Alan B. R. Thomson, MD, PhD, FRCPC, FACP, FACG Presented at the University of Alberta s Medical Grand Rounds, University
Committee Approval Date: October 14, 2014 Next Review Date: October 2015
 Medication Policy Manual Topic: esomeprazole-containing medications: - Nexium - Vimovo - esomeprazole strontium Policy No: dru039 Date of Origin: May 2001 Committee Approval Date: October 14, 2014 Next
Medication Policy Manual Topic: esomeprazole-containing medications: - Nexium - Vimovo - esomeprazole strontium Policy No: dru039 Date of Origin: May 2001 Committee Approval Date: October 14, 2014 Next
Four-Day Bravo ph Capsule Monitoring With and Without Proton Pump Inhibitor Therapy
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1083 1088 Four-Day Bravo ph Capsule Monitoring With and Without Proton Pump Inhibitor Therapy IKUO HIRANO, QING ZHANG, JOHN E. PANDOLFINO, and PETER J. KAHRILAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1083 1088 Four-Day Bravo ph Capsule Monitoring With and Without Proton Pump Inhibitor Therapy IKUO HIRANO, QING ZHANG, JOHN E. PANDOLFINO, and PETER J. KAHRILAS
Alginates Extended Abstract
 Alginates Extended Abstract III) Clinical practice guidelines: DeVault KR, Castell DO; American College of Gastroenterology. Updated guidelines for the diagnosis and treatment of gastroesophageal reflux
Alginates Extended Abstract III) Clinical practice guidelines: DeVault KR, Castell DO; American College of Gastroenterology. Updated guidelines for the diagnosis and treatment of gastroesophageal reflux
Treatments for Barrett s Oesophagus
 Is it really just Heartburn? Treatments for Barrett s Oesophagus Introduction This leaflet describes the various ways in which Barrett s Oesophagus is treated. It has been produced in association with
Is it really just Heartburn? Treatments for Barrett s Oesophagus Introduction This leaflet describes the various ways in which Barrett s Oesophagus is treated. It has been produced in association with
GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY
 GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY DEFINITIONS GERD -Involuntary, effortless passage of gastric contents into the oesophagus +/-ejected from the mouth resulting in troublesome symptoms or complications
GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY DEFINITIONS GERD -Involuntary, effortless passage of gastric contents into the oesophagus +/-ejected from the mouth resulting in troublesome symptoms or complications
Laryngopharyngeal Reflux
 Laryngopharyngeal Reflux The Silent Reflux What is Laryngopharyngeal Reflux? Also called Reflux laryngitis, laryngopharyngeal reflux is a condition where the acid from the stomach reaches the voicebox
Laryngopharyngeal Reflux The Silent Reflux What is Laryngopharyngeal Reflux? Also called Reflux laryngitis, laryngopharyngeal reflux is a condition where the acid from the stomach reaches the voicebox
Nonerosive reflux disease as a presentation of gastro-oesophageal reflux disease
 Nonerosive reflux disease as a presentation of gastro-oesophageal reflux disease Abstract Simmonds WM, MMed (Internal Medicine) Gastroenterology Fellow, Department of Internal Medicine, Free State University
Nonerosive reflux disease as a presentation of gastro-oesophageal reflux disease Abstract Simmonds WM, MMed (Internal Medicine) Gastroenterology Fellow, Department of Internal Medicine, Free State University
There are many different symptoms of GER. Your child may only have a few of these symptoms. The most common symptoms include:
 This document is a short Overview of Pediatric Acid Reflux and GERD from www.reflux.org web site. Dozens of other documents about Pediatric GERD can be found in the Reading Room section of this web site.
This document is a short Overview of Pediatric Acid Reflux and GERD from www.reflux.org web site. Dozens of other documents about Pediatric GERD can be found in the Reading Room section of this web site.
Gastro-oesophageal reflux related cough and its response to laparoscopic fundoplication
 Thorax 1998;53:963 968 963 Departments of Medicine and Surgery, McMaster University, St Joseph s Hospital, Hamilton, Ontario, Canada L8N 4A6 C J Allen M Anvari Correspondence to: Dr C Allen. Received 10
Thorax 1998;53:963 968 963 Departments of Medicine and Surgery, McMaster University, St Joseph s Hospital, Hamilton, Ontario, Canada L8N 4A6 C J Allen M Anvari Correspondence to: Dr C Allen. Received 10
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW
 PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
PRESCRIBING SUPPORT TEAM AUDIT: PROTON PUMP INHIBITOR PRESCRIBING REVIEW DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY Dyspepsia refers to a broad range of symptoms related
Symptomatic outcome following laparoscopic anterior 180 partial fundoplication: Our initial experience
 International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
ESOPHAGEAL CANCER AND GERD. Prof Salman Guraya FRCS, Masters MedEd
 ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
11/19/2012. Comparison between PPIs G CELL. Risk ratio (95% CI) Patient subgroup. gastrin. S-form of omeprazole. Acid sensitive. coated.
 REGULATION OF GASTRIC ACID SECRETION Comparison between PPIs Omeprazole Lansoprazole Rabeprazole Pantoprazole Esomeprazole gastrin G CELL + Acid sensitive Yes T1/2 30-60 minutes Main elimination Enteric
REGULATION OF GASTRIC ACID SECRETION Comparison between PPIs Omeprazole Lansoprazole Rabeprazole Pantoprazole Esomeprazole gastrin G CELL + Acid sensitive Yes T1/2 30-60 minutes Main elimination Enteric
IJBCP International Journal of Basic & Clinical Pharmacology
 Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20163218 Research Article A comparative prospective
Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20163218 Research Article A comparative prospective
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA
 GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
Definition of GERD American College of Gastroenterology
 Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine
 Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine none 32 yo male presents with a burning sensation in chest following most large meals for 2-3 months. He denies dysphagia,
Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine none 32 yo male presents with a burning sensation in chest following most large meals for 2-3 months. He denies dysphagia,
Medical treatments for the maintenance therapy of reflux oesophagitis and endoscopic negative reflux disease (Review)
 Medical treatments for the maintenance therapy of reflux oesophagitis and endoscopic negative reflux disease (Review) Donnellan C, Sharma N, Preston C, Moayyedi P This is a reprint of a Cochrane review,
Medical treatments for the maintenance therapy of reflux oesophagitis and endoscopic negative reflux disease (Review) Donnellan C, Sharma N, Preston C, Moayyedi P This is a reprint of a Cochrane review,
