JMSCR Vol 04 Issue 07 Page July 2016
|
|
|
- Darrell Cummings
- 5 years ago
- Views:
Transcription
1 Impact Factor Index Copernicus Value: ISSN (e) x ISSN (p) DOI: A Clinical Outcome of Dexamethasone therapy of Patients with Pyogenic Meningitis Authors Atul Kumar 1, Md Izhar Alam 2, Taskeen Ahmad Reza 3, Shruti Sonal 4, Kaushal Kumar Sinha 5, Karan Bhargav 6, Wasim Alam 7 1 Associate professor, Dept of Medicine, Katihar Medical College, Katihar, Bihar, India 2 Assistant professor, Dept of Pathology, Katihar Medical College, Katihar, Bihar, India 3 Assistant Professor, Dept of Medicine, Katihar Medical College, Katihar, Bihar, India 4,5,6,7 PGT, Department of Medicine, Katihar Medical College, Katihar, Bihar, India Corresponding Author Dr Atul Kumar Associate Professor, Dept of Medicine, Katihar, Medical College, Katihar, Bihar, India. dratulkumarkmc@gmail.com Ph: ABSTRACT Objective: Observation of hastening effect of dexamethasone on recovery time and reductions of case fatality and neurological complications of pyogenic meningitis. Methodology: A total of 39 patients with pyogenic meningitis were considered on the basis of short clinical history and laboratory findings like, fever, headache, projectile vomiting, confusion/delirium, unconsciousness and neck rigidity and kerning s sign, raised CSF pressure, presence of turbidity or purulent CSF with identification of bacteria on gram staining or culture of CSF, High CSF cell count (> 10 to < /Cumm) with neutrophilic predominance, Reduced CSF glucose level (<40mg%), Low CSF to blood glucose concentration ratio (<40 %), High CSF protein level (>50mg/dl). Results: Data was analyzed by using MS-Office software. Conclusions: Adjunctive dexamethasone therapy may improve the outcome of pyogenic meningitis in adolescent and adult patients. And the intensity of headache, vomiting and fever were also relieved by using dexamethasone therapy. Key words: pyogenic meningitis, dexamethasone therapy, clinical outcome. Introduction Acute Pyogenic (Bacterial) meningitis is a potentially life threatening disease that is an inflammation of the meninges and underlying subarachnoid cerebro-spinal fluid (CSF). Acute pyogenic meningitis and with its associated high morbidity and mortality remains a major health problem worldwide. At least 30 countries worldwide including the United States, have reported serious outbreaks of meningococcal meningitis in recent years. [1] Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11384
2 Organism s most commonly responsible community acquired Pyogenic Meningitis are: Streptococcus Pneumonia (-50 %), N. Meningitis (- 25 %), Group B Streptococci (- 15%), Listeria Monocytogens (-10%), H. Influenza (< 10%). Most of the organism gains entry into central nervous system via the blood stream secondary to respiratory tract infection giving rise to cerebral edema and raised intra cranial tension which impairs blood flow subsequently leading to complication of meningitis. Various investigators found that subarachnoid space inflammation and various inflammatory cytokines have a major role in pathophysiology of pyogenic meningitis that contributes to morbidity and mortality. [2] Lumbar puncture remains the gold standard in the diagnosis of meningitis there are people who argue strongly against it because of fear of brain herniation. Despite significant advances in the understanding of the pathogenesis and antibiotic treatment of acute Pyogenic meningitis, the mortality and morbidity from the disease remains unacceptably high. The large number of those who survive may have neurological disabilities and squeal. [3] The discovery penicillin by Alexander Fleming and its first uses in 1941 was the first major break in the treatment of Pyogenic infection including meningitis. It is uniformly accepted that empirical antibiotic treatment based on the age of the patient and health status should be instituted as soon as possible. If there is delay in detection of organisms and its antibiotic susceptibility, once the organisms isolated, drug treatment should be modified according to sensitivity pattern. [4] Much controversy exists in the use of Dexamethasone as an adjunctive therapy to antibiotics in the treatment of acute pyogenic meningitis especially in adults. Different clinical trial have revealed that suppression of inflammation by dexamethasone has brought significant reduction in CSF pressure, brain edema and lactate concentration in CSF in experimental models of S. Pneumoniae and H. influenza meningitis it decreases the leakage of low molecular weight proteins from serum into the CSF in the experimental models of Pneumococcal meningitis. [5] Dexamethsone given in children with meningitis at the initiation of antibiotics therapy significantly reduces the concentration of interleukin-1 B and prostaglandin E2 and the degree of inflammation in samples of CSF obtained 24 hours apart after the first dose as compared with the result in children who received placebo. It has now been shown in in-vitro experiment that interleukin 1b and tumor necrosis factor gene transcription is induced by lipopolysaccharides and that dexamethasone inhibits this gene. [6] Objective of our study was to observation the hastening effect of dexamethasone on recovery time and reductions of case fatality and neurological complications of pyogenic meningitis. Material and methods Study was done in emergency ward and indoor wards of Katihar Medical College, Katihar, Bihar, India, patients who were suffering of pyogenic meningitis, included in this study. A total of 39 cases (24 males and 15 females) of patients with age group 10 to 65 years were included. The attendant of entire subject signed an informed consent approved by institutional ethical committee of Katihar Medical College, Katihar, Bihar, India was sought. Data were collected in emergency ward and indoor ward of Katihar Medical College, Katihar, Bihar, India, during period of November 2013 to May Procedures It was divided into clinical criteria and laboratory criteria. Clinical criteria were short history of fever, headache, projectile vomiting, confusion/delirium, unconsciousness and neck rigidity and kernig s sign. Laboratory criteria were raised CSF pressure, presence of turbidity or purulent CSF with identification of bacteria on gram staining or culture of CSF, High CSF cell Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11385
3 count (> 10 to < /Cumm) with neutrophilic predominance, Reduced CSF glucose level (<40mg%), Low CSF to blood glucose concentration ratio (<40 %), High CSF protein level (>50mg/dl). Treatment Randomization There were two groups, group A and Group B. Group A were 22 patients, treated with dexamethasone and group B were 17 patients treated without dexamethasone. Group A: Dexamethasone therapy: Patients were randomly assigned to receive either dexamethasone (group A) or placebo (Group B) in case and control manner. 2 ml vials were prepared which contained a clear colorless solution and were identical in appearance. Group A patients received dexamethasone sodium phosphate in a dose of 0.6 mg/kg body weight per day in a 4 divided doses for four days. The first dose of dexamethasone was given 20 minutes prior to first dose of antimicrobial agents. The group receiving dexamethasone were further subdivided into two groups, (i) which received dexamethasone, 20 minutes prior to first dose of antibiotic and (ii) which received dexamethasone simultaneously with first dose of antibiotic. Antibiotic therapy The patients were assigned to receive either conventional antibiotic of third generation cephalosporins. Antibiotics used in this study are: ceftriaxone 2 gm twice daily (maximum 4 gm/day) and G penicillin million units, every four hours + chloramphenicol 1 gm 8 hourly + gentamycin 80 mg, 8 hourly. Antibiotic therapy was given for 10 to 14 days as a rule, and extended only in those patients whose condition failed to improve within this duration. Other supportive therapy was instituted, as required. Follow up assessment Course of illness during hospitalization Each patient was examined daily for fever, meningeal signs, level of consciousness, presence or absence of neurologic deficit and occurrence of seizures and mild treatment reviewed on the 5 th day and comparison was made. A cranial CT scan was done to find out the evidence of persistently raised intracranial pressure suggesting the possibility of hydrocephalus, subdural effusion or empyema or brain abscess, the presence of any focal neurologic deficit and the persistence of pyrexia beyond 7 days in the hospital. And at the time of discharge complete neurological examination was done. Statistical Analysis Data was analyzed by using Ms-Office software and standard statistical methods. Observations This present study was carried out on 39 patients of purulent meningitis admitted in Katihar Medical College, Katihar, during November 2013 to May Out of 39 patients 24 (61.15%) were male and 15 (38.5 %) were female. At the time of admission, 100 % patients were complaining headache, nausea, vomiting and fever % patients were symptom like sweating, % cases were myalgia, 58.9 % cases were photophobia, % cases were convulsion, % patients were confusion and % were in coma. Tachycardia were present in % cases, bradycardia in % cases, hypertension were present in % cases, hypotension in % cases, respiratory depression in % cases and tachypnea in % cases. Temperature was found in 100 % cases, altered sensoriums in 100 %, unconscious were found in % patients. Papillary abnormality was seen in % cases, cranial nerve palsies in % cases, neck rigidity and Kerning s sign were present in 66.6 % cases, and focal neurological deficit was found in Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11386
4 15.38 % cases % patients were presented with Glass Gow Coma scale (GCS) of 3-5 with males 70 % and female 30 % of the cases presented with the GCS between 6-10 with males being 60 % and females 40 %. Only 4 patients (10.3 %) were presented with a GCS between % cases were the positive history of predisposing factors of which 75 % of females and 25 % were males. 50 % were otitis media where as 25 % cases were pneumonia. And 12.5 % patients were head injury with CSF leak and with sinusitis % patients were received a combination of ceftriaoxone, and 33.3 % received a combination of C. penicillin, chloramphenicol and gentamycin % patients were received ceftriaoxone of which 57.7 % were received steroids and 42.3 % patients were not received steroids. Out of 15 patients of ceftriaoxone group, 53.3% patients with steroid therapy were GCS between 3-5, 33.3 % steroid therapy were GCS 6-10, and 13.3 % patients with steroid therapy were GCS Out of 11 patients of the ceftriaoxone group, 54.5 % patients of ceftriaoxone group was not received steroids had GCS 3-5, 27.3 % had GCS 6-10, 18.7 % had GCS In the penicillin group, 53.8 % out of 13 patients received steroids and 46.2 % were not received steroids. Out of 7 patients receiving steroids in penicillin group (57.1 % had a GCS 3-5, 28.6 % had a GCS 6-10 and 14.3 % had a GCS Penicillin group patients who were not received steroids (33.35 %) had a GCS 3-5, 3(50 %) had a GCS 6-10 and 1 (16.7% had a GCS) Symptomatically comparison of two groups, group I with steroid therapy and other group II without steroid therapy, on 5 th days of treatment was found that, In group I patients, out of 14 patients, 4 (28.57 %) patients were persisted with headache. In group II, Out of 12 patients, 6(50 %) patients were persisted with headache. In group I, 4 (22.2 %) patients were persisted with nausea and vomiting and in group II 4 (40 %) patients were persisted with nausea and vomiting on 4 th days of treatment. Fever was seen in 4 (28.5 %) patients in group I, and 6 (50 %) patients in group II. Confusion/delirium was present in 6 (46.15 %) out of 13 patients of group I, and 5 (50 %) patients of group II. 2 (15.3 %) patients were remained in coma of group I, and 3 (25 %) of group II after 4 th days of treatment. Comparison of signs of the two group, in group I, 14.2 % patients were persisted with tachycardia, and in group II, 16.6 % cases were persisted on 5 th days of treatment. Hypotension was seen in 33.3 % cases of each group and tachypnea was persisted in 25 % patients of group I, 20 % patients of group II % patients of group I, were remained febrile and 50 % patients of group II were febrile. Altered sensorium was seen in 46.1 % cases of group I, and 50 % patients of group II. Unconscious were persisted in 15.4 % patients of group I, and 25 % patients of group II. Neck rigidity was seen in 37.5 % cases of group I, and 30 % patients of group II. In group I, 68.6 % patients were reduced total leukocyte count of peripheral blood, and in group II, 79.5 % patients were reduced. In group I, 14.3 % patients were turbidity in CSF, and in group II, 67 % patients were turbidity in CSF. The total number of cells in the CSF was reduced to 39.5 % of the initial value, which receiving the dexamethasone as an adjunctive therapy, and 87.5 % patients were increase sugar who were not receiving dexamethason therapy. The decrease in CSF protein was to about % of the initial value and reduced to % of the initial value after 4 th days of treatment. When 9 (40.9 %) patients received dexamethasone 20 minutes prior to, in which 3 patients died. And patients 13 (59.1 %) who received simultaneously with the first dose of antibiotic, 5 patients died. Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11387
5 Comparison of clinical features in prime steroid group (1a) and concomitant steroid group (1b), headache in group 1a persisted in 1 (16.6 %) out of 6 patients on 5th days as compared to 3 (33.5 %) out of 9 patients in group Ib. Nausea / vomiting disappeared in all 3 patients in group 1a and in group 1b it persisted in 2 (33.3%) out of 6 patients. Fever in group 1a was seen in 1 (16.6 %) out of 6 patients where as in group 1b it persisted in 3 (33.5 %) out of 9 patients on 5 th days of treatment. Confusion / delirium persisted in 2 (33.3 %) patients in group 1a and 4 (50 %) in group Ib. neck rigidity and Kerning s sign was seen in 1 (33.3 %) in group 1a and 2 (40 %) in group 1b patients on 5th days of treatment. Unconsciousness disappeared in all 6 patients in group 1 a, 2 (25 %) out of 8 patients on 5 th days of treatment. Comparison of CSF finding in primed steroid group 1a and concomitant steroid group 1 b patients, it was shown that turbidity persisted in 1(16.6 %) patients of group 1a and 1(11.1%) of group 1b patients on 5 th days of treatment. Total cell count in group 1a was reduced to 28.7 % of the initial in group 1 a and 43.3 % in group 1b. polymorphs in CSF were reduced to 13.3 % of the initial value in group 1 a patient and 20 % in group 1 b patients. Sugar was showed an increase to about 150 % of the initial value in group 1a and 113 % in group 1 b patients. Protein was reduced to 50 % in group 1a and % in group 1b patients % patients who received dexamethasone were developed to manifestation of upper gastrointestinal bleeding. Risk of secondary fever of total of 39 patients, 42.8 % patients developed fever after receiving dexamethasone therapy. Only one patient developed acute psychosis on 4 th days of treatment. 7 (26.9 %) patients were death in ceftriaxone therapy group and 6 (46.2 %) patients were death in penicillin therapy group. Out of the 15 patients in the ceftriaoxone group, who received dexamethasone, 4 (26.7 %) were died. Out of the 11 patients in the ceftriaoxone group, who did not receive dexamethasone, 3 (27.3 %) were died. Out of the 7 patients in the penicillin group receiving dexamethasone, 3 (42.8 %) was died. Out of the 6 patients in the penicillin group not receiving dexamethasone 3 (50 %) were died. Mortality of patients with CSF glucose level < 20 mg/dl was 100 % and CSF glucose level > 40 mg/dl at the time of admission had no mortality. Table.1. Mortality of using various antibiotics with steroids and without steroids therapy. Sr. No GCS score Grade of coma Ceftriaoxone Total No. With steroids (n=15) III 20 3 (75%) II 15 1 (25%) No steroids (n=11) 2 (66.7%) 1 (33.3%) N (%) 5 2 (66.7%) 2 1 (33.3%) C. penicillin + chloramphenicol + gentamycin With No N (%) steroid steroid (n=7) (n=6) 2 (66.7%) 1 (33.3%) 4 (66.7%) 2 (33.3%) I (26.7%) (27.3%) (42.8%) (50%) (46.2%) Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11388
6 Series1 Series2 5 0 total No. of patient with steroids without steroids Figure.1. Mortality of using antibiotics with steroids and without steroids therapy. Discussion This study was carried out on 39 patients of purulent meningitis admitted in ward of Katihar Medical College, Bihar, India. Patients were randomly devided into two groups, Group 1 (n=22) which received dexamethasone as an adjunctive therapy along with antibiotics and group II (n=17) which did not received dexamethasone. Group I further subdivided into two groups, group 1a which received dexamethasone 20 minutes prior to first dose of antibiotics and group 1b, which received dexamethasone simultaneously with the first dose of antibiotics. Antibiotics used were either a combination of ceftriaoxone (n=26), or a combination of G. penicillin + chloramphenicol + gentamycin (n+13). Dexamethasone was used in a dose of 0.6 mg/kg body weight 6 hourly for 4 days. Tunkel AR and Scheld WM (1995) observed that headache, nausea, vomiting, meningismus, often with signs of cerebral dysfunction were in 85 % patients. Seizures were present in 40 % of the patients. Kerning s sign and/or Brudzinski s sign were elicited in only about 50 % cases. Papilloedema was present in <1% patients. When they examined the CSF, found that opening pressure was virtually elevated in all patients. The gross appearance was cloudy of turbid if the white cell count was elevated. Approximately 10 % of the cases presented initially with the predominance of lymphocyte in the CSF. Very low white cell counts in the CSF were also observed in few cases. [7] Our study was found that, headache, nausea, vomiting, and fever were in 100 % patients. Signs of cerebral dysfunction such confusion/delirium was seen in % patients and coma in % patients. Neck rigidity and Kerning s sign was seen in 66.6 % patients. Cranial nerve palsies and focal neurological deficit was seen in % patients. Seizure was present in 23 % patients. And cloudy or turbid CSF was found in almost all cases (>95%). 95 % patients presented with neutrophilic predominance. Only 5 % of the case had initial lumphocyte predominance but gram stain positive. CSF sugar concentration was <40 mg/dl in 95 % of the patients and CSF to blood glucose ratio was approximately 0.27 on an average. In our study mortality reached 100 % in patient having CSF glucose less than 20 mg/dl of CSF/serum glucose ratio of less than Tunkel et al also concluded that predisposing factors as otitis media, sinusitis, pneumonia were present in 30 % of the patients. [6] Our study was found that 20.5 % patients was a positive history of predisposing factors, out of Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11389
7 which 50 % had otitis media and 25 % had pneumonia. Aswasthi S, Moin S. et al (1997) was used of Glass Gow Coma scale and concluded that 42.2 % was pyogenic meningitis, 36.9 % was tubercular meningitis and 20.9 % was meningo-encephalitis. And within first three days of hospitalization 18.7 % patients were death. [7] In our study, 51.2 % patient were GCS between 3-5, 38.5 % patients were GCS between 6-10 and 10.3 % between Mortality was 33.3 %, 45 % of patients with GCS 3-5, 26 % of patients with GCS, % of the total mortality was within first 3 days of hospitalization. It was predicted that patients with pyogenic meningitis with GCS 3-5 only 55 % of the patients were discharged, and with GCS 6-10, 73.3 % of the patients were discharge and patients with GCS 11-15, 100 % were discharged. Dr. Lebels (1988) concluded that children treated by dexamethasone along with antibiotics, were less incidence of sensori neural deafness, more rapid increase in glucose concentration, and a rapid decrease in protein concentration in the CSF, and dexamethasone was not affected the sterilization of CSF. [8] Kanra, Ozan et al (1995) was also studied on children with pneumococcal meningitis and concluded that over all neurological sequel, including hearing loss, at one year were higher in the placebo group at 23 % vs 7.4 % and 26.9 % vs 7.4 % respectively. [9] In our study, we were observed that there was reduction in symptoms like headache, vomiting and fever in the group treated with dexamethasone. And the persistence of confusion/delirium and come were less in group, receiving the dexamethasone (46.15 % vs 50 % and 15.3 % vs 25.5 %). Similarly there was a significant increase in CSF glucose and decrease in CSF protein in the dexamethasone group, and total number of cells in the CSF was also decreased. Thus, our study was found that dexamethasone was played a beneficial role in bacterial meningitis patients in terms of clinical features and CSF findings. And this present study was also found that patients with dexamethasone and cetriaoxone were mortality 26.7 % and patients treated with alone ceftriaoxone mortality were 27.3 %. Patients treated with older combination of G. penicillin, chloramphenicol and gentamycin, mortality rate was higher than patients treated with ceftriaoxone. And found that appropriate antibiotics with dexamethasone combination was more effective. Dr. Odeo et al. was used the dexamethasone before administration of first dose of cefotaxim, and observed that mean opening CSF pressure was lesser in dexamethasone group patients, and after 12 hours of treatment cerebral perfusion increased by 21 %, tumour necrosis factor was also decreased, CSF glucose level was increased, and reduction of CSF protein and leukocytes. [10] Our study was observed that, patients who received dexamethasone prior to first dose of antibiotic were minimally persisted the symptoms such as headache, vomiting and fever, confusion/delirium and coma. Thus we were observed that the use of dexamethasone at least 20 minutes prior to first dose of antibiotics was more effective. Pichard E, Gillis D et al observed that 81.8 % patients treated with dexamethasone were secondary fever. Our study observed that 42.8 % patients treated with dexamethasone were secondary fever, and those patients who were not receiving dexamethasone, they were no fever. [11] Van Wees J, Tegtmeyer KF observed that neurological squeal and fatality rate were significantly decreases the patients who were receiving dexamethasone therapy. [12] Our study observed that, fatality rate was 28 % in S pneumonia, 40 % in Staphylococcus aureuos, 30 % in gram negative bacilli. Mortality rate of patients treated with ceftriaoxone was 26.9 %, and patients treated with G penicillin, chloramphenicol, gentamycin was %. Patients who receiving dexamethasone with Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11390
8 ceftriaoxne, mortality rate was 26.7 %, and patients treated dexamethasone with combination of penicillin, chloramphenical and gentamycin, mortality rate was 42.8 %. Patients treated with dexamethasone, mortality rate was 33.3 % and patients who treated without dexamethasone mortality rate was 35.3%. Our study was shown that mortality rate was higher with respect to other studies, because of, in our study 51.2 % patients were low GCS, we were used the penicillin + chloramphenicol + gentamycin in 33.3 % patients, and duration of our study was 5 days. And also observed that the poor prognostic factors were advanced age, longer duration of prehospitalisation period, low GCS at the time and admission, presence of cranial nerve palsies or focal neurological deficit at the time of admission, CSF leukocytes count > 1000 mm 3 and glucose < 20 mg/dl. Conclusion Adjunctive dexamethasone therapy may improve the outcome of pyogenic meningitis in adolescent and adults. And the intensity of headache, vomiting and fever were relieved, and reduction in neurological complications and mortality were seen in dexamethasone group patients. References 1. Karen L. Roos, Kenneth L. Tyler: Meningitis, Encephalitis brain abcess and empyema: Harrisons principles of internal medicine. Vol II, 16 th edition, McGraw Hill company, 2005;360: Enting R: Dexamethasone for bacterial meningitis; we need the answer; Lancet 1997 April 19;349 : McIntyre P. Dexamethasone treatment for acute bacterial meningitis; how strong is the evidence for routine use? J Neurol Neurosurg Psychiatry; 1996 April: 60(4): Venkatachalam R: Streroid/Dexamethasone in adults with bacterial meningitis. J. Assoc. Physician India 1996 September; 44(a): Townsend GD, Scheld WM: The use of corticosteroid in management of bacterial meningitis in adult. J Antimicrobe Chemother. 1996; 37: Tunkel AR, Scheld WM: Pathogenesis and pathophysiology of bacterial meningitis. Annu Rev Med 1993; 44 : Awasthi S, Moin S, Lyer SM, Renham H: Modified Glasgow Coma Scale to predict mortality in children with acute infection of the CNS. National Medical Journal of India, 1997 September ; 10(5): Lebell MH et al. dexamethasone therapy for bacterial meningitis: Results of two double blind, placebo controlled trials. N. Engld. J. Med. 319; 964: Kanra GY, Ozen H, Secmeer G et al. Beneficial effect of dexamethasone in children with pneumococcal meningitis. Pediatric infection disease J. 1995; 14: Odio CM et al. The beneficial effects of early dexamethasone administration in infant and children with bacterial meningitis. N. Engld. J Med. 1991; 324: Pilchard E Gillis D, Aker M, et al. Rebound fever in bacterial meningitis; Role of dexamethasone dosage. Isr. J Med. Sci May-June; 30(5-6): Van Wees J, Tegtmeyer KF: Value of dexamethasone therapy in bacterial meningitis. Monatsschr Kinderhailkd 1993 Sept; 141(9): 732. Atul Kumar et al JMSCR Volume 04 Issue 07 July Page 11391
Aurora Health Care South Region EMS st Quarter CE Packet
 Name: Dept: Date: Aurora Health Care South Region EMS 2010 1 st Quarter CE Packet Meningitis Meningitis is an inflammatory disease of the leptomeninges. Leptomeninges refer to the pia matter and the arachnoid
Name: Dept: Date: Aurora Health Care South Region EMS 2010 1 st Quarter CE Packet Meningitis Meningitis is an inflammatory disease of the leptomeninges. Leptomeninges refer to the pia matter and the arachnoid
Central Nervous System Infection
 Central Nervous System Infection Lingyun Shao Department of Infectious Diseases Huashan Hospital, Fudan University Definition Meningitis: an inflammation of the arachnoid membrane, the pia mater, and the
Central Nervous System Infection Lingyun Shao Department of Infectious Diseases Huashan Hospital, Fudan University Definition Meningitis: an inflammation of the arachnoid membrane, the pia mater, and the
GUIDELINE FOR THE MANAGEMENT OF MENINGITIS. All children with suspected or confirmed meningitis
 GUIDELINE FOR THE MANAGEMENT OF MENINGITIS Reference: Mennigitis Version No: 1 Applicable to All children with suspected or confirmed meningitis Classification of document: Area for Circulation: Author:
GUIDELINE FOR THE MANAGEMENT OF MENINGITIS Reference: Mennigitis Version No: 1 Applicable to All children with suspected or confirmed meningitis Classification of document: Area for Circulation: Author:
ANTIBIOTIC GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED MENINGITIS AND ENCEPHALITIS IN ADULTS
 ANTIBIOTIC GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED MENINGITIS AND ENCEPHALITIS IN ADULTS Version 4.0 Date ratified February 2009 Review date February 2011 Ratified by Authors Consultation Evidence
ANTIBIOTIC GUIDELINES FOR THE MANAGEMENT OF COMMUNITY-ACQUIRED MENINGITIS AND ENCEPHALITIS IN ADULTS Version 4.0 Date ratified February 2009 Review date February 2011 Ratified by Authors Consultation Evidence
CNS INFECTIONS 1 Acute meningitis
 Definition CNS INFECTIONS 1 Acute meningitis DR. BADRI PAUDEL Bacterial meningitis is a medical emergency. Meningitis is an acute infection within the subarachnoid space. usually secondary bacteremia or
Definition CNS INFECTIONS 1 Acute meningitis DR. BADRI PAUDEL Bacterial meningitis is a medical emergency. Meningitis is an acute infection within the subarachnoid space. usually secondary bacteremia or
Brain abscess rupturing into the lateral ventricle causing meningitis: a case report
 Brain abscess rupturing into the lateral ventricle causing meningitis: a case report Endry Martinez, and Judith Berger SBH Health System, 4422 Third Ave, Bronx, NY 10457 Key words: brain abscess, rupture
Brain abscess rupturing into the lateral ventricle causing meningitis: a case report Endry Martinez, and Judith Berger SBH Health System, 4422 Third Ave, Bronx, NY 10457 Key words: brain abscess, rupture
Narong Auervitchayapat,MD MD., Assist Prof Department of Pediatrics Faculty of Medicine KKU
 Narong Auervitchayapat,MD MD., Assist Prof Department of Pediatrics Faculty of Medicine KKU 5 common diseases:- 1. Bacterial meningitis 2. Tuberculous meningitis 3. Aseptic meningitis 4. Viral encephalitis
Narong Auervitchayapat,MD MD., Assist Prof Department of Pediatrics Faculty of Medicine KKU 5 common diseases:- 1. Bacterial meningitis 2. Tuberculous meningitis 3. Aseptic meningitis 4. Viral encephalitis
by author ESCMID Online Lecture Library Steroids in acute bacterial meningitis
 Steroids in acute bacterial meningitis Javier Garau, MD, PhD University of Barcelona Spain ESCMID Summer School, Porto, July 2009 Dexamethasone treatment in childhood bacterial meningitis in Malawi: a
Steroids in acute bacterial meningitis Javier Garau, MD, PhD University of Barcelona Spain ESCMID Summer School, Porto, July 2009 Dexamethasone treatment in childhood bacterial meningitis in Malawi: a
Meningitis. Author : - Dr. Edward Tsang (registered Chinese Herbalist & Acupuncturist ) Wu Zhu Metaphysician
 Meningitis Author : - Dr. Edward Tsang (registered Chinese Herbalist & Acupuncturist ) Wu Zhu Metaphysician Definition Meningitis is usually restricted to inflammation due to infective agents. Microorganisms
Meningitis Author : - Dr. Edward Tsang (registered Chinese Herbalist & Acupuncturist ) Wu Zhu Metaphysician Definition Meningitis is usually restricted to inflammation due to infective agents. Microorganisms
Mousa Suboh. Zaid Emad. Anas Abu -Humaidan
 1 Mousa Suboh Zaid Emad 1 P a g e Anas Abu -Humaidan In this lecture we will talk about the microbiology of the central nervous system The central nervous system is supposedly sterile, so there is no micro
1 Mousa Suboh Zaid Emad 1 P a g e Anas Abu -Humaidan In this lecture we will talk about the microbiology of the central nervous system The central nervous system is supposedly sterile, so there is no micro
Moath Darweesh. Zaid Emad. Anas Abu -Humaidan
 3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
BACTERIAL MENINGITIS: A FIVE YEAR ( ) RETROSPECTIVE STUDY AT UNIVERSITY MALAYA MEDICAL CENTer (UMMC), KUALA LUMPUR, MALAYSIA
 BACTERIAL MENINGITIS: A FIVE YEAR (2001-2005) RETROSPECTIVE STUDY AT UNIVERSITY MALAYA MEDICAL CENTer (UMMC), KUALA LUMPUR, MALAYSIA H Erleena Nur, I Jamaiah, M Rohela and V Nissapatorn Department of Parasitology,
BACTERIAL MENINGITIS: A FIVE YEAR (2001-2005) RETROSPECTIVE STUDY AT UNIVERSITY MALAYA MEDICAL CENTer (UMMC), KUALA LUMPUR, MALAYSIA H Erleena Nur, I Jamaiah, M Rohela and V Nissapatorn Department of Parasitology,
Dilemmas in the Management of Meningitis & Encephalitis HEADACHE AND FEVER. What is the best initial approach for fever, headache, meningisums?
 Dilemmas in the Management of Meningitis & Encephalitis Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine HEADACHE AND FEVER What is the best initial approach for fever,
Dilemmas in the Management of Meningitis & Encephalitis Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine HEADACHE AND FEVER What is the best initial approach for fever,
Managing meningitis not just antibiotics. Helena White December 2013
 Managing meningitis not just antibiotics Helena White December 2013 Case history 43 year old British-born Asian lady Legal advisor Married with a three year old child (on Amoxicillin for recent ear infection)
Managing meningitis not just antibiotics Helena White December 2013 Case history 43 year old British-born Asian lady Legal advisor Married with a three year old child (on Amoxicillin for recent ear infection)
Emergency Neurological Life Support Meningitis and Encephalitis
 Emergency Neurological Life Support Meningitis and Encephalitis Version: 2.0 Last Updated: 19-Mar-2016 Checklist & Communication Meningitis and Encephalitis Table of Contents Emergency Neurological Life
Emergency Neurological Life Support Meningitis and Encephalitis Version: 2.0 Last Updated: 19-Mar-2016 Checklist & Communication Meningitis and Encephalitis Table of Contents Emergency Neurological Life
CNS Infections in the Pediatric Age Group
 CNS Infections in the Pediatric Age Group Introduction CNS infections are frequently life-threatening In the Philippines, bacterial meningitis is one of the top leading causes of mortality in children
CNS Infections in the Pediatric Age Group Introduction CNS infections are frequently life-threatening In the Philippines, bacterial meningitis is one of the top leading causes of mortality in children
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
CNS Infections. Philip Gothard Consultant in Infectious Diseases Hospital for Tropical Diseases, London. Hammersmith Acute Medicine 2011
 CNS Infections Philip Gothard Consultant in Infectious Diseases Hospital for Tropical Diseases, London Hammersmith Acute Medicine 2011 Case 1 HISTORY 27y man Unwell 3 days Fever Headache Photophobia Previously
CNS Infections Philip Gothard Consultant in Infectious Diseases Hospital for Tropical Diseases, London Hammersmith Acute Medicine 2011 Case 1 HISTORY 27y man Unwell 3 days Fever Headache Photophobia Previously
Practice Guidelines for the Management of Bacterial Meningitis
 IDSA GUIDELINES Practice Guidelines for the Management of Bacterial Meningitis Allan R. Tunkel, 1 Barry J. Hartman, 2 Sheldon L. Kaplan, 3 Bruce A. Kaufman, 4 Karen L. Roos, 5 W. Michael Scheld, 6 and
IDSA GUIDELINES Practice Guidelines for the Management of Bacterial Meningitis Allan R. Tunkel, 1 Barry J. Hartman, 2 Sheldon L. Kaplan, 3 Bruce A. Kaufman, 4 Karen L. Roos, 5 W. Michael Scheld, 6 and
Medicine - Dr. Hawar - Lecture 5 - CNS Infections I
 Medicine - Dr. Hawar - Lecture 5 - CNS Infections I Infections of the nervous system can be caused by viruses, bacteria, fungi or protozoa. They may affect the lining of the brain, CSF, brain parenchyma,
Medicine - Dr. Hawar - Lecture 5 - CNS Infections I Infections of the nervous system can be caused by viruses, bacteria, fungi or protozoa. They may affect the lining of the brain, CSF, brain parenchyma,
Meningitis is an inflammation of the leptomeninges. Predictors of Unfavorable Outcome in Meningitis Patients
 Original Article Nepal Journal of Neuroscience1:10-16, 2010 Niraj Bam, MBBS Department of Internal Medicine Jagadish Prasad Agrawal, MD, MHPE Department of Internal Medicine Bharat Mani Pokhrel, Ph.D Department
Original Article Nepal Journal of Neuroscience1:10-16, 2010 Niraj Bam, MBBS Department of Internal Medicine Jagadish Prasad Agrawal, MD, MHPE Department of Internal Medicine Bharat Mani Pokhrel, Ph.D Department
Bacterial meningitis in adults: Host and pathogen factors, treatment and outcome Heckenberg, S.G.B.
 UvA-DARE (Digital Academic Repository) Bacterial meningitis in adults: Host and pathogen factors, treatment and outcome Heckenberg, S.G.B. Link to publication Citation for published version (APA): Heckenberg,
UvA-DARE (Digital Academic Repository) Bacterial meningitis in adults: Host and pathogen factors, treatment and outcome Heckenberg, S.G.B. Link to publication Citation for published version (APA): Heckenberg,
Symptoms of meningism and raised numbers of cells in the CSF with a sterile bacterial culture.
 Table 1. Definitions. Meningism Meningitis Sepsis Severe sepsis Septic shock Meningococcal sepsis Invasive meningococcal disease (IMD) Encephalitis Meningoencephalitis Aseptic Meningitis Symptoms associated
Table 1. Definitions. Meningism Meningitis Sepsis Severe sepsis Septic shock Meningococcal sepsis Invasive meningococcal disease (IMD) Encephalitis Meningoencephalitis Aseptic Meningitis Symptoms associated
Outline of Presentation 29/01/2013. Brain Abscess and Spinal Abscess Pathophysiology Manifestations Treatment Nursing Care
 CNA Certification Exam Tracy Snell RN Outline of Presentation Definitions Meningitis Encephalitis Brain Abscess Spinal Abscess Pathophysiology, Manifestations, Treatment and Nursing Care Meningitis Encephalitis
CNA Certification Exam Tracy Snell RN Outline of Presentation Definitions Meningitis Encephalitis Brain Abscess Spinal Abscess Pathophysiology, Manifestations, Treatment and Nursing Care Meningitis Encephalitis
ID Emergencies. BUMC-P Internal Medicine Edwin Yu
 ID Emergencies BUMC-P Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
ID Emergencies BUMC-P Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
Bacterial meningitis
 Bacterial meningitis Is an acute purulent infection in the subarachnoid space that is associated with inflammation reaction in the brain and cerebral blood vessels that causes decreased conciuosness, seizure,
Bacterial meningitis Is an acute purulent infection in the subarachnoid space that is associated with inflammation reaction in the brain and cerebral blood vessels that causes decreased conciuosness, seizure,
Dr Paul Holmes Guy s and St Thomas NHS Foundation Trust, London
 Dr Paul Holmes Guy s and St Thomas NHS Foundation Trust, London HIV and Lumbar punctures in 2018 Paul Holmes Consultant Neurologist Guy s and St Thomas Hospitals I have no competing interests Summary of
Dr Paul Holmes Guy s and St Thomas NHS Foundation Trust, London HIV and Lumbar punctures in 2018 Paul Holmes Consultant Neurologist Guy s and St Thomas Hospitals I have no competing interests Summary of
ID Emergencies. BGSMC Internal Medicine Edwin Yu
 ID Emergencies BGSMC Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
ID Emergencies BGSMC Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION?
 RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION? MR. Salehi Omrani MD¹, MR. Edraki MD 2, M. Alizadeh MD 3 Abstract: Objective Febrile convulsion is the most common
RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION? MR. Salehi Omrani MD¹, MR. Edraki MD 2, M. Alizadeh MD 3 Abstract: Objective Febrile convulsion is the most common
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Management of meningitis and meningococcal disease in children and young people in primary and secondary care. 1.1 Short title
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Management of meningitis and meningococcal disease in children and young people in primary and secondary care. 1.1 Short title
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Aetiology of meningitis at the Moi Teaching and Referral Hospital, Eldoret, Kenya. D. K. Lagat, MBChB, Mmed(Moi)
 Aetiology of meningitis at the Moi Teaching and Referral Hospital, Eldoret, Kenya D. K. Lagat, MBChB, Mmed(Moi) Introduction Meningitis is common and important Syndromes of meningitis: Acute bacterial
Aetiology of meningitis at the Moi Teaching and Referral Hospital, Eldoret, Kenya D. K. Lagat, MBChB, Mmed(Moi) Introduction Meningitis is common and important Syndromes of meningitis: Acute bacterial
Role of Dexamethasone in Acute Bacterial Meningitis in adults
 Role of Dexamethasone in Acute Bacterial Meningitis in adults T. Ahsan,M. Shahid,T. Mahmood,R. Jabeen,U. Jehangir,M. Saleem,N. Ahmed,A. Shaheer ( Medical Unit 2, Department of Medicine, Jinnah Postgraduate
Role of Dexamethasone in Acute Bacterial Meningitis in adults T. Ahsan,M. Shahid,T. Mahmood,R. Jabeen,U. Jehangir,M. Saleem,N. Ahmed,A. Shaheer ( Medical Unit 2, Department of Medicine, Jinnah Postgraduate
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.166 Estimation of C-Reactive rotein
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.166 Estimation of C-Reactive rotein
SEMINAR ON ACUTE BACTERIAL MENINGITIS AND ANTI MICROBIALS IN NEURO SURGERY. Presented By : DR. ROHIT K GOEL
 SEMINAR ON ACUTE BACTERIAL MENINGITIS AND ANTI MICROBIALS IN NEURO SURGERY. Presented By : DR. ROHIT K GOEL ACUTE BACTERIAL MENINGITIS ABM is acute purulent infection in the subarachnoid space It is associated
SEMINAR ON ACUTE BACTERIAL MENINGITIS AND ANTI MICROBIALS IN NEURO SURGERY. Presented By : DR. ROHIT K GOEL ACUTE BACTERIAL MENINGITIS ABM is acute purulent infection in the subarachnoid space It is associated
I n Australia and the USA, where vaccination against
 391 ORIGINAL ARTICLE A population based study of the impact of corticosteroid therapy and delayed diagnosis on the outcome of childhood pneumococcal meningitis P B McIntyre, C R MacIntyre, R Gilmour, H
391 ORIGINAL ARTICLE A population based study of the impact of corticosteroid therapy and delayed diagnosis on the outcome of childhood pneumococcal meningitis P B McIntyre, C R MacIntyre, R Gilmour, H
New Technique uses to Evaluate Cerebrospinal Fluid Lactic Acid as an Aid Differential Diagnosis of Bacterial and Viral Meningitis
 New Technique uses to Evaluate Cerebrospinal Fluid Lactic Acid as an Aid Differential Diagnosis of Bacterial and Viral Meningitis Mohammed Kadum Al-Araji College of Pharmacy, University of Al-Mustansiriyah
New Technique uses to Evaluate Cerebrospinal Fluid Lactic Acid as an Aid Differential Diagnosis of Bacterial and Viral Meningitis Mohammed Kadum Al-Araji College of Pharmacy, University of Al-Mustansiriyah
ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST
 www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
Gram Negative Bacillary Brain Abscess: Clinical Features And Therapeutic Outcome
 ISPUB.COM The Internet Journal of Neurosurgery Volume 4 Number 2 Gram Negative Bacillary Brain Abscess: Clinical Features And Therapeutic Outcome F Huda, V Sharma, W Ali, M Rashid Citation F Huda, V Sharma,
ISPUB.COM The Internet Journal of Neurosurgery Volume 4 Number 2 Gram Negative Bacillary Brain Abscess: Clinical Features And Therapeutic Outcome F Huda, V Sharma, W Ali, M Rashid Citation F Huda, V Sharma,
Clinical features and prognostic factors in childhood pneumococcal meningitis
 J Microbiol Immunol Infect. 2008;41:48-53 Original Article Clinical features and prognostic factors in childhood pneumococcal meningitis Yen-Nan Chao, Nan-Chang Chiu, Fu-Yuan Huang Department of Pediatrics,
J Microbiol Immunol Infect. 2008;41:48-53 Original Article Clinical features and prognostic factors in childhood pneumococcal meningitis Yen-Nan Chao, Nan-Chang Chiu, Fu-Yuan Huang Department of Pediatrics,
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Bacterial meningitis (NICE guideline CG102) Proposed surveillance decision We propose to update the NICE guideline on bacterial meningitis.
Surveillance proposal consultation document 2018 surveillance of Bacterial meningitis (NICE guideline CG102) Proposed surveillance decision We propose to update the NICE guideline on bacterial meningitis.
Chapter 57: Nursing Management: Acute Intracranial Problems
 Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
The Child with Alterations in Cerebral Function
 The Child with Alterations in Cerebral Function Neurologic Assessment VS HR, BP, Respirations, Temperature LOC Orientation Pediatric Glasgow Coma Scale Eyes Pupillary response and movement, extraoccular
The Child with Alterations in Cerebral Function Neurologic Assessment VS HR, BP, Respirations, Temperature LOC Orientation Pediatric Glasgow Coma Scale Eyes Pupillary response and movement, extraoccular
UK Meningitis Study CRF
 History Date of onset of symptoms Route of admission A and E GP Other Date of admission to hospital* / / Time of admission (24 hour clock) : *record time and date of admission to A and E if admitted ia
History Date of onset of symptoms Route of admission A and E GP Other Date of admission to hospital* / / Time of admission (24 hour clock) : *record time and date of admission to A and E if admitted ia
Cryptococcal Meningitis
 Cryptococcal Meningitis Dr N Thumbiran Infectious Diseases Department UKZN Index patient 27 year old female Presented to King Edward Hospital on 17/07/2005 with: Severe headaches Vomiting Photophobia X
Cryptococcal Meningitis Dr N Thumbiran Infectious Diseases Department UKZN Index patient 27 year old female Presented to King Edward Hospital on 17/07/2005 with: Severe headaches Vomiting Photophobia X
Menigitidis. Dr Rodney Itaki Lecturer Anatomical Pathology Discipline
 Menigitidis Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea Division of Pathology School of Medicine & Health Sciences Review Normal Microanatomy Image Ref: www.histology-world.com
Menigitidis Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea Division of Pathology School of Medicine & Health Sciences Review Normal Microanatomy Image Ref: www.histology-world.com
MANAGEMENT OF SUSPECTED VIRAL ENCEPHALITIS IN CHILDREN
 MANAGEMENT OF SUSPECTED VIRAL ENCEPHALITIS IN CHILDREN OVERVIEW 1980s: dramatically improved by aciclovir HSV encephalitis in adults Delays treatment(> 48h after hospital admission): associated with a
MANAGEMENT OF SUSPECTED VIRAL ENCEPHALITIS IN CHILDREN OVERVIEW 1980s: dramatically improved by aciclovir HSV encephalitis in adults Delays treatment(> 48h after hospital admission): associated with a
Alberta Health and Wellness Public Health Notifiable Disease Management Guidelines August Pneumococcal Disease, Invasive (IPD)
 August 2011 Pneumococcal Disease, Invasive (IPD) Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) Case Definition August
August 2011 Pneumococcal Disease, Invasive (IPD) Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) Case Definition August
NICE guideline Draft for consultation, October 2009
 Bacterial meningitis and meningococcal septicaemia: management of bacterial meningitis and meningococcal septicaemia in children and young people younger than 16 years in primary and secondary care NICE
Bacterial meningitis and meningococcal septicaemia: management of bacterial meningitis and meningococcal septicaemia in children and young people younger than 16 years in primary and secondary care NICE
Scottish Surveillance of Healthcare Associated Infection Programme (SSHAIP) Health Protection Scotland (HPS) SSI Surveillance Protocol 7th Edition
 1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
Pneumococcal Meningitis Meningitis is an inflammation of the lining around the brain and spinal cord. Most severe cases
 Pneumococcal Meningitis Meningitis is an inflammation of the lining around the brain and spinal cord. Most severe cases are caused by bacteria. Pneumococcal bacteria (Streptococcus pneumoniae) are the
Pneumococcal Meningitis Meningitis is an inflammation of the lining around the brain and spinal cord. Most severe cases are caused by bacteria. Pneumococcal bacteria (Streptococcus pneumoniae) are the
AMSER Case of the Month July 2018 Complicated Headache with Fever
 AMSER Case of the Month July 2018 Complicated Headache with Fever Benjamin Park, MS IV Dr. Karen Xie Department of Radiology University of Illinois College of Medicine at Chicago Patient Presentation CC:
AMSER Case of the Month July 2018 Complicated Headache with Fever Benjamin Park, MS IV Dr. Karen Xie Department of Radiology University of Illinois College of Medicine at Chicago Patient Presentation CC:
Acute neurology. CME Acute Medicine. Headache. Intracranial haemorrhage
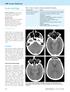 Acute neurology Table 1. Causes to consider in emergency presentation of headache. Headache type Causes Susan E Tomlinson BMed FRACP(Australia), Clinical Research Fellow, Department of Molecular Neuroscience,
Acute neurology Table 1. Causes to consider in emergency presentation of headache. Headache type Causes Susan E Tomlinson BMed FRACP(Australia), Clinical Research Fellow, Department of Molecular Neuroscience,
Dexamethasone for adult communityacquired bacterial meningitis: 20 years of experience in daily practice
 Dexamethasone for adult communityacquired bacterial meningitis: 20 years of experience in daily practice Vjerislav Peterković, Vladimir Trkulja, Marko Kutleša, Vladimir Krajinović & Dragan Lepur Journal
Dexamethasone for adult communityacquired bacterial meningitis: 20 years of experience in daily practice Vjerislav Peterković, Vladimir Trkulja, Marko Kutleša, Vladimir Krajinović & Dragan Lepur Journal
Meningitis. A fact sheet for patients and carers
 A fact sheet for patients and carers Meningitis This fact sheet provides information on meningitis. Our fact sheets are designed as general introductions to each subject and are intended to be concise.
A fact sheet for patients and carers Meningitis This fact sheet provides information on meningitis. Our fact sheets are designed as general introductions to each subject and are intended to be concise.
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Outcome of Severe Malaria in Endemic Zone - Study From a District Hospital of Bangladesh
 Dr. Md. AMIR HOSSAIN Department of Medicine Rangamati General Hospital Deputed to BSMMU, Dhaka. Outcome of Severe Malaria in Endemic Zone - Study From a District Hospital of Bangladesh 1 INTRODUCTION In
Dr. Md. AMIR HOSSAIN Department of Medicine Rangamati General Hospital Deputed to BSMMU, Dhaka. Outcome of Severe Malaria in Endemic Zone - Study From a District Hospital of Bangladesh 1 INTRODUCTION In
An Epidemiological Study of Meningitis in a Tertiary Care Centre and Role of Serum and CSF Creatine Kinase and Lactate Dehydrogenase in Its Diagnosis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.17 March. (2018), PP 26-30 www.iosrjournals.org An Epidemiological Study of Meningitis
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.17 March. (2018), PP 26-30 www.iosrjournals.org An Epidemiological Study of Meningitis
CNS Infections. GBS Streptococcus agalactiae. Meningitis - Neonate
 CNS Infections GBS Streptococcus agalactiae Bacterial meningitis - Pathophysiology - general Specific organisms - Age Hosts Treatment/Prevention Distinguish from viral disease Common commensal flora childbearing
CNS Infections GBS Streptococcus agalactiae Bacterial meningitis - Pathophysiology - general Specific organisms - Age Hosts Treatment/Prevention Distinguish from viral disease Common commensal flora childbearing
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Diagnostic Accuracy of Kernig s Sign, Brudzinski s Sign, and Nuchal Rigidity in Adults with Suspected Meningitis
 MAJOR ARTICLE The Diagnostic Accuracy of Kernig s Sign, Brudzinski s Sign, and Nuchal Rigidity in Adults with Suspected Meningitis Karen E. Thomas, 1 Rodrigo Hasbun, 1 James Jekel, 2 and Vincent J. Quagliarello
MAJOR ARTICLE The Diagnostic Accuracy of Kernig s Sign, Brudzinski s Sign, and Nuchal Rigidity in Adults with Suspected Meningitis Karen E. Thomas, 1 Rodrigo Hasbun, 1 James Jekel, 2 and Vincent J. Quagliarello
KAP conference 19 th March 2008: Dr Mohamed Hussein Jin.
 SENSITIVITY PATTERNS, SEROTYPES OF CRYPTOCOCCUS NEOFORMANS AND DIAGNOSTIC VALUE OF INDIA INK IN PATIENTS WITH CRYPTOCOCCAL MENINGITIS AT KENYATTA NATIONAL HOSPITAL. KAP conference 19 th March 2008: Dr
SENSITIVITY PATTERNS, SEROTYPES OF CRYPTOCOCCUS NEOFORMANS AND DIAGNOSTIC VALUE OF INDIA INK IN PATIENTS WITH CRYPTOCOCCAL MENINGITIS AT KENYATTA NATIONAL HOSPITAL. KAP conference 19 th March 2008: Dr
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
Subarachnoid Hemorrhage (SAH) Disclosures/Relationships. Click to edit Master title style. Click to edit Master title style.
 Subarachnoid Hemorrhage (SAH) William J. Jones, M.D. Assistant Professor of Neurology Co-Director, UCH Stroke Program Click to edit Master title style Disclosures/Relationships No conflicts of interest
Subarachnoid Hemorrhage (SAH) William J. Jones, M.D. Assistant Professor of Neurology Co-Director, UCH Stroke Program Click to edit Master title style Disclosures/Relationships No conflicts of interest
CNS INFECTIONS MENINGITIS
 CNS INFECTIONS MENINGITIS Learning Objectives: 1. Describe patient risk factors,signs and symptoms that may indicate meningitis 2. Identify tests and significant laboratory values used to diagnose meningitis
CNS INFECTIONS MENINGITIS Learning Objectives: 1. Describe patient risk factors,signs and symptoms that may indicate meningitis 2. Identify tests and significant laboratory values used to diagnose meningitis
Comparison of clinical and CSF profiles in 62 Adults with tuberculous and pyogenic meningitis
 International Journal of Research in Medical Sciences Kumar M et al. Int J Res Med Sci. 2017 May;5(5):2168-2172 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171863
International Journal of Research in Medical Sciences Kumar M et al. Int J Res Med Sci. 2017 May;5(5):2168-2172 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171863
Steroid Therapy for Bacterial Meningitis
 685 REVIEW ARTICLE Steroid Therapy for Bacterial Meningitis Urs B. Schaad, Sheldon L. Kaplan, and George H. McCracken, Jr. Front the Departments of Pediatrics, University of Basel, Basel, Switzerland;
685 REVIEW ARTICLE Steroid Therapy for Bacterial Meningitis Urs B. Schaad, Sheldon L. Kaplan, and George H. McCracken, Jr. Front the Departments of Pediatrics, University of Basel, Basel, Switzerland;
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
A cross sectional study of prevalance of tuberculous meningitis in Rohilkhand hospital in children
 Original article A cross sectional study of prevalance of tuberculous meningitis in Rohilkhand hospital in children Sumit Sachan, Ravi Singh Chauhan, Ajay Kumar Dept of Pediatrics, Rohilkhand Medical College
Original article A cross sectional study of prevalance of tuberculous meningitis in Rohilkhand hospital in children Sumit Sachan, Ravi Singh Chauhan, Ajay Kumar Dept of Pediatrics, Rohilkhand Medical College
Subdural Empyema: A Case Report from Southern Zambia and a Review of the Literature
 CASE REPORT Subdural Empyema: A Case Report from Southern Zambia and a Review of the Literature G Musa, A Gots Department of Surgery, Livingstone Central Hospital, P. O. Box 60091, Livingstone, Zambia
CASE REPORT Subdural Empyema: A Case Report from Southern Zambia and a Review of the Literature G Musa, A Gots Department of Surgery, Livingstone Central Hospital, P. O. Box 60091, Livingstone, Zambia
Profile of Cerebrospinal Fluid Analysis in Acute Central Nervous System Infections
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/121 Profile of Cerebrospinal Fluid Analysis in Acute Central Nervous System Infections K Vasanthan 1, Yeldho Verghese
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/121 Profile of Cerebrospinal Fluid Analysis in Acute Central Nervous System Infections K Vasanthan 1, Yeldho Verghese
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Bacterial Meningitis in Aging Adults
 AGING AND INFECTIOUS DISEASES Thomas T. Yoshikawa, Section Editor INVITED ARTICLE Bacterial Meningitis in Aging Adults Chester Choi Departments of Medicine, St. Mary Medical Center, Long Beach, and the
AGING AND INFECTIOUS DISEASES Thomas T. Yoshikawa, Section Editor INVITED ARTICLE Bacterial Meningitis in Aging Adults Chester Choi Departments of Medicine, St. Mary Medical Center, Long Beach, and the
Acute febrile encephalopathy and its outcome among children in a tertiary care hospital
 International Journal of Contemporary Pediatrics Deepthi CHA et al. Int J Contemp Pediatr. 2018 Mar;5(2):503-507 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Deepthi CHA et al. Int J Contemp Pediatr. 2018 Mar;5(2):503-507 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
Encephalitis following Purified Chick-Embryo Cell Anti-Rabies Vaccination
 CASE REPORT JIACM 2003; 4(3): 251-9 Encephalitis following Purified Chick-Embryo Cell Anti-Rabies Vaccination NS Neki*, Ashok Khurana**, Ashok Duggal*** Abstract A case of encephalitis following purified
CASE REPORT JIACM 2003; 4(3): 251-9 Encephalitis following Purified Chick-Embryo Cell Anti-Rabies Vaccination NS Neki*, Ashok Khurana**, Ashok Duggal*** Abstract A case of encephalitis following purified
11/9/2012. Group B Streptococcal Infections: Consensus and Controversies. Prevention of Early-Onset GBS Disease in the USA.
 Group B Streptococcal Infections: Consensus and Controversies Carol J. Baker, M.D. Professor of Pediatrics, Molecular Virology and Microbiology Executive Director, Center for Vaccine Awareness and Research
Group B Streptococcal Infections: Consensus and Controversies Carol J. Baker, M.D. Professor of Pediatrics, Molecular Virology and Microbiology Executive Director, Center for Vaccine Awareness and Research
Aciphin Ceftriaxone Sodium
 Aciphin Ceftriaxone Sodium Only for the use of Medical Professionals Description Aciphin is a bactericidal, long-acting, broad spectrum, parenteral cephalosporin preparation, active against a wide range
Aciphin Ceftriaxone Sodium Only for the use of Medical Professionals Description Aciphin is a bactericidal, long-acting, broad spectrum, parenteral cephalosporin preparation, active against a wide range
LUMBAR PUNCTURE. Multimedia Health Education
 LUMBAR PUNCTURE Disclaimer This film is an educational resource only and should not be used to make a decision on. All such decisions must be made in consultation with a physician or licensed healthcare
LUMBAR PUNCTURE Disclaimer This film is an educational resource only and should not be used to make a decision on. All such decisions must be made in consultation with a physician or licensed healthcare
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Scarborough M, Gordon SB, Whitty CJM, et al. Corticosteroids
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Scarborough M, Gordon SB, Whitty CJM, et al. Corticosteroids
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
CEREBROSPINAL FLUID [CSF]
![CEREBROSPINAL FLUID [CSF] CEREBROSPINAL FLUID [CSF]](/thumbs/89/100552494.jpg) CEREBROSPINAL FLUID [CSF] All question is compulsory Minimum passing mark is 15. 1. Full form of a) CSF = b) LDH = c) ADA = 2. If patient serum glucose level is 300 mg%,than expected csf glucose level
CEREBROSPINAL FLUID [CSF] All question is compulsory Minimum passing mark is 15. 1. Full form of a) CSF = b) LDH = c) ADA = 2. If patient serum glucose level is 300 mg%,than expected csf glucose level
VIRAL ENCEPHALITIS EASY TO MISS
 TAMORISH KOLE MBBS MRCS(EDIN) FRSM(UK) SENIOR CONSULTANT & HEAD, EMERGENCY MEDICINE, MAX HEALTHCARE, NEW DELHI, INDIA ADJUNCT ASSISTANT PROFESSOR, EMERGENCY MEDICINE, GEORGE WASHINGTON UNIVERSITY, WASHINGTON
TAMORISH KOLE MBBS MRCS(EDIN) FRSM(UK) SENIOR CONSULTANT & HEAD, EMERGENCY MEDICINE, MAX HEALTHCARE, NEW DELHI, INDIA ADJUNCT ASSISTANT PROFESSOR, EMERGENCY MEDICINE, GEORGE WASHINGTON UNIVERSITY, WASHINGTON
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Haemophilus influenzae
 Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
Viral Meningitis. 2. Use the information on the Possible Diseases sheet to complete the other four columns in the chart.
 Disease Detectives Part 1: What is wrong with Mike? Yesterday, Mike Wright developed a severe headache, a high fever, and a stiff neck. Then, he became nauseated and began vomiting. He just wanted medicine
Disease Detectives Part 1: What is wrong with Mike? Yesterday, Mike Wright developed a severe headache, a high fever, and a stiff neck. Then, he became nauseated and began vomiting. He just wanted medicine
When the drugs don t work- a case of HSV encephalitis.
 When the drugs don t work- a case of HSV encephalitis. Nicky Price Consultant Virologist Public Health Wales 67 year old Caucasian Female Presenting complaint 2 day history of: Confusion Shivering Headache
When the drugs don t work- a case of HSV encephalitis. Nicky Price Consultant Virologist Public Health Wales 67 year old Caucasian Female Presenting complaint 2 day history of: Confusion Shivering Headache
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
40 Current Status and
 40 Current Status and Management of Community Acquired Meningitis Abstract: Community acquired meningitis is associated with high mortality and morbidity. Bacterial meningitis is often a medical emergency,
40 Current Status and Management of Community Acquired Meningitis Abstract: Community acquired meningitis is associated with high mortality and morbidity. Bacterial meningitis is often a medical emergency,
Acute bacterial meningitis in Qatar ABSTRACT
 Acute bacterial meningitis in Qatar Mahmoud F. Elsaid, MBBCH, CABP, Amina A. Flamerzi, MBBCH, CABP, Mohammed S. Bessisso, DCH, MD, Sittana S. Elshafie, MSc, FRCP (Path). ABSTRACT Objectives: To study the
Acute bacterial meningitis in Qatar Mahmoud F. Elsaid, MBBCH, CABP, Amina A. Flamerzi, MBBCH, CABP, Mohammed S. Bessisso, DCH, MD, Sittana S. Elshafie, MSc, FRCP (Path). ABSTRACT Objectives: To study the
Challenges in Management of Cryptococcal Meningitis. Yunus Moosa Department of ID NRMSM Durban
 Challenges in Management of Cryptococcal Meningitis Yunus Moosa Department of ID NRMSM Durban Overview Epidemiology Pathogenesis Clinical presentation Diagnosis Prognostic factors Antifungal Treatment
Challenges in Management of Cryptococcal Meningitis Yunus Moosa Department of ID NRMSM Durban Overview Epidemiology Pathogenesis Clinical presentation Diagnosis Prognostic factors Antifungal Treatment
Bacterial Meningitis Concerns in Collegiate Athletics.5 hr. CEU
 Bacterial Meningitis Concerns in Collegiate Athletics.5 hr. CEU This unit is designed to increase your understanding of a highly dangerous infection, and help you protect your student athletes from its
Bacterial Meningitis Concerns in Collegiate Athletics.5 hr. CEU This unit is designed to increase your understanding of a highly dangerous infection, and help you protect your student athletes from its
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
M E N I N G I T I S. Meningitis is inflammation of the meninges, which is the lining that covers the brain and spinal cord. Many things can cause it:
 M E N I N G I T I S Meningitis is inflammation of the meninges, which is the lining that covers the brain and spinal cord. Many things can cause it: Bacterial Viral Fungal Parasitic Non-infectious, thus
M E N I N G I T I S Meningitis is inflammation of the meninges, which is the lining that covers the brain and spinal cord. Many things can cause it: Bacterial Viral Fungal Parasitic Non-infectious, thus
IMPACT #: Local Inventory #: form 04. Age at admission: d. mo yr. Postal code:
 - Date of birth: birth: Date of admission: year month day year month day Age at admission: d mo yr Postal code: Ethnic code: Hospital: Gender: 1 = male 2 = female 1 = Impact 2 = Other local, specify: Code
- Date of birth: birth: Date of admission: year month day year month day Age at admission: d mo yr Postal code: Ethnic code: Hospital: Gender: 1 = male 2 = female 1 = Impact 2 = Other local, specify: Code
Cerebral vasculitis complicating postoperative meningitis: the role of steroids revisited
 Published 29 October 2012, doi:10.4414/smw.2012.13697 Cite this as: Cerebral vasculitis complicating postoperative meningitis: the role of steroids revisited Katharine E. A. Darling a, Julien Niederhauser
Published 29 October 2012, doi:10.4414/smw.2012.13697 Cite this as: Cerebral vasculitis complicating postoperative meningitis: the role of steroids revisited Katharine E. A. Darling a, Julien Niederhauser
Bacterial meningitis in adults: Host and pathogen factors, treatment and outcome Heckenberg, S.G.B.
 UvA-DARE (Digital Academic Repository) Bacterial meningitis in adults: Host and pathogen factors, treatment and outcome Heckenberg, S.G.B. Link to publication Citation for published version (APA): Heckenberg,
UvA-DARE (Digital Academic Repository) Bacterial meningitis in adults: Host and pathogen factors, treatment and outcome Heckenberg, S.G.B. Link to publication Citation for published version (APA): Heckenberg,
FEBRILE SEIZURES. IAP UG Teaching slides
 FEBRILE SEIZURES 1 DEFINITION Febrile seizures are seizures that occur between the age of 6 and 60 months with a temperature of 38 C or higher, that are not the result of central nervous system infection
FEBRILE SEIZURES 1 DEFINITION Febrile seizures are seizures that occur between the age of 6 and 60 months with a temperature of 38 C or higher, that are not the result of central nervous system infection
