Essence. Essential Service Standards for Equitable National Cardiovascular Care. Phase Two Measurement Indicators April 2015
|
|
|
- Howard Marshall
- 6 years ago
- Views:
Transcription
1 Essence Essential Service Standards for Equitable Cardiovascular Care for Aboriginal and Torres Strait Islander people Phase Two Measurement Indicators April 2015 Essence Measurement Indicators - Consultation Draft March
2 Essential Service Standards for Equitable Cardiovascular Care for Aboriginal and Torres Strait Islander people: Measurement Indicators SAHMRI 2015 Suggested citation: The ESSENCE Steering Committee, Essential Service Standards for Equitable Cardiovascular Care for Aboriginal and Torres Strait Islander people: Measurement Indicators. SAHMRI, Adelaide. Enquiries should be directed to: Wardliparingga Aboriginal Research Unit South Australian Health and Medical Research Institute PO Box ADELAIDE SA 5001 Ph E. 2
3 Acknowledgements We acknowledge the traditional owners of country throughout Australia, and their continuing connection to land, sea and community. We pay our respects to them and their cultures, and to elders both past and present. The have been developed with funding provided by the Federal Government Department of Health and the Centre of Research Excellence to Reduce Inequality in Heart Disease. Many individuals and organisations have freely given their time and expertise in the development of the. In particular, the Chairs would like to thank the ESSENCE II Steering Committee and other key experts who have given their time and advice. Members of the ESSENCE II Steering Committee: Professor Gary Jennings, Baker IDI Heart & Diabetes Institute (Chair) Professor Alex Brown, SAHMRI (Deputy-Chair) Dr Ngiare Brown, NACCHO Dr Ian Cameron, Rural Doctors Association of Australia Dr Rob Grenfell, expert - CVD Ms Kirrily Harrison, NIGATSIHID Dr Robert Herkes, ACSQHC Mr Kelvin Hill, Stroke Foundation Assoc. Professor Simon Koblar, expert - stroke Professor Richmond Jeremy, CSANZ Dr Tim Mathew, Kidney Health Australia Mr James McVeigh, expert - cardiovascular rehabilitation Mr Shane Mohor, AHCSA Dr Katie Panaretto expert - primary care Ms Jessica Stewart, NHPA Dr Philip Tideman, expert - CVD Professor Andrew Tonkin, expert - CVD Ms Vicki Wade, Heart Foundation Dr Mark Wenitong, expert - Aboriginal and Torres Strait Islander primary care, Apunipima ESSENCE Project Team Professor Alex Brown Ms Wendy Keech, SAHMRI Ms Katharine McBride, SAHMRI Mr Tony Lawson, Tony Lawson Consulting Ms Kathy Mott, SAHMRI
4 Acknowledgements Organisations which gave generously with their time include: Aboriginal Health Council of South Australia Aboriginal Health Council of Western Australia Aboriginal Medical Services Alliance Northern Territory Apunipima Health Council Australian Commission on Safety and Quality in Health Care Australian Bureau of Statistics Australian Institute of Health and Welfare Australian Stroke Clinical Registry Baker IDI Cardiac Society of Australia and New Zealand Central Australia Health Service Department for Health and Ageing, Government of South Australia Department of Health, Government of Western Australia Department of Health, Northern Territory Government Department of Health, Queensland Government Department of Health and Ageing, Australian Government Department of Health and Human Services, Victorian Government Department of Prime Minister and Cabinet, Australian Government Heart Foundation Improvement Foundation Kidney Health Australia Aboriginal Community Controlled Health Organisation Members of Aboriginal and Torres Strait Islander Health Standing Committee Members of Advisory Group on Aboriginal and Torres Strait Islander Health Information and Data Health Performance Authority New South Wales Ministry of Health Productivity Commission RHDAustralia Rural Doctors Association of Australia Stroke Foundation
5 contents Section 1 Setting the Scene: ESSENCE Measurement Indicators overview + framework Section 2 ESSENCE measurement indicators summary Section 3 ESSENCE Indicator + measurement specifications Appendix 1 ESSENCE Standards Appendix 2 Development of the ESSENCE Measurement Indicators References
6 SEction 1 Setting the Scene: Essence measurement indicators overview + framework The Essential Service Standards for Equitable Cardiovascular care for Aboriginal and Torres Strait Islander people (ESSENCE) Measurement Indicator project was established to guide the development and implementation of policies that serve to reduce the gap in life expectancy between Aboriginal and Torres Strait Islander peoples and other Australians. Cardiovascular diseases are the single largest cause of death for all Australians and remains the primary contributor to the life expectancy gap. Focussed, well informed investment in this area has potential to have far reaching benefit for all Aboriginal and Torres Strait Islander people across Australia. This project aims to develop a set of measurement indicators with which we can measure the performance of health care systems with respect to evidence based care for Aboriginal and Torres Strait Islander people at risk of or with cardiovascular disease. The indicators: are agreed on through consensus; demonstrate strong alignment with the ESSENCE Standards; measure the key standards that have the potential to drive significant improvement in the mortality and morbidity associated with cardiovascular disease in Aboriginal and Torres Strait Islander peoples; align with existing indicators that are already being collected across Australia where ever possible; extend beyond measurement to support improvements in health service delivery; and guide reform and planning. This document outlines the agreed set of. It covers both ESSENCE Measures and Cardiovascular Outcome Measures. A full implementation and data development plan is required as the next steps for implementation. 6
7 1.1 Why a focus on Cardiovascular Disease in Aboriginal and Torres Strait People? Evidence indicates that the gap in life expectancy could be reduced by 37 percent if Aboriginal and Torres Strait Islander people shared the same cardiovascular mortality profile as non-indigenous Australians.(1) A focused effort on reducing disparities in cardiovascular disease and care can have a significant impact on the future prosperity of Aboriginal and Torres Strait Islander people. Aboriginal and Torres Strait Islander people are 20 percent more likely to have cardiovascular disease, and have 1.5 times the age-standardised mortality rate compared to non-indigenous Australians.(1) The incidence and mortality pattern of cardiovascular disease experienced by Aboriginal and Torres Strait Islander people is characterised by early onset and significant differentials, most notably at young ages. Aboriginal and Torres Strait Islander people are more likely to have multiple risk factors than non-indigenous Australians, including smoking, physical inactivity, obesity, diabetes and high blood pressure.(2) Approaches to reduce the burden of cardiovascular disease on morbidity and mortality therefore need to be holistic and address risk and disease progression across the continuum. It is evident that systematic approaches to delivering care, systems of care, are needed. 7
8 1.2 The vision for ESSENCE The Essential Service Standards for Equitable Cardiovascular CarE for Aboriginal and Torres Strait Islander people (ESSENCE) project was established to develop a systematic, policy-targeted approach to addressing inequities in cardiovascular health care based on sound evidence and consensus. It was recognised that until we can move from social, policy and political intent to practical and resourced implementation of equitable care for all Australians, the gap between Australians as defined by culture, ethnicity, location and socioeconomic status may continue to widen The ESSSENCE Standards See Appendix 1 The ESSENCE Standards were developed in to articulate existing evidence and guidelines into a clear, coherent form that could be translated into practice. The ESSENCE Standards are essential standards that outline the minimum, acceptable level of care below which activity should not be permitted to fall.(3) They represent the best available evidence and expert consensus. The standards articulate what elements of care are necessary to reduce disparities in access and outcomes for critical cardiovascular conditions including coronary heart disease, stroke, chronic heart failure, rheumatic heart disease and hypertension. The ESSENCE Standards were developed by a national Steering Committee of experts in Aboriginal and Torres Strait Islander cardiovascular care, with funding from the Commonwealth Department of Health. Also at that time, momentum from the Close the Gap agenda, and support from the Indigenous Health Equality Council and the Cardiac Society of Australia and New Zealand helped drive the creation of the ESSENCE Standards. The ESSENCE Standards are aligned with 10 policy relevant targets: 1. Closing the life expectancy gap; 2. Reducing population levels of cardiovascular disease; 3. Improving health literacy in the population; 4. Monitoring the burden of cardiovascular disease in the community; 5. Improving access to care; 6. Enhancing access to time critical services; 7. Integration across the continuum of care; 8. Ensuring and improving the quality of cardiovascular disease care; 9. Reducing patient and family suffering; and 10. Monitoring the impact of cardiovascular disease health care reform over time. The ESSENCE Standards have been endorsed by the Heart Foundation and the Cardiac Society of Australia and New Zealand Implementing the ESSENCE Standards The development of the ESSENCE Standards was the first phase of a long-term strategy to improve cardiovascular disease outcomes for Aboriginal and Torres Strait Islander people. In 2014, the first stages of the ESSENCE implementation was funded by the Federal Department of Health. As part of a comprehensive approach, outlined below, two projects have been undertaken with this funding. The first of these projects, the development of, is a key foundation stone of eventual full implementation of the ESSENCE Standards. The Measurement Indicators were developed to establish a comprehensive set of measures to monitor key processes and outcomes for reducing disparities in cardiovascular health for Aboriginal and Torres Strait Islander people. The second project funded in 2014 was the development of a resource kit to inform evidence based commissioning of cardiovascular care in primary health. This project was timely given the commencement of Primary Health Networks in July 2015, introducing a new structure of primary health care delivery based on a model of commissioning. 8
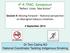
9 The next elements of implementing ESSENCE are: developing a primary care resource for service providers; reporting of the set across Australia; implementation of the ESSENCE Standards relevant to primary care into service commissioning, planning and service delivery practices; the establishment of clinical registries to monitor cardiovascular surgical interventions; the establishment of integrated regional service delivery networks across Australia; undertaking a gap analysis to consider required versus existing services; developing a master plan to drive all elements into coordinated practice with suitable mechanisms to evaluate and monitor. Diagram 1, on page 10, provides an overview of the evolution and future directions of ESSENCE. It is likely that other key features will emerge as valuable inclusions as we move along this journey of improving Aboriginal and Torres Strait Islander cardiovascular health. Additionally there will be a range of existing resources, processes, services, initiatives and strategies at local, regional, state and national levels that will be recognised and incorporated into this vision at it progresses the ESSENCE Standards within a national agenda Since 2007, there has been a national agenda focussed at closing the life expectancy gap for Aboriginal and Torres Strait Islander people. In 2009, discussions commenced with key cardiovascular stakeholders on the significant and devastating impact that cardiovascular disease has on the lives of Aboriginal and Torres Strait Islander people. In 2011, with the support of the Cardiac Society of Australia and New Zealand and the Federal Government, the ESSENCE vision was developed to target cardivascular disease. ESSENCE adopted a systematic, evidence-based, whole of life approach as an exemplar to closing the gap. In 2013, the Australian Health Ministers Advisory Council established the Better Cardiac Care for Aboriginal and Torres Strait Islander people agenda. This agenda was informed and shaped by the ESSENCE Standards, and members of the ESSENCE Steering Committee were strongly represented in these activities. The Better Cardiac Care for Aboriginal and Torres Strait Islander people agenda has developed agreed priority action areas and a set of measures to monitor action. In 2014, the Better Cardiac Care for Aboriginal and Torres Strait Islander people agenda was signed off by Australian Health Ministers Advisory Council and is now within the jurisdiction of State and Territory governments with data compilation occuring through the Australia Institute of Health and Welfare. The ESSENCE Standards,, and ESSENCE resource kit for Primary Health Networks are aligned with Better Cardiac Care for Aboriginal and Torres Strait Islander people and can be used to guide the implementation by each state and territory. The ESSENCE vision also aligns with other federally funded activities in the Aboriginal and Torres Strait Islander cardiovascular health space, including RHDAustralia and the Lighthouse project being undertaken by the Heart Foundation and Australian Healthcare and Hospitals Association. ESSENCE has been aligned to activities which are occuring nationally in a broader cardiovascular context. For example, the Measurement Indicator project has taken into consideration the work of many key groups including The Health Performance Authority, the Australian Commission for Safety and Quality in Healthcare, the Heart Foundation and Stroke Foundation. 9
10 DIAGRAM 1 Essential Service Standards for Equitable Cardiovascular Care for Aboriginal and Torres Strait Islander people (ESSENCE) - The Overview INPUTS ESSENCE I 2011/2012 ESSENCE II 2014/2015 The Vision for the Future Closing the Gap Cardiac Society of Aust. & NZ Support ESSENCE Standards Developed 2011/2012 Published 2014 Standards span prevention to tertiary care, and include systems of care. Current Project ESSENCE Measurement Indicators Implementation of ESSENCE Standards Performance Indicators set across Australia including measurement, synthesis and reporting The inclusion of the Primary Care ESSENCE Standards into service commissioning, planning and service delivery practices The establishment of clinical registries to monitor CHD and Stroke interventions Indigenous Health Equality Council Commonwealth Department of Health Funding Specific focus on Coronary Heart Disease, Stroke, Heart Failure, Rheumatic Heart Disease and Hypertension ESSENCE Resource Kit for Primary Health Networks The establishment of integrated Regional Service Delivery Networks across Australia A gap analysis of existing services against care as outlined in the ESSENCE Standards A development plan to drive all elements into coordinated practice with suitable mechanism to evaluate and monitor 10
11 1.3 The ESSENCE Measurement Indicator Framework Overview The ESSENCE Measurement Indicator framework is grounded on the continuum of care for Aboriginal and Torres Strait Islander people at risk of or with cardiovascular disease. This approach defines six domains of the ESSENCE indicators which measure the quality of care against the ESSENCE Standards and cardiovascular health outcomes. The specific conditions - coronary heart disease, stroke, chronic heart failure, rheumatic heart disease and hypertension - are spread across the domains as appropriate. The six domains of the are: Societal health Societal health recognises the geographical, social, economic and historical context that plays out in the cardiovascular wellbeing of Aboriginal and Torres Strait Islander people. It considers how these factors influence cardiovascular health in a contemporary context for individuals and affects the risk factors of cardiovascular disease. Impacting on societal health domain will support targets of: reducing population levels of cardiovascular disease improved access to care improved health literacy in the population Maintaining health and managing risk Maintaining health and managing risk is focused on the maintenance of wellbeing and assessment and managing cardiovascular risk and disease in a timely manner. Impacting the domain of maintaining health and managing risk will support targets of: improved access to care monitoring the burden of cardiovascular disease in the community Care of acute disease Care of acute disease is targeted at the access and delivery of time-critical, specialised acute care of cardiovascular disease, including heart attack and stroke. Impacting care of acute disease will support target of: enhanced access to time-critical services Ongoing care of disease Ongoing care of disease is the care of chronic cardiovascular disease in the community, and incorporates discharge following an acute event, ongoing management in primary care, and palliative and end of life care. Impacting the ongoing care of disease will support targets of: improved access to care reducing patient and family suffering Systems of care Systems of care is focused on the systems which should be in place to support the pathway of care across the continuum. These systems consider coordination, data collection and system monitoring. Impacting on the systems of care will support targets of: improved access to care integration across the continuum of care ensuring and improving the quality of cardiovascular care The cardiovascular outcome indicators focus on measuring the target of: monitoring the impact of cardiovascular health care reform over time. 11
12 Diagram 2 shows the domains and their link to the improving health cardiovascular outcomes. It also reflects the way the domains and their indicators are reflected along the continuum of care with the systems of care being all encompassing. The coloured dots highlight the link with each specific condition. In Diagram 3 all indicators are presented with their corresponding measures. There are 16 indicators that represent 33 measures and an additional 6 cardiovascular outcome indicators with 10 measures. Whilst the indicators are unapologetically specific to the continuum of care for cardiovascular disease, the framework recognises that cardiovascular care sits within a holistic approach to improving the physical, spiritual, cultural, emotion and social wellbeing of Aboriginal and Torres Strait Islander people. This framework directly reflects the way the ESSENCE Standards have been developed. The document is divided into 2 sections, in Section 1 the are presented in summary tables to facilitate easy access to all the indicators and measures. Each measure is explained by stage of measurement development and relevant health sector. If a measure has been identified in an existing indicator set, this indicator set has been listed. In Section 2 each indicator and measure is articulated in detail, with inclusion of the technical specifications. Appendix 2 explains the process used to identify and select indicators and measures that have now been included in this set. 12
13 DIAGRAM 2 ESSENCE Measurement Indicator Framework Societal Health Holistic Approach: Improvements of Aboriginal and Torres Strait Islander people s health must include attention to physical, spiritual, cultural, emotional and social wellbeing Systems of care Maintaining health and managing risk Cardiovascular Outcomes Ongoing care of disease Care of acute disease Societal Health 1. Socioeconomic determinants Maintaining health and managing risk 4. Smoking cessation 5. Risk Assessment Care of acute disease 8. Rapid assessment Ongoing care of disease 11. Discharge medications Systems of care 14. Integrated regional clinical network Cardiovascular Outcomes 1. CVD Mortality 2. Coronary Heart Disease 2. Comprehensive primary health care 3. Health behaviours 6. Risk Management 7. Secondary prevention & management of ARF/ RHD 9. Timely treatment 10. Specialised care 12. Coordination from hospital to community 13. Rehabilitation 15. RHD control Program 16. Surgical procedures registry 3. Chronic Heart Failure 4. Stroke 5. RHD 6. Hypertension Dot corresponds to condition covered in indicator: Coronary Heart Disease Chronic Heart Failure Stroke Acute Rheumatic Fever/Rheumatic Heart Disease Hypertension 13
14 DIAGRAM 3 Snapshot - ESSENCE Indicators and Measures assessing the quality of care against the ESSENCE Standards Societal Health 1. Socioeconomic determinants a. Household crowding b. Attainment of Year 12 education or equivalent c. Workforce participation 2. Comprehensive primary health care a. Aboriginal and Torres Strait Islander access to primary health care relative to need 3. Health behaviours a. Rate of current smokers b. Tobacco smoking during pregnancy c. People meeting guidelines for adequate intake of fruit and vegetables d. Adults meeting sufficient levels of physical activity Maintaining health and managing risk 4. Smoking cessation a. Smokers receiving nicotine replacement therapy 5. Risk assessment a. Absolute cardiovascular risk assessment for people aged 35 years and over b. MBS Health Assessment within the previous 12 months c. Number of people with relevant Medicare-listed diagnostic items claimed in the previous 12 months 6. Risk Management a. Hypertension: antihypertensive medications prescribed b. Documented evidence of primary care practitioner follow-up for people with elevated risk of cardiac disease 7. Secondary prevention & management of ARF/RHD a. People indicated for and who receive BPG secondary prophylaxis b. Priority 1 & 2 RHD cases receiving serial echocardiography Care of acute disease 8. Rapid assessment a. CHD: ECG performed and interpreted within 10 minutes of arrival for ACS b. Acute exacerbation of CHF: Receipt of echocardiography in the index admission c. Stroke: Brain imaging within 1 hour of presentation for thrombolysis eligible patients; and 3 hours for all other patients; of arrival to hospital 9. Timely treatment a. CHD: STEMI patients receiving fibrinolysis or PCI b. CHD: STEMI patients receiving fibrinolysis within 30 minutes of hospital arrival c. Stroke: Presentation and intravenous thrombolysis within 4.5 hours of symptom onset 10. Specialised care a. CHD & stroke: ACS and stroke patients admitted into a cardiac or stroke unit Ongoing care of disease 11. Discharge medications a. CHD, CHF, stroke & RHD: Patients prescribed appropriate, condition specific medications at discharge b. CHD, CHF, stroke & RHD: Patients prescribed medications remaining on them at least 12 months 12. Coordination from hospital to community a. CHD, stroke & RHD: Individualised care plan b. CHD, CHF & RHD: Review by a primary health care professional within 1 week of discharge 13. Rehabilitation a. Stroke: Rehabilitation therapy within 48 hours of initial assessment b. CHD, CHF & stroke: Patients referred to an appropriate rehabilitation or other secondary program c. CHD, CHF & stroke: Patients completing an appropriate rehabilitation or other secondary program Systems of care 14. Integrated regional clinical network a. Integrated regional clinical network scorecard 15. RHD control programme a. RHD control programme scorecard 16. Surgical procedures registry a. Services with a surgical procedures registry 14
15 DIAGRAM 4 Snapshot - Cardiovascular Outcome Indicators and Measures Cardiovascular Outcome Indicators 1. Cardiovascular Mortality a. Cardiovascular mortality rate 2. Coronary Heart Disease a. Coronary Heart Disease (I20-I25) hospitalisation rate b. 12 month mortality following hospitalisation for Acute Myocardial Infarction (I21) 3. Chronic Heart Failure a. Chronic Heart Failure (I50) hospitalisation rate 4. Stroke a. Stroke (I60-I69) hospitalisation rate b. 12 month mortality following hospitalisation for Stroke (I60-I69) 5. Rheumatic Heart Disease a. Acute Rheumatic Fever (I00-I02) incidence b. Acute Rheumatic Fever (I00-I02) recurrences c. Acute Rheumatic Fever (I00-I02) & Rheumatic Heart Disease (I05-I09) hospitalisation rate 6. Hypertension a. Hypertension (I10) prevalence 15
16 1.4 Data Considerations for the essence Measurement indicators Data limitations In undertaking the development of measurement indicators, a number of data limitations have been identified. Commentary is provided on some of these limitations. Indigenous identification Indigenous identification is a self-reported measure of cultural identity. Due to contextual issues in self-reporting personal information, Australia s history of racism and contemporary concerns by some staff to not offend patients and clients, it is widely observed that Indigenous status is inaccurately and inconsistently recorded. Routinely, the count of persons for whom Indigenous status is unknown is double the count of persons identifying themselves as Indigenous. Reasons for this inadequate recording can include where: the individual is concerned they may receive a poorer service if they identify the reason why the question has been asked is not clear the individual is not able to consider the question properly (eg they are unconscious or traumatised) at the point it is asked the healthcare worker concerned is uncertain how to ask the question and/or whether it should be asked of all service users regardless of their physical appearance indicating a likelihood that they may be of Indigenous descent. Under-identification of Indigenous status is a significant issue in developing effective responses to the high burden of disease. There are national efforts currently underway to improve the recording of Indigenous status. (4) Quality of care as defined by the client experience In recent years a series of initiatives have sought to create objective nationally applied criteria for measuring quality in healthcare as defined by the client. However, to date there is minimal data on quality of care as defined by Aboriginal and Torres Strait Islander clients, and initiatives that have included the views of Aboriginal and Torres Strait Islander people in their design have not been systematically applied and have not been at a national level. The ESSENCE Steering Committee recognises that the quality of care as defined by the client is a critical element in measuring performance of a system, and enables factors such as cultural safety to be measured. However, given the lack of data in this space and the difficulty of collecting such data, the ESSENCE Measurement Indicators do not incorporate such measures. Instead, the assess quality against the delivery of evidence-based care. Primary Care data availability In general, there is no systematic collection of data on the quality of care provided to Aboriginal and Torres Strait Islander clients by General Practitioners (GPs), and no national database providing such data from State run primary health care services. Data on quality in healthcare service delivery from Aboriginal Community Controlled Health Organisations is available and reported nationally. The ESSENCE Steering Committee acknowledges the quality of high standard of data collected through Aboriginal Community Controlled Health Organisations that should be applied across the primary care sector. 16
17 1.4.2 Current Status of the Measurement Indicators The indicators and measures differ in the stage of indicator and data development. Whilst some measures are already collected and reported on, others require both data and measure specification development. Measures are categorised into four stages of development: Measure currently collected as specified (Currently collected) Measure collected as specified, but not comprehensively collected across all relevant services across Australia. Further work remaining to ensure full coverage (Partially collected) Measure requires development, but there are existing data sources to inform measure (Requires development Data exists) Measure requires data collection development and new data collection (Requires development No data exists) Overview of stage of data development of measures 42 measures in total ESSENCE Measures Cardiovascular Outcome Measures Currently collected as specified Partially collected Requires development - data exists Requires development - no data exists Total Total The development of the ESSENCE Measurement Indicator specifically targeted inclusion of measures that are recognised in existing indicator sets and/or collected in existing data sets. Existing indicator sets which have been considered and aligned are: Overcoming Indigenous Disadvantage; Aboriginal and Torres Strait Islander Health Performance Framework; Indigenous Reform Agreement; nkpi - Indigenous primary health care key performance indicators Better Cardiac Care for Aboriginal and Torres Strait Islander people 2014; RHDAustralia Acute Rheumatic Fever/Rheumatic Heart Disease key performance indicators; Australian Commission on Safety and Quality in Health Care Acute Coronary Syndrome and Stroke Clinical Care Standards; and the Australian Council on Healthcare Standards Indicator and Data Development Plans When considering the next steps it will be important to develop indicator and data development plans. This would specifically consider the following: Measures that are currently collected could be incorporated into a short term implementation plan, focussed on information collation and reporting. Measures that are partially collected may need concerted advocacy with other key stakeholders to expand their remit to ensure they are integrated into current practice across the whole country to provide an accurate and representative picture of current practice. Measures that require development - existing data will fall into a medium term development plan. Some of these represent indicator priorities already established with other projects. Collective voices will be needed to drive implementation of the indicators to enable reporting from existing data sets. Measures that require development - no data will fall into a long term, aspirational development plan. Implementation of these will require significant resource investment as well as strong political will at a range of levels. A sophisticated data development plan, underpinned by evidence, community need and expert opinion, will be an important tool to advocate for improved reporting capability in this sphere. 17
18 SEction 2 ESSence measurement indicators summary Headline Measures Ten headline measures have been identified from the range of 43 measures. These measures have been selected based their potential impact to guide and measure sigificant improvements in cardiovascular outcomes for Aboriginal and Torres Strait Islander people. Eight measures assess quality of care against the ESSENCE Standards, and two measures are Cardiovascular Outcome measures. # Measure Stage of data development Cardiovascular Outcome Indicators 1a Cardiovascular mortality rate Currently collected 2b 12 month mortality following hospitalisation for AMI (I21) Requires development data exists Quality of care Indicators 2a Aboriginal and Torres Strait Islander access to primary health care relative to need Requires development, data exists 3a Rate of current smokers Currently collected 5a Absolute cardiovascular risk assessment for people aged 35 years and over Requires development, no data exists 9a CHD: STEMI Patients receiving fibrinolysis or PCI Requires development, no data exists 9c Stroke: Presentation and intravenous thrombolysis within 4.5 hours of symptom onset 11a 13c CHD, CHF & stroke: patients discharged with appropriate, condition specific medications CHD, CHF & stroke: Patients completing an appropriate, condition-specific rehabilitation or other secondary prevention program Partially collected through clinical audit Partially collected through clinical audit and registry Requires development, no data exists 14a Integrated regional clinical network Requires development, no data exists 18
19 The outline a total 22 indicators covering 43 measures. This number is in recognition that this is a comprehensive set of indicators covering the continuum of cardiovascular risk and disease. These span over the six domains. Measures highlighted in orange are headline measures. Societal health indicators Measure Indicator 1: Socioeconomic determinants 1a. Household crowding 1b. Attainment of Year 12 education or equivalent 1c. Workforce participation i. Employment to population ratio ii. Unemployment rate iii. Labour force participation rate Indicator 2: Comprehensive Primary Health Care 2a. Aboriginal and Torres Strait Islander access to primary health care relative to need Indicator 3: Health Behaviours 3a. Rate of current smokers Relevant ESSENCE Standard I.1.1: Socioeconomic determinants I.1.1: Socioeconomic determinants I.1.1: Socioeconomic determinants I.1.2: Comprehensive primary health care I.1.1: Socioeconomic determinants Existing indicator set OID, HPF HPF, NIRA, OID HPF, NIRA, OID HPF, AIHW HPF Stage of data development Currently collected Currently collected Currently collected Requires development - data exists Currently collected Reporting level Jurisdiction Jurisdiction Jurisdiction * Regional Jurisdiction * Service * Regional Jurisdiction 3b. Tobacco smoking during pregnancy 3c. People meeting guidelines for adequate intake of fruit and vegetables I.1.1: Socioeconomic determinants I.2.1: Socioeconomic determinants HPF, NIRA, OID HPF, NIRA, OID Currently collected Currently collected * Service Regional Jurisdiction * Regional Jurisdiction 3d. Adults meeting sufficient levels of physical activity I.1.1: Socioeconomic determinants HPF Currently collected * Regional Jurisdiction Key: OID - Overcoming indigenous Disadvantage, HPF Aboriginal and Torres Strait Islander Health Performance Framework,, NIRA Indigenous Reform Agreement, AIHW - Australian Institute of Health and Welfare * It is recommended that there be reporting at this level. However, this measure is not currently reported at this level. See ESSENCE Standards for details of standards 19
20 Maintaining health and managing risk indicators Measure Indicator 4: Smoking cessation 4a. Smokers receiving nicotine replacement therapy Indicator 5: Risk assessment 5a. Absolute cardiovascular risk assessment for people aged 35 years and over 5b. MBS Health Assessment within the previous 12 months 5c. People with relevant Medicare-listed diagnostic items claimed in the previous 12 months Indicator 6: Risk management 6a. Hypertension: Antihypertensive medications prescribed 6b. Documented evidence of primary care practitioner follow-up for people with elevated risk of cardiac disease Relevant ESSENCE Standard I.2.3: Supporting smoking cessation I.2.1: Identifying and managing risk I.2.1: Identifying and managing risk VI.1.3: Early identification of hypertension I.2.1: Identifying and managing risk I.2.2: Managing risk VI.2: Medication - I.2.1: Identifying and managing risk I.2.2: Managing risk 1.2.3: Supporting smoking cessation 1.2.4: Access to essential medicines Indicator 7: Secondary prevention and management of ARF and RHD 7a. People indicated for and who receive BPG secondary prophylaxis 7b. Priority 1 and 2 RHD cases receiving serial echocardiography V.3.1: Long acting penicillin V.3.2: Echocardiography - Existing indicator set Proposed nkpis HPF, BCC BCC BCC RHDA KPIs RHDA KPIs Stage of data development Requires development - no data exists Requires development no data exists Currently collected Requires development data exists Requires development no data exists Requires development no data exists Partially collected selected jurisdictions Partially collected selected jurisdictions Reporting level Service Regional Jurisdiction Service Regional * Service * Regional Jurisdiction Service Regional Service Regional Service Regional Jurisdiction * Regional Key: HPF Aboriginal and Torres Strait Islander Health Performance Framework, NIRA Indigenous Reform Agreement, nkpis Key Performance Indicators, BCC Better Cardiac Care for Aboriginal and Torres Strait Islander people, RHDA KPIs Rheumatic Heart Disease Australia ARF/RHD Key Performance Indicators * It is recommended that there be reporting at this level. However, this measure is not currently reported at this level. See ESSENCE Standards for details of standards 20
21 Care of acute disease indicators Measure Indicator 8: Rapid assessment 8a. CHD: ECG performed and interpreted within 10 minutes of arrival for ACS 8b. Acute exacerbation of CHF: Receipt of echocardiography in the index admission 8c. Stroke: Brain scan within: i. 1 hour of presentation for thrombolysis eligible patients ii. 3 hours for all other patients Indicator 9: Timely treatment Relevant ESSENCE Standard I I.3.1: Medical transport for streamlined access to the appropriate level of care I.6.1: Transport and referral protocol development II.2.1: Access to care II.2.2: Early ECG I.3.1: Medical transport for streamlined access to the appropriate level of care I.6.1: Transport and referral protocol development III.2.1: Establishment of cause I.3.1: Medical transport for streamlined access to the appropriate level of care I.6.1: Transport and referral protocol development IV.1.1: Access to care IV.1.2: Rapid assessment and risk stratification IV.1.3: Brain imaging Existing indicator set Stage of data development Requires development no data exists Requires development no data exists Partially collected clinical audit Reporting level Service Regional Service Regional Service Regional 9a. CHD: STEMI Patients receiving fibrinolysis or PCI II.2.4: Reperfusion therapy for STEMI ACSQHC ACS CCS Requires development data exists Service Regional 9b. CHD: STEMI patients receiving fibrinolysis within 30 minutes of hospital arrival 9c. Stroke: Presentation and intravenous thrombolysis within 4.5 hours of symptom onset Indicator 10: Specialised care 10a. CHD & Stroke: ACS and stroke patients admitted into a cardiac or stroke unit i. Cardiac unit ii. Stroke unit II.2.4: Reperfusion therapy for STEMI IV.1.5: Access to thrombolysis II.2.8: Cardiac units IV.1.4: Stroke units ACSQHC ACS CCS ACSQHC Stroke CCS ACSQHC Stroke CCS Requires development data exists Partially collected clinical audit Partially collected registry Service Regional Service * Regional * Service * Regional Key: ACSQHC ACS CCS Australian Commission on Safety and Quality in Health Care Acute Coronary Syndrome Clinical Care Standards, ACHS Australian Council on Healthcare Standards, ACSQHC Stroke CCS - Australian Commission on Safety and Quality in Health Care Stroke Clinical Care Standards * It is recommended that there be reporting at this level. However, this measure is not currently reported at this level. See ESSENCE Standards for details of standards 21
22 Ongoing care of disease indicators Measure Relevant ESSENCE Standard Indicator 11: Discharge medications 11a. CHD, CHF, Stroke: Patients discharged with appropriate, condition-specific medications I.2.4: Access to essential i. CHD: aspirin or other antiplatelet agent, medicines a statin, an ACE inhibitor or angiotensin I.3.2: Ongoing support receptor blocker, and a beta-blocker, as post-discharge appropriate I.4.1: Patient education ii. CHF: Patients prescribed ACEI or A2RA II.2.10: Adjuvant medical and beta blocker therapy iii. Haemorrhagic stroke: antihypertensive III.2.2: Adjuvant medical medication therapy iv. Ischaemic stroke: statin therapy, IV.2.1: Adjuvant medical antihypertensive and antithrombotic therapy medication 11b. CHD, CHF & Stroke: Patients prescribed medications remaining on them at 12 months i. CHD: aspirin or other antiplatelet agent, a statin, an ACE inhibitor or angiotensin receptor blocker, and a beta-blocker, as appropriate ii. CHF: Patients prescribed ACEI or A2RA and beta blocker iii. Haemorrhagic stroke: antihypertensive medication iv. Ischaemic stroke: statin therapy, antihypertensive and antithrombotic medication Indicator 12: Coordination from hospital to community 12a. CHD, Stroke & RHD: Individualised care plan i. Care plan for ACS ii. Care plan for Stroke iii. Care plan for RHD 12b. CHD, CHF & RHD: Review by a primary health care professional within 1 week of discharge Indicator 13: Rehabilitation 13a. Stroke: Rehabilitation therapy within 48 hours of initial assessment 13b. CHD, CHF & Stroke: Patients referred to an appropriate condition-specific rehabilitation or other secondary prevention program i. ACS patients ii. CHF patients iii. Stroke patients 13c. CHD, CHF & Stroke: Patients completing an appropriate condition-specific rehabilitation or other secondary prevention program i. ACS patients ii. CHF patients iii. Stroke patients I.2.4: Access to essential medicines I.3.2: Ongoing support post-discharge I.4.1: Patient education II.2.10: Adjuvant medical therapy III.2.2: Adjuvant medical therapy IV.2.1: Adjuvant medical therapy I.3.2: Ongoing support post-discharge I.3.2: Ongoing support post-discharge I.3.3: Clinical communication and handover I.4.1: Patient education IV.2.2: Inpatient stroke rehabilitation I.4.1: Patient education I.4.3: Community rehabilitation I.4.4: Lifestyle modification III.3.2: Cardiac rehabilitation I.4.1: Patient education I.4.3: Community rehabilitation I.4.4: Lifestyle modification III.3.2: Cardiac rehabilitation Existing indicator set BCC; ACSQHC Stroke CCS - ACSQHC ACS CCS; ACSQHC Stroke CCS BCC ACSQHC ACS CCS; ACHS; ACSQHC Stroke CCS Stage of data development Partially collected clinical audit and registry Requires development no data exists Requires development no data exists Requires development no data exists Partially collected clinical audit Partially collected - clinical audit Requires development no data exists Reporting level * Service Service Service Regional Regional Service Regional * Service * Regional Service Regional Key: BCC Better Cardiac Care for Aboriginal and Torres Strait Islander people, ACHS Australian Council on Healthcare Standards, ACSQHC Stroke CCS - Australian Commission on Safety and Quality in Health Care Stroke Clinical Care Standards, ACSQHC ACS CCS Australian Commission on Safety and Quality in Health Care Acute Coronary Syndrome Clinical Care Standards, * It is recommended that there be reporting at this level. However, this measure is not currently reported at this level. See ESSENCE Standards for details of standards 22
23 Systems of care indicators Measure Indicator 14: Integrated regional clinical network 14a. Integrated regional clinical network scorecard Indicator 15: RHD control programme 15a. RHD control programme scorecard Indicator 16: Surgical procedures registry 16a. Services with a surgical procedures registry Key: See ESSENCE Standards for details of standards Relevant ESSENCE Standard I.6.4: Standard service elements - V.4.1: RHD control programme - I.6.5: Data monitoring and performance of outcomes - Existing indicator set Stage of development Requires development no data exists Requires development no data exists Requires development no data exists Reporting level Regional Jurisdiction Jurisdiction Jurisdiction 23
24 Cardiovascular Outcome Indicators Measure Relevant ESSENCE Standard Cardiovascular Outcome Indicator 1: Cardiovascular mortality Existing indicator set Stage of development Reporting level 1a. Cardiovascular mortality rate i. All cardiovascular (I00-I99) ii. CHD (I20-I25) iii. CHF (I50) iv. Stroke (I60-I69) v. ARF (I00-I02) & RHD (I05-I09) All ESSENCE Standards HPF, NIRA, OID Currently collected Jurisdiction Cardiovascular Outcome Indicator 2: Coronary Heart Disease 2a. CHD (I20-I25) hospitalisation rate 2b. 12 month mortality following hospitalisation for AMI (I21) All overarching CVD standards (I) All standards for CHD (II) All overarching CVD standards (I) All standards for CHD (II) Cardiovascular Outcome Indicator 3: Chronic Heart Failure 3a. CHF (I50) hospitalisation rate Cardiovascular Outcome Indicator 4: Stroke 4a. Stroke (I60-I69) hospitalisation rate 4b. 12 month mortality following hospitalisation for Stroke (I60-I69) All overarching CVD standards (I) All standards for CHF (III) All overarching CVD standards (I) All standards for stroke (IV) All overarching CVD standards (I) All standards for stroke (IV) Cardiovascular Outcome Indicator 5: Rheumatic Heart Disease 5a. ARF (I00-I02) incidence 5b. ARF (I00-I02) recurrences All overarching CVD standards (I) All standards for RHD (V) All overarching CVD standards (I) All standards for RHD (V) HPF BCC HPF HPF - RDHA KPIs, HPF RDHA KPIs, HPF Currently collected Requires development data exists Currently collected Currently collected Requires development no data exists Partially collected - registry Partially collected - registry * Regional Jurisdiction Regional Jurisdiction Jurisdiction * Regional Jurisdiction Jurisdiction Jurisdiction Jurisdiction 5c. ARF (I00-I02) & RHD (I05-I09) hospitalisation rate i. ARF (I00-I02) ii. RHD (I05-I09) All overarching CVD standards (I) All standards for RHD (V) HPF Currently collected * Regional Jurisdiction Cardiovascular Outcome Indicator 6: Hypertension 6a. Proportion of population with selfreported/measured hypertension (I10) All overarching CVD standards (I) All standards for hypertension (VI) HPF Currently collected * Regional Jurisdiction Key: HPF Aboriginal and Torres Strait Islander Health Performance Framework, NIRA Indigenous Reform Agreement, BCC Better Cardiac Care for Aboriginal and Torres Strait Islander people, RHDA KPIs Rheumatic Heart Disease Australia ARF/RHD Key Performance Indicators * It is recommended that there be reporting at this level. However, this measure is not currently reported at this level. See ESSENCE Standards for details of standards 24
25 SEction 3 indicator and measure specifications 25
26 Indicator 1: Socioeconomic determinants Rationale: The relationship between the socioeconomic status of an individual and their health and wellbeing is well established. Relevant ESSENCE Standards: I.1.1 Primordial prevention - Socioeconomic determinants All Aboriginal and Torres Strait Islander Australians should have improved access to all necessary healthful social and environmental resources in their day to day lives, including enhanced access to education, improved living and working conditions, and safe environments. People should be able to live in an environment that encourages and supports healthy lifestyle choices. Measures: The indicator for socio-economic determinants has 3 measures which are currently collected across a range of agencies and reporting structures. The specific measures are: a) Household crowding b) Attainment of Year 12 education or equivalent c) Workforce participation 26
27 Indicator 1: Socioeconomic determinants Measure 1a: Description: ESSENCE Standard: Stage of development: Existing indicator set: Reporting level: Sector: Computation: Numerator: Denominator: Disaggregation: Data Source: Household crowding Proportion of people, of all ages, who live in overcrowded houses I.1.1: Socioeconomic determinants Measure currently collected as specified Overcoming Indigenous Disadvantage, Aboriginal and Torres Strait Islander Health Performance Framework Jurisdictional Across government 100 x (Numerator Denominator) Number of people who live in overcrowded housing Total population who reside in private dwellings, and State/Territory, by remoteness area and Indigenous status Numerator: Australian Bureau of Statistics Australian Aboriginal and Torres Strait Islander Health Survey, NATSIHS component; Australian Bureau of Statistics Aboriginal and Torres Strait Islander Social Survey; Australian Bureau of Statistics Australian Health Survey, NHS component; Australian Bureau of Statistics Census of Population and Housing Denominator: Australian Bureau of Statistics Australian Aboriginal and Torres Strait Islander Health Survey, NATSIHS component; Australian Bureau of Statistics Aboriginal and Torres Strait Islander Social Survey; Australian Bureau of Statistics Australian Health Survey, NHS component; Australian Bureau of Statistics Census of Population and Housing Note: Overcrowding is defined according to the Australian modification of the Canadian Occupancy Standard as the indicator of housing utilisation (and therefore overcrowding). For more information on this measure as specified in the Overcoming Indigenous Disadvantage reports, refer to the 2014 Report. (5) For more information on the Australian modification of the Canadian Occupancy Standard, refer to the Overcoming Indigenous Disadvantage Report 2014 (Box ).(5) 27
28 Indicator 1: Socioeconomic determinants Measure 1b: Description: ESSENCE Standard: Stage of development: Existing indicator set: Reporting level: Sector: Computation: Numerator: Denominator: Disaggregation: Data Source: Attainment of Year 12 education or equivalent Proportion of the year old population having attained at least a Year 12 or equivalent or Australian Qualifications Framework Certificate level II or above I.1.1: Socioeconomic determinants Measure currently collected as specified Aboriginal and Torres Strait Islander Health Performance Framework, Indigenous Reform Agreement, Overcoming Indigenous Disadvantage Jurisdictional Across government 100 x (Numerator Denominator) People aged years who have completed Year 12 or equivalent or whose level of highest non-school qualification is at Australian Qualifications Framework Certificate level II or above. Total population of people aged years, and state/territory by remoteness area by Indigenous status and sex [Refer to notes] Remoteness area by Indigenous status and sex [Refer to notes] Numerator: Australian Bureau of Statistics Australian Aboriginal and Torres Strait Islander Health Survey, Core component; Australian Bureau of Statistics Aboriginal and Torres Strait Islander Social Survey; Australian Bureau of Statistics Australian Health Survey, NHS component; Australian Bureau of Stastics Census of Population and Housing Denominator: Australian Bureau of Statistics Australian Aboriginal and Torres Strait Islander Health Survey, Core component; Australian Bureau of Statistics Aboriginal and Torres Strait Islander Social Survey; Australian Bureau of Statistics Australian Health Survey, NHS component; Australian Bureau of Stastics Census of Population and Housing Note: The ESSENCE Steering Committee recommends that this measure be disaggregated by sex. For more information on this measure as specified in the Aboriginal and Torres Strait Islander Health Performance Framework, refer to health.gov.au/indigenous-hpf For measure specifications as outlined in the Indigenous Reform Agreement, refer to meteor.aihw.gov.au 28
Better Cardiac Care measures. for Aboriginal and Torres Strait Islander people
 Better Cardiac Care measures for Aboriginal and Torres Strait Islander people Better Cardiac Care measures for Aboriginal and Torres Strait Islander people First national report 215 Australian Institute
Better Cardiac Care measures for Aboriginal and Torres Strait Islander people Better Cardiac Care measures for Aboriginal and Torres Strait Islander people First national report 215 Australian Institute
South Australian Aboriginal Cardiovascular Health Profile
 South Australian Cardiovascular Health Profile for the South Australian Heart and Stroke Plan 2017-2021 June 2016 This document was developed as part of the development of the South Australian Heart and
South Australian Cardiovascular Health Profile for the South Australian Heart and Stroke Plan 2017-2021 June 2016 This document was developed as part of the development of the South Australian Heart and
High Level Across Sector Support to Implement the Three Plans South Australian Aboriginal Chronic Disease Consortium Goal Vision
 Now I live my life like there s no tomorrow. I live for my children and I live for my family. It has been twenty years since my diagnosis with testicular cancer. I can truly say that I won the race and
Now I live my life like there s no tomorrow. I live for my children and I live for my family. It has been twenty years since my diagnosis with testicular cancer. I can truly say that I won the race and
April 2019 NATIONAL POLICY PLATFORM
 April 2019 NATIONAL POLICY PLATFORM There are crisis services available 24/7 if you or someone you know is in distress Lifeline: 13 11 14 www.lifeline.org.au people took their own lives in 2017 1 Over
April 2019 NATIONAL POLICY PLATFORM There are crisis services available 24/7 if you or someone you know is in distress Lifeline: 13 11 14 www.lifeline.org.au people took their own lives in 2017 1 Over
Essential Service Standards for Equitable National Cardiovascular Care for
 Heart, Lung and Circulation (2015) 24, 126 141 1443-9506/04/$36.00 http://dx.doi.org/10.1016/j.hlc.2014.09.021 ORIGINAL ARTICLE Essential Service s for Equitable National Cardiovascular Care for Aboriginal
Heart, Lung and Circulation (2015) 24, 126 141 1443-9506/04/$36.00 http://dx.doi.org/10.1016/j.hlc.2014.09.021 ORIGINAL ARTICLE Essential Service s for Equitable National Cardiovascular Care for Aboriginal
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Gippsland When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Gippsland When submitting this Activity Work Plan 2016-2018 to the Department
BRIDGING THE GAP. Know your population How bad is it? Is it changing? Why the difference? The continuum of care
 Aboriginal & Torres Strait Islander diabetes and coronary heart disease BRIDGING THE GAP Graeme Maguire Cairns Base Hospital James Cook University Deaths per 1 population 1 1 8 6 4 8 6 4 1977 1981 Ischaemic
Aboriginal & Torres Strait Islander diabetes and coronary heart disease BRIDGING THE GAP Graeme Maguire Cairns Base Hospital James Cook University Deaths per 1 population 1 1 8 6 4 8 6 4 1977 1981 Ischaemic
The first step to Getting Australia s Health on Track
 2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
3. Queensland Closing the Health Gap Accountability Framework. COAG national targets and indicators
 3. Queensland Closing the Health Gap Accountability Framework The accountability framework articulated in this section is designed to measure progress against the health targets and indicators included
3. Queensland Closing the Health Gap Accountability Framework The accountability framework articulated in this section is designed to measure progress against the health targets and indicators included
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Better Cardiac Care measures
 This is the second national report on the 21 Better Cardiac Care measures for Aboriginal and Torres Strait Islander people, with updated data available to report on 11 measures. For some of the measures,
This is the second national report on the 21 Better Cardiac Care measures for Aboriginal and Torres Strait Islander people, with updated data available to report on 11 measures. For some of the measures,
Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health
 Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health Pat Field National Director, Rural Remote and Indigenous Programs, Heart Foundation of Australia 5th National
Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health Pat Field National Director, Rural Remote and Indigenous Programs, Heart Foundation of Australia 5th National
HEART DISEASE. Six actions the next Australian Government must take to tackle our biggest killer: National Heart Foundation of Australia 2016
 Six actions the next Australian Government must take to tackle our biggest killer: HEART DISEASE National Heart Foundation of Australia 2016 NATIONAL HEART FOUNDATION OF AUSTRALIA 1 Contents The challenge
Six actions the next Australian Government must take to tackle our biggest killer: HEART DISEASE National Heart Foundation of Australia 2016 NATIONAL HEART FOUNDATION OF AUSTRALIA 1 Contents The challenge
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Aiming for Excellence in Stroke Care
 Training Centre in Sub-acute Care (TRACS WA) Aiming for Excellence in Stroke Care A tool for quality improvement in stroke care Developed by TRAining Centre in Subacute Care (TRACS WA) February 2016 For
Training Centre in Sub-acute Care (TRACS WA) Aiming for Excellence in Stroke Care A tool for quality improvement in stroke care Developed by TRAining Centre in Subacute Care (TRACS WA) February 2016 For
Submission to the Commonwealth Government on the New National Women s Health Policy
 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Authorised and written by: Patty Kinnersly, CEO, Women s Health Grampians Contact person for this submission:
Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Authorised and written by: Patty Kinnersly, CEO, Women s Health Grampians Contact person for this submission:
Policy Statement Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians
 Policy Statement 2.3.5 Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians Position Summary Research must be funded to better understand the dental needs and issues
Policy Statement 2.3.5 Delivery of Oral Health: Special groups: Aboriginal and Torres Strait Islander Australians Position Summary Research must be funded to better understand the dental needs and issues
Updated Activity Work Plan : Drug and Alcohol Treatment
 Web Version HPRM DOC/17/1043 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic
Web Version HPRM DOC/17/1043 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment This Drug and Alcohol Treatment Activity Work Plan template has the following parts: 1. The updated strategic
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 South Eastern Melbourne PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 South Eastern Melbourne PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Murray PHN When submitting this Activity Work Plan 2016-2018 to the Department
The National Framework for Gynaecological Cancer Control
 The National Framework for Gynaecological Cancer Control CNSA Annual Congress 13 May 2016 Jennifer Chynoweth General Manager, Cancer Care Cancer Australia Current and emerging issues in gynaecological
The National Framework for Gynaecological Cancer Control CNSA Annual Congress 13 May 2016 Jennifer Chynoweth General Manager, Cancer Care Cancer Australia Current and emerging issues in gynaecological
Consumer Participation Strategy
 Consumer Participation Strategy Plan Implementation Period 2011-2013 Date: 24 December 2010 Developed by: NEMICS Directorate in consultation with Acknowledgements and thank you to: s, Dr Ian Roos (Cancer
Consumer Participation Strategy Plan Implementation Period 2011-2013 Date: 24 December 2010 Developed by: NEMICS Directorate in consultation with Acknowledgements and thank you to: s, Dr Ian Roos (Cancer
Heart health CHD management gaps in general practice
 professional practice Nancy Huang MBBS, DipRACOG, MPH, is National Manager Clinical Programs, Heart Foundation, Melbourne, Victoria. nancy.huang@heartfoundation.org.au Marcus Daddo BSc(Hons), is Manager
professional practice Nancy Huang MBBS, DipRACOG, MPH, is National Manager Clinical Programs, Heart Foundation, Melbourne, Victoria. nancy.huang@heartfoundation.org.au Marcus Daddo BSc(Hons), is Manager
DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN
 DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN 2016-2019 1 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-2019 Primary Health Tasmania t: 1300 653 169 e: info@primaryhealthtas.com.au
DRUG AND ALCOHOL TREATMENT ACTIVITY WORK PLAN 2016-2019 1 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-2019 Primary Health Tasmania t: 1300 653 169 e: info@primaryhealthtas.com.au
Women s Health Association of Victoria
 Women s Health Association of Victoria PO Box 1160, Melbourne Vic 3001 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Contact person for this submission:
Women s Health Association of Victoria PO Box 1160, Melbourne Vic 3001 Submission to the Commonwealth Government on the New National Women s Health Policy 1 July, 2009. Contact person for this submission:
INDIGENOUS MALE HEALTH
 INDIGENOUS MALE HEALTH A report for Indigenous males, their families and communities, and those committed to improving Indigenous male health Dr Mark Wenitong Executive Officer, Australian Indigenous Doctors
INDIGENOUS MALE HEALTH A report for Indigenous males, their families and communities, and those committed to improving Indigenous male health Dr Mark Wenitong Executive Officer, Australian Indigenous Doctors
Primary Health Networks Drug and Alcohol Treatment Services Funding. Updated Activity Work Plan : Drug and Alcohol Treatment
 Primary Health Networks Drug and Alcohol Treatment Services Funding Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Adelaide PHN This Activity Work Plan is an update to the 2016-18 Activity
Primary Health Networks Drug and Alcohol Treatment Services Funding Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Adelaide PHN This Activity Work Plan is an update to the 2016-18 Activity
MidCentral District Health Board Rheumatic Fever Prevention Plan. October 2013
 MidCentral District Health Board Rheumatic Fever Prevention Plan October 2013 Contents Section 1: Introduction... 3 1.1 Executive summary... 3 1.2 Purpose... 5 Section 2: Overview of acute rheumatic fever
MidCentral District Health Board Rheumatic Fever Prevention Plan October 2013 Contents Section 1: Introduction... 3 1.1 Executive summary... 3 1.2 Purpose... 5 Section 2: Overview of acute rheumatic fever
Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for
 Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for Credentialling as a Diabetes Educator Guidelines for indigenous
Guidelines for indigenous allied health, indigenous enrolled nurses, Aboriginal health workers and Aboriginal health practitioners applying for Credentialling as a Diabetes Educator Guidelines for indigenous
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Adelaide PHN This template was used to submit the Primary Health Network s (PHN s) Activity Work Plans to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Adelaide PHN This template was used to submit the Primary Health Network s (PHN s) Activity Work Plans to the Department
State of Cardiovascular Health in the NT DR MARCUS ILTON
 State of Cardiovascular Health in the NT DR MARCUS ILTON Background NT Population For whom we provide Cardiac Care Population - 250,000 Darwin - 140,000 Alice Springs - 40,000 Katherine - 10,000 Tennant
State of Cardiovascular Health in the NT DR MARCUS ILTON Background NT Population For whom we provide Cardiac Care Population - 250,000 Darwin - 140,000 Alice Springs - 40,000 Katherine - 10,000 Tennant
A Framework for Optimal Cancer Care Pathways in Practice
 A to Guide Care Cancer Care A for Care in Practice SUPPORTING CONTINUOUS IMPROVEMENT IN CANCER CARE Developed by the National Cancer Expert Reference Group to support the early adoption of the A to Guide
A to Guide Care Cancer Care A for Care in Practice SUPPORTING CONTINUOUS IMPROVEMENT IN CANCER CARE Developed by the National Cancer Expert Reference Group to support the early adoption of the A to Guide
Primary Health Networks
 Primary Health Networks Activity Work Plan 2016-17 to 2018-19 Budget Central and Eastern Sydney PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN must ensure that
Primary Health Networks Activity Work Plan 2016-17 to 2018-19 Budget Central and Eastern Sydney PHN When submitting this Activity Work Plan 2016-2018 to the Department of Health, the PHN must ensure that
The Vision. The Objectives
 The Vision Older people participate to their fullest ability in decisions about their health and wellbeing and in family, whānau and community life. They are supported in this by co-ordinated and responsive
The Vision Older people participate to their fullest ability in decisions about their health and wellbeing and in family, whānau and community life. They are supported in this by co-ordinated and responsive
Primary Health Networks Greater Choice for At Home Palliative Care
 Primary Health Networks Greater Choice for At Home Palliative Care Brisbane South PHN When submitting the Greater Choice for At Home Palliative Care Activity Work Plan 2017-2018 to 2019-2020 to the Department
Primary Health Networks Greater Choice for At Home Palliative Care Brisbane South PHN When submitting the Greater Choice for At Home Palliative Care Activity Work Plan 2017-2018 to 2019-2020 to the Department
The National perspective Public Health England s vision, mission and priorities
 The National perspective Public Health England s vision, mission and priorities Dr Ann Hoskins Director Children, Young People and Families Public Health England May 2013 Mission Public Health England
The National perspective Public Health England s vision, mission and priorities Dr Ann Hoskins Director Children, Young People and Families Public Health England May 2013 Mission Public Health England
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
The Silent Disease Inquiry into Hepatitis C in Australia
 Australian Government response to the House of Representatives Standing Committee on Health report: The Silent Disease Inquiry into Hepatitis C in Australia November 2016 LIST OF ABBREVIATIONS AHPPC Australian
Australian Government response to the House of Representatives Standing Committee on Health report: The Silent Disease Inquiry into Hepatitis C in Australia November 2016 LIST OF ABBREVIATIONS AHPPC Australian
Accessibility and quality of mental health services in rural and remote Australia. August Recommendations
 AMSANT submission to the Senate Community Affairs References Committee Inquiry: Accessibility and quality of mental health services in rural and remote Australia August 2018 Recommendations 1) Mental health
AMSANT submission to the Senate Community Affairs References Committee Inquiry: Accessibility and quality of mental health services in rural and remote Australia August 2018 Recommendations 1) Mental health
Palliative Care. Working towards the future of quality palliative care for all
 Palliative Care Working towards the future of quality palliative care for all FEBRUARY 2019 Recommended citation Palliative Care Australia 2018, Palliative Care 2030 working towards the future of quality
Palliative Care Working towards the future of quality palliative care for all FEBRUARY 2019 Recommended citation Palliative Care Australia 2018, Palliative Care 2030 working towards the future of quality
FRAMEWORK FOR A HEALTHIER FUTURE:
 SEPTEMBER 2018 FRAMEWORK FOR A HEALTHIER FUTURE: A CONCEPTUAL FRAMEWORK FOR TAKING ACTION TO IMPROVE MEN AND BOYS HEALTH This paper was prepared by Glen Poole, Development Officer at the Australian Men
SEPTEMBER 2018 FRAMEWORK FOR A HEALTHIER FUTURE: A CONCEPTUAL FRAMEWORK FOR TAKING ACTION TO IMPROVE MEN AND BOYS HEALTH This paper was prepared by Glen Poole, Development Officer at the Australian Men
Burden of disease & the Australian Rheumatic Fever Strategy
 Burden of disease & the Australian Rheumatic Fever Strategy RHDA workshop March 2016 Brisbane Convention Exhibition & Centre Claire Boardman Deputy Director, RHDAustralia BN, Cert IC, MPH, CICP, Senior
Burden of disease & the Australian Rheumatic Fever Strategy RHDA workshop March 2016 Brisbane Convention Exhibition & Centre Claire Boardman Deputy Director, RHDAustralia BN, Cert IC, MPH, CICP, Senior
Secondary Prevention Alliance. Progress and Achievements Report. August 2014
 Progress and Achievements Report August 2014 Australian : c/- The George Institute for Global Health PO Box M201 Missenden Rd NSW 2050 Australia t 02 9993 4551 f 02 9993 4501 e seriksson@georgeinstitute.org.au
Progress and Achievements Report August 2014 Australian : c/- The George Institute for Global Health PO Box M201 Missenden Rd NSW 2050 Australia t 02 9993 4551 f 02 9993 4501 e seriksson@georgeinstitute.org.au
School of Rural Health Strategic plan
 School of Rural Health Strategic plan 2017-22 Contents Strategic intent 4 Goals 5 Strategic goals 2017-22 6 The University of Sydney School of Rural Health 2017 22 Strategic Plan October 2017 The School
School of Rural Health Strategic plan 2017-22 Contents Strategic intent 4 Goals 5 Strategic goals 2017-22 6 The University of Sydney School of Rural Health 2017 22 Strategic Plan October 2017 The School
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Peripheral arterial disease Potential output:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Peripheral arterial disease Potential output:
4 th A-TRAC Symposium
 4 th A-TRAC Symposium Reflect. Unite. Take Action Session 4: Moving Forward National perspective on Aboriginal tobacco initiatives 4 September 2014 Dr Tom Calma AO National Coordinator Tackling Indigenous
4 th A-TRAC Symposium Reflect. Unite. Take Action Session 4: Moving Forward National perspective on Aboriginal tobacco initiatives 4 September 2014 Dr Tom Calma AO National Coordinator Tackling Indigenous
Primary Health Networks
 Primary Health Networks REVISED Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 REVISED Drug and Alcohol Treatment Budget NEPEAN BLUE MOUNTAINS PHN When submitting this Activity Work Plan
Primary Health Networks REVISED Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 REVISED Drug and Alcohol Treatment Budget NEPEAN BLUE MOUNTAINS PHN When submitting this Activity Work Plan
Cost-effective actions to tackle the biggest killer of men and women HEART DISEASE
 Cost-effective actions to tackle the biggest killer of men and women HEART DISEASE Submission on the 2017-18 Federal Budget from the National Heart Foundation of Australia The Challenge This submission
Cost-effective actions to tackle the biggest killer of men and women HEART DISEASE Submission on the 2017-18 Federal Budget from the National Heart Foundation of Australia The Challenge This submission
Updated Activity Work Plan : Drug and Alcohol Treatment. Western NSW PHN
 Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Western NSW PHN 1 Overview This Drug and Alcohol Treatment Activity Work Plan covers the period from 1 July 2016 to 30 June 2019 and is
Updated Activity Work Plan 2016-2019: Drug and Alcohol Treatment Western NSW PHN 1 Overview This Drug and Alcohol Treatment Activity Work Plan covers the period from 1 July 2016 to 30 June 2019 and is
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme
 Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Aboriginal Health Data for Our Region. Newcastle/Hunter Aboriginal Partnership Forum Planning Day July 2017
 Aboriginal Health Data for Our Region Newcastle/Hunter Aboriginal Partnership Forum Planning Day July 2017 Aboriginal Health Needs Assessment Aimed to identify local health priorities for action, and inform
Aboriginal Health Data for Our Region Newcastle/Hunter Aboriginal Partnership Forum Planning Day July 2017 Aboriginal Health Needs Assessment Aimed to identify local health priorities for action, and inform
The Cancer Council NSW. Submission to the Legislative Assembly Public Accounts Committee. Inquiry into NSW State Plan Reporting
 The Cancer Council NSW Submission to the Legislative Assembly Public Accounts Committee Inquiry into NSW State Plan Reporting December 2007 2 Inquiry into NSW State Plan Reporting The Cancer Council NSW
The Cancer Council NSW Submission to the Legislative Assembly Public Accounts Committee Inquiry into NSW State Plan Reporting December 2007 2 Inquiry into NSW State Plan Reporting The Cancer Council NSW
PHYSIOTHERAPY AND DIABETES
 PHYSIOTHERAPY AND DIABETES March 2006 Executive Summary The Australian Physiotherapy Association (APA) strongly supports the use of multidisciplinary teams to provide evidence-based care to individuals
PHYSIOTHERAPY AND DIABETES March 2006 Executive Summary The Australian Physiotherapy Association (APA) strongly supports the use of multidisciplinary teams to provide evidence-based care to individuals
Martin Foley, Minister for Mental Health Message to the mental health sector
 Martin Foley, Minister for Mental Health Message to the mental health sector June 2015 There is a lot happening in mental health and wellbeing policy at both state and Commonwealth levels. The Andrews
Martin Foley, Minister for Mental Health Message to the mental health sector June 2015 There is a lot happening in mental health and wellbeing policy at both state and Commonwealth levels. The Andrews
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Myocardial infarction: secondary prevention in primary and secondary care for patients following a myocardial infarction 1.1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Myocardial infarction: secondary prevention in primary and secondary care for patients following a myocardial infarction 1.1
Review of Aboriginal Women s Health Check Day (AWHCD)
 April 2018 Review of Aboriginal Women s Health Check Day (AWHCD) Programme commenced from 2009 Tammy Yam Northern Sydney Central Coast Acknowledgements Clients of Aboriginal Women s Health Check Day Members
April 2018 Review of Aboriginal Women s Health Check Day (AWHCD) Programme commenced from 2009 Tammy Yam Northern Sydney Central Coast Acknowledgements Clients of Aboriginal Women s Health Check Day Members
Evaluation of the Victorian Aboriginal Spectacles Subsidy Scheme
 Evaluation of the Victorian Aboriginal Spectacles Subsidy Scheme A Summary Report 2016 We acknowledge Barry Atkinson, Yorta Yorta artist, for the artwork Up Stream Down Stream that is featured in this
Evaluation of the Victorian Aboriginal Spectacles Subsidy Scheme A Summary Report 2016 We acknowledge Barry Atkinson, Yorta Yorta artist, for the artwork Up Stream Down Stream that is featured in this
Towards a Decadal Plan for Australian Nutrition Science September 2018
 Towards a Decadal Plan for Australian Nutrition Science September 2018 The Dietitians Association of Australia (DAA) is the national association of the dietetic profession with over 6,400 members, and
Towards a Decadal Plan for Australian Nutrition Science September 2018 The Dietitians Association of Australia (DAA) is the national association of the dietetic profession with over 6,400 members, and
HEALTH CONSUMERS QUEENSLAND
 HEALTH CONSUMERS QUEENSLAND SUBMISSION TO The Inquiry into the establishment of a Queensland Health Promotion Commission Health and Ambulance Services Committee 27 th November 2015 Health Consumers Queensland
HEALTH CONSUMERS QUEENSLAND SUBMISSION TO The Inquiry into the establishment of a Queensland Health Promotion Commission Health and Ambulance Services Committee 27 th November 2015 Health Consumers Queensland
Aboriginal and Torres Strait Islander Health Performance Framework Report
 Aboriginal and Torres Strait Islander Health Performance Framework 26 Report Report Findings Tier 1: Health Status and Outcomes Improvements: Mortality Infant Mortality Deaths due to Circulatory Disease
Aboriginal and Torres Strait Islander Health Performance Framework 26 Report Report Findings Tier 1: Health Status and Outcomes Improvements: Mortality Infant Mortality Deaths due to Circulatory Disease
2.2 years. 35% higher 1/2. less 1/5. Remote and outer-regional Australians see mental health professionals at
 Remote and outer-regional death rates Remote and outer-regional life expectancy Remote and outer-regional Australians see doctors at Remote and outer-regional Australians see mental health professionals
Remote and outer-regional death rates Remote and outer-regional life expectancy Remote and outer-regional Australians see doctors at Remote and outer-regional Australians see mental health professionals
ceptions of Perceptions of mental health service delivery among staff and Indigenous consumers: it's still about communication
 ceptions of Perceptions of mental health service delivery among staff and Indigenous consumers: it's still about communication Diann Eley, Louise Young, Keith Hunter, Peter Baker, Ernest Hunter and Dominique
ceptions of Perceptions of mental health service delivery among staff and Indigenous consumers: it's still about communication Diann Eley, Louise Young, Keith Hunter, Peter Baker, Ernest Hunter and Dominique
NHS QIS National Measurement of Audit Acute Coronary Syndrome
 NHS QIS National Measurement of Audit Acute Coronary Syndrome Things have changed based on the experience and feedback from the first cycle of measurement and, for the better we think! The Acute Coronary
NHS QIS National Measurement of Audit Acute Coronary Syndrome Things have changed based on the experience and feedback from the first cycle of measurement and, for the better we think! The Acute Coronary
Associate Professor Gerry Devlin
 Associate Professor Gerry Devlin Clinical Cardiologist and Interventional Cardiologist NZ Heart Foundation Hamilton 9:00-9:15 Secondary Prevention of IHD The Challenge of Secondary Prevention Associate
Associate Professor Gerry Devlin Clinical Cardiologist and Interventional Cardiologist NZ Heart Foundation Hamilton 9:00-9:15 Secondary Prevention of IHD The Challenge of Secondary Prevention Associate
Peer Work Leadership Statement of Intent
 Peer Work Leadership Statement of Intent A National Professional Association for Mental Health Peer Workers Peer work leaders from Queensland, Victoria and NSW and colleagues from the USA participated
Peer Work Leadership Statement of Intent A National Professional Association for Mental Health Peer Workers Peer work leaders from Queensland, Victoria and NSW and colleagues from the USA participated
KEY QUESTIONS What outcome do you want to achieve for mental health in Scotland? What specific steps can be taken to achieve change?
 SCOTTISH GOVERNMENT: NEXT MENTAL HEALTH STRATEGY Background The current Mental Health Strategy covers the period 2012 to 2015. We are working on the development of the next strategy for Mental Health.
SCOTTISH GOVERNMENT: NEXT MENTAL HEALTH STRATEGY Background The current Mental Health Strategy covers the period 2012 to 2015. We are working on the development of the next strategy for Mental Health.
Statement about the release of the National Ice Taskforce Report, release of two Review report and various announcements by the Australian Government
 Statement about the release of the National Ice Taskforce Report, release of two Review report and various announcements by the Australian Government 9 December 2015 The Network of Australian State and
Statement about the release of the National Ice Taskforce Report, release of two Review report and various announcements by the Australian Government 9 December 2015 The Network of Australian State and
At the heart of health promotion: Health Promotion Policy & Advocacy. Rachelle Foreman
 . At the heart of health promotion: Australian About the Heart Maps Foundation & Health Promotion Policy & Advocacy Rachelle Foreman I would like to pay my respects to the Traditional Owners of the land
. At the heart of health promotion: Australian About the Heart Maps Foundation & Health Promotion Policy & Advocacy Rachelle Foreman I would like to pay my respects to the Traditional Owners of the land
THE AUSTRALIAN WOMEN S HEALTH CHARTER. The Australian Women s Health Network
 THE AUSTRALIAN WOMEN S HEALTH CHARTER The Australian Women s Health Network 2 THE AUSTRALIAN WOMEN S HEALTH CHARTER Our Vision We pledge to work to create a healthy society where Australian women experience
THE AUSTRALIAN WOMEN S HEALTH CHARTER The Australian Women s Health Network 2 THE AUSTRALIAN WOMEN S HEALTH CHARTER Our Vision We pledge to work to create a healthy society where Australian women experience
Australian asthma indicators. Five-year review of asthma monitoring in Australia
 Australian asthma indicators Five-year review of asthma monitoring in Australia The Australian Institute of Health and Welfare is Australia s national health and welfare statistics and information agency.
Australian asthma indicators Five-year review of asthma monitoring in Australia The Australian Institute of Health and Welfare is Australia s national health and welfare statistics and information agency.
Mental health and Aboriginal people and communities
 Mental health and Aboriginal people and communities 10-year mental health plan technical paper Contents Background...1 Aboriginal communities and the experience of poor mental health...2 Policy and program
Mental health and Aboriginal people and communities 10-year mental health plan technical paper Contents Background...1 Aboriginal communities and the experience of poor mental health...2 Policy and program
Exercise & Sports Science Australia Submission: global action plan to promote physical activity
 Exercise & Sports Science Australia Submission: global action plan to promote physical activity Australia needs to expand its allied health workforce and improve access to services that provide physical
Exercise & Sports Science Australia Submission: global action plan to promote physical activity Australia needs to expand its allied health workforce and improve access to services that provide physical
Community Needs Analysis Report
 Grampians Medicare Local Community Needs Analysis Report Summary October 2013 2 Contents Introduction 3 Snapshot of results 4 Stakeholder feedback 5 Health status of residents 6 Health behaviour of residents
Grampians Medicare Local Community Needs Analysis Report Summary October 2013 2 Contents Introduction 3 Snapshot of results 4 Stakeholder feedback 5 Health status of residents 6 Health behaviour of residents
Carers Australia Strategic Plan
 Carers Australia Strategic Plan 2012 2015 About Carers There are 2.6 million carers in Australia who provide unpaid care and support to family members and friends who have a disability, mental illness,
Carers Australia Strategic Plan 2012 2015 About Carers There are 2.6 million carers in Australia who provide unpaid care and support to family members and friends who have a disability, mental illness,
City of Moonee Valley Draft MV 2040 Strategy
 + City of Moonee Valley Draft MV 2040 Strategy Your neighbourhood, your vision May 2018 Contact: Louise Sadler (Acting)Director of Strategy, Advocacy and Community Engagement Women s Health West 317-319
+ City of Moonee Valley Draft MV 2040 Strategy Your neighbourhood, your vision May 2018 Contact: Louise Sadler (Acting)Director of Strategy, Advocacy and Community Engagement Women s Health West 317-319
Final Report & Evaluation
 Northern Adelaide Medicare Local Northern Respiratory Partnership Project Final Report & Evaluation May 2015 1 This publication is created by the Northern Adelaide Medicare Local (NAML) Ltd. in collaboration
Northern Adelaide Medicare Local Northern Respiratory Partnership Project Final Report & Evaluation May 2015 1 This publication is created by the Northern Adelaide Medicare Local (NAML) Ltd. in collaboration
Burden of end-stage renal disease
 Summary of Indigenous health: End-stage renal disease Neil Thomson and Sasha Stumpers Australian Indigenous HealthInfoNet, Edith Cowan University www.healthinfonet.ecu.edu.au This summary of end-stage
Summary of Indigenous health: End-stage renal disease Neil Thomson and Sasha Stumpers Australian Indigenous HealthInfoNet, Edith Cowan University www.healthinfonet.ecu.edu.au This summary of end-stage
The Cancer Council NSW
 The Cancer Council NSW Submission to the Legislative Assembly Social Issues Committee Inquiry into closing the gap: Overcoming Indigenous disadvantage January 2008 2 Inquiry into Closing the Gap Overcoming
The Cancer Council NSW Submission to the Legislative Assembly Social Issues Committee Inquiry into closing the gap: Overcoming Indigenous disadvantage January 2008 2 Inquiry into Closing the Gap Overcoming
Community Advisory Council Terms of Reference
 Community Advisory Council Terms of Reference The role of the Community Advisory Councils (CACs) is to provide the Board of the Sunshine Coast Health Network Ltd (SCHN) trading as Central Queensland, Wide
Community Advisory Council Terms of Reference The role of the Community Advisory Councils (CACs) is to provide the Board of the Sunshine Coast Health Network Ltd (SCHN) trading as Central Queensland, Wide
Cancer Control Council Evaluation and Monitoring Framework
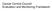 Cancer Control Council Evaluation and Monitoring Framework Table of contents 1. Purpose...1 2. Background...1 3. Clarification of key tasks...2 4. International evaluation and monitoring frameworks...3
Cancer Control Council Evaluation and Monitoring Framework Table of contents 1. Purpose...1 2. Background...1 3. Clarification of key tasks...2 4. International evaluation and monitoring frameworks...3
Our footprints: a traveller s guide to the COAG implementation process in Western Australia
 Our footprints: a traveller s guide to the COAG implementation process in Western Australia Beverley Stone 1, Kevin Cox 1, Rosalie Miles 1, Susan Powe 1, Vicki O Donnell, Linda Waters 1 WA Country Health
Our footprints: a traveller s guide to the COAG implementation process in Western Australia Beverley Stone 1, Kevin Cox 1, Rosalie Miles 1, Susan Powe 1, Vicki O Donnell, Linda Waters 1 WA Country Health
Beyond the Heart: Transforming Care
 Beyond the Heart: Transforming Care CHILDHOOD HEART DISEASE NATIONAL ACTION PLAN 2018 Draft for Public Consultation September 2018 2 Transforming childhood heart disease care in Australia is the best possible
Beyond the Heart: Transforming Care CHILDHOOD HEART DISEASE NATIONAL ACTION PLAN 2018 Draft for Public Consultation September 2018 2 Transforming childhood heart disease care in Australia is the best possible
Formal Reference Groups, Committees and Meetings
 Formal Reference Groups, s and Meetings Advocacy and representation Lead agency and meeting Meeting summary NADA and sector NGO Advisory Drug and Alcohol Program Council Program Council Quality in Treatment
Formal Reference Groups, s and Meetings Advocacy and representation Lead agency and meeting Meeting summary NADA and sector NGO Advisory Drug and Alcohol Program Council Program Council Quality in Treatment
NATIONAL RURAL HEALTH ALLIANCE. Pre-Budget Submission
 NATIONAL RURAL HEALTH ALLIANCE Pre-Budget Submission 2018-19 Introduction The National Rural Health Alliance (the Alliance) is Australia s peak representative body for rural and remote health. We are committed
NATIONAL RURAL HEALTH ALLIANCE Pre-Budget Submission 2018-19 Introduction The National Rural Health Alliance (the Alliance) is Australia s peak representative body for rural and remote health. We are committed
Myocardial Ischaemia National Audit Project (MINAP): Improving data capture and use across South Wales
 Myocardial Ischaemia National Audit Project (MINAP): Improving data capture and use across South Wales Author Owner Document Reference Alison Turner Cardiovascular Audit and Primary Care Nurse South Wales
Myocardial Ischaemia National Audit Project (MINAP): Improving data capture and use across South Wales Author Owner Document Reference Alison Turner Cardiovascular Audit and Primary Care Nurse South Wales
CONSUMER AND CARER PARTICIPATION POLICY. a framework for the mental health sector
 CONSUMER AND CARER PARTICIPATION POLICY a framework for the mental health sector developed by the National Consumer and Carer Forum Best Practice Principles for Inclusion in a Participation Policy
CONSUMER AND CARER PARTICIPATION POLICY a framework for the mental health sector developed by the National Consumer and Carer Forum Best Practice Principles for Inclusion in a Participation Policy
What's Needed to Close the Indigenous Health Inequality Gap!
 What's Needed to Close the Indigenous Health Inequality Gap! Professor Tom Calma AO National Coordinator Tackling Indigenous Smoking and Patron & Chair, Poche Indigenous Health Network What's Needed to
What's Needed to Close the Indigenous Health Inequality Gap! Professor Tom Calma AO National Coordinator Tackling Indigenous Smoking and Patron & Chair, Poche Indigenous Health Network What's Needed to
Time for Action on Health Policy
 Time for Action on Health Policy Northern Territory Federal Election Statement 2016 Overview The Royal Australasian College of Physicians (RACP) is committed to working with all political parties to inform
Time for Action on Health Policy Northern Territory Federal Election Statement 2016 Overview The Royal Australasian College of Physicians (RACP) is committed to working with all political parties to inform
Public Health Association of Australia: Policy-at-a-glance Prevention and Management of Overweight and Obesity in Australia Policy
 Public Health Association of Australia: Policy-at-a-glance Prevention and Management of Overweight and Obesity in Australia Policy Key message: PHAA will 1. Advocate that Federal, State and Territory governments:
Public Health Association of Australia: Policy-at-a-glance Prevention and Management of Overweight and Obesity in Australia Policy Key message: PHAA will 1. Advocate that Federal, State and Territory governments:
Provincial Cancer Control Advisory Committee
 Provincial Cancer Control Advisory Committee Annual Performance Report 2012-2013 Table of Contents 1.0 Overview... 4 2.0 Shared Partnerships... 7 3.0 Highlights and Accomplishments... 7 4.0 Report on
Provincial Cancer Control Advisory Committee Annual Performance Report 2012-2013 Table of Contents 1.0 Overview... 4 2.0 Shared Partnerships... 7 3.0 Highlights and Accomplishments... 7 4.0 Report on
Indigenous Eye Health Indicators
 Indigenous Eye Health Indicators This position paper frames pertinent Indigenous eye health indicators at the regional, jurisdictional, and national levels as recommended in the Roadmap to Close the Gap
Indigenous Eye Health Indicators This position paper frames pertinent Indigenous eye health indicators at the regional, jurisdictional, and national levels as recommended in the Roadmap to Close the Gap
Goldfields population and health snapshot
 Goldfields population and health snapshot The Goldfields region is located in the south east corner of Western Australia and incorporates eight local government areas. It is the largest health region in
Goldfields population and health snapshot The Goldfields region is located in the south east corner of Western Australia and incorporates eight local government areas. It is the largest health region in
NT Aboriginal Health KPIs: health, data and change Territory style. Pasqualina Coffey AMSANT
 NT Aboriginal Health KPIs: health, data and change Territory style Pasqualina Coffey AMSANT Overview NT Indigenous health care landscape Development of CQI and clinical indicators in the NT NT AHKPIs governance
NT Aboriginal Health KPIs: health, data and change Territory style Pasqualina Coffey AMSANT Overview NT Indigenous health care landscape Development of CQI and clinical indicators in the NT NT AHKPIs governance
Presentation to the Standing Committee on Health Chronic Diseases Related to Aging. October 17, 2011
 THE CANADIAN CHIROPRACTIC ASSOCIATION Presentation to the Standing Committee on Health Chronic Diseases Related to Aging October 17, 2011 Prevention as a mean to manage or delay chronic diseases related
THE CANADIAN CHIROPRACTIC ASSOCIATION Presentation to the Standing Committee on Health Chronic Diseases Related to Aging October 17, 2011 Prevention as a mean to manage or delay chronic diseases related
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Country WA PHN When submitting this Activity Work Plan 2016-2019 to the Department
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Drug and Alcohol Treatment Budget Country WA PHN When submitting this Activity Work Plan 2016-2019 to the Department
WAIS Sport and Athlete Planning, Monitoring and Management Policy
 WAIS Sport and Athlete Planning, Monitoring and Management Policy Owner: Performance Team Directors Version: 1.3 Approved by: Chief Executive Officer Next review date: December 2020 1. POLICY WAIS will
WAIS Sport and Athlete Planning, Monitoring and Management Policy Owner: Performance Team Directors Version: 1.3 Approved by: Chief Executive Officer Next review date: December 2020 1. POLICY WAIS will
Professor Norman Sharpe. Heart Foundation West Coast
 Professor Norman Sharpe Heart Foundation West Coast Primary Care the Keystone to Heart Health Improvement Norman Sharpe June 2013 The heart health continuum and the keystone position The culprit disease
Professor Norman Sharpe Heart Foundation West Coast Primary Care the Keystone to Heart Health Improvement Norman Sharpe June 2013 The heart health continuum and the keystone position The culprit disease
GOVERNING BODY REPORT
 GOVERNING BODY REPORT DATE OF MEETING: 20th September 2012 TITLE OF REPORT: KEY MESSAGES: NHS West Cheshire Clinical Commissioning Group has identified heart disease as one of its six strategic clinical
GOVERNING BODY REPORT DATE OF MEETING: 20th September 2012 TITLE OF REPORT: KEY MESSAGES: NHS West Cheshire Clinical Commissioning Group has identified heart disease as one of its six strategic clinical
Young onset dementia service Doncaster
 Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Equally Well framework for collaborative action
 Equally Well framework for collaborative action How we work and what actions we can take to improve the physical health of people who experience mental health and addiction problems Phase 3: 2015 Contents
Equally Well framework for collaborative action How we work and what actions we can take to improve the physical health of people who experience mental health and addiction problems Phase 3: 2015 Contents
