Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, cont
|
|
|
- Pamela Eunice Evans
- 5 years ago
- Views:
Transcription
1 Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at ORIGINAL RESEARCH n GENITOURINARY IMAGING Thomas J. Kroencke, MD, MBA Christian Scheurig, MD Alexander Poellinger, MD Maike Gronewold, MD Bernd Hamm, MD Uterine Artery Embolization for Leiomyomas: Percentage of Infarction Predicts Clinical Outcome 1 Purpose: To determine the effect of partial versus complete leiomyoma infarction on relief of leiomyoma-related symptoms and freedom from invasive reinterventions and to assess if patient age, location of the dominant leiomyoma, number of leiomyomas, or baseline uterine and dominant leiomyoma volume were associated with clinical failure. 1 From the Department of Radiology, Charité Universitätsmedizin Berlin, Campus Virchow-Klinikum, Augustenburger Platz 1, Berlin, Germany. Received June 2, 2009; revision requested July 16; revision received August 10; accepted September 2; final version accepted November 23. Address correspondence to T.J.K. ( thomas. kroencke@charite.de ). Materials and Methods: Results: Conclusion: Study protocol was approved by the institutional review board, and informed consent was obtained. One hundred fifteen consecutive women (median age, 42 years; range, years) with symptomatic uterine leiomyomas underwent contrast material enhanced magnetic resonance (MR) imaging at baseline and hours after uterine artery embolization (UAE) to determine the percentage of infarction of leiomyoma tissue (complete = 100%, almost complete = 90% 99%, and partial = 0% 89%). Clinical outcome and frequency of reinterventions were compared for up to 36 months. One hundred thirteen patients completed at least one clinical follow-up. Twenty-four months after UAE, 50% (standard error) of the patients with partial infarction and 80% (standard error) of patients with almost complete infarction had undergone no reintervention. No patient with complete infarction needed a second treatment ( P,.001). The hazard ratios for reintervention between the complete infarction group and the almost complete and partial infarction groups were (95% confidence interval [CI]: 1.22, ; P =.034) and (95% CI: 8.33, ; P,.001), respectively. There were significant differences in hazard ratios between patients with partial and those with complete infarction for persistence or recurrence of menorrhagia (hazard ratio, 7.45; 95% CI: 2.08, 28.31; P =.002) and bulk-related symptoms (hazard ratio, 5.90; 95% CI: 1.66, 21.92; P =.007). There was no significant correlation between patient age, number of leiomyomas, location of the dominant leiomyoma, or baseline uterine and dominant leiomyoma volume and clinical failure. Women with leiomyoma infarction above 90% on contrastenhanced MR images after UAE show significantly better symptom control and fewer reinterventions than do patients with a lower infarction rate. q RSNA, 2010 q RSNA, radiology.rsna.org n Radiology: Volume 255: Number 3 June 2010
2 Uterine artery embolization (UAE) is an effective treatment alternative to surgery in patients with symptomatic leiomyoma. It has been shown that infarction of leiomyoma tissue occurs after UAE and precedes volume reduction ( 1 3 ). Early and late clinical failure has been linked to incomplete leiomyoma infarction ( 4 7 ). However, most of these studies were retrospective in design, with a limited number of cases or a preselected study population. The primary objective of our prospective study was to determine the effect of partial versus complete leiomyoma infarction on clinical outcome with respect to relief of leiomyoma-related symptoms and freedom from invasive reinterventions. The secondary objective was to assess whether patient age, location of the dominant leiomyoma, number of leiomyomas, or baseline uterine and dominant leiomyoma volumes are associated with clinical failure. Materials and Methods At the time of patient enrollment, T.J.K. was receiving consulting fees from Terumo Medical (Tokyo, Japan), which is a distributor of BeadBlock embolization particles (Biocompatibles, Farnham, England), and Biosphere Medical (Rockland, Mass), which is the Advances in Knowledge n Leiomyoma infarction above 90% on contrast-enhanced MR images after uterine artery embolization (UAE) is associated with greater likelihood of sustained control of menorrhagia and bulk-related symptoms. n Patients with incomplete infarc- tion of leiomyoma are at higher risk to undergo a second invasive therapy after UAE compared with those with complete leiomyoma infarction. n Patient age, baseline uterine and dominant leiomyoma volume, number of leiomyomas, and leiomyoma location were not associated with clinical failure. manufacturer of Embosphere embolization particles. Our study protocol was approved by the institutional review board, and informed consent was obtained. Between May 2003 and June 2004, 115 consecutive women (median age, 42 years; range, years) who were scheduled for UAE as an alternative to surgery for symptomatic uterine leiomyoma were included in our study. Patients complained of either bulk-related symptoms or heavy menstrual bleeding, had previously been evaluated by a referring gynecologist, and refused initially offered surgical treatment. Study population demographics are given in Table 1. All patients underwent unenhanced and contrast material enhanced MR imaging prior to and within hours after UAE to determine the percentage of infarction of all leiomyoma tissue (leiomyoma load) and the baseline volumes of the uterus and the dominant leiomyoma. Patients were followed up clinically for up to 36 months and with MR imaging for up to 12 months. Embolization Technique Bilateral embolization of the uterine arteries was performed by an interventional radiologist (T.J.K., with 9 years experience with UAE) by using a transfemoral approach. Direct superselective catheterization of both uterine arteries was performed by using road-map guidance with 4- and 5-F end-hole catheters or a coaxially advanced microcatheter, at the discretion of the operator. The use of microcatheters and occurrences of flow-limiting spasms were noted. Embolization was achieved by deploying Implications for Patient Care n Contrast-enhanced MR images may be used to identify patients that are at risk for clinical failure after UAE. n The technical goal of UAE should be complete devascularization of all leiomyoma by controlling factors that have an influence on infarction rate, such as collateral supply, choice of embolic agent, and embolization endpoint m m-diameter gelatin-coated trisacryl microspheres (Embosphere; Biosphere Medical), m m- diameter polyvinyl alcohol microspheres (Contour-SE; Boston Scientific, Natick, Mass), or m m-diameter acrylamido polyvinyl alcohol microspheres (BeadBlock; Biocompatibles). The total volume of particles was noted. The angiographic endpoint of embolization was the devascularization of the perifibroid plexus and sluggish antegrade flow in both uterine arteries. Clinical Questionnaire Leiomyoma-related symptoms were assessed before UAE by means of a self-administered nonvalidated clinical questionnaire that specifically asked about menorrhagia and bulk-related symptoms on a yes-or-no basis. There was no categorization of the subjective severity of these symptoms at baseline. At follow-up clinical visits, patients were asked to characterize the change in the severity of the same symptoms after UAE as worsened, unchanged, improved, or resolved. Any recurrence of previously controlled or improved symptoms was also noted. For all patients, leiomyoma-related reinterventions during follow-up (eg, hysteroscopic resection, myomectomy, hysterectomy, or repeat UAE) were noted. Patients were censored (ie, excluded from further consideration before final outcome of the patient sample had been assessed) at the time of symptomatic failure Published online before print /radiol Radiology 2010; 255: Abbreviations: CI = confi dence interval UAE = uterine artery embolization Author contributions: Guarantors of integrity of entire study, T.J.K., C.S., M.G.; study concepts/study design or data acquisition or data analysis/interpretation, all authors; manuscript drafting or manuscript revision for important intellectual content, all authors; approval of fi nal version of submitted manuscript, all authors; literature research, T.J.K., C.S., A.P., M.G.; clinical studies, T.J.K., C.S., M.G.; statistical analysis, T.J.K., C.S.; and manuscript editing, T.J.K., A.P., M.G., B.H. See Materials and Methods for pertinent disclosures. Radiology: Volume 255: Number 3 June 2010 n radiology.rsna.org 835
3 Table 1 Demographics in 115 Patients Characteristic (defined as worsened, unchanged, or recurrent symptoms), reintervention for uncontrolled symptoms, or the last available follow-up. MR Imaging Datum Age (y)* 42 (34 61) Symptom at presentation Menorrhagia 104 (90) Bulk-related 78 (68) Baseline volume Uterus (cm 3 ) 312 ( ) Dominant leiomyoma (cm 3 ) 84 (27 170) Number of leiomyomas One 30 (26) Two to fi ve 41 (36) More than fi ve 44 (38) Dominant leiomyoma location Subserosal 23 (20) Intramural 67 (58) Submucosal 25 (22) Note. Unless otherwise specifi ed, data are numbers of patients, with percentages in parentheses. * Data are medians, with range in parentheses. Data are medians, with interquartile range in parentheses. Dominant leiomyoma = largest leiomyoma at baseline magnetic resonance (MR) imaging. All patients underwent MR imaging with a 1.5-T imager (Magnetom Vision or Magnetom Symphony; Siemens Medical Systems, Erlangen, Germany) with a torso phased-array coil. After an initial localization acquisition, sagittal and transaxial T2-weighted fast spin-echo (repetition time msec/echo time msec, / ; field of view, mm; matrix, ; section thickness, 5 mm; acquisition time, minutes) images covering the uterus were obtained after intramuscular injection of 20 mg of butylscopolamine to reduce bowel motion artifacts. Additional transaxial, coronal, and sagittal breathhold T2-weighted half-fourier acquired single-shot fast spin-echo ( /63; flip angle, 150 ; field of view, mm; matrix, ; section thickness, 7 mm; acquisition time, 21 seconds) images were obtained. Axial and sagittal unenhanced and contrast material enhanced nondynamic fatsaturated T1-weighted two-dimensional gradient-echo ( /4.1; flip angle, 90 ; field of view, mm; matrix, ; section thickness, 5 mm; acquisition time, seconds) images that covered the whole uterus were used to determine the viability of the leiomyoma and surrounding myometrium. Gadolinium-based contrast material (Magnevist; Schering, Berlin, Germany) was given at a dose of 0.1 mmol per kilogram of body weight and a flow rate of 2 ml/sec with an automatic power injector (Spectris; Medrad, Pittsburgh, Pa). MR imaging was repeated hours after UAE and at subsequent follow-up visits by using the same protocol. All MR images were assessed by two readers (T.J.K. and C.S., with 10 and 5 years experience with pelvic MR imaging, respectively) by using a digital workstation that allowed for interactive analysis of images. The breath-hold T2- weighted images were used for analysis. In patients with small leiomyomas, we used the T2-weighted fast spin-echo images for intraindividual confirmation of the findings. The T2-weighted images served to determine the number of uterine leiomyomas per patient, which were categorized as singular, two to five, or more than five. All leiomyomas that were at least 10 mm in diameter were assessed. The location of the dominant (largest) leiomyoma within the uterine wall was classified as subserosal, intramural, or submucosal. For a subserosal leiomyoma, a substantial distortion of the outer contour (serosa) had to be present, and for a submucosal leiomyoma, a substantial distortion of the endometrial stripe (mucosa) had to be present. The volume of the uterus and the dominant leiomyoma was measured at baseline and at a median follow-up of 7 months (range, 3 12 months) by using the formula for a prolate ellipsoid (length 3 width 3 height ). Infarction of a leiomyoma was defined as absence of contrast enhancement on follow-up T1-weighted MR images compared with baseline images. Unenhanced T1-weighted images served as controls for differentiating residual enhancement from hemorrhagic infarction after UAE. Percent infarction of leiomyoma load and dominant leiomyoma were rated in a blinded fashion by the two readers by using a scale from 0% to 100% infarction, with 10% increments. In case of a difference between readers, the mean of both scorings was calculated. For the dominant leiomyoma, an intraindividual comparison of the scoring for the percentage of infarction hours after UAE and that at the last follow-up examination was made by using contrast-enhanced MR images. Data Analysis On the basis of the percentage of infarction of leiomyoma load determined hours after UAE by using contrastenhanced MR images, patients were divided into three groups: complete infarction (100% infarction of all leiomyomas), almost complete infarction (90% 99% infarction of all leiomyomas), and partial infarction (, 90% infarction of all leiomyomas). Baseline clinical and imaging characteristics between groups were tested for significant differences. Differences in intraindividual scoring of the infarcted dominant leiomyoma hours after UAE and at the latest follow-up were examined by using the Mann-Whitney test. The baseline and follow-up volumes of the uterus and dominant leiomyoma were compared between groups by using the Mann-Whitney test. The Wilcoxon test for paired samples was applied to test changes in volume after UAE for significance. Clinical efficacy of UAE treatment was determined by comparison of questionnaire data at baseline with that at follow-up. Clinical success was defined as improved or resolved symptoms in the absence of reintervention or recurrence of symptoms during follow-up. Reintervention for fibroid sloughing or expulsion was not defined as clinical failure. Kaplan-Meier analysis was performed to determine freedom from 836 radiology.rsna.org n Radiology: Volume 255: Number 3 June 2010
4 reintervention and occurrence of a negative clinical event (ie, unchanged, worsening, or recurrent menorrhagia or bulk-related symptoms) for each group. Differences among groups were tested for significance by using the associated log-rank test. Cox proportional hazards regression was used to identify correlations between age, baseline imaging variables, percentage of infarction, and clinical failure. Because of large point estimates for the covariate devascularization, the Firth correction was used. When appropriate, the mean and standard deviation or median and 95% confidence interval (CI) were given. The Cohen k was used to determine the interobserver reliability regarding assessment of percentage of infarction of leiomyoma load. A probability value of less than 5% ( P,.05) was considered to indicate a significant difference. Statistical analysis was performed by using software (SPSS, version ; SPSS, Chicago, Ill). Results Technical Results Of the 115 patients, 112 (97%) underwent bilateral embolization. In three patients, a unilateral embolization was performed owing to an absent uterine artery, occlusion of a uterine artery owing to a surgical clip placed at preceding sterilization, or inability to catheterize the uterine artery on one side. Two of these patients showed partial leiomyoma infarction, and one had complete infarction of a single leiomyoma on subsequent contrast-enhanced MR images. UAE was performed without the use of a microcatheter in 64 (56%) patients, and a microcatheter was used bilaterally in 31 (27%) patients and unilaterally in 20 (17%) patients. There was no significant correlation between the use of a microcatheter and the percentage of infarction after UAE. Spasm was noted by the operator in 17 (15%) of 113 patients, while in two patients no information was recorded. In all but two of these patients a vasodilator (Trinitrosan; Merck, Darmstadt, Germany) was given intraarterially in aliquots of 100 m g to relieve spasm. No correlation was seen between spasm and the percentage of infarction after UAE. The amount of particles injected was recorded for 111 (97%) of 115 patients. The overall mean amount of particles injected was 4 ml (standard deviation) (range, 1 20 ml). In 90 (81%) of 111 patients, gelatin-coated trisacryl microspheres (Embosphere) were used as the embolic agent (mean, 4 ml [standard deviation]; range, 1 20 ml). In 18 (16%) of 111 patients, acrylamido polyvinyl alcohol microspheres (Bead- Block) were used as the embolic agent (mean, 6 ml [standard deviation]; range, 2 18 ml). In three (3%) of 111 patients, polyvinyl alcohol spheres (Contour-SE) were used as the embolic agent (mean, 1.3 ml; range, ml). An uneven distribution of particle type was seen between groups; however, no significant correlation with imaging or clinical outcome was found, although this comparison was limited by small sample size. Imaging Results Of the 115 patients treated, 60 (52%) were categorized as having complete infarction of all leiomyoma tissue; 32 (28%), as having almost complete infarction; and 23 (20%), as having partial infarction ( Fig 1 ) on contrast-enhanced MR images obtained hours after UAE. Interobserver reliability was high between the two observers (Cohen k = 0.978; P,.001). Intergroup differences in age, baseline uterine and dominant leiomyoma volume, and the number and location of leiomyomas were not significant ( P = ). MR imaging follow-up at a median of 7 months after UAE was available in 94 patients. The analysis of the volume changes after UAE on the basis of MR imaging showed significant reduction for both uterine and dominant leiomyoma volume for all three groups, with the least decrease seen in the partial infarction group ( Table 2 ). An increase of the percentage of viable (noninfarcted) tissue of the dominant leiomyoma between hours after and the last follow-up was observed in the almost complete and partial infarction groups ( P =.021). Clinical Results No patient with complete infarction of the leiomyoma load underwent reintervention in up to 36 months after UAE. As early as 24 months after UAE, significant differences between groups were observed. At this timepoint, 80% (standard error) of patients in the almost complete infarction group remained free of a re intervention, while only 50% (standard error) in the partial infarction group did not undergo a second invasive intervention to treat leiomyoma-associated symptoms ( Fig 2 ). Analysis of the clinical outcome revealed marked differences between groups regarding menorrhagia ( Fig 3 ). In the complete infarction group, 90% (standard error) of patients remained free from menorrhagia at 24 months, compared with 84% (standard error) in the almost complete infarction group and 72% (standard error) in the partial infarction group. Symptomatic failures became evident within 12 months after UAE. These differences remained stable during follow-up after UAE. Regarding bulk-related symptoms, no differences were seen between complete and almost complete infarction groups, with a near 10% failure rate in both groups during follow-up. However, up to 65% (standard error) of women in the partial infarction group had unchanged, worsened, or recurrent bulk-related symptoms, with most events reported within 6 months after UAE ( Fig 4 ). There was no significant correlation between variables such as patient age, baseline uterine and dominant leiomyoma volume, number of leiomyomas, or location of the dominant leiomyoma and clinical failure ( Table 3 ). Hazard ratio calculation showed a 16-fold higher risk for reintervention in patients with almost complete infarction ( P =.034) and a 73-fold higher risk for reintervention in patients with partial infarction ( P,.001) (Table 3). Patients with partial infarction also had a sevenfold higher risk for worsened, unchanged, or recurrent menorrhagia ( P =.002) and a sixfold higher risk for worsened, Radiology: Volume 255: Number 3 June 2010 n radiology.rsna.org 837
5 Figure 1 Figure 2 Figure 1: Bar graph of number of patients (N) and percentage of leiomyoma infarction (Devascularization) on contrast-enhanced MR images obtained hours after UAE. Figure 2: Graph of percentage of patients who remained free from reintervention over time in months (m) in complete, almost complete, and partial infarction groups. Patients were excluded from further consideration (censored) before fi nal outcome was assessed at time of either reintervention for uncontrolled symptoms or last available follow-up. unchanged, or recurrent bulk-related symptoms ( P =.007) during follow-up. Discussion UAE is a minimally invasive uterussparing treatment alternative to surgery that provides effective and sustained control of leiomyoma-related symptoms. While symptomatic improvement has been reported uniformly in the literature, conflicting results regarding the effect of baseline imaging variables (eg, number, location, leiomyoma and uterine volume, and percentage volume reduction after UAE) on clinical outcome have been reported ( 8 11 ). Technically, successful UAE leads to infarction of targeted leiomyomas, with subsequent volume reduction of the infarcted leiomyoma tissue ( 1,2 ). Infarction of leiomyoma occurs after UAE independent of size, location, or leiomyoma burden. Incomplete leiomyoma infarction has been reported to be a result of ovarian artery collateral supply, spasm, unilateral embolization, or the use of some embolic agents ( ). Pelage et al ( 4 ) reported that incomplete infarction of leiomyomas may lead to clinical failure owing to regrowth of viable tissue. Table 2 Changes in Uterine and Dominant Leiomyoma Volumes Median Volume (cm 3 )* Percentage Volume Decrease Infarction Group Baseline After UAE Median P Value Uterus Complete 258 ( ) 163 ( ) 36 (27, 43),.001 Almost complete 313 ( ) 196 ( ) 34 (29, 44),.001 Partial 283 ( ) 182 ( ) 14 (2, 34).005 Dominant Leiomyoma Complete 68 (26 129) 26 (6 55) 55 (48, 68),.001 Almost complete 58 (27 187) 29 (9 94) 59 (46, 73),.001 Partial 95 (14 137) 45 (11 68) 53 (13, 66).002 Note. After UAE = latest follow-up (median, 7 months; range, 3 12 months). * Data in parentheses are interquartile ranges. Data in parentheses are 95% CIs. Wilcoxon test for paired samples. P values for comparison of decrease in uterine volume determined with Mann-Whitney test between complete and almost complete infarction groups (.936), between complete and partial infarction groups (.022), and between almost complete and partial infarction groups (.016). P values for comparison of decrease in dominant leiomyoma volume determined with Mann-Whitney test between complete and almost complete infarction groups (.602), between complete and partial infarction groups (.306), and between almost complete and partial infarction groups (.308). However, the rates of reintervention and of failure to control symptoms in relation to baseline infarction rate have not, to our knowledge, been studied prospectively. Our findings show a strong correlation between percentage of infarction of leiomyoma tissue and clinical outcome. This holds true not only for the risk of a particular patient to undergo a second invasive therapy after UAE, but also for the chance of a clinical outcome of no improvement, 838 radiology.rsna.org n Radiology: Volume 255: Number 3 June 2010
6 Figure 3 Figure 4 Figure 3: Graph of percentage of patients who remained free of menorrhagia over time in months (m) in complete, almost complete, and partial infarction groups. Patients were excluded from further consideration (censored) before fi nal outcome was assessed at time of either symptomatic failure or last available follow-up. Figure 4: Graph of percentage of patients who remained free of bulk-related symptoms over time in months (m) in complete, almost complete, and partial infarction groups. Patients were excluded from further consideration (censored) before fi nal outcome was assessed at time of either symptomatic failure or last available follow-up. worsening, or recurrence of either menorrhagia or bulk-related symptoms. Patients in the complete infarction group did not undergo a second intervention, and control of bulk-related and bleeding symptoms was in the range of 85% 90% in these patients during 36-month follow-up. In contrast, no correlation between patient age, uterine volume, dominant leiomyoma volume, number of leiomyomas, or location of leiomyomas and clinical failure was found. Our work is in line with observations reported in other studies of nonsurgical therapeutic interventions with contrast-enhanced MR imaging correlation. Fennessy et al ( 15 ) noted improved symptomatic outcome in patients with a larger volume of nonperfused (ablated) leiomyoma tissue compared with a group with restricted ablation. Katsumori et al ( 7 ) reported findings similar to our results in a retrospective long-term analysis of gelfoam as the embolic agent for UAE. Significantly better symptom control and fewer reinterventions were reported for patients with evidence of complete devascularization of leiomyoma 1 week after UAE. In contrast to our study, a significant difference was also found between patients with 100% infarction versus those with 90% 99% infarction with respect to clinical outcome. This may be explained by the shorter follow-up in our study. Noninfarcted leiomyomas regrow over time, resulting in symptomatic recurrence and presumably leading to a pronounced difference in clinical outcome during long-term follow-up. Our study had limitations. There were large differences in the numbers of individuals in the different infarction groups. This led to wide CIs for the estimates, especially when looking at the Cox proportional hazards regression. The infarction covariate, in contrast to the other variables tested, showed large hazard ratios regarding the possibility of a reintervention. The distribution is highly skewed, with no event in the complete infarction group but seven in the partial infarction group resulting in wide CIs. Degree of infarction clearly separated itself from the other covariates and proved to be highly predictive for a possible reintervention. Therefore and because of the small sample size in the almost complete and partial infarction groups, the Firth correction for the regression analysis was used to estimate more precisely. We still faced high upper bounds of the CIs, so the point estimates of the hazard ratios are not as precise as we wished. However, the rate of infarction was highly predictive for the outcome. Even the lower bound predicted an eightfold higher risk for facing the necessity of reintervention for patients with partial infarction versus those with complete infarction. Using a larger number of patients could possibly narrow down the CIs and the hazard ratios. The number of patients treated with BeadBlock or Contour-SE particles was small, and it is possible that differences were in fact present in the infarction rates with each embolic agent, but that these differences were not detected owing to the small sample size (type II error). Also, the estimation of the extent of leiomyoma infarction on contrastenhanced MR images was performed subjectively. Although interobserver reliability was high in our study, consensus reading presents a biased (weighted) average of expert readers ( 16 ). In addition, the division of patients into three groups is a feasible but questionable approach. Variance in infarction rate was considerably higher in the partial infarction group compared with the complete and almost complete infarction groups. This artificially amplified differences between the groups. Radiology: Volume 255: Number 3 June 2010 n radiology.rsna.org 839
7 Table 3 Hazard Ratios for Reintervention, Menorrhagia, and Bulk-related Symptoms Variable Hazard Ratio * P Value Reintervention Infarction group Almost complete vs complete (1.22, ).034 Partial vs complete (8.33, ),.001 Age 0.89 (0.70, 1.06).214 Uterine volume 1.03 (0.98, 1.08).270 Dominant leiomyoma volume 0.98 (0.90, 1.06).540 No. of leiomyomas Singular vs two to fi ve 0.96 (0.12, 11.53).971 Singular vs more than fi ve 0.73 (0.12, 6.03).748 Dominant leiomyoma location Subserosal vs intramural 2.74 (0.51, 28.58).259 Subserosal vs submucosal 1.01 (0.08, 14.17).996 Menorrhagia Infarction group Almost complete vs complete 1.90 (0.42, 7.64).383 Partial vs complete 7.45 (2.08, 28.31).002 Age 0.94 (0.82, 1.05).261 Uterine volume 1.02 (0.99, 1.06).208 Dominant leiomyoma volume 0.95 (0.89, 1.02).152 No. of leiomyomas Singular vs two to fi ve 0.53 (0.13, 2.10).357 Singular vs more than fi ve 0.26 (0.05, 1.16).078 Dominant leiomyoma location Subserosal vs intramural 1.46 (0.36, 8.25).614 Subserosal vs submucosal 1.50 (0.27, 9.55).636 Bulk-related Symptoms Infarction group Almost complete vs complete 0.99 (0.173, 4.126).991 Partial vs complete 5.90 (1.66, 21.92).007 Age 1.07 (0.98, 1.17).124 Uterine volume 1.00 (0.97, 1.04).867 Dominant leiomyoma volume 0.96 (0.89, 1.03).272 No. of leiomyomas Singular vs two to fi ve 0.42 (0.10, 1.60).199 Singular vs more than fi ve 0.31 (0.08, 1.17).082 Dominant leiomyoma location Subserosal vs intramural 1.47 (0.49, 5.24).505 Subserosal vs submucosal 0.13 (0.00, 1.28).086 * Data in parentheses are 95% CIs. In 10-mL increments. ranted. Contrast-enhanced MR imaging is helpful for determining the efficacy of these techniques with respect to the uniform technical goal of these treatments, which is induction of cell death in viable leiomyoma tissue by means of thermal destruction or ischemia. The development of standardized measures of outcome will be of great benefit to future comparative studies. In summary, we conclude that infarction of leiomyoma tissue is the most important imaging parameter for clinical success after UAE and that differences in imaging outcome in the short run can be used to predict clinical improvement and chance of recurrence in the longer term. References 1. McCluggage WG, Ellis PK, McClure N, Walker WJ, Jackson PA, Manek S. Pathologic features of uterine leiomyomas following uterine artery embolization. Int J Gynecol Pathol 2000 ; 19 ( 4 ): Katsumori T, Nakajima K, Tokuhiro M. Gadolinium-enhanced MR imaging in the evaluation of uterine fibroids treated with uterine artery embolization. AJR Am J Roentgenol 2001 ; 177 ( 2 ): Banovac F, Ascher SM, Jones DA, Black MD, Smith JC, Spies JB. Magnetic resonance imaging outcome after uterine artery embolization for leiomyomata with use of tris-acryl gelatin microspheres. J Vasc Interv Radiol 2002 ; 13 ( 7 ): Pelage JP, Guaou NG, Jha RC, Ascher SM, Spies JB. Uterine fibroid tumors: long-term MR imaging outcome after embolization. Radiology 2004 ; 230 ( 3 ): Yousefi S, Czeyda-Pommersheim F, White AM, Banovac F, Hahn WY, Spies JB. Repeat uterine artery embolization: indications and technical findings. J Vasc Interv Radiol 2006 ; 17 ( 12 ): However, a significantly lower reintervention rate and a uniform trend toward better outcomes were evident even between women with complete devascularization and those with 90% 99% infarction of leiomyoma load. Finally, the clinical endpoints of our study were determined by using a nonstandardized questionnaire, and this limits their interpretability to some extent. To compare results of different nonsurgical techniques (eg, UAE, MRguided high-intensity focused ultrasound, or uterine artery ligation), use of a systematic anatomic classification system of leiomyoma burden and a standardized validated clinical outcome measure (such as the uterine fibroid symptom severity and quality-of-life questionnaire, or UFSQOL) are war- 6. Siskin GP, Beck A, Schuster M, Mandato K, Englander M, Herr A. Leiomyoma infarction after uterine artery embolization: a prospective randomized study comparing tris-acryl gelatin microspheres versus polyvinyl alcohol microspheres. J Vasc Interv Radiol 2008 ; 19 ( 1 ): Katsumori T, Kasahara T, Kin Y, Nozaki T. Infarction of uterine fibroids after embolization: relationship between postprocedural enhanced MRI findings and long-term clinical outcomes. Cardiovasc Intervent Radiol 2008 ; 31 ( 1 ): radiology.rsna.org n Radiology: Volume 255: Number 3 June 2010
8 8. Spies JB, Myers ER, Worthington-Kirsch R, et al. The FIBROID Registry: symptom and quality-of-life status 1 year after therapy. Obstet Gynecol 2005 ; 106 ( 6 ): Spies JB, Roth AR, Jha RC, et al. Leiomyomata treated with uterine artery embolization: factors associated with successful symptom and imaging outcome. Radiology 2002 ; 222 ( 1 ): desouza NM, Williams AD. Uterine arterial embolization for leiomyomas: perfusion and volume changes at MR imaging and relation to clinical outcome. Radiology 2002 ; 222 ( 2 ): Toor SS, Tan KT, Simons ME, et al. Clinical failure after uterine artery embolization: evaluation of patient and MR imaging characteristics. J Vasc Interv Radiol 2008 ; 19 ( 5 ): Matson M, Nicholson A, Belli AM. Anastomoses of the ovarian and uterine arteries: a potential pitfall and cause of failure of uterine embolization. Cardiovasc Intervent Radiol 2000 ; 23 ( 5 ): Volkers NA, Hehenkamp WJ, Birnie E, et al. Uterine artery embolization in the treatment of symptomatic uterine fibroid tumors (EMMY trial): periprocedural results and complications. J Vasc Interv Radiol 2006 ; 17 ( 3 ): Abramowitz SD, Israel GM, McCarthy SM, Pollak JS, White RI Jr, Tal MG. Comparison of four embolic materials at uterine artery embolization by using postprocedural MR imaging enhancement. Radiology 2009 ; 250 ( 2 ): Fennessy FM, Tempany CM, McDannold NJ, et al. Uterine leiomyomas: MR imagingguided focused ultrasound surgery results of different treatment protocols. Radiology 2007 ; 243 ( 3 ): Obuchowski NA, Zepp RC. Simple steps for improving multiple-reader studies in radiology. AJR Am J Roentgenol 1996 ; 166 ( 3 ): Radiology: Volume 255: Number 3 June 2010 n radiology.rsna.org 841
Practical Application of a Coronal MR Image during a Uterine Fibroid Embolization (UFE) 1
 Practical Application of a Coronal MR Image during a Uterine Fibroid Embolization (UFE) 1 Jin Young Jung, M.D., Man Deuk Kim, M.D., Hyun Seok Lee, M.D., Mee Hwa Lee, M.D. 2, Hee Jin Kim, M.D., Jin Ho Cho,
Practical Application of a Coronal MR Image during a Uterine Fibroid Embolization (UFE) 1 Jin Young Jung, M.D., Man Deuk Kim, M.D., Hyun Seok Lee, M.D., Mee Hwa Lee, M.D. 2, Hee Jin Kim, M.D., Jin Ho Cho,
Submucosal Fibroids Becoming Endocavitary Following Uterine Artery Embolization: Risk Assessment by MRI
 Women s Imaging Original Research Verma et al. MRI of Submucosal Fibroids Women s Imaging Original Research WOMEN S IMAGING Sachit K. Verma 1 Diane Bergin 1,2 Carin F. Gonsalves 1 Donald G. Mitchell 1
Women s Imaging Original Research Verma et al. MRI of Submucosal Fibroids Women s Imaging Original Research WOMEN S IMAGING Sachit K. Verma 1 Diane Bergin 1,2 Carin F. Gonsalves 1 Donald G. Mitchell 1
Clinical Efficacy and Complications of Uterine Artery Embolization in Symptomatic Uterine Fibroids
 Global Journal of Health Science; Vol. 8, No. 7; 2016 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Clinical Efficacy and Complications of Uterine Artery Embolization
Global Journal of Health Science; Vol. 8, No. 7; 2016 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Clinical Efficacy and Complications of Uterine Artery Embolization
Choosing The Right Size Particle. Gary Siskin, MD FSIR Professor and Chairman Department of Radiology Albany Medical Center Albany, New York
 Choosing The Right Size Particle Gary Siskin, MD FSIR Professor and Chairman Department of Radiology Albany Medical Center Albany, New York Gary Siskin, M.D. Consultant/Advisory Board: Boston Scientific,
Choosing The Right Size Particle Gary Siskin, MD FSIR Professor and Chairman Department of Radiology Albany Medical Center Albany, New York Gary Siskin, M.D. Consultant/Advisory Board: Boston Scientific,
Peritoneal Enclosure of Embolization Particles Mimicking Peritoneal Carcinomatosis
 CASE REPORT Peritoneal Enclosure of Embolization Particles Mimicking Peritoneal Carcinomatosis Giovanni Favero, MD, Christhardt Köhler, MD, Anna Jacob, MD, Tatiana Pfiffer, MD, Andrea Mölgg, MD Department
CASE REPORT Peritoneal Enclosure of Embolization Particles Mimicking Peritoneal Carcinomatosis Giovanni Favero, MD, Christhardt Köhler, MD, Anna Jacob, MD, Tatiana Pfiffer, MD, Andrea Mölgg, MD Department
Targeted Vessel Ablation for More Efficient Magnetic Resonance-Guided High-Intensity Focused Ultrasound Ablation of Uterine Fibroids
 Cardiovasc Intervent Radiol (2012) 35:1205 1210 DOI 10.1007/s00270-011-0313-9 TECHNICAL NOTE Targeted Vessel Ablation for More Efficient Magnetic Resonance-Guided High-Intensity Focused Ultrasound Ablation
Cardiovasc Intervent Radiol (2012) 35:1205 1210 DOI 10.1007/s00270-011-0313-9 TECHNICAL NOTE Targeted Vessel Ablation for More Efficient Magnetic Resonance-Guided High-Intensity Focused Ultrasound Ablation
MRI-Guided Focused Ultrasound (MRgFUS) for thetreatment of Uterine Fibroids and Other Tumors. Original Policy Date
 MP 7.01.89 MRI-Guided Focused Ultrasound (MRgFUS) for thetreatment of Uterine Fibroids and Other Tumors Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date
MP 7.01.89 MRI-Guided Focused Ultrasound (MRgFUS) for thetreatment of Uterine Fibroids and Other Tumors Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date
An MRI pictorial review of uterine fibroid expulsion after uterine artery embolisation
 An MRI pictorial review of uterine fibroid expulsion after uterine artery embolisation Poster No.: C-1893 Congress: ECR 2017 Type: Educational Exhibit Authors: E. Y. Auyoung, L. Ratnam, R. Das, S. Ameli-Renani,
An MRI pictorial review of uterine fibroid expulsion after uterine artery embolisation Poster No.: C-1893 Congress: ECR 2017 Type: Educational Exhibit Authors: E. Y. Auyoung, L. Ratnam, R. Das, S. Ameli-Renani,
Poster No.: C-0181 Congress: ECR Scientific Exhibit. Authors:
 Magnetic resonance imaging-guided focused ultrasound surgery for symptomatic uterine fibroids: Estimation of treatment efficacy using thermal dose calculations Poster No.: C-0181 Congress: ECR 2013 Type:
Magnetic resonance imaging-guided focused ultrasound surgery for symptomatic uterine fibroids: Estimation of treatment efficacy using thermal dose calculations Poster No.: C-0181 Congress: ECR 2013 Type:
Sang-Wook Yoon, 1 Chan Lee, 2 Kyoung Ah Kim, 1 and Sang Heum Kim Introduction
 Obstetrics and Gynecology International Volume 2010, Article ID 834275, 4 pages doi:10.1155/2010/834275 Case Report Contrast-Enhanced Dynamic MR Imaging of Uterine Fibroids as a Potential Predictor of
Obstetrics and Gynecology International Volume 2010, Article ID 834275, 4 pages doi:10.1155/2010/834275 Case Report Contrast-Enhanced Dynamic MR Imaging of Uterine Fibroids as a Potential Predictor of
Outcome of uterine embolization and hysterectomy for leiomyomas: Results of a multicenter study
 American Journal of Obstetrics and Gynecology (2004) 191, 22e31 www.elsevier.com/locate/ajog Outcome of uterine embolization and hysterectomy for leiomyomas: Results of a multicenter study James B. Spies,
American Journal of Obstetrics and Gynecology (2004) 191, 22e31 www.elsevier.com/locate/ajog Outcome of uterine embolization and hysterectomy for leiomyomas: Results of a multicenter study James B. Spies,
Keywords: Uterine artery embolization; Uterine leiomyomas; Contrast-enhanced. Introduction
 Elmer ress Original Article J Clin Gynecol Obstet. 2015;4(1):164-169 Normalized Relative Contrast Improves the Power of Pre- Therapy Contrast-Enhanced MRI to Predict the Prognosis of Uterine Leiomyoma
Elmer ress Original Article J Clin Gynecol Obstet. 2015;4(1):164-169 Normalized Relative Contrast Improves the Power of Pre- Therapy Contrast-Enhanced MRI to Predict the Prognosis of Uterine Leiomyoma
UAE for the treatment of symptomatic adenomyosis
 UAE for the treatment of symptomatic adenomyosis Poster No.: C-2074 Congress: ECR 2010 Type: Topic: Scientific Exhibit Interventional Radiology Authors: V. D. Souftas, P. Tsikouras, M. Mantatzis, E. Astrinakis,
UAE for the treatment of symptomatic adenomyosis Poster No.: C-2074 Congress: ECR 2010 Type: Topic: Scientific Exhibit Interventional Radiology Authors: V. D. Souftas, P. Tsikouras, M. Mantatzis, E. Astrinakis,
Magnetic Resonance-Guided High-Intensity Focused Ultrasound (MR-HIFU) in Treatment of Symptomatic Uterine Myomas
 Signature: Pol J Radiol, 2014; 79: 439-443 DOI: 10.12659/PJR.890606 REVIEW ARTICLE Received: 2014.02.28 Accepted: 2014.04.14 Published: 2014.11.27 Authors Contribution: A Study Design B Data Collection
Signature: Pol J Radiol, 2014; 79: 439-443 DOI: 10.12659/PJR.890606 REVIEW ARTICLE Received: 2014.02.28 Accepted: 2014.04.14 Published: 2014.11.27 Authors Contribution: A Study Design B Data Collection
Uterine artery embolisation for treating adenomyosis
 Uterine artery embolisation for treating Issued: December 2013 guidance.nice.org.uk/ipg NICE has accredited the process used by the NICE Interventional Procedures Programme to produce interventional procedures
Uterine artery embolisation for treating Issued: December 2013 guidance.nice.org.uk/ipg NICE has accredited the process used by the NICE Interventional Procedures Programme to produce interventional procedures
Not all roads point to hysterectomy: treatment options for fibroids
 Not all roads point to hysterectomy: treatment options for fibroids MAUREEN KOHI, MD DEPARTMENT OF RADIOLOGY JEANNETTE LAGER, MD DEPARTMENT OF OBSTETRICS, GYNECOLOGY AND REPRODUCTIVE SCIENCES A lady, recently
Not all roads point to hysterectomy: treatment options for fibroids MAUREEN KOHI, MD DEPARTMENT OF RADIOLOGY JEANNETTE LAGER, MD DEPARTMENT OF OBSTETRICS, GYNECOLOGY AND REPRODUCTIVE SCIENCES A lady, recently
Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the Uterus with Fibroids
 Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the
Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the
Fibroids. Very Common! Benign smooth muscle tumors of the myometrium 20-80% of women develop fibroids by age 50* 151 million women affected**
 Fibroids Very Common! Benign smooth muscle tumors of the myometrium 20-80% of women develop fibroids by age 50* 151 million women affected** * Uterine Fibroids Fact Sheet Office on Women s Health 2015
Fibroids Very Common! Benign smooth muscle tumors of the myometrium 20-80% of women develop fibroids by age 50* 151 million women affected** * Uterine Fibroids Fact Sheet Office on Women s Health 2015
Magnetic Resonance-guided Focused Ultrasound Surgery
 CLINICAL OBSTETRICS AND GYNECOLOGY Volume 51, Number 1, 159 166 r 2008, Lippincott Williams & Wilkins Magnetic Resonance-guided Focused Ultrasound Surgery SUSAN B. A. HUDSON, MD and ELIZABETH A. STEWART,
CLINICAL OBSTETRICS AND GYNECOLOGY Volume 51, Number 1, 159 166 r 2008, Lippincott Williams & Wilkins Magnetic Resonance-guided Focused Ultrasound Surgery SUSAN B. A. HUDSON, MD and ELIZABETH A. STEWART,
Uterine Artery Embolization for the Treatment of Adenomyosis: Clinical Response and Evaluation with MR Imaging
 Gary P. Siskin 1 Mitchell E. Tublin Brian F. Stainken Kyran Dowling Eric G. Dolen Received October 2, 2000; accepted after revision February 2, 2001. 1 All authors: Department of Radiology, A-113, Albany
Gary P. Siskin 1 Mitchell E. Tublin Brian F. Stainken Kyran Dowling Eric G. Dolen Received October 2, 2000; accepted after revision February 2, 2001. 1 All authors: Department of Radiology, A-113, Albany
Volumetric feedback ablation of uterine fibroids using magnetic resonance-guided high intensity focused ultrasound therapy
 Eur Radiol (2012) 22:411 417 DOI 10.1007/s00330-011-2262-8 INTERVENTIONAL Volumetric feedback ablation of uterine fibroids using magnetic resonance-guided high intensity focused ultrasound therapy M. J.
Eur Radiol (2012) 22:411 417 DOI 10.1007/s00330-011-2262-8 INTERVENTIONAL Volumetric feedback ablation of uterine fibroids using magnetic resonance-guided high intensity focused ultrasound therapy M. J.
CT and MRI features following Uterine Fibroid Embolization
 Thomas Jefferson University Jefferson Digital Commons Department of Radiology Faculty Papers Department of Radiology Winter 2-2010 CT and MRI features following Uterine Fibroid Embolization Sachit Verma
Thomas Jefferson University Jefferson Digital Commons Department of Radiology Faculty Papers Department of Radiology Winter 2-2010 CT and MRI features following Uterine Fibroid Embolization Sachit Verma
Management of Uterine Myomas
 Management of Uterine Myomas Deidre D. Gunn, MD Assistant Professor Division of Reproductive Endocrinology & Infertility February 16, 2018 Disclosures I have no relevant financial relationships to disclose.
Management of Uterine Myomas Deidre D. Gunn, MD Assistant Professor Division of Reproductive Endocrinology & Infertility February 16, 2018 Disclosures I have no relevant financial relationships to disclose.
Effect of intravenous contrast medium administration on prostate diffusion-weighted imaging
 Effect of intravenous contrast medium administration on prostate diffusion-weighted imaging Poster No.: C-1766 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit J. Bae, C. K. Kim, S.
Effect of intravenous contrast medium administration on prostate diffusion-weighted imaging Poster No.: C-1766 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit J. Bae, C. K. Kim, S.
Hiroshi ARIMOTO 1, Kazuhiro YAMAMOTO 1, Hiroyuki YAMAGUCHI 2, Yoshito TERAI 2, Masahide OHMICHI 2 and Isamu NARABAYASHI 1
 Uterine Artery Embolization for Leiomyomas: Examination of Correlation Between Degree of Leiomyoma Perfusion Determined by Enhanced MR i-drive Method and Leiomyoma Volume Change on MR
Uterine Artery Embolization for Leiomyomas: Examination of Correlation Between Degree of Leiomyoma Perfusion Determined by Enhanced MR i-drive Method and Leiomyoma Volume Change on MR
Randomised trial of two embolic agents for uterine artery embolisation for fibroids: Gelfoam versus Embospheres (RAGE trial)
 Yadavali et al. CVIR Endovascular (2019) 2:4 https://doi.org/10.1186/s42155-018-0044-y CVIR Endovascular ORIGINAL ARTICLE Open Access Randomised trial of two embolic agents for uterine artery embolisation
Yadavali et al. CVIR Endovascular (2019) 2:4 https://doi.org/10.1186/s42155-018-0044-y CVIR Endovascular ORIGINAL ARTICLE Open Access Randomised trial of two embolic agents for uterine artery embolisation
The follow-up of uterine fibroids treated with HIFU: role of DWI and Dynamic contrast-study MRI
 The follow-up of uterine fibroids treated with HIFU: role of DWI and Dynamic contrast-study MRI Poster No.: C-1137 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit V. Zampa, V. Vallini,
The follow-up of uterine fibroids treated with HIFU: role of DWI and Dynamic contrast-study MRI Poster No.: C-1137 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit V. Zampa, V. Vallini,
Uterine Artery Embolization for Symptomatic Fibroids with High Signal Intensity on T2-Weighted MR Imaging
 Original Article http://dx.doi.org/10.3348/kjr.2012.13.5.618 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(5):618-624 Uterine Artery Embolization for Symptomatic Fibroids with High Signal Intensity
Original Article http://dx.doi.org/10.3348/kjr.2012.13.5.618 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(5):618-624 Uterine Artery Embolization for Symptomatic Fibroids with High Signal Intensity
Noninvasive thermal ablation of uterine leiomyomas is possible with extracorporeal magnetic resonance (MR) imaging guided focused ultrasound surgery.
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Fiona M. Fennessy,
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Fiona M. Fennessy,
Diffusion-weighted MR imaging for Diagnosis of Uterine Leiomyomas
 Diffusion-weighted MR imaging for Diagnosis of Uterine Leiomyomas Poster No.: C-0111 Congress: ECR 2015 Type: Scientific Exhibit Authors: A. Er 1, G. Pekindil 2, M. Gök 3, A. R. Kandiloglu 2, A. G. Tamay
Diffusion-weighted MR imaging for Diagnosis of Uterine Leiomyomas Poster No.: C-0111 Congress: ECR 2015 Type: Scientific Exhibit Authors: A. Er 1, G. Pekindil 2, M. Gök 3, A. R. Kandiloglu 2, A. G. Tamay
Uterine-Sparing Treatment Options for Symptomatic Uterine Fibroids
 Uterine-Sparing Treatment Options for Symptomatic Uterine Fibroids Developed in collaboration Learning Objective Upon completion, participants should be able to: Review uterine-sparing fibroid therapies
Uterine-Sparing Treatment Options for Symptomatic Uterine Fibroids Developed in collaboration Learning Objective Upon completion, participants should be able to: Review uterine-sparing fibroid therapies
This copy is for personal use only. To order printed copies, contact Purpose: Materials and Methods: Results: Conclusion:
 This copy is for personal use only. To order printed copies, contact reprints@rsna.org Original Research n Pediatric Imaging Pediatric Brain: Repeated Exposure to Linear Gadolinium-based Contrast Material
This copy is for personal use only. To order printed copies, contact reprints@rsna.org Original Research n Pediatric Imaging Pediatric Brain: Repeated Exposure to Linear Gadolinium-based Contrast Material
Medical Management of Fibroids Esmya. Dr Paula Briggs Consultant in Sexual and Reproductive Health
 Medical Management of Fibroids Esmya Dr Paula Briggs Consultant in Sexual and Reproductive Health Treatment options for Uterine Fibroids ESMYA Selective Uterine Artery Embolisation Fibroid ablation (hysteroscopic
Medical Management of Fibroids Esmya Dr Paula Briggs Consultant in Sexual and Reproductive Health Treatment options for Uterine Fibroids ESMYA Selective Uterine Artery Embolisation Fibroid ablation (hysteroscopic
Populations Interventions Comparators Outcomes Individuals: With uterine fibroids
 Protocol Magnetic Resonance-Guided Focused Ultrasound (701109) Medical Benefit Effective Date: 07/01/15 Next Review Date: 05/18 Preauthorization No Review Dates: 05/09, 05/10, 05/11, 05/12, 05/13, 05/14,
Protocol Magnetic Resonance-Guided Focused Ultrasound (701109) Medical Benefit Effective Date: 07/01/15 Next Review Date: 05/18 Preauthorization No Review Dates: 05/09, 05/10, 05/11, 05/12, 05/13, 05/14,
CARDIAC MRI. Cardiovascular Disease. Cardiovascular Disease. Cardiovascular Disease. Overview
 CARDIAC MRI Dr Yang Faridah A. Aziz Department of Biomedical Imaging University of Malaya Medical Centre Cardiovascular Disease Diseases of the circulatory system, also called cardiovascular disease (CVD),
CARDIAC MRI Dr Yang Faridah A. Aziz Department of Biomedical Imaging University of Malaya Medical Centre Cardiovascular Disease Diseases of the circulatory system, also called cardiovascular disease (CVD),
DENOMINATOR: All patients undergoing uterine artery embolization for leiomyomas and/or adenomyosis
 Quality ID #465: Uterine Artery Embolization Technique: Documentation of Angiographic Endpoints and Interrogation of Ovarian Arteries National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL
Quality ID #465: Uterine Artery Embolization Technique: Documentation of Angiographic Endpoints and Interrogation of Ovarian Arteries National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 2/12/2011 Radiology Quiz of the Week # 7 Page 1 CLINICAL PRESENTATION AND RADIOLOGY QUIZ
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 2/12/2011 Radiology Quiz of the Week # 7 Page 1 CLINICAL PRESENTATION AND RADIOLOGY QUIZ
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.29 MRI in Clinically Suspected Uterine and
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.29 MRI in Clinically Suspected Uterine and
The Comparison of Ovarian Reserve After Uterine Artery Embolization and Hysterectomy for Uterine Fibroma
 Original Article Elmer Press The Comparison of Ovarian Reserve After Uterine Artery Embolization and Hysterectomy for Uterine Fibroma Firoozeh Veisi a, c, Negin Rezavand a, Maryam Zangeneh a, Shilir Fallahi
Original Article Elmer Press The Comparison of Ovarian Reserve After Uterine Artery Embolization and Hysterectomy for Uterine Fibroma Firoozeh Veisi a, c, Negin Rezavand a, Maryam Zangeneh a, Shilir Fallahi
Fibroid mapping. Haitham Hamoda MD FRCOG Consultant Gynaecologist, Subspecialist in Reproductive Medicine & Surgery King s College Hospital
 Fibroid mapping Haitham Hamoda MD FRCOG Consultant Gynaecologist, Subspecialist in Reproductive Medicine & Surgery King s College Hospital Fibroids Common condition >70% of women by onset of menopause.
Fibroid mapping Haitham Hamoda MD FRCOG Consultant Gynaecologist, Subspecialist in Reproductive Medicine & Surgery King s College Hospital Fibroids Common condition >70% of women by onset of menopause.
Freedom of Information
 ND ref. FOI/16/309 Freedom of Information Thank you for your 19/10/16 request for the following information: Under the Freedom of Information Act, please could you fill out the following Freedom of Information
ND ref. FOI/16/309 Freedom of Information Thank you for your 19/10/16 request for the following information: Under the Freedom of Information Act, please could you fill out the following Freedom of Information
Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms: a case report
 Chen et al. BMC Urology (2017) 17:120 DOI 10.1186/s12894-017-0311-6 CASE REPORT Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms:
Chen et al. BMC Urology (2017) 17:120 DOI 10.1186/s12894-017-0311-6 CASE REPORT Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms:
H. IVERSEN*, S. LENZ and M. DUEHOLM ABSTRACT
 Ultrasound Obstet Gynecol 2012; 40: 445 451 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.11118 Ultrasound-guided radiofrequency ablation of symptomatic uterine fibroids:
Ultrasound Obstet Gynecol 2012; 40: 445 451 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.11118 Ultrasound-guided radiofrequency ablation of symptomatic uterine fibroids:
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the
 Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
Whole-tumor apparent diffusion coefficient measurements in nephroblastoma: Can it identify blastemal predominance? Abstract Purpose To explore the potential relation between whole-tumor apparent diffusion
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
2D and 3D MR imaging in the assessment of Fallopian tube features
 2D and 3D MR imaging in the assessment of Fallopian tube features Poster No.: C-1292 Congress: ECR 2010 Type: Topic: Scientific Exhibit Genitourinary Authors: J. Takahama, S. Kitano, N. Marugami, A. Takahashi,
2D and 3D MR imaging in the assessment of Fallopian tube features Poster No.: C-1292 Congress: ECR 2010 Type: Topic: Scientific Exhibit Genitourinary Authors: J. Takahama, S. Kitano, N. Marugami, A. Takahashi,
NIH Public Access Author Manuscript Radiology. Author manuscript; available in PMC 2007 April 10.
 NIH Public Access Author Manuscript Published in final edited form as: Radiology. 2006 July ; 240(1): 263 272. Uterine Leiomyomas: MR Imaging based Thermometry and Thermal Dosimetry during Focused Ultrasound
NIH Public Access Author Manuscript Published in final edited form as: Radiology. 2006 July ; 240(1): 263 272. Uterine Leiomyomas: MR Imaging based Thermometry and Thermal Dosimetry during Focused Ultrasound
Considering Surgery for Fibroids? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Fibroids? Learn about minimally invasive da Vinci Surgery The Condition: Uterine Fibroid (Fibroid Tumor) A uterine fibroid is a benign (non-cancerous) tumor that grows in the uterine
Considering Surgery for Fibroids? Learn about minimally invasive da Vinci Surgery The Condition: Uterine Fibroid (Fibroid Tumor) A uterine fibroid is a benign (non-cancerous) tumor that grows in the uterine
Chen et al. Journal of Therapeutic Ultrasound (2016) 4:27 DOI /s
 Chen et al. Journal of Therapeutic Ultrasound (2016) 4:27 DOI 10.1186/s40349-016-0072-9 RESEARCH The safety and effectiveness of volumetric magnetic resonance-guided high-intensity focused ultrasound treatment
Chen et al. Journal of Therapeutic Ultrasound (2016) 4:27 DOI 10.1186/s40349-016-0072-9 RESEARCH The safety and effectiveness of volumetric magnetic resonance-guided high-intensity focused ultrasound treatment
MRI-guided Focused Ultrasound Surgery of Uterine Leiomyomas 1
 MRI-guided Focused Ultrasound Surgery of Uterine Leiomyomas 1 Fiona M. Fennessy, Clare M. Tempany Uterine fibroids are the most common pelvic tumors in women and are a significant cause of morbidity for
MRI-guided Focused Ultrasound Surgery of Uterine Leiomyomas 1 Fiona M. Fennessy, Clare M. Tempany Uterine fibroids are the most common pelvic tumors in women and are a significant cause of morbidity for
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
Excessive menstrual blood loss
 Ian Chilcott Excessive menstrual blood loss >80mls - That interferes with physical, emotional, social and material quality of life 1 in 20 women aged 30 to 49 years consult their GP each year with menorrhagia
Ian Chilcott Excessive menstrual blood loss >80mls - That interferes with physical, emotional, social and material quality of life 1 in 20 women aged 30 to 49 years consult their GP each year with menorrhagia
MP Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome
 Medical Policy MP 4.01.18 BCBSA Ref. Policy: 4.01.18 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: OB/GYN Reproduction Related Policies 4.01.11 Occlusion of Uterine Arteries Using Transcatheter
Medical Policy MP 4.01.18 BCBSA Ref. Policy: 4.01.18 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: OB/GYN Reproduction Related Policies 4.01.11 Occlusion of Uterine Arteries Using Transcatheter
Uterine fibroids are common in premenopausal
 For uterine-sparing fibroid treatment, consider laparoscopic ultrasoundguided radiofrequency ablation Profile of a new minimally invasive treatment option James A. Macer, MD IN THIS ARTICLE Technique,
For uterine-sparing fibroid treatment, consider laparoscopic ultrasoundguided radiofrequency ablation Profile of a new minimally invasive treatment option James A. Macer, MD IN THIS ARTICLE Technique,
SURGICAL PROBLEMS IN FERTILITY- FIBROIDS. Dr.Māris Arājs gyn-ob specialist Cell phone:
 SURGICAL PROBLEMS IN FERTILITY- FIBROIDS Dr.Māris Arājs gyn-ob specialist maris@myclinicriga.lv Cell phone: +371 26556466 There is NO Industry Sponsorship and Financial Conflict of Interest for this presentation
SURGICAL PROBLEMS IN FERTILITY- FIBROIDS Dr.Māris Arājs gyn-ob specialist maris@myclinicriga.lv Cell phone: +371 26556466 There is NO Industry Sponsorship and Financial Conflict of Interest for this presentation
Comparison of 1.5 T Tesla and 3.0 T Tesla Magnetic Resonance Imaging for Evaluating Local Extension of Endometrial Cancer
 Showa Univ J Med Sci 27 1, 21 28, March 2015 Original Comparison of 1.5 T Tesla and 3.0 T Tesla Magnetic Resonance Imaging for Evaluating Local Extension of Endometrial Cancer Naomi YAGI, Masanori HIROSE,
Showa Univ J Med Sci 27 1, 21 28, March 2015 Original Comparison of 1.5 T Tesla and 3.0 T Tesla Magnetic Resonance Imaging for Evaluating Local Extension of Endometrial Cancer Naomi YAGI, Masanori HIROSE,
UNDER REVIEW. Uterine artery embolisation for the treatment of uterine fibroids
 Uterine artery embolisation for the treatment of uterine fibroids This statement has been developed and reviewed by the Women s Health Committee and approved by the RANZCOG Board and Council. A list of
Uterine artery embolisation for the treatment of uterine fibroids This statement has been developed and reviewed by the Women s Health Committee and approved by the RANZCOG Board and Council. A list of
Body and Bone Applications of Magnetic Resonance ImageGuided Focused Ultrasound Treatment
 Body and Bone Applications of Magnetic Resonance ImageGuided Focused Ultrasound Treatment Award: Cum Laude Poster No.: C-2526 Congress: ECR 2013 Type: Educational Exhibit Authors: Y. T. Oh, S.-W. Yoon,
Body and Bone Applications of Magnetic Resonance ImageGuided Focused Ultrasound Treatment Award: Cum Laude Poster No.: C-2526 Congress: ECR 2013 Type: Educational Exhibit Authors: Y. T. Oh, S.-W. Yoon,
Cost-effectiveness of uterine artery embolization and hysterectomy for uterine fibroids Beinfeld M T, Bosch J L, Isaacson K B, Gazelle G S
 Cost-effectiveness of uterine artery embolization and hysterectomy for uterine fibroids Beinfeld M T, Bosch J L, Isaacson K B, Gazelle G S Record Status This is a critical abstract of an economic evaluation
Cost-effectiveness of uterine artery embolization and hysterectomy for uterine fibroids Beinfeld M T, Bosch J L, Isaacson K B, Gazelle G S Record Status This is a critical abstract of an economic evaluation
Half-Fourier Acquisition Single-Shot Turbo Spin-Echo (HASTE) MR: Comparison with Fast Spin-Echo MR in Diseases of the Brain
 Half-Fourier Acquisition Single-Shot Turbo Spin-Echo (HASTE) MR: Comparison with Fast Spin-Echo MR in Diseases of the Brain Mahesh R. Patel, Roman A. Klufas, Ronald A. Alberico, and Robert R. Edelman PURPOSE:
Half-Fourier Acquisition Single-Shot Turbo Spin-Echo (HASTE) MR: Comparison with Fast Spin-Echo MR in Diseases of the Brain Mahesh R. Patel, Roman A. Klufas, Ronald A. Alberico, and Robert R. Edelman PURPOSE:
Uterine artery embolization for symptomatic uterine fibroids(review)
 Cochrane Database of Systematic Reviews Uterine artery embolization for symptomatic uterine fibroids (Review) GuptaJK,SinhaA,LumsdenMA,HickeyM GuptaJK,SinhaA,LumsdenMA,HickeyM. Uterine artery embolization
Cochrane Database of Systematic Reviews Uterine artery embolization for symptomatic uterine fibroids (Review) GuptaJK,SinhaA,LumsdenMA,HickeyM GuptaJK,SinhaA,LumsdenMA,HickeyM. Uterine artery embolization
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
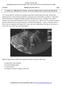 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/20/2011 Radiology Quiz of the Week # 34 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/20/2011 Radiology Quiz of the Week # 34 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Bilgin Keserci 1* and Nguyen Minh Duc 2
 Keserci and Duc Journal of Therapeutic Ultrasound (217) 5:22 DOI 1.1186/s4349-17-1-4 RESEARCH Open Access Volumetric magnetic resonance-guided high-intensity focused ultrasound ablation of uterine fibroids
Keserci and Duc Journal of Therapeutic Ultrasound (217) 5:22 DOI 1.1186/s4349-17-1-4 RESEARCH Open Access Volumetric magnetic resonance-guided high-intensity focused ultrasound ablation of uterine fibroids
Comparative Study Between Robotic Laparoscopic Myomectomy and Abdominal Myomectomy
 Comparative Study Between Robotic Laparoscopic Myomectomy and Abdominal Myomectomy Magdi Hanafi, M.D., FACOG, FACS. Medical Director GYN & Fertility Specialists Emory Saint Joseph s Hospital Atlanta, Georgia.
Comparative Study Between Robotic Laparoscopic Myomectomy and Abdominal Myomectomy Magdi Hanafi, M.D., FACOG, FACS. Medical Director GYN & Fertility Specialists Emory Saint Joseph s Hospital Atlanta, Georgia.
Description. Section: Surgery Effective Date: July 15, 2016 Subsection: Original Policy Date: December 7, 2011 Subject: Page: 1 of 10
 Last Review Status/Date: June 2016 Description Page: 1 of 10 An integrated system providing magnetic resonance guided focused ultrasound (MRgFUS) treatment is proposed as a noninvasive therapy for uterine
Last Review Status/Date: June 2016 Description Page: 1 of 10 An integrated system providing magnetic resonance guided focused ultrasound (MRgFUS) treatment is proposed as a noninvasive therapy for uterine
Magnetic Resonance Guided Focused Ultrasound
 Magnetic Resonance Guided Focused Ultrasound Policy Number: 7.01.109 Last Review: 8/2017 Origination: 3/2007 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Magnetic Resonance Guided Focused Ultrasound Policy Number: 7.01.109 Last Review: 8/2017 Origination: 3/2007 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Volumetric MR-guided high-intensity focused ultrasound ablation to treat uterine fibroids through the abdominal scars using scar patch: a case report
 Zhu et al. Journal of Therapeutic Ultrasound (2016) 4:20 DOI 10.1186/s40349-016-0064-9 CASE STUDY Volumetric MR-guided high-intensity focused ultrasound ablation to treat uterine fibroids through the abdominal
Zhu et al. Journal of Therapeutic Ultrasound (2016) 4:20 DOI 10.1186/s40349-016-0064-9 CASE STUDY Volumetric MR-guided high-intensity focused ultrasound ablation to treat uterine fibroids through the abdominal
Noninvasive thermal ablation of uterine leiomyomas is possible with extracorporeal magnetic resonance (MR) imaging guided focused ultrasound surgery.
 Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, use the Radiology Reprints form at the end of this article.
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, use the Radiology Reprints form at the end of this article.
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography
 Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
Questions to be answered by MRI in the planning and evaluation of fibroid embolization
 Questions to be answered by MRI in the planning and evaluation of fibroid embolization Award: Magna Cum Laude Poster No.: C-0076 Congress: ECR 2015 Type: Educational Exhibit Authors: C. Maciel, A. M. Madureira,
Questions to be answered by MRI in the planning and evaluation of fibroid embolization Award: Magna Cum Laude Poster No.: C-0076 Congress: ECR 2015 Type: Educational Exhibit Authors: C. Maciel, A. M. Madureira,
HERMES Time and Workflow Primary Paper. Statistical Analysis Plan
 HERMES Time and Workflow Primary Paper Statistical Analysis Plan I. Study Aims This is a post-hoc analysis of the pooled HERMES dataset, with the following specific aims: A) To characterize the time period
HERMES Time and Workflow Primary Paper Statistical Analysis Plan I. Study Aims This is a post-hoc analysis of the pooled HERMES dataset, with the following specific aims: A) To characterize the time period
Successful MRI-Guided Focused Ultrasound Uterine Fibroid Treatment Despite an Ostomy and Significant Abdominal Wall Scarring
 uccessful MRI-Guided ocused Ultrasound Uterine ibroid Treatment Despite an Ostomy and ignificant Abdominal Wall carring The Harvard community has made this article openly available. Please share how this
uccessful MRI-Guided ocused Ultrasound Uterine ibroid Treatment Despite an Ostomy and ignificant Abdominal Wall carring The Harvard community has made this article openly available. Please share how this
INTERVENTIONAL PROCEDURES PROGRAMME
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic laser myomectomy Introduction This overview has been prepared to assist
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic laser myomectomy Introduction This overview has been prepared to assist
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Endometrial Stromal Sarcoma
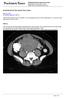 May 26, 2011 By Sushila Ladumor, MD [1] Endometrial stromal sarcoma (ESS) is a rare malignant tumor of the endometrium, occurring in the age group of 40-50 years. History The 50-year-old, female patient
May 26, 2011 By Sushila Ladumor, MD [1] Endometrial stromal sarcoma (ESS) is a rare malignant tumor of the endometrium, occurring in the age group of 40-50 years. History The 50-year-old, female patient
Supplementary Online Content
 1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
PI-RADS classification: prognostic value for prostate cancer grading
 PI-RADS classification: prognostic value for prostate cancer grading Poster No.: C-1622 Congress: ECR 2014 Type: Scientific Exhibit Authors: I. Platzek, A. Borkowetz, T. Paulus, T. Brauer, M. Wirth, M.
PI-RADS classification: prognostic value for prostate cancer grading Poster No.: C-1622 Congress: ECR 2014 Type: Scientific Exhibit Authors: I. Platzek, A. Borkowetz, T. Paulus, T. Brauer, M. Wirth, M.
Role of pelvic MRI in detection and characterization of uterine leiomyoma
 Role of pelvic MRI in detection and characterization of uterine leiomyoma Poster No.: C-1197 Congress: ECR 2016 Type: Educational Exhibit Authors: N. zouari, A. Ben Miled, E. KOULIBALY SANOU, S. Zaouali,
Role of pelvic MRI in detection and characterization of uterine leiomyoma Poster No.: C-1197 Congress: ECR 2016 Type: Educational Exhibit Authors: N. zouari, A. Ben Miled, E. KOULIBALY SANOU, S. Zaouali,
Case Report Successful MRI-Guided Focused Ultrasound Uterine Fibroid Treatment Despite an Ostomy and Significant Abdominal Wall Scarring
 International cholarly Research Network IRN Obstetrics and Gynecology Volume 2011, Article ID 962621, 4 pages doi:10.5402/2011/962621 Case Report uccessful MRI-Guided ocused Ultrasound Uterine ibroid Treatment
International cholarly Research Network IRN Obstetrics and Gynecology Volume 2011, Article ID 962621, 4 pages doi:10.5402/2011/962621 Case Report uccessful MRI-Guided ocused Ultrasound Uterine ibroid Treatment
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
OB/GYN CONTEMPORARY. Uterine Fibroid Embolization for the Management of Uterine Fibroids. JUNE
 Supplement to CONTEMPORARY OB/GYN Translating science into sound clinical practice JUNE 2006 www.contemporaryobgyn.net Uterine Fibroid Embolization for the Management of Uterine Fibroids Funded by and
Supplement to CONTEMPORARY OB/GYN Translating science into sound clinical practice JUNE 2006 www.contemporaryobgyn.net Uterine Fibroid Embolization for the Management of Uterine Fibroids Funded by and
Tissue Morcellation: Managing Risks to Drive Best Patient Outcomes
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
6/24/2013. John C. Lipman, MD, FACR, FSIR Atlanta, Georgia. Disclosure. Educational grant: Merit Medical, Boston Scientific
 John C. Lipman, MD, FACR, FSIR Atlanta, Georgia Disclosure Educational grant: Merit Medical, Boston Scientific Urban Myths 1. Need bilateral embolization. 2. Contraindicated to treat large fibroids/large
John C. Lipman, MD, FACR, FSIR Atlanta, Georgia Disclosure Educational grant: Merit Medical, Boston Scientific Urban Myths 1. Need bilateral embolization. 2. Contraindicated to treat large fibroids/large
Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome. Original Policy Date
 MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Time-resolved Magnetic Resonance Angiography for assessment of recanalization after coil embolization of visceral artery aneurysms
 Signature: Pol J Radiol, 2013; 78(1): 64-68 DOI: 10.12659/PJR.883769 CASE REPORT Received: 2012.09.29 Accepted: 2013.01.15 Time-resolved Magnetic Resonance Angiography for assessment of recanalization
Signature: Pol J Radiol, 2013; 78(1): 64-68 DOI: 10.12659/PJR.883769 CASE REPORT Received: 2012.09.29 Accepted: 2013.01.15 Time-resolved Magnetic Resonance Angiography for assessment of recanalization
Effectiveness of Contrast-enhanced MR Angiography for Visualization of the Prostatic Artery prior to Prostatic Arterial Embolization
 ORIGINAL RESEARCH GENITOURINARY IMAGING Effectiveness of Contrast-enhanced MR Angiography for Visualization of the Prostatic Artery prior to Prostatic Arterial Embolization Jin Long Zhang, MD Mao Qiang
ORIGINAL RESEARCH GENITOURINARY IMAGING Effectiveness of Contrast-enhanced MR Angiography for Visualization of the Prostatic Artery prior to Prostatic Arterial Embolization Jin Long Zhang, MD Mao Qiang
TECHNICAL NOTE. Introduction. Materials and Methods
 Magn Reson Med Sci 2018; XX; XXX XXX doi:10.2463/mrms.tn.2017-0103 Published Online: January 18, 2018 TECHNICAL NOTE MR-guided Focused Ultrasound for Uterine Fibroids: A Preliminary Study of Relationship
Magn Reson Med Sci 2018; XX; XXX XXX doi:10.2463/mrms.tn.2017-0103 Published Online: January 18, 2018 TECHNICAL NOTE MR-guided Focused Ultrasound for Uterine Fibroids: A Preliminary Study of Relationship
NIH Public Access Author Manuscript J Magn Reson Imaging. Author manuscript; available in PMC 2009 September 29.
 NIH Public Access Author Manuscript Published in final edited form as: J Magn Reson Imaging. 2009 February ; 29(2): 404 411. doi:10.1002/jmri.21688. MRI-based Thermal Dosimetry and Diffusion-weighted Imaging
NIH Public Access Author Manuscript Published in final edited form as: J Magn Reson Imaging. 2009 February ; 29(2): 404 411. doi:10.1002/jmri.21688. MRI-based Thermal Dosimetry and Diffusion-weighted Imaging
UTERINE FIBROID EMBOLIZATION
 INTERVENTIONAL RADIOLOGY PROTOCOLS UTERINE FIBROID EMBOLIZATION Interventional Radiology Tower Health Medical Group offers the option to treat uterine fibroids with fibroid embolization (UFE), an alternative
INTERVENTIONAL RADIOLOGY PROTOCOLS UTERINE FIBROID EMBOLIZATION Interventional Radiology Tower Health Medical Group offers the option to treat uterine fibroids with fibroid embolization (UFE), an alternative
Interobserver variation in cervical cancer tumor delineation for image-based radiotherapy planning among and within different specialties
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 6, NUMBER 4, FALL 2005 Interobserver variation in cervical cancer tumor delineation for image-based radiotherapy planning among and within different
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 6, NUMBER 4, FALL 2005 Interobserver variation in cervical cancer tumor delineation for image-based radiotherapy planning among and within different
Clinical Correlation of a New Practical MRI Method for Assessing Cervical Spinal Canal Compression
 Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Postoperative Outcomes After Robotic Versus Abdominal Myomectomy
 SCIENTIFIC PAPER Postoperative Outcomes After Robotic Versus Abdominal Myomectomy Leanne Griffin, MD, Joe Feinglass, PhD, Ariane Garrett, BA, Anne Henson, BA, Leeber Cohen, MD, Angela Chaudhari, MD, Alexander
SCIENTIFIC PAPER Postoperative Outcomes After Robotic Versus Abdominal Myomectomy Leanne Griffin, MD, Joe Feinglass, PhD, Ariane Garrett, BA, Anne Henson, BA, Leeber Cohen, MD, Angela Chaudhari, MD, Alexander
Purpose: Materials and Methods: Results: Conclusion: Original Research n Thoracic Imaging
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. MR Imaging of Pulmonary
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. MR Imaging of Pulmonary
Fast Breath-Hold T2-Weighted MR Imaging Reduces Interobserver Variability in the Diagnosis of Adenomyosis
 Marc Bazot 1 Emile Daraï 2 Sébastien Clément de Givry 1 Frank Boudghène 1 Serge Uzan 2 Alain Ferdinand Le Blanche 1 Received April 15, 2002; accepted after revision September 26, 2002. 1 Department of
Marc Bazot 1 Emile Daraï 2 Sébastien Clément de Givry 1 Frank Boudghène 1 Serge Uzan 2 Alain Ferdinand Le Blanche 1 Received April 15, 2002; accepted after revision September 26, 2002. 1 Department of
Treatment patterns for women with new episodes of uterine myomas in an insured population in the US
 Current Medical Research and Opinion Vol. 22, No. 1, 2006, 95 100 2006 LibraPharm Limited 0300-7995 doi:10.1185/030079906x80323 All rights reserved: reproduction in whole or part not permitted ORIGINAL
Current Medical Research and Opinion Vol. 22, No. 1, 2006, 95 100 2006 LibraPharm Limited 0300-7995 doi:10.1185/030079906x80323 All rights reserved: reproduction in whole or part not permitted ORIGINAL
Distinguishing high-flow from low-flow vascular malformations using maximum intensity projection images in dynamic magnetic resonance angiography
 Distinguishing high-flow from low-flow vascular malformations using maximum intensity projection images in dynamic magnetic resonance angiography Poster No.: C-2297 Congress: ECR 2016 Type: Scientific
Distinguishing high-flow from low-flow vascular malformations using maximum intensity projection images in dynamic magnetic resonance angiography Poster No.: C-2297 Congress: ECR 2016 Type: Scientific
Stephen Derek Quinn 1*, John Vedelago 2, Lesley Regan 1 and Wladyslaw M Gedroyc 2
 Quinn et al. Journal of Therapeutic Ultrasound 2013, 1:20 RESEARCH ARTICLE Open Access Safety and treatment volumes achieved following new developments of the magnetic resonance-guided focused ultrasound
Quinn et al. Journal of Therapeutic Ultrasound 2013, 1:20 RESEARCH ARTICLE Open Access Safety and treatment volumes achieved following new developments of the magnetic resonance-guided focused ultrasound
