The branching pattern of pulmonary vessels varies
|
|
|
- Albert French
- 5 years ago
- Views:
Transcription
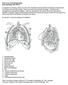
1 GENERAL THORACIC Right Upper Lobe Venous Drainage Posterior to the Bronchus Intermedius: Preoperative Identification by Computed Tomography Katsuyuki Asai, MD, Norikazu Urabe, MD, PhD, Kiyoshige Yajima, MD, Kazuya Suzuki, MD, PhD, and Teruhisa Kazui, MD, PhD Department of Thoracic Surgery, Numazu City Hospital, Numazu, Shizuoka, First Department of Surgery, Hamamatsu University School of Medicine, Hamamatsu, Shizuoka, Japan Background. Anatomical variations of the pulmonary vessels relevant to pulmonary surgery are of concern to thoracic surgeons. Among such variations, the right upper lobe vein posterior to the bronchus intermedius (UVPBI) has received little attention thus far. Methods. Chest computed tomographic images and medical records of 725 patients were retrospectively reviewed. The frequency, drainage pattern, diameter, and associated anatomical characteristics of the UVPBI were assessed, and our right thoracotomy cases with the UVPBI were examined. Results. The UVPBI was found in 41 (5.7%) of 725 computed tomography cases, and in 9 (3.9%) of 230 right thoracotomy cases. Three UVPBI drainage sites were observed: (1) the superior pulmonary vein group, 55%; (2) the inferior pulmonary vein group, 41%; and (3) the superior segmental vein group, 4%. The diameter of the UVPBI at the level of the bronchus intermedius ranged from 1 to 7 mm ( mm). The diameter of the UVPBI in the superior pulmonary vein group was significantly greater than that in the inferior pulmonary vein group (p < 0.01). The prevalence of a central vein was 43.9% for all UVPBI cases and 15.8% for large UVPBI cases (> 5 mm in diameter). Of the 9 right thoracotomy patients, 1 suffered UVPBI injury; this patient s UVPBI was not identified either preoperatively or intraoperatively. Conclusions. The UVPBI is not as rare as was previously believed. It can be a main drainage route of the right upper lobe. Preoperative identification of this venous variation by computed tomography is useful for safe and accurate surgical procedures. (Ann Thorac Surg 2005;79: ) 2005 by The Society of Thoracic Surgeons The branching pattern of pulmonary vessels varies widely, and some patterns associated with a potential risk of intraoperative bleeding can only be identified at surgery. Preoperative foreknowledge of individual vessel configurations is thus useful for ensuring a safe and accurate procedure during pulmonary surgery. Few reports have discussed anatomical variations of the right upper lobe vein posterior to the bronchus intermedius (UVPBI) relevant to pulmonary resection [1, 2]. Recent advances in noninvasive imaging methods such as multi-detector computed tomography and magnetic resonance angiography have facilitated the detection of pulmonary vessels [3, 4]. Because of its unique anatomical location, UVPBI can be identified easily by chest computed tomography (CT). The purpose of this study was to determine the frequency of UVPBI and to evaluate its associated anatomical characteristics on CT, the most familiar imaging method in our daily clinical practice. Patients and Methods Chest computed tomographic images and medical records of 780 consecutive patients who had undergone a chest CT Accepted for publication Dec 20, Address reprint requests to Dr Asai, Department of Thoracic Surgery, Numazu City Hospital, 550 Harunoki Higashi-shiiji, Numazu, Shizuoka, Japan; asaik@msc.biglobe.ne.jp. between January 1997 and March 2004 at the Department of Thoracic Surgery at Numazu City Hospital were retrospectively reviewed. We used our institution s routine protocol to analyze these computed tomographic images in a lung window setting. Computed tomographic scans were performed with either a helical scanner (ProSeed [GE Yokogawa Medical Systems, Tokyo, Japan]) or a conventional scanner (Quantex [GE Yokogawa Medical Systems]). Computed tomographic images were obtained with either 5-mm or 10-mm collimation and 10-mm intervals. Additional contrast-enhanced scanning was performed as needed. Computed tomographic images were analyzed by two thoracic surgeons (KA, NU), and a final interpretation of the findings was reached by consensus. The CT analysis for UVPBI identification consisted of the following three processes: (1) evaluation of the presence of nodular opacities attached posterior to the bronchus intermedius; (2) confirmation that the nodular opacities were veins by tracing the continuity of the nodule both cranially and caudally on contiguous CT slices; and (3) determination as to which lobe from which the vein drained (ie, the right upper or lower lobe). Depending on the drainage lobe, the vein was classified as either a UVPBI or as a right lower lobe vein posterior to the bronchus intermedius (LVPBI). The LVPBI was regarded as a branch of the right superior segmental vein (V 6 ). The UVPBI was rigorously limited to the pulmonary vein, 2005 by The Society of Thoracic Surgeons /05/$30.00 Published by Elsevier Inc doi: /j.athoracsur
2 Ann Thorac Surg ASAI ET AL 2005;79: CT IDENTIFICATION OF RIGHT PULMONARY VEIN VARIATION which could apparently be followed peripherally into the lung parenchyma of the right upper lobe. Furthermore, after identifying the UVPBI, we grouped them according to their courses towards the left atrium (LA) beyond the posterior wall of the bronchus intermedius. We evaluated the frequency of the UVPBI both in the whole population and in patients who had undergone a right thoracotomy, and we also measured the diameter of the UVPBI in each course group. In UVPBI cases, paying special attention to the fact that the central vein was prevalent in the right upper lobe, which was easily identified by CT, we checked for the presence of a central vein to determine the influence of the UVPBI on the whole drainage pattern in the right upper lobe, to the extent that we could determine this from CT study. The diameter of the UVPBI was measured at the level posterior to the bronchus intermedius. Whenever the nodular opacity was not round, the short-axis diameter was used for measurements. When the bronchus intermedius and the attached nodular opacities were observed in two or more contiguous CT slices, the maximum diameter was used. From a total of 780 computed tomographic images, 55 were excluded because of the absence of normal lung parenchyma necessary to identify anatomical structures in the relevant area. Thus, the study consisted of 725 eligible computed tomographic examinations (457 men, 268 women; age range, 6 to 89 years; mean age, 60 years). The reasons for exclusions were as follows: right pneumothorax (19), pleural effusion (3), tumor (11), inflammation (7), bulla (4), contusion (5), previous right-side pulmonary resection (4), right-sided thoracic aorta (1), and dextrocardia (1). Of the total 725 patients, 422 (58.2%) underwent surgery, 230 (31.7%) had a right thoracotomy (including surgical procedures by thoracoscopy and median sternotomy), and 137 (18.9%) had a right-sided major pulmonary resection (segmentectomy, lobectomy, and pneumonectomy). All vessel diameter measurements were recorded as mean standard deviation. Student s t test and Fisher s exact probability test were used for comparisons between groups. A p value of less than 0.05 was considered statistically significant. Results Abbreviations and Acronyms CT computed tomography IPV inferior pulmonary vein LA left atrium LVPBI right lower lobe vein posterior to the bronchus intermedius SPV superior pulmonary vein UVPBI right upper lobe vein posterior to the bronchus intermedius VATS video-assisted thoracic surgery V 6 superior segmental vein In all 725 eligible CT subjects, the bronchus intermedius and its posterior wall could be easily identified. Nodular opacities attached to the posterior wall of the bronchus intermedius were observed in 63 patients (8.7%). All the nodular opacities were identified as branches of pulmonary veins. Of the 725 computed tomographic images, the UVPBI was found in 41 (5.7%) and the LVPBI in 22 (3.0%). With respect to surgical findings, the UVPBI was found in 9 (3.9%) of 230 right thoracotomy cases, and in 6 (4.4%) of 137 cases of right major pulmonary resections. UVPBI was broadly classified according to its course towards the LA beyond the posterior wall of the bronchus intermedius. The superior pulmonary vein (SPV) group included cases in which the UVPBI ran horizontally into the mediastinum. In the remaining UVPBI cases, the UVPBI ran vertically into the inferior pulmonary vein (IPV) or V 6 while in contact with the posterior wall of the bronchus intermedius and the lower lobe bronchus. These cases were classified into two groups: (1) the IPV group (when the UVPBI joined the inferior pulmonary vein), and (2) the V 6 group (when a common trunk of UVPBI and V 6 joined the LA independently). Thus, the UVPBI cases comprised three drainage variation groups: (1) SPV group, (2) IPV group, and (3) V 6 group (Fig 1). Concerning the SPV group, since the exact course of the UVPBI within the mediastinum could not be detected by the lung window setting CT study, that portion of its course had to be deduced and supported by our limited contrast-enhanced, thin-section CT study, previous studies, and case reports. Anatomical schemata of the SPV, IPV, and V 6 groups and their diameters at the level posterior to the bronchus intermedius are shown in Fig 2. Among the UVPBI, the vessel diameter was significantly larger in the SPV group than that in the IPV group (p 0.01). The prevalence of the central vein in each of the UVPBI groups is shown in Table 1. In UVPBI cases, the prevalence of the central vein was not generally high. The prevalence of a central vein was significantly lower for cases with a large UVPBI ( 5 mm in diameter) than for cases with a small UVPBI ( 5 mm in diameter) (p 0.01). In particular, in large UVPBI cases within the SPV group, the prevalence of a central vein was only 8.3%. All UVPBI cases were drainage veins from the posterior segment. Nine patients with the UVPBI underwent a right thoracotomy (Fig 3). Clinical details of these patients are shown in Table 2. Intraoperative injury of the UVPBI occurred in one case from an electrocautery while a fissure between the right upper and lower lobe was being dissected during a lower lobectomy. In this case, the UVPBI was not identified preoperatively or intraoperatively. Comment 1867 Numerous anatomical variations of pulmonary arteries, veins and bronchi and their interrelations have been observed. In particular, pulmonary veins have great variability in their branching patterns [5 7]. Some vessel variations affect surgical procedures; the most familiar variations involve the middle lobe or lingular artery branching from the basal artery, the mediastinal branch of the lingular artery, the middle lobe vein into the IPV or GENERAL THORACIC
3 GENERAL THORACIC 1868 ASAI ET AL Ann Thorac Surg CT IDENTIFICATION OF RIGHT PULMONARY VEIN VARIATION 2005;79: Fig 1. Computed tomographic findings of each drainage course of the UVPBI (arrowheads): (A) superior pulmonary vein group, (B) inferior pulmonary vein (IPV) group, and (C) superior segmental vein (V 6 ) group. (BSV basal segmental vein; UVPBI right upper lobe vein posterior to the bronchus intermedius.) LA, and the common pulmonary vein [8]. The UVPBI is a less familiar variation, and its frequency is not well known. Thus far only a handful of studies and discussions have focused on the UVPBI [9 12]. Identifying pulmonary vessels by CT, especially at the hila, can sometimes be very difficult because of their complex anatomy. While three-dimensional images can more clearly depict pulmonary vessels [13], CT can also identify pulmonary vessels in certain areas. For instance, CT can clearly depict the posterior wall of the bronchus intermedius, sharply outlined by air in the bronchial lumen and lungs, and usually no other structure is behind it, except lung parenchyma. When CT visualizes a nodular opacity behind the tangentially depicted posterior wall of the bronchus intermedius, the UVPBI or LVPBI can be identified without much difficulty by careful tracing of the continuity of the nodule cranially and caudally. Before the advent of CT, Boyden [14] in 1955 and Yamashita [15] in 1978 described the details of the segmental anatomy of the lung in their textbooks. In his description of 50 cadaver specimens, Boyden [14] reported one case (2%) of segmental vein 2 (V 2 ) draining into the IPV, which he named the posterior segment of the right upper lung (S 3 ); therefore he actually called the vein V 3, not V 2, in his textbook) [14]. Similarly, Yamashita [15] stated that the frequency of V 2 draining into the IPV was 2.4% (4 cases out of 170 cadaver specimens). The frequency of UVPBI in the IPV group reported in these studies agrees with our data. However, neither author mentioned the drainage pattern into the SPV and the LA, posterior to the bronchus intermedius. Computed tomography studies of the UVPBI consist of only a few series [9 11]. In the largest one, Kim and colleagues [9] analyzed nodularity in the posterior wall of the bronchus intermedius on 280 normal CT scans. According to their report, the frequency of UVPBI was 3.6%, whereas that of LVPBI was 1.7%. Thus, the overall prev-
4 Ann Thorac Surg ASAI ET AL 2005;79: CT IDENTIFICATION OF RIGHT PULMONARY VEIN VARIATION 1869 GENERAL THORACIC Fig 2. Anatomical schema of each group: superior pulmonary vein (SPV) group, inferior pulmonary vein (IPV) group, and superior segmental vein (V 6 ) group. (AV azygos vein; BI bronchus intermedius; BSV basal segmental vein; E esophagus; LA left atrium; PA pulmonary artery; SVC superior vena cava; ULB upper lobe bronchus; UVPBI right upper lobe vein posterior to the bronchus intermedius.) alence of pulmonary veins posterior to the bronchus intermedius was 5.3%. In addition, with respect to the drainage pattern of the UVPBI, they reported that 30% (7 of 10) drained into the SPV and 70% (3 of 10) drained into the IPV. Jardin and Remy [11] reported that the frequency of the UVPBI in the IPV group was 9.3% (10 cases from 107 CT images of the right lower lobe). In all the reported cases in which the UVPBI was surgically confirmed, the preoperative CT also clearly detected the UVPBI [1, 2, 16]. Venous drainage patterns of the right upper lobe are usually classified as follows according to the degree of presence of a central vein: central vein type (V 1 and V 2 3 ), semi-central vein type (V 1 2 and V 3 ), or noncentral vein type. Of these, the central vein type is most common, with a reported frequency of 78.3% to 88% [15, 17]. The central vein is easily identified by routine CT. If the central vein is present, it is usually located tangentially within the angle formed by the bifurcation of the right upper lobe bronchus into B 2 and B 3. The CT level of this bifurcation is the key slice for identifying the central vein. In our study, the presence of UVPBI, especially the Table 1. The Prevalence of the Central Vein in Cases of UVPBI UVPBI (Diameter) n Central Vein (%) Total UVPBI Total (43.9) ( 5 mm) 19 3 (15.8) ( 5 mm) (68.2) SPV group Total 22 7 (31.8) ( 5 mm) 12 1 (8.3) ( 5 mm) 10 6 (60.0) IPV group Total (58.8) ( 5 mm) 5 1 (20.0) ( 5 mm) 12 9 (75.0) V 6 group Total 2 1 (50.0) ( 5 mm) 2 1 (50.0) IPV inferior pulmonary vein; SPV superior pulmonary vein; UVPBI right upper lobe vein posterior to the bronchus intermedius; V 6 superior segmental vein. Fig 3. Operative view after a right lower lobectomy in a patient with a right upper lobe vein posterior to the bronchus intermedius (UVPBI) (case 8 [see Table 2], superior pulmonary vein group). (BI bronchus intermedius; Bs bronchial stump; PAs pulmonary arterial stumps; UL upper lobe.)
5 GENERAL THORACIC 1870 ASAI ET AL Ann Thorac Surg CT IDENTIFICATION OF RIGHT PULMONARY VEIN VARIATION 2005;79: Table 2. Right Thoracotomy Cases of UVPBI Case Age/Gender Diagnosis Operation Approach UVPBI Type 1 71/F IN PR (S 4 ) VATS IPV 2 70/F LC ML PL SPV 3 44/M PTx PR (S 1 ) VATS IPV 4 52/M LC ML PL SPV 5 60/M LC LL PL SPV 7 61/M LC UL PL IPV 6 82/M LC UL PL SPV 8 72/F LC LL PL SPV 9 78/M LC PR (S 3 ) Ax IPV Diameter (mm) Preoperative Identification Intraoperative Identification UVPBI Injury UVPBI Treatment 5 no no no - 4 no no no - 1 no no no - 5 no no no - 3 no no yes divided 2 no no no - 6 yes yes no divided 5 yes yes no preserved 6 yes no no - Data are presented in chronological order. Ax axillary thoracotomy; IN inflammatory nodule; LC lung cancer; LL lower lobectomy; ML middle lobectomy; PL posterolateral thoracotomy; PR partial resection; PTx pneumothorax; UL upper lobectomy; UVPBI right upper lobe vein posterior to the bronchus intermedius; VATS video-assisted thoracic surgery. presence of a large UVPBI with drainage to the SPV, was significantly associated with a reduced frequency of a central vein. These data suggest that some of the UVPBI are the dominant drainage route of the right upper lobe, especially of the posterior segment, and that a venous drainage pattern containing a large UVPBI represents another independent type. The most probable operative procedure causing UVPBI injury is the dissection of the posterior aspect of the major fissure. Dissection of the subcarinal, right hilar, or interlobar lymph nodes can also cause UVPBI injury. These situations primarily involve right upper or lower lobectomies. Furthermore, because the UVPBI runs just inside the mediastinal visceral pleura, if the pleural space cannot be identified due to adhesions between the visceral and parietal pleurae, special care must be taken when dissecting the adhesion. Recently, video-assisted thoracic surgery lobectomy has been gaining popularity as a potential alternative to conventional thoracotomy for early stage lung cancer [18, 19]. Vascular injury within such minimally invasive approaches would make hemostasis difficult and force the surgeon to convert to a larger thoracotomy. In particular, massive bleeding from an unknown origin could rapidly lead to a critical situation. The UVPBI and some other vessel variations may thus pose a great danger during video-assisted thoracic surgery. In addition, during median sternotomy or an anterior thoracotomy, because the visibility around the UVPBI is poor, careful manipulation is required. In most cases, dividing the UVPBI first may make subsequent surgical maneuvers safer and easier. However, in cases of a large UVPBI in the SPV group, and especially with a limited pulmonary reserve, preserving the UVPBI may be preferable during a right lower lobectomy. We found two of the UVPBI in the V 6 group on CT. To our knowledge, this drainage variation has only been reported by Maciejewski [20]. For this group, he emphasized that V 6 and V 2 must be ligated separately during lobectomy. The importance of the UVPBI during esophageal resection as well as pulmonary resection, has been recognized [16]. Our study has several limitations. First, unlike thinsection CT, it is not always possible to completely discriminate between the upper lobe and the lower lobe on routine computed tomographic images, even if the lung has a complete interlobar fissure [21]. In the present study, we limited the UVPBI strictly to those veins that were apparently derived from the upper lobe. Thus, the true frequency of the UVPBI might actually be higher than our estimation because some of the veins we categorized as LVPBI might actually have been UVPBI. Second, two scan protocols were utilized in our CT examination: 5-mm collimation at 10-mm intervals, or 10-mm collimation at 10-mm intervals. The first of these two protocols might have made it difficult to detect the horizontal component of the UVPBI, especially in the SPV group, because of the 5-mm gap between two contiguous sections. Finally, because we analyzed computed tomographic images only at lung window settings,
6 Ann Thorac Surg ASAI ET AL 2005;79: CT IDENTIFICATION OF RIGHT PULMONARY VEIN VARIATION we could not visualize the exact courses of the UVPBI within the mediastinum. Thus, our SPV group might also include another group in which the UVPBI drains into the LA independently, a drainage course which Spaggiari and colleagues [1] have previously reported. Determination of a more detailed course of the UVPBI within the mediastinum, especially in the SPV group, would require additional contrast-enhanced CT studies. In conclusion, the UVPBI is not as infrequent as was previously believed. It can be the main drainage route of the right upper lobe. Preoperative identification of this variation is useful for decreasing the incidence of unexpected intraoperative bleeding. Computed tomography is an effective means of identifying the UVPBI and anticipating its course to the LA. A somewhat greater awareness of anatomical variations while interpreting CT studies may make pulmonary resection safer and more anatomically accurate. We thank Dr Hajime Fujimoto from the Department of Radiology, Numazu City Hospital, for his valuable suggestions; and Dr Koichi Mori from the Department of Radiology, Tsuchiura Kyodo General Hospital, for the motivation for this study. References 1. Spaggiari L, Solli P, Leo F, Veronesi G, Pastonno U. Anomalous segmental vein for right upper lobe: an unusual anatomical variation. Ann Thorac Surg 2002;74: Tsuboi M, Asamura H, Naruke T, Nakayama H, Kondo H, Tsuchiya R. A VATS lobectomy for lung cancer in a patient with an anomalous pulmonary vein: report of a case. Surg Today 1997;27: Schoepf UJ, Costello P. CT angiography for diagnosis of pulmonary embolism: state of the art. Radiology 2004;230: Vrachliotis TG, Bis KG, Shetty AN, Ravikrishan KP. Contrastenhanced three-dimensional MR angiography of the pulmonary vascular tree. Int J Cardiovasc Imaging 2002;18: Yazar F, Ozdogmus O, Tuccar E, Bayramoglu A, Ozan H. Drainage pattern of middle lobe vein of right lung: an anatomical study. Eur J Cardiothorac Surg 2002;22: Kato R, Lickfett L, Meininger G, et al. Pulmonary vein anatomy in patients undergoing catheter ablation of atrial fibrillation: lessons learned by use of magnetic resonance imaging. Circulation 2003;107: Marom EM, Herndon JE, Kim YH, et al. Variations in pulmonary venous drainage to the left atrium: implications for radiofrequency ablation. Radiology 2004;230: Sugimoto S, Izumiyama O, Yamashita A, Baba M, Hasegawa T. Anatomy of inferior pulmonary vein should be clarified in lower lobectomy. Ann Thorac Surg 1998;66: Kim JS, Choi D, Lee KS. CT of the bronchus intermedius: frequency and cause of a nodule in the posterior wall on normal scans. AJR 1995;165: Webb WR, Hirji M, Gamsu G. Posterior wall of the bronchus intermedius: radiographic CT correlation. AJR 1984;141: Jardin M, Remy J. Segmental bronchovascular anatomy of the lower lobes: CT analysis. AJR 1986;147: Austin JH. Right upper lobe venous drainage posterior to the bronchus intermedius. Ann Thorac Surg 2003;75: Watanabe S, Arai K, Watanabe T, Koda W, Urayama H. Use of three-dimensional computed tomographic angiography of pulmonary vessels for lung resections. Ann Thorac Surg 2003;75: Boyden EA. In: Boyden, ed. Segmental anatomy of the lungs. New York: McGraw-Hill, 1955: Yamashita H. Variations in the pulmonary segments and the bronchovascular trees. In: Yamashita H, ed. Roentgenologic anatomy of the lung. Tokyo: Igaku-shoin, 1978: Matsubara T. Rare but dangerous anomaly of the right pulmonary vein in subcarinal dissection. Ann Thorac Surg 2003;75: Lee KS, Bae WK, Lee BH, Kim IY, Choi EW, Lee BH. Bronchovascular anatomy of the upper lobes: evaluation with thin section CT. Radiology 1991;181: Gharagozloo F, Tempesta B, Margolis M, Alexander EP. Video-assisted thoracic surgery lobectomy for stage I lung cancer. Ann Thorac Surg 2003;76: Walker WS, Codispoti M, Soon SY, Stamenkovic S, Carnochan F, Pugh G. Long-term outcomes following VATS lobectomy for non-small cell bronchogenic carcinoma. Eur J Cardiothorac Surg 2003;23: Maciejewski R. The venous drainage of the apical segment of the right lower pulmonary lobe. Acta Anat 1994;150: Glazer HS, Anderson DJ, DiCroce JJ, et al. Anatomy of the major fissure: evaluation with standard and thin-section CT. Radiology 1991;180: GENERAL THORACIC
Variations of pulmonary vein drainage critical for lung resection assessed by three-dimensional computed tomography angiography
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Variations of pulmonary vein drainage critical for lung resection assessed by three-dimensional computed tomography angiography Nobuyuki Shiina 1, Kichizo
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Variations of pulmonary vein drainage critical for lung resection assessed by three-dimensional computed tomography angiography Nobuyuki Shiina 1, Kichizo
Research Article Variations in Draining Patterns of Right Pulmonary Veins at the Hilum and an Anatomical Classification
 International Scholarly Research Network ISRN Pulmonology Volume 0, Article ID 7869, pages doi:0.0/0/7869 Research Article Variations in Draining Patterns of Right Pulmonary Veins at the Hilum and an Anatomical
International Scholarly Research Network ISRN Pulmonology Volume 0, Article ID 7869, pages doi:0.0/0/7869 Research Article Variations in Draining Patterns of Right Pulmonary Veins at the Hilum and an Anatomical
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
Thoracoscopic S 6 segmentectomy: tricks to know
 Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Totally thoracoscopic left upper lobe tri-segmentectomy
 Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Reasons for conversion during VATS lobectomy: what happens with increased experience
 Review Article on Thoracic Surgery Page 1 of 5 Reasons for conversion during VATS lobectomy: what happens with increased experience Dario Amore, Davide Di Natale, Roberto Scaramuzzi, Carlo Curcio Division
Review Article on Thoracic Surgery Page 1 of 5 Reasons for conversion during VATS lobectomy: what happens with increased experience Dario Amore, Davide Di Natale, Roberto Scaramuzzi, Carlo Curcio Division
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Three Dimensional Computed Tomography Lung Modeling is Useful in Simulation and Navigation of Lung Cancer Surgery
 doi: 10.5761/atcs.ra.12.02174 Review Article Three Dimensional Computed Tomography Lung Modeling is Useful in Simulation and Navigation of Lung Cancer Surgery Norihiko Ikeda, MD, PhD, 1 Akinobu Yoshimura,
doi: 10.5761/atcs.ra.12.02174 Review Article Three Dimensional Computed Tomography Lung Modeling is Useful in Simulation and Navigation of Lung Cancer Surgery Norihiko Ikeda, MD, PhD, 1 Akinobu Yoshimura,
Chest and cardiovascular
 Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Video-assisted thoracic surgery tunnel technique: an alternative fissureless approach for anatomical lung resections
 Surgical Technique Page 1 of 8 Video-assisted thoracic surgery tunnel technique: an alternative fissureless approach for anatomical lung resections Herbert Decaluwé Department of Thoracic Surgery, Leuven
Surgical Technique Page 1 of 8 Video-assisted thoracic surgery tunnel technique: an alternative fissureless approach for anatomical lung resections Herbert Decaluwé Department of Thoracic Surgery, Leuven
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Pulmonary vascular anatomy & anatomical variants
 Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Accomplishes fundamental surgical tenets of R0 resection with systematic nodal staging for NSCLC Equivalent survival for Stage 1A disease
 Segmentectomy Made Simple Matthew J. Schuchert and Rodney J. Landreneau Department of Cardiothoracic Surgery University of Pittsburgh Medical Center Financial Disclosures none Why Consider Anatomic Segmentectomy?
Segmentectomy Made Simple Matthew J. Schuchert and Rodney J. Landreneau Department of Cardiothoracic Surgery University of Pittsburgh Medical Center Financial Disclosures none Why Consider Anatomic Segmentectomy?
Video-Mediastinoscopy Thoracoscopy (VATS)
 Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
An analysis of variations in the bronchovascular pattern of the right upper lobe using three-dimensional CT angiography and bronchography
 Gen Thorac Cardiovasc Surg (2015) 63:354 360 DOI 10.1007/s11748-015-0531-1 ORIGINAL ARTICLE An analysis of variations in the bronchovascular pattern of the right upper lobe using three-dimensional CT angiography
Gen Thorac Cardiovasc Surg (2015) 63:354 360 DOI 10.1007/s11748-015-0531-1 ORIGINAL ARTICLE An analysis of variations in the bronchovascular pattern of the right upper lobe using three-dimensional CT angiography
Lymph node dissection for lung cancer is both an old
 LOBE-SPECIFIC EXTENT OF SYSTEMATIC LYMPH NODE DISSECTION FOR NON SMALL CELL LUNG CARCINOMAS ACCORDING TO A RETROSPECTIVE STUDY OF METASTASIS AND PROGNOSIS Hisao Asamura, MD Haruhiko Nakayama, MD Haruhiko
LOBE-SPECIFIC EXTENT OF SYSTEMATIC LYMPH NODE DISSECTION FOR NON SMALL CELL LUNG CARCINOMAS ACCORDING TO A RETROSPECTIVE STUDY OF METASTASIS AND PROGNOSIS Hisao Asamura, MD Haruhiko Nakayama, MD Haruhiko
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
CT Chest. Verification of an opacity seen on the straight chest X ray
 CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
Collaborative Stage. Site-Specific Instructions - LUNG
 Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Uniportal complete video-assisted thoracoscopic surgery lobectomy with partial pulmonary arterioplasty for lung cancer with calcified lymph node
 Surgical Technique Uniportal complete video-assisted thoracoscopic surgery lobectomy with partial pulmonary arterioplasty for lung cancer with calcified lymph node Guang-Suo Wang, Jian Wang, Zhan-Peng
Surgical Technique Uniportal complete video-assisted thoracoscopic surgery lobectomy with partial pulmonary arterioplasty for lung cancer with calcified lymph node Guang-Suo Wang, Jian Wang, Zhan-Peng
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Mastering Thoracoscopic Upper Lobectomy
 Mastering Thoracoscopic Upper Lobectomy Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery, Duke University Medical
Mastering Thoracoscopic Upper Lobectomy Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery, Duke University Medical
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Uniportal video-assisted thoracoscopic right upper posterior segmentectomy with systematic mediastinal lymphadenectomy
 Surgical Technique Uniportal video-assisted thoracoscopic right upper posterior segmentectomy with systematic mediastinal lymphadenectomy Guofei Zhang 1, Zhijun Wu 2, Yimin Wu 1, Gang Shen 1, Ying Chai
Surgical Technique Uniportal video-assisted thoracoscopic right upper posterior segmentectomy with systematic mediastinal lymphadenectomy Guofei Zhang 1, Zhijun Wu 2, Yimin Wu 1, Gang Shen 1, Ying Chai
International Association for the Study of Lung Cancer lymph node map Lymph node stations Imaging CT
 Review of the International Association for the Study of Lung Cancer Lymph Node Classification System Localization of Lymph Node Stations on CT Imaging Hamza Jawad, MBBS a, Arlene Sirajuddin, MD b, Jonathan
Review of the International Association for the Study of Lung Cancer Lymph Node Classification System Localization of Lymph Node Stations on CT Imaging Hamza Jawad, MBBS a, Arlene Sirajuddin, MD b, Jonathan
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG
 LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
Monitor Images for Respiratory System Dissection
 Monitor Images for Respiratory System Dissection **This document includes extra images of the radiology of the bronchopulmonary segments. These imaged are an excellent way to review the three-dimensional
Monitor Images for Respiratory System Dissection **This document includes extra images of the radiology of the bronchopulmonary segments. These imaged are an excellent way to review the three-dimensional
The External Anatomy of the Lungs. Prof Oluwadiya KS
 The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 )
 Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Mediastinal and Hilar Lymphadenopathy: Cross-Referenced Anatomy on Axial and Coronal Images Displayed by Using Multi-detector row CT 1
 Mediastinal and Hilar Lymphadenopathy: Cross-Referenced natomy on xial and Coronal Images Displayed by Using Multi-detector row CT 1 Ju-Hyun Lee, M.D., Kyung Soo Lee, M.D., Tae Sung Kim, M.D., Chin Yi,
Mediastinal and Hilar Lymphadenopathy: Cross-Referenced natomy on xial and Coronal Images Displayed by Using Multi-detector row CT 1 Ju-Hyun Lee, M.D., Kyung Soo Lee, M.D., Tae Sung Kim, M.D., Chin Yi,
Minimally invasive lobectomy and thoracic lymph node
 Minimally Invasive Segmentectomy Joshua R. Sonett, MD, FACS Minimally invasive lobectomy and thoracic lymph node dissection is now widely established as a safe, anatomic, and oncologically sound procedure
Minimally Invasive Segmentectomy Joshua R. Sonett, MD, FACS Minimally invasive lobectomy and thoracic lymph node dissection is now widely established as a safe, anatomic, and oncologically sound procedure
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Edorium Journal of Anatomy and Embryology Type of Article: Case Report Title: Pulmonary
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Edorium Journal of Anatomy and Embryology Type of Article: Case Report Title: Pulmonary
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
Uniportal video-assisted thoracic surgery for complicated pulmonary resections
 Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Long-Term Survival After Video-Assisted Thoracic Surgery Lobectomy for Primary Lung Cancer
 Long-Term Survival After Video-Assisted Thoracic Surgery Lobectomy for Primary Lung Cancer Kazumichi Yamamoto, MD, Akihiro Ohsumi, MD, Fumitsugu Kojima, MD, Naoko Imanishi, MD, Katsunari Matsuoka, MD,
Long-Term Survival After Video-Assisted Thoracic Surgery Lobectomy for Primary Lung Cancer Kazumichi Yamamoto, MD, Akihiro Ohsumi, MD, Fumitsugu Kojima, MD, Naoko Imanishi, MD, Katsunari Matsuoka, MD,
Undergraduate Teaching
 Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure
 Original Article Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure Lu-Ming Wang, Jin-Lin Cao, Jian Hu Department of Thoracic Surgery, The First Affiliated Hospital,
Original Article Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure Lu-Ming Wang, Jin-Lin Cao, Jian Hu Department of Thoracic Surgery, The First Affiliated Hospital,
Thoracoscopic lobectomy for massive hemoptysis caused by complete pulmonary vein occlusion after radiofrequency ablation for atrial fibrillation
 ase Report Thoracoscopic lobectomy for massive hemoptysis caused by complete pulmonary vein occlusion after radiofrequency ablation for atrial fibrillation Shizhao heng 1, Xike Lu 1, Jing Wang 2, Ting
ase Report Thoracoscopic lobectomy for massive hemoptysis caused by complete pulmonary vein occlusion after radiofrequency ablation for atrial fibrillation Shizhao heng 1, Xike Lu 1, Jing Wang 2, Ting
Surgical atlas of thoracoscopic lobectomy and segmentectomy
 Art of Operative Technique Surgical atlas of thoracoscopic lobectomy and segmentectomy Tristan D. Yan 1,2 1 The Collaborative Research (CORE) Group, Macquarie University, Sydney, Australia; 2 Department
Art of Operative Technique Surgical atlas of thoracoscopic lobectomy and segmentectomy Tristan D. Yan 1,2 1 The Collaborative Research (CORE) Group, Macquarie University, Sydney, Australia; 2 Department
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC
 Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Uniportal video-assisted thoracoscopic surgery segmentectomy
 Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
Case Report on Thoracic Surgery Page 1 of 5 Uniportal video-assisted thoracoscopic surgery segmentectomy John K. C. Tam 1,2 1 Division of Thoracic Surgery, National University Heart Centre, Singapore;
Video-assisted thoracic surgery pneumonectomy: the first case report in Poland
 Case report Videosurgery Video-assisted thoracic surgery pneumonectomy: the first case report in Poland Cezary Piwkowski, Piotr Gabryel, Mariusz Kasprzyk, Wojciech Dyszkiewicz Thoracic Surgery Department,
Case report Videosurgery Video-assisted thoracic surgery pneumonectomy: the first case report in Poland Cezary Piwkowski, Piotr Gabryel, Mariusz Kasprzyk, Wojciech Dyszkiewicz Thoracic Surgery Department,
Robotic-assisted pulmonary resection - Right upper lobectomy
 Art of Operative Techniques Robotic-assisted pulmonary resection - Right upper lobectomy Robert J. Cerfolio, Ayesha S. Bryant JH Estes Family Endowed Chair for Lung Cancer Research, Division of Cardiothoracic
Art of Operative Techniques Robotic-assisted pulmonary resection - Right upper lobectomy Robert J. Cerfolio, Ayesha S. Bryant JH Estes Family Endowed Chair for Lung Cancer Research, Division of Cardiothoracic
VARIATION OF FISSURE AND LOBAR PATTERN OF LUNG: A CASE REPORT
 Original Research Article DOI - 10.26479/2016.0203.10 VARIATION OF FISSURE AND LOBAR PATTERN OF LUNG: A CASE REPORT Adhanom Gebreslassie Berhe, Dr. Peter Ekanem, Hafte Assefa Beyene Department of Anatomy
Original Research Article DOI - 10.26479/2016.0203.10 VARIATION OF FISSURE AND LOBAR PATTERN OF LUNG: A CASE REPORT Adhanom Gebreslassie Berhe, Dr. Peter Ekanem, Hafte Assefa Beyene Department of Anatomy
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Thoracoscopic wedge resection and segmentectomy for smallsized pulmonary nodules
 Perspective on Thoracic Surgery Thoracoscopic wedge resection and segmentectomy for smallsized pulmonary nodules Hirohisa Kato, Hiroyuki Oizumi, Jun Suzuki, Akira Hamada, Hikaru Watarai, Kenta Nakahashi,
Perspective on Thoracic Surgery Thoracoscopic wedge resection and segmentectomy for smallsized pulmonary nodules Hirohisa Kato, Hiroyuki Oizumi, Jun Suzuki, Akira Hamada, Hikaru Watarai, Kenta Nakahashi,
Anatomical Segmentectomy with a Hybrid VATS Approach in a Patient with Intralobar Pulmonary Sequestration after Severe Pneumonia: A Case Report
 THIEME Case Report e21 Anatomical Segmentectomy with a Hybrid VATS Approach in a Patient with Intralobar Pulmonary Sequestration after Severe Pneumonia: A Case Report Soichi Shibuya 1,2 Toru Nakamura 3
THIEME Case Report e21 Anatomical Segmentectomy with a Hybrid VATS Approach in a Patient with Intralobar Pulmonary Sequestration after Severe Pneumonia: A Case Report Soichi Shibuya 1,2 Toru Nakamura 3
ANALYSIS ANATOMY Medical Science, Volume 5, Number 18, February 26, 2014
 ANALYSIS ANATOMY Medical Science, Volume 5, Number 18, February 26, 2014 ISSN 2321 7359 EISSN 2321 7367 Medical Science The International Weekly Journal for Medicine A Study of Pulmonary Vein Variations
ANALYSIS ANATOMY Medical Science, Volume 5, Number 18, February 26, 2014 ISSN 2321 7359 EISSN 2321 7367 Medical Science The International Weekly Journal for Medicine A Study of Pulmonary Vein Variations
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Robotic-assisted right inferior lobectomy
 Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Video-assisted thoracoscopic subsegmentectomy for small-sized pulmonary nodules
 Perspective on Thoracic Surgery Video-assisted thoracoscopic subsegmentectomy for small-sized pulmonary nodules Hirohisa Kato, Hiroyuki Oizumi, Jun Suzuki, Akira Hamada, Hikaru Watarai, Kenta Nakahashi,
Perspective on Thoracic Surgery Video-assisted thoracoscopic subsegmentectomy for small-sized pulmonary nodules Hirohisa Kato, Hiroyuki Oizumi, Jun Suzuki, Akira Hamada, Hikaru Watarai, Kenta Nakahashi,
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
CT Depiction of Regional Nodal Stations for Lung Cancer Staging
 ownloaded from www.ajronline.org by 37.44.204.189 on 11/24/17 from IP address 37.44.204.189. opyright RRS. For personal use only; all rights reserved T epiction of Regional Nodal Stations for Lung ancer
ownloaded from www.ajronline.org by 37.44.204.189 on 11/24/17 from IP address 37.44.204.189. opyright RRS. For personal use only; all rights reserved T epiction of Regional Nodal Stations for Lung ancer
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L.
 Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
A pictorial review of normal anatomical appearences of Pericardial recesses on multislice Computed Tomography.
 A pictorial review of normal anatomical appearences of Pericardial recesses on multislice Computed Tomography. Poster No.: C-1787 Congress: ECR 2012 Type: Educational Exhibit Authors: N. Ahmed 1, G. Avery
A pictorial review of normal anatomical appearences of Pericardial recesses on multislice Computed Tomography. Poster No.: C-1787 Congress: ECR 2012 Type: Educational Exhibit Authors: N. Ahmed 1, G. Avery
Uniportal video-assisted lobectomy through a posterior approach
 Surgical Technique Uniportal video-assisted lobectomy through a posterior approach Francesco Paolo Caronia 1 *, Ettore Arrigo 1, Alfonso Fiorelli 2 * 1 Thoracic Surgery Unit, Istituto Oncologico del Mediterraneo,
Surgical Technique Uniportal video-assisted lobectomy through a posterior approach Francesco Paolo Caronia 1 *, Ettore Arrigo 1, Alfonso Fiorelli 2 * 1 Thoracic Surgery Unit, Istituto Oncologico del Mediterraneo,
Thorax Lecture 2 Thoracic cavity.
 Thorax Lecture 2 Thoracic cavity. Spring 2016 Dr. Maher Hadidi, University of Jordan 1 Enclosed by the thoracic wall. Extends between (thoracic inlet) & (thoracic outlet). Thoracic inlet At root of the
Thorax Lecture 2 Thoracic cavity. Spring 2016 Dr. Maher Hadidi, University of Jordan 1 Enclosed by the thoracic wall. Extends between (thoracic inlet) & (thoracic outlet). Thoracic inlet At root of the
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Learning Curve of a Young Surgeon s Video-assisted Thoracic Surgery Lobectomy during His First Year Experience in Newly Established Institution
 Korean J Thorac Cardiovasc Surg 2012;45:166-170 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Clinical Research http://dx.doi.org/10.5090/kjtcs.2012.45.3.166 Learning Curve of a Young Surgeon s Video-assisted
Korean J Thorac Cardiovasc Surg 2012;45:166-170 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Clinical Research http://dx.doi.org/10.5090/kjtcs.2012.45.3.166 Learning Curve of a Young Surgeon s Video-assisted
Posterior uniportal video-assisted thoracoscopic surgery for anatomical lung resections
 Original Article Posterior uniportal video-assisted thoracoscopic surgery for anatomical lung resections Davor Stamenovic 1, Korkut Bostanci 2, Antje Messerschmidt 1 1 Department of Thoracic Surgery, St.
Original Article Posterior uniportal video-assisted thoracoscopic surgery for anatomical lung resections Davor Stamenovic 1, Korkut Bostanci 2, Antje Messerschmidt 1 1 Department of Thoracic Surgery, St.
Video-assisted thoracoscopic lobectomy using a standardized three-port anterior approach - The Copenhagen experience
 Art of Operative Techniques Video-assisted thoracoscopic lobectomy using a standardized three-port anterior approach - The Copenhagen experience Henrik J. Hansen, René H. Petersen Department of Cardiothoracic
Art of Operative Techniques Video-assisted thoracoscopic lobectomy using a standardized three-port anterior approach - The Copenhagen experience Henrik J. Hansen, René H. Petersen Department of Cardiothoracic
Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line
 L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
minimally invasive techniques
 minimally invasive techniques VATS (Video-Assisted Thoracic Surgery) of Undefined Pulmonary Nodules* Preoperative Evaluation of Videoendoscopic Resectability Christian D. Schwarz, MD; Franz Lenglinger,
minimally invasive techniques VATS (Video-Assisted Thoracic Surgery) of Undefined Pulmonary Nodules* Preoperative Evaluation of Videoendoscopic Resectability Christian D. Schwarz, MD; Franz Lenglinger,
Introduction to Chest CT Interpretation. Objectives 8/28/2017
 Introduction to Chest CT Interpretation Deborah Stein ACNP BC, CCRN NP Education Specialist Department of Anesthesia and Critical Care Medicine August 28, 2017 Objectives Basic Principles Thoracic Anatomy
Introduction to Chest CT Interpretation Deborah Stein ACNP BC, CCRN NP Education Specialist Department of Anesthesia and Critical Care Medicine August 28, 2017 Objectives Basic Principles Thoracic Anatomy
Communicating Vein between the Left Renal Vein and Left Ascending Lumber Vein: Incidence and Significance on Abdominal CT
 YAO ET AL ORIGINAL ARTICLE Radiation Medicine: Vol. 21 No. 6, 252 257 p.p., 2003 Communicating Vein between the Left Renal Vein and Left Ascending Lumber Vein: Incidence and Significance on Abdominal CT
YAO ET AL ORIGINAL ARTICLE Radiation Medicine: Vol. 21 No. 6, 252 257 p.p., 2003 Communicating Vein between the Left Renal Vein and Left Ascending Lumber Vein: Incidence and Significance on Abdominal CT
THE GOOFY ANATOMIST QUIZZES
 THE GOOFY ANATOMIST QUIZZES 7. LUNGS Q1. Fill in the blanks: the lung has lobes and fissures. A. Right, three, two. B. Right, two, one. C. Left, three, two. D. Left, two, three. Q2. The base of the lung
THE GOOFY ANATOMIST QUIZZES 7. LUNGS Q1. Fill in the blanks: the lung has lobes and fissures. A. Right, three, two. B. Right, two, one. C. Left, three, two. D. Left, two, three. Q2. The base of the lung
Surgical resection is the first treatment of choice for
 Predictors of Lymph Node and Intrapulmonary Metastasis in Clinical Stage IA Non Small Cell Lung Carcinoma Kenji Suzuki, MD, Kanji Nagai, MD, Junji Yoshida, MD, Mitsuyo Nishimura, MD, and Yutaka Nishiwaki,
Predictors of Lymph Node and Intrapulmonary Metastasis in Clinical Stage IA Non Small Cell Lung Carcinoma Kenji Suzuki, MD, Kanji Nagai, MD, Junji Yoshida, MD, Mitsuyo Nishimura, MD, and Yutaka Nishiwaki,
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Lab #3. Mohammad Hisham Al-Mohtaseb. Jumana Jihad. Ammar Ramadan. 0 P a g e
 Lab #3 Mohammad Hisham Al-Mohtaseb Jumana Jihad Ammar Ramadan 0 P a g e Last anatomy lab: Lungs and structure on the mediastinal surfs: 1-the right lung: How do we know it s the right lung??? -the 3 lobes
Lab #3 Mohammad Hisham Al-Mohtaseb Jumana Jihad Ammar Ramadan 0 P a g e Last anatomy lab: Lungs and structure on the mediastinal surfs: 1-the right lung: How do we know it s the right lung??? -the 3 lobes
B-I-2 CARDIAC AND VASCULAR RADIOLOGY
 (YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
(YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
ANATOMY OF THE PLEURA. Dr Oluwadiya KS
 ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments
 Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Video-assisted thoracoscopic (VATS) lobectomy has
 Robot-Assisted Lobectomy for Early-Stage Lung Cancer: Report of 100 Consecutive Cases Farid Gharagozloo, MD, Marc Margolis, MD, Barbara Tempesta, MS, CRNP, Eric Strother, LSA, and Farzad Najam, MD Washington
Robot-Assisted Lobectomy for Early-Stage Lung Cancer: Report of 100 Consecutive Cases Farid Gharagozloo, MD, Marc Margolis, MD, Barbara Tempesta, MS, CRNP, Eric Strother, LSA, and Farzad Najam, MD Washington
The technique of VATS right pneumonectomy
 Surgical Technique on Thoracic Surgery The technique of VATS right pneumonectomy Fernando Vannucci 1,2, Arthur Vieira 3, Paula A. Ugalde 3 1 de Janeiro, Brazil; 2 Thoracic Surgery Department, Military
Surgical Technique on Thoracic Surgery The technique of VATS right pneumonectomy Fernando Vannucci 1,2, Arthur Vieira 3, Paula A. Ugalde 3 1 de Janeiro, Brazil; 2 Thoracic Surgery Department, Military
Seventh Edition of the Cancer Staging Manual and Stage Grouping of Lung Cancer. Quick Reference Chart and Diagrams
 CHEST Special Features Seventh Edition of the Cancer Staging Manual and Stage Grouping of Lung Cancer Quick Reference Chart and Diagrams Omar Lababede, MD ; Moulay Meziane, MD ; and Thomas Rice, MD, FCCP
CHEST Special Features Seventh Edition of the Cancer Staging Manual and Stage Grouping of Lung Cancer Quick Reference Chart and Diagrams Omar Lababede, MD ; Moulay Meziane, MD ; and Thomas Rice, MD, FCCP
Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy
 Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy Florian Loehe, MD, Sonja Kobinger, MD, Rudolf A. Hatz, MD, Thomas Helmberger, MD, Udo Loehrs, MD, and Heinrich Fuerst,
Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy Florian Loehe, MD, Sonja Kobinger, MD, Rudolf A. Hatz, MD, Thomas Helmberger, MD, Udo Loehrs, MD, and Heinrich Fuerst,
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
UERMMMC Department of Radiology. Basic Chest Radiology
 UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
Anatomy Lecture 8. In the previous lecture we talked about the lungs, and their surface anatomy:
 Anatomy Lecture 8 In the previous lecture we talked about the lungs, and their surface anatomy: 1-Apex:it lies 1 inch above the medial third of clavicle. 2-Anterior border: it starts from apex to the midpoint
Anatomy Lecture 8 In the previous lecture we talked about the lungs, and their surface anatomy: 1-Apex:it lies 1 inch above the medial third of clavicle. 2-Anterior border: it starts from apex to the midpoint
Dana Alrafaiah. - Moayyad Al-Shafei. -Mohammad H. Al-Mohtaseb. 1 P a g e
 - 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
- 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
Uniportal video-assisted thoracoscopic sleeve lobectomy and other complex resections
 Surgical Technique Uniportal video-assisted thoracoscopic sleeve lobectomy and other complex resections Diego Gonzalez-Rivas,2, Eva Fieira, Maria Delgado, Mercedes de la Torre,2, Lucia Mendez, Ricardo
Surgical Technique Uniportal video-assisted thoracoscopic sleeve lobectomy and other complex resections Diego Gonzalez-Rivas,2, Eva Fieira, Maria Delgado, Mercedes de la Torre,2, Lucia Mendez, Ricardo
Individual Pulmonary Vein Atresia in Adults: Report of Two Cases
 Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
Partial Anomalous Pulmonary Venous Drainage of the Left Upper Lobe vs Duplication of the Superior Vena Cava: Distinction
 375 Partial Anomalous Pulmonary Venous Drainage of the Left Upper Lobe vs Duplication of the Superior Vena Cava: Distinction Based on CT Findings Evan H. Dillon1 OBJECTIVE. Partial lobe Catharine Camputaro2
375 Partial Anomalous Pulmonary Venous Drainage of the Left Upper Lobe vs Duplication of the Superior Vena Cava: Distinction Based on CT Findings Evan H. Dillon1 OBJECTIVE. Partial lobe Catharine Camputaro2
Appearance And Visibility Of The Thoracic Duct On Computed Tomography Of The Chest
 ISPUB.COM The Internet Journal of Radiology Volume 12 Number 2 Appearance And Visibility Of The Thoracic Duct On Computed Tomography Of The Chest J Gossner Citation J Gossner. Appearance And Visibility
ISPUB.COM The Internet Journal of Radiology Volume 12 Number 2 Appearance And Visibility Of The Thoracic Duct On Computed Tomography Of The Chest J Gossner Citation J Gossner. Appearance And Visibility
Reminding the Pulmonary hila: From anatomy to pathology
 Reminding the Pulmonary hila: From anatomy to pathology Poster No.: C-2530 Congress: ECR 2015 Type: Educational Exhibit Authors: D. Roriz, I. Abreu, D. Andrade, P. Belo Soares, F. Caseiro 1 5 1 2 2 3 3
Reminding the Pulmonary hila: From anatomy to pathology Poster No.: C-2530 Congress: ECR 2015 Type: Educational Exhibit Authors: D. Roriz, I. Abreu, D. Andrade, P. Belo Soares, F. Caseiro 1 5 1 2 2 3 3
Signs in Chest Radiology
 Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS
 International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
Division of Diagnostic Imaging, The University of Texas M.D. Anderson Cancer Center, Houston, Texas, USA
 89 Lymphology 28 (1995) 89-94 Division of Diagnostic Imaging, The University of Texas M.D. Anderson Cancer Center, Houston, Texas, USA ABSTRACT The anatomy of the posterior intercostal lymphatics and lymph
89 Lymphology 28 (1995) 89-94 Division of Diagnostic Imaging, The University of Texas M.D. Anderson Cancer Center, Houston, Texas, USA ABSTRACT The anatomy of the posterior intercostal lymphatics and lymph
ROBOT SURGEY AND MINIMALLY INVASIVE TREATMENT FOR LUNG CANCER
 ROBOT SURGEY AND MINIMALLY INVASIVE TREATMENT FOR LUNG CANCER Giulia Veronesi European Institute of Oncology Milan Lucerne, Samo 24 th - 25 th January, 2014 DIAGNOSTIC REVOLUTION FOR LUNG CANCER - Imaging
ROBOT SURGEY AND MINIMALLY INVASIVE TREATMENT FOR LUNG CANCER Giulia Veronesi European Institute of Oncology Milan Lucerne, Samo 24 th - 25 th January, 2014 DIAGNOSTIC REVOLUTION FOR LUNG CANCER - Imaging
LOBAR TORSION FOLLOWING LEFT UPPER LOBECTOMY WITH VATS APPROACH: A CASE REPORT
 CASE REPORT LOBAR TORSION FOLLOWING LEFT UPPER LOBECTOMY WITH VATS APPROACH: A CASE REPORT George Kesov, Deyan Yordanov, Ivan Inkov,1,*, Vasil Yordanov, Teodor Badarov, Rumen Asenov, Aleksandra Dimitrova,
CASE REPORT LOBAR TORSION FOLLOWING LEFT UPPER LOBECTOMY WITH VATS APPROACH: A CASE REPORT George Kesov, Deyan Yordanov, Ivan Inkov,1,*, Vasil Yordanov, Teodor Badarov, Rumen Asenov, Aleksandra Dimitrova,
Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th & 12 th Eds.)
 PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
