Long-Term Results of Balloon Valvuloplasty as Primary Treatment for Congenital Aortic Valve Stenosis: a 20-Year Review
|
|
|
- Maria Benson
- 6 years ago
- Views:
Transcription
1 DOI /s ORIGINAL ARTICLE Long-Term Results of Balloon Valvuloplasty as Primary Treatment for Congenital Aortic Valve Stenosis: a 20-Year Review Camille Soulatges 1 Mona Momeni 2 Nadia Zarrouk 1 Stéphane Moniotte 1 Karlien Carbonez 1 Catherine Barrea 1 Jean Rubay 3 Alain Poncelet 3 Thierry Sluysmans 1,4 Received: 4 September 2014 / Accepted: 4 March 2015 Ó Springer Science+Business Media New York 2015 Abstract In the presence of new surgical techniques, the treatment of congenital valvular aortic stenosis is under debate. We reviewed the results and late outcomes of all 93 patients aged 1 day to 18 years, treated with balloon valvuloplasty (BAV) as first-line therapy for congenital aortic valve stenosis in our center from January 1991 to May Mean age at procedure time was 2.4 years; 37 patients underwent BAV at age B30 days (neonates), 29 patients at age C1 month and \1 year (infants), and 27 patients were older than 1 year (children). The invasive BAV peak-topeak aortic valve gradient (mean 59 ± 22 mmhg) was immediately reduced (mean 24 ± 12 mmhg). The observed diminution of gradient was similar for each age group. Four patients had significant post-bav AI. Mean follow-up after BAV was 11.4 ± 7 years. The last echo peak aortic gradient was 37 ± 18 mmhg and mean gradient was 23 ± 10 mmhg, and two patients had significant AI. Actuarial survival for the whole cohort was 88.2 and 72.9 % for the neonates. All infants, except one, and all children survived. Sixty-six percent of patients were free from surgery, and & Thierry Sluysmans Thierry.sluysmans@uclouvain.be Department of Pediatric Cardiology, Cliniques Universitaires Saint-Luc, Université Catholique de Louvain, Brussels, Belgium Department of Anesthesiology, Cliniques Universitaires Saint-Luc, Université Catholique de Louvain, Brussels, Belgium Department of Cardiac Surgery, Cliniques Universitaires Saint-Luc, Université Catholique de Louvain, Brussels, Belgium Cardiologie Pédiatrique, Cliniques Universitaires Saint-Luc, Avenue Hippocrate 10, 1200 Brussels, Belgium 58 % were free from any reintervention, with no difference according to age. Freedom from surgery after BAV at 5, 10, and 20 years, respectively, was 82, 72, and 66 %. Our study confirms that BAV as primary treatment for congenital AS is an efficient and low-risk procedure in infants and children. In neonates, the prognosis is more severe and clearly related to borderline. Keywords Congenital valvular aortic stenosis Balloon valvuloplasty Outcome Shone s syndrome Introduction Congenital valvular aortic stenosis (AS) is relatively common ( per 10,000 live births) [3, 8]. Since 30 years, balloon aortic valvuloplasty (BAV) is the firstline treatment in most centers worldwide [6, 9]. There is still debate, however, concerning what is the most appropriate treatment, especially in the context of new surgical techniques such as aortic valve reconstruction or the Ross procedure. We reviewed the results of all the patients treated with BAV as first-line therapy in our center, and we analyzed the results and late outcomes of the procedure. Materials and Methods We reviewed the medical records of all patients aged 1 day to 18 years, treated with BAV from January 1991 to May 2012 in the Cliniques Universitaires Saint Luc, UCL, Brussels. Age, weight, gender, echocardiographic and hemodynamic data, and need for re-intervention, and/or surgery were collected.
2 Transthoracic echocardiography (TTE) was used to evaluate the anatomy of the aortic valve, with Dopplerderived pressure gradients and insufficiency degree assessed before and after the procedure. Left ventricular shortening fraction (SF) and left ventricular end-diastolic diameter (DD) were collected. Peak and mean aortic valve gradients were measured using the modified Bernoulli equation. AS was considered significant if the peak gradient exceeded 70 mmhg, without dysfunction. Aortic insufficiency (AI), detected by means of color Doppler, was classified from 0 to 4, with grades 3 4 or 4 considered significant AI. Percutaneous BAV was performed under general anesthesia usually via retrograde femoral artery access. Peakto-peak gradient through the aortic valve, presence of AI, and annulus size were all assessed before and after the procedure. Balloon sizes ranged from 4 to 25 mm, never exceeding a balloon diameter to aortic annulus ratio of 0.9. Patients with sub- or supra-valvular aortic stenosis, or those exhibiting hypoplastic left heart syndrome (HLHS), were not included in the study. In addition, those who had undergone surgical aortic valvuloplasty as an initial treatment were excluded from analysis. SPSS statistical software was used for data analysis. Categorical variables were reported as absolute numbers and percentages. Continuous variables were expressed as either mean ± standard deviation (SD) or median values and ranges. For all tests, a p value \0.05 was considered statistically significant. Actuarial survival and freedom from reintervention were calculated using the Kaplan Meier method. The study was conducted in accordance with the Belgian regulatory requirements. Due to its retrospective study design, neither IRB approval nor patient written informed consent was required. Results From January 1991 to May 2012, 93 patients with congenital AS were referred to our center to undergo primary BAV. Figure 1a depicts the distribution and frequency over time. A description of the population and results can be found in Table 1 and Fig. 1b. The mean age at procedure time was 2.4 years, with 37 patients undergoing BAV aged B30 days (neonates), 29 aged between 1 month and 1 year (infants), and 27 aged over 1 year (children). The population was 18 % female and 82 % male. Isolated bicuspid aortic valve was diagnosed in 58 % of the cohort, with 16 % exhibiting Shone s syndrome. After reviewing patient data and evolution, nine patients who had been selected for BAV on account of an adequately sized left ventricle were diagnosed as having multiple small left ventricular structures, such as the mitral or aortic valve and the aortic arch. Prior to BAV, the Doppler-derived peak and mean aortic valve gradients were 71 ± 18 and 44 ± 12 mmhg, respectively. The mean SF was 42 ± 11 %, with dysfunction (SF \ 30 %) reported in only three patients, all neonates. During catheterization, the pre-bav peak-to-peak aortic valve gradient, measured invasively, was 59 ± 22 mmhg. The post-bav peak-to-peak gradient was immediately reduced to 24 ± 12 mmhg. The observed decrease in gradient was similar in all age groups. Only one patient (neonate) exhibited a post-bav peak-to-peak gradient exceeding 50 mmhg, which was considered a failure. Yet a spontaneous decrease in gradient was revealed on TTE during follow-up, decreasing to 15 mmhg after 12.3 years, despite no other procedure having been performed. Angiographic nonsignificant AI (grade 1 or 2) was present in eight patients before the procedure and in 37 patients after the procedure, considered significant in four patients (grade 3 or 4). Echocardiographic reports were available for follow-up in 88 patients (94.6 %), with five lost to late follow-up. At the last echo, the peak aortic gradient was 37 ± 18 mmhg and mean gradient was 23 ± 10 mmhg, with a higher residual gradient observed in the children group (42 ± 18 mmhg). AI was reported in 52 patients (59 %), with only two cases considered significant (one neonate and one infant). Mean follow-up duration after BAV was 11.4 ± 7years, with a maximum of 21.7 years. A total of 48 patients (51 %) were followed up for over 10 years. The Kaplan Meier method showed an actuarial survival for the whole cohort of 88 % at last follow-up (Fig. 2a). Only 72.9 % of the neonates were still alive, whereas all the children survived and all the infants, except one, who died from surgical complications (Fig. 2b). Out of the entire patient population, 66 % were free from surgery at last follow-up, with no significant difference observed according to age (Table 1), and over half (58 %) were free from any reintervention. A second intervention (additional BAV or surgery) was performed in 35 patients (37 %) after a mean time of 3.4 years. The results are presented in Table 2. A second intervention was significantly more common in the children, yet took place earlier in the neonate group. No differences were observed in the reintervention type among the three groups. A second BAV was performed in six children (22 %) after a mean time of 5.7 years, in six infants (20.7 %) after a mean time of 4.7 years, and in six neonates (16 %) after a mean time of 0.6 years. Surgery was performed as a second intervention in 17 patients (18.2 %): six children (22 %) after a mean time of 6 years,
3 Fig. 1 a Congenital AS distribution and frequency in Cliniques Universitaires Saint-Luc over study period, b flowchart of patient evolution four infants (13.8 %) after a mean time of 2.8 years, and seven neonates (18.9 %) after a mean time of 1.1 years. A Ross procedure was performed on 12 patients, a surgical aortic valvuloplasty on two, and sub-aortic membrane resection on three. Within this patient group, one 15-year-old patient required assistance and a heart transplant following the Ross procedure, performed due to predominant aortic stenosis. This patient exhibited good final evolution. Repeat BAV procedures (C3 percutaneous interventions) were conducted in five patients (5.4 %), comprising two neonates, two infants, and one child. For three of these
4 Table 1 Population data and BAV results in the whole cohort by age group Total Neonates Infants Children p Patients (n) Age at BAV 2.4 years 6.7 days 2.7 m ± years Gender (m/f) 76/17 32/5 22/7 22/5 Weight (kg) 10 ± ± ± ± 17 Pre-BAV TTE SF (%) 42 ± ± 8 46 ± ± 9 DD (mm) 23 ± ± ± 4 38 ± 10 Balloon aortic valvuloplasty Pre-BAV AO gradient (mmhg) 59 ± ± ± ± 21 Post-BAV AO gradient (mmhg) 24 ± ± ± ± 10 Aortic annular diameter (mm) 9.8 ± ± ± ± 3.5 Pre-BAV AI (1 4/4) Post-BAV significant AI (C3/4) Mean follow-up (years) 11.4 ( ) 7.4 ( ) 10 ( ) 18.2 ( ) TTE peak AO gradient (mmhg) 37 ± ± ± ± 18.7 TTE mean AO gradient (mmhg) 23 ± ± ± ± 9.5 Significant AI (C3/4) Overall survival 83 (89.2 %) 27 (72.9 %) 28 (97 %) 27 (100 %) p \ 0.01 Free from surgery 62 (66.7 %) 22 (72.9 %) 22(75.8 %) 18 (66.7 %) Free from reintervention 54 (58 %) 20 (54 %) 19 (65.5 %) 15 (55.5 %) patients (one neonate and two infants), surgery was eventually performed. Surgery was performed as third or fourth intervention in 12 patients (12.9 %), consisting of four Ross procedures (in two neonates, one infant, and one child), six aortic valvuloplasty (three infants and three children), one univentricular palliation (in one neonate, who died during surgery), and one heart transplantation (in the previously mentioned 15-year-old patient with severe dysfunction following the Ross procedure). The indications for reinterventions in the 24 patients operated on the aortic valve (16 Ross, eight aortic valve repairs) were aortic stenosis in ten patients, insufficiency in seven patients, and mixed stenosis and regurgitation in seven patients, with aortic valve surgery performed mainly to treat significant AI in 14 of those 24 patients (Fig. 1b). Patient deaths (Table 3) concerned 10 neonates who had undergone BAV at under 30 days of age, and one infant who underwent BAV at 41 days old and died from postoperative complications (Patient 10). Of the 10 neonates who died, two (20 %) had presented with dysfunction prior to BAV and eight either exhibited Shone s syndrome or were diagnosed as having multiple small or abnormal left heart structures. Seven patients died within the 2 months following BAV, and only two patients died after 1 year of age. In four patients, death was related to catheterization complications: Two patients developed significant AI following BAV (one infant [Patient 3] died 7 days after a rescue Ross procedure and the other [Patient 5] 2 weeks following BAV), one patient died from a mitral tear resulting in severe regurgitation during a second BAV procedure (Patient 8), and the fourth died from cerebral hemorrhage during streptokinase treatment for femoral artery thrombosis (Patient 9). Three patients died from surgical complications, consisting of aortic dissection during coarctation repair (Patient 4), air embolism (Patient 10), and stroke during extracorporeal life support following a heart transplant (Patient 11). In eight neonate patients, death was at least partially related to inadequate or left heart structure dimensions (Table 3). One of the eight neonates died following a rescue Norwood procedure (Patient 7), one from fibroelastosis revealed during the Ross procedure (Patient 6), and one from persistent diastolic dysfunction 6.8 years after a Ross procedure (Patient 11 who died from cerebral hemorrhage following a heart transplant). Discussion Our study presents the results and outcomes from a 20-year experience with BAV as an initial treatment for congenital AS in a pediatric population. BAV is an efficient procedure, demonstrated by the significant decrease in aortic
5 gradient we observed immediately after the procedure and at late follow-up in all groups. Our survival analysis, with a mean follow-up of 11.4 ± 7 years, revealed that 88 % of Fig. 2 a Patient survival at last follow-up was 89.2 %, b patient survival by age at first catheterization. Except one infant who died at 1 year of age from air embolism during surgical aortic valvuloplasty (patient 10, Table 3), all infant and children were alive (98 % survival rate); 72.9 % of the neonates were alive patients were alive at 20 years of age, with two-thirds of the cohort free from surgery and over half free from any reintervention. These findings are in line with the literature [1, 6, 9]. Nevertheless, a second intervention (either surgery or BAV 36 % in our series) appeared unavoidable in a third of patients in the long term [7, 12, 13]. The mortality rate was 11.8 % for the whole cohort and 27 % for the neonate subgroup. The 73 % survival reported in neonates with critical aortic stenosis in our series was similar to the 72 % survival at 5 years reported in the Congenital Heart Surgeons Society multicentric study [10]. In our series, all deaths involved neonates, except one. The causes of death were multifactorial: In four cases, death was considered secondary to BAV complications, and in eight cases (8/11 72 %), patients were finally diagnosed with a borderline with abnormal left heart structures or non-compliant, clearly associated with an increased risk of poor results and death [14]. When neonates are diagnosed with a borderline, predicting which is suitable for biventricular repair remains a substantial challenge [2, 5, 11] and the presence of endocardial fibroelastosis with diastolic dysfunction appears to be a more significant risk factor than volume or dimensions [14]. systolic dysfunction preceding BAV also tended to be associated with poor survival. Although as it concerned only three patients in our study, this assessment should be interpreted with caution. Another relevant observation was the fact that 66.7 % of the whole population was free from surgery at the last follow-up. The freedom from surgery after BAV of 82, 72, and 66 % at 5, 10, and 20 years of follow-up, respectively, is even more appealing for physicians in charge of young children (Fig. 3). This result should be compared to the 50 % freedom from surgical reintervention and valve replacement at 10 years that was recently reported in a pediatric population following aortic valve repair performed by the most skilled surgeons [4]. The graphs published in this actual surgical study demonstrated 70 % freedom of reintervention at 10 years after aortic valve repair with no cusp extension, yet only 30 % freedom of reintervention when cusp extension was performed. For neonates with critical aortic stenosis, the prospective non-randomized study by Table 2 Second intervention Total Neonates Infants Children p Secondnd intervention 35 (37.3 %) 13 (35.1 %) 10 (34.5 %) 12 (44.4 %) p \ 0.05 Mean time after first BAV (years) p \ 0.05 Cath 18 (19.3 %) 6 (16 %) 6 (20.7 %) 6 (22 %) Mean time after first BAV (years) p \ 0.05 Surgery 17 (18.2 %) 7 (18.9 %) 4 (13.8 %) 6 (22 %) Mean time after first BAV (years)
6 Table 3 Data of the patients who died Patient Age at first BAV (days) Age at death (days) Date of birth Causes of death Death related to abnormal Death related to cath complication Postoperative death Severe mitral regurgitation, Shone syndrome Severe dysfunction, Shone syndrome Cath complication, AO regurg, postop death (Ross day 1) AO regurgitation Ross procedure Shone syndrome, postop death (COA repair day 1) Cath complication, severe AO regurg Fibroelastosis, postop death (Ross-Kono, day 1) Fibroelastosis, postop death (Norwood, day 1) Cath complication (second procedure), mitral regurg Cath complication (second procedure), cerebral hemorrhage Postop death (valvuloplasty, day 1) Fibroelastosis, postop death (transplant, ECMO, day 2) AO regurgitation Mitral regurgitation Streptokinase for femoral thrombosis COA repair under bypass Ross procedure Norwood procedure Mitral plasty (6 days postcath) AO valvuloplasty air embolism Transplant, ECMO, cerebral hemorrhage the Congenital Heart Surgeons Society reported similar survival and outcomes following valvotomy, performed surgically or by transcatheter balloon dilatation [10]. Historical series demonstrate, as does our study, that balloon valvuloplasty achieves at least similar results to surgery in terms of survival and reoperation rates. For the pediatric population, even with the advent of new surgical techniques, aortic valve repair or replacement must be reserved for patients who failed to benefit from balloon valvuloplasty. Ultimately, most patients will require a reintervention by surgery or balloon dilatation (Fig. 4). Balloon valvuloplasty is easy to repeat if necessary, as it was performed twice in 18 patients and three times in five. This procedure did not preclude a successful aortic surgical valvuloplasty in eight children. Study Limitations Fig. 3 Freedom from surgery after BAV at 5, 10, and 20 years of follow-up were, respectively, 82, 72, and 66 % This was a retrospective, monocenter, and non-comparative study. Our cohort was not very large compared with other studies reported in the literature, and our results must thus be interpreted carefully. Furthermore, the data were collected over a long time period, and the
7 population remaining free from any reintervention after a mean period of 11.4 ± 7 years. In neonates with critical aortic stenosis selected for biventricular repair, the 72.9 % survival at 10 years in our series was in line with the 72 % survival at 5 years reported by BW. Mc Crindle in the Congenital Heart Surgeons Society prospective non-randomized study [10]. In neonates, the prognosis appears more severe, clearly related to borderline and the challenge of recognizing which is suitable or not for a biventricular management strategy [14]. Conflict of interest None to declare. References Fig. 4 Freedom from reintervention, 58 % of patients were free from any reintervention, surgery, or balloon dilatation at last follow-up interventions were performed by different physicians, using different materials and techniques, which could have impacted the results [15]. It is important to note that during the study period, BAV was performed by six different cardiologists. While our results reflect a realistic picture of general BAV outcomes, this could have reinforced differences in patient selection and treatment strategy, partially explaining some of the neonatal deaths. Echocardiographic data were collected by reviewing echo reports, although these were not standardized and had been performed by multiple cardiologists. Another limitation was the use of shortening fraction to assess systolic function, which does not precisely reflect myocardial contractility [9], as well as the use of enddiastolic dimension to assess dimensions. Our center uses BAV as standard management for congenital AS, and no primary surgical aortic valvuloplasty was performed during this time period. For this reason, it was not possible to compare the outcomes of primary BAV with those of primary surgical aortic valvuloplasty. Conclusion This study confirmed that BAV is an efficient and low-risk primary treatment for congenital AS in infants and children, resulting in a 98 % survival and over half the 1. Al Marshafawy H, Al Sawah GA, Hafez M, Matter M, El Gamal A, Sheishaa AG, El Kair MA (2012) Balloon valvuloplasty of aortic valve stenosis in childhood: midterm results in a Children s Hospital, Mansoura University, Egypt. Clin Med Insights Cardiol 6: Colan SD (1995) Correction. Predictors of survival in neonates with critical aortic stenosis. Circulation 92: De Wolf D, Daniëls O (2002) Management of valvar aortic stenosis in children. Pediatr Cardiol 23: d Udekem Y, Siddiqui J, Cameron S, Seaman S, Konstantinov IE, Galati JC, Cheung MMH, Brizard CP (2013) Long-term results of a strategy of aortic valve repair in the pediatric population. J Thorac Cardiovasc Surg 145: Eicken A, Georgiev S, Balling G, Schreiber C, Hager A, Hess J (2010) Neonatal balloon aortic valvuloplasty-predictive value of current risk score algorithms for treatment strategies. Catheter Cardiovasc Interv 76: Ewert P, Bertram H, Breuer J, Dähnert I, Dittrich S, Eicken A, Emmel M, Fischer G, Gitter R, Gorenflo M, Haas N, Kitzmüller E, Koch A, Kretschmar O, Lindinger A, Michel-Behnke I, Nuernberg JH, Peuster M, Walter K, Zartner P, Uhlemann F (2011) Balloon valvuloplasty in the treatment of congenital aortic valve stenosis a retrospective multicenter survey of more than 1000 patients. Int J Cardiol 149: Fratz S, Gildein HP, Balling G, Sebening W, Genz T, Eicken A, Hess J (2008) Aortic valvuloplasty in pediatric patients substantially postpones the need for aortic valve surgery: a single-center experience of 188 patients after up to 17.5 years of follow-up. Circulation 117: Khalid O, Luxenberg DM, Sable C, Benavidez O, Geva T, Hanna B, Abdulla R (2006) Aortic stenosis: the spectrum of practice. Pediatr Cardiol 27: Maskatia SA, Ing FF, Justino H, Crystal MA, Mullins CE, Mattamal RJ, O Brian Smith E, Petit CJ (2011) Twenty-five year experience with balloon aortic valvuloplasty for congenital aortic stenosis. Am J Cardiol 108: McCrindle BW, Blackstone EH, Williams WG, Sittiwangkul R, Spray TL, Azakie A, Jonas RA (2001) Are outcomes of surgical versus transcatheter balloon valvotomy equivalent in neonatal critical aortic stenosis? Circulation 104:I152 I McElhinney DB, Lock JE, Keane JF, Moran AM, Colan SD (2005) Left heart growth, function, and reintervention after balloon aortic valvuloplasty for neonatal aortic stenosis. Circulation 111: Petit CJ, Maskatia SA, Justino H, Mattamal RJ, Crystal MA, Ing FF (2013) Repeat balloon aortic valvuloplasty effectively delays
8 surgical intervention in children with recurrent aortic stenosis. Catheter Cardiovasc Interv 82: Thomson JDR (2004) Management of valvar aortic stenosis in children. Heart Br Cardiol Soc 90: Tuo G, Khambadkone S, Tann O, Kostolny M, Derriick G, Tsang V, Sullivan I, Marek J (2013) Obstructive left heart disease in neonates with a borderline left ventricle: diagnostic challenges to choosing the best outcome. Pediatr Cardiol 34: Weber HS (2006) Catheter management of aortic valve stenosis in neonates and children. Catheter Cardiovasc Interv 67:
Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension?
 Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension? Y d Udekem, J Siddiqui, C Seaman, I Konstantinov, J Galati, M Cheung, C Brizard Royal
Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension? Y d Udekem, J Siddiqui, C Seaman, I Konstantinov, J Galati, M Cheung, C Brizard Royal
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT
 LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
Treatment of congenital aortic valve disease: Neonatal surgical management. Pascal Vouhé - Sick Children Hospital, Paris
 Treatment of congenital aortic valve disease: Neonatal surgical management Pascal Vouhé - Sick Children Hospital, Paris Challenges. valvar lesions. associated lesions. status of left ventricle Valvar lesions.
Treatment of congenital aortic valve disease: Neonatal surgical management Pascal Vouhé - Sick Children Hospital, Paris Challenges. valvar lesions. associated lesions. status of left ventricle Valvar lesions.
Treatment of valvular aortic stenosis in children: a 20-year experience in a single institution
 Interactive CardioVascular and Thoracic Surgery 27 (2018) 410 416 doi:10.1093/icvts/ivy078 Advance Access publication 19 March 2018 ORIGINAL ARTICLE Cite this article as: Kjellberg Olofsson C, Berggren
Interactive CardioVascular and Thoracic Surgery 27 (2018) 410 416 doi:10.1093/icvts/ivy078 Advance Access publication 19 March 2018 ORIGINAL ARTICLE Cite this article as: Kjellberg Olofsson C, Berggren
S. Bruce Greenberg, MD FNASCI and President, NASCI Professor of Radiology and Pediatrics University of Arkansas for Medical Sciences
 S. Bruce Greenberg, MD FNASCI and President, NASCI Professor of Radiology and Pediatrics University of Arkansas for Medical Sciences No financial disclosures Aorta Congenital aortic stenosis/insufficiency
S. Bruce Greenberg, MD FNASCI and President, NASCI Professor of Radiology and Pediatrics University of Arkansas for Medical Sciences No financial disclosures Aorta Congenital aortic stenosis/insufficiency
Excellence in heart and lung care. Royal Brompton Hospital, Sydney Street, London SW3 6NP
 The Surgical Management of the Bicuspid Aortic Valve in Children Professor D.F Shore Royal Brompton & Harefield NHS Trust Excellence in heart and lung care Royal Brompton Hospital, Sydney Street, London
The Surgical Management of the Bicuspid Aortic Valve in Children Professor D.F Shore Royal Brompton & Harefield NHS Trust Excellence in heart and lung care Royal Brompton Hospital, Sydney Street, London
Balloon Valvuloplasty for Recurrent Aortic Stenosis After Surgical Valvotomy in Childhood: Immediate and Follow-Up Studies
 1106 JACC Vol. 13, No. 5 April 1989: 1106-10 Balloon Valvuloplasty for Recurrent Aortic Stenosis After Surgical Valvotomy in Childhood: Immediate and Follow-Up Studies JON N. MELIONES, MD, ROBERT H. BEEKMAN,
1106 JACC Vol. 13, No. 5 April 1989: 1106-10 Balloon Valvuloplasty for Recurrent Aortic Stenosis After Surgical Valvotomy in Childhood: Immediate and Follow-Up Studies JON N. MELIONES, MD, ROBERT H. BEEKMAN,
Outcomes after balloon dilation of congenital aortic stenosis in children and adolescents
 Cardiol Young 24; 14: 315 321 Greenwich Medical Media Ltd. ISSN 147-9511 Original Article Outcomes after balloon dilation of congenital aortic stenosis in children and adolescents Carlos A. C. Pedra, Roger
Cardiol Young 24; 14: 315 321 Greenwich Medical Media Ltd. ISSN 147-9511 Original Article Outcomes after balloon dilation of congenital aortic stenosis in children and adolescents Carlos A. C. Pedra, Roger
Since the Ross procedure was first described in 1967
 Ross-Konno Procedure With Mitral Valve Surgery Norihiko Oka, MD, PhD, Osman Al-Radi, MD, Abdullah A. Alghamdi, MD, Siho Kim, MD, and Christopher A. Caldarone, MD Division of Cardiovascular Surgery, The
Ross-Konno Procedure With Mitral Valve Surgery Norihiko Oka, MD, PhD, Osman Al-Radi, MD, Abdullah A. Alghamdi, MD, Siho Kim, MD, and Christopher A. Caldarone, MD Division of Cardiovascular Surgery, The
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Critical Aortic Stenosis in Early Infancy: Surgical Treatment for Residual Lesions After Balloon Dilation
 Critical Aortic Stenosis in Early Infancy: Surgical Treatment for Residual Lesions After Balloon Dilation Vladimiro L. Vida, MD, Tomaso Bottio, MD, Ornella Milanesi, MD, Elena Reffo, MD, Roberta Biffanti,
Critical Aortic Stenosis in Early Infancy: Surgical Treatment for Residual Lesions After Balloon Dilation Vladimiro L. Vida, MD, Tomaso Bottio, MD, Ornella Milanesi, MD, Elena Reffo, MD, Roberta Biffanti,
What is the Definition of Small Systemic Ventricle. Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University
 What is the Definition of Small Systemic Ventricle Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University Contents Introduction Aortic valve stenosis Aortic coarctation
What is the Definition of Small Systemic Ventricle Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University Contents Introduction Aortic valve stenosis Aortic coarctation
Trend and Outcomes of Direct Transcatheter Aortic Valve Replacement from a Single-Center Experience
 Cardiol Ther (2018) 7:191 196 https://doi.org/10.1007/s40119-018-0115-0 BRIEF REPORT Trend and Outcomes of Direct Transcatheter Aortic Valve Replacement from a Single-Center Experience Anthony A. Bavry.
Cardiol Ther (2018) 7:191 196 https://doi.org/10.1007/s40119-018-0115-0 BRIEF REPORT Trend and Outcomes of Direct Transcatheter Aortic Valve Replacement from a Single-Center Experience Anthony A. Bavry.
Imaging Assessment of Aortic Stenosis/Aortic Regurgitation
 Imaging Assessment of Aortic Stenosis/Aortic Regurgitation Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2014 Las Vegas Disclosure
Imaging Assessment of Aortic Stenosis/Aortic Regurgitation Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2014 Las Vegas Disclosure
Outline. Congenital Heart Disease. Special Considerations for Special Populations: Congenital Heart Disease
 Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Practice variation can lead to higher resource ORIGINAL ARTICLE
 1 ORIGINAL ARTICLE Acute Outcomes after Introduction of a Standardized Clinical Assessment and Management Plan (SCAMP) for Balloon Aortic Valvuloplasty in Congenital Aortic Stenosis Diego Porras, MD,*
1 ORIGINAL ARTICLE Acute Outcomes after Introduction of a Standardized Clinical Assessment and Management Plan (SCAMP) for Balloon Aortic Valvuloplasty in Congenital Aortic Stenosis Diego Porras, MD,*
Coarctation of the Aorta
 Interventional Management of Coarctation of the Aorta Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada Outline
Interventional Management of Coarctation of the Aorta Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada Outline
Research Presentation June 23, Nimish Muni Resident Internal Medicine
 Research Presentation June 23, 2009 Nimish Muni Resident Internal Medicine Research Question In adult patients with repaired Tetralogy of Fallot, how does Echocardiography compare to MRI in evaluating
Research Presentation June 23, 2009 Nimish Muni Resident Internal Medicine Research Question In adult patients with repaired Tetralogy of Fallot, how does Echocardiography compare to MRI in evaluating
Replacement of the Ascending Aorta in Early Childhood: Surgical Strategies and Long-Term Outcome
 Replacement of the Ascending Aorta in Early Childhood: Surgical Strategies and Long-Term Outcome Anne Moreau de Bellaing, MD O. Raisky, A. Haydar, D. Bonnet, F. Bajolle!! Unité médico-chirurgicale de Cardiologie
Replacement of the Ascending Aorta in Early Childhood: Surgical Strategies and Long-Term Outcome Anne Moreau de Bellaing, MD O. Raisky, A. Haydar, D. Bonnet, F. Bajolle!! Unité médico-chirurgicale de Cardiologie
The Ross Procedure: Outcomes at 20 Years
 The Ross Procedure: Outcomes at 20 Years Tirone David Carolyn David Anna Woo Cedric Manlhiot University of Toronto Conflict of Interest None The Ross Procedure 1990 to 2004 212 patients: 66% 34% Mean age:
The Ross Procedure: Outcomes at 20 Years Tirone David Carolyn David Anna Woo Cedric Manlhiot University of Toronto Conflict of Interest None The Ross Procedure 1990 to 2004 212 patients: 66% 34% Mean age:
Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results
 Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Which Type of Secondary Tricuspid Regurgitation Accompanying Mitral Valve Disease Should Be Surgically Treated?
 Ann Thorac Cardiovasc Surg 2013; 19: 428 434 Online January 31, 2013 doi: 10.5761/atcs.oa.12.01929 Original Article Which Type of Secondary Tricuspid Regurgitation Accompanying Mitral Valve Disease Should
Ann Thorac Cardiovasc Surg 2013; 19: 428 434 Online January 31, 2013 doi: 10.5761/atcs.oa.12.01929 Original Article Which Type of Secondary Tricuspid Regurgitation Accompanying Mitral Valve Disease Should
How to Assess and Treat Obstructive Lesions
 How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
Presenter Disclosure. Patrick O. Myers, M.D. No Relationships to Disclose
 Presenter Disclosure Patrick O. Myers, M.D. No Relationships to Disclose Aortic Valve Repair by Cusp Extension for Rheumatic Aortic Insufficiency in Children Long term Results and Impact of Extension Material
Presenter Disclosure Patrick O. Myers, M.D. No Relationships to Disclose Aortic Valve Repair by Cusp Extension for Rheumatic Aortic Insufficiency in Children Long term Results and Impact of Extension Material
The management of patients born with multiple left heart
 Predictors of Outcome of Biventricular Repair in Infants With Multiple Left Heart Obstructive Lesions Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Tal Geva, MD Background Decisions regarding surgical
Predictors of Outcome of Biventricular Repair in Infants With Multiple Left Heart Obstructive Lesions Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Tal Geva, MD Background Decisions regarding surgical
Minimalist Transcatheter Aortic Valve Replacement (MA-TAVR)
 Minimalist Transcatheter Aortic Valve Replacement (MA-TAVR) Jensen HA, Condado JF, Devireddy C, Binongo JN, Leshnower BG, Babaliaros V, Sarin EL, Lerakis S, Guyton RA, Stewart JP, Syed AQ, Mavromatis K,
Minimalist Transcatheter Aortic Valve Replacement (MA-TAVR) Jensen HA, Condado JF, Devireddy C, Binongo JN, Leshnower BG, Babaliaros V, Sarin EL, Lerakis S, Guyton RA, Stewart JP, Syed AQ, Mavromatis K,
Aortic coarctation: a benign lesion?
 Aortic coarctation: a benign lesion? A surgeon s path out of stubborness From hypoplastic arches to molecular biology Y. d'udekem The Royal Children s Hospital, Melbourne, Australia Coarctation of the
Aortic coarctation: a benign lesion? A surgeon s path out of stubborness From hypoplastic arches to molecular biology Y. d'udekem The Royal Children s Hospital, Melbourne, Australia Coarctation of the
Biventricular strategies for neonatal critical aortic stenosis: High mortality associated with early reintervention
 Hickey et al Congenital Heart Disease Biventricular strategies for neonatal critical aortic stenosis: High mortality associated with early reintervention Edward J. Hickey, MD, a Christopher A. Caldarone,
Hickey et al Congenital Heart Disease Biventricular strategies for neonatal critical aortic stenosis: High mortality associated with early reintervention Edward J. Hickey, MD, a Christopher A. Caldarone,
Long-term results (22 years) of the Ross Operation a single institutional experience
 Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
Role of Balloons and Stents in Congenital Heart Disease
 Role of Balloons and Stents in Congenital Heart Disease Rui Anjos Lisbon, Portugal No conflict of interest Balloon dilatation in Congenital Heart Disease Balloons in CHD Initially used in the 80s Learning
Role of Balloons and Stents in Congenital Heart Disease Rui Anjos Lisbon, Portugal No conflict of interest Balloon dilatation in Congenital Heart Disease Balloons in CHD Initially used in the 80s Learning
Left Ventricular Outflow Tract Obstruction
 Left Ventricular Outflow Tract Obstruction Department of Paediatrics Left Ventricular Outflow Tract Obstruction Subvalvular aortic stenosis Aortic Stenosis Supravalvular aortic stenosis Aortic Coarctation
Left Ventricular Outflow Tract Obstruction Department of Paediatrics Left Ventricular Outflow Tract Obstruction Subvalvular aortic stenosis Aortic Stenosis Supravalvular aortic stenosis Aortic Coarctation
가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY
 가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY PA c IVS (not only pulmonary valve disease) Edwards JE. Pathologic Alteration of the right heart. In: Konstam MA, Isner M, eds.
가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY PA c IVS (not only pulmonary valve disease) Edwards JE. Pathologic Alteration of the right heart. In: Konstam MA, Isner M, eds.
Prenatal Predictors of Postnatal Outcome in Pulmonary Atresia with Intact Ventricular Septum: A Multicenter Study
 Fetal Heart Society Concept Research Proposal Date: 10/20/15 Main Study Prenatal Predictors of Postnatal Outcome in Pulmonary Atresia with Intact Ventricular Septum: A Multicenter Study Shaji C. Menon,
Fetal Heart Society Concept Research Proposal Date: 10/20/15 Main Study Prenatal Predictors of Postnatal Outcome in Pulmonary Atresia with Intact Ventricular Septum: A Multicenter Study Shaji C. Menon,
Management of Difficult Aortic Root, Old and New solutions
 Management of Difficult Aortic Root, Old and New solutions Hani K. Najm MD, Msc, FRCSC,, FACC, FESC Chairman, Pediatric and Congenital Heart Surgery Cleveland Clinic Conflict of Interest None Difficult
Management of Difficult Aortic Root, Old and New solutions Hani K. Najm MD, Msc, FRCSC,, FACC, FESC Chairman, Pediatric and Congenital Heart Surgery Cleveland Clinic Conflict of Interest None Difficult
Inter-surgeon variability in long-term outcomes after transatrial repair of tetralogy of Fallot: 25 years experience with 675 patients.
 Inter-surgeon variability in long-term outcomes after transatrial repair of tetralogy of Fallot: 25 years experience with 675 patients. Y d'udekem, JC Galati, IE Konstantinov, MMH Cheung, CP Brizard Royal
Inter-surgeon variability in long-term outcomes after transatrial repair of tetralogy of Fallot: 25 years experience with 675 patients. Y d'udekem, JC Galati, IE Konstantinov, MMH Cheung, CP Brizard Royal
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Aortic Dissection in BAV Patients: The IRAD Experience and Beyond
 Aortic Dissection in BAV Patients: The IRAD Experience and Beyond Eduardo Bossone, MD, Ph.D, FESC, FACC Cardiology Division - Heart Dept. University of Salerno, Italy I have no financial relationships
Aortic Dissection in BAV Patients: The IRAD Experience and Beyond Eduardo Bossone, MD, Ph.D, FESC, FACC Cardiology Division - Heart Dept. University of Salerno, Italy I have no financial relationships
Reconstruction of the Aortic Valve and Root A Practical approach Failures after aortic valve repair. Diana Aicher. September 16 th -18 th 2015
 Reconstruction of the Aortic Valve and Root A Practical approach Failures after aortic valve repair Diana Aicher September 16 th -18 th 2015 Classification of failures- root repair 51/810 acute/ intraoperative
Reconstruction of the Aortic Valve and Root A Practical approach Failures after aortic valve repair Diana Aicher September 16 th -18 th 2015 Classification of failures- root repair 51/810 acute/ intraoperative
CIPG Transcatheter Aortic Valve Replacement- When Is Less, More?
 CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
Midterm Results of Balloon Dilation of Congenital Aortic Stenosis: Predictors of Success
 JACC Vol. 27, No. 5 1257 Midterm Results of Balloon Dilation of Congenital Aortic Stenosis: Predictors of Success PHILLIP MOORE, MD,* ERYBERTO EGITO, MD, HEATHER MOWREY, BS, STANTON B. PERRY, MD, JAMES
JACC Vol. 27, No. 5 1257 Midterm Results of Balloon Dilation of Congenital Aortic Stenosis: Predictors of Success PHILLIP MOORE, MD,* ERYBERTO EGITO, MD, HEATHER MOWREY, BS, STANTON B. PERRY, MD, JAMES
Outline. EuroScore II. Society of Thoracic Surgeons Score. EuroScore II
 SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
Severe left ventricular dysfunction and valvular heart disease: should we operate?
 Severe left ventricular dysfunction and valvular heart disease: should we operate? Laurie SOULAT DUFOUR Hôpital Saint Antoine Service de cardiologie Pr A. COHEN JESFC 16 janvier 2016 Disclosure : No conflict
Severe left ventricular dysfunction and valvular heart disease: should we operate? Laurie SOULAT DUFOUR Hôpital Saint Antoine Service de cardiologie Pr A. COHEN JESFC 16 janvier 2016 Disclosure : No conflict
Late Outcome of Survivors of Intervention for Neonatal Aortic Valve Stenosis
 Late Outcome of Survivors of Intervention for Neonatal Aortic Valve Stenosis J. William Gaynor, MD, Catherine Bull, MD, Ian D. Sullivan, MD, Brenda E. Armstrong, MD, John E. Deanfield, FRCP, James F. N.
Late Outcome of Survivors of Intervention for Neonatal Aortic Valve Stenosis J. William Gaynor, MD, Catherine Bull, MD, Ian D. Sullivan, MD, Brenda E. Armstrong, MD, John E. Deanfield, FRCP, James F. N.
Optimal initial treatment for congenital aortic valve
 ORIGINAL RESEARCH Surgical Valvotomy Versus Balloon Valvuloplasty for Congenital Aortic Valve Stenosis: A Systematic Review and Meta-Analysis Garick D. Hill, MD, MS; Salil Ginde, MD; Rodrigo Rios, MD;
ORIGINAL RESEARCH Surgical Valvotomy Versus Balloon Valvuloplasty for Congenital Aortic Valve Stenosis: A Systematic Review and Meta-Analysis Garick D. Hill, MD, MS; Salil Ginde, MD; Rodrigo Rios, MD;
E xtracardiac conduits placed between the right ventricle
 1058 INTERVENTIONAL CARDIOLOGY AND SURGERY Implantation of endovascular stents for the obstructive right ventricular outflow tract H Sugiyama, W Williams, L N Benson... See end of article for authors affiliations...
1058 INTERVENTIONAL CARDIOLOGY AND SURGERY Implantation of endovascular stents for the obstructive right ventricular outflow tract H Sugiyama, W Williams, L N Benson... See end of article for authors affiliations...
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a Patient With Severe Valvular Pulmonary Stenosis
 Case Report Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a 56-Year-Old Woman With Severe Valvular Pulmonary Stenosis: A Case Report Ata Firouzi 1, MD; Omid Shafe* 1, MD; Farzad
Case Report Percutaneous Coronary Intervention and Pulmonary Balloon Valvuloplasty in a 56-Year-Old Woman With Severe Valvular Pulmonary Stenosis: A Case Report Ata Firouzi 1, MD; Omid Shafe* 1, MD; Farzad
Indications and Late Results of Aortic Valve Repair
 Indications and Late Results of Aortic Valve Repair Prof. Gebrine El Khoury Department of Cardiovascular and Thoracic Surgery Cliniques St. Luc Brussels, Belgium Aortic Valve Repair Question # 1 Can the
Indications and Late Results of Aortic Valve Repair Prof. Gebrine El Khoury Department of Cardiovascular and Thoracic Surgery Cliniques St. Luc Brussels, Belgium Aortic Valve Repair Question # 1 Can the
Since first successfully performed by Jatene et al, the
 Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Aortic valve implantation using the femoral and apical access: a single center experience.
 Aortic valve implantation using the femoral and apical access: a single center experience. R. Hoffmann, K. Brehmer, R. Koos, R. Autschbach, N. Marx, G. Dohmen Rainer Hoffmann, University Aachen, Germany
Aortic valve implantation using the femoral and apical access: a single center experience. R. Hoffmann, K. Brehmer, R. Koos, R. Autschbach, N. Marx, G. Dohmen Rainer Hoffmann, University Aachen, Germany
Debate in Management of native COA; Balloon Versus Surgery
 Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Clinical material and methods. Fukui Cardiovascular Center, Fukui, Japan
 Mitral Valve Regurgitation after Atrial Septal Defect Repair in Adults Shohei Yoshida, Satoshi Numata, Yasushi Tsutsumi, Osamu Monta, Sachiko Yamazaki, Hiroyuki Seo, Takaaki Samura, Hirokazu Ohashi Fukui
Mitral Valve Regurgitation after Atrial Septal Defect Repair in Adults Shohei Yoshida, Satoshi Numata, Yasushi Tsutsumi, Osamu Monta, Sachiko Yamazaki, Hiroyuki Seo, Takaaki Samura, Hirokazu Ohashi Fukui
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
Introducing the COAPT Trial
 physician INFORMATION Eligible patients Symptomatic functional mitral regurgitation 3+ Not suitable candidates for open mitral valve surgery NYHA functional class II, III, or ambulatory IV Introducing
physician INFORMATION Eligible patients Symptomatic functional mitral regurgitation 3+ Not suitable candidates for open mitral valve surgery NYHA functional class II, III, or ambulatory IV Introducing
Results of Aortic Valve Preservation and Repair
 Results of Aortic Valve Preservation and Repair Department of Cardiothoracic and Vascular Surgery Cliniques Universitaires St. Luc Brussels, Belgium Gebrine Elkhoury Institutional experience in AV preservation
Results of Aortic Valve Preservation and Repair Department of Cardiothoracic and Vascular Surgery Cliniques Universitaires St. Luc Brussels, Belgium Gebrine Elkhoury Institutional experience in AV preservation
Pulmonary valve: Imaging assessment
 Pulmonary valve: Imaging assessment Fraisse Royal Brompton and Harefield Hospital London, U.K. Consultant and Proctor for medtronic Potential consequences of pulmonary valve Dysfunction RV obstruction
Pulmonary valve: Imaging assessment Fraisse Royal Brompton and Harefield Hospital London, U.K. Consultant and Proctor for medtronic Potential consequences of pulmonary valve Dysfunction RV obstruction
Valve Disease in Patients With Heart Failure TAVI or Surgery? Miguel Sousa Uva Hospital Cruz Vermelha Lisbon, Portugal
 Valve Disease in Patients With Heart Failure TAVI or Surgery? Miguel Sousa Uva Hospital Cruz Vermelha Lisbon, Portugal I have nothing to disclose. Wide Spectrum Stable vs Decompensated NYHA II IV? Ejection
Valve Disease in Patients With Heart Failure TAVI or Surgery? Miguel Sousa Uva Hospital Cruz Vermelha Lisbon, Portugal I have nothing to disclose. Wide Spectrum Stable vs Decompensated NYHA II IV? Ejection
Original Policy Date
 MP 7.01.111 Transcatheter Pulmonary Valve Implantation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to
MP 7.01.111 Transcatheter Pulmonary Valve Implantation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to
Percutaneous Mitral Valve Repair
 Percutaneous Mitral Valve Repair MitraClip: Procedure, Data, Patient Selection Chad Rammohan, MD FACC Director, Cardiac Cath Lab El Camino Hospital Mountain View, California Mitral Regurgitation MitraClip
Percutaneous Mitral Valve Repair MitraClip: Procedure, Data, Patient Selection Chad Rammohan, MD FACC Director, Cardiac Cath Lab El Camino Hospital Mountain View, California Mitral Regurgitation MitraClip
Hemodynamic Assessment After Complete Repair of Pulmonary Atresia With Major Aortopulmonary Collaterals
 Hemodynamic Assessment After Complete Repair of Pulmonary Atresia With Major Aortopulmonary Collaterals Richard D. Mainwaring, MD, V. Mohan Reddy, MD, Lynn Peng, MD, Calvin Kuan, MD, Michal Palmon, BS,
Hemodynamic Assessment After Complete Repair of Pulmonary Atresia With Major Aortopulmonary Collaterals Richard D. Mainwaring, MD, V. Mohan Reddy, MD, Lynn Peng, MD, Calvin Kuan, MD, Michal Palmon, BS,
(Ann Thorac Surg 2008;85:845 53)
 I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
Aortic Coarctation Imaging and Management in Adults. Michael D. Hope, MD
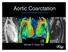 Aortic Coarctation Imaging and Management in Adults Michael D. Hope, MD 1 Background 2 Imaging - Morphology 3 Imaging - Hemodynamics 4 Associations and Complications Campbell M. British Heart Journal 1970
Aortic Coarctation Imaging and Management in Adults Michael D. Hope, MD 1 Background 2 Imaging - Morphology 3 Imaging - Hemodynamics 4 Associations and Complications Campbell M. British Heart Journal 1970
Edwards Sapien. Medtronic CoreValve. Inoperable FDA approved High risk: in trials. FDA approved
 Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Transcatheter Pulmonary Valve Implantation
 Transcatheter Pulmonary Valve Implantation Policy Number: 7.01.131 Last Review: 2/2014 Origination: 2/2012 Next Review: 2/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Transcatheter Pulmonary Valve Implantation Policy Number: 7.01.131 Last Review: 2/2014 Origination: 2/2012 Next Review: 2/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
PATENT DUCTUS ARTERIOSUS (PDA)
 PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
Comprehensive Hemodynamics By Doppler Echocardiography. The Echocardiographic Swan-Ganz Catheter.
 Comprehensive Hemodynamics By Doppler Echocardiography. The Echocardiographic Swan-Ganz Catheter. Itzhak Kronzon, MD, FASE, FACC, FESC, FAHA, FACP, FCCP North Shore HS, LIJ/Lenox Hill Hospital, New York
Comprehensive Hemodynamics By Doppler Echocardiography. The Echocardiographic Swan-Ganz Catheter. Itzhak Kronzon, MD, FASE, FACC, FESC, FAHA, FACP, FCCP North Shore HS, LIJ/Lenox Hill Hospital, New York
Percutaneous Aortic Valvuloplasty: Long-Term Survival
 Percutaneous Aortic Valvuloplasty: Long-Term Survival Angioplasty Summit Seoul April 27, 2007 James R. Margolis MD Carmen Paez MD, Kevin Coy MD, Edward Freeman PhD Miami International Cardiology Consultants
Percutaneous Aortic Valvuloplasty: Long-Term Survival Angioplasty Summit Seoul April 27, 2007 James R. Margolis MD Carmen Paez MD, Kevin Coy MD, Edward Freeman PhD Miami International Cardiology Consultants
Critical Left Ventricular Outflow Tract Obstruction (LVOTO) Fall Work Weekend Nov. 2013
 Critical Left Ventricular Outflow Tract Obstruction (LVOTO) Fall Work Weekend Nov. 03 Work Weekend Objectives General overview of cohort Generate feasible research question based on current data Early
Critical Left Ventricular Outflow Tract Obstruction (LVOTO) Fall Work Weekend Nov. 03 Work Weekend Objectives General overview of cohort Generate feasible research question based on current data Early
Transcatheter Pulmonary Valve Replacement Update on progress and outcomes
 Transcatheter Pulmonary Valve Replacement Update on progress and outcomes Barry Love, MD Director, Congenital Cardiac Catheterization Laboratory Mount Sinai Medical Center New York, New York Transcatheter
Transcatheter Pulmonary Valve Replacement Update on progress and outcomes Barry Love, MD Director, Congenital Cardiac Catheterization Laboratory Mount Sinai Medical Center New York, New York Transcatheter
The outlook for patients with hypoplastic left heart syndrome (HLHS) Tricuspid valve repair in hypoplastic left heart syndrome CHD
 Ohye et al Surgery for Congenital Heart Disease Tricuspid valve repair in hypoplastic left heart syndrome Richard G. Ohye, MD a Carlen A. Gomez, MD b Caren S. Goldberg, MD, MS b Holly L. Graves, BA a Eric
Ohye et al Surgery for Congenital Heart Disease Tricuspid valve repair in hypoplastic left heart syndrome Richard G. Ohye, MD a Carlen A. Gomez, MD b Caren S. Goldberg, MD, MS b Holly L. Graves, BA a Eric
Inflow Occlusion for Semilunar Valve Stenosis
 Inflow Occlusion for Semilunar Valve Stenosis Robert M. Sade, M.D., Fred A. Crawford, M.D., and Arno R. Hohn, M.D ABSTRACT Twenty-nine patients have had valvotomy with inflow occlusion since 1975 at our
Inflow Occlusion for Semilunar Valve Stenosis Robert M. Sade, M.D., Fred A. Crawford, M.D., and Arno R. Hohn, M.D ABSTRACT Twenty-nine patients have had valvotomy with inflow occlusion since 1975 at our
Aortic valvuloplasty (AoVP) is the therapeutic procedure
 Valvular Heart Disease Aortic Valvuloplasty in Pediatric Patients Substantially Postpones the Need for Aortic Valve Surgery A Single-Center Experience of 188 Patients After up to 17.5 Years of Follow-Up
Valvular Heart Disease Aortic Valvuloplasty in Pediatric Patients Substantially Postpones the Need for Aortic Valve Surgery A Single-Center Experience of 188 Patients After up to 17.5 Years of Follow-Up
Congenital Heart Disease. Fetal Aortic Valve Stenosis and the Evolution of Hypoplastic Left Heart Syndrome Patient Selection for Fetal Intervention
 Congenital Heart Disease Fetal Aortic Valve Stenosis and the Evolution of Hypoplastic Left Heart Syndrome Patient Selection for Fetal Intervention Kaarin Mäkikallio, MD, PhD; Doff B. McElhinney, MD; Jami
Congenital Heart Disease Fetal Aortic Valve Stenosis and the Evolution of Hypoplastic Left Heart Syndrome Patient Selection for Fetal Intervention Kaarin Mäkikallio, MD, PhD; Doff B. McElhinney, MD; Jami
CONGENITAL HEART DEFECTS IN ADULTS
 CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
MITRAL STENOSIS. Joanne Cusack
 MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
Implantation of the Melody transcatheter pulmonary valve PB1016 in patients with dysfunctional right ventricular outflow tract conduits
 Received: 20 July 2018 Revised: 26 September 2018 Accepted: 19 October 2018 DOI: 10.1002/ccd.27974 ORIGINAL STUDIES Implantation of the Melody transcatheter pulmonary valve PB1016 in patients with dysfunctional
Received: 20 July 2018 Revised: 26 September 2018 Accepted: 19 October 2018 DOI: 10.1002/ccd.27974 ORIGINAL STUDIES Implantation of the Melody transcatheter pulmonary valve PB1016 in patients with dysfunctional
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know
 Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
25 different brand names >44 different models Sizes mm
 Types of Prosthetic Valves BIOLOGIC STENTED Porcine xenograft Pericardial xenograft STENTLESS Porcine xenograft Pericardial xenograft Homograft (allograft) Autograft PERCUTANEOUS MECHANICAL Bileaflet Single
Types of Prosthetic Valves BIOLOGIC STENTED Porcine xenograft Pericardial xenograft STENTLESS Porcine xenograft Pericardial xenograft Homograft (allograft) Autograft PERCUTANEOUS MECHANICAL Bileaflet Single
Atrioventricular valve repair: The limits of operability
 Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Hypoplastic Left Heart Syndrome: Echocardiographic Assessment
 Hypoplastic Left Heart Syndrome: Echocardiographic Assessment Craig E Fleishman, MD, FACC, FASE Director, Non-invasive Cardiac Imaging The Hear Center at Arnold Palmer Hospital for Children, Orlando SCAI
Hypoplastic Left Heart Syndrome: Echocardiographic Assessment Craig E Fleishman, MD, FACC, FASE Director, Non-invasive Cardiac Imaging The Hear Center at Arnold Palmer Hospital for Children, Orlando SCAI
Valve Disease in the Pregnant Patient
 Valve Disease in the Pregnant Patient Julie B. Damp, MD December 6, 2012 VanderbiltHeart.com If single, do not allow marriage. If fertile, do not allow pregnancy. If pregnant, do not allow delivery. If
Valve Disease in the Pregnant Patient Julie B. Damp, MD December 6, 2012 VanderbiltHeart.com If single, do not allow marriage. If fertile, do not allow pregnancy. If pregnant, do not allow delivery. If
Richard L. Hallett, MD
 Richard L. Hallett, MD Chief, Cardiovascular Imaging Northwest Radiology Network Indianapolis, IN Adjunct Assistant Professor of Radiology Stanford University Hospital and Clinics Stanford, CA NASCI 2016
Richard L. Hallett, MD Chief, Cardiovascular Imaging Northwest Radiology Network Indianapolis, IN Adjunct Assistant Professor of Radiology Stanford University Hospital and Clinics Stanford, CA NASCI 2016
Annular Stabilization Techniques in the Context of Aortic Valve Repair
 Annular Stabilization Techniques in the Context of Aortic Valve Repair Prashanth Vallabhajosyula, MD MS University of Pennsylvania, Philadelphia, Pennsylvania 2 nd North American Aortic Valve Repair Symposium
Annular Stabilization Techniques in the Context of Aortic Valve Repair Prashanth Vallabhajosyula, MD MS University of Pennsylvania, Philadelphia, Pennsylvania 2 nd North American Aortic Valve Repair Symposium
NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY
 NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY FOTIOS A. MITROPOULOS, MD, PHD DEPARTMENT OF PEDIATRIC AND ADULT CONGENITAL HEART SURGERY MITERA HYGEIA HOSPITALS, ATHENS, GREECE
NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY FOTIOS A. MITROPOULOS, MD, PHD DEPARTMENT OF PEDIATRIC AND ADULT CONGENITAL HEART SURGERY MITERA HYGEIA HOSPITALS, ATHENS, GREECE
6 th European Echocardiography Course on Congenital Heart Disease
 6 th European Echocardiography Course on Congenital Heart Disease Munich, 16 th 19 th November 2011, Auditorium of the Deutsches Herzzentrum München, Lazarettstr. 36, D 80636 München Program Wednesday:
6 th European Echocardiography Course on Congenital Heart Disease Munich, 16 th 19 th November 2011, Auditorium of the Deutsches Herzzentrum München, Lazarettstr. 36, D 80636 München Program Wednesday:
Tissue vs Mechanical What s the Data??
 Biological (Tissue) Valve in a 60 year old patient: Debate Tissue vs Mechanical What s the Data?? Joseph E. Bavaria, MD Immediate-Past President - Society of Thoracic Surgeons (STS) Brooke Roberts-William
Biological (Tissue) Valve in a 60 year old patient: Debate Tissue vs Mechanical What s the Data?? Joseph E. Bavaria, MD Immediate-Past President - Society of Thoracic Surgeons (STS) Brooke Roberts-William
Parachute mitral valve: Morphologic descriptors, associated lesions, and outcomes after biventricular repair
 Parachute mitral valve: Morphologic descriptors, associated lesions, and outcomes after biventricular repair Bradley S. Marino, MD, MPP, MSCE, FACC, a,b Lydia E. Kruge, BA, b * Catherine J. Cho, MD, b
Parachute mitral valve: Morphologic descriptors, associated lesions, and outcomes after biventricular repair Bradley S. Marino, MD, MPP, MSCE, FACC, a,b Lydia E. Kruge, BA, b * Catherine J. Cho, MD, b
A Surgeon s Perspective Guidelines for the Management of Patients with Valvular Heart Disease Adapted from the 2006 ACC/AHA Guideline Revision
 A Surgeon s Perspective Guidelines for the Management of Patients with Valvular Heart Disease Adapted from the 2006 ACC/AHA Guideline Revision Prof. Pino Fundarò, MD Niguarda Hospital Milan, Italy Introduction
A Surgeon s Perspective Guidelines for the Management of Patients with Valvular Heart Disease Adapted from the 2006 ACC/AHA Guideline Revision Prof. Pino Fundarò, MD Niguarda Hospital Milan, Italy Introduction
Aortic Stenosis and TAVR TARUN NAGRANI, MD INTERVENTIONAL AND ENDOVASCULAR CARDIOLOGIST, SOMC
 Aortic Stenosis and TAVR TARUN NAGRANI, MD INTERVENTIONAL AND ENDOVASCULAR CARDIOLOGIST, SOMC No Financial Disclosures Aortic Stenosis AS is an insidious disease with a long latency period followed by
Aortic Stenosis and TAVR TARUN NAGRANI, MD INTERVENTIONAL AND ENDOVASCULAR CARDIOLOGIST, SOMC No Financial Disclosures Aortic Stenosis AS is an insidious disease with a long latency period followed by
CLINICAL COMMUNIQUE 16 YEAR RESULTS
 CLINICAL COMMUNIQUE 6 YEAR RESULTS Carpentier-Edwards PERIMOUNT Mitral Pericardial Bioprosthesis, Model 6900 Introduction The Carpentier-Edwards PERIMOUNT Mitral Pericardial Valve, Model 6900, was introduced
CLINICAL COMMUNIQUE 6 YEAR RESULTS Carpentier-Edwards PERIMOUNT Mitral Pericardial Bioprosthesis, Model 6900 Introduction The Carpentier-Edwards PERIMOUNT Mitral Pericardial Valve, Model 6900, was introduced
Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm
 CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
Long term outcomes of posterior leaflet folding valvuloplasty for mitral valve regurgitation
 Featured Article Long term outcomes of posterior leaflet folding valvuloplasty for mitral valve regurgitation Igor Gosev 1, Maroun Yammine 1, Marzia Leacche 1, Siobhan McGurk 1, Vladimir Ivkovic 1, Michael
Featured Article Long term outcomes of posterior leaflet folding valvuloplasty for mitral valve regurgitation Igor Gosev 1, Maroun Yammine 1, Marzia Leacche 1, Siobhan McGurk 1, Vladimir Ivkovic 1, Michael
Balloon Valvuloplasty and RF Perforation for PA-IVS and Critical Pulmonary Stenosis
 Balloon Valvuloplasty and RF Perforation for PA-IVS and Critical Pulmonary Stenosis Daniel Levi, MD, FSCAI Associate Professor of Pediatrics UCLA Biomedical Engineering Mattel Children s Hospital at UCLA,
Balloon Valvuloplasty and RF Perforation for PA-IVS and Critical Pulmonary Stenosis Daniel Levi, MD, FSCAI Associate Professor of Pediatrics UCLA Biomedical Engineering Mattel Children s Hospital at UCLA,
ROLE OF CONTRAST ENHANCED MR ANGIOGRAPHY IN AORTIC COARCTATION
 ROLE OF CONTRAST ENHANCED MR ANGIOGRAPHY IN AORTIC COARCTATION By Adel El Badrawy, Ahmed Abdel Razek, Nermin Soliman, Hala El Marsafawy *, Sameh Amer** From Radiodiagnosis, Pediatric Cardiology* & Cardiothoracic
ROLE OF CONTRAST ENHANCED MR ANGIOGRAPHY IN AORTIC COARCTATION By Adel El Badrawy, Ahmed Abdel Razek, Nermin Soliman, Hala El Marsafawy *, Sameh Amer** From Radiodiagnosis, Pediatric Cardiology* & Cardiothoracic
Case Report International Journal of Basic and Clinical Studies (IJBCS) 2013;1(1): Elbey MA et al.
 Treatment of Interrupted Aorta in Adult Patients; a Challenge Both in Surgery and Transcatheter Intervention Mehmet Ali Elbey MD 1, Ahmet Caliskan MD 2, Ferhat Isık MD 1, Faruk Ertas MD 1, Mehmet Serdar
Treatment of Interrupted Aorta in Adult Patients; a Challenge Both in Surgery and Transcatheter Intervention Mehmet Ali Elbey MD 1, Ahmet Caliskan MD 2, Ferhat Isık MD 1, Faruk Ertas MD 1, Mehmet Serdar
Mechanisms of Recurrent Aortic Regurgitation After Aortic Valve Repair
 JACC: CARDIOVASCULAR IMAGING VOL. 2, NO. 8, 2009 2009 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-878X/09/$36.00 PUBLISHED BY ELSEVIER INC. DOI:10.1016/j.jcmg.2009.04.013 Mechanisms of Recurrent
JACC: CARDIOVASCULAR IMAGING VOL. 2, NO. 8, 2009 2009 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-878X/09/$36.00 PUBLISHED BY ELSEVIER INC. DOI:10.1016/j.jcmg.2009.04.013 Mechanisms of Recurrent
Uptofate Study Summary
 CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
