Peripheral Circulation and Regulation
|
|
|
- Bertina Jefferson
- 6 years ago
- Views:
Transcription
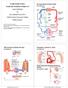
1 Peripheral Circulation and Regulation Functions of Peripheral Circulation 1. Contain the blood 2. Exchange nutrients, waste products, and gases with tissues 3. Transport 4. Regulate blood pressure, along with cardiac output 5. Control direction of blood flow 6. Participate in thermoregulation Blood Vessel Structure and Function Blood vessels closed system delivery system of dynamic structures that begins and ends at heart Work with lymphatic system to circulate fluids Arteries - delivery carry blood away from ventricles oxygenated except for pulmonary circulation and umbilical arteries of fetus closer to the heart, greater the pressure artery must tolerate Capillaries - exchange Numerous small vessels = high surface area direct contact with tissue cells; directly serve cellular needs endothelium only one layer of squamous cells Veins - return carry blood toward atria deoxygenated except for pulmonary circulation and umbilical veins of fetus Built to tolerate lower blood pressures and prevent backflow 60,000 miles of vessels in average body Large veins (capacitance vessels) Venous pathways are more interconnected Venous system Heart Large lymphatic vessels Lymph node Lymphatic system Arterial system Elastic arteries (conducting arteries) Muscular arteries (distributing arteries) Note subdivisions and by-pass vessels Small veins (capacitance vessels) Arteriovenous anastomosis Lymphatic capillaries Arteries run deep, whereas veins are both deep and superficial Sinusoid Arterioles (resistance vessels) Postcapillary venule Thoroughfare channel Capillaries (exchange vessels) Precapillary sphincter Terminal arteriole Metarteriole 1
2 Photomicrograph of Artery and Vein lumen Or externa Structure of Blood Vessel Wall Tunica intima Smooth, friction-reducing, innermost layer in contact with blood Endothelium: simple squamous epithelium lines lumen of all vessels is continuous with endocardium Tunica media Middle layer composed mostly of smooth muscle and sheets of elastin Sympathetic vasomotor nerve fibers innervate this layer Thickest in arteries - responsible for maintaining blood flow and blood pressure Tunica externa Outermost layer of wall mostly loose collagen fibers that protect and reinforce wall and anchor it to surrounding structures Infiltrated with nerve fibers, lymphatic vessels, and Vasa vasorum Capillaries Endothelium with sparse basal lamina Artery Tunica intima Endothelium Subendothelial layer Internal elastic membrane Tunica media (smooth muscle and elastic fibers) External elastic membrane Tunica externa (collagen fibers) Vasa vasorum Valve Vein Lumen Capillary network Lumen Capillary Basement membrane Endothelial cells Vasomotor tone: what s up with that? 2
3 conducting arteries -maintain pressure between contractions distributing arteries -deliver to organs resistance arteries -control perfusion locally capacitance vessels - Serve as blood reservoir Capillaries Functions: exchange between blood and interstitial fluid Small diameter vessels force RBCs to pass in single file Slows flow and promotes exchange Thin tunica intima; in smallest vessels, one cell forms entire circumference Supply almost every cell, except for cartilage, epithelia, cornea, and lens of eye Continuous capillary Continuous capillaries are the least permeable and most common. Pericyte Red blood cell in lumen Basement membrane Tight junction Endothelial nucleus Intercellular cleft Endothelial cell Pinocytotic vesicles Continuous Capillaries: Abundant in skin, muscles, lungs, and CNS. Often have associated pericytes. Pinocytotic vesicles ferry fluid across the endothelial cell. Brain capillary endothelial cells lack intercellular clefts and have tight junctions around their entire perimeter. Fenestrated Capillary: Occur in areas of active filtration (e.g., kidney) or absorption (e.g., small intestine), and areas of endocrine hormone secretion. Fenestrated capillary Fenestrated capillaries have large fenestrations (pores) that increase permeability. Pinocytotic vesicles Red blood cell in lumen Fenestrations (pores) Endothelial nucleus Basement membrane Intercellular cleft Endothelial cell Tight junction Fenestrations are Swiss cheese like holes that tunnel through endothelial cells. usually covered by a very thin diaphragm Readily allows solute and fluid movement. In some digestive tract organs, the number of fenestrations in capillaries increases during active absorption of nutrients. 3
4 Sinusoidal Capillaries: Occur in liver, bone marrow, spleen, and adrenal medulla. Have large intercellular clefts as well as fenestrations; few tight junctions; incomplete basement membranes. Are irregularly shaped and have larger lumens than other capillaries. Sinusoid capillary Sinusoid capillaries are the most permeable and occur in limited locations. Endothelial cell Red blood cell in lumen Large intercellular cleft Tight junction Incomplete basement membrane Nucleus of endothelial cell Allow large molecules and even cells to pass across their walls. Blood flows slowly through their channels. Macrophages may extend processes through the clefts to catch prey or, in liver, form part of the sinusoid wall. Anatomy of a capillary bed. Capillary bed: interwoven network of capillaries between arterioles and venules Microcirculation: flow of blood through bed Precapillary sphincters Terminal arteriole Metarteriole Vascular shunt Thoroughfare channel True capillaries Postcapillary venule Sphincters open blood flows through true capillaries. Capillary beds vessels 1. Vascular shunt: channel that connects arteriole directly with venule (metarteriole thoroughfare channel) 2. True capillaries: actual vessels involved in exchange Terminal arteriole Postcapillary venule Sphincters closed blood flows through metarteriole thoroughfare channel and bypasses true capillaries. Relative crosssectional area of different vessels of the vascular bed Total area (cm 2 ) of the vascular bed Velocity of blood flow (cm/s)
5 Capillary transport mechanisms Venules postcapillary venules consist of endothelium and a few pericytes Very porous; allow fluids and WBCs into tissues Larger venules have one or two layers of smooth muscle cells Veins Have all tunics Large lumen and thin walls make veins good storage vessels Blood pressure lower than in arteries, so adaptations ensure return of blood to heart Large-diameter lumens offer little resistance Venous valves Prevent backflow of blood Most abundant in veins of limbs filling effect Relative proportion of blood volume throughout the cardiovascular system. Pulmonary blood Systemic arteries and arterioles 15% vessels 12% Heart 8% Capillaries 5% Systemic veins and venules 60% Venous reservoir provides a source of blood to fill dilating arteries upon initiation of exercise compensation to maintain blood pressure Lumen Caveolae Pinocytotic vesicles Intercellular cleft Endothelial fenestration (pore) 4 Transport via vesicles or caveolae (large substances) 1 Diffusion through membrane (lipid-soluble substances) Basement membrane 2 Movement through intercellular clefts (water-soluble substances) 3 Movement through fenestrations (water-soluble substances) 5
6 Fluid Movements Out of Capillaries Capillary pressures 35 mm Hg at beginning of capillary bed 17 mm Hg at the end of the bed Low capillary pressure is desirable Fluid is forced out clefts of capillaries at arterial end, and most returns to blood at venous end Bulk fluid flow across capillary walls causes continuous mixing of fluid between plasma and interstitial fluid; maintains interstitial environment. Direction and amount of fluid flow depend on two opposing forces Hydrostatic pressures Colloid osmotic pressures Hydrostatic pressure (HP) Capillary hydrostatic pressure (HP c ) Interstitial fluid hydrostatic pressure (HP if ): assumed to be zero because lymphatic vessels drain interstitial fluid Capillary colloid osmotic pressure (oncotic pressure, OP c ) Remember the presence of plasma proteins Interstitial fluid colloid osmotic pressure (OP if ) inconsequential Hydrostatic-osmotic pressure interactions Net filtration pressure (NFP): NFP = (HP c + OP if) (HP if + OP c) Net fluid flow out at arterial end (filtration) Net fluid flow in at venous end (reabsorption) More fluid leaves at arterial end than is returned at venous end Excess interstitial fluid is returned to blood via lymphatic system How do the pressures drive fluid flow across a capillary? Net filtration occurs at the arteriolar end of a capillary. Capillary lumen Boundary (capillary wall) Interstitial fluid Hydrostatic pressure in capillary (HP c) pushes fluid out of capillary. HPc = 35 mm Hg Osmotic pressure in capillary (OPc) pulls fluid into capillary. OP c = 26 mm Hg Hydrostatic pressure HPif = 0 mm Hg (HP if) in interstitial fluid pushes fluid into capillary. Let s use w hat w e know about pressures to determine the net filtration pressure (NFP) at any point. (NFP is the pressure driving fluid out of the capillary.) To do this w e calculate the outw ard pressures (HP c and OP if) minus the inw ard pressures (HP if and OP c). So, OP if = 1 mm Hg Osmotic pressure (OPif) in interstitial fluid pulls fluid out of capillary. NFP = (HP c + OP if) (HP if + OP c) = (35 + 1) (0 + 26) = 10 mm Hg (net outward pressure) NFP = 10 mm Hg As a result, fluid moves from the capillary into the interstitial space. 6
7 Venule Arteriole Fluid moves through the interstitial space. Lymphatic capillary Net reabsorption occurs at the venous end of a capillary. Capillary lumen Hydrostatic pressure in capillary pushes fluid out of capillary. The pressure has dropped because of resistance encountered along the capillaries. HP c = 17 mm Hg Boundary (capillary wall) Interstitial fluid Osmotic pressure in capillary pulls fluid into capillary. OP c = 26 mm Hg HP if = 0 mm Hg OP if = 1 mm Hg NFP= 8 mm Hg Hydrostatic pressure in interstitial fluid pushes fluid into capillary. Osmotic pressure in interstitial fluid pulls fluid out of capillary. Again, w e calculate the NFP: NFP = (HP c + OP if) (HP if + OP c) = (17 + 1) (0 + 26) = 8 mm Hg (net inw ard pressure) Notice that the NFP at the venous end is a negative number. This means that reabsorption, not filtration, is occurring and so fluid moves from the interstitial space into the capillary. Arterial side NFP = 10; venous side NFP = -8 Capillary bed NFP is therefore 10 8 = 2 mm Hg 2 mm Hg pressure causes a net fluid loss from bed to tissues The big picture Each day, 20 L of fluid filters from capillaries at their arteriolar end and flows through the interstitial space. Most (17 L) is reabsorbed at the venous end. For all capillary beds, 20 L of fluid is filtered out per day almost 7 times the total plasma volume! 17 L of fluid per day is reabsorbed into the capillaries at the v enous end. About 3 L per day of fluid (and any leaked proteins) are removed by the lymphatic system Control Over Blood Pressure and Flow Blood pressure (BP) Expressed in mm Hg, systolic over diastolic Measured as systemic arterial BP in large arteries at same level as heart Pressure gradient provides driving force that keeps blood moving from higher- to lower-pressure areas Blood flow Measured in ml/min Overall is relatively constant when at rest, varies at individual organ level, based on needs Resistance (peripheral resistance) Measurement of amount of friction blood encounters with vessel walls, generally in peripheral (systemic) circulation Three important sources of resistance Blood viscosity Total blood vessel length Blood vessel diameter Turbulent flow constrictions in vessel interrupt laminar flow, eddys result Laminar flow frictional forces slow blood in direct contact with endothelium 7
8 Blood pressure (mm Hg) Blood viscosity The thickness or stickiness of blood due to formed elements and plasma proteins Increased viscosity equals increased resistance Increasing hematocrit increases viscosity Total blood vessel length The longer the vessel, the greater the resistance encountered Essentially remains constant once adulthood is reached Goal of blood pressure regulation is to keep blood pressure high enough to provide adequate tissue perfusion, but not so high that blood vessels are damaged Example: If BP to brain is too low, perfusion is inadequate, and person loses consciousness If BP to brain is too high, person could have stroke Pulse Pressure = mmhg Systolic pressure Diastolic pressure Mean pressure Pumping action of heart generates blood flow Pressure results when flow is opposed by resistance Systemic pressure is highest in aorta and declines throughout pathway Steepest drop occurs in arterioles Arterial Blood Pressure Pulse pressure and MAP both decline with increasing distance from heart With increasing distance, flow is nonpulsatile with a steady MAP pressure 8
9 Measuring Arterial Blood Pressure using auscultatory methods and a sphygmomanometer 1. Wrap cuff around arm superior to elbow 2. Increase pressure in cuff until it exceeds systolic pressure in brachial artery 3. Pressure is released slowly, and examiner listens for sounds of Korotkoff with a stethoscope Venous Blood Pressure Small pressure gradient, only about 15 mm Hg Factors aiding venous return 1. Backflow prevention 2. Muscular pump 3. Respiratory pump 4. Sympathetic venoconstriction The muscular pump. Venous valve (open) Contracted skeletal muscle Venous valve (closed) Vein Direction of blood flow 9
10 Regulation of Blood Pressure Maintaining blood pressure requires cooperation of heart, blood vessels, and kidneys All supervised by brain Three main factors regulating blood pressure Cardiac output (CO) Peripheral resistance (PR or just R) Blood volume Blood pressure varies directly with CO, PR, and blood volume Poiseuille s Law Simplifying: Flow = π ( P) r v l P = P 1 P 2 or the change in pressure over the length of the vessel v is the viscosity of the blood l is the length of the blood vessel from P 1 to P 2 r is the radius of the blood vessel (diameter = 2r) π is a constant 1. Resistance to flow is caused by viscosity, vessel length, and vessel radius 1. Once mature, length of vessel fairly constant no impact 2. Viscosity and flow are inversely proportional Homeostatic mechanisms control viscosity 3. Small changes in radius or diameter (vasoconstriction/dilation) significantly impact flow 2. Minimum pressure differential required - no difference, no flow a) Must maintain pressure above critical closing pressure b) Heart as the generator of pressure can compensate Regulation of Blood Pressure MAP = SV HR R Anything that increases SV, HR, or R will also increase MAP SV is affected by venous return (EDV) HR is maintained by medullary centers R is affected mostly by vessel diameter 10
11 Regulation of Blood Pressure Factors can be affected by: Short-term regulation: neural controls Neural controls operate via reflex arcs that involve: Cardiovascular center of medulla Baroreceptors Chemoreceptors Higher brain centers Short-term regulation: hormonal controls Long-term regulation: renal controls Baroreceptor reflex 2 Baroreceptors in carotid sinuses and aortic arch are stimulated. 1 Stimulus: Blood pressure (arterial blood pressure rises above normal range). 5 CO and R return blood pressure to homeostatic range. 3 Impulses from baroreceptors stimulate cardioinhibitorycenter (and inhibit cardioacceleratory center) and inhibit vasomotor center. 4b Rate of vasomotor impulses allows vasodilation, causing R. Homeostasis: Blood pressure in normal range 4b Vasomotor fibers stimulate vasoconstriction, causing R. 4a Sympathetic impulses to heart cause HR, contractility, and CO. 5 CO and R return blood pressure to homeostatic range. 1 Stimulus: Blood pressure (arterial blood pressure falls below normal range). 4a Sympathetic impulses to heart Cause HR, contractility, and CO. 3 Impulses from baroreceptors activate cardioacceleratorycenter (and inhibit cardioinhibitorycenter) and stimulate vasomotor center. 2 Baroreceptors in carotid sinuses and aortic arch are inhibited Short-Term Regulation: Neural Controls (cont.) Chemoreceptor reflexes Aortic arch and large arteries of neck detect increase in CO 2, or drop in ph or O 2 Cause increased blood pressure by: Signaling cardioacceleratory center to increase CO Signaling vasomotor center to increase vasoconstriction Influence of higher brain centers Reflexes that regulate BP are found in medulla Hypothalamus and cerebral cortex can modify arterial pressure via relays to medulla increases blood pressure during stress mediates redistribution of blood flow during exercise and changes in body temperature 11
12 Long-Term Mechanisms: Renal Regulation Short-Term Mechanisms: Hormonal Controls Hormones regulate BP in short term via changes in peripheral resistance or long term via changes in blood volume Adrenal medulla hormones Epinephrine and norepinephrine from adrenal gland increase CO and vasoconstriction Angiotensin II stimulates vasoconstriction ADH (or vasopressin): high levels can cause vasoconstriction Atrial natriuretic peptide decreases BP by antagonizing aldosterone, causing decreased blood volume Direct renal mechanism Indirect renal mechanism (renin-angiotensin-aldosterone) Arterial pressure Arterial pressure Initial stimulus Physiological response Result Inhibits baroreceptors Sympathetic nervous system activ ity Filtration by kidneys Angiotensinogen Renin release from kidneys Angiotensin I Angiotensin conv erting enzyme (ACE) Angiotensin II Urine formation Adrenal cortex ADH release by posterior pituitary Thirst v ia hypothalamus Vasoconstriction; peripheral resistance Secretes Aldosterone Blood v olume Sodium reabsorption by kidneys Water reabsorption by kidneys Water intake Blood v olume Mean arterial pressure Mean arterial pressure Summary of Factors that Increase MAP Activity of muscular pump and respiratory pump Release of ANP Fluid loss from hemorrhage, excessive sweating Crisis stressors: exercise, trauma, body temperature Vasomotor tone; bloodborne chemicals (epinephrine, NE, ADH, angiotensin II) Dehydration, high hematocrit Body size Conservation of Na + and water by kidneys Blood volume Blood pressure Blood ph O 2 CO 2 Blood volume Baroreceptors Chemoreceptors Venous return Activation of vasomotor and cardioacceleratory centers in brain stem Stroke volume Heart rate Diameter of blood vessels Blood viscosity Blood vessel length Cardiac output Peripheral resistance Initial stimulus Physiological response Result Mean arterial pressure (MAP) 12
13 Control of Blood Flow Tissue perfusion: blood flow through body tissues; involved in: 1. Delivery of O 2 and nutrients to, and removal of wastes from, tissue cells 2. Gas exchange (lungs) 3. Absorption of nutrients (digestive tract) 4. Urine formation (kidneys) Rate of blood flow is controlled by extrinsic and intrinsic factors Extrinsic control: sympathetic nervous system and hormones control blood flow through whole body Intrinsic control: Autoregulation (local) control of blood flow: blood flow is adjusted locally to meet specific tissue s requirements Local arterioles that feed capillaries can undergo modification of their diameters Organs regulate own blood flow by varying resistance of own arterioles Metabolic controls smooth muscle response to metabolic wastes Myogenic controls smooth muscle response to increasing and decreasing MAP Long-term autoregulation angiogenesis and vessel enlargement Intrinsic and extrinsic control of arteriolar smooth muscle in the systemic circulation Intrinsic controls (autoregulation) Metabolic or myogenic controls Distribute blood flow to individual organs and tissues as needed Vasodilators Metabolic Neural O2 Sympathetic tone CO2 H + Hormonal K + Atrial natriuretic Prostaglandins peptide Adenosine Nitric oxide Vasoconstrictors Extrinsic controls Neural or hormonal controls Maintain mean arterial pressure (MAP) Redistribute blood during exercise and thermoregulation Myogenic Stretch Metabolic Endothelins Neural Sympathetic tone Hormonal Angiotensin II Antidiuretic hormone Epinephrine Norepinephrine 750 Brain Heart Skeletal muscles Skin ,500 Kidneys 1100 Abdomen Other Total blood flow at rest 5800 ml/min Total blood flow during strenuous exercise 17,500 ml/min 13
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Copyright 2010 Pearson Education, Inc. Blood Vessel Structure
 Blood Vessel Structure Structure of Blood Vessel Walls Arteries and veins Tunica intima, tunica media, and tunica externa Lumen Central blood-containing space Capillaries Endothelium with sparse basal
Blood Vessel Structure Structure of Blood Vessel Walls Arteries and veins Tunica intima, tunica media, and tunica externa Lumen Central blood-containing space Capillaries Endothelium with sparse basal
Cardiovascular System. Blood Vessel anatomy Physiology & regulation
 Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular system: Blood vessels, blood flow. Latha Rajendra Kumar, MD
 Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Chapter 21 Peripheral circulation and Regulation
 Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Types of Blood Vessels
 Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
Physiology of Circulation
 Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Blood Vessels. Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels. Veins carry blood toward the heart
 C H A P T E R Blood Vessels 20 Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels The site of exchange of molecules between blood and tissue fluid Veins
C H A P T E R Blood Vessels 20 Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels The site of exchange of molecules between blood and tissue fluid Veins
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation
 Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
UNIT 4: BLOOD VESSELS
 UNIT 4: BLOOD VESSELS Dr. Moattar Raza Rizvi NRS237, Physiology Generalized Structure of Blood Vessels 1 Tunica interna (tunica intima) Endothelial layer that lines the lumen of all vessels In vessels
UNIT 4: BLOOD VESSELS Dr. Moattar Raza Rizvi NRS237, Physiology Generalized Structure of Blood Vessels 1 Tunica interna (tunica intima) Endothelial layer that lines the lumen of all vessels In vessels
The Cardiovascular System: Vessels and Routes. Pulmonary Circulation H E A R T. Systemic Circulation
 The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
Arteries AWAY. Branch. Typically oxygenated.
 Arteries AWAY Branch Typically oxygenated. Capillaries Smallest. Most abundant. 10 billion. Huge surface area. Exchange Veins TOWARDS Converge. Typically deoxygenated. 3 Layers of the Vascular Wall Tunica
Arteries AWAY Branch Typically oxygenated. Capillaries Smallest. Most abundant. 10 billion. Huge surface area. Exchange Veins TOWARDS Converge. Typically deoxygenated. 3 Layers of the Vascular Wall Tunica
Cardiovascular System Blood Vessels
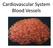 Cardiovascular System Blood Vessels Structure of Blood Vessels The three layers (tunics) Tunica intima composed of simple squamous epithelium Tunica media sheets of smooth muscle Contraction vasoconstriction
Cardiovascular System Blood Vessels Structure of Blood Vessels The three layers (tunics) Tunica intima composed of simple squamous epithelium Tunica media sheets of smooth muscle Contraction vasoconstriction
Chapter 21! Chapter 21 Blood Vessels and Circulation! Blood Vessels and Circulation!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Blood Vessels. Over view. We have about 60,000 miles of blood vessels!
 Blood Vessels Over view 3 types of blood vessels arteries - carry blood away from heart "branch", "diverge", and "fork" veins - carry blood toward heart "join", "merge", and "converge" capillaries - site
Blood Vessels Over view 3 types of blood vessels arteries - carry blood away from heart "branch", "diverge", and "fork" veins - carry blood toward heart "join", "merge", and "converge" capillaries - site
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21 (1) An Introduction to Blood Vessels and Circulation
 Chapter 21 (1) An Introduction to Blood Vessels and Circulation Lecture Objectives Compare and contrast the structure of an artery, arteriole, vein, venule, and capillary Discuss the structure and function
Chapter 21 (1) An Introduction to Blood Vessels and Circulation Lecture Objectives Compare and contrast the structure of an artery, arteriole, vein, venule, and capillary Discuss the structure and function
Chapter 19: Blood Vessels. 63 slides
 Chapter 19: Blood Vessels 63 slides 1 Blood Vessels The Blood Vessels are essentially a series of tubes. Three types of blood vessel tubes: Arteries (carry blood away from heart) Arterioles are the smallest
Chapter 19: Blood Vessels 63 slides 1 Blood Vessels The Blood Vessels are essentially a series of tubes. Three types of blood vessel tubes: Arteries (carry blood away from heart) Arterioles are the smallest
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
The Cardiovascular system: physiology of circulation
 Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Vascular System Part One
 Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM
 Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
I. Cardiac Output Chapter 14
 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
Blood Vessels. Chapter 20
 Blood Vessels Chapter 20 Summary of the Characteristics of Arteries and Veins Characteristic Artery Vein Wall thickness thick thin Shape in cross section round flattened Thickest tunic media externa Collagen
Blood Vessels Chapter 20 Summary of the Characteristics of Arteries and Veins Characteristic Artery Vein Wall thickness thick thin Shape in cross section round flattened Thickest tunic media externa Collagen
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
The cardiovascular system
 The cardiovascular system Components of the Cardiovascular system Heart Vessels: Arteries Capillaries Veins Functions of CVS: Transportation system where blood is the transporting vehicle Carries oxygen,
The cardiovascular system Components of the Cardiovascular system Heart Vessels: Arteries Capillaries Veins Functions of CVS: Transportation system where blood is the transporting vehicle Carries oxygen,
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) VESSELS P1 OF 7
 BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) VESSELS P1 OF 7 1. Blood vessels a. Tubes through which the heart pumps blood. b. 3 major types of blood vessels: arteries, capillaries,
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) VESSELS P1 OF 7 1. Blood vessels a. Tubes through which the heart pumps blood. b. 3 major types of blood vessels: arteries, capillaries,
Any of these questions could be asked as open question or lab question, thus study them well
 Any of these questions could be asked as open question or lab question, thus study them well describe the factors which regulate cardiac output describe the sympathetic and parasympathetic control of heart
Any of these questions could be asked as open question or lab question, thus study them well describe the factors which regulate cardiac output describe the sympathetic and parasympathetic control of heart
Physiology of Circulation. Dr. Hiwa Shafiq 16/12/2018
 Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
2. capillaries - allow exchange of materials between blood and tissue fluid
 Chapter 19 - Vascular System A. categories and general functions: 1. arteries - carry blood away from heart 2. capillaries - allow exchange of materials between blood and tissue fluid 3. veins - return
Chapter 19 - Vascular System A. categories and general functions: 1. arteries - carry blood away from heart 2. capillaries - allow exchange of materials between blood and tissue fluid 3. veins - return
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Histology of the Cardiac System. Dr. Nabil Khoury Anatomy Department
 Histology of the Cardiac System Dr. Nabil Khoury Anatomy Department Objectives 1. Identify the 3 layers of the heart endocardium, myocardium, epicardium 2. Differentiate cardiacmuscle 3. Define intercalated
Histology of the Cardiac System Dr. Nabil Khoury Anatomy Department Objectives 1. Identify the 3 layers of the heart endocardium, myocardium, epicardium 2. Differentiate cardiacmuscle 3. Define intercalated
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Cardivascular System Module 5: Structure and Function of Blood Vessels *
 OpenStax-CNX module: m49689 1 Cardivascular System Module 5: Structure and Function of Blood Vessels * Donna Browne Based on Structure and Function of Blood Vessels by OpenStax This work is produced by
OpenStax-CNX module: m49689 1 Cardivascular System Module 5: Structure and Function of Blood Vessels * Donna Browne Based on Structure and Function of Blood Vessels by OpenStax This work is produced by
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Collin County Community College
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 6 Blood Vessels 1 Anatomy of Blood Vessels Walls of blood vessels contain 3 distinct layers : Tunica intima innermost layer includes
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 6 Blood Vessels 1 Anatomy of Blood Vessels Walls of blood vessels contain 3 distinct layers : Tunica intima innermost layer includes
Microcirculation. Lecture Block 11 (contributions from Brett Burton)
 Lecture Block 11 (contributions from Brett Burton) Elements of Arterioles, capillaries, venules Structure and function: transport Fluid balance Lymph system Vessels of the Circulatory System Diameter Aorta
Lecture Block 11 (contributions from Brett Burton) Elements of Arterioles, capillaries, venules Structure and function: transport Fluid balance Lymph system Vessels of the Circulatory System Diameter Aorta
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Cardiovascular System B L O O D V E S S E L S 3
 Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Blood Flow, Blood Pressure, Cardiac Output. Blood Vessels
 Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
Structure. Arteries. 21_01d 4/18/12. The Cardiovascular System: Blood Vessels and Hemodynamics. Dr Badri Paudel GMC
 Goal of the Cardiovascular System: deliver blood to all parts of the body The Cardiovascular System: Blood Vessels and Hemodynamics Dr Badri Paudel GMC Does so by using different types of tubing, attached
Goal of the Cardiovascular System: deliver blood to all parts of the body The Cardiovascular System: Blood Vessels and Hemodynamics Dr Badri Paudel GMC Does so by using different types of tubing, attached
Physiology lecture 15 Hemodynamic
 Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
12/02/2012. Chapter 19: Blood Vessels. Blood Vessel Structure and Function
 Chapter 19: Blood Vessels 12/02/2012 Blood Vessel Structure and Function 3 major types: arteries capillaries veins as heart contracts it forces blood into the large arteries leaving the ventricles then
Chapter 19: Blood Vessels 12/02/2012 Blood Vessel Structure and Function 3 major types: arteries capillaries veins as heart contracts it forces blood into the large arteries leaving the ventricles then
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
1. Distinguish among the types of blood vessels on the basis of their structure and function.
 Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
CHAPTER 21 LECTURE OUTLINE
 CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
Major Function of the Cardiovascular System. Transportation. Structures of the Cardiovascular System. Heart - muscular pump
 Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 5 Cardiovascular System 3 Vasculature and Capillary Exchange Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Structure
BIOH122 Human Biological Science 2 Session 5 Cardiovascular System 3 Vasculature and Capillary Exchange Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Structure
Cardiovascular Physiology
 Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular (Circulatory) System
 Cardiovascular (Circulatory) System Piryaei May 2011 Circulatory System Heart Blood Vessels Macrovasculature (More than 0.1mm) Elastic Artery Muscular (Distributing) Artery Large Arteriol Small Vein Muscular
Cardiovascular (Circulatory) System Piryaei May 2011 Circulatory System Heart Blood Vessels Macrovasculature (More than 0.1mm) Elastic Artery Muscular (Distributing) Artery Large Arteriol Small Vein Muscular
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Chapter 21. Blood Vessels and Circulation
 Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
2402 : Anatomy/Physiology
 Dr. Chris Doumen Lecture 1 2402 : Anatomy/Physiology Hemo Dynamics and Blood Vessels I nt r oduc t i on TextBook Readings Pages 721 through 734. Make use of the figures in your textbook ; a picture is
Dr. Chris Doumen Lecture 1 2402 : Anatomy/Physiology Hemo Dynamics and Blood Vessels I nt r oduc t i on TextBook Readings Pages 721 through 734. Make use of the figures in your textbook ; a picture is
Blood vessels are the tubes through which the heart pumps blood. There are 3 major types of blood vessels: arteries, capillaries, and veins.
 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) VESSELS P1 OF 1 Blood vessels are the tubes through which the heart pumps blood. There are 3 major types of blood vessels: arteries, capillaries, and
LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) VESSELS P1 OF 1 Blood vessels are the tubes through which the heart pumps blood. There are 3 major types of blood vessels: arteries, capillaries, and
PHYSIOLOGY WEEK 9. vascular physiology - ED Primary Exam Teaching
 PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
The Cardiovascular and Lymphatic Systems Cardiovascular System Blood Vessels Blood Vessels Arteries Arteries Arteries
 CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
Chapter 21. Blood Vessels and Circulation
 Chapter 21 Openstax: Chapter 20 Blood Vessels and Circulation Chapter 21 Learning Outcomes After completing Chapter 21, you will be able to: 1. Distinguish among the types of blood vessels based on their
Chapter 21 Openstax: Chapter 20 Blood Vessels and Circulation Chapter 21 Learning Outcomes After completing Chapter 21, you will be able to: 1. Distinguish among the types of blood vessels based on their
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Anatomy and Physiology, Spring 2015 Exam II: Form A April 9, Name Student Number
 Anatomy and Physiology, Spring 2015 Exam II: Form A April 9, 2015 Name Student Number For Questions 1 2 refer to the following table. 1 Ventricular pressure is greater than aortic 6 AV valve is open 2
Anatomy and Physiology, Spring 2015 Exam II: Form A April 9, 2015 Name Student Number For Questions 1 2 refer to the following table. 1 Ventricular pressure is greater than aortic 6 AV valve is open 2
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Citation Jarvis S (2018) Vascular system 1: anatomy and physiology. Nursing Times [online]; 114: 4,
![Citation Jarvis S (2018) Vascular system 1: anatomy and physiology. Nursing Times [online]; 114: 4, Citation Jarvis S (2018) Vascular system 1: anatomy and physiology. Nursing Times [online]; 114: 4,](/thumbs/96/127077409.jpg) Vascular system Keywords Arteries/Veins// Blood flow/fluid movement This article has been double-blind peer reviewed In this article... Anatomy of the vascular system and structure of blood vessels The
Vascular system Keywords Arteries/Veins// Blood flow/fluid movement This article has been double-blind peer reviewed In this article... Anatomy of the vascular system and structure of blood vessels The
Essentials of Anatony and Physiology, 5e (Martini/Nath) Chapter 13 The Cardiovascular System: Blood Vessels and Circulation
 Essentials of Anatony and Physiology, 5e (Martini/Nath) Chapter 13 The Cardiovascular System: Blood Vessels and Circulation Multiple-Choice Questions 1) The muscular layer of blood vessels is the A) tunica
Essentials of Anatony and Physiology, 5e (Martini/Nath) Chapter 13 The Cardiovascular System: Blood Vessels and Circulation Multiple-Choice Questions 1) The muscular layer of blood vessels is the A) tunica
Cardiovascular System: Vessels and Circulation (Chapter 21)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Derived copy of Structure and Function of Blood Vessels *
 OpenStax-CNX module: m56696 1 Derived copy of Structure and Function of Blood Vessels * Stephanie Fretham Based on Structure and Function of Blood Vessels by OpenStax This work is produced by OpenStax-CNX
OpenStax-CNX module: m56696 1 Derived copy of Structure and Function of Blood Vessels * Stephanie Fretham Based on Structure and Function of Blood Vessels by OpenStax This work is produced by OpenStax-CNX
Human Anatomy, First Edition
 Human Anatomy, First Edition McKinley & O'Loughlin Chapter 23 : Vessels and Circulation 23-1 Blood Vessels An efficient style of transport for oxygen, nutrients, and waste products to and from body tissues.
Human Anatomy, First Edition McKinley & O'Loughlin Chapter 23 : Vessels and Circulation 23-1 Blood Vessels An efficient style of transport for oxygen, nutrients, and waste products to and from body tissues.
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
The Cardiovascular System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11PART B The Heart: Cardiac Output Cardiac output (CO) Amount of blood pumped
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11PART B The Heart: Cardiac Output Cardiac output (CO) Amount of blood pumped
Fluid and Electrolytes P A R T 2
 Fluid and Electrolytes P A R T 2 Fluid Shifts Extracellular fluid distribution is dynamic Interstitial fluid formation is continuous Venous system Large veins (capacitance vessels) Small veins (capacitance
Fluid and Electrolytes P A R T 2 Fluid Shifts Extracellular fluid distribution is dynamic Interstitial fluid formation is continuous Venous system Large veins (capacitance vessels) Small veins (capacitance
Cardiovascular System
 Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Microcirculation and Edema. Faisal I. Mohammed MD, PhD.
 Microcirculation and Edema Faisal I. Mohammed MD, PhD. Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchang in capillaries. Outline what
Microcirculation and Edema Faisal I. Mohammed MD, PhD. Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchang in capillaries. Outline what
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
The Circulatory System
 The Circulatory System Dr. Sami Zaqout The circulatory system Circulatory system Blood vascular systems Lymphatic vascular systems Blood vascular systems Blood vascular systems The circulatory system Circulatory
The Circulatory System Dr. Sami Zaqout The circulatory system Circulatory system Blood vascular systems Lymphatic vascular systems Blood vascular systems Blood vascular systems The circulatory system Circulatory
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp , , , I. Major Functions of the Circulatory System
 P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
Six main classes of blood vessels (on handout) Wall structure of arteries and veins (on handout) Comparison: Arteries vs. Veins (on handout)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
CVS HISTOLOGY. Dr. Nabil Khouri.
 CVS HISTOLOGY Dr. Nabil Khouri http://anatomy.kmu.edu.tw/blockhis/block3/slides/block4_24.html The Heart Wall Contract as a single unit Cardiac Muscle Simultaneous contraction due to depolarizing at the
CVS HISTOLOGY Dr. Nabil Khouri http://anatomy.kmu.edu.tw/blockhis/block3/slides/block4_24.html The Heart Wall Contract as a single unit Cardiac Muscle Simultaneous contraction due to depolarizing at the
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Lab Activity 25. Blood Vessels & Circulation. Portland Community College BI 232
 Lab Activity 25 Blood Vessels & Circulation Portland Community College BI 232 Artery and Vein Histology Walls have 3 layers: Tunica intima Tunica media Tunica externa 2 Tunica Intima Is the innermost layer
Lab Activity 25 Blood Vessels & Circulation Portland Community College BI 232 Artery and Vein Histology Walls have 3 layers: Tunica intima Tunica media Tunica externa 2 Tunica Intima Is the innermost layer
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
The Cardiovascular and Lymphatic Systems
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 12 The Cardiovascular and Lymphatic Systems Lecture Presentation Anne Gasc Hawaii Pacific University and
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 12 The Cardiovascular and Lymphatic Systems Lecture Presentation Anne Gasc Hawaii Pacific University and
Function: Transportation of. Oxygen Nutrients Waste Hormones gases
 Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
Cardiovascular system
 Cardiovascular system L-4 Blood pressure & special circulation Dr Than Kyaw 27 February 2012 Blood Pressure (BP) Pressure generation and flow Blood is under pressure within its closed system. Pressure
Cardiovascular system L-4 Blood pressure & special circulation Dr Than Kyaw 27 February 2012 Blood Pressure (BP) Pressure generation and flow Blood is under pressure within its closed system. Pressure
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Circulation. Sinoatrial (SA) Node. Atrioventricular (AV) Node. Cardiac Conduction System. Cardiac Conduction System. Linked to the nervous system
 Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Extra notes for lab- 1 histology. Slide 1 : cross section in the elastic artery ( aortic arch, ascending aorta, descending aorta )
 Extra notes for lab- 1 histology Slide 1 : cross section in the elastic artery ( aortic arch, ascending aorta, descending aorta ) - twin of ascending aorta is the pulmonary trunk. Ascending aorta represents
Extra notes for lab- 1 histology Slide 1 : cross section in the elastic artery ( aortic arch, ascending aorta, descending aorta ) - twin of ascending aorta is the pulmonary trunk. Ascending aorta represents
Ch. 12 The Circulatory System. The heart. The heart is a double pump. A quick note on arteries vs. veins. = the muscular pump of the CV system
 Ch. 12 The Circulatory System The heart A.k.a. the cardiovascular system Blood was discussed in Ch. 11 Focus of Ch. 12: heart and blood vessels = the muscular pump of the CV system ~ 100,000 heartbeats/day!
Ch. 12 The Circulatory System The heart A.k.a. the cardiovascular system Blood was discussed in Ch. 11 Focus of Ch. 12: heart and blood vessels = the muscular pump of the CV system ~ 100,000 heartbeats/day!
Microcirculation and Edema- L1 L2
 Microcirculation and Edema- L1 L2 Faisal I. Mohammed MD, PhD. University of Jordan 1 Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchanged
Microcirculation and Edema- L1 L2 Faisal I. Mohammed MD, PhD. University of Jordan 1 Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchanged
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
