Keywords COPD, helmet, hypoxemic respiratory failure, immunocompromised, noninvasive ventilation
|
|
|
- Thomasina Parks
- 6 years ago
- Views:
Transcription
1 Critical Care February 2005 Vol 9 No 1 Antonelli et al. Review Clinical review: Noninvasive ventilation in the clinical setting experience from the past 10 years Massimo Antonelli 1, Mariano Alberto Pennisi 2 and Luca Montini 3 1 Professor of Intensive Care and Anesthesiology, Unità Operativa di Rianimazione e Terapia Intensiva, Istituto di Anestesia e Rianimazione, Policlinico Universitario A Gemelli, Università Cattolica del Sacro Cuore, Roma, Italy 2 Assistant Professor of Intensive Care and Anesthesiology, Unità Operativa di Rianimazione e Terapia Intensiva, Istituto di Anestesia e Rianimazione, Policlinico Universitario A Gemelli, Università Cattolica del Sacro Cuore, Roma, Italy 3 Research Fellow, Unità Operativa di Rianimazione e Terapia Intensiva, Istituto di Anestesia e Rianimazione, Policlinico Universitario A Gemelli, Università Cattolica del Sacro Cuore, Roma, Italy Corresponding author: Massimo Antonelli, m.antonelli@rm.unicatt.it Published online: 25 August 2004 This article is online at BioMed Central Ltd Critical Care 2005, 9: (DOI /cc2933) Abstract This brief review analyses the progress of noninvasive ventilation (NIV) over the last decade. NIV has gained the dignity of first line intervention for acute exacerbation of chronic obstructive pulmonary disease, assuring reduction of the intubation rate, rate of infection and mortality. Despite positive results, NIV still remains controversial as a treatment for acute hypoxemic respiratory failure, largely due to the different pathophysiology of hypoxemia. The infection rate reduction effect achieved by NIV application is crucial for immunocompromised patients for whom the endotracheal intubation represents a high risk. Improvements in skills acquired with experience over time progressively allowed successful treatment of more severe patients. Keywords COPD, helmet, hypoxemic respiratory failure, immunocompromised, noninvasive ventilation Introduction The term acute respiratory failure (ARF) indicates a severe deterioration in gas exchange, often requiring mechanical ventilatory support with endotracheal intubation (ETI). Placement of an endotracheal tube is associated with increased risk for complications such as tracheal stenosis [1,2] and ventilation associated pneumonia [3]. Noninvasive ventilation (NIV; i.e. delivery of assisted breaths without an invasive artificial airway) is a safe and effective tool in correcting the pathophysiological mechanisms of ARF, and reduces the work of breathing while concomitant treatments correct the causes of the ARF. NIV has been used primarily in patients with acute hypercapnic ventilatory failure, and especially for acute exacerbation of chronic obstructive pulmonary disease (COPD; Table 1). Hypercapnic respiratory failure The efficacy of NIV in treating acute exacerbations of COPD was investigated by Brochard and colleagues [4] in a European, randomized, multicenter study conducted in 85 COPD patients assigned to receive conventional treatment (oxygen therapy plus drugs) or NIV. The group of patients treated with NIV had fewer intubations (26% versus 74%; P < 0.001), fewer complications (14% versus 45%; P < 0.01), shorter length of hospital stay (23 ± 17 days versus 35 ± 33 days; P < 0.02), and lower mortality (9% versus 29%; P < 0.02). In a recent meta analysis, Keenan and coworkers [5] reported that the addition of noninvasive positive pressure ventilation (NPPV) to standard care in patients with acute exacerbations 98 ARF = acute respiratory failure; CAP = community acquired pneumonia; CI = confidence interval; COPD = chronic obstructive pulmonary disease; CPAP = continuous positive airway pressure; CPE = cardiopulmonary edema; ETI = endotracheal intubation; FiO 2 = fractional inspired oxygen; ICU = intensive care unit; NIV = noninvasive ventilation; NPPV = noninvasive positive pressure ventilation; PaCO 2 = arterial carbon dioxide tension; PaO 2 = arterial oxygen tension.
2 Available online Table 1 Selection criteria for noninvasive ventilation candidates Conscious and cooperative patient (the patient with chronic obstructive pulmonary disease may be an exception) No need for urgent intubation to protect the airways or to remove copious secretions No acute facial trauma (helmet interface may permit an exception in selected cases) No recent gastroesophageal surgery No active gastrointestinal bleeding No impairment in swallowing Hemodynamic and rhythm stability Adequate fitting of the interface of COPD decreased the rate of ETI (28% risk reduction, 95% confidence interval [CI] 15 40%), length of hospital stay (4.57 days, 95% CI days), and in-hospital mortality rate (10% risk reduction, 95% CI 5 15%). Subgroup analysis showed that these beneficial effects occurred in those patients who were more severely ill, and not in those with milder exacerbations. That meta-analysis also included studies conducted in patients who had milder exacerbations of COPD. In these investigations the mean arterial ph of the study populations was close to normal and the benefit from NIV was limited. In these studies the enrolment of patients with only slightly compromised respiratory function may account for the absence of relevant physiological effects of NIV. A point that the meta-analysis did not elucidate is whether patients with severe hypercapnia or acidemia at hospital admission are less likely to respond to NIV, as was reported in previous studies [6,7]. A recent Cochrane systematic review and meta-analysis [8] evaluated randomized controlled trials that compared NPPV with usual medical care in COPD patients with ARF. It found that NPPV is associated with lower mortality (relative risk 0.41, 95% CI ), decreased rate of ETI (relative risk 0.42, 95% CI ), and greater improvements in arterial carbon dioxide tension (PaCO 2 ) and respiratory rate after 1 hour of treatment. Also, there were fewer complications with NPPV (relative risk 0.32, 95% CI ). Success rates with NIV improve with increasing physician experience. Carlucci and coworkers [9] reported an 8-year retrospective study in which they investigated the changes in clinical practice of NIV in COPD patients. In that survey the failure rate with NIV was constant over time, regardless of the increasing severity of illness over the years. Between 1992 and 1996 the risk for NIV failure in more severely ill patients (ph < 7.25 at admission) was threefold higher than during the period The authors concluded that improvements in skills acquired with experience over time progressively allowed successful treatment of patients who are more severely ill. NIV works not only in more experienced academic centers but also in the real, clinical world. In a multicenter trial of the use of NIV in general respiratory wards, Plant and colleagues [10] randomly assigned 236 patients suffering from COPD exacerbations to standard medical therapy alone or medical therapy combined with NIV. Intubation and mortality rates in the NIV group were lower than in the conventional therapy group (15% versus 27% [P = 0.02] and 10% versus 20% [P = 0.05], respectively). Patients in the NIV group had a more rapid improvement in arterial ph and respiratory rate. In patients who were more acidotic (ph < 7.30) the benefit from NIV was limited, suggesting that the appropriate location for treatment of this more severely ill subgroup of patients is the intensive care unit (ICU) and not the general ward. The British Thoracic Society guidelines on the use of NIV in ARF stated that it can be considered the first-line intervention for hypercapnic COPD with ARF, and that expert staff and the facilities necessary to apply NIV should be available 24 hours a day in all hospitals that are likely to admit such patients [11]. A recent review defined NPPV as a standard of care for moderate-to-severe COPD exacerbation [12]. Hypoxemic respiratory failure The use of NIV in the treatment of hypoxemic ARF is still controversial. Part of this controversy stems from the heterogeneity of patients classified as being hypoxemic, who respond differently to the application of NIV. Four prospective randomized studies have evaluated the usefulness of NIV in immunocompetent patients suffering from hypoxemic ARF of various origins [13 16]. Wysocki and coworkers [13] randomly assigned 41 patients with ARF to NIV via facemask or conventional medical therapy. NIV reduced the need for ETI (36% versus 100%; P = 0.02), the duration of ICU stay (13 ± 15 days versus 32 ± 30 days; P = 0.04), and mortality rate (9% versus 66%; P = 0.06) in patients with hypercapnia only (PaCO 2 > 45 mmhg); it conferred no significant advantages in the purely hypoxemic group. Antonelli and colleagues [14] conducted a study in 64 consecutive patients with hypoxemic ARF who met well defined criteria for mechanical ventilation, in which they compared NIV via a face mask versus ETI with conventional mechanical ventilation. After 1 hour of mechanical ventilation both groups had a significant improvement in arterial oxygen tension (PaO 2 )/fractional inspired oxygen (FiO 2 ) ratio. Ten (31%) patients randomized to NIV required ETI. Patients randomized to conventional ventilation developed more frequent and serious complications (38% versus 66%; P = 0.02) and infectious complications (pneumonia or 99
3 Critical Care February 2005 Vol 9 No 1 Antonelli et al. 100 sinusitis) related to the presence of the endotracheal tube (3% versus 31%; P = 0.004). Among the survivors patients randomly assigned to NIV had a lesser duration of mechanical ventilation (P = 0.006) and a shorter ICU stay (P = 0.002). In another prospective, randomized trial Martin and coworkers [15] compared NIV using bilevel positive airway pressure with usual medical care for therapy of ARF. Patients were subgrouped according to the disease that led to ARF and were then randomly assigned to to NIV or medical treatment. A total of 32 patients with hypoxemic ARF were included in the study; 14 out of 32 were treated by NIV and were compared with the 18 patients treated with conventional medical therapy. The NIV group had a lower ETI rate than did those in the conventional therapy group (7.46 intubations/100 ICU days versus intubations/100 ICU days; P = 0.026). Recently, Ferrer and colleagues [16] reported a randomized controlled trial conducted in 105 consecutive patients with hypoxemic ARF. When compared with oxygen therapy, NIV decreased the need for intubation (25% versus 52%: P = 0.010), the incidence of septic shock (12% versus 31%; P = 0.028), and the ICU mortality (18% versus 39%; P = 0.028). Multivariate analysis showed that NIV was independently associated with decreased risk for intubation and decreased 90-day mortality. Hypoxemic ARF can be the end-point of several pathologies, and the mechanisms responsible for PaO 2 decrease may be quite different (shunt, ventilation/perfusion mismatch, impairment of alveolar capillary diffusion). Many reported clinical studies have been focused on specific pathologic conditions, such as cardiopulmonary edema (CPE), community acquired pneumonia (CAP), ARF occurring after thoracic surgery, or ARF occurring in immunosuppressed patients [17 25]. In these cases the efficacy of NIV, and therefore the patient s outcome, depends not only on gas exchange impairment as measured by PaO 2 /FiO 2 ratio but also, and predominantly, on the underlying pathology. Domenighetti and coworkers [26], in a prospective observational study, compared the acute effects of NIV in two groups of hypoxemic ARF patients with CAP and CPE. Oxygenation improved significantly in both groups, but the subsequent outcomes differed and were strictly dependent on the nature of the acute lung injury. The mean total time spent on NIV was 9 ± 6.3 hours in the CPE and 37 ± 36 hours in the CAP group (P = 0.01). ICU mortaliy rate was 6.6% in the CPE and 28% in the CAP group. In general, CPE with hypoxemic ARF is a condition that responds well to NIV. The major advantages of NIV are related to the effects generated by the increase in intrathoracic pressure. These benefits include increases in functional residual capacity and oxygenation, reduction in the work of breathing, and reductions in preload and afterload. Five randomized controlled studies were conducted in 336 patients with hypoxemic ARF due to CPE [17 21]. Patients were treated using continuous positive airway pressure (CPAP) in three studies [17 19], and bilevel positive ariway pressure [20] and pressure support ventilation [21] in the remaining two. ETI was required in 28 (16%) of the 167 patients assigned to the NIV group and in 54 (32%) of the 169 patients assigned to conventional treatment. The absolute risk reduction for ETI was 16%, and the number of patients needed to treat with NIV to avoid one ETI was six. The mortality rate was 13% (22/167) in the conventional therapy group and 8% (14/169) in the NIV group, with an absolute risk reduction of 5%, corresponding to 21 NIV treatments to save one life. In a multicenter prospective cohort study conducted in 354 patients with a diagnosis of hypoxemic ARF [27], the intubation rate was lower for patients with CPE (10%), pulmonary contusion (18%), and atelectasis (32%). In contrast, a high failure rate with ETI was observed in patients with acute respiratory distress syndrome (51%) and CAP (50%). Multivariate analysis identified acute respiratory distress syndrome, CAP, and lack of improvement in PaO 2 / FiO 2 ratio after 1 hour of treatment as independent risk factors for failure of NIV. Reduction in infections Randomized and observational studies including more than 300 immunocompetent and immunocompromised patients showed that NIV, by avoiding ETI, drastically reduces rates of infection and sepsis [4,14,16,24,25,28,29]. In a study conducted in COPD patients with acute exacerbation [4], the rate of pneumonia was 17% in the group with conventional medical treatment and 5% in the NIV group. In another randomized controlled study of the use of NIV in the treatment of hypoxemic patients [14], those randomly assigned to conventional ventilation developed more frequent infectious complications (pneumonia or sinusitis) related to the presence of the endotracheal tube (3% versus 31%; P = 0.004). This beneficial effect of NIV is important in immunocompromised or immunosuppressed patients. A prospective randomized study conducted in 40 solid organ transplant recipients with acute hypoxemic respiratory failure [24] compared NIV with standard treatment with supplemental oxygen. The use of NIV was associated with a significant reduction in the rate of ETI (20% versus 70%; P = 0.002), rate of severe sepsis and septic shock (20% versus 50%; P = 0.05), length of ICU stay in survivors (5.5 ± 3 days versus 9 ± 4 days; P = 0.03), and ICU mortality (20% versus 50%; P = 0.05). Hospital mortality was not different. Hilbert and coworkers [25], in a randomized controlled trial in 104 immunocompromised patients with severe hypoxemic ARF, compared intermittent NIV with standard treatment and supplemental oxygen. Twelve patients in the NIV group
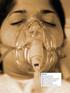
4 Available online Table 2 Figure 1 Criteria for discontinuation of noninvasive ventilation and endotracheal intubation Mask intolerance (discomfort or claustrophobia) Inability to improve gas exchanges and dyspnea Hemodynamic instability or evidence of cardiac ischemia or ventricular dysarrhythmia Need for urgent endotracheal intubation (because of inadequate management of secretions and protection of the airways) Failure to improve mental status, within 30 min after the application of noninvasive ventilation, in agitated hypoxemic patients compared with 20 in the standard treatment group required ETI (P = 0.03); NIV was associated with less serious complications, namely pneumonia and sepsis (P = 0.02), and with lower mortality (P = 0.02). New interfaces Recently, Navalesi and coworkers [30] elucidated the importance of the ventilatory interfaces for the success of NIV. Intolerance is one of the leading causes of NIV failure (Table 2) [9]. In an attempt to improve tolerability, a helmet (Fig. 1) has been proposed as a new interface for clinical use with CPAP and NIV. In a randomized physiologic study, Patroniti and collaborators [31] investigated the differences between facial mask and helmet in delivering CPAP. The authors concluded that both interfaces were effective and well tolerated, with similar reduction in the work of breathing, but the helmet needed flow rates greater than l/min to prevent rebreathing. In a prospective clinical pilot study [32], 33 patients with hypoxemic ARF, treated with noninvasive pressure support ventilation delivered by helmet, were compared with 66 matched control individuals treated with the same ventilatory technique by face mask. Oxygenation improved in both groups after NIV, and the number of patients requiring intubation was similar. No patients failed NIV because of intolerance to the technique in the helmet group, in comparison with eight patients (38%) in the mask group (P = 0.05). The duration of uninterrupted NIV was longer in the helmet group (36 ± 29 hours versus 26 ± 13 hours; P = 0.04). A similar study was conducted in 33 COPD patients with acute exacerbation, who were treated with helmet NPPV and compared with 33 patients with similar characteristics treated by face mask [33]. The ratio of patients requiring intubation and outcomes were similar in the two groups, with a significant reduction in PaCO 2. However, PaCO 2 decrease was more marked and faster in patients treated with the face mask (P = 0.01). The slower PaCO 2 decrease was not related Patient undergoing pressure support ventilation with a helmet. The transparency of the device permits interaction of the patient with their surroundings. ASV, antisuffocation valve, which opens automatically if disconnection from the ventilator occurs; Br, armpit braces that keep the helmet attached to the patient; C, collar; Inlet, inlet of medical gases, connected to the inspiratory port of the ventilator by conventional tubing; Outlet, outlet of gases, connected to expiratory port of the ventilator; P, sealed passage for the nasogastric tube (NGT), through which the patient can receive enteral feeding or drink through a straw (picture taken with patient permission). to rebreathing, which was similar with the two interfaces, but to the large volumes dissipated to distend the helmet. Nonivasive ventilation and weaning Three randomized trials conducted in Europe investigated the role of NIV in weaning failure [34 36]. In selected patients with COPD exacerbations and weaning failure, NIV facilitated extubation [34] and improved 3-month survival [35]. Ferrer and collaborators [36] investigated the role of NIV in patients who met criteria for a weaning attempt but failed a spontaneous breathing trial for 3 consecutive days. In that study NIV was effective in shortening the duration of invasive ventilation, and decreasing the incidence of nosocomial infections, mortality, and length of ICU and hospital stays. The International Consensus Conference [37] on the use of NIV in the treatment of ARF concluded that NIV may be effective in the setting of failed extubation. Recently, Keenan and coworkers [38] reported a small, single-center, randomized trial that compared the use of NIV with standard medical therapy in patients who had respiratory failure within 48 hours after extubation. They found no difference either in the rate of reintubation or in mortality. 101
5 Critical Care February 2005 Vol 9 No 1 Antonelli et al. 102 A multicenter randomized controlled trial recently reported by Esteban and colleagues [39] evaluated the impact that NIV had on extubation failure and mortality in a group of patients electively extubated after at least 48 hours of mechanical ventilation. There was no difference between the NIV and the standard therapy group in the need for reintubation (48% in both groups; P = 0.99). The rate of ICU death in the NIV group was greater than that in the standard therapy group (25% versus 14%; P = 0.048; relative risk 1.78, 95% CI ) and the median time from respiratory failure to reintubation was longer in the NIV group (12 hours versus 2.5 hours; P = 0.02). The authors concluded that NIV failed to reduce mortality or the need for reintubation among patients who had respiratory failure after extubation, and may be harmful. Conclusion NIV is now a first-line intervention for acute exacerbation of COPD; also, a growing body of evidence supports the use of NIV in hypoxemic respiratory failure, but this application requires careful selection of patients and close monitoring, in a setting in which intubation devices are readily available. Although NIV can be useful in avoiding weaning failure in selected patients admitted to specialized centers, at present there is no strong evidence to support extensive use of NIV to prevent weaning failure. Competing interests The author(s) declare that they have no competing interests. References 1. Torres A, Aznar R, Gatell JM, Jimenez P, Gonzalez J, Ferrer A, Celis R, Rodriguez-Roisin R: Incidence, risk and prognosis factors of nosocomial pneumonia in mechanically ventilated patients. Am Rev Respir Dis 1990, 142: Burns HP, Dayal VS, Scott A, Van Nostran ANP, Bryce DP: Laryngotracheal trauma: observations on its pathogenesis and its prevention following prolonged orotracheal intubation in the adult. Laryngoscope 1979, 89: Nourdine K, Combes P, Carton MJ, Beuret P, Cannamela A, Ducreux JC: Does NIV reduce the ICU nosocomial infection risk? A prospective clinical survey. Intensive Care Med 1999, 25: Brochard L, Mancebo J, Wysocki M, Lofaso F, Conti G, Rauss A, Simonneau G, Benito S, Gasparetto A, Lemaire F, et al.: NIV for acute exacerbations of chronic obstructive pulmonary disease. N Engl J Med 1995, 333: Keenan SP, Sinuff T, Cook DJ, Hill NS: Which patients with acute exacerbation of chronic obstructive pulmonary disease benefit from non-invasive positive-pressure ventilation? A systematic review of the literature. Ann Intern Med 2003, 138: Plant PK, Owen JL, Elliott MW: Non-invasive ventilation in acute exacerbations of chronic obstructive pulmonary disease: long term survival and predictors of in-hospital outcome. Thorax 2001, 56: Soo Hoo GW, Santiago S, Williams AJ: Nasal mechanical ventilation for hypercapnic respiratory failure in chronic obstructive pulmonary disease: determinants of success and failure. Crit Care Med 1994, 22: Lightowler JV, Wedzicha JA, Elliott MW, Ram FS: Non-invasive positive pressure ventilation to treat respiratory failure resulting from exacerbations of chronic obstructive pulmonary disease: Cochrane systematic review and meta-analysis. BMJ 2003, 326: Carlucci A, Delmastro M, Rubini F, Fracchia C, Nava S: Changes in the practice of noninvasive ventilation in treating COPD patients over 8 years. Intensive Care Med 2003, 29: Plant PK, Owen JL, Elliott MW: Early use of noninvasive ventilation for acute exacerbations of chronic obstructive pulmonary disease on general respiratory wards: a multicentre randomised controlled trial. Lancet 2000, 355: British Thoracic Society Standards of Care Committee: Non-invasive ventilation in acute respiratory failure. Thorax 2002, 57: Hill NS: Noninvasive ventilation for chronic obstructive pulmonary disease. Respir Care 2004, 49: Wysocki M, Tric L, Wolff MA, Millet H, Herman B: Noninvasive pressure support ventilation in patients with acute respiratory failure. A randomized comparison with conventional therapy. Chest 1995, 107: Antonelli M, Conti G, Rocco M, Bufi M, De Blasi RA, Vivino G, Gasparetto A, Meduri GU: A comparison of noninvasive positive-pressure ventilation and conventional mechanical ventilation in patients with acute respiratory failure. N Engl J Med 1998, 339: Martin TJ, Hovis JD, Costantino JP, Bierman MI, Donahoe MP, Rogers RM, Kreit JW, Sciurba FC, Stiller RA, Sanders MH: A randomized, prospective evaluation of noninvasive ventilation for acute respiratory failure. Am J Respir Crit Care Med 2000, 161: Ferrer M, Esquinas A, Leon M, Gonzalez G, Alarcon A, Torres A: Noninvasive ventilation in severe hypoxemic respiratory failure: a randomized clinical trial. Am J Respir Crit Care Med 2003, 168: Lin M, Yang Y, Chiany H, Chang M, Chiany BN, Chitlin MD: Reappraisal of continuous positive airway pressure therapy in acute cardiogenic pulmonary edema: short-term results and long-term follow-up. Chest 1995, 107: Bersten AD, Holt AW, Vedic AE, Skowronski GA, Baggoley CJ: Treatment of severe cardiogenic pulmonary edema with continuous positive airway pressure delivered by face mask. N Engl J Med 1991, 325: Rasanen J, Heikkila J, Downs J, Nikki P, Vaisanen I, Viitanen A: Continuous positive airway pressure by face mask in acute cardiogenic pulmonary edema. Am J Cardiol 1985, 55: Mehta S, Jay GD, Woolard RH, Hipona RA, Connolly EM, Cimini DM, Drinkwine JH, Hill NS: Randomized prospective trial of bilevel versus continous positive airway pressure in acute pulmonary edema. Crit Care Med 1997, 25: Nava S, Carbone G, DiBattista N, Bellone A, Baiardi P, Casentini R, Marengo M, Giostra F, Borasi G, Groff P: Noninvasive ventilation in cardiogenic pulmonary edema. A multicenter randomized trial. Am J Respir Crit Care Med 2003, 168: Auriant I, Jallot A, Herve P, Cerrina J, Le Roy Ladurie F, Fournier JL, Lescot B, Parquin F: Noninvasive ventilation reduces mortality in acute respiratory failure during lung resection. Am J Respir Crit Care Med 2001, 164: Confalonieri M, Potena A, Carbone G, Di Battista N, Bellone A, Baiardi P, Casentini R, Marenco M, Giostra F, Borasi G, et al.: Noninvasive ventilation in cardiogenic pulmonary edema a multicenter randomized trial. Am J Respir Crit Care Med 1999, 160: Antonelli M, Conti G, Bufi M, Costa MG, Lappa A, Rocco M, Gasparetto A, Meduri GU: Noninvasive ventilation for treatment of acute respiratory failure in patients undergoing solid organ transplantation. JAMA 2000, 283: Hilbert G, Gruson D, Vargas F, Valentino R: Noninvasive ventilation in immunosuppressed patients with pulmonary infiltrates, fever and acute respiratory failure. N Engl J Med 2001, 344: Domenighetti G, Gayer R, Gentilini R: Noninvasive pressure support ventilation in non COPD patients with acute cardiogenic pulmonary edema and severe community acquired penumonia: acute effect and outcome. Intensive Care Med 2002, 28: Antonelli M, Conti G, Moro ML, Esquinas A, Gonzalez-Diaz G, Confalonieri M, Pelaia P, Principi T, Gregoretti C, Beltrame F, et al.: Predictors of failure of noninvasive positive pressure ventilation in patients with acute hypoxemic respiratory failure: a multi center study. Intensive Care Med 2001, 27:
6 Available online Girou E, Schortgen F, Delclaux C, Brun-Buisson C, Blot F, Lefort Y, Lemaire F, Brochard L: Association of noninvasive ventilation with nosocomial infections and survival in critically ill patients. JAMA 2000, 284: Girou E, Brun-Buisson C, Taille S, Lemaire F, Brochard L: Secular trends in nosocomial infections and mortality associated with noninvasive ventilation in patients with exacerbation of COPD and pulmonary edema. JAMA 2003, 290: Navalesi P, Fanfulla F, Frigerio P, Gregoretti C, Nava S: Physiologic evaluation of noninvasive mechanical ventilation delivered with three types of masks in patients with chronic hypercapnic respiratory failure. Crit Care Med 2000, 28: Patroniti N, Foti G, Mangio A, Coppo A, Bellini G, Pesenti A: Head helmet versus face mask for non-invasive continuous positive airway pressure: physiological study. Intensive Care Med 2003, 29: Antonelli M, Conti G, Pelosi P, Gregoretti C, Pennisi MA, Costa R, Severgnini P, Chiaranda M, Proietti R: New treatment of acute hypoxemic respiratory failure: Non invasive pressure support ventilation delivered by helmet: a pilot controlled trial. Crit Care Med 2002, 30: Antonelli M, Pennisi MA, Pelosi P, Gregoretti C, Squadrone V, Rocco M, Cecchini L, Chiumello D, Severgnini P, Proietti R, et al.: Noninvasive positive pressure ventilation using a Helmet in patients with acute exacerbation of COPD: a feasibility study. Anesthesiology 2004, 100: Girault C, Daudenthun I, Chevron V, Tamion F, Leroy, Bonmarchand G: Noninvasive ventilation as a systematic extubation and weaning technique in acute on chronic respiratory failure: a prospective randomized controlled study. Am J Respir Crit Care Med 1999, 160: Nava S, Ambrosino N, Clini E, Prato M, Orlando G, Vitacca M, Brigada P, Fracchia C, Rubini F: Noninvasive mechanical in the weaning of patients with respiratory failure due to COPD: a randomized controlled study. Ann Intern Med 1998, 128: Ferrer M, Esquinas A, Arancibia F, Thonmas Bauer T, Gonzalez G, Carrillo A, Rodriguez-Roisin R, Torres A: Noninvasive ventilation during persistent weaning failure: a randomized controlled trial. Am J Respir Crit Care Med 2003, 168: International Consensus Conferences in Intensive Care Medicine: Noninvasive positive pressure ventilation in acute respiratory failure. Am J Respir Crit Care Med 2001, 163: Keenan SP, Powers C, Mc Cormack DG, Block G: Noninvasive positive-pressure ventilation for poextubation respiratory distress: a randomized controlled trial. JAMA 2002, 287: Esteban A, Frutos-Vivar F, Ferguson ND, Arabi Y, Apzteguia C, Gonzalez M, Epstein SK, Hill NS, Nava S, Soares MA, et al.: Noninvasive positive pressure ventilation for respiratory failure after extubation. N Engl J Med 2004, 350:
NIV in acute hypoxic respiratory failure
 All course materials, including the original lecture, are available as webcasts/podcasts at www.ers-education. org/niv2009.htm NIV in acute hypoxic respiratory failure Educational aims This presentation
All course materials, including the original lecture, are available as webcasts/podcasts at www.ers-education. org/niv2009.htm NIV in acute hypoxic respiratory failure Educational aims This presentation
Benefits and risks of success or failure of noninvasive ventilation
 Intensive Care Med (2006) 32:1756 1765 DOI 10.1007/s00134-006-0324-1 ORIGINAL Alexandre Demoule Emmanuelle Girou Jean-Christophe Richard Solenne Taille Laurent Brochard Benefits and risks of success or
Intensive Care Med (2006) 32:1756 1765 DOI 10.1007/s00134-006-0324-1 ORIGINAL Alexandre Demoule Emmanuelle Girou Jean-Christophe Richard Solenne Taille Laurent Brochard Benefits and risks of success or
Surgery Grand Rounds. Non-invasive Ventilation: A valuable tool. James Cromie, PGY 3 8/24/09
 Surgery Grand Rounds Non-invasive Ventilation: A valuable tool James Cromie, PGY 3 8/24/09 History of mechanical ventilation 1930 s: use of iron lung 1940 s: First NIV system (Bellevue Hospital) 1950 s:
Surgery Grand Rounds Non-invasive Ventilation: A valuable tool James Cromie, PGY 3 8/24/09 History of mechanical ventilation 1930 s: use of iron lung 1940 s: First NIV system (Bellevue Hospital) 1950 s:
NIV in hypoxemic patients
 NIV in hypoxemic patients Massimo Antonelli, MD Dept. of Intensive Care & Anesthesiology Università Cattolica del Sacro Cuore Rome - Italy Conflict of interest (research grants and consultations): Maquet
NIV in hypoxemic patients Massimo Antonelli, MD Dept. of Intensive Care & Anesthesiology Università Cattolica del Sacro Cuore Rome - Italy Conflict of interest (research grants and consultations): Maquet
Introduction ORIGINAL. G. Conti M. Antonelli P. Navalesi. M. Rocco M. Bufi G. Spadetta. G. U. Meduri
 Intensive Care Med (2002) 28:1701 1707 DOI 10.1007/s00134-002-1478-0 ORIGINAL G. Conti M. Antonelli P. Navalesi M. Rocco M. Bufi G. Spadetta G. U. Meduri Noninvasive vs. conventional mechanical in patients
Intensive Care Med (2002) 28:1701 1707 DOI 10.1007/s00134-002-1478-0 ORIGINAL G. Conti M. Antonelli P. Navalesi M. Rocco M. Bufi G. Spadetta G. U. Meduri Noninvasive vs. conventional mechanical in patients
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation: Non-COPD Applications
 Noninvasive Ventilation: Non-COPD Applications NONINVASIVE MECHANICAL VENTILATION Why Noninvasive Ventilation? Avoids upper A respiratory airway trauma system lacerations, protective hemorrhage strategy
Noninvasive Ventilation: Non-COPD Applications NONINVASIVE MECHANICAL VENTILATION Why Noninvasive Ventilation? Avoids upper A respiratory airway trauma system lacerations, protective hemorrhage strategy
N on-invasive ventilation (NIV) consists of mechanical
 772 ORIGINAL ARTICLE Non-invasive ventilation as a first-line treatment for acute respiratory failure: real life experience in the emergency department C Antro, F Merico, R Urbino, V Gai... See end of
772 ORIGINAL ARTICLE Non-invasive ventilation as a first-line treatment for acute respiratory failure: real life experience in the emergency department C Antro, F Merico, R Urbino, V Gai... See end of
Noninvasive positive-pressure ventilation in acute respiratory failure. Oscar Peñuelas MD, Fernando Frutos-Vivar MD, Andrés Esteban MD PhD
 Noninvasive positive-pressure ventilation in acute respiratory failure Oscar Peñuelas MD, Fernando Frutos-Vivar MD, Andrés Esteban MD PhD DOI:10.1503/cmaj.060147 Abstract Noninvasive positive-pressure
Noninvasive positive-pressure ventilation in acute respiratory failure Oscar Peñuelas MD, Fernando Frutos-Vivar MD, Andrés Esteban MD PhD DOI:10.1503/cmaj.060147 Abstract Noninvasive positive-pressure
PAPER DE LA VNI EN LA RETIRADA DE LA VENTILACIÓ INVASIVA I FRACÀS D EXTUBACIÓ
 PAPER DE LA VNI EN LA RETIRADA DE LA VENTILACIÓ INVASIVA I FRACÀS D EXTUBACIÓ Dr. Miquel Ferrer UVIIR, Servei de Pneumologia, Hospital Clínic, IDIBAPS, CibeRes, Barcelona. E- mail: miferrer@clinic.ub.es
PAPER DE LA VNI EN LA RETIRADA DE LA VENTILACIÓ INVASIVA I FRACÀS D EXTUBACIÓ Dr. Miquel Ferrer UVIIR, Servei de Pneumologia, Hospital Clínic, IDIBAPS, CibeRes, Barcelona. E- mail: miferrer@clinic.ub.es
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
NIV use in ED. Dr. Khalfan AL Amrani Emergency Resuscitation Symposium 2 nd May 2016 SQUH
 NIV use in ED Dr. Khalfan AL Amrani Emergency Resuscitation Symposium 2 nd May 2016 SQUH Outline History & Introduction Overview of NIV application Review of proven uses of NIV History of Ventilation 1940
NIV use in ED Dr. Khalfan AL Amrani Emergency Resuscitation Symposium 2 nd May 2016 SQUH Outline History & Introduction Overview of NIV application Review of proven uses of NIV History of Ventilation 1940
The Role of Noninvasive Ventilation in the Ventilator Discontinuation Process
 The Role of Noninvasive Ventilation in the Ventilator Discontinuation Process Dean R Hess PhD RRT FAARC Introduction NIV to Shorten the Length of Invasive Ventilation NIV to Prevent Extubation Failure
The Role of Noninvasive Ventilation in the Ventilator Discontinuation Process Dean R Hess PhD RRT FAARC Introduction NIV to Shorten the Length of Invasive Ventilation NIV to Prevent Extubation Failure
New advances in the use of noninvasive ventilation for acute hypoxaemic respiratory failure
 Eur Respir J 2003; 22: Suppl. 42, 65s 71s DOI: 10.1183/09031936.03.00421003 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2003 European Respiratory Journal ISSN 0904-1850 New advances in
Eur Respir J 2003; 22: Suppl. 42, 65s 71s DOI: 10.1183/09031936.03.00421003 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2003 European Respiratory Journal ISSN 0904-1850 New advances in
176 Airway pressure release ventilation, biphasic positive airway pressure Continuous positive airway pressure Figure 3.23 Figure 7.
 176 INTENSIVE CARE Airway pressure release ventilation, biphasic positive airway pressure Alveolar ventilation is achieved by the time-cycled switching between two levels of CPAP. Inspiratory and expiratory
176 INTENSIVE CARE Airway pressure release ventilation, biphasic positive airway pressure Alveolar ventilation is achieved by the time-cycled switching between two levels of CPAP. Inspiratory and expiratory
The Rapid Shallow Breathing Index as a Predictor of Failure of Noninvasive Ventilation for Patients With Acute Respiratory Failure
 Original Research The Rapid Shallow Breathing Index as a Predictor of Failure of Noninvasive Ventilation for Patients With Acute Respiratory Failure Katherine M Berg MD, Gerald R Lang RRT, Justin D Salciccioli,
Original Research The Rapid Shallow Breathing Index as a Predictor of Failure of Noninvasive Ventilation for Patients With Acute Respiratory Failure Katherine M Berg MD, Gerald R Lang RRT, Justin D Salciccioli,
Recent advances in mechanical ventilation
 The American Journal of Medicine (2005) 118, 584 591 REVIEW Recent advances in mechanical ventilation Carolyn S. Calfee, MD, a,b Michael A. Matthay, MD a,b,c a From the Cardiovascular Research Institute,
The American Journal of Medicine (2005) 118, 584 591 REVIEW Recent advances in mechanical ventilation Carolyn S. Calfee, MD, a,b Michael A. Matthay, MD a,b,c a From the Cardiovascular Research Institute,
with chronic obstructive pulmonary
 A multiple-center survey on the use in clinical practice of noninvasive ventilation as a first-line intervention for acute respiratory distress syndrome* Massimo Antonelli, MD; Giorgio Conti, MD; Antonio
A multiple-center survey on the use in clinical practice of noninvasive ventilation as a first-line intervention for acute respiratory distress syndrome* Massimo Antonelli, MD; Giorgio Conti, MD; Antonio
Noninvasive ventilation in patients with do-not-intubate orders: medium-term efficacy depends critically on patient selection
 Intensive Care Med (2007) 33:350 354 DOI 10.1007/s00134-006-0437-6 BRIEF REPORT Rafael Fernandez Francisco Baigorri Antonio Artigas Noninvasive ventilation in patients with do-not-intubate orders: medium-term
Intensive Care Med (2007) 33:350 354 DOI 10.1007/s00134-006-0437-6 BRIEF REPORT Rafael Fernandez Francisco Baigorri Antonio Artigas Noninvasive ventilation in patients with do-not-intubate orders: medium-term
A study of non-invasive ventilation in acute respiratory failure
 Original Research Article A study of non-invasive ventilation in acute respiratory failure Nilima Manohar Mane 1, Jayant L. Pednekar 2, Sangeeta Pednekar 3* 1 Consultant Physician and Diabetologist, Apollo
Original Research Article A study of non-invasive ventilation in acute respiratory failure Nilima Manohar Mane 1, Jayant L. Pednekar 2, Sangeeta Pednekar 3* 1 Consultant Physician and Diabetologist, Apollo
Non-invasive ventilation for surgical patients with acute respiratory failure. Byoung Chul Lee, Kyu Hyouck Kyoung, Young Hwan Kim, Suk-Kyung Hong
 J Korean Surg Soc 2011;80:390-396 DOI: 10.4174/jkss.2011.80.6.390 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Non-invasive ventilation for surgical patients
J Korean Surg Soc 2011;80:390-396 DOI: 10.4174/jkss.2011.80.6.390 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Non-invasive ventilation for surgical patients
GE Healthcare. Non Invasive Ventilation (NIV) For the Engström Ventilator. Relief, Relax, Recovery
 GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
Papers. Abstract. Methods. Introduction. Josephine V Lightowler, Jadwiga A Wedzicha, Mark W Elliott, Felix S F Ram
 Non-invasive positive pressure ventilation to treat respiratory failure resulting from exacerbations of chronic obstructive pulmonary disease: Cochrane systematic review and meta-analysis Josephine V Lightowler,
Non-invasive positive pressure ventilation to treat respiratory failure resulting from exacerbations of chronic obstructive pulmonary disease: Cochrane systematic review and meta-analysis Josephine V Lightowler,
Concerns and Controversial Issues in NPPV. Concerns and Controversial Issues in Noninvasive Positive Pressure Ventilation
 : Common Therapy in Daily Practice Concerns and Controversial Issues in Noninvasive Positive Pressure Ventilation Rongchang Chen Guangzhou Institute of Respiratory Disease as the first choice of mechanical
: Common Therapy in Daily Practice Concerns and Controversial Issues in Noninvasive Positive Pressure Ventilation Rongchang Chen Guangzhou Institute of Respiratory Disease as the first choice of mechanical
NONINVASIVE POSITIVE-PRESSURE VENTILATION VS. MECHANICAL VENTILATION IN ACUTE RESPIRATORY FAILURE
 A COMPARISON OF NONINVASIVE POSITIVE-PRESSURE VENTILATION AND CONVENTIONAL MECHANICAL VENTILATION IN PATIENTS WITH ACUTE RESPIRATORY FAILURE MASSIMO ANTONELLI, M.D., GIORGIO CONTI, M.D., MONICA ROCCO,
A COMPARISON OF NONINVASIVE POSITIVE-PRESSURE VENTILATION AND CONVENTIONAL MECHANICAL VENTILATION IN PATIENTS WITH ACUTE RESPIRATORY FAILURE MASSIMO ANTONELLI, M.D., GIORGIO CONTI, M.D., MONICA ROCCO,
ERJ Express. Published on August 9, 2012 as doi: /
 ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
Keeping Patients Off the Vent: Bilevel, HFNC, Neither?
 Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Non-invasive ventilation in acute exacerbations of chronic obstructive pulmonary disease: long term survival and predictors of in-hospital outcome
 708 Department of Respiratory Medicine, St James s University Hospital, Leeds LS9 7TF, UK P K Plant JLOwen M W Elliott Correspondence to: Dr P K Plant Paul.Plant@ gw.sjsuh.northy.nhs.uk Received 25 July
708 Department of Respiratory Medicine, St James s University Hospital, Leeds LS9 7TF, UK P K Plant JLOwen M W Elliott Correspondence to: Dr P K Plant Paul.Plant@ gw.sjsuh.northy.nhs.uk Received 25 July
POLICY. Number: Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE. Authorization
 POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
EFFICACY OF BIPAP IN PATIENTS ADMITTED WITH HYPERCAPNIC RESPIRATORY FAILURE; AN EXPERIENCE AT A TERTIARY CARE HOSPITAL
 ORIGINAL ARTICLE EFFICACY OF BIPAP IN PATIENTS ADMITTED WITH HYPERCAPNIC RESPIRATORY FAILURE; AN EXPERIENCE AT A TERTIARY CARE HOSPITAL Hussain Ahmad*, Saadia Ashraf*, Rukhsana Javed Farooqi*, Mukhtiar
ORIGINAL ARTICLE EFFICACY OF BIPAP IN PATIENTS ADMITTED WITH HYPERCAPNIC RESPIRATORY FAILURE; AN EXPERIENCE AT A TERTIARY CARE HOSPITAL Hussain Ahmad*, Saadia Ashraf*, Rukhsana Javed Farooqi*, Mukhtiar
Noninvasive Ventilation for Critical Care* Erik Garpestad, MD, FCCP; John Brennan, MD; and Nicholas S. Hill, MD, FCCP
 CHEST Noninvasive Ventilation for Critical Care* Erik Garpestad, MD, FCCP; John Brennan, MD; and Nicholas S. Hill, MD, FCCP Postgraduate Education Corner CONTEMPORARY REVIEWS IN CRITICAL CARE MEDICINE
CHEST Noninvasive Ventilation for Critical Care* Erik Garpestad, MD, FCCP; John Brennan, MD; and Nicholas S. Hill, MD, FCCP Postgraduate Education Corner CONTEMPORARY REVIEWS IN CRITICAL CARE MEDICINE
Recent Advances in Respiratory Medicine
 Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
Non-invasive Positive Pressure Mechanical Ventilation: NIPPV: CPAP BPAP IPAP EPAP. My Real Goals. What s new in 2018? OMG PAP?
 Non-invasive Positive Pressure Mechanical Ventilation: What s new in 2018? Geoffrey R. Connors, MD, FACP Associate Professor of Medicine University of Colorado School of Medicine Division of Pulmonary
Non-invasive Positive Pressure Mechanical Ventilation: What s new in 2018? Geoffrey R. Connors, MD, FACP Associate Professor of Medicine University of Colorado School of Medicine Division of Pulmonary
Bilevel positive airway pressure nasal mask ventilation in patients with acute hypercapnic respiratory failure
 Bilevel positive airway pressure nasal mask ventilation in patients with acute hypercapnic respiratory failure CK Chan, KS Lau, HC Fan, CW Lam The efficacy and complications of bilevel positive airway
Bilevel positive airway pressure nasal mask ventilation in patients with acute hypercapnic respiratory failure CK Chan, KS Lau, HC Fan, CW Lam The efficacy and complications of bilevel positive airway
The study had a total of 6 amendments submitted to and approved by the IRB. All were minor and received expedited approval.
 1 Summary of Protocol Amendments 2 3 4 The study had a total of 6 amendments submitted to and approved by the IRB. All were minor and received expedited approval. 5 6 7 8 9 10 11 12 13 The original protocol
1 Summary of Protocol Amendments 2 3 4 The study had a total of 6 amendments submitted to and approved by the IRB. All were minor and received expedited approval. 5 6 7 8 9 10 11 12 13 The original protocol
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning
 CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
Non-invasive ventilation for acute hypoxemic respiratory failure: intubation rate and risk factors
 Thille et al. Critical Care 2013, 17:R269 RESEARCH Open Access Non-invasive ventilation for acute hypoxemic respiratory failure: intubation rate and risk factors Arnaud W Thille 1,2,3*, Damien Contou 1,3,
Thille et al. Critical Care 2013, 17:R269 RESEARCH Open Access Non-invasive ventilation for acute hypoxemic respiratory failure: intubation rate and risk factors Arnaud W Thille 1,2,3*, Damien Contou 1,3,
ISPUB.COM. S Venkatram, S Rachmale, B Kanna, A Soni INTRODUCTION METHODS AND MATERIALS DESIGN SETTING INCLUSION CRITERIA
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Non-Invasive Positive Pressure Ventilation Compared To Invasive Mechanical Ventilation Among Patients With COPD Exacerbations In
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Non-Invasive Positive Pressure Ventilation Compared To Invasive Mechanical Ventilation Among Patients With COPD Exacerbations In
Noninvasive versus conventional ventilation to treat hypercapnic encephalopathy in chronic obstructive pulmonary disease
 Intensive Care Med DOI 10.1007/s00134-007-0837-2 ORIGINAL Raffaele Scala Stefano Nava Giorgio Conti Massimo Antonelli Mario Naldi Ivano Archinucci Giovanni Coniglio Nicholas S. Hill Noninvasive versus
Intensive Care Med DOI 10.1007/s00134-007-0837-2 ORIGINAL Raffaele Scala Stefano Nava Giorgio Conti Massimo Antonelli Mario Naldi Ivano Archinucci Giovanni Coniglio Nicholas S. Hill Noninvasive versus
ARF. 8 8 (PaO 2 / FIO 2 ) NPPV NPPV ( P = 0.37) NPPV NPPV. (PaO 2 / FIO 2 > 200 PaO 2 / FIO 2 NPPV > 100) (P = 0.02) NPPV ( NPPV P = 0.
 Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
Università Cattolica del Sacro Cuore, Rome, Italy. Abstract
 http://ccforum.com/content/4/1/015 Review Noninvasive positive pressure ventilation as treatment for acute respiratory failure in critically ill patients Massimo Antonelli and Giorgio Conti Università
http://ccforum.com/content/4/1/015 Review Noninvasive positive pressure ventilation as treatment for acute respiratory failure in critically ill patients Massimo Antonelli and Giorgio Conti Università
Noninvasive pressure support ventilation in COPD patients with postextubation hypercapnic respiratory insufficiency
 Eur Respir J 1998; 11: 1349 1353 DOI: 10.1183/09031936.98.11061349 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Noninvasive pressure support
Eur Respir J 1998; 11: 1349 1353 DOI: 10.1183/09031936.98.11061349 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Noninvasive pressure support
Noninvasive Ventilation during Persistent Weaning Failure A Randomized Controlled Trial
 Noninvasive Ventilation during Persistent Weaning Failure A Randomized Controlled Trial Miquel Ferrer, Antonio Esquinas, Francisco Arancibia, Torsten Thomas Bauer, Gumersindo Gonzalez, Andres Carrillo,
Noninvasive Ventilation during Persistent Weaning Failure A Randomized Controlled Trial Miquel Ferrer, Antonio Esquinas, Francisco Arancibia, Torsten Thomas Bauer, Gumersindo Gonzalez, Andres Carrillo,
Mechanical ventilation: invasive versus noninvasive
 Eur Respir J 2003; 22: Suppl. 47, 31s 37s DOI: 10.1183/09031936.03.00050403 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2003 European Respiratory Journal ISSN 0904-1850 Mechanical ventilation:
Eur Respir J 2003; 22: Suppl. 47, 31s 37s DOI: 10.1183/09031936.03.00050403 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2003 European Respiratory Journal ISSN 0904-1850 Mechanical ventilation:
Acute Applications of Noninvasive Positive Pressure Ventilation* Timothy Liesching, MD; Henry Kwok, MD, FCCP; and Nicholas S.
 reviews Acute Applications of Noninvasive Positive Pressure Ventilation* Timothy Liesching, MD; Henry Kwok, MD, FCCP; and Nicholas S. Hill, MD, FCCP Noninvasive positive-pressure ventilation (NPPV) has
reviews Acute Applications of Noninvasive Positive Pressure Ventilation* Timothy Liesching, MD; Henry Kwok, MD, FCCP; and Nicholas S. Hill, MD, FCCP Noninvasive positive-pressure ventilation (NPPV) has
Noninvasive ventilation for avoidance of reintubation in patients with various cough strength
 Duan et al. Critical Care (2016) 20:316 DOI 10.1186/s13054-016-1493-0 RESEARCH Open Access Noninvasive ventilation for avoidance of reintubation in patients with various cough strength Jun Duan *, Xiaoli
Duan et al. Critical Care (2016) 20:316 DOI 10.1186/s13054-016-1493-0 RESEARCH Open Access Noninvasive ventilation for avoidance of reintubation in patients with various cough strength Jun Duan *, Xiaoli
Noninvasive respiratory support:why is it working?
 Noninvasive respiratory support:why is it working? Paolo Pelosi Department of Surgical Sciences and Integrated Diagnostics (DISC) IRCCS San Martino IST University of Genoa, Genoa, Italy ppelosi@hotmail.com
Noninvasive respiratory support:why is it working? Paolo Pelosi Department of Surgical Sciences and Integrated Diagnostics (DISC) IRCCS San Martino IST University of Genoa, Genoa, Italy ppelosi@hotmail.com
Effect of noninvasive mechanical ventilation in elderly patients with hypercapnic acute-on-chronic respiratory failure and a do-not-intubate order
 ORIGINAL RESEARCH Effect of noninvasive mechanical ventilation in elderly patients with hypercapnic acute-on-chronic respiratory failure and a do-not-intubate order Paolo Scarpazza 1 Cristoforo Incorvaia
ORIGINAL RESEARCH Effect of noninvasive mechanical ventilation in elderly patients with hypercapnic acute-on-chronic respiratory failure and a do-not-intubate order Paolo Scarpazza 1 Cristoforo Incorvaia
What Is the Impact of Mildly Altered Consciousness on Acute Hypoxemic Respiratory Failure with Non-invasive Ventilation?
 doi: 10.2169/internalmedicine.9355-17 Intern Med 57: 1689-1695, 2018 http://internmed.jp ORIGINAL ARTICLE What Is the Impact of Mildly Altered Consciousness on Acute Hypoxemic Respiratory Failure with
doi: 10.2169/internalmedicine.9355-17 Intern Med 57: 1689-1695, 2018 http://internmed.jp ORIGINAL ARTICLE What Is the Impact of Mildly Altered Consciousness on Acute Hypoxemic Respiratory Failure with
Extubation Failure & Delay in Brain-Injured Patients
 Extubation Failure & Delay in Brain-Injured Patients Niall D. Ferguson, MD, FRCPC, MSc Director, Critical Care Medicine University Health Network & Mount Sinai Hospital Associate Professor of Medicine
Extubation Failure & Delay in Brain-Injured Patients Niall D. Ferguson, MD, FRCPC, MSc Director, Critical Care Medicine University Health Network & Mount Sinai Hospital Associate Professor of Medicine
NON-INVASIVE VENTILATION. Lijun Ding 23 Jan 2018
 NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
Noninvasive Ventilation for Acute Respiratory Failure: A National Survey of Veterans Affairs Hospitals
 Noninvasive Ventilation for Acute Respiratory Failure: A National Survey of Veterans Affairs Hospitals Gregory B Bierer MD and Guy W Soo Hoo MD MPH BACKGROUND: The utilization of noninvasive ventilation
Noninvasive Ventilation for Acute Respiratory Failure: A National Survey of Veterans Affairs Hospitals Gregory B Bierer MD and Guy W Soo Hoo MD MPH BACKGROUND: The utilization of noninvasive ventilation
, OR 8.73 (95% CI
 550 Thorax 2000;55:550 554 Department of Respiratory Medicine, St James s University Hospital, Leeds LS9 7TF, UK P K Plant JLOwen M W Elliott Correspondence to: Dr P K Plant email: mbriggs@alwoodley.u-net.com
550 Thorax 2000;55:550 554 Department of Respiratory Medicine, St James s University Hospital, Leeds LS9 7TF, UK P K Plant JLOwen M W Elliott Correspondence to: Dr P K Plant email: mbriggs@alwoodley.u-net.com
Where to perform noninvasive ventilation?
 Eur Respir J 2002; 19: 1159 1166 DOI: 10.1183/09031936.02.00297202 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 SERIES 0NONINVASIVE VENTILATION
Eur Respir J 2002; 19: 1159 1166 DOI: 10.1183/09031936.02.00297202 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 SERIES 0NONINVASIVE VENTILATION
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. This online publication has been corrected. The corrected
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. This online publication has been corrected. The corrected
PAOLO PELOSI, LAURA MARIA CHIERICHETTI, PAOLO SEVERGNINI
 MANAGEMENT OF WEANING EUROANESTHESIA 2005 Vienna, Austria 28-31 May 2005 12RC11 PAOLO PELOSI, LAURA MARIA CHIERICHETTI, PAOLO SEVERGNINI Dipartimento Ambiente, Salute e Sicurezza, Universita degli Studi
MANAGEMENT OF WEANING EUROANESTHESIA 2005 Vienna, Austria 28-31 May 2005 12RC11 PAOLO PELOSI, LAURA MARIA CHIERICHETTI, PAOLO SEVERGNINI Dipartimento Ambiente, Salute e Sicurezza, Universita degli Studi
Efficacy of High-Flow Nasal Cannula Therapy in Acute Hypoxemic Respiratory Failure: Decreased Use of Mechanical Ventilation
 Efficacy of High-Flow Nasal Cannula Therapy in Acute Hypoxemic Respiratory Failure: Decreased Use of Mechanical Kazuma Nagata MD, Takeshi Morimoto MD PhD MPH, Daichi Fujimoto MD, Takehiro Otoshi MD, Atsushi
Efficacy of High-Flow Nasal Cannula Therapy in Acute Hypoxemic Respiratory Failure: Decreased Use of Mechanical Kazuma Nagata MD, Takeshi Morimoto MD PhD MPH, Daichi Fujimoto MD, Takehiro Otoshi MD, Atsushi
Mémoire de Maîtrise en médecine No 778. Etudiant Tania Soccorsi. Tuteur Dr Jean-Pierre Revelly Service de Médecine Intensive Adulte, CHUV
 Mémoire de Maîtrise en médecine No 778 Clinical characteristics and outcome of patients admitted to a medicosurgical ICU requiring non invasive ventilation (NIV) for hypercapnic respiratory failure Etudiant
Mémoire de Maîtrise en médecine No 778 Clinical characteristics and outcome of patients admitted to a medicosurgical ICU requiring non invasive ventilation (NIV) for hypercapnic respiratory failure Etudiant
High Flow Oxygen Therapy in Acute Respiratory Failure. Laurent Brochard Toronto
 High Flow Oxygen Therapy in Acute Respiratory Failure Laurent Brochard Toronto Conflicts of interest Our clinical research laboratory has received research grants for clinical research projects from the
High Flow Oxygen Therapy in Acute Respiratory Failure Laurent Brochard Toronto Conflicts of interest Our clinical research laboratory has received research grants for clinical research projects from the
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Dean R Hess PhD RRT, Jessica M Pang, and Carlos A Camargo Jr MD DrPH
 Original Research A Survey of the Use of Noninvasive Ventilation in Academic Emergency Departments in the United States Dean R Hess PhD RRT, Jessica M Pang, and Carlos A Camargo Jr MD DrPH OBJECTIVE: To
Original Research A Survey of the Use of Noninvasive Ventilation in Academic Emergency Departments in the United States Dean R Hess PhD RRT, Jessica M Pang, and Carlos A Camargo Jr MD DrPH OBJECTIVE: To
Acute noninvasive ventilation what s the evidence? Respiratory Medicine Update: Royal College of Physicians & BTS Thu 28 th January 2016
 Acute noninvasive ventilation what s the evidence? Respiratory Medicine Update: Royal College of Physicians & BTS Thu 28 th January 2016 Annabel Nickol Consultant in Respiratory Medicine, Sleep & Ventilation
Acute noninvasive ventilation what s the evidence? Respiratory Medicine Update: Royal College of Physicians & BTS Thu 28 th January 2016 Annabel Nickol Consultant in Respiratory Medicine, Sleep & Ventilation
Acute exacerbations are common in patients with
 Predicting the Result of Noninvasive Ventilation in Severe Acute Exacerbations of Patients With Chronic Airflow Limitation* Antonio Antón, MD; Rosa Güell, MD; Juan Gómez, MD; José Serrano, MD; Abilio Castellano,
Predicting the Result of Noninvasive Ventilation in Severe Acute Exacerbations of Patients With Chronic Airflow Limitation* Antonio Antón, MD; Rosa Güell, MD; Juan Gómez, MD; José Serrano, MD; Abilio Castellano,
Non-invasive Ventilation
 Non-invasive Ventilation 163 29 Non-invasive Ventilation AM BHAGWATI Artificial ventilatory support has became an integral component in the management of critically ill patients in the intensive care units.
Non-invasive Ventilation 163 29 Non-invasive Ventilation AM BHAGWATI Artificial ventilatory support has became an integral component in the management of critically ill patients in the intensive care units.
2016 Year in Review: Noninvasive Ventilation
 2016 Year in Review: Noninvasive Ventilation Thomas Piraino RRT Introduction NIV Compared With High-Flow Nasal Cannula Immunocompromised Patients Postextubation in Patients at Risk of Extubation Failure
2016 Year in Review: Noninvasive Ventilation Thomas Piraino RRT Introduction NIV Compared With High-Flow Nasal Cannula Immunocompromised Patients Postextubation in Patients at Risk of Extubation Failure
Objectives. Health care significance of ARF 9/10/15 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION
 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
Alma Mater University of Bologna. Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy
 Alma Mater University of Bologna Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy Conflict of Interest I have affiliations with, special interests, or have conducted business with the
Alma Mater University of Bologna Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy Conflict of Interest I have affiliations with, special interests, or have conducted business with the
Authors: Corresponding author: Yasuhiro Kamii Tel: Fax:
 Investigation of chronic obstructive pulmonary disease patients discharged without home mechanical ventilation after in-hospital use of acute non-invasive ventilation Authors: Yasuhiro Kamii, MD Hirotoshi
Investigation of chronic obstructive pulmonary disease patients discharged without home mechanical ventilation after in-hospital use of acute non-invasive ventilation Authors: Yasuhiro Kamii, MD Hirotoshi
The Egyptian Society of Chest Diseases and Tuberculosis. Egyptian Journal of Chest Diseases and Tuberculosis
 Egyptian Journal of Chest Diseases and Tuberculosis (2012) 61, 95 101 The Egyptian Society of Chest Diseases and Tuberculosis Egyptian Journal of Chest Diseases and Tuberculosis www.elsevier.com/locate/ejcdt
Egyptian Journal of Chest Diseases and Tuberculosis (2012) 61, 95 101 The Egyptian Society of Chest Diseases and Tuberculosis Egyptian Journal of Chest Diseases and Tuberculosis www.elsevier.com/locate/ejcdt
Predictors of Successful Noninvasive Ventilation Treatment for Patients Suffering Acute Respiratory Failure
 ORIGINAL ARTICLE Predictors of Successful Noninvasive Ventilation Treatment for Patients Suffering Acute Respiratory Failure Ming-Shian Lin 1, How-Ran Guo 2,3, Ming-Hua Huang 4, Cheng-Ren Chen 1, Chen-Long
ORIGINAL ARTICLE Predictors of Successful Noninvasive Ventilation Treatment for Patients Suffering Acute Respiratory Failure Ming-Shian Lin 1, How-Ran Guo 2,3, Ming-Hua Huang 4, Cheng-Ren Chen 1, Chen-Long
Non-invasive ventilation:
 Glossary ARF: Acute respiratory failure CHF: Congestive heart failure COPD: Chronic obstructive pulmonary disease CPAP: Continuous positive airway pressure CPE: Cardiogenic pulmonary oedema DNI: Do not
Glossary ARF: Acute respiratory failure CHF: Congestive heart failure COPD: Chronic obstructive pulmonary disease CPAP: Continuous positive airway pressure CPE: Cardiogenic pulmonary oedema DNI: Do not
Key words: acute respiratory failure; bronchoscopy; hypoxemia; noninvasive positive pressure ventilation; pneumonia
 Noninvasive Positive-Pressure Ventilation vs Conventional Oxygen Supplementation in Hypoxemic Patients Undergoing Diagnostic Bronchoscopy* Massimo Antonelli, MD; Giorgio Conti, MD; Monica Rocco, MD; Andrea
Noninvasive Positive-Pressure Ventilation vs Conventional Oxygen Supplementation in Hypoxemic Patients Undergoing Diagnostic Bronchoscopy* Massimo Antonelli, MD; Giorgio Conti, MD; Monica Rocco, MD; Andrea
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Outcome at three months of COPD patients with acute hypercapnic respiratory failure treated with NPPV in an Acute Medicine Ward
 emergency care journal Outcome at three months of COPD patients with acute hypercapnic respiratory failure treated with NPPV in an Acute Medicine Ward Fabrizio Vincenti*, Adriano Basile*, Ernesto Contro*,
emergency care journal Outcome at three months of COPD patients with acute hypercapnic respiratory failure treated with NPPV in an Acute Medicine Ward Fabrizio Vincenti*, Adriano Basile*, Ernesto Contro*,
Respiratory Failure how the respiratory physicians deal with airway emergencies
 Respiratory Failure how the respiratory physicians deal with airway emergencies Dr Michael Davies MD FRCP Consultant Respiratory Physician Respiratory Support and Sleep Centre Papworth Hospital NHS Foundation
Respiratory Failure how the respiratory physicians deal with airway emergencies Dr Michael Davies MD FRCP Consultant Respiratory Physician Respiratory Support and Sleep Centre Papworth Hospital NHS Foundation
Charisma High-flow CPAP solution
 Charisma High-flow CPAP solution Homecare PNEUMOLOGY Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support charisma High-flow CPAP solution Evidence CPAP therapy
Charisma High-flow CPAP solution Homecare PNEUMOLOGY Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support charisma High-flow CPAP solution Evidence CPAP therapy
Non-invasive ventilation for acute respiratory disease
 Published Online March 31, 2005 Non-invasive ventilation for acute respiratory disease M. W. Elliott St James s University Hospital, Beckett Street, Leeds LS9 7TF, UK Non-invasive ventilation (NIV) has
Published Online March 31, 2005 Non-invasive ventilation for acute respiratory disease M. W. Elliott St James s University Hospital, Beckett Street, Leeds LS9 7TF, UK Non-invasive ventilation (NIV) has
BiLevel Pressure Device
 PROCEDURE - Page 1 of 7 Purpose Scope Classes/ Goals Define indications and care settings for acute and chronic initiation of Noninvasive Positive Pressure Ventilation. Identify the role of Respiratory
PROCEDURE - Page 1 of 7 Purpose Scope Classes/ Goals Define indications and care settings for acute and chronic initiation of Noninvasive Positive Pressure Ventilation. Identify the role of Respiratory
Noninvasive proportional assist ventilation may be useful in weaning patients who failed spontaneous breathing trial
 Egyptian Journal of Anaesthesia (2012) 28, 89 94 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Noninvasive proportional
Egyptian Journal of Anaesthesia (2012) 28, 89 94 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Noninvasive proportional
IN THE PAST 2 DECADES, ADVANCEments
 CARING FOR THE CRITICALLY ILL PATIENT for Treatment of Acute Respiratory Failure in Patients Undergoing Solid Organ Transplantation A Randomized Trial Massimo Antonelli, MD Giorgio Conti, MD Maurizio Bufi,
CARING FOR THE CRITICALLY ILL PATIENT for Treatment of Acute Respiratory Failure in Patients Undergoing Solid Organ Transplantation A Randomized Trial Massimo Antonelli, MD Giorgio Conti, MD Maurizio Bufi,
Matteo Giacomini, MD; Gaetano Iapichino, MD; Marco Cigada, MD; Aldo Minuto, MD; Rebecca Facchini, MD; Andrea Noto, MD; and Elena Assi, MD
 Short-term Noninvasive Pressure Support Ventilation Prevents ICU Admittance in Patients With Acute Cardiogenic Pulmonary Edema* Matteo Giacomini, MD; Gaetano Iapichino, MD; Marco Cigada, MD; Aldo Minuto,
Short-term Noninvasive Pressure Support Ventilation Prevents ICU Admittance in Patients With Acute Cardiogenic Pulmonary Edema* Matteo Giacomini, MD; Gaetano Iapichino, MD; Marco Cigada, MD; Aldo Minuto,
Application of BiPAP through Endotracheal Tube in Comatose Patients with COPD Exacerbation
 Original Article Application of BiPAP through Endotracheal Tube in Comatose Patients with COPD Exacerbation Nousheen Akhter 1, Nadeem Ahmed Rizvi 2 ABSTRACT Objective: To evaluate the effectiveness and
Original Article Application of BiPAP through Endotracheal Tube in Comatose Patients with COPD Exacerbation Nousheen Akhter 1, Nadeem Ahmed Rizvi 2 ABSTRACT Objective: To evaluate the effectiveness and
Noninvasive ventilation after intubation and mechanical ventilation
 Eur Respir J 2002; 19: 959 965 DOI: 10.1183/09031936.02.00299702 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 SERIES 0NONINVASIVE VENTILATION
Eur Respir J 2002; 19: 959 965 DOI: 10.1183/09031936.02.00299702 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 SERIES 0NONINVASIVE VENTILATION
Should a Patient Be Extubated and Placed on Noninvasive Ventilation After Failing a Spontaneous Breathing Trial?
 Should a Patient Be Extubated and Placed on Noninvasive Ventilation After Failing a Spontaneous Breathing Trial? Scott K Epstein MD and Charles G Durbin Jr MD FAARC Introduction Pro: A Patient Who Fails
Should a Patient Be Extubated and Placed on Noninvasive Ventilation After Failing a Spontaneous Breathing Trial? Scott K Epstein MD and Charles G Durbin Jr MD FAARC Introduction Pro: A Patient Who Fails
Use of Noninvasive Positive-Pressure Ventilation on the Regular Hospital Ward: Experience and Correlates of Success
 Use of Noninvasive Positive-Pressure Ventilation on the Regular Hospital Ward: Experience and Correlates of Success Samar Farha MD, Ziad W Ghamra MD, Edward R Hoisington RRT, Robert S Butler MSc, and James
Use of Noninvasive Positive-Pressure Ventilation on the Regular Hospital Ward: Experience and Correlates of Success Samar Farha MD, Ziad W Ghamra MD, Edward R Hoisington RRT, Robert S Butler MSc, and James
Basics of NIV. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC. Consultant, Critical Care Medicine Medanta, The Medicity
 Basics of NIV Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Objectives: Definitions Advantages and Disadvantages Interfaces Indications Contraindications
Basics of NIV Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Objectives: Definitions Advantages and Disadvantages Interfaces Indications Contraindications
High-flow nasal oxygen therapy and noninvasive ventilation in the management of acute hypoxemic respiratory failure
 Review Article Page 1 of 8 High-flow nasal oxygen therapy and noninvasive ventilation in the management of acute hypoxemic respiratory failure Jean-Pierre Frat 1,2,3, Rémi Coudroy 1,2,3, Nicolas Marjanovic
Review Article Page 1 of 8 High-flow nasal oxygen therapy and noninvasive ventilation in the management of acute hypoxemic respiratory failure Jean-Pierre Frat 1,2,3, Rémi Coudroy 1,2,3, Nicolas Marjanovic
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด
 Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
Early predictors of success of non-invasive positive pressure ventilation in hypercapnic respiratory failure
 ORIGINAL ARTICLE Early predictors of success of non-invasive positive pressure ventilation in hypercapnic respiratory failure Col D Bhattacharyya*, Brig BNBM Prasad, SM, VSM, Surg Capt PS Tampi (Retd)
ORIGINAL ARTICLE Early predictors of success of non-invasive positive pressure ventilation in hypercapnic respiratory failure Col D Bhattacharyya*, Brig BNBM Prasad, SM, VSM, Surg Capt PS Tampi (Retd)
The Use of Noninvasive Ventilation in Emergency Department Patients With Acute Cardiogenic Pulmonary Edema: A Systematic Review
 CARDIOLOGY/ORIGINAL RESEARCH The Use of Noninvasive Ventilation in Emergency Department Patients With Acute Cardiogenic Pulmonary Edema: A Systematic Review Sean P. Collins, MD, MSC Lisa M. Mielniczuk,
CARDIOLOGY/ORIGINAL RESEARCH The Use of Noninvasive Ventilation in Emergency Department Patients With Acute Cardiogenic Pulmonary Edema: A Systematic Review Sean P. Collins, MD, MSC Lisa M. Mielniczuk,
Key words: atelectasis; endotracheal intubation; extubation; noninvasive ventilation; postoperative complications
 Outcomes of Patients With Acute Respiratory Failure After Abdominal Surgery Treated With Noninvasive Positive Pressure Ventilation* Samir Jaber, MD, PhD; Jean-Marc Delay, MD; Gérald Chanques, MD; Mustapha
Outcomes of Patients With Acute Respiratory Failure After Abdominal Surgery Treated With Noninvasive Positive Pressure Ventilation* Samir Jaber, MD, PhD; Jean-Marc Delay, MD; Gérald Chanques, MD; Mustapha
Non-invasive positive pressure ventilation in acute hypercapnic respiratory failure: clinical experience of a respiratory ward
 Monaldi Arch Chest Dis 2004; 61: 2, 94-101 ORIGINAL ARTICLE Non-invasive positive pressure ventilation in acute hypercapnic respiratory failure: clinical experience of a respiratory ward R. Scala, M. Naldi,
Monaldi Arch Chest Dis 2004; 61: 2, 94-101 ORIGINAL ARTICLE Non-invasive positive pressure ventilation in acute hypercapnic respiratory failure: clinical experience of a respiratory ward R. Scala, M. Naldi,
Noninvasive mechanical ventilation in early. failure and acute respiratory distress syndrome:
 REVIEW ARTICLE Noninvasive mechanical ventilation in early acute respiratory distress syndrome Alice Grassi 1, Giuseppe Foti 1,2, John G. Laffey 3, Giacomo Bellani 1,2 1 Department of Emergency and Intensive
REVIEW ARTICLE Noninvasive mechanical ventilation in early acute respiratory distress syndrome Alice Grassi 1, Giuseppe Foti 1,2, John G. Laffey 3, Giacomo Bellani 1,2 1 Department of Emergency and Intensive
Prolonged Invasive Ventilation Following Acute Ventilatory Failure in COPD* Weaning Results, Survival, and the Role of Noninvasive Ventilation
 CHEST Prolonged Invasive Ventilation Following Acute Ventilatory Failure in COPD* Weaning Results, Survival, and the Role of Noninvasive Ventilation Timothy G. Quinnell, MRCP; Samantha Pilsworth, BSc;
CHEST Prolonged Invasive Ventilation Following Acute Ventilatory Failure in COPD* Weaning Results, Survival, and the Role of Noninvasive Ventilation Timothy G. Quinnell, MRCP; Samantha Pilsworth, BSc;
COMPLICACIONS DE LA VENTILACIÓ MECÀNICA NO INVASIVA
 COMPLICACIONS DE LA VENTILACIÓ MECÀNICA NO INVASIVA Dr. Miquel Ferrer UVIIR, Servei de Pneumologia, Hospital Clínic, IDIBAPS, CibeRes, Barcelona. E- mail: miferrer@clinic.ub.es Barcelona, 3 de novembre
COMPLICACIONS DE LA VENTILACIÓ MECÀNICA NO INVASIVA Dr. Miquel Ferrer UVIIR, Servei de Pneumologia, Hospital Clínic, IDIBAPS, CibeRes, Barcelona. E- mail: miferrer@clinic.ub.es Barcelona, 3 de novembre
CPAP Reduces Hypoxemia After Cardiac Surgery (CRHACS Trial). A randomized controlled trial
 CPAP Reduces Hypoxemia After Cardiac Surgery (CRHACS Trial). A randomized controlled trial Backgrounds Postoperative pulmonary complications are most frequent after cardiac surgery and lead to increased
CPAP Reduces Hypoxemia After Cardiac Surgery (CRHACS Trial). A randomized controlled trial Backgrounds Postoperative pulmonary complications are most frequent after cardiac surgery and lead to increased
Suzuki et al. Journal of Intensive Care 2014, 2:5
 Suzuki et al. Journal of Intensive Care 2014, 2:5 RESEARCH Open Access Evaluation of noninvasive positive pressure ventilation after extubation from moderate positive end-expiratory pressure level in patients
Suzuki et al. Journal of Intensive Care 2014, 2:5 RESEARCH Open Access Evaluation of noninvasive positive pressure ventilation after extubation from moderate positive end-expiratory pressure level in patients
