PUPILLARY AND CIRCULATORY CHANGES AT THE TERMINATION OF RELAXANT ANAESTHESIA
|
|
|
- Daniel Edwards
- 5 years ago
- Views:
Transcription
1 Brit. J. Anaesth. (9),, 79 PUPILLARY AND CIRCULATORY CHANGES AT THE TERMINATION OF RELAXANT ANAESTHESIA BY R. E. RAWSTRON AND B. R. HUTCHINSON Department of Anaesthesia, Palmerston North Hospital, Palmerston North, New Zealand SUMMARY Observations have been made of, as affected by intravenously administered atropine and neostigmine, and by extubation, during reversal of curarization. Pulse rate and blood pressure changes were also recorded. Some degree of mydriasis was observed in 7 per cent of patients after atropine, in 8 per cent after neostigmine, and in per cent at extubation. Pulse rate increased in 88 per cent after atropine and decreased in 8 per cent after neostigmine. Blood pressure rose in 7 per cent after atropine and in 8 per cent after neostigmine. Extubation caused no consistent pulse and blood pressure changes. It was considered that the pupillary changes noted would not be deleterious in intra-ocular surgery. For several years, approximately per cent of all intra-ocular operations in this hospital have been performed with a full relaxant-type general anaesthetic with endotracheal intubation. As d-tubocurarine has been the principal muscle relaxant used, atropine and neostigmine have been injected at the end of operation to reverse residual curarization. and allied belladonna drugs have long been known for their mydriatic effects but Goodman and Gilman (9a) state that neostigmine does not have much effect on the pupil. Are these drugs, when injected intravenously at the end of an operation, harmful to the intra-ocular surgery performed? Studies on intramuscularly administered atropine by Leopold and Comroe (948), Schwartz, de Roetth and Papper (97) and Herxheimer (98) suggest that it does not produce a strong pupillary dilatation. Schwartz, de Roetth and Papper (97) also show the safety of atropine and hyoscine when given pre-operatively to glaucomatous patients. However, there is little information about the effects of atropine and neostigmine on, when given intravenously at the end of operation, or if these drugs so used are contraindicated in intra-ocular surgery. STUDY A study was made to determine the pupillary effects of atropine sulphate and neostigmine methyl sul- 79 phate injected intravenously at the end of an operation. Note was also made of the effects of extubation on. Concurrently with the above observations, records were made of the effects of the atropine, neostigmine and extubation on the pulse rate and systolic blood pressure. It is stressed that we wished to find what changes occurred in normal clinical circumstances, so fifty adult patients having general anaesthetics for routine surgical conditions were studied. Premedication was not standardized, being morphine, pethidine or papaveretum with atropine or hyoscine. Anaesthesia was induced with thiopentone, intubation was facilitated by injection of suxamethonium chloride, and anaesthesia was maintained with nitrous oxide, oxygen and d-tubocurarine or gallamine. Hyperventilation of the lungs was effected by manual intermittent positive pressure respiration. At the end of the operation atropine was given intravenously and observations were made of, pulse rate and systolic blood pressure, every minutes for minutes, at which time neostigmine was given intravenously and further observations were made at -minute intervals. The effects of extubation on the pulse, systolic blood pressure and were noted in most cases. During this period artificial pulmonary ventilation was continued until spontaneous respiration was clinically adequate. Pulse rate was measured by counting the signals from a pulse
2 79 BRITISH JOURNAL OF ANAESTHESIA monitor and blood pressure was determined manually from the radial pulse with the cuff of a standard mercury sphygmomanometer round the upper arm. Pupillary size was estimated by inspection, and an arbitrary scale of to was adopted for pupil diameter, being pinpoint, half-dilated and fully dilated. Both workers cross-checked each other's estimations from time to time to standardize measurements. Late in the series, pupil diameters were measured directly and correlated with our scale. It was found that a size pupil was approximately. mm in diameter, a size was mm, and a difference of unit was approximately. mm. The method of assessing pupil diameter provided a rapid estimation of change in not possible with direct measurement, and while not entirely accurate, both workers found it gave good correlation in their cross-checks. The doses of atropine and neostigmine given to each patient were determined by age, weight, general condition and effect of relaxant drugs. RESULTS The results are presented in two parts: Pupillary changes after injection of atropine and neostigmine and associated with extubation. Pulse and systolic blood pressure changes after injection of atropine and neostigmine, and associated with extubation. It was realized that the premedicant drugs might affect the overall results. As a number of combinations of drugs were used, and some groups were small, this did not allow any accurate comparison. The overall impression was that different premedicants did not affect the results. Pupillary Changes. An initial intravenous dose of atropine.9 mg or. mg was given, and the results were analyzed according to which of these doses was used. Twentyseven patients were given atropine.9 mg and twenty-three atropine. mg. Pupillary changes have been recorded in table I under the following headings: (i) maximum change at any time between and minutes; (ii) difference in pupil size at and minutes. Table I shows the maximum changes following both doses within the -minute period. Of the fifty patients per cent () showed increases of less than units ( mm), per cent () showed either no change or a decrease in pupillary size and 8 per cent (4) an increase of more than mm. At the end of minutes, 4 per cent () of all cases showed increases of less than units ( mm), per cent (8) showed either no change or a decrease in size, and per cent () an increase of more than mm. Thus there was a tendency after minutes for the pupil diameter to decrease slightly from its maximum dilatation. Individual case records show that if the pupil was large at the beginning of the study, increases in size could make it widely dilated, although the maximum change in size was only TABLE I Changes in after injection of atropine in patients. An arbitrary scale was used, unit corresponding to pinpoint size and units corresponding to full dilatation. (units) Total (i) Maximum change between and C minutes i\tropine -9 mg - mg No No (ii) Differences at times and minutes C>-9 mg No mg
3 PUPILLARY AND CIRCULATORY CHANGES 797 average (e.g. less than units). In one patient atropine.9 mg caused a pupil increase of units to a maximum of units, while with atropine. mg in two patients dilatation to a maximum of 8 units, one from units and the other from units, was observed. After neostigmine, the results have been analyzed in five groups, depending on the combinations of atropine and neostigmine used:.9 mg with neostigmine. mg ()..9 mg with neostigmine. mg ().. mg with neostigmine. mg (). mg with neostigmine. mg (7) mg with neostigmine. mg () patients to whom further atropine was given with the neostigmine. Table II shows the difference in pupillary size when the final reading was at minutes and the initial reading was at minutes, i.e. when the neostigmine was given. This table shows that in per cent of all cases (8) there were increases of less than units dilatation difference at the times stated, with per cent () showing no change or miosis, and 4 per cent () an increase in diameter greater than mm. Table III shows the differences between the final reading at minutes and the initial reading at minutes (the original before atropine injection). In the table, 4 per cent () of patients showed less than units dilatation increase from the original, 44 per cent () showed no change or a diminution in size, and 4 per cent (7) an increase of more than mm. TABLE II Differences between size of pupil at time of neostigmine injection ( minutes after atropine injection) and minutes later. Change in (units) mg -9 mg -9 mg mg mg (divided) Neostigmine mg Neostigmine - mgneostigmine mg Neost: igmine - mg Neostigmine - mg o/ 4 4 Total 7 % Change in (units) TABLE III Differences between size of pupil before injection of atropine and minutes later ( minutes after neostigmine injection). mg -9 mg -9 mg - mg. mg (divided) Neostigmine mg Neostigmine- mg Neostigmine - mg Neostigmline - mg Neostigmine - mg 4»/ 4 4»/ Total 7
4 798 BRITISH JOURNAL OF ANAESTHESIA Change in (units) TABLE IV Maximum changes in during the -minute period after injection of neostigmine. - mg -9 mg -9 mg - mg - mg (divided) Neostigmine -mgneostigmine - mg Neostigmine mgneostigmine - mg Neostigmine - mg V so so V Table IV shows the maximum pupillary changes occurring at any moment during the -minute period after the neostigmine was injected. From table IV it can be seen that 7 per cent of cases () showed maximum changes of less than units, 4 per cent (7) showed no change or a miosis, and per cent (8) had increases over mm. Comparison of the results shown in tables II and IV shows that there is a tendency for the pupil to decrease from its maximum dilatation by the end of this -minute period. The maximum pupil sizes after neostigmine (also associated with extubation and wakening vide infra) were 8 units (one patient), 7 units (one patient) and units (two patients). In eight patients the pupil dilated to units and in the remaining thirty-nine patients dilatation reached a maximum diameter of less than units. Table V shows pupillary changes after extubation in forty-five patients. In 48.4 per cent of patients () the pupils increased in size less than units. In 44 per cent () no change or a constriction was observed and in. per cent () increases of more than mm diameter were noted. TABLE V Changes in after extubation (4 patients). Change in (units) of cases Per cent - -t DISCUSSION Table VI summarizes the changes which occurred after injection of atropine and neostigmine and in association with extubation. Some degree of mydriasis occurred in 7 per cent of all patients () after atropine, in 8 per cent (4) after neostigmine and in per cent () at the time of extubation. In a proportion of patients no change was observed, whilst in 4.4 per cent () to 4 per cent (7) some degree of pupillary constriction was evident. It is interesting that in per cent (8) of all patients the pupils showed no change, or even some constriction, during the minutes following the atropine injection, when some degree of dilatation would have been expected. The lightening of the level of anaesthesia may have been a factor here, because a number of patients began to breathe spontaneously during this period. During the period following the injection of neostigmine the anaesthetic level was decreased, so that while pupillary changes were attributed to the neostigmine, some of the results are partly due to the lightening level of anaesthesia with reactions to painful stimuli and the effects of extubation. It was not possible to differentiate between these three factors. What has been recorded is the effect of anaesthetic management on the pupil during this period. The 9.4 per cent (7) of patients showing changes with extubation will also be noted in table IV. This study shows that injection of atropine and neostigmine, and extubation (including painful stimuli) cause pupillary changes. In the majority of cases dilatation or constriction is slight, the change in diameter being mm or less. Do
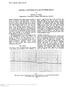
5 PUPILLARY AND CIRCULATORY CHANGES 799 TABLE VI Summary of pupil changes after injection of atropine and minutes later of neostigmine in patients, and changes associated with extubation in 4 patients. Changes expressed as percentage of series. Changes in at min maximum Neostigmine - min Neostigmine - min Neostigmine maximum Extubation Dilatation less than units 4% % % 4% 7% 48-4% Dilatation more than units % 8% 4% 4% % -% No change 4% 4% % % 8% 9'% Constriction 4% % % 4% % 4-4% TABLE VII Changes in pulse rate and blood pressure after injection of atropine and neostigmine ( patients), and associated with extubation. Increased Decreased No change Agent Measurement Neostigmine Extubation Pulse rate Blood pressure Pulse rate Blood pressure Pulse rate (4 cases) Blood pressure (4 cases) OO OO these changes produce any harmful effects on the eye in which intra-ocular surgery has been performed? It is usual to instill either atropine or physostigmine (eserine) after surgery to produce either mydriasis or miosis. These topically applied solutions contain a much higher total quantity of the drugs than could reach the eye as a unit of intravenous injection, so producing a more powerful effect. It is unlikely that the drugs given intravenously will affect the mydriasis or miosis produced by the local instillations. Whilst atropine is an antagonist to physostigmine (Goodman and Gilman, 9b), it is unlikely that the intravenous atropine will dilate the pupil already constricted by physostigmine. However, it must be remembered that all components studied can have an action on the pupil, either dilatating or constricting it. While we feel that these effects will not nullify pupillary changes produced by local instillations to an eye, efforts should be made to keep their effects to a minimum, especially reflexes due to painful stimuli and extubation. Changes in Pulse Rate and Blood Pressure. In fifty patients pulse and systolic blood pressure recordings were made at -minute intervals for minutes after the administration of atropine. The neostigmine was injected and recordings were made for a further minutes. The results are shown in table VII. Effects of atropine. In 88 per cent of the patients (44) there was a rise in pulse rate after atropine, varying from 4 to 7 beats/min. The majority of these (9 per cent, 4 cases) increased by to beats per minute (fig. ). Maximum pulse rates were 44, and 8 beats/min, one rate being doubled after atropine. There appeared to be no appreciable difference in pulse changes whether.9 or. mg of atropine had been given. In 7 per cent () of the patients there was elevation of the systolic blood pressure, varying from 4 to 44 mm Hg. The majority of these (9 per cent, cases) ranged from to 4 mm
6 8 BRITISH JOURNAL OF ANAESTHESIA a a. V a CL. JZL Decrease Increase (beats/min) FIG. Pulse rate changes after atropine ( patients).»_» C <u a i life o iim I Z ii m m I HI in ml ipfi l ffl nk l HI Fall Rise (mm/hg) FIG. Blood pressure changes after atropine ( patients). o H ill ill III ill iiiiiliiii!! LJBUB Decrease Increase (beats/min) Fall Rise (mm/hg) FIG. FIG. 4 Pulse rate changes after neostigmine ( patients). Blood pressure changes after neostigmine ( patients). sip i I in i li ( j H (fig. ). Again, the different doses of atropine appeared to have no effect. The correlation of pulse and blood pressure was interesting. Of the forty-four who showed cardiac acceleration, blood pressure rose in 8 per cent (), remained steady in 4 per cent (), but fell in 8 per cent (8). Of the four cases with cardiac slowing, one had a fall in blood pressure while three showed a rise. The pressure rose after atropine in the two patients in whom the pulse remained the same. Effects of neostigmine. Pulse rate was affected considerably, 8 per cent (4) developing bradycardia after neostigmine administration. The degree of cardiac slowing was quite marked, in spite of the prior administration of atropine, ranging from a decrease of 4 to beats/min. The majority (84 per cent; cases) slowed to beats/min (fig. ) and the lowest actual rates recorded were 48, and beats/min. In these few cases further atropine was given because of the unduly slow rhythm. There was no obvious difference in pulse or blood pressure changes, whether neostigmine. or. mg had been given. Fifty-eight per cent of patients (9) showed an elevation of blood pressure, and per cent () a fall. The rise varied from 8 to mm Hg, but 79 per cent () of those showing elevation ranged from to mm (fig. 4). Falls in pressure varied from 4 to 4 mm with a fairly even spread in this range. Correlation of pulse and blood pressure figures is of interest here too. Of the forty-three patients showing bradycardia,. per cent ()
7 PUPILLARY AND CIRCULATORY CHANGES 8 had a pressure rise, per cent (9) had a fall and in 8. per cent (8) the pressure remained steady. Of the four cases with tachycardia, two had a rise in pressure, one had a fall and one remained steady. Of the three cases with no change in pulse rate, two maintained a steady blood pressure while one showed an elevation. HI E Z rr 4 Decrease r i n Increase (beats/min) FIG. Pulse rate changes after extubation (4 patients). Effects of extubation. Extubation had a varying effect on pulse rate (4 cases), 9 per cent () showing an increase, 7 per cent () a decrease and 4 per cent (4) no change. The pulse rise varied from 4 to 48 beats/min, the majority being in the - range. Pulse falls varied from 4 to 4 beats/min, being fairly evenly spread in this range (fig. ). c Fall Rise (mm/hg) FIG. Blood pressure changes after extubation (4 patients). Blood pressure (forty-two cases) increased in seventeen patients (4 per cent), decreased in ten (4 per cent) and showed no change in fifteen ( per cent). These changes were mainly of the order of to mm Hg (fig. ). A pulse monitor (Burdick Telecor) was used in most patients throughout the study, and no cardiac arrhythmias were noted. While this is not ideal, it was felt that this gave a better chance of detection of arrhythmias than did mere palpation of the pulse. Unfortunately, it was not possible to obtain electrocardiographic tracings on these patients. DISCUSSION Bain and Broadbent (949) have stated that atropine may cause an initial slowing of the pulse rate, but Hunter (9) and Wood-Smith and Stewart (9a) state that this does not occur after intravenous injection. In only one of our forty-four patients who had pulse acceleration was there an initial slowing. On the other hand, four patients did show cardiac slowing without a subsequent acceleration, two of these cases returning to the pre-atropine pulse rate after several minutes. Of these five cases with pulse slowing, and in the two cases with no change, the rate had been-rapid (approximately beats/min) in five before atropine was injected. Morton and Thomas (98) have shown that initial slowing does not occur after intravenous atropine if the dose is large and is given rapidly (e.g. more than. mg in less than. minutes), or if atropine or hyoscine has been given previously as part of premedication. All patients in this series who showed pulse slowing had had long operations, so that the pre-operative atropine had been given to 4 hours prior to the intravenous atropine. This may have contributed to the slowing even though the intravenous atropine was given rapidly. A rise of blood pressure in the majority of cases after atropine supports findings quoted by Eger (9). Bradycardia after neostigmine was expected (Wylie and Churchill-Davidson, 9a), but the degree of cardiac slowing was quite marked, so that several cases required further atropine. Wood- Smith and Stewart (9b) state that blood pressure falls after the injection of neostigmine,
8 8 BRITISH JOURNAL OF ANAESTHESIA but in this series more showed an elevation than a depression. They further state, however, that when neostigmine and atropine have both been administered, the net result may be a rise in blood pressure and pulse rate. This concurs with our figures for blood pressure, but certainly not with our findings for heart rate. However, it must be remembered that the patients were beginning to awaken and to breathe spontaneously during this period, so that changes in blood pressure and pulse were not necessarily due to neostigmine alone, but could be associated with physical stimuli. Extubation showed no consistent effect on pulse and blood pressure, though there was a sufficient number showing pulse slowing (7 per cent; cases) to cause concern, particularly if this should be associated with a marked slowing produced by neostigmine. Converse, Landmesser and Harmel (9) state that there is a considerable incidence of arrhythmias on extubation in light planes of anaesthesia, and Shumacker and Hampton (9) report five cases of cardiac arrest following extubation. In four of these, death was associated directly with tracheobronchial suction and. extubation, and they sugget>t that hypoxia and vagal reflexes are involved in the cause of these mishaps. Riding and Robinson (9) show that cardiac irregularities are likely to occur with neostigmine if respiratory acidosis develops, so that a combination of neostigmine, extubation, hypoxia and lespiratory acidosis may well produce arrhythmias or even arrest. However, vagal stimulation may not be the only reaction to extubation, for 9 per cent of our patients showed a tachycardia, 4 per cent a blood pressure rise and per cent pupillary dilatation after extubation, so there seems a good case for postulating the presence of an orthosympathetic response. This response is described by Johnstone and Nisbet (9) and Stephen and Little (9) as a result of intubation, and there seems no reason why it should not occur following extubation. In conclusion, then, the major effect of intravenous atropine is to produce tachycardia, but if neostigmine is given minutes after atropine, a marked bradycardia may supervene and this, coupled with bradycardia due to extubation, is undesirable. Thus it appears that a -minute interval between atropine and neostigmine is too long. Wylie and Churchill-Davidson (9b) state that to minutes is the optimum, and Kemp and Morton (9) show that both drugs may be given simultaneously with safety. As stated before, the atropine in these cases was given rapidly, but the neostigmine was given slowly over minutes. Less marked changes with neostigmine may have resulted if this drug had been given even more slowly. If spontaneous respiration became clinically adequate during the period under study, no attempt was made to maintain anaesthesia or controlled respiration, as did Kemp and Morton (9), because it was desired to observe what actually happened to, pulse rate and blood pressure at the completion of a "normal" anaesthetic. Blood pressure changes should not cause concern unless the patient is hypertensive prior to administration of atropine and neostigmine and an elevation follows, or when he is hypotensive prior to atropine and neostigmine and the pressure falls. REFERENCES Bain, W. A., and Broadbent, J. L. (949). Death following neostigmine. Brit. med. J.,, 7. Converse. J. G., Landmesser, C. M., and Harmel, M. H. (9). Electrocardiograph^ changes during extubation. Anesthesiology,,. Eger, E. I. (n) (9)., scopolamine and related compounds. Anesthesiology,,. Goodman, L. S., and Gilman, A. (9a). The Pharmacological Basis of Therapeutics, nd ed., p. 4. New York: Macmillan. (9b). The Pharmacological Basis of Therapeutics, nd ed., p 44. New York: Macmillan. Herxheimer, A. (98). A comparison of some atropinelike drugs in man, with particular reference to their end-organ specificity. Brit. J. Pharmacol.,, 84. Hunter, A. R. (9). The anti-curare agents. Brit, med. J.,, 4. Johnstone, M., and Nisbet, H. I. A. (9). yentricular arrhythmia during halothane anaesthesia. Brit. J. Anaesth.,, 9. Kemp, S. W., and Morton, H. J. V. (9). The effect of atropine and neostigmine on the pulse rates of anaesthetised patients. Anaesthesia, 7, 7. Leopold, I. H., and Comroe, J. H. jr. (948). Effect of intramuscular administration of morphine, atropine, scopolamine and neostigmine on the human eye. Arch. Ophthal., 4, 8. Morton, H. J. V., and Thomas, E. T. (98). Effect of atropine on the heart rate. Lancet,,. Riding, J. E., and Robinson, J. S. (9). The safety of neostigmine. Anaesthesia,, 4. Schwartz, H., de Roetth, A. jr., and Papper, E. M. (97). Preanesthetic use of atropine and scopolamine in patients with glaucoma. /. Amer. med. Ass.,, 44.
9 PUPILLARY AND CIRCULATORY CHANGES 8 Shumacker, H. B., and Hampton, L. J. (9). Sudden death occurring immediately after operation in patients with cardiac disease, with particular reference to the role of aspiration through the endotracheal tube and extubation. J. thorac. Surg.,, 48. Stephen, C. R., and Little, D. M. (9). Halothane, st ed., p. 9. Baltimore: Williams and Wilkins. Wood-Smith, F. G., and Stewart, H. C. (9a). Drugs in Anaesthetic Practice, st ed., p. 7. London: Butterworths. (9b). Drugs in Anaesthetic Practice, st ed., p. 9. London: Butterworths. Wylie, W. D., and Churchill-Davidson, H. C. (9a). A Practice of Anaesthesia, st ed., p.. London: Lloyd-Luke. (9b). A Practice of Anaesthesia, st ed., p.. London: Lloyd-Luke. MODIFICATIONS DE LA PUPILLE ET DE LA CIRCULATION A LA FIN DUNE ANESTHfiSIE PROVOQUfiE PAR DES PRODUITS PLfiGIQUES SOMMAIRE Observations sur les dimensions de la pupille apres atropine ou ne'ostigmine i.v. et lors du de'tubage d inversion de curarisation. Les auteurs e'tudierent egalement le pouls et les modifications de la tension arterielle. Un certain degre de mydriase fut observe" chez 7% des patients apres atropine, chez 8% apres ne'ostigmine et chez % lors du detubage. Le pouls s'accelera chez 88% apres atropine, mais ralentit chez 8% apres neostigmine. Le tension arterielle augmenta chez 7% des patients apres atropine et chez 8% apres neostigmine. Le detubage ne modifia de facon consequente ni pouls ni tension arterielle. Les auteurs estiment que les modifications de la pupille ainsi provoquees n'auraient pas d'effet defavorable ou nuisible lors d'interventions intra-oculaires. PUPILLEN- UND KREISLAUFVERANDERUN- GEN BEI BEENDIGUNG EINER ANASTHESIE MIT RELAXANTIEN ZUSAMMENFASSUNO Es wurden Beobachtungen der Pupillenweite, wie sie nach intravenoser Verabfolgung von Atropin und Neostigmin und durch die Extubation wahrend der Umkehrung der Curarisierung auftreten, durchgefiihrt. Anderungen der Pulsfrequenz und des Blutdruckes wurden ebenfalls registriert. Bei 7 Prozent der Patienten mit Atropinverabfolgung wurde ein gewifies Mali an Pupillenerweiterung beobachtet, nach Neostigmin bei 8 Prozent und wahrend der Extubation bei Prozent. Die Pulsrate war nach Atropin in 88 Prozent gesteigert und nach Neostigmin bei 8 Prozent erniedrigt. Nach Atropin stieg bei 7 Prozent und nach Neostigmin bei 8 Prozent der Blutdruck an. Durch die Extubation wurden keine konstanten Puls- und Blutdruckveranderungen verursacht. Es kann angenommen werden, dafi die beobachteten Pupillenveranderungen sich nicht schadlich bei der intraokularen Chirurgie auswirken.
NITROUS OXIDE-CURARE ANESTHESIA UNSUPPLEMENTED WITH CENTRAL DEPRESSANTS
 Brit. J. Anasth. (1953). 25, 237 NITROUS OXIDE-CURARE ANESTHESIA UNSUPPLEMENTED WITH CENTRAL DEPRESSANTS By HENNING RUBEN The Finsen Institute, Copenhagen IN a previous communication (Ruben and Andreassen,
Brit. J. Anasth. (1953). 25, 237 NITROUS OXIDE-CURARE ANESTHESIA UNSUPPLEMENTED WITH CENTRAL DEPRESSANTS By HENNING RUBEN The Finsen Institute, Copenhagen IN a previous communication (Ruben and Andreassen,
CONCENTRATIONS OF DIETHYL ETHER IN THE BLOOD OF INTUBATED AND NON-INTUBATED PATIENTS
 Brit. J. Anaesth. (1954), 26, 111. CONCENTRATIONS OF DIETHYL ETHER IN THE BLOOD OF INTUBATED AND NON-INTUBATED PATIENTS BY A. MACKENZIE, E. A. PASK AND J. G. ROBSON Medical School, King's College, and
Brit. J. Anaesth. (1954), 26, 111. CONCENTRATIONS OF DIETHYL ETHER IN THE BLOOD OF INTUBATED AND NON-INTUBATED PATIENTS BY A. MACKENZIE, E. A. PASK AND J. G. ROBSON Medical School, King's College, and
THE ANALGESIC PROPERTIES OF SUB-ANAESTHETIC DOSES OF ANAESTHETICS IN THE MOUSE
 Brit. J. Pharmacol. (1964), 22, 596-63. THE ANALGESIC PROPERTIES OF SUB-ANAESTHETIC DOSES OF ANAESTHETICS IN THE MOUSE BY M. J. NEAL AND J. M. ROBSON From the Department of Pharmacology, Guy's Hospital
Brit. J. Pharmacol. (1964), 22, 596-63. THE ANALGESIC PROPERTIES OF SUB-ANAESTHETIC DOSES OF ANAESTHETICS IN THE MOUSE BY M. J. NEAL AND J. M. ROBSON From the Department of Pharmacology, Guy's Hospital
A COMPARISON OF THE EFFECTS OF SUXAMETHONIUM AND TUBOCURARINE IN PATIENTS IN LONDON AND NEW YORK
 Brit. J. Anaesth. (1969), 41, 1041 A COMPARISON OF THE EFFECTS OF SUXAMETHONIUM AND TUBOCURARINE IN PATIENTS IN LONDON AND NEW YORK BY R. L. KATZ, J. NORMAN, R. F. SEED AND L. CONRAD SUMMARY The effects
Brit. J. Anaesth. (1969), 41, 1041 A COMPARISON OF THE EFFECTS OF SUXAMETHONIUM AND TUBOCURARINE IN PATIENTS IN LONDON AND NEW YORK BY R. L. KATZ, J. NORMAN, R. F. SEED AND L. CONRAD SUMMARY The effects
ARRHYTHMIAS PRODUCED BY COMBINATIONS OF HALOTHANE AND SMALL AMOUNTS OF VASOPRESSOR
 ARRHYTHIAS PRODUCED BY COBINATIONS O HALOTHANE AND SALL AOUNTS O VASOPRESSOR WILLIA I. HIRSHO, 1 D..D., RICHARD G. TAYLOR, 2 B.D.S.,.S., D..D. and JOHN C. SHEEHAN, 3.D. WHEN epinephrine in relatively large
ARRHYTHIAS PRODUCED BY COBINATIONS O HALOTHANE AND SALL AOUNTS O VASOPRESSOR WILLIA I. HIRSHO, 1 D..D., RICHARD G. TAYLOR, 2 B.D.S.,.S., D..D. and JOHN C. SHEEHAN, 3.D. WHEN epinephrine in relatively large
ANESTHESIA WITH METHYL-N-PROPYL ETHER WITH SPECIAL REFERENCE TO THE CHANGES IN THE ELECTROCARDIOGRAM AND BLOOD SUGAR. By A. R.
 ANESTHESIA WITH METHYL-N-PROPYL ETHER WITH SPECIAL REFERENCE TO THE CHANGES IN THE ELECTROCARDIOGRAM AND BLOOD SUGAR By A. R. HUNTER M ETHYL-N-PROPYL ETHER, which is an isomer of ordinary di-ethyl ether,
ANESTHESIA WITH METHYL-N-PROPYL ETHER WITH SPECIAL REFERENCE TO THE CHANGES IN THE ELECTROCARDIOGRAM AND BLOOD SUGAR By A. R. HUNTER M ETHYL-N-PROPYL ETHER, which is an isomer of ordinary di-ethyl ether,
SORE THROAT AFTER ANAESTHESIA
 Brit. J. Anaesth. (1960), 32, 219 SORE THROAT AFTER ANAESTHESIA BY C. M. CONWAY, J. S. MILLER AND F. L. H. SUGDEN Department of Anaesthesia, Charing Cross Hospital Medical School, London, W.C.2 A sore
Brit. J. Anaesth. (1960), 32, 219 SORE THROAT AFTER ANAESTHESIA BY C. M. CONWAY, J. S. MILLER AND F. L. H. SUGDEN Department of Anaesthesia, Charing Cross Hospital Medical School, London, W.C.2 A sore
THE HEART RATE WITH EXERCISE IN PATIENTS WITH AURICULAR FIBRILLATION
 THE HEART RATE WTH EXERCSE N PATENTS WTH AURCULAR FBRLLATON BY n a previous article (Knox, 1940) an accurate method of recording the changes in heart rate during exercise was described, and results were
THE HEART RATE WTH EXERCSE N PATENTS WTH AURCULAR FBRLLATON BY n a previous article (Knox, 1940) an accurate method of recording the changes in heart rate during exercise was described, and results were
EFFECT OF HALOTHANE ON TUBOCURARINE AND SUXAMETHONIUM BLOCK IN MAN
 Brit. J. Anaesth. (1968), 40, 602 EFFECT OF HALOTHANE ON TUBOCURARINE AND SUXAMETHONIUM BLOCK IN MAN BY ANIS BARAKA SUMMARY The effect of halothane 2 per cent on neuromuscular transmission and its interaction
Brit. J. Anaesth. (1968), 40, 602 EFFECT OF HALOTHANE ON TUBOCURARINE AND SUXAMETHONIUM BLOCK IN MAN BY ANIS BARAKA SUMMARY The effect of halothane 2 per cent on neuromuscular transmission and its interaction
THE TOXICITY OF XYLOCAINE
 THE TOXICITY OF XYLOCAINE By A. R. HUNTER T HE local anaesthetic drug was discovered some years ago by Lofgren (1948), and has been used quite extensively in clinical anaesthesia in Sweden. It has proved
THE TOXICITY OF XYLOCAINE By A. R. HUNTER T HE local anaesthetic drug was discovered some years ago by Lofgren (1948), and has been used quite extensively in clinical anaesthesia in Sweden. It has proved
CLINICAL SIGNIFICANCE OF THE EFFECTS OF THIOPENTONE AND ADJUVANT DRUGS ON BLOOD SUGAR AND GLUCOSE TOLERANCE
 Brit. J. Anaesth. (195), 3, 77 CLINICAL SIGNIFICANCE OF THE EFFECTS OF THIOPENTONE AND ADJUVANT DRUGS ON BLOOD SUGAR AND GLUCOSE TOLERANCE BY JOHN W. DUNDEE AND URSULA M. TODD Department of Anaesthesia,
Brit. J. Anaesth. (195), 3, 77 CLINICAL SIGNIFICANCE OF THE EFFECTS OF THIOPENTONE AND ADJUVANT DRUGS ON BLOOD SUGAR AND GLUCOSE TOLERANCE BY JOHN W. DUNDEE AND URSULA M. TODD Department of Anaesthesia,
TRACHEOBRONCHIAL SUCTION IN INFANTS AND CHILDREN
 Brit. J. Anaesth. (1963), 35, 322 TRACHEOBRONCHIAL SUCTION IN INFANTS AND CHILDREN BY GORDON H. BUSH Department of Anaesthesia, University of Liverpool, England SUMMARY Angulated and straight catheters
Brit. J. Anaesth. (1963), 35, 322 TRACHEOBRONCHIAL SUCTION IN INFANTS AND CHILDREN BY GORDON H. BUSH Department of Anaesthesia, University of Liverpool, England SUMMARY Angulated and straight catheters
THE NEUROMUSCULAR BLOCKING PROPERTIES OF A NEW STEROID COMPOUND, PANCURONIUM BROMIDE A Pilot Study in Man
 Brit. J. Anaesth. (1967), 39, 775 THE NEUROMUSCULAR BLOCKING PROPERTIES OF A NEW STEROID COMPOUND, PANCURONIUM BROMIDE A Pilot Study in Man BY W. L. M. BAIRD AND A. M. REID Department of Anaesthetics,
Brit. J. Anaesth. (1967), 39, 775 THE NEUROMUSCULAR BLOCKING PROPERTIES OF A NEW STEROID COMPOUND, PANCURONIUM BROMIDE A Pilot Study in Man BY W. L. M. BAIRD AND A. M. REID Department of Anaesthetics,
THIOPENTONE INDUCTION AND THE ELECTROCARDIOGRAM. Royal Infirmary, Hull, England
 Brit. J. Anaesth. (1958), 3, 5 THIOPENTONE INDUCTION AND THE ELECTROCARDIOGRA SINCE 1932 the thiobarbiturates have been extensively used intravenously as a pleasant and effective means of inducing anaesthesia.
Brit. J. Anaesth. (1958), 3, 5 THIOPENTONE INDUCTION AND THE ELECTROCARDIOGRA SINCE 1932 the thiobarbiturates have been extensively used intravenously as a pleasant and effective means of inducing anaesthesia.
ROLE OF ORAL GLYCEROL IN GLAUCOMA*
 Brit. J. Ophthal. (1965) 49, 660 ROLE OF ORAL GLYCEROL IN GLAUCOMA* BY P. AWASTHI AND S. N. SRIVASTAVA Department of Ophthalmology,_Sarojni Naidu Medical College, Agra, India IN cases of acute glaucoma
Brit. J. Ophthal. (1965) 49, 660 ROLE OF ORAL GLYCEROL IN GLAUCOMA* BY P. AWASTHI AND S. N. SRIVASTAVA Department of Ophthalmology,_Sarojni Naidu Medical College, Agra, India IN cases of acute glaucoma
THE INFLUENCE OF BODY WEIGHT, SEX AND AGE ON THE DOSAGE OF THIOPENTONE
 Brit. J. Anaesth. (1954), 26, 164. THE INFLUENCE OF BODY WEIGHT, SEX AND AGE ON THE DOSAGE OF THIOPENTONE BY JOHN W. DUNDEE Department of Anaesthesia, University of Liverpool "... there is no definite
Brit. J. Anaesth. (1954), 26, 164. THE INFLUENCE OF BODY WEIGHT, SEX AND AGE ON THE DOSAGE OF THIOPENTONE BY JOHN W. DUNDEE Department of Anaesthesia, University of Liverpool "... there is no definite
FOLLOWING the demonstration by Bovetet al (1949) and,
 Brit. J. Anasth. (1952), 24, 245. A REPORT ON THE USE OF SUCCINYLCHOLINE CHLORIDE IN A THORACIC UNIT By NANCY S. G. BUTT Liverpool Thoracic Surgical Centre FOLLOWING the demonstration by Bovetet al (1949)
Brit. J. Anasth. (1952), 24, 245. A REPORT ON THE USE OF SUCCINYLCHOLINE CHLORIDE IN A THORACIC UNIT By NANCY S. G. BUTT Liverpool Thoracic Surgical Centre FOLLOWING the demonstration by Bovetet al (1949)
THE RELAXANTS AND PULMONARY VENTILATION
 Brit. J. Anaesth. (963), 35, 5 THE RELAXANTS AND PULMONARY VENTILATION BY JOHN UTTING Alder Hey Hospital, Liverpool, England THE INFLUENCE OF RELAXANTS ON and Gray (959) who described the use of passive
Brit. J. Anaesth. (963), 35, 5 THE RELAXANTS AND PULMONARY VENTILATION BY JOHN UTTING Alder Hey Hospital, Liverpool, England THE INFLUENCE OF RELAXANTS ON and Gray (959) who described the use of passive
Baseline Vital Signs and SAMPLE History. Chapter 5
 Baseline Vital Signs and SAMPLE History Chapter 5 Baseline Vital Signs and SAMPLE History Assessment is the most complex skill EMT-Bs learn. During assessment you will: Gather key information. Evaluate
Baseline Vital Signs and SAMPLE History Chapter 5 Baseline Vital Signs and SAMPLE History Assessment is the most complex skill EMT-Bs learn. During assessment you will: Gather key information. Evaluate
ELECTROCARDIOGRAPHIC STUDIES DURING ENDOTRACHEAL INTUBATION AND INFLATION OF THE CUFF
 Brit. J. Anaesth. (157), 2, 363 ELECTROCARDIOGRAPHIC STUDIES DURING ENDOTRACHEAL INTUBATION AND INLATION O THE CU INTRODUCTION THE electrocardiogram was introduced to clinical medicine in 5, and in it
Brit. J. Anaesth. (157), 2, 363 ELECTROCARDIOGRAPHIC STUDIES DURING ENDOTRACHEAL INTUBATION AND INLATION O THE CU INTRODUCTION THE electrocardiogram was introduced to clinical medicine in 5, and in it
THIS paper is written in an attempt to assess the value
 Brit. J. Anccsth. (1953). 25, 244 INTRAVENOUS PETHIDINE IN ANESTHESIA By PHILIP WOLFERS St. George's Hospital, London THIS paper is written in an attempt to assess the value of intravenous pethidine as
Brit. J. Anccsth. (1953). 25, 244 INTRAVENOUS PETHIDINE IN ANESTHESIA By PHILIP WOLFERS St. George's Hospital, London THIS paper is written in an attempt to assess the value of intravenous pethidine as
GENERAL ANAESTHESIA IN COMPLETE HEART BLOCK. Department of Anaesthetics, Glasgow Royal Infirmary, Scotland
 Brit. J. Anaesth. (1962), 34, 102 GENERAL ANAESTHESIA IN COMPLETE HEART BLOCK BY EDWARD D. T. ROSS Department of Anaesthetics, Glasgow Royal Infirmary, Scotland Modern anaesthesia has made surgery feasible
Brit. J. Anaesth. (1962), 34, 102 GENERAL ANAESTHESIA IN COMPLETE HEART BLOCK BY EDWARD D. T. ROSS Department of Anaesthetics, Glasgow Royal Infirmary, Scotland Modern anaesthesia has made surgery feasible
Departments of Physiology and Anaestliesiology, K. G's Medical College, Luck now,
 VAGAL r HIBITKO OF HEART :n.n HYPOXi:C DOGS. S. KUMAR, P. D. JAIN AND R. P. BADOLA Departments of Physiology and Anaestliesiology, K. G's Medical College, Luck now, Slowing of heart can be brought about
VAGAL r HIBITKO OF HEART :n.n HYPOXi:C DOGS. S. KUMAR, P. D. JAIN AND R. P. BADOLA Departments of Physiology and Anaestliesiology, K. G's Medical College, Luck now, Slowing of heart can be brought about
PROCAINE AMIDE IN THE CONTROL OF CARDIAC ARRHYTHMIAS
 PROCAINE AMIDE IN THE CONTROL OF CARDIAC ARRHYTHMIAS BY B. G. B. LUCAS AND D. S. SHORT From the National Heart Hospital Received March 21, 1952 Recent developments in cardiac surgery and modern methods
PROCAINE AMIDE IN THE CONTROL OF CARDIAC ARRHYTHMIAS BY B. G. B. LUCAS AND D. S. SHORT From the National Heart Hospital Received March 21, 1952 Recent developments in cardiac surgery and modern methods
Aaron J. Katz, AEMT-P, CIC Outward signs of what is occurring inside the body
 Vital Signs Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Vital Signs Outward signs of what is occurring inside the body Also give valuable information about the patient s condition They are taken
Vital Signs Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Vital Signs Outward signs of what is occurring inside the body Also give valuable information about the patient s condition They are taken
POSTOPERATIVE ANTEROGRADE AMNESIA
 Brit. J. Anaesth. (1968), 40, 845 POSTOPERATIVE ANTEROGRADE AMNESIA BY RONALD P. GRUBER AND DAVID R. REED SUMMARY The problems of defining and estimating pre- and postoperative amnesia are discussed. The
Brit. J. Anaesth. (1968), 40, 845 POSTOPERATIVE ANTEROGRADE AMNESIA BY RONALD P. GRUBER AND DAVID R. REED SUMMARY The problems of defining and estimating pre- and postoperative amnesia are discussed. The
Chapter 12 - Vital_Signs_and_Monitoring_Devices
 Introduction to Emergency Medical Care 1 OBJECTIVES 12.1 Define key terms introduced in this chapter. Slides 13 15, 17, 21 22, 26, 28, 30, 32 33, 35, 44, 47 48, 50, 55, 60 12.2 Identify the vital signs
Introduction to Emergency Medical Care 1 OBJECTIVES 12.1 Define key terms introduced in this chapter. Slides 13 15, 17, 21 22, 26, 28, 30, 32 33, 35, 44, 47 48, 50, 55, 60 12.2 Identify the vital signs
The first reversal of curare
 The first reversal of curare RWD Nickalls and EA Nickalls Anaesthesia (1985); vol. 40, p. 572 575 Abstract This paper describes an experiment performed by J. Pal of Vienna in 1900, which showed that physostigmine
The first reversal of curare RWD Nickalls and EA Nickalls Anaesthesia (1985); vol. 40, p. 572 575 Abstract This paper describes an experiment performed by J. Pal of Vienna in 1900, which showed that physostigmine
EFFECT OF ADRENERGIC BETA-RECEPTOR BLOCKER ON EPINEPHRINE-INDUCED CARDIAC ARRHYTHMIAS DURING HALOTHANE ANAESTHESIA
 EFFECT OF ADRENERGIC BETA-RECEPTOR BLOCKER ON EPINEPHRINE-INDUCED CARDIAC ARRHYTHMIAS DURING HALOTHANE ANAESTHESIA Lr.~N~aD T. T~, ~.v., D.A.(TOH.), ANDA. W. CONN, M.D., F.B.C.P.(C) * INTSOr~CTION RESULTS
EFFECT OF ADRENERGIC BETA-RECEPTOR BLOCKER ON EPINEPHRINE-INDUCED CARDIAC ARRHYTHMIAS DURING HALOTHANE ANAESTHESIA Lr.~N~aD T. T~, ~.v., D.A.(TOH.), ANDA. W. CONN, M.D., F.B.C.P.(C) * INTSOr~CTION RESULTS
ATROPINE AS AN ANTISIALOGOGUE, COMPARED WITH L-HYOSCYAMINE (BELLAFOLINE), SCOPOLAMINE BUTYLBROMIDE (BUSCOPAN) AND OXYPHENONIUM (ANTRENYL)
 Brit. J. Anaesth. (959), 3, 05 ATROPINE AS AN ANTISIALOGOGUE, COMPARED WITH LHYOSCYAMINE (BELLAFOLINE), SCOPOLAMINE BUTYLBROMIDE (BUSCOPAN) AND OXYPHENONIUM (ANTRENYL) BY H. DlAMANT The Ear, Nose and Throat
Brit. J. Anaesth. (959), 3, 05 ATROPINE AS AN ANTISIALOGOGUE, COMPARED WITH LHYOSCYAMINE (BELLAFOLINE), SCOPOLAMINE BUTYLBROMIDE (BUSCOPAN) AND OXYPHENONIUM (ANTRENYL) BY H. DlAMANT The Ear, Nose and Throat
Birds are hard to keep alive...
 Birds are hard to keep alive... Advances in Drugs Monitoring Understanding of birds Anaesthesia provides.. Immobilisation Analgesia Muscle relaxation Oxygen Reduced stress? Better control... Intubation
Birds are hard to keep alive... Advances in Drugs Monitoring Understanding of birds Anaesthesia provides.. Immobilisation Analgesia Muscle relaxation Oxygen Reduced stress? Better control... Intubation
Magnesium Sulphate - Management of Hypertensive Disorders of Pregnancy
 1. Purpose Magnesium sulphate is the anticonvulsant of choice for pre-eclampsia prophylaxis and treatment. This clinical guideline outlines the indications, contraindications, administration and monitoring
1. Purpose Magnesium sulphate is the anticonvulsant of choice for pre-eclampsia prophylaxis and treatment. This clinical guideline outlines the indications, contraindications, administration and monitoring
Effect of Vecuronium in different age group
 Original Research Article Effect of Vecuronium in different age group Bharti Rajani 1, Hitesh Brahmbhatt 2, Hemlata Chaudhry 2, Hiren Parmar 3* 1 Associate Professor, Department of Anesthesiology, GMERS
Original Research Article Effect of Vecuronium in different age group Bharti Rajani 1, Hitesh Brahmbhatt 2, Hemlata Chaudhry 2, Hiren Parmar 3* 1 Associate Professor, Department of Anesthesiology, GMERS
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
POSTOPERATIVE HEADACHE AFTER NITROUS OXIDE-OXYGEN- HALOTHANE ANAESTHESIA
 Brit. J. Anaesth. (969), 4, 972 POSTOPERATVE HEADACHE AFTER NTROUS OXDE-OXYGEN- HALOTHANE ANAESTHESA BY A. F. M. ZOHARY SUMMARY Observations were made in patients of both sexes on the frequency of in the
Brit. J. Anaesth. (969), 4, 972 POSTOPERATVE HEADACHE AFTER NTROUS OXDE-OXYGEN- HALOTHANE ANAESTHESA BY A. F. M. ZOHARY SUMMARY Observations were made in patients of both sexes on the frequency of in the
INTRAMUSCULAR SUXAMETHONIUM
 Brit. J. Anaesth. (1955), 27, 338. INTRAMUSCULAR SUXAMETHONIUM BY I. H. MCDONALD AND R. BRYCE-SMITH Nnffield Department of Anaesthetics, University of Oxford THE South American Indian hunting his (1949)
Brit. J. Anaesth. (1955), 27, 338. INTRAMUSCULAR SUXAMETHONIUM BY I. H. MCDONALD AND R. BRYCE-SMITH Nnffield Department of Anaesthetics, University of Oxford THE South American Indian hunting his (1949)
PRIMARY ANGLE-CLOSURE GLAUCOMA*t A REVIEW OF PROVOCATIVE TESTS
 Brit. J. Ophthal. (1967) 51, 727 PRIMARY ANGLE-CLOSURE GLAUCOMA*t A REVIEW OF PROVOCATIVE TESTS BY RONALD F. LOWE From The Glaucoma Unit of The Royal Victorian Eye and Ear Hospital, Melbourne, and The
Brit. J. Ophthal. (1967) 51, 727 PRIMARY ANGLE-CLOSURE GLAUCOMA*t A REVIEW OF PROVOCATIVE TESTS BY RONALD F. LOWE From The Glaucoma Unit of The Royal Victorian Eye and Ear Hospital, Melbourne, and The
GLYCOPYRROLATE-NEOSTIGMINE MIXTURE FOR ANTAGONISM OF NEUROMUSCULAR BLOCK: COMPARISON WITH ATROPINE- NEOSTIGMINE MIXTURE
 Br.J. Anaesth. (1977), 49, 82 GLYCOPYRROLATE-NEOSTIGMINE MIXTURE FOR ANTAGONISM OF NEUROMUSCULAR BLOCK: COMPARISON WITH ATROPINE- NEOSTIGMINE MIXTURE R. K. MIRAKHUR, J. W. DUNDEE AND R. S. J. CLARKE SUMMARY
Br.J. Anaesth. (1977), 49, 82 GLYCOPYRROLATE-NEOSTIGMINE MIXTURE FOR ANTAGONISM OF NEUROMUSCULAR BLOCK: COMPARISON WITH ATROPINE- NEOSTIGMINE MIXTURE R. K. MIRAKHUR, J. W. DUNDEE AND R. S. J. CLARKE SUMMARY
Chapter 9 Vital Signs and SAMPLE History DOT Directory
 Chapter 9 Vital Signs and SAMPLE History U.S. Objectives U.S. Objectives are covered and/or supported by the PowerPoint Slide Program and Notes for Emergency Care, 11th Ed. Please see the Chapter 9 correlation
Chapter 9 Vital Signs and SAMPLE History U.S. Objectives U.S. Objectives are covered and/or supported by the PowerPoint Slide Program and Notes for Emergency Care, 11th Ed. Please see the Chapter 9 correlation
Core Safety Profile. Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV FI/H/PSUR/0010/002 Date of FAR:
 Core Safety Profile Active substance: Esketamine Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV P-RMS: FI/H/PSUR/0010/002 Date of FAR: 29.05.2012 4.3 Contraindications
Core Safety Profile Active substance: Esketamine Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV P-RMS: FI/H/PSUR/0010/002 Date of FAR: 29.05.2012 4.3 Contraindications
ACUTE HYPERTENSION DURING INDUCTION OF ANAESTHESIA AND ENDOTRACHEAL INTUBATION IN NORMOTENSIVE MAN
 Brit. J. Anaesth. (1970), 42, 618 ACUTE HYPERTENSION DURING INDUCTION OF ANAESTHESIA AND ENDOTRACHEAL INTUBATION IN NORMOTENSIVE MAN BY A. MILLAR FORBES AND F. G. DALLY SUMMARY In twenty-two normotensive
Brit. J. Anaesth. (1970), 42, 618 ACUTE HYPERTENSION DURING INDUCTION OF ANAESTHESIA AND ENDOTRACHEAL INTUBATION IN NORMOTENSIVE MAN BY A. MILLAR FORBES AND F. G. DALLY SUMMARY In twenty-two normotensive
J. Physiol. (I957) I37, I4I-I53
 141 J. Physiol. (I957) I37, I4I-I53 EFFECTS OF NORADRENALINE AND ADRENALINE ON THE ATRIAL RHYTHM IN THE HEART-LUNG PREPARATION BY J. H. BURN, A. J. GUNNING AND J. M. WALKER From the Department of Pharmacology,
141 J. Physiol. (I957) I37, I4I-I53 EFFECTS OF NORADRENALINE AND ADRENALINE ON THE ATRIAL RHYTHM IN THE HEART-LUNG PREPARATION BY J. H. BURN, A. J. GUNNING AND J. M. WALKER From the Department of Pharmacology,
Experience with hypotensive anaesthesia in a peripheral General Hospital
 Med. J. Malaysia Vol. 44 No. 4 December 1989 Experience with hypotensive anaesthesia in a peripheral General Hospital A.F. Miranda, MBBS, FFARCS Consultant Anaesthesiologist General Hospital, 15.200 Kota
Med. J. Malaysia Vol. 44 No. 4 December 1989 Experience with hypotensive anaesthesia in a peripheral General Hospital A.F. Miranda, MBBS, FFARCS Consultant Anaesthesiologist General Hospital, 15.200 Kota
Objectives: This presentation will help you to:
 emergency Drugs Objectives: This presentation will help you to: Five rights for medication administration Recognize different cardiac arrhythmias and determine the common drugs used for each one List the
emergency Drugs Objectives: This presentation will help you to: Five rights for medication administration Recognize different cardiac arrhythmias and determine the common drugs used for each one List the
Anesthesia Monitoring
 Anesthesia Monitoring Horatiu V. Vinerean, DVM, DACLAM Anesthesia Monitoring Anesthesia can be divided into four progressive phases. The signs relating to a certain phase are based upon the presence or
Anesthesia Monitoring Horatiu V. Vinerean, DVM, DACLAM Anesthesia Monitoring Anesthesia can be divided into four progressive phases. The signs relating to a certain phase are based upon the presence or
The Systemic Effect Of Topical Timolol On Some Cardiovascular Parameters In Owerri Municipality
 ISPUB.COM The Internet Journal of Third World Medicine Volume 5 Number 1 The Systemic Effect Of Topical Timolol On Some Cardiovascular Parameters In Owerri Municipality G Oze, M Emegwamuo, P Eleanya, H
ISPUB.COM The Internet Journal of Third World Medicine Volume 5 Number 1 The Systemic Effect Of Topical Timolol On Some Cardiovascular Parameters In Owerri Municipality G Oze, M Emegwamuo, P Eleanya, H
Bronchoscopes: Occurrence and Management
 ORIGIAL ARTICLES Res tk iratory Acidosis wi the Small Ston-Hopkins Bronchoscopes: Occurrence and Management Kang H. Rah, M.D., Arnold M. Salzberg, M.D., C. Paul Boyan, M.D., and Lazar J. Greenfield, M.D.
ORIGIAL ARTICLES Res tk iratory Acidosis wi the Small Ston-Hopkins Bronchoscopes: Occurrence and Management Kang H. Rah, M.D., Arnold M. Salzberg, M.D., C. Paul Boyan, M.D., and Lazar J. Greenfield, M.D.
OBSERVATIONS IN THE IMMEDIATE POSTANAESTHESIA PERIOD II. MODE OF RECOVERY
 Brit. J. Anaesth. (960),, 8 OBSERVATIONS IN THE IMMEDIATE POSTANAESTHESIA PERIOD II. MODE OF RECOVERY BY ANDRE SMESSAERT,* CLAIRE A. SCHEHR AND JOSEPH F. ARTUSIO, JR. Department of Anesthesiology, The
Brit. J. Anaesth. (960),, 8 OBSERVATIONS IN THE IMMEDIATE POSTANAESTHESIA PERIOD II. MODE OF RECOVERY BY ANDRE SMESSAERT,* CLAIRE A. SCHEHR AND JOSEPH F. ARTUSIO, JR. Department of Anesthesiology, The
BLOOD OXYGEN SATURATION DURING ANAESTHESIA WITH VOLATILE AGENTS VAPORIZED IN ROOM AIR*
 Brit. J. Anaesth. (96),, 6 BLOOD OXYGEN SATURATION DURING ANAESTHESIA WITH VOLATILE AGENTS VAPORIZED IN ROOM AIR* BY P. V. COLE AND J. PARKHOUSE Nuffield Department of Anaesthetics, Oxford, England ANAESTHETISTS
Brit. J. Anaesth. (96),, 6 BLOOD OXYGEN SATURATION DURING ANAESTHESIA WITH VOLATILE AGENTS VAPORIZED IN ROOM AIR* BY P. V. COLE AND J. PARKHOUSE Nuffield Department of Anaesthetics, Oxford, England ANAESTHETISTS
THE PERMANENT PACEMAKER SYSTEM FOR THE TREATMENT OF HEART BLOCK IN THE DOG. Lanqford House, Lanqford, Bristol
 - 30 - THE PERMANENT PACEMAKER SYSTEM FOR THE TREATMENT OF HEART BLOCK IN THE DOG J. N. Lucke - Department of Veterinary Surqery, University of Bristol, Lanqford House, Lanqford, Bristol -- I IGTRODUCT
- 30 - THE PERMANENT PACEMAKER SYSTEM FOR THE TREATMENT OF HEART BLOCK IN THE DOG J. N. Lucke - Department of Veterinary Surqery, University of Bristol, Lanqford House, Lanqford, Bristol -- I IGTRODUCT
MUSCLE relaxants are used to provide better operating conditions for
 CLEVELAND CLINIC QUARTERLY Copyright 1970 by The Cleveland Clinic Foundation Volume 37, July 1970 Printed in U.S.A. Pancuronium bromide A new non-depolarizing muscle relaxant Preliminary in fifty patients
CLEVELAND CLINIC QUARTERLY Copyright 1970 by The Cleveland Clinic Foundation Volume 37, July 1970 Printed in U.S.A. Pancuronium bromide A new non-depolarizing muscle relaxant Preliminary in fifty patients
IN this paper is described a patient who, though young and
 Brit. J. Ancesth. (1953), 25, 116. LONG ACTION OF SUXAMETHONIUM (SUCCINYLCHOLINE) CHLORIDE By J. G. BOURNE St. Thomas's Hospital, London, and Salisbury Hospital Group IN this paper is described a patient
Brit. J. Ancesth. (1953), 25, 116. LONG ACTION OF SUXAMETHONIUM (SUCCINYLCHOLINE) CHLORIDE By J. G. BOURNE St. Thomas's Hospital, London, and Salisbury Hospital Group IN this paper is described a patient
Side-effects of opioids what are they, are they common, and how do I deal with them?
 Side-effects of opioids what are they, are they common, and how do I deal with them? Professor Derek Flaherty BVMS, DVA, DipECVAA, MRCA, MRCVS RCVS and European Specialist in Veterinary Anaesthesia Opioid
Side-effects of opioids what are they, are they common, and how do I deal with them? Professor Derek Flaherty BVMS, DVA, DipECVAA, MRCA, MRCVS RCVS and European Specialist in Veterinary Anaesthesia Opioid
A STUDY OF THE BIPHASIC VENTILATORY EFFECTS OF PROPANIDID
 Brit. J. Anaesth. (1964), 36, 655 A STUDY OF THE BIPHASIC VENTILATORY EFFECTS OF PROPANIDID BY EVA HARNIK Department Anaesthesia, Royal Free Hospital, London SUMMARY The respiratory effects propanidid
Brit. J. Anaesth. (1964), 36, 655 A STUDY OF THE BIPHASIC VENTILATORY EFFECTS OF PROPANIDID BY EVA HARNIK Department Anaesthesia, Royal Free Hospital, London SUMMARY The respiratory effects propanidid
SOME surgeons have been of the opinion for a number of
 DOES ETHER AFFECT THE EXTENSIBILITY OR ELASTIC RECOIL OF MUSCLE? By J. D. P. GRAHAM and the late R. ST. A. HEATHCOTE Department of Pharmacology, Welsh National School of Medicine, Cardiff SOME surgeons
DOES ETHER AFFECT THE EXTENSIBILITY OR ELASTIC RECOIL OF MUSCLE? By J. D. P. GRAHAM and the late R. ST. A. HEATHCOTE Department of Pharmacology, Welsh National School of Medicine, Cardiff SOME surgeons
POSTOPERATIVE VOMITING Some factors affecting its incidence. Middlesex Hospital, London
 Brit. J. Anaesth. (957), 9, 4 INTRODUCTION NAUSEA, retching and have been distressingly common since the earliest days of surgical procedures carried out under general anaesthesia. During the last century
Brit. J. Anaesth. (957), 9, 4 INTRODUCTION NAUSEA, retching and have been distressingly common since the earliest days of surgical procedures carried out under general anaesthesia. During the last century
Comparison of Intubating Conditions of Succinylcholine and Rocuronium
 Comparison of Intubating Conditions of Succinylcholine and Rocuronium 1 Dr. Vaishali Kotambkar, 2 Dr. Sunil Tuljapure Abstract: The aim of study on neuromuscular drugs was to have nondepolarising muscle
Comparison of Intubating Conditions of Succinylcholine and Rocuronium 1 Dr. Vaishali Kotambkar, 2 Dr. Sunil Tuljapure Abstract: The aim of study on neuromuscular drugs was to have nondepolarising muscle
DBL NALOXONE HYDROCHLORIDE INJECTION USP
 Name of medicine Naloxone hydrochloride Data Sheet New Zealand DBL NALXNE HYDRCHLRIDE INJECTIN USP Presentation DBL Naloxone Hydrochloride Injection USP is a sterile, clear, colourless solution, free from
Name of medicine Naloxone hydrochloride Data Sheet New Zealand DBL NALXNE HYDRCHLRIDE INJECTIN USP Presentation DBL Naloxone Hydrochloride Injection USP is a sterile, clear, colourless solution, free from
Note: At the end of the instructions, you will find a table which must be filled in to complete the exercise.
 Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
THE SEDATIVE PROPERTIES OF PENTAZOCINE (FORTRAL)
 Brit. J. Anaesth. (1968), 40, 341 THE SEDATIVE PROPERTIES OF PENTAZOCINE (FORTRAL) BY WALTER NORMS AND A. B. M TELFER SUMMARY In 100 healthy gynaecological patients the sedative properties of pentazocine
Brit. J. Anaesth. (1968), 40, 341 THE SEDATIVE PROPERTIES OF PENTAZOCINE (FORTRAL) BY WALTER NORMS AND A. B. M TELFER SUMMARY In 100 healthy gynaecological patients the sedative properties of pentazocine
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Vital Signs and Oxygen Administration
 Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
BLOOD PRESSURE AND OLD AGE
 BLOOD PRESSURE AND OLD AGE BY TREVOR H. HOWELL From the Royal Hospital, Chelsea Received June 20, 1942 Twenty years ago, Thompson and Todd (1922) published an article entitled "Old age and blood pressure
BLOOD PRESSURE AND OLD AGE BY TREVOR H. HOWELL From the Royal Hospital, Chelsea Received June 20, 1942 Twenty years ago, Thompson and Todd (1922) published an article entitled "Old age and blood pressure
EMT. Chapter 14 Review
 EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff
 Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
THE EFFECT OF GENERAL ANAESTHETICS ON THE RESPONSE TO TETANIC STIMULUS IN MAN
 Brit. J. Anaesth. (1970), 42, 543 THE EFFECT OF GENERAL ANAESTHETICS ON THE RESPONSE TO TETANIC STIMULUS IN MAN BY P. J. COHEN, D. V. HEISTERKAMP AND P. SKOVSTED SUMMARY The effects of cyclopropane, diethyl
Brit. J. Anaesth. (1970), 42, 543 THE EFFECT OF GENERAL ANAESTHETICS ON THE RESPONSE TO TETANIC STIMULUS IN MAN BY P. J. COHEN, D. V. HEISTERKAMP AND P. SKOVSTED SUMMARY The effects of cyclopropane, diethyl
Time factor in the measurement of response
 Thorax (1967), 22, 538. Time factor in the measurement of response to bronchodilators G. J. MUSHIN From Pritnce Heairv's Hospital, Melbournie, A ustralia Trhe measurement of response to bronchodilators
Thorax (1967), 22, 538. Time factor in the measurement of response to bronchodilators G. J. MUSHIN From Pritnce Heairv's Hospital, Melbournie, A ustralia Trhe measurement of response to bronchodilators
RECENT ADVANCES AND FUTURE PROSPECTS IN THE MEDICAL TREATMENT OF OCULAR HYPERTENSION*
 Brit. J. Ophthal. (1954) 38, 742. RECENT ADVANCES AND FUTURE PROSPECTS IN THE MEDICAL TREATMENT OF OCULAR HYPERTENSION* BY R. WEEKERS, E. PRIJOT, AND J. GUSTIN From the Ophthalmological Clinic of the University
Brit. J. Ophthal. (1954) 38, 742. RECENT ADVANCES AND FUTURE PROSPECTS IN THE MEDICAL TREATMENT OF OCULAR HYPERTENSION* BY R. WEEKERS, E. PRIJOT, AND J. GUSTIN From the Ophthalmological Clinic of the University
RMP section VI.2 Elements for Public Summary
 RMP section VI.2 Elements for Public Summary Product: Atropin Stragen, 0,1 mg/ml solution for injection in pre-filled syringe Atropin Stragen, 0,2 mg/ml solution for injection in pre-filled syringe RMP:
RMP section VI.2 Elements for Public Summary Product: Atropin Stragen, 0,1 mg/ml solution for injection in pre-filled syringe Atropin Stragen, 0,2 mg/ml solution for injection in pre-filled syringe RMP:
ACID-BASE CHANGES IN ARTERIAL BLOOD AND CEREBROSPINAL FLUID DURING CRANIOTOMY AND HYPERVENTILATION SUMMARY
 Br. 7. Anaesth. (1974), 46, 263 ACID-BASE CHANGES IN ARTERIAL BLOOD AND CEREBROSPINAL FLUID DURING CRANIOTOMY AND HYPERVENTILATION T. V. CAMPKIN, R. G. BARKER, M. PABARI AND L. H. GROVE SUMMARY Several
Br. 7. Anaesth. (1974), 46, 263 ACID-BASE CHANGES IN ARTERIAL BLOOD AND CEREBROSPINAL FLUID DURING CRANIOTOMY AND HYPERVENTILATION T. V. CAMPKIN, R. G. BARKER, M. PABARI AND L. H. GROVE SUMMARY Several
a central pulse located at the apex of the heart Apical pulse Apical-radial pulse a complete absence of respirations Apnea
 Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Anitschkov (1936) investigated the effect of chemoreceptor denervation. of ammonium chloride. He maintained, however, that the hyperpnoea was
 J. Phy8iol. (1962), 161, pp. 351-356 351 With 4 text-figure8 Printed in Great Britain THE ROLE OF THE CHEMORECEPTORS IN THE HYPERPNOEA CAUSED BY INJECTION OF AMMONIUM CHLORIDE BY N. JOELS AND E. NEIL From
J. Phy8iol. (1962), 161, pp. 351-356 351 With 4 text-figure8 Printed in Great Britain THE ROLE OF THE CHEMORECEPTORS IN THE HYPERPNOEA CAUSED BY INJECTION OF AMMONIUM CHLORIDE BY N. JOELS AND E. NEIL From
SUMMARY OF PRODUCT CHARACTERISTICS. 1 ml solution contains 75 micrograms of sufentanilcitrate, corresponding to 50 micrograms of sufentanil.
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Sufentanil Narcomed, 50 microgram / ml, solution for injection 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 ml solution contains 75
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Sufentanil Narcomed, 50 microgram / ml, solution for injection 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 ml solution contains 75
PHARMACOLOGICAL PROBLEMS
 PHARMACOLOGICAL PROBLEMS 1. A 69 year old woman suffering from CHF has been treated with.25 mg Digoxin tablet daily for last 3 months. But the heart failure is not controlled adequately. What will be the
PHARMACOLOGICAL PROBLEMS 1. A 69 year old woman suffering from CHF has been treated with.25 mg Digoxin tablet daily for last 3 months. But the heart failure is not controlled adequately. What will be the
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
EXPERIMENTAL EVIDENCE SUPPORTING THE CONCEPTION OF ADAPTATION ENERGY
 EXPERIMENTAL EVIDENCE SUPPORTING THE CONCEPTION OF ADAPTATION ENERGY HANS SELYE Fro,m the Department of Anatomy, Histology and Embryology, McGill University, Montreal, Canada Received for publication May
EXPERIMENTAL EVIDENCE SUPPORTING THE CONCEPTION OF ADAPTATION ENERGY HANS SELYE Fro,m the Department of Anatomy, Histology and Embryology, McGill University, Montreal, Canada Received for publication May
INTRAOPERATIVE MYOCARDIAL ISCHAEMIA IN SURGICAL PATIENTS WITH TREATED ISCHAEMIC HEART DISEASE
 INTRAOPERATIVE MYOCARDIAL ISCHAEMIA IN SURGICAL PATIENTS WITH TREATED ISCHAEMIC HEART DISEASE Pages with reference to book, From 80 To 82 Rashid M. Khan, Tosifa Z. Khan, Punam Sud, G. Haq, M. Zafaruddin
INTRAOPERATIVE MYOCARDIAL ISCHAEMIA IN SURGICAL PATIENTS WITH TREATED ISCHAEMIC HEART DISEASE Pages with reference to book, From 80 To 82 Rashid M. Khan, Tosifa Z. Khan, Punam Sud, G. Haq, M. Zafaruddin
Chapter 15: Measuring Height, Weight, and Vital Signs. Copyright 2012 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 15: Measuring Height, Weight, and Vital Signs Height and Weight Weight Baseline measurement at patient s first visit Measured in kg or lbs Common types of scales Balance beam Dial Digital Height
Chapter 15: Measuring Height, Weight, and Vital Signs Height and Weight Weight Baseline measurement at patient s first visit Measured in kg or lbs Common types of scales Balance beam Dial Digital Height
Comparison of the Hemodynamic Responses with. with LMA vs Endotracheal Intubation
 Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Chapter 29 1/8/2018. Vital Signs. Measuring and Reporting Vital Signs. Key Terms
 Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
INFLUENCE OF VARIOUS DRUGS ON THE ACTION SYSTEM OF THE CAT OF CURARE ON THE CENTRAL NERVOUS
 Brit. J. Pharmacol. (1952), 7, 14. INFLUENCE OF VARIOUS DRUGS ON THE ACTION OF CURARE ON THE CENTRAL NERVOUS SYSTEM OF THE CAT BY S. SALAMA* AND SAMSON WRIGHT From the Department of Physiology, Middlesex
Brit. J. Pharmacol. (1952), 7, 14. INFLUENCE OF VARIOUS DRUGS ON THE ACTION OF CURARE ON THE CENTRAL NERVOUS SYSTEM OF THE CAT BY S. SALAMA* AND SAMSON WRIGHT From the Department of Physiology, Middlesex
Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical]
![Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical]](/thumbs/87/96512765.jpg) Children s Acute Transport Service Clinical Guidelines Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Document Control Information Author D Lutman Author Position Head of Clinical
Children s Acute Transport Service Clinical Guidelines Acute Neurosurgical Emergency Transfer [see also CATS SOP neurosurgical] Document Control Information Author D Lutman Author Position Head of Clinical
ADVANCED ASSESSMENT Vital Signs
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Vital Signs 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Vital Signs AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager Grey-Bruce-Huron
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Vital Signs 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Vital Signs AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager Grey-Bruce-Huron
ESTERS AND SODIUM NITRITE IN MAN
 ACQUIRED TOLERANCE TO AND CROSS TOLERANCE BETWEEN THE NITROUS AND NITRIC ACID ESTERS AND SODIUM NITRITE IN MAN L. A. CRANDALL, JR., C. D. LEAKE, A. S. LOEVENHART AND C. W. MUEHLBERGER From the Pharmacological
ACQUIRED TOLERANCE TO AND CROSS TOLERANCE BETWEEN THE NITROUS AND NITRIC ACID ESTERS AND SODIUM NITRITE IN MAN L. A. CRANDALL, JR., C. D. LEAKE, A. S. LOEVENHART AND C. W. MUEHLBERGER From the Pharmacological
Shaded areas=not MARKETED 24/2/09
 PACKAGE INSERT SCHEDULING STATUS Schedule 6 PROPRIETARY NAME AND DOSAGE FORM RAPIFEN 2 ml IV injection RAPIFEN 10 ml IV injection COMPOSITION Each ml contains alfentanil hydrochloride 0,544 mg (equivalent
PACKAGE INSERT SCHEDULING STATUS Schedule 6 PROPRIETARY NAME AND DOSAGE FORM RAPIFEN 2 ml IV injection RAPIFEN 10 ml IV injection COMPOSITION Each ml contains alfentanil hydrochloride 0,544 mg (equivalent
Topic: Baseline Vitals and Sample History Company Drill
 Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE
 Br. J. Anaesth. (987), 59, 24-28 SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE J. M. LAMBERTY AND I. H. WILSON Two studies have demonstrated that the induction of anaesthesia using a single breath
Br. J. Anaesth. (987), 59, 24-28 SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE J. M. LAMBERTY AND I. H. WILSON Two studies have demonstrated that the induction of anaesthesia using a single breath
A COMPARISON OF VENTURI AND SIDE-ARM VENTILATION IN ANAESTHESIA FOR BRONCHOSCOPY
 A COMPARISON OF VENTURI AND SIDE-ARM VENTILATION IN ANAESTHESIA FOR BRONCHOSCOPY EDWARD CARDEN, M.A., M.B., B.CHm., F.R.C.P.(C), WALTER W. BURNS, M.D., NOEL B. MCDEvITr, M.D., AND TED CARSON, M.D. ~ EVER
A COMPARISON OF VENTURI AND SIDE-ARM VENTILATION IN ANAESTHESIA FOR BRONCHOSCOPY EDWARD CARDEN, M.A., M.B., B.CHm., F.R.C.P.(C), WALTER W. BURNS, M.D., NOEL B. MCDEvITr, M.D., AND TED CARSON, M.D. ~ EVER
Clinical Problem. Management. Discussion
 Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
Atropine therapy in acute anticholinesterase (Organophosphorus / carbamate) poisoning; adherence to current guidelines
 Atropine therapy in acute anticholinesterase (Organophosphorus / carbamate) poisoning; adherence to current guidelines 1,,3 1 3 Jayasinghe SS, Fernando A, Pathirana KD, K Kishanthi Gunasinghe 1 Department
Atropine therapy in acute anticholinesterase (Organophosphorus / carbamate) poisoning; adherence to current guidelines 1,,3 1 3 Jayasinghe SS, Fernando A, Pathirana KD, K Kishanthi Gunasinghe 1 Department
Pharmacokinetics. Inhalational Agents. Uptake and Distribution
 Pharmacokinetics Inhalational Agents The pharmacokinetics of inhalational agents is divided into four phases Absorption Distribution (to the CNS Metabolism (minimal Excretion (minimal The ultimate goal
Pharmacokinetics Inhalational Agents The pharmacokinetics of inhalational agents is divided into four phases Absorption Distribution (to the CNS Metabolism (minimal Excretion (minimal The ultimate goal
Indian Diploma in Critical Care Nursing
 Indian Diploma in Critical Care Nursing MCQ Section A - Only one answer is correct 1. Four emergency interventions used in resuscitating a patient in cardiac arrest. a. Adrenaline/Atropine/ Amiodarone/Defibrillation
Indian Diploma in Critical Care Nursing MCQ Section A - Only one answer is correct 1. Four emergency interventions used in resuscitating a patient in cardiac arrest. a. Adrenaline/Atropine/ Amiodarone/Defibrillation
THE CARDIOVASCULAR ACTIONS OF SUXAAiETHONIUM IN THE CAT
 Brit. J. Anaesth. (1961), 33, 560 THE CARDIOVASCULAR ACTIONS OF SUXAAiETHONIUM IN THE CAT BY C. M. CONWAY Department of Anaesthetics, Hammersmith Hospital and Postgraduate Medical School, London Since
Brit. J. Anaesth. (1961), 33, 560 THE CARDIOVASCULAR ACTIONS OF SUXAAiETHONIUM IN THE CAT BY C. M. CONWAY Department of Anaesthetics, Hammersmith Hospital and Postgraduate Medical School, London Since
Dr.R.K.Yadava Associate Prof.&Head Department of kayachikitsa SRM Govt.Ayu.College&Hospital, Bareilly
 Dr.R.K.Yadava Associate Prof.&Head Department of kayachikitsa SRM Govt.Ayu.College&Hospital, Bareilly Email-drrky68@gmail.com General examination is most important aspect in clinical practice. Learn the
Dr.R.K.Yadava Associate Prof.&Head Department of kayachikitsa SRM Govt.Ayu.College&Hospital, Bareilly Email-drrky68@gmail.com General examination is most important aspect in clinical practice. Learn the
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
How To Measure Vital Signs
 How To Measure Vital Signs How to Use This Tutorial This tutorial is intended for healthcare providers or students to teach basic vital signs skills Use the navigation buttons below to move through the
How To Measure Vital Signs How to Use This Tutorial This tutorial is intended for healthcare providers or students to teach basic vital signs skills Use the navigation buttons below to move through the
Atropine in Down's Syndrome
 Archives of Disease in Childhood, 1971, 46, 61. Response to Atropine in G. H. MIR and GORDON R. CUMMING From The Clinical Investigation Unit, Children's Hospital of Winnipeg, and The Department of Pediatrics,
Archives of Disease in Childhood, 1971, 46, 61. Response to Atropine in G. H. MIR and GORDON R. CUMMING From The Clinical Investigation Unit, Children's Hospital of Winnipeg, and The Department of Pediatrics,
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
RSPT Tracheal Aspiration. Tracheal Aspiration. RSPT 1410 Tracheal Aspiration
 1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
