Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC
|
|
|
- Randell McDonald
- 6 years ago
- Views:
Transcription
1 Puzzling Pacemakers Cheryl Herrmann, APN, CCRN, CCNS-CSC-CMC Pacemaker: An electric device implanted in the body to regulate the heart beat. Delivers electrical stimuli over leads with electrodes in contact with the heart Consists of a generator and leads Generator Mini computer with power source Leads Electrical wires used to transmit electrical data back & forth from the heart to the pulse generator The NASPE/BPEG generic (NBG) code Position I II III IV V Category Chamber(s) Paced Chamber(s) sensed Response to Sensing Programmability, Rate Antitachyarrhythmia Letters used A = Atrium V = Ventricle D = Dual (A+V) A = Atrium V = Ventricle D = Dual (A+V) T= Triggered I = Inhibited D = Dual (T+I) First Letter: Indicates what leads are available to pace A = Atrium V = Ventricle D = Dual (A+V) Modulation P = Simple Programmable M = Multi- Programmable C = Communicating R = Rate modulation Functions P = Pacing (antitachyarrhythmia S = Shock D = Dual (P+S) Second Letter: Indicates which chamber that the pulse generator will monitor for spontaneous depolarization A = Atrium V = Ventricle D = Dual (A+V) Third Letter: Indicates what the pacemaker will do when it senses an event Asynchronous pacing Also called fixed rate or magnet mode Delivers a pacing stimulus at a fixed rate regardless of the heart s intrinsic activity It will cause competition with the heart s intrinsic activity, and the pacing stimulus may land during the descending limb of the T-wave
2 T = Triggered When the pacemaker activates a depolarization wave to a sensed event An example of a triggered response is when the pacemaker fires an impulse to the ventricles after it senses an atrial depolarization I = Inhibited Demand or synchronous pacing Pacemaker responds to a sensed event by NOT firing a response for a certain amount of time. Paces only when patient s heart rate falls below set rate Avoids R on T phenomenon and ventricular dysrhythmias D = Dual (T+I) Pacemaker can respond in a triggered manner for some pre-programmed cases and in an inhibitory manner for other pre-programmed events Codes are combined to describe: The mode of pacing The mode of sensing How the pacemaker will respond to the presence or absence of intrinsic beats AOO AAI VOO VVI Pacemaker Indications Junctional Rhythms Second-degree AV block -- Mobitz type II Third-degree AV block SA node conduction problems Heart Failure with ventricular dysynchrony Single-Chamber Systems The pacing lead is implanted in the atrium or ventricle, depending on the chamber to be paced and sensed VVI Ventricular Demand Pacing Pacer spike should be just before the QRS when no intrinsic event sensed Ventricular Sensing Sensed intrinsic QRS inhibits ventricular pacing Used as backup pacing Does not provide AV synchrony -- may get pacemaker syndrome
3 AAI Atrial Demand Pacing Pacer spike should be just before the p wave when no intrinsic event sensed Atrial Sensing Sensed intrinsic p wave inhibits atrial pacing Used to provide atrial contraction with SA node conduction problems AOO Atrial asynchronous pacing at programmed pacing rate No Sensing Used to provide atrial contraction with SA node conduction problems Dual-Chamber Systems The pacing leads are implanted in both the atrium and ventricle. DDD Pacing in both the atrium and ventricle Pacer spike should be just before the p wave when no intrinsic event sensed Pacer spike should be just before the QRS when no intrinsic event sensed Sensing in both the atrium and ventricle Intrinsic p wave and intrinsic QRS can inhibit pacing Intrinsic p wave can trigger a paced QRS Four Functions (faces) of DDD Pacing: 1. Atrial Sense, Ventricular Sense (AS/VS) Native atrial and ventricular depolarization present. No pacing needed. 2. Atrial Pace, Ventricular Sense (AP/VS) No atrial depolarization present. Atrial pacing occurs. Native ventricular depolarization present. Good for junctional rhythms 3. Atrial Sense, Ventricular Pace (AS/ VP) Native atrial depolarization present. No atrial pacing needed. No ventricular depolarization present. Ventricular pacing occurs. Good for complete heart block or Mobitz II 4. Atrial Pace, Ventricular Pace (AP/VP) No atrial or ventricular depolarization present. Atrial and ventricular pacing occurs. Good for SA arrest, asystole
4 These four functions occur on a beat to beat basis depending on the conduction system of the individual s heart. AP/VP AS/VP AS/VS AP/VS DDI or DDIR Paces both the atrium and ventricle Senses atrial and ventricle however does not track the atrium. Good with for high atrial rates to prevent a high ventricular response (atrial tachyarrhythmias) DVI: Paces both the atrium and ventricle No atrial sensing --- does not track the atrium. Senses ventricle Not commonly used. Good when atria silent. DOO Atrial and ventricular asynchronous pacing at programmed pacing rate No Sensing of the atrium or ventricle Used when no attempt to synchronize paced events with intrinsic activity Contraindicated in the case of a competing intrinsic rhythm Good when individual is pacer dependent Pacemaker Terminology & Troubleshooting MA (Milliamps) The amount of energy needed to make the heart depolarize with the electrode (capture) Range from Usually set just above a patient s threshold to ensure a good capture Threshold is the minimal output required to capture the heart. On DDD pacemakers the MA is set for both the atrium and ventricle
5 Threshold Level The minimum stimulus required to cause stimulation of the myocardium (pacing) or minimum voltage for an intrinsic complex to be sensed. Also known as stimulation threshold Fire The spike that is produced when the pacemaker elicits an electrical stimulus Capture An effective, consistent cardiac depolarization of the heart caused by the pacemaker s electrical stimulus To assess capture it is necessary to see pacemaker spikes followed by depolarization For example an atrial spike followed by a p wave or a ventricular spike followed by a QRS. Failure to Capture The presence of one or more pacer spikes that are not followed by an appropriately timed atrial and/or ventricular response Treatment: failure to capture Increase MA until capture present o Transvenous pacing typically requires MA 3 5 to capture o Epicardial pacing typically requires MA o Transcutaneous (external) pacing typically requires MA o Permanent pacing typically requires MA 3-5 Transvenous Pacing o Have patient change positions to see if the lead will float back to make contact with the ventricular wall Epicardial Pacing o After increasing MA, try switching polarity of wires. The negative lead is the wire that paces and the positive lead is the wire that is providing the ground. o If only one epicardial wire is functional, place a skin lead. This lead should be in the positive pole. Permanent Pacing o May be a dislodged lead All Pacing treat underlying conditions o Acidosis o Electrolyte imbalances especially hyperkalemia
6 Sensing/Sensitivity Sensing is the ability of the pacemaker to see when an intrinsic depolarization is occurring. The level at which intrinsic atrial or ventricular activity is recognized by the sensing electrodes; the lower the number, the greater the sensitivity With proper sensing, no pacer spike should occur during the escape interval Undersensing (Failure to Sense) Undersensing leads to overpacing Pacemaker does not see or missed the intrinsic beat, and responds with a spike Pacemaker spikes where they should not be. Treatment of Undersensing Decrease the sensitivity (millivolt setting) to make the pacemaker more sensitive The lower the number, the greater the sensitivity If the ventricular mv is set at 2 mv, the pacemaker will not see any QRS that is less than 2mV. If the QRS is small, the mv needs to be decreased to make the pacer more sensitive and see all the QRSs. Check all connections and batteries on temporary pacemakers. With epicardial pacing, try switching polarity. Oversensing (Failure to Pace) Oversensing leads to underpacing Pacemaker sees complexes that are not p waves or QRSs and stops the pacer from firing or delivering a spike. An electrical signal other than the intended P or R wave is detected. For example a peaked T wave may be detected as an R wave. On EKG, an inappropriate long pause between pacing spikes
7 Treatment of Oversensing Increase the sensitivity (millivolt setting) to make the pacemaker less sensitive The higher the number, the less the sensitivity If the ventricular mv is set at 2 mv, the pacemaker will detect any complex that is greater than 2mV and stops the pacer from firing or delivering a spike. Typically this is a peaked T wave so the mv needs to be increased to number larger than the mv of the T wave. Failure to Pace not related to sensitivity settings The absence of packing artifacts when the intrinsic heart rate is slower than the pacemakers set rate. Treatment: Failure to pace Temporary Pacemakers o Change the battery as many times it is a dead battery o Check for loose or disconnected lead connections o With epicardial pacing, if only one epicardial wire is functional, place a skin lead. This lead should be in the positive pole. Permanent Pacemaker o Battery may need to be changed or leads may be fractured Timing Intervals When the pacemaker senses an atrial or ventricular complex, it starts the stopwatch of the generator. The stopwatch starts to measure a pre-designated amount of time during which the pacemaker will not fire Atrial and Ventricular Intervals A - A interval V- V Interval V- A Interval AV Interval Refractory Periods In pacing, a programmable parameter that controls the length of time following a paced or sensed beat, during which the pacemaker s sensing circuit does not respond to sensed events. PVARP=Post Ventricular Atrial Refractory Period=atrial refractory period VRP=Ventricular Refractory Period Rate Intervals Lower Rate Defines the lowest rate the pacemaker will pace Upper Rate Defines the shortest interval (highest rate) the pacemaker can pace as dictated by the sensor
8 Atrial Tracking Ventricular pacing rate follows or tracks the atrial activity Provides AV synchrony to get the benefit of the atrial kick (contraction) or 15 20% more of the cardiac output and thus prevents pacemaker syndrome If the atrial rate exceeds the upper rate limit, the pacer will postpone a ventricular output pulse until the upper rate limit interval times out. It does this by causing a paced Wenckebach or paced Mobitz II Steps to interpret Pacemaker rhythms 1. Select the lead in which the pacemaker spike(s) is seen the best 2. Identify the pacemaker spikes a. Atrial spikes should be noted immediately before the p wave b. Ventricular spikes should be noted immediately before the QRS c. Dual chamber pacing --- may or may not have two spikes depending on the intrinsic activity 3. After identifying the pacer spikes as atrial and/or ventricular, note where they are falling in relation to the p wave and to the QRS. Are they falling where they should be? If not, where are they falling and why. 4. When the pacer spikes are not falling where they should be then be prepared to treat immediately. 5. Is there capture? 6. What are the pacemaker settings including rate?
9 ICD: Internal Cardiac Defibrillator Treats tachydysthythmias by tiered functions Antitachycardia Pacing o The device fires a preset number of rapid pulses in succession in an attempt to terminate the ventricular tachycardia Cardioversion/Defibrillation at low voltage Back up pacing for bradyarrhythmias post cardioversion or defibrillation Pacemaker Magnet Mode When a magnet is applied the pacemaker paces asynchronously (no sensing) The pacemaker returns to previously programmed settings when the magnet is removed. The magnet mode is used to check the programming of the pacemaker and the battery life When a patient places the magnet over his device, it will go asynchronous to get a pacemaker strip to determine how well the device is functioning. A magnet does not turn off a pacemaker. A pacemaker is only turned off with a programming device. ICD Magnet Mode Magnet application will NOT affect the Brady pacing function- it will continue as programmed. ICD magnet placement will disable the sensing function of the device and therefore- no therapy will be delivered It will continue to pace but will not defibrillate Once the magnet is removed, Tachy function will be enabled (restored) When to use the magnet in ICDs: Inappropriate Shocks Use until the company representative can interrogate the device and determine the cause for the inappropriate shocks Surgery: patient must be on monitor in the OR Suite and Turned back on in Recovery Area End stage disease states/hospice care (Physician ordered) March 2014
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART I Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 PROFESSIONAL NURSING PRACTICE CAN ONLY ADVANCE AS MUCH AS INDIVIDUAL
Figure 2. Normal ECG tracing. Table 1.
 Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Figure 2. Normal ECG tracing that navigates through the left ventricle. Following these bundle branches the impulse finally passes to the terminal points called Purkinje fibers. These Purkinje fibers are
Pacing Codes and Modes Concepts
 Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
Pacing Codes and Modes Concepts Pacing codes and modes concepts Objectives Upon completion of this program the participant will be able to: State what the first four positions of the NBG code represent.
Pediatric pacemakers & ICDs:
 Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Pediatric pacemakers & ICDs: perioperative management Manchula Navaratnam Clinical Assistant Professor LPCH, Stanford SPA 2016 Conflict of interest: none Objectives Indications in pediatrics Components
Timing cycles. Objectives Upon completion of this program the participant will be able to:
 Timing Cycles Timing cycles Objectives Upon completion of this program the participant will be able to: Identify the basic timing cycles of a single and dual chamber pacemaker. Describe the characteristics
Timing Cycles Timing cycles Objectives Upon completion of this program the participant will be able to: Identify the basic timing cycles of a single and dual chamber pacemaker. Describe the characteristics
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO
 Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! What is a
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! What is a
RN-BC, MS, CCRN, FAHA
 Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! 1 A. Atropine
Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Follow me on Twitter! CEE Med Updates@BarbaraFurryRN Like me on Facebook! 1 A. Atropine
SARASOTA MEMORIAL HOSPITAL
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE PACEMAKERS AND DETERMINING PACEMAKER DATE: REVIEWED: PAGES: 10/99 11/18 1 of 7 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: *Qualified RN PURPOSE: To establish
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE PACEMAKERS AND DETERMINING PACEMAKER DATE: REVIEWED: PAGES: 10/99 11/18 1 of 7 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: *Qualified RN PURPOSE: To establish
Cardiac Rhythm Device Management. PBL STOP Your acronym for a standardized follow-up
 Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
Cardiac Rhythm Device Management PBL STOP Your acronym for a standardized follow-up What s in it for you? What do you need to feel comfortable with a pacemaker/icd follow-up? 2 CORE OBJECTIVE Provide a
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ
 ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
ΤΟ ΗΚΓ ΣΤΟΝ ΒΗΜΑΤΟΔΟΤΟΥΜΕΝΟ ΑΣΘΕΝΗ ΤΖΩΡΤΖ ΔΑΔΟΥΣ ΕΠΙΚΟΥΡΟΣ ΚΑΘΗΓΗΤΗΣ Α.Π.Θ. ΜΑΡΙΑ ΚΑΡΑΛΙΟΛΙΟΥ ΕΙΔΙΚΕΥΟΜΕΝΗ ΙΑΤΡΟΣ ΚΑΡΔΙΟΛΟΓΟΣ Β ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Α.Π.Θ. ΙΠΠΟΚΡΑΤΕΙΟ Γ.Ν.Θ. 5 Why a Pacemaker is Implanted
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS
 Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
Temporary pacemaker 삼성서울병원 심장혈관센터심장검사실 박정왜 RN, CCDS NBG Codes 1st Letter 2nd Letter 3rd Letter A V D Chamber(s) Paced = atrium = ventricle = dual (both atrium and ventricle) Chamber(s) Sensed A = atrium
TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER)
 TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER) TYPES OF PACERS 2018 1 TRANSCUTANEOUS: ( VENTRICULAR pacing only) Through the skin via gel electrode pads placed on the chest and back. Disadvantage:
TEMPORARY PACEMAKERS HINTS ( DUAL CHAMBER 5392 PACER) TYPES OF PACERS 2018 1 TRANSCUTANEOUS: ( VENTRICULAR pacing only) Through the skin via gel electrode pads placed on the chest and back. Disadvantage:
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS
 INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
INTERPRETING THE ECG IN PATIENTS WITH PACEMAKERS BEFORE INTERPRETING THE ECG: Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS. Cardiology San Francisco General Hospital UCSF Disclosures: None 1 2 QUESTIONS
MODEL EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER
 MODEL 53401 EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER In-service Guide 53401 TRAINING LEARNING OBJECTIVES Identify the control knobs and be able to explain how to use them to program device. Distinguish
MODEL 53401 EPG SINGLE CHAMBER TEMPORARY EXTERNAL PACEMAKER In-service Guide 53401 TRAINING LEARNING OBJECTIVES Identify the control knobs and be able to explain how to use them to program device. Distinguish
The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node.
 PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
PACEMAKER Natural pacemaker: The heart's "natural" pacemaker is called the sinoatrial (SA) node or sinus node. Artificial pacemaker: It is a small, battery-operated device that helps the heart beat in
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 10: Pacemaker Rhythms and Bundle Branch Block Learning Outcomes 10.1 Describe the various pacemaker rhythms. 10.2
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital
 Treatment Bradyarrhythmia Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital 1 What is the rhythm? Sinus Bradycardia What s rhythm Sinus Bradycardia Treatment Asymptomatic No treatment
Treatment Bradyarrhythmia Ass. Prof. Tomon Thongsri, MD Buddhachinaraj Phitsanuloke Hospital 1 What is the rhythm? Sinus Bradycardia What s rhythm Sinus Bradycardia Treatment Asymptomatic No treatment
Review of Pacemakers and ICD Therapy: Overview and Patient Management
 Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
Review of Pacemakers and ICD Therapy: Overview and Patient Management Pacing Systems Charles J. Love, MD FACC FAHA FHRS CCDS Professor of Medicine Director, Cardiac Rhythm Device Services OSU Division
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
Contents. Example: Pacemaker in DDD Mode. I. Introduction II. Website and Relevant Documents III. Background Information IV.
 Contents I. Introduction II. Website and Relevant Documents III. Background Information IV. Pacemaker System V. i. Components ii. Operating Modes iii. Parameters Example: Pacemaker in DDD Mode Pacemaker
Contents I. Introduction II. Website and Relevant Documents III. Background Information IV. Pacemaker System V. i. Components ii. Operating Modes iii. Parameters Example: Pacemaker in DDD Mode Pacemaker
Is This Thing Working?
 Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Is This *#@!* Thing Working? Pacemaker (and ICD) ECG and Telemetry Pitfalls Wayne O. Adkisson, MD adki0004@umn.edu Disclosures I currently receive research support from Medtronic, Inc. I have been compensated
Chapter 80 Implantable Cardiac Devices
 Chapter 80 Implantable Cardiac Devices Episode Overview: 1. List 5 Indications for permanent pacing 2. Pacemaker nomenclature - what do the 5 letters mean a. What are common Pacemaker types? 3. List the
Chapter 80 Implantable Cardiac Devices Episode Overview: 1. List 5 Indications for permanent pacing 2. Pacemaker nomenclature - what do the 5 letters mean a. What are common Pacemaker types? 3. List the
ICD: Basics, Programming and Trouble-shooting
 ICD: Basics, Programming and Trouble-shooting Amir AbdelWahab, MD Electrophysiology and Pacing Service Cardiology Department Cairo University Feb 2013 Evolution of ICD Technology ICD Evolution Indications
ICD: Basics, Programming and Trouble-shooting Amir AbdelWahab, MD Electrophysiology and Pacing Service Cardiology Department Cairo University Feb 2013 Evolution of ICD Technology ICD Evolution Indications
MEDTRONIC CARELINK NETWORK FOR PACEMAKERS. Comparison between the Medtronic CareLink Network for Pacemakers and Transtelephonic Monitoring
 MEDTRONIC CARELINK NETWORK FOR PACEMAKERS Comparison between the Medtronic CareLink Network for Pacemakers and Transtelephonic Monitoring Transtelephonic Monitoring Transmission What can you determine
MEDTRONIC CARELINK NETWORK FOR PACEMAKERS Comparison between the Medtronic CareLink Network for Pacemakers and Transtelephonic Monitoring Transtelephonic Monitoring Transmission What can you determine
Model 5392 EPG Temporary Pacer
 Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale
 Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Pacing and Device Jargon Made Simple. Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital
 Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Pacing and Device Jargon Made Simple Dr Jonathan Timperley MB ChB MD FRCP Consultant Cardiologist Northampton General Hospital Disclosure Dr Jonathan Timperley Honorarium from Bayer Arne Larson (1915
Temporary Pacemakers
 07 Part I Anaesthesia Refresher Course 2018 University of Cape Town Dr Owen Porrill Private Practice Honorary lecturer- University of Cape Town Temporary pacemakers are usually inserted as part of the
07 Part I Anaesthesia Refresher Course 2018 University of Cape Town Dr Owen Porrill Private Practice Honorary lecturer- University of Cape Town Temporary pacemakers are usually inserted as part of the
Implant Procedure Concepts
 1 4 7 2 5 LV Lead 8 3 6 Implant Procedure Concepts 9 ICD and CRT LV Lead This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is
1 4 7 2 5 LV Lead 8 3 6 Implant Procedure Concepts 9 ICD and CRT LV Lead This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is
Sinus rhythm with premature atrial beats 2 and 6 (see Lead II).
 Cardiac Pacemaker Premature Beats When one of ectopic foci becomes irritable, it may spontaneously fire, leading to one or more premature beats. Atrial and junctional foci may become irritable from excess
Cardiac Pacemaker Premature Beats When one of ectopic foci becomes irritable, it may spontaneously fire, leading to one or more premature beats. Atrial and junctional foci may become irritable from excess
Cardiac Assist Devices. Wayne E. Ellis, Ph.D., CRNA
 Cardiac Assist Devices Wayne E. Ellis, Ph.D., CRNA Types Pacemakers AICDs VADs 2 History First pacemaker implanted in 1958 First ICD implanted in 1980 Greater than 500,000 patients in the US population
Cardiac Assist Devices Wayne E. Ellis, Ph.D., CRNA Types Pacemakers AICDs VADs 2 History First pacemaker implanted in 1958 First ICD implanted in 1980 Greater than 500,000 patients in the US population
Project Title Temporary Pacemaker Training Simulator
 Project Title Temporary Pacemaker Training Simulator Project Description Problem: There is no available training device for temporary pacemakers (pacemakers). A training device will have to essentially
Project Title Temporary Pacemaker Training Simulator Project Description Problem: There is no available training device for temporary pacemakers (pacemakers). A training device will have to essentially
PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II
 1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II 2012 Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 ADDITIVES IN DEVICE THERAPY Key Choice / CNEA 1 Adaptive Rate
1 PACEMAKER INTERPRETATION AND DEVICE MANAGEMENT PART II 2012 Cynthia Webner DNP, RN, CCNS, CCRN-CMC Karen Marzlin DNP, RN, CCNS, CCRN-CMC 2 ADDITIVES IN DEVICE THERAPY Key Choice / CNEA 1 Adaptive Rate
Pacemakers 12/04. Pacemakers. 1. What is a pacemaker?
 Pacemakers 12/04 1-What is a pacemaker? 2- What does intrinsic mean? 3- How exactly do pacemakers work on the heart? 4- What are the parts of a pacemaker? 5- Are there different kinds of pacemakers? 6-
Pacemakers 12/04 1-What is a pacemaker? 2- What does intrinsic mean? 3- How exactly do pacemakers work on the heart? 4- What are the parts of a pacemaker? 5- Are there different kinds of pacemakers? 6-
Intermittent episodes of paced tachycardia: what is the cause?
 Intermittent episodes of paced tachycardia: what is the cause? Lindsey Parkinson and Lucy Broadhurst, Rotherham NHS Foundation Trust Contact: Lindsey.Parkinson@rothgen.nhs.uk Introduction A hospital in-patient
Intermittent episodes of paced tachycardia: what is the cause? Lindsey Parkinson and Lucy Broadhurst, Rotherham NHS Foundation Trust Contact: Lindsey.Parkinson@rothgen.nhs.uk Introduction A hospital in-patient
The Cardiac Pacemaker Case Study and its implementation in Safety-Critical Java and Ravenscar Ada
 The Cardiac Pacemaker Case Study and its implementation in Safety-Critical Java and Ravenscar Ada Neeraj Kumar Singh, Andy Wellings, Ana Cavalcanti University of York, United Kingdom JTRES, 24-26 October
The Cardiac Pacemaker Case Study and its implementation in Safety-Critical Java and Ravenscar Ada Neeraj Kumar Singh, Andy Wellings, Ana Cavalcanti University of York, United Kingdom JTRES, 24-26 October
Pacemaker Concepts and Terminology*
 Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
Pacemaker Concepts and Terminology* BAROUH V BERKOVITS, E.E., Ing. Associate in Surgery, Harvard Medical School, Boston, Mass., Associate in Electrophysiology, Miami University, Miami, Fla., Senior Research
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS
 PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
PERIOPERATIVE MANAGEMENT: CARDIAC PACEMAKERS AND DEFIBRILLATORS DR SUSAN CORCORAN CARDIOLOGIST ONCE UPON A TIME.. Single chamber pacemakers Programmed at 70/min VVI 70 UNIPOLAR SYSTEMS A Unipolar Pacing
Size (mm) (H W D) Mass (g) Volume (cc)
 The FORMIO pacing system from Boston Scientific provides an ImageReady * MR conditional pacing system. FORMIO offers RightRate the newest generation of MV sensor technology, and the only MV sensor clinically
The FORMIO pacing system from Boston Scientific provides an ImageReady * MR conditional pacing system. FORMIO offers RightRate the newest generation of MV sensor technology, and the only MV sensor clinically
Essentials of Pacemakers and ICD s. Rajesh Banker, MD, MPH
 Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Pacing Lead Implant Testing. Document Identifier
 Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
Pacing Lead Implant Testing 1 Objectives Upon completion of this presentation, the participant should be able to: Name the two primary surgical options for implanting pacing leads Describe three significant
Advanced ICD Concepts
 1 4 2 5 7 3 6 8 Advanced ICD Concepts This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is subject to FDA regulations. This presentation
1 4 2 5 7 3 6 8 Advanced ICD Concepts This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is subject to FDA regulations. This presentation
Need to Know: Implantable Devices. Carolyn Brown RN, MN, CCRN Education Coordinator Emory Healthcare Atlanta, Georgia
 Need to Know: Implantable Devices Carolyn Brown RN, MN, CCRN Education Coordinator Emory Healthcare Atlanta, Georgia Disclosure Statement I have no relationships to disclose. Objectives Discuss the most
Need to Know: Implantable Devices Carolyn Brown RN, MN, CCRN Education Coordinator Emory Healthcare Atlanta, Georgia Disclosure Statement I have no relationships to disclose. Objectives Discuss the most
Title and contents page 1 Who should read this document 2 Scope of the Guideline 2 Background 2 What is new in this version 2
 Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
Temporary Transvenous Pacing Guideline Classification: Clinical Guideline Lead Author: Dr Peter Woolfson Additional author(s): Dr Alan Fitchet Sister Joanne Hughes, Matron Julie Winstanley Authors Division:
Review Packet EKG Competency This packet is a review of the information you will need to know for the proctored EKG competency test.
 Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
BEDSIDE ECG INTERPRETATION
 BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
Temporary pacemaker : Programming &Trouble shooting
 2015 춘계심장학회 Temporary pacemaker : Programming &Trouble shooting 서울아산병원 한두영 Temporary Pacemaker Overview Indication of Temporary Pacemaker Programming ; NBG Code, Pacing/Sensing Device Trouble shooting
2015 춘계심장학회 Temporary pacemaker : Programming &Trouble shooting 서울아산병원 한두영 Temporary Pacemaker Overview Indication of Temporary Pacemaker Programming ; NBG Code, Pacing/Sensing Device Trouble shooting
TIP CARD. Model Temporary External Pacemaker
 TIP CARD Model 5392 Temporary External Pacemaker PRE-USE What to do... What NOT to do... Battery Replace the battery for each new patient. Do NOT reuse battery. Physical Check case for cracks/damage.**
TIP CARD Model 5392 Temporary External Pacemaker PRE-USE What to do... What NOT to do... Battery Replace the battery for each new patient. Do NOT reuse battery. Physical Check case for cracks/damage.**
Supplemental Material
 Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Practice Questions.
 IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
IBHRE Prep Practice Questions Question 1 The relative refractory yperiod of the ventricular myocardium corresponds to which of the following phases of the action potential? A. (0) B. (1) C. (2) D. (3)
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University. OBHG Education Subcommittee
 -RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
Cardiac Pacing. Learning outcomes. Introduction. The cardiac impulse - its formation and its failure CHAPTER. To understand:
 Cardiac Pacing CHAPTER 10 Learning outcomes To understand: The indications for cardiac pacing in the peri-arrest setting How to perform percussion pacing How to apply non-invasive, transcutaneous electrical
Cardiac Pacing CHAPTER 10 Learning outcomes To understand: The indications for cardiac pacing in the peri-arrest setting How to perform percussion pacing How to apply non-invasive, transcutaneous electrical
ECG Interpretation. Introduction to Cardiac Telemetry. Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services
 ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
ECG Interpretation Introduction to Cardiac Telemetry Michael Peters, RN, CCRN, CFRN CALSTAR Air Medical Services Disclosures Nothing to disclose Objectives Describe the electrical conduction pathway in
Answer: The electrical current has difficulty traveling down the normal conduction pathway.
 1 Electrocardiography for Healthcare Professionals Chapter 8: Heart Block Dysrhythmias 2 3 4 5 6 Learning Outcomes 8.1 Describe the various heartblock dysrhythmias 8.2 Identify first degree heartblock
1 Electrocardiography for Healthcare Professionals Chapter 8: Heart Block Dysrhythmias 2 3 4 5 6 Learning Outcomes 8.1 Describe the various heartblock dysrhythmias 8.2 Identify first degree heartblock
2017 BDKA Review. Regularity Rate P waves PRI QRS Interpretation. Regularity Rate P waves PRI QRS Interpretation 1/1/2017
 1. 2017 BDKA Review 2. 3. 4. Interpretation 5. QT 6. 7. 8. 9. 10. QT 11. 12. 13. 14. 15. 16. 17. 18. QT 19. 20. QT 21. 22. QT 23. 24. Where are pacer spikes? Before the P wave or before the QRS complex?
1. 2017 BDKA Review 2. 3. 4. Interpretation 5. QT 6. 7. 8. 9. 10. QT 11. 12. 13. 14. 15. 16. 17. 18. QT 19. 20. QT 21. 22. QT 23. 24. Where are pacer spikes? Before the P wave or before the QRS complex?
Newer pacemakers also can monitor your blood temperature, breathing, and other factors and adjust your heart rate to changes in your activity.
 Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
Timothy Graham, M.D. Case Western Reserve University School of Medicine University Hospitals Case Medical Center Cleveland, Ohio
 Perioperative Management of Pacemakers and Implantable Cardioverter-Defibrillators Timothy Graham, M.D. Case Western Reserve University School of Medicine University Hospitals Case Medical Center Cleveland,
Perioperative Management of Pacemakers and Implantable Cardioverter-Defibrillators Timothy Graham, M.D. Case Western Reserve University School of Medicine University Hospitals Case Medical Center Cleveland,
You have a what, inside you?
 Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
The Nuts and Bolts of ICD Therapy
 Electrical Management of Cardiac Rhythm Disorders For Cardiology Fellows December 5-8 Austin, Texas The Nuts and Bolts of ICD Therapy 1 2 Action Potential Localized Differences in Conduction Conduction
Electrical Management of Cardiac Rhythm Disorders For Cardiology Fellows December 5-8 Austin, Texas The Nuts and Bolts of ICD Therapy 1 2 Action Potential Localized Differences in Conduction Conduction
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
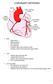 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
You have a what, inside you?
 Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
DEFIBRILLATORS. Prof. Yasser Mostafa Kadah
 DEFIBRILLATORS Prof. Yasser Mostafa Kadah Basics Defibrillation is definitive treatment for life-threatening cardiac arrhythmias such as ventricular fibrillation Defibrillation consists of delivering therapeutic
DEFIBRILLATORS Prof. Yasser Mostafa Kadah Basics Defibrillation is definitive treatment for life-threatening cardiac arrhythmias such as ventricular fibrillation Defibrillation consists of delivering therapeutic
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
12 th International Winter Arrhythmia School Collingwood, Ontario February 7, Dr. Derek Yung. MD, FRCPC
 12 th International Winter Arrhythmia School Collingwood, Ontario February 7, 2015 Dr. Derek Yung. MD, FRCPC Presenter: Dr. Derek Yung Relationships with industry: Educational material provided by Biotronik,
12 th International Winter Arrhythmia School Collingwood, Ontario February 7, 2015 Dr. Derek Yung. MD, FRCPC Presenter: Dr. Derek Yung Relationships with industry: Educational material provided by Biotronik,
SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000. SJM-EDTR Item approved for U.S. use only.
 SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000 1 APPROVED MRI SCAN CONDITIONS 1.5 TESLA FULL BODY 2 SETUP SJM MRI ACTIVATOR HANDHELD DEVICE The SJM MRI Activator handheld device must be enabled
SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000 1 APPROVED MRI SCAN CONDITIONS 1.5 TESLA FULL BODY 2 SETUP SJM MRI ACTIVATOR HANDHELD DEVICE The SJM MRI Activator handheld device must be enabled
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS
 NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
CONSULTA CRT-P Model C4TR01
 CONSULTA CRT-P Model C4TR01 Physical characteristics Volume a 15 cm 3 Mass H x W x D Surface area of titanium device can Surface area of each titanium nitride LECG electrode Radiopaque ID Materials in
CONSULTA CRT-P Model C4TR01 Physical characteristics Volume a 15 cm 3 Mass H x W x D Surface area of titanium device can Surface area of each titanium nitride LECG electrode Radiopaque ID Materials in
Antibradycardia Pacemakers
 #90802 Antibradycardia Pacemakers COURSE #90802 15 CONTACT HOURS/CREDITS Release Date: 09/01/17 Expiration Date: 08/31/20 Antibradycardia Pacemakers HOW TO RECEIVE CREDIT Read the enclosed course. Complete
#90802 Antibradycardia Pacemakers COURSE #90802 15 CONTACT HOURS/CREDITS Release Date: 09/01/17 Expiration Date: 08/31/20 Antibradycardia Pacemakers HOW TO RECEIVE CREDIT Read the enclosed course. Complete
Specified Tolerance (ms)
 SigmaPace TM 1000: Medtronic Temporary External Pacemaker Model 5388 Checkout Procedure 1. PRELIMINARY SET UP a. Connect the pacemaker output to the analyzer s ATRIAL and VENTRICULAR 4 mm interface jacks
SigmaPace TM 1000: Medtronic Temporary External Pacemaker Model 5388 Checkout Procedure 1. PRELIMINARY SET UP a. Connect the pacemaker output to the analyzer s ATRIAL and VENTRICULAR 4 mm interface jacks
EnTrust D154VRC Single Chamber ICD 35J delivered 8 seconds BOL, 11.8 seconds ERI 10.7 years**** 35cc, 68g Programmable Active Can
 EnTrust D154ATG Dual Chamber ICD 35J delivered 8 seconds BOL, 11 seconds ERI 7.7 years** 35cc***, 68g Programmable Active Can EnTrust D154VRC Single Chamber ICD 35J delivered 8 seconds BOL, 11.8 seconds
EnTrust D154ATG Dual Chamber ICD 35J delivered 8 seconds BOL, 11 seconds ERI 7.7 years** 35cc***, 68g Programmable Active Can EnTrust D154VRC Single Chamber ICD 35J delivered 8 seconds BOL, 11.8 seconds
Course Objectives. Proper Lead Placements. Review the ECG print paper. Review the mechanics of the Myocardium. Review basics of ECG Rhythms
 ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
PRACTICE advisories are systematically developed reports
 for the Perioperative Management of Patients with Cardiac Implantable Electronic Devices: Pacemakers and Implantable Cardioverter-Defibrillators An Updated Report by the American Society of Anesthesiologists
for the Perioperative Management of Patients with Cardiac Implantable Electronic Devices: Pacemakers and Implantable Cardioverter-Defibrillators An Updated Report by the American Society of Anesthesiologists
Supplementary Online Content
 Supplementary Online Content Tseng ZH, Hayward RM, Clark NM, et al. Sudden death in patients with cardiac implantable electronic devices. JAMA Intern Med. Published online June 22, 2015. doi:10.1001/jamainternmed.2015.2641.
Supplementary Online Content Tseng ZH, Hayward RM, Clark NM, et al. Sudden death in patients with cardiac implantable electronic devices. JAMA Intern Med. Published online June 22, 2015. doi:10.1001/jamainternmed.2015.2641.
09/05/2018. True/False: All pacemakers have defibrillation capabilities.
 Paul G. Tarasi M.D. Staff Anesthesiologist Allegheny Health Network Adjunct Clinical Assistant Professor of Anesthesiology Temple University School of Medicine Describe different types of implanted cardiac
Paul G. Tarasi M.D. Staff Anesthesiologist Allegheny Health Network Adjunct Clinical Assistant Professor of Anesthesiology Temple University School of Medicine Describe different types of implanted cardiac
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
Biventricular Pacemakers Sensing
 Biventricular Pacemakers Sensing Sergio Dubner Director Arrhythmias and Electrophisiology Service, Clinica y Maternidad Suizo-Argentina, Buenos Aires, Argentina Left ventricular pacemaker lead technology
Biventricular Pacemakers Sensing Sergio Dubner Director Arrhythmias and Electrophisiology Service, Clinica y Maternidad Suizo-Argentina, Buenos Aires, Argentina Left ventricular pacemaker lead technology
8/20/2012. Learning Outcomes (Cont d)
 1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
CORONARY ARTERIES HEART
 CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
CARDIAC/ECG MODULE THE HEART CORONARY ARTERIES FIBRILLATING HEART CORONARY ARTERIES HEART PRACTICE RHYTHMS PRACTICE RHYTHMS ELECTRICAL CONDUCTION SA Node (60 100) Primary pacemaker AV Node (40 60) ***Creates
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE. Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology
 PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
12/1/2010. Human Heart. CS5219 Term Project Pacemaker: Modeling and Verification. Natural Pacemaker. Bradycardia
 CS5219 Term Project Pacemaker: Modeling and Verication Human Heart Lecturer: Abhik Roychoudhury TA: Lei JU National Univ. of Singapore For more questions about the requirements document, contact julei@comp.nus.edu.sg
CS5219 Term Project Pacemaker: Modeling and Verication Human Heart Lecturer: Abhik Roychoudhury TA: Lei JU National Univ. of Singapore For more questions about the requirements document, contact julei@comp.nus.edu.sg
Manual Defibrillators, Automatic External Defibrillators, Cardioversion, and External Pacing. D. J. McMahon cewood rev
 Manual Defibrillators, Automatic External Defibrillators, Cardioversion, and External Pacing D. J. McMahon 141001 cewood rev 2017-10-04 Key Points Defibrillators: - know the definition & electrical value
Manual Defibrillators, Automatic External Defibrillators, Cardioversion, and External Pacing D. J. McMahon 141001 cewood rev 2017-10-04 Key Points Defibrillators: - know the definition & electrical value
A Rare Type of Pacemaker Mediated Tachycardia
 A Rare Type of Pacemaker Mediated Tachycardia Serkan ÇAY M.D., Ümit GÜRAY M.D., Cihan DEMİR M.D. Yuksek Ihtisas Heart-Education and Research Hospital, Department of Cardiology, Ankara, Turkey ABSTRACT
A Rare Type of Pacemaker Mediated Tachycardia Serkan ÇAY M.D., Ümit GÜRAY M.D., Cihan DEMİR M.D. Yuksek Ihtisas Heart-Education and Research Hospital, Department of Cardiology, Ankara, Turkey ABSTRACT
Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator ; Phillips MRX SOP Dr Randal McRoberts
 Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator
Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Transcutaneous Pacing on Zoll Defibrillator Version 4 Related Documents SOP-Zoll defibrillator
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
11/21/18. EKG Pop Quiz. Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants
 EKG Pop Quiz Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants 1 Disclosures No financial relationships to disclose. EKG #1 75 y/o woman with a dual-chamber pacemaker
EKG Pop Quiz Michael Giocondo, MD Cardiac Electrophysiology Saint Luke s Cardiovascular Consultants 1 Disclosures No financial relationships to disclose. EKG #1 75 y/o woman with a dual-chamber pacemaker
MONITORING PATIENTS WITH A TEMPORARY EXTERNAL EPICARDIAL PACEMAKER PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES
 PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
PURPOSE Guidelines for caring for and monitoring patients with a temporary external epicardial pacemaker. Epicardial pacemaker monitoring is performed on a continuous basis by a nurse to evaluate the effectiveness
Dual Chamber Temporary External Pacemaker
 5392 Dual Chamber Temporary External Pacemaker Technical Manual Caution: Federal law (USA) restricts this device to sale by or on the order of a physician. The following list includes trademarks or registered
5392 Dual Chamber Temporary External Pacemaker Technical Manual Caution: Federal law (USA) restricts this device to sale by or on the order of a physician. The following list includes trademarks or registered
Friedman, Rott, Wokhlu, Asirvatham, Hayes 201. Figure 65.7 Shortening of the AV interval during pacing.
 Friedman, Rott, Wokhlu, Asirvatham, Hayes 201 Figure.7 Shortening of the AV interval during pacing. 202 A Case-Based Approach to Pacemakers, ICDs, and Cardiac Resynchronization Figure.8 is obtained from
Friedman, Rott, Wokhlu, Asirvatham, Hayes 201 Figure.7 Shortening of the AV interval during pacing. 202 A Case-Based Approach to Pacemakers, ICDs, and Cardiac Resynchronization Figure.8 is obtained from
Programming of Bradycardic Parameters. C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany
 Programming of Bradycardic Parameters C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany Carsten.Israel@evkb.de Programming of ICD Brady Parameters Conflict of Interest Biotronik
Programming of Bradycardic Parameters C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany Carsten.Israel@evkb.de Programming of ICD Brady Parameters Conflict of Interest Biotronik
Troubleshooting ICD. NASPE Training Lancashire & South Cumbria Cardiac Network
 Troubleshooting ICD NASPE Training Lancashire & South Cumbria Cardiac Network Bradycardia Pacing by ICD Isolated ICD discharge Multiple discharges Appropriate Inappropriate No ICD Therapy or delay in ICD
Troubleshooting ICD NASPE Training Lancashire & South Cumbria Cardiac Network Bradycardia Pacing by ICD Isolated ICD discharge Multiple discharges Appropriate Inappropriate No ICD Therapy or delay in ICD
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
Arrhythmias. Pulmonary Artery
 Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
FRONTIER II. User s Manual. Model 5586 Model Biventricular Cardiac Resynchronization Device with AF Suppression Algorithm
 FRONTIER II Model 5586 Model 5596 Biventricular Cardiac Resynchronization Device with AF Suppression Algorithm User s Manual Unless otherwise noted, indicates that the name is a trademark of, or licensed
FRONTIER II Model 5586 Model 5596 Biventricular Cardiac Resynchronization Device with AF Suppression Algorithm User s Manual Unless otherwise noted, indicates that the name is a trademark of, or licensed
856 Unintentional Deactivation of ICDs Mayo Clin Proc, August 2002, Vol 77 Figure 1. Case 3. Printout from Guidant programmer (Guidant Corp, St Paul,
 Mayo Clin Proc, August 2002, Vol 77 Unintentional Deactivation of ICDs 855 Case Report Unintentional Deactivation of Implantable Cardioverter-Defibrillators in Health Care Settings MARY JANE RASMUSSEN,
Mayo Clin Proc, August 2002, Vol 77 Unintentional Deactivation of ICDs 855 Case Report Unintentional Deactivation of Implantable Cardioverter-Defibrillators in Health Care Settings MARY JANE RASMUSSEN,
DEFIBRILLATORS ATRIAL AND VENTRICULAR FIBRILLATION
 1 DEFIBRILLATORS The two atria contract together and pump blood through the valves into the two ventricles, when the action potentials spread rapidly across the atria surface. After a critical time delay,
1 DEFIBRILLATORS The two atria contract together and pump blood through the valves into the two ventricles, when the action potentials spread rapidly across the atria surface. After a critical time delay,
ISO INTERNATIONAL STANDARD. Implants for surgery Active implantable medical devices Part 2: Cardiac pacemakers
 INTERNATIONAL STANDARD ISO 14708-2 Second edition 2012-08-15 Implants for surgery Active implantable medical devices Part 2: Cardiac pacemakers Implants chirurgicaux Dispositifs médicaux implantables actifs
INTERNATIONAL STANDARD ISO 14708-2 Second edition 2012-08-15 Implants for surgery Active implantable medical devices Part 2: Cardiac pacemakers Implants chirurgicaux Dispositifs médicaux implantables actifs
