The current status of magnetic sphincter augmentation in the management of gastroesophageal reflux disease
|
|
|
- Whitney Mathews
- 5 years ago
- Views:
Transcription
1 Review Article Page 1 of 9 The current status of magnetic sphincter augmentation in the management of gastroesophageal reflux disease Mazen R. Al-Mansour, Kyle A. Perry, Jeffrey W. Hazey Division of General and Gastrointestinal Surgery, Department of Surgery, Ohio State University Wexner Medical Center, Columbus, OH, USA Contributions: (I) Conception and design: None; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: None; (V) Data analysis and interpretation: None; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Jeffrey W. Hazey, MD, FACS. Division of General and Gastrointestinal Surgery, Department of Surgery, Ohio State University Wexner Medical Center, N729 Doan Hall, 410 West 10th Avenue, Columbus, OH 43210, USA. Jeffrey.hazey@osumc.edu. Abstract: Magnetic sphincter augmentation (MSA) using the LINX Reflux Management System is a surgical option for the management of gastroesophageal reflux disease (GERD). This technique involves the laparoscopic placement of a band of magnetic beads around the distal esophagus. The beads augment the function of lower esophageal sphincter (LES) by preventing the proximal reflux of gastric contents at rest, while expanding during swallowing to allow the unimpeded passage of food boluses. Despite the lack of randomized controlled trials evaluating the efficacy of MSA, recent long-term retrospective studies support the procedure s safety and efficacy in controlling reflux symptoms and improving quality of life. When compared to laparoscopic fundoplication for the management of reflux, MSA has shown comparable symptoms control and acceptable side effect/complication profile. Complications including dysphagia and erosion have been described. The device can be removed laparoscopically if intolerance or complications develop. Careful patient selection is paramount in order to select the appropriate patients for this technique. Keywords: LINX, magnetic sphincter augmentation (MSA); gastroesophageal reflux disease (GERD); GORD Received: 17 May 2017; Accepted: 13 June 2017; Published: 20 September doi: /ales View this article at: Introduction Gastroesophageal reflux disease (GERD) is among the most common gastrointestinal diseases with a prevalence of 10 20% (1). GERD significantly impairs patient quality of life, often due to symptoms of heartburn and regurgitation. Reflux disease can also cause complications including erosive esophagitis, peptic stricture and Barrett s esophagus, a precursor of esophageal adenocarcinoma. The first line of treatment of GERD consists of lifestyle modifications and gastric acid suppression. However, these measures do not address the underlying physiologic cause of reflux in many patients, namely ineffective lower esophageal sphincter (LES) function, and breakthrough acid reflux symptoms occur in 17 44% of patients while taking proton pump inhibitors (PPI) (2). Following its initial description in 1956 and its subsequent refinement, Nissen fundoplication has been the gold-standard surgical treatment for GERD (3). Surgical fundoplication creates a supraphysiologic antireflux valve that is highly effective in controlling acid reflux and eliminating GERD symptoms, but is also associated with significant postoperative side-effects including dysphagia, bloating, and the inability to vomit or belch. Also, the outcomes of laparoscopic fundoplication may vary significantly due to a center s case volume and surgeon s expertise. Currently, it is estimated that only 1% of patients with GERD receive a fundoplication procedure (4). In response to the need for highly efficacious minimally invasive treatment options, several laparoscopic and endoscopic procedures have been developed including
2 Page 2 of 9 Annals of Laparoscopic and Endoscopic Surgery, 2017 Titanium beads laparoscopic magnetic sphincter augmentation (MSA) using the LINX Reflux Management System (Torax Medical, St Paul, MN, USA). The purpose of this article is to review the technique, outcomes and complications of MSA. Independent titanium wires Multi-directional locking clasp Magnetic cores Figure 1 Structure of the LINX Reflux Management System. A B Figure 2 Closed (A) and open (B) configurations of the LINX Reflux Management System. The device The LINX Reflux Management System is a band of magnetic beads that forms a ring around the lower esophagus (Figure 1). Each bead has a magnetic core that is covered by a titanium casing. The beads are interconnected by titanium wires that allow each bead to move independently. This structure maintains the ring in the contracted form at rest and allows it to expand during the passage of a food bolus (Figure 2). At rest, the short distance between the magnetic beads results in a higher attraction force. This force augments the barrier function of the LES and prevents the gastric juice from refluxing proximally. When a food bolus passes through the LES the ring expands and the attraction force decreases allowing unimpeded passage of the bolus (Figure 3). The same happens when intragastric pressure increases during belching or vomiting. The device is available in multiple sizes which are determined by the number of beads in the ring (13 to 17 beads). The appropriate device is selected using a sizing instrument that is passed around the esophagus and correlates the esophageal size with the appropriately sized device. The placement of a prosthetic ring around the GE A B Esophagus Esophagus Food Stomach Stomach LINX System LINX System Figure 3 Depiction of the LINX Reflux Management System during rest (A) and passage of fluid bolus (B).
3 Annals of Laparoscopic and Endoscopic Surgery, 2017 Page 3 of 9 A B C Figure 4 Laparoscopic LINX Reflux Management System placement. (A) A tunnel is created between the posterior vagus nerve (asterisk) and the esophagus; (B) the sizing instrument is used to determine the size of the device used; (C) the final position of the device. Figure 5 Laparoscopic placement of the LINX Reflux Management System (7). junction is not a novel idea. The Angelchik device, introduced in 1979, was a silicone ring that was surgically placed around the GE junction in patients with GERD and secured in place with Dacron tape. This device fell out of favor after poor long-term outcomes were shown including dysphagia rates of up to 45% and high reoperation, removal and complication rates (5). In contrast to the Angelchik device, MSA using the LINX Reflux Management System allows the dynamic changes of the diameter of the magnetic ring with the closed configuration preventing reflux and the open configuration allowing passage of food boluses. Patients who underwent esophageal manometry before and after MSA were noted to have improvement (increase) in LES resting pressure, LES residual pressure and distal esophageal contraction amplitude (6). Surgical technique Video 1. Laparoscopic placement of the LINX Reflux Management System Mazen R. Al-Mansour, Kyle A. Perry, Jeffrey W. Hazey* Division of General and Gastrointestinal Surgery, Department of Surgery, Ohio State University Wexner Medical Center, Columbus, OH, USA Available online: MSA is performed using a 4-port laparoscopic technique similar to that utilized for laparoscopic Nissen fundoplication (LNF). After obtaining laparoscopic access, the pars flaccida of the gastrohepatic ligament is opened to expose the right crus of the diaphragm. Any sliding hiatal hernia is reduced and a circumferential esophageal dissection is completed at the level of the hiatus. If necessary, a posterior cruroplasty is performed using interrupted non-absorbable sutures. When this is complete, the posterior vagus nerve is dissected free from the posterior wall of the distal esophagus. The appropriate position of the MSA device is two centimeters proximal to the gastroesophageal (GE) junction as determined laparoscopically by the gastric fat pad. A Penrose drain is placed around the esophagus excluding the posterior vagus nerve. The sizing instrument is then used to determine the appropriate size of the device, and the device is introduced and passed around the esophagus. The magnetized ends are mated and the device is locked in place around the lower esophagus (Figures 4,5). Patient selection The preoperative evaluation for MSA device placement is the same as that for laparoscopic fundoplication. Objective documentation of GERD is needed in the form of ambulatory ph testing. Barium esophagogram and upper endoscopy are helpful in evaluating the anatomy including the identification of large hiatal hernias, severe esophagitis or Barrett s esophagus. Esophageal manometry is essential to ensure that the distal esophageal peristalsis is sufficient to overcome the mmhg device opening pressure. There are no specific manometric parameters that determine the appropriate use of MSA. MSA has not been evaluated when distal esophageal peristaltic amplitude is less than 35 mmhg on wet swallows or when less than 70% of swallows demonstrate peristaltic contractions. Furthermore, MSA should be avoided in the presence a known motility disorder such as achalasia, nutcracker esophagus, diffuse esophageal
4 Page 4 of 9 Annals of Laparoscopic and Endoscopic Surgery, 2017 spasm or hypertensive LES. The ideal patient for MSA is a patient with: (I) Partially PIP responsive typical GERD symptoms; (II) Positive ambulatory ph testing; (III) Absent or small (<3 cm) hiatal hernia. Exclusion criteria for MSA include: (I) Large hiatal hernia (>3 cm); (II) Severe esophagitis; (III) Long-segment Barrett s esophagus; (IV) Significant abnormality in esophageal manometry; (V) Allergy to stainless steel, titanium, nickel or iron. The manufacturer reports the device to be MRI scanning compatible up to 0.7 or 1.5 Tesla depending on the version of the device used (8). Outcomes The initial feasibility studies of MSA showed its safety and feasibility in porcine models (9). These were shortly followed by human feasibility studies from Italy showing that the device can be placed laparoscopically with minimal dissection and a short learning curve compared to LNF (10). Receiving the approval from the US Food and Drug Administration (FDA) in 2012 has facilitated the use of the device in the USA (11). The feasibility trial evaluated 44 patients who underwent MSA at four centers in Italy, USA and Netherlands between 2007 and This single arm trial, where patients serve as their own controls, compared the outcomes following MSA implantation to patient s baseline characteristics. The outcomes were reported at 1 to 2 years, 3 to 4 years and more than 5 years postoperatively. GERD healthrelated quality of life (HRQL) scores improved from 25.7 at baseline to 3.8 at 1 year, 2.4 at 2 years, 3.3 at 4 years and 2.9 at more than 5 years. All patients were taking PPIs at baseline. The rate of PPI cessation was 90% at 1 year, 85% at 2 years, 80% at 3 to 4 years and 88% at more than 5 years. The percentage of time the ph was less than 4 was 11.9% at baseline and this improved to 3.1% at 1 year, 2.4% at 2 years, 3.8% at 3 years and 4.6% at more than 5 years. More than 86% of patients reported satisfaction with their current condition while off-ppis at 1, 2, 4 and more than 5 years compared to 0% at baseline (12-14). These sustained outcomes were replicated in the pivotal trial. This multi-center prospective trial evaluated 100 patients who underwent laparoscopic MSA at 14 centers (13 in USA and one in the Netherlands). The median time to implant the device was 36 minutes (range, minutes). All patients were discharged within 1 day after surgery. Postoperative outcomes were evaluated at 3 and 5 years. GERD HRQL scores improved from 11 on-ppi and 27 off-ppi to 2 at 3 years and 4 at 5 years postoperatively. More than 50% improvement in GERD HRQL scores was achieved in 92% of patients at 3 years. More than 50% improvement in PPI use was achieved in 93% of patients at 3 years and PPI use decreased from 100% preoperatively to 15% at 5 years. Normalization of ambulatory ph testing or more than 50% improvement in ph testing was achieved in 64% of patients at 3 years. No device erosions, migrations of malfunctions were reported at 5 years. Table 1 summarizes the studies evaluating MSA outcomes. Comparison to other surgical GERD treatments To date, there have been no randomized controlled trials comparing laparoscopic MSA to laparoscopic antireflux surgery. However, several retrospective studies have compared the outcomes of laparoscopic MSA to laparoscopic fundoplication. Warren et al. performed a retrospective review of 201 patient who underwent MSA and 214 patients who underwent LNF for a total of 415 patients. The procedures were performed at three high-volume esophageal centers in the USA. Propensity score matching was performed and 114 patients were analyzed in each arm. The mean follow up was 11 months for MSA and 16 months for LNF (P<0.001). There was no statistically significant difference in preoperative GERD HRQL (21 vs. 19; P=0.56) or postoperative GERD HRQL (6 vs. 5; P=0.54). MSA patients had greater ability to belch (97% vs. 66%; P<0.001) and vomit (88% vs. 40%; P<0.001). The MSA group reported gas-bloat symptoms less frequently than LNF group (41% vs. 59%; P=0.008). Mild dysphagia was more common with MSA (44% vs. 32%; P=0.04). Moderate and severe dysphagia rates were similar in both groups. The MSA group was more likely to require postoperative PPI (24% vs. 12%; P=0.02). Patient satisfaction was similar in both groups (88% vs. 89%; P=0.61) (21). Table 2 summarizes the studies comparing laparoscopic MSA and fundoplication procedures (18,21-26). Skubleny et al. conducted a systematic review of studies comparing MSA to LNF and included three studies in the meta-analysis. These included a total of 688 patients of which 415 underwent MSA and 273 underwent LNF. Operative time was shorter for MSA compared to LNF (63.7 vs minutes). MSA was found to be superior to LNF in maintaining the patient s ability to belch (95.2%
5 Annals of Laparoscopic and Endoscopic Surgery, 2017 Page 5 of 9 Table 1 Studies evaluating short and long-term outcomes of magnetic sphincter augmentation Source N Follow-up Description Bonavina, 2010 (12)* 44 1 and 2 years Multi-institutional prospective study. Participating institutions from Italy, USA and the Netherlands Lipham, 2012 (13)* years Multi-institutional prospective study. Participating institutions from Italy, USA and the Netherlands Bonavina, 2013 (15) 100 Median of 3 years Single center prospective study of consecutive cases from Italy Ganz, 2013 (16)** years Multi-institutional prospective study. 14 participating institutions from USA and the Netherlands Reynolds, 2014 (17) 67 Median of 5 months Prospective study from two institutions Riegler, 2015 (18) year Multicenter prospective study (22 institutions) from four countries (Austria, Germany, Italy and the UK). Also included 47 patients who underwent laparoscopic Nissen fundoplication Saino, 2015 (14)* patients followed 5 years Multi-institutional prospective study. Participating institutions from Italy, USA and the Netherlands Czosnyka, 2016 (19) 102 Mean 7.6 months Two community-based health systems in USA Ganz, 2016 (20)** patients followed 5 years Multi-institutional prospective study. 14 participating institutions from USA and the Netherlands *, feasibility trial reporting short-term, mid-term & 4-year outcomes; **, piroted trial reporting 3- & 5-year outcomes. Table 2 Studies comparing magnetic sphincter augmentation and laparoscopic fundoplication procedures Source (year) Total number MSA (n) LNF (n) Follow-up Description Louie, 2014 (22) months Retrospective case-controlled study of consecutive patients, included patients with hiatal hernia <3 cm Reynolds, 2015 (23) year Retrospective, patients matched using propensity scoring Sheu, 2015 (24) months Retrospective, single-center, case-controlled study; matched patients for age, gender and hiatal hernia Riegler, 2015 (18) year LNF patients were older, more likely to have Barrett s esophagus and had larger hiatal hernias Warren, 2016 (21) patients (MSA 169, LNF 185) were followed for 1 year Multi-institutional retrospective study (three highvolume centers in USA). Included a propensity matched comparison Reynolds, 2016 (25) year Retrospective Asti, 2016 (26) >1 year Propensity matched cohort MSA, magnetic sphincter augmentation; LNF, laparoscopic Nissen fundoplication.
6 Page 6 of 9 Annals of Laparoscopic and Endoscopic Surgery, 2017 vs. 65.9%; P<0.01) and vomit (93.5% vs. 49.5%; P<0.01). Bloating was more common with LNF compared to MSA but this did not reach statistical significance (53.4% vs. 26.7%; P=0.06). Postoperative dysphagia and PPI elimination rates were similar. Seeing as reflux is a chronic disease, and long-term outcomes are of paramount importance, studies are needed to compare the long-term efficacy, complications, and need for repeat intervention (endoscopic dilations and reoperations) between MSA and laparoscopic fundoplication procedures. No studies have compared MSA to PPI therapy. The CALIBER study is an ongoing randomized controlled trial designed to compare MSA to double-dose PPIs for the management of GERD symptoms. Special situations As experience with MSA procedure accumulates, the indications for this procedure may expand to include patients with larger hiatal hernias (>3 cm) and patients with GERD following bariatric procedures. These situations have been evaluated in small cohort studies. Hiatal hernia Video 2. Laparoscopic removal of the LINX Reflux Management System Mazen R. Al-Mansour, Kyle A. Perry, Jeffrey W. Hazey* Division of General and Gastrointestinal Surgery, Department of Surgery, Ohio State University Wexner Medical Center, Columbus, OH, USA Figure 6 Laparoscopic removal of the LINX Reflux Management System (36). Available online: The presence of a large hiatal hernia was initially thought of as an exclusion criterion for MSA device placement. However, some early data are showing encouraging results of MSA in this patient population. Rona et al. retrospectively reviewed 192 patients who underwent MSA placement in their institution. Fifty-two patients (27%) had a hiatal hernia 3 cm (range, 3 7 cm). In these patients their mean GERD-HRQL score decreased from 20.5 preoperatively to 3.6 postoperatively (P<0.01). When compared to patients with smaller hernias, patients with large hiatal hernias had lower postoperative PPI requirement (9.6% vs. 26.6%; P=0.01) and lower mean postoperative GERD HRQL scores (3.6 vs. 5.6; P=0.03). The rates of severe dysphagia and symptom resolution were similar to patients with smaller hiatal hernias (27). GERD following bariatric procedures The management of GERD following sleeve gastrectomy is complicated. The altered gastric anatomy makes traditional treatments such as fundoplication impossible. While this issue is controversial, many believe that sleeve gastrectomy can worsen pre-existing reflux disease or create de novo GERD (28). Off-label use of MSA to manage GERD in patients with a prior sleeve gastrectomy has been described in a case series (29). Other case reports have also describes the use of MSA to treat GERD following Roux-en-Y gastric bypass (30-32). More studies are needed to further explore the role of MSA procedure in this growing subset of patients. The RELIEF study is an ongoing prospective, multicenter study evaluating the safety and efficacy of MSA in sleeve gastrectomy patients with GERD. Complications The most common complication of MSA is dysphagia. Some degree of postoperative dysphagia can be observed in 34% to 79% of patients. Dysphagia is most noticeable shortly after MSA device placement but it tends to resolve over time with conservative management. Significant improvement is usually noticed 8 weeks postoperatively. The reported rates of dysphagia beyond 3 years postoperatively are 4% to 6% compared to 5% rate of dysphagia at baseline (prior to MSA device placement) (10,16,17,20,21,23,33,34). In a small proportion of patients (6.7%) recurrent reflux symptoms or severe dysphagia can lead to MSA device removal (35). In some patients the device was removed due to the need to obtain an MRI for an unrelated problem. This issue was more common with the first generation devices which were only compatible up to 0.7 Tesla. The device removal can be achieved laparoscopically in the majority of patients (Figure 6). This requires locating the device and incising the fibrous capsule that envelops each of the beads. Once a few beads are freed the connecting wire is divided to facilitate removal. We recommend obtaining a preoperative x-ray as well as consulting the previous
7 Annals of Laparoscopic and Endoscopic Surgery, 2017 Page 7 of 9 operative implant record to allow a count of the beads in order to ensure complete device removal. Laparoscopic fundoplication performed as a concomitant procedure with device removal has been described. Asti et al described the removal of 11 devices out of 164 implants with a 48 month median follow up. A partial or total fundoplication procedure was performed concurrently in all patients. Recurrent heartburn or regurgitation was the most common indication for removal (46%) followed by dysphagia (37%). There were no morbidities associated with the procedure. Follow duration ranged from 12 to 58 months at which time all patients reported satisfaction with their condition and GERD HRQL scores were within normal limits (37). Device erosion into the esophagus has been described. The exact incidence of this complication is unknown. Eleven cases of device erosion was reported to the FDA Manufacturer s and User s Device Experiences (MAUDE) database in 2016 (38). This seemingly uncommon complication mandates removal of the device. The technique for endoscopic removal has been described and follows similar concepts to the endoscopic removal of eroded gastric bands (39). The chronic erosion process allows scarring on the extraluminal portion of the device that prevents a full thickness defect of the esophageal wall when the device is retrieved. Other potential complications include migration and device malfunction (40). Conclusions MSA is a novel surgical option for the management of GERD. Short- and long-term data demonstrate excellent control of reflux symptoms, objective GERD control, and improvement in patient quality of life with an acceptable side-effect profile. MSA compares favorably to LNF in retrospective trials, but randomized controlled trials comparing MSA to best medical management and LNF are needed to confirm the findings of the currently available retrospective studies. Acknowledgements KA Perry has received Research funding from Torax medical. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Dent J, El-Serag HB, Wallander MA, et al. Epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut 2005;54: Becher A, El-Serag H. Systematic review: the association between symptomatic response to proton pump inhibitors and health-related quality of life in patients with gastrooesophageal reflux disease. Aliment Pharmacol Ther 2011;34: Nissen R. A simple operation for control of reflux esophagitis. Schweiz Med Wochenschr 1956;86: Bonavina L, Saino G, Lipham JC, et al. LINX( ) Reflux Management System in chronic gastroesophageal reflux: a novel effective technology for restoring the natural barrier to reflux. Therap Adv Gastroenterol 2013;6: Thibault C, Marceau P, Biron S, et al. The Angelchik antireflux prosthesis: long-term clinical and technical follow-up. Can J Surg 1994;37: Warren HF, Louie BE, Farivar AS, et al. Manometric Changes to the Lower Esophageal Sphincter After Magnetic Sphincter Augmentation in Patients With Chronic Gastroesophageal Reflux Disease. Ann Surg 2017;266: Al-Mansour MR, Perry KA, Hazey JW. Laparoscopic placement of the LINX Reflux Management System. Asvide 2017;4:406. Available online: com/articles/ Torax. Frequently Asked Questions. cited 2017 Mar 28. Available online: FAQs.php 9. Ganz RA, Gostout CJ, Grudem J, et al. Use of a magnetic sphincter for the treatment of GERD: a feasibility study. Gastrointest Endosc 2008;67: Bonavina L, Saino GI, Bona D, et al. Magnetic augmentation of the lower esophageal sphincter: results of a feasibility clinical trial. J Gastrointest Surg 2008;12: FDA Approves LINX System for the Treatment of Reflux Disease. cited 2017 Mar 14. Available online: LINXFDAApproval.pdf 12. Bonavina L, DeMeester T, Fockens P, et al. Laparoscopic sphincter augmentation device eliminates reflux symptoms and normalizes esophageal acid exposure: one- and 2-year results of a feasibility trial. Ann Surg 2010;252: Lipham JC, DeMeester TR, Ganz RA, et al. The LINX reflux management system: confirmed safety and efficacy now at 4 years. Surg Endosc 2012;26:
8 Page 8 of 9 Annals of Laparoscopic and Endoscopic Surgery, Saino G, Bonavina L, Lipham JC, et al. Magnetic Sphincter Augmentation for Gastroesophageal Reflux at 5 Years: Final Results of a Pilot Study Show Long-Term Acid Reduction and Symptom Improvement. J Laparoendosc Adv Surg Tech A 2015;25: Bonavina L, Saino G, Bona D, et al. One hundred consecutive patients treated with magnetic sphincter augmentation for gastroesophageal reflux disease: 6 years of clinical experience from a single center. J Am Coll Surg 2013;217: Ganz RA, Peters JH, Horgan S, et al. Esophageal sphincter device for gastroesophageal reflux disease. N Engl J Med 2013;368: Reynolds JL, Zehetner J, Bildzukewicz N, et al. Magnetic sphincter augmentation with the LINX device for gastroesophageal reflux disease after U.S. Food and Drug Administration approval. Am Surg 2014;80: Riegler M, Schoppman SF, Bonavina L, et al. Magnetic sphincter augmentation and fundoplication for GERD in clinical practice: one-year results of a multicenter, prospective observational study. Surg Endosc 2015;29: Czosnyka NM, Buckley FP, Doggett SL, et al. Outcomes of magnetic sphincter augmentation - A community hospital perspective. Am J Surg 2017;213: Ganz RA, Edmundowicz SA, Taiganides PA, et al. Long-term Outcomes of Patients Receiving a Magnetic Sphincter Augmentation Device for Gastroesophageal Reflux. Clin Gastroenterol Hepatol 2016;14: Warren HF, Reynolds JL, Lipham JC, et al. Multiinstitutional outcomes using magnetic sphincter augmentation versus Nissen fundoplication for chronic gastroesophageal reflux disease. Surg Endosc 2016;30: Louie BE, Farivar AS, Shultz D, et al. Short-term outcomes using magnetic sphincter augmentation versus Nissen fundoplication for medically resistant gastroesophageal reflux disease. Ann Thorac Surg 2014;98: ;discussion Reynolds JL, Zehetner J, Wu P, et al. Laparoscopic Magnetic Sphincter Augmentation vs Laparoscopic Nissen Fundoplication: A Matched-Pair Analysis of 100 Patients. J Am Coll Surg 2015;221: Sheu EG, Nau P, Nath B, et al. A comparative trial of laparoscopic magnetic sphincter augmentation and Nissen fundoplication. Surg Endosc 2015;29: Reynolds JL, Zehetner J, Nieh A, et al. Charges, outcomes, and complications: a comparison of magnetic sphincter augmentation versus laparoscopic Nissen fundoplication for the treatment of GERD. Surg Endosc 2016;30: Asti E, Bonitta G, Lovece A, et al. Longitudinal comparison of quality of life in patients undergoing laparoscopic Toupet fundoplication versus magnetic sphincter augmentation: Observational cohort study with propensity score analysis. Medicine (Baltimore) 2016;95:e Rona KA, Reynolds J, Schwameis K, et al. Efficacy of magnetic sphincter augmentation in patients with large hiatal hernias. Surg Endosc 2017;31: Mahawar KK, Jennings N, Balupuri S, et al. Sleeve gastrectomy and gastro-oesophageal reflux disease: a complex relationship. Obes Surg 2013;23: Desart K, Rossidis G, Michel M, et al. Gastroesophageal Reflux Management with the LINX System for Gastroesophageal Reflux Disease Following Laparoscopic Sleeve Gastrectomy. J Gastrointest Surg 2015;19: Hawasli A, Phillips A, Tarboush M. Laparoscopic management of reflux after Roux-en-Y gastric bypass using the LINX system and repair of hiatal hernia: a case report. Surg Obes Relat Dis 2016;12:e Hawasli A, Tarakji M, Tarboush M. Laparoscopic management of severe reflux after sleeve gastrectomy using the LINX( ) system: Technique and one year follow up case report. Int J Surg Case Rep 2017;30: Muñoz-Largacha JA, Hess DT, Litle VR, et al. Lower Esophageal Magnetic Sphincter Augmentation for Persistent Reflux After Roux-en-Y Gastric Bypass. Obes Surg 2016;26: Schwameis K, Schwameis M, Zörner B, et al. Modern GERD treatment: feasibility of minimally invasive esophageal sphincter augmentation. Anticancer Res 2014;34: Skubleny D, Switzer NJ, Dang J, et al. LINX magnetic esophageal sphincter augmentation versus Nissen fundoplication for gastroesophageal reflux disease: a systematic review and meta-analysis. Surg Endosc 2017;31: Harnsberger CR, Broderick RC, Fuchs HF, et al. Magnetic lower esophageal sphincter augmentation device removal. Surg Endosc 2015;29: Al-Mansour MR, Perry KA, Hazey JW. Laparoscopic removal of the LINX Reflux Management System. Asvide 2017;4:407. Available online: com/articles/ Asti E, Siboni S, Lazzari V, et al. Removal of the Magnetic Sphincter Augmentation Device: Surgical Technique
9 Annals of Laparoscopic and Endoscopic Surgery, 2017 Page 9 of 9 and Results of a Single-center Cohort Study. Ann Surg 2017;265: Bielefeldt K. Adverse Events After Implantation of a Magnetic Sphincter Augmentation Device for Gastroesophageal Reflux. Clin Gastroenterol Hepatol 2016;14: Bauer M, Meining A, Kranzfelder M, et al. Endoluminal perforation of a magnetic antireflux device. Surg Endosc 2015;29: Lipham JC, Taiganides PA, Louie BE, et al. Safety analysis of first 1000 patients treated with magnetic sphincter augmentation for gastroesophageal reflux disease. Dis. Esophagus 2015;28: doi: /ales Cite this article as: Al-Mansour MR, Perry KA, Hazey JW. The current status of magnetic sphincter augmentation in the management of gastroesophageal reflux disease. Ann Laparosc Endosc Surg 2017;2:146.
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER AUGMENTATION FOR THE TREATMENT OF GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD)
 Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2018 Origination: 02/2014 Next Review: 02/2019 Policy Blue Cross and Blue
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2018 Origination: 02/2014 Next Review: 02/2019 Policy Blue Cross and Blue
Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD)
 Medical Policy Manual Surgery, Policy No. 190 Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD) Next Review: January 2019 Last Review: January 2018 Effective: March 1, 2018 IMPORTANT
Medical Policy Manual Surgery, Policy No. 190 Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD) Next Review: January 2019 Last Review: January 2018 Effective: March 1, 2018 IMPORTANT
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD)
 Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2019 Origination: 02/2014 Next Review: 02/2020 Policy Blue Cross and Blue
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2019 Origination: 02/2014 Next Review: 02/2020 Policy Blue Cross and Blue
Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD)
 7.01.137 Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD) Section 7.0 Surgery Effective Date January 30, 2015 Subsection Original Policy Date June 28, 2013 Next Review Date October
7.01.137 Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD) Section 7.0 Surgery Effective Date January 30, 2015 Subsection Original Policy Date June 28, 2013 Next Review Date October
Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel?
 Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel? Brian R. Smith, MD, FACS, FASMBS Associate Professor of Surgery & General Surgery Residency Program Director UC Irvine Medical
Endoscopic vs Surgical Therapies for GERD: Is it Time to Put down the Scalpel? Brian R. Smith, MD, FACS, FASMBS Associate Professor of Surgery & General Surgery Residency Program Director UC Irvine Medical
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
LINX. A new, FDA approved treatment for GERD
 LINX A new, FDA approved treatment for GERD What Causes Reflux? Gastroesophageal reflux disease (GERD), also called reflux, is a chronic, often progressive disease caused by a weak lower esophageal sphincter
LINX A new, FDA approved treatment for GERD What Causes Reflux? Gastroesophageal reflux disease (GERD), also called reflux, is a chronic, often progressive disease caused by a weak lower esophageal sphincter
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic insertion of a magnetic titanium ring for gastrooesophageal reflux
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic insertion of a magnetic titanium ring for gastrooesophageal reflux
A PROVEN TREATMENT FOR CHRONIC REFLUX
 A PROVEN TREATMENT FOR CHRONIC REFLUX This booklet is for patients who have discussed the LINX Reflux Management System during a consultation with their surgeon. It will answer some of the questions that
A PROVEN TREATMENT FOR CHRONIC REFLUX This booklet is for patients who have discussed the LINX Reflux Management System during a consultation with their surgeon. It will answer some of the questions that
Instructions for Use Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician.
 Instructions for Use Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. LINX Reflux Management System Instructions for Use Page 1 of 16 1. SYSTEM DESCRIPTION The
Instructions for Use Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. LINX Reflux Management System Instructions for Use Page 1 of 16 1. SYSTEM DESCRIPTION The
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO
 L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
LINX Reflux Management System. Patient Information. Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician.
 LINX Reflux Management System Patient Information Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. 2 Table of Contents What is the LINX System? 3 Why doctors
LINX Reflux Management System Patient Information Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. 2 Table of Contents What is the LINX System? 3 Why doctors
Options for Gastroesophageal Reflux: Endoluminal. W. Scott Melvin, M.D. Montefiore Medical System and the Albert Einstein School of Medicine
 Options for Gastroesophageal Reflux: Endoluminal W. Scott Melvin, M.D. Montefiore Medical System and the Albert Einstein School of Medicine The patient with GERD The Therapy Gap Effectively Treated with
Options for Gastroesophageal Reflux: Endoluminal W. Scott Melvin, M.D. Montefiore Medical System and the Albert Einstein School of Medicine The patient with GERD The Therapy Gap Effectively Treated with
Innovations in Surgical Therapy for GERD: A tale of two therapies
 Innovations in Surgical Therapy for GERD: A tale of two therapies Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery Program
Innovations in Surgical Therapy for GERD: A tale of two therapies Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery Program
Gastroesophageal Reflux Disease, Paraesophageal Hernias &
 530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
LINX Reflux Management System
 LINX Reflux Management System Patient Information Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. LINX Reflux Management System 2 Table of Contents What is the
LINX Reflux Management System Patient Information Caution: Federal (USA) Law restricts this device to sale by or on the order of a physician. LINX Reflux Management System 2 Table of Contents What is the
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Novel Approaches for Managing Reflux. Marcus Reddy Consultant General and Upper GI surgeon
 Novel Approaches for Managing Reflux Marcus Reddy Consultant General and Upper GI surgeon Medigus SRS Endoscope (TIFS) EsophyX STRETTA LINX Persistent GORD RF delivery for GORD RF fits in the
Novel Approaches for Managing Reflux Marcus Reddy Consultant General and Upper GI surgeon Medigus SRS Endoscope (TIFS) EsophyX STRETTA LINX Persistent GORD RF delivery for GORD RF fits in the
LINX Reflux Management System: magnetic sphincter augmentation in the treatment of gastroesophageal reflux disease
 LINX Reflux Management System: magnetic sphincter augmentation in the treatment of gastroesophageal reflux disease Expert Rev. Gastroenterol. Hepatol. 6(6) 2012) Luigi Bonavina* 1, Tom R DeMeester 2 and
LINX Reflux Management System: magnetic sphincter augmentation in the treatment of gastroesophageal reflux disease Expert Rev. Gastroenterol. Hepatol. 6(6) 2012) Luigi Bonavina* 1, Tom R DeMeester 2 and
Medicine. Emanuele Asti, MD, Gianluca Bonitta, MSc, Andrea Lovece, MD, Veronica Lazzari, MD, Luigi Bonavina, MD, PhD, FACS. Observational Study
 Observational Study Medicine Longitudinal comparison of quality of life in patients undergoing laparoscopic Toupet fundoplication versus magnetic sphincter augmentation Observational cohort study with
Observational Study Medicine Longitudinal comparison of quality of life in patients undergoing laparoscopic Toupet fundoplication versus magnetic sphincter augmentation Observational cohort study with
Symptomatic outcome following laparoscopic anterior 180 partial fundoplication: Our initial experience
 International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
LINX Reflux Management System. Gastroenterology and Urology Medical Devices Panel Meeting, January 11, 2012 Gaithersburg, MD
 LINX Reflux Management System Gastroenterology and Urology Medical Devices Panel Meeting, January 11, 2012 Gaithersburg, MD AGENDA Introduction Pathophysiology of GERD Device Overview and Pre-Clinical
LINX Reflux Management System Gastroenterology and Urology Medical Devices Panel Meeting, January 11, 2012 Gaithersburg, MD AGENDA Introduction Pathophysiology of GERD Device Overview and Pre-Clinical
Electrical neuromodulation of the lower esophageal sphincter for the treatment of gastroesophageal reflux disease
 Review Article Page 1 of 7 Electrical neuromodulation of the lower esophageal sphincter for the treatment of gastroesophageal reflux disease Alejandro Nieponice 1, Mauricio Ramirez 1, Adolfo Badaloni 1,
Review Article Page 1 of 7 Electrical neuromodulation of the lower esophageal sphincter for the treatment of gastroesophageal reflux disease Alejandro Nieponice 1, Mauricio Ramirez 1, Adolfo Badaloni 1,
Oesophageal Disorders
 Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
For over half a century, the treatment options for patients with
 ORIGINAL ARTICLE Objective Evidence of Reflux Control After Magnetic Sphincter Augmentation One Year Results From a Post Approval Study Brian E. Louie, MD, C. Daniel Smith, MD,y Christopher C. Smith, MD,z
ORIGINAL ARTICLE Objective Evidence of Reflux Control After Magnetic Sphincter Augmentation One Year Results From a Post Approval Study Brian E. Louie, MD, C. Daniel Smith, MD,y Christopher C. Smith, MD,z
Prevalence of Barrett s Esophagus in Bariatric Patients Undergoing Sleeve Gastrectomy
 OBES SURG (2016) 26:710 714 DOI 10.1007/s11695-015-1574-1 ORIGINAL CONTRIBUTIONS Prevalence of Barrett s Esophagus in Bariatric Patients Undergoing Sleeve Gastrectomy Italo Braghetto Attila Csendes Published
OBES SURG (2016) 26:710 714 DOI 10.1007/s11695-015-1574-1 ORIGINAL CONTRIBUTIONS Prevalence of Barrett s Esophagus in Bariatric Patients Undergoing Sleeve Gastrectomy Italo Braghetto Attila Csendes Published
Achalasia is a rare disease with an annual incidence estimated REVIEWS. Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
Guiding Principles. Trans-oral Incisionless Fundoplication (TIF) for GERD: When, Why & How 4/6/18
 Gastroesophageal Reflux Disease Shaping the Future of GERD Management Treating patients with the TIF procedure using the EsophyX device (EndoGastric Solutions) Gonzalo Pandolfi, MD Trans-oral Incisionless
Gastroesophageal Reflux Disease Shaping the Future of GERD Management Treating patients with the TIF procedure using the EsophyX device (EndoGastric Solutions) Gonzalo Pandolfi, MD Trans-oral Incisionless
Medical Policy Manual. Topic: Gastric Reflux Surgery Date of Origin: November Section: Surgery Last Reviewed Date: March 2014
 Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation. Introduction. Predisposing factor. Introduction.
 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
A CURIOUS CASE OF HYPERTENSIVE LES. Erez Hasnis Department of Gastroenterology Rambam Health Care Campus
 A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
MINIMALLY INVASIVE PROCEDURES FOR GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 UnitedHealthcare Commercial Medical Policy MINIMALLY INVASIVE PROCEDURES FOR GASTROESOPHAGEAL REFLUX DISEASE (GERD) Policy Number: 2017T0322T Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS
UnitedHealthcare Commercial Medical Policy MINIMALLY INVASIVE PROCEDURES FOR GASTROESOPHAGEAL REFLUX DISEASE (GERD) Policy Number: 2017T0322T Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS
ENDOLUMINAL THERAPIES FOR GERD. University of Colorado Department of Surgery Grand Rounds March 31st, 2008
 ENDOLUMINAL THERAPIES FOR GERD University of Colorado Department of Surgery Grand Rounds March 31st, 2008 Overview GERD Healthcare significance Definitions Treatment objectives Endoscopic options Plication
ENDOLUMINAL THERAPIES FOR GERD University of Colorado Department of Surgery Grand Rounds March 31st, 2008 Overview GERD Healthcare significance Definitions Treatment objectives Endoscopic options Plication
Lower Esophageal Sphincter Augmentation for Gastroesophageal Reflux Disease: The Safety of a Modern Implant
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 27, Number 6, 2017 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2017.0025 Full Report Lower Esophageal Sphincter Augmentation for Gastroesophageal
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 27, Number 6, 2017 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2017.0025 Full Report Lower Esophageal Sphincter Augmentation for Gastroesophageal
Efficacy of magnetic sphincter augmentation in patients with large hiatal hernias
 DOI 10.1007/s00464-016-5204-3 and Other Interventional Techniques Efficacy of magnetic sphincter augmentation in patients with large hiatal hernias Kais A. Rona 1 Jessica Reynolds 1 Katrin Schwameis 1
DOI 10.1007/s00464-016-5204-3 and Other Interventional Techniques Efficacy of magnetic sphincter augmentation in patients with large hiatal hernias Kais A. Rona 1 Jessica Reynolds 1 Katrin Schwameis 1
PeriOperative Concerns for Anti Reflux Procedure Patients
 PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
Esophageal Sphincter Device for Gastroesophageal Reflux Disease
 original article Esophageal Sphincter Device for Gastroesophageal Reflux Disease Robert A. Ganz, M.D., Jeffrey H. Peters, M.D., Santiago Horgan, M.D., Willem A. Bemelman, M.D., Ph.D., Christy M. Dunst,
original article Esophageal Sphincter Device for Gastroesophageal Reflux Disease Robert A. Ganz, M.D., Jeffrey H. Peters, M.D., Santiago Horgan, M.D., Willem A. Bemelman, M.D., Ph.D., Christy M. Dunst,
The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality
 Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Effective Health Care
 Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
Role of Endoscopy in Gastroesophageal Reflux Disease
 Role of Endoscopy in Gastroesophageal Reflux Disease Joachim Mössner University of Leipzig Berlin, May 4, 2006 Role of Endoscopy in Gastroesophageal Reflux Disease In Diagnosis Magnifying endoscopy Chromoendoscopy
Role of Endoscopy in Gastroesophageal Reflux Disease Joachim Mössner University of Leipzig Berlin, May 4, 2006 Role of Endoscopy in Gastroesophageal Reflux Disease In Diagnosis Magnifying endoscopy Chromoendoscopy
David Markowitz, MD. Physicians and Surgeons
 Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Management of the Difficult Patient with Type 3 Achalasia. Steven R. DeMeester Professor and Clinical Scholar Department of Surgery
 Management of the Difficult Patient with Type 3 Achalasia Steven R. DeMeester Professor and Clinical Scholar Department of Surgery Achalasia Treatment Concepts Disease leads to non-relaxing LES and loss
Management of the Difficult Patient with Type 3 Achalasia Steven R. DeMeester Professor and Clinical Scholar Department of Surgery Achalasia Treatment Concepts Disease leads to non-relaxing LES and loss
Myogenic Control. Esophageal Motility. Enteric Nervous System. Alimentary Tract Motility. Determinants of GI Tract Motility.
 Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Esophageal Motility. Alimentary Tract Motility
 Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Refractory GERD. Kenneth R. DeVault, MD, FACG President American College of Gastroenterology Chair Department of Medicine Mayo Clinic Florida
 Refractory GERD Kenneth R. DeVault, MD, FACG President American College of Gastroenterology Chair Department of Medicine Mayo Clinic Florida Objectives Define the terminology associated with refractory
Refractory GERD Kenneth R. DeVault, MD, FACG President American College of Gastroenterology Chair Department of Medicine Mayo Clinic Florida Objectives Define the terminology associated with refractory
Falk Symposium, , , Portorož. Physiology of Swallowing and Anti-Gastroesophageal. Reflux-Mechanisms. Mechanisms: C.
 Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Achalasia is a primary esophageal motility disorder of unknown
 Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Clinical Study Management of Gastroesophageal Reflux Disease: A Review of Medical and Surgical Management
 Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2014, Article ID 654607, 5 pages http://dx.doi.org/10.1155/2014/654607 Clinical Study Management of Gastroesophageal Reflux Disease: A Review
Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2014, Article ID 654607, 5 pages http://dx.doi.org/10.1155/2014/654607 Clinical Study Management of Gastroesophageal Reflux Disease: A Review
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Achalasia, barium esophagography for, 57 58 Acid pocket, 18 19 Acid-sensing ion, 20 Acupuncture, 128 Adiponectin, in obesity, 166 ADX10059 metabotropic
Note: Page numbers of article titles are in boldface type. A Achalasia, barium esophagography for, 57 58 Acid pocket, 18 19 Acid-sensing ion, 20 Acupuncture, 128 Adiponectin, in obesity, 166 ADX10059 metabotropic
34th Annual Toronto Thoracic Surgery Refresher Course
 34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
Traditionally, surgical antireflux therapy has been
 Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
ORIGINAL ARTICLE. Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation
 ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540
 Electrical stimulation of the lower oesophageal sphincter for treating gastro-oesophageal reflux disease Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540 Your
Electrical stimulation of the lower oesophageal sphincter for treating gastro-oesophageal reflux disease Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540 Your
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): November 26, 2013 Most Recent Review Date (Revised): November 26, 2013 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
Original Issue Date (Created): November 26, 2013 Most Recent Review Date (Revised): November 26, 2013 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword?
 A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword? Pavlos Kaimakliotis, MD Department of Gastroenterology Lahey Hospital and Medical Center Assistant Professor of Medicine
A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword? Pavlos Kaimakliotis, MD Department of Gastroenterology Lahey Hospital and Medical Center Assistant Professor of Medicine
Gastrointestinal Imaging Clinical Observations
 Esophageal Motility Disorders After Laparoscopic Nissen Fundoplication Gastrointestinal Imaging Clinical Observations Natasha E. Wehrli 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer
Esophageal Motility Disorders After Laparoscopic Nissen Fundoplication Gastrointestinal Imaging Clinical Observations Natasha E. Wehrli 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer
Achalasia: Classic View
 Achalasia: Dilate, Botox, Knife or POEM Prateek Sharma, MD Kansas University School of Medicine Achalasia: Classic View 1 Diagnosis of Achalasia Endoscopy may be normal in as many as 44% Upper GI series
Achalasia: Dilate, Botox, Knife or POEM Prateek Sharma, MD Kansas University School of Medicine Achalasia: Classic View 1 Diagnosis of Achalasia Endoscopy may be normal in as many as 44% Upper GI series
ORIGINAL ARTICLE. Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease
 ORIGINAL ARTICLE Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease Emmanuel Chrysos, MD; George Prokopakis, MD; Elias Athanasakis, MD; George Pechlivanides, MD; John Tsiaoussis,
ORIGINAL ARTICLE Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease Emmanuel Chrysos, MD; George Prokopakis, MD; Elias Athanasakis, MD; George Pechlivanides, MD; John Tsiaoussis,
127 Chapter 1 Chapter 2 Chapter 3
 CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
What can you expect from the lab?
 Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
Protocol. This trial protocol has been provided by the authors to give readers additional information about their work.
 Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Ganz RA, Peters JH, Horgan S, et al. Esophageal sphincter device for
Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Ganz RA, Peters JH, Horgan S, et al. Esophageal sphincter device for
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
ORIGINAL ARTICLE GRAPHICAL ABSTRACT
 ORIGINAL ARTICLE Laparoscopic magnetic sphincter augmentation versus doubledose proton pump inhibitors for management of moderate-tosevere regurgitation in GERD: a randomized controlled trial Reginald
ORIGINAL ARTICLE Laparoscopic magnetic sphincter augmentation versus doubledose proton pump inhibitors for management of moderate-tosevere regurgitation in GERD: a randomized controlled trial Reginald
Surgical Evaluation for Benign Esophageal Disease. Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018
 Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Diagnosis and Management of Achalasia: Past, Present, & Future
 Diagnosis and Management of Achalasia: Past, Present, & Future Kyle A. Perry, MD, FACS Assistant Professor of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical
Diagnosis and Management of Achalasia: Past, Present, & Future Kyle A. Perry, MD, FACS Assistant Professor of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease
 ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
Gastro esophageal reflux disease DR. AMMAR I. ABDUL-LATIF
 Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
Treating Achalasia. When to consider surgery and New options for therapy
 Treating Achalasia When to consider surgery and New options for therapy James B. Wooldridge,Jr., MD Ochsner Medical Center Senior Staff Surgeon General, Laparoscopic, and Bariatric Surgery Disclosures
Treating Achalasia When to consider surgery and New options for therapy James B. Wooldridge,Jr., MD Ochsner Medical Center Senior Staff Surgeon General, Laparoscopic, and Bariatric Surgery Disclosures
GERD: 2014 Dilemmas and Solutions. Ronnie Fass MD, FACP Professor of Medicine Case Western Reserve University
 GERD: 2014 Dilemmas and Solutions Ronnie Fass MD, FACP Professor of Medicine Case Western Reserve University How to Maximize Your PPI Treatment? Improve compliance and adherance Fass R. Am J Gastroenterol.
GERD: 2014 Dilemmas and Solutions Ronnie Fass MD, FACP Professor of Medicine Case Western Reserve University How to Maximize Your PPI Treatment? Improve compliance and adherance Fass R. Am J Gastroenterol.
9/18/2015. Disclosures. Objectives. Dysphagia Sherri Ekobena PA-C. I have no relevant financial interests to disclose I have no conflicts of interest
 Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
The impact of fibrin glue in the prevention of failure after Nissen fundoplication
 Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
Accepted Manuscript. To appear in: Gastrointestinal Endoscopy. Received Date: 18 April Accepted Date: 11 July 2018
 Accepted Manuscript Laparoscopic magnetic sphincter augmentation versus double-dose proton pump inhibitors for management of moderate-to-severe regurgitation in GERD: a randomized controlled trial R.C.
Accepted Manuscript Laparoscopic magnetic sphincter augmentation versus double-dose proton pump inhibitors for management of moderate-to-severe regurgitation in GERD: a randomized controlled trial R.C.
Putting Chronic Heartburn On Ice
 Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
NCD, LCD, LCA Non-Covered Services (L35008)
 Clinical Review Criteria Treatment of Gastroesophageal Reflux Disease - GERD Stretta Procedure CR BARD s Endoscopic Suturing System Endoscopic Placement of a Bulking Material at the Lower Esophageal Sphincter
Clinical Review Criteria Treatment of Gastroesophageal Reflux Disease - GERD Stretta Procedure CR BARD s Endoscopic Suturing System Endoscopic Placement of a Bulking Material at the Lower Esophageal Sphincter
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Combined Experience of Two European Centers
 Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Primary Achalasia : POEM Vs Heller's Myotomy AMOL BAPAYE MD (MS ), FAS GE
 Primary Achalasia : POEM Vs Heller's Myotomy AMOL BAPAYE MD (MS ), FAS GE SHIVANAND DESAI CENTER FOR DIG EST IVE DISOR DERS DEENANAT H MANGESHKAR HOSPITAL & R ESEAR C H C ENTER, PUNE, INDIA What is Achalasia
Primary Achalasia : POEM Vs Heller's Myotomy AMOL BAPAYE MD (MS ), FAS GE SHIVANAND DESAI CENTER FOR DIG EST IVE DISOR DERS DEENANAT H MANGESHKAR HOSPITAL & R ESEAR C H C ENTER, PUNE, INDIA What is Achalasia
Gastroesophageal reflux disease (GERD) is the most common
 Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD
 Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Ang D, Misselwitz B, Hollenstein M, et al.
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Ang D, Misselwitz B, Hollenstein M, et al.
Diagnosis and management of early gastric band slip after laparoscopic adjustable gastric banding
 Case report Videosurgery Diagnosis and management of early gastric band slip after laparoscopic adjustable gastric banding Mehmet Sertkaya, Arif Emre, Fatih Mehmet Yazar, Ertan Bülbüloğlu Department of
Case report Videosurgery Diagnosis and management of early gastric band slip after laparoscopic adjustable gastric banding Mehmet Sertkaya, Arif Emre, Fatih Mehmet Yazar, Ertan Bülbüloğlu Department of
ORIGINAL ARTICLE. Endoluminal Full-Thickness Plication and Radiofrequency Treatments for GERD
 ORIGINAL ARTICLE Endoluminal Full-Thickness Plication and Radiofrequency Treatments for GERD An Outcomes Comparison Louis O. Jeansonne IV, MD; Brent C. White, MD; Vien Nguyen, MD; Syed M. Jafri, BS; Vickie
ORIGINAL ARTICLE Endoluminal Full-Thickness Plication and Radiofrequency Treatments for GERD An Outcomes Comparison Louis O. Jeansonne IV, MD; Brent C. White, MD; Vien Nguyen, MD; Syed M. Jafri, BS; Vickie
MINIMALLY INVASIVE PROCEDURES FOR GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 UnitedHealthcare of California (HMO) UnitedHealthcare Benefits Plan of California (EPO/POS) UnitedHealthcare of Oklahoma, Inc. UnitedHealthcare of Oregon, Inc. UnitedHealthcare Benefits of Texas, Inc.
UnitedHealthcare of California (HMO) UnitedHealthcare Benefits Plan of California (EPO/POS) UnitedHealthcare of Oklahoma, Inc. UnitedHealthcare of Oregon, Inc. UnitedHealthcare Benefits of Texas, Inc.
ESOPHAGEAL CANCER AND GERD. Prof Salman Guraya FRCS, Masters MedEd
 ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
Nissen Fundoplication
 Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
THORACIC SURGERY: Dysphagia. Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone. Thoracic Surgery Toronto East General Hospital
 THORACIC SURGERY: Dysphagia Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone Thoracic Surgery Toronto East General Hospital Objectives Definitions Common causes Investigations Treatment options Anatomy
THORACIC SURGERY: Dysphagia Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone Thoracic Surgery Toronto East General Hospital Objectives Definitions Common causes Investigations Treatment options Anatomy
ORIGINAL ARTICLE. Gastric Banding Interferes With Esophageal Motility and Gastroesophageal Reflux
 ORIGINAL ARTICLE Gastric Banding Interferes With Esophageal Motility and Gastroesophageal Reflux Michel Suter, MD, PD; Gian Dorta, MD; Vittorio Giusti, MD, PD; Jean-Marie Calmes, MD Background: Gastroesophageal
ORIGINAL ARTICLE Gastric Banding Interferes With Esophageal Motility and Gastroesophageal Reflux Michel Suter, MD, PD; Gian Dorta, MD; Vittorio Giusti, MD, PD; Jean-Marie Calmes, MD Background: Gastroesophageal
INFORMED CONSENT FOR LAPAROSCOPIC ADJUSTABLE GASTRIC BAND. Please read this form carefully and ask about anything you may not understand.
 Please read this form carefully and ask about anything you may not understand. I consent to undergo laparoscopic placement of a laparoscopic Adjustable Gastric Band for the purposes of weight loss. I met
Please read this form carefully and ask about anything you may not understand. I consent to undergo laparoscopic placement of a laparoscopic Adjustable Gastric Band for the purposes of weight loss. I met
SURGERY LAPAROSCOPIC ANTI-REFLUX (GORD) SURGERY
 LAPAROSCOPIC ANTI-REFLUX (GORD) If you suffer from heartburn, your surgeon may have recommended Laparoscopic Anti-reflux Surgery to treat this condition, technically referred to as Gastro-oesophageal Reflux
LAPAROSCOPIC ANTI-REFLUX (GORD) If you suffer from heartburn, your surgeon may have recommended Laparoscopic Anti-reflux Surgery to treat this condition, technically referred to as Gastro-oesophageal Reflux
The Lower Esophageal Sphincter in Health and Disease. Steven R. DeMeester Professor and Clinical Scholar Department of Surgery
 The Lower Esophageal Sphincter in Health and Disease Steven R. DeMeester Professor and Clinical Scholar Department of Surgery The Lower Esophageal Sphincter Dual function: allow bolus from esophagus into
The Lower Esophageal Sphincter in Health and Disease Steven R. DeMeester Professor and Clinical Scholar Department of Surgery The Lower Esophageal Sphincter Dual function: allow bolus from esophagus into
Speaker disclosure. Objectives. GERD: Who and When to Treat 7/21/2015
 GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
Description. Section: Medicine Effective Date: January 15, 2015 Subsection: Original Policy Date: December 6, 2013 Subject: Page: 1 of 7
 Last Review Status/Date: December 2014 Page: 1 of 7 Description Esophageal achalasia is characterized by prolonged occlusion of the lower esophageal sphincter (LES) and reduced peristaltic activity, making
Last Review Status/Date: December 2014 Page: 1 of 7 Description Esophageal achalasia is characterized by prolonged occlusion of the lower esophageal sphincter (LES) and reduced peristaltic activity, making
Gastroesophageal Reflux Disease:
 Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Robotics in General Surgery. Objectives
 Robotics in General Surgery Jennifer S. Schwartz, MD Assistant Professor of Surgery Department of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical Center
Robotics in General Surgery Jennifer S. Schwartz, MD Assistant Professor of Surgery Department of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical Center
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of endoscopic augmentation of the lower oesophageal sphincter using hydrogel
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of endoscopic augmentation of the lower oesophageal sphincter using hydrogel
Gastroesophageal Reflux Disease
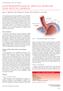 gastrointestinal tract and abdomen Gastroesophageal Reflux Disease and Hiatal Hernia James A. Rydlewicz, MD, Matthew R. Pittman, MD, and Kyle A. Perry, MD Gastroesophageal reflux disease (GERD) was not
gastrointestinal tract and abdomen Gastroesophageal Reflux Disease and Hiatal Hernia James A. Rydlewicz, MD, Matthew R. Pittman, MD, and Kyle A. Perry, MD Gastroesophageal reflux disease (GERD) was not
