The evaluation of a patient with dizziness
|
|
|
- Alexis Spencer
- 6 years ago
- Views:
Transcription
1 The evaluation of a patient with dizziness Kevin A. Kerber and Robert W. Baloh Neurol Clin Pract 2011;1;24 DOI /CPJ.0b013e31823d07b6 This information is current as of December 28, 2011 The online version of this article, along with updated information and services, is located on the World Wide Web at: Neurology Clinical Practice is an official journal of the American Academy of Neurology. Copyright 2011 by AAN Enterprises, Inc. All rights reserved. Print ISSN: Online ISSN:
2 Neurology Clinical Practice The evaluation of a patient with dizziness Kevin A. Kerber, MD Robert W. Baloh, MD Summary Dizziness is the quintessential symptom presentation in all of clinical medicine. It can stem from a disturbance in nearly any system of the body. Patient descriptions of the symptom are often vague and inconsistent, so careful probing is essential. The physical examination is performed by observing the patient at rest and following simple movements or bedside tests. In general, no special tools are required. The causes of dizziness range from benign to life-threatening disorders, and features that distinguish among these may be subtle. When diagnostic testing is considered, parsimony should be the rule. Identifying common peripheral vestibular disorders is a priority. Picking this low hanging fruit can be the key component to excluding more serious central causes of dizziness. Neurologists play an important role in the evaluation and management of patients with dizziness. The possibility of a serious neurologic disorder is unnerving to front-line physicians who have ranked decision support for identifying central causes of vertigo as a top priority. 1 Although dangerous central disorders do not commonly present as isolated dizziness, stroke and other neurologic disorders can occur in this manner. The history and physical examination are the critical elements in determining the management of these patients. In this article, we review the approach to the evaluation and management of patients with dizziness. History The first step in assessing a patient presenting with dizziness is to define the symptom (table 1). The patient s report is subjective and thus can be unreliable and inconsistent. 2 For example, vertigo, defined as an illusion of movement, indicates an imbalance within the vestibular system. However, just because a patient reports vertigo does not mean that the cause is a Department of Neurology (KAK), University of Michigan Health System, Ann Arbor; and Departments of Neurology and Surgery (Head and Neck) (RWB), David Geffen School of Medicine at UCLA, Los Angeles. Correspondence to: kakerber@umich.edu 24 Copyright 2011 by AAN Enterprises, Inc.
3 Evaluation of a patient with dizziness Table 1 Common types of dizziness symptoms Descriptions Vertigo (e.g., visualized spinning, tilting, dropping of the environment) Lightheaded/woozy Near-faint Out of body, floating, spinning inside (e.g., no visualized movement of the environment) Motion sickness or intolerance Gait unsteadiness Common causes Imbalance in tonic vestibular signals due to unilateral peripheral or central lesion Blood pressure, metabolic, drugs, vestibular, psychophysiological Decreased cerebral blood flow (diffuse) Psychophysiological Sensory conflict Loss of vestibular, proprioceptive, cerebellar, or motor function vestibular disorder; similarly, just because a patient denies vertigo does not mean that a vestibular disorder is excluded. Even patients with obvious vestibular nystagmus during caloric testing may deny vertigo, and instead report a feeling of lightheadedness, wooziness, or disorientation. Lightheadedness is a very nonspecific type of dizziness. When accompanied by a near-faint symptom, it is suggestive of diffuse decreased cerebral blood flow, such as occurs with cardiac arrhythmia or orthostatic hypotension. But lightheadedness also occurs with anxiety, metabolic derangements, drug intoxication, and vestibular disorders. Some patients describe their dizziness as an out-of-body experience, floating, or an internal spinning sensation (i.e., no visualized spinning of the environment). These descriptions suggest a psychophysiological symptom (i.e., a combination of psychiatric factors and physiologic responses such as hyperventilation or neurotransmitter release). Some patients, particularly patients with migraine, are chronically sensitive to motion (self and surround). Genetic factors presumably are important but the mechanism is unknown. Disequilibrium refers to a sense of unsteadiness when standing or walking and is a common accompanying symptom of vertigo or lightheadedness. Because symptoms are subjective, defining the characteristics (e.g., onset, triggers, duration) of the symptom may be more important than defining the actual symptom (table 2). Patients tend to be more reliable and consistent with this information 2 which is critical to formulating the differential diagnosis. The key characteristics include the onset date, whether it is constant or episodic, the duration, the triggers, any aggravating or alleviating factors, or any other patterns associated with the symptom. Examination The general examination should focus on the cardiovascular system including cardiac rhythm and orthostatic blood pressure measurements. The neurologic examination focuses on oculomotor function and balance. Spontaneous and gaze-evoked nystagmus In primary gaze, the most common oculomotor abnormality observed in patients with dizziness is spontaneous nystagmus. Finding spontaneous nystagmus indicates an imbalance within the central or peripheral vestibular system. A unidirectional horizontal spontaneous nystagmus (e.g., a spontaneous left-beating nystagmus that does not convert to right-beating on gaze testing to the right) is characteristic of an acute peripheral vestibular imbalance, but this pattern can also occur in lesions of the central vestibular pathways. Spontaneous vertical or pure torsional nystagmus indicates a central lesion. After observing for spontaneous eye movements in primary gaze, next observe eye movements during and after gaze in each direction. End gaze nystagmus, which occurs variably in Neurology: Clinical Practice December
4 Kevin A. Kerber and Robert W. Baloh Table 2 Clinical features, diagnosis, and treatment of common causes of dizziness Disorder Duration Triggers Diagnosis First-line treatments a BPPV Seconds Turning in bed, reaching top shelf Vestibular neuritis Ménière syndrome Migraineassociated dizziness Upbeating-torsional nystagmus on the Dix- Hallpike test Days to weeks Usually spontaneous Spontaneous unidirectional horizontal nystagmus, corresponding positive head thrust test Canalith repositioning maneuver Symptomatic, corticosteroids, physical therapy Hours Sodium intake Fluctuating hearing loss Restrict salt, diuretic Minutes days Stress, lack of sleep, diet Personal or family history of migraine headaches; other associated migrainous symptoms Stroke Days to weeks Usually spontaneous Central nystagmus, negative head thrust test, other neurologic signs or symptoms Posterior circulation TIA Orthostatic hypotension Lifestyle factors, migraine prophylactic medications Stroke management Minutes Usually spontaneous Other neurologic symptoms TIA management Seconds Standing from sitting or lying Vasovagal Seconds minutes Prolonged standing, heat, stress Postural drop in blood pressure Positive tilt table test Cardiogenic Seconds minutes Exertion, heart failure Arrhythmia, valvular disease Vestibular paroxysmia Seconds Spontaneous multiple spells per day Anxiety disorders Minutes days Stress, complex visual surround, crowds Bilateral vestibulopathy Chronic Walking in dark or on uneven surfaces Associated clicking tinnitus, hearing loss Associated anxiety and other somatic symptoms Bilateral positive head thrust Cerebellar ataxia Chronic Alcohol Downbeat nystagmus, ataxia, gene test Motion sickness Hours days Passive head motion Autonomic symptoms and motion exposure Mal de debarquement Weeks months Ocean voyage, plane trip Feels better in motion Hydration, reduce offending medications Hydration Cardiology management Carbamazepine, oxcarbazepine, gabapentin Anxiety disorder management Vestibular rehabilitation Symptomatic and supportive care Meclizine, diphenhydramine, scopolamine Benzodiazepines, exercise Abbreviations: BPPV benign paroxysmal positional vertigo; SSRI selective serotonin reuptake inhibitor; TIA transient ischemic attack. a Adequate high-level evidence to support intervention efficacy in the associated disorder is generally lacking. Exceptions to the lack of evidence include the canalith repositioning maneuver for BPPV and the broadly stated management interventions for stroke, TIA, cardiac disorders, and anxiety disorders. normal subjects, is the term used to describe a few beats of nonsustained and symmetric nystagmus with gaze more than 30 degrees off center. Conversely, persistent nystagmus that occurs when looking about 30 degrees to the side, gaze-evoked nystagmus, is a pathologic finding. A partially compensated unilateral vestibular lesion (e.g., vestibular neuritis) can result in gaze-evoked nystagmus that only occurs in one direction (for example, left-beating gaze-evoked nystagmus does not convert to right-beating nystagmus on right gaze). Central lesions typically lead to gaze-evoked nystagmus that is bidirec- 26 Copyright 2011 by AAN Enterprises, Inc.
5 Evaluation of a patient with dizziness Figure 1 The head thrust test The head thrust test is a test of vestibular function that is performed as part of the bedside examination. This maneuver tests the vestibulo-ocular reflex (VOR). The patient sits in front of the examiner and the examiner holds the patient s head steady in the midline. The patient is instructed to maintain gaze on the nose of the examiner. The examiner then quickly turns the patient s head about degrees to one side and observes the ability of the patient to keep the eyes locked on the examiner s nose. Note that the test can also be performed by starting with the head turned to the side, and then making the quick movement back to the midline. If the patient s eyes stay locked on the examiner s nose (i.e., no corrective saccade) (A), then the peripheral vestibular system is assumed to be intact. Thus in a patient with acute dizziness, the absence of a corrective saccade suggests a CNS localization. If, however, the patient s eyes move with the head (B) and then the patient makes a voluntary eye movement back to the examiner s nose (i.e., corrective saccade), then this suggests a lesion of the peripheral vestibular system and not the CNS. When a patient presents with the acute vestibular syndrome, the test result shown in A would suggest a CNS lesion, whereas the test result in B would suggest a peripheral vestibular lesion (thus, vestibular neuritis). From: Edlow JA, Newman-Toker DE, Savitz SI. Diagnosis and initial management of cerebellar infarction. Lancet Neurol 2008;7: Neurology: Clinical Practice December
6 Kevin A. Kerber and Robert W. Baloh Patients who present with new-onset severe dizziness, imbalance, and nausea and vomiting are especially challenging because serious neurologic causes such as brainstem and cerebellar stroke must be considered. tional (i.e., left-beating nystagmus on left gaze, and right-beating nystagmus on right gaze) or vertical (i.e., upbeat on upgaze, downbeat on downgaze, or downbeat on side gaze). Bedside vestibulo-ocular reflex assessment The head thrust, or head impulse, test is used to assess the vestibulo-ocular reflex (VOR), and can uncover a unilateral or bilateral vestibulopathy at the bedside (figure 1). To perform the head thrust test, the physician stands directly in front of the patient seated on the examination table. The patient s head is held in the examiner s hands and the patient is instructed to focus on the examiner s nose. The head is then quickly moved about degrees to one side. In patients with normal vestibular function, the VOR results in movement of the eyes in the direction opposite the head movement. This occurs very quickly such that the patient s eyes remain on the examiner s nose at all times during and after the sudden movement. The test is repeated in the opposite direction. Impairment of the VOR is identified when the eyes move off the target and a voluntary saccade (so-called refixation saccade) is observed bringing the patient s eyes back to the target after the head thrust test. Positional testing Positional testing can trigger peripheral or central nystagmus. The Dix-Hallpike test is used to diagnose the posterior semicircular canal variant of benign paroxysmal positional vertigo (BPPV) (figure 2, steps 1 and 2). With the patient sitting, the head is turned 45 degrees to the side placing the posterior canal on that side in the sagittal plain. The patient is then moved to the head-hanging position. If the patient has debris moving in the posterior canal, this will lead to a very specific pattern of nystagmus: a burst of upbeat-torsional nystagmus lasting about 15 seconds. Pure vertical nystagmus, particularly persistent downbeat nystagmus, suggests a central lesion, usually involving the midline cerebellum. If the Dix-Hallpike test is applied to a patient with vestibular neuritis, then the spontaneous unidirectional horizontal pattern of nystagmus will be accentuated. This positional nystagmus leads some clinicians to erroneously diagnose BPPV in patients with vestibular neuritis. To diagnose the horizontal canal variant of BPPV, the patient lies supine and the head is turned to one side and then the other inducing a transient horizontal nystagmus that changes direction based on the side of the head turn. In the most common form of horizontal canal BPPV, a head turn to the right leads to right-beating nystagmus, whereas a head turn to the left leads to left-beating nystagmus (the abnormal side is the side with the more intense nystagmus). In the less common form of horizontal canal BPPV, the nystagmus beats in the direction opposite the head turn. Gait and balance testing The patient is observed while walking normally, while walking in tandem, and in the Romberg position with eyes opened and closed. Impaired gait and balance can accompany dizziness of any cause but as a general rule severe gait impairment suggests a neurologic disorder. 28 Copyright 2011 by AAN Enterprises, Inc.
7 Evaluation of a patient with dizziness Figure 2 The Dix-Hallpike test and the canalith repositioning maneuver The Dix-Hallpike test is performed by turning the patient s head about 45 degrees toward the side to be tested (step 1) and then laying the patient down quickly (step 2). If BPPV is present, nystagmus ensues usually within seconds. The patient is held in the right head-hanging position (step 2) for 20 to 30 seconds, and then the remaining steps of the canalith repositioning maneuver can be performed (steps 3 5). In step 3, the head is turned 90 degrees toward the unaffected side. Step 3 is held for 20 to 30 seconds before turning the head another 90 degrees (step 4) so the head is nearly in the face-down position. Step 4 is held for 20 to 30 seconds, and then the patient is brought quickly back up to the sitting up position. The movement of the otolith material within the labyrinth is depicted with each step, showing how otoliths are moved from the posterior semicircular canal to the vestibule. From: Fife T, Iverson T, Lempert J, et al. Practice parameter: therapies for benign paroxysmal positional vertigo. Neurology 2008;70: Patients with peripheral vestibular lesions (labyrinth and eighth nerve) are off-balance but usually can walk with assistance. Patients with peripheral neuropathy or bilateral vestibulopathy may be unable to stand in the Romberg position with eyes closed. Common dizziness presentations Acute prolonged severe dizziness Patients who present with new onset severe dizziness, imbalance, and nausea and vomiting are espe- Neurology: Clinical Practice December
8 Kevin A. Kerber and Robert W. Baloh cially challenging because serious neurologic causes such as brainstem and cerebellar stroke must be considered. 3 Which patients need to undergo immediate neuroimaging and which patients can be reassured and managed conservatively? Although no validated tool has been developed to provide support for this decision, the finding of unidirectional horizontal spontaneous nystagmus and a corresponding positive head thrust test in a patient without other neurologic symptoms and signs suggests a peripheral vestibular lesion, usually vestibular neuritis, a presumed viral inflammation of the vestibular nerve. 4 A patient with vestibular neuritis on the right side will have spontaneous left-beating nystagmus and a positive head thrust test to the right side. The presence of vascular risk factors, associated neurologic symptoms, direction-changing nystagmus, or absent head thrust sign increases the likelihood of a central lesion. The optimal selection of patients for MRI is not completely clear, and currently is influenced by the preferences of the physician and patient. One should keep in mind that MRI can miss small infarcts in the posterior fossa. Recurrent spontaneous attacks of dizziness When assessing patients with recurrent attacks of dizziness, clinicians have the bonus information of the natural history of the disorder. A patient with isolated recurrent attacks of dizziness occurring over many months or years is unlikely to have a sinister central cause. Transient ischemic attacks (TIAs) in the posterior circulation should be considered when the recurrent attacks are recent in onset and of short duration (minutes), particularly when accompanied by other neurologic signs or symptoms. Occasionally, dizziness can be the only symptom of a TIA but repeated episodes of dizziness over many months without associated neurologic symptoms would be highly atypical for TIAs. Of note, auditory symptoms can accompany central ischemic events if the anterior inferior cerebellar artery is involved. Ménière disease is characterized by recurrent dizziness with associated auditory symptoms, fluctuating hearing loss, ear fullness, and tinnitus. Migraine-associated dizziness occurs with or without a headache. 5 Recurrent spontaneous dizziness attacks that are not associated with auditory or neurologic symptoms over time are most likely migrainous in origin. Very brief spontaneous vertigo episodes, often labeled vestibular paroxysmia, may be caused by a mechanism analogous to that of hemifacial spasm or trigeminal neuralgia. Recurrent positionally triggered dizziness Two of the most common causes of dizziness are positionally triggered: orthostatic hypotension and BPPV. BPPV is typically triggered by lying down, rolling over in bed, or looking up to reach for something. By contrast, dizziness associated with orthostatic hypotension is triggered by getting up from a sitting or lying position and is relieved by lying down. The diagnosis of BPPV is confirmed by the Dix-Hallpike test while the diagnosis of orthostatic hypotension is made if symptoms and a drop in blood pressure occur after standing. Variants of BPPV include cupulolithiasis (particles adherent to the cupula), particles plugging the canal, and particles in other affected canals. The symptoms are similar to those of the usual posterior canal variant of BPPV but the dizziness lasts longer and the Chronic persistent dizziness and imbalance associated with movement-induced oscillopsia should raise suspicion for bilateral vestibulopathy, which can be readily identified at the bedside by a head thrust test that is positive to both sides. 30 Copyright 2011 by AAN Enterprises, Inc.
9 Evaluation of a patient with dizziness Because symptoms are subjective, defining the characteristics (e.g., onset, triggers, duration) of the symptom may be more important than defining the actual symptom. Patients tend to be more reliable and consistent with this information, which is critical to formulating the differential diagnosis. positional nystagmus has different characteristics. As noted earlier, central lesions can also present with positional dizziness but the pattern of induced nystagmus is also different, usually persistent downbeat. Chronic persistent dizziness Anxiety disorders commonly present with chronic continuous dizziness. 6 Patients often do not recognize the interrelationship of the dizziness and anxiety symptoms. Chronic persistent dizziness and imbalance associated with movement-induced oscillopsia should raise suspicion for bilateral vestibulopathy, which can be readily identified at the bedside by a head thrust test that is positive to both sides. Patients with a bilateral vestibulopathy will have substantial disability if it is acute in onset, such as with gentamicin ototoxicity. However, a patient with gradual progressive bilateral vestibulopathy may report only mild nonspecific symptoms of dizziness. Mal de debarquement is a dizziness syndrome characterized by a continuous perception of rocking, bobbing, or swaying, as if on a boat. The syndrome is typically preceded by a boat or airplane trip and remarkably patients feel better when they are in motion such as riding in an automobile. Cerebellar ataxia syndromes can present with subacute (e.g., paraneoplastic disorders) or chronic (e.g., spinocerebellar ataxia) dizziness. These disorders are generally readily identifiable based on appendicular or truncal ataxia and central eye movement abnormalities such as saccadic intrusions, impaired smooth pursuit, gaze-evoked nystagmus, or overshooting saccades. Management Treatment exists for most of the common causes of dizziness (table 2) although adequate randomized controlled treatment trials are sparse. Patients with vestibular neuritis may benefit from a short course of high-dose oral corticosteroids. A randomized controlled study found patients treated with corticosteroids had an improved outcome on average compared with controls. 7 However, the outcome was recovery of vestibular function as measured by caloric response at 1 year and thus the effect on symptomatic or functional outcome is unknown. Vestibular physical therapy can play an important role in the functional recovery of patients with vestibular neuritis. 8 The posterior canal variant of BPPV is effectively treated with the canalith repositioning maneuver (figure 2). Two Class I and 3 Class II randomized controlled trials have been performed, which demonstrate the resolution of symptoms (measured at 1 day to 4 weeks) after one maneuver in 61% to 80% of treated patients compared with 10% to 48% of untreated patients. 9 This degree of treatment benefit is among the largest effects achievable in clinical medicine. The benefit is particularly impressive because the outcome was cure as opposed to improvement or a surrogate measure. Strategies for the treatment of horizontal canal BPPV are also available, but less well tested. In patients with Ménière disease, a destructive procedure of the affected vestibular apparatus, including vestibular nerve section or intratympanic gentamicin, can lead to the resolution of recur- Neurology: Clinical Practice December
10 Kevin A. Kerber and Robert W. Baloh rent vertigo attacks. However, only a small percentage of patients require surgery since the natural history of Ménière disease is such that spontaneous remissions are common and dizziness attacks often decline in frequency over time. Although salt restriction, diuretics, and other procedures are often used in patients with Ménière disease, high-level evidence to support these interventions is lacking. The optimal management of patients with migraine-associated dizziness is yet to be adequately defined. These patients have a high rate of spontaneous improvement. 10 Randomized controlled trials of migraine preventative medications have established efficacy for headache outcomes, but none have measured dizziness outcomes. Lifestyle changes that address stress management and aim to optimize sleep, exercise, and diet may be helpful but specific trials are also lacking. REFERENCES 1. Eagles D, Stiell IG, Clement CM, et al. International survey of emergency physicians priorities for clinical decision rules. Acad Emerg Med 2008;15: Newman-Toker DE, Cannon LM, Stofferahn ME, Rothman RE, Hsieh YH, Zee DS. Imprecision in patient reports of dizziness symptom quality: a cross-sectional study conducted in an acute care setting. Mayo Clin Proc 2007;82: Kerber KA, Brown DL, Lisabeth LD, Smith MA, Morgenstern LB. Stroke among patients with dizziness, vertigo, and imbalance in the emergency department: a population-based study. Stroke 2006;37: Kattah JC, Talkad AV, Wang DZ, Hsieh YH, Newman-Toker DE. HINTS to diagnose stroke in the acute vestibular syndrome: three-step bedside oculomotor examination more sensitive than early MRI diffusion-weighted imaging. Stroke 2009;40: Neuhauser H, Lempert T. Vestibular migraine. Neurol Clin 2009;27: Ruckenstein MJ, Staab JP. Chronic subjective dizziness. Otolaryngol Clin North Am 2009;42: Strupp M, Zingler VC, Arbusow V, et al. Methylprednisolone, valacyclovir, or the combination for vestibular neuritis. N Engl J Med 2004;351: Baloh RW, Kerber KA. Clinical Neurophysiology of the Vestibular System, 4th ed. Philadelphia: Oxford University Press; Fife TD, Iverson DJ, Lempert T, et al. Practice parameter: therapies for benign paroxysmal positional vertigo (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology 2008;70: Neuhauser H, Radtke A, von Brevern M, Lempert T. Zolmitriptan for treatment of migrainous vertigo: a pilot randomized placebo-controlled trial. Neurology 2003;60: DISCLOSURES Dr. Kerber has served as a consultant for and received speaker honoraria from the American Academy of Neurology; receives publishing royalties for Clinical Neurophysiology of the Vestibular System, 4th edition (Oxford University Press, 2010); and receives research support from the NIH/NCRR and the Agency for Healthcare Research and Quality. Dr. Baloh has received speaker honoraria from the American Academy of Neurology; serves on the editorial board of Neurology ; receives publishing royalties for Clinical Neurophysiology of the Vestibular System, 4th edition (Oxford University Press, 2010); and receives research support from the NIH. 32 Copyright 2011 by AAN Enterprises, Inc.
11 Evaluation of a patient with dizziness Related articles from other AAN physician and patient resources Neurology Book Review: Dizziness: A Practical Approach to Diagnosis and Management. June 16, 2009;72:2139. Pearls & Oy-sters: Vestibular neuritis or not? The significance of head tilt in a patient with rotatory vertigo. May 19, 2009;72:e101 e102. Neurology Now Spin doctors. September/October 2007;3: Neurology Today Letter to the Editor: Report on balance is unbalanced. February 18, 2010;10:4. Neurology: Clinical Practice December
12 The evaluation of a patient with dizziness Kevin A. Kerber and Robert W. Baloh Neurol Clin Pract 2011;1;24 DOI /CPJ.0b013e31823d07b6 This information is current as of December 28, 2011 Updated Information & Services References Permissions & Licensing Reprints including high resolution figures, can be found at: This article cites 9 articles, 5 of which can be accessed free at: Information about reproducing this article in parts (figures, tables) or in its entirety can be found online at: Information about ordering reprints can be found online:
Vertigo Presentations in the Emergency Department
 Vertigo Presentations in the Emergency Department Kevin A. Kerber, M.D. 1 ABSTRACT Vertigo is among the most common reasons that patients present to the emergency department. Even though the cause is typically
Vertigo Presentations in the Emergency Department Kevin A. Kerber, M.D. 1 ABSTRACT Vertigo is among the most common reasons that patients present to the emergency department. Even though the cause is typically
Acute Vestibular Syndrome (AVS) 12/5/2017
 Sharon Hartman Polensek, MD, PhD Dept of Neurology, Emory University Atlanta VA Medical Center DIAGNOSTIC GROUPS FOR PATIENTS PRESENTING WITH DIZZINESS TO EMERGENCY DEPARTMENTS Infectious 2.9% Genitourinary
Sharon Hartman Polensek, MD, PhD Dept of Neurology, Emory University Atlanta VA Medical Center DIAGNOSTIC GROUPS FOR PATIENTS PRESENTING WITH DIZZINESS TO EMERGENCY DEPARTMENTS Infectious 2.9% Genitourinary
EMU 2017 DIZZINESS AND VERTIGO Walter Himmel MD
 EMU 2017 DIZZINESS AND VERTIGO Walter Himmel MD There is only one essential challenge in the world of dizziness and vertigo: Don t miss a posterior circulation stroke (vertebral/basilar artery) or TIA.
EMU 2017 DIZZINESS AND VERTIGO Walter Himmel MD There is only one essential challenge in the world of dizziness and vertigo: Don t miss a posterior circulation stroke (vertebral/basilar artery) or TIA.
Because dizziness is an imprecise term, a major role of the clinician is to sort patients out into categories
 Dizziness and Imbalance Timothy C. Hain, MD Clinical Professor of Neurology, Otolaryngology, Physical Therapy Chicago Dizziness and Hearing 645 N. Michigan, Suite 410 312-274-0197 Lecture Goals 1. What
Dizziness and Imbalance Timothy C. Hain, MD Clinical Professor of Neurology, Otolaryngology, Physical Therapy Chicago Dizziness and Hearing 645 N. Michigan, Suite 410 312-274-0197 Lecture Goals 1. What
Physical Therapy Examination of the Acutely Vertiginous Patient. Objectives. Prevalence/Incidence of Dizziness 3/20/2018
 Physical Therapy Examination of the Acutely Vertiginous Patient Andrew Wagner, PT, DPT, NCS Jennifer Williams, PT, DPT, NCS April 13, 2018 Objectives The learner will integrate basic examination principles
Physical Therapy Examination of the Acutely Vertiginous Patient Andrew Wagner, PT, DPT, NCS Jennifer Williams, PT, DPT, NCS April 13, 2018 Objectives The learner will integrate basic examination principles
Vertigo: A practical approach to diagnosis and treatment. John Waterston
 Vertigo: A practical approach to diagnosis and treatment John Waterston Background. Vertigo is a symptom that has diverse causes. The diagnosis may remain elusive even after exhaustive clinical enquiry
Vertigo: A practical approach to diagnosis and treatment John Waterston Background. Vertigo is a symptom that has diverse causes. The diagnosis may remain elusive even after exhaustive clinical enquiry
Acute Dizziness: Is It a Stroke? Gordon Kelley MD November 2017
 Acute Dizziness: Is It a Stroke? Gordon Kelley MD November 2017 No Disclosures Dizziness Occurs in nearly ¾ of cerebellar strokes 4 categories in classic teaching*: Vertigo Presyncope Imbalance Non-specific
Acute Dizziness: Is It a Stroke? Gordon Kelley MD November 2017 No Disclosures Dizziness Occurs in nearly ¾ of cerebellar strokes 4 categories in classic teaching*: Vertigo Presyncope Imbalance Non-specific
The Clinical Differentiation of Cerebellar Infarction from Common Vertigo Syndromes
 REVIEW ARTICLE The Clinical Differentiation of from Common Vertigo Syndromes James A. Nelson, MD* Erik Viirre MD, PhD * University of California at San Diego, Department of Emergency Medicine University
REVIEW ARTICLE The Clinical Differentiation of from Common Vertigo Syndromes James A. Nelson, MD* Erik Viirre MD, PhD * University of California at San Diego, Department of Emergency Medicine University
Acoustic neuroma s/p removal BPPV (Crystals)- 50% of people over 65 y/ o with dizziness will have this as main reason for dizziness
 Dizziness and the Heart Mended Hearts Inservice Karen Hansen, PT, DPT, Cert Vestibular Rehab, CEAS Tennessee Therapy & Balance Center, LLC July 21, 2016 Balance We maintain balance with input from our
Dizziness and the Heart Mended Hearts Inservice Karen Hansen, PT, DPT, Cert Vestibular Rehab, CEAS Tennessee Therapy & Balance Center, LLC July 21, 2016 Balance We maintain balance with input from our
What could be reffered to as dizziness by the patient?
 What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea Loss of memory Loss of confidence
What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea Loss of memory Loss of confidence
BENIGN PAROXYSMAL POSITIONAL VERTIGO (BPPV)
 5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG VESTIBULAR.ORG BENIGN PAROXYSMAL POSITIONAL VERTIGO (BPPV) By Sheelah Woodhouse, BScPT WHAT IS BPPV? Benign Paroxysmal
5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG VESTIBULAR.ORG BENIGN PAROXYSMAL POSITIONAL VERTIGO (BPPV) By Sheelah Woodhouse, BScPT WHAT IS BPPV? Benign Paroxysmal
NIH Public Access Author Manuscript Emerg Med Clin North Am. Author manuscript; available in PMC 2010 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: Emerg Med Clin North Am. 2009 February ; 27(1): 39 viii. doi:10.1016/j.emc.2008.09.002. Vertigo and Dizziness in the Emergency Department
NIH Public Access Author Manuscript Published in final edited form as: Emerg Med Clin North Am. 2009 February ; 27(1): 39 viii. doi:10.1016/j.emc.2008.09.002. Vertigo and Dizziness in the Emergency Department
Vertigo. Definition. Causes. (Dizziness) Benign Paroxysmal Positional Vertigo (BPPV) Labyrinthitis. by Karen Schroeder, MS, RD
 Vertigo (Dizziness) by Karen Schroeder, MS, RD En Español (Spanish Version) Definition Vertigo is a feeling of spinning or whirling when you are not moving. It can also be an exaggerated feeling of motion
Vertigo (Dizziness) by Karen Schroeder, MS, RD En Español (Spanish Version) Definition Vertigo is a feeling of spinning or whirling when you are not moving. It can also be an exaggerated feeling of motion
LA CLINICA E LA DIAGNOSI DELLA VERTIGINE VASCOLARE
 LA CLINICA E LA DIAGNOSI DELLA VERTIGINE VASCOLARE M. Mandalà Azienda Ospedaliera Universitaria Senese WHY ARE WE SCARED? NEED TO BETTER UNDERSTAND PATHOPHYSIOLOGY WHAT IS KNOWN WHAT IS EFFECTIVE and SIMPLE
LA CLINICA E LA DIAGNOSI DELLA VERTIGINE VASCOLARE M. Mandalà Azienda Ospedaliera Universitaria Senese WHY ARE WE SCARED? NEED TO BETTER UNDERSTAND PATHOPHYSIOLOGY WHAT IS KNOWN WHAT IS EFFECTIVE and SIMPLE
Vertigo. Tunde Magyar MD, PhD
 Vertigo Tunde Magyar MD, PhD What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea
Vertigo Tunde Magyar MD, PhD What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea
CITY & HACKNEY PATHFINDER CLINICAL COMMISSIONING GROUP. Vertigo. (1) Vertigo. (4) Provisional Diagnosis. (5) Investigations. lasting days or weeks
 Authors: Dr Lucy O'Rouke and Mr N Eynon-Lewis Review date: January 2017 Vertigo (1) Vertigo (2) History (3) Examination (4) Provisional Diagnosis (5) Investigations (6) Medical Cause (7) Psychiatric Cause
Authors: Dr Lucy O'Rouke and Mr N Eynon-Lewis Review date: January 2017 Vertigo (1) Vertigo (2) History (3) Examination (4) Provisional Diagnosis (5) Investigations (6) Medical Cause (7) Psychiatric Cause
Sasan Dabiri, MD, Assistant Professor
 Sasan Dabiri, MD, Assistant Professor Department of Otorhinolaryngology Head & Neck Surgery Amir A lam hospital Tehran University of Medical Sciences October 2015 Outlines Anatomy of Vestibular System
Sasan Dabiri, MD, Assistant Professor Department of Otorhinolaryngology Head & Neck Surgery Amir A lam hospital Tehran University of Medical Sciences October 2015 Outlines Anatomy of Vestibular System
The Big 3 of Vertigo
 They feel it, you see it, few know it: Common vertigo conditions seen, but rarely diagnosed Peter Johns MD, FRCPC University of Ottawa pjohns@toh.ca Twitter @peterjohns84 The Big 3 of Vertigo BPPV Vestibular
They feel it, you see it, few know it: Common vertigo conditions seen, but rarely diagnosed Peter Johns MD, FRCPC University of Ottawa pjohns@toh.ca Twitter @peterjohns84 The Big 3 of Vertigo BPPV Vestibular
Differential Diagnosis: Vestibular Pathology. Causes of Dizziness. Benign Paroxysmal Positional Vertigo
 Differential Diagnosis: Vestibular Learning objective: The participant will identify the pathologies associated with complaints of imbalance and dizziness Anne K Galgon PT, PhD, NCS Vestibular and Related
Differential Diagnosis: Vestibular Learning objective: The participant will identify the pathologies associated with complaints of imbalance and dizziness Anne K Galgon PT, PhD, NCS Vestibular and Related
Vestibular Differential Diagnosis
 Vestibular Differential Diagnosis P R E S E N T E D B Y : S H A R I K I C K E R, P T, M P T C E R T I F I C A T E I N V E S T I B U L A R R E H A B I L I T A T I O N 2 0 1 7 L A C E Y H A L E, P T, D P
Vestibular Differential Diagnosis P R E S E N T E D B Y : S H A R I K I C K E R, P T, M P T C E R T I F I C A T E I N V E S T I B U L A R R E H A B I L I T A T I O N 2 0 1 7 L A C E Y H A L E, P T, D P
Dizziness: Neurological Aspect
 Dizziness: Neurological Aspect..! E-mail: somtia@kku.ac.th http://epilepsy.kku.ac.th Features between peripheral and central vertigo 1. Peripheral Central 2.! " # $ " Imbalance Mild-moderate Severe 3.!
Dizziness: Neurological Aspect..! E-mail: somtia@kku.ac.th http://epilepsy.kku.ac.th Features between peripheral and central vertigo 1. Peripheral Central 2.! " # $ " Imbalance Mild-moderate Severe 3.!
Vertigo. David Clark, DO Oregon Neurology Associates Springfield, OR
 Vertigo David Clark, DO Oregon Neurology Associates Springfield, OR 44F vertigo, nausea & vomiting Unidirectional Nystagmus 44F vertigo, nausea & vomiting Impaired VOR Gain to the right Vertigo History
Vertigo David Clark, DO Oregon Neurology Associates Springfield, OR 44F vertigo, nausea & vomiting Unidirectional Nystagmus 44F vertigo, nausea & vomiting Impaired VOR Gain to the right Vertigo History
Evaluation of the Dizzy Patient
 Evaluation of the Dizzy Patient S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 1, 2007 Who Sees Dizzy Patients? ED physicians Internists Neurologists ENT
Evaluation of the Dizzy Patient S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 1, 2007 Who Sees Dizzy Patients? ED physicians Internists Neurologists ENT
Control of eye movement
 Control of eye movement Third Nerve Palsy Eye down and out Trochlear Nerve Palsy Note: Right eye Instead of intorsion and depression action of superior oblique See extorsion and elevation Observe how
Control of eye movement Third Nerve Palsy Eye down and out Trochlear Nerve Palsy Note: Right eye Instead of intorsion and depression action of superior oblique See extorsion and elevation Observe how
Dominic J Mort 23/03/17 Spire Bushey Hospital
 Dominic J Mort 23/03/17 Spire Bushey Hospital Dizziness Good grief! Hx: Pre-syncope Dizziness As if you might faint? Vertigo Mostly about this As if on a merry-go-round? Non-rotational commoner than spinning
Dominic J Mort 23/03/17 Spire Bushey Hospital Dizziness Good grief! Hx: Pre-syncope Dizziness As if you might faint? Vertigo Mostly about this As if on a merry-go-round? Non-rotational commoner than spinning
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 04/26/2014 Radiology Quiz of the Week # 108 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 04/26/2014 Radiology Quiz of the Week # 108 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Chapter 19 Dizziness and Vertigo
 Chapter 19 Dizziness and Vertigo Episode overview: 1) Compare characteristics of peripheral and central vertigo 2) What are risk factors for central causes of vertigo? 3) List 4 vestibulotoxic drugs. 4)
Chapter 19 Dizziness and Vertigo Episode overview: 1) Compare characteristics of peripheral and central vertigo 2) What are risk factors for central causes of vertigo? 3) List 4 vestibulotoxic drugs. 4)
OBJECTIVES BALANCE EVALUATION COMMON CAUSES OF BALANCE DEFICITS POST TBI BRAIN INJURY BALANCE RELATIONSHIP
 OBJECTIVES Understand variables that contribute to balance deficits Understand the relationship between a brain injury and balance Become familiar with the components of a vestibular/balance assessment
OBJECTIVES Understand variables that contribute to balance deficits Understand the relationship between a brain injury and balance Become familiar with the components of a vestibular/balance assessment
Quick Guides Vestibular Diagnosis and Treatment:
 VNG - Balance Testing Quick Guides Vestibular Diagnosis and Treatment: A Physical Therapy Approach Dix-Hallpike Test for Diagnosis of BPPV Epley Canalith Repositioning Procedure (CRP) Semont Maneuver for
VNG - Balance Testing Quick Guides Vestibular Diagnosis and Treatment: A Physical Therapy Approach Dix-Hallpike Test for Diagnosis of BPPV Epley Canalith Repositioning Procedure (CRP) Semont Maneuver for
Acute Vestibular Syndrome (VS or Stroke?) Three-step H.I.N.T.S. eye examination
 Acute Vestibular Syndrome (VS or Stroke?) Three-step H.I.N.T.S. eye examination Head Impulse (right- and leftward) Nystagmus type Test of Skew (cover test for skew deviation) Stroke findings: I.N.F.A.R.C.T.
Acute Vestibular Syndrome (VS or Stroke?) Three-step H.I.N.T.S. eye examination Head Impulse (right- and leftward) Nystagmus type Test of Skew (cover test for skew deviation) Stroke findings: I.N.F.A.R.C.T.
Predictors of Protracted Recovery
 CONCUSSION MANAGEMENT SPECIALIST ON LINE CURRICULUM Protracted Recovery and Clinical Rehabilitation All rights reserved. Sports Medicine Concepts Concussion Management Specialist Program 1 Predictors of
CONCUSSION MANAGEMENT SPECIALIST ON LINE CURRICULUM Protracted Recovery and Clinical Rehabilitation All rights reserved. Sports Medicine Concepts Concussion Management Specialist Program 1 Predictors of
BPPV and Pitfalls in its Management. Reza Golrokhian Sani MD, Otolaryngologist- Head & Neck Surgeon Otologist & Neurotologist
 BPPV and Pitfalls in its Management Reza Golrokhian Sani MD, Otolaryngologist- Head & Neck Surgeon Otologist & Neurotologist Objectives 1-The best methods of diagnosis of BPV 2-How to differentiate between
BPPV and Pitfalls in its Management Reza Golrokhian Sani MD, Otolaryngologist- Head & Neck Surgeon Otologist & Neurotologist Objectives 1-The best methods of diagnosis of BPV 2-How to differentiate between
Dizziness Cases. Martin A. Samuels Chair, Department of Neurology Brigham and Women s Hospital Boston
 Dizziness Cases Martin A. Samuels Chair, Department of Neurology Brigham and Women s Hospital Boston Basic Principles Take an open ended history Know the synonyms for dizziness A patient can have more
Dizziness Cases Martin A. Samuels Chair, Department of Neurology Brigham and Women s Hospital Boston Basic Principles Take an open ended history Know the synonyms for dizziness A patient can have more
Managing Acute Vertigo for the Non-Vestibular PT. Objectives 4/12/2018
 Managing Acute Vertigo for the Non-Vestibular PT Dalerie Lieberz, PT, DPT, GCS Assistant Professor and DCE at The College of St. Scholastica & staff therapist with the Balance & Dizziness Center at Essentia
Managing Acute Vertigo for the Non-Vestibular PT Dalerie Lieberz, PT, DPT, GCS Assistant Professor and DCE at The College of St. Scholastica & staff therapist with the Balance & Dizziness Center at Essentia
An Introduction to Dizziness and Vertigo
 An Introduction to Dizziness and Vertigo Tamara Mijovic MD CM FRCSC Clinical Assistant Professor Department of Otolaryngology Head and Neck Surgery Otology, Neurotology & Skull Base Surgery McGill University
An Introduction to Dizziness and Vertigo Tamara Mijovic MD CM FRCSC Clinical Assistant Professor Department of Otolaryngology Head and Neck Surgery Otology, Neurotology & Skull Base Surgery McGill University
Peripheral vestibular disorders will affect 1 of 13 people in their lifetime
 Peripheral vestibular disorders will affect 1 of 13 people in their lifetime 80% of affected persons seek medical consultation Unclear how many of these are for peripheral vs central disorders Generally:
Peripheral vestibular disorders will affect 1 of 13 people in their lifetime 80% of affected persons seek medical consultation Unclear how many of these are for peripheral vs central disorders Generally:
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
SIGNS AND SYMPTOMS OF CENTRAL VESTIBULAR DISORDERS
 SIGNS AND SYMPTOMS OF CENTRAL VESTIBULAR DISORDERS By Neil T. Shepard, PhD, CCC-A - Mayo Clinic Emeritus With contributions from Jordan Tucker, PT, DPT [Note: A version of this article was originally published
SIGNS AND SYMPTOMS OF CENTRAL VESTIBULAR DISORDERS By Neil T. Shepard, PhD, CCC-A - Mayo Clinic Emeritus With contributions from Jordan Tucker, PT, DPT [Note: A version of this article was originally published
Update '08: Vestibular and Balance Rehabilitation Therapy
 Update '08: Vestibular and Balance Rehabilitation Therapy In Context with Surgery Medicine & Diet Symptoms of Dizziness Dizziness non-specific term; encompasses any and all of the specific symptoms: Vertigo
Update '08: Vestibular and Balance Rehabilitation Therapy In Context with Surgery Medicine & Diet Symptoms of Dizziness Dizziness non-specific term; encompasses any and all of the specific symptoms: Vertigo
Monitoring of Caloric Response and Outcome in Patients With Benign Paroxysmal Positional Vertigo
 Otology & Neurotology 28:798Y800 Ó 2007, Otology & Neurotology, Inc. Monitoring of Caloric Response and Outcome in Patients With Benign Paroxysmal Positional Vertigo *Maria I. Molina, *Jose A. López-Escámez,
Otology & Neurotology 28:798Y800 Ó 2007, Otology & Neurotology, Inc. Monitoring of Caloric Response and Outcome in Patients With Benign Paroxysmal Positional Vertigo *Maria I. Molina, *Jose A. López-Escámez,
Benign paroxysmal positional. Labyrinth. Canalolithiasis. Specialized dizzy clinic - most frequent diagnoses. Semicircular canals
 Specialized dizzy clinic - most frequent diagnoses Canalolithiasis Unclear vertigo/dizziness multisensory vertigo/dizziness Benign paroxysmal positional vertigo (BPPV) hands on unilateral vestibulopathy
Specialized dizzy clinic - most frequent diagnoses Canalolithiasis Unclear vertigo/dizziness multisensory vertigo/dizziness Benign paroxysmal positional vertigo (BPPV) hands on unilateral vestibulopathy
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: vestibular_function_testing 5/2017 N/A 10/2017 5/2017 Description of Procedure or Service Dizziness, vertigo,
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: vestibular_function_testing 5/2017 N/A 10/2017 5/2017 Description of Procedure or Service Dizziness, vertigo,
Saccades. Assess volitional horizontal saccades with special attention to. Dysfunction indicative of central involvement (pons or cerebellum)
 Saccades Assess volitional horizontal saccades with special attention to Amplitude? Duration? Synchrony? Dysfunction indicative of central involvement (pons or cerebellum) Dynamic Visual Acuity Compare
Saccades Assess volitional horizontal saccades with special attention to Amplitude? Duration? Synchrony? Dysfunction indicative of central involvement (pons or cerebellum) Dynamic Visual Acuity Compare
Characters of nystagmus
 Characters of nystagmus Special types of nystagmus Ocular bobbing Ocular flutter Ocular myoclonus Characters of nystagmus Special types of nystagmus Disconjugate Nystagmus Circumduction Nystagmus Nystagmus
Characters of nystagmus Special types of nystagmus Ocular bobbing Ocular flutter Ocular myoclonus Characters of nystagmus Special types of nystagmus Disconjugate Nystagmus Circumduction Nystagmus Nystagmus
2/8/2017 WHERE ARE WE? East Amherst East Aurora Hamburg West Seneca Williamsville Boulevard
 2/8/2017 WHERE ARE WE? East Amherst East Aurora Hamburg West Seneca Williamsville Boulevard 1 2/8/2017 MY GOAL TODAY. 1. Provide a quick overview on falls 2. How our balance systems work 3. What treatments
2/8/2017 WHERE ARE WE? East Amherst East Aurora Hamburg West Seneca Williamsville Boulevard 1 2/8/2017 MY GOAL TODAY. 1. Provide a quick overview on falls 2. How our balance systems work 3. What treatments
Defining Dizziness: An Acute Approach to Vestibular Dysfunction in the Hospital Setting Friday, February 17, :00 AM-10:00 AM
 Defining Dizziness: An Acute Approach to Vestibular Dysfunction in the Hospital Setting Friday, February 17, 2017 8:00 AM-10:00 AM Kerry Lammers, PT, DPT Gabrielle Steinhorn, PT, DPT, NCS Vestibular dysfunction
Defining Dizziness: An Acute Approach to Vestibular Dysfunction in the Hospital Setting Friday, February 17, 2017 8:00 AM-10:00 AM Kerry Lammers, PT, DPT Gabrielle Steinhorn, PT, DPT, NCS Vestibular dysfunction
Vertigo. Definition Important history questions Examination Common vertigo cases and management Summary
 Vertigo Vertigo Definition Important history questions Examination Common vertigo cases and management Summary Cases 1) 46 year old man presents two weeks after knocking his head with recurrent episodes
Vertigo Vertigo Definition Important history questions Examination Common vertigo cases and management Summary Cases 1) 46 year old man presents two weeks after knocking his head with recurrent episodes
Benign Paroxysmal Positional Vertigo
 Benign Paroxysmal Positional Vertigo Information for patients and families Read this booklet to learn about: What Benign Paroxysmal Positional Vertigo (BPPV) is Symptoms How your doctor will diagnose it
Benign Paroxysmal Positional Vertigo Information for patients and families Read this booklet to learn about: What Benign Paroxysmal Positional Vertigo (BPPV) is Symptoms How your doctor will diagnose it
Dizziness: Natural Treatment for Vertigo and BPPV
 Wellness and WBV Studio Home» Bodywork» Massage» CranioSacral Therapy» Dizziness: Natural Treatment for Vertigo and BPPV CRANIOSACRAL THERAPY HOLISTIC HEALING Dizziness: Natural Treatment for Vertigo and
Wellness and WBV Studio Home» Bodywork» Massage» CranioSacral Therapy» Dizziness: Natural Treatment for Vertigo and BPPV CRANIOSACRAL THERAPY HOLISTIC HEALING Dizziness: Natural Treatment for Vertigo and
Benign Paroxysmal Positional Vertigo. Jeff Walter PT, DPT, NCS
 Benign Paroxysmal Positional Vertigo Jeff Walter PT, DPT, NCS Benign Paroxysmal Positional Vertigo: (BPPV) Benign = not malignant Paroxysmal = recurrent, sudden intensification of symptoms Positional =
Benign Paroxysmal Positional Vertigo Jeff Walter PT, DPT, NCS Benign Paroxysmal Positional Vertigo: (BPPV) Benign = not malignant Paroxysmal = recurrent, sudden intensification of symptoms Positional =
Problem based review: the patient with dizziness on the AMU
 240 Acute Medicine 2012 11(4): 240-245 Trainee Section Problem based review: the patient with dizziness on the AMU A Kennedy & N Cooper Abstract Unsteadiness, balance disturbance, and dizziness are common
240 Acute Medicine 2012 11(4): 240-245 Trainee Section Problem based review: the patient with dizziness on the AMU A Kennedy & N Cooper Abstract Unsteadiness, balance disturbance, and dizziness are common
met het oog op evenwicht
 met het oog op evenwicht Herman Kingma, Department of ORL, Maastricht University Medical Centre Faculty of Biomedical Technology, Technical University Eindhoven problems in patients with dizziness and
met het oog op evenwicht Herman Kingma, Department of ORL, Maastricht University Medical Centre Faculty of Biomedical Technology, Technical University Eindhoven problems in patients with dizziness and
VESTIBULAR SYSTEM. Deficits cause: Vertigo. Falling Tilting Nystagmus Nausea, vomiting
 VESTIBULAR SYSTEM Objectives: Understand the functions of the vestibular system: What is it? How do you stimulate it? What are the consequences of stimulation? Describe the vestibular apparatus, the 2
VESTIBULAR SYSTEM Objectives: Understand the functions of the vestibular system: What is it? How do you stimulate it? What are the consequences of stimulation? Describe the vestibular apparatus, the 2
Dizziness, postural hypotension and postural blackouts: Two cases suggesting multiple system atrophy
 Dizziness, postural hypotension and postural blackouts: Two cases suggesting multiple system atrophy Dr Rahul Chakor, Associate Prof and Head Dept of Neurology, Dr Anand Soni, Senior Resident, T N Medical
Dizziness, postural hypotension and postural blackouts: Two cases suggesting multiple system atrophy Dr Rahul Chakor, Associate Prof and Head Dept of Neurology, Dr Anand Soni, Senior Resident, T N Medical
Vestibular Evaluation
 Chris Carpino, MPT Vestibular Evaluation 1. History Most important aspect of evaluation (see DHI) 2. Vital Signs Check blood pressure in supine and sitting 3. Eye Exam 4. Positional Testing 5. Balance
Chris Carpino, MPT Vestibular Evaluation 1. History Most important aspect of evaluation (see DHI) 2. Vital Signs Check blood pressure in supine and sitting 3. Eye Exam 4. Positional Testing 5. Balance
Paediatric Balance Assessment
 BAA regional meeting 11 th March 2016 Paediatric Balance Assessment Samantha Lear, Lead Clinical Scientist, Hearing Services, SCH overview The balance system Vestibular disorders referrals Vestibular assessment
BAA regional meeting 11 th March 2016 Paediatric Balance Assessment Samantha Lear, Lead Clinical Scientist, Hearing Services, SCH overview The balance system Vestibular disorders referrals Vestibular assessment
Acute vestibular syndrome stroke vs. neuritis
 08.05.18 Background Acute vestibular syndrome stroke vs. neuritis PD Dr. med. Alexander A. Tarnutzer Department of Neurology University Hospital Zurich EAN Spring School 2018 Staré Splavy, Czech Republic
08.05.18 Background Acute vestibular syndrome stroke vs. neuritis PD Dr. med. Alexander A. Tarnutzer Department of Neurology University Hospital Zurich EAN Spring School 2018 Staré Splavy, Czech Republic
Speaker Disclosures: 12/4/2015 DIZZINESS AND NEAR SYNCOPE. I have no relevant commercial relationships to disclose
 DIZZINESS AND NEAR SYNCOPE Bernard Gran, M.D. Neurologist, Co-Chief, Department of Neuroscience Baptist Health Neuroscience Center Speaker Disclosures: I have no relevant commercial relationships to disclose
DIZZINESS AND NEAR SYNCOPE Bernard Gran, M.D. Neurologist, Co-Chief, Department of Neuroscience Baptist Health Neuroscience Center Speaker Disclosures: I have no relevant commercial relationships to disclose
Benign Paroxysmal Positional Vertigo (a.k.a.) Diagnosis: Dix-Hallpike Maneuver. Case SH. BPPV nystagmus. Video Frenzel Goggles make it easier
 Canalith Repositioning for Benign Paroxysmal Positional Vertigo Benign Paroxysmal Positional Vertigo (a.k.a.) Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern
Canalith Repositioning for Benign Paroxysmal Positional Vertigo Benign Paroxysmal Positional Vertigo (a.k.a.) Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern
Otologic (Ear) Dizziness Fistula SCD Bilateral. Other. Neuritis BPPV. Menieres
 Otologic Dizziness (Dizziness from Ear) Ear Structures of importance Timothy C. Hain, MD Northwestern University, Chicago t-hain@northwestern.edu The ear is an inertial navigation device Semicircular Canals
Otologic Dizziness (Dizziness from Ear) Ear Structures of importance Timothy C. Hain, MD Northwestern University, Chicago t-hain@northwestern.edu The ear is an inertial navigation device Semicircular Canals
A Case of Vestibular and Oculomotor. Pathology from Bilateral AICA Watershed. Infarcts Treated with Basilar Artery Stenting
 Bilateral AICA Strokes. Kattah J, et al 1 A Case of Vestibular and Oculomotor Pathology from Bilateral AICA Watershed Infarcts Treated with Basilar Artery Stenting Jorge C Kattah, M.D * Deepak Nair M.D,
Bilateral AICA Strokes. Kattah J, et al 1 A Case of Vestibular and Oculomotor Pathology from Bilateral AICA Watershed Infarcts Treated with Basilar Artery Stenting Jorge C Kattah, M.D * Deepak Nair M.D,
Vestibular Symptoms in Concussion: Medical/Surgical Perspective. Jacob R. Brodsky, MD Boston Children s Hospital
 Vestibular Symptoms in Concussion: Medical/Surgical Perspective Jacob R. Brodsky, MD Boston Children s Hospital jacob.brodsky@childrens.harvard.edu On Field Symptoms Headache Dizziness Confusion Fatigue
Vestibular Symptoms in Concussion: Medical/Surgical Perspective Jacob R. Brodsky, MD Boston Children s Hospital jacob.brodsky@childrens.harvard.edu On Field Symptoms Headache Dizziness Confusion Fatigue
Workshop: The Assessment of Patients with Dizziness and Vertigo
 Workshop: The Assessment of Patients with Dizziness and Vertigo Tamara Mijovic MD CM FRCSC Clinical Assistant Professor Department of Otolaryngology Head and Neck Surgery Otology, Neurotology & Skull Base
Workshop: The Assessment of Patients with Dizziness and Vertigo Tamara Mijovic MD CM FRCSC Clinical Assistant Professor Department of Otolaryngology Head and Neck Surgery Otology, Neurotology & Skull Base
VESTIBULAR FUNCTION TESTING
 VESTIBULAR FUNCTION TESTING Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
VESTIBULAR FUNCTION TESTING Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
Vestibular System. Dian Yu, class of 2016
 Vestibular System Dian Yu, class of 2016 Objectives 1. Describe the functions of the vestibular system: What is it? How do you stimulate it? What are the consequences of stimulation? 2. Describe the vestibular
Vestibular System Dian Yu, class of 2016 Objectives 1. Describe the functions of the vestibular system: What is it? How do you stimulate it? What are the consequences of stimulation? 2. Describe the vestibular
OBJECTIVES TYPES OF DIZZINESS TYPES OF DIZZINESS. Type III Disequilibrium. Classifying Common Position Sense Disturbances
 OBJECTIVES Define four major types of dizziness Emphasizing vertigo Describe pathophysiology of dizziness Emphasizing BPPV Review how to cure BPPV How do you know where you are in 3-dimensional space?
OBJECTIVES Define four major types of dizziness Emphasizing vertigo Describe pathophysiology of dizziness Emphasizing BPPV Review how to cure BPPV How do you know where you are in 3-dimensional space?
Classic Cases. Interesting Dizzy Cases. Case 1. Case 2. Case 3. Case 4. Timothy C. Hain, MD
 Interesting Dizzy Cases Classic Cases Timothy C. Hain, MD Case 1 A 30 year old Chicago Park District Worker came in because of dizziness. He fell off of a truck two years ago, hit his head, and now he
Interesting Dizzy Cases Classic Cases Timothy C. Hain, MD Case 1 A 30 year old Chicago Park District Worker came in because of dizziness. He fell off of a truck two years ago, hit his head, and now he
Balance Assessment and Rehabilitation in Audiology. Andy Phillips Director of Therapies and Health Science ABMU Health Board
 Balance Assessment and Rehabilitation in Audiology Andy Phillips Director of Therapies and Health Science ABMU Health Board Balance Mechanism This has 3 components -Sensory Input -Central Processing -Motor
Balance Assessment and Rehabilitation in Audiology Andy Phillips Director of Therapies and Health Science ABMU Health Board Balance Mechanism This has 3 components -Sensory Input -Central Processing -Motor
Benign paroxysmal positional vertigo: clinical characteristics of dizzy patients referred to a Falls and Syncope Unit
 Q J Med 2005; 98:357 364 Advance Access publication 8 April 2005 doi:10.1093/qjmed/hci057 Benign paroxysmal positional vertigo: clinical characteristics of dizzy patients referred to a Falls and Syncope
Q J Med 2005; 98:357 364 Advance Access publication 8 April 2005 doi:10.1093/qjmed/hci057 Benign paroxysmal positional vertigo: clinical characteristics of dizzy patients referred to a Falls and Syncope
Vestibular testing: what patients can expect
 American Hearing Research Foundation Symposium on Dizziness & Balance Disorders April 6, 2013 Vestibular testing: what patients can expect Marcello Cherchi, MD PhD Assistant Professor of Neurology Northwestern
American Hearing Research Foundation Symposium on Dizziness & Balance Disorders April 6, 2013 Vestibular testing: what patients can expect Marcello Cherchi, MD PhD Assistant Professor of Neurology Northwestern
Vestibular Function Testing
 Vestibular Function Testing Timothy C. Hain, MD Professor Vestibular Tests ENG (electronystagmography) VEMP (Vestibular evoked myogenic responses) Rotatory Chair Posturography Five motion sensors can measure
Vestibular Function Testing Timothy C. Hain, MD Professor Vestibular Tests ENG (electronystagmography) VEMP (Vestibular evoked myogenic responses) Rotatory Chair Posturography Five motion sensors can measure
I m dizzy-what can I expect at my doctor visit? Dennis M. Moore, M.D. Lutheral General
 I m dizzy-what can I expect at my doctor visit? Dennis M. Moore, M.D. Lutheral General Dizziness and Balance is a broad area encompassing multiple fields: primary care (internal medicine, pediatrics),
I m dizzy-what can I expect at my doctor visit? Dennis M. Moore, M.D. Lutheral General Dizziness and Balance is a broad area encompassing multiple fields: primary care (internal medicine, pediatrics),
So Young Moon, M.D., Kwang-Dong Choi, M.D., Seong-Ho Park, M.D., Ji Soo Kim, M.D.
 So Young Moon, M.D., Kwang-Dong Choi, M.D., Seong-Ho Park, M.D., Ji Soo Kim, M.D. Background: Benign positional vertigo (BPV) is characterized by episodic vertigo and nystagmus provoked by head motion.
So Young Moon, M.D., Kwang-Dong Choi, M.D., Seong-Ho Park, M.D., Ji Soo Kim, M.D. Background: Benign positional vertigo (BPV) is characterized by episodic vertigo and nystagmus provoked by head motion.
Benign Paroxysmal Positional Vertigo (BPPV) Structures of importance. The ear is an inertial navigation device. Vestibular Reflexes
 Otologic Dizziness (Dizziness from Ear) Structures of importance Timothy C. Hain, MD Northwestern University, Chicago t-hain@northwestern.edu The ear is an inertial navigation device Semicircular Canals
Otologic Dizziness (Dizziness from Ear) Structures of importance Timothy C. Hain, MD Northwestern University, Chicago t-hain@northwestern.edu The ear is an inertial navigation device Semicircular Canals
what is the permanent impact of loss of the vestibular sense? for balance, vision and spatial orientation)
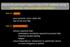 what is the permanent impact of loss of the vestibular sense? for balance, vision and spatial orientation) loss of speed - poor dynamic vision (daily life) - fear to fall and falls loss of automatisation
what is the permanent impact of loss of the vestibular sense? for balance, vision and spatial orientation) loss of speed - poor dynamic vision (daily life) - fear to fall and falls loss of automatisation
3) Approach to Ataxia - Dr. Zana
 3) Approach to Ataxia - Dr. Zana Introduction Ataxia is derived from Greek word a -not, taxis -orderly, (not orderly/ not in order) Ataxia is the inability to make smooth, accurate and coordinated movements
3) Approach to Ataxia - Dr. Zana Introduction Ataxia is derived from Greek word a -not, taxis -orderly, (not orderly/ not in order) Ataxia is the inability to make smooth, accurate and coordinated movements
Usage of the HINTS exam and neuroimaging in the assessment of peripheral vertigo in the emergency department
 Quimby et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:54 https://doi.org/10.1186/s40463-018-0305-8 ORIGINAL RESEARCH ARTICLE Open Access Usage of the HINTS exam and neuroimaging in
Quimby et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:54 https://doi.org/10.1186/s40463-018-0305-8 ORIGINAL RESEARCH ARTICLE Open Access Usage of the HINTS exam and neuroimaging in
How to take the patient history
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 3 Bedside examination of the vestibular and ocular motor system - Level 2 How to take the
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 3 Bedside examination of the vestibular and ocular motor system - Level 2 How to take the
DIZZINESS & VERTIGO A MULTIDISCIPLINARY APPROACH
 DIZZINESS & VERTIGO A MULTIDISCIPLINARY APPROACH Dr DOSH SANDOORAM MB ChB, MD, FRCS Consultant ENT Surgeon, City Clinic Group Labyrinthine disturbance may make one feel like the end of the world has arrived...
DIZZINESS & VERTIGO A MULTIDISCIPLINARY APPROACH Dr DOSH SANDOORAM MB ChB, MD, FRCS Consultant ENT Surgeon, City Clinic Group Labyrinthine disturbance may make one feel like the end of the world has arrived...
Dizziness is VERY Common. Dizziness is an imprecise term. Diagnostic Categories. Question. Answer 1. The Dizzy Patient Recent advances (2007)
 The Dizzy Patient Recent advances (2007) Timothy C. Hain, MD Chicago Dizziness and Hearing Neurology, Otolaryngology, Physical Therapy Northwestern University, Chicago t-hain@northwestern.edu Dizziness
The Dizzy Patient Recent advances (2007) Timothy C. Hain, MD Chicago Dizziness and Hearing Neurology, Otolaryngology, Physical Therapy Northwestern University, Chicago t-hain@northwestern.edu Dizziness
Benign Paroxysmal Positional Vertigo (a.k.a.) Diagnosis: Dix-Hallpike Maneuver. Case SH. BPPV nystagmus. Video Frenzel Goggles make it easier
 Positional Vertigo Office Diagnosis and Treatment Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern University, Chicago, IL Janet O. Helminski, PhD Physical
Positional Vertigo Office Diagnosis and Treatment Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern University, Chicago, IL Janet O. Helminski, PhD Physical
Evaluation & Management of Vestibular Disorders
 Evaluation & Management of Vestibular Disorders Richard A. Roberts, Ph.D., FAAA Alabama Hearing & Balance Associates, Inc. Disclosure and Copyright Statements Richard Roberts has no financial or nonfinancial
Evaluation & Management of Vestibular Disorders Richard A. Roberts, Ph.D., FAAA Alabama Hearing & Balance Associates, Inc. Disclosure and Copyright Statements Richard Roberts has no financial or nonfinancial
Session 10: Practical Approaches to the "Dizzy" Patient Learning Objectives
 Session 10: Practical Approaches to the "Dizzy" Patient Learning Objectives 1. Consider the potential etiologies for symptoms of lightheadedness or vertigo. 2. Appropriately determine next steps, such
Session 10: Practical Approaches to the "Dizzy" Patient Learning Objectives 1. Consider the potential etiologies for symptoms of lightheadedness or vertigo. 2. Appropriately determine next steps, such
Quick Guides Vestibular Diagnosis and Treatment:
 VNG - Balance Testing Quick Guides Vestibular Diagnosis and Treatment: Utilizing Videonystagmography (VNG) Spontaneous Nystagmus Gaze Test Smooth Pursuit Tracking Saccade Test Optokinetics (OKN) Dix-Hallpike
VNG - Balance Testing Quick Guides Vestibular Diagnosis and Treatment: Utilizing Videonystagmography (VNG) Spontaneous Nystagmus Gaze Test Smooth Pursuit Tracking Saccade Test Optokinetics (OKN) Dix-Hallpike
Balance disorders What is a balance disorder? How does the vestibular system work?
 Balance disorders What is a balance disorder? A balance disorder is a condition that makes you feel unsteady or dizzy, as if you are moving, spinning, or floating, even though you are standing still or
Balance disorders What is a balance disorder? A balance disorder is a condition that makes you feel unsteady or dizzy, as if you are moving, spinning, or floating, even though you are standing still or
Benign Paroxysmal Positional Vertigo (a.k.a.) Diagnosis: Dix-Hallpike Maneuver. Case SH. BPPV nystagmus. MMT ENG course --- BPPV 6/3/2012
 Benign Paroxysmal Positional Vertigo Benign Paroxysmal Positional Vertigo (a.k.a.) Timothy C. Hain, MD Departments of Otolaryngology and Physical Therapy Northwestern University, Chicago, IL BPPV BPV (Benign
Benign Paroxysmal Positional Vertigo Benign Paroxysmal Positional Vertigo (a.k.a.) Timothy C. Hain, MD Departments of Otolaryngology and Physical Therapy Northwestern University, Chicago, IL BPPV BPV (Benign
Differential Diagnosis of Dizziness in SCI. Jordan Cabrera, PT, DPT, NCS Jorge Neira, PT, DPT, NCS
 Differential Diagnosis of Dizziness in SCI Jordan Cabrera, PT, DPT, NCS Jorge Neira, PT, DPT, NCS Learning Objectives Participant will be able to identify the need to perform a basic oculomotor and vestibular
Differential Diagnosis of Dizziness in SCI Jordan Cabrera, PT, DPT, NCS Jorge Neira, PT, DPT, NCS Learning Objectives Participant will be able to identify the need to perform a basic oculomotor and vestibular
BENIGN PAROXYSMAL POSITIONAL VERTIGO
 BENIGN PAROXYSMAL POSITIONAL VERTIGO Timothy C. Hain, MD In Benign Paroxysmal Positional Vertigo (BPPV) dizziness is generally thought to be due to debris which has collected within a part of the inner
BENIGN PAROXYSMAL POSITIONAL VERTIGO Timothy C. Hain, MD In Benign Paroxysmal Positional Vertigo (BPPV) dizziness is generally thought to be due to debris which has collected within a part of the inner
I m Weak and Dizzy. Dr. Peter J. Lin Director Primary Care Initiative Canadian Heart Research Centre
 I m Weak and Dizzy Dr. Peter J. Lin Director Primary Care Initiative Canadian Heart Research Centre Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
I m Weak and Dizzy Dr. Peter J. Lin Director Primary Care Initiative Canadian Heart Research Centre Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
The Geriatric Patient The EM Perspective. Advice from a neophyte
 The Geriatric Patient The EM Perspective Advice from a neophyte Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any
The Geriatric Patient The EM Perspective Advice from a neophyte Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any
Inner Ear Disorders. Information for patients and families
 Inner Ear Disorders Information for patients and families Read this booklet to learn about: What are inner ear disorders Symptoms Tests you may need Treatment options Please visit the UHN Patient Education
Inner Ear Disorders Information for patients and families Read this booklet to learn about: What are inner ear disorders Symptoms Tests you may need Treatment options Please visit the UHN Patient Education
The Dizziness Handicap Inventory and Its Relationship with Vestibular Diseases
 Int. Adv. Otol. 2012; 8:(1) 69-77 ORIGINAL ARTICLE The Dizziness Handicap Inventory and Its Relationship with Vestibular Diseases Mi Joo Kim, Kyu-Sung Kim, Yeon Hee Joo, Soo Young Park, Gyu Cheol Han Department
Int. Adv. Otol. 2012; 8:(1) 69-77 ORIGINAL ARTICLE The Dizziness Handicap Inventory and Its Relationship with Vestibular Diseases Mi Joo Kim, Kyu-Sung Kim, Yeon Hee Joo, Soo Young Park, Gyu Cheol Han Department
ORIGINAL ARTICLE. A New Physical Maneuver for the Treatment of Benign Paroxysmal Positional Vertigo
 ORIGINAL ARTICLE Victor Vital, MD; Athanasia Printza, MD; Joseph Vital, MD; Stefanos Triaridis, MD; Miltiadis Tsalighopoulos, MD From the Department of Otolaryngology, Aristotle University of Thessaloniki,
ORIGINAL ARTICLE Victor Vital, MD; Athanasia Printza, MD; Joseph Vital, MD; Stefanos Triaridis, MD; Miltiadis Tsalighopoulos, MD From the Department of Otolaryngology, Aristotle University of Thessaloniki,
Medical Coverage Policy Vestibular Function Tests
 Medical Coverage Policy Vestibular Function Tests EFFECTIVE DATE:01 01 2017 POLICY LAST UPDATED: 04 18 2017 OVERVIEW Dizziness, vertigo, and balance impairments can arise from a loss of vestibular function.
Medical Coverage Policy Vestibular Function Tests EFFECTIVE DATE:01 01 2017 POLICY LAST UPDATED: 04 18 2017 OVERVIEW Dizziness, vertigo, and balance impairments can arise from a loss of vestibular function.
No Running Is BPPV Blocking the Path to a Carefree Childhood?
 WELCOME BACK to an ongoing series that challenges the audiologist to identify a diagnosis for a case study based on a listing and explanation of the nonaudiology and audiology test battery. It is important
WELCOME BACK to an ongoing series that challenges the audiologist to identify a diagnosis for a case study based on a listing and explanation of the nonaudiology and audiology test battery. It is important
Cross Country Education Leading the Way in Continuing Education and Professional Development.
 To comply with professional boards/associations standards: I declare that I or my family do not have any financial relationship in any amount, occurring in the last 12 months with a commercial interest
To comply with professional boards/associations standards: I declare that I or my family do not have any financial relationship in any amount, occurring in the last 12 months with a commercial interest
DOWNLOAD OR READ : VERTIGO AND DIZZINESS REHABILITATION THE MCS METHOD PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : VERTIGO AND DIZZINESS REHABILITATION THE MCS METHOD PDF EBOOK EPUB MOBI Page 1 Page 2 vertigo and dizziness rehabilitation the mcs method vertigo and dizziness rehabilitation pdf vertigo
DOWNLOAD OR READ : VERTIGO AND DIZZINESS REHABILITATION THE MCS METHOD PDF EBOOK EPUB MOBI Page 1 Page 2 vertigo and dizziness rehabilitation the mcs method vertigo and dizziness rehabilitation pdf vertigo
THE STATS KEEPING YOUR BALANCE THE PROFESSIONALS 2/23/2018 THE STATS QUALITY OF LIFE QUALITY OF LIFE - FALLS
 KEEPING YOUR BALANCE EVAL & MANAGEMENT OF INNER EAR BALANCE DISORDERS Dr. Lily V. Hughes, Audiologist Fairbanks Hearing & Balance Center at the ENT Clinic THE STATS THE STATS QUALITY OF LIFE Vestibular
KEEPING YOUR BALANCE EVAL & MANAGEMENT OF INNER EAR BALANCE DISORDERS Dr. Lily V. Hughes, Audiologist Fairbanks Hearing & Balance Center at the ENT Clinic THE STATS THE STATS QUALITY OF LIFE Vestibular
Lecture Goals. Dizziness is VERY Common. Dizziness is an imprecise term. Question 1. Diagnostic Categories
 Otoneurologist Approach to the Dizzy Patient Timothy C. Hain, MD Clinical Professor Neurology, Otolaryngology, Physical Therapy Northwestern University, Chicago t-hain@northwestern.edu Lecture Goals Describe
Otoneurologist Approach to the Dizzy Patient Timothy C. Hain, MD Clinical Professor Neurology, Otolaryngology, Physical Therapy Northwestern University, Chicago t-hain@northwestern.edu Lecture Goals Describe
Pseudo-Spontaneous Nystagmus in Lateral Semicircular Canal Benign Paroxysmal Positional Vertigo
 Original Article Clinical and Experimental Otorhinolaryngology Vol. 5, No. 4: 201-206, December 2012 http://dx.doi.org/10.3342/ceo.2012.5.4.201 pissn 1976-8710 eissn 2005-0720 Pseudo-Spontaneous Nystagmus
Original Article Clinical and Experimental Otorhinolaryngology Vol. 5, No. 4: 201-206, December 2012 http://dx.doi.org/10.3342/ceo.2012.5.4.201 pissn 1976-8710 eissn 2005-0720 Pseudo-Spontaneous Nystagmus
