ACUTE PLEUROPULMONARY COMPLICATIONS DETECTED BY COMPUTED TOMOGRAPHY FOLLOWING MYOCARDIAL REVASCULARIZATION
|
|
|
- Eugenia Lawrence
- 6 years ago
- Views:
Transcription
1 JULY-AUGUST REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 ACUTE PLEUROPULMONARY COMPLICATIONS DETECTED BY COMPUTED TOMOGRAPHY FOLLOWING MYOCARDIAL REVASCULARIZATION Francisco S. Vargas, Kiyomi K. Uezumi, Fabio B. Janete, Mario Terra-Filho, Whady Hueb, Alberto Cukier and Richard W. Light RHCFAP/3085 VARGAS FS et al. - Acute pleuropulmonary complications detected by computed tomography following myocardial revascularization. Rev. Hosp. Clín. Fac. Med. S. Paulo 57(4): , INTRODUCTION: Pleuropulmonary changes are common following coronary artery bypass grafting surgery performed with a saphenous vein graft, with or without an internal mammary artery. The presence of atelectasis or pleural effusions reflects the thoracic trauma. PURPOSE: To define the postoperative incidence of changes in the lung and in the pleural space and to evaluate the influence of the trauma. METHODS: Thirty patients underwent elective coronary artery bypass grafting surgery (8 saphenous vein grafts and 22 saphenous vein grafts and internal mammary artery grafts with pleurotomy). Chest tubes in the left pleural space were used in all internal mammary artery patients. On the second (day 2) and seventh (day 7) postoperative day, patients underwent a computed tomography, and pleural effusions were rated as follows: grade 0 = no fluid to grade 4 = fluid in more than 75% of the hemithorax. Atelectasis was rated as follows: laminar = 1, segmental = 3, and lobar = 10 points. RESULTS: All patients had pleural effusion or atelectasis. Between day 2 and day 7, the number of patients with effusions or atelectasis on the right side decreased (P < 0.05). The incidence of effusions on day 2 in the saphenous vein graft group (87.5%) was higher (P < 0.05) than in the internal mammary artery group (52.3%). The incidence of atelectasis in the lower right lobe decreased (P < 0.05) from 86.7% (day 2) to 26.7% (day 7). The degree of atelectasis in both sides did not differ on day 2 (P = 0.42) but did on day 7 (P < ). There was a decrease in the atelectasis from day 2 to day 7 on the right side (P < 0.001), but not on the left (P = 0.21). On day 2 there was a relationship between atelectasis and effusion on the right (P = 0.04), but not on the left (P = 0.113). CONCLUSION: The present series demonstrates that there is a high incidence of both minimal pleural effusion and atelectasis after coronary artery bypass grafting surgery, which drops on the right side from day 2 to day 7 post surgery. Factors that contribute to the persistence of changes on the left side include the thoracic trauma and the presence of chest tubes and pericardial effusion. DESCRIPTORS: Atelectasis. Pleural effusion. Coronary artery bypass surgery. Pleuropulmonary changes are common following coronary artery bypass grafting (CABG) surgery 1-3. The surgery is performed with a saphenous vein graft (SVG) with or without an internal mammary artery (IMA) graft. The IMA has become the graft conduit of choice because of its improved survival and high long-term patency rate 4. However, the postoperative incidence of pleural changes may be higher in patients who receive an IMA graft. We previously showed that on the seventh postoperative day, the incidence of pleural changes observed on the chest radiograph was about 40% (SVG: 43%; From the Heart Institute (InCor), Hospital das Clínicas, Faculty of Medicine, University of São Paulo, Brazil. IMA: 41%) and by ultrasound is about 80% (SVG: 70%; IMA: 100%), higher than the incidence of atelectasis observed on chest radiograph (about 30%) 1-3. The presence of atelectasis or pleural changes probably reflects the fact that the patient has been subjected to a thoracic trauma and that the intensity of the trauma is higher in IMA pa- 135
2 REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 JULY-AUGUST tients. We hypothesized that the trauma is responsible for these changes. In that case, the patients undergoing left-sided pleurotomy (IMA grafts) should have a higher incidence of complications immediately after the surgery. We further hypothesized that recovery from these changes would take longer in the IMA patients. The purpose of this project was to define the acute postoperative incidence of changes in the lung and pleural space identified by computed tomography and to determine the influence of trauma on the development of these complications. METHODS Table 1 - Subjects and surgery characteristics. Thirty-seven consecutive patients undergoing elective CABG surgery at the Instituto do Coração (FMUSP) were selected for further study. After the surgery, 30 patients were retained on this protocol; 8 had undergone only SVG grafts with no excessive manipulation of the pleura (SVG group), and 22 patients had received at least one IMA graft with pleurotomy in addition to the SVG grafts (IMA group). The remaining 7 patients did not fit the criteria for continuing in the study. Coronary bypass grafting was carried out through a midline sternotomy. Moderate hypothermia (28 o C to 30 o C) was applied, and cardiopulmonary bypass was carried out with a disposable bubble oxygenator. The decision to use SVG or both grafts was made by the operating surgeon. Postoperatively, a small tube was used in all patients to drain the mediastinum. Chest tubes for draining the left pleural space were used in all IMA patients. Only patients with a normal chest radiograph before surgery were included in the study. All subjects underwent computed tomography (CT) 48 hours after surgery (immediately after they had been discharged from the intensive care unit) and on the seventh postoperative day. Computed tomographic scanning was performed on a 4 th generation CT scanner (Tomoscan LX-Philips) with contiguous 10 mm collimation scans through the whole lung field. All images were obtained at the end of inspiration without contrast enhancement. The CT scans were evaluated, and the presence or absence of pleural effusions and atelectasis was recorded. We considered laminar atelectasis to be any linear wedge-shaped parenchymal density without volume loss. Segmental or lobar atelectasis was identified when a trapezoidal or wedge-shaped parenchymal density occupied more than 50% of the corresponding segmental or lobar projection. Volume loss without parenchymal density was not included in this analysis because of difficulties in correct classification 5,6. We evaluated the degree of atelectasis semiquantitatively in each hemithorax by totaling the sums of the scores for lobar atelectasis (10 points per lobe), segmental atelectasis (3 points per segment) and laminar atelectasis (1 point per occurrence). The size of the pleural effusion was evaluated according to the following scale: grade 0 (no pleural fluid present) to grade 4 (pleural fluid occupying more than 75% of hemithorax). Statistical analysis: data are expressed as the mean + standard deviation unless otherwise noted. Chisquare was used for statistical analysis when the proportion in the different groups was compared. Since the semiquantitative data for the atelectasis and pleural effusions were not normally distributed, we used the Mann- Whitney Rank Sum Test to compare groups. Probability values of less than 0.05 were regarded as significant. RESULTS The demographic characteristics of the two groups were very comparable (Table 1). The only significant difference (P < 0.05) was in age, but this was not felt to be clinically important. Only IMA patients received left chest tubes for draining the pleural space; tubes were left in place for hours, and the total volume drained was ml. After CABG surgery, abnormalities on the CT scans were very common Saphenous Vein P < 0.05 Internal Mammary Graft Group Artery Group Demographic Data n 8 22 Gender (M/F) 6/2 17/5 Age (yr) * Weight (kg) Smoke (pack/yr) Times Anesthesia (min) Pump (min) Intubation (min) Left Chest Tube (hs) Drained Volume Mediastinum (ml) Left Pleural Space (ml)
3 JULY-AUGUST REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 Table 2 - Incidence of pleural effusion and atelectasis on Computed Tomography scan 2 and 7 days post-coronary artery bypass grafting surgery. Saphenous Vein Internal Mammary TOTAL Graft Group (n = 8) Artery Group (n = 22) (n = 30) PLEURAL EFFUSION Right Hemithorax 2 nd day 7 (87.5%) 10 (45.5%) 17 (56.7%) 7 th day 3 (37.5%) 4 (18.2%) 7 (23.3%) Left Hemithorax 2 nd day 7 (87.5%) 13 (59.1%) 20 (66.7%) 7 th day 4 (50.0%) 15 (68.2%) 19 (63.3%) ATELECTASIS Right Hemithorax 2 nd day 6 (75.0%) 20 (90.1%) 26 (86.7%) 7 th day 2 (25.0%) 7 (31.8%) 9 (30.0%) Left Hemithorax 2 nd day 6 (75.0%) 20 (90.1%) 26 (86.7%) 7 th day 5 (62.5%) 21 (95.5%) 26 (86.7%) (Table 2). All of the patients had either pleural effusion or atelectasis on the second postoperative day (day 2), and all but one IMA patient had an abnormal exam on the seventh postoperative day (day 7). Pleural effusions: There was a high incidence of pleural effusions following CABG surgery (Table 2). On day 2, 17 (56.7%) of the patients had effusions on the right side and 20 (66.7%) on the left side; 15 (50.0%) of the patients had bilateral effusions. Between day 2 and day 7, the number of patients with effusions on the right side decreased, while the number of effusions on the left side stayed almost the same. The right side differed significantly from the left (X 2 = 10.3, P < 0.01). This difference was primarily due to the fact that the effusions on the left persisted in the IMA group. The incidence of pleural effusion in the SVG (87.5%) group tended to be higher on day 2 than in the IMA (52.3%) group (14/16 sides vs 23/44 sides, X 2 = 5.11, P < 0.05). However, by day 7, the incidence of pleural effusion did not differ significantly (7/ 16 sides vs 19/44 sides, X 2 = 0.06, P = 0.79). All pleural effusions were small (Table 3). On the right side on both day 2 and day 7, all the effusions (24/ 30) were classified as grade 1, with the fluid occupying only the costophrenic Table 3 - Semiquantitative evaluation of pleural effusions. PLEURAL EFFUSION angle. On the left side, only 2 pleural effusions (2/20; 10%) in the SVG group were graded as 2 (small pleural effusion) on the day 2. However, the incidence of grade 2 effusions on day 7 increased to 8/19 (42%). Only 1 patient (1/8; 12.5%) with effusion grade 2 was in the SVG group; 7 patients (7/ 8; 87.5%) were in the IMA group. Atelectasis: The incidence of atelectasis was even higher than the incidence of pleural effusion following CABG surgery (Table 2). On day 2, 26 (86.7%) of the patients had atelectasis on the right side, and 26 (86.7%) of the patients had atelectasis on the left side. Bilateral atelectasis were present in 24 (80%) patients. Between day 2 and day 7, the number of patients with atelectasis on the right side decreased, while the number of patients with atelectasis on the left remained constant. The differences in the two sides were statistically significant (X 2 = 22.4, P < 0.001). The incidence of atelectasis Saphenous Vein Internal Mammary TOTAL Graft Group (n = 8) Artery Group (n = 22) (n = 30) Grade Total Grade Total Grade Total Right Hemithorax 2 nd day th day Left Hemithorax 2 nd day th day Table 4 - Incidence of lower lobe atelectasis on Computed Tomography scan, 2 and 7 days post- coronary artery bypass grafting surgery. Saphenous Vein Internal Mammary TOTAL Graft Group (n = 8) Artery Group (n = 22) (n = 30) RIGHT LOWER LOBE 2 nd day 5 (62.5%) 21 (95.5%) 26 (86.7%) 7 nd day 2 (25.0%) 6 (27.3%) 8 (26.7%) LEFT LOWER LOBE 2 nd day 6 (75.0%) 20 (90.9%) 26 (86.7%) 7 nd day 4 (50.0%) 19 (86.4%) 23 (76.7%) 137
4 REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 JULY-AUGUST was comparable in the two groups on both day 2 and day 7. Almost all the atelectasis were in the lower lobe (Table 4). The incidence in the right lower lobe decreased significantly (P < 0.05) from 86.7% (26/30) on day 2 to 26.7% (8/30) on day 7. The incidence on the left side was similar (P > 0.05) on day 2 (26/ 30; 86.7%) but did not decrease significantly as it did on the right side either in the SVG group or in the IMA group (23/30; 76.7%). Since the atelectasis varied from lobar atelectasis to laminar atelectasis, we also analyzed the degree of atelectasis semiquantitatively. When atelectasis were analyzed in this manner (Table 5), we found that the degree of atelectasis in the two sides did not differ significantly (P = 0.42) on day 2, but it did differ significantly on day 7 (P < ). There was a significant decrease in the amount of atelectasis from day 2 to day 7 on the right side (P < 0.001), but there was no significant decrease in the amount of atelectasis from day 2 to day 7 on the left side (P = 0.21). Relationship between pleural effusion and atelectasis: There appeared to be a significant relationship between the occurrence of atelectasis and pleural effusion. On day 2 there was a significant correlation between the degree of atelectasis and the degree of pleural effusion on the right (r = 0.38, P = 0.04), but not on the left (r = 0.295, P = 0.113). However, between day 2 and day 7, there was a significant relationship between changes in the degree of atelectasis and the degree of pleural effusion (r = 0.53, P = ). On day 7 there was not a significant correlation between atelectasis and pleural effusion on either the right (r = , P = 0.91) or on the left (r = 0.198, P = 0.29). DISCUSSION Table 5 - Semiquantitative evaluation of atelectasis. Saphenous Vein Internal Mammary TOTAL Graft Group (n = 8) Artery Group (n = 22) (n = 30) Right Hemithorax 2 nd day th day Left Hemithorax 2 nd day th day The present series demonstrates that there is a high incidence of both pleural effusion and atelectasis after coronary artery bypass surgery. The predominance was of minimal pleural effusions that reduced in incidence on the right side from day 2 to day 7. Similar results were found concerning atelectasis; high incidence of laminar atelectasis was observed in the lower lobes on day 2. This incidence was reduced on the right side on day 7. The incidence of pleural effusion in the present series is about 65% on both day 2 and day 7. This incidence is substantially higher than the 43% reported previously 1 and lower than the nearly 90% observed subsequently from the same institution 2. The probable explanation for the differences in the 3 reports is that the presence of pleural effusion was assessed only via chest radiograph in the first paper, while it was assessed by ultrasound in the second, and by computed tomography in the present study. Therefore, the nearly 65% incidence of pleural effusions in the present study could reflect an improvement in surgical technique. The explanation for the occurrence of pleural effusion after CABG surgery is unknown, but there are several possibilities. First, the pleural effusion could be secondary to pulmonary edema, either cardiogenic, caused by heart failure, or noncardiogenic, caused by acute injury of the lung after cardiopulmonary bypass. An inflammatory response from contact activation triggers a cascade of cytokines that retain activated blood cells in the pulmonary circulation 7. Additionally, reperfusion injury in cold and ischemic lung tissue generates oxygen free radicals that modify the vascular permeability. In the other hand, fluid administration during cardiopulmonary bypass is dictated by the need to maintain adequate perfusion flow and reservoir volume. Sequestration of volume in the extravascular space reduces venous return and mandates replenishment through the cardiopulmonary bypass apparatus. Therefore, changes in volume may reflect the permeability of the vascular membrane; the increased vascular permeability resulting from these processes causes diffuse pulmonary edema and pleural effusion 8. In general, pleural effusions caused by pulmonary edema either from heart failure or from acute lung injury are bilateral and approximately equal in size 9. In our opinion, pulmonary edema could be an important causative factor for the effusions, since 50% of the effusions on the day 2 day were bilateral. However, the reduction of the cardiac function causing a pleural effusion should be considered a remote possibility. Our patients did not present evidence of heart failure, and in our previous study in a similar population, the left ventricular ejection fraction 7 days after the surgery was normal 2 ; moreover, most of our patients 138
5 JULY-AUGUST REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 (92%) were in functional class 1 preoperatively. If some degree of heart failure is present immediately after the surgery, the reduction in the heart function should be short-lived, given that in the present series, the incidence of bilateral pleural effusion on the day 7 was only 16.7% (5/30). Therefore, if it exists, cardiac failure caused by surgical trauma rapidly improves, and heart function returns to normal values during the first postoperative days resulting in the absorption of the pleural fluid. Second, the postcardiac injury syndrome has been suggested as an adjuvant to the formation of pleural effusions. We feel this possibility is unlikely, since the syndrome is usually manifested after the second or third week of surgery 10. Third, the lymphatic drainage from the pleural space could be decreased postoperatively, particularly in patients who received an IMA graft. During the mobilization of the IMA pedicle, the associated lymphatics are transected. This disruption could be expected to decrease the lymphatic clearance from the pleural space and result in the accumulation of pleural fluid 11. We believe that this explanation is unlikely, since the incidence of pleural effusion on day 2 tended to be higher in the SVG group. Fourth, the presence of a chest tube could have led to a pleural inflammation and the development of the effusion. The results of the present study offer no support for this hypothesis. Fifth, the performance of pleurotomy could have led to the accumulation of pleural fluid. The trauma during surgery could have damaged the thoracic structures and in particular the pleura such that the rate of pleural fluid formation was increased or the rate of fluid absorption was decreased or both. Previous studies assessing the relationship between pleurotomy and postoperative pleural effusions have been in conflict The present study does not provide any support for the contention that pleural effusions are related to the performance of pleurotomy. Even though all patients in the IMA group underwent pleurotomy, the incidence of pleural effusion was no greater in this group. Sixth, the pleural effusion could be related to the pericardial inflammation. A possibility exists that the pericardial fluid flows directly into the pleural space, since Fukuo et al. 14 showed the presence of numerous small fenestrations, which provide direct communication between the pericardial and the pleural cavities. Ikaheimo et al. 15 demonstrated pericardial effusion by echocardiography in 63% of their patients 1 week after cardiac surgery. However, we previously demonstrated that there was no association between the presence of pleural and pericardial effusion but that the persistence of pericardial effusion was related to a persistence of a pleural effusion in the IMA group 2. It is interesting to observe in the present series that the incidence of left pleural effusion in the IMA group did not decrease from day 2 (59.1%) to day 7 (68.2%). Two factors should be considered in the explanation of the persistence of a left pleural effusion on day 7. First, the chest tubes are removed on day 2, allowing the accumulation of fluid into the pleural cavity, and second, pericardial effusion persisted. Seventh, the development of a pleural effusion could be related to the presence of atelectasis, the most common pulmonary complication after cardiac surgery (up to 70%) and more prominent in the dependent portions of the lung 16. Surgical procedures including anesthesia during CAGB surgery with cardiopulmonary bypass significantly affect the mechanical properties of the lungs. Before cardiopulmonary bypass, the patient is subjected to sternotomy and chest wall retraction for surgical exposure. Pleurotomy, required for harvesting the internal mammary artery, produces a partial pneumothorax. During cardiopulmonary bypass, to allow cardiac asystole and surgical repair, the lungs are not ventilated and remain collapsed, below functional residual capacity; after cardioplegic arrest, pulmonary blood flow ceases. These changes facilitate the production of atelectasis and pulmonary edema 17. For these reasons, the development of pleural effusions could be related to the presence of atelectasis. A previous study 18 showed that following abdominal surgery, pleural effusions were more common if atelectasis was present. Atelectasis has been recognized as a common postoperative complication after open-heart surgery. Wilcox et al. 19 found roentgenographic evidence of atelectasis on the first postoperative day in 87.7% of the patients. Hurlbut et al. 11 reported with the same methodology an incidence of nearly 50% on day 2, decreasing to approximately 40% six days after the surgery. Recently, Daganou et al. 20 reported evidence of atelectasis on chest radiographs in 51% of patients on the first postoperative day and in 25% on the fourth postoperative day. However, in the present study as well as in the study by Gale et al. 21, there was no a clear relationship between the presence of atelectasis and the development of effusion. From this study, we concluded that in these patients undergoing CABG surgery, the incidence of pleural effusion observed via computed tomography was about 65% both on day 2 and day 7, and most of the pleural effusions were minimal. The incidence of pleural effusion on the right side dropped from day 2 (56.7%) to day 7 (23.3%). However, on the left side, the incidence did not change. The factors involved in the persistence of the left effusion 139
6 REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 JULY-AUGUST included the previous removal of the chest tubes and the probable persistence of a pericardial effusion. No differences were observed between the SVG and IMA groups. The evaluation of atelectasis showed similar results. There was a high incidence of atel- ectasis (86.7%), mainly the laminar type, on the lower lobes, with no differences between the right and left lung or between the SVG group and IMA group. The incidence of atelectasis dropped on the right side from 86.7% (day 2) to 30.0% (day 7) but not on the left side (86.7% on both days). These postoperative pleuropulmonary changes were caused by thoracic trauma, in particular by the effects of the inflammatory response to the cardiopulmonary bypass. RESUMO RHCFAP/3085 VARGAS FS e col. - Cirurgia de revascularização do miocárdio: complicações pleuro-pulmonares agudas caracterizadas por tomografia computadorizada de tórax. Rev. Hosp. Clín. Fac. Med. S. Paulo 57(4): , INTRODUÇÃO: O comprometimento pleuro-pulmonar é freqüente após cirurgia de revascularização do miocárdio independente do uso de veia safena ou de artéria mamária interna. A presença de atelectasias e derrame pleural tem sido atribuída ao trauma torácico. OBJETIVOS: Definir a incidência do comprometimento pleuro-pulmonar observado através de tomografia computadorizada, analisando a influência do trauma no desenvolvimento destas complicações. MÉTODOS: Trinta pacientes foram submetidos a cirurgia eletiva de revascularização do miocárdio (8 safena e 22 também mamária com pleurotomia). Foi drenada a cavidade pleural esquerda de todos os pacientes do grupo mamária. Realizada Tomografia Computadorizada do tórax no 2 o e 7 o dias pós-op, avaliando-se o derrame pleural (0: sem líquido e 4: derrame em mais de 75% do 140
7 JULY-AUGUST REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 hemitórax) e atelectasias (laminar: 1, segmentar: 3 e lobar: 10 pontos). RESULTADOS: Todos os pacientes apresentaram derrame pleural ou atelectasia. Entre o 2 o e o 7 o dia, o número de pacientes com derrame ou com atelectasia, no lado direito, diminuiu (p < 0.05). A prevalência de derrames, no 2 o dia, no grupo safena, (87.5%) foi maior (p < 0.05) do que no grupo mamária (52.3%). A prevalência de atelectasias no lobo inferior direito diminuiu (p < 0.05) de 86.7% (2 o dia) para 26.7% (7 o dia). O grau de atelectasias, em ambos os lados, não diferiu no dia 2 (p = 0,42) mas sim no dia 7 (p < ). Houve diminuição das atelectasias do dia 2 para o 7, à direita (p < 0.001), mas não à esquerda (p = 0.21). Houve correlação (dia 2) entre as atelectasias e os derrames à direita (p = 0.04), mas não à esquerda (p = 0.113). CONCLUSÃO: Este estudo evidencia alta prevalência de derrame pleural e atelectasias após cirurgia de revascularização do miocárdio, que se reduz à direita no 7 o dia de pós-operatório. Os fatores envolvidos na persistência das alterações à esquerda incluem o maior trauma torácico, ressaltando-se a drenagem e a presença de derrame pericárdico. DESCRITORES: Atelectasia. Derrame pleural. Cirurgia de revascularização do miocardio. REFERENCES 1. PENG MJ, VARGAS FS, CUKIER A et al. - Postoperative pleural changes after coronary revascularization. Comparison between saphenous vein and internal mammary artery grafting. Chest 1992;101: VARGAS FS, CUKIER A, HUEB W et al. - Relationship between pleural effusion and pericardial involvement after myocardial revascularization. Chest 1994;105: VARGAS FS, CUKIER A, TERRA-FILHO M et al. - Influence of atelectasis on pulmonary function after coronary artery bypass grafting. Chest 1993;104: ANGELINI GD, BRYAN AJ, WEST RR et al. - Coronary artery bypass surgery: current practice in the United Kingdom. Thorax 1989;44: NAIDICH DP, ZERHOUNI EA & SIEGELMAN SS - Lobar collapse. In: Computed tomography and magnetic resonance of the thorax. 2 nd ed. New York, Raven Press p WEBB WR, MÜLLER NL & NAIDICH DP - HRCT findings of lung disease. In: High-resolution CT of the lung. New York, Raven Press, p MASSOUDY P, ZAHLER S, BECKER BF et al. - Evidence of inflammatory responses of the lungs during coronary artery bypass grafting with cardiopulmonary bypass. Chest 2001;119: GILBERT TB, BARNAS GM & SEQUEIRA AJ - Impact of pleurotomy, continuous positive airway pressure and fluid balance during cardiopulmonary bypass on lung mechanics and oxygenation. J Cardiothorac Vasc Anesth 1996;7: WEISS JM & SPODICK DH - Laterality of pleural effusions in chronic congestive heart failure. Am J Cardiology 1984;53: LIGHT RW - Pleural effusion due to miscellaneous disease. In: LIGHT RW. Pleural disease. 3 nd ed. Philadelphia, Lea,
8 REV. HOSP. CLÍN. FAC. MED. S. PAULO 57(4): , 2002 JULY-AUGUST 11.HURLBUT D, MYERS ML, LEFCOE M et al. - Pleuropulmonary morbidity: Internal thoracic artery versus saphenous vein graft. Ann Thorac Surg 1991;50: LANDYMORE RW & HOWELL F - Pulmonary complications following myocardial revascularization with the internal mammary artery graft. European J Cardiothorac Surg 1990;4: OLEARCHYK AS & MAGOVERN GJ - Internal mammary artery grafting. J Thorac Cardiovasc Surg 1986;92: FUKUO Y, NAKATANI T, SHINOHARA H et al. - Pericardium of rodents: pores connect the pericardial and pleural cavities. Anat Res 1988; 220: IKAHEIMO MJ, HUIKURI HV, AIRAKSINEN J et al. - Pericardial effusion after cardiac surgery: Incidence, relation to the type of surgery, antithrombotic therapy and early coronary bypass graft patency. Am Heart J 1988;116: SLADEN RN & BERKOWITZ DE - Cardiopulmonary bypass and the lungs. In: GRAVLEE GP, DAVIS RF & UTLEY JR. Cardiopulmonary bypass. Baltimore, Williams & Wilkins, BARNAS GM, WATSON RJ, GREEN MD et al. - Lung and chest wall mechanical properties before and after cardiac surgery with cardiopulmonary bypass. J Appl Physiol 1994;76: LIGHT RW & GEORGE RB - Incidence and significance of pleural effusion after abdominal surgery. Chest 1976;69: WILCOX P, BAILE EM, HARDS J et al. - Phrenic nerve function and its relationship to atelectasis after coronary artery bypass surgery. Chest 1988;93: DAGANOU M, DIMOPOULOU I, MICHALOPOULOS N et al. - Respiratory complications after coronary artery bypass surgery with unilateral or bilateral internal mammary artery grafting. Chest 1998;113: GALE GD, TEASADALE SJ, SANDERS DE et al. - Pulmonary atelectasis and other respiratory complications after cardiopulmonary bypass and investigation of aetiological factors. Canad Anaesth Soc J 1979;26: Received for publication on September 04,
Evaluation of routine postoperative chest X-rays in the management of the cardiac surgical patient 1
 European Journal of Cardio-thoracic Surgery 12 (1997) 72 729 Evaluation of routine postoperative chest X-rays in the management of the cardiac surgical patient 1 Podila Sita Rama Rao *, Qamar Abid, Khalid
European Journal of Cardio-thoracic Surgery 12 (1997) 72 729 Evaluation of routine postoperative chest X-rays in the management of the cardiac surgical patient 1 Podila Sita Rama Rao *, Qamar Abid, Khalid
Alfonso Fiorelli 1, Francesco Caronia 2, Aldo Prencipe 3, Mario Santini 1, Brendon Stiles 4. Evidenced-Based Clinical Problem Solving Article
 Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Immediate pulmonary dysfunction in ischemic heart disease patients undergoing off-pump versus on-pump CABG
 Available online at www.sciencedirect.com ScienceDirect Journal of the Egyptian Society of Cardio-Thoracic Surgery 24 (2016) 15e20 http://www.journals.elsevier.com/journal-of-the-egyptian-society-of-cardio-thoracic-surgery/
Available online at www.sciencedirect.com ScienceDirect Journal of the Egyptian Society of Cardio-Thoracic Surgery 24 (2016) 15e20 http://www.journals.elsevier.com/journal-of-the-egyptian-society-of-cardio-thoracic-surgery/
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Pleural effusion occurs in up to 89% of patients
 Symptomatic Persistent Post-Coronary Artery Bypass Graft Pleural Effusions Requiring Operative Treatment* Clinical and Histologic Features Y. C. Gary Lee, MBChB; Marcelo A. C. Vaz, MD; Kim A. Ely, MD;
Symptomatic Persistent Post-Coronary Artery Bypass Graft Pleural Effusions Requiring Operative Treatment* Clinical and Histologic Features Y. C. Gary Lee, MBChB; Marcelo A. C. Vaz, MD; Kim A. Ely, MD;
Unilateral pulmonary oedema, a forgotten presentation.
 Unilateral pulmonary oedema, a forgotten presentation. Poster No.: C-2146 Congress: ECR 2018 Type: Educational Exhibit Authors: C. A. Arboleda Vallejo, M. I. carvajal, M. Perez ; Medellin, 1 2 1 1 2 Antioquia/CO,
Unilateral pulmonary oedema, a forgotten presentation. Poster No.: C-2146 Congress: ECR 2018 Type: Educational Exhibit Authors: C. A. Arboleda Vallejo, M. I. carvajal, M. Perez ; Medellin, 1 2 1 1 2 Antioquia/CO,
Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis?
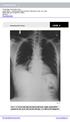 1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
1 Interpreting Chest X-Rays CASE 1 Fig. 1.1 Case 1. A 35-year-old male presented with fever, cough, and purulent sputum for one week. This was his CXR (Fig. 1.1). What is the diagnosis? CASE 1 Interpreting
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Effect of using pump on postoperative pleural effusion in the patients that underwent CABG
 Özülkü M & Aygün ORIGINAL F - Effect ARTICLE of using pump on postoperative pleural effusion Effect of using pump on postoperative pleural effusion Efeito da circulação extracorpórea no derrame pleural
Özülkü M & Aygün ORIGINAL F - Effect ARTICLE of using pump on postoperative pleural effusion Effect of using pump on postoperative pleural effusion Efeito da circulação extracorpórea no derrame pleural
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
OPCABG for Full Myocardial Revascularisation How we do it
 OPCABG for Full Myocardial Revascularisation How we do it 28 th SHA Conferance Dr.Farouk Oueida Head of Cardiac Surgery Dept. SBCC-Dammam KSA The Less Invasive CABG Full Revascularisation Full Sternotomy
OPCABG for Full Myocardial Revascularisation How we do it 28 th SHA Conferance Dr.Farouk Oueida Head of Cardiac Surgery Dept. SBCC-Dammam KSA The Less Invasive CABG Full Revascularisation Full Sternotomy
Respiratory Complications After Coronary Artery Bypass Surgery With Unilateral or Bilateral Internal Mammary Artery Grafting*
 Respiratory Complications After Coronary Artery Bypass Surgery With Unilateral or Bilateral Internal Mammary Artery Grafting* Maria Daganou, MD; Joanna Dinwpoulou, MD; Nickolaos Michalopoulos, MD; Konstantinos
Respiratory Complications After Coronary Artery Bypass Surgery With Unilateral or Bilateral Internal Mammary Artery Grafting* Maria Daganou, MD; Joanna Dinwpoulou, MD; Nickolaos Michalopoulos, MD; Konstantinos
Pulmonary function may decrease significantly after
 Effects of Minimal Invasive Coronary Artery Bypass on ulmonary Function and ostoperative ain Artur Lichtenberg, MD, Christian Hagl, MD, Wolfgang Harringer, MD, Uwe Klima, MD, and Axel Haverich, MD Division
Effects of Minimal Invasive Coronary Artery Bypass on ulmonary Function and ostoperative ain Artur Lichtenberg, MD, Christian Hagl, MD, Wolfgang Harringer, MD, Uwe Klima, MD, and Axel Haverich, MD Division
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Retrospective Study Of Redo Cardiac Surgery In A Single Centre. R Karthekeyan, K Selvaraju, L Ramanathan, M Rakesh, S Rao, M Vakamudi, K Balakrishnan
 ISPUB.COM The Internet Journal of Anesthesiology Volume 12 Number 2 Retrospective Study Of Redo Cardiac Surgery In A Single Centre R Karthekeyan, K Selvaraju, L Ramanathan, M Rakesh, S Rao, M Vakamudi,
ISPUB.COM The Internet Journal of Anesthesiology Volume 12 Number 2 Retrospective Study Of Redo Cardiac Surgery In A Single Centre R Karthekeyan, K Selvaraju, L Ramanathan, M Rakesh, S Rao, M Vakamudi,
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
B-I-2 CARDIAC AND VASCULAR RADIOLOGY
 (YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
(YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
Assignable revenue codes: Explanation of services:
 computed tomography Chest/Cardiac Assignable revenue codes: Explanation of services: 0350 CT Scan General Classification 0351 CT Scan Head Scan 0352 CT Scan Body Scan 0359 CT Scan Other CT Scans Known
computed tomography Chest/Cardiac Assignable revenue codes: Explanation of services: 0350 CT Scan General Classification 0351 CT Scan Head Scan 0352 CT Scan Body Scan 0359 CT Scan Other CT Scans Known
On-Pump vs. Off-Pump CABG: The Controversy Continues. Miguel Sousa Uva Immediate Past President European Association for Cardiothoracic Surgery
 On-Pump vs. Off-Pump CABG: The Controversy Continues Miguel Sousa Uva Immediate Past President European Association for Cardiothoracic Surgery On-pump vs. Off-Pump CABG: The Controversy Continues Conflict
On-Pump vs. Off-Pump CABG: The Controversy Continues Miguel Sousa Uva Immediate Past President European Association for Cardiothoracic Surgery On-pump vs. Off-Pump CABG: The Controversy Continues Conflict
Phrenic Nerve Injury Associated With High Free Right Internal Mammary Artery Harvesting
 Phrenic Nerve Injury Associated With High Free Right Internal Mammary Artery Harvesting Yongzhi Deng, MD, Karen Byth, PhD, and Hugh S. Paterson, FRACS Department of Cardiothoracic Surgery, Westmead Hospital,
Phrenic Nerve Injury Associated With High Free Right Internal Mammary Artery Harvesting Yongzhi Deng, MD, Karen Byth, PhD, and Hugh S. Paterson, FRACS Department of Cardiothoracic Surgery, Westmead Hospital,
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
SBCCV BOLETIM CIENTÍFICO
 03 2018 BOLETIM CIENTÍFICO SBCCV Editores: Dr. Domingo Marcolino Braile Dr. Fernando Ribeiro de Moraes Neto Dr. Luciano Cabral Albuquerque Dr. Orlando Petrucci Junior Dr. Walter José Gomes J Am Coll Cardiol
03 2018 BOLETIM CIENTÍFICO SBCCV Editores: Dr. Domingo Marcolino Braile Dr. Fernando Ribeiro de Moraes Neto Dr. Luciano Cabral Albuquerque Dr. Orlando Petrucci Junior Dr. Walter José Gomes J Am Coll Cardiol
Ischemic Mitral Valve Disease: Repair, Replace or Ignore?
 Ischemic Mitral Valve Disease: Repair, Replace or Ignore? Fabio B. Jatene Full Professor of Cardiovascular Surgery, Medical School, University of São Paulo, Brazil DISCLOSURE I have no financial relationship
Ischemic Mitral Valve Disease: Repair, Replace or Ignore? Fabio B. Jatene Full Professor of Cardiovascular Surgery, Medical School, University of São Paulo, Brazil DISCLOSURE I have no financial relationship
Early chest tube removal after coronary artery bypass graft surgery
 Original Article OPEN ACCESS Early chest tube removal after coronary artery bypass graft surgery Mohsen Mirmohammad-Sadeghi, MD 1, Ali Etesampour, MD 2, Mojgan Gharipour, MSc 3, Zeinab Shariat, MD 4 Peyman
Original Article OPEN ACCESS Early chest tube removal after coronary artery bypass graft surgery Mohsen Mirmohammad-Sadeghi, MD 1, Ali Etesampour, MD 2, Mojgan Gharipour, MSc 3, Zeinab Shariat, MD 4 Peyman
Surgical myocardial revascularization versus stents
 ORIGINAL RESEARCH Surgical myocardial revascularization versus stents Jose Carlos Rossini Iglezias, Alex Chi, Luis Alberto Oliveira Dallan, Luis Felipe Pinho Moreira, Fabio Biscegli Jatene Instituto do
ORIGINAL RESEARCH Surgical myocardial revascularization versus stents Jose Carlos Rossini Iglezias, Alex Chi, Luis Alberto Oliveira Dallan, Luis Felipe Pinho Moreira, Fabio Biscegli Jatene Instituto do
Postoperative Phrenic Nerve Palsy
 Postoperative Phrenic Nerve Palsy in Patients with Open-Heart Surgery Omkar N. Markand, M.D., F.R.C.P.(C), S. S. Moorthy, M.D., Yousuf Mahomed, M.D., Robert D. King, M.D., and John W. Brown, M.D. ABSTRACT
Postoperative Phrenic Nerve Palsy in Patients with Open-Heart Surgery Omkar N. Markand, M.D., F.R.C.P.(C), S. S. Moorthy, M.D., Yousuf Mahomed, M.D., Robert D. King, M.D., and John W. Brown, M.D. ABSTRACT
Lung-Volume Reduction Surgery ARCHIVED
 Lung-Volume Reduction Surgery ARCHIVED Policy Number: Original Effective Date: MM.06.008 04/15/2005 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST 03/22/2013 Section: Surgery Place(s) of
Lung-Volume Reduction Surgery ARCHIVED Policy Number: Original Effective Date: MM.06.008 04/15/2005 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST 03/22/2013 Section: Surgery Place(s) of
Prophylactic respiratory physiotherapy after cardiac surgery
 Prophylactic respiratory physiotherapy after cardiac surgery Patrick Pasquina; Martin R Tramèr, MD, D. Phil; Bernhard Walder, MD Divisions of Surgical Intensive Care (Mr Pasquina) and Anaesthesia (Drs
Prophylactic respiratory physiotherapy after cardiac surgery Patrick Pasquina; Martin R Tramèr, MD, D. Phil; Bernhard Walder, MD Divisions of Surgical Intensive Care (Mr Pasquina) and Anaesthesia (Drs
Influence of Pleurotomy on Pulmonary Function After Off-Pump Coronary Artery Bypass Grafting
 Influence of Pleurotomy on Pulmonary Function After Off-Pump Coronary Artery Bypass Grafting CARDIOVASCULAR Solange Guizilini, PhD, Walter J. Gomes, MD, PhD, Sonia M. Faresin, MD, PhD, Douglas W. Bolzan,
Influence of Pleurotomy on Pulmonary Function After Off-Pump Coronary Artery Bypass Grafting CARDIOVASCULAR Solange Guizilini, PhD, Walter J. Gomes, MD, PhD, Sonia M. Faresin, MD, PhD, Douglas W. Bolzan,
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
X-Rays. Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady
 X-Rays Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady CHEST X-RAYS Normal Chest X-ray Comments on chest X ray includes examination of 1- Bony cage (ribs,clavicles &vertebral column
X-Rays Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady CHEST X-RAYS Normal Chest X-ray Comments on chest X ray includes examination of 1- Bony cage (ribs,clavicles &vertebral column
Myocardial enzyme release after standard coronary artery bypass grafting
 Cardiopulmonary Support and Physiology Schachner et al Myocardial enzyme release in totally endoscopic coronary artery bypass grafting on the arrested heart Thomas Schachner, MD, a Nikolaos Bonaros, MD,
Cardiopulmonary Support and Physiology Schachner et al Myocardial enzyme release in totally endoscopic coronary artery bypass grafting on the arrested heart Thomas Schachner, MD, a Nikolaos Bonaros, MD,
Interpreting thoracic x-ray of the supine immobile patient: Syllabus
 Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kang D-H, Kim Y-J, Kim S-H, et al. Early surgery versus conventional
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kang D-H, Kim Y-J, Kim S-H, et al. Early surgery versus conventional
Cost-effectiveness of minimally invasive coronary artery bypass surgery Arom K V, Emery R W, Flavin T F, Petersen R J
 Cost-effectiveness of minimally invasive coronary artery bypass surgery Arom K V, Emery R W, Flavin T F, Petersen R J Record Status This is a critical abstract of an economic evaluation that meets the
Cost-effectiveness of minimally invasive coronary artery bypass surgery Arom K V, Emery R W, Flavin T F, Petersen R J Record Status This is a critical abstract of an economic evaluation that meets the
CEU Final Exam for Code It! Sixth Edition
 CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
CEU Final Exam for 3-2-1 Code It! Sixth Edition Note to CEU applicant In order to receive CEU credit for taking this exam, the following criteria must be met: You must be certified by AAPC prior to purchasing
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Declaration of conflict of interest NONE
 Declaration of conflict of interest NONE Claudio Muneretto MD, PhD Director of Division of Cardiac Surgery University of Brescia Medical School Italy Hybrid Chymera Different features and potential advantages
Declaration of conflict of interest NONE Claudio Muneretto MD, PhD Director of Division of Cardiac Surgery University of Brescia Medical School Italy Hybrid Chymera Different features and potential advantages
Pericardial Effusion
 Pericardial Effusion How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Pericardial Effusion How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
About OMICS International Conferences
 About OMICS Group OMICS Group is an amalgamation of Open Access publications and worldwide international science conferences and events. Established in the year 2007 with the sole aim of making the information
About OMICS Group OMICS Group is an amalgamation of Open Access publications and worldwide international science conferences and events. Established in the year 2007 with the sole aim of making the information
Off-Pump Cardiac Surgery is not Dead
 Off-Pump Cardiac Surgery is not Dead Gonzalo J. Carrizo, M.D. Fellow Cardiothoracic Surgery Division Cardiothoracic Surgery Department of Surgery University of Colorado Hopeman Lectureship September 10,2007
Off-Pump Cardiac Surgery is not Dead Gonzalo J. Carrizo, M.D. Fellow Cardiothoracic Surgery Division Cardiothoracic Surgery Department of Surgery University of Colorado Hopeman Lectureship September 10,2007
(Ann Thorac Surg 2008;85:845 53)
 I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
Perioperative Management of TAPVC
 Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
Off-pump coronary artery bypass (OPCAB) grafting has
 Tips and Techniques for Multivessel OPCAB John D. Puskas, MD Off-pump coronary artery bypass (OPCAB) grafting has been adopted worldwide and is recognized as a valuable alternative to conventional coronary
Tips and Techniques for Multivessel OPCAB John D. Puskas, MD Off-pump coronary artery bypass (OPCAB) grafting has been adopted worldwide and is recognized as a valuable alternative to conventional coronary
ORIGINAL RESEARCH. KEYWORDS: Coronary artery bypass surgery.arterial conduits. Radial artery. Emergency. Coronary disease.
 CLINICS 2005;60(3):227-32 ORIGINAL RESEARCH CORONARY REVASCULARIZATION WITH THE LEFT INTERNAL THORACIC ARTERY AND RADIAL ARTERY. COMPARISON OF SHORT-TERM CLINICAL EVOLUTION BETWEEN ELECTIVE AND EMERGENCY
CLINICS 2005;60(3):227-32 ORIGINAL RESEARCH CORONARY REVASCULARIZATION WITH THE LEFT INTERNAL THORACIC ARTERY AND RADIAL ARTERY. COMPARISON OF SHORT-TERM CLINICAL EVOLUTION BETWEEN ELECTIVE AND EMERGENCY
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
Post Harvest Wound Infection and Patient s Perception: Comparative Study between Radial Artery and Saphenous Vein Harvest Sites
 Original Article Post Harvest Wound Infection and Patient s Perception: Comparative Study between Radial Artery and Saphenous Vein Harvest Sites Mitsumasa Hata, MD, Jai Raman, FRACS, George Matalanis,
Original Article Post Harvest Wound Infection and Patient s Perception: Comparative Study between Radial Artery and Saphenous Vein Harvest Sites Mitsumasa Hata, MD, Jai Raman, FRACS, George Matalanis,
I internal mammary artery (IMA) is widely accepted as
 Routine Use of the Left Internal Mammary Artery Graft in the Elderly Timothy J. Gardner, MD, Peter S. Greene, MD, Mary F. Rykiel, RN, William A. Baumgartner, MD, Duke E. Cameron, MD, Alfred S. Casale,
Routine Use of the Left Internal Mammary Artery Graft in the Elderly Timothy J. Gardner, MD, Peter S. Greene, MD, Mary F. Rykiel, RN, William A. Baumgartner, MD, Duke E. Cameron, MD, Alfred S. Casale,
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
Protocol. Lung Volume Reduction Surgery for Severe Emphysema
 Protocol Lung Volume Reduction Surgery for Severe Emphysema (70171) Medical Benefit Effective Date: 01/01/12 Next Review Date: 09/14 Preauthorization Yes Review Dates: 02/07, 01/08, 11/08, 09/09, 09/10,
Protocol Lung Volume Reduction Surgery for Severe Emphysema (70171) Medical Benefit Effective Date: 01/01/12 Next Review Date: 09/14 Preauthorization Yes Review Dates: 02/07, 01/08, 11/08, 09/09, 09/10,
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Myocardial contusion injury (MCI) may occur as a rare
 Cardiovascular Images Myocardial Contusion in an 8-Year-Old Boy A Kick to the Heart Danielle M. Moyé, MD; Adrian K. Dyer, MD; Poonam P. Thankavel, MD Myocardial contusion injury (MCI) may occur as a rare
Cardiovascular Images Myocardial Contusion in an 8-Year-Old Boy A Kick to the Heart Danielle M. Moyé, MD; Adrian K. Dyer, MD; Poonam P. Thankavel, MD Myocardial contusion injury (MCI) may occur as a rare
Original Article RESUMO ABSTRACT
 Rev Bras Cardiol Invasiva. Original Article Very Late Evaluation of the Use of Drug-Eluting Stents for the Treatment of Patients with Saphenous Vein Graft Lesions: One-Decade Experience of the Bruno Palmieri
Rev Bras Cardiol Invasiva. Original Article Very Late Evaluation of the Use of Drug-Eluting Stents for the Treatment of Patients with Saphenous Vein Graft Lesions: One-Decade Experience of the Bruno Palmieri
Distribution Of Grafts In Aortocoronary Bypass Surgery: Cardiovascular Surgery Fellowship Experience.
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 17 Number 1 Distribution Of Grafts In Aortocoronary Bypass Surgery: Cardiovascular Surgery Fellowship Experience. J C Eze Citation
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 17 Number 1 Distribution Of Grafts In Aortocoronary Bypass Surgery: Cardiovascular Surgery Fellowship Experience. J C Eze Citation
Intraoperative application of Cytosorb in cardiac surgery
 Intraoperative application of Cytosorb in cardiac surgery Dr. Carolyn Weber Heart Center of the University of Cologne Dept. of Cardiothoracic Surgery Cologne, Germany SIRS & Cardiopulmonary Bypass (CPB)
Intraoperative application of Cytosorb in cardiac surgery Dr. Carolyn Weber Heart Center of the University of Cologne Dept. of Cardiothoracic Surgery Cologne, Germany SIRS & Cardiopulmonary Bypass (CPB)
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
Preoperative Management. Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee
 Preoperative Management Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee Perioperative Care Consideration Medical care provided to prepare
Preoperative Management Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee Perioperative Care Consideration Medical care provided to prepare
Transfusion & Mortality. Philippe Van der Linden MD, PhD
 Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
SURGICAL MYOCARDIAL REVASCULARIZATION: ARTERIAL VS VENOUS GRAFTS, SINGLE VS MULTIPLE GRAFTS?
 SURGICAL MYOCARDIAL REVASCULARIZATION: ARTERIAL VS VENOUS GRAFTS, SINGLE VS MULTIPLE GRAFTS? Luigi Martinelli Chief, Dept. of Surgery Istituto Clinico Ligure di Alta Specialità RAPALLO During 1987 2006,
SURGICAL MYOCARDIAL REVASCULARIZATION: ARTERIAL VS VENOUS GRAFTS, SINGLE VS MULTIPLE GRAFTS? Luigi Martinelli Chief, Dept. of Surgery Istituto Clinico Ligure di Alta Specialità RAPALLO During 1987 2006,
Disclosures The PREVENT IV Trial was supported by Corgentech and Bristol-Myers Squibb
 Saphenous Vein Grafts with Multiple Versus Single Distal Targets in Patients Undergoing Coronary Artery Bypass Surgery: One-Year Graft Failure and Five-Year Outcomes from the Project of Ex-vivo Vein Graft
Saphenous Vein Grafts with Multiple Versus Single Distal Targets in Patients Undergoing Coronary Artery Bypass Surgery: One-Year Graft Failure and Five-Year Outcomes from the Project of Ex-vivo Vein Graft
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
University of Bristol - Explore Bristol Research
 Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Undergraduate Teaching
 Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
DESCRIPTION: Percentage of patients aged 18 years and older undergoing isolated CABG surgery who received an IMA graft
 Measure #43 (NQF 0134): Coronary Artery Bypass Graft (CABG): Use of Internal Mammary Artery (IMA) in Patients with Isolated CABG Surgery National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS
Measure #43 (NQF 0134): Coronary Artery Bypass Graft (CABG): Use of Internal Mammary Artery (IMA) in Patients with Isolated CABG Surgery National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS
OPCAB IS NOT BETTER THAN CONVENTIONAL CABG
 OPCAB IS NOT BETTER THAN CONVENTIONAL CABG Harold L. Lazar, M.D. Harold L. Lazar, M.D. Professor of Cardiothoracic Surgery Boston Medical Center and the Boston University School of Medicine Boston, MA
OPCAB IS NOT BETTER THAN CONVENTIONAL CABG Harold L. Lazar, M.D. Harold L. Lazar, M.D. Professor of Cardiothoracic Surgery Boston Medical Center and the Boston University School of Medicine Boston, MA
CABG Surgery following STEMI
 CABG Surgery following STEMI Susana Harrington, MS,APRN-NP Cardio-Thoracic Surgery Nebraska Methodist Hospital February 15, 2018 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction:
CABG Surgery following STEMI Susana Harrington, MS,APRN-NP Cardio-Thoracic Surgery Nebraska Methodist Hospital February 15, 2018 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction:
Importance of the third arterial graft in multiple arterial grafting strategies
 Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
SUPPLEMENTAL MATERIAL. Supplemental digital content 1, Appendix 1. Ischemic symptoms and electrocardiography
 SUPPLEMENTAL MATERIAL Supplemental digital content 1, Appendix 1. Ischemic symptoms and electrocardiography findings 1. Ischemic symptoms included any of the following: chest discomfort, arm discomfort,
SUPPLEMENTAL MATERIAL Supplemental digital content 1, Appendix 1. Ischemic symptoms and electrocardiography findings 1. Ischemic symptoms included any of the following: chest discomfort, arm discomfort,
TSDA ACGME Milestones
 TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
Listing Form: Heart or Cardiovascular Impairments. Medical Provider:
 Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
A Practical Approach to Ultrasound Assessment of Respiratory Distress
 A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
Left Internal Mammary Artery to the Left Anterior Descending Artery: Effect on Morbidity and Mortality and Reasons for Nonusage
 Left Internal Mammary Artery to the Left Anterior Descending Artery: Effect on Morbidity and Mortality and Reasons for Nonusage Shishir Karthik, FRCS, Arun K. Srinivasan, FRCS, Antony D. Grayson, BS, Mark
Left Internal Mammary Artery to the Left Anterior Descending Artery: Effect on Morbidity and Mortality and Reasons for Nonusage Shishir Karthik, FRCS, Arun K. Srinivasan, FRCS, Antony D. Grayson, BS, Mark
Despite advances in perioperative care, postoperative
 DOI: 10.1590/0100-69912017003011 Original Article Incidence and risk factors for postoperative pulmonary complications in patients undergoing thoracic and abdominal surgeries Incidência e fatores de complicações
DOI: 10.1590/0100-69912017003011 Original Article Incidence and risk factors for postoperative pulmonary complications in patients undergoing thoracic and abdominal surgeries Incidência e fatores de complicações
TAMPONADE CARDIAQUE. Dr Cédrick Zaouter TUSAR 15 décembre 2015
 TAMPONADE CARDIAQUE Dr Cédrick Zaouter TUSAR 15 décembre 2015 OUTLINE History Incidence Definition Pathophysiology Aetiologies Investigations - Echocardiography Treatment of cardiac tamponade Pericardial
TAMPONADE CARDIAQUE Dr Cédrick Zaouter TUSAR 15 décembre 2015 OUTLINE History Incidence Definition Pathophysiology Aetiologies Investigations - Echocardiography Treatment of cardiac tamponade Pericardial
Is bypass surgery needed for elderly patients with LMT disease? From the surgical point of view
 CCT 2003 (Kobe) Is bypass surgery needed for elderly patients with LMT disease? From the surgical point of view Hitoshi Yaku, MD, PhD Department of Cardiovascular Surgery Kyoto Prefectural University of
CCT 2003 (Kobe) Is bypass surgery needed for elderly patients with LMT disease? From the surgical point of view Hitoshi Yaku, MD, PhD Department of Cardiovascular Surgery Kyoto Prefectural University of
Surgery for Acquired Cardiovascular Disease
 Effect of posterior pericardial drainage on the incidence of pericardial effusion after ascending aortic surgery Sadik Eryilmaz, MD, Ozan Emiroglu, MD, Zeynep Eyileten, MD, Ruchan Akar, MD, Levent Yazicioglu,
Effect of posterior pericardial drainage on the incidence of pericardial effusion after ascending aortic surgery Sadik Eryilmaz, MD, Ozan Emiroglu, MD, Zeynep Eyileten, MD, Ruchan Akar, MD, Levent Yazicioglu,
Parenchymal air leak is a frequent complication after. Pleural Tent After Upper Lobectomy: A Randomized Study of Efficacy and Duration of Effect
 Pleural After Upper Lobectomy: A Randomized Study of Efficacy and Duration of Effect Alessandro Brunelli, MD, Majed Al Refai, MD, Marco Monteverde, MD, Alessandro Borri, MD, Michele Salati, MD, Armando
Pleural After Upper Lobectomy: A Randomized Study of Efficacy and Duration of Effect Alessandro Brunelli, MD, Majed Al Refai, MD, Marco Monteverde, MD, Alessandro Borri, MD, Michele Salati, MD, Armando
Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm
 CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
. : . (CABG Coronary Artery Bypass Graft Surgery)
 88/10/2 : 88/4/31 : 1389 /104 / 4 3 2 1 4 5 1 (CT Chest Tube) :.. (CABG Coronary Artery Bypass Graft Surgery) 24 307 : ) 4 40 48 ( ) (. ( ) ( 34/5 40/2). 67/1 59/60 ± 9/24 : ( 85 92/5) ( 2 2/88) ( 36 45/8).
88/10/2 : 88/4/31 : 1389 /104 / 4 3 2 1 4 5 1 (CT Chest Tube) :.. (CABG Coronary Artery Bypass Graft Surgery) 24 307 : ) 4 40 48 ( ) (. ( ) ( 34/5 40/2). 67/1 59/60 ± 9/24 : ( 85 92/5) ( 2 2/88) ( 36 45/8).
Faculty/Presenter Disclosure
 Faculty/Presenter Disclosure Faculty: Andre Lamy Relationships with commercial interests: Grants/Research Support: None Speakers Bureau/Honoraria: None Consulting Fees: None Other: None CORONARY: The Coronary
Faculty/Presenter Disclosure Faculty: Andre Lamy Relationships with commercial interests: Grants/Research Support: None Speakers Bureau/Honoraria: None Consulting Fees: None Other: None CORONARY: The Coronary
EACTS Adult Cardiac Database
 EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications
 Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
ORIGINAL ARTICLE. Rev Bras Cir Cardiovasc 2012;27(1):103-9
 ORIGINAL ARTICLE Subxyphoid pleural drain confers lesser impairment in respiratory muscle strength, oxygenation and lower chest pain after off-pump coronary artery bypass grafting: a randomized Dreno pleural
ORIGINAL ARTICLE Subxyphoid pleural drain confers lesser impairment in respiratory muscle strength, oxygenation and lower chest pain after off-pump coronary artery bypass grafting: a randomized Dreno pleural
Alfa Ferry FRCS Cardiac Surgeon OPERATIVE MANAGEMENT IN CORONARY ARTERY DISEASE
 Alfa Ferry FRCS Cardiac Surgeon OPERATIVE MANAGEMENT IN CORONARY ARTERY DISEASE Management in CHD Medical (medikamentosa) Intervensi 1. Percutaneous ( PTCA & stenting ) 2. Surgical ( CABG, CABG & mitral
Alfa Ferry FRCS Cardiac Surgeon OPERATIVE MANAGEMENT IN CORONARY ARTERY DISEASE Management in CHD Medical (medikamentosa) Intervensi 1. Percutaneous ( PTCA & stenting ) 2. Surgical ( CABG, CABG & mitral
Learning Radiology: Recognizing the Basics. Text with Student Consult Online Access Code
 Learning Radiology: Recognizing the Basics. Text with Student Consult Online Access Code Herring, W ISBN-13: 9780323074445 Table of Contents 1. Recognizing Anything The "colorful" world of radiology A
Learning Radiology: Recognizing the Basics. Text with Student Consult Online Access Code Herring, W ISBN-13: 9780323074445 Table of Contents 1. Recognizing Anything The "colorful" world of radiology A
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Measure #164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clinical Care
 Measure #164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
Measure #164 (NQF 0129): Coronary Artery Bypass Graft (CABG): Prolonged Intubation National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
DOWNLOAD PDF MYOCARDIAL CONTRAST TWO DIMENSIONAL ECHOCARDIOGRAPHY (DEVELOPMENTS IN CARDIOVASCULAR MEDICINE)
 Chapter 1 : Imaging Cardiovascular Medicine Stanford Medicine contrast two-dimensional echocardiography (MC-2DE), a new and exciting diagnostic methodology for assessment of myocardial perfusion, which
Chapter 1 : Imaging Cardiovascular Medicine Stanford Medicine contrast two-dimensional echocardiography (MC-2DE), a new and exciting diagnostic methodology for assessment of myocardial perfusion, which
SBCCV BOLETIM CIENTÍFICO
 02 2018 BOLETIM CIENTÍFICO SBCCV Editores: Dr. Domingo Marcolino Braile Dr. Fernando Ribeiro de Moraes Neto Dr. Luciano Cabral Albuquerque Dr. Orlando Petrucci Junior Dr. Walter José Gomes Lancet 2018;391:939-48
02 2018 BOLETIM CIENTÍFICO SBCCV Editores: Dr. Domingo Marcolino Braile Dr. Fernando Ribeiro de Moraes Neto Dr. Luciano Cabral Albuquerque Dr. Orlando Petrucci Junior Dr. Walter José Gomes Lancet 2018;391:939-48
F mary artery (IMA) graft carries a greater long-term
 Internal Mammary Artery Grafts: The Shortest Route to the Coronarv Arteries J Thomas J. Vander Salm, MD, Sultan Chowdhary, MD,. N. Okike, MD, A. Thomas ezzella, MD, and Michael K. asque, MD University
Internal Mammary Artery Grafts: The Shortest Route to the Coronarv Arteries J Thomas J. Vander Salm, MD, Sultan Chowdhary, MD,. N. Okike, MD, A. Thomas ezzella, MD, and Michael K. asque, MD University
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
PRE-OPERATIVE INCENTIVE SPIROMETRY; EFFECTIVENESS TO IMPROVE POST-OPERATIVE OXYGENATION IN PATIENTS UNDERGOING CABG SURGERY
 The Professional Medical Journal DOI: 10.17957/TPMJ/16.3579 ORIGINAL PROF-3579 PRE-OPERATIVE INCENTIVE SPIROMETRY; EFFECTIVENESS TO IMPROVE POST-OPERATIVE OXYGENATION IN PATIENTS UNDERGOING CABG SURGERY
The Professional Medical Journal DOI: 10.17957/TPMJ/16.3579 ORIGINAL PROF-3579 PRE-OPERATIVE INCENTIVE SPIROMETRY; EFFECTIVENESS TO IMPROVE POST-OPERATIVE OXYGENATION IN PATIENTS UNDERGOING CABG SURGERY
Analysis of Mortality Within the First Six Months After Coronary Reoperation
 Analysis of Mortality Within the First Six Months After Coronary Reoperation Frans M. van Eck, MD, Luc Noyez, MD, PhD, Freek W. A. Verheugt, MD, PhD, and Rene M. H. J. Brouwer, MD, PhD Departments of Thoracic
Analysis of Mortality Within the First Six Months After Coronary Reoperation Frans M. van Eck, MD, Luc Noyez, MD, PhD, Freek W. A. Verheugt, MD, PhD, and Rene M. H. J. Brouwer, MD, PhD Departments of Thoracic
