Sex - Male Medical Record Number Physician Robert A. M.D. Reason for Visit Elective Pacemaker Replacement. Patient is pacemaker dependent.
|
|
|
- Ronald Dawson
- 5 years ago
- Views:
Transcription
1 Patient Name - Nestor J. Date of Visit Check-In Time 9:45 am. Date of Birth Insurance - Medicare Sex - Male Medical Record Number Physician Robert A. M.D. Reason for Visit Elective Pacemaker Replacement. Patient is pacemaker dependent. Diagnoses: Pacemaker Dependent Hypertension Hyperlipidemia
2 HISTORY HPI - The patient is a very pleasant 88-year-old gentleman status post initial single-chamber ventricular pacemaker insertion 01/10/02, and status post pacemaker generator replacement 02/12/10. Recent testing found that the pacemaker was at elective replacement interval. He is pacemaker dependent. He was referred for pacemaker generator replacement. The indications, risks, benefits of procedure were explained to the patient as well as to his wife and niece. He understood and consented for the operation Past Medical History - Patient also has a history of hypertension, hyperlipemia and past tobacco use. FAMILY HISTORY: Patient s father died of an MI in his 50s and a brother had his first MI and bypass surgery at 54. SOCIAL HISTORY: Patient has smoked tobacco in the past. There is no abuse of alcohol, no use of illicit drugs. ALLERGIES: No allergies to medications. REVIEW OF SYSTEMS: Patient denies a history of stroke, cancer, vomiting up blood, coughing up blood, bright red blood per rectum, bleeding stomach ulcers, renal calculi, cholelithiasis, asthma, emphysema, pneumonia, tuberculosis, home oxygen use or sleep apnea. No morning headaches or fatigue. No psychiatric diagnosis. No psoriasis, no lupus. Electronically signed by Robert A. M.D. on at 9:45 am.
3 PHYSICAL EXAMINATION: GENERAL: Patient is in no acute distress. VITAL SIGNS: Height 5 feet 11 inches, weight 188 pounds, temperature 97.2 degrees Fahrenheit, blood pressure 142/70, pulse 67, respiratory rate 16, and O2 saturation 95% HEENT: Cranium is normocephalic and atraumatic. Patient has moist mucosal membranes. Patient wears a hearing aid. NECK: Veins are not distended. There are no carotid bruits. LUNGS: Clear to auscultation and percussion without wheezes. HEART: S1 and S2, regular rate. No significant murmurs, rubs or gallops. PMI nondisplaced. Patient is pacemaker dependent. ABDOMEN: Soft and non-distended. Bowel sounds present. EXTREMITIES: Without significant clubbing, cyanosis or edema. Pulses grossly intact. Bilateral groins are inspected, status post as the right femoral artery was used for access for the diagnostic cardiac catheterization here and left femoral artery used for PCI. There is no evidence of hematoma or bruit and intact distal pulses. LABORATORY DATA: EKG reviewed which shows the rate of 65 beats per minute and no acute disease. Current Medications Glucosamine 500/400 mg once a day Multivitamin p.o. daily. Nitroglycerin sublingual Toprol-XL 25 mg once a day Aspirin 325 mg once a day. Plavix 75 mg once a day. Diovan 160 mg once a day.
4 Norvasc 5 mg once a day. Lipitor 5 mg once a day. Diagnoses: Pacemaker Dependent Hypertension Hyperlipidemia Electronically signed by Robert A. M.D. on at 9:45 am.
5 OPERATIVE REPORT PROCEDURE: Pacemaker generator replacement PREOPERATIVE DIAGNOSIS: 1. End-of-service with pacemaker generator. 2. Pacemaker dependent. POSTOPERATIVE DIAGNOSIS: 1. End-of-service with pacemaker generator. 2. Pacemaker dependent. PROCEDURE: ANESTHESIA: Pacemaker generator replacement. MAC plus local. ESTIMATED BLOOD LOSS: None. FINDINGS: The explanted pacemaker is a St. Jude Medical model #5136, serial # The chronic right ventricular lead is a St. Jude Medical model # 1246, T/58, serial #CB The implanted pacemaker is a St. Jude Medical Zephyr XL SR, single chamber rate responsive pacemaker, model #5626, serial # Pacing parameters for the right ventricular lead, R-waves were not measured as he is pacemaker dependent, impedance 648 ohms, and pacing threshold 0.4 volts. PROCEDURE IN DETAIL: A time-out was performed prior to start of the operation. The patient was correctly identified as well as the procedure. With the patient under monitored anesthesia care, the patient's left upper chest and neck were prepped with DuraPrep and draped sterilely. A 1% Xylocaine was infiltrated locally over the more superior of the two
6 pacemaker scars. The pacemaker scar was incised. The subcutaneous tissues were divided with electrocautery. The fibrous capsule surrounding the pacemaker generator was opened and the pacemaker explanted. The lead was loosened and removed from the pacemaker generator and quickly attached to the pacemaker cable for pacing and testing, as the patient is pacemaker dependent. Pacing parameters were excellent. The lead was then inserted into the receptacle of the pacemaker generator and tightened down. The pocket was irrigated with antibiotic solution. Hemostasis was good. The generator was inserted into the pocket. The incision was closed in layers with continuous Vicryl sutures including the subcuticular layer. Dermabond and a Coverlet were applied. The patient tolerated the procedure well and there were no complications. Sponge, instruments, and needle counts were correct. The patient was transported to the post-care unit in stable condition. POSTOPERATIVE DIAGNOSIS: 1. End-of-service with pacemaker generator. 2. Pacemaker dependent. Electronically signed by Robert A. M.D. on at 11:45 am.
7 Date Patient Nestor J. Sex M Medical Record Number GENERAL CHEMISTRY TEST RESULT L=Low H = High NORMAL RANGE Sodium 120 L Potassium Chloride 89 L CO2 34 H Glucose 139 H Random BUN 49 H 8-20 Creatinine 1.7 H Calcium 8.4 L Total Protein 4.8 L Albumin 2.1 L Bilirubin Total AST ALT ALK Phos BUN / Creat 29.1 H Ratio Calaculated Osmo KEY - L=Abnormal Low H=Abnormal High UNITS
8 COMPLETE BLOOD COUNT REPORT Patient Name Nestor J. Report Date Medical Record Number Ordering Physician Robert A. COMPLETE BLOOD COUNT TEST NORMAL ABNORMAL FLAG UNITS REFERENCE RANGE WBC RBC HB/Hgb HCT MCV 79 L MCH MCHC R Platelet Count 451 H Mean Platelet Volume WBC DIFFERENTIAL TEST NORMAL ABNORMAL FLAG UNITS REFERENCE RANGE Neutrophil 62 % Lymphocyte 31 % Monocyte 8 % 0-10 Esoinophil 4 % 0-5 Basophil 1 % 0-2 Neutrophil 4.0 K/mcL Absolute Lymphocyte 4.4 K/mcL Absolute Monocyte 0.6 K/mcL Absolute Esosinophil 0.32 K/mcL Absolute Asophil Absolute 0.1 K/mcL KEY - L=Abnormal Low H=Abnormal High ** = Critical Value Contact Physician Immediately
9 RADIOLOGY / NUCLEAR MEDICINE REPORTING INTERPRETATION PROVIDED BY: HITNOTS HEALTH RADIOLOGY GROUP CHEST- ONE VIEW: Patient Nestor J. Sex M Medical Record Number INDICATION: Patient is here for evaluation of possible pneumothorax. Patient had a pacemaker inserted this a.m. Cardiac pacing unit is positioned at the tip of the left axilla with leads extending into the right atrium as well as in the right ventricle. No pneumothorax is visualized. There is a small, unilateral pleural effusion on the left side. Broad pulmonary function is seen bilaterally which may reflect chronic changes or congestive heart failure. No cardiomegaly. IMPRESSION: No pneumothorax status post cardiac pacemaker. No cardiomegaly.
10 Measurments Heart Rate 61 bpm P Duration 77 ms ECG Report PR Interval 155 ms QRS Duration 92 ms QT Interval 386 ms QTc Interval 386 ms P,QRS T Axia 67, 68, 69 Interpretation 004 Normal rhythm 244 Ischemic ST T changes in anterior leads 279 Poor R. Progression in right precordial leads Date Time 10:14 am.
11 OPERATIVE CHECKLIST Patient Nestor J. Sex M Medical Record Number Date Time 10:16am Items to Check Yes No N/A Explain No Answer Initials Pre-op Teaching Seen by Anesthesia ID Band Fall Precaution Band Allergy List / Band N/A Operative Consent H&P EKG CBC Previous Record, if ordered Dentures Removed N/A Eye glasses/ Contacts Removed Hearing Aid Removed Jewelry Removed Hairpieces / Pins Removed Body Piercing Removed Electronically signed by Diane W., RN at 10:02 am on N/A N/A
12 INFORMED CONSENT FOR SURGICAL PROCEDURE It is your doctor s obligation to provide you with the information you need in order to decide whether to consent to the surgery or special procedure that your doctors have recommended. The purpose of this form is to verify that you have received this information and have given your consent to the surgery or special procedure recommended to you. You should be involved in any and all decisions concerning the surgical procedure. Sign this form only after you understand the procedure, the risks, the alternatives, the risks associated with the alternatives, and all of your questions have been answered. Please initial and date directly below this paragraph indicating your understanding of this paragraph. NJ Patient's Initials or Authorized Representative Date Your doctors have recommended the following operation or procedure- Pacemaker Replacement. I, Nestor J. hereby authorize Robert A., MD and any associates or assistants the doctor deems appropriate, to perform a Pacemaker Replacement The risks and benefits associated with the procedure have been explained to me. However, I understand there is no certainty that I will achieve these benefits and no guarantee has been made to me regarding the outcome of the procedure(s). I also authorize the administration of sedation and/or anesthesia as may be deemed advisable or necessary for my comfort, well being and safety. The risks and possible undesirable consequences associated with the procedure have been explained to me including, but not limited to, blood loss, transfusion reactions, infection, heart complications, blood clots, loss of or loss of use of body part or other neurological injury or death. If your doctor determines that there is a reasonable possibility that you may need a blood transfusion as a result of the surgery or procedure to which you are consenting, your doctor will inform you of this and will provide you with information concerning the benefits and risks of the various options for blood transfusion, including pre-donation by yourself or others. You also have the right to have adequate time before your procedure to arrange for pre-donation, but you can waive this right if you do not wish to wait. Transfusion of blood or blood products involves certain risks, including the transmission of disease such as hepatitis or Human Immunodeficiency Virus (HIV), and you have a right to consent or refuse consent to any transfusion. You should discuss any questions that you may have about transfusions with your doctor.
13 INFORMED CONSENT FOR SURGICAL PROCEDURE Page 2. - In permitting my doctor to perform the procedure(s), I understand that unforeseen conditions may be revealed that may necessitate change or extension of the original procedure(s) or a different procedure(s) than those already explained to me. I therefore authorize and request that the abovenamed physician, his assistants, or his designees perform such procedure(s) as necessary and desirable in the exercise of his/her professional judgment. The reasonable alternative(s) to the procedure(s) have been explained to me. I hereby authorize my doctor to utilize or dispose of removed tissues, parts or organs resulting from the procedure(s) authorized above. I consent to any photographing or videotaping of the procedure(s) that may be performed, provided my identity is not revealed by the pictures or by descriptive texts accompanying them. I also consent to the admittance of students or authorized equipment representatives to the procedure room for purposes of advancing medical education or obtaining important product information. As required by the Safe Medical Device Act, I consent to the release of my name, address, and social security number to the manufacturer of any medical device I receive. By signing below, I am indicating that I have had an opportunity to ask the doctor all questions concerning risks, alternatives, and risks of those alternatives. Date_ Signature Nestor J. AUTHORIZED REPRESENTATIVE: The Patient/Authorized Representative states that he/she understands this information and has no further questions. Electronically signed on 6/2/2016 at 5:03 pm CERTIFICATION OF PHYSICIAN: I hereby certify that the facts, risks, the risks associated with the alternatives of the procedure(s) described in this form have been discussed with the individual granting consent. In addition, I have answered any questions asked of me.
14 DISCHARGE INSTRUCTIONS PACEMAKER INSERTION Wound Care - You should be able to get back to your normal activities in 2 to 4 days. For 2 to 3 weeks, do not lift anything heavier than 10 to 15 pounds. Also, do not push, pull or twist too much. Do not lift your arm above your shoulder for several weeks. DO NOT wear clothes that rub on the wound for 2 or 3 weeks. Keep your incision completely dry for 5 days. Take sponge baths. Do not submerge incision into any water. After 5 days, you may take a shower and then pat the area dry. Always wash your hands before touching the wound. Follow-up - Your physician will tell you how often you will need to have your pacemaker checked. In most cases, it will be every 6 months to a year. The exam will take about 15 to 30 minutes. The batteries in your pacemaker should last 6 to 15 years. Regular checkups can detect if the battery is wearing down or if there are any problems with the leads (wires). Your provider will change both the generator and battery when the battery gets low. When to Call the Doctor - Call your physician if: Your wound looks infected (redness, increased drainage or pus, swelling, pain). You have an odor coming from the incision. You have openings at the edges of the incision. You have a temperature. You are having the symptoms you had before the pacemaker was implanted. You feel dizzy or short of breath. You have chest pain.
15 There are no stitches that need to be removed. Steri-strips of tape will begin to fall off in about days. Your incision should begin to look better every day. Call your physician if you have any questions. Be sure that you have the phone number of your physician s office. I have received the discharge instructions, and had an opportunity to ask any questions for clarification. Nestor J Patient Signature Date Diane H. RN Witness Signature Date
16 This medical record information is being used for study and is totally fictitious. Any similarity to a real person, living or dead, is incidental. The medical content of this record may not be totally clinically accurate, and therefore should not be used as an example for diagnosis or treatment.
Insurance Cigna Date of Birth- 08/09/1949. Preferred Language - English Emergency Contact Mary J. (Wife) Phone (555)
 Visit Type Ambulatory Surgery Patient Name Marquis J. Date of Visit - 2/1/2017 Time 12:15 p.m. Insurance Cigna Date of Birth- 08/09/1949 Medical Record # 05-16-31 Sex Male Marital Status - Married Preferred
Visit Type Ambulatory Surgery Patient Name Marquis J. Date of Visit - 2/1/2017 Time 12:15 p.m. Insurance Cigna Date of Birth- 08/09/1949 Medical Record # 05-16-31 Sex Male Marital Status - Married Preferred
I,, hereby authorize Dr. and any associates or assistants the doctor deems appropriate, to perform removal of the adjustable gastric band surgery.
 INFORMED CONSENT FOR LAPAROSCOPIC ADJUSTABLE BAND REMOVAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
INFORMED CONSENT FOR LAPAROSCOPIC ADJUSTABLE BAND REMOVAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
INFORMED CONSENT REDUCTION MAMMAPLASTY
 INFORMED CONSENT REDUCTION MAMMAPLASTY INSTRUCTIONS This is an informed-consent document that has been prepared to help your plastic surgeon inform you abut reduction mammaplasty surgery, its risks, and
INFORMED CONSENT REDUCTION MAMMAPLASTY INSTRUCTIONS This is an informed-consent document that has been prepared to help your plastic surgeon inform you abut reduction mammaplasty surgery, its risks, and
Patient Encounters in the Primary Care Setting
 Patient Encounters in the Primary Care Setting Carmine D Amico, D.O. Clinical Cases Overview Learning objectives Clinical case presentations Questions for audience participation 1 Clinical Cases Learning
Patient Encounters in the Primary Care Setting Carmine D Amico, D.O. Clinical Cases Overview Learning objectives Clinical case presentations Questions for audience participation 1 Clinical Cases Learning
Med 536 Communicating About Prognosis Workshop. Case 2
 Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
CARDIOVASCULAR CASE-BASED SMALL GROUP DISCUSSION
 MHD I Session VIII Student Copy Page 1 CARDIOVASCULAR CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION VIII OCTOBER 22, 2014 STUDENT COPY MHD I Session VIII Student Copy Page 2 Case 1 Chief Complaint I
MHD I Session VIII Student Copy Page 1 CARDIOVASCULAR CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION VIII OCTOBER 22, 2014 STUDENT COPY MHD I Session VIII Student Copy Page 2 Case 1 Chief Complaint I
There are different types of ICDs:
 Guidelines for Patients with Implantable Devices o Implantable Cardioverter Defibrillator (ICD) Your ICD is approximately the size of a pager and includes the following parts: The ICD: A battery powered
Guidelines for Patients with Implantable Devices o Implantable Cardioverter Defibrillator (ICD) Your ICD is approximately the size of a pager and includes the following parts: The ICD: A battery powered
INFORMED CONSENT EXTREMITY TUMOR REMOVAL SURGERY
 . Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
Documentation Dissection
 History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
Kadlec Regional Medical Center Cardiac Electrophysiology
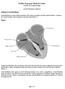 Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
ALTERNATIVE TREATMENTS
 INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you of otoplasty surgery, its risks, as well as alternative treatments. It is important that you read this information
INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you of otoplasty surgery, its risks, as well as alternative treatments. It is important that you read this information
Kadlec Regional Medical Center Cardiac Electrophysiology
 Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
INFORMED CONSENT TRIGGER FINGER SURGERY
 . Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
About Your Ventricular Assist Device (VAD) Surgery
 About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
X-Plain Pacemaker Reference Summary
 X-Plain Pacemaker Reference Summary Introduction A pacemaker is a device that regulates the heart beat. More than half a million Americans use a pacemaker. If your doctor recommends that you have a pacemaker,
X-Plain Pacemaker Reference Summary Introduction A pacemaker is a device that regulates the heart beat. More than half a million Americans use a pacemaker. If your doctor recommends that you have a pacemaker,
INFORMED-CONSENT - OTOPLASTY SURGERY
 INFORMED-CONSENT - OTOPLASTY SURGERY INSTRUCTIONS This is an informed consent document that has been prepared to help inform you of otoplasty surgery, as well as alternative treatments. It is important
INFORMED-CONSENT - OTOPLASTY SURGERY INSTRUCTIONS This is an informed consent document that has been prepared to help inform you of otoplasty surgery, as well as alternative treatments. It is important
Note for Jane Doe on 02/10/ Chart 3642
 Note for Jane Doe on 02/10/2005 - Chart 3642 Consultation was requested by Dr. Smith Chief Complaint (1/1): This 31 year old Caucasian female presents today for evaluation of chest pain. Chest pains HPI:
Note for Jane Doe on 02/10/2005 - Chart 3642 Consultation was requested by Dr. Smith Chief Complaint (1/1): This 31 year old Caucasian female presents today for evaluation of chest pain. Chest pains HPI:
CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I. October 14, 2015
 Session 6, MHD I, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I October 14, 2015 Helpful Resources McPhee, SJ, Hammer GD. Pathophysiology of Disease: An Introduction to Clinical
Session 6, MHD I, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I October 14, 2015 Helpful Resources McPhee, SJ, Hammer GD. Pathophysiology of Disease: An Introduction to Clinical
INFORMED CONSENT FOR SLEEVE GASTRECTOMY
 INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT
 Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT Instructions This is an informed consent document that has been prepared to assist your plastic surgeon
Dr. James B. Lowe Plastic Surgery ORAL SOFT TISSUE SURGERY INFORMATION SHEET AND INFORMED CONSENT Instructions This is an informed consent document that has been prepared to assist your plastic surgeon
ANY FAMILY HISTORY OF ANEURYSM OR DVT?
 NAME: D/O/B: DATE: MR# WHAT PROBLEM(S) BRINGS YOU HERE TODAY? WHO SENT YOU TO US? DOCTOR/OTHER WHICH DOCTOR? WHAT SURGERY HAVE YOU HAD AND WHEN? (LIST) 1. 2. 3. 4. 5. 6. 7. HOW MUCH ALCOHOL DO YOU DRINK
NAME: D/O/B: DATE: MR# WHAT PROBLEM(S) BRINGS YOU HERE TODAY? WHO SENT YOU TO US? DOCTOR/OTHER WHICH DOCTOR? WHAT SURGERY HAVE YOU HAD AND WHEN? (LIST) 1. 2. 3. 4. 5. 6. 7. HOW MUCH ALCOHOL DO YOU DRINK
* Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by
 Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
INFORMED CONSENT OTOPLASTY SURGERY
 2005 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use
2005 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use
You and your pacemaker
 You and your pacemaker You and your pacemaker Why do I need a pacemaker? A pacemaker will help improve your heart s rate. It is used to help your heart beat at a normal rate. What is a pacemaker? A pacemaker
You and your pacemaker You and your pacemaker Why do I need a pacemaker? A pacemaker will help improve your heart s rate. It is used to help your heart beat at a normal rate. What is a pacemaker? A pacemaker
INFORMED CONSENT REDUCTION MAMMAPLASTY
 Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Atrial Fibrillation. Damage to your heart caused by a heart attack or rheumatic heart disease
 Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Rural STEMI System of Care Success. Nicole Huber, PA-C Cumberland Healthcare Emergency Department
 Rural STEMI System of Care Success Nicole Huber, PA-C Cumberland Healthcare Emergency Department DISCLOSURES I HAVE NO ACTUAL OR POTENTIAL CONFLICT OF INTEREST IN RELATION TO THIS PRESENTATION Ideal Process
Rural STEMI System of Care Success Nicole Huber, PA-C Cumberland Healthcare Emergency Department DISCLOSURES I HAVE NO ACTUAL OR POTENTIAL CONFLICT OF INTEREST IN RELATION TO THIS PRESENTATION Ideal Process
Cardiac Catheterization
 Cardiac Catheterization What is cardiac catheterization? Cardiac catheterization is a procedure used to diagnose and treat cardiovascular conditions. During cardiac catheterization, a long thin tube called
Cardiac Catheterization What is cardiac catheterization? Cardiac catheterization is a procedure used to diagnose and treat cardiovascular conditions. During cardiac catheterization, a long thin tube called
Occupation Agency Code Work Location Work Supervisor Duty tel. #
 PRIVACY ACT STATEMENT: This information is subject to the Privacy Act of 1974 (5 U.S.C. Section 552a). This information may be provided to appropriate Government agencies when relevant to civil, criminal
PRIVACY ACT STATEMENT: This information is subject to the Privacy Act of 1974 (5 U.S.C. Section 552a). This information may be provided to appropriate Government agencies when relevant to civil, criminal
Transcatheter Aortic Valve Replacement (TAVR)
 Transcatheter Aortic Valve Replacement (TAVR) Welcome to the Sanford Health Heart Clinic. It is a privilege to care for you. Your doctor has told you that you may need to have a TAVR procedure. TAVR stands
Transcatheter Aortic Valve Replacement (TAVR) Welcome to the Sanford Health Heart Clinic. It is a privilege to care for you. Your doctor has told you that you may need to have a TAVR procedure. TAVR stands
INFORMED-CONSENT LOWER BODY LIFT SURGERY
 INFORMED-CONSENT LOWER BODY LIFT SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help your plastic surgeon inform you of Lower Body Lift surgery, its risks, as well
INFORMED-CONSENT LOWER BODY LIFT SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help your plastic surgeon inform you of Lower Body Lift surgery, its risks, as well
Interventional Pain Medicine. P. Tennent Slack, M.D. Dr. Greg Jackson, M.D. Ben Fleming, PA-C
 Interventional Pain Medicine P. Tennent Slack, M.D. Dr. Greg Jackson, M.D. Ben Fleming, PA-C Gainesville Braselton Medical Park 1, Suite 300 Medical Plaza B, Suite 402 1315 Jesse Jewell Parkway 1404 River
Interventional Pain Medicine P. Tennent Slack, M.D. Dr. Greg Jackson, M.D. Ben Fleming, PA-C Gainesville Braselton Medical Park 1, Suite 300 Medical Plaza B, Suite 402 1315 Jesse Jewell Parkway 1404 River
PATIENTS DEMOGRAPHICS
 PATIENTS DEMOGRAPHICS Date: First Name MI Last Name Sex: M or F (Circle one) Age: Address: City: State: Zip Code: Home Telephone: Work Telephone: Cell/Pager No: Date of Birth: Single: Married: Social Security
PATIENTS DEMOGRAPHICS Date: First Name MI Last Name Sex: M or F (Circle one) Age: Address: City: State: Zip Code: Home Telephone: Work Telephone: Cell/Pager No: Date of Birth: Single: Married: Social Security
Total Shoulder Replacement Patient Guide
 About Your Surgery and Recovery WELCOME This booklet has been designed to answer your questions about what to expect if you will need surgery. I truly hope that this will make your surgery an easier and
About Your Surgery and Recovery WELCOME This booklet has been designed to answer your questions about what to expect if you will need surgery. I truly hope that this will make your surgery an easier and
relieve pressure on the lungs treat symptoms such as shortness of breath and pain determine the cause of excess fluid in the pleural space.
 Scan for mobile link. Thoracentesis Thoracentesis uses imaging guidance and a needle to help diagnose and treat pleural effusions, a condition in which the space between the lungs and the inside of the
Scan for mobile link. Thoracentesis Thoracentesis uses imaging guidance and a needle to help diagnose and treat pleural effusions, a condition in which the space between the lungs and the inside of the
Care of Your Child with a Pacemaker
 Patient and Family Education Care of Your Child with a Pacemaker A pacemaker watches for slow heart rates. It can send signals to make the heart beat. Here is how to take care of your child s pacemaker.
Patient and Family Education Care of Your Child with a Pacemaker A pacemaker watches for slow heart rates. It can send signals to make the heart beat. Here is how to take care of your child s pacemaker.
Name of Pa. tient: Last. First. per day) 50 mg. X-ray dye or. IV contract. Name (Last) (First) Address. City, state/ zip code
 Division of Cardiology for the Academic Medical Center of the University of Texas Medical School at Houston NEW PATIENT HISTORY FORM Please complete and fax to 713-512-2245 Name of Pa tient: Last _ First
Division of Cardiology for the Academic Medical Center of the University of Texas Medical School at Houston NEW PATIENT HISTORY FORM Please complete and fax to 713-512-2245 Name of Pa tient: Last _ First
UNDERSTANDING PACEMAKERS
 UNDERSTANDING PACEMAKERS Living Well with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at the right speed. Problems with this system can make your heart
UNDERSTANDING PACEMAKERS Living Well with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at the right speed. Problems with this system can make your heart
INFORMED-CONSENT-REDUCTION MAMMAPLASTY
 INFORMED-CONSENT-REDUCTION MAMMAPLASTY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
INFORMED-CONSENT-REDUCTION MAMMAPLASTY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Nipple reconstruction may be performed as a single surgical procedure, or combined with other breast reconstruction procedures.
 INSTRUCTIONS This informed-consent document has been prepared to help inform you about nipple reconstruction surgery, its risks, and alternative treatment(s). It is important that you read this information
INSTRUCTIONS This informed-consent document has been prepared to help inform you about nipple reconstruction surgery, its risks, and alternative treatment(s). It is important that you read this information
BREAST REDUCTION. Based on my discussions with Dr Gutowski, I understand and agree to the following:
 INFORMED CONSENT FOR BREAST REDUCTION PLEASE REVIEW AND BRING WITH YOU ON THE DAY OF YOUR PROCEDURE PATIENT NAME Based on my discussions with Dr Gutowski, I understand and agree to the following: Dr. Gutowski
INFORMED CONSENT FOR BREAST REDUCTION PLEASE REVIEW AND BRING WITH YOU ON THE DAY OF YOUR PROCEDURE PATIENT NAME Based on my discussions with Dr Gutowski, I understand and agree to the following: Dr. Gutowski
Chapter 1. Perioperative Evaluation and Management of Surgical Patients. Oral Exam Questions
 Chapter 1 Perioperative Evaluation and Management of Surgical Patients Oral Exam Questions Case 1 A 62-year-old man with a PMH significant for hypertension, and a 40-pack-year history of smoking is found
Chapter 1 Perioperative Evaluation and Management of Surgical Patients Oral Exam Questions Case 1 A 62-year-old man with a PMH significant for hypertension, and a 40-pack-year history of smoking is found
KNEE ARTHROSCOPY SURGERY
 KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
INFORMED CONSENT GYNAECOMASTIA SURGERY
 INFORMED CONSENT GYNAECOMASTIA SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning gynaecomastia (male breast reduction) surgery, its risks, as
INFORMED CONSENT GYNAECOMASTIA SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning gynaecomastia (male breast reduction) surgery, its risks, as
RISK REVIEW & PHYSICIAN APPROVAL FORM
 RISK REVIEW & PHYSICIAN APPROVAL FORM Burke Restorative Neurology Clinic is offering services meant to target community members with neurological impairments. The program is supervised by medical professionals
RISK REVIEW & PHYSICIAN APPROVAL FORM Burke Restorative Neurology Clinic is offering services meant to target community members with neurological impairments. The program is supervised by medical professionals
Anesthesia Preoperative Patient History
 Anesthesia Preoperative Patient History Please Complete and BRING WITH YOU to Your Anesthesia Appointment Patient Name: Date of Birth: Phone Number: Kind of Surgery You are Having: Date of Your Surgery:
Anesthesia Preoperative Patient History Please Complete and BRING WITH YOU to Your Anesthesia Appointment Patient Name: Date of Birth: Phone Number: Kind of Surgery You are Having: Date of Your Surgery:
UW MEDICINE PATIENT EDUCATION. Treatment for blocked heart arteries DRAFT. What are arteries? How do heart arteries become blocked?
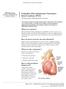 UW MEDICINE PATIENT EDUCATION Complex Percutaneous Coronary Intervention (PCI) Treatment for blocked heart arteries This handout explains complex percutaneous intervention (PCI) treatment of a coronary
UW MEDICINE PATIENT EDUCATION Complex Percutaneous Coronary Intervention (PCI) Treatment for blocked heart arteries This handout explains complex percutaneous intervention (PCI) treatment of a coronary
Patient Health History
 Patient Health History This information is very important in your care. Please complete as carefully and accurately as possible. Name: Date: Height: inches Weight: lbs Age: Symptoms: 1. Type of symptoms
Patient Health History This information is very important in your care. Please complete as carefully and accurately as possible. Name: Date: Height: inches Weight: lbs Age: Symptoms: 1. Type of symptoms
Patient s guide to surgery
 Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
Patient s guide to surgery Surgery date: Time for arrival will be given a day before surgery Please make a pre-operative appointment at the hospital. Remember to take the preoperative paperwork with you
Gynecomastia Consent. Gynecomastia Surgery (Male Breast Reduction)
 Gynecomastia Consent 1. I hereby authorize Dr. Stratis and such assistants as may be selected to perform the following procedure or treatment: Gynecomastia Surgery (Male Breast Reduction) I have received
Gynecomastia Consent 1. I hereby authorize Dr. Stratis and such assistants as may be selected to perform the following procedure or treatment: Gynecomastia Surgery (Male Breast Reduction) I have received
CHOLECYSTECTOMY CONSENT FORM
 1 of 6 Patient Name: I, have been asked to carefully read all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described
1 of 6 Patient Name: I, have been asked to carefully read all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described
Pacemaker Therapy (PPM)
 Patient information Pacemaker Therapy (PPM) i Important information for all patients requiring pacemaker therapy. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Patient information Pacemaker Therapy (PPM) i Important information for all patients requiring pacemaker therapy. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion
 Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion Cervical Corpectomy is intended for the surgical correction and stabilization of the spine where vertebral bone removal is necessary.
Cervical Corpectomy (Vertebral Body Replacement) and Spinal Fusion Cervical Corpectomy is intended for the surgical correction and stabilization of the spine where vertebral bone removal is necessary.
OTOPLASTY (EAR RESHAPING)
 INFORMED CONSENT FOR OTOPLASTY (EAR RESHAPING) PLEASE REVIEW AND BRING WITH YOU ON THE DAY OF YOUR PROCEDURE PATIENT NAME KAROL A. GUTOWSKI, MD, FACS AESTHETIC SURGERY CERTIFIED BY THE AMERICAN BOARD OF
INFORMED CONSENT FOR OTOPLASTY (EAR RESHAPING) PLEASE REVIEW AND BRING WITH YOU ON THE DAY OF YOUR PROCEDURE PATIENT NAME KAROL A. GUTOWSKI, MD, FACS AESTHETIC SURGERY CERTIFIED BY THE AMERICAN BOARD OF
INFORMED CONSENT MEDIAL THIGH LIFT SURGERY
 INFORMED CONSENT MEDIAL THIGH LIFT SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning medial thigh lift surgery, its risks, as well as alternative
INFORMED CONSENT MEDIAL THIGH LIFT SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning medial thigh lift surgery, its risks, as well as alternative
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
You or your child has been scheduled for Tympanomastoidectomy and/or Ossicular Chain Reconstruction.
 Low Country ENT is happy you have chosen us to assist you and your family in obtaining your healthcare needs. The following packet is to help you further understand your future surgical procedure as well
Low Country ENT is happy you have chosen us to assist you and your family in obtaining your healthcare needs. The following packet is to help you further understand your future surgical procedure as well
Patient to complete this information
 Patient to complete this information Patient s Name Birth date Today s date Referring Physician Primary Care Physician Age Occupation Retired, how long? Prior operations Medications Type Date Name Dose
Patient to complete this information Patient s Name Birth date Today s date Referring Physician Primary Care Physician Age Occupation Retired, how long? Prior operations Medications Type Date Name Dose
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP
 INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT GYNECOMASTIA SURGERY
 Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Subject ID: I N D # # U A * Consent Date: Day Month Year
 IND Study # Eligibility Checklist Pg 1 of 15 Instructions: Check the appropriate box for each Inclusion and Exclusion Criterion below. Each criterion must be marked and all protocol criteria have to be
IND Study # Eligibility Checklist Pg 1 of 15 Instructions: Check the appropriate box for each Inclusion and Exclusion Criterion below. Each criterion must be marked and all protocol criteria have to be
INFORMED CONSENT - NASAL INJURY REPAIR SURGERY
 Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
A separate consent form for the use of breast implants in conjunction with mastopexy is necessary.
 INFORMED-CONSENT-BREAST LIFT (MASTOPEXY) INSTRUCTIONS This is an informed-consent document that has been prepared to help your plastic surgeon inform you about mastopexy surgery, its risks, and alternative
INFORMED-CONSENT-BREAST LIFT (MASTOPEXY) INSTRUCTIONS This is an informed-consent document that has been prepared to help your plastic surgeon inform you about mastopexy surgery, its risks, and alternative
SMALL GROUP DISCUSSION
 MHD II, Seesion II Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session II JANUARY 15, 2014 Recent Review highlighting disease process in Case 2: Fasano A, Catassi, C. NEJM 2012; 367: 2419-26 STUDENT
MHD II, Seesion II Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session II JANUARY 15, 2014 Recent Review highlighting disease process in Case 2: Fasano A, Catassi, C. NEJM 2012; 367: 2419-26 STUDENT
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery
 Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Informed consent Ganglion cyst surgery
 Informed consent Ganglion cyst surgery Instructions This is an informed-consent document that has been prepared to help inform you of ganglion cyst surgery, its risks, as well as alternative treatments.
Informed consent Ganglion cyst surgery Instructions This is an informed-consent document that has been prepared to help inform you of ganglion cyst surgery, its risks, as well as alternative treatments.
CONSENT FOR GYNECOMASTIA
 CONSENT FOR GYNECOMASTIA Gynecomastia surgery is a procedure to remove excess fat, glandular tissue and/or skin from overdeveloped or enlarged male breasts. In severe cases of gynecomastia, the weight
CONSENT FOR GYNECOMASTIA Gynecomastia surgery is a procedure to remove excess fat, glandular tissue and/or skin from overdeveloped or enlarged male breasts. In severe cases of gynecomastia, the weight
ALTERNATIVE TREATMENT
 INFORMED CONSENT LIPOSUCTION (SUCTION- ASSISTED LIPECTOMY SURGERY) (ULTRASOUND- ASSISTED LIPECTOMY SURGERY) (LASER ASSISTED LIPOSUCTION SURGERY) INSTRUCTIONS This is an informed- consent document that
INFORMED CONSENT LIPOSUCTION (SUCTION- ASSISTED LIPECTOMY SURGERY) (ULTRASOUND- ASSISTED LIPECTOMY SURGERY) (LASER ASSISTED LIPOSUCTION SURGERY) INSTRUCTIONS This is an informed- consent document that
SMALL GROUP DISCUSSION
 MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
MEDIAL THIGHPLASTY CONSENT
 INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning medial thigh lift surgery, its risks, as well as alternative treatment(s). It is important that you
INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning medial thigh lift surgery, its risks, as well as alternative treatment(s). It is important that you
Patient Name Date of Birth MALE / FEMALE Date. Left handed or Right handed. Marital Status: Single Married Divorced Widowed Children?
 PH NEW PATIENT HISTORY Patient Name Date of Birth MALE / FEMALE Date Occupation: Left handed or Right handed Marital Status: Single Married Divorced Widowed Children? Y or N # Previous Treating Physician:
PH NEW PATIENT HISTORY Patient Name Date of Birth MALE / FEMALE Date Occupation: Left handed or Right handed Marital Status: Single Married Divorced Widowed Children? Y or N # Previous Treating Physician:
ÇENE PROTEZ AMELİYATI İNGİLİZCE BİLGİLENDİRİLMİŞ ONAM FORMU
 Sayfa No: 5/1 INFORMED CONSENT Chin Augmentation with Silicone Implant INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you about Chin Augmentation surgery, its risks,
Sayfa No: 5/1 INFORMED CONSENT Chin Augmentation with Silicone Implant INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you about Chin Augmentation surgery, its risks,
INFORMED CONSENT GYNECOMASTIA SURGERY INSTRUCTIONS
 INFORMED CONSENT GYNECOMASTIA SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning gynecomastia (male breast reduction) surgery, its risks, as
INFORMED CONSENT GYNECOMASTIA SURGERY INSTRUCTIONS This is an informed-consent document that has been prepared to help inform you concerning gynecomastia (male breast reduction) surgery, its risks, as
New Patient Documentation. Name: (Last) (First) (Middle) Address: (Street) (Apt#) (City) (State) (Zip) Home Phone: ( ) Cell: ( ) Work: ( )
 New Patient Documentation Name: (Last) (First) (Middle) Address: (Street) (Apt#) (City) (State) (Zip) Home Phone: ( ) Cell: ( ) Work: ( ) Age: Birthdate: E Email: Social: Sex: Male Female Height: Weight:
New Patient Documentation Name: (Last) (First) (Middle) Address: (Street) (Apt#) (City) (State) (Zip) Home Phone: ( ) Cell: ( ) Work: ( ) Age: Birthdate: E Email: Social: Sex: Male Female Height: Weight:
MHD I SESSION X. Renal Disease
 MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
3855 Burton Street SE Suite A, Grand Rapids, MI Phone Fax Patient Information. Address: City: State: Zip:
 3855 Burton Street SE Suite A, Grand Rapids, MI 49546 Phone 616.323.3102 Fax 616.323.3061 Patient Information Patient Name: Preferred Language: Address: City: State: Zip: Home Phone: Cell Phone: Cell Carrier:
3855 Burton Street SE Suite A, Grand Rapids, MI 49546 Phone 616.323.3102 Fax 616.323.3061 Patient Information Patient Name: Preferred Language: Address: City: State: Zip: Home Phone: Cell Phone: Cell Carrier:
Implantation of an Implantable Cardioverter Defibrillator (ICD)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an Implantable? Your doctor has recommended that you have an Implantable.
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an Implantable? Your doctor has recommended that you have an Implantable.
Dr. Nuelle Knee Replacement: Discharge Care Instructions
 Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
M F HOME ADDRESS CITY STATE ZIP CODE MARITAL STATUS SINGLE MARRIED DIVORCED WIDOWED PREFERRED PHONE NUMBER TO BE CONTACTED
 PRESENT ILLNESS INFORMATION INSURANCE PATIENT HISTORY AND PHYSICAL APPOINTMENT DATE: NAME-LAST FIRST M.I. DATE OF BIRTH AGE SEX SOCIAL SECURITY NO. M F HOME ADDRESS CITY STATE ZIP CODE MARITAL STATUS SINGLE
PRESENT ILLNESS INFORMATION INSURANCE PATIENT HISTORY AND PHYSICAL APPOINTMENT DATE: NAME-LAST FIRST M.I. DATE OF BIRTH AGE SEX SOCIAL SECURITY NO. M F HOME ADDRESS CITY STATE ZIP CODE MARITAL STATUS SINGLE
Consent for NIL (Tickle Liposuction) and BodyTite
 Consent for NIL (Tickle Liposuction) and BodyTite I authorize a Zelko Aesthetic surgeon to perform Liposuction on me using the Nutational Infrasonic Liposuction (NIL) (aka Tickle Lipo) to facilitate the
Consent for NIL (Tickle Liposuction) and BodyTite I authorize a Zelko Aesthetic surgeon to perform Liposuction on me using the Nutational Infrasonic Liposuction (NIL) (aka Tickle Lipo) to facilitate the
R. John Brewer EMT-P Dental Education Inc. PATIENT ASSESSMENT
 R. John Brewer EMT-P Dental Education Inc. PATIENT ASSESSMENT Patient Assessment Patient assessment is made up of two parts - History - Physical Exam Patient assessment In medical cases obtaining an adequate
R. John Brewer EMT-P Dental Education Inc. PATIENT ASSESSMENT Patient Assessment Patient assessment is made up of two parts - History - Physical Exam Patient assessment In medical cases obtaining an adequate
Laparoscopy. What is Laparoscopy? Why is this surgery used? How do I prepare for surgery?
 What is? Laparoscopic surgery is where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the belly button. To help with the surgery,
What is? Laparoscopic surgery is where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the belly button. To help with the surgery,
Diagnostic Laparoscopy
 PATIENT & CAREGIVER EDUCATION Diagnostic Laparoscopy This information describes your diag nostic laparoscopy. About Your Diagnostic Laparoscopy A diag nostic laparoscopy is a minimally invasive procedure.
PATIENT & CAREGIVER EDUCATION Diagnostic Laparoscopy This information describes your diag nostic laparoscopy. About Your Diagnostic Laparoscopy A diag nostic laparoscopy is a minimally invasive procedure.
KAROL A. GUTOWSKI, MD, FACS AESTHETIC SURGERY CERTIFIED BY THE AMERICAN BOARD OF PLASTIC SURGERY MEMBER AMERICAN SOCIETY OF PLASTIC SURGEONS
 INFORMED CONSENT FOR SKIN LESION AND SOFT TISSUE MASS REMOVAL WITH PATHOLOGY EVALUATION WITHOUT PATHOLOGY EVALUATION PLEASE REVIEW AND BRING WITH YOU ON THE DAY OF YOUR PROCEDURE PATIENT NAME KAROL A.
INFORMED CONSENT FOR SKIN LESION AND SOFT TISSUE MASS REMOVAL WITH PATHOLOGY EVALUATION WITHOUT PATHOLOGY EVALUATION PLEASE REVIEW AND BRING WITH YOU ON THE DAY OF YOUR PROCEDURE PATIENT NAME KAROL A.
What to expect when having a pacemaker implantation
 What to expect when having a pacemaker implantation Cardiology Department Patient information leaflet What is a pacemaker? A pacemaker is a small metal device which contains an electronic circuit and a
What to expect when having a pacemaker implantation Cardiology Department Patient information leaflet What is a pacemaker? A pacemaker is a small metal device which contains an electronic circuit and a
INFORMED CONSENT SKIN GRAFT SURGERY
 Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Guide to Cardiology Care at Scripps
 Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you.
 Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
Cardiac Catheterization Lab Procedures
 Patient Education Cardiac Catheterization Lab Procedures This booklet describes cardiac catheterization. It also details how to prepare for the procedure and the care needed after it is done. Before You
Patient Education Cardiac Catheterization Lab Procedures This booklet describes cardiac catheterization. It also details how to prepare for the procedure and the care needed after it is done. Before You
Respiratory Questionnaire
 Respiratory Questionnaire Date: Name: SS#: Sex: M F Height: Weight: DOB: Age: Employer: Department: Job Title: Phone # where you can be reached regarding this questionnaire (include area code): What is
Respiratory Questionnaire Date: Name: SS#: Sex: M F Height: Weight: DOB: Age: Employer: Department: Job Title: Phone # where you can be reached regarding this questionnaire (include area code): What is
INFORMED CONSENT - BREAST LIFT (MASTOPEXY)
 Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only. All
relieve pressure on the lungs treat symptoms such as shortness of breath and pain determine the cause of excess fluid in the pleural space.
 Scan for mobile link. Chest Interventions What are Chest Interventions? Chest interventions are minimally invasive procedures used to diagnose and treat pleural effusions, a condition in which there is
Scan for mobile link. Chest Interventions What are Chest Interventions? Chest interventions are minimally invasive procedures used to diagnose and treat pleural effusions, a condition in which there is
INFORMED CONSENT FOR GASTRIC BALLOON INSERTION
 INFORMED CONSENT FOR GASTRIC BALLOON INSERTION This informed consent document has been prepared to help inform you about the Gastric Balloon Insertion procedure including the risks and benefits, as well
INFORMED CONSENT FOR GASTRIC BALLOON INSERTION This informed consent document has been prepared to help inform you about the Gastric Balloon Insertion procedure including the risks and benefits, as well
INFORMED-CONSENT-ABDOMINOPLASTY SURGERY
 INFORMED-CONSENT-ABDOMINOPLASTY SURGERY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein
INFORMED-CONSENT-ABDOMINOPLASTY SURGERY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein
Pre-Admission Testing Questionnaire
 Pre-Admission Testing Questionnaire Approximately 2 weeks prior to your surgery date you will receive a telephone call from our Pre-Admission Testing department. During this conversation, a Registered
Pre-Admission Testing Questionnaire Approximately 2 weeks prior to your surgery date you will receive a telephone call from our Pre-Admission Testing department. During this conversation, a Registered
Las Vegas Urogynecology
 Las Vegas Urogynecology 7500 Smoke Ranch Road - #200 Las Vegas, NV 89128 Telephone: (702) 233-0727 Fax: (702) 233-4799 Physician's Surgical Procedure Disclosure and Patient s Consent TO THE PATIENT: You
Las Vegas Urogynecology 7500 Smoke Ranch Road - #200 Las Vegas, NV 89128 Telephone: (702) 233-0727 Fax: (702) 233-4799 Physician's Surgical Procedure Disclosure and Patient s Consent TO THE PATIENT: You
INFORMED CONSENT - BREAST LIFT (MASTOPEXY)
 2004 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use
2004 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use
