SOD (Sphincter of Oddi Dysfunction)
|
|
|
- Kelley Dixon
- 6 years ago
- Views:
Transcription
1 SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum. The sphincter can malfunction, not letting the digestive juices through as it should. Without proper regulation, bile and pancreatic enzymes do not drain properly, leading to symptoms such as pain, increased liver enzymes and/or recurrent pancreatitis. What is the Sphincter of Oddi? The Spincter of Oddi is a cylindrical shaped muscle located where the bile duct and pancreatic duct meet at the entrance to the first part of the small intestine (duodenum). It functions like a one way valve, regulating the flow of bile and pancreatic enzymes from each of the ducts into your digestive tract. Bile is produced in the liver, and drains down the bile duct, where it is stored in the gall bladder or released directly into the duodenum. The pancreatic enzymes are made in the pancreas and flow down the pancreatic duct and into the duodenum. Food or liquid goes down your esophagus, into your stomach and into your duodenum. Your brain sends signals to the Sphincter of Oddi to regulate the release of the digestive juices according to your food intake, such as releasing more bile for a fatty meal. A properly functioning Sphincter of Oddi contracts and relaxes accordingly to let out the appropriate amounts of bile and enzymes to allow for the digestion of food. The Sphincter of Oddi also prevents contents from the duodenum from flowing back up into the bile duct and pancreatic duct. What causes dysfunction? SOD is the condition where the Sphincter of Oddi is not functioning properly. This can mean that the muscle is too tight and not letting enough of the digestive juices into the duodenum because the muscle has too much pressure or that it is rigid or stiff and narrowed. When the bile and pancreatic juices are not let through the Sphincter of Oddi into the duodenum, they can become backed up which can lead to abdominal pain, nausea and vomiting as well as increase in liver function tests and/or pancreatitis. It is not known why the muscle becomes too tight in some people. What are the symptoms of SOD? The most common and prominent symptom of SOD is upper abdominal pain. This is often experienced as a sharp pain in the middle of the abdomen right below the rib cage. Pain is often described as severe in nature and can radiate to either side of the abdomen and/or to the back. The pain often becomes worse after eating, and particularly worse after eating a fatty meal such as pizza. Page 1
2 Nausea and vomiting can accompany the abdominal pain but are usually not the predominant symptoms. The severe abdominal pain can last for several hours and often requires pain medication and anti-nausea medication for relief. The severe pain episodes can be constant or intermittent, occurring anywhere from once a day to weekly or monthly. Patients will often describe debilitating pain that brings them to the Emergency Department several times a year and/or keeps them from living their normal life. Another presentation of SOD can be acute recurrent pancreatitis, as diagnosed with lab tests and imaging studies, with no other clear cause. Fever, chills, extreme weight loss and/or jaundice are uncommon symptoms. What kind of people are affected by SOD? SOD is most often seen in women between the ages of 30 and 50, however, it can occur in anyone. What are the types of SOD? There are three classifications for SOD patients. Type I patients have biliary pain, elevated liver enzymes at least twice normal levels on two occasions, dilated common bile duct and delayed drainage of the common bile duct. Type II patients have pain in addition to one or two of the criteria listed above. Type III patients have only biliary pain and no other documented abnormalities. These classifications help in predicting the likelihood of SOD before diagnosis with ERCP. How is SOD II diagnosed & treated? SOD type II is diagnosed by measuring the pressure in the sphincter muscle using Manometry during an ERCP (Endoscopic Retrograde Cholangio-Pancreatography). Like a regular ERCP, the doctor passes an endoscope (a thin flexible lighted tube with a camera on the end) into your mouth and down your esophagus to inspect your stomach and duodenum to where the opening of the sphincter is. With Manometry, the doctor utilizes a special catheter and apparatus for measuring the pressures of the sphincters in the bile duct and pancreatic duct at the time of the ERCP. In order for pressures to be accurate, you must be off any pain medication for 12 hours before the procedure because the pain medication can affect the pressure reading and lead to improper diagnosis. If the sphincter pressures are higher than normal, the doctor will treat the SOD. If pressures are found to be higher than normal in the bile duct or the pancreatic duct, the doctor can enlarge the openings (sphincters) by cutting the duct (a Sphincterotomy). This procedure is done with an electrically heated wire, which you will not feel. Performing a small cut in the sphincter can release the increased pressure and allow the pancreatic and bile juices to flow easier. A temporary pancreatic stent is often put in place during the ERCP to reduce the chances of pancreatitis. It is designed to fall out by itself, but an x-ray within 3 weeks of your ERCP will make sure of this. Additionally, an Page 2
3 indomethacin suppository is placed after the procedure, which has been shown to decrease the rate of post-ercp pancreatitis. How is SOD III diagnosed and treated? SOD III is no longer diagnosed with manometry and treated with sphincterotomy since a recent NIH study showed that this procedure was more risky than beneficial for this specific group of patients. SOD type III is now usually diagnosed based on clinical symptoms and treated medically with medications such as anti-spasmotics and/or medicine that deals with the nerves of the digestive system. Do all people respond to treatment? Two-thirds (66%) of patients with SOD type II and documented high pressures who undergo ERCP with Sphincterotomy will experience some sort of relief. This is not usually a complete cure, but often, it is a reduction in severity or frequency of symptoms. Many patients report a significant improvement in their symptoms post procedure. The remainder (33%) of patients with SOD type II and documented high pressures, report no change at all in symptoms after treatment. Are there risks associated with the treatment? All ERCP s can result in complications, the most common (6-10%) being inflammation of the pancreas (pancreatitis) which causes abdominal pain with nausea and vomiting. Pancreatitis can be mild to severe with treatment including hospitalization, observation, rest, IV hydration, and medication for abdominal pain. It usually resolves spontaneously within a few days. People with SOD have been found to have an increased (10-30%) propensity for getting pancreatitis after ERCP s. Most episodes of post ERCP pancreatitis are not severe. Other less common risks include reactions to the anesthesia medications, making a hole in the bowel wall (perforation of the esophagus, stomach or intestines), bleeding, infection and inflammation of the bile duct (cholangitis). While these complications are not common, in certain cases they can be very serious and may require urgent treatment, an extended hospitalization, or even an operation. Very rarely, serious injury or even death has resulted from a serious complication. Can SOD be treated without an ERCP? There is an option for medical therapy for SOD. Drugs that relax smooth muscle have been found to relieve SOD symptoms for some people. This is likely due to the fact that the sphincter itself is composed of smooth muscle. However, these drugs also can have side effects. Additionally, just as ERCP with Manometry and Sphincterotomy does not cure all patients, only some people will see a decrease of symptoms from medical therapy. What can I expect if I have an ERCP with Manometry? Before It is extremely important NOT to take any pain medication 12 hours before your procedure (including long or short acting pills, patches, creams or analgesic lollypops) as this can affect the pressure readings and make them appear falsely low. Do not eat or drink anything after midnight Page 3
4 the night before your procedure. On the day of your ERCP with Manometry, you will arrive 60 minutes before the procedure is scheduled. The doctor and/or nurse will explain the procedure again and answer any questions you might still have. You will be asked to sign a consent form giving your permission for the procedure. You will need to put on a hospital gown and remove any jewelry, eyeglasses, contacts, and dentures. A nurse will put in an IV in your arm before the procedure starts for hydration and for the anesthesiologist to administer the sedation medication. You will be connected to a machine that will monitor your heart rate, blood pressure and blood oxygen level throughout the procedure. During The examination is performed on an x-ray table. Local anesthetic will be sprayed onto your throat to make it numb, and you will be given medication through the IV by the anesthesiologist to make you fall asleep. A mouth guard will be placed to protect your teeth and gums. While in a comfortable position on your stomach, the doctor will pass the endoscope through your mouth and down your throat. The endoscope will not interfere with your breathing and generally causes only mild throat and abdominal discomfort. The doctor will guide the endoscope through your esophagus, stomach and duodenum until it reaches the papilla/sphincter of Oddi where the pancreas and bile ducts meet. A thin tube will be passed through the endoscope and into the Sphincter of Oddi to measure the pressures of the muscle in the bile duct and the pancreatic duct. The doctor can inject contrast dye through another small tube into the ducts so that when the x-ray is taken, any abnormalities can be seen. If pressures are normal, no treatment is necessary. If the pressures are found to be high, a small cut (sphincterotomy) is made in the duct to relieve the pressure. Before the doctor takes the endoscope out, a small pancreatic stent will be placed in the pancreatic duct to minimize the risk of pancreatitis. This stent is designed to fall out on its own; however, you should schedule an x-ray in three weeks to be sure it has fallen out. Additionally, you may have an indomethacin suppository placed after the procedure, which has been shown to decrease the rate of post-ercp pancreatitis. The ERCP with Manometry generally takes minutes depending on findings and treatment. After You will wake up from the sedation in the recovery room. Your throat may feel sore. Because of the local anesthetic and sedation, you should not attempt to take anything by mouth for at least one hour from the time you first wake up. It is wise to take clear liquids for the remainder of the day. Your belly may also feel bloated and full from air inflated through the endoscope during the procedure. You will be admitted to the hospital overnight for observation and will be allowed to go home the next day if you show no signs of complications. Please take the time to consider the benefits and risks this procedure has to offer you. Drs. Jamidar, Aslanian, Farrell & Muniraj want you to have the best procedure experience possible. Please call with any questions, concerns or problems. M-F 8:30 am-4:30 pm at (203) Page 4 July 2017
5 Your ERCP with Manometry is scheduled for at am/pm; am/pm arrival with Dr. Jamidar/ Dr. Aslanian/ Dr. Farrell/ Dr. Muniraj at the Yale Center for Advanced Endoscopy on Smilow 4. Instructions for your ERCP with Manometry Two Weeks before your ERCP with Manometry 1. Call us if you have allergies or bad reactions to antibiotics, medications or anesthesia. 2. Call us if you have heart or breathing problems, as we will need recent records of tests and visits from your heart and lung doctor before the procedure. 3. Call us if you take blood thinners like Coumadin/warfarin or Plavix or aspirin, as they may need to be adjusted before your procedure. 4. Call us if you have diabetes, as your medications may need to be adjusted the AM of, or PM before your procedure. 5. Call us if you are on dialysis or have kidney problems, as you will need bloodwork before your procedure. The Night before your ERCP with Manometry 1. Do not eat or drink ANYTHING after midnight, including gum/candy or cigarettes. You may take regular PM and AM medications with a small sip of water (though blood thinners and diabetes medications may have to be adjusted). 2. Do not use ANY PAIN MEDICATION within 12 hours of your ERCP (including long or short acting pills, patches, creams, or analgesic lollypops) as it alters the pressure readings. The Day of your ERCP with Manometry 1. Arrive at the Center for Advanced Endoscopy 60 minutes before your ERCP is scheduled. 2. Validated parking is available at the Smilow Cancer Hospital Valet Service. After your ERCP with Manometry 1. You will stay overnight in the hospital for monitoring after the procedure. 2. If you have any increased pain, rectal bleeding, tarry stools, vomiting blood, fever, chills or jaundice please call us immediately at It is your responsibility to call and schedule an X-Ray and upper endoscopy in days from your ERCP to ensure pancreatic stent removal. Following these instructions is very important; not doing so may result in delaying, rescheduling or canceling the procedure. Drs. Jamidar, Aslanian, Farrell & Muniraj want you to have the best procedure experience possible. Please call with any questions, concerns or problems. M-F 8:30 am-4:30 pm at (203) Page 5 July 2017
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
ERCP. Patient Information
 ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
Endoscopy Unit Pyloric and Duodenal Stent insertion
 Endoscopy Unit Pyloric and Duodenal Stent insertion Information for patients Your doctor has recommended that you have a Pyloric or Duodenal Stent Insertion. This leaflet will explain the procedure and
Endoscopy Unit Pyloric and Duodenal Stent insertion Information for patients Your doctor has recommended that you have a Pyloric or Duodenal Stent Insertion. This leaflet will explain the procedure and
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
Patient Gastroscopy Package
 2014 Patient Gastroscopy Package BARRIE ENDOSCOPY 5 Quarry Ridge Road, Barrie, Ontario- L4M 7G1 General Patient Information THE FOLLOWING INFORMATION PERTAINS TO ALL PATIENTS HAVING PROCEDURES AT BARRIE
2014 Patient Gastroscopy Package BARRIE ENDOSCOPY 5 Quarry Ridge Road, Barrie, Ontario- L4M 7G1 General Patient Information THE FOLLOWING INFORMATION PERTAINS TO ALL PATIENTS HAVING PROCEDURES AT BARRIE
Having an ERCP (endoscopic retrograde cholangio pancreatogram)
 Having an ERCP (endoscopic retrograde cholangio pancreatogram) The aim of this information sheet is to help answer some of the questions you may have about having an ERCP. It explains what it is, why it
Having an ERCP (endoscopic retrograde cholangio pancreatogram) The aim of this information sheet is to help answer some of the questions you may have about having an ERCP. It explains what it is, why it
HEALTH SYSTEM UPPER ENDOSCOPY
 Altru HEALTH SYSTEM UPPER ENDOSCOPY It is important to read these instructions upon receiving. Please review the Preparation instructions in the back of this booklet for important information regarding
Altru HEALTH SYSTEM UPPER ENDOSCOPY It is important to read these instructions upon receiving. Please review the Preparation instructions in the back of this booklet for important information regarding
What Is an Endoscopic Ultrasound (EUS)?
 ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
ENDOSCOPIC ULTRASOUND (EUS)
 ENDOSCOPIC ULTRASOUND (EUS) What you need to know before your procedure Your doctor has decided that an EUS is necessary for further evaluation and treatment of your condition. This information sheet has
ENDOSCOPIC ULTRASOUND (EUS) What you need to know before your procedure Your doctor has decided that an EUS is necessary for further evaluation and treatment of your condition. This information sheet has
Having an ERCP. A guide to the test. Information for patients Endoscopy
 Having an ERCP A guide to the test Information for patients Endoscopy Welcome to the Endoscopy Unit Introduction You have been advised by your doctor to have a procedure called ERCP (Endoscopic Retrograde
Having an ERCP A guide to the test Information for patients Endoscopy Welcome to the Endoscopy Unit Introduction You have been advised by your doctor to have a procedure called ERCP (Endoscopic Retrograde
Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) Fax- (760) Preparation for ERCP
 Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for ERCP Patient Name- Procedure Date and Time- Please do not
Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for ERCP Patient Name- Procedure Date and Time- Please do not
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
ERCP investigation of the bile duct and pancreatic duct
 ERCP investigation of the bile duct and pancreatic duct Information for patients ERCP investigation of the bile duct and pancreatic duct 2 ERCP investigation of the bile duct and pancreatic duct 3 INTRODUCTION
ERCP investigation of the bile duct and pancreatic duct Information for patients ERCP investigation of the bile duct and pancreatic duct 2 ERCP investigation of the bile duct and pancreatic duct 3 INTRODUCTION
Patient information/declaration of consent for ERCP (imaging of the bile ducts and pancreas with a contrast substance)
 - 1 - Patient information/declaration of consent for ERCP (imaging of the bile ducts and pancreas with a contrast substance) Declaration of informed consent provided by: Date: Dear Patient, Please be so
- 1 - Patient information/declaration of consent for ERCP (imaging of the bile ducts and pancreas with a contrast substance) Declaration of informed consent provided by: Date: Dear Patient, Please be so
DRAFT. Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect. What is a transjugular intrahepatic portosystemic shunt?
 UW MEDICINE PATIENT EDUCATION Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect This handout explains a transjugular intrahepatic portosystemic shunt and what to expect when
UW MEDICINE PATIENT EDUCATION Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect This handout explains a transjugular intrahepatic portosystemic shunt and what to expect when
Endoscopic Ultrasonography (EUS) Medical Imaging of the Digestive Tract and Internal Organs
 Endoscopic Ultrasonography (EUS) Medical Imaging of the Digestive Tract and Internal Organs More Detailed Pictures for Better Diagnoses Endoscopic ultrasonography allows your doctor to examine your stomach
Endoscopic Ultrasonography (EUS) Medical Imaging of the Digestive Tract and Internal Organs More Detailed Pictures for Better Diagnoses Endoscopic ultrasonography allows your doctor to examine your stomach
What is an Upper GI Endoscopy?
 What is an Upper GI Endoscopy? An upper GI endoscopy is a test your doctor does to see inside part of your digestive system. Your doctor will look at the inside of your esophagus (the tube that links your
What is an Upper GI Endoscopy? An upper GI endoscopy is a test your doctor does to see inside part of your digestive system. Your doctor will look at the inside of your esophagus (the tube that links your
Endoscopic Ultrasound
 Patient & Family Guide Endoscopic Ultrasound 2017 Aussi disponible en français : Endoéchographie (FF85-1793) www.nshealth.ca Endoscopic Ultrasound What is an endoscopic ultrasound? An endoscopic ultrasound
Patient & Family Guide Endoscopic Ultrasound 2017 Aussi disponible en français : Endoéchographie (FF85-1793) www.nshealth.ca Endoscopic Ultrasound What is an endoscopic ultrasound? An endoscopic ultrasound
PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Gastroscopy (Upper GI Endoscopy) Frequently Asked Questions and Preparation
 Gastroscopy (Upper GI Endoscopy) Frequently Asked Questions and Preparation Day of the Procedure Your Procedure has been arranged for: Date: Time: Please report to: Admitting Department ½ hour before procedure.
Gastroscopy (Upper GI Endoscopy) Frequently Asked Questions and Preparation Day of the Procedure Your Procedure has been arranged for: Date: Time: Please report to: Admitting Department ½ hour before procedure.
Having a therapeutic gastroscopy with oesophageal dilatation
 Please telephone the Endoscopy Unit with regards information contained within this leaflet. A member of the nursing team will be glad to advise you. For all general enquiries please use the following contact
Please telephone the Endoscopy Unit with regards information contained within this leaflet. A member of the nursing team will be glad to advise you. For all general enquiries please use the following contact
Endoscopic Mucosal Resection (EMR) & Endoscopic Submucosal Dissection (ESD)
 Endoscopic Mucosal Resection (EMR) & Endoscopic Submucosal Dissection (ESD) Minimally Invasive Polyp Removal IE-02700-Understanding EMR and ESD Brochure_R3.indd 1 Occasionally, a polyp that infiltrates
Endoscopic Mucosal Resection (EMR) & Endoscopic Submucosal Dissection (ESD) Minimally Invasive Polyp Removal IE-02700-Understanding EMR and ESD Brochure_R3.indd 1 Occasionally, a polyp that infiltrates
OGD / Gastroscopy. Patient Information. Introduction
 OGD / Gastroscopy (Oesophago-gastro-duodenoscopy) Patient Information Introduction Your doctor has recommended that you have an OGD. It is your decision, however, whether or not to go ahead with the procedure.
OGD / Gastroscopy (Oesophago-gastro-duodenoscopy) Patient Information Introduction Your doctor has recommended that you have an OGD. It is your decision, however, whether or not to go ahead with the procedure.
Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure
 Patient Education Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure This handout explains what a transjugular intrahepatic portosystemic shunt is and what to expect when you have
Patient Education Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure This handout explains what a transjugular intrahepatic portosystemic shunt is and what to expect when you have
Upper Gastrointestinal Endoscopy -Open Access
 Upper Gastrointestinal Endoscopy - Open Access Facility:... A. INTERPRETER / CULTURAL NEEDS An Interpreter Service is required? Yes No If Yes, is a qualified Interpreter present? Yes No A Cultural Support
Upper Gastrointestinal Endoscopy - Open Access Facility:... A. INTERPRETER / CULTURAL NEEDS An Interpreter Service is required? Yes No If Yes, is a qualified Interpreter present? Yes No A Cultural Support
What Is Peptic Ulcer Disease?
 What Is Peptic Ulcer Disease? Peptic ulcer disease is when painful sores form in the lining of the stomach, duodenum (start of the small intestine) or bowels. An ulcer can cause belly pain and, in some
What Is Peptic Ulcer Disease? Peptic ulcer disease is when painful sores form in the lining of the stomach, duodenum (start of the small intestine) or bowels. An ulcer can cause belly pain and, in some
SURGERY LAPAROSCOPIC ANTI-REFLUX (GORD) SURGERY
 LAPAROSCOPIC ANTI-REFLUX (GORD) If you suffer from heartburn, your surgeon may have recommended Laparoscopic Anti-reflux Surgery to treat this condition, technically referred to as Gastro-oesophageal Reflux
LAPAROSCOPIC ANTI-REFLUX (GORD) If you suffer from heartburn, your surgeon may have recommended Laparoscopic Anti-reflux Surgery to treat this condition, technically referred to as Gastro-oesophageal Reflux
This information will help you prepare for your Barrx ablation procedure at Memorial Sloan Kettering (MSK).
 PATIENT & CAREGIVER EDUCATION About Your Barrx Ablation This information will help you prepare for your Barrx ablation procedure at Memorial Sloan Kettering (MSK). Barrx ablation is a procedure used to
PATIENT & CAREGIVER EDUCATION About Your Barrx Ablation This information will help you prepare for your Barrx ablation procedure at Memorial Sloan Kettering (MSK). Barrx ablation is a procedure used to
Gallstones Information Leaflet THE DIGESTIVE SYSTEM. Gutscharity.org.uk
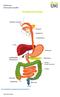 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
Gastroscopy and dilatation/stent insertion
 Gastroscopy and dilatation/stent insertion GI Unit Patient Information Leaflet Introduction This leaflet is for patients who need dilatation of the oesophagus, which means stretching of the food pipe,
Gastroscopy and dilatation/stent insertion GI Unit Patient Information Leaflet Introduction This leaflet is for patients who need dilatation of the oesophagus, which means stretching of the food pipe,
Having an ERCP. Patient Information
 Having an ERCP Patient Information Author ID: NP Leaflet Number: End 004 Version: 6 Name of Leaflet: Having an ERCP Date Produced: January 2017 Review Date: January 2019 Having an ERCP Page 1 of 9 Please
Having an ERCP Patient Information Author ID: NP Leaflet Number: End 004 Version: 6 Name of Leaflet: Having an ERCP Date Produced: January 2017 Review Date: January 2019 Having an ERCP Page 1 of 9 Please
OGD / Gastroscopy (Oesohago-gastro-duodenoscopy) Patient Information
 Introduction Your doctor has recommended that you have an OGD. However, it is your decision whether or not to go ahead with the procedure. This leaflet gives you information about the OGD, its benefits
Introduction Your doctor has recommended that you have an OGD. However, it is your decision whether or not to go ahead with the procedure. This leaflet gives you information about the OGD, its benefits
If you have any questions about the risks of this procedure please ask the endoscopist doing the test or the person who has referred you.
 What is a gastroscopy? A gastroscopy is an examination of the lining of the gullet (oesophagus), stomach, and first part of the small bowel (duodenum). It involves an endoscope (a thin, flexible tube with
What is a gastroscopy? A gastroscopy is an examination of the lining of the gullet (oesophagus), stomach, and first part of the small bowel (duodenum). It involves an endoscope (a thin, flexible tube with
Parathyroidectomy. Surgery for Parathyroid Problems
 Parathyroidectomy Surgery for Parathyroid Problems Why You Need Parathyroid Surgery Has your doctor just recommended that you have parathyroid surgery? If so, you likely have many questions. What are the
Parathyroidectomy Surgery for Parathyroid Problems Why You Need Parathyroid Surgery Has your doctor just recommended that you have parathyroid surgery? If so, you likely have many questions. What are the
What is a Gastroscopy?
 GASTROSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE Why do I need to have a Gastroscopy? You have been advised to undergo
GASTROSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE Why do I need to have a Gastroscopy? You have been advised to undergo
Intranet version. Bradford Teaching Hospitals. NHS Foundation Trust. Having a Gastroscopy. Gastroenterology Unit patient information booklet
 Intranet version Bradford Teaching Hospitals NHS Foundation Trust Having a Gastroscopy Gastroenterology Unit patient information booklet What is a gastroscopy? Gastroscopy is a procedure that allows us
Intranet version Bradford Teaching Hospitals NHS Foundation Trust Having a Gastroscopy Gastroenterology Unit patient information booklet What is a gastroscopy? Gastroscopy is a procedure that allows us
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
Colonic (Large Intestine) Manometry
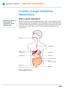 Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Colon Cancer Surgery
 Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Gastroscopy Instructions
 Patient information Gastroscopy Instructions i Important pre operative information for all patients. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Patient information Gastroscopy Instructions i Important pre operative information for all patients. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Laparoscopic Gastric Bypass Information
 1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
National Digestive Diseases Information Clearinghouse
 Upper GI Endoscopy National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is upper gastrointestinal (GI) endoscopy? Upper
Upper GI Endoscopy National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is upper gastrointestinal (GI) endoscopy? Upper
Percutaneous transhepatic cholangiogram (PTC) and biliary drainage. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Percutaneous transhepatic cholangiogram (PTC) and biliary drainage An information guide Percutaneous transhepatic cholangiogram (PTC) and
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Percutaneous transhepatic cholangiogram (PTC) and biliary drainage An information guide Percutaneous transhepatic cholangiogram (PTC) and
Gastroscopy instructions
 Golden Jubilee National Hospital NHS National Waiting Times Centre Gastroscopy instructions Pre operative patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Golden Jubilee National Hospital NHS National Waiting Times Centre Gastroscopy instructions Pre operative patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Endoscopy Unit Having an Oesophageal dilatation
 Endoscopy Unit Having an Oesophageal dilatation Information for patients 2 Your doctor as recommended that you have an Oesophageal Dilatation. This leaflet will explain the procedure and what to expect
Endoscopy Unit Having an Oesophageal dilatation Information for patients 2 Your doctor as recommended that you have an Oesophageal Dilatation. This leaflet will explain the procedure and what to expect
What is a Small Bowel Capsule Endoscopy?
 What is a Small Bowel Capsule Endoscopy? Capsule endoscopy is a way for your doctor to see inside part of your digestive system. A small bowel capsule endoscopy looks at the lining of the small intestine.
What is a Small Bowel Capsule Endoscopy? Capsule endoscopy is a way for your doctor to see inside part of your digestive system. A small bowel capsule endoscopy looks at the lining of the small intestine.
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
North York Endoscopy Instructions
 North York Endoscopy Instructions IMPORTANT INFORMATION: Prior to taking the preparation, please read the details of the procedure, including the risks and benefits. If you agree to the procedure after
North York Endoscopy Instructions IMPORTANT INFORMATION: Prior to taking the preparation, please read the details of the procedure, including the risks and benefits. If you agree to the procedure after
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
PERCUTANEOUS BILIARY DRAINAGE
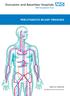 PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
Oesophagogastro. duodenoscopy (OGD)
 Oesophagogastro duodenoscopy (OGD) Information Sheet, Appointment Details and Postal Consent Form Please bring this booklet with you Your Appointment: Date & Day Time Place Daycase & Endoscopy Unit Stamford
Oesophagogastro duodenoscopy (OGD) Information Sheet, Appointment Details and Postal Consent Form Please bring this booklet with you Your Appointment: Date & Day Time Place Daycase & Endoscopy Unit Stamford
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Why Choose Wudassie Diagnostic Center for GI service? Ease of Use: One Location: Reduced Cross-Infection: Focus on the Patient: Reduced Cost:
 Why Choose Wudassie Diagnostic Center for GI service? In our center, patients find that the process much more convenient, as well as more personal. Our center offers a relaxed environment with medical
Why Choose Wudassie Diagnostic Center for GI service? In our center, patients find that the process much more convenient, as well as more personal. Our center offers a relaxed environment with medical
For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU)
 Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
SPHINCTER OF ODDI DYSFUNCTION (SOD)
 SPHINCTER OF ODDI DYSFUNCTION (SOD) Sphincter of Oddi dysfunction refers to structural or functional disorders involving the biliary sphincter that may result in impedance of bile and pancreatic juice
SPHINCTER OF ODDI DYSFUNCTION (SOD) Sphincter of Oddi dysfunction refers to structural or functional disorders involving the biliary sphincter that may result in impedance of bile and pancreatic juice
Upper gastrointestinal endoscopy and colonoscopy
 Upper gastrointestinal endoscopy and colonoscopy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Upper gastrointestinal endoscopy and colonoscopy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Ureteral Stenting and Nephrostomy
 Scan for mobile link. Ureteral Stenting and Nephrostomy Ureteral stenting and nephrostomy help restore urine flow through blocked ureters and return the kidney to normal function. Ureters are long, narrow
Scan for mobile link. Ureteral Stenting and Nephrostomy Ureteral stenting and nephrostomy help restore urine flow through blocked ureters and return the kidney to normal function. Ureters are long, narrow
Treatment for cancer of the gall bladder
 Treatment for cancer of the gall bladder Hepatobiliary Services Information for Patients Liver i Stomach Pancreas Gall bladder Introduction The aim of this booklet is to help you understand more about
Treatment for cancer of the gall bladder Hepatobiliary Services Information for Patients Liver i Stomach Pancreas Gall bladder Introduction The aim of this booklet is to help you understand more about
Undergoing a gastroscopy with colonoscopy
 Page 1 of 9 Undergoing a gastroscopy with colonoscopy Introduction You have been advised to have a gastroscopy and colonoscopy. Other names for these tests are an endoscopy, and you may hear staff refer
Page 1 of 9 Undergoing a gastroscopy with colonoscopy Introduction You have been advised to have a gastroscopy and colonoscopy. Other names for these tests are an endoscopy, and you may hear staff refer
What Is Pancreatitis?
 What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
Endoscopy Unit Treatment of varices
 Endoscopy Unit Treatment of varices Information for patients 2 Your doctor has recommended that you have the Varices (dilated veins) in your oesophagus or stomach treated. This leaflet will explain the
Endoscopy Unit Treatment of varices Information for patients 2 Your doctor has recommended that you have the Varices (dilated veins) in your oesophagus or stomach treated. This leaflet will explain the
PATIENT INFORMATION FROM YOUR SURGEON & SAGES. Laparoscopic Colon Resection
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Colon Resection About Conventional
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Colon Resection About Conventional
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Investigations for Pancreatic, Biliary Tract and Duodenal Cancers
 Investigations for Pancreatic, Biliary Tract and Duodenal Cancers Information for Patients Excellent Care with Compassion 2 The following investigations will help your Cancer Specialist Team decide on
Investigations for Pancreatic, Biliary Tract and Duodenal Cancers Information for Patients Excellent Care with Compassion 2 The following investigations will help your Cancer Specialist Team decide on
This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation.
 Page 1 of 5 Your anaesthetic Introduction This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation. Who is an anaesthetist? Anaesthetists
Page 1 of 5 Your anaesthetic Introduction This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation. Who is an anaesthetist? Anaesthetists
EGD (Esophagogastroduodenoscopy) or Upper Gastrointestinal Endoscopy Exam
 Louis N. Aurisicchio, MD Georgia M. Close, MD Parantap Gupta, MD Robert Mendelsohn, MD Roxan F. Saidi, MD Harvey J. Rosenberg, MD Gastroenterologists Putnam Hospital Center 672 Stoneleigh Avenue Carmel,
Louis N. Aurisicchio, MD Georgia M. Close, MD Parantap Gupta, MD Robert Mendelsohn, MD Roxan F. Saidi, MD Harvey J. Rosenberg, MD Gastroenterologists Putnam Hospital Center 672 Stoneleigh Avenue Carmel,
Frequently Asked Questions
 Frequently Asked Questions I. Questions about your Medications II. Questions about your Prep III. Questions about your Escort IV. Pre-Procedure Questions V. Post-Procedure Questions I. Questions About
Frequently Asked Questions I. Questions about your Medications II. Questions about your Prep III. Questions about your Escort IV. Pre-Procedure Questions V. Post-Procedure Questions I. Questions About
General Surgery. Gallbladder Surgery
 General Surgery Gallbladder Surgery APOLLO_Krames_Spectra_The gallbladder surgery_print_10 May 16.indd 1 5/10/2016 11:50:39 AM A common problem If you have had a painful attack of gallbladder symptoms,
General Surgery Gallbladder Surgery APOLLO_Krames_Spectra_The gallbladder surgery_print_10 May 16.indd 1 5/10/2016 11:50:39 AM A common problem If you have had a painful attack of gallbladder symptoms,
Hepatobiliary investigations
 Hepatobiliary investigations Hepatobiliary Services Information for patients Liver i Stomach Pancreas Gall bladder Introduction You have been referred to the Hepatobiliary Unit. We specialise in procedures
Hepatobiliary investigations Hepatobiliary Services Information for patients Liver i Stomach Pancreas Gall bladder Introduction You have been referred to the Hepatobiliary Unit. We specialise in procedures
LAPAROSCOPIC APPENDICECTOMY
 LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
EASTERN SHORE ENDOSCOPY, LLC (ESE)
 EASTERN SHORE ENDOSCOPY, LLC (ESE) Endoscopy Consent An endoscopy is a medical procedure where your doctor, using a flexible video instrument (endoscope), looks at various areas inside of your body, which
EASTERN SHORE ENDOSCOPY, LLC (ESE) Endoscopy Consent An endoscopy is a medical procedure where your doctor, using a flexible video instrument (endoscope), looks at various areas inside of your body, which
Gastroscopy. GI Unit Patient Information Leaflet
 Gastroscopy GI Unit Patient Information Leaflet Introduction This leaflet is for people who are having a gastroscopy. It gives information on what a gastroscopy is, the benefits and risks of this and what
Gastroscopy GI Unit Patient Information Leaflet Introduction This leaflet is for people who are having a gastroscopy. It gives information on what a gastroscopy is, the benefits and risks of this and what
Esophageal Stent Placement
 PATIENT & CAREGIVER EDUCATION Esophageal Stent Placement This information explains your esophag eal stent placement, including how to prepare for your procedure and how to care for yourself after your
PATIENT & CAREGIVER EDUCATION Esophageal Stent Placement This information explains your esophag eal stent placement, including how to prepare for your procedure and how to care for yourself after your
Aortic and Iliac Artery Occlusive Disease (Updated 10.08)
 S PATIENT INFORMATION oregon surgical specialists Aortic and Iliac Artery Occlusive Disease (Updated 10.08) Abdominal aortic and iliac artery occlusive disease occurs when the arteries in your abdomen
S PATIENT INFORMATION oregon surgical specialists Aortic and Iliac Artery Occlusive Disease (Updated 10.08) Abdominal aortic and iliac artery occlusive disease occurs when the arteries in your abdomen
preparing for an UPPER GI ENDOSCOPY A patient s guide from your doctor and
 preparing for an UPPER GI ENDOSCOPY A patient s guide from your doctor and Your doctor has recommended that you have a medical procedure called upper GI (gastrointestinal) endoscopy to evaluate or treat
preparing for an UPPER GI ENDOSCOPY A patient s guide from your doctor and Your doctor has recommended that you have a medical procedure called upper GI (gastrointestinal) endoscopy to evaluate or treat
Capsule Endoscopy Preparation Instructions
 Capsule Endoscopy Preparation Instructions 1 day before your capsule endoscopy Prior to 2pm - Have your normal breakfast and a light lunch. After 2pm - You must have NO SOLID FOODS and only APPROVED clear
Capsule Endoscopy Preparation Instructions 1 day before your capsule endoscopy Prior to 2pm - Have your normal breakfast and a light lunch. After 2pm - You must have NO SOLID FOODS and only APPROVED clear
Having a gastroscopy A guide for patients and their carers
 Having a gastroscopy A guide for patients and their carers Contents Welcome to the integrated procedures unit....1 Why do I need a gastroscopy?...1 What is the benefit of a gastroscopy?...2 Are there any
Having a gastroscopy A guide for patients and their carers Contents Welcome to the integrated procedures unit....1 Why do I need a gastroscopy?...1 What is the benefit of a gastroscopy?...2 Are there any
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Gastroenterology Darcie Gorman, MD Melvin Kuwahara, MD Joseph T. Merrill, MD Dan A. Collins, MD
 324 E 10th Ave Suite 200 Salt Lake City, UT 84103 801.408.8399 801.408.5152 (fax) Gastroenterology Darcie Gorman, MD Melvin Kuwahara, MD Joseph T. Merrill, MD Dan A. Collins, MD UPPER ENDOSCOPY Thank you
324 E 10th Ave Suite 200 Salt Lake City, UT 84103 801.408.8399 801.408.5152 (fax) Gastroenterology Darcie Gorman, MD Melvin Kuwahara, MD Joseph T. Merrill, MD Dan A. Collins, MD UPPER ENDOSCOPY Thank you
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
Lung Surgery: Thoracoscopy
 Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Gallstones and Cholecystectomy Information Sheet
 Gallstones and Cholecystectomy Information Sheet Gallstones & Cholecystectomy This information sheet desrcibes what they are, the treatment options, and what to expect following a operation. The following
Gallstones and Cholecystectomy Information Sheet Gallstones & Cholecystectomy This information sheet desrcibes what they are, the treatment options, and what to expect following a operation. The following
Endoscopic ultrasound scan
 Endoscopic ultrasound scan GI Unit Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called an endoscopic ultrasound scan (EUS). It gives information on what
Endoscopic ultrasound scan GI Unit Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called an endoscopic ultrasound scan (EUS). It gives information on what
UNC HOSPITALS CHAPEL HILL, NORTH CAROLINA REQUEST AND AUTHORIZATION FOR UPPER GASTROINTESTINAL ENDOSCOPY AND BIOPSY MIM#180
 UNC HOSPITALS CHAPEL HILL, NORTH CAROLINA 27514 REQUEST AND AUTHORIZATION FOR UPPER GASTROINTESTINAL ENDOSCOPY AND BIOPSY MIM#180 I request and authorize and/or associates or assistants of his/her choice
UNC HOSPITALS CHAPEL HILL, NORTH CAROLINA 27514 REQUEST AND AUTHORIZATION FOR UPPER GASTROINTESTINAL ENDOSCOPY AND BIOPSY MIM#180 I request and authorize and/or associates or assistants of his/her choice
Having an Endoscopic Ultrasound
 Having an Endoscopic Ultrasound Information for patients and carers UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having an Endoscopic Ultrasound Information for patients and carers UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Oesophago-Gastro Duodenoscopy (OGD) with Argon Plasma Coagulation (APC)
 South Tyneside NHS Foundation Trust Oesophago-Gastro Duodenoscopy (OGD) with Argon Plasma Coagulation (APC) Patient information booklet Endoscopy Unit Providing a range of NHS services in Gateshead, South
South Tyneside NHS Foundation Trust Oesophago-Gastro Duodenoscopy (OGD) with Argon Plasma Coagulation (APC) Patient information booklet Endoscopy Unit Providing a range of NHS services in Gateshead, South
Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) Fax- (760)
 Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for EGD and/or PEG Placement Patient Name- Procedure Date and
Gary M. Annunziata, D.O., F.A.C.P. / Anh T. Duong, M.D. / Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for EGD and/or PEG Placement Patient Name- Procedure Date and
Tracheal or Bronchial Stent Placement
 PATIENT & CAREGIVER EDUCATION Tracheal or Bronchial Stent Placement This information will help you prepare for your tracheal or bronchial stent placement at Memorial Sloan Kettering (MSK). Many diseases
PATIENT & CAREGIVER EDUCATION Tracheal or Bronchial Stent Placement This information will help you prepare for your tracheal or bronchial stent placement at Memorial Sloan Kettering (MSK). Many diseases
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Drainage UHB is a no smoking Trust
 Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Drainage UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Drainage UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Treatment for early pancreatic cancer
 13 11 20 Information and support Treatment for pancreatic cancer Contents Treatment for early pancreatic cancer Surgery What to expect after surgery Neoadjuvant and adjuvant therapies Treatment for advanced
13 11 20 Information and support Treatment for pancreatic cancer Contents Treatment for early pancreatic cancer Surgery What to expect after surgery Neoadjuvant and adjuvant therapies Treatment for advanced
Robotic-Assisted Laparoscopic Pyeloplasty
 Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
COLONOSCOPY PREPARATION INSTRUCTIONS Osmoprep
 COLONOSCOPY PREPARATION INSTRUCTIONS Osmoprep WHAT IS A COLONOSCOPY? Your physician has recommended that you have a colonoscopy. This test is a visual examination of the lining of the large intestine.
COLONOSCOPY PREPARATION INSTRUCTIONS Osmoprep WHAT IS A COLONOSCOPY? Your physician has recommended that you have a colonoscopy. This test is a visual examination of the lining of the large intestine.
