Suboccipital Surgery for Acoustic Neuroma
|
|
|
- Homer Lewis Nichols
- 6 years ago
- Views:
Transcription
1 Suboccipital Surgery for Acoustic Neuroma Overview A suboccipital craniotomy is a surgery performed to remove an acoustic neuroma growing from the nerve responsible for balance and hearing. During surgery, a section of the skull is removed behind the ear to access the tumor and nerves. Acoustic neuromas cause hearing loss, ringing in the ears, and dizziness. The goals of surgery are: first, the maintenance of facial nerve function; second, the preservation of socially useful hearing in the affected ear; and third, tumor removal. What is suboccipital acoustic neuroma surgery? A craniotomy is a bony opening that is cut into the skull. The cut section of skull, called a bone flap, is removed to allow access to the brain underneath. After the tumor is removed, the bone flap is placed back in its original position and secured to the skull with titanium plates and screws. An acoustic neuroma is approached by one of three different craniotomies: suboccipital, translabyrinthine, and middle fossa. The choice of a particular craniotomy depends on the tumor size, tumor position, and hearing status. The suboccipital craniotomy (also called retrosigmoid) is the most versatile approach. It involves removing a portion of the occipital bone behind the ear to remove the tumor (Fig. 1). Who is a candidate? You may be a candidate for suboccipital acoustic neuroma surgery if you have: A medium or large acoustic neuroma that is causing symptoms, especially balance problems caused by brainstem compression Serviceable hearing in the affected ear Neurofibromatosis type 2 (NF-2) Who performs the surgery? A neurosurgeon or neuro-otologist can remove acoustic neuromas. The suboccipital approach is performed by a neurosurgeon. Because each patient and each acoustic neuroma is unique, it is important to seek treatment at a center that offers the full range of options, including surgery, radiation, and hearing rehabilitation. Preventing or treating deafness in both ears for people with NF-2 Figure 1. The suboccipital approach involves removing a portion of the bone behind the ear. The cerebellum is gently held back to remove the acoustic neuroma. requires a team approach. Studies show that tumor size and the surgeon's experience are the most significant factors influencing facial nerve function and hearing outcome after removal [1]. What happens before surgery? You will have an office visit with a neurosurgeon, otologic surgeon, and an audiologist before surgery. An audiologist will perform a hearing test and a presurgical assessment of cranial nerve function. During the office visit, the surgeon will explain the procedure, its risks and benefits, and answer any questions. Next, you will sign consent forms and complete paperwork to inform the surgeon about your medical history (i.e., allergies, medicines, vitamins, bleeding history, anesthesia reactions, prior surgeries). Discuss all medications (prescription, over-the-counter, and herbal supplements) you are taking with your healthcare provider. Some medications will need to be continued or stopped the day of surgery. You will be scheduled for presurgical tests (e.g., a blood test, electrocardiogram, chest X-ray, and CT scan) several days before surgery. > 1
2 Stop taking all non-steroidal anti-inflammatory medicines (Naprosyn, Advil, Motrin, Nuprin, Aleve) and blood thinners (coumadin, Plavix, aspirin) 1 week before surgery. Additionally, stop smoking and chewing tobacco 1 week before and 2 weeks after surgery, as these activities can cause bleeding problems. Wash your hair with Hibiclens (chlorhexidine) antiseptic soap for 3 consecutive days prior to surgery. No food or drink is permitted past midnight the night before surgery. Morning of surgery Shower using antibacterial soap. Dress in freshly washed, loose-fitting clothing. Wear flat-heeled shoes with closed backs. If you have instructions to take regular medication the morning of surgery, do so with small sips of water. Remove make-up, hairpins, contacts, body piercings, nail polish, etc. Leave all valuables and jewelry at home (including wedding bands). Bring a list of medications (prescriptions, overthe-counter, and herbal supplements) with dosages and the times of day usually taken. Bring a list of allergies to medication or foods. Arrive at the hospital 2 hours before your scheduled surgery time to complete the necessary paperwork and pre-procedure work-ups. You will meet with a nurse who will ask your name, date of birth, and what procedure you are having. The nurse will explain the preoperative process and discuss any questions you may have. An anesthesiologist will talk with you to explain the effects of anesthesia and its risks. An intravenous (IV) line will be placed in your arm before transport to the operating room. Figure 2. A high-arching skin incision is made behind the ear (dashed line) that crosses the occipital nerves at the end branches. This incision also avoids deep dissection of the neck muscles and is less likely to cause chronic postoperative headache compared to a straight incision. What happens during surgery? There are 6 steps to the procedure, which generally takes 4-6 hours, depending on the tumor size. Step 1: prepare the patient You will lie on your back on the operative table and be given anesthesia. Once you are asleep, your head will be placed in a 3-pin skull-fixation device, which attaches to the table and holds your head in position during surgery. The hair near the incision area will be shaved and the scalp prepped with an antiseptic. The audiologist will attach electrodes to your face and ear to monitor the facial nerve, hearing, and brainstem functions during surgery. Step 2: make a skin incision The lesser and greater occipital nerves innervate the skin on the back of the scalp. These nerves can be cut, stretched or trapped in scar tissue from the incision. Chronic headache and occipital neuralgia (electric-shock pain) may be related to damage of these nerves. A high-arching skin incision crosses the nerves at their end branches and is less likely to cause damage (Fig. 2). The skin and muscles are lifted off the bone and folded back. Figure 3. A 1.5 inch-wide craniotomy is made in the occipital bone and the bone flap is removed. The cerebellum is gently held back to expose a small tumor and its attachments to the nerve. > 2
3 Step 3: perform a craniotomy A 1.5 inch-wide craniotomy is made in the occipital bone with a drill. The bone flap is removed to expose the protective covering of the brain called the dura. The dura is opened and folded back to expose the brain. Retractors are used to gently hold back the cerebellum, allowing the surgeon to see the acoustic neuroma and the nerves (Fig. 3). Step 4: debulk the tumor Depending on the size, acoustic neuromas can be attached to the facial nerve, trigeminal nerve, brainstem, and blood vessels. If the tumor is large, its size must be reduced so that the surgeon has enough room to see its attachments to nerves. An incision is made in the tumor capsule and the center is hollowed out (debulked). A drill is used to open the bony internal auditory canal to expose the origin of the tumor (Fig. 4). Step 5: remove the tumor The tumor origin at the vestibular nerve is cut, and attachments to the facial nerve are carefully dissected. Damage to the facial nerve may result in facial weakness or paralysis. Every effort is made to remove the tumor without damaging hearing, the facial nerve, and vital brainstem functions. Throughout tumor removal, an evoked potential monitoring probe is used to stimulate and monitor the nerves and brainstem. A decrease in nerve waveform signals the surgeon to stop dissecting. In some cases it may be best to leave remnants of tumor capsule attached to critical structures (Fig. 5 and 6). This is called a near-total removal. Because these tumors grow slowly, the risk of regrowth is far less than the risk of damaging the nerves. Step 6: close the craniotomy After the tumor is removed, the internal auditory canal is sealed with bone wax, and a small piece of muscle is glued over the opening. This prevents cerebrospinal fluid (CSF) from leaking into the middle ear. The dura is closed in watertight fashion and biologic glue is applied to prevent CSF leakage. The bone flap is replaced and secured with titanium plates and screws. The muscles and skin incisions are then rejoined and sutured together. Figure 4. A drill is used to open the internal auditory canal (IAC) to expose the tumor origin. Figure 5. In large tumors, the bulk of the tumor is hollowed out and cut away. The tumor capsule adherent to the delicate facial nerve is not removed. What happens after surgery? You will wake up in the recovery area called the post-anesthesia care unit (PACU). You may have a sore throat from the tube used during surgery to assist your breathing. After you awaken, you ll be moved to the neuroscience intensive care unit (NSICU) for overnight monitoring. Your blood pressure, heart rate, and respiration will be monitored. You may experience nausea, unsteadiness, and headache after surgery. Medication can control these symptoms. When your condition stabilizes, you will be transferred to a regular room, where you will continue to be monitored and will begin to increase your activity level. Figure 6. In small tumors, a near-total or total removal may be accomplished. The amount of tumor removal is guided by evoked potential monitoring during dissection. >3
4 The length of the hospital stay varies but is usually 2 to 3 days. When you are released from the hospital, you will be given discharge instructions. Discharge instructions Discomfort 1. After surgery, headache and incision pain are managed with narcotic medication. Because narcotic pain pills are addictive, they are used for a limited period of 2 to 4 weeks. Their regular use may also cause constipation, so drink lots of water and eat high-fiber foods. Stool softeners (e.g., Colace, Docusate) and laxatives (e.g., Dulcolax, Senokot, Milk of Magnesia) can be bought without a prescription. Thereafter, pain is managed with acetaminophen (e.g., Tylenol). 2. Ask your surgeon before taking nonsteroidal anti-inflammatory drugs (NSAIDs) (e.g., ibuprofen, Advil, Motrin, Nuprin; naproxen sodium, Aleve). NSAIDs may cause bleeding and interfere with bone healing. Restrictions 1. Do not drive after surgery until you are cleared to do so by your surgeon and avoid sitting for long periods of time. 2. Do not lift anything heavier than 5 pounds (e.g., a 2-liter bottle of soda), including children. 3. Housework and yard work are limited until the first follow-up office visit. This includes gardening, mowing, vacuuming, ironing, and loading/unloading the dishwasher, washer, or dryer. 4. Do not drink alcohol or operate a vehicle while using pain medication. Activity 5. You may feel that you do not have your normal energy level for 1 to 2 weeks after surgery. Gradually return to your normal activities. Fatigue is common. 6. Walking is encouraged; start with short walks and gradually increase the distance. Wait to participate in other forms of exercise until discussed with your surgeon. 7. Gentle stretches for the neck may be advised. Bathing/Incision Care 8. You may shower and get your incision or sutures wet. Use mild baby shampoo with no harsh fragrances. Be careful not to let the water directly hit your incision. Gently clean any old dried blood from the incision area. 9. Do not submerge your head in a bath. 10. Inspect your incision daily and check for signs of infection, such as swelling, redness, yellow or green discharge, warm to the touch. Minimal swelling around your incision is expected. Face / Eye care Do not rub your eyes. Use eye drops 3 to 4 times a day in the affected eye. Inspect your eye daily for signs of redness, irritation, or blurring of vision. If any of these conditions occur, notify your surgeon. Eat slowly and avoid tough foods. You may find it helpful to chew and swallow on the opposite side of your mouth until facial weakness improves. When to Call Your Doctor A temperature that exceeds 101.5º F. An incision that shows signs of infection, such as redness, swelling, pain, or drainage. Increased headache with nausea or vomiting, along with increased swelling at the incision site. Leaking cerebrospinal fluid may accumulate under the skin incision. Drowsiness, balance problems, or rashes. Decreased alertness, increased drowsiness, weakness of arms or legs, increased headaches, vomiting, or severe neck pain that prevents lowering your chin toward the chest. Recovery and prevention Before you leave the hospital, appointments with the neurosurgeon will be scheduled 10 to 14 days after surgery to remove your sutures and check your recovery. Recovery time varies from 4 to 6 weeks, depending on the tumor size and your general health. Patients typically return to work in 6 weeks, provided their balance is recovering, but be sure to check with your surgeon. What are the risks? No surgery is without risk. General complications of any surgery include bleeding, infection, blood clots, and reactions to anesthesia. Specific complications related to a craniotomy may include stroke, seizures, venous sinus occlusion, swelling of the brain, and CSF leakage. Risks related to acoustic neuroma surgery may include: Facial weakness is the loss of muscle control on one side of the face caused by nerve swelling or damage; it may be temporary or permanent. Temporary facial paralysis or weakness is common after surgery and may persist for 6 to 12 months. Those with facial weakness will need to take extra care of their eye with artificial tears and lubricant until facial nerve function improves. Facial nerve function is directly related to the size of the tumor. The House-Brackmann Scale is used to evaluate facial nerve function before and after surgery (Fig. 7). Massage and facial exercises are recommended to improve facial nerve function [2]. It is possible > 4
5 for facial weakness to improve, e.g., Grade 4 to a Grade 2. A high-grade weakness may not recover completely. A weakness of Grade 4 to 6 may need facial surgery to protect the eye and improve one s appearance. Permanent facial paralysis (Grade 5 or 6) is less common, usually occurring with large tumors, and results in an inability to close the eye, loss of facial expression, and facial droop. If a patient still has facial paralysis 1 year after surgery, the chance of further recovery is reduced. Consultation with an ENT surgeon who specializes in facial reconstruction may be needed to restore facial tone and appearance at rest. Options include: Gold weight implant: places a small implant in the upper eyelid to improve eyelid closure. Lower eyelid tightening: pulls up a sagging lower eyelid. Brow lift: lifts sagging brows. Botulinum injection: reduces abnormal facial twitching (injection lasts 3 to 6 months). Temporalis muscle sling: borrows other muscles to increase facial movement. Static sling: uses materials to support sagging tissues. Nerve transfer: borrows other nerves to increase facial movement (facial-to-hypoglossal nerve anastomosis). This option is recommended as soon as there is no possibility of facial nerve recovery. After years of facial paralysis, the facial nerve may become scarred and unresponsive to reconstructive surgery. Eye problems may occur as the result of facial weakness or paralysis that prevents the eye from closing completely. This allows the eye to become dry and unprotected. Artificial tears, eye lubricants, protective glasses, bandage contact lenses, and taping the eye shut are all options to protect the cornea. Care by an eye specialist may be indicated. Call the doctor if you have signs of a corneal abrasion, which include blurred vision, redness, and a sensation of something in your eye that doesn t improve after applying eye drops. If prolonged facial nerve paralysis is expected, various procedures may be performed to protect the cornea and improve one's appearance. For example, to improve eyelid position and closure, acanthoplasty -- the bringing together of the tendons in the corners of the eye -- may be performed. To simulate blinking, a palpebral spring device may be inserted in the upper eyelid to provide a blink reflex synchronous with the other eye, or a silastic elastic prosthesis may be secured through and around the upper and lower eyelids. Alternatively, a gold weight may be implanted in the upper eyelid to enhance lid closure. House-Brackmann Facial Weakness Scale I: Normal symmetrical function in all areas. II: Slight weakness; complete eye closure with minimal effort; slight asymmetry of smile; synkinesis barely noticeable, contracture, or spasm absent. III: Obvious weakness, but not disfiguring; may not be able to lift eyebrow; complete eye closure and strong but asymmetrical mouth movement; obvious, but not disfiguring synkinesis, mass movement or spasm. IV: Obvious disfiguring weakness; inability to lift brow; incomplete eye closure and asymmetry of mouth; severe synkinesis, mass movement, spasm. V: Motion barely perceptible; incomplete eye closure, slight movement corner mouth; synkinesis, contracture, and spasm usually absent. VI: No movement, loss of tone, no synkinesis, contracture, or spasm. Figure 7. The House-Brackmann facial weakness scale. Grades I and II are considered socially acceptable facial function by most physicians, although some patients cope well with a Grade III. Figure 7. The House-Brackmann facial Exercises for Facial Weakness Use a mirror to do these exercises 2 to 3 times daily. Begin with 8 to 10 repetitions and gradually increase. 1. Raise eyebrows, wrinkling the forehead as in surprise or fright. 2. Draw the eyebrows together, as in frowning. 3. Close eyelids firmly, forming wrinkles radiating from the outer angles. 4. Widen the nostrils of your nose. 5. Draw the point of the nose downward, narrowing the nostrils. 6. Raise the skin of chin and protrude the lower lip, as in pouting. 7. Draw the angle of the mouth backward, as in grinning. 8. Move the angles of the mouth upward and outward, as in smiling. 9. Raise and protrude the upper lip. 10. Close the lips and pucker them. 11. Pull down the angles of your mouth with your fingers. 12. Suck in sides of mouth, puff out cheeks. (Do not let air escape from behind the lips.) 13. Protrude the lower jaw on each side. 14. Bite firmly on each side. 15. Depress the lower jaw against resistance. Hold hand firmly under chin and try to open your mouth. > 5
6 Hearing loss is the most common complication and may be permanent in the affected ear because the tumor is wrapped around the cochlear nerve. In small tumors it is possible to save hearing when removing the tumor. Larger tumors usually have already caused some hearing loss or deafness prior to surgery. Two to 3 months after surgery, a hearing test is performed to determine your degree of useful hearing (Fig. 8). An audiologist or speech therapist can help you learn tips for coping with one-sided hearing loss. Understanding speech in difficult listening situations may be helped with a CROS (contralateral routing of sound) aid. The CROS aid is an instrument that receives sound on the deaf side, amplifies it, and then routes it to the good hearing ear. A small aid is worn on each ear. Sound may also be conducted from the tumor side to hearing side via the bone using a BAHA implant (bone-anchored hearing aid). This device has gained popularity in habilitating single-sided deafness related to acoustic neuromas because of the excellent sound quality and the need for only one device, which is worn behind, not in, the ear. Balance problems are common and generally improve after surgery with head exercises, Pilates, or Tai Chi. Care should be taken when using stairs or escalators. Persistent balance or dizziness problems may need treatment with vestibular (balance) rehabilitation. Cerebrospinal fluid (CSF) leakage is the escape of CSF that flows around the brain. This usually takes the form of a squishy pocket of fluid around the incision. Contact the surgeon immediately if leakage is suspected. A pressure dressing may be applied over the incision to stop the leak. Sometimes a lumbar drain is inserted in the lower back to reduce CSF pressure and close off the leak. If the leak continues, surgical repair may be necessary. New closure techniques and use of biologic glue greatly reduces CSF leakage. Headache is common after acoustic neuroma surgery and usually subsides within several weeks. Persistent headache (>3 months) can occur after suboccipital craniotomy. The best way to prevent post-craniotomy headaches is to use a high-arching skin incision. Cutting of the nerve branches causes numbness of the scalp. Conversely, partial injury or entrapment of the nerves from instruments and muscle retraction can cause occipital neuralgia and headache pain. Typical postoperative headaches occur more than once daily (46%), last 1 to 4 hours in duration (43%), and are of moderate intensity (63%) [3]. Treatment with NSAIDs typically provides relief. For severe chronic headaches, nonnarcotic medications may be prescribed (e.g., Neurontin, Lyrica). Shooting headache pain that has a specific trigger point can be treated with steroid injections into the painful area. Gardner-Robertson Hearing Scale Grade PTA (db) SD (%) I: Good II: Serviceable III: Non-serviceable IV: Poor V: Deaf 0 0 PTA = pure tone average SD = speech discrimination score Figure 8. The Gardner-Robertson hearing scale. Grades I and II are considered "useful hearing" and can hear a phone conversation. Exercises for Dizziness & Balance Problems Exercises to be carried out for 15 minutes 2 times daily, increasing to 30 minutes. Dizziness is expected when first beginning the exercises. Eye Exercises (do each 20 times): Look up, then down. At first slowly, then quickly. Look from one side to the other. At first slowly, then quickly. Focus on your finger at arm s length. Move finger one foot closer and back again. Head Exercises (do each 20 times): With your eyes open, bend your head forward then backward. At first slowly, then quickly. Turn your head from one side to the other side. At first slowly, then quickly. As dizziness decreases, do these exercises with your eyes closed. Sitting (do each 20 times): While sitting, shrug your shoulders. Turn your shoulders to the right, then left. Bend forward, pick up an object from the ground, and sit up. Standing (do each 20 times): Change from sitting to standing and back again with your eyes open. Repeat with eyes closed. Throw a small rubber ball from hand to hand above eye level. Throw ball from hand to hand under one knee. Moving About (do each 10 times): Walk across the room with your eyes open, then eyes closed. Walk up and down a slope with your eyes open, then eyes closed. Walk up and down steps with your eyes open, then eyes closed. > 6
7 What are the results? Outcomes of surgery depend on the size and adherence of the tumor, the use of cranial nerve monitoring, and the skill of the surgical team. Removing the tumor will usually restore balance, facial function and sensation, eyelid function, and tear production. Hearing loss is usually permanent because the tumor is wrapped around the eighth cranial nerve (the nerve responsible for hearing). The medical literature reports vary, but overall, facial movement is preserved in 90% of patients, especially with small tumors, and useful hearing is preserved in 20 to 80% [4,5,6]. Delayed hearing loss may occur after surgery in 30 to 50% of patients who had useful hearing immediately after surgery. Partial-removal techniques have higher rates of hearing and facial function preservation; however, a recent long-term study revealed that subtotal resection had a three-fold higher rate of tumor regrowth and no long-term impact on facial nerve function or hearing [7]. Tumor recurrence is less than 5% after total surgical removal. Sources & links If you have more questions, please contact Mayfield Brain & Spine at or For information about the University of Cincinnati Neuroscience Institute s Brain Tumor Center, call Sources 1. Wiet RJ, et al. Long-term results of the first 500 cases of acoustic neuroma surgery. Otolaryngol Head Neck Surg 124:645-51, Ryzenman JM, Pensak ML, Tew JM Jr. Facial paralysis and surgical rehabilitation: a quality of life analysis in a cohort of 1,595 patients after acoustic neuroma surgery. Otol Neurotol 26:516-21, Ryzenman JM, Pensak ML, Tew JM Jr. Headache: a quality of life analysis in a cohort of 1,657 patients undergoing acoustic neuroma surgery, results from the acoustic neuroma association. Laryngoscope 115:703-11, Raftopoulos C, et al. Microsurgical results with large vestibular schwannomas with preservation of facial and cochlear nerve function as primary aim. Acta Neurochir 147: , Samii M, et al. Hearing Preservation after Complete Microsurgical Removal in Vestibular Schwannomas. Régis J, Roche P-H (eds): Modern Management of Acoustic Neuroma. Prog Neurol Surg 21: , Anaizi AN, DiNapoli VV, Pensak M, Theodosopoulos PV. Small Vestibular Schwannomas: Does Surgery Remain a Viable Treatment Option? J Neurol Surg B Skull Base 77(3):212-8, Monfared A, Corrales E, Theodosopoulos P, et al. Facial Nerve Outcome and Tumor Control Rate as a Function of Degree of Resection in Treatment of Large Acoustic Neuromas: Preliminary Report of the Acoustic Neuroma Subtotal Resection Study. Neurosurgery Nov 28. [Epub ahead of print] Links Acoustic Neuroma Association Vestibular Disorders Association Glossary BAHA (bone-anchored hearing aid): a hearing device used for conductive hearing loss. It transmits sound through the bone of the skull to the inner ear, bypassing the middle ear. cerebrospinal fluid (CSF): a clear fluid produced by the choroid plexus in the ventricles of the brain that bathes the brain and spinal cord, giving them support and buoyancy to protect from injury. craniotomy: the surgical opening of a portion of the skull, allowing access to the intracranial structures, and the replacement of the bone flap. CROS (contralateral routing of sound): a hearing device used with one-sided deafness. It receives sound on the deaf side, amplifies it, and carries it to the good ear. dura: the outer protective covering of the brain. facial nerve: the seventh cranial nerve, responsible for movement of the face. facial palsy: paralysis of the facial muscles on one side. facial synkinesis: involuntary movement of facial muscles that accompanies purposeful movement of some other set of muscles; e.g., facial synkinesis may cause the mouth to involuntarily grimace when the eyes are purposefully closed. occipital neuralgia: a persistent pain in the neck and back of the head that is caused by an injury or irritation of the greater or lesser occipital nerves. seizure: uncontrollable convulsion, spasm, or series of jerking movements of the face, trunk, arms, or legs. tinnitus: ringing or buzzing noise in the ear. vertigo: a feeling of spinning, whirling or turning. updated > reviewed by > Norberto Andaluz, MD, Mario Zuccarello, MD, Mayfield Clinic Mayfield Certified Health Info materials are written and developed by the Mayfield Clinic. We comply with the HONcode standard for trustworthy health information. This information is not intended to replace the medical advice of your health care provider. Mayfield Clinic > 7
Overview What is a craniotomy? Who performs the procedure? What happens before surgery? > 1
 Craniotomy Overview Craniotomy is a surgery to cut a bony opening in the A section of the skull, called a bone flap, is removed to access the brain underneath. A craniotomy may be small or large depending
Craniotomy Overview Craniotomy is a surgery to cut a bony opening in the A section of the skull, called a bone flap, is removed to access the brain underneath. A craniotomy may be small or large depending
Acoustic Neuroma (vestibular schwannoma)
 1 2 Acoustic Neuroma (vestibular schwannoma) Overview An acoustic neuroma is a tumor that grows from the nerves responsible for balance and hearing. These tumors grow from the sheath covering the vestibulocochlear
1 2 Acoustic Neuroma (vestibular schwannoma) Overview An acoustic neuroma is a tumor that grows from the nerves responsible for balance and hearing. These tumors grow from the sheath covering the vestibulocochlear
ACOUSTIC NEUROMAS. University of Florida ENT Clinic Patrick J. Antonelli, MD Matthew R. O Malley, MD
 ACOUSTIC NEUROMAS University of Florida ENT Clinic Patrick J. Antonelli, MD Matthew R. O Malley, MD Rev. 10.31.2011 ACOUSTIC TUMORS Acoustic tumors are non-malignant fibrous growths, originating from the
ACOUSTIC NEUROMAS University of Florida ENT Clinic Patrick J. Antonelli, MD Matthew R. O Malley, MD Rev. 10.31.2011 ACOUSTIC TUMORS Acoustic tumors are non-malignant fibrous growths, originating from the
Acoustic Neuroma (vestibular schwannoma) basic level
 Acoustic Neuroma (vestibular schwannoma) basic level Overview An acoustic neuroma is a tumor that grows from the nerves responsible for balance and hearing. More accurately called vestibular schwannoma,
Acoustic Neuroma (vestibular schwannoma) basic level Overview An acoustic neuroma is a tumor that grows from the nerves responsible for balance and hearing. More accurately called vestibular schwannoma,
The time required for surgery will vary depending upon the procedure recommended. The surgery may last 3 8 hours.
 PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
PROCEDURE Your surgeon has recommended the removal of a spine tumor. Lesions of the spine may occur in the neck region (cervical), mid-back region (thoracic), or low-back region (lumbar-sacral). There
While complications from surgery are uncommon some can be serious and may include:
 PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
Acoustic Neuroma (vestibular schwannoma)
 Acoustic Neuroma (vestibular schwannoma) Overview An acoustic neuroma is a tumor that grows from the nerves responsible for balance and hearing. These tumors grow from the sheath covering the vestibulocochlear
Acoustic Neuroma (vestibular schwannoma) Overview An acoustic neuroma is a tumor that grows from the nerves responsible for balance and hearing. These tumors grow from the sheath covering the vestibulocochlear
Shoulder Instability Latarjet Procedure
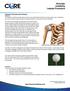 Explanation of Procedure and/or Diagnosis Anatomy The shoulder is a ball and socket joint and is the most mobile joint of the body. Its plays a major role in positioning your arm and hand in space. Because
Explanation of Procedure and/or Diagnosis Anatomy The shoulder is a ball and socket joint and is the most mobile joint of the body. Its plays a major role in positioning your arm and hand in space. Because
GEORGETOWN ORTHOPAEDIC SPINE SURGERY POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION)
 POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
POSTERIOR CERVICAL SURGERY (LAMINOPLASTY, LAMINECTOMY WITH FUSION) PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
You or your child has been scheduled for Tympanomastoidectomy and/or Ossicular Chain Reconstruction.
 Low Country ENT is happy you have chosen us to assist you and your family in obtaining your healthcare needs. The following packet is to help you further understand your future surgical procedure as well
Low Country ENT is happy you have chosen us to assist you and your family in obtaining your healthcare needs. The following packet is to help you further understand your future surgical procedure as well
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery
 Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Endoscopic Pituitary Surgery (transsphenoidal)
 Endoscopic Pituitary Surgery (transsphenoidal) Overview Endoscopic surgery is performed through the nose to remove tumors from the pituitary gland and skull base. In this minimally invasive surgery, the
Endoscopic Pituitary Surgery (transsphenoidal) Overview Endoscopic surgery is performed through the nose to remove tumors from the pituitary gland and skull base. In this minimally invasive surgery, the
ADULT SPINAL DEFORMITY SURGERY
 PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications can increase bleeding
POSTERIOR CERVICAL LAMINECTOMY AND FUSION
 PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
PROCEDURE A Posterior Cervical Laminectomy and Fusion surgical procedure is usually performed to treat spinal cord compression resulting from cervical canal narrowing. At times, it is also recommended
ANTERIOR CERVICAL DISCECTOMY AND FUSION
 PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
PROCEDURE An Anterior Cervical Discectomy is the surgical removal of a disc. The procedure is used when a disc protrusion or arthritic bone spur is placing pressure on a nerve and causing arm or neck pain.
Anterior Cervical Discectomy and Fusion (ACDF)
 Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Anterior Cervical Discectomy and Fusion (ACDF) What Is an ACDF? Anterior Cervical Discectomy and Fusion (ACDF) is a surgical procedure that involves decompressing spinal cord and nerves in the cervical
Spinal Cord Stimulation
 1 2 Spinal Cord Stimulation Overview Spinal cord stimulation uses low voltage stimulation to the spine to block the feeling of pain. A small device implanted in the body transmits an electrical current
1 2 Spinal Cord Stimulation Overview Spinal cord stimulation uses low voltage stimulation to the spine to block the feeling of pain. A small device implanted in the body transmits an electrical current
MIDDLE EAR SURGERY. For Better Health and Hearing
 MIDDLE EAR SURGERY For Better Health and Hearing Help for Ongoing Ear Problems Your doctor has found a problem with your middle ear. This is a part of the ear that you can t see. You may have taken medication,
MIDDLE EAR SURGERY For Better Health and Hearing Help for Ongoing Ear Problems Your doctor has found a problem with your middle ear. This is a part of the ear that you can t see. You may have taken medication,
ANTERIOR LUMBAR INTERBODY FUSION (ALIF)
 PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
PROCEDURE An Anterior Lumbar Interbody Fusion (ALIF) is a surgical procedure performed when there is disabling pain from a degenerated disc or nerve root compression. During the operation, your surgeon
Posterior Lumbar Discectomy
 1 2 Posterior Lumbar Discectomy Overview Posterior lumbar discectomy is a surgery to remove a herniated or degenerative disc in the lower spine. The incision is made posterior, through the back muscles,
1 2 Posterior Lumbar Discectomy Overview Posterior lumbar discectomy is a surgery to remove a herniated or degenerative disc in the lower spine. The incision is made posterior, through the back muscles,
Going home after breast surgery without drains
 Going home after breast surgery without drains Princess Margaret Information for patients and families Read this resource to learn: How to care for yourself when you go home What activities you can do
Going home after breast surgery without drains Princess Margaret Information for patients and families Read this resource to learn: How to care for yourself when you go home What activities you can do
Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri)
 1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
Patient s guide to surgery
 Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
POSTERIOR LATERAL FUSION LUMBAR
 PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
PROCEDURE A Posterior Lateral Fusion (PLF) is spine surgery performed to treat disabling back pain, leg pain, leg weakness or numbness, or spinal instability. During this procedure, your surgeon will remove
WHAT TO EXPECT FOLLOWING MASTECTOMY AND IMMEDIATE RECONSTRUCTION WITH TISSUE EXPANDERS OR IMPLANTS
 WHAT TO EXPECT FOLLOWING MASTECTOMY AND IMMEDIATE RECONSTRUCTION WITH TISSUE EXPANDERS OR IMPLANTS Before Your Surgery 1 week before your surgery, please stop taking the following medications: o NSAIDs
WHAT TO EXPECT FOLLOWING MASTECTOMY AND IMMEDIATE RECONSTRUCTION WITH TISSUE EXPANDERS OR IMPLANTS Before Your Surgery 1 week before your surgery, please stop taking the following medications: o NSAIDs
GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY Please
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING CERVICAL DISCECTOMY AND FUSION SURGERY Please
Home Care Instructions. Cervical Laminoplasty
 Home Care Instructions Cervical Laminoplasty You are recovering from a posterior cervical decompression in which your surgeon removed the pressure on your spinal nerves in an attempt to reduce pain and/or
Home Care Instructions Cervical Laminoplasty You are recovering from a posterior cervical decompression in which your surgeon removed the pressure on your spinal nerves in an attempt to reduce pain and/or
GEORGETOWN ORTHOPAEDIC SPINE SURGERY. Lumbar Decompression
 Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Minimally Invasive Discectomy/ Decompression
 Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
Minimally Invasive Discectomy/ Decompression What Is A Minimally Invasive Lumbar Discectomy? A lumbar discectomy is a surgical procedure that involves relieving the pressure placed on nerve roots and/or
CERVICAL STRAIN AND SPRAIN
 CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN (Whiplash)
 CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
Cerebral Bypass Surgery
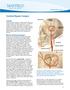 Cerebral Bypass Surgery Overview Cerebral bypass surgery is performed to restore, or revascularize, blood flow to the brain. A cerebral bypass is the brain's equivalent of a coronary bypass in the heart.
Cerebral Bypass Surgery Overview Cerebral bypass surgery is performed to restore, or revascularize, blood flow to the brain. A cerebral bypass is the brain's equivalent of a coronary bypass in the heart.
Pituitary Tumour Surgery. Remember to bring this handout to the hospital with you.
 Pituitary Tumour Surgery Remember to bring this handout to the hospital with you. 1 Pituitary Tumour Surgery Table of contents Page What is the pituitary gland?... 2 What is a pituitary tumour?... 3 Why
Pituitary Tumour Surgery Remember to bring this handout to the hospital with you. 1 Pituitary Tumour Surgery Table of contents Page What is the pituitary gland?... 2 What is a pituitary tumour?... 3 Why
HAVING SURGERY WITH DR. LUCAS
 HAVING SURGERY WITH DR. LUCAS Dr. Brennen Lucas 316-631-1600 x255 www.aoaortho.com You have been scheduled to have surgery by Dr. Lucas. The following information is provided so that you will know what
HAVING SURGERY WITH DR. LUCAS Dr. Brennen Lucas 316-631-1600 x255 www.aoaortho.com You have been scheduled to have surgery by Dr. Lucas. The following information is provided so that you will know what
Spinal Cord Stimulation
 Spinal Cord Stimulation Overview Spinal cord stimulation is a therapy that masks pain signals before they reach the brain. A small device, similar to a pacemaker, is implanted in the body to deliver electrical
Spinal Cord Stimulation Overview Spinal cord stimulation is a therapy that masks pain signals before they reach the brain. A small device, similar to a pacemaker, is implanted in the body to deliver electrical
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
Spine Surgery Discharge Instructions
 Spine Surgery Discharge Instructions Your sutures or staples need to stay in place for at least 10 days after surgery. To have them removed you can: Call your surgeon s office (the number is on your discharge
Spine Surgery Discharge Instructions Your sutures or staples need to stay in place for at least 10 days after surgery. To have them removed you can: Call your surgeon s office (the number is on your discharge
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read this
Functional rehab after breast reconstruction surgery A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read this
Cervical Spine Discharge Instructions
 Pain After surgery you may experience pain in the region of the incision. Some neck and arm pain as well as tingling or numbness may also be present. Initially it may be of greater intensity than pre-operatively,
Pain After surgery you may experience pain in the region of the incision. Some neck and arm pain as well as tingling or numbness may also be present. Initially it may be of greater intensity than pre-operatively,
Discharge Instructions What to Expect After Cervical Fusion
 Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 NASOLACRIMAL DUCT SURGERY (Post-Op
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 NASOLACRIMAL DUCT SURGERY (Post-Op
 Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Introduction Posterior cervical fusion is done through the back posterior of the neck. The surgery joins two or more neck vertebrae into one solid section of bone. The medical term for fusion is arthrodesis.
Mark J. Syms, M.D North 3 rd Street Suite 201 Phoenix, AZ (P) (F) BAHA / PONTO Device
 Mark J. Syms, M.D. 2627 North 3 rd Street Suite 201 Phoenix, AZ 85004 (P) 602.307.9919 (F) 602.307.5905 BAHA / PONTO Device POST OPERATIVE INSTRUCTIONS Please Read Before Surgery This information is to
Mark J. Syms, M.D. 2627 North 3 rd Street Suite 201 Phoenix, AZ 85004 (P) 602.307.9919 (F) 602.307.5905 BAHA / PONTO Device POST OPERATIVE INSTRUCTIONS Please Read Before Surgery This information is to
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion
 Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion Cervical Corpectomy is intended for the surgical correction and stabilization of the spine where vertebral bone removal is necessary.
Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion Cervical Corpectomy is intended for the surgical correction and stabilization of the spine where vertebral bone removal is necessary.
Ophthalmology Department. 2009, The Permanente Medical Group, Inc. All rights reserved, Ophthalmology Department.
 Glaucoma: Title of article Trabeculectomy is Ahmed positioned Valve here POST-SURGICAL SUB TITLE POSITIONED INSTRUCTIONS HERE These instructions are for patients recovering from one of the following eye
Glaucoma: Title of article Trabeculectomy is Ahmed positioned Valve here POST-SURGICAL SUB TITLE POSITIONED INSTRUCTIONS HERE These instructions are for patients recovering from one of the following eye
Neurosurgery: Neck Surgery
 Patient & Family Guide 2015 Neurosurgery: Neck Surgery www.nshealth.ca Neurosurgery: Neck Surgery Types of surgery Discectomy is the removal of part of the disc which is pressing on a nerve. The pressure
Patient & Family Guide 2015 Neurosurgery: Neck Surgery www.nshealth.ca Neurosurgery: Neck Surgery Types of surgery Discectomy is the removal of part of the disc which is pressing on a nerve. The pressure
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Discharge Instructions: What to Expect After Lumbar Fusion
 Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
Table of Contents. What is Spinal Fusion? Pre-Register for Surgery How Do I Prepare for Surgery?... 3
 www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
www.cpmc.org/learning Spinal Fusion Table of Contents What is Spinal Fusion?... 2 Pre-Register for Surgery... 2 How Do I Prepare for Surgery?... 3 What Can I Expect During My Hospital Stay?... 3 If You
Daniel Calva, M.D. PHONE: (305) FAX: (305) Post Operative Instructions Breast Augmentation Surgery
 PHONE: (305) 203-3938 FAX: (305) 602-5956 Post Operative Instructions Breast Augmentation Surgery The goal is to make your surgical experience and recovery as comfortable as possible. Please call us with
PHONE: (305) 203-3938 FAX: (305) 602-5956 Post Operative Instructions Breast Augmentation Surgery The goal is to make your surgical experience and recovery as comfortable as possible. Please call us with
Dr. Nuelle Knee Replacement: Discharge Care Instructions
 Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Your rotator cuff is made up of four small muscles arising from your shoulder
 The Rotator Cuff Your rotator cuff is made up of four small muscles arising from your shoulder blade. As these muscles travel from the shoulder blade towards your shoulder joint, they join together forming
The Rotator Cuff Your rotator cuff is made up of four small muscles arising from your shoulder blade. As these muscles travel from the shoulder blade towards your shoulder joint, they join together forming
Anterior Cervical Discectomy & Fusion
 1 2 Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck area of the spine. The incision is
1 2 Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck area of the spine. The incision is
Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide
 1 Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide Introduction The purpose of this guide is to provide you and your family with information regarding your medical
1 Cervical Artificial Disc Replacement Preoperative, Postoperative and Home Recovery Guide Introduction The purpose of this guide is to provide you and your family with information regarding your medical
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
Reverse Total Shoulder Replacement
 Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS
 PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS Medications: Narcotics: The orthopaedic office does not prescribe narcotics for pain prior to operations, with some exceptions. If you have pain that
PRE- AND POST-SURGERY INSTRUCTIONS FOR SPINE PATIENTS Medications: Narcotics: The orthopaedic office does not prescribe narcotics for pain prior to operations, with some exceptions. If you have pain that
CM01 Facelift. Copyright 2007 Page 1 of 6
 CM01 Facelift What is a facelift? A facelift is an operation to tighten and lift the soft tissues of your face and neck. Your surgeon will assess you and let you know if a facelift is suitable for you.
CM01 Facelift What is a facelift? A facelift is an operation to tighten and lift the soft tissues of your face and neck. Your surgeon will assess you and let you know if a facelift is suitable for you.
Author: Vancouver Island Neurosurgical Foundation. Reviewed: July 28/2016
 My Anterior Cervical Spine Surgery The Surgery Team has prepared this insert containing discharge information to help you and your family after surgery. It has information about what you can do after your
My Anterior Cervical Spine Surgery The Surgery Team has prepared this insert containing discharge information to help you and your family after surgery. It has information about what you can do after your
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction
 Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Jason Barry, M.D. Knee Arthroscopy with Anterior Cruciate Ligament (ACL) Reconstruction Arthroscopy (scope) is a minimally invasive surgical procedure orthopedic surgeons use to visualize, diagnose and
Robot Assisted Total Laparoscopic Hysterectomy
 Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Instructions for MACS LIFT Post- Operative
 Instructions for MACS LIFT Post- Operative INTRODUCTION The following instructions are based on experience with many MACS- Lift operations. They will answer practically every question that may arise regarding
Instructions for MACS LIFT Post- Operative INTRODUCTION The following instructions are based on experience with many MACS- Lift operations. They will answer practically every question that may arise regarding
Michael T. Brown, M.D., F.A.C.S. P. Kurt Bamberger, M.D., F.A.C.S. Amber D. Brown, PA-C (610) fax (610) BEFORE YOUR SURGERY
 BEFORE YOUR SURGERY Prior to your surgery, you will have a PRE-ADMISSION TESTING APPOINTMENT (PAT). Some PAT appointments require you to go to the hospital for an in-person appointment; the other option
BEFORE YOUR SURGERY Prior to your surgery, you will have a PRE-ADMISSION TESTING APPOINTMENT (PAT). Some PAT appointments require you to go to the hospital for an in-person appointment; the other option
Dr. Clark s Frequently Asked Questions
 Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery
 THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery Clearance: Prior to surgery you will need surgical clearance from your Primary Care Physician and/ or Cardiologist, if recommended.
THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery Clearance: Prior to surgery you will need surgical clearance from your Primary Care Physician and/ or Cardiologist, if recommended.
Spinal Fusion: Axial Lumbar Interbody Fusion (AxiaLIF)
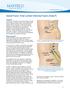 1 2 Spinal Fusion: Axial Lumbar Interbody Fusion (AxiaLIF) Overview AxiaLIF is a minimally invasive spinal fusion to treat disc problems in the low back. Fusion stabilizes the spine to stop the painful
1 2 Spinal Fusion: Axial Lumbar Interbody Fusion (AxiaLIF) Overview AxiaLIF is a minimally invasive spinal fusion to treat disc problems in the low back. Fusion stabilizes the spine to stop the painful
Pain Relief During Labor and Delivery
 Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Anterior Cervical Discectomy & Fusion
 Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck. An incision is made in the throat area
Anterior Cervical Discectomy & Fusion Overview Anterior cervical discectomy and fusion (ACDF) is a surgery to remove a herniated or degenerative disc in the neck. An incision is made in the throat area
MASTOID EXPLORATION (MASTOID SURGERY) AND MASTOIDECTOMY
 MASTOID EXPLORATION (MASTOID SURGERY) AND MASTOIDECTOMY This information leaflet is to support your decision with your Specialist. This leaflet will explain about the ear are and what surgery can be offered
MASTOID EXPLORATION (MASTOID SURGERY) AND MASTOIDECTOMY This information leaflet is to support your decision with your Specialist. This leaflet will explain about the ear are and what surgery can be offered
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
To Our Patients: Sincerely, Anjali B. Sheth, MD Micah Rothstein, MD
 To Our Patients: In anticipation of your glaucoma surgery, you may feel anxious and have many questions. We hope that the attached information will answer your questions and help to ease your worries.
To Our Patients: In anticipation of your glaucoma surgery, you may feel anxious and have many questions. We hope that the attached information will answer your questions and help to ease your worries.
Pre-Op. What to expect on your initial visit. Special instructions before surgery
 Pre-Op What to expect on your initial visit Thorough history and physical. Review of your existing labs, x- rays and other information. Ultrasound of your thyroid and neck if indicated. Fine needle aspiration
Pre-Op What to expect on your initial visit Thorough history and physical. Review of your existing labs, x- rays and other information. Ultrasound of your thyroid and neck if indicated. Fine needle aspiration
Minimally Invasive Endoscopic Resection of the Pituitary (MIERP) Patient Information
 Minimally Invasive Endoscopic Resection of the Pituitary (MIERP) Patient Information Introduction The pituitary gland is located at the base of the brain behind the sphenoid sinus and between the eyes.
Minimally Invasive Endoscopic Resection of the Pituitary (MIERP) Patient Information Introduction The pituitary gland is located at the base of the brain behind the sphenoid sinus and between the eyes.
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions
 Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Nasal Surgery. Types of Surgery. This handout explains different types of nasal surgery and what to expect.
 Nasal Surgery This handout explains different types of nasal surgery and what to expect. Types of Surgery Septoplasty is a surgery done to straighten the septum. The septum is made of bone and cartilage.
Nasal Surgery This handout explains different types of nasal surgery and what to expect. Types of Surgery Septoplasty is a surgery done to straighten the septum. The septum is made of bone and cartilage.
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Help Your Body Heal. Clinic Visits. After weight loss surgery
 UW MEDICINE PATIENT EDUCATION Follow-up After weight loss surgery This section of the Guide to Your Weight Loss Surgery explains clinic visits and medical and other concerns in the weeks after surgery.
UW MEDICINE PATIENT EDUCATION Follow-up After weight loss surgery This section of the Guide to Your Weight Loss Surgery explains clinic visits and medical and other concerns in the weeks after surgery.
Elbow Arthroscopy. Anatomy of the Elbow
 Elbow Arthroscopy Elbow arthroscopy is a minimally invasive surgical technique that allows Dr. Omid to evaluate and in some cases treat certain elbow conditions. During the procedure Dr. Omid will make
Elbow Arthroscopy Elbow arthroscopy is a minimally invasive surgical technique that allows Dr. Omid to evaluate and in some cases treat certain elbow conditions. During the procedure Dr. Omid will make
POST-OPERATIVE INSTRUCTIONS Knee Arthroscopy: Meniscus Repair Dr. Sostak visit for more detailed instructions
 POST-OPERATIVE INSTRUCTIONS Knee Arthroscopy: Meniscus Repair Dr. Sostak visit www.healthy-txt.com/drsostak for more detailed instructions PAIN MEDICATION: You will receive your pain medication prescription
POST-OPERATIVE INSTRUCTIONS Knee Arthroscopy: Meniscus Repair Dr. Sostak visit www.healthy-txt.com/drsostak for more detailed instructions PAIN MEDICATION: You will receive your pain medication prescription
Physiotherapy Advice: Post-operative advice following vestibular schwannoma / acoustic neuroma surgery
 Physiotherapy Advice: Post-operative advice following vestibular schwannoma / acoustic neuroma surgery Irving Building Physiotherapy 0161 206 5332 All Rights Reserved 2018. Document for issue as handout.
Physiotherapy Advice: Post-operative advice following vestibular schwannoma / acoustic neuroma surgery Irving Building Physiotherapy 0161 206 5332 All Rights Reserved 2018. Document for issue as handout.
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS
 TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
Total Knee Replacement: Your Guide to Preparation and Recovery
 Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Your ear consists of three parts that play a vital role in hearing-the external ear, middle ear, and inner ear.
 What is a Cochlear Implant? A cochlear implant is an electronic device that restores partial hearing to the deaf. It is surgically implanted in the inner ear and activated by a device worn outside the
What is a Cochlear Implant? A cochlear implant is an electronic device that restores partial hearing to the deaf. It is surgically implanted in the inner ear and activated by a device worn outside the
Shoulder Joint Replacement
 UW MEDICINE PATIENT EDUCATION Shoulder Joint Replacement How to prepare and what to expect This handout for UW Medicine patients explains how to prepare and what to expect when having shoulder joint replacement
UW MEDICINE PATIENT EDUCATION Shoulder Joint Replacement How to prepare and what to expect This handout for UW Medicine patients explains how to prepare and what to expect when having shoulder joint replacement
Patient Education Ulnar Collateral Ligament Reconstruction
 Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
Cardiac Catheterization Lab Procedures
 Patient Education Cardiac Catheterization Lab Procedures This handout describes how cardiac catheterization works. It also explains how to prepare for your procedure and the self-care needed after you
Patient Education Cardiac Catheterization Lab Procedures This handout describes how cardiac catheterization works. It also explains how to prepare for your procedure and the self-care needed after you
I will be contacting you with the day, time and location of the scheduled procedure.
 Low Country ENT is happy you have chosen us to assist you and your family in obtaining your healthcare needs. The following packet is to help you further understand your future surgical procedure as well
Low Country ENT is happy you have chosen us to assist you and your family in obtaining your healthcare needs. The following packet is to help you further understand your future surgical procedure as well
Stretching of the corners of the mouth that may lead to cracking or bruising.
 INFORMED CONSENT FOR REMOVAL OF CYST OR TUMOR Practice Administrator 9450 E Ironwood Square Dr. Scottsdale, AZ 85258 Phone: (480) 551-0581 Fax: (480) 551-0585 www.anewbeautifulyou.com Patient s Name Please
INFORMED CONSENT FOR REMOVAL OF CYST OR TUMOR Practice Administrator 9450 E Ironwood Square Dr. Scottsdale, AZ 85258 Phone: (480) 551-0581 Fax: (480) 551-0585 www.anewbeautifulyou.com Patient s Name Please
Table of Contents: What is a laparoscopic nissen fundoplication?...3. Where will surgery be performed?...3
 Table of Contents: What is a laparoscopic nissen fundoplication?...3 Planning and preparing for the surgery...3-4 Where will surgery be performed?...3 What to expect during surgery and your hospital stay.
Table of Contents: What is a laparoscopic nissen fundoplication?...3 Planning and preparing for the surgery...3-4 Where will surgery be performed?...3 What to expect during surgery and your hospital stay.
UW MEDICINE PATIENT EDUCATION. What to expect and how to prepare DRAFT. What are liposuction and fat grafting? How do I prepare?
 UW MEDICINE PATIENT EDUCATION Liposuction and Fat Grafting for Breast Reconstruction What to expect and how to prepare This handout explains liposuction and fat grafting when used in breast reconstruction.
UW MEDICINE PATIENT EDUCATION Liposuction and Fat Grafting for Breast Reconstruction What to expect and how to prepare This handout explains liposuction and fat grafting when used in breast reconstruction.
Surgical Instructions. Wisdom Tooth TREASURE VALLEY ORAL & FACIAL SURGERY
 TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
Laparoscopy. What is Laparoscopy? Why is this surgery used? How do I prepare for surgery?
 What is? Laparoscopic surgery is where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the belly button. To help with the surgery,
What is? Laparoscopic surgery is where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the belly button. To help with the surgery,
Patient Education GANZ PERIACETABULAR OSTEOTOMY
 GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
ONCOPLASTIC SURGERY FOR A LUMPECTOMY
 Patient Information for : ONCOPLASTIC SURGERY FOR A LUMPECTOMY Dr. Terence Myckatyn & Dr. Marissa Tenenbaum Surgery Scheduling Secretary/Dr. Tenenbaum Carol 314-996-3040 Surgery Scheduling Secretary/Dr.
Patient Information for : ONCOPLASTIC SURGERY FOR A LUMPECTOMY Dr. Terence Myckatyn & Dr. Marissa Tenenbaum Surgery Scheduling Secretary/Dr. Tenenbaum Carol 314-996-3040 Surgery Scheduling Secretary/Dr.
Dr. Nuelle Fracture Surgery Discharge Care Instructions
 Dr. Nuelle Fracture Surgery Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your injury. We hope that you had a good stay with us. These discharge instructions are
Dr. Nuelle Fracture Surgery Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your injury. We hope that you had a good stay with us. These discharge instructions are
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
