Aminoglycosides as an antibiotic class maintain
|
|
|
- Mae Douglas
- 6 years ago
- Views:
Transcription
1 SURGICAL INFECTIONS Volume 17, Number 3, 2016 ª Mary Ann Liebert, Inc. DOI: /sur An Argument for the Use of Aminoglycosides in the Empiric Treatment of Ventilator-Associated Pneumonia Addison K. May Abstract Background: Appropriate empiric antibiotic therapy for ventilator-associated pneumonia improves outcomes. Controversy exists regarding the inclusion of aminoglycosides in empiric therapeutic regimens. Methods: The Ovid and Cochrane databases were searched for relevant literature regarding the use of aminoglycosides in combination therapy for ventilator-associated pneumonia. The data supporting the use of aminoglycosides in certain populations and strategies to limit toxicity are summarized. Results: In patients at high risk of infection with antibiotic-resistant gram-negative bacilli and in those with severe illness, aminoglycosides improve clinical outcomes. In critically ill populations, short-duration therapy and high-dose extended-interval dosing of aminoglycosides can improve therapeutic efficacy while limiting nephrotoxicity. Conclusions: In selected populations using appropriate dosing strategies, aminoglycosides should be considered for empiric treatment of ventilator-associated pneumonia. Aminoglycosides as an antibiotic class maintain broad-spectrum activity against both gram-negative bacilli and gram-positive cocci, with the rate of resistance to this class remaining relatively stable despite decades of use [1]. Their mechanism of action is believed to be interruption of protein synthesis at the ribosomal level, demonstrating both in vitro synergism with b-lactam antibiotics for many gram-negative bacilli and gram-positive cocci and substantial post-antibiotic effect [1,2]. Thus, two separate rationales may support the use of aminoglycosides for empiric therapy: (1) Improvement of the coverage of resistant gram-negative bacilli and (2) obtaining better outcomes as a result of therapeutic synergy with other agents. The routine use of aminoglycosides commonly is limited by their potential to induce or potentiate nephrotoxicity. However, when dosed appropriately and de-escalated when culture and sensitivity data show they are not appropriate, nephrotoxicity should be limited. An appropriate risk/benefit analysis for the use of empiric aminoglycosides requires knowledge of the relatively complex data regarding appropriate empiric antibiotic therapy (i.e., pathogens sensitive to empiric regimen), the likelihood of resistant pathogens, mortality risk stratification, aminoglycoside dosing strategies, and the risk of nephrotoxicity. An argument for the use of aminoglycoside agents in combination therapy for the empiric therapy for ventilatorassociated pneumonia (VAP) in selected patients is presented here, as well as a strategy to limit nephrotoxicity. Increasing the Adequacy of Empiric Coverage of Resistant GNB In certain patient populations, aminoglycosides may improve substantially the likelihood of appropriate empiric coverage of VAP caused by gram-negative bacilli. Observational data demonstrate the importance of correctly treating causative pathogens empirically in VAP, with inadequate treatment significantly increasing the risk of death [1,3 7]. In hospital-acquired pneumonia, resistance among gram-negative pathogens may limit the ability to cover all likely pathogens with a single agent or class [1,7 9]. Thus, combination therapy, including aminoglycosides, may increase the likelihood of adequate empiric therapy and improve outcomes. The importance of adequate empiric coverage of pathogens in those patients suspected of having VAP was suggested in the late 1980s by Celis et al. [10] and was established in the mid-1990s through a series of observational studies by various authors [3 6]. Four studies demonstrated Departments of Surgery and Anesthesiology, Division of Trauma and Surgical Critical Care, Vanderbilt University Medical Center, Nashville, Tennessee. Presented at the 33rd Annual Meeting of the Surgical Infection Society. Las Vegas, Nevada. April 12 15,
2 330 MAY roughly a doubling of both crude and attributable death if empiric therapy did not provide adequate coverage of pathogens [3,5,6,10]. These findings were supported by a subsequent prospective observational study by Kollef et al. in 1999 [4]. Those authors followed all critically ill patients admitted to either of two surgical intensive care units (ICUs). Six hundred fifty-five patients had infections (either communityor hospital-acquired), and 26% received inadequate empiric therapy. Those latter patients had a greater than a two-fold increase in the risk of death. Of the gram-negative pathogens isolated in this study, a quarter were antibiotic resistant. The importance of adequate empiric coverage for serious infections, including VAP, continues to be confirmed in recent observational studies [7,11 13]. Table 1 outlines 17 studies examining the outcome of VAP with and without appropriate antibiotic therapy. All studies demonstrate greater numbers of deaths with inadequate empiric coverage, the differences in 13 of these studies reaching statistical significance [3 7,10,12 22]. A delay in appropriate antibiotic therapy is associated with more deaths even if antibiotics are adjusted when sensitivity data are returned after 48 to 72 h [5,19,23]. Multivariable analysis of independent risk factors for the 30-day mortality rate in patients with gram-negative VAP demonstrates that inappropriate initial antibiotic therapy is strongly and significantly associated with the risk of death (adjusted odds ratio [OR] 11.7) [12]. The presence of multi-drug-resistant (MDR) pathogens greatly increases the risk of inadequate empiric antibiotic therapy. As noted above in the study by Kollef et al., antibiotic resistance is common, with a quarter of the isolated gram-negative pathogens being antibiotic resistant [4]. Multi-drug-resistant gram-negative pathogens within ICUs are a serious concern. In a prospective observational study of nosocomial infections in 24 ICUs in Belgium from , 49.6% of the gram-negative pathogens were MDR, and in 36% of all nosocomial infections, antibiotic therapy was classified as inadequate [24]. Prior antibiotic exposure within the last 90 d or during the hospital stay appears to be among Series the strongest risk factors for the presence of MDR bacteria [24 26]. Other risk factors include exposure to healthcare environments in the previous 90 d, current hospital length of stay greater than five d, and chronic illness or immunosuppression. Unless highly effective antibiotic stewardship programs are in place, and efforts to reduce resistant pathogens have been highly successful within the local environment, the risk of MDR pathogens as a cause of hospital-acquired infection remains significant. Thus, to improve the adequacy of empiric antibiotic treatment for patients at risk of MDR pathogens, existing guidelines recommend combination therapy [25]. The use of local data to establish guidelines can increase compliance with adequate empiric therapy for VAP by targeting therapy to the most common pathogens historically isolated within an institution or specific ICU and their antibiotic sensitivities [8,27]. In a before and after study of implementing such a locally developed guideline, Ibrahim et al. demonstrated an increase in compliance with appropriate empiric therapy to greater than 90% coverage with the combination of a b-lactam and fluoroquinolone [27]. In contrast, in a similar study by Beardsley et al., the combination of a b-lactam and fluoroquinolone achieved appropriate empiric coverage in only 70% of episodes of late-onset pneumonia, whereas a combination including an aminoglycoside achieved appropriate coverage in 93% of cases [8]. At the author s institution, empiric antibiotic therapy for VAP using combination therapy with aminoglycosides is based on risk stratification utilizing local unit-specific data to ensure adequate coverage, a system employed for more than 10 years [28]. Additionally, aggressive antibiotic stewardship and infection-reduction programs have been employed during the same period. Stewardship protocols include limiting antibiotic prophylaxis to evidence-supported indications with the narrowest appropriate coverage for 24 h or less, quantitative cultures for the diagnosis of VAP, and de-escalation of therapy based on culture results. In 2005, a program to maintain antibiotic heterogeneity while eliminating an Table 1. Influence of Adequate Initial Antibiotic Therapy on Mortality Rate in Ventilator-Associated Pneumonia Year No. of patients Adequate treatment death/pts (%) Inadequate treatment death/pts (%) Celis et al. [10] /118 (28) 11/ 12 (92) <0.001 Alvarez-Lerma [3] /284 (16) 36/146 (25) 0.03 Luna et al. [5] / 16 (38) 31/ 34 (91) <0.01 Rello et al. [6] / 86 (15) 10/ 27 (37) <0.05 Sanchez-Nieto et al. [22] / 24 (25) 6/ 14 (43) NS Kollef et al. [4] /106 (45) 51/305 (17) <0.01 Bercault & Boulain [14] / 92 (40) 18/ 34 (53) NS Dupont et al. [16] / 55 (38) 27/ 57 (47) NS Iregui et al. [19] / 74 (28) 23/ 33 (70) <0.01 Hanes et al. [18] / 79 (11) 21/ 84 (25) 0.02 Dupont et al. [17] /220 (17) 21/ 92 (23) NS Leroy et al. [20] /106 (40) 16/ 26 (62) 0.04 Clec h C et al. [15] / 27 ( 7) 16/ 43 (37) <0.01 Mueller et al. [21] / 28 ( 4) 12/ 54 (22) <0.01 Kollef et al. [12] / 59 (14) 11/ 17 (65) <0.01 Rello et al. [11] (35) (48) 0.01 Tseng et al. [13] / 71 (28) 37/ 60 (62) p NS = non-significant.
3 AMINOGLYCOSIDES IN VAP 331 FIG. 1. Percentage of gram-negative pathogens that were either pansensitive or multi-drug resistant by quarter after initiation of an antibiotic stewardship program in Trend lines demonstrate significant increase in percentage of pathogens that were pansensitive and decrease in those that were multi-drug resistant in both the trauma (TICU) and the surgical (SICU) intensive care units. (Reprinted with permission from Dortch et al. [28]). antibiotic class on a rotating quarterly schedule was instituted. Antibiotic resistance to one or multiple classes of drugs among local gram-negative pathogens has declined significantly over time in the trauma and surgical ICUs (Fig. 1). During the 8-y period from 2001 to 2008, these ICUs have had a 77% relative reduction in MDR gram-negative pathogens and a 56% relative increase in the percentage of pansensitive pathogens [28]. Despite these positive effects of antibiotic stewardship initiatives, combination empiric coverage of potential gramnegative pathogens, including aminoglycosides, have still proved to be beneficial. Analysis of our empiric combination therapy for VAP over a 5-y period demonstrated that aminoglycoside use was required to achieve adequate coverage in 20% of cases. Adequate empiric therapy was achieved for 94% and 88% of pathogens, respectively, for the trauma and surgical ICUs. Additionally, no pathogens resistant to aminoglycosides were sensitive to fluoroquinolones during this time. However, the majority of pathogens resistant to fluoroquinolones were sensitive to aminoglycosides (63%). Thus, the addition of aminoglycosides to our empiric regimen has improved the frequency of adequate empiric coverage substantially. Improved Outcomes Secondary to Therapeutic Synergy As noted above, the combination of an aminoglycoside with a b-lactam antibiotic demonstrates a synergistic bacteriocidal effect for both gram-negative bacilli and grampositive cocci in vitro [1]. However, demonstrating a therapeutic benefit from this combination therapy in the clinical setting has been much more complex, perhaps because of an offsetting detrimental effect of aminoglycoside nephrotoxicity. On the basis of an analysis of both observational and interventional studies, the combination of an aminoglycoside and a b-lactam appears to offer therapeutic benefit in more severely ill populations while potentially being detrimental in those who are less ill [1,11,29,30]. Aminoglycosides have been studied extensively in both pneumonia and sepsis and several meta-analyses published. Most studies published prior to 2010 have not demonstrated a clear benefit to combination therapy for pneumonia or sepsis as long as empiric therapy appropriately covered the pathogen [26,31 34]. However, most of these studies either did not include the most severely ill patient population or did not perform analyses based on severity of illness stratification [35]. In a prospective study of 200 consecutive cases of P. aeruginosa bacteremia, combination therapy resulted in a significantly lower mortality than monotherapy (27% vs 47%; p < 0.02) [36]. These findings were confirmed in a metaanalysis of combination therapy for gram-negative bacilli bacteremia by Safdar et al., demonstrating a clear benefit to the use of combination therapy in patients with P. aeruginosa bacteremia with roughly a 50% reduction in the number of deaths [33]. Combination therapy improves outcomes in patients with severe community-acquired pneumonia (i.e., those with septic shock or requiring mechanical ventilation) even when the b-lactam therapy appropriately covers the pathogen [35 37]. Therapeutic benefit for combination therapy with an aminoglycoside has been demonstrated in patients with bacteremia who present in septic shock or who are neutropenic [11]. In a meta-analysis of studies of combination therapy versus monotherapy for the treatment of serious infections associated with sepsis and septic shock, Kumar et al demonstrated that combination therapy improves survival and clinical response in high-risk, life-threatening infections but may be detrimental in those patients who are at low risk [30]. Dosing Strategies and Nephrotoxicity The main concern about using aminoglycosides in empiric therapy for pneumonia is the fear of nephrotoxicity. However, if aminoglycosides are dosed appropriately and deescalated as indicated when sensitivity data become available,
4 332 MAY nephrotoxicity should rarely, if ever, occur. Nephrotoxicity from aminoglycosides is correlated most strongly with trough levels and total time of exposure [38]. Extended dosing regimens should be employed for aminoglycosides, maximizing concentration-dependent killing and limiting toxicity by allowing troughs to fall below 0.5 mcg/ml [1]. The majority of the therapeutic effect from combination therapy is believed to occur early in the course of treatment, and appropriate de-escalation should limit aminoglycoside exposure to 3 d or less. Meta-analysis of extended versus routine dosing regimens clearly demonstrated reduced nephrotoxicity of extended regimens, with an overall rate of acute kidney injury of 5.5% for patients receiving full therapeutic courses of aminoglycosides [39]. However, in one large observational study of more than 2,000 patients with a median therapeutic course of 3 d of aminoglycoside, the overall rate of a creatinine concentration 0.5 mg/dl above the baseline was 1.2% [40]. Thus, the overall rate of severe renal dysfunction as a result of empiric therapy should be well under 1%. At our institution, all cases of renal failure developing in our surgical ICUs are reviewed as part of our quality assurance and process improvement programs. No cases of acute renal failure have been attributed to empiric exposure to aminoglycosides during the period of the program. In summary, the addition of an aminoglycoside to b-lactam therapy for empiric coverage of pathogens in patients suspected of having VAP should be considered when the risk of gram-negative bacilli resistance is significant or when patients are more severely ill, particularly in the presence of septic shock. The need to cover the involved pathogens empirically has substantial support on the literature. Even in settings with aggressive antibiotic stewardship and infection reduction programs, aminoglycosides increase the percentage of gram-negative pathogens that are adequately covered empirically. If quantitative techniques for the diagnosis of pneumonia, extended dosing of aminoglycosides, short therapeutic courses, and appropriate de-escalation are all employed, nephrotoxicity should be eliminated. Extending the use of aminoglycosides to double cover pathogens for longer therapeutic courses is not supported in the literature. Author Disclosure Statement The author has no conflicts of interest in relation to this manuscript. References 1. Boyer A, Gruson D, Bouchet S, et al. Aminoglycosides in septic shock: An overview, with specific consideration given to their nephrotoxic risk. Drug Saf 2013;36: Davis BD. Mechanism of bactericidal action of aminoglycosides. Microbiol Rev 1987;51: Alvarez-Lerma F. Modification of empiric antibiotic treatment in patients with pneumonia acquired in the intensive care unit. ICU-Acquired Pneumonia Study Group. Intensive Care Med 1996;22: Kollef MH, Sherman G, Ward S, Fraser VJ. Inadequate antimicrobial treatment of infections: A risk factor for hospital mortality among critically ill patients. Chest 1999;115: Luna CM, Vujacich P, Niederman MS, et al. Impact of BAL data on the therapy and outcome of ventilatorassociated pneumonia. Chest 1997;111: Rello J, Gallego M, Mariscal D, et al. The value of routine microbial investigation in ventilator-associated pneumonia. Am J Respir Crit Care Med 1997;156: Rello J, Ulldemolins M, Lisboa T, Koulenti D, et al. Determinants of prescription and choice of empirical therapy for hospital-acquired and ventilator-associated pneumonia. Eur Respir J 2011;37: Beardsley JR, Williamson JC, Johnson JW, et al. Using local microbiologic data to develop institution-specific guidelines for the treatment of hospital-acquired pneumonia. Chest 2006;130: Bhat S, Fujitani S, Potoski BA, et al. Pseudomonas aeruginosa infections in the Intensive care unit: Can the adequacy of empirical beta-lactam antibiotic therapy be improved? Int J Antimicrob Agents 2007;30: Celis R, Torres A, Gatell JM, et al. Nosocomial pneumonia: A multivariate analysis of risk and prognosis. Chest 1988; 93: Martinez JA, Cobos-Trigueros N, Soriano A, et al. Influence of empiric therapy with a beta-lactam alone or combined with an aminoglycoside on prognosis of bacteremia due to gram-negative microorganisms. Antimicrob Agents Chemother 2010;54: Kollef KE, Schramm GE, Wills AR, et al. Predictors of 30-day mortality and hospital costs in patients with ventilatorassociated pneumonia attributed to potentially antibioticresistant gram-negative bacteria. Chest 2008;134: Tseng CC, Liu SF, Wang CC, et al. Impact of clinical severity index, infective pathogens, and initial empiric antibiotic use on hospital mortality in patients with ventilatorassociated pneumonia. Am J Infect Control 2012;40: Bercault N, Boulain T. Mortality rate attributable to ventilator-associated nosocomial pneumonia in an adult intensive care unit: A prospective case-control study. Crit Care Med 2001;29: Clec h C, Timsit JF, De LA, et al. Efficacy of adequate early antibiotic therapy in ventilator-associated pneumonia: Influence of disease severity. Intensive Care Med 2004;30: Dupont H, Mentec H, Sollet JP, Bleichner G. Impact of appropriateness of initial antibiotic therapy on the outcome of ventilator-associated pneumonia. Intensive Care Med 2001;27: Dupont H, Montravers P, Gauzit R, et al. Outcome of postoperative pneumonia in the Eole study. Intensive Care Med 2003;29: Hanes SD, Demirkan K, Tolley E, et al. Risk factors for late-onset nosocomial pneumonia caused by Stenotrophomonas maltophilia in critically ill trauma patients. Clin Infect Dis 2002;35: Iregui M, Ward S, Sherman G, et al. Clinical importance of delays in the initiation of appropriate antibiotic treatment for ventilator-associated pneumonia. Chest 2002;122: Leroy O, Meybeck A, d Escrivan T, et al. Impact of adequacy of initial antimicrobial therapy on the prognosis of patients with ventilator-associated pneumonia. Intensive Care Med 2003;29: Mueller EW, Hanes SD, Croce MA, et al. Effect from multiple episodes of inadequate empiric antibiotic ther-
5 AMINOGLYCOSIDES IN VAP 333 apy for ventilator-associated pneumonia on morbidity and mortality among critically ill trauma patients. J Trauma 2005;58: Sanchez-Nieto JM, Torres A, Garcia-Cordoba F, et al. Impact of invasive and noninvasive quantitative culture sampling on outcome of ventilator-associated pneumonia: A pilot study. Am J Respir Crit Care Med 1998;157: Luna CM, Blanzaco D, Niederman MS, et al. Resolution of ventilator-associated pneumonia: Prospective evaluation of the clinical pulmonary infection score as an early clinical predictor of outcome. Crit Care Med 2003;31: Vogelaers D, De BD, Foret F, et al. Patterns of antimicrobial therapy in severe nosocomial infections: Empiric choices, proportion of appropriate therapy, and adaptation rates A multicentre, observational survey in critically ill patients. Int J Antimicrob Agents 2010;35: Guidelines for the management of adults with hospitalacquired, ventilator-associated, and healthcare-associated pneumonia. Am J Respir Crit Care Med 2005;171: Eggimann P, Revelly JP. Should antibiotic combinations be used to treat ventilator-associated pneumonia? Semin Respir Crit Care Med 2006;27: Ibrahim EH, Ward S, Sherman G, et al. Experience with a clinical guideline for the treatment of ventilator-associated pneumonia. Crit Care Med 2001;29: Dortch MJ, Fleming SB, Kauffmann RM, et al. Infection reduction strategies including antibiotic stewardship protocols in surgical and trauma intensive care units are associated with reduced resistant gram-negative healthcareassociated infections. Surg Infect 2011;12: Kumar A, Zarychanski R, Light B, et al. Early combination antibiotic therapy yields improved survival compared with monotherapy in septic shock: A propensity-matched analysis. Crit Care Med 2010;38: Kumar A, Safdar N, Kethireddy S, Chateau D. A survival benefit of combination antibiotic therapy for serious infections associated with sepsis and septic shock is contingent only on the risk of death: A meta-analytic/ meta-regression study. Crit Care Med 2010;38: Garnacho-Montero J, Sa-Borges M, Sole-Violan J, et al. Optimal management therapy for Pseudomonas aeruginosa ventilator-associated pneumonia: An observational, multicenter study comparing monotherapy with combination antibiotic therapy. Crit Care Med 2007;35: Paul M, Silbiger I, Grozinsky S, et al. Beta lactam antibiotic monotherapy versus beta lactam-aminoglycoside antibiotic combination therapy for sepsis. Cochrane Database Syst Rev 2006;(1):CD Safdar N, Handelsman J, Maki DG. Does combination antimicrobial therapy reduce mortality in gram-negative bacteraemia? A meta-analysis. Lancet Infect Dis 2004;4: Aarts MA, Hancock JN, Heyland D, et al. Empiric antibiotic therapy for suspected ventilator-associated pneumonia: A systematic review and meta-analysis of randomized trials. Crit Care Med 2008;36: Salva S, Borgatta B, Rello J. Pneumonia in immunocompetent patients: Combination antibiotic therapy. Minerva Anestesiol 2014;80: Hilf M, Yu VL, Sharp J, Zuravleff JJ, et al. Antibiotic therapy for Pseudomonas aeruginosa bacteremia: Outcome correlations in a prospective study of 200 patients. Am J Med 1989;87: Pereira JM, Paiva JA, Rello J. Severe sepsis in communityacquired pneumonia Early recognition and treatment. Eur J Intern Med 2012;23: Mueller EW, Boucher BA. The use of extended-interval aminoglycoside dosing strategies for the treatment of moderate-to-severe infections encountered in critically ill surgical patients. Surg Infect 2009;10: Barza M, Ioannidis JP, Cappelleri JC, Lau J. Single or multiple daily doses of aminoglycosides: A meta-analysis. BMJ 1996;312: Nicolau DP, Freeman CD, Belliveau PP, et al. Experience with a once-daily aminoglycoside program administered to 2,184 adult patients. Antimicrob Agents Chemother 1995; 39: Address correspondence to: Dr. Addison K. May Division of Trauma and Surgical Critical Care Vanderbilt University Medical Center st Avenue South 404 Medical Arts Building Nashville, TN addison.may@vanderbilt.edu
Guess or get it right?
 Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION
 HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
Potential Conflicts of Interests
 Potential Conflicts of Interests Research Grants Agency for Healthcare Research and Quality Akers Bioscience, Inc. Pfizer, Inc. Scientific Advisory Boards Pfizer, Inc. Cadence Pharmaceuticals Kimberly
Potential Conflicts of Interests Research Grants Agency for Healthcare Research and Quality Akers Bioscience, Inc. Pfizer, Inc. Scientific Advisory Boards Pfizer, Inc. Cadence Pharmaceuticals Kimberly
Abstract. Introduction
 ORIGINAL ARTICLE INFECTIOUS DISEASES Accuracy of American Thoracic Society/Infectious Diseases Society of America criteria in predicting infection or colonization with multidrug-resistant bacteria at intensive-care
ORIGINAL ARTICLE INFECTIOUS DISEASES Accuracy of American Thoracic Society/Infectious Diseases Society of America criteria in predicting infection or colonization with multidrug-resistant bacteria at intensive-care
HAP/VAP care bundle interventions - a UK approach. Dr R G Masterton NHS Ayrshire & Arran
 HAP/VAP care bundle interventions - a UK approach Dr R G Masterton NHS Ayrshire & Arran How Hazardous Is Health Care? (Leape and Amalberti) Total lives lost per year 100,000 10,000 1,000 100 10 1 HAZARDOUS
HAP/VAP care bundle interventions - a UK approach Dr R G Masterton NHS Ayrshire & Arran How Hazardous Is Health Care? (Leape and Amalberti) Total lives lost per year 100,000 10,000 1,000 100 10 1 HAZARDOUS
Ventilator Associated
 Ventilator Associated Pneumonia: Key and Controversial Issues Christopher P. Michetti, MD, FACS Inova Fairfax Hospital, Falls Church, VA Forrest Dell Moore, MD, FACS Banner Healthcare System, Phoenix,
Ventilator Associated Pneumonia: Key and Controversial Issues Christopher P. Michetti, MD, FACS Inova Fairfax Hospital, Falls Church, VA Forrest Dell Moore, MD, FACS Banner Healthcare System, Phoenix,
Inadequate Empiric Antibiotic Therapy among Canadian. Hospitalized Solid-Organ Transplant Patients: Incidence and Impact on Hospital Mortality
 Inadequate Empiric Antibiotic Therapy among Canadian Hospitalized Solid-Organ Transplant Patients: Incidence and Impact on Hospital Mortality by Bassem Hamandi A thesis submitted in conformity with the
Inadequate Empiric Antibiotic Therapy among Canadian Hospitalized Solid-Organ Transplant Patients: Incidence and Impact on Hospital Mortality by Bassem Hamandi A thesis submitted in conformity with the
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Professor of Medicine Vice-Chairman, Department of Medicine SUNY at Stony Brook
 Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
The Clinical Management of Hospital Acquired Pneumonia. NHS Ayrshire & Arran
 The Clinical Management of Hospital Acquired Pneumonia Dr R G Masterton NHS Ayrshire & Arran What s new in HAP/VAP? Care bundles MRSA VAP Improving outcomes with current antimicrobial New antimicrobials
The Clinical Management of Hospital Acquired Pneumonia Dr R G Masterton NHS Ayrshire & Arran What s new in HAP/VAP? Care bundles MRSA VAP Improving outcomes with current antimicrobial New antimicrobials
Diagnosis of Ventilator- Associated Pneumonia: Where are we now?
 Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES
 MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES 1 Marin H. Kollef, MD Professor of Medicine Virginia E. and Sam J. Golman Chair in Respiratory Intensive Care Medicine Washington University School of
MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES 1 Marin H. Kollef, MD Professor of Medicine Virginia E. and Sam J. Golman Chair in Respiratory Intensive Care Medicine Washington University School of
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
Department of Clinical Pharmacy, University of Michigan College of Pharmacy, Pharmacy Faculty, Siam University, Bangkok, Thailand
 1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
Community Acquired & Nosocomial Pneumonias
 Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
Empirical Antibiotic Therapy Combo vs Mono : Best
 Empirical Antibiotic Therapy Combo vs Mono : Best Anand Kumar MD, FRCPC, FCCP, FCCM Professor of Medicine University of Manitoba Health Sciences Centre St. Boniface Hospital Winnipeg, Manitoba For available
Empirical Antibiotic Therapy Combo vs Mono : Best Anand Kumar MD, FRCPC, FCCP, FCCM Professor of Medicine University of Manitoba Health Sciences Centre St. Boniface Hospital Winnipeg, Manitoba For available
Marcos I. Restrepo, MD, MSc, FCCP
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Clinical Practice Management Guideline for Ventilator-Associated Pneumonia: Diagnosis, Treatment & Prevention
 Clinical for Ventilator-Associated Pneumonia: Diagnosis, Treatment & Prevention Background Ventilator-associated pneumonia (VAP), a pneumonia that develops 48hrs after initiation of mechanical ventilation,
Clinical for Ventilator-Associated Pneumonia: Diagnosis, Treatment & Prevention Background Ventilator-associated pneumonia (VAP), a pneumonia that develops 48hrs after initiation of mechanical ventilation,
Outline. Pharmacists Improving Outcomes in the Management of. of Infectious Diseases. Threats Against Desired Outcomes 7/11/2010
 Pharmacists Improving Outcomes in the Management of Infectious Diseases Christine Teng, MSc(Clin Pharm) BCPS Assistant Professor Dept of Pharmacy, National University of Singapore Principal Pharmacist
Pharmacists Improving Outcomes in the Management of Infectious Diseases Christine Teng, MSc(Clin Pharm) BCPS Assistant Professor Dept of Pharmacy, National University of Singapore Principal Pharmacist
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia
 Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
ICU Volume 11 - Issue 3 - Autumn Series
 ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
Speed is Life but a Sledgehammer Helps Too: Combination Antibiotic Therapy For Septic Shock
 Speed is Life but a Sledgehammer Helps Too: Combination Antibiotic Therapy For Septic Shock Anand Kumar MD, FRCPC, FCCP, FCCM Associate Professor of Medicine University of Manitoba Health Sciences Centre
Speed is Life but a Sledgehammer Helps Too: Combination Antibiotic Therapy For Septic Shock Anand Kumar MD, FRCPC, FCCP, FCCM Associate Professor of Medicine University of Manitoba Health Sciences Centre
Disclosures. Objectives. Procalcitonin: Pearls and Pitfalls in Daily Practice
 Procalcitonin: Pearls and Pitfalls in Daily Practice Sarah K Harrison, PharmD, BCCCP Clinical Pearl Disclosures The author of this presentation has no disclosures concerning possible financial or personal
Procalcitonin: Pearls and Pitfalls in Daily Practice Sarah K Harrison, PharmD, BCCCP Clinical Pearl Disclosures The author of this presentation has no disclosures concerning possible financial or personal
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT
 Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
Institute of Hygiene and Environmental Medicine. Charité University Medicine Berlin. Mail:
 AAC Accepts, published online ahead of print on 13 April 2009 Antimicrob. Agents Chemother. doi:10.1128/aac.01070-08 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 13 April 2009 Antimicrob. Agents Chemother. doi:10.1128/aac.01070-08 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions.
Implementation of guidelines for management of possible multidrug-resistant pneumonia in intensive care: an observational, multicentre cohort study
 Implementation of guidelines for management of possible multidrug-resistant pneumonia in intensive care: an observational, multicentre cohort study Daniel H Kett, Ennie Cano, Andrew A Quartin, Julie E
Implementation of guidelines for management of possible multidrug-resistant pneumonia in intensive care: an observational, multicentre cohort study Daniel H Kett, Ennie Cano, Andrew A Quartin, Julie E
P. aeruginosa: Present therapeutic options in Intensive Care. Y. Van Laethem (CHU St-Pierre & Université libre de Bruxelles, Brussels, Belgium)
 P. aeruginosa: Present therapeutic options in Intensive Care Y. Van Laethem (CHU St-Pierre & Université libre de Bruxelles, Brussels, Belgium) Activity vs Pseudomonas aeruginosa Pseudomonas aeruginosa
P. aeruginosa: Present therapeutic options in Intensive Care Y. Van Laethem (CHU St-Pierre & Université libre de Bruxelles, Brussels, Belgium) Activity vs Pseudomonas aeruginosa Pseudomonas aeruginosa
Pharmacologyonline 1: (2010) ewsletter Singh and Kochbar. Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of
 Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece
 A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
BC Sepsis Network Emergency Department Sepsis Guidelines
 The provincial Sepsis Clinical Expert Group developed the BC, taking into account the most up-to-date literature (references below) and expert opinion. For more information about the guidelines, and to
The provincial Sepsis Clinical Expert Group developed the BC, taking into account the most up-to-date literature (references below) and expert opinion. For more information about the guidelines, and to
Clinical characteristics of health care-associated pneumonia in a Korean teaching hospital
 Respiratory Medicine (2010) 104, 1729e1735 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Clinical characteristics of health care-associated pneumonia in a Korean teaching
Respiratory Medicine (2010) 104, 1729e1735 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Clinical characteristics of health care-associated pneumonia in a Korean teaching
Portugal. From SACiUCI to InfAUCI. Sepsis epidemiology: an update. You re only given a little spark of madness. You mustn t lose it.
 Sepsis epidemiology: an update Portugal João Gonçalves Pereira ICU director Vila Franca Xira Hospital From SACiUCI to InfAUCI You re only given a little spark of madness. You mustn t lose it. Robin Williams
Sepsis epidemiology: an update Portugal João Gonçalves Pereira ICU director Vila Franca Xira Hospital From SACiUCI to InfAUCI You re only given a little spark of madness. You mustn t lose it. Robin Williams
Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure
 Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Early- and Late-Onset Pneumonia: Is This Still a Useful Classification?
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 2009, p. 2714 2718 Vol. 53, No. 7 0066-4804/09/$08.00 0 doi:10.1128/aac.01070-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Early-
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 2009, p. 2714 2718 Vol. 53, No. 7 0066-4804/09/$08.00 0 doi:10.1128/aac.01070-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Early-
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016
 Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
La farmacologia in aiuto
 Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
ORIGINAL ARTICLE DOI: (e) ISSN Online: (p) ISSN Print: Anand Kumar Singh 1, Poonam Verma 2. Sciences, Dehradun
 ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
without the permission of the author Not to be copied and distributed to others
 Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY
 HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
VAP in COPD patients. Ignacio Martin-Loeches. St James s University Hospital. Trinity Centre for Health Sciences. Dublin Ireland.
 VAP in COPD patients Ignacio Martin-Loeches St James s University Hospital. Trinity Centre for Health Sciences. Dublin Ireland. Outline Pathophysiology Is enough information? COPD trends in ICU How do
VAP in COPD patients Ignacio Martin-Loeches St James s University Hospital. Trinity Centre for Health Sciences. Dublin Ireland. Outline Pathophysiology Is enough information? COPD trends in ICU How do
Guidelines 2017 for the management of hospitalacquired pneumonia (HAP) and. ventilator-associated. pneumonia (VAP)
 Guidelines 2017 for the management of hospitalacquired pneumonia (HAP) and ventilator-associated Modifiez le style des sous-titres du masque pneumonia (VAP) Filip Moerman Présentation pour les soins int
Guidelines 2017 for the management of hospitalacquired pneumonia (HAP) and ventilator-associated Modifiez le style des sous-titres du masque pneumonia (VAP) Filip Moerman Présentation pour les soins int
Terapia delle infezioni da Pseudomonas aeruginosa MDR
 Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches
 Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
Impact of Inactive Empiric Antimicrobial Therapy on Inpatient Mortality and Length of Stay
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2006, p. 3355 3360 Vol. 50, No. 10 0066-4804/06/$08.00 0 doi:10.1128/aac.00466-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Impact
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2006, p. 3355 3360 Vol. 50, No. 10 0066-4804/06/$08.00 0 doi:10.1128/aac.00466-06 Copyright 2006, American Society for Microbiology. All Rights Reserved. Impact
Severe and Tertiary Peritonitis
 Severe and Tertiary Peritonitis Addison K. May, MD FACS Professor of Surgery and Anesthesiology Division of Trauma and Surgical Critical Care Vanderbilt University Medical Center PS204: The Bad Infections:
Severe and Tertiary Peritonitis Addison K. May, MD FACS Professor of Surgery and Anesthesiology Division of Trauma and Surgical Critical Care Vanderbilt University Medical Center PS204: The Bad Infections:
The Value of Routine Microbial Investigation in Ventilator-Associated Pneumonia
 The Value of Routine Microbial Investigation in Ventilator-Associated Pneumonia JORDI RELLO, MIGUEL GALLEGO, DOLORS MARISCAL, ROSARIO SOÑORA, and JORDI VALLES Intensive Care, Respiratory and Microbiology
The Value of Routine Microbial Investigation in Ventilator-Associated Pneumonia JORDI RELLO, MIGUEL GALLEGO, DOLORS MARISCAL, ROSARIO SOÑORA, and JORDI VALLES Intensive Care, Respiratory and Microbiology
Terapia della candidiasi addomaniale
 Verona 16 marzo 2018 Terapia della candidiasi addomaniale Pierluigi Viale Infectious Disease Unit Teaching Hospital S. Orsola Malpighi Bologna INTRA ABDOMINAL CANDIDIASIS open questions a single definition
Verona 16 marzo 2018 Terapia della candidiasi addomaniale Pierluigi Viale Infectious Disease Unit Teaching Hospital S. Orsola Malpighi Bologna INTRA ABDOMINAL CANDIDIASIS open questions a single definition
CARE OF THE ADULT PNEUMONIA PATIENT
 Care Guideline CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: The target audience for this Care Guideline is all MultiCare providers and staff, including those associated with our clinically integrated
Care Guideline CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: The target audience for this Care Guideline is all MultiCare providers and staff, including those associated with our clinically integrated
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients
 Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Top 5 papers in clinical mycology
 Top 5 papers in clinical mycology Dirk Vogelaers Department of General Internal Medicine University Hospital Ghent Joint symposium BVIKM/BSIMC and SBMHA/BVMDM Influenza-associated aspergillosis in critically
Top 5 papers in clinical mycology Dirk Vogelaers Department of General Internal Medicine University Hospital Ghent Joint symposium BVIKM/BSIMC and SBMHA/BVMDM Influenza-associated aspergillosis in critically
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine
 Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital
 Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
New Surveillance Definitions for VAP
 New Surveillance Definitions for VAP 2012 Critical Care Canada Forum Toronto Dr. John Muscedere Associate Professor of Medicine, Queen s University Kingston, Ontario Presenter Disclosure Dr. J. G. Muscedere
New Surveillance Definitions for VAP 2012 Critical Care Canada Forum Toronto Dr. John Muscedere Associate Professor of Medicine, Queen s University Kingston, Ontario Presenter Disclosure Dr. J. G. Muscedere
PREVALENCE PATTERN OF MORBIDITY AND MORTALITY IN VENTILATION ASSOCIATED PNEUMONIA (VAP) PATIENTS OF INTENSIVE CARE UNIT (ICU) IN MAHARASHTRA REGION.
 Original research article International Journal of Medical Science and Education pissn- 2348 4438 eissn-2349-3208 PREVALENCE PATTERN OF MORBIDITY AND MORTALITY IN VENTILATION ASSOCIATED PNEUMONIA (VAP)
Original research article International Journal of Medical Science and Education pissn- 2348 4438 eissn-2349-3208 PREVALENCE PATTERN OF MORBIDITY AND MORTALITY IN VENTILATION ASSOCIATED PNEUMONIA (VAP)
PREVENTION AND TREATMENT OF BACTERIAL INFECTIONS IN CIRRHOSIS
 PREVENTION AND TREATMENT OF BACTERIAL INFECTIONS IN CIRRHOSIS Dr. J. Fernández. Head of the Liver Unit Hospital Clinic Barcelona, Spain AEEH Postgraduate Course, Madrid, February 15 2017 Prevalence of
PREVENTION AND TREATMENT OF BACTERIAL INFECTIONS IN CIRRHOSIS Dr. J. Fernández. Head of the Liver Unit Hospital Clinic Barcelona, Spain AEEH Postgraduate Course, Madrid, February 15 2017 Prevalence of
Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), MT. Nguyen 1, TD. Dang Nguyen 1* 1
 Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), 195-202 Investigation on hospital-acquired pneumonia and the association between hospital-acquired pneumonia and chronic comorbidity at the Department
Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), 195-202 Investigation on hospital-acquired pneumonia and the association between hospital-acquired pneumonia and chronic comorbidity at the Department
SBUH Aminoglycoside Dosing Protocol
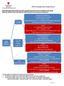 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
BIP Endotracheal Tube
 Bactiguard Infection Protection BIP Endotracheal Tube For prevention of healthcare associated infections Ventilator associated pneumonia Infections of the respiratory tract are serious and common healthcare
Bactiguard Infection Protection BIP Endotracheal Tube For prevention of healthcare associated infections Ventilator associated pneumonia Infections of the respiratory tract are serious and common healthcare
VAP Are strict diagnostic criteria advisable?
 VAP Are strict diagnostic criteria advisable? Javier Garau, MD, PhD 18th Infection and Sepsis Symposium, Porto, 27th February 2013 Limitations of current definitions Alternatives -Streamlined definition
VAP Are strict diagnostic criteria advisable? Javier Garau, MD, PhD 18th Infection and Sepsis Symposium, Porto, 27th February 2013 Limitations of current definitions Alternatives -Streamlined definition
Ventilator Associated Pneumonia. ICU Fellowship Training Radboudumc
 Ventilator Associated Pneumonia ICU Fellowship Training Radboudumc Attributable mortality VAP Meta-analysis of individual patient data from randomized prevention studies Attributable mortality mainly results
Ventilator Associated Pneumonia ICU Fellowship Training Radboudumc Attributable mortality VAP Meta-analysis of individual patient data from randomized prevention studies Attributable mortality mainly results
Biomarkers in sepsis: Utility in critical care
 Biomarkers in sepsis: Utility in critical care Fathima Paruk, PhD Charlotte Maxeke Johannesburg Academic Hospital and University of Witwatersrand Kumar A et al, Chest 2009; 136:1237-48. von Gunten et al
Biomarkers in sepsis: Utility in critical care Fathima Paruk, PhD Charlotte Maxeke Johannesburg Academic Hospital and University of Witwatersrand Kumar A et al, Chest 2009; 136:1237-48. von Gunten et al
Implementation and evaluation of the impact of a "ventilator-bundle at Kinshasa University Clinics: Before and after study.
 Research Article http://www.alliedacademies.org/journal-infectious-diseases-medical-microbiology/ Implementation and evaluation of the impact of a "ventilator-bundle at Kinshasa University Clinics: Before
Research Article http://www.alliedacademies.org/journal-infectious-diseases-medical-microbiology/ Implementation and evaluation of the impact of a "ventilator-bundle at Kinshasa University Clinics: Before
Consequences for the clinicians
 30th Symposium : What will change in your daily practice with the new Elewijt, 26-05-2008 EUCAST breakpoints for antibiotic susceptibility testing Consequences for the clinicians Y.Van Laethem,MD CHU St
30th Symposium : What will change in your daily practice with the new Elewijt, 26-05-2008 EUCAST breakpoints for antibiotic susceptibility testing Consequences for the clinicians Y.Van Laethem,MD CHU St
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more)
 Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
ALERT. Clinical microbiology considerations related to the emergence of. New Delhi metallo beta lactamases (NDM 1) and Klebsiella
 ALERT Clinical microbiology considerations related to the emergence of New Delhi metallo beta lactamases (NDM 1) and Klebsiella pneumoniae carbapenemases (KPC) amongst hospitalized patients in South Africa
ALERT Clinical microbiology considerations related to the emergence of New Delhi metallo beta lactamases (NDM 1) and Klebsiella pneumoniae carbapenemases (KPC) amongst hospitalized patients in South Africa
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center
 CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
Choc septique. Frédéric Pène
 Choc septique Frédéric Pène Réanimation Médicale, Hôpital Cochin, AP-HP Université Paris Descartes Institut Cochin, Inserm U1016, CNRS UMR-8104, Département 3i No conflict of interest A 54 y.o. male patient
Choc septique Frédéric Pène Réanimation Médicale, Hôpital Cochin, AP-HP Université Paris Descartes Institut Cochin, Inserm U1016, CNRS UMR-8104, Département 3i No conflict of interest A 54 y.o. male patient
Title:Bloodstream infections and sepsis in Greece: over-time change of epidemiology and impact of de-escalation on final outcome
 Author's response to reviews Title:Bloodstream infections and sepsis in Greece: over-time change of epidemiology and impact of de-escalation on final outcome Authors: Marina Koupetori (e_lambros@hotmail.gr)
Author's response to reviews Title:Bloodstream infections and sepsis in Greece: over-time change of epidemiology and impact of de-escalation on final outcome Authors: Marina Koupetori (e_lambros@hotmail.gr)
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017
 i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING
 CLINICAL EVIDENCE GUIDE WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING Weaning readiness and spontaneous breathing trial monitoring protocols can help you make the right weaning decisions at
CLINICAL EVIDENCE GUIDE WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING Weaning readiness and spontaneous breathing trial monitoring protocols can help you make the right weaning decisions at
Augmented Renal Clearance: Let s Get the Discussion Flowing
 Augmented Renal Clearance: Let s Get the Discussion Flowing Terry Makhoul, PharmD PGY-2 Emergency Medicine Pharmacy Resident University of Rochester Medical Center Strong Memorial Hospital Disclosures
Augmented Renal Clearance: Let s Get the Discussion Flowing Terry Makhoul, PharmD PGY-2 Emergency Medicine Pharmacy Resident University of Rochester Medical Center Strong Memorial Hospital Disclosures
Initiating Aminoglycosides Safely. Last updated: July 2016, Version 5 Questions/Comments?
 Initiating Aminoglycosides Safely Last updated: July 2016, Version 5 Questions/Comments? Email Mark.McIntyre@uhn.ca Click orange buttons to navigate protocol. Index: Aminoglycoside Dosing Algorithms Objective
Initiating Aminoglycosides Safely Last updated: July 2016, Version 5 Questions/Comments? Email Mark.McIntyre@uhn.ca Click orange buttons to navigate protocol. Index: Aminoglycoside Dosing Algorithms Objective
Community Acquired Pneumonia. Background & Rationale to North American Guidelines. Lionel Mandell MD FRCPC Brussels Belgium
 Community Acquired Pneumonia Background & Rationale to North American Guidelines Lionel Mandell MD FRCPC Brussels Belgium Consider Impact of the disease Issues to reflect upon Impact of the Disease 3-4
Community Acquired Pneumonia Background & Rationale to North American Guidelines Lionel Mandell MD FRCPC Brussels Belgium Consider Impact of the disease Issues to reflect upon Impact of the Disease 3-4
The Ever Changing World of Sepsis Management. Laura Evans MD MSc Medical Director of Critical Care Bellevue Hospital
 The Ever Changing World of Sepsis Management Laura Evans MD MSc Medical Director of Critical Care Bellevue Hospital COI Disclosures No financial interests to disclose Learning Objectives Review the evolution
The Ever Changing World of Sepsis Management Laura Evans MD MSc Medical Director of Critical Care Bellevue Hospital COI Disclosures No financial interests to disclose Learning Objectives Review the evolution
Intracheal antibiotics administration
 Intracheal antibiotics administration Jean Chastre, M.D. www.reamedpitie.com Disclosure Conflicts of interest: Consulting or Lecture fees: Bayer, Pfizer, Cubist/Merck, Basilea, Kenta/Aridis, Roche, AstraZeneca/Medimmune
Intracheal antibiotics administration Jean Chastre, M.D. www.reamedpitie.com Disclosure Conflicts of interest: Consulting or Lecture fees: Bayer, Pfizer, Cubist/Merck, Basilea, Kenta/Aridis, Roche, AstraZeneca/Medimmune
Antisepsis Bath and Oral.. Should We Change Practice? DR AZMIN HUDA ABDUL RAHIM
 Antisepsis Bath and Oral.. Should We Change Practice? DR AZMIN HUDA ABDUL RAHIM Chlorhexidine Exposure in ICU Chlorhexidine gluconate Long acting topical antiseptic In use since 1954 Water soluble Remains
Antisepsis Bath and Oral.. Should We Change Practice? DR AZMIN HUDA ABDUL RAHIM Chlorhexidine Exposure in ICU Chlorhexidine gluconate Long acting topical antiseptic In use since 1954 Water soluble Remains
Ventilator Associated Pneumonia. ICU Fellowship Training Radboudumc
 Ventilator Associated Pneumonia ICU Fellowship Training Radboudumc Attributable mortality VAP Meta-analysis of individual patient data from randomized prevention studies Attributable mortality mainly results
Ventilator Associated Pneumonia ICU Fellowship Training Radboudumc Attributable mortality VAP Meta-analysis of individual patient data from randomized prevention studies Attributable mortality mainly results
CURRENT GUIDELINES FOR SEPSIS MANAGEMENT
 HELLENIC SEPSIS STUDY GROUP www.sepsis.gr CURRENT GUIDELINES FOR SEPSIS MANAGEMENT Evangelos J. Giamarellos-Bourboulis, MD, PhD Associate Professor of Medicine 4 th Department of Internal Medicine, National
HELLENIC SEPSIS STUDY GROUP www.sepsis.gr CURRENT GUIDELINES FOR SEPSIS MANAGEMENT Evangelos J. Giamarellos-Bourboulis, MD, PhD Associate Professor of Medicine 4 th Department of Internal Medicine, National
Development of a Clinical Tracheostomy Score to Identify Spinal Cord Injury Patients Requiring Prolonged Ventilator Support
 Development of a Clinical Tracheostomy Score to Identify Spinal Cord Injury Patients Requiring Prolonged Ventilator Support Dane Scantling, Teerin Meckmongkol, Brendan McCracken Drexel University College
Development of a Clinical Tracheostomy Score to Identify Spinal Cord Injury Patients Requiring Prolonged Ventilator Support Dane Scantling, Teerin Meckmongkol, Brendan McCracken Drexel University College
Pneumonia Community-Acquired Healthcare-Associated
 Pneumonia Community-Acquired Healthcare-Associated Edwin Yu Clin Infect Dis 2007;44(S2):27-72 Am J Respir Crit Care Med 2005; 171:388-416 IDSA / ATS Guidelines Microbiology Principles and Practice of Infectious
Pneumonia Community-Acquired Healthcare-Associated Edwin Yu Clin Infect Dis 2007;44(S2):27-72 Am J Respir Crit Care Med 2005; 171:388-416 IDSA / ATS Guidelines Microbiology Principles and Practice of Infectious
Targeted literature review:
 Targeted literature review: What are the key infection prevention and control recommendations to inform a minimising ventilator associated pneumonia (VAP) quality improvement tool? Part of HAI Delivery
Targeted literature review: What are the key infection prevention and control recommendations to inform a minimising ventilator associated pneumonia (VAP) quality improvement tool? Part of HAI Delivery
Initial Resuscitation of Sepsis & Septic Shock
 Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
An Early Predictor of the Outcome of Patients with Ventilator-associated Pneumonia
 Original Article 274 An Early Predictor of the Outcome of Patients with Ventilator-associated Pneumonia Kuo-Tung Huang, MD; Chia-Cheng Tseng, MD; Wen-Feng Fang, MD; Meng-Chih Lin, MD Background: Ventilator-associated
Original Article 274 An Early Predictor of the Outcome of Patients with Ventilator-associated Pneumonia Kuo-Tung Huang, MD; Chia-Cheng Tseng, MD; Wen-Feng Fang, MD; Meng-Chih Lin, MD Background: Ventilator-associated
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
Predictive scoring model of mortality in Gram-negative bloodstream infection
 ORIGINAL ARTICLE INFECTIOUS DISEASES Predictive scoring model of mortality in Gram-negative bloodstream infection M. N. Al-Hasan 1,2, B. D. Lahr 3, J. E. Eckel-Passow 3 and L. M. Baddour 2 1) Department
ORIGINAL ARTICLE INFECTIOUS DISEASES Predictive scoring model of mortality in Gram-negative bloodstream infection M. N. Al-Hasan 1,2, B. D. Lahr 3, J. E. Eckel-Passow 3 and L. M. Baddour 2 1) Department
Pneumonia Severity Scores:
 Pneumonia Severity Scores: Are they Accurate Predictors of Mortality? JILL McEWEN, MD FRCPC Clinical Professor Department of Emergency Medicine University of British Columbia Vancouver, BC Canada President,
Pneumonia Severity Scores: Are they Accurate Predictors of Mortality? JILL McEWEN, MD FRCPC Clinical Professor Department of Emergency Medicine University of British Columbia Vancouver, BC Canada President,
The EMPIRICUS trial the final nail in the coffin of empirical antifungal therapy in the intensive care unit?
 Editorial The EMPIRICUS trial the final nail in the coffin of empirical antifungal therapy in the intensive care unit? Michael Osthoff 1,2, Nina Khanna 1,2, Martin Siegemund 3 1 Division of Infectious
Editorial The EMPIRICUS trial the final nail in the coffin of empirical antifungal therapy in the intensive care unit? Michael Osthoff 1,2, Nina Khanna 1,2, Martin Siegemund 3 1 Division of Infectious
La neutropenia febbrile
 XII Corso Avanzato di Terapia Antibiotica Pisa, 15-16 novembre 2017 La neutropenia febbrile Alessandra Micozzi Dipartimento di Biotecnologie Cellulari ed Ematologia Sapienza Università di Roma Fever developing
XII Corso Avanzato di Terapia Antibiotica Pisa, 15-16 novembre 2017 La neutropenia febbrile Alessandra Micozzi Dipartimento di Biotecnologie Cellulari ed Ematologia Sapienza Università di Roma Fever developing
Acute Kidney Injury for the General Surgeon
 Acute Kidney Injury for the General Surgeon UCSF Postgraduate Course in General Surgery Maui, HI March 20, 2011 Epidemiology & Definition Pathophysiology Clinical Studies Management Summary Hobart W. Harris,
Acute Kidney Injury for the General Surgeon UCSF Postgraduate Course in General Surgery Maui, HI March 20, 2011 Epidemiology & Definition Pathophysiology Clinical Studies Management Summary Hobart W. Harris,
ORIGINAL ARTICLE /j x. Greece; and 4 Tufts University School of Medicine, Boston, MA, USA
 ORIGINAL ARTICLE 10.1046/j.1469-0691.2004.01043.x Colistin treatment in patients with ICU-acquired infections caused by multiresistant Gram-negative bacteria: the renaissance of an old antibiotic A. S.
ORIGINAL ARTICLE 10.1046/j.1469-0691.2004.01043.x Colistin treatment in patients with ICU-acquired infections caused by multiresistant Gram-negative bacteria: the renaissance of an old antibiotic A. S.
Sepsis Treatment: Early Identification Remains the Key Issue
 Sepsis Treatment: Early Identification Remains the Key Issue Marin H. Kollef, MD Professor of Medicine Washington University School of Medicine Director, Medical Critical Care Director, Respiratory Care
Sepsis Treatment: Early Identification Remains the Key Issue Marin H. Kollef, MD Professor of Medicine Washington University School of Medicine Director, Medical Critical Care Director, Respiratory Care
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Educational Workshop
 Educational Workshop EW02: Management of severe sepsis and septic shock anno 2015 Arranged with ESGBIS & International Sepsis Forum (ISF) Convenors: W. Joost Wiersinga, Amsterdam, NL Tom van der Poll,
Educational Workshop EW02: Management of severe sepsis and septic shock anno 2015 Arranged with ESGBIS & International Sepsis Forum (ISF) Convenors: W. Joost Wiersinga, Amsterdam, NL Tom van der Poll,
Guidelines. 14 Nov Marc Bonten
 Guidelines 14 Nov 2014 Marc Bonten Treatment of Community-Acquired Pneumonia SWAB/ NVALT guideline 2011, replaced SWAB guideline 2005 Empirical treatment must cover the most likely causative pathogen.
Guidelines 14 Nov 2014 Marc Bonten Treatment of Community-Acquired Pneumonia SWAB/ NVALT guideline 2011, replaced SWAB guideline 2005 Empirical treatment must cover the most likely causative pathogen.
The promise of nebulized antibiotic therapy
 1 st ATHENA International Conference Athens, 19-20 November 2015 Let s Talk About Inhaled Antibiotics Inhaled Antibiotics: The Story Stijn BLOT Dept. of Internal Medicine Faculty of Medicine & Health Science
1 st ATHENA International Conference Athens, 19-20 November 2015 Let s Talk About Inhaled Antibiotics Inhaled Antibiotics: The Story Stijn BLOT Dept. of Internal Medicine Faculty of Medicine & Health Science
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Ventilator-associated pneumonia after pediatric cardiac surgery in southern Taiwan
 J Microbiol Immunol Infect. 2009;42:413-419 Ventilator-associated pneumonia after pediatric cardiac surgery in southern Taiwan Chia-Wan Tang 1, Po-Yen Liu 1, Yung-Feng Huang 1, Jun-Yen Pan 2, Susan Shin-Jung
J Microbiol Immunol Infect. 2009;42:413-419 Ventilator-associated pneumonia after pediatric cardiac surgery in southern Taiwan Chia-Wan Tang 1, Po-Yen Liu 1, Yung-Feng Huang 1, Jun-Yen Pan 2, Susan Shin-Jung
