Pediatric Heart Transplantation after Declaration of Cardiocirculatory Death
|
|
|
- Johnathan Davis
- 6 years ago
- Views:
Transcription
1 The new england journal of medicine brief report Pediatric Heart Transplantation after Declaration of Cardiocirculatory Death Mark M. Boucek, M.D., Christine Mashburn, B.S.N., Susan M. Dunn, M.B.A., Rebecca Frizell, B.S.N., Leah Edwards, Ph.D., Biagio Pietra, M.D., and David Campbell, M.D., for the Denver Children s Pediatric Heart Transplant Team* SUMMARY In three infants awaiting orthotopic cardiac transplantation, transplantation was successfully performed with the use of organs from donors who had died from cardiocirculatory causes. The three recipients had blood group O and were in the highestrisk waiting-list category. The mean age of donors was 3.7 days, and the mean time to death after withdrawal from life support was 18.3 minutes. The 6-month survival rate was 100% for the 3 transplant recipients and 84% for 17 control infants who received transplants procured through standard organ donation. The mean number of rejection episodes among the three infants during the first 6 months after surgery was 0.3 per patient, as compared with 0.4 per patient among the controls. Echocardiographic measures of ventricular size and function at 6 months were similar among the three infants and the controls (left ventricular shortening fraction, 43.6% and 44.9%, respectively; P = 0.73). No late deaths (within 3.5 years) have occurred in the three infants, and they have had functional and immunologic outcomes similar to those of controls. Mortality while awaiting a transplant is an order of magnitude higher in infants than in adults, and donors who died from cardiocirculatory causes offer an opportunity to decrease this waiting-list mortality. Pediatric heart transplantation after the declaration of brain death in donors has been performed for more than 25 years in more than 6000 recipients. 1 The first successful heart-transplant procedure in an infant was reported 20 years ago, and decades-long survival has been reported. 1,2 The average survival for children who are alive 1 year after transplantation is more than 15 years and exceeds that of adults. 3 However, the risk of death while awaiting a donor is highest for children awaiting a cardiac transplant. 4 Infant heart-transplant recipients face up to a 25% waiting-list mortality, which is an order of magnitude higher than that of adult heart-transplant recipients. 4,5 Mechanical circulatory support, which can be crucial for many adult heart-transplant recipients, is generally unavailable for infants. Organ donation after death from cardiocirculatory causes has been increasingly used for kidney, liver, and even lung transplantation. 6 The first successful heart transplantation in an adult involved a donor who died from cardiocirculatory causes, 7 but concerns about the vulnerability of the heart to ischemic injury has limited further transplantation in adults of hearts from donors who died from cardiocirculatory causes. To our knowledge, there have been no previous reports of transplantation in children of hearts from donors who died from cardiocirculatory causes. From the Department of Pediatrics, Joe DiMaggio Children s Hospital, Hollywood, FL (M.M.B., C.M.); Donor Alliance, Denver (S.M.D., R.F.); United Network for Organ Sharing, Richmond, VA (L.E.); and the Division of Pediatrics and Cardiothoracic Surgery, University of Colorado Health Sciences Center, Denver (B.P., D.C.). Address reprint requests to Dr. Boucek at the Department of Pediatrics, Joe DiMaggio Children s Hospital, 1150 North Ave., Suite 575, Hollywood, FL, 33021, or at mboucek@mhs.net. *Members of the Denver Children s Hospital Pediatric Heart Transplant Team are listed in the Appendix. N Engl J Med 2008;359: Copyright 2008 Massachusetts Medical Society. n engl j med 359;7 august 14,
2 The new england journal of medicine However, pediatric heart transplantation has been performed after prolonged ischemic injury in a donor, including in children who have died from the sudden infant death syndrome, and the results were similar to those for donors without ischemic cardiac injury. 1,8 On the basis of experiments in animals, heart transplantation involving donors who died from cardiocirculatory causes can be performed successfully. 9 End-of-life care is an important part of the family-centered environment in pediatric care facilities, and families of dying children overwhelmingly support organ donation. In the typical children s hospital, on any given day, there are between 2.2 and 10.6 children who will die in the hospital, and approximately half of these children were receiving ventilator support and were hospitalized for a mean of 16 days before death. 10 A survey at a leading children s hospital reported that 35% of deaths followed withdrawal of life support, and transplants from donors who died from cardiocirculatory causes would have been the only possible route to organ donation available to the family. 11 According to the same survey, 75% of patients died within 30 minutes after the withdrawal of life support. Thus, a child s death can be anticipated and considered within a family-centered end-of-life care plan, which can include the possibility of donation after withdrawal of life support and subsequent circulatory or cardiac death. We report on an institutional clinical trial of heart transplantation involving three infants who underwent orthotopic transplantation of hearts from donors who died from cardiocirculatory causes. The recipients were followed for a minimum of 6 months after surgery, while receiving standard immunosuppression therapy and undergoing surveillance for rejection episodes. Methods The transplantations were performed between May 2004 and May 2007 at the Denver Children s Hospital. Written informed consent was obtained from the parents of the recipient infants as part of the protocol, which was approved by the institutional review board and the hospital ethics committee. Families of all infants (<18 months old) who were potential transplant recipients (with United Network for Organ Sharing [UNOS] status 1A) were given the options of consenting to receive an organ from a donor who died from cardiocirculatory causes or from a donor after the declaration of brain death. Physicians not involved in the care of recipients made the medical decision to withdraw life support in potential donors, with the consent of their families, on the basis of the futility of ongoing care and the requirement for life support to maintain viability; the decision was made independently of considerations of organ donation. Families of potential donors who were predicted to die from cardiocirculatory causes were then referred to the organ-procurement organization. If the organization had a local potential recipient of a compatible blood group awaiting heart transplantation and with the highest UNOS status (1A), the family was given the option of organ donation from a donor who died from cardiocirculatory causes. In addition to the three donors described here, nine other potential donors underwent withdrawal from life support and died during the study but could not donate because there was no suitable recipient. Written informed consent for donation, as well as for the use of heparin and invasive central catheters, was obtained from the parents or guardians of patients who died from cardiocirculatory causes by the organ-procurement organization. Organ-Donation Protocol Donor care was provided under the direction of the intensive care team. Withdrawal of life-supporting ventilation was performed in the operating room by the intensivist and the primary nurse. On one occasion, the family chose to be with their child during withdrawal of life support. Each patient was prepared for surgery and monitored with the use of electrocardiography and pulse oximetry. Femoral venous and arterial sheaths were placed with the use of local anesthesia, and an initial heparin bolus of 100 U per kilogram of body weight was given intravenously. Comfort care was given by the intensive care team and included sedation and analgesia typical for withdrawal of life support: fentanyl at a mean dose of 4 µg per kilogram and lorazepam at a mean dose of 0.1 mg per kilogram. Extubation was performed, followed by an additional intravenous dose of 300 U of heparin per kilogram. The attending physician in the critical care unit monitored the patient for evidence of cardiocirculatory function by means of auscultation and observation for arterial pulsation. 710 n engl j med 359;7 august 14, 2008
3 Brief Report When cardiocirculatory function ceased, the first patient was observed for 3 minutes before death was declared and the organ-donation process initiated. On the basis of recommendations of the ethics committee, for the other two donors, the observation period was shortened to 1.25 minutes. If death occurred within 30 minutes after extubation, the patient was considered to be a candidate for donation, and cold preservation fluid (30 to 50 ml per kilogram) was infused through the distal port of a balloon arterial catheter placed in the ascending aorta. At the same time, a median sternotomy was performed, and topical cooling was begun. The inferior vena cava was immediately opened. In the second and third donors, venous-blood withdrawal was performed simultaneously with aortic infusion to prevent cardiac distention. After organ donation, the family of the donor was offered the choice of spending time with their child. Transplantation and Follow-up Transplantation was performed with the use of standard techniques, and routine immunosuppression therapy was started. Rejection surveillance was performed according to clinical and echocardiographic criteria. Troponin I levels were measured before extubation of the donor and 12 hours after transplantation. Statistical Analysis Both the data and safety monitoring board and the hospital ethics committee reviewed the outcome for each transplant recipient. The primary end point was death within 6 months after transplantation. Secondary end points were waiting time to transplantation, systolic function at 6 months (as determined on echocardiography), and occurrence of a rejection episode within 6 months. The continuous variables were compared between the three recipients and control infants with the use of a two-sided t-test. P values less than 0.05 were considered to indicate statistical significance. Results Transplantation Orthotopic heart transplantation involving donors who died from cardiocirculatory causes was performed in three recipients at a mean age of 2.2 months. The diagnosis leading to transplantation was complex congenital heart disease in two patients (one with a double-outlet right ventricle, transposition of the great vessels, a ventricular septal defect, and coarctation and the other with a hypoplastic left ventricle, mitral stenosis, aortic stenosis, and severely restricted atrial septal communication) and, in the third patient, severe dilated cardiomyopathy requiring continuous intravenous inotropic support. Both infants with congenital heart disease had previously undergone procedures to either attempt to correct or to palliate the anatomical problem and were believed to be at an unacceptably high risk for further interventions. The first recipient had undergone cardiac repair and was discharged home before being readmitted for cardiovascular collapse associated with coronary artery occlusion and left ventricular infarction. Extracorporeal membrane oxygenation was initiated before transplantation to maintain cardiac output, and he required such support for 36 hours after transplantation. Table 1. Characteristics of Heart Transplantation Involving Three Donors Who Died from Cardiocirculatory Causes.* Donor Time to Death after Withdrawal of Life Support min Total Ischemic Time Before Withdrawal of Life Support (in Donor) Troponin I Level ng/ml After Transplantation (in Recipient) Recipient Outcome at 6 Mo Alive Alive Alive All 18.3± ±51 0.3±0.2 60±58 * Plus minus values are means ±SD. n engl j med 359;7 august 14,
4 The new england journal of medicine After explantation of the donor s heart, the mean cold ischemic time was 106 minutes and the mean total ischemic time (to aortic cross-clamp removal in the recipient) was 162 minutes (Table 1). The mean troponin I level at 12 hours after surgery was 60 ng per milliliter. The postoperative course and amount of inotropic support did not differ from those of traditional donors. The mean length of hospital stay after transplantation was 20 days, similar to that among traditional transplant recipients. Heart transplantation was performed in 17 infants less than 18 months old (mean age, 3.0 months), with the use of traditional donation after brain death, at Denver Children s Hospital during the same period. The 6-month survival rate was 100% among the 3 recipients of transplants from donors who died from cardiocirculatory causes and 84% among the 17 recipients of transplants from traditional donors. Coronary artery disease has not developed in any of the patients whose donors died from cardiocirculatory causes. Care of Donors All the donors who died from cardiocirculatory causes were born at other hospitals and were transferred for neonatal critical care. They underwent continuous bedside amplitude-integrated electroencephalography and daily neurologic examinations, which revealed severe neurologic injury. A complete 16-lead electroencephalogram and a separate, formal neurologic consultation were obtained, confirming the injury and the poor prognosis, before the decision was made to withdraw life support. Organ donation followed release by the coroner. The mean time to declaration of death was 18.3 minutes (range, 11.5 to 27.5) (Table 1). The cause of death of all three donors was birth asphyxia; in one, the asphyxia was precipitated by placental rupture. The mean age at donation was 3.7 days, and the mean weight at donation was 3.2 kg. The mean troponin I level before withdrawal of life support was 0.33 ng per milliliter (normal level, <0.10). All families of donors who died from cardiocirculatory causes chose to meet only with the critical care staff and staff of the organ-procurement organization after donation. The families reported no adverse experiences associated with this family-centered approach to end-of-life care and organ donation. Follow-up All three heart-transplant recipients survived to 6 months. The mean number of rejection episodes was 0.3 per patient, which was not significantly different from the rate of 0.4 episode when standard organ donation was used. Echocardiographic measures of cardiac function were similar between the three recipients and the controls. The mean (±SD) left ventricular shortening fraction during systole at 6 months was 43.6±3.4% among the three patients who received transplants from donors who died from cardiocirculatory causes and 44.9±6.6% among controls (P = 0.73). The left ventricular end-diastolic volume (expressed as the percent of the predicted normal value) was 72.6±13% among the three recipients and 81.9±16% among controls (P = 0.36). Discussion Children, and infants in particular, have the greatest risk of death while awaiting orthotopic heart transplantation. In addition, increased waiting time before transplantation adversely affects late neurologic development. 12 Many children die in children s hospitals each day after withdrawal of futile care. Thus, we developed this clinical trial of the feasibility of pediatric heart transplantation involving donors who died from cardiocirculatory causes. Before the trial was begun, an extensive period of education, discussion, and preparation was undertaken within our hospital and in programs already using donors who died from cardiocirculatory causes. After each transplantation involving these donors, there was extensive institutional debriefing and review by the ethics committee and the data and safety monitoring board. The outcomes after transplantation of hearts from donors who died from cardiocirculatory causes were similar to those associated with traditional organ donation. All three recipients survived despite being at high risk for death, with excellent late heart function and no evidence of increased immunologic risk. The small number of patients involved limits the conclusions that can be drawn beyond proof of principle. Still, the potential effect is large. During the 3-year period of this trial, a total of 12 potential donors who died from cardiocirculatory causes were identified, 712 n engl j med 359;7 august 14, 2008
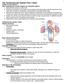
5 Brief Report which could represent a 70% increase in organ donation (based on the total number of transplantations in infants at Denver Children s Hospital) and confirms previous estimates. 11 However, during this same 3-year period, only one pediatric heart donor who was declared braindead and no newborn heart donors defined by traditional criteria were identified within Denver Children s Hospital. Thus, even just the three transplants from donors who died from cardiocirculatory causes represent a 300% increase in the rate of local donation. The donation protocol we used for patients who died from cardiocirculatory causes was successful, but some features may not be required. The mean time to death was 18 minutes, less than the maximum of 30 minutes according to the protocol. The analgesia regimen given as comfort care at the time of withdrawal from life support actually involved lower doses than would have been given to similar infants who could not be considered for organ donation. The dose of heparin has not been critically evaluated but is within the range used for cardiopulmonary bypass. The importance of cold perfusion of the ascending aorta has been shown in experiments 13 but has not been critically evaluated in this or other clinical trials. The appropriate period of observation after the cessation of cardiocirculatory function and before the declaration of death has not been established. We initially used a 3-minute period after loss of cardiac function. This time was based on a recommendation of 2 minutes in the critical care literature. 14 After the first donation, the ethics committee recommended a period of observation of 1.25 minutes to reduce the risk of injury from warm ischemia. This recommendation was based on the longest reported period before autoresuscitation of a child or adult, 60 seconds. The subsequent two donations were performed after an observation period of 1.25 minutes after the loss of cardiocirculatory function. The postoperative and immunosuppressive care followed our standard protocol for traditional donors. The absence of previous pediatric experience and the small number of patients reported on here precludes recommendations of the limit of warm ischemia time or unique care that could apply to pediatric heart donors who died from cardiocirculatory causes and the subsequent recipients. The first recipient required extracorporeal membrane oxygenation after transplantation, but this Predicted Probability of Survival (%) Year Figure 1. Predicted Probability of Survival of the First Recipient. The probability of survival was based on International Society for Heart and Lung Transplantation risk factors of the donor and recipient at the time of transplantation, assuming donation from a patient after brain death. This recipient was a 2-month-old boy who had congenital heart disease diagnosed at birth, weighed 4.1 kg, had a creatinine level of 1.5 mg per deciliter (133 mmol per liter), and was receiving extracorporeal membrane oxygenation and ventilator support. The donor was a 3-day-old boy weighing 2.8 kg. The upper and lower curves indicate the 95% confidence interval. requirement was not surprising, because the surgery was high risk: the patient was critically ill despite extracorporeal membrane oxygenation before transplantation, and the donor:recipient weight ratio was 0.7 (Fig. 1). This trial does not allow us to answer the question of how long warm ischemia can be tolerated and still permit recovery of heart function. The experience with these three high-risk patients supports the concept that the heart, like other solid organs, is capable of functioning adequately in a physiologically viable recipient after transplantation, despite cardiocirculatory death in the donor. Perhaps the previous ischemic injury in the donor, as evidenced by the increased troponin I level before donation, confers some ischemic preconditioning that makes recovery more likely. 15 Donors who died from cardiocirculatory causes offer an opportunity to reduce waiting time and waiting-list mortality among children whose survival depends on a heart transplant. This study was performed in the context of a large pediatric transplant program, yet most potential donors who underwent withdrawal from life support could not be considered, because there was no compatible local recipient. The majority of pediatric donor hearts are shared among transplan- n engl j med 359;7 august 14,
6 Brief Report tation regions. For pediatric heart donation and transplantation involving patients who die from cardiocirculatory causes to become a more frequent option for end-of-life care and to affect significantly the nationwide risk of dying while waiting, the concept of distant sharing of donated organs from these donors should be considered. Supported by a grant from the Department of Health and Human Services, Health Resources and Services Administration, and Division of Transplantation (R38OT ). Its contents are solely the responsibility of Denver Children s Hospital and do not necessarily represent the official views of the Health Resources and Services Administration. Additional institutional support was provided by the Division of Pediatric Cardiology, Denver Children s Hospital. No potential conflict of interest relevant to this article was reported. We thank Drs. Marianne Anderson, Francis Delmonico, John Fung, Dan Hall, and William Harmon for their criticisms, suggestions, and guidance. APPENDIX Members of the Denver Children s Hospital Pediatric Heart Transplant Team were as follows: M.M. Boucek, B. Pietra, S. Miyamoto, D. Campbell, M. Mitchell, C. Mashburn, D. Gilbert, A. Ballard, C. Connell, D. Ripe, B. Diamond, F. Legette, S. Anderson. References 1. Boucek MM, Aurora P, Edwards LB, et al. Registry of the International Society for Heart and Lung Transplantation: tenth official pediatric heart transplantation report J Heart Lung Transplant 2007;26: Bailey LL, Nehlsen-Cannarella SL, Doroshow RW, et al. Cardiac allotransplantation in newborns as therapy for hypoplastic left heart syndrome. N Engl J Med 1986;315: Taylor DO, Edwards LD, Boucek MM, et al. Registry of the International Society for Heart and Lung Transplantation: twenty-second official adult heart transplant report J Heart Lung Transplant 2005;24: Magee JC, Bucuvalas JC, Farmer DG, Harmon WE, Hulbert-Shearon TE, Mendeloff EN. Pediatric transplantation. Am J Transplant 2004;4:Suppl 9: Chrisant MR, Naftel DC, Drummond- Webb J, et al. Fate of infants with hypoplastic left heart syndrome listed for cardiac transplantation: a multicenter study. J Heart Lung Transplant 2005;24: Bernat JL, D Alessandro AM, Port FK, et al. Report of a national conference on donation after cardiac death. Am J Transplant 2006;6: Barnard CN. The operation a human cardiac transplant: an interim report of a successful operation performed at Groote Schuur Hospital, Cape Town. S Afr Med J 1967;41: Boucek MM, Kanakriyeh MS, Mathis CM, Trim RF III, Bailey LL. Cardiac transplantation in infancy: donors and recipients. J Pediatr 1990;116: Gundry SR, Fukushima N, Eke CC, Hill AC, Zuppan C, Bailey LL. Successful survival of primates receiving transplantation with dead, nonbeating donor hearts. J Thorac Cardiovasc Surg 1995;109: Feudtner C, Christakis DA, Zimmerman FJ, Muldoon JH, Neff JM, Koepsell TD. Characteristics of deaths occurring in children s hospitals: implications for supportive care services. Pediatrics 2002;109: Koogler T, Costarino AT Jr. The po- tential benefits of the pediatric nonheartbeating organ donor. Pediatrics 1998; 101: Ikle L, Hale K, Fashaw L, Boucek M, Rosenberg AA. Developmental outcome of patients with hypoplastic left heart syndrome treated with heart transplantation. J Pediatr 2003;142: Scheule AM, Beierlein W, Zurakowski D, et al. Emergency donor heart protection: application of the port access catheter technique using a pig heart transplantation model. Transplantation 2004;77: Recommendations for nonheartbeating organ donation: a position paper by the Ethics Committee, American College of Critical Care Medicine, Society of Critical Care Medicine. Crit Care Med 2001; 29: Murry CE, Jennings RB, Reimer KA. Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 1986;74: Copyright 2008 Massachusetts Medical Society. apply for jobs electronically at the nejm careercenter Physicians registered at the NEJM CareerCenter can apply for jobs electronically using their own cover letters and CVs. You can keep track of your job-application history with a personal account that is created when you register with the CareerCenter and apply for jobs seen online at our Web site. Visit for more information. 714 n engl j med 359;7 august 14, 2008
Pediatric Cardiac Transplantation Using DCD Donors. Canadian Critical Care Forum David N. Campbell, MD
 Pediatric Cardiac Transplantation Using DCD Donors Canadian Critical Care Forum David N. Campbell, MD No disclosures Disclosure Statement DCD: What is Old is New Again Early solid organ recoveries were
Pediatric Cardiac Transplantation Using DCD Donors Canadian Critical Care Forum David N. Campbell, MD No disclosures Disclosure Statement DCD: What is Old is New Again Early solid organ recoveries were
CARDIOVASCULAR SURGERY
 Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
DCD Heart Donation Understanding the Regulatory, Ethical and Clinical Issues. Valluvan Jeevanandam MD University of Chicago Medicine
 DCD Heart Donation Understanding the Regulatory, Ethical and Clinical Issues Valluvan Jeevanandam MD University of Chicago Medicine Disclosure Txn None MCS Scientific Advisor Thoratec/Abbott: Chairman
DCD Heart Donation Understanding the Regulatory, Ethical and Clinical Issues Valluvan Jeevanandam MD University of Chicago Medicine Disclosure Txn None MCS Scientific Advisor Thoratec/Abbott: Chairman
Policy Specific Section: May 16, 1984 April 9, 2014
 Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Survival after listing for cardiac transplantation in children
 Ž. Progress in Pediatric Cardiology 11 2000 99 105 Survival after listing for cardiac transplantation in children W. Robert Morrow a,, Elizabeth Frazier a, David C. Naftel b a Di ision of Pediatric Cardiology,
Ž. Progress in Pediatric Cardiology 11 2000 99 105 Survival after listing for cardiac transplantation in children W. Robert Morrow a,, Elizabeth Frazier a, David C. Naftel b a Di ision of Pediatric Cardiology,
Transplant in Pediatric Heart Failure
 Transplant in Pediatric Heart Failure Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart and Lung Transplantation
Transplant in Pediatric Heart Failure Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart and Lung Transplantation
Emergency surgery in acute coronary syndrome
 Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
Defining Death. Defining Death. Defining Death. Death at 50 & Organ Donation ORGAN TRANSPLANTATION. Dying (obvious) Death (not so obvious)
 Page 2 Page 4 Page 2 Page 4 Page 3 Page 5 Page 3 Page 5 Death at 50 & Organ Donation Dr. Mark Twite MA MB BChir FRCP Director of Congenital Cardiac Anesthesiology Associate Professor Department of Anesthesiology
Page 2 Page 4 Page 2 Page 4 Page 3 Page 5 Page 3 Page 5 Death at 50 & Organ Donation Dr. Mark Twite MA MB BChir FRCP Director of Congenital Cardiac Anesthesiology Associate Professor Department of Anesthesiology
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Outline. Congenital Heart Disease. Special Considerations for Special Populations: Congenital Heart Disease
 Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
I worldwide [ 11. The overall number of transplantations
 Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
Management of Cardiogenic Shock. Dr Stephen Pettit, Consultant Cardiologist
 Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Heart-lung transplantation: adult indications and outcomes
 Brief Report Heart-lung transplantation: adult indications and outcomes Yoshiya Toyoda, Yasuhiro Toyoda 2 Temple University, USA; 2 University of Pittsburgh, USA Correspondence to: Yoshiya Toyoda, MD,
Brief Report Heart-lung transplantation: adult indications and outcomes Yoshiya Toyoda, Yasuhiro Toyoda 2 Temple University, USA; 2 University of Pittsburgh, USA Correspondence to: Yoshiya Toyoda, MD,
DIAGNOSIS, MANAGEMENT AND OUTCOME OF HEART DISEASE IN SUDANESE PATIENTS
 434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
The Organ & Tissue Donation Process. Wendy Sherry, RN BScN Bernard Tremblay, RN MUHC Nurse Clinicians for Organ & Tissue Donation
 The Organ & Tissue Donation Process Wendy Sherry, RN BScN Bernard Tremblay, RN MUHC Nurse Clinicians for Organ & Tissue Donation Conflict of Interest I do not have an affiliation (financial or otherwise)
The Organ & Tissue Donation Process Wendy Sherry, RN BScN Bernard Tremblay, RN MUHC Nurse Clinicians for Organ & Tissue Donation Conflict of Interest I do not have an affiliation (financial or otherwise)
The Effect of Ventricular Assist Devices on Post-Transplant Mortality
 Journal of the American College of Cardiology Vol. 53, No. 3, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.070
Journal of the American College of Cardiology Vol. 53, No. 3, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.070
Heart Transplantation in Patients with Superior Vena Cava to Pulmonary Artery Anastomosis: A Single-Institution Experience
 Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
Curricular Components for Cardiology EPA
 Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
Curricular Components for Cardiology EPA 1. EPA Title 2. Description of the Activity Diagnosis and management of patients with acute congenital or acquired cardiac problems requiring intensive care. Upon
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, radiofrequency, anesthetic considerations for, 479 489 Acute aortic syndrome, thoracic endovascular repair of, 457 462 aortic
Index Note: Page numbers of article titles are in boldface type. A Ablation, radiofrequency, anesthetic considerations for, 479 489 Acute aortic syndrome, thoracic endovascular repair of, 457 462 aortic
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE
 SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients
 The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
Clinical Policy: Pediatric Heart Transplant
 Clinical Policy: Reference Number: CP.MP.138 Review Date: 01/19 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Clinical Policy: Reference Number: CP.MP.138 Review Date: 01/19 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Data Fact Sheet. Congestive Heart Failure in the United States: A New Epidemic
 National Heart, Lung, and Blood Institute Data Fact Sheet Congestive Heart Failure National Heart, Lung, and Blood Institute National Institutes of Health Data Fact Sheet Congestive Heart Failure in the
National Heart, Lung, and Blood Institute Data Fact Sheet Congestive Heart Failure National Heart, Lung, and Blood Institute National Institutes of Health Data Fact Sheet Congestive Heart Failure in the
Implantable Ventricular Assist Devices and Total Artificial Hearts. Policy Specific Section: June 13, 1997 March 29, 2013
 Medical Policy Implantable Ventricular Assist Devices and Total Artificial Hearts Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective
Medical Policy Implantable Ventricular Assist Devices and Total Artificial Hearts Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective
Debate in Management of native COA; Balloon Versus Surgery
 Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator
 Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Meyer, D; et al. The Future Direction of the Adult Heart Allocation System in the United States. Am J Transplant 2015; Jan 15(1):
 January Journal Watch 2015 Burhan Mohamedali, MD Rush University Chicago, Illinois, USA Burhan.mohamedali@gmail.com Rajeev Mohan, MD Scripps Clinic and Green Hospital La Jolla, California, USA Mohan.Rajeev@scrippshealth.org
January Journal Watch 2015 Burhan Mohamedali, MD Rush University Chicago, Illinois, USA Burhan.mohamedali@gmail.com Rajeev Mohan, MD Scripps Clinic and Green Hospital La Jolla, California, USA Mohan.Rajeev@scrippshealth.org
Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart. O Wenker, L Chaloupka, R Joswiak, D Thakar, C Wood, G Walsh
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
Donation after Circulatory Determination of Death: Ethical Tensions
 Donation after Circulatory Determination of Death: Ethical Tensions Robert D. Truog, MD Frances Glessner Lee Professor of Medical Ethics, Anaesthesia, & Pediatrics, Harvard Medical School Director, Center
Donation after Circulatory Determination of Death: Ethical Tensions Robert D. Truog, MD Frances Glessner Lee Professor of Medical Ethics, Anaesthesia, & Pediatrics, Harvard Medical School Director, Center
Heart transplantation is the gold standard treatment for
 Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Cardiogenic Shock. Carlos Cafri,, MD
 Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
Original Policy Date
 MP 7.03.07 Heart/Lung Transplant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 7.03.07 Heart/Lung Transplant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Covered Critical Illness Conditions Appendix
 Covered Critical Illness Conditions Appendix Effective Date: February 1, 2010 This Appendix contains definitions for those Conditions that are covered under the Manulife Financial Group Critical Illness
Covered Critical Illness Conditions Appendix Effective Date: February 1, 2010 This Appendix contains definitions for those Conditions that are covered under the Manulife Financial Group Critical Illness
AllinaHealthSystem 1
 : Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
: Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Candidates about. Lung Allocation Policy. for Transplant. Questions & A n s we r s TA L K I N G A B O U T T R A N S P L A N TAT I O N
 TA L K I N G A B O U T T R A N S P L A N TAT I O N Questions & A n s we r s for Transplant Candidates about Lung Allocation Policy U N I T E D N E T W O R K F O R O R G A N S H A R I N G What are the OPTN
TA L K I N G A B O U T T R A N S P L A N TAT I O N Questions & A n s we r s for Transplant Candidates about Lung Allocation Policy U N I T E D N E T W O R K F O R O R G A N S H A R I N G What are the OPTN
Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results
 Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
The Impact of Length of Post-Operative Ventilator Support on Outcome of the Arterial Switch Operation Report from a Single Institute
 Original Article Post-Operative Ventilator Support after Arterial Switch Operation Acta Cardiol Sin 2010;26:173 8 Cardiovascular Surgery The Impact of Length of Post-Operative Ventilator Support on Outcome
Original Article Post-Operative Ventilator Support after Arterial Switch Operation Acta Cardiol Sin 2010;26:173 8 Cardiovascular Surgery The Impact of Length of Post-Operative Ventilator Support on Outcome
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine
 Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
Living Donor Paired Exchange (LDPE)
 Living Donor Paired Exchange (LDPE) Why do we need Living Donation? 3,796 patients waiting for an organ transplant 2,679 (71%) waiting for a kidney transplant 249 people died while waiting for an organ
Living Donor Paired Exchange (LDPE) Why do we need Living Donation? 3,796 patients waiting for an organ transplant 2,679 (71%) waiting for a kidney transplant 249 people died while waiting for an organ
Detailed Order Request Checklists for Cardiology
 Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
The Gift of Life. Organ Donation and its Challenges Presented by Jessica Roth, RN, BSN, CPTC
 The Gift of Life Organ Donation and its Challenges Presented by Jessica Roth, RN, BSN, CPTC Nebraska Organ Recovery System (NORS) Federally designated as an organ procurement organization (OPO) Tasked
The Gift of Life Organ Donation and its Challenges Presented by Jessica Roth, RN, BSN, CPTC Nebraska Organ Recovery System (NORS) Federally designated as an organ procurement organization (OPO) Tasked
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Understanding the Pediatric Ventricular Assist Device
 Understanding the Pediatric Ventricular Assist Device W. James Parks, MSc., MD Pediatric Cardiologist Assistant Professor of Pediatrics and Radiology Children s Healthcare of Atlanta Sibley Heart Center
Understanding the Pediatric Ventricular Assist Device W. James Parks, MSc., MD Pediatric Cardiologist Assistant Professor of Pediatrics and Radiology Children s Healthcare of Atlanta Sibley Heart Center
Ischemic Ventricular Septal Rupture
 Ischemic Ventricular Septal Rupture Optimal Management Strategies Juan P. Umaña, M.D. Chief Medical Officer FCI Institute of Cardiology Disclosures Abbott Mitraclip Royalties Johnson & Johnson Proctor
Ischemic Ventricular Septal Rupture Optimal Management Strategies Juan P. Umaña, M.D. Chief Medical Officer FCI Institute of Cardiology Disclosures Abbott Mitraclip Royalties Johnson & Johnson Proctor
In newborns with a functional single ventricle and
 Pulmonary Vascular Resistance of Children Treated With Nitrogen During Early Infancy Ronald W. Day, MD, Alan J. Barton, MD, Theodore J. Pysher, MD, and Robert E. Shaddy, MD Division of Pediatric Cardiology,
Pulmonary Vascular Resistance of Children Treated With Nitrogen During Early Infancy Ronald W. Day, MD, Alan J. Barton, MD, Theodore J. Pysher, MD, and Robert E. Shaddy, MD Division of Pediatric Cardiology,
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Stabilization and Transportation guidelines for Neonates and infants with Heart disease:
 Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Left Ventricular Assist Devices (LVADs): Overview and Future Directions
 Left Ventricular Assist Devices (LVADs): Overview and Future Directions FATIMA KARAKI, M.D. PGY-3, DEPARTMENT OF MEDICINE WASHINGTON UNIVERSITY IN ST. LOUIS ST. LOUIS, MISSOURI, USA St. Louis, Missouri,
Left Ventricular Assist Devices (LVADs): Overview and Future Directions FATIMA KARAKI, M.D. PGY-3, DEPARTMENT OF MEDICINE WASHINGTON UNIVERSITY IN ST. LOUIS ST. LOUIS, MISSOURI, USA St. Louis, Missouri,
Section 6 Intra Aortic Balloon Pump
 Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to:
 The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
Clinical Policy: Heart-Lung Transplant Reference Number: CP.MP.132
 Clinical Policy: Reference Number: CP.MP.132 Effective Date: 01/18 Last Review Date: 05/18 Coding Implications Revision Log Description Heart-lung transplantation is treatment of choice for patients with
Clinical Policy: Reference Number: CP.MP.132 Effective Date: 01/18 Last Review Date: 05/18 Coding Implications Revision Log Description Heart-lung transplantation is treatment of choice for patients with
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
ECMO CPR. Ravi R. Thiagarajan MBBS, MPH. Cardiac Intensive Care Unit
 ECMO CPR Ravi R. Thiagarajan MBBS, MPH Staff Intensivist Cardiac Intensive Care Unit Children s Hospital Boston PCICS 2008, Miami, FL No disclosures Disclosures Outline Outcomes for Pediatric in-hospital
ECMO CPR Ravi R. Thiagarajan MBBS, MPH Staff Intensivist Cardiac Intensive Care Unit Children s Hospital Boston PCICS 2008, Miami, FL No disclosures Disclosures Outline Outcomes for Pediatric in-hospital
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Case Report. Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation.
 Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation Mustafa Gulgun and Michael Slack Associated Profesor Children National Medical
Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation Mustafa Gulgun and Michael Slack Associated Profesor Children National Medical
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
MODERATOR Felix Rapaport, other members of this
 The First Lung Transplant in Man (1963) and the First Heart Transplant in Man (1964) J.D. Hardy MODERATOR Felix Rapaport, other members of this distinguished panel, and members of the audience, I will
The First Lung Transplant in Man (1963) and the First Heart Transplant in Man (1964) J.D. Hardy MODERATOR Felix Rapaport, other members of this distinguished panel, and members of the audience, I will
IMPORTANT REMINDER DESCRIPTION
 Medical Policy Manual Transplant, Policy No. 02 Heart Transplant Next Review: March 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical Policies are developed to provide guidance
Medical Policy Manual Transplant, Policy No. 02 Heart Transplant Next Review: March 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical Policies are developed to provide guidance
ADVANCED CARDIOVASCULAR IMAGING. Medical Knowledge. Goals and Objectives PF EF MF LF Aspirational
 Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Complications of Acute Myocardial Infarction
 Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
PhD in Bioengineering and Medical-Surgical Sciences
 PhD in Bioengineering and Medical-Surgical Sciences Research Title: Influence of different perfusion and aortic clamping techniques in minimally invasive mitral valve surgery Funded by None Supervisor
PhD in Bioengineering and Medical-Surgical Sciences Research Title: Influence of different perfusion and aortic clamping techniques in minimally invasive mitral valve surgery Funded by None Supervisor
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
PCI in Patients with Transplant Coronary Artery Disease. Michael S. Lee, MD, FACC, FSCAI Assistant Professor UCLA School of Medicine
 PCI in Patients with Transplant Coronary Artery Disease Michael S. Lee, MD, FACC, FSCAI Assistant Professor UCLA School of Medicine Faculty Disclosure Honararia for Boston Scientific, BMS, Daiichi Sankyo,
PCI in Patients with Transplant Coronary Artery Disease Michael S. Lee, MD, FACC, FSCAI Assistant Professor UCLA School of Medicine Faculty Disclosure Honararia for Boston Scientific, BMS, Daiichi Sankyo,
Rhondalyn C. McLean. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume VII, A. Study Purpose and Rationale
 A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
Obstructed total anomalous pulmonary venous connection
 Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
Cardiac anaesthesia. Simon May
 Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Management of a Patient after the Bidirectional Glenn
 Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
SEX, BIRTH ORDER, AND MATERNAL AGE CHARACTERISTICS OF INFANTS WITH CONGENITAL HEART DEFECTS
 AMERICAN JOURNAL OF EPIDEMIOLOGY Copyright 1 by The Johns Hopkins University School of Hygiene and Public Health Vol., Xo. Printed in U.S.A. SEX, BIRTH ORDER, AND MATERNAL AGE CHARACTERISTICS OF INFANTS
AMERICAN JOURNAL OF EPIDEMIOLOGY Copyright 1 by The Johns Hopkins University School of Hygiene and Public Health Vol., Xo. Printed in U.S.A. SEX, BIRTH ORDER, AND MATERNAL AGE CHARACTERISTICS OF INFANTS
ECMO as a Bridge to Heart Transplant in the Era of LVAD s.
 Christian Bermudez MD. Associate Professor Director Thoracic Transplantation Division Cardiac Surgery Department of Surgery University of Pennsylvania ECMO as a Bridge to Heart Transplant in the Era of
Christian Bermudez MD. Associate Professor Director Thoracic Transplantation Division Cardiac Surgery Department of Surgery University of Pennsylvania ECMO as a Bridge to Heart Transplant in the Era of
Policy Specific Section: March 30, 2012 March 7, 2013
 Medical Policy Transcatheter Aortic Valve Replacement for Aortic Stenosis Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date:
Medical Policy Transcatheter Aortic Valve Replacement for Aortic Stenosis Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date:
Assessing Cardiac Anatomy With Digital Subtraction Angiography
 485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012
 Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
ADULT CONGENITAL HEART DISEASES NURSING CARE: PRESENT AND FUTURE CHALLENGES. Haitham Kanan, Clinical Instructor King Faisal specialist Hospital
 ADULT CONGENITAL HEART DISEASES NURSING CARE: PRESENT AND FUTURE CHALLENGES Haitham Kanan, Clinical Instructor King Faisal specialist Hospital Nursing Development and Saudization Objectives es At the
ADULT CONGENITAL HEART DISEASES NURSING CARE: PRESENT AND FUTURE CHALLENGES Haitham Kanan, Clinical Instructor King Faisal specialist Hospital Nursing Development and Saudization Objectives es At the
CONGENITAL HEART DISEASE (CHD)
 CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
Heart Transplant. Policy Number: Last Review: 8/2018 Origination: 8/2001 Next Review: 8/2019
 Heart Transplant Policy Number: 7.03.09 Last Review: 8/2018 Origination: 8/2001 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for a heart transplant
Heart Transplant Policy Number: 7.03.09 Last Review: 8/2018 Origination: 8/2001 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for a heart transplant
Classic options for treating hypoplastic left heart syndrome
 Birth Weight and Complexity Are Significant Factors for the Management of Hypoplastic Left Heart Syndrome John H. Artrip, MD, David N. Campbell, MD, D. Dunbar Ivy, MD, Melvin C. Almodovar, MD, Kak-Chen
Birth Weight and Complexity Are Significant Factors for the Management of Hypoplastic Left Heart Syndrome John H. Artrip, MD, David N. Campbell, MD, D. Dunbar Ivy, MD, Melvin C. Almodovar, MD, Kak-Chen
Coding Companion for Cardiology/Cardiothoracic/ Vascular Surgery. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Cardiology/Cardiothoracic/ Vascular Surgery A comprehensive illustrated guide to coding and reimbursement 2014 Contents Getting Started with Coding Companion...i Chest Wall...1 General
Coding Companion for Cardiology/Cardiothoracic/ Vascular Surgery A comprehensive illustrated guide to coding and reimbursement 2014 Contents Getting Started with Coding Companion...i Chest Wall...1 General
PIAF study: Placental insufficiency and aortic isthmus flow Jean-Claude Fouron, MD
 Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Accepted Manuscript. Will the fourth dimension guide us toward the perfect Norwood arch reconstruction? Minoo N. Kavarana, MD, FACS
 Accepted Manuscript Will the fourth dimension guide us toward the perfect Norwood arch reconstruction? Minoo N. Kavarana, MD, FACS PII: S0022-5223(19)30714-7 DOI: https://doi.org/10.1016/j.jtcvs.2019.03.040
Accepted Manuscript Will the fourth dimension guide us toward the perfect Norwood arch reconstruction? Minoo N. Kavarana, MD, FACS PII: S0022-5223(19)30714-7 DOI: https://doi.org/10.1016/j.jtcvs.2019.03.040
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
transplantations in the United States have more than doubled over the past 20 years (see line graph), the demand for organs continues to dwarf
 The NEW ENGLA ND JOURNAL of MEDICINE Perspective july 19, 2007 Robert Steinbrook, M.D. Although the numbers of organ donors and transplantations in the United States have more than doubled over the past
The NEW ENGLA ND JOURNAL of MEDICINE Perspective july 19, 2007 Robert Steinbrook, M.D. Although the numbers of organ donors and transplantations in the United States have more than doubled over the past
