S PECIAL A RTICLE. Combination Antiplatelet Therapy: Implications for Pharmacists
|
|
|
- Charity Hudson
- 6 years ago
- Views:
Transcription
1 S PECIAL A RTICLE Combination Antiplatelet Therapy: Implications for Pharmacists Robert L. Talbert, Pharm.D., FCCP, Sarah A. Spinler, Pharm.D., FCCP, Jean M. Nappi, Pharm.D., FCCP, and Michael B. Bottorff, Pharm.D., FCCP Objectives. To present two case reports of patients who received suboptimal oral antiplatelet therapy and to review recent changes in national guidelines for management of acute coronary syndromes. Data Sources. Personal observation by the authors, and clinical practice guidelines and related clinical trials of the American Heart Association and the American College of Cardiology. Summary. The American College of Cardiology and the American Heart Association revised the guidelines for administration of antiplatelet and anticoagulant therapy in patients with unstable angina and non ST-segment elevation myocardial infarction in March Two cases observed by the authors illustrate the consequences of suboptimal antiplatelet therapy when a combination of two antiplatelet drugs should have been administered. Conclusion. Evidence from recent randomized controlled trials led to changes in the national guidelines for administration of oral antiplatelet therapy in patients with acute coronary syndromes. Pharmacists should be aware of these changes and counsel patients about appropriate administration of antiplatelet drugs. (Pharmacotherapy 2002;22(10): ) The following two case reports involving patients who received suboptimal antiplatelet therapy point out disparities between national guidelines and actual clinical practice that led to undesirable consequences in both patients. Case Reports Patient No. 1 A 61-year-old African-American man with a From the College of Pharmacy, University of Texas, and the Departments of Medicine and Pharmacology, University of Texas Health Science Center, San Antonio, Texas (Dr. Talbert); the Philadelphia College of Pharmacy, University of the Sciences in Philadelphia, Philadelphia, Pennsylvania (Dr. Spinler); the College of Pharmacy, Medical University of South Carolina, Charleston, South Carolina (Dr. Nappi); and the College of Pharmacy, University of Cincinnati, Cincinnati, Ohio (Dr. Bottorff). Address reprint requests to Robert L. Talbert, Pharm.D., Clinical Pharmacy Program, University of Texas Health Science Center at San Antonio, 7703 Floyd Curl Drive, San Antonio, TX ; talbert@uthscsa.edu. history of coronary artery disease, hypertension, diabetes mellitus type 2, and a left ventricular ejection fraction of 35% based on echocardiography was admitted to the hospital with progressing angina 2 months after the echocardiogram was obtained. He underwent percutaneous coronary intervention, with stents placed in the right coronary and circumflex arteries. He was discharged the next day with the following drug regimen: aspirin 325 mg/day, carvedilol mg twice/day, glyburide 10 mg twice/day, hydrochlorothiazide 25 mg/day, and clopidogrel loading dose 300 mg once, then 75 mg/day. Eleven days after discharge, the patient s wife found him on the floor, and he was taken to the emergency department. His blood pressure was 110/50 mm Hg, pulse 80 beats/minute. He was afebrile. An electrocardiogram revealed ST depression in V2 V5, with T-wave inversion in V5 V6. The first set of cardiac biomarkers revealed a creatine kinase level of 3445 IU/L
2 1212 PHARMACOTHERAPY Volume 22, Number 10, 2002 (normal IU/L), with an MB fraction of 7.5% (normal < 5%) and a troponin T level of 8.86 ng/ml (normal < 0.2 ng/ml). Other pertinent laboratory test results were white blood cell count 23.6 x 10 3 /mm 3, hematocrit 28.8%, hemoglobin 9.6 g/dl, platelets 357 x 10 3 /mm 3, sodium 133 meq/l, potassium 4.4 meq/l, chloride 92 meq/l, bicarbonate 24 meq/l, glucose 263 mg/dl, blood urea nitrogen 24 mg/dl, and serum creatinine 2 mg/dl. The patient was taken to the cardiac catheterization laboratory, and angiography revealed total occlusion of both stents, which were subsequently restented. He received heparin, eptifibitide, and intravenous nitroglycerin. An interview with the patient s wife revealed that the patient never filled his prescription for the clopidogrel; he and his wife considered it unnecessary and expensive. The assessment was acute non ST-segment myocardial infarction secondary to acute stent closure resulting from inadequate antiplatelet therapy. The plan consisted of restenting, administering eptifibitide, and restarting aspirin plus clopidogrel. The patient was discharged 3 days later, with a drug regimen consisting of isosorbide dinitrate 10 mg 3 times/day, hydralazine 10 mg 4 times/day, carvedilol 6.25 mg twice/day, aspirin 325 mg/day, clopidogrel 75 mg/day, and insulin. Patient No. 2 A 42-year-old Caucasian woman with a history of coronary artery disease had received multiple interventions, such as left anterior coronary artery stent placement. She underwent percutaneous coronary intervention of in-stent restenosis. She came to the emergency department approximately 6 weeks later after awakening with crushing substernal chest pain. The pain radiated to both arms and was accompanied by shortness of breath, diaphoresis, nausea, and lightheadedness. She rated her pain, which was similar to her previous anginal pain, as 9 on a scale of Her medical history was significant for hypertension, hyperlipidemia, cigarette smoking, coronary artery disease (stent placements in the right coronary artery 5 years earlier and left anterior descending coronary artery within the last year, in addition to the percutaneous coronary intervention described above). Her ejection fraction according to echocardiography performed about 2 months earlier was 40%. Family history revealed that her mother had experienced an acute myocardial infarction at age 54, and her father had coronary artery disease and hypertension. The patient had once smoked 50 packs/year but had not smoked for over a year and consumed no ethanol; she was married and unemployed at the time. On admission to the hospital, the patient s drug regimen consisted of aspirin 325 mg/day, atorvastatin 10 mg/day, metoprolol 50 mg twice/day, benazepril 40 mg/day, and clopidogrel 75 mg/day for 4 weeks after her stent 2 months earlier and after her percutaneous coronary intervention a month after that. Physical examination indicated that she was hemodynamically stable; her blood pressure was 118/82 mm Hg, heart rate 72 beats/minute, with no respiratory distress. Cardiovascular examination revealed a regular rate and rhythm without murmur, rubs, or gallops. She had normal S 1 and S 2 heart sounds, no jugular venous distention, clear lungs, and no edema. Electrocardiography revealed ST elevation of 3 mm in the anterior leads with reciprocal changes in the inferior leads. Initial laboratory test results were normal. In the emergency department she received aspirin, heparin, nitroglycerin, and morphine. She continued to experience substernal chest pain with ST elevation, and preparations were made to take her to the catheterization laboratory immediately for diagnostic left heart catheterization and possible coronary intervention. Left heart catheterization revealed that her left main, right, and circumflex coronary arteries were angiographically normal, but the left anterior descending coronary artery had a 100% stenosis proximally. Percutaneous coronary intervention of the left anterior descending coronary artery was performed, with new stents placed proximal and distal to the previous stent. The patient received tirofiban for 24 hours after the procedure. No residual stenosis was noted. Clopidogrel and aspirin were restarted without complications, and the plan was to continue administering both antiplatelet agents indefinitely. The assessment was that the patient was experiencing repeated episodes of myocardial ischemia and infarction, and that inconsistent clopidogrel therapy as well as possible resistance to aspirin may have been contributing to her unstable course. Discussion Changes in the American College of Cardiology and American Heart Association Guidelines The American College of Cardiology and the
3 COMBINATION ANTIPLATELET THERAPY Talbert et al 1213 Table 1. American College of Cardiology and American Heart Association Guidelines for Administration of Antiplatelet and Anticoagulant Therapy in Patients with Unstable Angina and Non ST-Segment Elevation Myocardial Infarction (revised March 2002) Level of Evidence Class Recommendation A I Antiplatelet therapy should be started promptly. Aspirin should be administered as soon as possible after patient s condition is identified and continued indefinitely. A/B I In hospitalized patients for whom an early noninterventional approach is planned, clopidogrel should be added to aspirin as soon as possible after admission and administered for at least 1 month (A) and up to 9 months (B). A/B I In patients for whom percutaneous coronary intervention is planned, clopidogrel should be started and continued for at least 1 month (A) and up to 9 months in patients who are not at high risk for bleeding (B). B I For patients taking clopidogrel and for whom coronary artery bypass graft surgery is planned, the drug should be withheld, if possible, for at least 5 and preferably 7 days. A I Anticoagulation with subcutaneous low-molecular-weight heparin or intravenous unfractionated heparin should be added to antiplatelet therapy with aspirin and/or clopidogrel (A). A I A platelet glycoprotein IIb-IIIa antagonist should be administered in addition to aspirin and heparin to patients in whom catheterization and percutaneous coronary intervention are planned. The glycoprotein IIb-IIIa antagonist also may be administered just before the percutaneous coronary intervention (A). A I Aspirin mg/day (in the absence of contraindications) should be administered. A I Clopidogrel 75 mg/day (in the absence of contraindications) should be administered when aspirin is not tolerated because of hypersensitivity or gastrointestinal intolerance. B I The combination of aspirin and clopidogrel should be administered for 9 months after unstable angina and non ST-segment elevation myocardial infarction. B I For long-term medical therapy, the combination of aspirin and clopidogrel is recommended for 9 months after unstable angina and non ST-segment elevation myocardial infarction. American Heart Association revised the guidelines for administration of antiplatelet and anticoagulant therapy for unstable angina and non ST-segment elevation myocardial infarction in March The guidelines incorporate a system of classifying the level of benefit and evidence based on randomized controlled trials. Briefly, the system ranks evidence into three levels (Table 1): A the highest class, in which data are derived from many randomized controlled trials involving large numbers of patients; B intermediate, in which data are derived from a limited number of trials involving comparatively small numbers of patients or from well-conceived data analyses of nonrandomized studies or observational data registries; and C the lowest class, in which the consensus of expert opinion is the primary source of information. Usually, this source is used only when data from randomized controlled trials are not available. The system incorporates the levels of evidence into three classes of recommendations: class I conditions for which there is evidence and/or general agreement that a given procedure or treatment is beneficial, useful, and effective; class II conditions for which conflicting evidence and/or a divergence of opinion exists regarding the usefulness or efficacy of a procedure or treatment; class IIA in which weight of evidence or opinion is in favor of usefulness or efficacy; class IIB in which usefulness or efficacy is less well established by evidence or opinion; class III conditions exist for which evidence and/or general agreement indicate that a procedure or treatment is not useful or effective and in some cases may be harmful. Major changes in the new guidelines from the original published guidelines 2 of 2000 are as follows: 1. Rather than specifying a thienopyridine, the revised guidelines recommend clopidogrel specifically. The rationale for this change is that clopidogrel has fewer adverse effects than ticlopidine (diarrhea, abdominal pain, nausea, vomiting, or neutropenia in approximately 2.4% of patients, severe neutropenia in 0.8% of patients, and, rarely, thrombotic thrombocytopenia purpura) and requires less monitoring. Clopidogrel also has a more rapid onset of activity than ticlopidine; however, in emergency situations a loading dose of 300 mg is often given.
4 1214 PHARMACOTHERAPY Volume 22, Number 10, Based on results of the Clopidogrel in Unstable Angina to Prevent Recurrent Ischemic Events (CURE) study, 3 it is recommended that clopidogrel be added to aspirin as soon as possible and administered for 1 9 months. Treatment for at least 1 month is strongly recommended, and up to 9 months based on average duration of treatment of patients with unstable angina to prevent recurrent ischemic events. This should not be interpreted to mean that benefit ceases after 9 months, but rather that data are limited beyond that time. 3. When percutaneous coronary intervention is planned, clopidogrel and aspirin should be given for at least 1 month and up to 9 months Because thienopyridines have a delayed onset and cessation of activity, they should be withheld for 5 7 days to minimize bleeding complications in patients for whom coronary artery bypass graft surgery is elective. 5. Anticoagulation, preferably with enoxaparin (IIA recommendation), should be administered with antiplatelet therapy with aspirin and/or clopidogrel, based on the Efficacy and Safety of Subcutaneous Enoxaparin in Non Qwave Events (ESSENCE) 5 study and other combination trials. Ensuring Administration of Optimal Treatment What should pharmacists do to ensure that patients receive optimal treatment with antiplatelet therapy for unstable angina and non ST-segment elevation myocardial infarction? In the inpatient setting, identifying a champion and a team of physicians, nurses, and pharmacists to lead the development of treatment algorithms and pathways would increase recognition of appropriate situations for administering combination antiplatelet therapy. All staff must understand that antiplatelet drugs work through different mechanisms, and that monotherapy with any agent is prone to failure in patients who are at high risk for developing unstable angina and non ST-segment elevation myocardial infarction and in patients undergoing percutaneous coronary intervention with stent placement. A set of standing orders would be a useful tool so that routine consideration of combination therapy would not overlooked. In the outpatient setting, comprehensive counseling by a pharmacist for all patients bringing prescriptions for an aspirin-clopidogrel combination would help minimize misunderstanding about potential deleterious interactions and emphasize the role for appropriate combinations. Patient counseling is imperative to enhance patient compliance and persistence with longterm regimens. Patients should understand some important points about combination oral antiplatelet therapy, as follows: 1. Combination antiplatelet therapy with aspirin and clopidogrel after percutaneous coronary intervention reduces the risk of recurrent myocardial infarction, hospitalization for angina, and need for additional procedures. This combination is safe and effective for up to 12 months. 2. The most common (~25%) symptoms occurring in patients taking clopidogrel are gastrointestinal, such as abdominal pain, dyspepsia, gastritis, and constipation; these symptoms occur about as frequently with aspirin. Combination therapy with aspirin and clopidogrel has to be discontinued in only about 2% of patients due to gastrointestinal adverse effects. 3. Rash and other skin disorders occur in up to 15% of patients taking clopidogrel, similar to the rate with aspirin. The effects on skin do not commonly lead to discontinuation of therapy. 4. Headache or dizziness led to discontinuation of combination therapy in 2 3% of patients in the CURE study The risk of major bleeding is increased with aspirin or clopidogrel; in combination, the major bleeding rate was 3.7% versus 2.7% with aspirin alone in the CURE study. 3 The risk for bleeding with clopidogrel increased with higher dosages of aspirin. 6. Low white blood cell counts (neutropenia or agranulocytosis) occur very rarely (2/9599 patients in the CURE study 3 ) with clopidogrel and are more common (0.8%) with ticlopidine, a closely related drug. No routine monitoring is required. Conclusion The two case reports presented here illustrate the consequences of suboptimal antiplatelet therapy when a combination of two antiplatelet drugs should have been administered. Also, evidence from recent randomized controlled trials led to changes in the national guidelines for administration of oral antiplatelet therapy in patients with acute coronary syndromes.
5 COMBINATION ANTIPLATELET THERAPY Talbert et al 1215 Pharmacists should be aware of these changes and counsel patients about appropriate administration of antiplatelet drugs. References 1. Braunwald E, Antman EM, Beasley JW, et al. ACC/AHA 2002 guideline update for the management of patients with unstable angina and non ST-segment elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association task force on practice guidelines (committee on the management of patients with unstable angina), Available from pdf. Accessed June 24, Braunwald E, Antman EM, Beasley JW, et al. ACC/AHA guidelines for the management of patients with unstable angina and non ST-segment elevation myocardial infarction: executive summary and recommendations: a report of the American College of Cardiology/American Heart Association task force on practice guidelines (committee on the management of patients with unstable angina). Circulation 2000;102: Yusuf S, Zhao F, Mehta SR, et al. Effects of clopidogrel in addition to aspirin in patients with acute coronary syndromes without ST-segment elevation: the clopidogrel in unstable angina to prevent recurrent events (CURE) trial investigators. N Engl J Med 2001;345: Mehta SR, Yusuf S, Peters RJ, et al. Effects of pretreatment with clopidogrel and aspirin followed by long-term therapy in patients undergoing percutaneous coronary intervention: the PCI-CURE study. Lancet 2001;358: Cohen M, Demers C, Gurfinkel EP, et al. A comparison of lowmolecular-weight heparin with unfractionated heparin for unstable coronary artery disease: efficacy and safety of subcutaneous enoxaparin in non Q-wave coronary events study group. N Engl J Med 1997;337:
Appendix: ACC/AHA and ESC practice guidelines
 Appendix: ACC/AHA and ESC practice guidelines Definitions for guideline recommendations and level of evidence Recommendation Class I Class IIa Class IIb Class III Level of evidence Level A Level B Level
Appendix: ACC/AHA and ESC practice guidelines Definitions for guideline recommendations and level of evidence Recommendation Class I Class IIa Class IIb Class III Level of evidence Level A Level B Level
Acute Myocardial Infarction. Willis E. Godin D.O., FACC
 Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
Acute Myocardial Infarction Willis E. Godin D.O., FACC Acute Myocardial Infarction Definition: Decreased delivery of oxygen and nutrients to the myocardium Myocardial tissue necrosis causing irreparable
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA
 Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
Case Study 50 YEAR OLD MALE WITH UNSTABLE ANGINA Case History A 50-year-old man with type 1 diabetes mellitus and hypertension presents after experiencing 1 hour of midsternal chest pain that began after
Acute Myocardial Infarction
 Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Learning Objectives. Epidemiology of Acute Coronary Syndrome
 Cardiovascular Update: Antiplatelet therapy in acute coronary syndromes PHILLIP WEEKS, PHARM.D., BCPS-AQ CARDIOLOGY Learning Objectives Interpret guidelines as they relate to constructing an antiplatelet
Cardiovascular Update: Antiplatelet therapy in acute coronary syndromes PHILLIP WEEKS, PHARM.D., BCPS-AQ CARDIOLOGY Learning Objectives Interpret guidelines as they relate to constructing an antiplatelet
QUT Digital Repository:
 QUT Digital Repository: http://eprints.qut.edu.au/ This is the author s version of this journal article. Published as: Doggrell, Sheila (2010) New drugs for the treatment of coronary artery syndromes.
QUT Digital Repository: http://eprints.qut.edu.au/ This is the author s version of this journal article. Published as: Doggrell, Sheila (2010) New drugs for the treatment of coronary artery syndromes.
Acute coronary syndrome (ACS) is an
 OVERVIEW OF MEDICAL MANAGEMENT OF ACUTE CORONARY SYNDROMES Robert B. Parker, PharmD * Acute coronary syndrome (ACS) is an umbrella term used to describe any group of symptoms of acute myocardial ischemia
OVERVIEW OF MEDICAL MANAGEMENT OF ACUTE CORONARY SYNDROMES Robert B. Parker, PharmD * Acute coronary syndrome (ACS) is an umbrella term used to describe any group of symptoms of acute myocardial ischemia
Clinical Practice Guideline
 Clinical Practice Guideline Secondary Prevention for Patients with Coronary and Other Vascular Disease Since the 2001 update of the American Heart Association (AHA)/American College of Cardiology (ACC)
Clinical Practice Guideline Secondary Prevention for Patients with Coronary and Other Vascular Disease Since the 2001 update of the American Heart Association (AHA)/American College of Cardiology (ACC)
Acute Coronary Syndromes
 Overview Acute Coronary Syndromes Rabeea Aboufakher, MD, FACC, FSCAI Section Chief of Cardiology Altru Health System Grand Forks, ND Epidemiology Pathophysiology Clinical features and diagnosis STEMI management
Overview Acute Coronary Syndromes Rabeea Aboufakher, MD, FACC, FSCAI Section Chief of Cardiology Altru Health System Grand Forks, ND Epidemiology Pathophysiology Clinical features and diagnosis STEMI management
FastTest. You ve read the book now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. The answers will refer you back to
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. The answers will refer you back to
STEMI Presentation and Case Discussion. Case #1
 STEMI Presentation and Case Discussion Scott M Lilly MD PhD, Interventional Cardiology The Ohio State University Contemporary Multidisciplinary Cardiovascular Conference Orlando, Florida September 17 th,
STEMI Presentation and Case Discussion Scott M Lilly MD PhD, Interventional Cardiology The Ohio State University Contemporary Multidisciplinary Cardiovascular Conference Orlando, Florida September 17 th,
Unstable angina and NSTEMI
 Issue date: March 2010 Unstable angina and NSTEMI The early management of unstable angina and non-st-segment-elevation myocardial infarction This guideline updates and replaces recommendations for the
Issue date: March 2010 Unstable angina and NSTEMI The early management of unstable angina and non-st-segment-elevation myocardial infarction This guideline updates and replaces recommendations for the
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008.
 Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
6/1/18 LEARNING OBJECTIVES PATIENT POPULATION PRESENTATIONS
 PREVENTING HOSPITAL READMISSIONS IN CARDIOVASCULAR PATIENTS Christina Cortez Perry, MSN, FNP-C, CCCC Cardiology Coordinator- Corpus Christi Medical Center 1 2 LEARNING OBJECTIVES Identify the target patient
PREVENTING HOSPITAL READMISSIONS IN CARDIOVASCULAR PATIENTS Christina Cortez Perry, MSN, FNP-C, CCCC Cardiology Coordinator- Corpus Christi Medical Center 1 2 LEARNING OBJECTIVES Identify the target patient
Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines)
 Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Performance and Quality Measures 1. NQF Measure Number. Coronary Artery Disease Measure Set
 Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS EPTIFIBATIDE (INTEGRILIN) PROTOCOL
 NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE S EPTIFIBATIDE (INTEGRILIN) I. PURPOSE: A. Integrilin (Eptifibatide) is a specific and potent inhibitor of the platelet receptor glycoprotein
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE S EPTIFIBATIDE (INTEGRILIN) I. PURPOSE: A. Integrilin (Eptifibatide) is a specific and potent inhibitor of the platelet receptor glycoprotein
Non ST Elevation-ACS. Michael W. Cammarata, MD
 Non ST Elevation-ACS Michael W. Cammarata, MD Case Presentation 65 year old man PMH: CAD s/p stent in 2008 HTN HLD Presents with chest pressure, substernally and radiating to the left arm and jaw, similar
Non ST Elevation-ACS Michael W. Cammarata, MD Case Presentation 65 year old man PMH: CAD s/p stent in 2008 HTN HLD Presents with chest pressure, substernally and radiating to the left arm and jaw, similar
Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines)
 Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Acute coronary syndrome (ACS) is a potentially
 DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD* ABSTRACT Acute coronary syndrome is a form of coronary artery disease and has a broad range of clinical presentations.
DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD* ABSTRACT Acute coronary syndrome is a form of coronary artery disease and has a broad range of clinical presentations.
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina
 Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
The PAIN Pathway for the Management of Acute Coronary Syndrome
 2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
2 The PAIN Pathway for the Management of Acute Coronary Syndrome Eyal Herzog, Emad Aziz, and Mun K. Hong Acute coronary syndrome (ACS) subsumes a spectrum of clinical entities, ranging from unstable angina
DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN
 DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN Objectives Gain competence in evaluating chest pain Recognize features of moderate risk unstable angina Review initial management of UA and
DIFFERENTIATING THE PATIENT WITH UNDIFFERENTIATED CHEST PAIN Objectives Gain competence in evaluating chest pain Recognize features of moderate risk unstable angina Review initial management of UA and
Continuing Medical Education Post-Test
 Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Timing of Surgery After Percutaneous Coronary Intervention
 Timing of Surgery After Percutaneous Coronary Intervention Deepak Talreja, MD, FACC Bayview/EVMS/Sentara Outline/Highlights Timing of elective surgery What to do with medications Stopping anti-platelet
Timing of Surgery After Percutaneous Coronary Intervention Deepak Talreja, MD, FACC Bayview/EVMS/Sentara Outline/Highlights Timing of elective surgery What to do with medications Stopping anti-platelet
NOVEL ANTI-THROMBOTIC THERAPIES FOR ACUTE CORONARY SYNDROME: DIRECT THROMBIN INHIBITORS
 Judd E. Hollander, MD Professor, Clinical Research Director, Department of Emergency Medicine University of Pennsylvania School of Medicine, Philadelphia, Pennsylvania OBJECTIVES: 1. Discuss the concept
Judd E. Hollander, MD Professor, Clinical Research Director, Department of Emergency Medicine University of Pennsylvania School of Medicine, Philadelphia, Pennsylvania OBJECTIVES: 1. Discuss the concept
Disclosures. Inpatient Management of Non-ST Elevation Acute Coronary Syndromes. Edward McNulty MD, FACC. None
 Inpatient Management of Non-ST Elevation Acute Coronary Syndromes Edward McNulty MD, FACC Assistant Clinical Professor UCSF Director, SF VAMC Cardiac Catheterization Laboratory Disclosures None New Guidelines
Inpatient Management of Non-ST Elevation Acute Coronary Syndromes Edward McNulty MD, FACC Assistant Clinical Professor UCSF Director, SF VAMC Cardiac Catheterization Laboratory Disclosures None New Guidelines
CLINICIAN INTERVIEW RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE. An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA
 RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA Dr Lincoff is an interventional cardiologist and the Vice Chairman for Research
RECOGNIZING ACS AND STRATIFYING RISK IN PRIMARY CARE An interview with A. Michael Lincoff, MD, and Eric R. Bates, MD, FACC, FAHA Dr Lincoff is an interventional cardiologist and the Vice Chairman for Research
Role of Clopidogrel in Acute Coronary Syndromes. Hossam Kandil,, MD. Professor of Cardiology Cairo University
 Role of Clopidogrel in Acute Coronary Syndromes Hossam Kandil,, MD Professor of Cardiology Cairo University ACS Treatment Strategies Reperfusion/Revascularization Therapy Thrombolysis PCI (with/ without
Role of Clopidogrel in Acute Coronary Syndromes Hossam Kandil,, MD Professor of Cardiology Cairo University ACS Treatment Strategies Reperfusion/Revascularization Therapy Thrombolysis PCI (with/ without
Prospective Comparison of Hemorrhagic Complications After Treatment With Enoxaparin
 Prospective Comparison of Hemorrhagic Complications After Treatment With Versus Unfractionated Heparin for Unstable Angina Pectoris or Non ST-Segment Elevation Acute Myocardial Infarction Scott D. Berkowitz,
Prospective Comparison of Hemorrhagic Complications After Treatment With Versus Unfractionated Heparin for Unstable Angina Pectoris or Non ST-Segment Elevation Acute Myocardial Infarction Scott D. Berkowitz,
What oral antiplatelet therapy would you choose? a) ASA alone b) ASA + Clopidogrel c) ASA + Prasugrel d) ASA + Ticagrelor
 76 year old female Prior Hypertension, Hyperlipidemia, Smoking On Hydrochlorothiazide, Atorvastatin New onset chest discomfort; 2 episodes in past 24 hours Heart rate 122/min; BP 170/92 mm Hg, Killip Class
76 year old female Prior Hypertension, Hyperlipidemia, Smoking On Hydrochlorothiazide, Atorvastatin New onset chest discomfort; 2 episodes in past 24 hours Heart rate 122/min; BP 170/92 mm Hg, Killip Class
A walk through a STEMI
 A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
Cardiology. Self Learning Package. Module 5: Pharmacology: Treatment of Acute Coronary. Prevention
 Cardiology Self Learning Package Module 5: Pharmacology: Treatment of Acute Coronary Syndromes, Module 5: Pharmacology: Hyperlipidaemia, Treatment of Acute Coronary Hypertension, Symdrome, Hyperlipidaemia,
Cardiology Self Learning Package Module 5: Pharmacology: Treatment of Acute Coronary Syndromes, Module 5: Pharmacology: Hyperlipidaemia, Treatment of Acute Coronary Hypertension, Symdrome, Hyperlipidaemia,
Clopidogrel Date: 15 July 2008
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinicalTrials.gov
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinicalTrials.gov
New Guidelines for Evaluating Acute Coronary Syndrome
 New Guidelines for Evaluating Acute Coronary Syndrome The American College of Cardiology and the American Heart Association [Clinician Reviews 11(1):73-86, 2001. 2001 Clinicians Publishing Group] Introduction
New Guidelines for Evaluating Acute Coronary Syndrome The American College of Cardiology and the American Heart Association [Clinician Reviews 11(1):73-86, 2001. 2001 Clinicians Publishing Group] Introduction
Cangrelor: Is it the new CHAMPION for PCI? Robert Barcelona, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Intensive Care Unit November 13, 2015
 Cangrelor: Is it the new CHAMPION for PCI? Robert Barcelona, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Intensive Care Unit November 13, 2015 Objectives Review the pharmacology and pharmacokinetic
Cangrelor: Is it the new CHAMPION for PCI? Robert Barcelona, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Intensive Care Unit November 13, 2015 Objectives Review the pharmacology and pharmacokinetic
Cardiovascular Health Practice Guideline Outpatient Management of Coronary Artery Disease 2003
 Authorized By: Medical Management Guideline Committee Approval Date: 12/13/01 Revision Date: 12/11/03 Beta-Blockers Nitrates Calcium Channel Blockers MEDICATIONS Indicated in post-mi, unstable angina,
Authorized By: Medical Management Guideline Committee Approval Date: 12/13/01 Revision Date: 12/11/03 Beta-Blockers Nitrates Calcium Channel Blockers MEDICATIONS Indicated in post-mi, unstable angina,
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Acute Coronary Syndrome. Sonny Achtchi, DO
 Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Program Metrics. New Unique ID. Old Unique ID. Metric Set Metric Name Description. Old Metric Name
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Acute Coronary syndrome
 Acute Coronary syndrome 7th Annual Pharmacotherapy Conference ACS Pathophysiology rupture or erosion of a vulnerable, lipidladen, atherosclerotic coronary plaque, resulting in exposure of circulating blood
Acute Coronary syndrome 7th Annual Pharmacotherapy Conference ACS Pathophysiology rupture or erosion of a vulnerable, lipidladen, atherosclerotic coronary plaque, resulting in exposure of circulating blood
Severe Coronary Vasospasm Complicated with Ventricular Tachycardia
 Severe Coronary Vasospasm Complicated with Ventricular Tachycardia Göksel Acar, Serdar Fidan, Servet İzci and Anıl Avcı Kartal Koşuyolu High Specialty Education and Research Hospital, Cardiology Department,
Severe Coronary Vasospasm Complicated with Ventricular Tachycardia Göksel Acar, Serdar Fidan, Servet İzci and Anıl Avcı Kartal Koşuyolu High Specialty Education and Research Hospital, Cardiology Department,
Acute coronary syndromes
 Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Heart disease is the leading cause of death
 ACS AND ANTIPLATELET MANAGEMENT: UPDATED GUIDELINES AND CURRENT TRIALS Christopher P. Cannon, MD,* ABSTRACT Acute coronary syndrome (ACS) is an important cause of morbidity and mortality in the US population
ACS AND ANTIPLATELET MANAGEMENT: UPDATED GUIDELINES AND CURRENT TRIALS Christopher P. Cannon, MD,* ABSTRACT Acute coronary syndrome (ACS) is an important cause of morbidity and mortality in the US population
Dual Antiplatelet Therapy Made Practical
 Dual Antiplatelet Therapy Made Practical David Parra, Pharm.D., FCCP, BCPS Clinical Pharmacy Program Manager in Cardiology/Anticoagulation VISN 8 Pharmacy Benefits Management Clinical Associate Professor
Dual Antiplatelet Therapy Made Practical David Parra, Pharm.D., FCCP, BCPS Clinical Pharmacy Program Manager in Cardiology/Anticoagulation VISN 8 Pharmacy Benefits Management Clinical Associate Professor
TCTAP Upendra Kaul MD,DM,FACC,FSCAI,FAMS,FCSI
 Indian TUXEDO Trial In Medically Treated Diabetics Upendra Kaul MD,DM,FACC,FSCAI,FAMS,FCSI Executive Director and Dean Escorts Heart Institute & Medical Research Center and Fortis Hospitals, New Delhi
Indian TUXEDO Trial In Medically Treated Diabetics Upendra Kaul MD,DM,FACC,FSCAI,FAMS,FCSI Executive Director and Dean Escorts Heart Institute & Medical Research Center and Fortis Hospitals, New Delhi
ST-elevation myocardial infarctions (STEMIs)
 Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
ST Elevation Myocardial Infarction
 ST Elevation Myocardial Infarction Scott M. Lilly, MD, PhD Assistant Professor Clinical Department of Cardiovascular Medicine The Ohio State University Wexner Medical Center Outline Case Presentation STEMI
ST Elevation Myocardial Infarction Scott M. Lilly, MD, PhD Assistant Professor Clinical Department of Cardiovascular Medicine The Ohio State University Wexner Medical Center Outline Case Presentation STEMI
ST Elevation Myocardial Infarction
 ST Elevation Myocardial Infarction Scott M. Lilly, MD, PhD Assistant Professor Clinical Department of Cardiovascular Medicine The Ohio State University Wexner Medical Center Case Presentation 46 year old
ST Elevation Myocardial Infarction Scott M. Lilly, MD, PhD Assistant Professor Clinical Department of Cardiovascular Medicine The Ohio State University Wexner Medical Center Case Presentation 46 year old
ARMYDA-RECAPTURE (Atorvastatin for Reduction of MYocardial Damage during Angioplasty) trial
 ARMYDA-RECAPTURE ( for Reduction of MYocardial Damage during Angioplasty) trial Prospective, multicenter, randomized, double blind trial investigating efficacy of atorvastatin reload in patients on chronic
ARMYDA-RECAPTURE ( for Reduction of MYocardial Damage during Angioplasty) trial Prospective, multicenter, randomized, double blind trial investigating efficacy of atorvastatin reload in patients on chronic
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist. Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI
 Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
Diagnosis and Management of Acute Myocardial Infarction
 Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
EPTIFIBATIDE INDUCED SEVERE THROMBOCYTOPENIA IN AN ASYMPTOMATIC PATIENT
 EPTIFIBATIDE INDUCED SEVERE THROMBOCYTOPENIA IN AN ASYMPTOMATIC PATIENT 1 Dr. M. Adnan Raufi MD FACC FSCAI, 2 Ayesha S. BaigMDRama Siddiqui, 3 Nouman Akbar 4 Shakaib Jaffery International Journal of Drug
EPTIFIBATIDE INDUCED SEVERE THROMBOCYTOPENIA IN AN ASYMPTOMATIC PATIENT 1 Dr. M. Adnan Raufi MD FACC FSCAI, 2 Ayesha S. BaigMDRama Siddiqui, 3 Nouman Akbar 4 Shakaib Jaffery International Journal of Drug
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE. Jules B. Puschett, M.D.
 DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
APPENDIX F: CASE REPORT FORM
 APPENDIX F: CASE REPORT FORM Instruction: Complete this form to notify all ACS admissions at your centre to National Cardiovascular Disease Registry. Where check boxes are provided, check ( ) one or more
APPENDIX F: CASE REPORT FORM Instruction: Complete this form to notify all ACS admissions at your centre to National Cardiovascular Disease Registry. Where check boxes are provided, check ( ) one or more
Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report
 Concurrent subarachnoid hemorrhage and AMI 155 Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report Chen-Chuan Cheng 1, Wen-Shiann Wu 1, Chun-Yen Chiang 1, Tsuei-Yuang Huang
Concurrent subarachnoid hemorrhage and AMI 155 Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report Chen-Chuan Cheng 1, Wen-Shiann Wu 1, Chun-Yen Chiang 1, Tsuei-Yuang Huang
Practice-Level Executive Summary Report
 PINNACLE Registry Metrics 0003, Test Practice_NextGen [Rolling: 1st April 2015 to 31st March 2016 ] Generated on 5/11/2016 11:37:35 AM American College of Cardiology Foundation National Cardiovascular
PINNACLE Registry Metrics 0003, Test Practice_NextGen [Rolling: 1st April 2015 to 31st March 2016 ] Generated on 5/11/2016 11:37:35 AM American College of Cardiology Foundation National Cardiovascular
Clopidogrel and ASA after CABG for NSTEMI
 Clopidogrel and ASA after CABG for NSTEMI May 17, 2007 Justin Lee Pharmacy Resident University Health Network Objectives At the end of this session, you should be able to: Explain the rationale for antiplatelet
Clopidogrel and ASA after CABG for NSTEMI May 17, 2007 Justin Lee Pharmacy Resident University Health Network Objectives At the end of this session, you should be able to: Explain the rationale for antiplatelet
Διάρκεια διπλής αντιαιμοπεταλιακής αγωγής. Νικόλαος Γ.Πατσουράκος Καρδιολόγος, Επιμελητής Α ΕΣΥ Τζάνειο Γενικό Νοσοκομείο Πειραιά
 Διάρκεια διπλής αντιαιμοπεταλιακής αγωγής Νικόλαος Γ.Πατσουράκος Καρδιολόγος, Επιμελητής Α ΕΣΥ Τζάνειο Γενικό Νοσοκομείο Πειραιά International ACS guidelines: Recommendations on duration of dual
Διάρκεια διπλής αντιαιμοπεταλιακής αγωγής Νικόλαος Γ.Πατσουράκος Καρδιολόγος, Επιμελητής Α ΕΣΥ Τζάνειο Γενικό Νοσοκομείο Πειραιά International ACS guidelines: Recommendations on duration of dual
STEMI ST Elevation Myocardial Infarction
 STEMI ST Elevation Myocardial Infarction Breakout Session One Moderators: Quinn Capers IV, MD and Scott M. Lilly, MD, PhD Cases Presented by: Umair S. Ahmad, MD 1 Outline 1. Multivessel Revascularization
STEMI ST Elevation Myocardial Infarction Breakout Session One Moderators: Quinn Capers IV, MD and Scott M. Lilly, MD, PhD Cases Presented by: Umair S. Ahmad, MD 1 Outline 1. Multivessel Revascularization
Coronary Artery Disease: Revascularization (Teacher s Guide)
 Stephanie Chan, M.D. Updated 3/15/13 2008-2013, SCVMC (40 minutes) I. Objectives Coronary Artery Disease: Revascularization (Teacher s Guide) To review the evidence on whether percutaneous coronary intervention
Stephanie Chan, M.D. Updated 3/15/13 2008-2013, SCVMC (40 minutes) I. Objectives Coronary Artery Disease: Revascularization (Teacher s Guide) To review the evidence on whether percutaneous coronary intervention
Prehospital and Hospital Care of Acute Coronary Syndrome
 Ischemic Heart Diseases Prehospital and Hospital Care of Acute Coronary Syndrome JMAJ 46(8): 339 346, 2003 Katsuo KANMATSUSE* and Ikuyoshi WATANABE** * Professor, Second Internal Medicine, Nihon University,
Ischemic Heart Diseases Prehospital and Hospital Care of Acute Coronary Syndrome JMAJ 46(8): 339 346, 2003 Katsuo KANMATSUSE* and Ikuyoshi WATANABE** * Professor, Second Internal Medicine, Nihon University,
Otamixaban for non-st-segment elevation acute coronary syndrome
 Otamixaban for non-st-segment elevation acute coronary syndrome September 2011 This technology summary is based on information available at the time of research and a limited literature search. It is not
Otamixaban for non-st-segment elevation acute coronary syndrome September 2011 This technology summary is based on information available at the time of research and a limited literature search. It is not
Consultation Group: Cardiology Consultants Clinical lead for cardiology: Dr Andrew Hannah. Review Date: Uncontrolled when printed.
 NHS Grampian Staff Guidelines For The In-Hospital Management Of Unstable Angina And Non-ST-Segment- Elevation Myocardial Infarction Patients (17 Years And Older) Co-ordinators: Cardiology Specialist Clinical
NHS Grampian Staff Guidelines For The In-Hospital Management Of Unstable Angina And Non-ST-Segment- Elevation Myocardial Infarction Patients (17 Years And Older) Co-ordinators: Cardiology Specialist Clinical
DUKECATHR Dataset Dictionary
 DUKECATHR Dataset Dictionary Version of DUKECATH dataset for educational use that has been modified to be unsuitable for clinical research or publication (Created Date and Time: 28OCT16 14:35) Table of
DUKECATHR Dataset Dictionary Version of DUKECATH dataset for educational use that has been modified to be unsuitable for clinical research or publication (Created Date and Time: 28OCT16 14:35) Table of
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
Coronary Artery Disease Clinical Practice Guidelines
 Coronary Artery Disease Clinical Practice Guidelines Guidelines are systematically developed statements to assist patients and providers in choosing appropriate healthcare for specific clinical conditions.
Coronary Artery Disease Clinical Practice Guidelines Guidelines are systematically developed statements to assist patients and providers in choosing appropriate healthcare for specific clinical conditions.
UNSTABLE angina pectoris is a transitory syndrome
 Journal of Gerontology: MEDICAL SCIENCES 2003, Vol. 58A, No. 10, 927 933 Copyright 2003 by The Gerontological Society of America Review Article Treatment of Unstable Angina Pectoris/ Non-ST-Segment Elevation
Journal of Gerontology: MEDICAL SCIENCES 2003, Vol. 58A, No. 10, 927 933 Copyright 2003 by The Gerontological Society of America Review Article Treatment of Unstable Angina Pectoris/ Non-ST-Segment Elevation
2008, American Heart Association. All rights reserved.
 AHA 2008 Cocaine-Associated Chest Pain and Myocardial Infarction Slide Set Based on the AHA 2008 Scientific Statement for Management of Cocaine-Associated Chest Pain and Myocardial Infarction George J.
AHA 2008 Cocaine-Associated Chest Pain and Myocardial Infarction Slide Set Based on the AHA 2008 Scientific Statement for Management of Cocaine-Associated Chest Pain and Myocardial Infarction George J.
Controversies in Cardiac Pharmacology
 Controversies in Cardiac Pharmacology Thomas D. Conley, MD FACC FSCAI Disclosures I have no relevant relationships with commercial interests to disclose. 1 Doc, do I really need to take all these medicines?
Controversies in Cardiac Pharmacology Thomas D. Conley, MD FACC FSCAI Disclosures I have no relevant relationships with commercial interests to disclose. 1 Doc, do I really need to take all these medicines?
Acute Coronary Syndrome: Management of the patients with Unstable Angina and Non-ST Segment Elevation Myocardial Infarction Rahman S, Rahman KA
 Acute Coronary Syndrome: Management of the patients with Unstable Angina and Non-ST Segment Elevation Myocardial Infarction Rahman S, Rahman KA Introduction Acute Coronary Syndrome (ACS) kills and disables
Acute Coronary Syndrome: Management of the patients with Unstable Angina and Non-ST Segment Elevation Myocardial Infarction Rahman S, Rahman KA Introduction Acute Coronary Syndrome (ACS) kills and disables
Acute Coronary Syndrome. Cindy Baker, MD FACC Director Peripheral Vascular Interventions Division of Cardiovascular Medicine
 Acute Coronary Syndrome Cindy Baker, MD FACC Director Peripheral Vascular Interventions Division of Cardiovascular Medicine Topics Timing is everything So many drugs to choose from What s a MINOCA? 2 Acute
Acute Coronary Syndrome Cindy Baker, MD FACC Director Peripheral Vascular Interventions Division of Cardiovascular Medicine Topics Timing is everything So many drugs to choose from What s a MINOCA? 2 Acute
REVIEW DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK. Edith A. Nutescu, PharmD * ABSTRACT INTRODUCTION
 DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD * ABSTRACT Acute coronary syndrome is a form of coronary artery disease, which has a broad range of clinical presentations.
DIAGNOSING ACUTE CORONARY SYNDROME AND DETERMINING PATIENT RISK Edith A. Nutescu, PharmD * ABSTRACT Acute coronary syndrome is a form of coronary artery disease, which has a broad range of clinical presentations.
More than 1 million percutaneous coronary intervention
 n report n Percutaneous Coronary Intervention: Assessing Coronary Vascular Risk Associated With Bare-Metal and Drug-Eluting Stents Sarah A. Spinler, PharmD, FCCP, BCPS (AQ Cardiology) Abstract Percutaneous
n report n Percutaneous Coronary Intervention: Assessing Coronary Vascular Risk Associated With Bare-Metal and Drug-Eluting Stents Sarah A. Spinler, PharmD, FCCP, BCPS (AQ Cardiology) Abstract Percutaneous
Acute coronary syndromes (ACS), including unstable
 n report n Acute Coronary Syndromes: Morbidity, Mortality, and Pharmacoeconomic Burden Daniel M. Kolansky, MD Abstract Acute coronary syndromes (ACS), which include unstable angina and myocardial infarction
n report n Acute Coronary Syndromes: Morbidity, Mortality, and Pharmacoeconomic Burden Daniel M. Kolansky, MD Abstract Acute coronary syndromes (ACS), which include unstable angina and myocardial infarction
Prevention of Coronary Stent Thrombosis and Restenosis
 Prevention of Coronary Stent Thrombosis and Restenosis Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea 9/12/03 Coronary
Prevention of Coronary Stent Thrombosis and Restenosis Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea 9/12/03 Coronary
Preoperative Cardiac Risk Assessment: Approach & Guidelines
 Preoperative Cardiac Risk Assessment: Approach & Guidelines By, Liam Morris, MD., FACC (02/03/18) CPG : Clinical Practice Guidelines GDMT : Guidelines Directed Medical Therapy GWC : Guideline Writing Committee
Preoperative Cardiac Risk Assessment: Approach & Guidelines By, Liam Morris, MD., FACC (02/03/18) CPG : Clinical Practice Guidelines GDMT : Guidelines Directed Medical Therapy GWC : Guideline Writing Committee
Biphasic T-wave in patient with chest pain (Wellens syndrome)
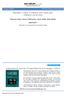 www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Biphasic T-wave in patient with chest pain (Wellens syndrome) Ahmed Zedan, Osama Mukarram, Umer Malik, Raja Naidu ABSTRACT Abstract is
www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS Biphasic T-wave in patient with chest pain (Wellens syndrome) Ahmed Zedan, Osama Mukarram, Umer Malik, Raja Naidu ABSTRACT Abstract is
STEMI update. Vijay Krishnamoorthy M.D. Interventional Cardiology
 STEMI update Vijay Krishnamoorthy M.D. Interventional Cardiology OVERVIEW Current Standard of Care in Management of STEMI Update in management of STEMI Pre-Cath Lab In the ED/Office/EMS. Cath Lab Post
STEMI update Vijay Krishnamoorthy M.D. Interventional Cardiology OVERVIEW Current Standard of Care in Management of STEMI Update in management of STEMI Pre-Cath Lab In the ED/Office/EMS. Cath Lab Post
Belinda Green, Cardiologist, SDHB, 2016
 Acute Coronary syndromes All STEMI ALL Non STEMI Unstable angina Belinda Green, Cardiologist, SDHB, 2016 Thrombus in proximal LAD Underlying pathophysiology Be very afraid for your patient Wellens
Acute Coronary syndromes All STEMI ALL Non STEMI Unstable angina Belinda Green, Cardiologist, SDHB, 2016 Thrombus in proximal LAD Underlying pathophysiology Be very afraid for your patient Wellens
Clopidogrel has been evaluated in clinical trials that included cardiovascular patients
 REVIEW ARTICLE Comparative Benefits of Clopidogrel and Aspirin in High-Risk Patient Populations Lessons From the CAPRIE and CURE Studies Jack Hirsh, CM, MD, FRCPC, FRACP, FRSC, DSc; Deepak L. Bhatt, MD,
REVIEW ARTICLE Comparative Benefits of Clopidogrel and Aspirin in High-Risk Patient Populations Lessons From the CAPRIE and CURE Studies Jack Hirsh, CM, MD, FRCPC, FRACP, FRSC, DSc; Deepak L. Bhatt, MD,
ISAR-LEFT MAIN: A Randomized Clinical Trial on Drug-Eluting Stents for Unprotected Left Main Lesions
 Julinda Mehilli, MD Deutsches Herzzentrum Technische Universität Munich Germany ISAR-LEFT MAIN: A Randomized Clinical Trial on Drug-Eluting Stents for Unprotected Left Main Lesions Background Left main
Julinda Mehilli, MD Deutsches Herzzentrum Technische Universität Munich Germany ISAR-LEFT MAIN: A Randomized Clinical Trial on Drug-Eluting Stents for Unprotected Left Main Lesions Background Left main
CABG Surgery following STEMI
 CABG Surgery following STEMI Susana Harrington, MS,APRN-NP Cardio-Thoracic Surgery Nebraska Methodist Hospital February 15, 2018 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction:
CABG Surgery following STEMI Susana Harrington, MS,APRN-NP Cardio-Thoracic Surgery Nebraska Methodist Hospital February 15, 2018 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction:
2016 ACC/AHA Guideline Focused Update on Duration of Dual Antiplatelet Therapy in Patients With Coronary Artery Disease
 2016 ACC/AHA Guideline Focused Update on Duration of Dual Antiplatelet Therapy in Patients With Coronary Artery Disease Developed in Collaboration with American Association for Thoracic Surgery, American
2016 ACC/AHA Guideline Focused Update on Duration of Dual Antiplatelet Therapy in Patients With Coronary Artery Disease Developed in Collaboration with American Association for Thoracic Surgery, American
Inter-regional differences and outcome in unstable angina
 European Heart Journal (2000) 21, 1433 1439 doi:10.1053/euhj.1999.1983, available online at http://www.idealibrary.com on Inter-regional differences and outcome in unstable angina Analysis of the International
European Heart Journal (2000) 21, 1433 1439 doi:10.1053/euhj.1999.1983, available online at http://www.idealibrary.com on Inter-regional differences and outcome in unstable angina Analysis of the International
Case Report Simultaneous Two-Vessel Subacute Stent Thrombosis Caused by Clopidogrel Resistance from CYP2C19 Polymorphism
 Case Reports in Medicine Volume 2016, Article ID 2312078, 4 pages http://dx.doi.org/10.1155/2016/2312078 Case Report Simultaneous Two-Vessel Subacute Stent Thrombosis Caused by Clopidogrel Resistance from
Case Reports in Medicine Volume 2016, Article ID 2312078, 4 pages http://dx.doi.org/10.1155/2016/2312078 Case Report Simultaneous Two-Vessel Subacute Stent Thrombosis Caused by Clopidogrel Resistance from
Acute Coronary Syndrome. ACC/AHA 2002 Guidelines
 Acute Coronary Syndrome ACC/AHA 2002 Guidelines ACS Unstable Angina Non ST elevation MI ST elevation MI ACS UA and Non STEMI described in these guidelines Management of STEMI described in separate guidelines
Acute Coronary Syndrome ACC/AHA 2002 Guidelines ACS Unstable Angina Non ST elevation MI ST elevation MI ACS UA and Non STEMI described in these guidelines Management of STEMI described in separate guidelines
The risk of death or ischemic events in patients with
 Prediction of Outcome after Percutaneous Coronary Intervention for the Acute Coronary Syndrome Annapoorna S. Kini, MD, Paul C. Lee, MD, Cristina A. Mitre, MD, Michael C. Kim, MD, Mazullah Kamran, MD, Mary
Prediction of Outcome after Percutaneous Coronary Intervention for the Acute Coronary Syndrome Annapoorna S. Kini, MD, Paul C. Lee, MD, Cristina A. Mitre, MD, Michael C. Kim, MD, Mazullah Kamran, MD, Mary
ACS and Heart Failure
 ACS and Heart Failure Jonathon Firnhaber, MD, FAAFP Associate Professor The Brody School of Medicine at East Carolina University Greenville, North Carolina Learning Objectives Establish the diagnosis and
ACS and Heart Failure Jonathon Firnhaber, MD, FAAFP Associate Professor The Brody School of Medicine at East Carolina University Greenville, North Carolina Learning Objectives Establish the diagnosis and
A CASE REPORT AND LITERATURE REVIEW ON MYOCARDIAL INFARCTION WITH NORMAL CORONARY ARTERIES
 A CASE REPORT AND LITERATURE REVIEW ON MYOCARDIAL INFARCTION WITH NORMAL CORONARY ARTERIES Niyamtullah Musalman 1*, Lijun Jin 2 and Farhan Khan 3 *12 Department of Cardiology, Yangtze Medical University
A CASE REPORT AND LITERATURE REVIEW ON MYOCARDIAL INFARCTION WITH NORMAL CORONARY ARTERIES Niyamtullah Musalman 1*, Lijun Jin 2 and Farhan Khan 3 *12 Department of Cardiology, Yangtze Medical University
Continuing Medical Education Post-Test
 Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
Continuing Medical Education Post-Test Based on the information presented in this monograph, please choose one correct response for each of the following questions or statements. Record your answers on
An update on the management of UA / NSTEMI. Michael H. Crawford, MD
 An update on the management of UA / NSTEMI Michael H. Crawford, MD New ACC/AHA Guidelines 2007 What s s new in the last 5 years CT imaging advances Ascendancy of troponin and BNP Clarification of ACEI/ARB
An update on the management of UA / NSTEMI Michael H. Crawford, MD New ACC/AHA Guidelines 2007 What s s new in the last 5 years CT imaging advances Ascendancy of troponin and BNP Clarification of ACEI/ARB
The MAIN-COMPARE Study
 Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Tailoring adjunctive antithrombotic therapy to reperfusion strategy in STEMI
 Tailoring adjunctive antithrombotic therapy to reperfusion strategy in STEMI Adel El-Etriby; MD Professor of Cardiology Ain Shams University President of the Egyptian Working Group of Interventional Cardiology
Tailoring adjunctive antithrombotic therapy to reperfusion strategy in STEMI Adel El-Etriby; MD Professor of Cardiology Ain Shams University President of the Egyptian Working Group of Interventional Cardiology
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 21 July 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 21 July 2010 DUOPLAVIN 75 mg/75 mg, film-coated tablet B/30 (CIP code: 359 022-6) B/30 (CIP code: 382 063-7) DUOPLAVIN
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 21 July 2010 DUOPLAVIN 75 mg/75 mg, film-coated tablet B/30 (CIP code: 359 022-6) B/30 (CIP code: 382 063-7) DUOPLAVIN
North Wales Cardiac Network Guidelines on oral antiplatelet therapy in cardiovascular disease
 Guidelines on oral antiplatelet therapy in cardiovascular disease This guidance should be considered as one part of the wider therapeutic management of patients. The indication for antiplatelet therapy
Guidelines on oral antiplatelet therapy in cardiovascular disease This guidance should be considered as one part of the wider therapeutic management of patients. The indication for antiplatelet therapy
Case Report Left Main Stenosis. Percutaneous Coronary Intervention (PCI) or Coronary Artery Bypass Graft Surgery (CABG)?
 Cronicon OPEN ACCESS CARDIOLOGY Case Report Left Main Stenosis. Percutaneous Coronary Intervention (PCI) or Coronary Artery Bypass Graft Surgery (CABG)? Valentin Hristov* Department of Cardiology, Specialized
Cronicon OPEN ACCESS CARDIOLOGY Case Report Left Main Stenosis. Percutaneous Coronary Intervention (PCI) or Coronary Artery Bypass Graft Surgery (CABG)? Valentin Hristov* Department of Cardiology, Specialized
