Environmental Emergencies. Objectives. Case Study 1: Snake Bite
|
|
|
- Ophelia Mitchell
- 6 years ago
- Views:
Transcription
1 Environmental Emergencies Objectives Identify the early manifestations of a snake bite, appropriate care, and use of antivenin. Recognize serious spider bites and describe management. Distinguish among types of heat illness. Discuss management of hypothermia. Discuss the management of submersion injuries. Case Study 1: Snake Bite 2-year-old boy stepped on a snake and was bitten. He arrives in the emergency department 2 hours later He is alert but tearful, has no increased work of breathing, and his skin is pink. His parents think he stepped on a rattlesnake. 1
2 Initial Assessment (1 of 2) PAT: Normal appearance, normal breathing, normal circulation Vital signs: Heart rate 120/min, respiratory rate 26/min, blood pressure 90/60 mm Hg, temperature 37.2 C, weight 13 kg Initial Assessment (2 of 2) A: Patent, no stridor B: Clear breath sounds C: Pulse is strong and regular. D: Awake, alert; nonfocal motor examination findings E: Right calf has 1 set of fang marks surrounded by 6 in of red induration. Key Questions What is your general impression of this patient? What other information may be helpful? 2
3 General Impression Stable Concern regarding type of snake Cottonmouth Rattlesnake Copperhead Pit Viper Envenomation Assessment: ABCs and resuscitate as indicated Circumstances and number of bites First-aid methods and transport time Stage severity of bite Pit Vipers (Crotalidae) Envenomation severity varies with species. Venoms differ in enzyme components: Myonecrotic, cardiotoxins, nephrotoxins, hemotoxins, neurotoxins Extensive capillary leak and local tissue necrosis may result in circulatory shock. 3
4 Envenomation Staging (1 of 3) No envenomation dry bites In 25% of strikes, no venom is released. Only fang marks present Mild envenomation Fang mark(s) Local edema and tissue necrosis No evidence of systemic effects Envenomation Staging (2 of 3) Moderate envenomation Edema, bullae, ecchymoses beyond local area Tender adenopathy may be present. Evidence of systemic effects Envenomation Staging (3 of 3) Severe envenomation Rapid extension of edema, bullae, ecchymoses involving entire extremity Shock: Tachycardia, hypotension, altered level of consciousness Laboratory: Elevation of prothrombin time/ creatine kinase, depression of platelet count/fibrinogen 4
5 Case Progression Child receives wound care, ibuprofen, and intravenous line access is established. Baseline lab studies obtained After 2 hours, the wound, surrounding erythema, and leg size are unchanged. Vital signs: Heart rate 100/min, respiratory rate 26/min, blood pressure 85/60 mm Hg, temperature 37.2 C, all laboratory study results normal Key Questions Does this patient need antivenin? Does he need hospital admission? Pit Viper Envenomation (1 of 2) Management: Based on bite staging Reassurance: Child and caregivers Keep child quiet and limb at heart level. Serial bite measurements and limb circumference: Every 15 to 20 minutes for 6 hours Every 4 hours for a total of 24 hours 5
6 Pit Viper Envenomation (2 of 2) Establish IV line access Laboratory studies every 2 to 6 hours Local wound care and analgesia Crotalidae Antivenin Crotalidae polyvalent immune Fab antivenin (Crotalidae Fab, Cro Fab) Ovine derived Lower-risk hypersensitivity reactions Antivenin Crotalidae polyvalent Horse serum derived High-risk acute and delayed hypersensitivity reactions Crotalidae Polyvalent Antivenin Indicated in moderate to severe stages Useful in most diamondback rattlesnake bites Mild envenomation: Skin testing followed by 5 vials Moderate envenomation: Skin testing followed by 10 vials Severe envenomation: Skin testing followed by 15 vials 6
7 Case Outcome Because parents are certain rattlesnake bit the boy and diamondback rattlesnakes are known to exist in this geographic area, 5 vials of antivenin were given after skin testing. Patient admitted with serial measurements of lower limb. Discharged home the next day with scheduled follow-up in 5 days. Coral Snakes (Elapidae) 3 varieties found in United States Eastern: Southeast (more toxic) Sonoran/Western: Arizona and New Mexico Texas Account for 1% snakebites Coral Snakes (Elapidae) Bite is 2 puncture wounds less than 1 cm apart. Initially causes mild pain and minimal edema In 4 hours, develop paresthesia, weakness, diplopia, bulbar signs May progress to respiratory failure 7
8 Coral Snake Envenomation Management Supportive care in pediatric intensive care unit No US antivenin (other countries manufacture): useful for Eastern or Texas bites Sonoran: No antivenin needed Follow-up after antivenin Case Study 2: Spider Bite 4-year-old boy bitten by spider at family campsite; tells ED staff spider was dark, no other details Alert and calm, no increased work of breathing, skin pink Initial Assessment (1 of 2) PAT: Normal appearance, normal breathing, normal circulation Vital signs: Heart rate 130/min, respiratory rate 26/min, blood pressure 102/66 mm Hg, temperature 37 C, weight 17 kg 8
9 Initial Assessment (2 of 2) A: Patent, no stridor B: Unlabored, no retractions C: Pulse strong and regular D: Awake but reports experiencing pain at bite E: Right forearm swollen and red with 2 small marks in center of wound. Hand pink, fingers move normally Key Question What is your initial impression of this patient? General impression Patient is stable: Mild pain No muscle rigidity No hypertension No nausea/vomiting Need geographic location Additional observation 9
10 Differential Diagnosis: What Else? Black widow spider Brown recluse spider Nontoxic spider Additional Questions What signs or symptoms would help distinguish the type of spider bite? What studies are needed? What treatment is necessary? Black Widow Spider Genus Latrodectus: Female with red hourglass Venom peptides cause release of: Acetylcholine at myoneural junction Norepinephrine 10
11 Black Widow Spider Bite: Clinical Signs Onset of symptoms 30 to 90 minutes after bite and peak in 3 to 12 hours Hypertension Irritability Muscle rigidity, especially abdominal Respiratory distress, 2 muscle paralysis Periorbital swelling Black Widow Envenomation: Management Supportive care and cardiorespiratory monitoring Benzodiazepines for muscle rigidity Narcotic analgesics for pain Antivenin for hypertension, tachycardia, seizures or symptoms unresponsive to benzodiazepine and narcotic therapy Admit for monitored observation Brown Recluse Spider Loxosceles reclusa: Brown recluse spider Common in Southern and Midwestern states Venom contains calciumdependent enzyme sphingomyelinase D. Has lytic effect on red blood cells 11
12 Brown Recluse Spider Bite Brown Recluse Spider Bite Little pain at time of bite Itching, swelling, erythema, tenderness in a few hours Classically, erythema surrounds dull blue-gray macula. 3-4 days, necrotic base with black eschar Brown Recluse Spider Envenomation Dull blue-gray macule, surrounded by erythema and a ring or halo of pallor Fever Muscle pain Nausea Vomiting Rash Headache Anthalgia Hemolysis Shock 12
13 Brown Recluse Spider Bite: Management Supportive care Local wound care Tetanus prophylaxis Immobilize the affected extremity. Apply ice to reduce pain. Administer antihistamines. Case Discussion/Outcome Child has no signs of severe envenomation a few hours after the bite. Black widow envenomation unlikely with no muscle rigidity, hypertension, or irritability Brown recluse envenomation possible, but no dull blue-gray macule with surrounding pallor, no systemic signs Other nonvenomous spider bite likely Case Study 3: Collapsed, Delirious 13-year-old boy collapses on running track. Coach finds him delirious but breathing. In ED, boy is drowsy and nauseated. He has no increased work of breathing. His skin is hot and sweaty but pink. 13
14 Initial Assessment (1 of 2) PAT: Abnormal appearance, normal breathing, normal circulation Vital signs: Heart rate 80/min, respiratory rate 14/min, blood pressure 100/60 mm Hg, tympanic temperature, 39 C, weight, 40 kg Initial Assessment (2 of 2) A: Patent, no stridor B: Unlabored, no retractions C: Pulse strong and regular D: He knows his name but not the date or how he arrived in the ED. E: No hematoma, bruises Question What is your general impression of this patient? 14
15 General Impression Primary CNS dysfunction Unclear origin Review AEIOU-TIPS. What are your initial management plans? Management Priorities Administer oxygen. Obtain vascular access, give 20-mL/kg fluid bolus (normal saline or lactated Ringer solution) Bedside glucose, baseline laboratory studies ECG Core temperature Cool: Antipyretics, mechanical Differential Diagnosis: What Else? Heat exhaustion Heat stroke Heat syncope Dehydration Cardiac syncope Ingestion 15
16 Heat Exhaustion vs Heat Stroke Temperature <41.1 C Sweating Headache Nausea/vomiting Tachycardia Intact mental status Temperature 41.1 C Dehydration Headache Nausea/vomiting Syncope Change in mental status Seizures Case Discussion Patient had not eaten today and was ill yesterday. Temperature outside 90 F and humid Persistent altered level of consciousness is a concern. Rectal temperature of 39.3 C Sweating should not alter diagnosis. Thermoregulation Normal body temperature 36 C to 37.5 C Anterior hypothalamus preoptic nucleus thermostat regulates body temperature. Heat generation: Basal metabolism, catecholamines and thyroxine, muscle activity, heat-accelerated chemical reactions Heat loss: Radiation, conduction, convection, and evaporation 16
17 Hyperthermia 688 deaths in United States per year 4% in children younger than 14 years Predisposing factors: Age: Infants and elderly Drugs: Malignant hyperthermia Fever and infection Obesity, dehydration, skin abnormalities Lack of acclimatization, fatigue, clothing Previous episode of heat stroke Hyperthermia Pathophysiology At rest, body generates sufficient heat to cause 1 C per hour increase in temperature. Exercise, hard work cause 12-fold increase. Hypothalamus triggers heat-losing mechanism: Increased cardiac output Vasodilation and sweating Acclimatization occurs via activation of reninangiotension-aldosterone system. Minor Heat Illness Heat edema: Cutaneous vasodilatation Heat cramps: Severe cramps of heavily exercised muscles after exertion Heat syncope: Syncopal episode during heat exposure in unacclimatized people 17
18 Major Heat Illness Heat exhaustion Precursor to heat stroke Temperature regulatory mechanisms intact Heat stroke Life-threatening emergency Loss of thermoregulatory mechanism Types of Heat Stroke Exertional heat stroke: Unacclimatized athlete Rapid onset Severe prostration Sweating intact Classic/nonexertional heat stroke: More common in infants and elderly individuals Slower onset Marked dehydration Sweating may be absent Heat Stroke: Signs and Symptoms Temperature >41.1 C Changes in mental status Dehydration Nausea and vomiting Headache Ataxia Syncope Seizures Coma 18
19 Heat Stroke: Management (1 of 2) Give supportive care and cardiorespiratory monitoring. Begin cooling measures: Ice packs to axillae and groin Cool water spray and fan Begin fluid resuscitation with 20 ml/kg of normal saline Heat Stroke: Management (2 of 2) Do laboratory studies: CBC, renal and liver function, glucose, coagulation, creatine kinase MB, arterial blood gas, urinalysis Admit to monitored setting. Stop cooling when core temperature is below 39 C. Case Outcome After fluids and cooling, patient is more alert and responsive. Baseline laboratory study and ECG results normal Patient hospitalized, no complications Coach stressed oral rehydration and had mandatory breaks when temperature >80 F. 19
20 Heat Stroke: Prevention Avoid exertion during warmest daytime hours (10 AM to 4 PM). Light clothing and frequent breaks Adequate intake of electrolyte solutions Avoid salt supplements. Case Study 4: Submersion 7-year-old girl falls out of boat in shallow lake, struggles at surface then goes underwater Another boat occupant dives in and rescues her within 10 minutes. At shoreline, emergency medical services reports that she is breathing fast but on her own. She is very sleepy. They immobilize her and transport her with 100% oxygen. Initial Assessment (1 of 2) PAT: Abnormal appearance, abnormal breathing, normal circulation Vital signs: Heart rate 124/min, respiratory rate 30/min, blood pressure 100/70 mm Hg, temperature 35 C 20
21 Initial Assessment (2 of 2) A: Patent, no stridor B: Tachypneic with retractions C: Pulse strong and regular D: She slowly responds to questions. E: No obvious injuries Detailed Physical Examination Head: No bruises, no hematoma Neck: In collar, denies pain Lungs: Wheezes and rhonchi bilaterally Abdomen: Soft Extremities: Able to wiggle fingers, toes Neurologic: Sleepy but good sensation and strength Key Question What is your general impression of this patient? 21
22 General Impression Respiratory distress Submersion injury Hypothermic (mild): Temperature of 35 C What are your management priorities? Case Management Provide warm, humidified oxygen. Provide warm intravenous fluids. Obtain chest radiograph. Remove cold, wet clothing and provide warm blankets. Reassess. Submersion Injury Second leading cause of unintentional injury in children aged 1 to 14 years Peak incidence in boys: Younger than 4 years 15 to 19 years Definition of drowning: Respiratory impairment from submersion (totally covered) or immersion (partially covered) in a liquid 22
23 Submersion Injury: Pathophysiology Global hypoxia: Acidosis 90% of patients aspirate: Surfactant wash out 10% of cases have laryngospasm: Dry drowning Central nervous system hypoxia: Most common cause of death Coagulopathy and renal failure can develop after hypoxia. Cardiac arrest Managing the Responsive Patient Assess ABCs and apply cardiac monitor/pulse oximeter. Assess rectal temperature and remove wet clothing. Rule out underlying comorbidity, especially drugs, alcohol, and possible child abuse. Monitor glucose level. Image chest and cervical spine if diving/fall. Admit for any oxygen requirement: Observe for delayed oxygen requirement. Submersion Injury: Predictors for Death or Severe Neurologic Sequelae After 25 minutes of resuscitation with no return of spontaneous circulation in non-icy waters >5 C (>41.1 F), survival is unlikely If icy water submersion, attempt rewarming. 23
24 Managing the Unresponsive Patient (1 of 2) ABCs and cervical spine stabilization Bag-mask ventilation with 100% oxygen, intubate, insert nasogastric/orogastric tube CPR and ECG: Initiate medications and electrical interventions as indicated. Intravenous access: Normal saline, check glucose Assess rectal temperature and remove wet clothing. Managing the Unresponsive Patient (2 of 2) Perform baseline laboratory tests, blood gas analysis, and chest radiography and consider performing a toxicology screen. Ventilate with positive end-expiratory pressure (5-10 cm H 2 O). Begin rewarming if hypothermic. Neurologic status: Rule out underlying condition. Admit to PICU. Hypothermia Pathophysiology Core temperature below 35 C (95 F) Classification: Mild, moderate, or severe Preoptic anterior hypothalamus initiates sympathetic neurogenic signals: Increased muscle tone Increased metabolic rate Shivering Cutaneous vasoconstriction Bradycardia Apnea and asystole 24
25 Hypothermia: Predisposing Factors Endocrine or metabolic derangements, hypoglycemia, hypothyroidism Infection: Meningitis, sepsis Intoxication: Alcohol, opiates Intracranial disease Environmental exposure/submersion injury Dermatologic: Burns Iatrogenic Mild Hypothermia 32 C to 35 C (89.6 F-95 F) Shivering preserved Inappropriate judgment or mental slowing Treat with passive rewarming (warm blankets). Moderate Hypothermia (1 of 2) 28 C to 32 C (82.4 F-89.6 F) Muscle rigidity Progressive loss of consciousness/coma Difficult to detect vital signs ECG change of an Osborn (J) wave 25
26 Moderate Hypothermia (2 of 2) Treatment: ABCs: Control airway CPR Intravenous access and laboratory studies Active rewarming Myocardium is resistant to defibrillation and medications below 30 C. Active Rewarming Method Warm humidified oxygen Warm intravenous fluids Gastric or rectal lavage Open thoracotomy with mediastinal irrigation Extracorporeal blood rewarming (bypass) Severe Hypothermia <28 C (82.4 F) Appear dead Coma Dilated unresponsive pupils Respiratory arrest and ventricular fibrillation Treatment: ABCs: Control airway CPR, laboratory studies Active rewarming to 30 C 26
27 Case Outcome Repeat temperature of 37.1 C Initial radiographs negative Patient requires 2 L of oxygen to keep SaO 2 arterial oxygen saturation >92% Patient is admitted to the hospital. Promises to wear personal floatation device next time Key Points: Submersion Injury Prompt, effective CPR improves prognosis and outcome. Aggressive out-of-hospital resuscitation if patient arrested Prolonged in-hospital resuscitation of nonhypothermia patients is not indicated. Patients with altered level of consciousness should be intubated, provided with mechanical ventilation, and transported to the PICU. The Bottom Line Environmental emergencies are a diverse group of conditions that result from environmental insults, each with unique signs, symptoms, and management. Recognition of symptoms and consideration of an environmental cause of the clinical features will result in early diagnosis and appropriate management. Prevention is key in reducing injuries. 27
28 Credits Unless otherwise indicated, all photographs and illustrations are under copyright of Jones & Bartlett Learning, courtesy of Maryland Institute for Emergency Medical Services Systems, or the American Academy of Pediatrics. Slide 1: David R. Frazier/Photo Researchers, Inc. Slide 7A-C: SuperStock/Alamy Images, Photos.com, Courtesy of Ray Rauch/U.S. Fish & Wildlife Service Slide 20: Courtesy of Luther C. Goldman/U.S. Fish & Wildlife Service Slide 30: Crystal Kirk/ShutterStock, Inc. Slide 33: Courtesy of Kenneth Cramer, Monmouth College Slide 34: Courtesy of Department of Entomology, University of Nebraska Slide 83: Photos.com 28
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
ENVIRONMENTAL EMERGENCIES
 SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
Thermoregulation 2015 WMA
 1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Environmental Emergencies
 chapter 17 Environmental Emergencies Susan Fuchs, MD, FAAP, FACEP Dee Hodge III, MD, FAAP Objectives 1 2 Identify the early manifestations of a serious pit viper envenomation, the appropriate supportive
chapter 17 Environmental Emergencies Susan Fuchs, MD, FAAP, FACEP Dee Hodge III, MD, FAAP Objectives 1 2 Identify the early manifestations of a serious pit viper envenomation, the appropriate supportive
Overview. Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control
 Overview Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control 1 Causal Factors Age, weight, degree of physical fitness Degree of acclimatization, metabolism Intercurrent illnesses
Overview Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control 1 Causal Factors Age, weight, degree of physical fitness Degree of acclimatization, metabolism Intercurrent illnesses
Heat Illness in Children
 Heat Illness in Children Charles G. Macias MD, MPH Baylor College of Medicine Attending Physician, Texas Children s Hospital Emergency Department Houston, Texas Scope of the problem Heat stroke mortality
Heat Illness in Children Charles G. Macias MD, MPH Baylor College of Medicine Attending Physician, Texas Children s Hospital Emergency Department Houston, Texas Scope of the problem Heat stroke mortality
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Drowning is a leading cause of death and loss of years of life with over 90% of cases occurring in lower- and middle-income countries.
 Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2
 CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
Gatorade Heat Safety Package
 Gatorade Heat Safety Package 1. The Four Downs of Heat Safety 2. Tips to Hydrate and Fuel for the Football Season 3. Preventing Heat-Related Illnesses The 4 Downs of Heat Safety Know the plays of heat
Gatorade Heat Safety Package 1. The Four Downs of Heat Safety 2. Tips to Hydrate and Fuel for the Football Season 3. Preventing Heat-Related Illnesses The 4 Downs of Heat Safety Know the plays of heat
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Pediatric advanced life support. Management of decreased conscious level in children. Virgi ija Žili skaitė 2017
 Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
HEAT STROKE. Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC
 HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
Management Of Medical Emergencies
 Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
2012 Heat Safety Kit
 2012 Heat Safety Kit PREVENTING HEAT-RELATED ILLNESSES HEAT ILLNESS AND EMERGENCIES Heat-related illnesses have many factors but can be caused when an individual is subjected to extreme temperatures and
2012 Heat Safety Kit PREVENTING HEAT-RELATED ILLNESSES HEAT ILLNESS AND EMERGENCIES Heat-related illnesses have many factors but can be caused when an individual is subjected to extreme temperatures and
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
INTRODUCTION: DEFINITION OF HEAT ILLNESS:
 Coastal Carolina University Athletic Training Department Policy and Procedure Manual Exertional Heat Illness Management Fluid Replacement/Rehydration Protocol Revised/Reviewed 3/2013 INTRODUCTION: The
Coastal Carolina University Athletic Training Department Policy and Procedure Manual Exertional Heat Illness Management Fluid Replacement/Rehydration Protocol Revised/Reviewed 3/2013 INTRODUCTION: The
Darren Manthey, MD Division of Emergency Medicine Sanford School of Medicine ENVIRONMENTAL EMERGENCIES
 Darren Manthey, MD Division of Emergency Medicine Sanford School of Medicine ENVIRONMENTAL EMERGENCIES Objectives Review: hypothermia frostbite heat illness sunburn lightning strike injuries drowning envonimations
Darren Manthey, MD Division of Emergency Medicine Sanford School of Medicine ENVIRONMENTAL EMERGENCIES Objectives Review: hypothermia frostbite heat illness sunburn lightning strike injuries drowning envonimations
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Homework Assignment Complete and Place in Binder
 Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Disclaimer: All photos and/or videos included in the following presentation are permitted by subjects or are not subject to privacy laws due to lack
 Disclaimer: All photos and/or videos included in the following presentation are permitted by subjects or are not subject to privacy laws due to lack of patient information or identifying factors. Pediatric
Disclaimer: All photos and/or videos included in the following presentation are permitted by subjects or are not subject to privacy laws due to lack of patient information or identifying factors. Pediatric
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
2.5 HEALTH AND SAFETY
 2.5 HEALTH AND SAFETY 2.5.1 Fundamentals of Heat Illness Prevention and Management (a) A Certified Athletic Trainer or 1 st Responder MUST be in attendance at all football practices and games. (b) The
2.5 HEALTH AND SAFETY 2.5.1 Fundamentals of Heat Illness Prevention and Management (a) A Certified Athletic Trainer or 1 st Responder MUST be in attendance at all football practices and games. (b) The
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
2. Heat-Related Illness
 2. Heat-Related Illness Only fit and heat-acclimatized athletes can participate safely. TEMPERATURE ( F) 100 95 90 85 80 75 70 65 Heat sensitive and unacclimatized athletes may suffer. Little danger of
2. Heat-Related Illness Only fit and heat-acclimatized athletes can participate safely. TEMPERATURE ( F) 100 95 90 85 80 75 70 65 Heat sensitive and unacclimatized athletes may suffer. Little danger of
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
2/13/2014. Lori Weichenthal, MD, FACEP Associate Professor of Clinical Emergency Medicine UCSF Fresno
 Lori Weichenthal, MD, FACEP Associate Professor of Clinical Emergency Medicine UCSF Fresno 1 INTRODUCTION Thermoregulation Acclimatization Field Management of Heat Illness Solar Injury Questions and Conclusion
Lori Weichenthal, MD, FACEP Associate Professor of Clinical Emergency Medicine UCSF Fresno 1 INTRODUCTION Thermoregulation Acclimatization Field Management of Heat Illness Solar Injury Questions and Conclusion
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
Case Presentation #4: A Pretty Worm
 Case Presentation #4: Presented by Brent R. King, MD, FAAP, FACEP A three year-old child arrives via EMS with ptosis, stridor, hypersalivation, hypotonia, and poor respiratory effort. The symptoms began
Case Presentation #4: Presented by Brent R. King, MD, FAAP, FACEP A three year-old child arrives via EMS with ptosis, stridor, hypersalivation, hypotonia, and poor respiratory effort. The symptoms began
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
HealthCare Training Service
 HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
HealthCare Training Service Advanced Life Support Exam Time: Perusal Time: 20 minutes 5 minutes Total Marks: 25 Instructions: Read each question carefully. Using a pencil, record your response to each
Northwest Community EMS System Continuing Education Class Credit Questions for April 2014 Summer Emergencies
 Northwest Community EMS System Continuing Education Class Credit Questions for April 2014 Summer Emergencies Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete The answers are
Northwest Community EMS System Continuing Education Class Credit Questions for April 2014 Summer Emergencies Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete The answers are
Resuscitation in Special Situations what s new
 Resuscitation in Special Situations what s new Asc. Prof. Dr. Serkan Şener Acıbadem University, School of Medicine Department of Emergency Medicine Acıbadem Ankara Hospital Objectives To understand the
Resuscitation in Special Situations what s new Asc. Prof. Dr. Serkan Şener Acıbadem University, School of Medicine Department of Emergency Medicine Acıbadem Ankara Hospital Objectives To understand the
ENVIRONMENTAL EMERGENCIES
 Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
Bill Hall, MD Mesa County EMS System
 Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Causes. 95 F An air temperature of 95 Fahrenheit is high risk regardless of the humidity. 85 F + 60% humidity
 HOT WEATHER SAFETY TIPS An important step in avoiding heat illness is adjusting practice or game length and intensity to the environmental conditions. Temperature and humidity combine to create conditions
HOT WEATHER SAFETY TIPS An important step in avoiding heat illness is adjusting practice or game length and intensity to the environmental conditions. Temperature and humidity combine to create conditions
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Northwest Community EMS System May 2018 CE: Summer Emergencies Credit Questions
 Northwest Community EMS System May 2018 CE: Summer Emergencies Credit Questions Name: EMS Agency/hospital: EMSC/Educator reviewer: Date submitted: Credit awarded (date): Returned for revisions: Revisions
Northwest Community EMS System May 2018 CE: Summer Emergencies Credit Questions Name: EMS Agency/hospital: EMSC/Educator reviewer: Date submitted: Credit awarded (date): Returned for revisions: Revisions
CHAIN OF COMMAND: THE FOLLOWING CHAIN OF COMMAND WILL OCCUR:
 LEWISVILLE ISD COLD WEATHER POLICY Cold exposure can be uncomfortable, impair performance and even become life threatening. Conditions created by cold exposure include frostbite and hypothermia. Wind chill
LEWISVILLE ISD COLD WEATHER POLICY Cold exposure can be uncomfortable, impair performance and even become life threatening. Conditions created by cold exposure include frostbite and hypothermia. Wind chill
Environmental Emergencies. Emergency Medical Response
 Environmental Emergencies Lesson 26: Environmental Emergencies You Are the Emergency Medical Responder As the nearest park ranger in the area, you are summoned to a campsite for an incident involving a
Environmental Emergencies Lesson 26: Environmental Emergencies You Are the Emergency Medical Responder As the nearest park ranger in the area, you are summoned to a campsite for an incident involving a
HEAT PRODUCTION HEAT DISSIPATION
 Heat Illness Shaylon Rettig, MD, MBA HEAT PRODUCTION Heat is a byproduct of the metabolic process Muscle contributes the largest amount of heat produced at rest Muscle work increases heat production Fever
Heat Illness Shaylon Rettig, MD, MBA HEAT PRODUCTION Heat is a byproduct of the metabolic process Muscle contributes the largest amount of heat produced at rest Muscle work increases heat production Fever
SNAKEBITE / CROTALID ANTIVENOMS
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES. Justin Astafan, EMT-P, CIC
 ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES Justin Astafan, EMT-P, CIC NYS EMT-P NYS CIC 17 years in the fire and ems profession Work both career and volunteer side Worked for commercial and notfor
ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES Justin Astafan, EMT-P, CIC NYS EMT-P NYS CIC 17 years in the fire and ems profession Work both career and volunteer side Worked for commercial and notfor
THERMOREGULATION 05 JUNE 2013
 THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
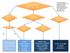 Suspected Hypothermia Temp
Suspected Hypothermia Temp
Altered Mental Status Basic Emergency Care Course
 Altered Mental Status Basic Emergency Care Course Objectives Recognize key history findings suggestive of different causes of altered mental status Recognize key physical findings suggestive of different
Altered Mental Status Basic Emergency Care Course Objectives Recognize key history findings suggestive of different causes of altered mental status Recognize key physical findings suggestive of different
Bites, Stings and Venomous Things Amanda Wickman, MBA Southwest Center for Agricultural Health, Injury Prevention and Education
 Bites, Stings and Venomous Things Amanda Wickman, MBA Southwest Center for Agricultural Health, Injury Prevention and Education Midwest Migrant Stream Forum November 2015 Background Objectives 1. Dispel
Bites, Stings and Venomous Things Amanda Wickman, MBA Southwest Center for Agricultural Health, Injury Prevention and Education Midwest Migrant Stream Forum November 2015 Background Objectives 1. Dispel
Allergic Reactions and Envenomations. Chapter 16
 Allergic Reactions and Envenomations Chapter 16 Allergic Reactions Allergic reaction Exaggerated immune response to any substance Histamines and leukotrienes Chemicals released by the immune system Anaphylaxis
Allergic Reactions and Envenomations Chapter 16 Allergic Reactions Allergic reaction Exaggerated immune response to any substance Histamines and leukotrienes Chemicals released by the immune system Anaphylaxis
All Things Cold: Hypothermia, Altitude Illness and Frostbite. Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine
 All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off.
 1 2 EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. 3 4 5 6 Course Outline Introduction
1 2 EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. 3 4 5 6 Course Outline Introduction
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1
 Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Lesson 13: Heat Related Illnesses. Emergency Reference Guide p
 Lesson 13: Heat Related Illnesses Emergency Reference Guide p. 59-64 Objectives Define heat exhaustion, heat stroke & hyponatremia Describe prevention techniques List signs/symptoms for heat related illnesses
Lesson 13: Heat Related Illnesses Emergency Reference Guide p. 59-64 Objectives Define heat exhaustion, heat stroke & hyponatremia Describe prevention techniques List signs/symptoms for heat related illnesses
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
Naloxone Intranasal EMT OPTIONAL SKILL. Cell Phones and Pagers. Course Outline 09/2017
 EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and Overview
EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and Overview
HENRY COUNTY SCHOOL DISTRICT GUIDELINES FOR OUTDOOR EXTRACURRICULAR ACTIVITIES DURING EXTREME HOT AND HUMID WEATHER
 HENRY COUNTY SCHOOL DISTRICT GUIDELINES FOR OUTDOOR EXTRACURRICULAR ACTIVITIES DURING EXTREME HOT AND HUMID WEATHER 1. Each school shall have and use a digital psychrometer, or a similar device for measuring
HENRY COUNTY SCHOOL DISTRICT GUIDELINES FOR OUTDOOR EXTRACURRICULAR ACTIVITIES DURING EXTREME HOT AND HUMID WEATHER 1. Each school shall have and use a digital psychrometer, or a similar device for measuring
VACCINE-RELATED ALLERGIC REACTIONS
 VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Module Summaries: The emergency plan is a crucial part of the total sports program.
 Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Module Summaries: Summary - The Emergency Plan The emergency plan is a crucial part of the total sports program. Prior to each season and game, those individuals responsible for the program and athletes
Preparing for your upcoming PALS course
 IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
Animal caused Injuries פגיעות בעלי חיים כל הזכויות שמורות למד"א מרחב ירושלים
 Animal caused Injuries פגיעות בעלי חיים Snake bite נחש In Israel there are 9 kinds of poisonous snakes. 3 mechanisms of venom action: Vascular Neurological Cardiac Small amount of venom goes through the
Animal caused Injuries פגיעות בעלי חיים Snake bite נחש In Israel there are 9 kinds of poisonous snakes. 3 mechanisms of venom action: Vascular Neurological Cardiac Small amount of venom goes through the
HEAT STRESS BLUE COLLAR SILVICULTURE LTD.
 HEAT STRESS BLUE COLLAR SILVICULTURE LTD. TRAINING OVERVIEW What is heat stress Primary contributing factors Sources of heat Removal of heat from the body Personal risk factors Recognizing heat stress
HEAT STRESS BLUE COLLAR SILVICULTURE LTD. TRAINING OVERVIEW What is heat stress Primary contributing factors Sources of heat Removal of heat from the body Personal risk factors Recognizing heat stress
Regulation of Body Temperature. Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY
 Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Cold Injuries: An Update on Hypothermia and Frostbite
 Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Chapter Goal. Learning Objectives 9/12/2012. Chapter 36. Geriatrics. Use assessment findings to formulate management plan for geriatric patients
 Chapter 36 Geriatrics Chapter Goal Use assessment findings to formulate management plan for geriatric patients Learning Objectives Describe dependent & independent living environments Identify local resources
Chapter 36 Geriatrics Chapter Goal Use assessment findings to formulate management plan for geriatric patients Learning Objectives Describe dependent & independent living environments Identify local resources
Bites and Envenomations
 Bites and Envenomations Type of bite/sting Description or bring creature with patient (preferably dead) Time, location, size of bite/sting Previous reaction to bite/sting Domestic vs. wild Tetanus and
Bites and Envenomations Type of bite/sting Description or bring creature with patient (preferably dead) Time, location, size of bite/sting Previous reaction to bite/sting Domestic vs. wild Tetanus and
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Pediatric Assessment Objectives
 Pediatric Assessment Objectives Distinguish the 3 components of the PAT. Assess pediatric-specific features of initial assessment. Integrate findings to form a general impression. Describe the focused
Pediatric Assessment Objectives Distinguish the 3 components of the PAT. Assess pediatric-specific features of initial assessment. Integrate findings to form a general impression. Describe the focused
Prevention of Heat Stress
 Prevention of Heat Stress Presentation Outline What is heat stress? Body s response to heat stress Why does heat stress occur? Heat stress predisposing factors Effects of heat Prevention Management Thermoregulation
Prevention of Heat Stress Presentation Outline What is heat stress? Body s response to heat stress Why does heat stress occur? Heat stress predisposing factors Effects of heat Prevention Management Thermoregulation
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Diabetic Emergencies. Chapter 15
 Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
EXERTIONAL HEAT ILLNESS
 EXERTIONAL HEAT ILLNESS EXERTIONAL HEAT ILLNESS (EHI) EHI is composed of four different conditions. Heat Cramps Heat Syncope Heat Exhaustion Heat Stroke HEAT CRAMPS Acute, Painful, involuntary muscle contraction
EXERTIONAL HEAT ILLNESS EXERTIONAL HEAT ILLNESS (EHI) EHI is composed of four different conditions. Heat Cramps Heat Syncope Heat Exhaustion Heat Stroke HEAT CRAMPS Acute, Painful, involuntary muscle contraction
Evans Middle School Practice Procedures for High Heat and Humidity
 Evans Middle School Practice Procedures for High Heat and Humidity The Coweta County School System and Evans Middle School are concerned about the health and safety of all student athletes. In accordance
Evans Middle School Practice Procedures for High Heat and Humidity The Coweta County School System and Evans Middle School are concerned about the health and safety of all student athletes. In accordance
Vital Signs. Vital Signs. Vital Signs
 Vital Signs Vital Signs Why do vital signs? Determine relative status of vital organs Establish baseline Monitor response to Rx, meds Observe trends Determine need for further evaluation, Rx, intervention
Vital Signs Vital Signs Why do vital signs? Determine relative status of vital organs Establish baseline Monitor response to Rx, meds Observe trends Determine need for further evaluation, Rx, intervention
Unit 7 INJURY MANAGEMENT Review Game
 Unit 7 INJURY MANAGEMENT Review Game Print and cut out the playing cards. Divide the class into groups of 3 or 4. Each group will need a set of playing cards. Directions for the Review game 1. Stack all
Unit 7 INJURY MANAGEMENT Review Game Print and cut out the playing cards. Divide the class into groups of 3 or 4. Each group will need a set of playing cards. Directions for the Review game 1. Stack all
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Frostbite. Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department
 Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
CBC with Differential. PHYSICIAN SIGNATURE DATE TIME DRUG ALLERGIES WT: KG
 DRUG AND TREATMENT Non Categorized SUB ED Snakebite Protocol (SUB)* Non Categorized ***(NOTE)*** This plan is designed to be used as part of a larger plan, not independently. Please do NOT order individually.
DRUG AND TREATMENT Non Categorized SUB ED Snakebite Protocol (SUB)* Non Categorized ***(NOTE)*** This plan is designed to be used as part of a larger plan, not independently. Please do NOT order individually.
CETEP PRE-TEST For questions 1 through 3, consider the following scenario:
 CETEP PRE-TEST For questions 1 through 3, consider the following scenario: A two and half month infant comes to the health centre looking very lethargic. Her mother reports that the infant has felt very
CETEP PRE-TEST For questions 1 through 3, consider the following scenario: A two and half month infant comes to the health centre looking very lethargic. Her mother reports that the infant has felt very
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
HYPERTHERMIA: A REVIEW OF DEFINITION, SYMPTOMS, AND TREATMENT FOR THE ENDURANCE ATHLETE Authors: Brian J. Krabak, M.D., MBA, and Allen Chen, M.D.
 HYPERTHERMIA: A REVIEW OF DEFINITION, SYMPTOMS, AND TREATMENT FOR THE ENDURANCE ATHLETE Authors: Brian J. Krabak, M.D., MBA, and Allen Chen, M.D. Overview Hyperthermia is defined by Webster's simply as
HYPERTHERMIA: A REVIEW OF DEFINITION, SYMPTOMS, AND TREATMENT FOR THE ENDURANCE ATHLETE Authors: Brian J. Krabak, M.D., MBA, and Allen Chen, M.D. Overview Hyperthermia is defined by Webster's simply as
PALS PRETEST. PALS Pretest
 PALS PRETEST 1. A child with a fever, immune system compromise, poor perfusion and hypotension is most likely to be experiencing which type of shock A. cardiogenic B. Neurogenic C. Septic D. Hypovolemic
PALS PRETEST 1. A child with a fever, immune system compromise, poor perfusion and hypotension is most likely to be experiencing which type of shock A. cardiogenic B. Neurogenic C. Septic D. Hypovolemic
Poisoning KNOWLEDGE OBJECTIVES SKILL OBJECTIVES. 1. List the four ways poisons enter the body.
 KNOWLEDGE OBJECTIVES Poisoning 1. List the four ways poisons enter the body. 2. List at least six signs and symptoms of poisoning. 3. Describe the role of a poison centre. 4. Identify the general principles
KNOWLEDGE OBJECTIVES Poisoning 1. List the four ways poisons enter the body. 2. List at least six signs and symptoms of poisoning. 3. Describe the role of a poison centre. 4. Identify the general principles
