Proposal to national Health Technology Assessments (Norway)
|
|
|
- Monica Cook
- 6 years ago
- Views:
Transcription
1 Forslagsskjema, Versjon mars 2014 Proposal to national Health Technology Assessments (Norway) Proposals to national Health Technology Assessments (HTA) will be published in its entirety. Please contact the Secretariat before submission if necessary information for completing the form cannot be published. The proposer know that this form will be published in its entirety: Contact information: Organisation: St Jude Medical Contact person: Marcus Simon: Manager Health technology assessment and reimbursement, International Phone: msimon@sjm.com Place and date: 1. Title of proposal: Continuous monitoring of pulmonary artery pressure via an implanted leadless and battery less pressure sensor for the management of patients with moderate to severe heart failure (New York Heart Association class III) Side 1 av 13
2 2. Brief description of the technology: The device can be implanted in the pulmonary artery of NYHA class III heart failure patients during a minimally invasive catheter based procedure. The sensor is implanted via a catheter introduced into the right femoral vein and advanced through the venous system into the pulmonary artery. The procedure is similar to a right heart catheterisation procedure (common in heart failure patients) and has a low complication rate and similar low risk profile to right heart catheterisation. The system consists of three components: the implantable device; the home monitoring unit and a secure database storing the recorded pressure data accessible by the physician responsible for that patients care. Patients record their pulmonary artery pressures once a day using the home monitoring unit which transmits this pressure recording to the database where it can be regularly reviewed by their physician. Weekly review of the pressure recordings by physicians is sufficient for the technology to be effective. 3. Brief description of current situation (Which technology (s) is currently in use? Status for technology (providing curative treatment, extended life etc.) Will the technology proposed assessed replace, or be in addition to current situation?) There are currently no alternative systems providing continuous pulmonary artery pressure monitoring. There are systems which report daily patient body weights in an effort to predict episodes of acute heart failure but these systems have not demonstrated the same efficacy as internal pressure monitoring. 4. The technology applies? New technology Side 2 av 13
3 A new recommended use or a new indication for an established technology A comparison of several technologies An existing technology already in use If yes - used in clinical practice? If yes - adopted in research / testing? Physicians can use the pulmonary artery pressure recordings to assist in managing the patient s medication. Physicians should prescribe treatment to keep patients pressures within an optimal therapeutic range. The pulmonary artery pressure rises in the days preceding episodes of acute heart failure. These events are life threatening if not treated quickly, treatment requires emergency admission to hospital, intensive monitoring and medical therapy in the first few days of the admission and a lengthy stay to stabilise patients. Currently patient symptoms are the only guide to impending hospitalisation and when symptoms manifest it is too late to avoid the hospitalisation. The pulmonary artery data can give an early warning of episodes of acute heart failure and allow physicians to make changes to those patients drug therapy in order to stabilise them before the event requires hospitalisation and before the event becomes life threatening. 5. The technology involves (several options are possible)? Pharmaceuticals Medical devices Procedures Screening Highly specialized services /national services Organisational structure of health services Other (Please describe) 6. The technology s utility area: Preventive health care Assessment and diagnosis Medical treatment Rehabilitation Specialist health services Primary health services Side 3 av 13
4 The technology provides diagnostic data to guide heart failure treatment. In contrast to other diagnostic technologies the implantable pulmonary artery pressure provides continuous diagnostic data for the lifetime of the patient, there is no battery. Therefore the treatment effect can be considered as a lifetime benefit. 7. Does the technology involve use of radiation (ionizing / non ionizing) Please shortly describe type of radiation, equipment and exposure 8. Which clinical disciplines are involved by the technology, and which patient groups are affected? (Are other groups affected by the technology (personnel, relatives)? The sensor should be implanted by physicians skilled in catheter based cardiac procedures. Sensors should be implanted in NYHA III heart failure patients with a history of heart failure hospitalisations as recommended by a specialised heart failure physician. Hospitals that are specialised in treating heart failure should decide how to integrate the pressure monitoring component into their existing heart failure management program. Some centres may want to divide the responsibility of regularly reviewing patient pressure data among a team of specialists, which could include specialist nurses as well as or instead of physicians whilst other physicians might prefer to do this task themselves. The choice of action based on changes in pulmonary pressure data should be made by the heart failure specialist physician responsible for that patient s treatment. 9. Which aspects are relevant for the assessment? (several options are possible) Clinical effectiveness Safety/adverse effect Costs/use of resources Cost efficiency Organisational consequences Ethical Legal Side 4 av 13
5 10. Please identify the main research question, as well as any sub questions ( in accordance with section 8): Category Criteria Population Patients with a diagnosis of moderate to severe HF (NYHA class III) for 3 months, on a stable and optimised medication regimen, and have had a HF-related hospitalisation within the previous 12 months Intervention Comparator Outcomes to be assessed Healthcare resources to be considered CardioMEMS HF System, in addition to usual practice Usual practice HF-related hospitalisations; QALYs; Mortality; Safety (device-related and procedure-related) Hospital stay Medical staff Nursing staff Medications Surgical devices and consumables 11. Please shortly describe why it is important to perform an HTA on the proposed technology The CardioMEMS system has randomised clinical evidence demonstrating its safety and efficacy in reducing heart failure hospitalisations in NYHA III heart failure patients with a history of heart failure hospitalisations. This is a new telemonitoring diagnostic technology available to patients in the US following FDA approval which although CE marked for use in Europe has not been evaluated within the context of European healthcare systems or by any HTA agencies. An HTA performed by a European HTA agency is now the next step in making this technology available to European heart failure patients. 12. Please comment on the proposed technology in relation to: Severity Side 5 av 13
6 Heart failure (HF) is a complex clinical syndrome that results from any structural or functional impairment of ventricular filling or ejection of blood. The ESC definition of heart failure is an abnormality of cardiac structure or function leading to a failure of the heart to deliver oxygen at a rate commensurate with the requirements of the metabolizing tissues, despite normal filling pressures (or only at the expense of increased filling pressures)[1]. Clinical definitions vary but the ESC suggest the following and use this in the latest update of their heart failure guidelines a syndrome in which patients have typical symptoms (e.g. breathlessness, ankle swelling, and fatigue) and signs (e.g. elevated jugular venous pressure, pulmonary crackles, and displaced apex beat) resulting from an abnormality of cardiac structure or function [2]. Diagnosis can be difficult and if a diagnosis is suspected based on clinical grounds (medical history, clinical signs and symptoms) then this should be supported and confirmed by objective evidence of cardiac dysfunction. The main causes of heart failure are structural abnormalities resulting from ischemic heart disease, although there are many other conditions which can lead to heart failure such as hypertension, cardiomyopathies, valvular and congenital heart disease, myocarditis, pulmonary hypertension and cardio-toxic substances. The cardinal manifestations of HF are dyspnoea and fatigue, which may limit exercise tolerance; and fluid retention, which may lead to pulmonary oedema and/or peripheral oedema. There are two distinct heart failure aetiologies heart failure with reduced ejection fraction (HF-REF, also called systolic heart failure) and heart failure with preserved ejection fraction (HF-PEF, also called diastolic heart failure. Treatment for both types is predominantly pharmacological although there is no convincing evidence to support any treatment for HF-PEF[2]. HF-REF patients with a broad ECG QRS complex (>120ms) and remaining in New York Heart Association (NYHA) class II to III despite drug therapy are indicated for implantation with cardiac resynchronisation devices and patients with narrow QRS with ICD s[2] HF is a progressive disease associated with high patient morbidity and mortality and a poor quality of life. Prognosis following a diagnosis of heart failure is poor and 5 year survival rates compare badly with those of most cancers[5], heart failure is incurable and whilst patients may die from other causes not directly linked to heart failure once diagnosed with heart failure they will not be cured of the syndrome by any currently available therapy. Patients with a heart failure diagnosis are generally referred to as suffering chronic heart failure and will be managed out of hospital in many cases by general practitioners. If onset or change in heart failure signs and symptoms is sudden then patients are considered to be suffering Acute Heart Failure (AHF). AHF is a life threatening condition usually resulting in urgent hospitalisation. Onset of AHF can vary from very sudden (perhaps triggered by ventricular arrhythmia or acute myocardial infarction MI ) to deterioration over a period of days or weeks, characterised by increasing dyspnoea or oedema[2]. AHF is treated pharmacologically, in general the aim is to stabilise patients using combinations of oxygen, diuretics and vasodilators. Opiates and inotropes are sometimes used and rarely mechanical circulatory support, non-invasive and occasionally invasive ventilation. A recently published study based on data from patients covered by the national health insurance general scheme in France highlights the burden that heart failure hospitalisations place on hospitals[7]. The study included 69,958 incident hospitalisations for heart failure. Mean length of stay for each hospitalisation was 9 days. Patients hospitalised for the first time with heart failure accounted for 1.2% of all patients hospitalised in France in 2009; 2.6% of all hospitalisations for patients aged years; 6.2% for those aged years and 10.9% of patients hospitalised aged 90 years and above. The mortality rate for these first hospitalisations was 6.4% and 4.4% during 30 days after discharge with no readmission for 75% of those deaths. In patients who survived 30 days after discharge 18% were readmitted at least once.[7] Side 6 av 13
7 Expected effect of treatment One previous randomised controlled trial, CHAMPION, has been conducted in the United States[3]. The primary efficacy endpoint of the CHAMPION trial was the rate of hospitalizations for heart failure (as adjudicated by an independent blinded Clinical Events Committee) during the first 6 months of Randomized Access. There were 84 heart failure hospitalizations in the Treatment group compared with 120 heart failure hospitalizations in the Control group. This difference between the groups represented a 28% reduction in the rate of hospitalization for heart failure in the Treatment group (0.32 hospitalizations per patient in the Treatment group vs hospitalizations per patient in the Control group, p = ), (Table 1). Treatment Group (n=270) Control Group (n=280) Number of Heart Failure Hospitalizations 6 Month Rates of Hospitalization for Heart Failure Hazard Ratio (95% CI) [p-value] ( ) p= Table 1: Primary Efficacy Endpoint- Rates of Hospitalization for Heart Failure during First 6 months of Randomized Access Side 7 av 13
8 Safety The study met the two primary safety endpoints: (1) freedom from device/system related complications (DSRC) and (2) freedom from sensor failure. The protocol prespecified objective performance criterion (OPC) were that at least 80% of patients were to be free from DSRC and at least 90% were to be free from pressure sensor failure. Of the 575 patients in the safety population, 567 (98.6%) were free from DSRC at 6 months (lower confidence limit 97.3%, p<0.0001) (Table 2). This lower limit of 97.3% is greater than the pre-specified OPC of 80%. There were no sensor explants or repeat implants and all sensors were operational at 6 months for a freedom from sensor failure of 100% (lower confidence limit 99.3%, p<0.0001) (Table 3). This lower limit of 99.3% is greater than the pre-specified OPC of 90%. Device/System Related Complications (n=575) Yes No Lower 95.2% Confidence Limit 2 Objective Performance Criterion (OPC) p-value 3 8 (1.4%) (98.6%) 97.3% 80% p< DSRCs (8 total) by group: Consented but not randomized (2), Treatment (3), Control (3) 2 Exact 95.2% Clopper-Pearson lower confidence limit 3 p-value from exact test of binomial proportions compared to 80% for all patients Table 2: Primary Safety Endpoint Freedom from Device/System Related Complications Pressure Sensor Failures (n=550) Yes No Lower 95.2% Confidence Limit 2 Objective Performance Criterion (OPC) p-value 3 0 (0.0%) 550 (100%) % 90% p< Pressure sensor failure counts by group: Treatment (0), Control (0) 2 Exact 95.2% Clopper-Pearson lower confidence limit 3 p-value from exact test of binomial proportions compared to 90% for all patients Table 3: Primary Safety Endpoint Freedom from Pressure Sensor Failures No additional device/system related complications or sensor failures occurred during the remainder of the Randomized Access period (beyond the 6-month primary endpoint period) or during the Open Access period of the trial. Hence, there were 8 device system related complications and no sensor failures over an experience of 1167 patient-years (mean follow-up period of 26 months with longest follow-up of 3.6 years). Side 8 av 13
9 Number of patients (in Norway) the proposed technology may be appropriate for? As of April 01, 2015, the population of Norway is 5,176,998.[8] The findings from the Hillingdon HF study in the United Kingdom showed that the incidence of definitive HF was 9.3/1000 per year with a mean age of the population with definitive heart failure being 77 years of age.[9] Doctors usually classify patients' HF according to the severity of their symptoms. The New York Heart Association (NYHA) Functional Classification is commonly used. It places patients in one of four categories based on how much they are limited during physical activity.[10] The initial state distribution of NYHA Class III patient is about 23%.[11] The probability of NYHA Class III patients that requires hospitalization in a six-month period is 0.2.[11] The following diagram shows the probability of NYHA Class III patients who may require hospitalization in a 12-month period. Diagram 1 The probability of NYHA Class III Patients who require hospitalization in a 12-month period The probability of NYHA Class III patients who may be hospitalised once in a 12-month period is 0.2* * *0.2 = By extension the estimated number of patients which may benefit from heart failure therapy guided by continuous pulmonary artery pressure monitoring are approximately 5,176,998*0.0093*0.23*0.36 = 3, In summary it is believed that close to 4,000 patients per annum could benefit from the technology (NYHA class III HF patients with at least one previous heart failure hospitalisation) Side 9 av 13
10 Use of health care resources (equipment, personnel etc) Elevations in PA pressures are observable several days prior to worsening signs and symptoms that lead to HF hospitalizations. Medication and/or other therapy changes made in response to elevated PA pressures allows for earlier intervention by physicians to prevent these events and improve clinical outcomes for their patients. An elevation of PA pressures should be considered a volume overloaded status. Response to these signs are dependent on the doctors clinical opinion but in most cases doctors start with intensification of diuretic therapy to reduce the elevated PA pressures followed by vasodilator therapy, primarily using long-acting nitro-glycerine therapy, in those patients where PA pressures continue to remain elevated in order to achieve successful volume depletion. Most will pursue a similar strategy as an episode of acute heart failure but of course the therapy can be less aggressive as there is more time to stabilise the patient prior to the volume overload triggering an episode of full decompensation. NICE have published a care pathway for the treatment of chronic heart failure and the CardioMEMS Heart failure system clearly fits within the treatment and monitoring section[4]. Indeed, pulmonary artery pressure monitors are referred to in this section and there is a NICE interventional procedure guidance (463) on insertion and use of implantable pulmonary artery pressure monitors in chronic heart failure [6]. The need to revise the existing national professional guidelines Norwegian guidelines for heart failure treatment are based on the European Society of Cardiology guidelines. Specialist centres, where this technology will be best implemented, develop their own care pathways based on these guidelines. Pulmonary artery pressure guided treatment using CardioMEMS can be easily integrated into these care pathways because the system does not replace guideline recommended therapy but offers an opportunity to optimise therapy based on real time monitoring of a disease relevant physiological signal.[12] Side 10 av 13
11 13. Please enter references to documentation about the method's efficiency and safety (eg. Former HTAs, Up to 10 references may be given. Do not send attachments at this stage of the process) 1. Abraham, W. T. et al. Wireless pulmonary artery haemodynamic monitoring in chronic heart failure: a randomised controlled trial. The Lancet 377, , doi: /s (11) (2011). 2. Abraham, W. T. et al. Safety and accuracy of a wireless pulmonary artery pressure monitoring system in patients with heart failure. American heart journal 161, , doi: /j.ahj (2011). 3. Abraham, W. T. et al. Trials of implantable monitoring devices in heart failure: which design is optimal? Nature reviews. Cardiology 11, , doi: /nrcardio (2014). 4. Adamson, P. B. et al. CHAMPION trial rationale and design: the long-term safety and clinical efficacy of a wireless pulmonary artery pressure monitoring system. J Card Fail 17, 3-10, doi: /j.cardfail (2011). 5. Adamson, P. B. et al. Wireless pulmonary artery pressure monitoring guides management to reduce decompensation in heart failure with preserved ejection fraction. Circulation. Heart failure 7, , doi: /circheartfailure (2014). 6. Benza, R. L. et al. Pulmonary hypertension related to left heart disease: Insight from a wireless implantable hemodynamic monitor. The Journal of heart and lung transplantation : the official publication of the International Society for Heart Transplantation, doi: /j.healun (2014). 7. Castro, P. F. et al. A wireless pressure sensor for monitoring pulmonary artery pressure in advanced heart failure: initial experience. The Journal of heart and lung transplantation : the official publication of the International Society for Heart Transplantation 26, 85-88, doi: /j.healun (2007). 8. Krahnke, J. S. et al. Heart Failure and respiratory hospitalizations are reduced in heart failure subjects with chronic obstructive pulmonary disease using an implantable pulmonary artery pressure monitoring device. J Card Fail, doi: /j.cardfail (2014). 9. Ritzema, J. et al. Physician-directed patient self-management of left atrial pressure in advanced chronic heart failure. Circulation 121, , doi: /circulationaha (2010). Side 11 av 13
12 14. Please provide the name of the manufacturers / suppliers regarding the technology if possible St Jude Medical Inc. One St Jude Medical Drive St Paul, Minnesota USA 15. Status for Marked authorization (MA) or CE-marking: (At what time is MA expected? Is there a planned time for marketing the proposed technology?) The CardioMEMS HF System first obtained CE marking in 2011 and the current CE marking was completed with BSI on 1st May The CardioMEMS HF System received US FDA approval on May 28, Additional relevant information, up to 300 words In order to put the treatment effect size of the CardioMEMS HF System into an appropriate context, the treatment effect observed in CHAMPION can be compared to the treatment effect observed in other pivotal HF drug trials for ACCF/AHA and ESC guideline directed medical therapies ACE inhibitors, angiotensin receptor blockers, beta blockers, aldosterone antagonists, and digoxin. The CardioMEMS HF System had an equivalent or greater treatment effect than HF drug therapy trials for HF hospitalization rates, mortality, deaths and HF hospitalization rates, and total deaths and all-cause hospitalization rates. These data demonstrate the substantial clinical improvement over standard of care physicians could provide to HF patients by using the CardioMEMS HF System. It is important to note that patients in the CHAMPION trial were required to have been treated with all appropriate drug and device treatments for heart failure at optimal or best-tolerated stable doses prior to enrolment in accordance with ACCF/AHA guidelines. Therefore, the treatment effect observed in the CHAMPION trial using the CardioMEMS HF System could be considered as incremental to the benefit associated with the current guideline recommended standard of care. References 1. Dickstein, K., et al., ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2008: the Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2008 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association of the ESC (HFA) and endorsed by the European Society of Intensive Care Medicine (ESICM). Eur Heart J, (19): p McMurray, J.J., et al., ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC. Eur Heart J, (14): p Abraham, W.T., et al., Wireless pulmonary artery haemodynamic monitoring in chronic heart failure: a randomised controlled trial. The Lancet, (9766): p (NICE), N.I.f.H.a.C.E., Chronic heart failure treatment and monitoring pathway, in Chronic heart failure pathway. 2014, UK. 5. Stewart, S., et al., More 'malignant' than cancer? Five-year survival following a first admission for heart failure. Eur J Heart Fail, (3): p (NICE), N.I.f.H.a.C.E., Insertion and use of implantable pulmonary artery pressure monitors in chronic heart failure, in Nice interventional procedure guidance Side 12 av 13
13 7. Tuppin, P., et al., First hospitalization for heart failure in France in 2009: patient characteristics and 30-day follow-up. Arch Cardiovasc Dis, (11): p Statistics Norway, 9. K. Guha and T. McDonagh, Heart Failure Epidemology: European Perspective. Curr Cardiol Rev May; 9(2): Classes of Heart Failure. American Heart Association. Heart-Failure_UCM_306328_Article.jsp 11. Patricia A. Cowper, PhD, et al., Economic Effects of Beta-Blocker Therapy in Patients with Heart Failure. Am J Med. 2004; 116: Tove Rosstad, et al., Development of a patient-centred care pathway across healthcare providers: a qualitative study. BMC Health Services Research 2013, 13:121. Side 13 av 13
National Horizon Scanning Centre. Irbesartan (Aprovel) for heart failure with preserved systolic function. August 2008
 Irbesartan (Aprovel) for heart failure with preserved systolic function August 2008 This technology summary is based on information available at the time of research and a limited literature search. It
Irbesartan (Aprovel) for heart failure with preserved systolic function August 2008 This technology summary is based on information available at the time of research and a limited literature search. It
Philip B. Adamson, MD, FACC
 Sensed Hemodynamics Coupled to Remote Patient Monitoring in Heart Failure: Has the Search for the Holy Grail Ended? Philip B. Adamson, MD, FACC Director, Heart Failure Institute at Oklahoma Heart Hospital
Sensed Hemodynamics Coupled to Remote Patient Monitoring in Heart Failure: Has the Search for the Holy Grail Ended? Philip B. Adamson, MD, FACC Director, Heart Failure Institute at Oklahoma Heart Hospital
1/28/2016. The Weight is Over! Heart Failure Epidemic. Heart Failure Epidemic. U.S. Census Bureau Projections. Burden on Society
 Remote Monitoring for Heart Failure: The Weight is Over! Heart Failure Epidemic Jamie Pelzel, MD Cardiologist, CentraCare Heart & Vascular Center Medical Director, CentraCare Heart Failure Program Kannel
Remote Monitoring for Heart Failure: The Weight is Over! Heart Failure Epidemic Jamie Pelzel, MD Cardiologist, CentraCare Heart & Vascular Center Medical Director, CentraCare Heart Failure Program Kannel
CARDIOMEMS HF SYSTEM HOW TO STAY ABOVE HEART FAILURE: TALKING TO YOUR PATIENT ABOUT THE
 CARDIOMEMS HF SYSTEM HOW TO STAY ABOVE HEART FAILURE: TALKING TO YOUR PATIENT ABOUT THE CARDIOMEMS HF SYSTEM This overview of clinical workflow best practices and patient talking points is based on in-depth
CARDIOMEMS HF SYSTEM HOW TO STAY ABOVE HEART FAILURE: TALKING TO YOUR PATIENT ABOUT THE CARDIOMEMS HF SYSTEM This overview of clinical workflow best practices and patient talking points is based on in-depth
Heart Failure 101 The Basic Principles of Diagnosis & Management
 Heart Failure 101 The Basic Principles of Diagnosis & Management Bill Tran, MD Non Invasive Cardiologist February 24, 2018 What the eye does not see and the mind does not know, does not exist. DH Lawrence
Heart Failure 101 The Basic Principles of Diagnosis & Management Bill Tran, MD Non Invasive Cardiologist February 24, 2018 What the eye does not see and the mind does not know, does not exist. DH Lawrence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Proposed Health Technology Appraisal. Serelaxin for treating acute decompensation of heart failure
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Serelaxin for treating acute decompensation of heart Draft scope (pre-referral) Draft remit/appraisal objective To
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Serelaxin for treating acute decompensation of heart Draft scope (pre-referral) Draft remit/appraisal objective To
BETTER HEART FAILURE MANAGEMENT FROM THE COMFORT OF YOUR HOME
 BETTER HEART FAILURE MANAGEMENT FROM THE COMFORT OF YOUR HOME Staying Ahead of Heart Failure with the CardioMEMS HF System The CardioMEMS HF System A UNIQUE APPROACH TO HEART FAILURE MANAGEMENT THAT CAN
BETTER HEART FAILURE MANAGEMENT FROM THE COMFORT OF YOUR HOME Staying Ahead of Heart Failure with the CardioMEMS HF System The CardioMEMS HF System A UNIQUE APPROACH TO HEART FAILURE MANAGEMENT THAT CAN
Disclosures. Overview. Goal statement. Advances in Chronic Heart Failure Management 5/22/17
 Disclosures Advances in Chronic Heart Failure Management I have nothing to disclose Van N Selby, MD UCSF Advanced Heart Failure Program May 22, 2017 Goal statement To review recently-approved therapies
Disclosures Advances in Chronic Heart Failure Management I have nothing to disclose Van N Selby, MD UCSF Advanced Heart Failure Program May 22, 2017 Goal statement To review recently-approved therapies
Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year
![Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year](/thumbs/76/74263761.jpg) PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
Slide 1. Slide 2. Slide 3. Managing Acute Heart Failure Trials and Tribulations. Declaration of
 Slide 1 Managing Acute Heart Failure Trials and Tribulations Martin R Cowie MD MSc FRCP FRCP (Ed) FESC Professor of Cardiology, Imperial College London m.cowie@imperial.ac.uk @ProfMartinCowie Slide 2 Declaration
Slide 1 Managing Acute Heart Failure Trials and Tribulations Martin R Cowie MD MSc FRCP FRCP (Ed) FESC Professor of Cardiology, Imperial College London m.cowie@imperial.ac.uk @ProfMartinCowie Slide 2 Declaration
Innovation therapy in Heart Failure
 Innovation therapy in Heart Failure P. Laothavorn September 2015 Topics of discussion Basic Knowledge about heart failure Standard therapy New emerging therapy References: standard Therapy in Heart Failure
Innovation therapy in Heart Failure P. Laothavorn September 2015 Topics of discussion Basic Knowledge about heart failure Standard therapy New emerging therapy References: standard Therapy in Heart Failure
Clinical Policy Title: Wireless pulmonary artery pressure monitoring devices for heart failure
 Clinical Policy Title: Wireless pulmonary artery pressure monitoring devices for heart failure Clinical Policy Number: 04.01.08 Effective Date: January 1, 2017 Initial Review Date: September 21, 2016 Most
Clinical Policy Title: Wireless pulmonary artery pressure monitoring devices for heart failure Clinical Policy Number: 04.01.08 Effective Date: January 1, 2017 Initial Review Date: September 21, 2016 Most
The Failing Heart in Primary Care
 The Failing Heart in Primary Care Hamid Ikram How fares the Heart Failure Epidemic? 4357 patients, 57% women, mean age 74 years HFSA 2010 Practice Guideline (3.1) Heart Failure Prevention A careful and
The Failing Heart in Primary Care Hamid Ikram How fares the Heart Failure Epidemic? 4357 patients, 57% women, mean age 74 years HFSA 2010 Practice Guideline (3.1) Heart Failure Prevention A careful and
Disclosures. Preventing Heart Failure Re-admissions in Deaths Due to Cardiovascular Disease (United States: ) Heart Failure
 29 th Annual Cardiology for Clinicians Spring Symposium Workshop #3 Alumni Hallway, Northeastern Conference Room, 1-9525 Thursday, May 5, 2016 Preventing Heart Failure Re-admissions in 2016 Leway Chen,
29 th Annual Cardiology for Clinicians Spring Symposium Workshop #3 Alumni Hallway, Northeastern Conference Room, 1-9525 Thursday, May 5, 2016 Preventing Heart Failure Re-admissions in 2016 Leway Chen,
CARDIOMEMS HF SYSTEM PATIENT MANAGEMENT CLINICAL QUICK GUIDE
 CARDIOMEMS HF SYSTEM PATIENT MANAGEMENT CLINICAL QUICK GUIDE CLINICAL QUICK GUIDE CARDIOMEMS HF SYSTEM Information in this Clinical Quick Guide is based on: In-depth clinician feedback 1 on the common
CARDIOMEMS HF SYSTEM PATIENT MANAGEMENT CLINICAL QUICK GUIDE CLINICAL QUICK GUIDE CARDIOMEMS HF SYSTEM Information in this Clinical Quick Guide is based on: In-depth clinician feedback 1 on the common
PRESS RELEASE. New NICE guidance will improve diagnosis and treatment of chronic heart failure
 Tel: 0845 003 7782 www.nice.org.uk Ref: 2010/118 ISSUED: WEDNESDAY, 25 AUGUST 2010 PRESS RELEASE New NICE guidance will improve diagnosis and treatment of chronic heart failure The National Institute for
Tel: 0845 003 7782 www.nice.org.uk Ref: 2010/118 ISSUED: WEDNESDAY, 25 AUGUST 2010 PRESS RELEASE New NICE guidance will improve diagnosis and treatment of chronic heart failure The National Institute for
Disclosures. Advances in Chronic Heart Failure Management 6/12/2017. Van N Selby, MD UCSF Advanced Heart Failure Program June 19, 2017
 Advances in Chronic Heart Failure Management Van N Selby, MD UCSF Advanced Heart Failure Program June 19, 2017 I have nothing to disclose Disclosures 1 Goal statement To review recently-approved therapies
Advances in Chronic Heart Failure Management Van N Selby, MD UCSF Advanced Heart Failure Program June 19, 2017 I have nothing to disclose Disclosures 1 Goal statement To review recently-approved therapies
The role of remote monitoring in preventing readmissions after acute heart failure
 The role of remote monitoring in preventing readmissions after acute heart failure October 20, 2017 Randall C Starling MD MPH FACC FAHA FESA FHFSA Professor of Medicine Kaufman Center for Heart Failure
The role of remote monitoring in preventing readmissions after acute heart failure October 20, 2017 Randall C Starling MD MPH FACC FAHA FESA FHFSA Professor of Medicine Kaufman Center for Heart Failure
PROCORALAN MAKING A STRONG ENTRY TO THE NEW ESC GUIDELINES FOR THE MANAGEMENT OF HEART FAILURE
 Press Release Issued on behalf of Servier Date: June 6, 2012 PROCORALAN MAKING A STRONG ENTRY TO THE NEW ESC GUIDELINES FOR THE MANAGEMENT OF HEART FAILURE The new ESC guidelines for the diagnosis and
Press Release Issued on behalf of Servier Date: June 6, 2012 PROCORALAN MAKING A STRONG ENTRY TO THE NEW ESC GUIDELINES FOR THE MANAGEMENT OF HEART FAILURE The new ESC guidelines for the diagnosis and
ESC Guidelines for the Diagnosis and Treatment of Acute and Chronic Heart Failure
 Patients t with acute heart failure frequently develop chronic heart failure Patients with chronic heart failure frequently decompensate acutely ESC Guidelines for the Diagnosis and A clinical response
Patients t with acute heart failure frequently develop chronic heart failure Patients with chronic heart failure frequently decompensate acutely ESC Guidelines for the Diagnosis and A clinical response
LIVE WEBINAR Boston Scientific External Use. Show and Distribute CRM AA-June 2017
 LIVE WEBINAR www.hf-channel.com 1 LIVE WEBINAR AGENDA 2 The use of diagnostics in the management of HF Patients Prof. Martin Cowie 3 The patient journey is complex 4 Remote monitoring Initially, telephone
LIVE WEBINAR www.hf-channel.com 1 LIVE WEBINAR AGENDA 2 The use of diagnostics in the management of HF Patients Prof. Martin Cowie 3 The patient journey is complex 4 Remote monitoring Initially, telephone
Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update)
 Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update) NICE guideline Apendix C The algorithms Draft for consultation, January 2010 Chronic
Chronic heart failure: management of chronic heart failure in adults in primary and secondary care (partial update) NICE guideline Apendix C The algorithms Draft for consultation, January 2010 Chronic
Clinical Policy Title: Wireless pulmonary artery pressure monitoring devices for heart failure
 Clinical Policy Title: Wireless pulmonary artery pressure monitoring devices for heart failure Clinical Policy Number: 04.01.08 Effective Date: January 1, 2017 Initial Review Date: September 21, 2016 Most
Clinical Policy Title: Wireless pulmonary artery pressure monitoring devices for heart failure Clinical Policy Number: 04.01.08 Effective Date: January 1, 2017 Initial Review Date: September 21, 2016 Most
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance FINAL SCOPE ENDURALIFE-powered CRT-D devices for the treatment of heart failure 1 Technology 1.1 Description of the technology
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance FINAL SCOPE ENDURALIFE-powered CRT-D devices for the treatment of heart failure 1 Technology 1.1 Description of the technology
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT
 NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT
 Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT Key Messages Heart Failure is Common Heart failure is complex Heart Failure is a major issue for the NHS Heart Failure has a worse prognosis
Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT Key Messages Heart Failure is Common Heart failure is complex Heart Failure is a major issue for the NHS Heart Failure has a worse prognosis
Heart Failure with Preserved EF (HFPEF) Epidemiology and management
 Heart Failure with Preserved EF (HFPEF) Epidemiology and management Karl Swedberg Senior Professor of Medicine Sahlgrenska Academy University of Gothenburg Gothenburg, Sweden e-mail: karl.swedberg@gu.se
Heart Failure with Preserved EF (HFPEF) Epidemiology and management Karl Swedberg Senior Professor of Medicine Sahlgrenska Academy University of Gothenburg Gothenburg, Sweden e-mail: karl.swedberg@gu.se
Neprilysin Inhibitor (Entresto ) Prior Authorization and Quantity Limit Program Summary
 Neprilysin Inhibitor (Entresto ) Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Indication Entresto Reduce the risk of cardiovascular (sacubitril/valsartan) death
Neprilysin Inhibitor (Entresto ) Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Indication Entresto Reduce the risk of cardiovascular (sacubitril/valsartan) death
Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment
 ESC 2012 27Aug - 3Sep, 2012, Munich, Germany Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment Marco Metra, MD, FESC Cardiology University
ESC 2012 27Aug - 3Sep, 2012, Munich, Germany Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment Marco Metra, MD, FESC Cardiology University
eplerenone 25, 50mg film-coated tablets (Inspra ) SMC No. (793/12) Pfizer Ltd
 eplerenone 25, 50mg film-coated tablets (Inspra ) SMC No. (793/12) Pfizer Ltd 08 June 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises NHS Boards
eplerenone 25, 50mg film-coated tablets (Inspra ) SMC No. (793/12) Pfizer Ltd 08 June 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises NHS Boards
CHANGING THE WAY HEART FAILURE IS TREATED. VAD Therapy
 CHANGING THE WAY HEART FAILURE IS TREATED VAD Therapy VAD THERAPY IS BECOMING AN ESSENTIAL PART OF HEART FAILURE PROGRAMS AROUND THE WORLD. Patients with advanced heart failure experience an impaired quality
CHANGING THE WAY HEART FAILURE IS TREATED VAD Therapy VAD THERAPY IS BECOMING AN ESSENTIAL PART OF HEART FAILURE PROGRAMS AROUND THE WORLD. Patients with advanced heart failure experience an impaired quality
Topic Page: congestive heart failure
 Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
Implementing the CardioMEMS HF System into the Management of Heart Failure Patients
 Implementing the CardioMEMS HF System into the Management of Heart Failure Patients Robert W. Hull MD FACC Associate Professor of Medicine WVU Heart Institute Co-director, Arrhythmia Service Director,
Implementing the CardioMEMS HF System into the Management of Heart Failure Patients Robert W. Hull MD FACC Associate Professor of Medicine WVU Heart Institute Co-director, Arrhythmia Service Director,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion and use of implantable pulmonary artery pressure monitors in chronic
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of insertion and use of implantable pulmonary artery pressure monitors in chronic
The right heart: the Cinderella of heart failure
 The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
Synopsis. Study title. Investigational Product Indication Design of clinical trial. Number of trial sites Duration of clinical trial / Timetable
 Synopsis Study title Investigational Product Indication Design of clinical trial Number of trial sites Duration of clinical trial / Timetable Repetitive levosimendan infusions for patients with advanced
Synopsis Study title Investigational Product Indication Design of clinical trial Number of trial sites Duration of clinical trial / Timetable Repetitive levosimendan infusions for patients with advanced
Therapeutic Targets and Interventions
 Therapeutic Targets and Interventions Ali Valika, MD, FACC Advanced Heart Failure and Pulmonary Hypertension Advocate Medical Group Midwest Heart Foundation Disclosures: 1. Novartis: Speaker Honorarium
Therapeutic Targets and Interventions Ali Valika, MD, FACC Advanced Heart Failure and Pulmonary Hypertension Advocate Medical Group Midwest Heart Foundation Disclosures: 1. Novartis: Speaker Honorarium
WHAT S NEW IN HEART FAILURE
 WHAT S NEW IN HEART FAILURE Drugs, Devices and Diagnostics John M. Herre, MD, FACC, FACP Director, Advanced Heart Failure Program Sentara Helathcare Professor of Medicine Eastern Virginia Medical School
WHAT S NEW IN HEART FAILURE Drugs, Devices and Diagnostics John M. Herre, MD, FACC, FACP Director, Advanced Heart Failure Program Sentara Helathcare Professor of Medicine Eastern Virginia Medical School
Heart Failure Challenges and Unmet needs
 Heart Failure Challenges and Unmet needs. Angelo Auricchio, MD FESC Director, Cardiac Electrophysiology Programme, Fondazione Cardiocentro Ticino, Lugano, Switzerland Professor of Cardiology, University
Heart Failure Challenges and Unmet needs. Angelo Auricchio, MD FESC Director, Cardiac Electrophysiology Programme, Fondazione Cardiocentro Ticino, Lugano, Switzerland Professor of Cardiology, University
Remote management of heart failure using implanted devices and formalized follow-up procedures (REM-HF)
 Remote management of heart failure using implanted devices and formalized follow-up procedures (REM-HF) Martin R Cowie Professor of Cardiology, Imperial College London (Royal Brompton Hospital) London,
Remote management of heart failure using implanted devices and formalized follow-up procedures (REM-HF) Martin R Cowie Professor of Cardiology, Imperial College London (Royal Brompton Hospital) London,
2016 ESC Heart Failure Guidelines: what is new? Piotr Ponikowski Wroclaw, Poland
 2016 ESC Heart Failure Guidelines: what is new? Piotr Ponikowski Wroclaw, Poland Disclosures Consultancy fees and speaker s honoraria from: Amgen, Servier, Novartis, Johnson & Johnson, Merck, Berlin Chemie,
2016 ESC Heart Failure Guidelines: what is new? Piotr Ponikowski Wroclaw, Poland Disclosures Consultancy fees and speaker s honoraria from: Amgen, Servier, Novartis, Johnson & Johnson, Merck, Berlin Chemie,
Heart Failure Management. Waleed AlHabeeb, MD, MHA Assistant Professor of Medicine Consultant Heart Failure Cardiologist
 Heart Failure Management Waleed AlHabeeb, MD, MHA Assistant Professor of Medicine Consultant Heart Failure Cardiologist Heart failure prevalence is expected to continue to increase¹ 21 MILLION ADULTS WORLDWIDE
Heart Failure Management Waleed AlHabeeb, MD, MHA Assistant Professor of Medicine Consultant Heart Failure Cardiologist Heart failure prevalence is expected to continue to increase¹ 21 MILLION ADULTS WORLDWIDE
COPD as a comorbidity of heart failure in elderly patients
 COPD as a comorbidity of heart failure in elderly patients Professor Mitja Lainscak, MD, PhD, FESC, FHFA Departments of Cardiology and Research&Education, General Hospital Celje Faculty of Medicine, University
COPD as a comorbidity of heart failure in elderly patients Professor Mitja Lainscak, MD, PhD, FESC, FHFA Departments of Cardiology and Research&Education, General Hospital Celje Faculty of Medicine, University
The NEW Heart Failure Guidelines
 The NEW Heart Failure Guidelines Daily Practice HF scenario of the Case Presentations HF as a complex and heterogeneous syndrome Several proposed pathophysiological mechanisms involving the heart and the
The NEW Heart Failure Guidelines Daily Practice HF scenario of the Case Presentations HF as a complex and heterogeneous syndrome Several proposed pathophysiological mechanisms involving the heart and the
Incidence. 4.8 million in the United States. 400,000 new cases/year. 20 million patients with asymptomatic LV dysfunction
 Heart Failure Diagnosis According to the Working Group in Heart Failure, CHF is a syndrome where the diagnosis has the following essential components: A combination of: Symptoms, typically breathlessness
Heart Failure Diagnosis According to the Working Group in Heart Failure, CHF is a syndrome where the diagnosis has the following essential components: A combination of: Symptoms, typically breathlessness
NICE Chronic Heart Failure Guidelines in Adults 2018
 NICE Chronic Heart Failure Guidelines in Adults 2018 The Whys, Whats and Hows of the importance of effectively managing heart failure in Primary Care and the community. Foreword Dr Clare J Taylor, General
NICE Chronic Heart Failure Guidelines in Adults 2018 The Whys, Whats and Hows of the importance of effectively managing heart failure in Primary Care and the community. Foreword Dr Clare J Taylor, General
Diagnosis and management of Chronic Heart Failure in 2018: What does NICE say? PCCS Meeting Issues and Answers Conference Nottingham
 Diagnosis and management of Chronic Heart Failure in 2018: What does NICE say? PCCS Meeting Issues and Answers Conference Nottingham NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Chronic heart failure
Diagnosis and management of Chronic Heart Failure in 2018: What does NICE say? PCCS Meeting Issues and Answers Conference Nottingham NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Chronic heart failure
Treat the Numbers and Not the Patients The Revolution of Pulmonary Artery Pressure Guided Medical Therapy in Heart Failure
 Treat the Numbers and Not the Patients The Revolution of Pulmonary Artery Pressure Guided Medical Therapy in Heart Failure Stan Skaluba, M.D. Advanced Heart Failure Program Advocate Heart Institute AHI
Treat the Numbers and Not the Patients The Revolution of Pulmonary Artery Pressure Guided Medical Therapy in Heart Failure Stan Skaluba, M.D. Advanced Heart Failure Program Advocate Heart Institute AHI
The Role of Information Technology in Disease Management: A Case for Heart Failure
 The Role of Information Technology in Disease Management: A Case for Heart Failure Teresa De Peralta, MSN, APN-C Heart Failure Product Workflow Consultant Medtronic Population Management Level 3: As patient
The Role of Information Technology in Disease Management: A Case for Heart Failure Teresa De Peralta, MSN, APN-C Heart Failure Product Workflow Consultant Medtronic Population Management Level 3: As patient
Lo scompenso cardiaco: le riammissioni, un problema in parte evitabile?
 Lo scompenso cardiaco: le riammissioni, un problema in parte evitabile? E. Gronda UO di Cardiologia e Ricerca Clinica IRCCS MultiMedica Dipartimento Cardiovascolare Interaziendale Gruppo MultiMedica Heart
Lo scompenso cardiaco: le riammissioni, un problema in parte evitabile? E. Gronda UO di Cardiologia e Ricerca Clinica IRCCS MultiMedica Dipartimento Cardiovascolare Interaziendale Gruppo MultiMedica Heart
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal. Drugs for the treatment of pulmonary arterial hypertension
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Draft remit / appraisal objective: Draft scope To appraise the clinical and cost effectiveness
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Draft remit / appraisal objective: Draft scope To appraise the clinical and cost effectiveness
Management Strategies for Advanced Heart Failure
 Management Strategies for Advanced Heart Failure Mary Norine Walsh, MD, FACC Medical Director, HF and Cardiac Transplantation St Vincent Heart Indianapolis, IN USA President American College of Cardiology
Management Strategies for Advanced Heart Failure Mary Norine Walsh, MD, FACC Medical Director, HF and Cardiac Transplantation St Vincent Heart Indianapolis, IN USA President American College of Cardiology
ESC Guidelines. ESC Guidelines Update For internal training purpose. European Heart Journal, doi: /eurheart/ehn309
 ESC Guidelines Update 2008 ESC Guidelines Heart failure update 2008 For internal training purpose. 0 Agenda Introduction Classes of recommendations Level of evidence Treatment algorithm Changes to ESC
ESC Guidelines Update 2008 ESC Guidelines Heart failure update 2008 For internal training purpose. 0 Agenda Introduction Classes of recommendations Level of evidence Treatment algorithm Changes to ESC
Estimated 5.7 million Americans with HF. 915, 000 new HF cases annually, HF incidence approaches
 Heart Failure: Management of a Chronic Disease Jenny Bauerly RN, CHFN, APRN-BC Heart Failure (HF) Definition A complex clinical syndrome that can result from any structural or functional cardiac disorder
Heart Failure: Management of a Chronic Disease Jenny Bauerly RN, CHFN, APRN-BC Heart Failure (HF) Definition A complex clinical syndrome that can result from any structural or functional cardiac disorder
Chronic heart failure in adults: diagnosis and management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Chronic heart failure in adults: diagnosis and management NICE guideline: short version Draft for consultation, March 0 This guideline covers diagnosing
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Chronic heart failure in adults: diagnosis and management NICE guideline: short version Draft for consultation, March 0 This guideline covers diagnosing
8:30-10:30 WS #4: Cardiology :00-13:00 WS #11: Cardiology 101 (Repeated)
 Professor Ralph Stewart Cardiologist Auckland City Hospital Green Lane Cardiovascular Research Unit Auckland Heart Group Fiona Stewart Cardiologist Green Lane Hospital National Women's Hospital Professor
Professor Ralph Stewart Cardiologist Auckland City Hospital Green Lane Cardiovascular Research Unit Auckland Heart Group Fiona Stewart Cardiologist Green Lane Hospital National Women's Hospital Professor
Cardiac resynchronisation therapy (biventricular pacing) for the treatment of heart failure
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal for the treatment of heart failure Final scope Appraisal objective To appraise the clinical and cost effectiveness of cardiac
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal for the treatment of heart failure Final scope Appraisal objective To appraise the clinical and cost effectiveness of cardiac
Dronedarone for the treatment of non-permanent atrial fibrillation
 Dronedarone for the treatment of non-permanent atrial Issued: August 2010 last modified: December 2012 guidance.nice.org.uk/ta197 NICE has accredited the process used by the Centre for Health Technology
Dronedarone for the treatment of non-permanent atrial Issued: August 2010 last modified: December 2012 guidance.nice.org.uk/ta197 NICE has accredited the process used by the Centre for Health Technology
Talking points included in this deck are for internal/speaker use only, and are not to be distributed.
 1 Talking points included in this deck are for internal/speaker use only, and are not to be distributed. Before presenting the CHAMPION study, I would like to provide a brief overview of the CardioMEMS
1 Talking points included in this deck are for internal/speaker use only, and are not to be distributed. Before presenting the CHAMPION study, I would like to provide a brief overview of the CardioMEMS
Technology appraisal guidance Published: 28 November 2012 nice.org.uk/guidance/ta267
 Ivabradine adine for treating chronic heart failure Technology appraisal guidance Published: 28 November 2012 nice.org.uk/guidance/ta267 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Ivabradine adine for treating chronic heart failure Technology appraisal guidance Published: 28 November 2012 nice.org.uk/guidance/ta267 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
The ACC Heart Failure Guidelines
 The ACC Heart Failure Guidelines Fakhr Alayoubi, Msc,R Ph President of SCCP Cardiology Clinical Pharmacist Assistant Professor At King Saud University King Khalid University Hospital Riyadh-KSA 2017 ACC/AHA/HFSA
The ACC Heart Failure Guidelines Fakhr Alayoubi, Msc,R Ph President of SCCP Cardiology Clinical Pharmacist Assistant Professor At King Saud University King Khalid University Hospital Riyadh-KSA 2017 ACC/AHA/HFSA
How might biomarkers and other strategies help establish adequacy of care?
 How might biomarkers and other strategies help establish adequacy of care? James L. Januzzi, Jr, MD, FACC, FESC Hutter Family Professor of Medicine, Harvard Medical School Cardiology Division, Massachusetts
How might biomarkers and other strategies help establish adequacy of care? James L. Januzzi, Jr, MD, FACC, FESC Hutter Family Professor of Medicine, Harvard Medical School Cardiology Division, Massachusetts
Value of Continuous Monitoring of. Pulmonary Artery Pressures in Heart Failure. Financial Relationship Disclosure. Liviu Klein MD, MS
 Liviu Klein MD, MS Associate Professor Director, Mechanical Circulatory Support and Heart Failure Device Programs Liviu.Klein@ucsf.edu Value of Continuous Monitoring of Pulmonary Artery Pressures in Heart
Liviu Klein MD, MS Associate Professor Director, Mechanical Circulatory Support and Heart Failure Device Programs Liviu.Klein@ucsf.edu Value of Continuous Monitoring of Pulmonary Artery Pressures in Heart
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 27 May 2009
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 May 2009 CARDENSIEL 1.25 mg, film-coated tablet B/30 (CIP code: 352 968-1) CARDENSIEL 2.5 mg, film-coated tablet
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 May 2009 CARDENSIEL 1.25 mg, film-coated tablet B/30 (CIP code: 352 968-1) CARDENSIEL 2.5 mg, film-coated tablet
Gerasimos Filippatos MD, FESC, FCCP, FACC
 Gerasimos Filippatos MD, FESC, FCCP, FACC Head of HF Unit at Athens University Hospital, Greece President (2014-2016) of the HF Association of the European Society of Cardiology (ESC) Served as Chair of
Gerasimos Filippatos MD, FESC, FCCP, FACC Head of HF Unit at Athens University Hospital, Greece President (2014-2016) of the HF Association of the European Society of Cardiology (ESC) Served as Chair of
2/3/2017. Objectives. Effective Heart Failure Management through Evidence Based Practice and Innovation
 Effective Heart Failure Management through Evidence Based Practice and Innovation Jennifer Bauerly RN, CHFN, APRN-BC CentraCare Heart and Vascular Center Objectives Describe the scope and impact of heart
Effective Heart Failure Management through Evidence Based Practice and Innovation Jennifer Bauerly RN, CHFN, APRN-BC CentraCare Heart and Vascular Center Objectives Describe the scope and impact of heart
Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes?
 Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor
Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor
A patient with decompensated HF
 A patient with decompensated HF Professor Michel KOMAJDA University Pierre & Marie Curie Pitie Salpetriere Hospital Department of Cardiology Paris (France) Declaration Of Interest 2010 Speaker : Servier,
A patient with decompensated HF Professor Michel KOMAJDA University Pierre & Marie Curie Pitie Salpetriere Hospital Department of Cardiology Paris (France) Declaration Of Interest 2010 Speaker : Servier,
Remote Monitoring in Heart Failure
 Remote Monitoring in Heart Failure Michael P Frenneaux 1 ; Nicholas D Gollop 1 ; Brodie L Loudon 1 ; Sathish Parasuraman 1 1 Professor Michael P Frenneaux, MD, FRCP, FRACP, FACC, FESC (Corresponding Author)
Remote Monitoring in Heart Failure Michael P Frenneaux 1 ; Nicholas D Gollop 1 ; Brodie L Loudon 1 ; Sathish Parasuraman 1 1 Professor Michael P Frenneaux, MD, FRCP, FRACP, FACC, FESC (Corresponding Author)
Acute heart failure, beyond conventional treatment: persisting low output
 Acute heart failure, beyond conventional treatment: persisting low output Alexandre Mebazaa, FESC Hôpital Lariboisière, Université Paris 7 U942 Inserm Conflict of Interest Lecture fee: Orion No other conflicts
Acute heart failure, beyond conventional treatment: persisting low output Alexandre Mebazaa, FESC Hôpital Lariboisière, Université Paris 7 U942 Inserm Conflict of Interest Lecture fee: Orion No other conflicts
1000 Lives Key Components of Reliable, Evidence-Based Chronic Heart Failure Care how do we compare?
 1000 Lives Key Components of Reliable, Evidence-Based Chronic Heart Failure Care how do we compare? Dr Nerys Davies, GPST Ms B. Davies, Specialist Nurse (Heart Failure) Dr J. Taylor, Consultant Cardiologist
1000 Lives Key Components of Reliable, Evidence-Based Chronic Heart Failure Care how do we compare? Dr Nerys Davies, GPST Ms B. Davies, Specialist Nurse (Heart Failure) Dr J. Taylor, Consultant Cardiologist
Heart Failure (HF) - Primary Care Flow Charts. Pre diagnosis Symptoms or signs suggestive of HF
 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts. Symptoms or signs suggestive of HF. Pre diagnosis. Refer to the Heart Failure Clinic at VHK for
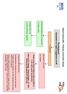 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
Chronic heart failure
 Chronic heart failure Management of chronic heart failure in adults in primary and secondary care Issued: August 2010 NICE clinical guideline 108 guidance.nice.org.uk/cg108 NICE has accredited the process
Chronic heart failure Management of chronic heart failure in adults in primary and secondary care Issued: August 2010 NICE clinical guideline 108 guidance.nice.org.uk/cg108 NICE has accredited the process
Summary Protocol ISRCTN / NCT REVIVED-BCIS2 Summary protocol version 4, May 2015 Page 1 of 6
 Summary Protocol REVIVED-BCIS2 Summary protocol version 4, May 2015 Page 1 of 6 Background: Epidemiology In 2002, it was estimated that approximately 900,000 individuals in the United Kingdom had a diagnosis
Summary Protocol REVIVED-BCIS2 Summary protocol version 4, May 2015 Page 1 of 6 Background: Epidemiology In 2002, it was estimated that approximately 900,000 individuals in the United Kingdom had a diagnosis
Heart Failure. Guillaume Jondeau Hôpital Bichat, Paris, France
 Heart Failure Guillaume Jondeau Hôpital Bichat, Paris, France Epidemiology Importance of PEF Europe I-PREFER study. Abstract: 2835 Prevalence of HF Preserved LV systolic Function older (65 vs 62 y, p
Heart Failure Guillaume Jondeau Hôpital Bichat, Paris, France Epidemiology Importance of PEF Europe I-PREFER study. Abstract: 2835 Prevalence of HF Preserved LV systolic Function older (65 vs 62 y, p
Implantierbarer hämodynamischer Monitor bei Herzinsuffizienzpatienten
 22. Dresdner Symposium Herz und Gefäße 2016 Implantierbarer hämodynamischer Monitor bei Herzinsuffizienzpatienten Ein sinnvolles neues Monitoring-Tool? Dr. Mattias Roser, MD Head of Electrophysiology Dept.
22. Dresdner Symposium Herz und Gefäße 2016 Implantierbarer hämodynamischer Monitor bei Herzinsuffizienzpatienten Ein sinnvolles neues Monitoring-Tool? Dr. Mattias Roser, MD Head of Electrophysiology Dept.
Title BRITISH SOCIETY FOR HEART FAILURE NATIONAL HEART FAILURE AUDIT APRIL MARCH 2016
 Title BRITISH SOCIETY FOR HEART FAILURE NATIONAL HEART FAILURE AUDIT 1 APRIL 2015 - MARCH 2016 NICOR (National Institute for Cardiovascular Outcomes Research) is a partnership of clinicians, IT experts,
Title BRITISH SOCIETY FOR HEART FAILURE NATIONAL HEART FAILURE AUDIT 1 APRIL 2015 - MARCH 2016 NICOR (National Institute for Cardiovascular Outcomes Research) is a partnership of clinicians, IT experts,
Program Metrics. New Unique ID. Old Unique ID. Metric Set Metric Name Description. Old Metric Name
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Diagnosis & Management of Heart Failure. Abena A. Osei-Wusu, M.D. Medical Fiesta
 Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Polypharmacy - arrhythmic risks in patients with heart failure
 Influencing sudden cardiac death by pharmacotherapy Polypharmacy - arrhythmic risks in patients with heart failure Professor Dan Atar Head, Dept. of Cardiology Oslo University Hospital Ullevål Norway 27.8.2012
Influencing sudden cardiac death by pharmacotherapy Polypharmacy - arrhythmic risks in patients with heart failure Professor Dan Atar Head, Dept. of Cardiology Oslo University Hospital Ullevål Norway 27.8.2012
Heart Failure. GP Update Refresher 18 th January 2018
 GP Update Refresher 18 th January 2018 Heart Failure Dr. Alexander Lyon Senior Lecturer and Consultant Cardiologist Clinical Lead in Cardio-Oncology Royal Brompton Hospital, London UK President of British
GP Update Refresher 18 th January 2018 Heart Failure Dr. Alexander Lyon Senior Lecturer and Consultant Cardiologist Clinical Lead in Cardio-Oncology Royal Brompton Hospital, London UK President of British
Heart Failure Treatments
 Heart Failure Treatments Past & Present www.philippelefevre.com Background Background Chronic heart failure Drugs Mechanical Electrical Background Chronic heart failure Drugs Mechanical Electrical Sudden
Heart Failure Treatments Past & Present www.philippelefevre.com Background Background Chronic heart failure Drugs Mechanical Electrical Background Chronic heart failure Drugs Mechanical Electrical Sudden
Heart Failure from a GP perspective
 Heart Failure from a GP perspective Jane Gilmour, Alison Wright Clinical Nurse Specialists for Heart Failure The Heart failure Team Dr Ganesan Kumar- Consultant Cardiologist Dr D Maras- Staff Grade Cardiology
Heart Failure from a GP perspective Jane Gilmour, Alison Wright Clinical Nurse Specialists for Heart Failure The Heart failure Team Dr Ganesan Kumar- Consultant Cardiologist Dr D Maras- Staff Grade Cardiology
ESC Guidelines for the Diagnosis and Treatment of Chronic Heart Failure
 ESC Guidelines for the Diagnosis and Treatment of Chronic Heart Failure - 2005 Karl Swedberg Professor of Medicine Department of Medicine Sahlgrenska University Hospital/Östra Göteborg University Göteborg
ESC Guidelines for the Diagnosis and Treatment of Chronic Heart Failure - 2005 Karl Swedberg Professor of Medicine Department of Medicine Sahlgrenska University Hospital/Östra Göteborg University Göteborg
I have no disclosures. Disclosures
 I have no disclosures Disclosures What is Heart Failure? Heart Failure (HF) A complex clinical syndrome where patients present with symptoms (i.e. dyspnea, fatigue, fluid retention) that result from any
I have no disclosures Disclosures What is Heart Failure? Heart Failure (HF) A complex clinical syndrome where patients present with symptoms (i.e. dyspnea, fatigue, fluid retention) that result from any
Title BRITISH SOCIETY FOR HEART FAILURE NATIONAL HEART FAILURE AUDIT
 Title BRITISH SOCIETY FOR HEART FAILURE NATIONAL HEART FAILURE AUDIT APRIL 2014 - MARCH 2015 1 National Heart Failure Audit April 2014-March 2015 NICOR (National Institute for Cardiovascular Outcomes Research)
Title BRITISH SOCIETY FOR HEART FAILURE NATIONAL HEART FAILURE AUDIT APRIL 2014 - MARCH 2015 1 National Heart Failure Audit April 2014-March 2015 NICOR (National Institute for Cardiovascular Outcomes Research)
Performance and Quality Measures 1. NQF Measure Number. Coronary Artery Disease Measure Set
 Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
HFpEF. April 26, 2018
 HFpEF April 26, 2018 (J Am Coll Cardiol 2017;70:2476 86) HFpEF 50% or more (40-71%) of patients with CHF have preserved LV systolic function. HFpEF is an increasingly frequent hospital discharge. Outcomes
HFpEF April 26, 2018 (J Am Coll Cardiol 2017;70:2476 86) HFpEF 50% or more (40-71%) of patients with CHF have preserved LV systolic function. HFpEF is an increasingly frequent hospital discharge. Outcomes
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Efficacy of beta-blockers in heart failure patients with atrial fibrillation: An individual patient data meta-analysis
 Efficacy of beta-blockers in heart failure patients with atrial fibrillation: An individual patient data meta-analysis Dipak Kotecha, MD PhD on behalf of the Selection of slides presented at the European
Efficacy of beta-blockers in heart failure patients with atrial fibrillation: An individual patient data meta-analysis Dipak Kotecha, MD PhD on behalf of the Selection of slides presented at the European
Advanced Heart Failure Management. Dr Andrew Hannah Consultant Cardiologist Aberdeen Royal Infirmary
 Advanced Heart Failure Management Dr Andrew Hannah Consultant Cardiologist Aberdeen Royal Infirmary Grading of heart failure Mr WY age 73 3/12 dyspnoea, fatigue and some ankle oedema PMH: hypertension
Advanced Heart Failure Management Dr Andrew Hannah Consultant Cardiologist Aberdeen Royal Infirmary Grading of heart failure Mr WY age 73 3/12 dyspnoea, fatigue and some ankle oedema PMH: hypertension
A Global perspective on Heart Failure: What needs to change? Martin R Cowie London, United Kingdom
 A Global perspective on Heart Failure: What needs to change? Martin R Cowie London, United Kingdom Global perspective on heart failure: what needs to change? Martin R Cowie Professor of Cardiology National
A Global perspective on Heart Failure: What needs to change? Martin R Cowie London, United Kingdom Global perspective on heart failure: what needs to change? Martin R Cowie Professor of Cardiology National
Pravin Manga Division of Cardiology Department of Medicine University of Witwatersrand
 Pravin Manga Division of Cardiology Department of Medicine University of Witwatersrand Overview Definition Epidemiology Biomarkers Treatment Clinical Heart Failure: Syndrome in which patients have typical
Pravin Manga Division of Cardiology Department of Medicine University of Witwatersrand Overview Definition Epidemiology Biomarkers Treatment Clinical Heart Failure: Syndrome in which patients have typical
Long-Term Care Updates
 Long-Term Care Updates July 2015 By Amy Friedman Wilson, PharmD Heart failure (HF) is a clinical condition in which ventricular filling or ejection of blood is structurally or functionally impaired. 1
Long-Term Care Updates July 2015 By Amy Friedman Wilson, PharmD Heart failure (HF) is a clinical condition in which ventricular filling or ejection of blood is structurally or functionally impaired. 1
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Report on the Expert Group Meeting of Paediatric Heart Failure, London 29 November 2010
 Report on the Expert Group Meeting of Paediatric Heart Failure, London 29 November Clinical trials in Paediatric Heart Failure List of participants: Michael Burch, Hugo Devlieger, Angeles Garcia, Daphne
Report on the Expert Group Meeting of Paediatric Heart Failure, London 29 November Clinical trials in Paediatric Heart Failure List of participants: Michael Burch, Hugo Devlieger, Angeles Garcia, Daphne
