In uremia, plasma levels of anti-protein C and anti-protein S antibodies are associated with thrombosis
|
|
|
- Christopher Ford
- 6 years ago
- Views:
Transcription
1 Kidney International, Vol. 68 (2005), pp In uremia, plasma levels of anti-protein C and anti-protein S antibodies are associated with thrombosis DANIELA MOLINO,DOMENICO DE LUCIA, ROSAMAROTTA, ALESSANDRA PERNA, CINZIA LOMBARDI, MASSIMO CIRILLO, and NATALE GASPARE DE SANTO First Division of Nephrology; and Department of General Pathology, Clinical Pathology and Laboratory of Hemostasis and Thrombosis, Second University of Naples, Naples, Italy In uremia, plasma levels of anti-protein C and anti-protein S antibodies are associated with thrombosis. Background. Vascular access thrombosis is an important cause of morbidity in patients with end-stage renal failure on maintenance hemodialysis (MHD). However, little is known about its risk factors. The present study was undertaken to evaluate the role of coagulation factors, fibrinolytic factors, and antiphospholipid antibodies (apl). In particular, we have evaluated the role of anti-protein C and anti-protein S antibodies in patients on MHD with and without thrombosis because no data are available in the literature. Methods. The study group comprised 30 patients with thrombotic complications (TC), 40 patients matched for age, sex, and dialytic age with no thrombotic complications (NTC) and 400 controls. We have measured: anti-protein C antibodies, antiprotein S antibodies, anticardiolipin antibodies (ACA), antib2-glycoprotein antibodies (b2-gpi), and anti-prothrombin antibodies (apt), along with prothrombin time, fibrinogen, plasminogen, protein C, protein S, anti-thrombin III, APCresistance test, D-dimer, tissue-type plasminogen s activator, plasminogen activator inhibitor-1 (PAI-1), prothrombin fragment 1+2, factors of the intrinsic and extrinsic pathway, C- reactive protein, and homocysteine. Results. There were no significant differences between groups for prothrombin time, fibrinogen, plasminogen, protein C, protein S, anti-thrombin III, activated protein C (APC) resistance, D-dimer, tpa, C-reactive protein, Factors II, X, and VII. The anti-b2-gp1 and apt were elevated in both TC and NTC patients, compared to the control group. Significant differences between TC and NTC groups were found for anti-protein C and anti-protein S antibodies, ACA-IgM, PAI-1, Factor VIII, prothrombin fragments 1+2, and homocysteine. Conclusion. The most novel finding was a significant elevation of anti-protein C antibodies and anti-protein S antibodies in the TC group (i.e., in patients on MHD with thrombosis of vascular access). It indicates that other pathogenetic mechanisms in addition to endothelial damage may cause hypercoagulability in uremia. Keywords: hemostasis, dialysis, thrombosis, endothelial damage, antiprotein C antibody. Received for publication April 26, 2004 and in revised form December 18, 2004 and March 10, 2005 Accepted for publication April 14, 2005 C 2005 by the International Society of Nephrology Patients with chronic renal failure on maintenance hemodialysis (MHD) frequently undergo thrombotic events that occur at the site of vascular access, as well as in the coronary, cerebral, and retinal arteries [1 6]. The pathogenetic mechanism is still unknown. Available data have disclosed a state of hypofibrinolysis characterized by elevated plasma levels of the inhibitor of tissue activator of plasminogen (PAI-1) in uremia. Data on other coagulation factors are still being debated [7 11]. Some studies have pointed to increased levels of Factor VII and Factor VIII [12]; other studies have disclosed a reduction in the concentration of activated Factor XII. Reduced plasma concentrations of protein C (PC), anti-thrombin III (AT III), and plasminogen have been described, but the data need further confirmation [13]. Progress in the clinical pathology of thrombotic events has focused on antiphospholipid (apl) antibodies (Abs), a heterogeneous family present in systemic lupus erythematosus where thrombotic phenomena occur frequently. These antibodies are also found in patients without lupus. They have been considered to be primers for the hypercoagulative state, although available literature does not provide a clear-cut mechanism. In fact, apl have been found in a variety of clinical conditions, such as venous and arterial thrombosis, thrombocytopenia, cerebrovascular ischemic diseases, recurrent abortion, and cutaneous lesions [14]. It is now possible to measure lupus anticoagulant antibodies (LAC), anticardiolipin antibodies (ACA), antibodies to b2-glycoprotein type I (b2-gpi), anti-prothrombin antibodies (apt) [15 19], anti-protein C antibodies, and anti-protein S antibodies. The presence of apl might induce a prothrombotic state by blocking protein C and protein S, potent natural anticoagulants [15]. Plasma from patients with elevated apl is resistant to activated protein C and, therefore, has a tendency to formation of thrombin. These antibodies could bind with negatively charged target molecules represented by cofactors to Factors V and VIII, thus causing continuously elevated levels of plasma thrombin. Current 1223
2 1224 Molino et al: Thrombosis of vascular access in MHD Table 1. Characteristics of patients with thrombotic complications (TC) and patients with no thrombotic complications (NTC) TC NTC P value a Number of patients N M/F 15/15 22/ Age years 54 ± 4 53 ± Dialytic age months (mean) 30 ± ± Hemoglobin g/dl 11.8 ± ± Lipoprotein a mg/dl 16.5 ± ± Diabetes mellitus% Hypertension% Cigarette smoking% Hyperlipidemia% Percent of patients requiring at least 2 AVF% History of TIA% Ischemic cardiopathy% Amputation of a limb% Arterial thrombotic events% History of aspirin use% a By chi-square analysis for categorial variables (sex, diabetes, hypertension, smoking, hyperlipidemia, need of at least 2 AVF, TIA, ischemic cardiopathy, amputation of a limb, arterial thrombotic events, aspirin use); by ANOVA for continuous variables (age, dialytic age, hemoglobin, and lipoprotein a). theory holds that apl may induce a procoagulant activity in endothelial cells and monocytes. Recently, apl, specifically LAC, IgG, and IgM anticardiolipin antibodies (ACA-IgG and ACA-IgM), antiprothrombin antibodies, and anti-2-gpi antibodies, have been extensively studied in patients on MHD [15 18]. However, the role of these antibodies in the pathogenesis of thrombosis is still controversial [19 22] and further studies on their potential procoagulative role are indicated. In summary, the data suggest that vascular endothelial cell damage associated with thrombin formation is implicated in vascular occlusion in primary and secondary apl syndrome. The present study explores the alternative or additional role of a different class of antibodies, anti-protein C and anti-protein S, on vascular endothelial cell damage associated with hypercoagulability, in patients on MHD with and without thrombosis of vascular access. METHODS Patients and controls A total of 70 patients on MHD for 24 to 36 months were enrolled for the study. Their characteristics are given in Table 1. Thirty patients presented thrombotic complications of the vascular access and other vascular locations, such as coronaries, retina, and inferior limbs, and were assigned to the TC group. Forty patients were without thrombotic complications and were termed the NTC group (Table 1). All patients were dialyzed using an end-to-side veinartery anastomosis of the cephalic vein and radial artery. Arteriovenous fistula (AVF) was monitored by Doppler Table 2. Characteristics of vascular access at beginning of the study Type of vascular access TC NTC Arteriovenous fistula 100% 100% Time to first event of thrombosis After 3 months of dialysis 33.3% 0% After 6 months of dialysis 13.3% 0% After 12 months of dialysis 20% 0% After 24 months of dialysis 33.3% 0% Doppler analysis Sluggish flow 0% 0% Stenosis 0% 0% Recirculation Glucose test (positivity) 0% 0% ultrasound every 6 months for dysfunction (Table 2). Patients with alterations of the primary fistula, for example, stenosis of a portion of vascular access, were not included in the study. Absence of recirculation was assessed every 3 months by a conventional glucose test. All patients received conventional hemodialysis with bicarbonate bath and used polysulfone membranes. The average length of each dialysis was 4 hours, average blood flow was 300 to 350 ml/min, and the adequacy of dialysis was assessed on a monthly basis using the Kt/V, which was kept in the range 1.3 to 1.4. Heparin was used as anticoagulant in patients in all patients. Patients were studied along with 400 healthy age- and sex-matched blood donor volunteers recruited at our University Hospital. The causes of uremia in patients of the TC group were: polycystic kidney disease (PCKD) (4 cases), chronic pyelonephritis (14 cases), nephroangiosclerosis (4 cases), diabetic nephropathy (5 cases), glomerulonephritis of unknown origin (3 cases). In the NTC group causes for uremia were: PCKD (6 cases), chronic pyelonephritis (14 cases), nephroangiosclerosis (6 cases), diabetic nephropathy (7 cases), focal and segmental glomerulosclerosis (3 cases), and glomerulonephritis of unknown origin (4 cases). Hypertension, cigarette smoking, diabetes, and dyslipidemia are now equally distributed between groups. All patients, with the exception of those with PCKD, received erythropoietin. There were significant differences (P < ) between TC and NTC patients: 60% of TC patients needed at least 2 AVF, one third had history of TIA, 23% of them had ischemic cardiopathy, 16.6% underwent amputation of a limb, 100% had arterial thrombotic events. Laboratory investigations All patients were tested for prothrombin time (PT), activated partial thromboplastin time (APTT), fibrinogen (Fg), coagulation Factors of the intrinsic and extrinsic pathway, antithrombin III (AT-III), protein C (PC), protein S (PS), resistance to activated protein C (APCresistance), prothrombin fragment 1+2 (F1+2), plasminogen (PLG), tissue type plasminogen activator (tpa),
3 Molino et al: Thrombosis of vascular access in MHD 1225 plasminogen activator inhibitor-1 (PAI-1), homocysteine (Hcy), C-reactive protein, anticardiolipin antibodies type M and G (ACA-IgM and ACA-IgG), anti-prothrombin antibodies type M and G (apt IgM and IgG), anti-b 2 GPI, anti-protein C antibodies, and anti-protein S antibodies. Genetic analysis of Factor V Leiden mutation and prothrombin mutation were tested in all patients as very common cardiovascular risk factors. Blood samples (4.5 ml) were collected in siliconetreated glass tubes by venipuncture, immediately before the midweek hemodialysis session. Blood samples in TC patients were collected 6 weeks after the acute ischemic event. In this respect, the hemostatic storm was definitively quenched. All patients and controls were asked to provide base-line EDTA anticoagulated samples of whole blood. Trisodium citrate (0.1 mol/l) in 1/10 volume ratio was added as anticoagulant. Citrated blood was centrifuged for 20 minutes at 1700g at 4 C. The supernatant was divided into aliquots and stored at 80 C. Coagulation factors were determined with a one-stage clotting assay using commercially available reagents. Fibrinogen concentration was determined in an automated coagulation laboratory autoanalyzer (ACL 2000; Instrumentation Laboratory, Milan, Italy). Protein C (Berichrom Protein C, Dade Behring; Marburg, Germany) and S (Instrumentation Laboratory) plasma levels were estimated with a functional clotting assay. Tissue-type plasminogen activator and PAI-1 were assayed by enzyme immunoassay (Hyphen Biomed, Andresy, France). Prothrombin fragment 1+2 levels was measured by an enzyme-linked immunosorbent assay (ELISA) method (Enzygnost F1+2 micro; Dade Behring). Anticardiolipin antibodies (ACA-IgG and IgM), antiprothrombin antibodies (apt-igm and IgG), and antib 2 GPI (Hyphen Biomed) were measured by ELISA using commercially available kits (Hyphen Biomed). Anti-protein C and anti-protein S were measured by ELISA using an experimental kit (Hyphen Biomed). Hcy concentration was determined according to Perna et al [23]. Briefly, the procedure involves a preliminary step of reduction and release from albumin, using tri-n-butyl-phosphine in dimethylformamide, followed by precolumn derivatization with ammonium 7-fluorobenzo-2-oxa-1, 3-diazole-4-sulphonate (SBD-F). Separation was accomplished on a C18, 5-lm, mm, reverse phase column ( Luna; Phenomenex, Torrance, CA, USA). The mobile phase was 0.1 mol/l KH 2 PO 4, ph 2.1, containing 4% acetonitrile, with a flow rate of 1.0 ml/min. Micromolar concentrations of homocysteine are referred to 1 liter. Detection conditions were optimized for homocysteine. Fluorescence intensities were measured with excitation at 385 nm and emission at 515 nm using a Shimadzu RF-535 fluorescence detector (Shimadzu Co., Kyoto, Japan), equipped Table 3. Factor II, Factor V, Factor VII, Factor X, ATIII, protein C, protein S, plasminogen (PLG), APCr tpa, homocysteine, C-reactive protein, PAI-1, F1+2, and Factor VIII in TC, NTC, and controls Variables TC NTC Controls P FII% 90 ± 5 86 ± ± 25 n.s. FV% 76 ± ± 7 80 ± 20 n.s. FVII% 96 ± ± ± 25 n.s. FX% 102 ± ± ± 25 n.s. ATIII% 103 ± ± 3 98 ± 15 n.s. Protein C% 92 ± 4 91 ± 4 98 ± 15 n.s. Functional 80 ± 4 93 ± 6 98 ± 15 n.s. protein S% PLG mg/dl 87 ± ± ± 12 n.s. APCr N ratio 1 ± ± 0.01 >0.75 n.s. tpa ng/ml 2 ± ± ± 0.5 n.s. C-reactive protein 1.19 ± ± ± 0.10 P = Homocysteine 27.8 ± ± ± 1.48 P = PAI-1 ng/ml 49 ± ± ± 11.5 P = 0.01 F1+2 ng/ml 5.4 ± ± ± 0.35 P = F VIII% 180 ± ± ± 2.75 P = with a Shimadzu Chromatopac C-R6A data processor (Shimadzu Co.). C-reactive protein measurement was carried out according to an immunoenzymatic method (Roche Diagnostics, Milan, Italy). Genomic DNA (200 ng) from peripheral white blood cells was extracted according to standard international procedures. Factor V G 1691A mutation and Factor II G20210A polymorphisms were searched using polymerase chain reaction (PCR) technique in a second laboratory, where the investigators were unaware of each subject s status as a case patient or control. Statistical analysis Statistical evaluation was performed using the Statistical Package for Social Science (SPSS 6.1 for Macintosh, Chicago, IL, USA). The analysis of variance (ANOVA) test or chi-square was used to determine the significance of differences between groups. Data were expressed as mean values ± standard deviation (SD) and as prevalence. Values of P < 0.05 were considered significant. RESULTS No significant difference was found between TC, NTC, and controls with respect to plasma Factor II, Factor V, Factor VII, Factor X, protein C, protein S, ATIII, PLG, APC-resistance and tpa (Table 3). Also, data on PT, PTT, and fibrinogen (not included) did not disclose statistical differences between TC and NTC patients. C-reactive protein was increased in TC and NTC patients in comparison with healthy controls (P = 0.001). Hcy was increased significantly both in TC and NTC compared to the control group (P = 0.001) (Table 3). Patients with TC showed a significant elevation of Factor VIII procoagulant concentration (P = 0.007), a
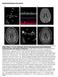
4 1226 Molino et al: Thrombosis of vascular access in MHD Table 4. Prevalence of anti-phospholipid antibodies in patients TC and NTC Anti-phospholipid Normal TC NTC antibodies values prevalence% prevalence% P value a anti-protein S U/mL <10 47% 8% anti-protein C U/mL <10 100% 6% ACA IgG U/mL <7 84% 56% ACA IgM U/mL <5 64% 15% apt IgG U/mL <7 34% 37% apt IgM U/mL <7 14% 12% anti-b2 GPI U/mL <5 57% 32% Significance for P <.05. a Chi-square test. Table 5. Absolute values of anti-phospholipid antibodies in patients TC, NTC, and controls Anti-phospholipid antibodies TC NTC Control P anti-protein S U/mL 10.1 ± ± ± anti-protein C U/mL 24.3 ± ± ± ACA IgG U/mL 13 ± ± ± ACA IgM U/mL 7.0 ± ± ± apt IgG U/mL 5.65 ± ± ± apt IgM U/mL 7.48 ± ± ± anti-b2 GPI U/mL 5.51 ± ± ± significant elevation of F1+2 plasma level (P = 0.006), and an increased PAI-1 level (P = 0.01) compared to NTC and the control group (Table 3). Factor VIII did not correlate significantly with CRP. The antiphospholipid levels are reported in Table 4 and Table 5. Elevated anti-protein C (IgM) plasma levels are found in 100% of TC patients and in only 6% of NTC patients (P = ), with a significant difference with the ANOVA test (P = 0.001). Anti-protein S (IgG) plasma levels were elevated in 47% of TC patients and in 8% of NTC patients (P = ), with a significant difference with the ANOVA tests. Positivity for anti-b 2 GPI was found in 57% of TC patients and 32% of NTC patients (P = 0.056), with a significant difference in mean ± SD plasma levels at ANOVA test (Table 5). The prevalence of ACA-IgG antibodies was 84% in TC and 56% in NTC (P = 0.115), while the prevalence of ACA IgM antibodies was 64% in TC and 15% in NTC, respectively (P = 0.001), with a significant difference for ANOVA test only for ACA IgM plasma levels (P = 0.001). No differences in the prevalence of apt-igg and apt-igm antibodies were found between TC and NTC patients, while a significant difference was found at ANOVA test considering the different group of subjects for apt-igg and apt-igm (P = 0.04). Genetic analysis shows that Factor V Leiden mutation was found in 1 TC patient and in none of the patients of the NTC group. One patient over 70 represents 1.4% of all patients. The prothrombin mutation was not found in both groups. In the general population Factor V mutation is found in about 2% of healthy subjects, while prothrombin polymorphism heterozygosity is found in 4%. DISCUSSION Anti-protein C and anti-protein S antibodies were measured for the first time in uremic patients on maintenance hemodialysis. All available knowledge in the field has been obtained either in patients with systemic lupus erythematosus (SLE) or in patients without SLE but with venous thromboembolism [24 27]. The data demonstrate a significantly greater prevalence of anti-protein C antibodies and anti-protein S antibodies in hemodialyzed patient on MHD with thrombosis of vascular access (TC), a novel finding indicating that in uremia, in addition to endothelial damage [28, 29], other pathogenetic mechanisms may cause hypercoagulability. In order to understand the importance of present results, it might be instrumental to assign a proper role to each of the factors studied by including them in a possible model of hemostatic derangement in uremia. PAI-1 is a molecule of endothelial origin and is overproduced in endothelial dysfunctions, such as in uremia. Patients with thrombotic complications show a significant increase in PAI-1, FVIII, F1+2 compared to controls, as well as to patients without thrombotic complications. The excess PAI-1 released in the bloodstream inhibits tpa and blocks the fibrinolysis system, causing hypofibrinolysis (i.e., low efficiency thrombolysis). Despite hypofibrinolysis, an increase of D-dimers was observed, but it should be stressed that their increase is lower than expected, considering that the coagulation pathway is activated in excess (Fig. 1). F1+2, an indicator of abnormal activation of the coagulation pathway, is a molecule released during the activation of prothrombin to thrombin. Increased levels of F1+2 could be related to the presence of antiprothrombin antibodies (Abs) and anti-b2 GP-I Abs. In fact, anti-prothrombin blocks the prothrombinase complex in a status of activation. This mechanism continuously stimulates the transformation of prothrombin to thrombin and the consequent release of F1+2 (Fig. 1). In turn, anti-b2 GP-I antibodies compete with Factor V in binding b2 GP-I. Therefore, when b2 GP-I is bound to the antibody, it is no longer available to bind Factor V and present it to the protein C system, which is the pathway that inactivates activated Factor V [30]. Factor V (not inactivated) forms the prothrombinase complex and increases the formation of thrombin and F1+2 (Fig. 1). Increased Factor VIII causes activation of the coagulation pathway because Factor VIII (Fig. 1) is an important cofactor in the activation of Factor X by the tenase complex. Elevated Factor VIII could be potentially prothrombotic either by increasing the stability of the tenase complex or by conferring a relative resistance
5 Molino et al: Thrombosis of vascular access in MHD 1227 Secondary hemostasis FXII Intrinsic pathway aps apc APC FXIIa T.F. FXIa FVIIIa FXIa Ca ++ Xa FVIIIa Ca ++ PL FVa Prothrombin PL Extrinsic pathway ATIII apt Fg Thrombin T β 2 -GPI ACA F1+2 PLG PS TM PAI-1 tpa Endothelial cells Fibrin Fig. 1. Synopsis of all intrinsic and extrinsic pathways of secondary hemostasis that lead to thrombin formation and fibrin deposition. White squares and circles indicate derangements in patients on maintenance hemodialysis. Broken lines indicate inhibition. to APC degradation. Elevated levels of Factor VIII were associated with venous thrombosis in the Leiden Thrombophilia Study, and the association has also been observed subsequently [31]. It is well known that an increase in Factor VIII is due to endothelial damage as well to the presence of the antiprotein C antibodies. Elevations of Factor VIII in the present study were not associated with the inflammatory state (PCR vs. FVIII, R = 0.112, P = 0.742). Hcy levels produce interactions with the anticoagulant pathway, as well as with the fibrinolytic system and the endothelial functions. These interactions lead to inhibition of thrombomodulin-dependent activated protein C system, which, in turn, leads to persistent thrombin activation and formation. The activated protein C system also interferes with tpa endothelial release into the vasculature, thus predisposing to hypofibrinolysis. Finally, high Hcy plasma levels may interfere with subendothelial cell proliferation via metalloproteinase inducible gene activation such as MPP-9 subtype. Biologically plausible mechanisms of vascular damage have been suggested, including effects on endothelium, platelet functions, coagulation factors, and lipoprotein oxidation. Interactions between Hcy plasma levels and conventional risk factors may have implications for risk management and for our understanding of the causes of vascular access thrombosis [32, 33]. In order to understand the possible role for anti-protein C and anti-protein S antibodies in the hemostatic derangement in uremia, one should start from the fact that anti-protein C antibodies induce hypercoagulability by inhibiting the protein C system, and by blocking the enzymatic inactivation of Factor VIII, resulting in an increase of activated Factor VIII. This, in turn, stimulates the formation of thrombin, which, after saturating all the thrombomodulin binding sites, is diverted to the formation of fibrin. The thrombin excess increases the procoagulation pathway rather than showing the anticoagulation effect of binding with thrombomodulin. Activated protein C acts as an anticoagulant by cleaving multiple bonds and thereby destroying the membrane-bound activated forms of coagulation Factors V (Va) and VIII (VIIIa). This reaction is accelerated by protein S acting as a cofactor. Like protein C, protein S is a glycoprotein that undergoes vitamin K dependent post-translational carboxylations to form gamma-carboxyglutamic acid ( Gla ) residues that allow its binding to negatively charged phospholipid surfaces. Protein S acts as a cofactor by increasing the affinity of activated protein C for phospholipids in the formation of the membrane-bound protein C-ase complex. Anti-protein S antibodies target protein S, which is cofactor of protein Cact. We can hypothesize that antiprotein S antibodies induce hypercoagulability by inhibiting the protein C system and by blocking the enzymatic inactivation of Factor VIII, resulting in an increase of activated Factor VIII (Fig. 1). The present data do not assign a role to Factor V and prothrombin mutations; however, further investigation is warranted to define the role of genetic analysis in vascular access thrombosis. For the sake of comparison, the above data are presented in Table 6 along with data from some very relevant papers in the field. In the table, one can appreciate the
6 1228 Molino et al: Thrombosis of vascular access in MHD Table 6. Summary of principal studies on coagulation in hemodialysis patients Year of Number of Vascular Values of PAI-1 Values of F1+2 Values of FVIII Values of Hcy Prevalence of Prevalence of Prevalence of Prevalence of Authors publication patients access ng/ml nmol/l % lmol/l apc-abs aps-abs ACA IgG-abs b2-gpi-abs Not indicated Not studied Not studied 108 ± 9 Not studied Not studied Not studied Not studied Not studied Vaziri ND et al patients (17 men and 14 women) Not studied Not studied Not studied Not studied Not studied Not studied 6% Not studied Prakash R et al patients Arteriovenous fistula (AVF) 57.5 ± 33.6 FD 3.09 ± 0.96 FD AVF 24.7 ± 21.1 WFD 3.14 ± 0.87 WFD Not studied Not studied Not studied Not studied Not studied Not studied De Marchi S et al patients (18 men and 12 women) Manns BJ et al patients AVF Not studied Not studied Not studied 29.8 Not studied Not studied Yes Not studied Segarra A et al patients Not indicated 35.4 ± 7.2 Not studied Not studied Not studied Not studied Not studied Not studied Not studied (120 men and 80 women) AVF Not studied Not studied Not studied Not studied Not studied Not studied 6.7% 4.3% Palomo I et al patients (96 men and 112 women) 49 ± 3.3 TC 5.4 ± 1.3 TC 180 ± 25 TC 27.8 ± 1.3 TC 100% TC 47% TC 84% TC 57% TC Present data 70 patients AVF 33 ± 3.4 NTC 4.5 ± 0.9 NTC 122 ± 8 NTC 23.6 ± 1.5 NTC 6% NTC 8% NTC 56% NTC 32% NTC role of our data and the time course of advancement in the field. It is evident that previous studies on coagulation in uremia have mainly focused their attention on differences in coagulation cascade, and/or on anticardiolipin antibodies and lupus anticoagulant, without screening for different subclasses of autoantibodies against phospholipid, endothelial, or platelet antigens. CONCLUSION We conclude that thrombotic complications in uremic patients are the result of changes in the secondary hemostasis and in fibrinolysis, differentiating them from hemorrhagic complications due to changes in primary hemostasis. The alterations of secondary hemostasis and fibrinolysis are due to endothelial damage and to the additive effects of some classes of antiphospholipid antibodies. These changes, for unknown reasons, are more severe in some patients, who are consequently more prone to thrombotic complications. Studies on the antigens of vascular endothelium to which autoantibodies bind might provide a further insight into their pathogenicity for thrombosis in patients on MHD. ACKNOWLEDGMENTS The study was supported by Italian Space Agency (ASI), the Ministry for University and Research, and by the University of Naples. The authors wish to express their warmest thanks to Molly Fudge Mastrangelo (Ph.D.) and to Giovanni Mastrangelo (M.D.), Cumberland (Maryland- USA), for their critical review of the manuscript. Reprint requests to Natale Gaspare De Santo, First Division of Nephrology, Second University of Naples, Via Pansini, , Napoli, Italy. nataleg.desanto@unina2.it REFERENCES 1. VAZIRI ND, GONZALES EC, WANG J, et al: Blood coagulation, fibrinolytic, and inhibitory proteins in end-stage renal disease: Effect of hemodialysis. Am J Kidney Dis 23: , RABELIN KTJ, ZWAGINGER JJ, KROMANS HA, et al: Thrombosis and haemostasis in renal disease. Kidney Int 46: , FELDMAN HI, HELD PJ, HUTCHINSON JT, et al: Haemodialysis vascular access morbidity in the United States. Kidney Int 43: , VAZIRI ND, TOOHEY J, PAULE P, et al: Coagulation abnormalities in patients with end-stage renal disease treated with hemodialysis. Int J Artif Organs 7: , VANHERWEGHEM JL, YASSINE T, GOLDMANN M, et al: Subclavian vein thrombosis: A frequent complication of subclavian vein cannulation for hemodialysis. Clin Nephrol 26: , OPATRNY K, JR., MARES J, VIT L, et al: Fibrinolysis and metabolic disturbances in hemodialysis patients. Nieren- und Hochdruckkrankheiten 11: , OPATRNY K, JR., ZEMANOVÀ P, MARES J, et al: Fibrinolysis defect in long term hemodialysis patients with type 2 diabetes mellitus and its relation to metabolic disorders. Am J Nephrol 22: , DE MARCHI S, FALLETI E, GIACOMELLO R, et al: Risk factors for vascular disease and arteriovenous fistula dysfunction in hemodialysis patients. JAmSoc Nephrol 7: , SEGARRA A, CHACON P, MARTINEZ-EYARRE C, et al: Circulating levels of plasminogen activator inhibitor type-1, tissue plasminogen activator, and thrombomodulin in hemodialysis patients: Biochemical
7 Molino et al: Thrombosis of vascular access in MHD 1229 correlations and role as independent predictors of coronary artery stenosis. JAmSoc Nephrol 12: , VAZIRI ND, TOOHEY J, PAULE P, et al: Coagulation abnormalities in patients with end-stage renal disease treated with hemodialysis. Int J Artif Organs 7: , ISHII Y, YANO S, KANAI H, et al: Evaluation of blood coagulationfibrinolysis system in patients receiving chronic hemodialysis. Nephron 73: , BASKIN E, DUMAN O, BESBAS N, et al: Hypercoagulopathy in a hemodialysis patient: Are elevations in Factors VII and VIII effective? Nephron 83:180, LAI K, YIN JA, YUEN PMP, et al: Effect of hemodialysis on protein C, protein S and antithrombin II levels. Am J Kidney Dis 17:38 42, PALOMO I, PEREIRA J, ALARCON M, et al: Vascular access thrombosis is not related to presence of antiphospholipid antibodies in patients on chronic hemodialysis. Nephron 92: , DUCLOUX D, FLOREA A, REBIBOU JM, et al: Anti-beta2-glycoprotein I and anti-prothrombin antibodies in haemodialysis patients. Nephrol Dial Transplant 12:2466, ADLER S, SZCZECH L, QURESHI A, et al: IgM anticardiolipin antibodies are associated with stenosis of vascular access in hemodialysis patients but do not predict thrombosis. Clin Nephrol 56: , ASHERSON RA, HARRIS EN: Anticardiolipin antibodies-clinical associations. Postgrad Med J 62: , MANNS BJ, BURGESS ED, PARSONS HG, et al: Hyperhomocysteinemia, anticardiolipin antibody status, and risk for vascular access thrombosis in hemodialysis patients. Kidney Int 55: , PRAKASH R, MILLER CC 3RD, SUKI WN: Anticardiolipin antibody in patients on maintenance hemodialysis and its association with recurrent arteriovenous graft thrombosis. Am J Kidney Dis 26: , MOLINO D, DE SANTO NG, MAROTTA R, et al: Plasma levels of plasminogen activator inhibitor type 1, Factor VIII, prothrombin activation fragment 1+2, anticardiolipin, and antiprothrombin antibodies are risk factors for thrombosis in hemodialysis patients. Semin Nephrol 24: , CHEW SL, LINS RL, DAELEMANS R, et al: Are antiphospholipid antibodies clinically relevant in dialysis patients? Nephrol Dial Transplant 14: , ANGLES-CANO E, GUILLIN MC: Antiphospholipid antibodies and the coagulation cascade. Clin Chem 47: , PERNA AF, INGROSSO D, DE SANTO NG, et al: Mechanism of erythrocyte accumulation of methylation inhibitor S- adenosylhomocysteine in uremia. Kidney Int 47: , NOJIMA J, KURATSUNE H, SUEHISA E, et al: Acquired activated protein C resistance associated with anti-protein S antibody as a strong risk Factor for DVT in non-sle patients. Thromb Haemost 88: , NOJIMA J, KURATSUNE H, SUEHISA E, et al: Association between the prevalence of antibodies to beta(2)-glycoprotein I, prothrombin, protein C, protein S, and annexin V in patients with systemic lupus erythematosus and thrombotic and thrombocytopenic complications. Clin Chem 47: , NOJIMA J: Association between anti-phospholipid antibodies and thrombotic complications in systemic lupus erythematosus. Rinsho Byori 51: , PENGO V, BIASIOLO A, BROCCO T, et al: Autoantibodies to phospholipid-binding plasma proteins in patients with thrombosis and phospholipid-reactive antibodies. Thromb Haemost 75: , SPITTLE MA, HOENICH NA, HANDELMAN GJ, et al: Oxidative stress and inflammation in hemodialysis patients. Am J Kidney Dis 38: , BORAWSKI J, NAUMNIK B, PAWLAK K, et al: Endothelial dysfunction marker von Willebrand Factor antigen in haemodialysis patients: Associations with pre-dialysis blood pressure and the acute phase response. Nephrol Dial Transplant 16: , ATSUMI T, KHAMASHTA A, AMENGUAL O, et al: Binding of anticardiolipin antibodies to protein C via beta2-glycoprotein I (beta2-gpi): A possible mechanism in the inhibitory effect of antiphospholipid antibodies on the protein C system. Clin Exp Immunol 112: , KOUKE-MARCHANT K: Genetic polymorphisms associated with venous and arterial thrombosis. Arch Pathol Lab Med 126: , PERNA AF, INGROSSO D, DE SANTO NG: Homocysteine and oxidative stress. Amino Acids 25: , PERNA AF, INGROSSO D, LOMBARDI C, et al: Possible mechanisms of homocysteine toxicity. Kidney Int 84: , 2003
Daniela Molino,*,, Natale G. De Santo,* Rosa Marotta,*,, Pietro Anastasio,* Mahrokh Mosavat, and Domenico De Lucia
 Plasma Levels of Plasminogen Activator Inhibitor Type 1, Factor VIII, Prothrombin Activation Fragment 1 2, Anticardiolipin, and Antiprothrombin Antibodies are Risk Factors for Thrombosis in Hemodialysis
Plasma Levels of Plasminogen Activator Inhibitor Type 1, Factor VIII, Prothrombin Activation Fragment 1 2, Anticardiolipin, and Antiprothrombin Antibodies are Risk Factors for Thrombosis in Hemodialysis
Diagnosis of hypercoagulability is by. Molecular markers
 Agenda limitations of clinical laboratories to evaluate hypercoagulability and the underlying cause for thrombosis what is the INR the lupus anticoagulant and the antiphospholipid antibody syndrome hassouna
Agenda limitations of clinical laboratories to evaluate hypercoagulability and the underlying cause for thrombosis what is the INR the lupus anticoagulant and the antiphospholipid antibody syndrome hassouna
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Blood coagulation and fibrinolysis. Blood clotting (HAP unit 5 th )
 Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Primary Exam Physiology lecture 5. Haemostasis
 Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
Introduction to coagulation and laboratory tests
 Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
COAGULATION INHIBITORS LABORATORY DIAGNOSIS OF PROTHROMBOTIC STATES REGULATION OF. ANTICOAGULANT PROTEIN DEFICIENCY Disease entities COAGULATION
 LABORATORY DIAGNOSIS OF PROTHROMBOTIC COAGULATION INHIBITORS Tissue Factor Pathway Inhibitor (TFPI) Lipoprotein Associated Coagulation Inhibitor (LACI) Extrinsic Pathway Inhibitor (EPI) Complexes with
LABORATORY DIAGNOSIS OF PROTHROMBOTIC COAGULATION INHIBITORS Tissue Factor Pathway Inhibitor (TFPI) Lipoprotein Associated Coagulation Inhibitor (LACI) Extrinsic Pathway Inhibitor (EPI) Complexes with
Part IV Antithrombotics, Anticoagulants and Fibrinolytics
 Part IV Antithrombotics, Anticoagulants and Fibrinolytics "The meaning of good and bad, of better and worse, is simply helping or hurting" Emerson Chapter 16: Blood Coagulation and Fibrinolytic System
Part IV Antithrombotics, Anticoagulants and Fibrinolytics "The meaning of good and bad, of better and worse, is simply helping or hurting" Emerson Chapter 16: Blood Coagulation and Fibrinolytic System
Blood clotting. Subsequent covalent cross-linking of fibrin by a transglutaminase (factor XIII) further stabilizes the thrombus.
 Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Mohammadreza Tabatabaei IBTO COAG LAB
 Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Thrombophilia. Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS
 Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma
 Chapt. 45 Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma Inheritance of X-linked gene for Factor VIII hemophilia A Explain the
Chapt. 45 Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma Inheritance of X-linked gene for Factor VIII hemophilia A Explain the
Consultative Coagulation How to Effectively Answer Common Questions About Hemostasis Testing Session #5000
 Consultative Coagulation How to Effectively Answer Common Questions About Hemostasis Testing Session #5000 Dorothy M. (Adcock) Funk, M.D. Karen A. Moser, M.D. Esoterix Coagulation September 20, 2013 Disclosures
Consultative Coagulation How to Effectively Answer Common Questions About Hemostasis Testing Session #5000 Dorothy M. (Adcock) Funk, M.D. Karen A. Moser, M.D. Esoterix Coagulation September 20, 2013 Disclosures
Thrombosis. By Dr. Sara Mohamed Abuelgasim
 Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
Approach to Thrombosis
 Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
Chapter 1. General introduction
 Chapter 1 General introduction 8 Haemostasis All organs and tissues of higher organisms are provided with nutrients and oxygen through the bloodstream. The bloodstream is an extensive vascular system that
Chapter 1 General introduction 8 Haemostasis All organs and tissues of higher organisms are provided with nutrients and oxygen through the bloodstream. The bloodstream is an extensive vascular system that
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Laboratory Evaluation of Venous Thrombosis Risk
 Laboratory Evaluation of Venous Thrombosis Risk Dorothy M. Adcock, MD Volume 17, Number 12 December 2003 Objective: The reader will be able to discuss the concepts of risk factor, risk potential and thrombotic
Laboratory Evaluation of Venous Thrombosis Risk Dorothy M. Adcock, MD Volume 17, Number 12 December 2003 Objective: The reader will be able to discuss the concepts of risk factor, risk potential and thrombotic
Hemostasis. Learning objectives Dr. Mária Dux. Components: blood vessel wall thrombocytes (platelets) plasma proteins
 Hemostasis Learning objectives 14-16 Dr. Mária Dux Components: blood vessel wall thrombocytes (platelets) plasma proteins Hemostatic balance! procoagulating activity anticoagulating activity 1 Thrombocytes
Hemostasis Learning objectives 14-16 Dr. Mária Dux Components: blood vessel wall thrombocytes (platelets) plasma proteins Hemostatic balance! procoagulating activity anticoagulating activity 1 Thrombocytes
Disseminated Intravascular Coagulation. M.Bahmanpour MD Assistant professor IUMS
 به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
Inherited Thrombophilia Testing. George Rodgers, MD, PhD Kristi Smock MD
 Inherited Thrombophilia Testing George Rodgers, MD, PhD Kristi Smock MD Prevalence and risk associated with inherited thrombotic disorders Inherited Risk Factor % General Population % Patients w/ Thrombosis
Inherited Thrombophilia Testing George Rodgers, MD, PhD Kristi Smock MD Prevalence and risk associated with inherited thrombotic disorders Inherited Risk Factor % General Population % Patients w/ Thrombosis
Chapter 1 Introduction
 Chapter 1 Introduction There are several disorders which carry an increased risk of thrombosis, clots that interfere with normal circulation, including: venous thromboembolism (VTE), comprising both deep
Chapter 1 Introduction There are several disorders which carry an increased risk of thrombosis, clots that interfere with normal circulation, including: venous thromboembolism (VTE), comprising both deep
THROMBOPHILIA SCREENING
 THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche
 L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
Antiphospholipid Syndrome ( APS)
 Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
PHASES OF HAEMOSTASIS
 HAEMOSTASIS Maintains the integrity of a closed, highpressure circulatory system after vascular damage Vessel Wall Injury events in the vessel wall and in the blood which seal breach Delicate balance exists
HAEMOSTASIS Maintains the integrity of a closed, highpressure circulatory system after vascular damage Vessel Wall Injury events in the vessel wall and in the blood which seal breach Delicate balance exists
Thrombophilia: To test or not to test
 Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Clinical Study Procoagulant and Anticoagulant Factors in Childhood Hypothyroidism
 International Endocrinology Volume 2012, Article ID 156854, 4 pages doi:10.1155/2012/156854 Clinical Study Procoagulant and Anticoagulant Factors in Childhood Hypothyroidism Nevin Kilic, 1 Yildiz Dallar,
International Endocrinology Volume 2012, Article ID 156854, 4 pages doi:10.1155/2012/156854 Clinical Study Procoagulant and Anticoagulant Factors in Childhood Hypothyroidism Nevin Kilic, 1 Yildiz Dallar,
THROMBOTIC DISORDERS: The Final Frontier
 THROMBOTIC DISORDERS: The Final Frontier Jeffrey I. Weitz, MD, FRCP(C), FACP Professor of Medicine and Biochemistry McMaster University Canada Research Chair in Thrombosis Heart & Stroke Foundation/ J.F.
THROMBOTIC DISORDERS: The Final Frontier Jeffrey I. Weitz, MD, FRCP(C), FACP Professor of Medicine and Biochemistry McMaster University Canada Research Chair in Thrombosis Heart & Stroke Foundation/ J.F.
Thrombosis. Jeffrey Jhang, M.D.
 Thrombosis Jeffrey Jhang, M.D. Introduction The human hemostatic system has evolved to maintain blood flow under normal physiologic conditions while remaining primed to rapidly respond to vascular injury
Thrombosis Jeffrey Jhang, M.D. Introduction The human hemostatic system has evolved to maintain blood flow under normal physiologic conditions while remaining primed to rapidly respond to vascular injury
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus
 CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case Report and Review of the Literature
 Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Insights on the Quality of Coagulation Testing
 Insights on the Quality of Coagulation Testing Piet Meijer ECAT Foundation The Netherlands No conflicts of interest HAEMOSTATIC BALANCE BLEEDING HAEMOSTATIC BALANCE THROMBOSIS HAEMOSTATIC BALANCE Thrombosis
Insights on the Quality of Coagulation Testing Piet Meijer ECAT Foundation The Netherlands No conflicts of interest HAEMOSTATIC BALANCE BLEEDING HAEMOSTATIC BALANCE THROMBOSIS HAEMOSTATIC BALANCE Thrombosis
Reprinted in the IVIS website with the permission of the ACVP and ASVCP
 Proceedings of the Annual Meeting of the American College of Veterinary Pathologists and American Society for Veterinary Clinical Pathology - Tucson, Arizona 2006 - Reprinted in the IVIS website with the
Proceedings of the Annual Meeting of the American College of Veterinary Pathologists and American Society for Veterinary Clinical Pathology - Tucson, Arizona 2006 - Reprinted in the IVIS website with the
Anti β 2. -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With Antiphospholipid Syndrome
 Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion
 This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
DISCLOSURE. Presented by: Merav Sendowski, MD Oregon Health and Science University
 Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Haemostasis & Coagulation disorders Objectives:
 Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
PROTEÓMICA y SAF. Maria Josė Cuadrado Lupus Research Unit St. Thomas Hospital London UK
 PROTEÓMICA y SAF Maria Josė Cuadrado Lupus Research Unit St. Thomas Hospital London UK Aknowledgments Chary López-Pedrera Angeles Aguirre Francisco Velasco Hospital Reina Sofia, Córdoba, España Laura Bertolaccini
PROTEÓMICA y SAF Maria Josė Cuadrado Lupus Research Unit St. Thomas Hospital London UK Aknowledgments Chary López-Pedrera Angeles Aguirre Francisco Velasco Hospital Reina Sofia, Córdoba, España Laura Bertolaccini
UNIT VI. Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav. Copyright 2011 by Saunders, an imprint of Elsevier Inc.
 UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
Hemostasis and thrombosis in patients with liver disease. Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands
 Hemostasis and thrombosis in patients with liver disease Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands Importance of the liver in hemostasis Synthesis of Coagulation factors Fibrinolytic proteins
Hemostasis and thrombosis in patients with liver disease Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands Importance of the liver in hemostasis Synthesis of Coagulation factors Fibrinolytic proteins
Chapter 3. Haemostatic abnormalities in patients with liver disease
 Chapter 3 Haemostatic abnormalities in patients with liver disease Ton Lisman, Frank W.G. Leebeek 1, and Philip G. de Groot Thrombosis and Haemostasis Laboratory, Department of Haematology, University
Chapter 3 Haemostatic abnormalities in patients with liver disease Ton Lisman, Frank W.G. Leebeek 1, and Philip G. de Groot Thrombosis and Haemostasis Laboratory, Department of Haematology, University
Antiphospholipid Syndrome
 Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
DR NAGY VALÉRIA RETINAL VASCULAR DISEASES: THE RARE FORMS OF THROMBOPHILIA.
 DR NAGY VALÉRIA RETINAL VASCULAR DISEASES: THE RARE FORMS OF THROMBOPHILIA. UNIVERSITY OF DEBRECEN MEDICAL AND HEALTH SCIENCE CENTRE FACULTY OF MEDICINE Department of Ophthalmology and Division of Rare
DR NAGY VALÉRIA RETINAL VASCULAR DISEASES: THE RARE FORMS OF THROMBOPHILIA. UNIVERSITY OF DEBRECEN MEDICAL AND HEALTH SCIENCE CENTRE FACULTY OF MEDICINE Department of Ophthalmology and Division of Rare
St George Hospital Renal Department Guideline: INTERNAL ONLY ANTICOAGULATION - COMMENCEMENT OF HAEMODIALYSIS
 ANTICOAGULATION - COMMENCEMENT OF HAEMODIALYSIS Summary Aim: To prevent clotting of the extracorporeal circuit during haemodialysis If there are no contraindications, heparin can be used. In the first
ANTICOAGULATION - COMMENCEMENT OF HAEMODIALYSIS Summary Aim: To prevent clotting of the extracorporeal circuit during haemodialysis If there are no contraindications, heparin can be used. In the first
Bleeding and Thrombotic Disorders. Kristine Krafts, M.D.
 Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Comparison of Samples Obtained From 3.2% Sodium Citrate Glass and Two 3.2% Sodium Citrate Plastic Blood Collection Tubes Used in Coagulation Testing
 Coagulation and Transfusion Medicine / GLASS VS PLASTIC IN HEMOSTASIS TESTING Comparison of Samples Obtained From 3.2% Sodium Citrate Glass and Two 3.2% Sodium Citrate Plastic Blood Collection Tubes Used
Coagulation and Transfusion Medicine / GLASS VS PLASTIC IN HEMOSTASIS TESTING Comparison of Samples Obtained From 3.2% Sodium Citrate Glass and Two 3.2% Sodium Citrate Plastic Blood Collection Tubes Used
Optimal Utilization of Thrombophilia Testing
 Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
The effect of the direct oral anticoagulants (DOACs) on haemostasis tests.
 The effect of the direct oral anticoagulants (DOACs) on haemostasis tests. Emmanuel J Favaloro, Haematology, ICPMR, Pathology West, Sydney Centres for Thrombosis and Haemostasis, Westmead Hospital (with
The effect of the direct oral anticoagulants (DOACs) on haemostasis tests. Emmanuel J Favaloro, Haematology, ICPMR, Pathology West, Sydney Centres for Thrombosis and Haemostasis, Westmead Hospital (with
Key words: antiphospholipid syndrome, trombosis, pathogenesis
 26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
Bleeding and Haemostasis. Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon
 Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Coagulation Disorders. Dr. Muhammad Shamim Assistant Professor, BMU
 Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Internal Quality Control in the Haemostasis laboratory. Dr Steve Kitchen Sheffield Haemophilia and Thrombosis centre & UK NEQAS Blood Coagulation
 Internal Quality Control in the Haemostasis laboratory Dr Steve Kitchen Sheffield Haemophilia and Thrombosis centre & UK NEQAS Blood Coagulation Why do we need Quality control? Philadelphia Enquirer Aug
Internal Quality Control in the Haemostasis laboratory Dr Steve Kitchen Sheffield Haemophilia and Thrombosis centre & UK NEQAS Blood Coagulation Why do we need Quality control? Philadelphia Enquirer Aug
Topics of today lectures: Hemostasis
 Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
Important Considera/ons for Coagula/on Tests on Children and Neonates
 Important Considera/ons for Coagula/on Tests on Children and Neonates Cindy Neunert, MD MSCS Associate Professor Pediatric Hematology/Oncology/Bone Marrow Transplant Columbia University Medical Center
Important Considera/ons for Coagula/on Tests on Children and Neonates Cindy Neunert, MD MSCS Associate Professor Pediatric Hematology/Oncology/Bone Marrow Transplant Columbia University Medical Center
Thrombophilia. Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC. GASCO Atlanta Sept 8 th, Disclosures. Conflicts of interest: NONE
 LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
Comparison of Three Methods for Measuring Factor VIII Levels in Plasma
 Coagulation and Transfusion Medicine / THREE FACTOR VIII ASSAYS Comparison of Three Methods for Measuring Factor VIII Levels in Plasma Wayne L. Chandler, MD, Chris Ferrell, MT(ASCP), Joo Lee, MT(ASCP),
Coagulation and Transfusion Medicine / THREE FACTOR VIII ASSAYS Comparison of Three Methods for Measuring Factor VIII Levels in Plasma Wayne L. Chandler, MD, Chris Ferrell, MT(ASCP), Joo Lee, MT(ASCP),
A Case of Factor XII Deficiency Which was Found in Recurrent Spontaneous Abortion. Y. S. Nam, I. H. Kim, T. K. Yoon, C. N. Lee and K. Y.
 12 1 A Case of Factor XII Deficiency Which was Found in Recurrent Spontaneous Abortion Y S Nam, I H Kim, T K Yoon, C N Lee and K Y Cha Department of Obstetrics and Gynecology, College of Medicine, Pocheon
12 1 A Case of Factor XII Deficiency Which was Found in Recurrent Spontaneous Abortion Y S Nam, I H Kim, T K Yoon, C N Lee and K Y Cha Department of Obstetrics and Gynecology, College of Medicine, Pocheon
TECHNICAL SERIES. Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss. ...Setting trends TULIP DIAGNOSTICS (P) LTD.
 For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
Annals of RSCB Vol. XVI, Issue 1
 THE STUDY OF PROTHROBOTIC STATE IN PATIENTS WITH TYPE 2 DIABETES MELLITUS AND CARDIOVASCULAR DISEASES Oana Bădulescu 1, Codruţa Bădescu 2, Manuela Ciocoiu 1, Magda Bădescu 1 1 DEPARTMENT OF PATHOPHYSIOLOGY;
THE STUDY OF PROTHROBOTIC STATE IN PATIENTS WITH TYPE 2 DIABETES MELLITUS AND CARDIOVASCULAR DISEASES Oana Bădulescu 1, Codruţa Bădescu 2, Manuela Ciocoiu 1, Magda Bădescu 1 1 DEPARTMENT OF PATHOPHYSIOLOGY;
The effect of oral anticoagulation on clotting during hemodialysis
 Kidney International, Vol. 68 (2005), pp. 862 866 The effect of oral anticoagulation on clotting during hemodialysis FARZAD ZIAI,THOMAS BENESCH,KATHARINA KODRAS, IRMGARD NEUMANN, LIDA DIMOPOULOS-XICKI,
Kidney International, Vol. 68 (2005), pp. 862 866 The effect of oral anticoagulation on clotting during hemodialysis FARZAD ZIAI,THOMAS BENESCH,KATHARINA KODRAS, IRMGARD NEUMANN, LIDA DIMOPOULOS-XICKI,
What are blood clots?
 What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
Lupus Anticoagulants (LA), Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update. Antiphospholipid. Antiphospholipid
 , Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
, Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
Determination of APTT factor sensitivity the misguiding guideline
 International Journal of Laboratory Hematology ORIGINAL ARTICLE The Official journal of the International Society for Laboratory Hematology INTERNATIONAL JOURNAL OF LABORATORY HEMATOLOGY Determination
International Journal of Laboratory Hematology ORIGINAL ARTICLE The Official journal of the International Society for Laboratory Hematology INTERNATIONAL JOURNAL OF LABORATORY HEMATOLOGY Determination
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/28736 holds various files of this Leiden University dissertation. Author: Debeij, Jan Title: The effect of thyroid hormone on haemostasis and thrombosis
Cover Page The handle http://hdl.handle.net/1887/28736 holds various files of this Leiden University dissertation. Author: Debeij, Jan Title: The effect of thyroid hormone on haemostasis and thrombosis
EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION
 EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
Hemostasis and. Blood Coagulation
 Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
Supplemental Figures and Legends
 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Blood Thinner Agent. Done by: Meznah Al-mutairi Pharm.D Candidate PNU Collage of Pharmacy
 Blood Thinner Agent Done by: Meznah Al-mutairi Pharm.D Candidate PNU Collage of Pharmacy Outline: Blood thinner agent definition. anticoagulants drugs. Thrombolytics. Blood thinner agent Therapeutic interference
Blood Thinner Agent Done by: Meznah Al-mutairi Pharm.D Candidate PNU Collage of Pharmacy Outline: Blood thinner agent definition. anticoagulants drugs. Thrombolytics. Blood thinner agent Therapeutic interference
Antiphospholipid antibodies in patients with venous thrombosis at Kenyatta National Hospital
 Research article Department of Human Pathology, School of Medicine, University of Nairobi, P. O. Box 19676 00202, Nairobi, Kenya Corresponding author: Dr KA Barasa, Department of Human Pathology, School
Research article Department of Human Pathology, School of Medicine, University of Nairobi, P. O. Box 19676 00202, Nairobi, Kenya Corresponding author: Dr KA Barasa, Department of Human Pathology, School
VTE in Children: Practical Issues
 VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK?
 VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
Recent studies have found that elevated levels of coagulation
 Elevated Hemostatic Factor Levels as Potential Risk Factors for Thrombosis Wayne L. Chandler, MD; George M. Rodgers, MD, PhD; Jason T. Sprouse, MD; Arthur R. Thompson, MD, PhD Recent studies have found
Elevated Hemostatic Factor Levels as Potential Risk Factors for Thrombosis Wayne L. Chandler, MD; George M. Rodgers, MD, PhD; Jason T. Sprouse, MD; Arthur R. Thompson, MD, PhD Recent studies have found
Hemodynamic Disorders, Thrombosis, and Shock. Richard A. McPherson, M.D.
 Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
Haemostasis, thrombosis risk and hormone replacement therapy
 Haemostasis, thrombosis risk and hormone replacement therapy Serge Motte Brussels 13.05.17 - MY TALK TODAY The coagulation cascade and its regulation Effects of hormone replacement therapy on haemostasis
Haemostasis, thrombosis risk and hormone replacement therapy Serge Motte Brussels 13.05.17 - MY TALK TODAY The coagulation cascade and its regulation Effects of hormone replacement therapy on haemostasis
Thyroid disease and haemostasis: a relationship with clinical implications? Squizzato, A.
 UvA-DARE (Digital Academic Repository) Thyroid disease and haemostasis: a relationship with clinical implications? Squizzato, A. Link to publication Citation for published version (APA): Squizzato, A.
UvA-DARE (Digital Academic Repository) Thyroid disease and haemostasis: a relationship with clinical implications? Squizzato, A. Link to publication Citation for published version (APA): Squizzato, A.
Generate Knowledge Lupus Anticoagulant Testing Made Simple
 Generate Knowledge Lupus Anticoagulant Testing Made Simple Paul Riley, PhD, MBA Learning objectives Describe antiphospholipid syndrome (aps) and role of the lupus anticoagulant (LA) in thrombosis Present
Generate Knowledge Lupus Anticoagulant Testing Made Simple Paul Riley, PhD, MBA Learning objectives Describe antiphospholipid syndrome (aps) and role of the lupus anticoagulant (LA) in thrombosis Present
Coagulation an Overview Dr.Abdolreza Abdolr Afrasiabi Thal assem a & Heamophili hilia G ene i tic R esearc C en er Shiraz Medical Medic University
 In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
by accumulation of pathological mast cells in potentially any or all organs and tissues and/or
 1 Supplementary Material to Seidel et al. Bleeding diathesis in patients with mast cell activation disease (Thromb Haemost 2011; 106.5) Definition of mast cell activation disease The term mast cell activation
1 Supplementary Material to Seidel et al. Bleeding diathesis in patients with mast cell activation disease (Thromb Haemost 2011; 106.5) Definition of mast cell activation disease The term mast cell activation
Biochemical Reaction Networks and Blood Clotting
 Biochemical Reaction Networks and Blood Clotting Yasmeen Hussain, Aaron Fogelson Abstract Following an injury to the walls of a blood vessel, platelet aggregation and blood coagulation are induced. Through
Biochemical Reaction Networks and Blood Clotting Yasmeen Hussain, Aaron Fogelson Abstract Following an injury to the walls of a blood vessel, platelet aggregation and blood coagulation are induced. Through
Plasma Levels of Protein Z and Antiphospholipid Protein Antibodies in Patients with Ischemic Stroke
 Mohamed Elkhateeb et al. Plasma Levels of Protein Z and Antiphospholipid Protein Antibodies in Patients with Ischemic Stroke Mohamed Elkhateeb 1, Ibrahim Elmenshawy 1, Hanan Azzam 2, Tarek Selim 2, Nashwa
Mohamed Elkhateeb et al. Plasma Levels of Protein Z and Antiphospholipid Protein Antibodies in Patients with Ischemic Stroke Mohamed Elkhateeb 1, Ibrahim Elmenshawy 1, Hanan Azzam 2, Tarek Selim 2, Nashwa
Disclosures. Anticoagulation in Kidney Disease: Considerations for Patients with Nephrotic Syndrome
 Anticoagulation in Kidney Disease: Considerations for Patients with Nephrotic Syndrome Vimal K. Derebail Glomerular Disease Collaborative Network May 20 th, 2017 Disclosures Employer: University of North
Anticoagulation in Kidney Disease: Considerations for Patients with Nephrotic Syndrome Vimal K. Derebail Glomerular Disease Collaborative Network May 20 th, 2017 Disclosures Employer: University of North
Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time
 Clin. Lab. 2009;55:XXX-XXX Copyright ORIGINAL ARTICLE Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time HORATIU OLTEANU 2, KATHARINE. A. DOWNES 1, JIGAR
Clin. Lab. 2009;55:XXX-XXX Copyright ORIGINAL ARTICLE Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time HORATIU OLTEANU 2, KATHARINE. A. DOWNES 1, JIGAR
Hemostasis. Clo)ng factors and Coagula4on NORMAL COAGULATION. Overview of blood coagula4on. The Cascade Theory 5/1/12. Clot
 Hemostasis Clo)ng factors and Coagula4on Dr Badri Paudel www.badripaudel.com Hemostasis is defined as a property of circula4on whereby blood is maintained within a vessel and the ability of the system
Hemostasis Clo)ng factors and Coagula4on Dr Badri Paudel www.badripaudel.com Hemostasis is defined as a property of circula4on whereby blood is maintained within a vessel and the ability of the system
Menopausal Hormone Therapy & Haemostasis
 Menopausal Hormone Therapy & Haemostasis The Haematologist Perspective Dr. Batia Roth-Yelinek Coagulation unit Hadassah MC Menopausal Hormone Therapy & Hemostasis Hemostatic mechanism Mechanism of estrogen
Menopausal Hormone Therapy & Haemostasis The Haematologist Perspective Dr. Batia Roth-Yelinek Coagulation unit Hadassah MC Menopausal Hormone Therapy & Hemostasis Hemostatic mechanism Mechanism of estrogen
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients. David Liff MD Oklahoma Heart Institute Vascular Center
 DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
COAGULATIONS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin)
 COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
Hemostasis. PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures
 Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Recommendations for Celiac Disease Testing. IgA & ttg IgA
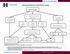 Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO
 THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
Anticoagulants. Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT
 Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
CLINICAL FELLOWSHIP PROGRAM IN COAGULATION
 CLINICAL FELLOWSHIP PROGRAM IN COAGULATION The Department of Pathology and Laboratory Medicine University of Alberta, Faculty of Medicine and Dentistry and Alberta Health Services CLINICAL FELLOWSHIP IN
CLINICAL FELLOWSHIP PROGRAM IN COAGULATION The Department of Pathology and Laboratory Medicine University of Alberta, Faculty of Medicine and Dentistry and Alberta Health Services CLINICAL FELLOWSHIP IN
Improved Distinction of Factor V Wild-Type and Factor V Leiden Using a Novel Prothrombin-Based Activated Protein C Resistance Assay
 Coagulation and Transfusion Medicine / A NOVEL PROTHROMBIN-BASED APC-R ASSAY Improved Distinction of Factor V Wild-Type and Factor V Leiden Using a Novel Prothrombin-Based Activated Protein C Resistance
Coagulation and Transfusion Medicine / A NOVEL PROTHROMBIN-BASED APC-R ASSAY Improved Distinction of Factor V Wild-Type and Factor V Leiden Using a Novel Prothrombin-Based Activated Protein C Resistance
For personal use only. Clopidogrel diminishes hemodialysis access graft thrombosis INTRODUCTION
 The Journal of Vascular Access 2005; 6: 29-33 ORIGINAL ARTICLE Clopidogrel diminishes hemodialysis access graft thrombosis H. TRIMARCHI 1, P. YOUNG 2, M. FORRESTER 1, J. SCHROPP 1, H. PEREYRA 1, E. FREIXAS
The Journal of Vascular Access 2005; 6: 29-33 ORIGINAL ARTICLE Clopidogrel diminishes hemodialysis access graft thrombosis H. TRIMARCHI 1, P. YOUNG 2, M. FORRESTER 1, J. SCHROPP 1, H. PEREYRA 1, E. FREIXAS
Annals of RSCB Vol. XVII, Issue 1/2012
 CORRELATIONS BETWEEN ENDOTHELIAL DYSFUNCTION AND GLYCEMIA IN VENOUS THROMBOSIS PATHOGENESIS Codruţa Bădescu 1, Oana Bădulescu 2, Manuela Ciocoiu 2, Magda Bădescu 2, M. Costuleanu 2 1 DEPARTMENT OF INTERNAL
CORRELATIONS BETWEEN ENDOTHELIAL DYSFUNCTION AND GLYCEMIA IN VENOUS THROMBOSIS PATHOGENESIS Codruţa Bădescu 1, Oana Bădulescu 2, Manuela Ciocoiu 2, Magda Bădescu 2, M. Costuleanu 2 1 DEPARTMENT OF INTERNAL
Faculty Disclosure. Hypercoagulable States. Learning Objectives. Hereditary Thombophilia. Acquired Hypercoagulable States 5/9/2016
 Faculty Disclosure Hypercoagulable States Dr. Rizal has no actual or potential conflict of interest associated with this presentation By: Dr. Anuja Rizal Pharm. D., RPh., CACP Clinical Coordinator UConn
Faculty Disclosure Hypercoagulable States Dr. Rizal has no actual or potential conflict of interest associated with this presentation By: Dr. Anuja Rizal Pharm. D., RPh., CACP Clinical Coordinator UConn
Dr Kirsten Herbert. Dr Melita Kenealy. MBBS(Hons) FRCPA FRACP. Common Blood Tests
 Common Blood Tests Your Haematologist may order numerous blood and urine tests to help diagse or manage your condition. Listed below are some of the more common tests that can be ordered in a haematology
Common Blood Tests Your Haematologist may order numerous blood and urine tests to help diagse or manage your condition. Listed below are some of the more common tests that can be ordered in a haematology
