Homocystinuria: what about mild
|
|
|
- Suzan Goodwin
- 5 years ago
- Views:
Transcription
1 Postgrad Med J 1996; 72: ( The Fellowship of Postgraduate Medicine, 1996 Classic diseases revisited Summary Hyperhomocysteinaemia is associated with an increased risk of atherosclerotic vascular disease and thromboembolism, in both men and women. A variety of conditions can lead to elevated homocysteine levels, but the relation between high levels and vascular disease is present regardless of the underlying cause. Pooled data from a large number of studies demonstrate that mild hyperhomocysteinaemia after a standard methionine load is present in 21% of young patients with coronary artery disease, in 24 % of patients with cerebrovascular disease, and in 32% of patients with peripheral vascular disease. From such data an odds ratio of 13.0 (95% confidence interval 5.9 to 28.1), as an estimate ofthe relative risk of vascular disease at a young age, can be calculated in subjects with an abnormal response to methionine loading. Furthermore, mild hyperhomo-cysteinaemia can lead to a two- or three-fold increase in the risk of recurrent venous thrombosis. Elevated homocysteine levels can be reduced to normal in virtually all cases by simple and safe treatment with vitamin B6, folic acid, and betaine, each of which is involved in methionine metabolism. A clinically beneficial effect of such an intervention, currently under investigation, would make largescale screening for this risk factor mandatory. Keywords: hyperhomocysteinaemia, atherosclerosis, pathogenesis, homocystinuria Institute for Cardiovascular Research, Departnent of Vascular Surgery, Free University Hospital, PO Box 7057, 1007 MB Amsterdam, The Netherlands M van den Berg Department of Internal Medicine, University Hospital Nijmegen, 6500 HB Nijmegen, The Netherlands GHJ Boers Accepted 22 November 1995 Homocystinuria: what about mild hyperhomocysteinaemia? M van den Berg, GHJ Boers Atherosclerotic disease, notably coronary artery disease, remains the major cause of death in the western world. This increased risk of mortality from cardiovascular disease cannot be fully explained by traditional risk factors such as hyperlipoproteinaemia, smoking, hypertension and male sex. Since the last decade, mildly elevated homocysteine levels have also been recognised as a serious risk factor in the development of atherosclerotic disease and thromboembolism. Severe hyperhomocysteinaemia, such as in homocystinuria due to cystathionine synthase deficiency, is inherited as an autosomal recessive trait and may lead to occlusive arterial disease and thromboembolism even in early infancy.1 From a collaborative study on more than 600 homozygous patients, Mudd et al observed that there was a 50% chance for untreated patients to suffer from a vascular event before the age of 30 years.2 In line with this observation, the hypothesis has been put forward that even mild hyperhomocysteinaemia may predispose for arterial occlusive disease, even at a young age. Indeed, casecontrolled, cross-sectional, and prospective epidemiological studies have shown that mildly elevated homocysteine levels are associated with an increased risk of arterial occlusive disease. This relationship has been reported for both fasting homocysteine levels and for hyperhomocysteinaemia unmasked by means of a methionine loading test in which homocysteine metabolism is stressed with an oral dose of L-methionine (0.1 g/kg body weight). Whether fasting or postmethionine plasma homocysteine level is the better predictor ofvascular disease has not been clarified. It has been shown that safe doses of vitamins can induce normalisation of such increased homocysteine blood levels4'5 and may ameliorate endothelial function in mildly hyperhomocysteinaemic vascular patients.8 In conclusion, mild hyperhomocysteinaemia has been recognised as an important risk factor for atherosclerotic disease, thus providing the rationale for large-scale screening and intervention with innocuous vitamins in patients with elevated homocysteine levels. Relevant aspects of this unconventional risk factor are briefly discussed in this paper. Metabolism and aetiology of hyperhomocysteinaemia The essential amino acid methionine, which is present in protein of animal origin, is the only source of homocysteine in man.' Normally, homocysteine is rapidly catabolised by transsulphuration into cysteine or is remethylated to methionine (figure 1). Cystathionine synthase catalyses the first step in transsulphuration with vitamin B6 in its active form, pyridoxal phosphate, as cofactor. In many body tissues remethylation by the folate- and vitamin B12- dependent enzyme N5-methyltetrahydrofolate-homocysteine methyltransferase is operational and in the liver homocysteine is also remethylated by betaine (trimethylglycine), formed from choline. Plasma homocysteine is the sum of homocysteine, whether free or bound to proteins, and the homocysteinyl moieties of the disulphides homocystine and cysteine-homocysteine. Hyperhomocysteinaemia refers to levels of such 'total' homocysteine level in the blood, plasma or serum. Epidemiological studies strongly suggest a graded response rather than a threshold effect of homocysteine levels, but for practical reasons the following classification has been made: moderate, intermediate and severe fasting hyperhomocysteinaemia, with levels between 16 and 30, 31 and 100, and more than 100,umol/l, respectively.9 In diagnosing hyperhomocysteinaemia in the individual patient it is preferable to perform a methionine loading testll1, as stated later. The generally used cut-off points for post-load hyperhomocysteinaemia are sex specific, ie, in men 54, in premenopausal women 51, and in postmenopausal women 69 jumol/l, respectively. '0" Severe hyperhomocysteinaemia, also known as homocystinuria, is an
2 514 van den Berg, Boers Figure 1 Methionine homocysteine metabolism. 1, cystathionine synthase; 2, methionine synthase; 3, methylenetetrahydrofolate reductase Causes of mild hyperhomocysteinaemia Genetic * cystathionine synthase deficiency * methylenetetrahydrofolate reductase deficiency * methionine synthase deficiency Environmental * deficiencies of vitamin B6, folic acid, vitamin B12 * renal failure * dietary changes: excessive protein intake * drug use: nitrous oxide, methotrexate, anti-epileptics Box 1..., *~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~ N.~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~...._ U~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~ ~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~... lenis mafni etrs an etl retar Figure 2 The severely elevated homocysteine levels datio, in but classical at thsae.tl homocystinua.may ovsua lead to a syndrome characterised by ectopia lentis, marfanoid shw an symto features, mental exep fo retardation, mnrotpeniai:_3 and/or thromboembolic and atherosclerotic events. Two extremes in the clinical expression are shown here: the patient on the left is a morer seirioiusl affected boy, 15ye%uars of agei METHIONINE S-ADENOSYLMETHIONINE A TETRAHYDROFOLATE DIMETHYLGLYCINE It BETAINE / \2 S-ADENOSYLHOMOCYSTEINE \ I\ vmethyl- I COBALAMIN 5, 10-METHYLENE- BETAINE 2 TETRAHYDROFOLATE HOMOCYSTEINE 5-METHYL- TETRAHYDROFOLATE 1 PYRIDOXAL-5-PHOSPHATE CYSTATHIONINE CYSTEINE PYRIDOXAL-5-PHOSPHATE abnormal biochemical phenotype (figure 2) associated with deficient activity of one of several enzymes in methionine metabolism, notably cystathionine synthase, 5,10-methylenetetrahydrofolate reductase, and disorders of methionine synthase activity due to a defect in synthesis of methylcobalamin (figure 1). Disorders of cystathionine synthase impair homocysteine flux through the transsulphuration pathway; disorders of the other two enzymes affect homocysteine remethylation to methionine.' Mild hyperhomocysteinaemia, either in the fasting state or after a standardised methionine load, can be the consequence of intermediate deficiency (about 50% rest activity) of one of the involved enzymes as mentioned above. Such an intermediate effect is known to cause mild hyperhomocysteinaemia in heterozygotes for cystathionine synthase deficiency, 2,13 but not in carriers of 5,10-methylenetetrahydrofolate reductase deficiency.'2 Recently the existence of an inherited mutant variant of 5,10- methylenetetrahydrofolate reductase characterised by thermolability has been demonstrated (box 1). Homozygotes for this mutation can show mild hyperhomocysteinaemia although it is not obligatory,'5 whereas heterozygotes are normohomocysteinaemic.1 Compound heterozygotes of both reductase mutations are also hyperhomocysteinaemic in the majority of cases.'4 The variation in individual plasma homocysteine levels is caused not only by genetic but also by environmental factors. Homocysteine plasma levels rise with decreasing folate and vitamin B6 intakes and blood levels.'6 Dietary vitamin B6 deficiency has been shown to increase the excretion of homocysteine in the urine after a methionine load.'7 An effect on the fasting homocysteine blood level, however, could not be demonstrated by such a deficiency,'8 and in another study, low plasma vitamin B6 levels were not related to homocysteine concentrations before and after methionine loading (box 1).19 Plasma homocysteine is increased in patients with renal failure. This has been hypothesized to contribute to the high incidence of occlusive arterial disease in these patients. The increase of plasma homocysteine is moderate to marked (up to 50 yumol/l) and is positively correlated with serum creatinine.20 Impaired methionine clearance after loading with the amino acid is reported in chronic liver disease and hepatic insufficiency and supposedly will affect homocysteine concentrations in the blood, although data on such measurements are not available.20 Increased homocysteine levels have been reported in type 1 diabetic mellitus patients with serum creatinine levels above 1 15,umol/l due to diabetic nephropathy, but not in those with minimal nephropathy.2' In addition, a lack of association between plasma homocysteine and microangiopathy was recently reported in patients with type 1 diabetes mellitus, however, patients with clinical signs of nephropathy had higher plasma homocysteine levels.22 In conclusion, type 1 diabetes is not per se associated with increased plasma homocysteine levels but, if homocysteine accumulates due to advanced nephropathy, it may 3
3 Mild hyperhomocysteinaemia and vascular disease 515 Prevalence of mild (post-load) hyperhomocysteinaemia * 1-2% in the general population3 Among 730 screened vascular patients: * 25-33% of those with peripheral arterial disease4'5 * 20-28% of those with cerebrovascular disease4'5 * 15% of those with coronary artery disease4 Box 2 Diagnosis * elevated homocysteine levels in the fasting state, and/or * after methionine loading (0.1 g/kg orally) Box 3 contribute to the accelerated development of macroangiopathy in diabetics. These findings should therefore be considered in the context of a positive relation between homocysteine and creatinine. The intra-individual day-to-day variation in fasting homocysteine levels is rather wide, up to 25%. One of the causes of this variation could be dietary changes during the day preceding the fasting samplings because it has been shown that a protein-rich meal may affect plasma homocysteine levels for at least eight hours.23 A post-methionine-load homocysteine determination, four to six hours after the methionine intake, will have a distance in time from the last protein-containing meal of at least 16 hours and during the test itself the protocol inhibits protein intake. Therefore, less intra-individual variation in post-methionine plasma homocysteine levels might be expected (box 1). The antifolate drug methotrexate, folate-deficiency-inducing anti-epileptics, and nitrous oxide, which inactivates vitamin B,2, will increase plasma homocysteine (box 1). Recently, the modulation of plasma homocysteine by these and various other pharmacological agents, such as penicillamine and oestrogens, has been extensively reviewed.20'24 Mild hyperhomocysteinaemia and vascular disease In 1976, Wilcken and Wilcken were the first to publish results suggesting that even mild hyperhomocysteinaemia could have a possible role in the pathogenesis of coronary artery disease.25 They showed that about 30% ofyoung patients with angiographically proven coronary artery disease demonstrated mild hyperhomocysteinaemia, four hours after a methionine load. This unique finding suggested an important role for even mild hyperhomocysteinaemia in the pathogenesis of vascular disease at a young age. Since then, numerous studies have shown that mild hyperhomocysteinaemia is a frequent finding amongst vascular patients. In 1992 pooled data revealed a prevalence of 32% in patients with peripheral vascular disease, 24% in patients with cerebrovascular disease, and 21% in patients with coronary artery disease.3'26 From pooled data an odds ratio of 13.0 (95% CI ) could be calculated as an estimate of the relative cardiovascular risk in subjects with an abnormal response to methionine loading compared to normal responders.3 The recently published data by van den Berg et al4 and Franken et a1 are in line with the finding of high prevalences of mild post-load hyperhomocysteinaemia amongst vascular patients (box 2). Recently, prospective studies have indeed confirmed that mild hyperhomocysteinaemia in men is associated with an increased incidence of myocardial infarction6'7 and, possibly, of stroke.27 In addition, a dose-response relationship is supported by the fact that hyperhomocysteinaemia is reported to be associated with the severity of peripheral arterial disease28 and with the number of stenosed coronary vessels29 in arteriosclerotic patients. Malinow et a130 observed a graded increase in the prevalence of carotid artery intimal-medial thickening with increasing random homocysteine levels in asymptomatic subjects, which was more pronounced in women. Selhub et a13' reported a relationship between random homocysteine levels and the prevalence of carotid artery stenosis. Taken together, the epidemiologic evidence may indicate a graded effect of plasma homocysteine levels, as in hypercholesterolaemia, rather than a threshold effect. It has recently been shown that mild hyperhomocysteinaemia is a strong risk factor for recurrent venous thrombosis and can lead to a two-fold or three-fold increase in risk.32 Possible relationships between plasma homocysteine and convential risk factors for vascular disease have been studied but no such relation was established for tobacco smoking, hypertension, serum lipids, or diabetes mellitus. Therefore, so far, hyperhomocysteinaemia seems to be an independent risk factor for cardiovascular disease.12'33 At this stage, it is unresolved which is the most sensitive indicator of excess cardiovascular risk, either the fasting, the post-load homocysteine level, or both (box 3). Identification of patients at risk simply on the basis of their fasting homocysteine level might be insufficient because, depending on the cut-off point, about 40-54% of patients with high post-methionine homocysteine have a normal fasting level.4"0 The latter finding, moreover, suggests the existence of multiple underlying metabolic deficits, because fasting and post-methionine homocysteine levels are thought to be determined by different pathways, ie, remethylation and transsulphuration of homocysteine, respectively. A serious argument against the use of the post-methionine homocysteine level as the criterion of hyperhomocysteinaemia is the fact that the methionine loading test is too laborious and expensive to include in the design of epidemiological studies with large numbers of participants. Even in diagnostic procedures in individual vascular patients, the practical concerns and high costs of establish-
4 516 van den Berg, Boers Atherogenetic mechanisms of homocysteine * damaging endothelial cells by generation of hydrogen peroxide, oxidation of low-density lipoprotein, and depletion of nitric oxide * proliferation of smooth muscle cells * coagulation/fibrinolysis interaction: inhibiting expression of thrombomodulin Box 4 ing post-methionine homocysteine levels suggest that this test is not feasible as a routine screening procedure. If it is to become so, more effort is needed to standardise the sampling of fasting homocysteine levels and more attention should be paid to the food intake on the day preceding the blood sampling, to minimise the wide intra-individual daily variation of these levels, as mentioned before. Pathogenesis of vascular disease in mild hyperhomocysteinaemia Homocysteine, an amino acid with a free sulphhydryl group, is generally held to be atherogenic and thrombogenic, although the exact pathophysiological sequence has not been clarified. Homocysteine is thought to damage endothelial cells by several mechanisms, eg, generation of hydrogen peroxide4 oxidation of low-density lipoproteins, and depletion of nitric oxide-mediated detoxification of homocysteine.35 In studies in animals, high homocysteine levels have been shown to induce endothelial cell injury.36'3 In vitro studies indicate that cultured endothelial cells from obligate heterozygotes for homocystinuria are more susceptible to homocysteine-mediated injury than normal cells.38 Another potential mechanism, recently described by Tsai et a139 is that homocysteine induces the proliferation of smooth muscle cells, a key feature of atherogenesis. It has also been reported that homocysteine inhibits the expression of thrombomodulin on the surface of the endothelial cell, leading to decreased protein C activation and thus, possibly, contributing to the development of thrombosis in hyperhomocysteinaemic patients.40 Although data in humans are scarce, van den Berg et a18 showed in hyperhomocysteinaemic patients with lower extremity occlusive atherosclerotic disease that endothelial dysfunction, as estimated by increased plasma von Willebrand factor concentrations, was ameliorated by treatment of hyperhomocysteinaemia with folic acid and vitamin B6. In conclusion, abnormalities of endothelial cells, platelets, clotting factors, serum lipids or disorders in the complex interaction of these factors have been held responsible for the vascular damage and thrombogenesis. A survey of all proposed hypotheses has been presented elsewhere (box 4).1,3 The cause of mild hyperhomocysteinaemia in vascular patients Analogous to the first observation by Sardharwalla et al of mildly elevated homocysteine levels in obligate heterozygotes for cystathionine synthase deficiency,41 it has been proposed that such hyperhomocysteinemia detected in vascular patients also originates from heterozygosity for this specific enzyme defect. In the two reports presenting determinations of cystathionine synthase activity in cultured fibroblasts from hyperhomocysteinaemic vascular patients, an intermediate enzyme deficiency was indeed found.'2'13 In recent years, however, it has become increasingly clear that the identification of patients with vascular disease as heterozygotes for cystathionine synthase deficiency is not convincing.42'43 More recent determinations of enzyme assays in hyperhomocysteinaemic vascular patients show that cystathionine synthase activity is deficient only in sporadic cases and wide variability in activity in cultured fibroblasts may occur, even in healthy persons'2 and recently it has been shown that heterozygous carriers and homocystinuric patients were free from inactivating mutations.44 The role of the cystathionine synthase gene may have been overestimated in the past and, therefore, the re-methylation pathway has gained more interest in recent years. Recently, Rozen's group cloned the gene responsible for the enzyme methylenetetrahydrofolate reductase, which has permitted mutational analysis in this gene, facilitating the evaluation of the re-methylation pathway in the aetiology of hyperhomocysteinaemia.46 Thermolability of 5,10 methylenetetrahydrofolate reductase proves to be a far more common genetic defect among these patients.'4'42 Homozygotes for this mutation have been detected in 5% of the general population and in up to 17% of 212 coronary patients. 5 Recently, a common mutation in 5,1 0-methylenetetrahydrofolate reductase has been identified, which in the heterozygous or homozygous state correlates with reduced enzyme activity and decreased thermostability in lymphocyte extracts.46 In addition, individuals homozygous for the mutation have significantly elevated plasma homocysteine levels, both in the fasting state and after methionine loading.46 Notwithstanding the occurrence of thermolabile enzyme in 28% of some groups of hyperhomocysteinaemic vascular patients,42 this prevalence still does not seem high enough to predict a predominant role of this defect among possible causes of mild hyperhomocysteinaemia in vascular patients.
5 Mild hyperhomocysteinaemia and vascular disease 517 Treatment In fasting homocysteine folic acid: 0.65 mg daily: 40% reduction 2.5 mg daily: 37% reduction 5 mg daily: 50% reduction 10 mg daily: 50% reduction vitamin B6: no effect vitamin B12: only modest effect (-15%), but should be added to avoid folic acid refractoriness and deterioration of neuropathy in vitamin B12- deficient cases. A sufficient dose is 0.4 mg daily In post-methionine hyperhomocysteinaemia vitamin B6, 100 mg + folic acid, 5 mg daily: 50% reduction vitamin B6, 100 to 250 mg daily: 40% reduction folic acid (n = 6 patients only): 45% reduction (lower doses of vitamin B6 and/or folic acid have not been studied) To lower fasting homocysteine levels 0.65 mg folic acid plus 0.4 mg cyanocobalamin To lower post-methionine homocysteine levels 100 mg vitamin B6 plus 5 mg folic acid Box 5 Homocysteine-lowering interventions FASTING HOMOCYSTEINE LEVELS From pooled data' 1 it can be estimated that it is possible to induce a reduction of about 40% of mildly elevated fasting plasma homocysteine levels by the use of doses of folic acid as low as 0.65 mg daily. A lower dose has not been studied. A dose of 2.5 mg daily had the same effect as 0.65 mg, 5 mg daily resulted in a slightly larger decrease of about 50%, and increasing the dose up to 10 mg daily had no extra effect. Supplementation of vitamin B6 did not affect fasting homocysteine levels significantly. Vitamin B12 in an oral dose of 0.4 mg cyanocobalamin daily has only a modest effect but is added to folic acid therapy mainly to avoid folic-acid refractoriness in the case of vitamin B12 deficiency and to prevent the development of neuropathy due to unrecognised pernicious anaemia (box 5). In summary, the prescription of 0.65 mg folic acid plus 0.4 mg cyanocobalamin daily is sufficient to lower a mild fasting hyperhomocysteinaemia by about 50%. POST-METHIONINE HOMOCYSTEINE LEVELS Available data on the effect of various homocysteine-lowering regimens upon mildly elevated post-methionine homocysteine levels, show that the use of 100 mg vitamin B6 plus 5 mg folic acid decreases homocysteine levels by about 50%. Vitamin B6 as a single agent in doses from 100 to 250 mg daily resulted in a slightly lower reduction of about 40%. Folic acid as the sole therapy has been studied in only six patients so far and showed a 45% decrease in these patients. The efficacy of lower doses of vitamin B6 and/or folic acid as a single or combined therapy has not been explored. Remarkably, only the combination of vitamin B6 plus folic acid resulted in normalisation of post-methionine homocysteine levels in 90% or more of the treated patients, whereas the respective single treatments did much less, ie, about 50% (box 5). In summary, 100 mg vitamin B6 and 5 mg folic acid daily should be prescibed for the treatment of post-methionine hyperhomocysteinaemia. Conclusions The prevalence of mild hyperhomocysteinemia in young patients with arterial occlusive disease is high and hyperhomocysteinaemia has to be accepted as a serious risk factor for vascular disease. Future studies will hopefully elucidate in which way atherosclerosis and thromboembolic events are induced in patients with hyperhomocysteinaemia. Furthermore, simple and inexpensive therapy with innocuous vitamins can normalise homocysteine metabolism, as assessed by the homocysteine plasma level before and after methionine loading, in virtually all these patients. Intervention studies are needed to clarify if such treatment will also reduce morbidity and mortality. The demonstration of a clinical benefit of homocysteine-lowering interventions would be required to
6 518 van den Berg, Boers 1 Mudd SH, Levy HL, Skovby F. Disorders of transsulfuration. In: Scriver CR, Beaudet AL, Sly WS, Valle D, eds. The metabolic and molecular basis of inherited disease. New York: McGraw- Hill, 1995; pp Mudd SH, Skovby F, Levy HL, et al. The natural history of homocystinuria due to cystathionine-synthase deficiency. Am 7 Hum Genet 1985; 37: Ueland PM, Refsum H, Brattstrom L. Plasma homocysteine and cardiovascular disease. In: Francis RB Jr, ed. Atherosclerotic cardiovascular disease, hemostasis, and endothelial function. New York: Marcel Dekker, 1992; pp van den Berg M, Franken DG, Boers GHJ, et al. Combined vitamin B6 plus folic acid therapy in young patients with arteriosclerosis and hyperhomocysteinemia. 7 Vasc Surg 1994; 20: Franken DG, Boers GHJ, Blom HJ, et al. Treatment of mild hyperhomocysteinaemia in vascular patients. Arterioscler Thromb 1994; 14: Stampfer MJ, Malinow MR, Willett WC, et al. A prospective study of plasma homocyst(e)ine and risk of myocardial infarction in US physicians. JAAMA 1992; 268: Arnesen E, Refsum H, Bonaa KH, et al. The Tromso study: serum total homocysteine and myocardial infarction, a prospective study. In: Abstracts, 3rd International Conference on Preventive Cardiology. Oslo 1993; p78. 8 van den Berg M, Boers GHJ, Franken DG, et al. Hyperhomocysteinaemia and endothelial dysfunction in young patients with peripheral occlusive disease. Eur 7 Clin Invest 1995; 25: Malinow MR. Homocyst(e)ine and arterial occlusive diseases. 7 Intern Med 1994; 236: Bostom AG, Jacques PF, Nadeau MR, et al. Post-methionine load hyperhomocysteinaemia in persons with normal fasting total plasma homocysteine: initial results from the NHLBI family heart study. Atherosclerosis 1995; 116: Boers GHJ, van den Berg M, Franken DG. Treatment of mild hyperhomocysteinaemia. In: IH Rosenberg, I Graham, P Ueland, H Refsurn, eds. Homocysteine metabolism, from basic science to dinical medicine. Norwell, USA: Kluwer Academic Publishers, 1996; (in press). 12 Clarke R, Daly L, Robinson K, et al. Hyperhomocysteinemia: an independent risk factor for vascular disease. N Engl I Med 1991; 324: Boers GHJ, Fowler B, Smals AGH, et al. Improved identification of heterozygotes for homocystinuria due to cystathionine synthase deficiency by the combination of methionine loading and enzyme determination in cultured fibroblasts. Hum Genet 1985; 69: Kang SS, Wong PWK, Bock HG, et al. Intermediate hyperhomocysteinemia resulting from compound heterozygosity of methylenetetrahydrofolate reductase mutations. Am J Hum Genet 1991; 48: Kang SS, Wong PWK, Susmano A, et al. Thermolabile methylenetetrahydrofolate reductase: an inherited risk factor for coronary artery disease. Am J Hum Genet 1991; 48: Learning points * mild hyperhomocysteinaemia is a risk factor for atherosclerotic disease and venous thrombosis * a methionine loading test is recommended for the diagnosis of hyperhomocysteinaemia in the individual patient * in the case of an abnormal test result, treatment with vitamins involved in homocysteine metabolism should be considered Box 6 justify routine screening for this risk factor on a large scale. Meanwhile, to clarify the individual patient's risk of developing atherosclerosis or thromboembolic events, it is advisable to perform a methionine loading test for the screening of hyperhomocysteinaemia, at least in those cases in which conventional risk factors are absent (box 6). 16 Selhub J, Jacques PF, Wilson PWF, Rush D, Rosenberg IH. Vitamin status and intake as primary determinants of homocysteine in elderly patients. JAMA 1993; 270: Shin HK, Linkswiler HM. Tryptophan and methionine metabolism of adult females as affected by vitamin B-6 deficiency. J Nutr 1974; 104: Miller JW, Ribaya-Mercado JD, Russell RM, et al. Effect of vitamin B-6 deficiency on fasting plasma homocysteine concentrations. Am J7 Clin Nutr 1992; 55: Brattstrom I, Israelsson B, Norrving B, et al. Impaired homocysteine metabolism in earlyonset cerebral and peripheral occlusive arterial disease. Effects of pyridoxine and folic acid treatment. Atherosclerosis 1990; 81: Ueland PM, Refsum H. Plasma homocysteine, a risk factor for vascular disease plasma levels in health, disease, and drug therapy. _J Lab Clin Med 1989;114: Hultberg B, Agardh E, Andersson A, et al. Increased levels of plasma homocysteine are associated with nephropathy, but not severe retinopathy in type 1 diabetes mellitus. Scand J7 Clin Lab Invest 1991; 51: Agardh CD, Agardh E, Andersson A, et al. Lack of association between plasma homocysteine levels and microangiopathy in type 1 diabetes mellitus. ScandJ7 Clin Lab Invest 1994; 54: Guttormsen AB, Schneede J, Fiskerstrand T, et al. Plasma concentrations of homocysteine and other amino compounds are related to food intake in healthy human subjects. J Nutr 1994; 124: Refsum H, Ueland PM. Clinical significance of pharmacological modulation of homocysteine metabolism. Trends Pharmacol Sci 1990; 11: Wilcken DEL, Wilcken B. The pathogenesis of coronary artery disease. A possible role for methionine metabolism. J Clin Invest 1976; 57: Boers GHJ. Hyperhomocysteinaemia: a newly recognized risk factor for vascular disease. Neth J Med 1994; 45: Verhoef P, Hennekens CH, Malinow R, et al. A prospective study of plasma homocyst(e)ine and risk of ischemic stroke. Stroke 1994; 25: Taylor LM, DeFrang RD, Harris EJ, et al. The association of elevated plasma homocyst(e)ine with progression of symptomatic peripheral arterial disease. J Vasc Surg 1991; 13: von Eckardstein A, Malinow MR, Upson B, et al. Effects of age, lipoproteins, and hemostatic parameters on the role of homocyst(e)inemia as a cardiovascular risk factor in men. Arterioscler Thromb 1994; 14: Malinow MR, Nieto FJ, Szklo M, et al. Carotid artery intimal-medial wall thickening and plasma homocyst(e)ine in asymptomatic adults: the Atherosclerosis Risk in Communities Study. Circulation 1993; 87: Selhub J, Jacques PF, Bostom AG, et al. Association between plasma homocysteine concentrations and extracranial carotid-artery stenosis. N Engl J7 Med 1995; 332: den Heijer M, Blom HJ, Gerrits WBJ, et al. Is hyperhomocysteinaemia a risk factor for recurrent venous thrombosis? Lancet 1995; 345: Molgaard J, Malinow MR, Lassvik C, et al. Hyperhomocyst(e)inaemia: an independent risk factor for intermittent claudication. Jf Intern Med Res 1992; 231: Starkebaum G, Harlan JM. Endothelial cell injury due to copper-catalyzed hydrogen peroxide generation from homocysteine. J Clin Invest 1986; 77: Stamler JS, Osborne JA, Jaraki A. Adverse vascular effects of homocysteine are modulated by endothelium-derived relaxing factor and related oxides of nitrogen. J Clin Invest 1993; 91: Harker LA, Slichter SJ, Scott CR, et al. Homocystinemia. Vascular injury and arterial thrombosis. NEnglJMed 1974; 291: Harker LA, Ross R, Slichter SJ, Scott CR. Homocysteine-induced atherosclerosis. The role of endothelial cell injury and platelet response in its genesis. J Clin Invest 1976; 58: de Groot PG, Willems C, Boers GHJ, et al Endothelial cell dysfunction in homocystinuria. Eur _J Clin Invest 1983;13: Tsai J-C, Perrella MA, Yoshizumi M, et al. Promotion of vascular smooth muscle cell growth by homocysteine: a link to atherosclerosis. Proc Nadl Acad Sci USA 1994; 91: Lentz SR, Sadler JE. Inhibition of thrombomodulin surfase expression and protein C activation by the thrombogenetic agent homocysteine. J Clin Invest 1993; 91: Sardharwalla IB, Fowler B, Robins AJ, et al. Detection of heterozygotes for homocystinuria. Arch Dis Child 1974; 49: Engbersen AMT, Blom HJ, Franken DG, et al. Thermolabile 5, 10-methylenetetrahydrofolate reductase as the cause of mild hyperhomocysteinemia. Am J Hum Genet 1995; 56: Whitehead AS, Ward P, Tan S, et al. The molecular genetics of homocystinuria, hyperhomocysteinaemia, and premature vascular disease in Ireland. In: Mato JM, Caballero A, eds. Methionine metabolism: molecular mechanisms and clinical implications. Madrid: CSIC, 1994; pp Kozich V, Kraus E, de Franchis R, et al. Hyperhomocysteineamia in premature arterial disease: examination of cystathionine B-synthase alleles at the molecular level. Hum Molec Genet 1995; 4: Goyette, Sumner JS, Milos R, et al. Human methylenetetrahydrofolate reductase: isolation of cdna, mapping and mutation identification. Nat Genet 1994; 7: Frosst P, Blom HJ, Milos R, et al. A candidate genetic risk factor for vascular disease: a common mutation in methylenetetrahydrofolate reductase. Nat Genet 1995; 10:
Serum Total Homocysteine and Coronary Heart Disease
 International Journal of Epidemiology O International Eptctemlotoglcal Association 1995 Vol. 24, No. 4 Printed In Great Britain Serum Total Homocysteine and Coronary Heart Disease EGIL ARNESEN,* HELGA
International Journal of Epidemiology O International Eptctemlotoglcal Association 1995 Vol. 24, No. 4 Printed In Great Britain Serum Total Homocysteine and Coronary Heart Disease EGIL ARNESEN,* HELGA
METHYLENETETRAHYDROFOLATE REDUCTASE GENE AMONG THE JAPANESE
 Jpn J Human Genet 41, 247 251, 1996 Short Communication A COMMON MUTATION IN METHYLENETETRAHYDROFOLATE REDUCTASE GENE AMONG THE JAPANESE POPULATION Hisahide NISHIO, L* Myeong Jin LEE, ~ Motoko FuJlI, 1
Jpn J Human Genet 41, 247 251, 1996 Short Communication A COMMON MUTATION IN METHYLENETETRAHYDROFOLATE REDUCTASE GENE AMONG THE JAPANESE POPULATION Hisahide NISHIO, L* Myeong Jin LEE, ~ Motoko FuJlI, 1
Hyperhomocysteinemia is known to be an. Methylenetetrahydrofolate Reductase Gene Polymorphism. Relation to Blood Pressure and Cerebrovascular Disease
 AJH 1998;11:1019 1023 BRIEF COMMUNICATIONS Methylenetetrahydrofolate Reductase Gene Polymorphism Relation to Blood Pressure and Cerebrovascular Disease Yukiko Nakata, Tomohiro Katsuya, Seiju Takami, Noriyuki
AJH 1998;11:1019 1023 BRIEF COMMUNICATIONS Methylenetetrahydrofolate Reductase Gene Polymorphism Relation to Blood Pressure and Cerebrovascular Disease Yukiko Nakata, Tomohiro Katsuya, Seiju Takami, Noriyuki
Homocysteine is an amino acid produced as an intermediate
 CLINICAL REVIEW Homocysteine and Vascular Disease Christopher A. Friedrich, MD, PhD, and Daniel J. Rader, MD Homocysteine is an amino acid produced as an intermediate product in the metabolism of methionine,
CLINICAL REVIEW Homocysteine and Vascular Disease Christopher A. Friedrich, MD, PhD, and Daniel J. Rader, MD Homocysteine is an amino acid produced as an intermediate product in the metabolism of methionine,
REVIEW ARTICLE. Blood Levels of Homocysteine and Increased Risks of Cardiovascular Disease
 Blood Levels of Homocysteine and Increased Risks of Cardiovascular Disease Causal or Casual? REVIEW ARTICLE William G. Christen, ScD; Umed A. Ajani, MBBS; Robert J. Glynn, ScD; Charles H. Hennekens, MD
Blood Levels of Homocysteine and Increased Risks of Cardiovascular Disease Causal or Casual? REVIEW ARTICLE William G. Christen, ScD; Umed A. Ajani, MBBS; Robert J. Glynn, ScD; Charles H. Hennekens, MD
HOMOCYSTEINE METABOLISM
 Annu. Rev. Nutr. 1999. 19:217 46 Copyright c 1999 by Annual Reviews. All rights reserved HOMOCYSTEINE METABOLISM J. Selhub Jean Mayer USDA Human Nutrition Research Center on Aging, Tufts University, Boston,
Annu. Rev. Nutr. 1999. 19:217 46 Copyright c 1999 by Annual Reviews. All rights reserved HOMOCYSTEINE METABOLISM J. Selhub Jean Mayer USDA Human Nutrition Research Center on Aging, Tufts University, Boston,
Classic homocystinuria, due to homozygosity for
 465 Treatment of Mild Hyperhomocysteinemia in Vascular Disease Patients Diana G. Franken, Godfried H.J. Boers, Henk J. Blom, Frans J.M. Trijbels, Peter W.C. Kloppenborg Abstract Mild hyperhomocysteinemia
465 Treatment of Mild Hyperhomocysteinemia in Vascular Disease Patients Diana G. Franken, Godfried H.J. Boers, Henk J. Blom, Frans J.M. Trijbels, Peter W.C. Kloppenborg Abstract Mild hyperhomocysteinemia
Hyperhomocysteinaemia A Risk Factor Worth Considering
 REVIEW ARTICLE JIACM 2003; 4(2): 147-51 Hyperhomocysteinaemia A Risk Factor Worth Considering Pramood C Kalikiri* At least nine well-known risk factors are known to play a role in the development of coronary
REVIEW ARTICLE JIACM 2003; 4(2): 147-51 Hyperhomocysteinaemia A Risk Factor Worth Considering Pramood C Kalikiri* At least nine well-known risk factors are known to play a role in the development of coronary
Plasma homocysteine concentrations in a Belgian school-age population 1 3
 Plasma homocysteine concentrations in a Belgian school-age population 1 3 Corinne De Laet, Jean-Claude Wautrecht, Daniel Brasseur, Michèle Dramaix, Jean-Marie Boeynaems, Jean Decuyper, and André Kahn ABSTRACT
Plasma homocysteine concentrations in a Belgian school-age population 1 3 Corinne De Laet, Jean-Claude Wautrecht, Daniel Brasseur, Michèle Dramaix, Jean-Marie Boeynaems, Jean Decuyper, and André Kahn ABSTRACT
Protein-bound Homocyst(e)ine A Possible Risk Factor for Coronary Artery Disease
 Protein-bound Homocyst(e)ine A Possible Risk Factor for Coronary Artery Disease Soo-Sang Kang, Paul W. K. Wong, Heron Y. Cook, Marija Norusis, and Joseph V. Messer Departments ofpediatrics, Preventive
Protein-bound Homocyst(e)ine A Possible Risk Factor for Coronary Artery Disease Soo-Sang Kang, Paul W. K. Wong, Heron Y. Cook, Marija Norusis, and Joseph V. Messer Departments ofpediatrics, Preventive
CBS Deficient Homocystinuria.
 CBS Deficient Homocystinuria. Kenneth N. Maclean PhD University of Colorado School of Medicine Department of Pediatrics The methionine cycle Alternative metabolic fates for Hcy Extrusion into the extracellular
CBS Deficient Homocystinuria. Kenneth N. Maclean PhD University of Colorado School of Medicine Department of Pediatrics The methionine cycle Alternative metabolic fates for Hcy Extrusion into the extracellular
HOMOCYSTEINE AND CARDIOVASCULAR DISEASE
 Annu. Rev. Medicine 1998. 49:31 62 Copyright 1998 by Annual Reviews Inc. All rights reserved HOMOCYSTEINE AND CARDIOVASCULAR DISEASE H. Refsum, MD and P. M. Ueland, MD Department of Pharmacology, University
Annu. Rev. Medicine 1998. 49:31 62 Copyright 1998 by Annual Reviews Inc. All rights reserved HOMOCYSTEINE AND CARDIOVASCULAR DISEASE H. Refsum, MD and P. M. Ueland, MD Department of Pharmacology, University
Methylene Tetrahydrofolate Reductase Gene and Coronary Artery Disease
 Methylene Tetrahydrofolate Reductase Gene and Coronary Artery Disease M. P. Iqbal,P. M. Frossard ( Department of Biological and Biomedical Sciences, The Aga Khan University, Karachi. ) Hyperhomocysteinemia
Methylene Tetrahydrofolate Reductase Gene and Coronary Artery Disease M. P. Iqbal,P. M. Frossard ( Department of Biological and Biomedical Sciences, The Aga Khan University, Karachi. ) Hyperhomocysteinemia
In spite of the large number of reports showing. review Haematologica 1997; 82:
 review Haematologica 1997; 82:211-219 Advances in Basic, Laboratory and Clinical Aspects of Thromboembolic Diseases* HYPERHOMOCYSTEINEMIA AND VENOUS THROMBOEMBOLIC DISEASE ARMANDO D ANGELO, GIUSEPPINA
review Haematologica 1997; 82:211-219 Advances in Basic, Laboratory and Clinical Aspects of Thromboembolic Diseases* HYPERHOMOCYSTEINEMIA AND VENOUS THROMBOEMBOLIC DISEASE ARMANDO D ANGELO, GIUSEPPINA
International Journal of Current Research in Medical Sciences
 International Journal of Current Research in Medical Sciences ISSN: 2454-5716 www.ijcrims.com Coden: IJCRPP(USA) Research Article http://s-o-i.org/1.15/ijcrms-2016-2-1-5 How Raised Homocysteine is Correlated
International Journal of Current Research in Medical Sciences ISSN: 2454-5716 www.ijcrims.com Coden: IJCRPP(USA) Research Article http://s-o-i.org/1.15/ijcrms-2016-2-1-5 How Raised Homocysteine is Correlated
Impaired Homocysteine Metabolism and Atherothrombotic Disease. Philippe Durand, Michel Prost, Nadine Loreau, Suzanne Lussier-Cacan, and Denis Blache
 0023-6837/01/8105-645$03.00/0 LABORATORY INVESTIGATION Vol. 81, No. 5, p. 645, 2001 Copyright 2001 by The United States and Canadian Academy of Pathology, Inc. Printed in U.S.A. MINIREVIEW Impaired Homocysteine
0023-6837/01/8105-645$03.00/0 LABORATORY INVESTIGATION Vol. 81, No. 5, p. 645, 2001 Copyright 2001 by The United States and Canadian Academy of Pathology, Inc. Printed in U.S.A. MINIREVIEW Impaired Homocysteine
Hyperhomocysteinaemia and premature coronary artery disease in the Chinese
 Heart 1996;76:117-122 Department of Chemical Pathology, The Chinese University of Hong Kong, Prince of Wales Hospital, Hong Kong Y I Lolin S K Cheng C F Chan C P Pang J R L Masarei Department of Medicine,
Heart 1996;76:117-122 Department of Chemical Pathology, The Chinese University of Hong Kong, Prince of Wales Hospital, Hong Kong Y I Lolin S K Cheng C F Chan C P Pang J R L Masarei Department of Medicine,
Prospective blinded study of the relationship between plasma homocysteine and progression of symptomatic peripheral arterial disease
 Prospective blinded study of the relationship between plasma homocysteine and progression of symptomatic peripheral arterial disease Lloyd M. Taylor, Jr, MD, Gregory L. Moneta, MD, Gary J. Sexton, PhD,
Prospective blinded study of the relationship between plasma homocysteine and progression of symptomatic peripheral arterial disease Lloyd M. Taylor, Jr, MD, Gregory L. Moneta, MD, Gary J. Sexton, PhD,
Review Article. Mechanisms of Disease
 Review Article Mechanisms of Disease F RANKLIN H. EPSTEIN, M.D., Editor HMCYSTEINE AND ATHERTHRMBSIS GERGE N. WELCH, M.D., AND JSEPH LSCALZ, M.D., PH.D. IN 1969, McCully made the clinical observation linking
Review Article Mechanisms of Disease F RANKLIN H. EPSTEIN, M.D., Editor HMCYSTEINE AND ATHERTHRMBSIS GERGE N. WELCH, M.D., AND JSEPH LSCALZ, M.D., PH.D. IN 1969, McCully made the clinical observation linking
Clinical Policy: Homocysteine Testing Reference Number: CP.MP.121
 Clinical Policy: Reference Number: CP.MP.121 Effective Date: 08/16 Last Review Date: 08/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.121 Effective Date: 08/16 Last Review Date: 08/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Importance of Elevated Plasma Homocysteine Levels as a Risk Factor for Atherosclerosis
 Importance of Elevated Plasma Homocysteine Levels as a Risk Factor for Atherosclerosis Philippe A. Masser, MD, Lloyd M. Taylor, Jr, MD, and John M. Porter, MD Division of Vascular Surgery, Oregon Health
Importance of Elevated Plasma Homocysteine Levels as a Risk Factor for Atherosclerosis Philippe A. Masser, MD, Lloyd M. Taylor, Jr, MD, and John M. Porter, MD Division of Vascular Surgery, Oregon Health
Nitrous Oxide induced Elevation of Plasma Homocysteine and Methylmalonic Acid Levels and their Clinical Implications
 SHORT COMMUNICATION JIACM 2005; 6(1): 48-52 Abstract Nitrous Oxide induced Elevation of Plasma Homocysteine and Methylmalonic Acid Levels and their Clinical Implications Pramood C Kalikiri*, Reena G Sachan*
SHORT COMMUNICATION JIACM 2005; 6(1): 48-52 Abstract Nitrous Oxide induced Elevation of Plasma Homocysteine and Methylmalonic Acid Levels and their Clinical Implications Pramood C Kalikiri*, Reena G Sachan*
HOMOCYSTEINE (H(e)) is a nonprotein-forming, thiolcontaining
 0163-769X/99/$03.00/0 Endocrine Reviews 20(5): 738 759 Copyright 1999 by The Endocrine Society Printed in U.S.A. Hyperhomocysteinemia and the Endocrine System: Implications for Atherosclerosis and Thrombosis
0163-769X/99/$03.00/0 Endocrine Reviews 20(5): 738 759 Copyright 1999 by The Endocrine Society Printed in U.S.A. Hyperhomocysteinemia and the Endocrine System: Implications for Atherosclerosis and Thrombosis
ORIGINAL INVESTIGATION. Homocysteine and Ischemic Heart Disease. Results of a Prospective Study With Implications Regarding Prevention
 ORIGINAL INVESTIGATION Homocysteine and Ischemic Heart Disease Results of a Prospective Study With Implications Regarding Prevention Nicholas J. Wald, DSc (Med), FRCP; Hilary C. Watt, MSc; Malcolm R. Law,
ORIGINAL INVESTIGATION Homocysteine and Ischemic Heart Disease Results of a Prospective Study With Implications Regarding Prevention Nicholas J. Wald, DSc (Med), FRCP; Hilary C. Watt, MSc; Malcolm R. Law,
The methylenetetrahydrofolate reductase gene is associated with increased cardiovascular risk in Japan, but not in other populations
 Atherosclerosis 153 (2000) 161 168 www.elsevier.com/locate/atherosclerosis The methylenetetrahydrofolate reductase gene is associated with increased cardiovascular risk in Japan, but not in other populations
Atherosclerosis 153 (2000) 161 168 www.elsevier.com/locate/atherosclerosis The methylenetetrahydrofolate reductase gene is associated with increased cardiovascular risk in Japan, but not in other populations
Interrelation of Hyperhomocyst(e)inemia, Factor V Leiden, and Risk of Future Venous Thromboembolism
 (Circulation. 1997;95:1777-1782.) 1997 American Heart Association, Inc. Interrelation of Hyperhomocyst(e)inemia, Factor V Leiden, and Risk of Future Venous Thromboembolism Paul M. Ridker, MD; Charles H.
(Circulation. 1997;95:1777-1782.) 1997 American Heart Association, Inc. Interrelation of Hyperhomocyst(e)inemia, Factor V Leiden, and Risk of Future Venous Thromboembolism Paul M. Ridker, MD; Charles H.
Homocysteine and thiol metabolites in vitamin B 12 deficiency
 Clinical Science (2001) 100, 111 116 (Printed in Great Britain) 111 Homocysteine and thiol metabolites in vitamin B 12 deficiency L. R. RANGANATH*, M. BAINES and N. B. ROBERTS *Department of Chemical Pathology,
Clinical Science (2001) 100, 111 116 (Printed in Great Britain) 111 Homocysteine and thiol metabolites in vitamin B 12 deficiency L. R. RANGANATH*, M. BAINES and N. B. ROBERTS *Department of Chemical Pathology,
Relationship of Total Homocysteine, Cholesterol, Triglyceride in the Serum and Diastolic Blood Pressure of Patients with Myocardial Infarction
 Relationship of Total Homocysteine, Cholesterol, Triglyceride in the Serum and Diastolic Blood Pressure of Patients with Myocardial Infarction Durdi Qujeq *1, Laia Hossini 1 and M. Taghi Salehi Omran 2
Relationship of Total Homocysteine, Cholesterol, Triglyceride in the Serum and Diastolic Blood Pressure of Patients with Myocardial Infarction Durdi Qujeq *1, Laia Hossini 1 and M. Taghi Salehi Omran 2
Association between Plasma Homocysteine Concentrations and Carotid Intima-Media Thickness in Patients with Coronary Artery Disease
 Association between Plasma Homocysteine Concentrations and Carotid Intima-Media Thickness in Patients with Coronary Artery Disease ROXANA BUZAŞ, CORINA ŞERBAN, IOANA SUCEAVA, DANIEL LIGHEZAN University
Association between Plasma Homocysteine Concentrations and Carotid Intima-Media Thickness in Patients with Coronary Artery Disease ROXANA BUZAŞ, CORINA ŞERBAN, IOANA SUCEAVA, DANIEL LIGHEZAN University
Metabolism of. Sulfur Containing Amino Acids
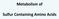 Metabolism of Sulfur Containing Amino Acids Methionine S CH 3 CH 2 cysteine CH 2 SH CH 2 CHNH 2 COOH CHNH 2 COOH Essential amino acid Non-polar amio acid Glucogenic amino acid Methionine IMPORTANCE: As
Metabolism of Sulfur Containing Amino Acids Methionine S CH 3 CH 2 cysteine CH 2 SH CH 2 CHNH 2 COOH CHNH 2 COOH Essential amino acid Non-polar amio acid Glucogenic amino acid Methionine IMPORTANCE: As
Abundant evidence has accumulated supporting the association
 Folate, Vitamin B 6, and B 12 Intakes in Relation to Risk of Stroke Among Men Ka He, MD; Anwar Merchant, DMD; Eric B. Rimm, ScD; Bernard A. Rosner, PhD; Meir J. Stampfer, MD; Walter C. Willett, MD; Alberto
Folate, Vitamin B 6, and B 12 Intakes in Relation to Risk of Stroke Among Men Ka He, MD; Anwar Merchant, DMD; Eric B. Rimm, ScD; Bernard A. Rosner, PhD; Meir J. Stampfer, MD; Walter C. Willett, MD; Alberto
This review is contributed by Professor Helene McNulty RD and Dr Mary Ward RD from the University of Ulster, Northern Ireland.
 1.1.1 Folate This review is contributed by Professor Helene McNulty RD and Dr Mary Ward RD from the University of Ulster, Northern Ireland. 1.1.1.1 Summary In recent years there has been much interest
1.1.1 Folate This review is contributed by Professor Helene McNulty RD and Dr Mary Ward RD from the University of Ulster, Northern Ireland. 1.1.1.1 Summary In recent years there has been much interest
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/25097
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/25097
Independent Risk Factors of Cardiovascular Disease Achieving Healthy Homocysteine Levels
 Independent Risk Factors of Cardiovascular Disease Achieving Healthy Homocysteine Levels AUTHORS: JON LEGERE, BRADLEY RALPH, DR. RON LEGERE 15344 N 83RD WAY, SCOTTSDALE, AZ 85260 TEL: 800.528.3144 EMAIL:
Independent Risk Factors of Cardiovascular Disease Achieving Healthy Homocysteine Levels AUTHORS: JON LEGERE, BRADLEY RALPH, DR. RON LEGERE 15344 N 83RD WAY, SCOTTSDALE, AZ 85260 TEL: 800.528.3144 EMAIL:
Determinants and Vitamin Responsiveness of Intermediate Hyperhomocysteinemia ( 40 mol/liter)
 Determinants and Vitamin Responsiveness of Intermediate Hyperhomocysteinemia ( 40 mol/liter) The Hordaland Homocysteine Study Anne Berit Guttormsen,* Per Magne Ueland,* Ingerid Nesthus, Ottar Nygård, Jörn
Determinants and Vitamin Responsiveness of Intermediate Hyperhomocysteinemia ( 40 mol/liter) The Hordaland Homocysteine Study Anne Berit Guttormsen,* Per Magne Ueland,* Ingerid Nesthus, Ottar Nygård, Jörn
P H Whincup, H Refsum, I J Perry, R Morris, M Walker, L Lennon, A Thomson, P M Ueland, S B J Ebrahim
 448 Cardiovascular Research Unit, Department of Primary Care and Population Sciences, Royal Free Hospital School of Medicine, London NW3 2PF, UK P H Whincup R Morris M Walker L Lennon A Thomson S B J Ebrahim
448 Cardiovascular Research Unit, Department of Primary Care and Population Sciences, Royal Free Hospital School of Medicine, London NW3 2PF, UK P H Whincup R Morris M Walker L Lennon A Thomson S B J Ebrahim
in a population with low plasma
 518 Cardiology, Hacettepe University Faculty of Medicine, Ankara 06100, Turkey S L Tokgözoğlu E Atalar K Aytemir N Özer K Övünç S Kes Paediatric Genetics, Hacettepe University Faculty of Medicine M Alikaşifoğlu
518 Cardiology, Hacettepe University Faculty of Medicine, Ankara 06100, Turkey S L Tokgözoğlu E Atalar K Aytemir N Özer K Övünç S Kes Paediatric Genetics, Hacettepe University Faculty of Medicine M Alikaşifoğlu
Homocysteine, Vitamins, and Prevention of Vascular Disease
 MILITARY MEDICINE, 169, 4:325, 2004 Homocysteine, Vitamins, and Prevention of Vascular Disease Guarantor: Kilmer S. McCully, MD Contributor: Kilmer S. McCully, MD Within the past four decades, the efforts
MILITARY MEDICINE, 169, 4:325, 2004 Homocysteine, Vitamins, and Prevention of Vascular Disease Guarantor: Kilmer S. McCully, MD Contributor: Kilmer S. McCully, MD Within the past four decades, the efforts
The Effect of a Subnormal Vitamin B-6 Status on Homocysteine Metabolism
 The Effect of a Subnormal Vitamin B-6 Status on Homocysteine Metabolism Johan B. Ubbink,* Annatjie van der Merwe,* Rhena Delport,* Robert H. Allen, Sally P. Stabler, Reiner Riezler, and Vermaak* *Department
The Effect of a Subnormal Vitamin B-6 Status on Homocysteine Metabolism Johan B. Ubbink,* Annatjie van der Merwe,* Rhena Delport,* Robert H. Allen, Sally P. Stabler, Reiner Riezler, and Vermaak* *Department
Nitrous Oxide Induced Elevation Of Plasma Homocysteine And Methylmalonic Acid Levels And Their Clinical Implications
 ISPUB.COM The Internet Journal of Anesthesiology Volume 8 Number 2 Nitrous Oxide Induced Elevation Of Plasma Homocysteine And Methylmalonic Acid Levels And Their Clinical Implications P Kalikiri, R Sachan
ISPUB.COM The Internet Journal of Anesthesiology Volume 8 Number 2 Nitrous Oxide Induced Elevation Of Plasma Homocysteine And Methylmalonic Acid Levels And Their Clinical Implications P Kalikiri, R Sachan
Asubstantial body of evidence from observational epidemiological
 Effect of Dietary Patterns on Serum Homocysteine Results of a Randomized, Controlled Feeding Study Lawrence J. Appel, MD, MPH; Edgar R. Miller III, MD, PhD; Sun Ha Jee, PhD; Rachael Stolzenberg-Solomon,
Effect of Dietary Patterns on Serum Homocysteine Results of a Randomized, Controlled Feeding Study Lawrence J. Appel, MD, MPH; Edgar R. Miller III, MD, PhD; Sun Ha Jee, PhD; Rachael Stolzenberg-Solomon,
CLINICAL CHEMISTRY Review Article. 1985, Boers 12 described accelerated vascular disease associmature
 CLINICAL CHEMISTRY Review Article H y p e r h o m o c y s t e i n e m i a An Emerging and Important Risk Factor for Thromboembolic and Cardiovascular Disease SUSAN C. GUBA, MD, 1 " 3 LOUIS M. FINK, MD,"
CLINICAL CHEMISTRY Review Article H y p e r h o m o c y s t e i n e m i a An Emerging and Important Risk Factor for Thromboembolic and Cardiovascular Disease SUSAN C. GUBA, MD, 1 " 3 LOUIS M. FINK, MD,"
The Molecular Basis of Cystathionine
 Am. J. Hum. Genet. 65:59 67, 1999 The Molecular Basis of Cystathionine b-synthase Deficiency in Dutch Patients with Homocystinuria: Effect of CBS Genotype on Biochemical and Clinical Phenotype and on Response
Am. J. Hum. Genet. 65:59 67, 1999 The Molecular Basis of Cystathionine b-synthase Deficiency in Dutch Patients with Homocystinuria: Effect of CBS Genotype on Biochemical and Clinical Phenotype and on Response
Clinical Importance of MTHFR Gene Polymorphism in Coronary Artery Disease: A Study from India
 Human Journals Research Article September 2018 Vol.:13, Issue:2 All rights are reserved by Alpana Saxena et al. Clinical Importance of MTHFR Gene Polymorphism in Coronary Artery Disease: A Study from India
Human Journals Research Article September 2018 Vol.:13, Issue:2 All rights are reserved by Alpana Saxena et al. Clinical Importance of MTHFR Gene Polymorphism in Coronary Artery Disease: A Study from India
Homocysteine and ischaemic stroke in men: the Caerphilly study
 J Epidemiol Community Health 2001;55:91 96 91 Homocysteine and ischaemic stroke in men: the Caerphilly study U B Fallon, P Elwood, Y Ben-Shlomo, J B Ubbink, R Greenwood, G Davey Smith Department of Social
J Epidemiol Community Health 2001;55:91 96 91 Homocysteine and ischaemic stroke in men: the Caerphilly study U B Fallon, P Elwood, Y Ben-Shlomo, J B Ubbink, R Greenwood, G Davey Smith Department of Social
Correspondence should be addressed to: Jelena Paovic; Received date: 23 April 2014; Accepted date: 7 July 2014; Published date: 8 June 2015
 IBIMA Publishing Research in Immunology: An International Journal http://www.ibimapublishing.com/journals/immu/immu.html Vol. 2015 (2015), Article ID 246396, 11 pages DOI: 10.5171/2015.246396 Research
IBIMA Publishing Research in Immunology: An International Journal http://www.ibimapublishing.com/journals/immu/immu.html Vol. 2015 (2015), Article ID 246396, 11 pages DOI: 10.5171/2015.246396 Research
One third to one half of the variation in vascular disease
 Plasma Homocysteine Predicts Mortality Independently of Traditional Risk Factors and C-Reactive Protein in Patients With Angiographically Defined Coronary Artery Disease Jeffrey L. Anderson, MD; Joseph
Plasma Homocysteine Predicts Mortality Independently of Traditional Risk Factors and C-Reactive Protein in Patients With Angiographically Defined Coronary Artery Disease Jeffrey L. Anderson, MD; Joseph
MTHFR gene polymorphism, homocysteine and cardiovascular disease
 Public Health Nutrition: 4(2B), 493±497 DOI: 10.1079/PHN2001159 MTHFR gene polymorphism, homocysteine and cardiovascular disease Claudio Cortese 1 * and Corradino Motti 2 1 Department of Internal Medicine,
Public Health Nutrition: 4(2B), 493±497 DOI: 10.1079/PHN2001159 MTHFR gene polymorphism, homocysteine and cardiovascular disease Claudio Cortese 1 * and Corradino Motti 2 1 Department of Internal Medicine,
Homocyst(e)ine and Coronary Heart Disease Pharmacoeconomic Support for Interventions to Lower Hyperhomocyst(e)inaemia
 REVIEW ARTICLE Pharmacoeconomics 2002; 20 (7): 429-442 1170-7690/02/0007-0429/$25.00/0 Adis International Limited. All rights reserved. Homocyst(e)ine and Coronary Heart Disease Pharmacoeconomic Support
REVIEW ARTICLE Pharmacoeconomics 2002; 20 (7): 429-442 1170-7690/02/0007-0429/$25.00/0 Adis International Limited. All rights reserved. Homocyst(e)ine and Coronary Heart Disease Pharmacoeconomic Support
High Blood Pressure in Irish Adults
 High Blood Pressure in Irish Adults Preliminary findings and lessons learned from two JINGO cohorts Helene McNulty Northern Ireland Centre for Food and Health (NICHE) University of Ulster Mortality due
High Blood Pressure in Irish Adults Preliminary findings and lessons learned from two JINGO cohorts Helene McNulty Northern Ireland Centre for Food and Health (NICHE) University of Ulster Mortality due
The Role of Homocysteine in Human Health
 K.J. McLaughlin, B.P.E., B.Sc., D.C., MA.Sc., R.N.C. 1 Introduction For the last two decades, the Modus Operandi of most health care providers managing their patients with atherosclerosis was to prescribe
K.J. McLaughlin, B.P.E., B.Sc., D.C., MA.Sc., R.N.C. 1 Introduction For the last two decades, the Modus Operandi of most health care providers managing their patients with atherosclerosis was to prescribe
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24050
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24050
Thrombosis. By Dr. Sara Mohamed Abuelgasim
 Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
Hyperhomocystinemia in patients with coronary artery disease
 Brazilian Journal of Medical and Biological Research (2006) 39: 455-463 Hyperhomocystinemia and coronary disease ISSN 0100-879X 455 Hyperhomocystinemia in patients with coronary artery disease J.R. Faria-Neto
Brazilian Journal of Medical and Biological Research (2006) 39: 455-463 Hyperhomocystinemia and coronary disease ISSN 0100-879X 455 Hyperhomocystinemia in patients with coronary artery disease J.R. Faria-Neto
Among the determinants and correlates of total plasma
 Genetic Aspects of Hyperhomocysteinemia in Chronic Kidney Disease Gere Sunder-Plassmann, Wolfgang C. Winkelmayer, and Manuela Födinger Patients with chronic kidney disease who are on dialysis or with a
Genetic Aspects of Hyperhomocysteinemia in Chronic Kidney Disease Gere Sunder-Plassmann, Wolfgang C. Winkelmayer, and Manuela Födinger Patients with chronic kidney disease who are on dialysis or with a
The New England Journal of Medicine PLASMA HOMOCYSTEINE LEVELS AND MORTALITY IN PATIENTS WITH CORONARY ARTERY DISEASE
 PLASMA HOMOCYSTEINE LEVELS AND MORTALITY IN PATIENTS WITH CORONARY ARTERY DISEASE OTTAR NYGÅRD, M.D., JAN ERIK NORDREHAUG, M.D., HELGA REFSUM, M.D., PER MAGNE UELAND, M.D., MIKAEL FARSTAD, M.D., AND STEIN
PLASMA HOMOCYSTEINE LEVELS AND MORTALITY IN PATIENTS WITH CORONARY ARTERY DISEASE OTTAR NYGÅRD, M.D., JAN ERIK NORDREHAUG, M.D., HELGA REFSUM, M.D., PER MAGNE UELAND, M.D., MIKAEL FARSTAD, M.D., AND STEIN
Homocysteine (plasma, urine, dried blood spots)
 Homocysteine (plasma, urine, dried blood spots) 1 Name and description of analyte 1.1 Name of analyte Homocysteine 1.2 Alternative names None 1.3 NLMC code To follow 1.4. Function(s) of analyte Homocysteine
Homocysteine (plasma, urine, dried blood spots) 1 Name and description of analyte 1.1 Name of analyte Homocysteine 1.2 Alternative names None 1.3 NLMC code To follow 1.4. Function(s) of analyte Homocysteine
CardioGenomicPlus Profile
 CardioGenomicPlus Profile Patient: SAMPLE PATIENT DOB: Sex: MRN: Apo E Chromosome 19 APOE APO E2: cys / cys APO E3: cys / arg APO E4: arg / arg The two SNPs lead to 3 possible variants for each chromosome,
CardioGenomicPlus Profile Patient: SAMPLE PATIENT DOB: Sex: MRN: Apo E Chromosome 19 APOE APO E2: cys / cys APO E3: cys / arg APO E4: arg / arg The two SNPs lead to 3 possible variants for each chromosome,
Folate and Vitamin B 6 From Diet and Supplements in Relation to Risk of Coronary Heart Disease Among Women
 Original Contributions Folate and Vitamin B 6 From Diet and Supplements in Relation to Risk of Coronary Heart Disease Among Women Eric B. Rimm, ScD; Walter C. Willett, MD, DrPH; Frank B. Hu, MD, PhD; Laura
Original Contributions Folate and Vitamin B 6 From Diet and Supplements in Relation to Risk of Coronary Heart Disease Among Women Eric B. Rimm, ScD; Walter C. Willett, MD, DrPH; Frank B. Hu, MD, PhD; Laura
Hyperhomocysteinaemia in Black patients with cerebral thrombosis
 Q J Med 1997; 90:635-639 Hyperhomocysteinaemia in Black patients with cerebral thrombosis R. DELPORT 1, J.B. UBBINK\ W.J.H. VERMAAK 1, H. ROSSOUW 1, P.J. BECKER 2 andj. JOUBERT 3 * From the ^Department
Q J Med 1997; 90:635-639 Hyperhomocysteinaemia in Black patients with cerebral thrombosis R. DELPORT 1, J.B. UBBINK\ W.J.H. VERMAAK 1, H. ROSSOUW 1, P.J. BECKER 2 andj. JOUBERT 3 * From the ^Department
Hyperhomocysteinemia is an independent risk factor for. Improved Vascular Endothelial Function After Oral B Vitamins
 Improved Vascular Endothelial Function After Oral B Vitamins An Effect Mediated Through Reduced Concentrations of Free Plasma Homocysteine John C. Chambers, MD; Per M. Ueland, MD; Omar A. Obeid, PhD; Jane
Improved Vascular Endothelial Function After Oral B Vitamins An Effect Mediated Through Reduced Concentrations of Free Plasma Homocysteine John C. Chambers, MD; Per M. Ueland, MD; Omar A. Obeid, PhD; Jane
Non-commercial use only
 Familial hyperhomocysteinemia, age and peripheral vascular diseases - an Italian study Sandro Michelini, 1 Marco Cardone, 1 Adriano Micci, 1 Francesco Cappellino, 1 Alessandro Fiorentino, 1 Vincenzo Sainato,
Familial hyperhomocysteinemia, age and peripheral vascular diseases - an Italian study Sandro Michelini, 1 Marco Cardone, 1 Adriano Micci, 1 Francesco Cappellino, 1 Alessandro Fiorentino, 1 Vincenzo Sainato,
Lipid Markers. Independent Risk Factors. Insulin Resistance Score by Lipid Fractionation
 Patient: SAMPLE PATIENT DOB: Sex: MRN: 3701 CV Health Plus Genomics - Plasma, Serum & Buccal Swab Methodology: Chemiluminescent, Enzymatic, Immunoturbidimetric, NMR and PCR Lipid Markers Cholesterol LDL-
Patient: SAMPLE PATIENT DOB: Sex: MRN: 3701 CV Health Plus Genomics - Plasma, Serum & Buccal Swab Methodology: Chemiluminescent, Enzymatic, Immunoturbidimetric, NMR and PCR Lipid Markers Cholesterol LDL-
REAGENTS. RANDOX sdldl CHOLESTEROL (sdldl-c) SIZE MATTERS: THE TRUE WEIGHT OF RISK IN LIPID PROFILING
 REAGENTS RANDOX sdldl CHOLESTEROL (sdldl-c) SIZE MATTERS: THE TRUE WEIGHT OF RISK IN LIPID PROFILING Randox sdldl Cholesterol (sdldl-c) Size Matters: The True Wight of Risk in Lipid Profiling 1. BACKGROUND
REAGENTS RANDOX sdldl CHOLESTEROL (sdldl-c) SIZE MATTERS: THE TRUE WEIGHT OF RISK IN LIPID PROFILING Randox sdldl Cholesterol (sdldl-c) Size Matters: The True Wight of Risk in Lipid Profiling 1. BACKGROUND
Correlation between Low Folate Levels and Hyperhomocysteinemia, but not with Vitamin B12 in Hypertensive Patients
 286 Available online at www.annclinlabsci.org Correlation between Low Folate Levels and Hyperhomocysteinemia, but not with Vitamin B12 in Hypertensive Patients C. Scazzone 1, A. Bono 1, F. Tornese 2, R.
286 Available online at www.annclinlabsci.org Correlation between Low Folate Levels and Hyperhomocysteinemia, but not with Vitamin B12 in Hypertensive Patients C. Scazzone 1, A. Bono 1, F. Tornese 2, R.
Homocystinuria due to CBS deficiency
 Homocystinuria due to CBS deficiency Introductory information Written by: U. Wendel, P. Burgard & V. Konstantopoulou Reviewed & Revised for North America by: S. van Calcar HCU Homocystinuria Homocystine
Homocystinuria due to CBS deficiency Introductory information Written by: U. Wendel, P. Burgard & V. Konstantopoulou Reviewed & Revised for North America by: S. van Calcar HCU Homocystinuria Homocystine
Homocysteine is a chemical in
 CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Homocysteine and MTHFR Mutations Relation to Thrombosis and Coronary Artery Disease Elizabeth A. Varga, MS; Amy C. Sturm, MS; Caron P. Misita, PharmD; Stephan
CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Homocysteine and MTHFR Mutations Relation to Thrombosis and Coronary Artery Disease Elizabeth A. Varga, MS; Amy C. Sturm, MS; Caron P. Misita, PharmD; Stephan
Homocysteine Determination in Plasma
 omocysteine Determination in Plasma Bruce Peary Solomon, Ph.D. Chester T. Duda, Ph.D. Bioanalytical Systems, Inc. West Lafayette, IN E-mail: bp@bioanalytical.com Recent publications suggest that high homocysteine
omocysteine Determination in Plasma Bruce Peary Solomon, Ph.D. Chester T. Duda, Ph.D. Bioanalytical Systems, Inc. West Lafayette, IN E-mail: bp@bioanalytical.com Recent publications suggest that high homocysteine
HYPERHOMOCYSTEINEMIA: RELATION TO CARDIOVASCULAR DISEASE (PDF) HOMOCYSTEINE AND RELATED B-VITAMIN STATUS IN COELIAC
 PDF HYPERHOMOCYSTEINEMIA: RELATION TO CARDIOVASCULAR DISEASE (PDF) HOMOCYSTEINE AND RELATED B-VITAMIN STATUS IN COELIAC 1 / 5 2 / 5 3 / 5 homocysteine related vitamins pdf Hyperhomocysteinemia: Relation
PDF HYPERHOMOCYSTEINEMIA: RELATION TO CARDIOVASCULAR DISEASE (PDF) HOMOCYSTEINE AND RELATED B-VITAMIN STATUS IN COELIAC 1 / 5 2 / 5 3 / 5 homocysteine related vitamins pdf Hyperhomocysteinemia: Relation
Homocysteine enzymatic assay A strong, independent risk factor for cardiovascular disease
 References 1 World Health rganization. Fact sheet No. 317. Cardiovascular diseases (CVDs). Available at: www.who.int/mediacentre/factsheets/fs317/en/index.html [Accessed ctober 19, 2012]. 2 World Health
References 1 World Health rganization. Fact sheet No. 317. Cardiovascular diseases (CVDs). Available at: www.who.int/mediacentre/factsheets/fs317/en/index.html [Accessed ctober 19, 2012]. 2 World Health
Folate and Neural Tube Defect Risk: Paradigm Shift after Forty Years of Research
 Folate and Neural Tube Defect Risk: Paradigm Shift after Forty Years of Research From Holland to Jamaica; from the 18th Century to 1988 In the 18th century, a midwife in Friesland, in the northern part
Folate and Neural Tube Defect Risk: Paradigm Shift after Forty Years of Research From Holland to Jamaica; from the 18th Century to 1988 In the 18th century, a midwife in Friesland, in the northern part
Byung-Ok Choi, M.D., Yong Seong Kim, Ph.D.*, Ok-Joon Kim, M.D., Jung-Ho Seo, M.D., Nam-Keun Kim, Ph.D.
 Hyperhomocysteinemia as an Independent Risk Factor for Silent Brain Infarction - Inverse Correlation with Folate in Patients with MTHFR 677TT Genotype - Byung-Ok Choi, M.D., Yong Seong Kim, Ph.D.*, Ok-Joon
Hyperhomocysteinemia as an Independent Risk Factor for Silent Brain Infarction - Inverse Correlation with Folate in Patients with MTHFR 677TT Genotype - Byung-Ok Choi, M.D., Yong Seong Kim, Ph.D.*, Ok-Joon
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23219
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23219
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
Arteriosclerosis & Atherosclerosis
 Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Methylation demand: a key determinant of homocysteine metabolism
 Vol. 51 No. 2/2004 405 413 QUARTERLY Review Methylation demand: a key determinant of homocysteine metabolism John T. Brosnan 1, Rene L. Jacobs 2, Lori M. Stead 1 and Margaret E. Brosnan 1 1 Department
Vol. 51 No. 2/2004 405 413 QUARTERLY Review Methylation demand: a key determinant of homocysteine metabolism John T. Brosnan 1, Rene L. Jacobs 2, Lori M. Stead 1 and Margaret E. Brosnan 1 1 Department
A Second Common Mutation in the Methylenetetrahydrofolate Reductase Gene: An Additional Risk Factor for Neural-Tube Defects?
 Am. J. Hum. Genet. 62:1044 1051, 1998 A Second Common Mutation in the Methylenetetrahydrofolate Reductase Gene: An Additional Risk Factor for Neural-Tube Defects? Nathalie M. J. van der Put, 1 Fons Gabreëls,
Am. J. Hum. Genet. 62:1044 1051, 1998 A Second Common Mutation in the Methylenetetrahydrofolate Reductase Gene: An Additional Risk Factor for Neural-Tube Defects? Nathalie M. J. van der Put, 1 Fons Gabreëls,
Folic Acid Improves Arterial Endothelial Function in Adults With Hyperhomocystinemia
 Journal of the American College of Cardiology Vol. 34, No. 7, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00469-6 Folic
Journal of the American College of Cardiology Vol. 34, No. 7, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00469-6 Folic
ORIGINAL INVESTIGATION. Homocysteine and Short-term Risk of Myocardial Infarction and Stroke in the Elderly
 Homocysteine and Short-term Risk of Myocardial Infarction and Stroke in the Elderly The Rotterdam Study ORIGINAL INVESTIGATION Michiel L. Bots, MD, PhD; Lenore J. Launer, PhD; Jan Lindemans, PhD; Arno
Homocysteine and Short-term Risk of Myocardial Infarction and Stroke in the Elderly The Rotterdam Study ORIGINAL INVESTIGATION Michiel L. Bots, MD, PhD; Lenore J. Launer, PhD; Jan Lindemans, PhD; Arno
Vascular complications in patients with hyperhomocysteinemia
 Relation of a Common Methylenetetrahydrofolate Reductase Mutation and Plasma Homocysteine With Intimal Hyperplasia After Coronary Stenting Tai Kosokabe, MD; Kenji Okumura, MD; Takahito Sone, MD; Junichiro
Relation of a Common Methylenetetrahydrofolate Reductase Mutation and Plasma Homocysteine With Intimal Hyperplasia After Coronary Stenting Tai Kosokabe, MD; Kenji Okumura, MD; Takahito Sone, MD; Junichiro
Over the last 10 years, there has been an explosion of interest in homocysteine, a sulfurcontaining
 Homocysteine and Neurologic Disease Ramon Diaz-Arrastia, MD, PhD NEUROLOGICAL REVIEW Over the last 10 years, there has been an explosion of interest in homocysteine, a sulfurcontaining amino acid that
Homocysteine and Neurologic Disease Ramon Diaz-Arrastia, MD, PhD NEUROLOGICAL REVIEW Over the last 10 years, there has been an explosion of interest in homocysteine, a sulfurcontaining amino acid that
Stroke is the second most common cause of death in the
 Association Between High Homocyst(e)ine and Ischemic Stroke due to Large- and Small-Artery Disease but Not Other Etiologic Subtypes of Ischemic Stroke John W. Eikelboom, MBBS, FRACP, FRCPA; Graeme J. Hankey,
Association Between High Homocyst(e)ine and Ischemic Stroke due to Large- and Small-Artery Disease but Not Other Etiologic Subtypes of Ischemic Stroke John W. Eikelboom, MBBS, FRACP, FRCPA; Graeme J. Hankey,
Hyperhomocysteinemia is associated with increased risk
 Supplementation of Atherogenic Diet With B Vitamins Does Not Prevent Atherosclerosis or Vascular Dysfunction in Monkeys Steven R. Lentz, MD, PhD; Donald J. Piegors, MBA; M. René Malinow, MD; Donald D.
Supplementation of Atherogenic Diet With B Vitamins Does Not Prevent Atherosclerosis or Vascular Dysfunction in Monkeys Steven R. Lentz, MD, PhD; Donald J. Piegors, MBA; M. René Malinow, MD; Donald D.
Prevalence Of Hyperhomocysteinemia In Patients With Predialysis Chronic Kidney Disease After Folic Acid Food Fortification Of The Canadian Food Supply
 Prevalence Of Hyperhomocysteinemia In Patients With Predialysis Chronic Kidney Disease After Folic Acid Food Fortification Of The Canadian Food Supply Pauline B. Darling PhD RD Research Team Research Team
Prevalence Of Hyperhomocysteinemia In Patients With Predialysis Chronic Kidney Disease After Folic Acid Food Fortification Of The Canadian Food Supply Pauline B. Darling PhD RD Research Team Research Team
KEY COMPONENTS. Metabolic Risk Cardiovascular Risk Vascular Inflammation Markers
 CardioMetabolic Risk Poor blood sugar regulation and unhealthy triglyceride and lipoprotein levels often present long before the diagnosis of type 2 Diabetes. SpectraCell s CardioMetabolic and Pre-Diabetes
CardioMetabolic Risk Poor blood sugar regulation and unhealthy triglyceride and lipoprotein levels often present long before the diagnosis of type 2 Diabetes. SpectraCell s CardioMetabolic and Pre-Diabetes
Homocysteine is a sulfur-containing amino acid whose
 Diet-Induced Hyperhomocysteinemia Exacerbates Neointima Formation in Rat Carotid Arteries After Balloon Injury Hiroyuki Morita, MD; Hiroki Kurihara, MD; Shigetaka Yoshida, MD; Yuichiro Saito, MD; Takayuki
Diet-Induced Hyperhomocysteinemia Exacerbates Neointima Formation in Rat Carotid Arteries After Balloon Injury Hiroyuki Morita, MD; Hiroki Kurihara, MD; Shigetaka Yoshida, MD; Yuichiro Saito, MD; Takayuki
Introduction. Summary
 Am. J. Hum. Genet. 64:1045 1055, 1999 The Thermolabile Variant of Methylenetetrahydrofolate Reductase and Neural Tube Defects: An Evaluation of Genetic Risk and the Relative Importance of the Genotypes
Am. J. Hum. Genet. 64:1045 1055, 1999 The Thermolabile Variant of Methylenetetrahydrofolate Reductase and Neural Tube Defects: An Evaluation of Genetic Risk and the Relative Importance of the Genotypes
Elevated serum homocysteine level has a positive correlation with serum cardiac troponin I in patients with acute myocardial infarction
 Bangladesh Med Res Counc Bull 2012; 38: 9-13 Elevated serum homocysteine level has a positive correlation with serum cardiac troponin I in patients with acute myocardial infarction Abstract Alam N, Khan
Bangladesh Med Res Counc Bull 2012; 38: 9-13 Elevated serum homocysteine level has a positive correlation with serum cardiac troponin I in patients with acute myocardial infarction Abstract Alam N, Khan
Homocystinuria. Reduced folate levels during pyridoxine treatment
 Archives of Disease in Childhood, 1973, 48, 58. Homocystinuria Reduced folate levels during pyridoxine treatment BRIDGET WILCKEN and BRIAN TURNER* From the Oliver Latham Laboratory, The Psychiatric Centre,
Archives of Disease in Childhood, 1973, 48, 58. Homocystinuria Reduced folate levels during pyridoxine treatment BRIDGET WILCKEN and BRIAN TURNER* From the Oliver Latham Laboratory, The Psychiatric Centre,
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 31 Amino Acid Synthesis 2013 W. H. Freeman and Company Chapter 31 Outline Although the atmosphere is approximately 80% nitrogen,
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 31 Amino Acid Synthesis 2013 W. H. Freeman and Company Chapter 31 Outline Although the atmosphere is approximately 80% nitrogen,
General introduction
 1 General introduction Essentials of homocysteine and 1-carbon metabolism Cardiovascular disease (CVD) is one of the most prominent causes of death in the modern world. Research has shown that a combination
1 General introduction Essentials of homocysteine and 1-carbon metabolism Cardiovascular disease (CVD) is one of the most prominent causes of death in the modern world. Research has shown that a combination
Annals of RSCB Vol. XVI, Issue 1
 THE STUDY OF PROTHROBOTIC STATE IN PATIENTS WITH TYPE 2 DIABETES MELLITUS AND CARDIOVASCULAR DISEASES Oana Bădulescu 1, Codruţa Bădescu 2, Manuela Ciocoiu 1, Magda Bădescu 1 1 DEPARTMENT OF PATHOPHYSIOLOGY;
THE STUDY OF PROTHROBOTIC STATE IN PATIENTS WITH TYPE 2 DIABETES MELLITUS AND CARDIOVASCULAR DISEASES Oana Bădulescu 1, Codruţa Bădescu 2, Manuela Ciocoiu 1, Magda Bădescu 1 1 DEPARTMENT OF PATHOPHYSIOLOGY;
Increased Homocysteine in a Patient Diagnosed with Marfan Syndrome
 Clinical Chemistry 56:11 1665 1670 (2010) Clinical Case Study Increased Homocysteine in a Patient Diagnosed with Marfan Syndrome Olajumoke Oladipo, 1 Laurie Spreitsma, 2 Dennis J. Dietzen, 1,2* and Marwan
Clinical Chemistry 56:11 1665 1670 (2010) Clinical Case Study Increased Homocysteine in a Patient Diagnosed with Marfan Syndrome Olajumoke Oladipo, 1 Laurie Spreitsma, 2 Dennis J. Dietzen, 1,2* and Marwan
Folic acid inhibits homocysteine-induced proliferation of human arterial smooth muscle cells
 From the Eastern Vascular Society BASIC RESEARCH STUDIES Folic acid inhibits homocysteine-induced proliferation of human arterial smooth muscle cells Brennan J. Carmody, MD, Subodh Arora, MD, Ricardo Avena,
From the Eastern Vascular Society BASIC RESEARCH STUDIES Folic acid inhibits homocysteine-induced proliferation of human arterial smooth muscle cells Brennan J. Carmody, MD, Subodh Arora, MD, Ricardo Avena,
Meeting folate and related B-vitamin requirements through food: Is it enough? Role of fortification and dietary supplements
 Meeting folate and related B-vitamin requirements through food: Is it enough? Role of fortification and dietary supplements Helene McNulty PhD RD Northern Ireland Centre for Food and Health (NICHE) University
Meeting folate and related B-vitamin requirements through food: Is it enough? Role of fortification and dietary supplements Helene McNulty PhD RD Northern Ireland Centre for Food and Health (NICHE) University
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
ON MATTERS OF METHYLATION WHAT IS METHYLATION? CAUSES OF METHYLATION IMPAIRMENT
 METHYL BENEFITS ON MATTERS OF METHYLATION Methylation is more than just a buzzword. Methylation reactions are critical to our bodies proper function, as they impact such crucial components of health as
METHYL BENEFITS ON MATTERS OF METHYLATION Methylation is more than just a buzzword. Methylation reactions are critical to our bodies proper function, as they impact such crucial components of health as
Preventive Cardiology. Riboflavin Lowers Homocysteine in Individuals Homozygous
 Preventive Cardiology Riboflavin Lowers Homocysteine in Individuals Homozygous for the MTHFR 677C3 T Polymorphism Helene McNulty, PhD; Le Roy C. Dowey, PhD; J.J. Strain, PhD; Adrian Dunne, PhD; Mary Ward,
Preventive Cardiology Riboflavin Lowers Homocysteine in Individuals Homozygous for the MTHFR 677C3 T Polymorphism Helene McNulty, PhD; Le Roy C. Dowey, PhD; J.J. Strain, PhD; Adrian Dunne, PhD; Mary Ward,
Plasma homocysteine concentrations and risk of coronary heart disease in UK Indian Asian and European men
 Plasma homocysteine concentrations and risk of coronary heart disease in UK Indian Asian and European men John C Chambers, Omar A Obeid, Helga Refsum, Per Ueland, David Hackett, James Hooper, Rebecca M
Plasma homocysteine concentrations and risk of coronary heart disease in UK Indian Asian and European men John C Chambers, Omar A Obeid, Helga Refsum, Per Ueland, David Hackett, James Hooper, Rebecca M
