Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2018; 162:XX.
|
|
|
- Phyllis Lawrence
- 5 years ago
- Views:
Transcription
1 Extraction of a dislocated leadless pacemaker in a patient with infective endocarditis and repeated endocardial and epicardial pacing system infections Milos Taborsky a, Tomas Skala a, Martin Kocher b, Marian Fedorco a Background. Leadless pacemakers (PMs) were recently introduced to address the complication rate of standard PMs with transvenous leads. Methods and Results. A 34-year old male with a history of intravenous substance abuse and a chronic type C hepatitis developed a complete atrioventricular block after cardiac surgery for infective endocarditis. Repeatedly, endo- and epi-cardially implanted PMs had to be explanted due to infection. A leadless MICRA pacemaker was successfully implanted with a dislocation into pulmonary artery several days after implantation. The PM was successfully retrieved using a single-loop retrieval snare guided by a steerable sheath. Subsequently, another Micra PM was successfully implanted with no further issues. Conclusion. In the case of a Micra leadless pacemaker dislocation, a conventional gooseneck snare in combination with a steerable sheath can be used to retrieve the device, improving the overall safety of leadless pacemakers. Key words: Micra, leadless, pacemaker, dislocation, extraction, gooseneck snare Received: January 2, 2018; Accepted with revision: April 13, 2018; Available online: May 23, a Department of Internal Medicine I Cardiology, Faculty of Medicine and Dentistry, Palacky University Olomouc and University Hospital Olomouc, I.P. Pavlova 6, Olomouc, Czech Republic b Department of Radiological Methods, Faculty of Health Sciences, Palacky University Olomouc and Department of Radiology, University Hospital Olomouc, I.P. Pavlova 6, Olomouc, Czech Republic Corresponding author: Tomas Skala, tomasskala@gmail.com INTRODUCTION Standard pacemakers (PMs) with transvenous leads have a considerable complications rate. The short-term complication rate is approximately 9-10% (ref. 1,2 ). The most significant complications are pocket hematoma, endocarditis, pneumothorax, lead dislodgement, venous obstruction, tricuspid regurgitation and cardiac tamponade 3. Cardiac device infections occur in approximately 2.2% of device implantation and revision procedures, with 24% occurring more than two years after the device-related procedure 4. Endovascular infection related to PM with transvenous leads implantation is associated with a mortality risk around 20% (ref. 5 ). Transvenous leads can be affected with insulation breaks and lead body fracture that require another intervention with significant morbidity risk 6. In many cases of PM infections and transvenous lead impairment, the stimulation system has to be extracted. Major vascular injury or cardiac perforation requiring emergency surgical or endovascular intervention during transvenous lead extraction is uncommon but carries significant inhospital mortality 7. Leadless PMs were recently introduced to address some of these lead- and pocket-related complications. Two leadless pacing systems are currently clinically available: (A) the Nanostim Leadless Cardiac PM (LCP; St. Jude Medical), and (B) the Micra Transcatheter Pacing System (TPS; Medtronic) (ref. 8,9 ). Case report A 34-year old male with a history of intravenous substance abuse and chronic type C hepatitis was admitted to hospital for infective endocarditis of the aortic and tricuspid valves. Infective endocarditis resulted in acute heart failure and the patient underwent cardiac surgery consisting of aortic valve replacement with bioprosthesis and tricuspid valve repair. An intracardiac abscess was treated by reconstruction of aortic bulbus and interventricular septum. An immediate postoperative period was complicated with pneumonia and respiratory failure. The patient was kept on a veno-venous extracorporeal membrane oxygenation system (ECMO) for six days. A complete atrioventricular block (AVB) emerged right after surgery resulting in the need for temporary ventricular stimulation. While the AVB lasted, a transvenous PM was implanted after inflammatory markers levels decreased. One month after PM implantation, the patient presented with PM pocket infection. The pacing system had to be explanted. At that time, the patient was referred to our hospital. We extracted the whole pacing system and inserted a temporary pacing electrode. After prolonged antibiotics (ATB) treatment and decline in inflammatory marker levels, we performed a second transvenous PM implantation from the contralateral side. Unfortunately, 10 days after the implantation, PM pocket got infected again and the stimulation system had to be explanted for the second time. 1
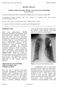
2 Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2018; 162:XX. Since there was still a complete AVB, and since we had performed two extractions of the whole stimulation system, we decided to implant a leadless PM. Before the implantation, inflammatory markers levels were normal and focal infections were excluded. A leadless Micra pacemaker was implanted exactly according to the provided implantation protocol via right femoral vein with a stimulation threshold 0.9 V (0.40 ms) after three stability tests. The stimulation threshold was considered adequate and the PM was released. Three days after the implantation, the pacing threshold rose to 3.6 V (0.40 ms) without a change in PM position or the detected signal. Due to the patient`s dependence on stimulation, a screwed-in temporary pacing electrode was inserted as a safety measure to ensure stable stimulation. Fluoroscopy did not reveal any visible dislodgment of the pacemaker (Fig. 1.). We administered corticosteroid therapy aiming at improving the pacing threshold without apparent success. One week after the implantation, loss of leadless pacemaker capture was detected and fluoroscopy revealed an apparent dislocation of the PM into the left branch of the pulmonary artery. We tried to extract the dislocated leadless pacemaker. Since a dedicated extraction system was not available, a single-loop retrieval snare (COOK Medical, Bloomington, IN, USA) was inserted through right femoral vein. We have used a steerable sheath (Agilis, St. Jude Medical, St. Paul, MN, USA) that allowed us to manipulate the snare through the right ventricular outflow tract into the particular part of pulmonary artery where the PM was localized. The pacemaker was grasped and pulled back under fluoroscopic control and then surgically removed through the right femoral vein. The patient was still dependent on the pacing and thus as a next possible step we decided to implant an epicardial pacing electrode. This was performed via anterolateral minithoracotomy with standard stimulation parameters. A permanent pacemaker was put under the left musculus rectus abdominis in the upper middle epigastrium and connected with the pacing electrode. After several days, there was a purulent secretion in thoracotomy. Microbiological analysis revealed Staphylococcus aureus as an infectious agent. The whole epicardial stimulation system had to be explanted again. Vacuum-assisted closure (VAC) therapy was needed to treat the non-healing chest wounds. Subsequently, the patient had a spontaneous junctional rhythm of 42 beats per minute without bradycardia symptoms. This allowed us to treat him with prolonged combined antibiotics therapy under careful observation without any, not even a temporary, pacemaker lead inserted to minimize the possibility of persistent infection despite aggressive ATB therapy. During this treatment, the patient had a short worsening of bradycardia with syncope, so the need for a permanent pacemaker clearly remained and the patient could not have been left without a long-lasting PM stimulation. Thus, once the inflammatory markers declined and focal infection was excluded again, we decided to implant another pacemaker. Since all pacemakers with transvenous leads had to be explanted, we decided to implant another leadless pacemaker Micra. The venous and epicardial access was limited. The left groin was not usable due to severe scarring after initial cardiosurgery and ECMO. The right groin was also severely scarred after surgical explantation of the first leadless PM. We decided to use suprapubic approach in the right groin. After several attempts in various parts of the right ventricle (RV), we were not able to find a spot with satisfactory stimulation parameters. Finally, two centimeters from the RV apex we found a spot with ac- Fig. 1. Leadless pacemaker MICRA (red arrow). Screwed-in temporary pacing electrode. Fig. 2. Dislocated leadless pacemaker MICRA (red arrow). 2
3 ceptable pacing / sensing parameters and stability. Several measurements proved stable stimulation parameters even after the stability test. After many attempts, the best place found in the RV resulted in a stimulation threshold of 2.9 V (0.40 ms). This threshold was high but there was no better spot in RV and since we ran out of options we decided to implant there. The next day the PM parameters were as follows: threshold 2.25 V, R-wave amplitude 8.4 mv, impedance 540 Ohm. These parameters remained stable from that moment on. In the subsequent follow-up, the patient had no symptoms, he did not develop any sign of inflammation and the pacing parameters remained unchanged. The PM parameters are controlled remotely. The leadless PM was, the only viable option of stimulation in the long run. DISCUSSION Implantable transcatheter leadless PMs have several advantages over conventional pacing systems. Obviously, the use of these devices offers a reduction in pocket- and transvenous-lead- related issues. Nevertheless, the risk of a leadless pacemaker dislocation has to be considered. The risk is mostly related to the implant procedure: cardiac perforation, device dislocation, and femoral vascular access site complications 10. However, in cases such as the presented one, a leadless PM can be a viable option of stimulation and sometimes even the only one. The stimulation threshold in Micra patients can change over time. Pacing threshold in most Micra patients with elevated thresholds decrease after implant. According to the Results from the Micra Transcatheter Pacing System Global Clinical Trial, stimulation thresholds of Micra patients with high (>1.0 V) and very high (>1.5 V) thresholds decreased significantly by 1 month, with 87% and 85% having 6-month thresholds lower than the implant value. However, when the capture threshold at implant was >2 V, only 18.2% had a threshold of 1 V at 6 months and 45.5% had a capture threshold of >2 V. Micra device repositioning thus may not be necessary if the pacing threshold is 2 V (ref. 11 ). The delivery system allows for the PM to be repositioned several times during the implantation. After de- Fig. 3. Extraction of leadless pacemaker MICRA using singleloop retrieval snare (red arrow). Fig. 4. Extraction of leadless pacemaker MICRA using singleloop retrieval snare (red arrow). 3
4 livery of the PM the recapture is more difficult but it is feasible using available foreign body removal snares even several weeks after implantation 12. In the presented case, in the first leadless PM implantation the stimulation threshold was 0.9 V after stability test. It was considered adequate and the PM was released. However, in three days a routine inspection of stimulation parameters after implantation revealed the stimulation threshold increase to 3.6 V without a change in PM position or the detected signal. To the best of our knowledge, such an impairment of stimulation parameters is extremely rare and the only plausible explanation is a PM micro-dislodgement, although the PM is actively fixed using the nitinol tines. A macro-dislodgement was observed after a few days and thus has to be expected in such a case and a temporary pacing electrode insertion should be considered. In the FDA investigational device exemption (IDE) Micra TPS Trial (Micra Transcatheter Pacing Study, n = 745), an increased pacing threshold was documented in 0.3% of patients. No device dislodgements were observed, the implant success rate was excellent (99.2%) and the major complication rate through 12 months post implant was low (4%) (ref. 9 ). According to the real-world data from a worldwide Post-Approval Micra Registry, device dislodgement was documented in only 1 of 795 implantations (0.13%) so far. Performance of the Micra transcatheter pacemaker in a real-world setting demonstrates a high rate (99.6%) of implant success and low rate (1.51%) of major complications through 30 days post implant 9. Remarkably, across a combined 1521 patients from both the IDE and registry studies, only 1 macrodislodgement has been reported so far (0.066%) (ref. 13 ). So the presented case is an extremely rare complication. This does not mean that leadless PMs are more prone to lead dislodgement than standard transvenous PM systems. In the FOLLOWPACE study (n = 1517), lead dislodgement in transvenous PM systems was reported at a rate of 3.3% within 2 months of implant 1. When the patients from the Pre-market Micra Transcatheter Pacing Study and the Micra Transcatheter Pacing System Continued Access Study (TPS; N = 989) were analyzed and compared directly with patients with transvenous pacemakers (TVP; n = 2667) the actual rate for revision at 24 months postimplant was 1.4% for the TPS group (11 revisions in 10 patients), 75% (95% confidence interval 53% 87%; P<0.001) lower than the 5.3% for the TVP group (123 revisions in 117 patients) (ref. 14 ). In the first Micra implantation, we proceeded precisely according to the company recommendations and the stimulation threshold was acceptable after three stability tests and device release. We were not able to find an operator-based fault leading to the dislodgement. This is supported by the fact, that in the Micra study, there was no evidence of a relationship between operator experience and major complications 15. Moreover, the implanting operator in this case is an extremely experienced one, well beyond the learning curve. The precise reason for the PM dislodgment in the presented case is unknown. We can only speculate, that in a patient with a long history of intravenous substance abuse and infective endocarditis, the right ventricle trabeculae are remodeled resulting in difficulties in stable fixation of leadless PM with passive fixation. Since device dislodgment is possible, the leadless PMs retrievability is an important feature. The Nanostim Leadless Cardiac PM has a dedicated steerable retrieval catheter 10. The Micra Transcatheter Pacing System does not but use of a conventional gooseneck snare was reported to be feasible 12. We also solved this rare complication using a conventional gooseneck snare. This possibility of device retrieval is really important for the overall safety of the Micra leadless stimulation system. In second leadless PM implantation, the stimulation parameters were suboptimal from the beginning. After many attempts, the best place that could be found in RV resulted in a stimulation threshold of 2.9 V and we were not able to find a better spot. In the Post-Approval Micra Registry population, 97% of patients had an implant threshold of <2V, and 87.2% 1 V, similar to what was reported for the IDE study 9,13. The threshold in our case was very high, but since we ran out of options, we decided to implant the PM at the spot with the best, though suboptimal, parameters. Fortunately the stimulation threshold slightly decreased the next day and no dislodgment occurred in the follow-up. The patient has been well so far. The leadless PM was the only possibility and literally saved his life. CONCLUSION Leadless pacemakers were recently introduced to address lead- and pocket-related complications. In cases such as the presented one, a leadless pacemaker can be a viable option for stimulation and sometimes even the only one. The risk of a leadless pacemaker dislocation is extremely small but it has to be considered. In the case of a Micra pacemaker dislodgment, a conventional steerable sheath in combination with a gooseneck snare can be used to retrieve the device, improving the overall safety of leadless pacemakers. Author contributions: All authors contributed to the management and presentation of the case equally. Conflict of interest statement: None declared REFERENCES 1. Udo EO, Zuithoff NP, van Hemel NM, de Cock CC, Hendriks T, Doevendans PA, Moons KG. Incidence and predictors of short- and long-term complications in pacemaker therapy: the FOLLOWPACE study. Heart Rhythm 2012;9: Kirkfeldt RE, Johansen JB, Nohr EA, Jorgensen OD, Nielsen JC. Complications after cardiac implantable electronic device implantations: an analysis of a complete, nationwide cohort in Denmark. Eur Heart J 2014;35(18): Harcombe AA, Newell SA, Ludman PF, Wistow TE, Sharples LD, Schofield PM, Stone DL, Shapiro LM, Cole T, Petch MC. Late compli- 4
5 cations following permanent pacemaker implantation or elective unit replacement. Heart 1998;80: Lekkerkerker JC, van Nieuwkoop C, Trines SA, van der Bom JG, Bernards A, van de Velde ET, Bootsma M, Zeppenfeld K, Jukema JW, Borleffs JW, Schalij MJ, van Erven L. Risk factors and time delay associated with cardiac device infections: Leiden device registry. Heart 2009;95: Tarakji KG, Wazni OM, Harb S, Hsu A, Saliba W, Wilkoff BL. Risk factors for 1-year mortality among patients with cardiac implantable electronic device infection undergoing transvenous lead extraction: the impact of the infection type and the presence of vegetation on survival. Europace 2014;16: Hauser RG, Hayes DL, Kallinen LM, Cannom DS, Epstein AE, Almquist AK, Song SL, Tyers GF, Vlay SC, Irwin M. Clinical experience with pacemaker pulse generators and transvenous leads: an 8-year prospective multicenter study. Heart Rhythm 2007;4: Brunner MP, Cronin EM, Wazni O, Baranowski B, Saliba WI, Sabik JF, Lindsay BD, Wilkoff BL, Tarakji KG. Outcomes of patients requiring emergent surgical or endovascular intervention for catastrophic complications during transvenous lead extraction. Heart Rhythm 2014;11: Reddy VY, Exner DV, Cantillon DJ, Doshi R, Bunch TJ, Tomassoni GF, Plunkitt K. Percutaneous implantation of an entirely intracardiac leadless pacemaker. N Engl J Med 2015;373(12), Reynolds D, Duray GZ, Omar R, Soejima K, Neuzil P, Zhang S, Narasimhan C, Steinwender C, Brugada J, Lloyd M, Roberts PR, Sagi V, Hummel J, Bongiorni MG, Knops RE, Ellis CR, Gornick CC, Bernabei MA, Laager V, Stromberg K, Williams ER, Hudnall JH, Ritter P, Micra Transcatheter Pacing Study Group. A leadless intracardiac transcatheter pacing system. N Engl J Med 2016;374: Tjong FVY, Reddy VY. Permanent Leadless Cardiac Pacemaker Therapy. Circulation 2017; 135(15): Piccini JP, Stromberg K, Jackson KP, Laager V, Duray GZ, El-Chami M, Ellis CR, Hummel J, Jones R, Kowal RC, Narasimhan C, Omar R, Ritter P, Roberts PR, Soejima K, Zhang S, Reynolds D. Long-term outcomes in leadless Micra transcatheter pacemakers with elevated thresholds at implantation: Results from the Micra Transcatheter Pacing System Global Clinical Trial. Heart Rhythm 2017;14(5): Karim S, Abdelmessih M, Marieb M, Reiner E, Grubman E. Extraction of a Micra Transcatheter Pacing System: first-in-human experience. Heart Rhythm Case Reports 2016;2(1): Roberts PR, Clementy N, Al Samadi F, Garweg C, Martinez-Sande JL, Iacopino S, Johansen JB, Prat XV, Kowal RC, Klug D, Mont L, Steffel J, Li S, Osch DV, El-Chami LF. A leadless pacemaker in the real-world setting: The Micra Transcatheter Pacing System Post-Approval Registry. Heart Rhythm 2017; 14(9): doi: /j. hrthm Grubman E, Ritter P, Ellis CR, Giocondo M, Augostini R, Neuzil P, Ravindran B, Patel AM, Omdahl P, Pieper K, Stromberg K, Hudnall JH, Reynolds D. To retrieve, or not to retrieve: System revisions with the Micra transcatheter pacemaker. Heart Rhythm 2017;14(12): doi: /j.hrthm Kowal R, Soejima K, Ritter P, Duray GZ, Hudhall JH, Stromberg K, Reynolds D. Relationship between operator experience and procedure outcomes with the Micra transcatheter leadless pacing system. Heart Rhythm 2016;13:S169. 5
REVIEW ARTICLE. Leadless Cardiac Pacemaker Therapy. An Overview for the Hospitalist Richard Weachter 1
 Leadless Cardiac Pacemaker Therapy. An Overview for the Hospitalist Richard Weachter 1 1 Division of Cardiovascular Medicine, Department of Medicine, University of Missouri, Columbia, MO Correspondence:
Leadless Cardiac Pacemaker Therapy. An Overview for the Hospitalist Richard Weachter 1 1 Division of Cardiovascular Medicine, Department of Medicine, University of Missouri, Columbia, MO Correspondence:
New generations pacemakers and ICDs: an update
 Advances in Cardiac Arrhythmias and Great Innovations in Cardiology XXVII Giornate Cardiologiche Torinesi New generations pacemakers and ICDs: an update Prof. Fiorenzo Gaita, MD Division of Cardiology
Advances in Cardiac Arrhythmias and Great Innovations in Cardiology XXVII Giornate Cardiologiche Torinesi New generations pacemakers and ICDs: an update Prof. Fiorenzo Gaita, MD Division of Cardiology
Performance of a Miniaturized Transcatheter Pacing System: First-in-human experience
 Performance of a Miniaturized Transcatheter Pacing System: First-in-human experience Philippe Ritter, MD Gabor Z Duray, MD, PhD, FESC; Clemens Steinwender, MD, FESC; Kyoko Soejima, MD; Razali Omar, MD;
Performance of a Miniaturized Transcatheter Pacing System: First-in-human experience Philippe Ritter, MD Gabor Z Duray, MD, PhD, FESC; Clemens Steinwender, MD, FESC; Kyoko Soejima, MD; Razali Omar, MD;
MEET MICRA. Micra TM ACTUAL SIZE. Transcatheter Pacing System
 MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 6 Completely self contained within the heart,
MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 6 Completely self contained within the heart,
MEET MICRA. Micra TM ACTUAL SIZE. Transcatheter Pacing System
 MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 7 Completely self contained within the heart,
MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 7 Completely self contained within the heart,
Leadless pacemakers a panacea for bradyarrhythmias?
 Leadless pacemakers a panacea for bradyarrhythmias? Peysh A Patel Take Home Messages Why may leadless systems be required? Where the cessation of vital action is very complete, and continues long, we ought
Leadless pacemakers a panacea for bradyarrhythmias? Peysh A Patel Take Home Messages Why may leadless systems be required? Where the cessation of vital action is very complete, and continues long, we ought
Performance of Leadless Pacemaker in Japanese Patients vs. Rest of the World. Results From a Global Clinical Trial
 Circ J 2017; 81: 1589 1595 doi: 10.1253/circj.CJ-17-0259 ORIGINAL ARTICLE Arrhythmia/Electrophysiology Performance of Leadless Pacemaker in ese Patients vs. Rest of the World Results From a Global Clinical
Circ J 2017; 81: 1589 1595 doi: 10.1253/circj.CJ-17-0259 ORIGINAL ARTICLE Arrhythmia/Electrophysiology Performance of Leadless Pacemaker in ese Patients vs. Rest of the World Results From a Global Clinical
Comparator cohort In order to compare the Micra pacing thresholds with transvenous thresholds, we analyzed transvenous pacing thresholds
 Long-term outcomes in leadless Micra transcatheter pacemakers with elevated thresholds at implantation: Results from the Micra Transcatheter Pacing System Global Clinical Trial Jonathan P. Piccini, MD,
Long-term outcomes in leadless Micra transcatheter pacemakers with elevated thresholds at implantation: Results from the Micra Transcatheter Pacing System Global Clinical Trial Jonathan P. Piccini, MD,
NOVEL DEVICE TECHNOLOGIES
 NOVEL DEVICE TECHNOLOGIES Leadless Pacemakers and Subcutaneous ICDs Do the Benefits Outweigh MRI Incompatibility? Disclosures None Background PPMs and ICDs are very effective therapy for treating bradyarrhythmias
NOVEL DEVICE TECHNOLOGIES Leadless Pacemakers and Subcutaneous ICDs Do the Benefits Outweigh MRI Incompatibility? Disclosures None Background PPMs and ICDs are very effective therapy for treating bradyarrhythmias
How to Implant a Leadless Pacemaker With a Tine-Based Fixation
 Techniques, Technology, and Innovations Section Editor: Samuel J. Asirvatham, M.D. How to Implant a Leadless Pacemaker With a Tine-Based Fixation MIKHAEL F. EL-CHAMI, M.D., PAUL R. ROBERTS, M.D., ALEX
Techniques, Technology, and Innovations Section Editor: Samuel J. Asirvatham, M.D. How to Implant a Leadless Pacemaker With a Tine-Based Fixation MIKHAEL F. EL-CHAMI, M.D., PAUL R. ROBERTS, M.D., ALEX
Pacing Without Wires: Leadless Cardiac Pacing
 REVIEWS AND CONTEMPORARY UPDATES Ochsner Journal 16:238 242, 2016 Ó Academic Division of Ochsner Clinic Foundation Pacing Without Wires: Leadless Cardiac Pacing Michael L. Bernard, MD, PhD Department of
REVIEWS AND CONTEMPORARY UPDATES Ochsner Journal 16:238 242, 2016 Ó Academic Division of Ochsner Clinic Foundation Pacing Without Wires: Leadless Cardiac Pacing Michael L. Bernard, MD, PhD Department of
Leadless Pacing. Osama Diab Assistant Prof. of Cardiology Ain Shams University Egypt
 Leadless Pacing Osama Diab Assistant Prof. of Cardiology Ain Shams University Egypt The weakest link in Pacemaker system the lead. The more the leads the more the complications Dislodgement Fracture Insulation
Leadless Pacing Osama Diab Assistant Prof. of Cardiology Ain Shams University Egypt The weakest link in Pacemaker system the lead. The more the leads the more the complications Dislodgement Fracture Insulation
Essentials of Pacemakers and ICD s. Rajesh Banker, MD, MPH
 Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Long-term Performance of a Transcatheter Pacing System: 12 month results from the Micra Transcatheter Pacing Study
 Accepted Manuscript Long-term Performance of a Transcatheter Pacing System: 12 month results from the Micra Transcatheter Pacing Study Gabor Z. Duray, MD, PhD, Philippe Ritter, MD, Mikhael El-Chami, MD,
Accepted Manuscript Long-term Performance of a Transcatheter Pacing System: 12 month results from the Micra Transcatheter Pacing Study Gabor Z. Duray, MD, PhD, Philippe Ritter, MD, Mikhael El-Chami, MD,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
The learning curve associated with the implantation of the Nanostim leadless pacemaker
 Journal of Interventional Cardiac Electrophysiology (2018) 53:239 247 https://doi.org/10.1007/s10840-018-0438-8 MULTIMEDIA REPORT The learning curve associated with the implantation of the Nanostim leadless
Journal of Interventional Cardiac Electrophysiology (2018) 53:239 247 https://doi.org/10.1007/s10840-018-0438-8 MULTIMEDIA REPORT The learning curve associated with the implantation of the Nanostim leadless
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of a leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of a leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
Use of leadless pacemakers in Europe: results of the European Heart Rhythm Association survey
 Europace (2018) 20, 555 559 doi:10.1093/europace/eux381 EP WIRE Use of leadless pacemakers in Europe: results of the European Heart Rhythm Association survey Serge Boveda 1 *, Radoslaw Lenarczyk 2, Kristina
Europace (2018) 20, 555 559 doi:10.1093/europace/eux381 EP WIRE Use of leadless pacemakers in Europe: results of the European Heart Rhythm Association survey Serge Boveda 1 *, Radoslaw Lenarczyk 2, Kristina
FREQUENTLY ASKED QUESTIONS
 FREQUENTLY ASKED QUESTIONS Micra TPS U.S. Private Payer Prior Authorization Micra Transcatheter Pacing System Most commercial payers in the United States do not have a positive coverage policy for Micra
FREQUENTLY ASKED QUESTIONS Micra TPS U.S. Private Payer Prior Authorization Micra Transcatheter Pacing System Most commercial payers in the United States do not have a positive coverage policy for Micra
A Leadless Intracardiac Transcatheter Pacing System
 Original Article A Leadless Intracardiac Transcatheter Pacing System Dwight Reynolds, M.D., Gabor Z. Duray, M.D., Ph.D., Razali Omar, M.D., Kyoko Soejima, M.D., Petr Neuzil, M.D., Shu Zhang, M.D., Calambur
Original Article A Leadless Intracardiac Transcatheter Pacing System Dwight Reynolds, M.D., Gabor Z. Duray, M.D., Ph.D., Razali Omar, M.D., Kyoko Soejima, M.D., Petr Neuzil, M.D., Shu Zhang, M.D., Calambur
Percutaneous Implantation of an Entirely Intracardiac Leadless Pacemaker
 Original Article Percutaneous Implantation of an Entirely Intracardiac Leadless Pacemaker Vivek Y. Reddy, M.D., Derek V. Exner, M.D., M.P.H., Daniel J. Cantillon, M.D., Rahul Doshi, M.D., T. Jared Bunch,
Original Article Percutaneous Implantation of an Entirely Intracardiac Leadless Pacemaker Vivek Y. Reddy, M.D., Derek V. Exner, M.D., M.P.H., Daniel J. Cantillon, M.D., Rahul Doshi, M.D., T. Jared Bunch,
INNOVATIONS IN DEVICE THERAPY:
 INNOVATIONS IN DEVICE THERAPY: Subcutaneous ICDs, Leadless Pacemakers, CRT Indications David J Wilber MD Loyola University Medical Center Disclosures: ACC Foundation: Consultant; Biosense / Webster: Consultant,
INNOVATIONS IN DEVICE THERAPY: Subcutaneous ICDs, Leadless Pacemakers, CRT Indications David J Wilber MD Loyola University Medical Center Disclosures: ACC Foundation: Consultant; Biosense / Webster: Consultant,
Left Atrial Appendage Closure: The Good, The Bad and The Ugly
 Left Atrial Appendage Closure: The Good, The Bad and The Ugly John D. Hummel, MD Director of Electrophysiology Research Ross Heart Hospital, The Ohio State University Columbus, Ohio USA Disclosures Modest
Left Atrial Appendage Closure: The Good, The Bad and The Ugly John D. Hummel, MD Director of Electrophysiology Research Ross Heart Hospital, The Ohio State University Columbus, Ohio USA Disclosures Modest
Transvenous Pacemaker Procedures
 Cardiology: Pacemaker and Defibrillator Coding Presented By: Moderate Sedation 2017 99151 : under age 5, initial 15 minutes by MD performing intervention 99152: age 5 or older, initial 15 minutes by MD
Cardiology: Pacemaker and Defibrillator Coding Presented By: Moderate Sedation 2017 99151 : under age 5, initial 15 minutes by MD performing intervention 99152: age 5 or older, initial 15 minutes by MD
Acute and 3-Month Performance of A Communicating Leadless Anti-Tachycardia Pacemaker and Subcutaneous Implantable Defibrillator
 Accepted Manuscript Acute and 3-Month Performance of A Communicating Leadless Anti-Tachycardia Pacemaker and Subcutaneous Implantable Defibrillator Fleur V.Y. Tjong, MD, Tom F. Brouwer, MD, Brendan Koop,
Accepted Manuscript Acute and 3-Month Performance of A Communicating Leadless Anti-Tachycardia Pacemaker and Subcutaneous Implantable Defibrillator Fleur V.Y. Tjong, MD, Tom F. Brouwer, MD, Brendan Koop,
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
Leadless Cardiac Pacemaker
 Leadless Cardiac Pacemaker Policy Number: Original Effective Date: MM.02.042 XXXMay 1, 2019 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration; FED87 XXXMay 1, 2019 Section: Medicine
Leadless Cardiac Pacemaker Policy Number: Original Effective Date: MM.02.042 XXXMay 1, 2019 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration; FED87 XXXMay 1, 2019 Section: Medicine
Introduction. Case Report ECG & EP CASES ABSTRACT
 Successful extraction of an implantable cardioverter-defibrillator lead in a patient with pocket infection via the femoral approach with a basket snare Jin-Bae Kim, MD, PhD. Cardiology Division, Department
Successful extraction of an implantable cardioverter-defibrillator lead in a patient with pocket infection via the femoral approach with a basket snare Jin-Bae Kim, MD, PhD. Cardiology Division, Department
Update on Device Innovation (S-ICD, Wearable, Leadless)
 Update on Device Innovation (S-ICD, Wearable, Leadless) C. W. Israel Dept. of Medicine - Cardiology Evangelical Hospital Bielefeld J. W. Goethe University Frankfurt Carsten.Israel@em.uni-frankfurt.de Conflicts
Update on Device Innovation (S-ICD, Wearable, Leadless) C. W. Israel Dept. of Medicine - Cardiology Evangelical Hospital Bielefeld J. W. Goethe University Frankfurt Carsten.Israel@em.uni-frankfurt.de Conflicts
Pediatric Pacemaker Implantation Endocardial or Epicardial
 Pediatric Pacemaker Implantation Endocardial or Epicardial HAITHAM BADRAN, MD, FEHRA CONSULTANT OF INTERVENTIONAL CARDIOLOGY CONSULTANT OF CARDIAC PACING AND ELECTROPHYSIOLOGY LECTURER OF CARDIOLOGY AIN
Pediatric Pacemaker Implantation Endocardial or Epicardial HAITHAM BADRAN, MD, FEHRA CONSULTANT OF INTERVENTIONAL CARDIOLOGY CONSULTANT OF CARDIAC PACING AND ELECTROPHYSIOLOGY LECTURER OF CARDIOLOGY AIN
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Complications of Lead Extraction: Prevention and treatment. Maria Grazia Bongiorni, MD, FESC
 Complications of Lead Extraction: Prevention and treatment Maria Grazia Bongiorni, MD, FESC Director of Cardiovascular Division University Hospital of Pisa (Italy) ourtesy of Dr Eivind Platou Potential
Complications of Lead Extraction: Prevention and treatment Maria Grazia Bongiorni, MD, FESC Director of Cardiovascular Division University Hospital of Pisa (Italy) ourtesy of Dr Eivind Platou Potential
Leadless Pacemakers: practice and promise in congenital heart disease
 Clarke et al. Journal of Congenital Cardiology (2017) 1:4 DOI 10.1186/s40949-017-0007-5 Journal of Congenital Cardiology REVIEW Leadless Pacemakers: practice and promise in congenital heart disease T.S.O.
Clarke et al. Journal of Congenital Cardiology (2017) 1:4 DOI 10.1186/s40949-017-0007-5 Journal of Congenital Cardiology REVIEW Leadless Pacemakers: practice and promise in congenital heart disease T.S.O.
Right Ventricular Outflow Tract Septal Pacing in Hue Central Hospital
 Right Ventricular Outflow Tract Septal Pacing in Hue Central Hospital Huỳnh Văn Minh Nguyễn Cửu Lợi Tô Hưng Thụy 1 Introduction Apical pacing has been introduced over the past 5 decades to save and improve
Right Ventricular Outflow Tract Septal Pacing in Hue Central Hospital Huỳnh Văn Minh Nguyễn Cửu Lợi Tô Hưng Thụy 1 Introduction Apical pacing has been introduced over the past 5 decades to save and improve
Left ventricular guidewire pacing for transcatheter aortic valve. implantation
 Page 1 of 8 Left ventricular guidewire pacing for transcatheter aortic valve implantation Ênio E. Guérios, MD 1, 2, Peter Wenaweser, MD 1, Bernhard Meier, MD 1 1 Department of Cardiology, Bern University
Page 1 of 8 Left ventricular guidewire pacing for transcatheter aortic valve implantation Ênio E. Guérios, MD 1, 2, Peter Wenaweser, MD 1, Bernhard Meier, MD 1 1 Department of Cardiology, Bern University
Recent Advances in Pacing and Defibrillation Harish Doppalapudi, MD
 Recent Advances in Pacing and Defibrillation Harish Doppalapudi, MD Harish Doppalapudi, MD Assistant Professor of Medicine Director, Clinical Cardiac Electrophysiology Training Program University of Alabama
Recent Advances in Pacing and Defibrillation Harish Doppalapudi, MD Harish Doppalapudi, MD Assistant Professor of Medicine Director, Clinical Cardiac Electrophysiology Training Program University of Alabama
Permanent Pacemaker Implantation via the Iliac Vein: An Alternative in 4 Cases with Contraindications to the Pectoral Approach
 Case Report Permanent Pacemaker Implantation via the Iliac Vein: An Alternative in 4 Cases with Contraindications to the Pectoral Approach Koji Tsutsumi MD, Kenichi Hashizume MD, Naritaka Kimura MD, Shinichi
Case Report Permanent Pacemaker Implantation via the Iliac Vein: An Alternative in 4 Cases with Contraindications to the Pectoral Approach Koji Tsutsumi MD, Kenichi Hashizume MD, Naritaka Kimura MD, Shinichi
What s New in CIEDs. Keimyung University Dongsan Medical Center Hyoung-Seob Park
 What s New in CIEDs Keimyung University Dongsan Medical Center Hyoung-Seob Park Transvenous CIEDs Technology: - Highly mature & reliable - Still includes generator, connectors and leads Procedure : -
What s New in CIEDs Keimyung University Dongsan Medical Center Hyoung-Seob Park Transvenous CIEDs Technology: - Highly mature & reliable - Still includes generator, connectors and leads Procedure : -
COMMONLY BILLED CODES AND ASSOCIATED 2018 MEDICARE RATES
 CRHF REIMBURSEMENT & HEALTH POLICY Pacemaker Therapy COMMONLY BILLED CODES AND ASSOCIATED 2018 MEDICARE RATES This document reflects commonly billed codes for Pacemaker Therapy and their associated National
CRHF REIMBURSEMENT & HEALTH POLICY Pacemaker Therapy COMMONLY BILLED CODES AND ASSOCIATED 2018 MEDICARE RATES This document reflects commonly billed codes for Pacemaker Therapy and their associated National
EBR Systems, Inc. 686 W. Maude Ave., Suite 102 Sunnyvale, CA USA
 Over 200,000 patients worldwide are estimated to receive a CRT device each year. However, limitations prevent some patients from benefiting. CHALLENGING PROCEDURE 5% implanted patients fail to have coronary
Over 200,000 patients worldwide are estimated to receive a CRT device each year. However, limitations prevent some patients from benefiting. CHALLENGING PROCEDURE 5% implanted patients fail to have coronary
Technical option of surgical approach for trouble-shooting
 JHRS Corner Device and lead trouble-shooting - standard strategy and technical option - Technical option of surgical approach for trouble-shooting Katsuhiko IMAI Department of Cardiovascular surgery, Hiroshima
JHRS Corner Device and lead trouble-shooting - standard strategy and technical option - Technical option of surgical approach for trouble-shooting Katsuhiko IMAI Department of Cardiovascular surgery, Hiroshima
Leadless pacing: Technical challenges and concerns. Panos Vardas President Elect of the ESC, Prof. of Cardiology, Heraklion University Hospital
 Leadless pacing: Technical challenges and concerns Panos Vardas President Elect of the ESC, Prof. of Cardiology, Heraklion University Hospital Modest consultancy fees/honoraria from Bayer Boehringer Ingelheim
Leadless pacing: Technical challenges and concerns Panos Vardas President Elect of the ESC, Prof. of Cardiology, Heraklion University Hospital Modest consultancy fees/honoraria from Bayer Boehringer Ingelheim
Leadless pacemakers and subcutaneous ICD s: will we use them for most of our patients? K.-H. Kuck Asklepios Klinik St. Georg Hamburg, Germany
 Leadless pacemakers and subcutaneous ICD s: will we use them for most of our patients? K.-H. Kuck Asklepios Klinik St. Georg Hamburg, Germany Disclosure Statement Research Grants Consultant / Advisory
Leadless pacemakers and subcutaneous ICD s: will we use them for most of our patients? K.-H. Kuck Asklepios Klinik St. Georg Hamburg, Germany Disclosure Statement Research Grants Consultant / Advisory
Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect
 The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
CRF procedure PROCEDURE FLOW. PATIENT ASSESSMENT Symptoms and indication. Pacemaker & ICD registration. Procedures. Procedure ICD.
 Pacemaker & ICD registration Procedures CRF procedure PROCEDURE FLOW Procedure ICD ICD PM ICM lead only PATIENT ASSESSMENT Symptoms and indication Symptoms and events (multiple possibilities) Asymptomatic
Pacemaker & ICD registration Procedures CRF procedure PROCEDURE FLOW Procedure ICD ICD PM ICM lead only PATIENT ASSESSMENT Symptoms and indication Symptoms and events (multiple possibilities) Asymptomatic
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Implantation of a Permanent Tined Endocardial Electrode into Right Atrium during Open-heart Surgery: Report of 3 Cases
 Case Report Implantation of a Permanent Tined Endocardial Electrode into Right Atrium during Open-heart Surgery: Report of 3 Cases Koji Tsutsumi MD, Tatsuru Niibori MD, Keiichiro Katsumoto MD Department
Case Report Implantation of a Permanent Tined Endocardial Electrode into Right Atrium during Open-heart Surgery: Report of 3 Cases Koji Tsutsumi MD, Tatsuru Niibori MD, Keiichiro Katsumoto MD Department
Lead Selection and Subcutaneous ICD Considerations. The Future of CIEDs
 Lead Selection and Subcutaneous ICD Considerations The Future of CIEDs February, 2013 Steven P. Kutalek, MD Director, Cardiac Electrophysiology Drexel University College of Medicine New Technologies 2012
Lead Selection and Subcutaneous ICD Considerations The Future of CIEDs February, 2013 Steven P. Kutalek, MD Director, Cardiac Electrophysiology Drexel University College of Medicine New Technologies 2012
Charging Considerations. Agenda 1/30/2013
 February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 Agenda Cardiology special considerations 2013 Cardiology Codes Deleted Codes
February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 Agenda Cardiology special considerations 2013 Cardiology Codes Deleted Codes
February Jean C. Russell, MS, RHIT Richard Cooley, BA, CCS
 February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 Agenda Cardiology special considerations 2013 Cardiology Codes Deleted Codes
February 2013 Jean C. Russell, MS, RHIT jrussell@epochhealth.com Richard Cooley, BA, CCS rcooley@epochhealth.com 518-430-1144 2 Agenda Cardiology special considerations 2013 Cardiology Codes Deleted Codes
MICRA TRANSCATHETER PACING SYSTEM (TPS) REIMBURSEMENT OVERVIEW
 MICRA TRANSCATHETER PACING SYSTEM (TPS) REIMBURSEMENT OVERVIEW MARCH 20, 2017 DISCLAIMER This presentation is intended only for educational use. Any duplication is prohibited without written consent of
MICRA TRANSCATHETER PACING SYSTEM (TPS) REIMBURSEMENT OVERVIEW MARCH 20, 2017 DISCLAIMER This presentation is intended only for educational use. Any duplication is prohibited without written consent of
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS
 Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Cardiac implantable electronic devices (CIEDs) in children include pacemakers and implantable cardioverter defibrillators (ICDs).
 Management of Children with Cardiac Devices Guideline originally developed by Leann Miles, APRN; Lindsey Pumphrey, RN; Srikant Das, MD, and the ANGELS Team. Last reviewed by Lindsey Pumphrey, RN, Srikant
Management of Children with Cardiac Devices Guideline originally developed by Leann Miles, APRN; Lindsey Pumphrey, RN; Srikant Das, MD, and the ANGELS Team. Last reviewed by Lindsey Pumphrey, RN, Srikant
2017 HRS Expert Consensus Statement on Cardiovascular Implantable Electronic Device Lead Management and Extraction
 Summary of Expert Consensus Statement for CLINICIANS 2017 HRS Expert Consensus Statement on Cardiovascular Implantable Electronic Device Lead Management and Extraction This is a summary of the Heart Rhythm
Summary of Expert Consensus Statement for CLINICIANS 2017 HRS Expert Consensus Statement on Cardiovascular Implantable Electronic Device Lead Management and Extraction This is a summary of the Heart Rhythm
PACING AT THE BUNDLE OF HIS
 PACING AT THE BUNDLE OF HIS Cardiac Rhythm Heart Failure Coding Corner Disclaimer While Medtronic offers opinions about how to code when using our technology according to its FDA-approved labeling, these
PACING AT THE BUNDLE OF HIS Cardiac Rhythm Heart Failure Coding Corner Disclaimer While Medtronic offers opinions about how to code when using our technology according to its FDA-approved labeling, these
The development of implantable. Original Research
 Original Research Hellenic J Cardiol 2016; 57: 33-38 Complications Related to Cardiac Rhythm Management Device Therapy and Their Financial Implication: A Prospective Single-Center Two- Year Survey John
Original Research Hellenic J Cardiol 2016; 57: 33-38 Complications Related to Cardiac Rhythm Management Device Therapy and Their Financial Implication: A Prospective Single-Center Two- Year Survey John
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
Riata lead extraction- a single centre experience
 Riata lead extraction- a single centre experience Rebecca L Noad, Keith W Morrice, Vivek N Kodoth, Carol M Wilson, Michael JD Roberts. Royal Victoria Hospital, Belfast, United Kingdom Background of previous
Riata lead extraction- a single centre experience Rebecca L Noad, Keith W Morrice, Vivek N Kodoth, Carol M Wilson, Michael JD Roberts. Royal Victoria Hospital, Belfast, United Kingdom Background of previous
Apparent Failure of Automated Threshold Evaluation: What is the Mechanism? Vikas Kalra, M.B.B.S. Lynne Foreman, R.N. Deepak Bhakta, M.D.
 Apparent Failure of Automated Threshold Evaluation: What is the Mechanism? Vikas Kalra, M.B.B.S. Lynne Foreman, R.N. Deepak Bhakta, M.D. Case Summary A 57-year-old man developed severe symptomatic tricuspid
Apparent Failure of Automated Threshold Evaluation: What is the Mechanism? Vikas Kalra, M.B.B.S. Lynne Foreman, R.N. Deepak Bhakta, M.D. Case Summary A 57-year-old man developed severe symptomatic tricuspid
Title and contents page 1 Who should read this document 2 Scope of the Guideline 2 Background 2 What is new in this version 2
 Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
Supplemental Material
 Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Late complications following permanent pacemaker implantation or elective unit replacement
 240 Regional Cardiac Unit, Papworth Hospital NHS Trust, Cambridge CB3 8RE, UK A A Harcombe S A Newell P F Ludman T E Wistow P M Schofield D L Stone L M Shapiro T Cole M C Petch MRC Biostatistics Unit,
240 Regional Cardiac Unit, Papworth Hospital NHS Trust, Cambridge CB3 8RE, UK A A Harcombe S A Newell P F Ludman T E Wistow P M Schofield D L Stone L M Shapiro T Cole M C Petch MRC Biostatistics Unit,
Implantable cardioverter defibrillator, Inappropriate shock, Lead failure
 Inappropriate Discharges of Intravenous Implantable Cardioverter Defibrillators Owing to Lead Failure Takashi WASHIZUKA, 1 MD, Masaomi CHINUSHI, 1 MD, Ryu KAZAMA, 1 MD, Takashi HIRONO, 1 MD, Hiroshi WATANABE,
Inappropriate Discharges of Intravenous Implantable Cardioverter Defibrillators Owing to Lead Failure Takashi WASHIZUKA, 1 MD, Masaomi CHINUSHI, 1 MD, Ryu KAZAMA, 1 MD, Takashi HIRONO, 1 MD, Hiroshi WATANABE,
Finally, a pacemaker may be either permanent or temporary, which will also factor into your code selections.
 2015 Cardiology Survival Guide Chapter 15: Pacemakers With more than 30 codes and many variables to choose from, you must weigh your options carefully when reporting insertion, revision, or removal of
2015 Cardiology Survival Guide Chapter 15: Pacemakers With more than 30 codes and many variables to choose from, you must weigh your options carefully when reporting insertion, revision, or removal of
Transvenous Pacemaker Implantation 22 years after the Mustard Procedure
 Case Report Transvenous Pacemaker Implantation 22 years after the Mustard Procedure Masato Sakamoto MD, Yoshie Ochiai MD, Yutaka Imoto MD, Akira Sese MD, Mamie Watanabe MD, Kunitaka Joo MD Department of
Case Report Transvenous Pacemaker Implantation 22 years after the Mustard Procedure Masato Sakamoto MD, Yoshie Ochiai MD, Yutaka Imoto MD, Akira Sese MD, Mamie Watanabe MD, Kunitaka Joo MD Department of
Outcomes of Defibrillator Lead Implants Performed by High Volume Operators vs. Low Volume Operators:
 Outcomes of Defibrillator Lead Implants Performed by High Volume Operators vs. Low Volume Operators: Results from the Pacemaker and Implantable Defibrillator Leads Survival Study ( PAIDLESS ) Partially
Outcomes of Defibrillator Lead Implants Performed by High Volume Operators vs. Low Volume Operators: Results from the Pacemaker and Implantable Defibrillator Leads Survival Study ( PAIDLESS ) Partially
Broken leads with proximal endings in the cardiovascular system: Serious consequences and extraction difficulties
 ORIGINAL ARTICLE Cardiology Journal 2013, Vol. 20, No. 2, pp. 161 169 DOI: 10.5603/CJ.2013.0029 Copyright 2013 Via Medica ISSN 1897 5593 Broken leads with proximal endings in the cardiovascular system:
ORIGINAL ARTICLE Cardiology Journal 2013, Vol. 20, No. 2, pp. 161 169 DOI: 10.5603/CJ.2013.0029 Copyright 2013 Via Medica ISSN 1897 5593 Broken leads with proximal endings in the cardiovascular system:
Original Article Analysis of clinical efficacy and factors affecting complications of permanent pacemaker implantation
 Int J Clin Exp Med 2019;12(2):1972-1978 www.ijcem.com /ISSN:1940-5901/IJCEM0084739 Original Article Analysis of clinical efficacy and factors affecting complications of permanent pacemaker implantation
Int J Clin Exp Med 2019;12(2):1972-1978 www.ijcem.com /ISSN:1940-5901/IJCEM0084739 Original Article Analysis of clinical efficacy and factors affecting complications of permanent pacemaker implantation
Case Report Intermittent Right Ventricular Outflow Tract Capture due to Chronic Right Atrial Lead Dislodgement
 217 Case Report Intermittent Right Ventricular Outflow Tract Capture due to Chronic Right Atrial Lead Dislodgement Partha Prateem Choudhury, Vivek Chaturvedi, Saibal Mukhopadhyay, Jamal Yusuf Department
217 Case Report Intermittent Right Ventricular Outflow Tract Capture due to Chronic Right Atrial Lead Dislodgement Partha Prateem Choudhury, Vivek Chaturvedi, Saibal Mukhopadhyay, Jamal Yusuf Department
Cardiac Rhythm Management Coder 2018
 Cardiac Rhythm Management Coder 2018 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of MedLearn Media, Inc. 445 Minnesota Street,
Cardiac Rhythm Management Coder 2018 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of MedLearn Media, Inc. 445 Minnesota Street,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Riata implantable cardioverter-defibrillator lead failure: Analysis of explanted leads with a unique insulation defect
 Riata implantable cardioverter-defibrillator lead failure: Analysis of explanted leads with a unique insulation defect Robert G. Hauser, MD, FHRS, Deepa McGriff, BS, Linda Kallinen Retel, BS, FHRS From
Riata implantable cardioverter-defibrillator lead failure: Analysis of explanted leads with a unique insulation defect Robert G. Hauser, MD, FHRS, Deepa McGriff, BS, Linda Kallinen Retel, BS, FHRS From
Key Words: Balloon Venoplasty of Subclavian Vein, Cardiac Resynchronisation Therapy. Case report
 221 Case Report Balloon Venoplasty of Subclavian Vein and Brachiocephalic Junction to Enable Left Ventricular Lead Placement for Cardiac Resynchronisation Therapy Thanh Trung Phan, Simon James, Andrew
221 Case Report Balloon Venoplasty of Subclavian Vein and Brachiocephalic Junction to Enable Left Ventricular Lead Placement for Cardiac Resynchronisation Therapy Thanh Trung Phan, Simon James, Andrew
Concurrent Failure of Active and Redundant Ventricular Epicardial Electrodes in Children
 Concurrent Failure of Active and Redundant Ventricular Epicardial Electrodes in Children ERALD A. SERWER, M.D., MACDONALD DICK 11, M.D., KAREN UZARK, R.N., Ph.D., WILLIAM A. SCOTT, M.D., and EDWARD L.
Concurrent Failure of Active and Redundant Ventricular Epicardial Electrodes in Children ERALD A. SERWER, M.D., MACDONALD DICK 11, M.D., KAREN UZARK, R.N., Ph.D., WILLIAM A. SCOTT, M.D., and EDWARD L.
King s Research Portal
 King s Research Portal DOI: 10.1016/j.tcm.2016.03.003 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Rinaldi, C. A. (2016).
King s Research Portal DOI: 10.1016/j.tcm.2016.03.003 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Rinaldi, C. A. (2016).
CONGENITAL HEART DEFECTS IN ADULTS
 CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
Leadless pacing. P.E. Vardas Professor of Cardiology University of Crete, Greece
 Leadless pacing P.E. Vardas Professor of Cardiology University of Crete, Greece DISCLOSURES Small teaching fees from: Bayer/J&J, Boeringer, Menarini Small consulting fees from: Medtronic 1957: First External
Leadless pacing P.E. Vardas Professor of Cardiology University of Crete, Greece DISCLOSURES Small teaching fees from: Bayer/J&J, Boeringer, Menarini Small consulting fees from: Medtronic 1957: First External
CIEDs Infection: Lead Extraction, First or Last option?
 CIEDs Infection: Lead Extraction, First or Last option? More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009.
CIEDs Infection: Lead Extraction, First or Last option? More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009.
1. Technology Name: WATCHMAN Left Atrial Appendage Closure Technology. 3. Trade Brand of Technology: WATCHMAN Left Atrial Appendage Closure Technology
 1. Technology Name: REASANZ (serelaxin) Injection 1 mg/ml Solution for I.V. Infusion 2. Manufacturer Name: Novartis Pharmaceuticals Corporation 3. Trade Brand of Technology: The brand name of the new technology
1. Technology Name: REASANZ (serelaxin) Injection 1 mg/ml Solution for I.V. Infusion 2. Manufacturer Name: Novartis Pharmaceuticals Corporation 3. Trade Brand of Technology: The brand name of the new technology
How to treat Cardiac Resynchronization Therapy complications? C. Leclercq Departement of Cardiology Centre Cardio-Pneumologique Rennes, France
 How to treat Cardiac Resynchronization Therapy complications? C. Leclercq Departement of Cardiology Centre Cardio-Pneumologique Rennes, France Presenter Disclosure Information Christophe Leclercq, MD,
How to treat Cardiac Resynchronization Therapy complications? C. Leclercq Departement of Cardiology Centre Cardio-Pneumologique Rennes, France Presenter Disclosure Information Christophe Leclercq, MD,
Cardiac Rhythm Management Coder 2017
 Cardiac Rhythm Management Coder 2017 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of Panacea Healthcare Solutions, Inc. 287 East
Cardiac Rhythm Management Coder 2017 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of Panacea Healthcare Solutions, Inc. 287 East
Leadless Pacemakers A Review
 Leadless Pacemakers A Review Mikhael El-Chami, MD, FACC Emory University Atlanta, Ga Consultant: Medtronic Boston Scientific Disclosure One of the leadless pacemakers discussed in this presentation is
Leadless Pacemakers A Review Mikhael El-Chami, MD, FACC Emory University Atlanta, Ga Consultant: Medtronic Boston Scientific Disclosure One of the leadless pacemakers discussed in this presentation is
Selecting the Best ICD for your Patient-SICD v. TV. Martin C. Burke DO, FACOI CorVita Science Foundation & Academic Medical Center, Amsterdam
 Selecting the Best ICD for your Patient-SICD v. TV Martin C. Burke DO, FACOI CorVita Science Foundation & Academic Medical Center, Amsterdam COI DISCLOSURES I have received lecture and proctoring honoraria
Selecting the Best ICD for your Patient-SICD v. TV Martin C. Burke DO, FACOI CorVita Science Foundation & Academic Medical Center, Amsterdam COI DISCLOSURES I have received lecture and proctoring honoraria
Management of RT patients with implanted cardiac devices: From recommendation to implementation
 Management of RT patients with implanted cardiac devices: From recommendation to implementation Coen Hurkmans Clinical Physicist Catharina Hospital Eindhoven The Netherlands 1/22 Outline CIED relocation.
Management of RT patients with implanted cardiac devices: From recommendation to implementation Coen Hurkmans Clinical Physicist Catharina Hospital Eindhoven The Netherlands 1/22 Outline CIED relocation.
Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504
 Transcatheter valve-in-valve e implantation for aortic bioprosthetic valve dysfunction Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504 Your responsibility This
Transcatheter valve-in-valve e implantation for aortic bioprosthetic valve dysfunction Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504 Your responsibility This
Portico (St. Jude Medical Inc, St.
 Review Article Portico Transcatheter Heart Valve Apostolos Tzikas 1,2, Michael Chrissoheris 2, Antonios Halapas 2, Konstantinos Spargias 2 1 Interbalkan European Medical Centre, Thessaloniki, 2 Hygeia
Review Article Portico Transcatheter Heart Valve Apostolos Tzikas 1,2, Michael Chrissoheris 2, Antonios Halapas 2, Konstantinos Spargias 2 1 Interbalkan European Medical Centre, Thessaloniki, 2 Hygeia
Pacemaker and Internal Cardioverter Defibrillator Lead Extraction: A Safe and Effective Surgical Approach
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Pacemakers, Defibrillators, and Electrophysiology in 2012
 Pacemakers, Defibrillators, and Electrophysiology in 2012 Presented by: David B. Dunn, MD, FACS, CIRCC, CPC-H, CCC National Coding Standards Sources of information Centers for Medicare & Medicaid (CMS)
Pacemakers, Defibrillators, and Electrophysiology in 2012 Presented by: David B. Dunn, MD, FACS, CIRCC, CPC-H, CCC National Coding Standards Sources of information Centers for Medicare & Medicaid (CMS)
Positive Results with a New Screw-in Electrode with Isolated Screw and Fractal Coating of the Ring: the RETROX Electrode in the Atrial Position
 314 June 1999 Positive Results with a New Screw-in Electrode with Isolated Screw and Fractal Coating of the Ring: the RETROX Electrode in the Atrial Position M. BOKERN Waterland Ziekenhuis, Purmerend,
314 June 1999 Positive Results with a New Screw-in Electrode with Isolated Screw and Fractal Coating of the Ring: the RETROX Electrode in the Atrial Position M. BOKERN Waterland Ziekenhuis, Purmerend,
TWIDDLER S syndrome is characterized by coiling of the pacemaker lead due
 Reel Syndrome and Pulsatile Liver in a Patient With a Two-chamber Pacemaker Ahmet VURAL, 1 MD, Aysen AGACDIKEN, 1 MD, Dilek URAL, 1 MD, and Baki KOMSUOGLU, 1 MD, FESC SUMMARY Twiddler s syndrome is characterized
Reel Syndrome and Pulsatile Liver in a Patient With a Two-chamber Pacemaker Ahmet VURAL, 1 MD, Aysen AGACDIKEN, 1 MD, Dilek URAL, 1 MD, and Baki KOMSUOGLU, 1 MD, FESC SUMMARY Twiddler s syndrome is characterized
Lead Extraction: Challenges in our area
 Lead Extraction: Challenges in our area More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009. 2) Boston Scientific
Lead Extraction: Challenges in our area More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009. 2) Boston Scientific
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS. HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate
 PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
Clinical Management of the Infected Pacemaker
 Clinical Management of the Infected Pacemaker W. B. Firor, M.D., J. F. Lopez, M.D., E. M. Nanson, F.R.C.S., and M. Mori, M.D. T he totally implantable electronic pacemaker has proved to be a remarkable
Clinical Management of the Infected Pacemaker W. B. Firor, M.D., J. F. Lopez, M.D., E. M. Nanson, F.R.C.S., and M. Mori, M.D. T he totally implantable electronic pacemaker has proved to be a remarkable
1. Patient Characteristics
 ELECTRa Registry CRF European Lead Extraction ConTRolled Registry * mandatory fields *Site Number 1. Patient Characteristics *Patient Number - 1.1 Demographics and Enrolment Data Inclusion criteria: All
ELECTRa Registry CRF European Lead Extraction ConTRolled Registry * mandatory fields *Site Number 1. Patient Characteristics *Patient Number - 1.1 Demographics and Enrolment Data Inclusion criteria: All
Riata Lead Extraction. Thomas D. Callahan, MD, FACC, FHRS
 Riata Lead Extraction Thomas D. Callahan, MD, FACC, FHRS Outline Riata lead history Lead design Lead Failure Extraction outcomes Techniques Special considerations Riata Lead Background 8F introduced in
Riata Lead Extraction Thomas D. Callahan, MD, FACC, FHRS Outline Riata lead history Lead design Lead Failure Extraction outcomes Techniques Special considerations Riata Lead Background 8F introduced in
Arrhythmia/Electrophysiology. Permanent Leadless Cardiac Pacing Results of the LEADLESS Trial
 Arrhythmia/Electrophysiology Permanent Leadless Cardiac Pacing Results of the LEADLESS Trial Vivek Y. Reddy, MD; Reinoud E. Knops, MD; Johannes Sperzel, MD; Marc A. Miller, MD; Jan Petru, MD; Jaroslav
Arrhythmia/Electrophysiology Permanent Leadless Cardiac Pacing Results of the LEADLESS Trial Vivek Y. Reddy, MD; Reinoud E. Knops, MD; Johannes Sperzel, MD; Marc A. Miller, MD; Jan Petru, MD; Jaroslav
Lead extraction. Dr. Mervat Abo El Maaty Professor of Cardiology Ain shams University 2013
 Lead extraction Dr. Mervat Abo El Maaty Professor of Cardiology Ain shams University 2013 Agenda Introduction History of consensus Definitions Complications Indications Lead management environment Extraction
Lead extraction Dr. Mervat Abo El Maaty Professor of Cardiology Ain shams University 2013 Agenda Introduction History of consensus Definitions Complications Indications Lead management environment Extraction
